Journal Description
Complications
Complications
(ISSN 2813-4966) is an international, peer-reviewed, open access journal on the prevention, diagnosis, etiology, and management of complications in all aspects of basic, translational, and clinical research, as well as epidemiology. The journal seeks to offer best practices and expert experience, and recommendations on intra-operative and post-operative adverse events, published quarterly online by MDPI.
- Open Access— free for readers, with article processing charges (APC) paid by authors or their institutions.
- Rapid Publication: manuscripts are peer-reviewed and a first decision is provided to authors approximately 32.6 days after submission; acceptance to publication is undertaken in 4.8 days (median values for papers published in this journal in the second half of 2025).
- Recognition of Reviewers: APC discount vouchers, optional signed peer review, and reviewer names published annually in the journal.
- Complications is a companion journal of JCM.
Latest Articles
A Retrospective Study on Perioperative IV Fluid Restriction After a Disaster-Induced Fluid Shortage: Postoperative Pain and Complication Outcomes in Pediatric Adenotonsillectomies
Complications 2026, 3(2), 10; https://doi.org/10.3390/complications3020010 - 5 May 2026
Abstract
Intravenous fluids are integral to pediatric perioperative care, yet optimal fluid volumes during adenotonsillectomy remain debated. In 2024, Hurricane Helene disrupted IV fluid supply chains, necessitating an involuntary shift to restrictive intraoperative fluid administration. This event created an opportunity to evaluate whether reduced
[...] Read more.
Intravenous fluids are integral to pediatric perioperative care, yet optimal fluid volumes during adenotonsillectomy remain debated. In 2024, Hurricane Helene disrupted IV fluid supply chains, necessitating an involuntary shift to restrictive intraoperative fluid administration. This event created an opportunity to evaluate whether reduced intraoperative fluids affected postoperative pain or complication rates in pediatric adenotonsillectomies. We conducted a retrospective cohort study of children under 12 years who underwent adenotonsillectomy between 1 October 2024, and 31 January 2025. Patients were stratified into a restrictive fluid group (<10 mL/kg) and a non-restrictive group (≥10 mL/kg). Collected data included demographics, intraoperative fluid volumes, postoperative FLACC pain scores, and documented complications. Pain scores were compared using Mann–Whitney U tests, due to non-normal data distribution with descriptive analysis. A total of 133 patients were included (63 restrictive, 70 non-restrictive). Mean postoperative FLACC scores were similar between groups (4.53 ± 2.62 vs. 4.57 ± 3.44; p = 0.50), with comparable operative times. Complications occurred in both groups without a consistent association with fluid strategy. These findings suggest that intraoperative fluid restriction below 10 mL/kg does not significantly affect postoperative pain or overall complication rates in pediatric adenotonsillectomy. Short-term fluid restriction may be safe in resource-limited settings, though prospective studies are warranted.
Full article
Open AccessCase Report
Misleading Mediastinal Fluid Collection: A Rare Presentation of Chylothorax
by
Giacomo Grisorio, Ivan Lomangino, Luca Vecchiarelli and Andrea Dell’Amore
Complications 2026, 3(2), 9; https://doi.org/10.3390/complications3020009 - 10 Apr 2026
Abstract
►▼
Show Figures
We report the case of a 68-year-old man presenting with rapidly progressive left cervical swelling, sialorrhea, and dysphagia. Imaging revealed a cervical fluid collection extending into the anterior mediastinum, initially suggestive of descending mediastinitis. Broad-spectrum antibiotic therapy was initiated, and surgical drainage was
[...] Read more.
We report the case of a 68-year-old man presenting with rapidly progressive left cervical swelling, sialorrhea, and dysphagia. Imaging revealed a cervical fluid collection extending into the anterior mediastinum, initially suggestive of descending mediastinitis. Broad-spectrum antibiotic therapy was initiated, and surgical drainage was planned. Intraoperative exploration, however, revealed opalescent, milky fluid consistent with chyle, leading to a revised diagnosis of spontaneous chylocervical collection associated with chylothorax. Cultures were negative, and biochemical analysis confirmed markedly elevated triglyceride levels. Conservative management with total parenteral nutrition and a nil per os regimen achieved rapid resolution. Lymphangiography demonstrated normal thoracic duct anatomy without leakage. The patient was discharged in good condition, and follow-up imaging showed complete recovery. This case highlights the diagnostic challenge of differentiating chylous from infectious mediastinal collections, particularly when clinical presentation mimics descending mediastinitis. Accurate intraoperative assessment and multidisciplinary management are essential to avoid unnecessary invasive procedures. Rare etiologies such as idiopathic chylothorax should be considered in atypical presentations of cervical and mediastinal fluid collections.
Full article

Figure 1
Open AccessReview
Non-Invasive Ventilatory Support in Postoperative Respiratory Failure: A Phenotype-Driven Approach to Risk Stratification and Modality Selection
by
Roshan Shaik, Dylan Persaud, Rohail Gul and Perry Tiberio
Complications 2026, 3(2), 8; https://doi.org/10.3390/complications3020008 - 3 Apr 2026
Abstract
►▼
Show Figures
Postoperative respiratory failure (PRF) remains a pervasive clinical challenge that substantially contributes to perioperative morbidity, mortality, and prolonged ICU stay. Although conventional oxygen therapy is often sufficient, a significant subset of high-risk patients requires escalation to advanced non-invasive support to avoid reintubation and
[...] Read more.
Postoperative respiratory failure (PRF) remains a pervasive clinical challenge that substantially contributes to perioperative morbidity, mortality, and prolonged ICU stay. Although conventional oxygen therapy is often sufficient, a significant subset of high-risk patients requires escalation to advanced non-invasive support to avoid reintubation and invasive mechanical ventilation. Evidence from recent randomized trials, including the 2025 RENOVATE and Goret et al. studies, indicates that both non-invasive ventilation (NIV) and high-flow nasal oxygen (HFNO) reduce postoperative pulmonary complications and reintubation in selected high-risk populations. While NIV is preferred for hypercapnic ventilatory failure and is commonly used in selected high-risk cardiac surgery patients, HFNO offers comparable outcomes in pure hypoxemic failure with the added benefits of superior patient tolerance and a lower incidence of interface-related complications. Effective PRF management necessitates an individualized, physiology-based approach. By implementing a phenotype-driven algorithm that aligns device mechanics with the dominant pathophysiology, such as atelectasis versus pump failure, clinicians can optimize patient outcomes while minimizing the specific risks associated with delayed intubation.
Full article

Figure 1
Open AccessArticle
Does Incision Type Impact Culture Positivity in Implant-Based Reconstruction Complications for Breast Cancer and Breast Cancer Prophylaxis?
by
Kyuseok Im, Steven Yoshinaga, Yilan Jiangliu, Michael W. Chu, Antoine L. Carre and Anna M. Leung
Complications 2026, 3(1), 7; https://doi.org/10.3390/complications3010007 - 3 Mar 2026
Abstract
Background: Implant-based reconstruction (IBR) is the most common method of breast reconstruction after mastectomy. Prior studies have demonstrated that complications rates vary with incision type. We evaluated whether incision type affected culture positivity in IBR complications. Methods: A retrospective cohort study was performed
[...] Read more.
Background: Implant-based reconstruction (IBR) is the most common method of breast reconstruction after mastectomy. Prior studies have demonstrated that complications rates vary with incision type. We evaluated whether incision type affected culture positivity in IBR complications. Methods: A retrospective cohort study was performed of all patients undergoing mastectomy for cancer or cancer prophylaxis with IBR from 2012 to 2023. Abstracted data included patient characteristics, oncologic treatment history, mastectomy and reconstruction characteristics, culture positivity, infectious organism, and antibiotic treatment history. Results: A total of 6901 patients underwent post-mastectomy implant-based reconstruction, 183 (2.7%) patients had unplanned operative intervention for IBR complications, and 80/183 (43.7%) had culture-positive IBR infections. Culture-negative and culture-positive groups were similar in patient characteristics and oncologic treatment history. There was no difference in mastectomy incision types. The most common organisms were methicillin-sensitive Staphylococcus aureus, Pseudomonas aeruginosa, and coagulase-negative Staphylococcus. More patients in the culture-positive group were treated with antibiotics (81.2% vs. 51.5%, p = 0.0005). Antibiotic therapy duration was longer in the culture-negative group (8.52 vs. 5.78 days, p = 0.039). Among different incision types, there was no significant difference in duration of antibiotic therapy. Conclusions: No association between mastectomy incision type and culture-positive infections was observed among IBR complications in this study. Antibiotics may sterilize cultures, but operative intervention is still often required for IBR infections.
Full article
(This article belongs to the Special Issue Preventing and Managing Surgical Complications: Perspectives from Surgeons: 2nd Edition)
►▼
Show Figures

Figure 1
Open AccessReview
Posterior Cruciate Ligament Reconstruction Surgery: Tips and Tricks to Avoid Complications from a High-Volume Center
by
Simone Pavone, Simone Giusti, Angelo Matteucci, Marco Susca and Ezio Adriani
Complications 2026, 3(1), 6; https://doi.org/10.3390/complications3010006 - 2 Mar 2026
Abstract
Background: Posterior cruciate ligament reconstruction (PCLR) remains one of the most technically demanding procedures in knee ligament surgery, with complication rates considerably higher than those observed for other arthroscopic procedures. Residual laxity, arthrofibrosis, neurovascular injury, tunnel-related complications, and heterotopic ossification (HO) represent the
[...] Read more.
Background: Posterior cruciate ligament reconstruction (PCLR) remains one of the most technically demanding procedures in knee ligament surgery, with complication rates considerably higher than those observed for other arthroscopic procedures. Residual laxity, arthrofibrosis, neurovascular injury, tunnel-related complications, and heterotopic ossification (HO) represent the most frequent adverse events. With increasing surgical volumes and complexity—particularly in multiligament knee injuries (MLKIs)—structured, evidence-based strategies for complication avoidance are essential. The objective of this review is to provide a comprehensive, evidence-based overview of the main complications associated with PCLR and to propose a structured, reproducible protocol for complication prevention integrating current literature and high-volume institutional experience. Methods: A narrative review of the literature was conducted using PubMed and Google Scholar to identify clinical, biomechanical, and systematic studies on PCLR complications published between 2010 and 2025. Overall, 58 studies were screened and 33 were included for qualitative synthesis. Among the included studies, the level of evidence was Level I in five systematic reviews/meta-analyses, Level III–IV in seven observational clinical studies and registries, and Level V in biomechanical studies, narrative reviews, and expert consensus reports. In parallel, the recommendations were informed by the cumulative experience of a high-volume tertiary referral center with 187 PCLR procedures performed between 2010 and 2025 (136 MLKI, 51 isolated). Results: Evidence identifies several key predictors of postoperative complications: low posterior tibial slope (<6.54°), small graft diameter (<7.0 mm), untreated posterolateral corner insufficiency, excessive tibial tunnel angle, and surgical trauma at the “killer turn.” Neurovascular complications primarily arise during tibial tunnel instrumentation, with knee hyperflexion (>90°) significantly improving safety. Suture tape augmentation (STA) reduces graft elongation by 45–58% and is associated with improved biomechanical stability without increasing complication rates. Early controlled motion is critical to prevent arthrofibrosis, whereas HO—affecting up to 45% of MLKI patients—requires delayed surgical excision after maturation. Conclusions: Optimal outcomes after PCLR derive from a structured, complication-focused approach encompassing anatomical risk assessment, meticulous tunnel planning, neurovascular protection, biological augmentation, and disciplined postoperative rehabilitation. Adoption of standardized protocols—particularly in MLKIs—can substantially reduce the incidence of adverse events and improve long-term knee stability.
Full article
(This article belongs to the Special Issue Preventing and Managing Surgical Complications: Perspectives from Surgeons: 2nd Edition)
►▼
Show Figures

Figure 1
Open AccessArticle
The Impact of Radiotherapy Timing on Postoperative Outcomes in Chordoma Patients—A TriNetX Study
by
Kamal Shaik, Spencer T. Rasmussen, Mohammad Chowdhury, Clayton Rawson, Rudy Rahme and Michael Karsy
Complications 2026, 3(1), 5; https://doi.org/10.3390/complications3010005 - 10 Feb 2026
Abstract
Introduction: Chordomas are rare, locally aggressive tumors of the spine and skull base typically managed with maximal surgical resection followed by adjuvant radiotherapy. Although postoperative radiotherapy improves local control, the optimal interval for initiation remains uncertain, as early delivery may exacerbate wound-related complications
[...] Read more.
Introduction: Chordomas are rare, locally aggressive tumors of the spine and skull base typically managed with maximal surgical resection followed by adjuvant radiotherapy. Although postoperative radiotherapy improves local control, the optimal interval for initiation remains uncertain, as early delivery may exacerbate wound-related complications while delayed initiation may allow tumor progression. Methods: We performed a retrospective cohort analysis using the multi-center, national TriNetX Research Network. Adults with histologically confirmed skull base and/or spinal chordoma who underwent surgical resection followed by radiotherapy were stratified into ultraearly (≤2 weeks), standard (4–6 weeks), or delayed (≥10 weeks) radiotherapy initiation groups. Propensity score matching was used to adjust for demographic and clinical covariates. The primary outcome was all-cause mortality at 1, 3, and 5-years. Secondary outcomes included wound dehiscence, surgical site infection, and neurologic complications. Results: A total of 378 patients met the inclusion criteria. Ultraearly radiotherapy was not associated with significant differences in mortality at 1 year (RR 1.338; 95% CI 0.833–2.15; p = 0.22), 3 years (RR 1.233; 95% CI 0.858–1.772; p = 0.25), or 5 years (RR 1.196; 95% CI 0.876–1.633; p = 0.25) compared with standard timing. Delayed radiotherapy, however, demonstrated significantly reduced mortality at 1 year (RR: 0.53; 95% CI: 0.331–0.851; p = 0.01), 3 years (RR 0.641; 95% CI 0.449–0.914; p = 0.01), and 5 years (RR 0.654; 95% CI 0.473–0.905; p = 0.01) compared with standard timing. Event counts for secondary outcomes were insufficient for robust statistical comparison. Conclusions: Radiotherapy timing following surgical resection of chordoma did not impact short-term survival, but delayed radiotherapy significantly decreased 1, 3 and 5-year mortality. Rare secondary complications were seen. These findings suggest that the delayed initiation of radiotherapy may be helpful for patients with chordoma, supporting the need for prospective, long-term studies to clarify the balance between oncologic efficacy and perioperative morbidity.
Full article
(This article belongs to the Special Issue Preventing and Managing Surgical Complications: Perspectives from Surgeons: 2nd Edition)
►▼
Show Figures

Figure 1
Open AccessCase Report
Fatal Postoperative Deterioration Consistent with Sepsis After Burr-Hole Drainage for Chronic Subdural Hematoma in a Frail Older Adult with Diabetes: Suspected Abdominal Source and a Failure-to-Rescue Case Highlighting Delayed Abdominal Assessment
by
Yuta Arakaki, Takuto Nishihara, Kotaro Makita, Kosei Goto and Nobuo Kutsuna
Complications 2026, 3(1), 4; https://doi.org/10.3390/complications3010004 - 2 Feb 2026
Abstract
►▼
Show Figures
Chronic subdural hematoma (CSDH) in frail older adults is increasingly recognized as a sentinel event, with mortality often driven by medical complications rather than neurosurgical factors. We report a failure-to-rescue case in which rapid postoperative deterioration occurred after burr-hole drainage for bilateral CSDH
[...] Read more.
Chronic subdural hematoma (CSDH) in frail older adults is increasingly recognized as a sentinel event, with mortality often driven by medical complications rather than neurosurgical factors. We report a failure-to-rescue case in which rapid postoperative deterioration occurred after burr-hole drainage for bilateral CSDH in a frail older adult with diabetes. A clinical picture consistent with sepsis was suspected, and a gastrointestinal source was considered, but the infectious focus could not be confirmed due to limited diagnostic work-up. On admission, chest-computed tomography showed mild right lower-lobe pneumonia, and incidental transverse colonic dilatation was also visible. Burr-hole drainage was uneventful and oxygenation rapidly normalized on room air. On postoperative day (POD) 3, the patient developed a high fever (39 °C), rising C-reactive protein (CRP; 14 mg/dL), abrupt leukopenia (15,300 → 3300/µL), and, several hours later, profuse watery diarrhea. At that time, an evaluation for an infectious source and escalation of therapy (e.g., blood cultures, serum lactate, and abdominal imaging) were not performed. In the early hours of POD 4, he suffered sudden desaturation, shock, and cardiac arrest, and died despite resuscitation. A portable radiograph after intubation showed no new diffuse pulmonary infiltrates but marked colonic gas distension. This case highlights the need to reassess diagnostic framing when discordant postoperative “red flags” emerge and proposes practical triggers for early sepsis evaluation and escalation—prioritizing early recognition and timely rescue rather than a definitive determination of the cause of death—in high-risk CSDH patients.
Full article

Figure 1
Open AccessReview
Anesthesia Management in Carotid Paraganglioma Surgery: How to Address the Complexities and Ensure Safety
by
Marco Franchin, Luca Guzzetti, Matteo Tozzi, Martina Baiardo Redaelli, Maria Cristina Cervarolo, Noemi Graziano, Gabriele Piffaretti, Luca Cabrini, Alessandro Bacuzzi and Mario D’Oria
Complications 2026, 3(1), 3; https://doi.org/10.3390/complications3010003 - 30 Jan 2026
Abstract
Carotid paragangliomas are rare neuroendocrine tumors that, despite being typically benign, present significant surgical and anesthetic challenges. This manuscript outlines the anesthetic management for surgical resection, highlighting preoperative assessment, intraoperative monitoring, and postoperative care. A multidisciplinary approach is essential, particularly for functional tumors,
[...] Read more.
Carotid paragangliomas are rare neuroendocrine tumors that, despite being typically benign, present significant surgical and anesthetic challenges. This manuscript outlines the anesthetic management for surgical resection, highlighting preoperative assessment, intraoperative monitoring, and postoperative care. A multidisciplinary approach is essential, particularly for functional tumors, requiring preoperative screening and pharmacologic preparation. Intraoperatively, cerebral perfusion monitoring is critical to prevent ischemic events. Postoperative vigilance is necessary to detect complications such as bleeding, cranial nerve deficits, and hemodynamic instability. A multidisciplinary team skilled in these surgical procedures is essential to improve safety in carotid paraganglioma surgery.
Full article
(This article belongs to the Special Issue Preventing and Managing Surgical Complications: Perspectives from Surgeons: 2nd Edition)
►▼
Show Figures

Figure 1
Open AccessCase Report
Managing Gallstone Ileus and Surgical Considerations in Resource-Limited Settings: A Case Series from the Amazon Jungle
by
Santiago Andrés Suárez-Gómez, Valentina Velasco-Muñoz, Nicolás Escobar, Fernando Escobar Castañeda and Oscar Guevara
Complications 2026, 3(1), 2; https://doi.org/10.3390/complications3010002 - 9 Jan 2026
Abstract
Gallstone ileus is a rare but serious complication of gallstone disease, often requiring surgical intervention. While enterolithotomy remains the standard treatment, the role of additional biliary surgery, particularly subtotal cholecystectomy, remains controversial. This study examines the management of gallstone ileus in a rural
[...] Read more.
Gallstone ileus is a rare but serious complication of gallstone disease, often requiring surgical intervention. While enterolithotomy remains the standard treatment, the role of additional biliary surgery, particularly subtotal cholecystectomy, remains controversial. This study examines the management of gallstone ileus in a rural setting, where limited surgical resources and access to specialized biliary interventions pose unique challenges. We present a case series of four patients diagnosed with gallstone ileus in a rural healthcare facility. All patients underwent initial enterolithotomy for bowel obstruction relief. Surgical outcomes, complications, and the necessity for a second intervention, including subtotal cholecystectomy, were evaluated. Ever patient had a successful recovery. Of the four cases, two patients underwent a subtotal cholecystectomy. No perioperative mortality was observed, but limited access to advanced imaging and specialized biliary surgery influenced clinical decision-making. The rural setting in which these series occurred comes with its unique challenges regarding resource management and technological demands.
Full article
(This article belongs to the Special Issue Preventing and Managing Surgical Complications: Perspectives from Surgeons)
►▼
Show Figures

Figure 1
Open AccessReview
Ureteral and Vascular Events During Robotic Post-Chemotherapy Retroperitoneal Lymph Node Dissection: Technical Insights and Management Considerations
by
Manuel Saavedra Centeno, Eduardo Albers Acosta, Clara Velasco Balanza, Lira Pelari Mici, Carlos Márquez Güemez, Marta Pérez Pérez, Ana Sánchez Ramírez and Luis Alberto San José Manso
Complications 2026, 3(1), 1; https://doi.org/10.3390/complications3010001 - 8 Jan 2026
Abstract
Robotic retroperitoneal lymph node dissection (R-RPLND) represents an evolution in the surgical management of testicular germ cell tumors, offering reduced morbidity compared with open approaches. However, this procedure remains technically challenging, particularly after chemotherapy, due to dense fibrosis and distortion of the retroperitoneal
[...] Read more.
Robotic retroperitoneal lymph node dissection (R-RPLND) represents an evolution in the surgical management of testicular germ cell tumors, offering reduced morbidity compared with open approaches. However, this procedure remains technically challenging, particularly after chemotherapy, due to dense fibrosis and distortion of the retroperitoneal anatomy. We report a case of an unrecognized intraoperative thermal injury causing a partial transection of the proximal ureter presenting postoperatively as a urinary fistula following R-RPLND for residual mass resection, along with a focused review of the contemporary literature on procedure-related complications. A review of large series highlights severe complications (Clavien–Dindo ≥ III) occurring in 6–12% of cases, with ureteral injuries occurring in up to 6%, often identified after surgery. This case underscores the importance of meticulous dissection, awareness of altered anatomy, and prompt intervention when unexpected events arise during R-RPLND.
Full article
(This article belongs to the Special Issue Preventing and Managing Surgical Complications: Perspectives from Surgeons: 2nd Edition)
►▼
Show Figures

Figure 1
Open AccessReview
Biologic Reconstruction in the Compromised Spine: A Review of Vascularized Bone Grafts to Mitigate Complications After Sarcoma Resection
by
Tanner Carcione, Jonathan Jeger, Nicholas W. Jungbauer, Jenna Meyer and Edward Reece
Complications 2025, 2(4), 30; https://doi.org/10.3390/complications2040030 - 12 Dec 2025
Abstract
►▼
Show Figures
Spinal sarcomas are rare, aggressive tumors requiring wide resection that creates large, challenging defects. Conventional reconstruction using allografts or metallic implants is prone to failure in compromised settings like irradiated or infected tissue. This narrative review synthesizes the literature on biologic reconstruction strategies,
[...] Read more.
Spinal sarcomas are rare, aggressive tumors requiring wide resection that creates large, challenging defects. Conventional reconstruction using allografts or metallic implants is prone to failure in compromised settings like irradiated or infected tissue. This narrative review synthesizes the literature on biologic reconstruction strategies, focusing on vascularized bone grafts (VBGs) and the ‘spinoplastic’ reconstruction approach, to provide a clinical framework for their application. We performed a narrative literature review using PubMed and Scopus to synthesize clinical studies describing biologic spinal reconstruction in compromised host beds. The main findings show that pedicled VBGs (e.g., rib, iliac crest) and free VBGs (e.g., fibula) function as living structural components. ‘Spinoplastic’ reconstruction leverages these grafts to promote biologic fusion, with clinical series reporting high union rates, even in irradiated or revision settings, offering a durable alternative to avascular constructs. Biologic reconstruction using VBGs is a critical strategy for achieving durable spinal stability in these challenging scenarios, and future directions point toward hybrid strategies combining 3D-printed implants with the biologic power of VBGs.
Full article

Figure 1
Open AccessReview
Complications Associated with Ileal Conduit: A Narrative Review
by
Laura Karina Fumero, Luis G. Medina, Federico Eskenazi, Samer Jaber, Alvaro Gonzalo-Balbas, Camilo Andres Giedelman, Roberto Soto Suarez and Rene Sotelo
Complications 2025, 2(4), 29; https://doi.org/10.3390/complications2040029 - 18 Nov 2025
Abstract
►▼
Show Figures
Introduction: Rerouting urine flow is often required following radical cystectomy (RC). In this context, the ileal conduit (IC) has become the most common technique for urinary diversion, primarily due to its technical simplicity and suitability for patients with compromised renal function, elderly individuals,
[...] Read more.
Introduction: Rerouting urine flow is often required following radical cystectomy (RC). In this context, the ileal conduit (IC) has become the most common technique for urinary diversion, primarily due to its technical simplicity and suitability for patients with compromised renal function, elderly individuals, and those unable to perform self-catheterization. Objective: This review aims to highlight the complications of IC and categorize them into metabolic and surgical complications, further subdivided by timing (intraoperative, short-term, intermediate-term, and long-term) and anatomical location (uretero-ileal anastomosis, stoma, and ileal segment). Methods: A comprehensive narrative review was conducted to summarize the most common complications of IC, their clinical presentation, and management using Google Scholar, PubMed, and Embase databases to identify studies published from 1950 to 2024. Results: The morbidity associated with IC, especially when compared to continent diversions, remains a subject of debate. Notably, IC-related complications have been described with an incidence rate ranging from 39% to 67%. Conclusions: Providing a comprehensive overview of IC complications and management strategies can enhance clinical practice and improve patient outcomes.
Full article

Figure 1
Open AccessArticle
Early Results Utilizing a Novel Fibular Nail for Surgical Fixation of Ankle Fractures—A Retrospective Case Series
by
Julia E. Ralph, Crystal Jing, Albert T. Anastasio and Samuel B. Adams
Complications 2025, 2(4), 28; https://doi.org/10.3390/complications2040028 - 17 Nov 2025
Abstract
Ankle fractures are extremely common and often require surgical management, historically with open reduction and internal fixation (ORIF), although fibular intramedullary nailing (IMN) has demonstrated promising results in recent years. The purpose of this study is to report on risk factors, quality of
[...] Read more.
Ankle fractures are extremely common and often require surgical management, historically with open reduction and internal fixation (ORIF), although fibular intramedullary nailing (IMN) has demonstrated promising results in recent years. The purpose of this study is to report on risk factors, quality of reduction, and complications in a series of patients undergoing fibular IMN for management of ankle fractures using a novel device via a retrospective case series. Patients undergoing locked fibular IMN with the Flex-Thread nail (Conventus Flower Orthopedics, Horsham, PA, USA) by a single surgeon from January 2023 to March 2025 were included, with at least 6 months of follow-up. Demographics, comorbidities, injury characteristics, reduction quality, and post-operative complications were recorded. Descriptive analyses were reported for categorical variables. A total of 15 patients were included, with a mean age of 58.9 ± 22.0 (range 18–91) and mean BMI of 31.5 ± 5.7 kg/m2. All patients experienced a fall as their mechanism of injury, with 12 Weber B and 3 Weber C fractures. The mean time to surgery from the date of injury was 9.5 ± 5.5 days. Of 15 patients, 66.7% had good reduction quality, 26.7% had fair, and 1 patient experienced poor reduction quality requiring subsequent hardware removal. There was one patient who experienced delayed wound healing. Patients undergoing fibular fixation using the novel Flex-Thread nail experience a fair to good quality of reduction, with limited complications. Both young and elderly patients have relatively positive early post-operative outcomes. Additional research with longer-term follow-up will be required to confirm its efficacy.
Full article
Open AccessArticle
Impact of BMI on Complications, Readmissions, and Perioperative Metrics in a Mature Direct Anterior Approach Total Hip Arthroplasty (THA) Practice
by
Stefan W. Fleps and Christopher J. Drinkwater
Complications 2025, 2(4), 27; https://doi.org/10.3390/complications2040027 - 3 Nov 2025
Abstract
This study analyzed complication rates, perioperative metrics, and hospital readmissions across BMI cohorts in patients undergoing direct anterior approach (DAA) total hip arthroplasty (THA) in a mature hip practice. Currently, the precise BMI cutoff points for risk in THA are not fully understood.
[...] Read more.
This study analyzed complication rates, perioperative metrics, and hospital readmissions across BMI cohorts in patients undergoing direct anterior approach (DAA) total hip arthroplasty (THA) in a mature hip practice. Currently, the precise BMI cutoff points for risk in THA are not fully understood. A retrospective review was conducted of patients who underwent DAA THA by a single, highly experienced, fellowship-trained surgeon between January 2021 and January 2023. The use of single-surgeon cases allows for control of many potentially confounding variables but may limit the generalizability of the findings. Data collected included patient demographics, hospital readmissions, 12-month complication rates, and intraoperative metrics. Patients with Class II obesity (BMI 35–39.9) kg/m2 and Class I obesity (BMI 30–34.9) kg/m2 had significantly higher intraoperative blood loss and longer operative times compared to the control group (BMI 20–24.9 kg/m2). No statistically significant differences in hospital readmission rates or complication rates were observed between BMI cohorts. Higher BMI was associated with increased intraoperative blood loss and longer operation time; however, no differences were found in hospital readmissions or complication rates between BMI cohorts.
Full article
Open AccessSystematic Review
Factors Influencing Major Amputation and Death Following Limb Salvage Surgery in a Diabetic Population: Systematic Review and Real-World Comparison
by
Kit Ferguson, Sifat M. Alam, Connor Phillips, Lia Spencer, Michelle Goodeve, Selina Begum, Harrison Travis, Jade Tang, Richard Feinn, Douglas McHugh and Ewan Kannegieter
Complications 2025, 2(4), 26; https://doi.org/10.3390/complications2040026 - 22 Oct 2025
Cited by 3
Abstract
Diabetic foot ulcers drive non-traumatic lower-limb amputation; limb salvage surgery is often pursued to preserve function and survival. Predictors of adverse outcomes remain incompletely defined, and evidence for multidisciplinary team (MDT) care is heterogeneous. We aimed to clarify risk factors for major amputation
[...] Read more.
Diabetic foot ulcers drive non-traumatic lower-limb amputation; limb salvage surgery is often pursued to preserve function and survival. Predictors of adverse outcomes remain incompletely defined, and evidence for multidisciplinary team (MDT) care is heterogeneous. We aimed to clarify risk factors for major amputation and death after diabetic limb salvage and evaluate MDT impact. We systematically reviewed 49 studies (2020–2025) reporting major amputation or mortality after limb salvage in diabetes (PROSPERO CRD420251044859). Risk factors spanned demographic, clinical, and surgical domains (e.g., older age, male sex, renal/cardiovascular disease, ischemia, osteomyelitis, advanced ulcer classification). MDT models generally showed lower amputation rates and improved wound healing, with occasional survival benefits; heterogeneity precluded meta-analysis. As a real-world comparator, the Mid Essex Diabetes Amputation Reduction Plan (MEDARP) treated 72 high-risk patients using a “toe and flow” MDT. Major amputation occurred in 6.9% and mortality in 12.5%, both at or below published ranges, with gains in patient-reported outcomes. Findings support MDT-based strategies, but conclusions should be interpreted cautiously given the predominantly observational evidence, and highlight the need for standardized outcome definitions and reporting.
Full article
(This article belongs to the Special Issue Preventing and Managing Surgical Complications: Perspectives from Surgeons: 2nd Edition)
►▼
Show Figures

Figure 1
Open AccessReview
Combustible Tobacco, Smokeless Tobacco, and Cannabis Use in Foot and Ankle Surgery: A Scoping Review of Postoperative Outcomes
by
Jennifer A. Kipp and Lindsay K. LeSavage
Complications 2025, 2(4), 25; https://doi.org/10.3390/complications2040025 - 20 Oct 2025
Cited by 1
Abstract
►▼
Show Figures
Introduction: Tobacco smoking is a known risk factor for adverse surgical outcomes, including delayed wound healing and an increased risk of infection and nonunion. The rising use of cannabis products and alternative nicotine products, such as smokeless tobacco and electronic cigarette devices
[...] Read more.
Introduction: Tobacco smoking is a known risk factor for adverse surgical outcomes, including delayed wound healing and an increased risk of infection and nonunion. The rising use of cannabis products and alternative nicotine products, such as smokeless tobacco and electronic cigarette devices present new challenges for perioperative management, yet their influence in foot and ankle surgery is not well studied. Objectives: This scoping review aims to synthesize the existing literature on tobacco use, cannabis, and electronic cigarettes and their influence on postoperative outcomes in foot and ankle surgery. Methods: A comprehensive search of PubMed was performed using PRISMA-ScR guidelines. Eligible studies included observational studies and reviews that focus on the relationship between perioperative substance use and foot and ankle surgery complications. Results: There is a wide range of evidence that supports increased wound and bone healing complications with use of combustible tobacco. Data on the effects of smokeless tobacco, electronic cigarettes, and cannabis on this patient population is limited, with most evidence drawn from animal studies or broader orthopaedic literature. Conclusions: The existing data raises potential concern for adverse effects with use of these products. By identifying existing findings and gaps in the literature, this review highlights the need for further research on the perioperative effects of these substances in foot and ankle surgery.
Full article
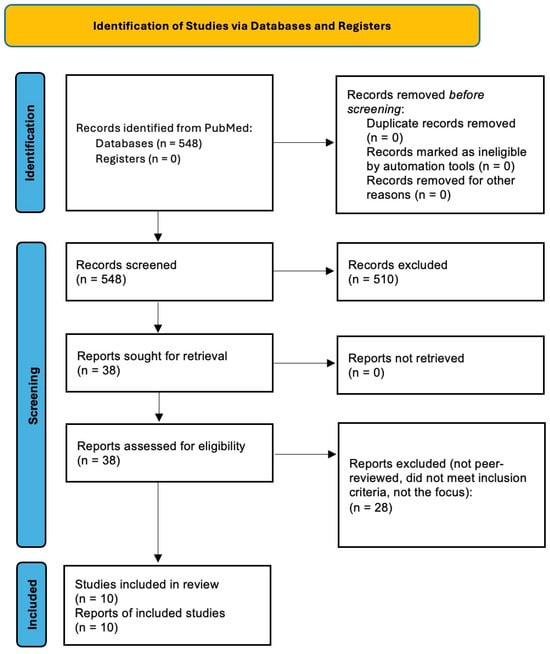
Figure 1
Open AccessReview
Navigating the Spectrum of Pancreatic Surgery Complications: A Review
by
Sibi Krishna Thiyagarajan, Alfredo Verastegui, John A. Stauffer and Katherine Poruk
Complications 2025, 2(4), 24; https://doi.org/10.3390/complications2040024 - 2 Oct 2025
Cited by 1
Abstract
Background: Despite advances in surgical techniques and perioperative care, pancreatic resections such as pancreaticoduodenectomy (PD) and distal pancreatectomy (DP) remain high-risk procedures. Postoperative complications significantly impact morbidity, mortality, and patient quality of life. Methods: This narrative review summarizes recent literature on major complications
[...] Read more.
Background: Despite advances in surgical techniques and perioperative care, pancreatic resections such as pancreaticoduodenectomy (PD) and distal pancreatectomy (DP) remain high-risk procedures. Postoperative complications significantly impact morbidity, mortality, and patient quality of life. Methods: This narrative review summarizes recent literature on major complications following pancreatic surgery, including postoperative pancreatic fistula (POPF), delayed gastric emptying (DGE), and post-pancreatectomy hemorrhage (PPH), with an emphasis on incidence, risk factors, outcomes, and current preventive strategies. Results: POPF is a leading complication, occurring in 5–22% of cases and often linked with sepsis and hemorrhage. Key risk factors include high BMI, soft pancreatic texture, and small duct size. Preventive measures like Pasireotide, modified anastomosis techniques, and neoadjuvant therapy show variable success. DGE affects up to 57% of PD patients and is associated with prolonged recovery; antecolic reconstruction and erythromycin may reduce incidence. PPH, though less frequent (3–13%), can be life-threatening, particularly when secondary to POPF. Endovascular approaches are now favored for late arterial bleeding. Other complications include wound infections, abscesses, bile leaks, and pulmonary issues, all contributing to extended hospital stays and diminished quality of life. Conclusions: Pancreatic surgery continues to carry significant risks, with POPF, DGE, and PPH being the most impactful complications. While multiple interventions have shown promise, standardized protocols and predictive tools are still needed. Surgery should be performed in high-volume centers with experienced multidisciplinary teams to optimize outcomes.
Full article
(This article belongs to the Special Issue Preventing and Managing Surgical Complications: Perspectives from Surgeons)
Open AccessReview
Fulminant Necrotizing Soft Tissue Infection Following Abdominal Liposuction: Comprehensive Literature Review and Case Report
by
Claudia Viviana Jaimes Gonzalez, Joan Sebastian Barrera Guaca, Maria Angela Gomez Martinez, Felipe Caballero Paz and Luis Fernando Alvarez Molina
Complications 2025, 2(3), 23; https://doi.org/10.3390/complications2030023 - 11 Sep 2025
Abstract
Necrotizing soft tissue infection (NSTI) is a rapidly progressive, life-threatening soft tissue infection that involves the skin, subcutaneous tissue, and fascia, with a natural evolution to septic shock and death if not treated. NSTI is typically associated with trauma, and rarely reported as
[...] Read more.
Necrotizing soft tissue infection (NSTI) is a rapidly progressive, life-threatening soft tissue infection that involves the skin, subcutaneous tissue, and fascia, with a natural evolution to septic shock and death if not treated. NSTI is typically associated with trauma, and rarely reported as a complication of aesthetic procedures such as liposuction. We report the case of a previously healthy 34-year-old woman who developed fulminant necrotizing soft tissue infection shortly after undergoing abdominal liposuction in a suspected non-accredited facility. She arrived at our institution with severe thoracoabdominal pain, ecchymosis, and refractory shock within hours postoperatively. Imaging studies performed in the emergency department revealed gas in the soft tissues, confirming the diagnosis. Emergent surgical debridement exposed extensive necrosis affecting a large body surface area. The patient required multiple surgeries, intensive care support, and broad-spectrum antibiotics to achieve infection control. Reconstructive treatment was initiated once stabilization was achieved, leading to full wound closure and a favorable clinical outcome. In addition, we provide a comprehensive review of the current literature regarding necrotizing soft tissue infection, emphasizing this condition as a postoperative complication, including its epidemiology, microbial etiology, pathophysiology, diagnostic challenges, treatment strategies, and reported cases. This review aims to contextualize this rare but severe postoperative complication and to guide clinicians in its early recognition and management, while also raising awareness about the potential consequences of aesthetic procedures performed in unregulated settings.
Full article
(This article belongs to the Special Issue Preventing and Managing Surgical Complications: Perspectives from Surgeons: 2nd Edition)
►▼
Show Figures

Figure 1
Open AccessSystematic Review
Complications of Vertebroplasty in Adults: Incidence, Etiology, and Therapeutic Strategies—A Comprehensive, Systematic Literature Review
by
Juan Pablo Zuluaga-Garcia, Maria Alejandra Sierra, Francisco Alfredo Call-Orellana, David Herrera, Romulo A. Andrade-Almeida, Pawan Kishore Ravindran and Esteban Ramirez-Ferrer
Complications 2025, 2(3), 22; https://doi.org/10.3390/complications2030022 - 2 Sep 2025
Cited by 1
Abstract
►▼
Show Figures
Percutaneous vertebroplasty (PVP) has emerged as a key intervention for painful vertebral compression fractures in osteoporotic and metastatic disease, but its safety profile warrants comprehensive evaluation. We conducted a PRISMA-compliant systematic review of studies published between 2009 and 2024, identifying 15 clinical studies
[...] Read more.
Percutaneous vertebroplasty (PVP) has emerged as a key intervention for painful vertebral compression fractures in osteoporotic and metastatic disease, but its safety profile warrants comprehensive evaluation. We conducted a PRISMA-compliant systematic review of studies published between 2009 and 2024, identifying 15 clinical studies (n ≈ 8500 patients) that reported PVP-related complications in adults with osteoporotic or neoplastic fractures. Data extraction focused on complication incidence, presentation, imaging findings, risk factors, and management strategies. Cement leakage was the most frequently detected event (20–70% of levels, higher in neo-plastic lesions), yet symptomatic neural or vascular sequelae occurred in <1%. Pulmonary cement embolism appeared on imaging in 2–26% of cases but was clinically evident in ≤0.5%, with conservative management or brief anticoagulation sufficing for most patients. New vertebral fractures developed in 8–20% of osteoporotic and up to 30% of metastatic cohorts, paralleling underlying bone fragility rather than PVP itself. Postprocedural infection (0.2–0.5%) and neurologic injury (<0.5%) were uncommon but required prompt surgical and antibiotic interventions. Overall, PVP’s benefits—rapid pain relief and mechanical stabilization—outweigh its risks when performed with meticulous technique, vigilant imaging, and multidisciplinary follow-up, confirming its favorable safety profile in both osteoporosis and spinal malignancy.
Full article

Figure 1
Open AccessReview
Practical Strategies to Predict, Avoid and Manage the Complications of Robotic-Assisted Partial Nephrectomy
by
Andrew R. H. Shepherd and Benjamin J. Challacombe
Complications 2025, 2(3), 21; https://doi.org/10.3390/complications2030021 - 8 Aug 2025
Abstract
Background/objectives: Robotic-assisted partial nephrectomy (RAPN) is increasingly utilised for the management of renal masses, with the growing use of different robotic platforms and increasing complexity of renal masses managed robotically. Appropriate patient selection, the development of operative skills and experience and sensible surgical
[...] Read more.
Background/objectives: Robotic-assisted partial nephrectomy (RAPN) is increasingly utilised for the management of renal masses, with the growing use of different robotic platforms and increasing complexity of renal masses managed robotically. Appropriate patient selection, the development of operative skills and experience and sensible surgical decision making are required to optimise the outcomes of RAPN and minimise the risk of complications. We provide a comprehensive review of strategies to predict, avoid and manage the complications of RAPN. Methods: We conducted a comprehensive literature review to outline many of the reported complications arising from RAPN, with a focus on preoperative considerations (patient selection, imaging, 3D modelling and predictive models), intraoperative considerations (positioning and kidney exposure complications) and practical management strategies to identify and manage the complications of this procedure. Results: Many complications of RAPN can be predicted, and we outline strategies to mitigate these risks through careful preparation prior to surgery, including descriptions of preventative strategies and important preoperative considerations. We also present a detailed outline of management for the most common complications of RAPN, including bleeding/haemorrhage, urine leak and intraoperative complications such as adjacent organ injuries. Conclusions: RAPN can be a challenging procedure with a significant risk of complications. Assiduous preoperative planning, thoughtful intraoperative decision making and the early recognition and management of complications are essential to optimise patient outcomes following RAPN.
Full article
(This article belongs to the Special Issue Preventing and Managing Surgical Complications: Perspectives from Surgeons)
►▼
Show Figures

Figure 1
Highly Accessed Articles
Latest Books
E-Mail Alert
News
Topics

Conferences
Special Issues
Special Issue in
Complications
Types of Clinical Complications in Inpatients in Internal Medicine
Guest Editors: Pierpaolo Di Micco, Carmine SiniscalchiDeadline: 4 January 2027




