-
 Soft Tissue Scaffolds in Breast Reconstruction: Evolution from Acellular Dermal Matrices to Synthetic Polymers
Soft Tissue Scaffolds in Breast Reconstruction: Evolution from Acellular Dermal Matrices to Synthetic Polymers -
 Preclinical Rheumatoid Arthritis: Pathogenesis, Risk Stratification, and Therapeutic Interception
Preclinical Rheumatoid Arthritis: Pathogenesis, Risk Stratification, and Therapeutic Interception -
 Cardiac Involvement in Emery–Dreifuss Muscular Dystrophy, from Arrhythmias to Heart Failure and Sudden Death: A Contemporary Review
Cardiac Involvement in Emery–Dreifuss Muscular Dystrophy, from Arrhythmias to Heart Failure and Sudden Death: A Contemporary Review -
 Adherence to CPAP in Randomized Controlled Trials in Obstructive Sleep Apnoea—A Meta-Analysis and Investigation of Predictors
Adherence to CPAP in Randomized Controlled Trials in Obstructive Sleep Apnoea—A Meta-Analysis and Investigation of Predictors -
 Navigating the Hemostatic Balance: Anticoagulation and Antiplatelet Therapy in Patients with Thrombocytopenia
Navigating the Hemostatic Balance: Anticoagulation and Antiplatelet Therapy in Patients with Thrombocytopenia
Journal Description
Journal of Clinical Medicine
Journal of Clinical Medicine
is an international, peer-reviewed, open access journal of clinical medicine, published semimonthly online by MDPI. The International Bone Research Association (IBRA), Spanish Society of Hematology and Hemotherapy (SEHH), Japan Association for Clinical Engineers (JACE), European Independent Foundation in Angiology/ Vascular Medicine (VAS) and others are all affiliated with JCM, and their members receive a discount on article processing charges.
- Open Access— free for readers, with article processing charges (APC) paid by authors or their institutions.
- High Visibility: indexed within Scopus, SCIE (Web of Science), PubMed, PMC, Embase, CAPlus / SciFinder, and other databases.
- Journal Rank: JCR - Q1 (Medicine, General and Internal) / CiteScore - Q1 (General Medicine)
- Rapid Publication: manuscripts are peer-reviewed and a first decision is provided to authors approximately 18.5 days after submission; acceptance to publication is undertaken in 2.7 days (median values for papers published in this journal in the second half of 2025).
- Recognition of Reviewers: reviewers who provide timely, thorough peer-review reports receive vouchers entitling them to a discount on the APC of their next publication in any MDPI journal, in appreciation of the work done.
- Companion journals for JCM include: Epidemiologia, Transplantology, Uro, Sinusitis, Rheumato, Journal of Clinical & Translational Ophthalmology, Journal of Vascular Diseases, Osteology, Complications, Therapeutics, Sclerosis, Pharmacoepidemiology, Journal of CardioRenal Medicine and Rare Diseases and Therapeutics.
- Journal Clusters of Hematology: Hemato, Hematology Reports, Thalassemia Reports and Journal of Clinical Medicine.
Impact Factor:
2.9 (2024);
5-Year Impact Factor:
3.3 (2024)
Latest Articles
Vasoproliferative Retinal Tumor with Hemangioblastoma-Like Features: Evaluation with von Wilebrand Factor
J. Clin. Med. 2026, 15(12), 4440; https://doi.org/10.3390/jcm15124440 (registering DOI) - 8 Jun 2026
Abstract
Objectives: To investigate the clinicopathologic characteristics and molecular biomarkers of atypical vasoproliferative retinal tumor (VPRT) with hemangioblastoma-like histopathologic features and concomitant von Willebrand factor (VWF) abnormalities. Methods: A 48-year-old woman undergoing phacoemulsification and 25-gauge pars plana vitrectomy with tumor resection was
[...] Read more.
Objectives: To investigate the clinicopathologic characteristics and molecular biomarkers of atypical vasoproliferative retinal tumor (VPRT) with hemangioblastoma-like histopathologic features and concomitant von Willebrand factor (VWF) abnormalities. Methods: A 48-year-old woman undergoing phacoemulsification and 25-gauge pars plana vitrectomy with tumor resection was evaluated. Histopathological findings and immunohistochemical study of the resected tumor were performed using CD34, α-smooth muscle actin (αSMA), and glial fibrillary acidic protein (GFAP) markers. Preoperative plasma and intraoperative vitreous fluid VWF antigen levels, as well as ristocetin cofactor activity, were quantified using latex immunoturbidimetry. Results: Ultra-widefield imaging and angiography demonstrated a peripheral retinal tumor with intense vascular leakage and surrounding capillary nonperfusion. Histopathology showed hyalinized vascular components supportive of VPRT, along with abundant CD34/α-SMA-positive microvessels and scant GFAP-positive glial cells. Notably, numerous foamy vacuolated poorly differentiated cells suggested mixed hemangioblastoma-like features. Preoperative plasma VWF antigen (182.6%) and ristocetin cofactor activity (147.7%) were elevated, and vitreous VWF antigen was successfully detected at a low but distinct level (7.7%).and suggests that VWF abnormalities in the plasma and vitreous may reflect endothelial activation and/or blood–retinal barrier disruption in a subset of vascularized retinal tumors. Conclusions: Our findings demonstrate that VPRT may exhibit mixed clinicopathologic features, including hemangioblastoma-like components, which underscores the necessity of immunohistochemical assessment for definitive diagnosis. Furthermore, the quantification of VWF abnormalities in the plasma and vitreous suggests that VWF serves as a potential biomarker reflecting endothelial activation and/or blood–retinal barrier disruption in vascularized retinal tumors.
Full article
(This article belongs to the Special Issue New Sights in Retinal Diseases Therapeutics: Innovation and Clinical Practice)
Open AccessArticle
Flow-Controlled Ventilation as a Rescue Strategy in Advanced COVID-19 ARDS: A Retrospective Observational Study
by
Meltem Ceylan Delice and Nilgun Kavrut Ozturk
J. Clin. Med. 2026, 15(12), 4439; https://doi.org/10.3390/jcm15124439 (registering DOI) - 8 Jun 2026
Abstract
Background: Acute respiratory distress syndrome (ARDS), particularly in COVID-19–related severe respiratory failure, remains a major challenge in intensive care. Flow-controlled ventilation (FCV) may improve gas exchange by enabling precise airway pressure control; however, clinical data on its prolonged use in ARDS are limited.
[...] Read more.
Background: Acute respiratory distress syndrome (ARDS), particularly in COVID-19–related severe respiratory failure, remains a major challenge in intensive care. Flow-controlled ventilation (FCV) may improve gas exchange by enabling precise airway pressure control; however, clinical data on its prolonged use in ARDS are limited. Methods: This single-center retrospective observational study included adult patients with moderate to severe ARDS who underwent FCV during invasive mechanical ventilation. FCV was delivered using the Evone® ventilator with the Tritube®. Demographic data, ventilatory settings, and arterial blood gas values were analyzed before and during 48 h of FCV and for 8 h after transition to conventional ventilation. Results: Seven patients with COVID-19–related ARDS were included. Following initiation of FCV, PaO2 increased within the first 8 h (median increase: +24 mmHg), accompanied by a median 38% improvement in the PaO2/FiO2 ratio, which remained above baseline throughout follow-up. Arterial PCO2 progressively declined, with the most pronounced reduction observed within the first 24 h (median decrease: −14 mmHg; approximately 22%). After transition back to conventional ventilation, mild deterioration in gas exchange parameters was observed; however, none returned to baseline values. All patients died during their ICU stay, mainly due to secondary infections and pulmonary embolism. Conclusions: In advanced COVID-19–related ARDS unresponsive to conventional ventilation, prolonged FCV application was technically feasible under controlled ICU conditions and associated with descriptively observed improvements in gas exchange parameters. However, late initiation of FCV did not translate into survival benefit. Prospective studies are required to define the optimal timing and patient selection for FCV. The present findings primarily support the technical feasibility and short-term physiological effects of FCV rather than clinical efficacy.
Full article
(This article belongs to the Section Intensive Care)
Open AccessSystematic Review
Prediction Models and Risk Factors for Steroid Resistance in Children with Nephrotic Syndrome: A Systematic Review and Meta-Analysis
by
Yuanhui Hu, Zehui Zhang, Sha Diao, Yannan Guo, Yangtingting Gao, Zheng Xu, Qilin Peng, Yao Xu, Zhenyan Bo, Linan Zeng, Liang Huang, Jingjing Chen, Yizhun Zhu, Hailong Li and Lingli Zhang
J. Clin. Med. 2026, 15(12), 4438; https://doi.org/10.3390/jcm15124438 (registering DOI) - 8 Jun 2026
Abstract
Background: Steroid resistance indicates poor prognosis in pediatric nephrotic syndrome, but predictive models and risk factors for steroid-resistant nephrotic syndrome (SRNS) remain poorly understood. Methods: We searched PubMed, Embase, Scopus, CNKI, SinoMed, Wanfang, and VIP (inception to 1 March 2025) for studies developing
[...] Read more.
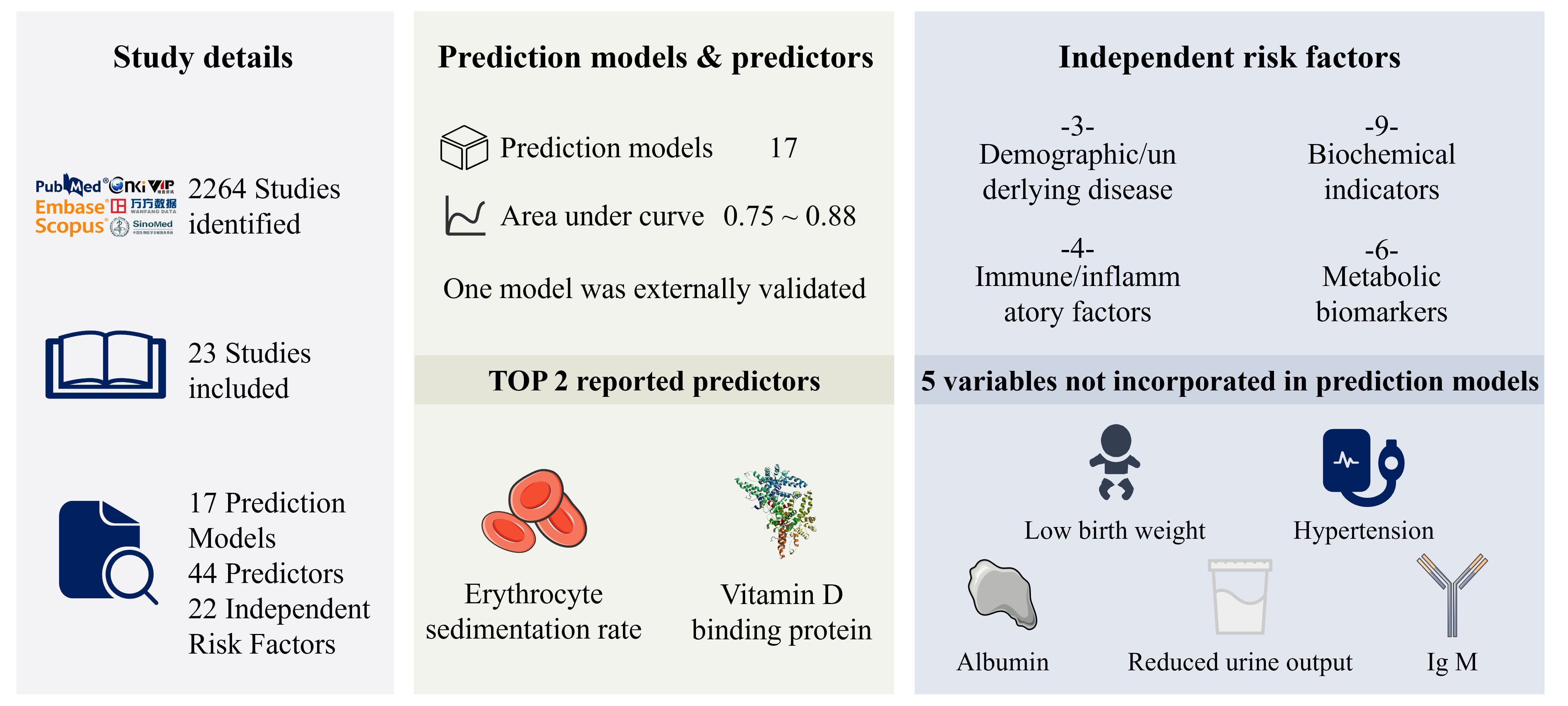
Background: Steroid resistance indicates poor prognosis in pediatric nephrotic syndrome, but predictive models and risk factors for steroid-resistant nephrotic syndrome (SRNS) remain poorly understood. Methods: We searched PubMed, Embase, Scopus, CNKI, SinoMed, Wanfang, and VIP (inception to 1 March 2025) for studies developing SRNS prediction models or identifying risk factors. Odds ratios and AUC were pooled using random-effects meta-analysis. Risk of bias was assessed with PROBAST and Newcastle-Ottawa Scale. Results: Out of 2264 studies, 23 were included. Prediction models were mainly developed using logistic regression (16/17, 94.1%). The most frequently reported predictors included erythrocyte sedimentation rate and vitamin D binding protein. The reported AUC ranged from 0.75 to 0.88. Only one model had undergone external validation with an accuracy of 0.94. A total of 22 independent risk factors were identified, five of which—low birth weight, decreased urine output, hypertension, serum albumin, and serum IgM—were not in existing models. In total, 76% of model studies and 26% of risk factor analyses were at high or moderate risk of bias. Conclusions: Existing SRNS prediction models reported apparent discrimination but had a high risk of bias and very limited external validation, which substantially restricts their current clinical applicability. Several relevant risk factors remain unincorporated. Future research should prioritize rigorous model development and multi-center external validation.
Full article
(This article belongs to the Section Clinical Pediatrics)
►▼
Show Figures
Graphical abstract
Open AccessArticle
Clinical and Perioperative Determinants of Postoperative Pneumonia After Craniotomy for Tumor Resection
by
Anatoli Pinchuk, Nikolay Tonchev, Anna Schaufler, Claudia A. Dumitru, Belal Neyazi, Klaus-Peter Stein, I. Erol Sandalcioglu and Ali Rashidi
J. Clin. Med. 2026, 15(12), 4437; https://doi.org/10.3390/jcm15124437 (registering DOI) - 8 Jun 2026
Abstract
Background/Objectives: Postoperative pneumonia is a common complication in surgical patients. Despite its clinical significance, there is limited evidence regarding its occurrence following intracranial tumor resection, the most common procedure in neurosurgery. The objective of this study is to determine the incidence of postoperative
[...] Read more.
Background/Objectives: Postoperative pneumonia is a common complication in surgical patients. Despite its clinical significance, there is limited evidence regarding its occurrence following intracranial tumor resection, the most common procedure in neurosurgery. The objective of this study is to determine the incidence of postoperative pneumonia, to examine its association with length of hospital stay, and to identify potential risk factors. Methods: A retrospective cohort study was conducted on 1481 patients who underwent intracranial tumor resection in our department over a ten-year period, excluding the influence of anticoagulant or antiplatelet medications. Results: Of the 1481 patients included in this study, postoperative pneumonia occurred in 1.48% of cases. Smoking status (p = 0.014) and prolonged hospital stay (p = 0.011) emerged as significant risk factors in the univariate analysis for postoperative pneumonia in patients undergoing brain tumor resection. In contrast, demographic factors (age, sex, body mass index), pre-existing comorbidities (hypertension, diabetes, cardiovascular disease, chronic inflammatory conditions), and laboratory parameters did not show significant associations with the development of postoperative pulmonary infection. Conclusions: This study identified pre- and postoperative risk factors associated with pneumonia following craniotomy for intracranial tumors. These findings may provide a valuable framework for pre- und postoperative risk assessment and guide strategies to mitigate the occurrence of postoperative pneumonia.
Full article
(This article belongs to the Topic Innovations in Brain Tumor Surgery: Techniques and Outcomes)
►▼
Show Figures
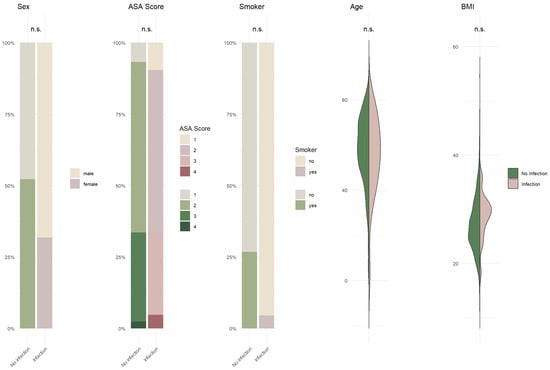
Figure 1
Open AccessArticle
Complementary Error Patterns Between Human Evaluators and GPT-4o in Video-Based Cardiopulmonary Resuscitation Skills Assessment: Implications for Artificial Intelligence-Assisted Second Reading
by
Hye Ji Park, Daun Choi and Choung Ah Lee
J. Clin. Med. 2026, 15(12), 4436; https://doi.org/10.3390/jcm15124436 (registering DOI) - 8 Jun 2026
Abstract
Background/Objectives: Cardiopulmonary resuscitation (CPR) skill assessments are susceptible to evaluator subjectivity, cognitive fatigue, and observational limitations. Although recent advances in multimodal artificial intelligence have increased the possibility of automated video-based assessment, its validity for clinical skill evaluation remains insufficiently examined. Methods: In
[...] Read more.
Background/Objectives: Cardiopulmonary resuscitation (CPR) skill assessments are susceptible to evaluator subjectivity, cognitive fatigue, and observational limitations. Although recent advances in multimodal artificial intelligence have increased the possibility of automated video-based assessment, its validity for clinical skill evaluation remains insufficiently examined. Methods: In this cross-sectional study, we enrolled 130 laypersons who underwent Basic Life Support training and skill testing. Twenty recordings were used for prompt development and 110 recordings were analyzed. Expert evaluators and GPT-4o independently assessed participants’ skills using a 12-item checklist. The manikin sensor data were the reference standard for the four chest compression metrics. Agreement was evaluated using Gwet’s agreement coefficient 1 (AC1) and intraclass correlation coefficient (2,1). Diagnostic accuracy, sensitivity, and specificity were compared using McNemar’s test. Results: Procedural items such as confirming cardiac arrest, calling 119, and requesting an automated external defibrillator showed a near-perfect agreement between experts and GPT-4o (AC1 > 0.8). However, the agreement was poor for the compression depth (AC1 = 0.374) and full chest recoil (AC1 = 0.355). Experts demonstrated high sensitivity (77.8–84.3%) but low specificity (24.6–47.8%), whereas GPT-4o showed low sensitivity (35.6–40.6%) but high specificity (69.2–76.1%). Conclusions: GPT-4o cannot serve as a standalone evaluator because of its inherent limitations in inferring three-dimensional spatial information from two-dimensional videos. However, its high agreement on procedural items and complementary error patterns with that of human evaluators on compression metrics suggests its potential as a decision support tool to mitigate expert leniency bias in CPR education.
Full article
(This article belongs to the Special Issue Novel Technologies to Assist Emergency Medical Care)
Open AccessArticle
An Innovative Dendrimer-Based Retinol Delivery System for Xerosis Care: Stability, Tolerance, and Sustained Hydration
by
Hafid Belhadj-Tahar and Lamri Naidja
J. Clin. Med. 2026, 15(12), 4435; https://doi.org/10.3390/jcm15124435 (registering DOI) - 8 Jun 2026
Abstract
Background: Retinol is a mainstay of dermatological care due to its central role in epidermal differentiation, skin barrier repair, and tissue regeneration. However, its clinical use is limited by poor physicochemical stability, rapid photodegradation, and frequent skin intolerance, particularly in individuals with impaired
[...] Read more.
Background: Retinol is a mainstay of dermatological care due to its central role in epidermal differentiation, skin barrier repair, and tissue regeneration. However, its clinical use is limited by poor physicochemical stability, rapid photodegradation, and frequent skin intolerance, particularly in individuals with impaired skin barrier function. Supramolecular biovectorization strategies could overcome these limitations. Objectives: This study aimed to evaluate the impact of third-generation dendritic poly-L-lysine (PLL_G3; 22 kDa, ~7 nm) on retinol stability, skin tolerance, and skin functional performance. Methods: A supramolecular retinol-poly-L-lysine complex was characterized in terms of encapsulation efficiency and physicochemical stability using HPLC and UV spectroscopy under oxidative, thermal, and photochemical stress. The stability of the formulation was evaluated as hydrophilic emulsion over a three-month period. Skin functional efficacy was evaluated by corneometric analysis of stratum corneum hydration after topical application, as well as by clinical assessment of tolerance and efficacy after repeated daily use over 28 days in subjects presenting xerosis, defined as dry to very dry skin. Results: Retinol remained structurally intact in the PLL_G3 matrix, confirming a reversible, non-covalent encapsulation mechanism. The formulation exhibited high physicochemical stability, with only minimal changes after prolonged UV exposure. Corneometric measurements showed a rapid and sustained increase in skin hydration, reaching +61.5% two hours after application. After 28 days of repeated use, the formulation was well tolerated, with no signs of irritation or sensitization, and demonstrated significant improvements in skin dryness, suppleness, and comfort. Conclusions: PLL_G3-based supramolecular vectorization significantly improves stability, tolerance, and functional hydration of the skin by retinol. By enabling controlled release while preserving the integrity of the epidermal barrier, poly-L-lysine dendrimers represent a clinically relevant strategy for safer and more effective topical use of retinol, particularly on sensitive, xerotic, inflammatory, and photoaged skin.
Full article
(This article belongs to the Special Issue Emerging Therapies: Clinical Trials and Insights in Psoriasis)
Open AccessArticle
Influence of Ongoing Antibiotic Therapy on the Detection of Pathogenic Microorganisms Using Metagenomic Next-Generation Sequencing and Blood Culture in ICU Patients
by
Torsten H. Schroeder, Mamoun Eliwi Alsaffan, Heiner Stäudle and Albion Dervishi
J. Clin. Med. 2026, 15(12), 4434; https://doi.org/10.3390/jcm15124434 (registering DOI) - 8 Jun 2026
Abstract
Background: Blood cultures often yield negative results in critically ill patients, particularly after antimicrobial therapy has started. Plasma metagenomic next-generation sequencing enables culture-independent pathogen detection, but its diagnostic performance relative to blood cultures, especially under ongoing antibiotic exposure in ICU populations, remains unclear.
[...] Read more.
Background: Blood cultures often yield negative results in critically ill patients, particularly after antimicrobial therapy has started. Plasma metagenomic next-generation sequencing enables culture-independent pathogen detection, but its diagnostic performance relative to blood cultures, especially under ongoing antibiotic exposure in ICU populations, remains unclear. Methods: In this retrospective single-center study, we analyzed adult ICU patients who underwent plasma metagenomic next-generation sequencing testing with paired contemporaneous blood culture between March 2023 and September 2024. Patients were classified according to antibiotic exposure at the time of sampling, and the diagnostic yield and performance of metagenomic next-generation sequencing and blood culture were compared overall and stratified by duration of antibiotic exposure. Results: A total of 393 paired metagenomic next-generation sequencing-blood culture samples from 302 ICU patients were analyzed. Blood culture positivity was significantly lower in patients receiving antibiotics at the time of sampling (10.4% vs. 30.4%), whereas metagenomic next-generation sequencing positivity for bacteria remained stable (52.6% vs. 50.8%). With increasing antibiotic exposure, blood culture yield declined sharply, while metagenomic next-generation sequencing detection showed minimal variation. Overall, the concordance of metagenomic next-generation sequencing compared with blood culture as a comparator was 75.3%, with a negative predictive value of 88.0%. Across all subgroups, metagenomic next-generation sequencing demonstrated a higher diagnostic yield than blood culture, with the greatest relative advantage in antibiotic-treated patients. Conclusions: In critically ill patients receiving antimicrobial therapy, blood culture diagnostic yield is markedly reduced, whereas plasma metagenomic next-generation sequencing maintains pathogen detection across varying durations of antibiotic exposure. Metagenomic next-generation sequencing represents a valuable complementary diagnostic tool alongside blood cultures in pretreated ICU patients.
Full article
(This article belongs to the Special Issue Clinical Management and Challenges of Sepsis and Septic Shock)
Open AccessArticle
Erectile Function Before and After Elective Inguinal Hernia Repair: A Paired IIEF-5 Study Comparing Laparoscopic and Open Techniques
by
Volkan Sayur, Mehmet Avcı, Erkan Güler, Berk Can Karabağ and Taylan Özgür Sezer
J. Clin. Med. 2026, 15(12), 4433; https://doi.org/10.3390/jcm15124433 (registering DOI) - 8 Jun 2026
Abstract
Objective: This study aimed to evaluate changes in erectile function, assessed using the International Index of Erectile Function-5 (IIEF-5), in male patients undergoing elective inguinal hernia repair and to compare outcomes according to surgical technique and hernia characteristics. Materials and Methods: A total
[...] Read more.
Objective: This study aimed to evaluate changes in erectile function, assessed using the International Index of Erectile Function-5 (IIEF-5), in male patients undergoing elective inguinal hernia repair and to compare outcomes according to surgical technique and hernia characteristics. Materials and Methods: A total of 126 male patients who underwent elective unilateral inguinal hernia repair using either laparoscopic transabdominal preperitoneal/totally extraperitoneal repair or open Lichtenstein repair were included. Patients with severe comorbid conditions that could affect erectile function or surgical outcomes were excluded. Preoperative erectile function was assessed using the IIEF-5 questionnaire during routine preoperative evaluation within one month before surgery, and postoperative assessment was performed using the same questionnaire at the sixth postoperative month. Routine tacker fixation was used in all laparoscopic procedures. Subgroup analyses were performed according to the presence of scrotal hernia, and independent predictors of postoperative change in IIEF-5 score were evaluated using multivariate linear regression analysis. Results: Laparoscopic repair was performed in 59 patients (46.8%), whereas 67 patients (53.2%) underwent open Lichtenstein repair. In the overall cohort, the mean IIEF-5 score increased from 22.85 ± 3.12 preoperatively to 23.35 ± 1.98 at the sixth postoperative month (p < 0.05). No significant difference in IIEF-5 score change was observed between laparoscopic and open repair groups (p > 0.05). Although the overall postoperative increase in IIEF-5 score was statistically significant, its magnitude was small. Patients with scrotal hernia showed a greater postoperative IIEF-5 score increase compared with those without scrotal hernia (p < 0.001), but this subgroup was small. In multivariate analysis, scrotal hernia status (β = +2.41; p = 0.041) and lower baseline IIEF-5 score (β = −0.425; p = 0.001) were associated with greater postoperative score increase. Conclusions: In this retrospective paired comparative study, erectile function was evaluated in male patients undergoing elective inguinal hernia repair using paired preoperative and sixth-month postoperative IIEF-5 scores. Erectile function appeared to be largely preserved after surgery, and the overall postoperative increase in IIEF-5 score was statistically significant but small in magnitude. No significant difference in IIEF-5 score change was observed between laparoscopic and open Lichtenstein repair. Scrotal hernia status and lower baseline IIEF-5 scores were associated with greater postoperative IIEF-5 score increase; however, this subgroup finding should be interpreted as exploratory and requires confirmation in larger prospective cohorts. These findings may help provide more realistic expectations during preoperative counseling, while avoiding causal interpretation.
Full article
(This article belongs to the Section General Surgery)
Open AccessArticle
Frequency of Acute Adverse Transfusion Reactions at King Saud Medical City, Riyadh, Saudi Arabia
by
Ibrahim Mansour Aboshaya, Muhammed Raihan Sajid, Rimah Abdullah Saleem, Salman Aldosari and Hibba Siraj
J. Clin. Med. 2026, 15(12), 4432; https://doi.org/10.3390/jcm15124432 (registering DOI) - 8 Jun 2026
Abstract
Background: Blood transfusion is a life-saving intervention but is associated with adverse reactions in a subset of recipients. An acute transfusion reaction (ATR) is defined as any unfavorable response occurring within 24 h of blood component administration. This retrospective observational study aimed to
[...] Read more.
Background: Blood transfusion is a life-saving intervention but is associated with adverse reactions in a subset of recipients. An acute transfusion reaction (ATR) is defined as any unfavorable response occurring within 24 h of blood component administration. This retrospective observational study aimed to determine the frequency and characteristics of ATRs at King Saud Medical City (KSMC), Riyadh, Saudi Arabia. Methods: We conducted a retrospective study using data from the Transfusion Medicine Laboratory (TML) at KSMC between January 2019 and December 2023. Demographic, clinical, and laboratory data from 238 confirmed ATR records were analyzed using SPSS v21.0. Chi-square, Mann–Whitney U, and risk ratio analyses were performed; p < 0.05 was considered statistically significant. Results: Among 238 patients (59.2% female; mean age 33.7 ± 18.5 years), allergic reactions were the most frequent ATR (70.2%, n = 167), followed by febrile non-hemolytic transfusion reactions (FNHTRs); (24.4%, n = 58). Packed red blood cell (PRBC) transfusion was the most commonly implicated product (82.4%; n = 196; p < 0.001). Fever, rash, itching, and chills were significantly associated with specific reaction subtypes (p < 0.001). The pattern of post-transfusion workup differed significantly across reaction types (p < 0.001). Age, gender, ward distribution, and reaction timing were not significant predictors of ATR occurrence. Conclusions: Allergic reactions are the predominant ATR form at KSMC. Demographic variables are not reliable predictors of ATR. Strengthening hemovigilance systems and clinician education is recommended to improve transfusion safety.
Full article
(This article belongs to the Section Hematology)
Open AccessArticle
An Open Comparative Study on the Effectiveness of Customized and Non-Customized Sound Therapy for Tinnitus Patients
by
Hongbo Xie, Yuehong Liu, Siyi Yang, Tianyi Ni, Jian Ruan, Yun Jiang, Ziyuan Lin, Lingling Zhou, Songpo He and Zhao Han
J. Clin. Med. 2026, 15(12), 4431; https://doi.org/10.3390/jcm15124431 (registering DOI) - 8 Jun 2026
Abstract
Objectives: Sound therapy is a common treatment for tinnitus. This study aims to explore the efficacy of non-customized and customized sound therapy for subjective tinnitus. Treatment progress was assessed by comparing changes in monthly scales. The main scales used are the Tinnitus Handicap
[...] Read more.
Objectives: Sound therapy is a common treatment for tinnitus. This study aims to explore the efficacy of non-customized and customized sound therapy for subjective tinnitus. Treatment progress was assessed by comparing changes in monthly scales. The main scales used are the Tinnitus Handicap Inventory, Hospital Anxiety and Depression Scale, and Loudness Visual Analogue Scale. Methods: The subjects of this study were patients with tinnitus who visited outpatient from 2024 to 2025. Total of 732 patients were included (customized group, n = 653; non-customized group, n = 79). Customized sound therapy is tailored to patient’s specific tinnitus condition, while non-customized sound consists of soothing natural sounds. The daily treatment duration was 2 h. Treatment assignment was not randomized; patients were free to choose between customized and non-customized sound therapy, which may have introduced a preference bias. Results: The study found that, in both groups of patients, regardless of whether they were treated or not, the severity of tinnitus was positively correlated with the level of anxiety (p < 0.01)/depression (p < 0.01) and the loudness of tinnitus (p < 0.01). Patients with severe tinnitus were more likely to choose customized sound therapy (p < 0.01). THI score for the non-customized group showed a downward trend at 1 and 3 months after treatment (p < 0.01 at 1 and 3months). HADS-A score also decreased 1 and 3 months after treatment compared to before treatment (p < 0.05 at 1 and 3months). THI scores for the customized group showed a downward trend at 1, 3, 6, 9, and 12 months after treatment (p < 0.001 at 1 and 3 & 6 and 9 & 12 months). HADS-A/D scores decreased at 1, 3, 6, 9 and 12 months after treatment (p < 0.01 at 1 & 3 & 6 and 9 & 12months). The efficacy of the customized group was greater than that of the non-customized group 1 month after treatment (χ2 = 6.39, p = 0.011). Conclusions: Both sound therapies can alleviate tinnitus severity and reduce anxiety in the short term. Customized sound therapy is superior to non-customized therapy in terms of short-term efficacy. Additionally, customized sound therapy is more effective than non-customized therapy in alleviating tinnitus severity and managing anxiety and depression over a longer period. Therefore, customized sound therapy may be a more effective treatment option for subjective tinnitus. However, it should be emphasized that this was an open study in which patients freely chose between the two therapies, which may have introduced bias. Therefore, these findings are not as well founded as those from a randomized controlled trial, and future RCTs are warranted to verify the observed benefits.
Full article
(This article belongs to the Section Otolaryngology)
Open AccessReview
Update on Obesity and Its Relationship to Atherosclerotic Cardiovascular Disease and Associated Risk Factors
by
Yaser Ahmad, Raj Wasan, Jordan D. Perchik and Navin C. Nanda
J. Clin. Med. 2026, 15(12), 4430; https://doi.org/10.3390/jcm15124430 (registering DOI) - 8 Jun 2026
Abstract
Background/Objectives: Obesity is a multifactorial chronic condition characterized by the accumulation of excess adiposity and complex interplay between intrinsic and extrinsic factors. It is an increasingly common condition, closely implicated with the incidence and progression of cardiovascular disease and its risk factors.
[...] Read more.
Background/Objectives: Obesity is a multifactorial chronic condition characterized by the accumulation of excess adiposity and complex interplay between intrinsic and extrinsic factors. It is an increasingly common condition, closely implicated with the incidence and progression of cardiovascular disease and its risk factors. This narrative review synthesizes and summarizes recent evidence on obesity, with a focus on the diagnosis of obesity, an exploration of both visceral and subcutaneous adipose tissue, available interventions for obesity ranging from dietary modifications to novel anti-obesity medications, and key associations with obesity and cardiovascular diseases. This review is distinct in its integrated focus on obesity definition and diagnosis, imaging modalities, the latest non-pharmacologic and pharmacologic interventions, and also the interplay between obesity and certain cardiovascular conditions as well as their risk factors. Results: The diagnosis of obesity has been evolving with the incorporation of anthropometric measurements and imaging modalities rather than simply the body mass index. There is a wide array of contributors to obesity including genetic factors, behavior, hormonal regulators, the brain–gut axis, and psychosocial stressors. Anti-obesity medications have been evolving rapidly, with current emphasis on glucagon-like peptide 1 receptor agonists. Obesity is closely implicated in cardiovascular conditions such as atherosclerotic disease, heart failure, atrial fibrillation, and hypertension as well as related risk factors such as diabetes mellitus, chronic kidney disease and sleep apnea. Conclusions: Obesity is a widely prevalent, chronic, and complex disease. The use of a variety of anthropometric measurements can help risk-stratify individuals. Imaging techniques are also helpful in evaluating body fat. Evaluating individuals from a holistic perspective is imperative to appreciate the various contributors to obesity. There are a variety of interventions available for obesity management including lifestyle interventions, bariatric surgery, and pharmacologic therapy. Notably, obesity is closely tied with cardiovascular diseases and recent pharmacologic anti-obesity agents may mitigate cardiovascular risk.
Full article
(This article belongs to the Section Cardiovascular Medicine)
►▼
Show Figures
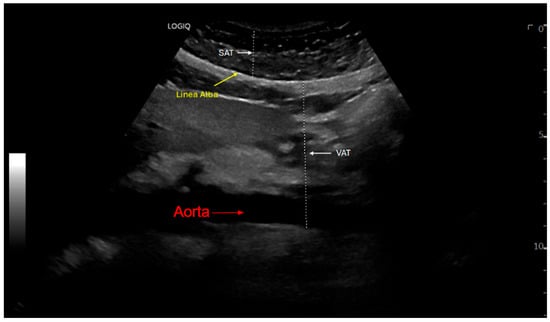
Figure 1
Open AccessArticle
Association of Pretreatment Serum Albumin and Systemic Inflammatory Markers with Pathologic Response to Neoadjuvant Chemotherapy in Breast Cancer
by
Selçuk Cin, Merve Tokocin, Özgecan Gündoğar, Merve Cin, Ali Muhammedoğlu, Murat Yüce and Ahu Senem Demiröz
J. Clin. Med. 2026, 15(12), 4429; https://doi.org/10.3390/jcm15124429 (registering DOI) - 8 Jun 2026
Abstract
Background: Pathological complete response (pCR) to neoadjuvant chemotherapy (NACT) in breast cancer is influenced by multiple tumor- and host-related factors, and readily available pretreatment biomarkers of response are still limited. This study aimed to evaluate the association between pretreatment systemic inflammatory and nutritional
[...] Read more.
Background: Pathological complete response (pCR) to neoadjuvant chemotherapy (NACT) in breast cancer is influenced by multiple tumor- and host-related factors, and readily available pretreatment biomarkers of response are still limited. This study aimed to evaluate the association between pretreatment systemic inflammatory and nutritional parameters and pCR assessed by the Miller–Payne grading system, with a specific focus on the independent predictive value of pretreatment serum albumin compared with established inflammatory ratios. Methods: A total of 226 patients with breast carcinoma who received NACT between May 2017 and September 2023 were retrospectively evaluated. Pretreatment laboratory parameters—including neutrophil-to-lymphocyte ratio (NLR), platelet-to-lymphocyte ratio (PLR), C-reactive protein (CRP), serum albumin, and the CRP/albumin ratio (CAR)—were recorded. Pathological response was assessed using the Miller–Payne grading system by two breast pathologists blinded to laboratory data. Univariable and multivariable logistic regression and receiver operating characteristic (ROC) curve analyses were performed, complemented by bootstrap validation of the optimal cut-off, a sensitivity analysis using the contemporary ypT0/is ypN0 definition of pCR, and a subgroup analysis by molecular subtype. Results: pCR was observed in 41 patients (18.1%). Pretreatment serum albumin levels were significantly lower in responders than in non-responders (p = 0.027), whereas NLR, PLR, CRP, and CAR were not significantly associated with response. In multivariable analysis, pretreatment serum albumin, Ki-67, and HER2 status emerged as independent predictors of pCR. ROC analysis demonstrated moderate discriminatory ability for albumin (AUC = 0.64); the optimal cut-off was 4.22 g/dL (bootstrap 95% CI 3.50–4.53 g/dL), with values below this threshold associated with a higher likelihood of pCR. The association between low pretreatment albumin and pCR was particularly pronounced in the triple-negative subgroup (3.30 vs. 4.02 g/dL, p = 0.027). The albumin signal remained significant under the stricter ypT0/is ypN0 definition of pCR in univariable analysis (OR 0.47, p = 0.045). Conclusions: Pretreatment serum albumin, independent of systemic inflammatory ratios, is associated with pCR to NACT in breast cancer and may serve as a candidate biomarker for pretreatment risk stratification, particularly when interpreted alongside established tumor-related predictors such as Ki-67 and HER2 status. The association appears especially relevant in the triple-negative subgroup, suggesting that patients with TNBC and low pretreatment serum albumin may warrant heightened multidisciplinary attention during NACT. Validation in larger, prospective, multicenter cohorts is needed before routine clinical implementation.
Full article
(This article belongs to the Section Oncology)
►▼
Show Figures

Graphical abstract
Open AccessArticle
Beyond the Cornea: Early Changes in Scleral, Iris, and Corneal Parameters After Corneal Collagen Cross-Linking
by
Tunahan Akyol, Osman Parca, Emine Seker Un, Ibrahim Toprak and Gokhan Pekel
J. Clin. Med. 2026, 15(12), 4428; https://doi.org/10.3390/jcm15124428 - 8 Jun 2026
Abstract
Background/Objectives: To evaluate early postoperative changes in scleral and iris thicknesses together with corneal layer thicknesses and tomographic parameters following corneal collagen cross-linking (CXL) in eyes with progressive keratoconus. Methods: This retrospective study included 94 eyes of 94 patients with progressive keratoconus who
[...] Read more.
Background/Objectives: To evaluate early postoperative changes in scleral and iris thicknesses together with corneal layer thicknesses and tomographic parameters following corneal collagen cross-linking (CXL) in eyes with progressive keratoconus. Methods: This retrospective study included 94 eyes of 94 patients with progressive keratoconus who underwent standard epithelium-off CXL using the Dresden protocol. Corneal tomography (Pentacam) and anterior segment optical coherence tomography (AS-OCT) measurements were obtained preoperatively and at the early postoperative follow-up (3 months ± 2 weeks). Thickness measurements of the tear film, corneal epithelium, Bowman layer, stroma, Descemet–endothelium complex, sclera (1–3 mm from the limbus), and iris (1–2 mm from the pupillary margin) were analyzed. Pre- and post-CXL values were compared using paired statistical tests, and effect sizes were calculated. Results: In the early postoperative period, scleral thickness showed a significant increase at all measured distances from the limbus, with medium effect sizes, while iris thickness demonstrated a significant decrease at all measurement points with large effect sizes (p < 0.001). Tear film, epithelial, and stromal thicknesses decreased significantly after CXL, whereas Bowman layer and Descemet–endothelium complex thicknesses remained unchanged. Pachymetric measurements revealed significant thinning at the pupil center, corneal apex, and thinnest point. No significant changes were observed in Kmax or anterior chamber depth, indicating stabilization rather than progression in the early postoperative period. Conclusions: Corneal collagen cross-linking was associated with measurable early structural changes in corneal layers and extra-corneal anterior segment tissues during the postoperative period. The observed increase in scleral thickness and decrease in iris thickness suggest that structural alterations may occur in extra-corneal anterior segment tissues following CXL. These findings support the concept that CXL influences anterior segment biomechanics in a tissue-specific manner and that extra-corneal parameters may serve as complementary markers for early postoperative assessment.
Full article
(This article belongs to the Special Issue Diagnosis and Management of Corneal Diseases)
►▼
Show Figures

Figure 1
Open AccessArticle
Atrial Fibrillation, Cerebral Small Vessel Disease and Gender Medicine: Focus on Biomarkers and Neuroimaging
by
Francesco Alfano, Martina Berteotti, Francesca Cesari, Anna Maria Gori, Emilia Salvadori, Betti Giusti, Alessia Bertelli, Luca Bicchi, Filippo Fratini, Benedetta Formelli, Eleonora Barucci, Giulia Salti, Enrico Fainardi, Andrea Ginestroni, Stefano Chiti, Anna Poggesi and Rossella Marcucci
J. Clin. Med. 2026, 15(12), 4427; https://doi.org/10.3390/jcm15124427 - 8 Jun 2026
Abstract
Background/Objectives: Atrial fibrillation (AF) is the most common supraventricular arrhythmia and one of the most commonly encountered heart conditions in clinical practice. Emerging evidence suggests a significant role of inflammation, endothelial disfunction and extracellular matrix (ECM) remodeling in the pathogenesis of AF.
[...] Read more.
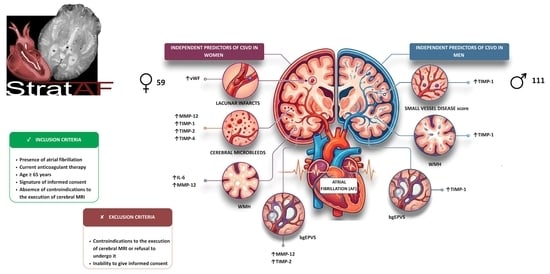
Background/Objectives: Atrial fibrillation (AF) is the most common supraventricular arrhythmia and one of the most commonly encountered heart conditions in clinical practice. Emerging evidence suggests a significant role of inflammation, endothelial disfunction and extracellular matrix (ECM) remodeling in the pathogenesis of AF. Population studies have also suggested an association between AF and cerebral small vessel disease (CSVD), with growing evidence indicating that the burden of certain markers of CSVD is greater in women. However, the association between female sex and CSVD remains poorly understood. The aim of this study was thus to investigate the role of female sex in the association between circulating biomarkers and the presence of CSVD in AF patients undergoing oral anticoagulant therapy. Methods: The Strat-AF study is an observational, prospective, single-center, hospital-based study enrolling elderly patients with AF. Results refer to 170 patients (59 women and 111 men). Recruited patients are evaluated by means of a comprehensive protocol, with clinical, cerebral magnetic resonance imaging (MRI) and circulating biomarker assessments. Results: From a multivariate logistic regression analysis adjusted for multiple confounders, independent predictors were: in women, elevated vWF levels for the presence of lacunar infarcts [OR 3.24 (1.23–8.55), p = 0.018], elevated MMP-12, TIMP-1, TIMP-2, and TIMP-4 levels for the presence of CMBs [OR 7.76 (1.60–37.69), p = 0.021; OR 1.90 (1.02–3.52), p = 0.042; OR 2.46 (1.27–4.80), p = 0.008; and OR 2.36 (1.12–4.95), p = 0.023, respectively], elevated IL-6 and MMP-2 levels for the presence of WMH [OR 10.65 (1.31–86.67), p = 0.027; OR 3.36 (1.23–9.15), p = 0.018, respectively] and elevated MMP-12 and TIMP-2 levels for the presence of bgEPVS [OR 2.57 (1.22–5.93), p = 0.027; OR 2.15 (1.03–4.53), p = 0.043, respectively]; and in men: elevated TIMP-1 levels for the presence of WMH [OR 2.10 (1.08–4.08), p = 0.030], elevated TIMP-1 levels for the presence of bgEPVS [OR 2.20 (1.11–4.38), p = 0.025] and elevated TIMP-1 levels for SVDs positivity [OR 7.25 (2.18–24.15), p = 0.001]. Conclusions: These results from the Strat-AF study demonstrated that a complete biohumoral and instrumental assessment can jointly identify female patients with AF at higher risk of CSVD. These findings pave the way for the implementation of clinical protocols incorporating brain MRI and circulating biomarkers as potential innovative tools for an increasingly refined—and sex-specific—stratification of cardiovascular risk in AF patients undergoing oral anticoagulant therapy.
Full article
(This article belongs to the Section Cardiovascular Medicine)
►▼
Show Figures
Graphical abstract
Open AccessSystematic Review
Underestimation of Intraocular Pressure (IOP) After LASIK and PRK: Systematic Review and Meta-Analysis
by
Stamatios Lampsas, Efthymios Karmiris, George D. Kymionis and Irini Chatziralli
J. Clin. Med. 2026, 15(12), 4426; https://doi.org/10.3390/jcm15124426 - 8 Jun 2026
Abstract
Background/Objectives: Refractive corneal surgery alters corneal biomechanics and thickness, affecting the accuracy of intraocular pressure (IOP) measurements. This systematic review and meta-analysis aimed to quantify the postoperative underestimation of IOP following such procedures. Methods: This systematic review and meta-analysis, conducted based
[...] Read more.
Background/Objectives: Refractive corneal surgery alters corneal biomechanics and thickness, affecting the accuracy of intraocular pressure (IOP) measurements. This systematic review and meta-analysis aimed to quantify the postoperative underestimation of IOP following such procedures. Methods: This systematic review and meta-analysis, conducted based on PRISMA guidelines, evaluated pre- and postoperative IOP changes following LASIK and PRK using GAT, ORA, and CORVIS ST, based on studies identified through PubMed, Scopus, Cochrane Library, and ScienceDirect up to 31 December 2025, with results synthesized using random-effects models and reported as mean differences (MD) with 95% confidence intervals (CI). Results: Of the 1796 articles identified, 54 studies met the inclusion criteria, encompassing a total of 4730 eyes. After LASIK, a statistically significant underestimation of IOP was observed with all methods: GAT (MD: 3.23 mmHg, 95% CI: 2.77–3.69, p < 0.001), ORA (MD: 2.13 mmHg, 95% CI: 1.56–2.70, p < 0.001), and CORVIS ST (MD: 1.39 mmHg, 95% CI: 0.53–2.24, p = 0.001). Similarly, after PRK, a significant reduction in IOP was recorded with GAT (MD: 2.04 mmHg, 95% CI: 1.24–2.84, p < 0.001) and ORA (MD: 2.46 mmHg, 95% CI: 0.62–4.29, p < 0.01), while the difference measured by CORVIS ST was not statistically significant. Conclusions: LASIK and PRK result in systematic underestimation of IOP, most pronounced with GAT and less evident with ORA and CORVIS ST, highlighting the importance of selecting appropriate tonometry methods for accurate monitoring, especially in patients at risk of glaucoma or elevated IOP.
Full article
(This article belongs to the Special Issue Glaucoma: Diagnosis and Management Insights)
►▼
Show Figures
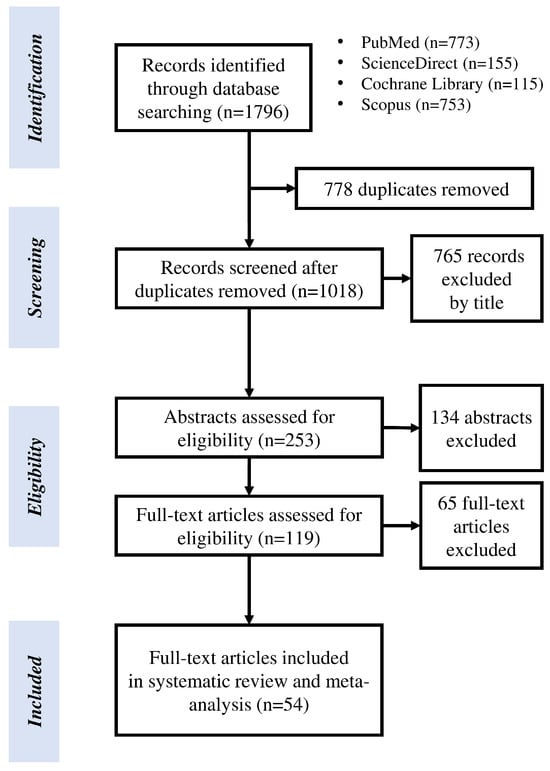
Figure 1
Open AccessReview
Precision Medicine in Non-Hodgkin Lymphoma: Advances in BTK Inhibition, CD30-Directed Antibody–Drug Conjugates, and HDAC-Mediated Epigenetic Therapy with Pirtobrutinib, Brentuximab Vedotin, and Belinostat
by
Piotr Kawczak and Tomasz Bączek
J. Clin. Med. 2026, 15(12), 4425; https://doi.org/10.3390/jcm15124425 (registering DOI) - 8 Jun 2026
Abstract
Non-Hodgkin lymphoma (NHL) encompasses a biologically diverse group of malignancies for which the integration of precision medicine has markedly reshaped therapeutic strategies. Recent advances in molecular profiling, target identification, and drug development have led to the introduction of highly selective agents capable of
[...] Read more.
Non-Hodgkin lymphoma (NHL) encompasses a biologically diverse group of malignancies for which the integration of precision medicine has markedly reshaped therapeutic strategies. Recent advances in molecular profiling, target identification, and drug development have led to the introduction of highly selective agents capable of overcoming resistance mechanisms and improving outcomes in relapsed or refractory disease. This review highlights three targeted therapies—pirtobrutinib, brentuximab vedotin, and belinostat—and their evolving roles in modern NHL management. Pirtobrutinib, a next-generation, non-covalent Bruton tyrosine kinase (BTK) inhibitor, demonstrates preserved activity in patients previously treated with covalent BTK inhibitors (BTKi), addressing a critical unmet need in B-cell lymphomas. Brentuximab vedotin, an antibody–drug conjugate targeting CD30, has significantly improved therapeutic precision by delivering cytotoxic agents directly to lymphoma cells and has become a central component of treatment for CD30-expressing NHL subtypes. Belinostat, a broad-spectrum histone deacetylase (HDAC) inhibitor, offers a mechanistically distinct epigenetic approach, particularly in peripheral T-cell lymphomas (PTCL), where conventional chemotherapy has limited efficacy. Together, these agents exemplify three complementary paradigms of precision oncology in NHL: kinase signaling inhibition, antigen-directed cytotoxic delivery, and epigenetic modulation. This review synthesizes current evidence, clinical trial data, and future perspectives regarding the integration of pirtobrutinib, brentuximab vedotin, and belinostat into evolving treatment paradigms. Cumulatively, these therapies illustrate both the progress and the ongoing challenges of biomarker-driven treatment in NHL, including resistance mechanisms, toxicity management, optimal therapeutic sequencing, and variability in evidence maturity across targeted strategies. While pirtobrutinib and brentuximab vedotin are supported by increasingly robust clinical evidence in selected lymphoma subtypes, the role of belinostat remains constrained by modest response rates and limited randomized data, underscoring the continued need for biomarker refinement and more precisely individualized therapeutic approaches in NHL precision medicine.
Full article
(This article belongs to the Special Issue Therapeutic Advances in Hematological Malignancies: New Breakthroughs and Future Directions)
►▼
Show Figures
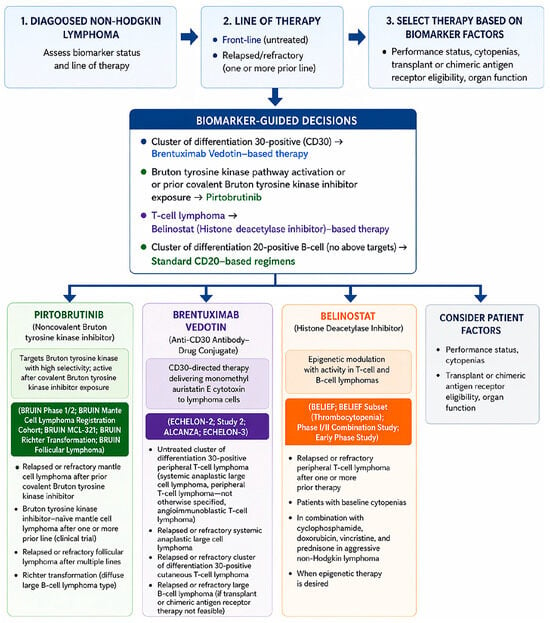
Figure 1
Open AccessArticle
Expanding the Boundaries of Minimally Invasive Cardiac Surgery: Initial Experience with Multivalve Procedures
by
Wojciech Karolak, Aleksandra Stańska, Igor Tomczyk and Andrzej Klapkowski
J. Clin. Med. 2026, 15(12), 4424; https://doi.org/10.3390/jcm15124424 - 8 Jun 2026
Abstract
Background/Objectives: Minimally invasive valve surgery via right minithoracotomy is well established for isolated aortic and mitral procedures, but its application to multivalve operations remains uncommon and clinical data are scarce. We report our initial single-center experience with minimally invasive multivalve surgery—defined as
[...] Read more.
Background/Objectives: Minimally invasive valve surgery via right minithoracotomy is well established for isolated aortic and mitral procedures, but its application to multivalve operations remains uncommon and clinical data are scarce. We report our initial single-center experience with minimally invasive multivalve surgery—defined as a small skin incision without rib spreading or internal mammary artery dissection—in patients with combined aortic and mitral disease. Methods: We retrospectively analyzed 10 consecutive patients who underwent minimally invasive multivalve cardiac surgery at our institution. All operations were performed through a 5–7 cm right minithoracotomy in the third or fourth intercostal space, with femoral cannulation for cardiopulmonary bypass (CPB). Nine patients underwent a double-valve procedure (aortic and mitral) and one a triple-valve procedure (aortic, mitral, and tricuspid). Operative variables, perioperative complications, and early echocardiographic outcomes were assessed. Results: The mean age of patients was 69.8 ± 5.2 years and 60% were female. Mean CPB and aortic cross-clamp times were 197.6 ± 48.3 min and 148.1 ± 34.7 min, respectively. All procedures were completed via the minimally invasive approach, with no conversion to sternotomy and no in-hospital deaths. No rethoracotomies, wound infections, or peripheral vascular complications occurred. Postoperative atrial fibrillation, observed in five patients (50%), was the most common complication. Early echocardiography showed good valve function in nine patients (90%); one had a moderate aortic paravalvular leak managed conservatively. Conclusions: In a center with established experience in single-valve minimally invasive surgery, multivalve procedures can be safely extended to a right minithoracotomy approach, with low perioperative morbidity and no early mortality despite operative times reflecting the early learning curve.
Full article
(This article belongs to the Special Issue Advances in Minimally Invasive Cardiothoracic Surgery: Current Techniques and Future Innovations)
Open AccessArticle
GeriAIGastroNet: AI-Assisted Gastrointestinal Polyp Segmentation and Severity-Based Triage for Tele-Gastroenterology in Underserved Geriatric Populations
by
Masrufa Akter Muni, Mustafizur Rahaman, Saima Tasnim, Mousumi Akter, Sabrina Shamim Moushi and Rakibul Islam
J. Clin. Med. 2026, 15(12), 4423; https://doi.org/10.3390/jcm15124423 - 8 Jun 2026
Abstract
Background/Objectives: Colorectal cancer is a leading cause of cancer-related mortality worldwide, and early detection of gastrointestinal (GI) polyps through endoscopy is critical for improving patient outcomes. However, access to specialist gastroenterology care remains severely limited in Federal Health Professional Shortage Areas (HPSAs), particularly
[...] Read more.
Background/Objectives: Colorectal cancer is a leading cause of cancer-related mortality worldwide, and early detection of gastrointestinal (GI) polyps through endoscopy is critical for improving patient outcomes. However, access to specialist gastroenterology care remains severely limited in Federal Health Professional Shortage Areas (HPSAs), particularly for high-acuity geriatric patients. This study proposes GeriAIGastroNet, a clinically oriented deep learning framework designed to support AI-assisted tele-gastroenterology workflows in resource-limited settings, with the primary objective of enabling AI-powered risk stratification and colonoscopy referral triage for elderly patients who lack on-site gastroenterology access. Methods: The framework integrates an EfficientNet-B4 backbone with multi-scale attention fusion and a geriatric severity-aware classification head to enable accurate GI polyp segmentation and automated clinical risk stratification from endoscopic images. Patients identified as high-risk are referred to colonoscopy-capable centers; such centers typically offer diagnostic colonoscopy with polypectomy capability for smaller and intermediate-complexity polyps, while patients with larger, sessile, or morphologically complex lesions requiring advanced endoscopic resection (e.g., endoscopic mucosal resection or endoscopic submucosal dissection) are further referred to tertiary endoscopy centers with specialized expertise. The model was trained and evaluated on the publicly available HyperKvasir dataset (1000 annotated polyp images). Results: GeriAIGastroNet achieved a classification accuracy of 96.77%, F1-score of 96.90%, Dice coefficient of 89.18%, and Intersection over Union (IoU) of 80.80%, outperforming established baselines, including U-Net, Attention U-Net, TransUNet, and Hybrid CNN-Transformer architectures. The integrated tele-gastroenterology decision support layer enables severity-based patient triage and automated referral triggering. Conclusions: These results demonstrate the potential of AI-powered polyp analysis to strengthen equitable access to GI care by facilitating risk stratification and specialist referral in HPSAs where direct endoscopy is unavailable, making the system deployable in telehealth infrastructures serving underserved elderly populations.
Full article
(This article belongs to the Section Machine Learning and Artificial Intelligence in Clinical Medicine)
►▼
Show Figures

Figure 1
Open AccessSystematic Review
Percutaneous Coronary Intervention Without Sustained Return of Spontaneous Circulation Under Extracorporeal Cardiopulmonary Resuscitation: A Phenotype-Oriented Descriptive Systematic Review
by
Yi-Hsiang Chao, Zhi-Hao Tay and Chong-Chao Hsieh
J. Clin. Med. 2026, 15(12), 4422; https://doi.org/10.3390/jcm15124422 - 7 Jun 2026
Abstract
Background: Percutaneous coronary intervention (PCI) during extracorporeal cardiopulmonary resuscitation (ECPR) before sustained return of spontaneous circulation (ROSC) is increasingly performed, yet most published reports fail to document ROSC status at the time of intervention—leaving this specific clinical phenotype poorly characterized. We aimed to
[...] Read more.
Background: Percutaneous coronary intervention (PCI) during extracorporeal cardiopulmonary resuscitation (ECPR) before sustained return of spontaneous circulation (ROSC) is increasingly performed, yet most published reports fail to document ROSC status at the time of intervention—leaving this specific clinical phenotype poorly characterized. We aimed to clarify this ambiguity by systematically separating studies with explicit no-ROSC documentation from those in which the phenotype is only inferred and to describe selection, feasibility, and outcomes for the resulting cohorts. Methods: PubMed, Embase, and Cochrane CENTRAL were searched on 30 January 2026. Studies were pre-classified as DEFINITE (explicit no-sustained-ROSC documentation at PCI) or PROBABLE (workflow strongly implying no sustained ROSC). The 13 DEFINITE studies served as the primary analysis population; the 14 PROBABLE studies provided supportive evidence. Risk of bias was assessed using ROBINS-I (DEFINITE, primary) and JBI checklists (all studies). Sensitivity analyses excluded overlapping registries (ELSO, SAVE-J). Data were synthesized descriptively along three axes—selection, feasibility, and outcomes—without meta-analysis. Registered in PROSPERO (CRD420251252255); PRISMA 2020 compliant. Results: Twenty-seven studies encompassing 12,882 patients were included. In the DEFINITE primary cohort (13 studies, N = 3320), median survival to discharge was 30.3% (IQR 26.5–40.8; range 21.0–69.0; and n = 11) and favourable neurological outcome (CPC 1–2) 33.5% (IQR 16.8–45.8; range 10.4–92.0; and n = 12). Exclude-overlap sensitivity analysis (19 studies, N = 2741) yielded concordant estimates (survival 31.1%, IQR 27.2–37.0). PCI rates spanned 24–100% and post-procedural TIMI 3 flow 62.4–84.0%. ROBINS-I rated 9/13 DEFINITE studies at serious overall risk of bias and 4/13 at moderate (none low), predominantly from confounding by indication and selection bias—substantially more stringent than the JBI appraisal. Conclusions: PCI without sustained ROSC under ECPR is technically feasible, but the practice is widespread while remaining insufficiently standardized in ROSC reporting. Descriptive benchmarks from DEFINITE studies provide realistic outcome ranges for shared decision-making; no inference regarding comparative effectiveness is possible from observational data. Standardized documentation of ROSC status at PCI initiation is an immediate priority for future ECPR research.
Full article
(This article belongs to the Section Cardiovascular Medicine)
►▼
Show Figures

Figure 1
Open AccessArticle
Effects of Semaglutide on Cardiometabolic Risk in People with Obesity, With and Without Type 2 Diabetes: A Retrospective Observational Study
by
Loredana Deaconu, Oana Albai, Bogdan Timar, Adina Braha, Simona Popescu, Teodora Sorescu, Laura Gaita, Liana Iordan and Romulus Timar
J. Clin. Med. 2026, 15(12), 4421; https://doi.org/10.3390/jcm15124421 - 7 Jun 2026
Abstract
Background and Objectives: Obesity and insulin resistance are major contributors to cardiometabolic disease and type 2 diabetes mellitus (T2DM). This study evaluated the real-world effects of semaglutide on metabolic parameters, body composition, and cardiometabolic risk factors in people with obesity, with and
[...] Read more.
Background and Objectives: Obesity and insulin resistance are major contributors to cardiometabolic disease and type 2 diabetes mellitus (T2DM). This study evaluated the real-world effects of semaglutide on metabolic parameters, body composition, and cardiometabolic risk factors in people with obesity, with and without T2DM, and explored predictors of treatment response. Materials and Methods: This retrospective longitudinal observational study included 70 adults with obesity (42 with T2DM and 28 without T2DM) treated with semaglutide according to current clinical guidelines. The primary outcomes were changes in body weight, waist circumference, fasting plasma glucose, and glycated hemoglobin (HbA1c). Secondary outcomes included changes in lipid profile, insulin resistance indices, inflammatory markers, hepatic parameters, and body composition assessed by bioelectrical impedance analysis (InBody770). Results: Semaglutide treatment was associated with significant reductions in body weight (−9 kg), waist circumference (−8 cm), HbA1c (−1.1%), systolic blood pressure (−7.5 mmHg), visceral fat area (−30.1 cm2), and insulin resistance markers. Improvements in glycemic parameters were more pronounced in participants with T2DM. Skeletal muscle mass (SMM) was relatively preserved during treatment. Baseline HbA1c and visceral adiposity were independently associated with metabolic response. Conclusions: In this real-world observational cohort, semaglutide was associated with significant improvements in metabolic parameters, body composition, and cardiometabolic risk markers in people with obesity, with and without T2DM. Baseline metabolic characteristics may influence treatment response.
Full article
(This article belongs to the Section Endocrinology & Metabolism)
►▼
Show Figures
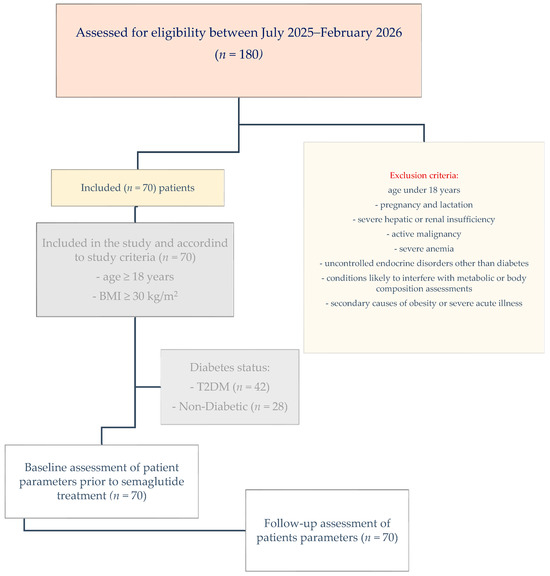
Figure 1

Journal Menu
► ▼ Journal Menu-
- JCM Home
- Aims & Scope
- Editorial Board
- Reviewer Board
- Topical Advisory Panel
- Instructions for Authors
- Special Issues
- Topics
- Sections & Collections
- Article Processing Charge
- Indexing & Archiving
- Editor’s Choice Articles
- Most Cited & Viewed
- Journal Statistics
- Journal History
- Journal Awards
- Society Collaborations
- Conferences
- Editorial Office
Journal Browser
► ▼ Journal BrowserHighly Accessed Articles
Latest Books
E-Mail Alert
News
Topics
Topic in
Cells, JCM, Organoids, JMP
Novel Discoveries in Oncology 2nd Edition
Topic Editors: Michela Campolo, Giovanna Casili, Alessia Filippone, Marika LanzaDeadline: 20 June 2026
Topic in
Biomedicines, IJMS, JCM, Medicina, Neurology International
Advances in Exercise-Induced Neurogenesis, Neuronal and Functional Adaptations in Neurorehabilitation
Topic Editors: Carlos Bernal-Utrera, Cleofas Rodriguez-Blanco, Maria Livia Carrascal MorenoDeadline: 29 June 2026
Topic in
Dentistry Journal, IJMS, JCM, Medicina, Applied Sciences
Oral Health Management and Disease Treatment
Topic Editors: Christos Rahiotis, Felice Lorusso, Sergio Rexhep TariDeadline: 31 July 2026
Topic in
Cancers, Diagnostics, Gastrointestinal Disorders, JCM, Current Oncology
Metastatic Colorectal Cancer: From Laboratory to Clinical Studies, 2nd Edition
Topic Editors: Ioannis Ntanasis-Stathopoulos, Diamantis I. TsilimigrasDeadline: 20 August 2026

Conferences
Special Issues
Special Issue in
JCM
Surgical Management of Maxillofacial Fractures and Reconstruction of Facial Deformities
Guest Editors: Gian Marco Prucher, Andrea Cassoni, Francesco ArcuriDeadline: 10 June 2026
Special Issue in
JCM
Clinical Research and Personalized Medicine in Inflammatory Bowel Disease
Guest Editors: Alfredo Papa, Loris Riccardo LopetusoDeadline: 10 June 2026
Special Issue in
JCM
Cardiomyopathy: Diagnosis and Therapeutic Advances
Guest Editors: Ilaria Dentamaro, Annagrazia CecereDeadline: 10 June 2026
Special Issue in
JCM
New Technologies for Personalized Medicine in Head and Neck Surgery
Guest Editors: Carlos Navarro-Cuéllar, José Luis Cebríán-CarreteroDeadline: 10 June 2026
Topical Collections
Topical Collection in
JCM
Pediatric and Adolescent Gynecology
Collection Editor: Panagiotis Christopoulos
Topical Collection in
JCM
Percutaneous Coronary Interventions in Acute Coronary Syndromes: Techniques, Imaging and Clinical Outcomes
Collection Editor: Ioannis Skalidis










