-
 In the Mouth or in the Gut? Innovation Through Implementing Oral and Gastrointestinal Health Science in Chronic Pain Management
In the Mouth or in the Gut? Innovation Through Implementing Oral and Gastrointestinal Health Science in Chronic Pain Management -
 An Overview of Severe Myalgic Encephalomyelitis
An Overview of Severe Myalgic Encephalomyelitis -
 Effectiveness of Pharmacological Treatments for Adult ADHD on Psychiatric Comorbidity: A Systematic Review
Effectiveness of Pharmacological Treatments for Adult ADHD on Psychiatric Comorbidity: A Systematic Review -
 Non-Surgical Correction of Facial Asymmetry: A Narrative Review of Non-Surgical Modalities and Clinical Case Examples
Non-Surgical Correction of Facial Asymmetry: A Narrative Review of Non-Surgical Modalities and Clinical Case Examples -
 Breast Imaging Findings in Women with Lipedema: A Retrospective Cross-Sectional Descriptive Study
Breast Imaging Findings in Women with Lipedema: A Retrospective Cross-Sectional Descriptive Study
Journal Description
Journal of Clinical Medicine
Journal of Clinical Medicine
is an international, peer-reviewed, open access journal of clinical medicine, published semimonthly online by MDPI. The International Bone Research Association (IBRA), Spanish Society of Hematology and Hemotherapy (SEHH), Japan Association for Clinical Engineers (JACE), European Independent Foundation in Angiology/ Vascular Medicine (VAS) and others are all affiliated with JCM, and their members receive a discount on article processing charges.
- Open Access— free for readers, with article processing charges (APC) paid by authors or their institutions.
- High Visibility: indexed within Scopus, SCIE (Web of Science), PubMed, PMC, Embase, CAPlus / SciFinder, and other databases.
- Journal Rank: JCR - Q1 (Medicine, General and Internal) / CiteScore - Q1 (General Medicine)
- Rapid Publication: manuscripts are peer-reviewed and a first decision is provided to authors approximately 18.5 days after submission; acceptance to publication is undertaken in 2.7 days (median values for papers published in this journal in the second half of 2025).
- Recognition of Reviewers: reviewers who provide timely, thorough peer-review reports receive vouchers entitling them to a discount on the APC of their next publication in any MDPI journal, in appreciation of the work done.
- Companion journals for JCM include: Epidemiologia, Transplantology, Uro, Sinusitis, Rheumato, Journal of Clinical & Translational Ophthalmology, Journal of Vascular Diseases, Osteology, Complications, Therapeutics, Sclerosis, Pharmacoepidemiology and Journal of CardioRenal Medicine.
- Journal Clusters of Hematology: Hemato, Hematology Reports, Thalassemia Reports and Journal of Clinical Medicine.
Impact Factor:
2.9 (2024);
5-Year Impact Factor:
3.3 (2024)
Latest Articles
Clinical Utility of a Feedback Device in High-Quality Cardiopulmonary Resuscitation: The Guardian Angel
J. Clin. Med. 2026, 15(8), 2839; https://doi.org/10.3390/jcm15082839 (registering DOI) - 9 Apr 2026
Abstract
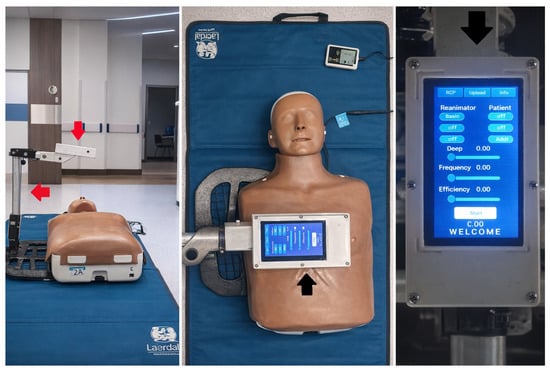
Background/Objectives: High-quality cardiopulmonary resuscitation (CPR) is essential for improving clinical outcomes in patients experiencing cardiac arrest. Feedback devices designed to guide CPR must offer real-time feedback on chest compression quality for use by both medical personnel and laypersons. To describe the impact of
[...] Read more.
Background/Objectives: High-quality cardiopulmonary resuscitation (CPR) is essential for improving clinical outcomes in patients experiencing cardiac arrest. Feedback devices designed to guide CPR must offer real-time feedback on chest compression quality for use by both medical personnel and laypersons. To describe the impact of using an infrared-based device to provide feedback on chest compression quality during CPR performed by healthcare personnel. Methods: A before-and-after study conducted in a simulated hospital from February 2019 to February 2020 evaluated the difference in the percentage of adequate chest compressions in depth and rate. This was assessed by comparing the number of adequate compressions to the total performed in one minute, both with and without the use of a feedback device. Results: A total of 90 participants were recruited, with an average age of 31.2 years (SD: 8.86), of which 60% (54/90) were women. In infants and schoolchildren/adults, high-quality compressions improved by 66% (85% vs. 19%; p < 0.001) and 54% (79% vs. 25%; p < 0.001), respectively, when guided by the GA compared to the control group. In participants without training and experience in CPR, the use of the Guardian Angel achieved high-quality compressions of 45% (10/22) and 66% (25/42), respectively, when evaluating depth for the schoolchildren/adults group. The use of the device during CPR, even in situations of moderate or severe fatigue, resulted in an improvement in high-quality compressions in terms of frequency, reaching 73% (16/22) in infants and 68% (15/22) in schoolchildren/adults. Conclusions: The Guardian Angel improves both the frequency and depth of compressions in participants without previous CPR experience or training. Additionally, the device demonstrated notable improvements in compression frequency, even in situations of moderate or severe fatigue.
Full article
(This article belongs to the Section Respiratory Medicine)
►
Show Figures
Open AccessArticle
Clinical Factors Associated with Termination of Pregnancy Recommendations Following Prenatal Diagnosis of Congenital Heart Disease: A Multidisciplinary Council-Based Study
by
Ilayda Gercik Arzik, Hakan Golbasi, Zubeyde Emiralioglu Cakir, Hale Ankara Aktas, Bahar Konuralp Atakul, Didem Gul Saritas, Deniz Boz Eravci and Atalay Ekin
J. Clin. Med. 2026, 15(8), 2838; https://doi.org/10.3390/jcm15082838 (registering DOI) - 9 Apr 2026
Abstract
Objective: To evaluate clinical factors associated with termination of pregnancy (TOP) recommendations following prenatal diagnosis of congenital heart disease (CHD) within a multidisciplinary fetal council model. Methods: This retrospective cohort study included 146 fetuses with prenatally diagnosed CHD discussed in a tertiary referral
[...] Read more.
Objective: To evaluate clinical factors associated with termination of pregnancy (TOP) recommendations following prenatal diagnosis of congenital heart disease (CHD) within a multidisciplinary fetal council model. Methods: This retrospective cohort study included 146 fetuses with prenatally diagnosed CHD discussed in a tertiary referral center fetal council between October 2023 and December 2025. The primary outcome was council-issued recommendation for TOP (yes/no). Variables included gestational age (GA) at diagnosis, cardiac severity (Davey scale grouped as low, moderate, high), extracardiac anomalies, fetal growth restriction (FGR), and genetic evaluation/results. Group comparisons were performed using Mann–Whitney U and χ2 tests. Independent associations were assessed using binary logistic regression. A subgroup analysis was conducted in isolated CHD cases (no extracardiac structural anomalies). Results: A total of 146 fetuses with prenatal CHD were included in the analysis. TOP was recommended in 71 cases (48.6%). GA at diagnosis did not differ between groups when analyzed continuously; however, categorical GA showed significant differences, with earlier diagnoses more frequent among TOP-recommended cases. Cardiac severity distribution differed significantly between groups. In multivariable analysis, GA at diagnosis and cardiac severity were independently associated with TOP recommendation. Compared with <20 weeks, diagnosis at 20–23+6 weeks (OR 17.96, 95% CI 3.50–92.22) and ≥24 weeks (OR 3.92, 95% CI 1.53–10.06) increased the odds of TOP recommendation. Relative to high severity, moderate (OR 0.23, 95% CI 0.07–0.72) and low severity (OR 0.20, 95% CI 0.08–0.50) were associated with lower odds of TOP recommendation. Extracardiac anomalies, genetic findings, and FGR were not independently associated after adjustment. Similar patterns were observed in isolated CHD cases. Conclusions: In a multidisciplinary prenatal counseling setting, TOP recommendations after prenatal CHD diagnosis were primarily driven by cardiac severity and GA at diagnosis, rather than extracardiac or genetic findings alone.
Full article
(This article belongs to the Section Obstetrics & Gynecology)
►▼
Show Figures
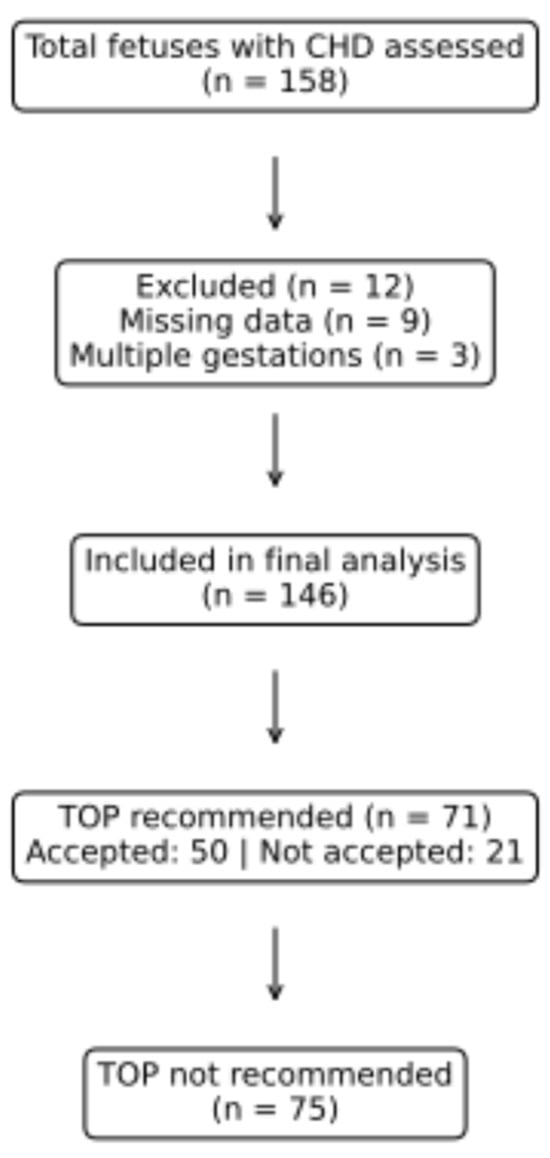
Figure 1
Open AccessReview
Hepatitis E in Thailand: From Seroprevalence to Foodborne and Transfusion-Associated Risks
by
Yong Poovorawan, Sitthichai Kanokudom, Pornjarim Nilyanimit and Jiratchaya Puenpa
J. Clin. Med. 2026, 15(8), 2837; https://doi.org/10.3390/jcm15082837 (registering DOI) - 9 Apr 2026
Abstract
Background: Hepatitis E virus (HEV) is an increasingly recognized cause of acute viral hepatitis in Thailand as the burden of hepatitis A, B, and C has declined. HEV is a positive-sense RNA virus in the family Hepeviridae with three major open reading frames
[...] Read more.
Background: Hepatitis E virus (HEV) is an increasingly recognized cause of acute viral hepatitis in Thailand as the burden of hepatitis A, B, and C has declined. HEV is a positive-sense RNA virus in the family Hepeviridae with three major open reading frames encoding replication proteins (ORF1), the capsid protein (ORF2), and an accessory protein involved in viral egress (ORF3). Unlike highly endemic regions where genotypes 1 and 2 are linked to waterborne outbreaks, infections in Thailand are reported mainly as sporadic cases associated with zoonotic transmission, most commonly genotype 3. Objectives: This review summarizes the epidemiology, transmission routes, and public health implications of HEV infection in Thailand. Methods: Peer-reviewed studies on HEV seroprevalence, molecular epidemiology, and transmission in Thailand were identified through PubMed using combinations of the keywords “HEV” and “Thailand”. Two investigators independently screened titles, abstracts, and full texts. Eligible studies were synthesized qualitatively. Results: Earlier studies suggested low population exposure, but more recent evidence indicates substantial cumulative risk. A nationwide survey among blood donors reported anti-HEV IgG seroprevalence of about 30%, with geographic variation and increasing prevalence with age. Detection of HEV RNA in pigs, slaughterhouse environments, and retail pork products, together with links to raw or undercooked pork consumption, supports pigs as the principal reservoir and foodborne exposure as an important route. Transfusion-associated infection has also been documented. Conclusions: In Thailand, HEV infection is linked mainly to zoonotic and foodborne transmission involving genotype 3. Stronger surveillance, food safety measures, and risk-based blood safety policies are needed.
Full article
(This article belongs to the Special Issue Advances in Hepatitis: Prevention, Treatment, and Global Health Impact)
►▼
Show Figures

Figure 1
Open AccessArticle
Five-Year Changes in Pachydrusen with Late-Phase Hyperfluorescence on Indocyanine Green Angiography
by
Hiroyuki Kamao, Katsutoshi Goto, Kenichi Mizukawa, Ryutaro Hiraki, Atsushi Miki and Shuhei Kimura
J. Clin. Med. 2026, 15(8), 2836; https://doi.org/10.3390/jcm15082836 (registering DOI) - 9 Apr 2026
Abstract
Background/Objectives: Pachydrusen are a drusen subtype associated with the pachychoroid disease spectrum; however, their long-term natural history and pathophysiological significance remain unclear. We investigated 5-year morphological and topographic changes in pachydrusen using diagnostic criteria incorporating late-phase indocyanine green angiography (ICGA) hyperfluorescence. Methods: This
[...] Read more.
Background/Objectives: Pachydrusen are a drusen subtype associated with the pachychoroid disease spectrum; however, their long-term natural history and pathophysiological significance remain unclear. We investigated 5-year morphological and topographic changes in pachydrusen using diagnostic criteria incorporating late-phase indocyanine green angiography (ICGA) hyperfluorescence. Methods: This retrospective observational study included fellow eyes with pachydrusen from patients with unilateral neovascular age-related macular degeneration. Pachydrusen were defined as sub-retinal pigment epithelium (RPE) deposits ≥ 125 µm in size with corresponding hyperfluorescence on late-phase ICGA. Lesion number, size, and spatial distribution (ETDRS grid and quadrant-based classification) were evaluated at baseline and 5 years. The incidence of macular neovascularization (MNV) and its colocalization with pachydrusen were assessed. Results: Among 57 fellow eyes with pachydrusen, incident MNV developed in 8 eyes (14.0%) during follow-up; the mean time to onset was 25.6 ± 16.3 months. No clear colocalization between pachydrusen and incident MNV was observed. Nineteen eyes completed the 5-year follow-up period. Pachydrusen were predominantly located outside the 6000 µm ETDRS grid at baseline (63.4%) and 5 years (66.3%), significantly exceeding the expected proportion based on the area ratio (p < 0.001). The lesions were most frequently observed in the superotemporal quadrant (52.6%). Over 5 years, 19.8% of the lesions increased in size, 67.2% remained stable, and 12.9% regressed; none of the regressed lesions were accompanied by RPE atrophy. Conclusions: Pachydrusen, defined as late-phase ICGA hyperfluorescence, was predominantly distributed outside the ETDRS grid with a superotemporal predilection and could increase or decrease over a 5-year follow-up period. No colocalization with MNV was observed, and no accompanying RPE atrophy after pachydrusen regression was identified, suggesting that late-phase ICGA–hyperfluorescent pachydrusen may represent a pathophysiology distinct from that of soft drusen.
Full article
(This article belongs to the Special Issue Advances in the Diagnosis and Management of Age-Related Macular Degeneration: 3rd Edition)
►▼
Show Figures

Figure 1
Open AccessArticle
Psychometric Properties of Pain Catastrophizing Scale in Patients with Carpometacarpal Osteoarthritis of Thumb—Item Response Theory Analysis
by
Sara Suomela, Mikhail Saltychev, Juhani Juhola and Hanna-Stiina Taskinen
J. Clin. Med. 2026, 15(8), 2835; https://doi.org/10.3390/jcm15082835 - 8 Apr 2026
Abstract
Objectives: The aim of this study was to evaluate the psychometric properties of the Pain Catastrophizing Scale (PCS) in patients with carpometacarpal osteoarthritis of the thumb. Methods: In this cross-sectional register-based study of 253 patients with carpometacarpal osteoarthritis of the thumb, a two-parameter
[...] Read more.
Objectives: The aim of this study was to evaluate the psychometric properties of the Pain Catastrophizing Scale (PCS) in patients with carpometacarpal osteoarthritis of the thumb. Methods: In this cross-sectional register-based study of 253 patients with carpometacarpal osteoarthritis of the thumb, a two-parameter item response theory analysis was used to evaluate the items’ difficulty and discrimination parameters. Results: Of 253 patients, 245 (57%) were women. The mean age was 56.0 (SD 16.5) years. The mean total PCS score was 14.0 (SD 10.5) points. Difficulty estimates were distributed fairly evenly across the item score scale, with a slight shift towards higher scores. Discrimination of both total and subscale scores was perfect, varying from 1.91 to 2.84. Conclusions: PCS was able to discriminate well between different levels of catastrophizing. PCS performed slightly more accurately when the catastrophizing level was above average in the studied sample. PCS can be recommended for clinical use when assessing catastrophizing in patients with carpometacarpal osteoarthritis of the thumb.
Full article
(This article belongs to the Section Orthopedics)
►▼
Show Figures
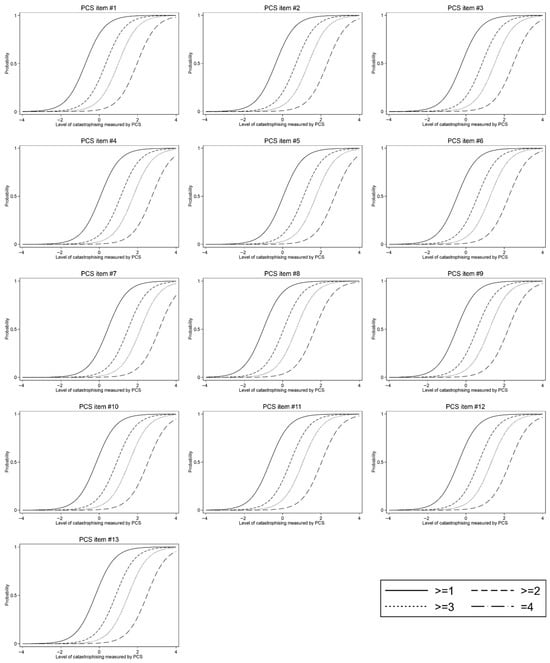
Figure 1
Open AccessArticle
Revolutionizing Pediatric Myopia Care: A Machine Learning Approach for Rapid and Accurate Pre-clinical Screening
by
Siqi Zhang and Qi Zhao
J. Clin. Med. 2026, 15(8), 2834; https://doi.org/10.3390/jcm15082834 - 8 Apr 2026
Abstract
Background/Objective: Myopia has become a prominent public health issue in China, significantly impacting the visual health of children and adolescents. The condition is characterized by a high incidence rate, increasing prevalence, and a trend toward earlier onset, highlighting the critical need for early
[...] Read more.
Background/Objective: Myopia has become a prominent public health issue in China, significantly impacting the visual health of children and adolescents. The condition is characterized by a high incidence rate, increasing prevalence, and a trend toward earlier onset, highlighting the critical need for early and accurate diagnosis. Current clinical diagnostic methods primarily depend on subjective evaluations by optometrists and the use of isolated parameters, leading to inefficiencies and inconsistent outcomes. Moreover, there remains a lack of diagnostic tools that can effectively integrate multi-parameter analysis while ensuring robust data privacy protection. This study aims to develop an artificial intelligence (AI) diagnostic model that achieves objective, accurate, and safe diagnosis of myopia in children without cycloplegia through multi-parameter fusion and to enable local deployment. The proposed model is intended to be a reliable tool for clinical applications and large-scale screening projects, while ensuring strong protection of patient privacy. Methods: We built a transparent, rule-driven AI framework using clinical guidelines. Key ocular parameters—visual acuity, spherical equivalent, axial length, corneal curvature, and axial ratio—were encoded as logical rules in Python and incorporated via instruction fine-tuning. The model was trained and validated on retrospective clinical data (70% training, 15% validation, 15% test) using five algorithms: gradient boosting, logistic regression, random forest, SVM, and XGBoost. Performance was evaluated using accuracy, precision, recall, F1 score, and mean AUC across classes. Results: The model classifies refractive status into five categories: hyperopia, pre-myopia, mild, moderate, and high myopia. All five different algorithms demonstrated excellent diagnostic and classification performance. Gradient boosting achieved the best overall performance, with an accuracy of 98.67%, an F1 score of 98.67%, and a mean AUC of 0.957—outperforming all other models. Conclusions: This study successfully developed an artificial intelligence-based myopia diagnosis system for children under non-dilated pupil conditions. The system is interpretable and privacy-preserving, and has excellent diagnostic and classification performance, making it suitable for clinical decision support and large-scale screening applications. It has great potential to promote the development of early intervention, precision prevention, and control strategies for childhood myopia.
Full article
(This article belongs to the Section Ophthalmology)
Open AccessArticle
Neurological Severity Versus Biomarker Dynamics in Post-Stroke Dysphagia: A Dual-Pathway Model for Functional Recovery and Feeding Transition
by
Merve Savas, Senanur Kahraman Begen, Mehmet Serif Onen and Hafize Uzun
J. Clin. Med. 2026, 15(8), 2833; https://doi.org/10.3390/jcm15082833 - 8 Apr 2026
Abstract
Background: Post-stroke dysphagia is a frequent complication associated with aspiration, malnutrition, and prolonged dependence on enteral feeding. Systemic inflammation and impaired nutritional status may adversely affect neuromuscular recovery; however, their relative and combined associations with swallowing recovery and transition from enteral to oral
[...] Read more.
Background: Post-stroke dysphagia is a frequent complication associated with aspiration, malnutrition, and prolonged dependence on enteral feeding. Systemic inflammation and impaired nutritional status may adversely affect neuromuscular recovery; however, their relative and combined associations with swallowing recovery and transition from enteral to oral feeding remain insufficiently characterized. Objective: This study aimed to examine the independent associations of inflammatory and nutritional indices with swallowing function recovery and to evaluate their relationship with enteral-to-oral feeding transition in patients with post-stroke dysphagia. Methods: In this retrospective observational study, patients with dysphagia following ischemic stroke were evaluated before (T0) and after (T1) routine dysphagia rehabilitation. Inflammatory indices including the neutrophil-to-lymphocyte ratio (NLR), platelet-to-lymphocyte ratio (PLR), systemic immune–inflammation index (SII), systemic inflammation response index (SIRI), and pan-immune–inflammation value (PIV), as well as the prognostic nutritional index (PNI), were calculated at both time points. Changes in indices (Δ = T1 − T0) were analyzed in relation to changes in swallowing function assessed by the Functional Oral Intake Scale (FOIS) and the Penetration–Aspiration Scale (PAS). Results: Changes in PNI were independently associated with greater improvement in functional oral intake (ΔFOIS) and reductions in aspiration severity for both liquid and soft consistencies (ΔPAS; all p < 0.01). In contrast, changes in inflammatory indices (ΔSIRI, ΔSII, ΔPLR, and ΔPIV) were consistently associated with less favorable swallowing outcomes. In multivariable logistic regression analysis, baseline stroke severity (NIHSS) was the only independent determinant of transition from enteral to oral feeding (OR = 0.72, p = 0.002). The model demonstrated good discrimination (AUC = 0.81). Conclusions: Changes in nutritional status, as reflected by ΔPNI over time, were the biomarker most consistently associated with functional swallowing recovery and reduced aspiration severity in patients with post-stroke dysphagia. While inflammatory burden was associated with less favorable swallowing physiology, transition from enteral to oral feeding appeared to be primarily driven by neurological severity rather than inflammatory or nutritional indices alone. These findings may support the clinical value of monitoring nutritional reserve alongside inflammatory burden during dysphagia rehabilitation.
Full article
(This article belongs to the Special Issue Advances in Neurological Rehabilitation: Innovations and Clinical Insights)
►▼
Show Figures

Figure 1
Open AccessReview
Endoscopy for Metabolic Diseases
by
Maria Valeria Matteo, Jana Kefah Ibrahim Hussein, Giorgio Carlino, Vincenzo Bove, Valerio Pontecorvi, Loredana Gualtieri, Martina De Siena, Mariachiara Di Vincenzo, Lorenzo Zileri Dal Verme, Daniele Salvi, Clarissa Ferrari, Cristiano Spada and Ivo Boskoski
J. Clin. Med. 2026, 15(8), 2832; https://doi.org/10.3390/jcm15082832 - 8 Apr 2026
Abstract
Endoscopic bariatric and metabolic therapies (EBMTs) offer minimally invasive treatment options for obesity and related metabolic disorders such as type 2 diabetes mellitus (T2DM) and metabolic dysfunction-associated steatotic liver disease (MASLD). These therapies are broadly categorized into gastric and small bowel interventions. Gastric
[...] Read more.
Endoscopic bariatric and metabolic therapies (EBMTs) offer minimally invasive treatment options for obesity and related metabolic disorders such as type 2 diabetes mellitus (T2DM) and metabolic dysfunction-associated steatotic liver disease (MASLD). These therapies are broadly categorized into gastric and small bowel interventions. Gastric EBMTs, including intragastric balloons and endoscopic sleeve gastroplasty, promote weight loss primarily through mechanical restriction and delayed gastric emptying, thereby improving metabolic outcomes. Small bowel therapies target the proximal intestine to modulate nutrient-sensing and hormonal pathways, providing metabolic benefits that may occur independently of weight loss. Techniques such as duodenal mucosal resurfacing, electroporation-based re-cellularization, and duodenal-jejunal bypass liners demonstrate promising effects on glycemic control, insulin sensitivity, and liver health. Emerging technologies utilizing thermal, vapor, and laser ablation further expand therapeutic possibilities. While these interventions show favorable safety profiles and potential as standalone or adjunctive treatments, further long-term studies and randomized trials are necessary to optimize patient selection and procedural protocols. Collectively, EBMTs represent an evolving paradigm in the management of obesity and metabolic diseases, bridging the gap between conservative medical therapies and bariatric surgery.
Full article
(This article belongs to the Special Issue Novel Developments in Digestive Endoscopy)
►▼
Show Figures
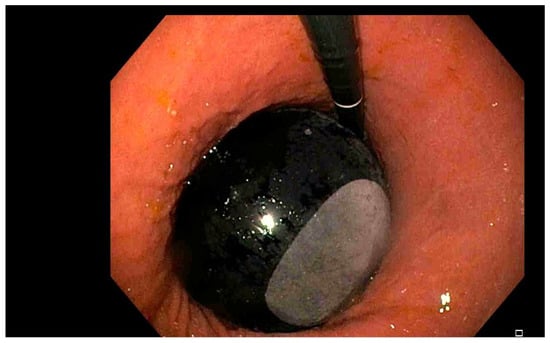
Figure 1
Open AccessArticle
Evaluation of Inpatient Surveillance After High-Energy Accident Without Apparent Serious Injury: Retrospective Analysis of Necessary Interventions and Their Predictors
by
Andreas Gather, Alexandra Braun, Matthias K. Jung von Landenberg, Paul Alfred Gruetzner and Philipp Raisch
J. Clin. Med. 2026, 15(8), 2831; https://doi.org/10.3390/jcm15082831 - 8 Apr 2026
Abstract
Background/Objectives: Patients involved in high-energy accidents (HEAs) are frequently admitted for inpatient surveillance despite normal clinical examination and imaging, although the yield of this practice is uncertain. This study evaluated the frequency and nature of clinical events, interventions during surveillance and missed injuries
[...] Read more.
Background/Objectives: Patients involved in high-energy accidents (HEAs) are frequently admitted for inpatient surveillance despite normal clinical examination and imaging, although the yield of this practice is uncertain. This study evaluated the frequency and nature of clinical events, interventions during surveillance and missed injuries in such low-risk patients and explored potential predictors. Methods: Retrospective study at a Level I trauma center including patients ≥18 years admitted between January 2022 and September 2023 solely due to HEA mechanism, without apparent injury requiring inpatient treatment. Baseline characteristics, clinical presentation, imaging findings, and laboratory values were extracted. Outcomes included additional diagnostics, new diagnoses, therapeutic interventions, and missed injuries. Patients with eventful and uneventful stays were compared using univariate statistical tests. Results: Among 363 included patients, 86.0% experienced an uneventful stay. Fifty-one patients (14.0%) had an eventful stay, most commonly requiring additional radiological examinations (8.5%) or blood tests (6.9%). New diagnoses occurred in 6.6%, and 6.1% received additional therapeutic interventions. Missed injuries were detected in 3.9%, including two potentially life-threatening injuries (0.6%). No robust predictors for missed injuries were identified. Established predictors of missed injuries from broader trauma populations were absent in this selected low-risk cohort. However, individuals after bicycle accidents were significantly more likely to experience any event during their stay (p = 0.009). Conclusions: Inpatient surveillance of patients without apparent injury after HEAs has a low overall yield but occasionally identifies clinically significant conditions. As no reliable predictors for adverse events were found, selective admission remains challenging. Hybrid models combining short-term observation with structured outpatient reassessment may represent a resource-efficient alternative for low-risk patients.
Full article
(This article belongs to the Special Issue Assessment and Treatment of Trauma Patients)
Open AccessArticle
Efficacy of Large Language Models for Screening of Systematic Reviews on Periprosthetic Joint Infection
by
Woojin Shin, Jaeyoung Hong, Sunwoo Lee, Seongchan Park, Hyoungtae Kim and Suenghwan Jo
J. Clin. Med. 2026, 15(8), 2830; https://doi.org/10.3390/jcm15082830 - 8 Apr 2026
Abstract
Background: Periprosthetic joint infection (PJI) remains a devastating complication following arthroplasty. Systematic reviews of PJI provide essential evidence to inform clinical practice; however, the screening process remains labor-intensive. Recent advancements in large language models (LLMs) offer potential for automating literature screening, though
[...] Read more.
Background: Periprosthetic joint infection (PJI) remains a devastating complication following arthroplasty. Systematic reviews of PJI provide essential evidence to inform clinical practice; however, the screening process remains labor-intensive. Recent advancements in large language models (LLMs) offer potential for automating literature screening, though evaluation of current generation models is needed. Methods: This validation study evaluated GPT-5, GPT-5 Pro, and Gemini 2.5 Pro in replicating the title/abstract and full-text screening stages of a published systematic review on intraosseous versus intravenous antibiotic prophylaxis in total joint arthroplasty. Title/abstract screening was performed on 165 articles, followed by a full-text eligibility assessment of 26 articles. Accuracy, sensitivity, specificity, and Cohen’s kappa (κ) were calculated against human screening decisions as the gold standard. Results: In title/abstract screening, GPT-5 Pro achieved the highest accuracy (92.1–92.7%) and specificity (98.6–99.3%), while GPT-5 demonstrated the highest sensitivity (84.6–96.1%). In full-text screening, Gemini 2.5 Pro showed the most consistent performance across repeated evaluations (κ = 0.839 in both trials), whereas GPT-5 Pro exhibited marked intra-model variability (κ = 0.399 to 0.920). Conclusions: Current-generation LLMs achieve near-human accuracy in systematic review screening for PJI research, though substantial intra-model variability underscores the continued need for human oversight in systematic review workflows.
Full article
(This article belongs to the Section Orthopedics)
►▼
Show Figures

Figure 1
Open AccessArticle
Comparison of Endoscopic and Intraoperative Approaches in the Management of Delayed Gastric Conduit Emptying After Minimally Invasive Esophagectomy: A Single-Center Retrospective Analysis
by
Ramin Raul Ossami Saidy, Philippa Seika, Max M. Maurer, Paul Viktor Ritschl, Matthias Biebl, Dino Kröll, Johann Pratschke and Christian Denecke
J. Clin. Med. 2026, 15(8), 2829; https://doi.org/10.3390/jcm15082829 - 8 Apr 2026
Abstract
Introduction: As multimodal therapy for esophageal cancer advances, addressing immediate and long-term functional outcomes following surgery has become more important. Despite surgical advancements, delayed gastric conduit emptying (DGCE) remains a primary cause of functional impairment after esophageal cancer resection. The literature addressing pylorus
[...] Read more.
Introduction: As multimodal therapy for esophageal cancer advances, addressing immediate and long-term functional outcomes following surgery has become more important. Despite surgical advancements, delayed gastric conduit emptying (DGCE) remains a primary cause of functional impairment after esophageal cancer resection. The literature addressing pylorus management following minimally invasive esophagectomy (MIE) is scarce. The effects of pyloric drainage with pyloromyotomy or postoperative approaches such as intrapyloric Botox injection or dilatation on the incidence and course of DGCE were the focus of this study. Methods: A retrospective analysis of consecutive patients after minimally invasive esophagectomy with thoracic esophagogastric anastomosis and gastric tube reconstruction between 2014 and 2023 was performed. Univariate analyses were used to identify significant patient-, tumor-, and procedure-related factors affecting DGCE. Results: A total of 276 patients were included. DGCE was observed in 80 (28.9%) patients. Demographics did not differ with statistical significance. Postoperative complications were not increased in patients with DGCE. Pyloric intervention (PI) did not reduce postoperative occurrence of DGCE (PI: n = 19/23.75% compared to no PI: n = 62 (30.5%), p = 0.342). Median length of hospital stay was significantly longer, and total costs were significantly higher in patients with DGCE (p = 0.03 and p = 0.047, respectively). Analysis of endoscopic approaches was not associated with a statistically significant difference between botulinum toxin injection and pyloric dilatation with regard to reinterventions. Conclusions: While DGCE is frequent after esophagectomy, it is not associated with short-term morbidity but with prolonged total hospital stay and increased costs. Intraoperative pyloric intervention does not influence the incidence of DGCE after esophagectomy and endoscopic management was associated with therapeutic success, but choice of specific, optimal approach remains elusive. Novel concepts, including preoperative dilatation should be investigated.
Full article
(This article belongs to the Special Issue Esophageal and Upper Gastrointestinal Surgery: Clinical Advances and Practical Updates)
Open AccessReview
Periodontal Status of Patients with Celiac Disease and Non-Celiac Gluten Sensitivity: A Literature Review
by
Thaleia Angelopoulou and Yiorgos A. Bobetsis
J. Clin. Med. 2026, 15(8), 2828; https://doi.org/10.3390/jcm15082828 - 8 Apr 2026
Abstract
Background/Objectives: Celiac disease (CD) is a chronic, immune-mediated enteropathy induced by dietary gluten exposure in genetically predisposed individuals. Along with non-celiac gluten sensitivity (NCGS), these disorders present with multiple intestinal and extra-intestinal symptoms leading to multisystemic involvement, with complications documented in the
[...] Read more.
Background/Objectives: Celiac disease (CD) is a chronic, immune-mediated enteropathy induced by dietary gluten exposure in genetically predisposed individuals. Along with non-celiac gluten sensitivity (NCGS), these disorders present with multiple intestinal and extra-intestinal symptoms leading to multisystemic involvement, with complications documented in the oral cavity as well. Persistent immune activation and dysregulation, chronic inflammation, nutrient deficiencies, xerostomia, and microbial dysbiosis found in CD and NCGS constitute shared pathological findings, providing biological plausibility for an association with periodontitis. Methods: A narrative literature review was conducted based on a systematic search of four databases (PubMed, Scopus, Web of Science, Cochrane Library) and the gray literature through January 2026. A comprehensive set of clinical, radiographic, biochemical and immunological parameters was assessed. Two reviewers independently screened and selected studies, with disagreements resolved by consensus. Results: A total of 15 studies met the eligibility criteria and were included in the review. Available evidence, mainly derived from cross-sectional observational studies, remains limited, methodologically heterogeneous, and largely inconclusive. Across adult and pediatric populations, findings do not consistently demonstrate a clinically meaningful association between CD or NCGS and periodontal inflammation, irrespective of gluten-free diet (GFD) adherence. Observed differences, when reported, are modest and inconsistent, and can be mainly attributed to oral hygiene behaviors and dental visit patterns. Conclusions: Despite considerable biological plausibility linking gluten-related disorders with periodontal inflammation, current evidence does not support a definitive conclusion regarding the impact of CD or NCGS on periodontal health.
Full article
(This article belongs to the Section Dentistry, Oral Surgery and Oral Medicine)
►▼
Show Figures
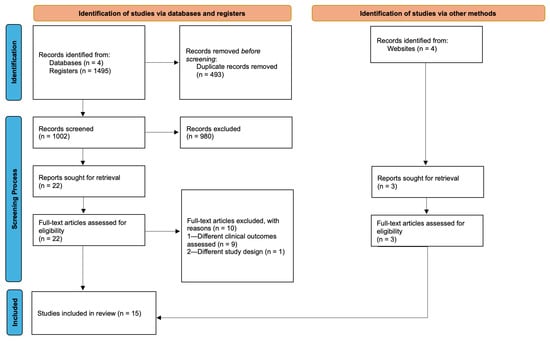
Figure 1
Open AccessArticle
Pregnancy Complications in Uterine Anomalies—A Pilot Study
by
Claudiu Voic, Melinda Ildiko Mitranovici, Septimiu Voidazan, Cezara Maria Mureşan and Elene Silvia Bernad
J. Clin. Med. 2026, 15(8), 2827; https://doi.org/10.3390/jcm15082827 - 8 Apr 2026
Abstract
Uterine malformation represents a rare disease with a prevalence of up to 7% of the general population. Background/Objectives: Higher pregnancy complication rates have been reported in the literature; thus, in our study, we aimed to examine not only the obstetric complications encountered
[...] Read more.
Uterine malformation represents a rare disease with a prevalence of up to 7% of the general population. Background/Objectives: Higher pregnancy complication rates have been reported in the literature; thus, in our study, we aimed to examine not only the obstetric complications encountered but also the psychological interventions and multidisciplinary approaches for parental counseling in our department in the context of preterm birth at the limit of viability. Methods: A retrospective pilot study was conducted on all the women in our department between 2010 and 2017 with congenital uterine malformations associated with infertility or pregnancy. In the study group, we included women with AUCs (n = 26), while the control group included pregnant women with normal uteri (n = 25) (total: n = 51), and then pregnancy complications were investigated. Results: Highly significant pregnancy complications were observed in the study group, the most important being preterm birth (p = 0.003) in comparison with the control group. Out of 26 patients with AUCs, only 14 gave birth to a live fetus compared to 22 out of the 25 with normal pregnancies, meaning that failure to give birth to a live newborn statistically significantly increased among the former group (p = 0.004). In terms of birth weight (p = 0.0001), Apgar score (p = 0.029) and intensive care unit admission (p = 0.0001), we observed significant differences between the newborns in the study group versus controls, with an impact on mental state that required psychological support. Conclusions: A clear correlation was observed in our study between uterine congenital malformations and pregnancy complications. The most common pregnancy outcome was premature delivery, with statistical significance. In addition, higher neonate admissions to the intensive care unit associated with lower Apgar scores were encountered compared with normal pregnancies. Appropriate parental counseling by obstetricians, neonatologists and psychologists could enhance pregnancy outcomes.
Full article
(This article belongs to the Special Issue Pregnancy and Delivery Complications: Bridging Research and Clinical Practice)
Open AccessReview
Exercise-Based Cardiac Rehabilitation for Peripheral Artery Disease
by
Francesco Giallauria, Mario Pacileo, Gianluigi Cuomo, Giuseppe Vallefuoco, Fabrizio Catalini, Crescenzo Testa, Cristina Savarese, Alfredo Mauriello, Carmine Izzo, Michele Ciccarelli, Vincenzo Russo and Antonello D’Andrea
J. Clin. Med. 2026, 15(8), 2826; https://doi.org/10.3390/jcm15082826 - 8 Apr 2026
Abstract
Peripheral artery disease (PAD) is a pervasive atherosclerotic condition affecting well over 100 million adults worldwide and associated with major functional limitations, reduced quality of life, and elevated risks of myocardial infarction, stroke, limb events, and mortality. Exercise therapy—preferably supervised or delivered through
[...] Read more.
Peripheral artery disease (PAD) is a pervasive atherosclerotic condition affecting well over 100 million adults worldwide and associated with major functional limitations, reduced quality of life, and elevated risks of myocardial infarction, stroke, limb events, and mortality. Exercise therapy—preferably supervised or delivered through structured, monitored home-based programs—is a first-line, guideline-endorsed therapy that improves walking performance and patient-reported outcomes and contributes to comprehensive secondary prevention. This review synthesizes mechanistic underpinnings (endothelial, angiogenic, metabolic, and autonomic) and appraises the comparative effectiveness, safety, and implementation models of supervised exercise therapy (SET), structured home-based and hybrid programs, and alternative modalities in PAD. Finally, we summarize policy aspects and persistent gaps to guide clinical practice and future research.
Full article
(This article belongs to the Section Clinical Rehabilitation)
►▼
Show Figures

Figure 1
Open AccessArticle
Surgical Technique and Oro-Nasal Fistula Formation After Primary Palatoplasty: A Comparative Study of Closed Intravelar and Modified Veau–Wardill–Kilner Techniques
by
Kostadin Gigov, Ivan Ginev, Petra Kavradjieva, Ivaylo Minev and Mariya Miteva
J. Clin. Med. 2026, 15(8), 2825; https://doi.org/10.3390/jcm15082825 - 8 Apr 2026
Abstract
Background: Oro-nasal fistula formation remains one of the most common complications following primary palatoplasty, while the influence of surgical technique on fistula incidence and characteristics remains controversial. This study aimed to compare the occurrence and features of oro-nasal fistulas after two primary
[...] Read more.
Background: Oro-nasal fistula formation remains one of the most common complications following primary palatoplasty, while the influence of surgical technique on fistula incidence and characteristics remains controversial. This study aimed to compare the occurrence and features of oro-nasal fistulas after two primary palatal repair techniques. Methods: A retrospective comparative analysis was conducted in patients undergoing one-stage primary palatoplasty using either closed intravelar palatoplasty or a modified Veau–Wardill–Kilner pushback technique. Oro-nasal fistulas were evaluated according to presence, size, anatomical location, and functional impact. Secondary corrective procedures, including fistula repair and pharyngoplasty, were also analyzed. Results: Oro-nasal fistula formation was significantly associated with the surgical technique. Closed intravelar palatoplasty demonstrated a significantly lower fistula rate compared with the modified Veau–Wardill–Kilner technique. Cleft type and syndromic status were not independently associated with fistula development. Rates of secondary corrective procedures and pharyngoplasty were significantly lower in the intravelar group. Conclusions: Surgical technique plays a decisive role in oro-nasal fistula development after primary palatoplasty. Muscle-oriented repair with limited incisions is associated with reduced fistula formation and a lower need for secondary surgical interventions.
Full article
(This article belongs to the Section Plastic, Reconstructive and Aesthetic Surgery/Aesthetic Medicine)
►▼
Show Figures
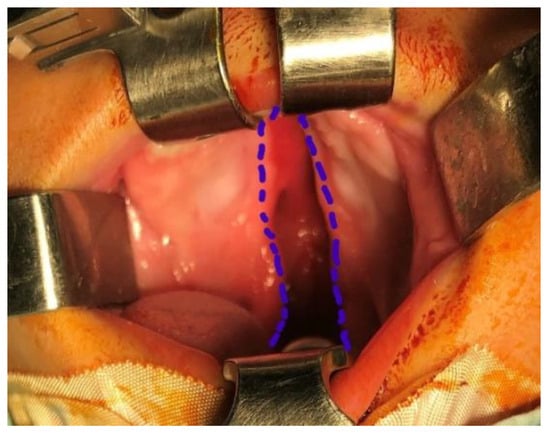
Figure 1
Open AccessSystematic Review
Gynecologic Malignancies in Obstructed Hemivagina and Ipsilateral Renal Anomaly (OHVIRA) Syndrome: A Systematic Review
by
Giuseppe Parisi, Emanuele Perrone, Ilaria Capasso, Matteo Bruno, Maria Consiglia Giuliano, Nicola Macellari, Marco D’Indinosante and Francesco Fanfani
J. Clin. Med. 2026, 15(8), 2824; https://doi.org/10.3390/jcm15082824 - 8 Apr 2026
Abstract
Background: Obstructed hemivagina and ipsilateral renal anomaly (OHVIRA) syndrome, also known as Herlyn–Werner–Wunderlich syndrome (HWWS), is a rare Müllerian malformation. Gynaecologic malignancies reported in association with OHVIRA syndrome/HWWS are exceptional and scattered across isolated case reports and small case series, leading to significant
[...] Read more.
Background: Obstructed hemivagina and ipsilateral renal anomaly (OHVIRA) syndrome, also known as Herlyn–Werner–Wunderlich syndrome (HWWS), is a rare Müllerian malformation. Gynaecologic malignancies reported in association with OHVIRA syndrome/HWWS are exceptional and scattered across isolated case reports and small case series, leading to significant challenges for screening, early diagnosis, and optimal management. The primary aim of this study was to comprehensively review and synthesize the clinicopathologic features, treatment approaches, and reported outcomes of patients with OHVIRA-associated gynaecologic neoplasms. Methods: A systematic review of published cases of gynecologic malignancies in OHVIRA/HWWS was conducted using PubMed/MEDLINE and Scopus from database inception through January 2026. To expand the current evidence, an illustrative novel institutional case is also presented and integrated into the analysis. Results: A total of 21 cases were identified and analysed; reported tumours predominantly involved the lower genital tract (vagina/cervix), with a recurrent representation of adenocarcinoma, particularly clear cell histology, and a frequent origin from the obstructed or non-visible compartment when side was described. Endometrial and ovarian involvement was uncommon. Conclusions: The anatomical complexity of OHVIRA syndrome creates a diagnostic blind spot that warrants heightened clinical suspicion, rigorous MRI-based anatomic delineation, and side-specific evaluation in symptomatic patients. By synthesizing the available literature, this review underscores the necessity for tailored, multidisciplinary management and proactive surveillance strategies in this rare population.
Full article
(This article belongs to the Special Issue Emerging Diagnostic and Treatment Approaches for Gynecological Cancers)
►▼
Show Figures
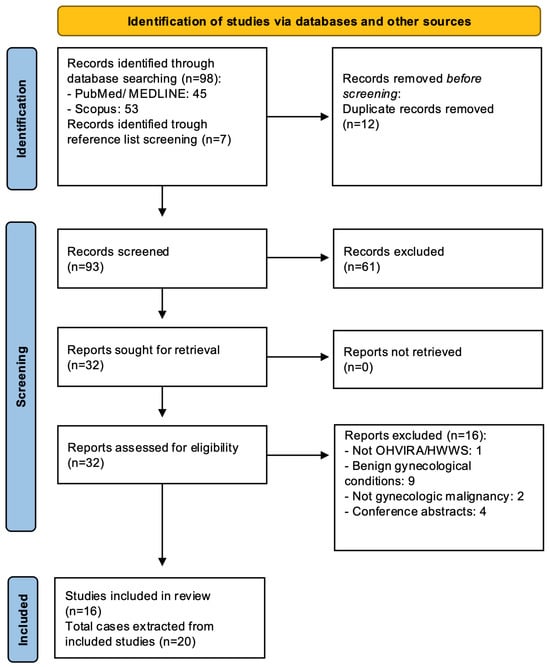
Figure 1
Open AccessCase Report
A Rare Pediatric Presentation: Concurrent Detection of All Five Hepatitis B Virus (HBV) Serological Markers
by
Menglan Zhang, Wensheng Li, Zhengxiang Gao and Chenxi Liu
J. Clin. Med. 2026, 15(8), 2823; https://doi.org/10.3390/jcm15082823 - 8 Apr 2026
Abstract
Background: This case report presents a 12-year-old male with vertically transmitted chronic hepatitis B virus (HBV) infection, exhibiting a rare pan-reactive serological profile (concurrent HBsAg, HBsAb, HBeAg, HBeAb, and HBcAb positivity) alongside fluctuating low-level viremia (HBV DNA: 1.06 × 102 IU/mL to
[...] Read more.
Background: This case report presents a 12-year-old male with vertically transmitted chronic hepatitis B virus (HBV) infection, exhibiting a rare pan-reactive serological profile (concurrent HBsAg, HBsAb, HBeAg, HBeAb, and HBcAb positivity) alongside fluctuating low-level viremia (HBV DNA: 1.06 × 102 IU/mL to undetectable). Rigorous exclusion of technical artifacts confirmed the authenticity of this atypical serologic pattern, observed in <0.001% of the general population. Methods: Liver biopsy and immunohistochemical staining were performed to evaluate hepatic inflammation and fibrosis. HBV serological markers and viral load were quantified using commercial diagnostic kits, with longitudinal monitoring for 18 months. Results: Liver biopsy revealed Grade 2 inflammation with focal HBsAg/HBcAg expression, supporting immune-active chronic hepatitis B (CHB) despite partial seroconversion. The patient’s clinical course highlights key challenges in pediatric HBV management: (1) delayed immune reconstitution (18-month longitudinal HBeAg/HBeAb dynamics), (2) non-linear virologic-ALT correlation, and (3) diagnostic ambiguity in pan-positive serology—potentially reflecting S-gene escape mutants or transitional immune responses. Initiation of tenofovir disoproxil fumarate (TDF) achieved sustained virologic suppression, underscoring the importance of early antiviral therapy in pediatric CHB with atypical markers. Conclusions: This case provides preliminary insights into the complex interplay between viral evolution and immature host immunity, advocating for refined monitoring protocols integrating high-sensitivity HBV DNA, quantitative serology, and non-invasive fibrosis assessment in pediatric HBV care.
Full article
(This article belongs to the Section Clinical Pediatrics)
►▼
Show Figures

Figure 1
Open AccessArticle
Impact of In-House 3D-Printed Models on Re-Operation Rates and Volumetric Precision in Orbital Floor Reconstruction: A Comparative Study
by
Ilze Prikule, Ieva Bagante, Oskars Radzins and Girts Salms
J. Clin. Med. 2026, 15(8), 2822; https://doi.org/10.3390/jcm15082822 - 8 Apr 2026
Abstract
Background/Objectives: Reconstruction of orbital floor fractures remains surgically challenging due to limited intraoperative visibility and complex anatomy. Inaccurate implant placement often leads to persistent complications and the need for a revision surgery. This study evaluated the clinical accuracy and re-operation rates of
[...] Read more.
Background/Objectives: Reconstruction of orbital floor fractures remains surgically challenging due to limited intraoperative visibility and complex anatomy. Inaccurate implant placement often leads to persistent complications and the need for a revision surgery. This study evaluated the clinical accuracy and re-operation rates of a preoperative 3D-printed model-assisted technique compared to the conventional intraoperative free-hand mesh bending method. Methods: A comparative ambispective study was conducted on 74 patients with isolated orbital floor fractures. The control group (n = 34, retrospective) underwent reconstruction using intraoperatively formed titanium meshes. In the study group (n = 40, prospective), patient-specific 3D-printed models, created by mirroring the healthy contralateral orbit, were used for preoperative mesh adaptation. Primary outcomes included the rate of revision surgery due to implant malposition, changes in orbital volume, and postoperative diplopia. Results: The 3D model group demonstrated a significantly lower rate of revision surgery compared to the control group. In the retrospective group, 5 patients (15%) required reoperation due to implant malposition, whereas no patients (0%) in the prospective 3D group required secondary intervention (p = 0.017). While both techniques effectively restored orbital volume, the 3D group showed greater volumetric precision with less variance. The mean volume difference in the affected orbit was 3078 ± 2204 mm3 in the control group, compared to 2390 ± 1893 mm3 in the study 3D group. At the 6-month follow-up, persistent diplopia was observed in 12% of the control group compared to only 3% in the study group. Conclusions: The use of in-house 3D-printed models for preoperative mesh forming significantly enhances surgical precision and eliminates the need for revision surgery due to implant malposition. This workflow offers a cost-effective, predictable, and accessible alternative to expensive patient-specific implants (PSIs) or intraoperative navigation systems, improving patient safety and long-term clinical outcomes.
Full article
(This article belongs to the Special Issue Innovations in Maxillofacial Surgery)
►▼
Show Figures
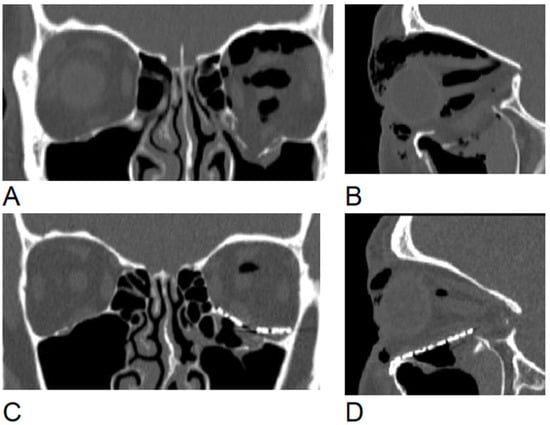
Figure 1
Open AccessSystematic Review
Contraindications to Lateral Extra-Articular Tenodesis: A Systematic Review
by
Jakub Erdmann, Jan Czerwiński, Adam Kwapisz, Maria Zabrzyńska, Gazi Huri, Piotr Walus and Jan Zabrzyński
J. Clin. Med. 2026, 15(8), 2821; https://doi.org/10.3390/jcm15082821 - 8 Apr 2026
Abstract
Background: Lateral extra-articular tenodesis (LET) is a surgical procedure that is additionally implemented in concurrent anterior cruciate ligament reconstruction (ACLR). Although numerous articles have addressed the use of LET in conjunction with ACLR, few definitive contraindications were identified. Given the scarcity of
[...] Read more.
Background: Lateral extra-articular tenodesis (LET) is a surgical procedure that is additionally implemented in concurrent anterior cruciate ligament reconstruction (ACLR). Although numerous articles have addressed the use of LET in conjunction with ACLR, few definitive contraindications were identified. Given the scarcity of literature evaluating contraindications for LET modality, this study aimed to systematically review the reported contraindications of this procedure in the context of concurrent ACLR. Methods: The searched key terms: (extra-articular OR extraarticular) AND (tenodesis OR plasty OR augmentation OR procedure or reconstruction OR reconstructive OR surgical OR surgery OR technique) AND (ACL OR anterior cruciate ligament), with no publication date restrictions in PubMed, ScienceDirect, Cochrane Central, Web of Science, and Embase databases. We included clinical human studies, with levels of evidence I–III and in the English language. Results: The analysis evaluated fourteen articles published between 2012 and 2024. Level III evidence was found in the majority of studies (n = 9) and Level I evidence was found in the rest (n = 5). The majority of the included articles were retrospective (n = 8) and there were also prospective studies (n = 6). The articles reviewed showed that articular cartilage damage and concomitant injuries to other knee ligaments, alongside ACL injury, are the most frequently mentioned. Conclusions: This is the first study that systematized the contraindications for the LET procedure in ACLR. The contraindications remain unclear; however, the following may be highlighted: articular cartilage damage and injury to another ligament in the knee, in addition to ACL injury.
Full article
(This article belongs to the Special Issue Advances in Anterior Cruciate Ligament Injury Treatment)
►▼
Show Figures
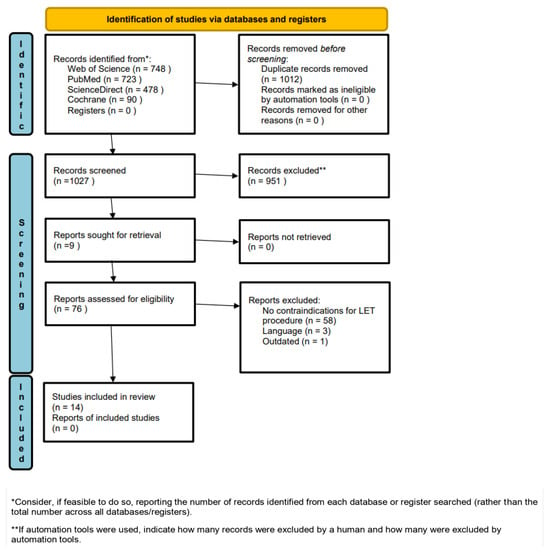
Figure 1
Open AccessArticle
First Experience with Hypothermic Oxygenated Perfusion in Human Uteri: Feasibility and Metabolic Characterization
by
Keyue Sun, Nasim Eshraghi, Fernanda Walsh Fernandes, Sangeeta Satish, Chunbao Jiao, Fatma Selin Yildirim, Geofia Crasta, Omer F. Karakaya, Koki Takase, Hiroshi Horie, Karen S. Keslar, Dylan Isaacson, William Baldwin 3rd, Robert L. Fairchild, Koji Hashimoto, Alejandro Pita, Alvin Wee, Mariam AlHilli, Charles Miller, Mohamed Eltemamy, Tommaso Falcone, Andreas Tzakis, Elliot Richards and Andrea Schlegeladd
Show full author list
remove
Hide full author list
J. Clin. Med. 2026, 15(8), 2820; https://doi.org/10.3390/jcm15082820 - 8 Apr 2026
Abstract
Background: Uterus transplantation (UTx) is an emerging treatment for absolute uterine factor infertility. However, the use of deceased donors is limited, and donation after circulatory death (DCD) has not yet been utilized. Ischemic injury remains a major barrier, particularly compared with living
[...] Read more.
Background: Uterus transplantation (UTx) is an emerging treatment for absolute uterine factor infertility. However, the use of deceased donors is limited, and donation after circulatory death (DCD) has not yet been utilized. Ischemic injury remains a major barrier, particularly compared with living donor procedures. Hypothermic oxygenated perfusion (HOPE), which has shown protective effects in heart, liver, and kidney transplantation, may offer similar benefits for uterine grafts. Methods: We report the first series applying HOPE to human uteri to improve preservation and enable metabolic injury assessment during perfusion. Six uteri (3 DBD, 3 DCD; median donor age 53 years) underwent 8 h of HOPE following procurement, while paired tissue controls were preserved using static cold storage (SCS). Perfusion was delivered using a pressure-controlled system (15 mmHg, 10 ± 1 °C, VitaSmart®). Perfusate and tissue samples were analyzed for mitochondrial injury, inflammation, and transcriptional responses. Results: HOPE maintained stable flows (70–150 mL/min), delivered high oxygen levels (pO2 ≈ 1000 hPa), and increased tissue ATP levels. Stratification based on perfusate flavin mononucleotide (FMN) release identified grafts with greater Complex I/II injury. HOPE was associated with lower levels of mitochondrial injury markers and inflammatory signals, preserved tissue architecture, and promoted gene expression patterns consistent with metabolic recovery compared with paired SCS tissue controls. Conclusions: These findings suggest that HOPE may serve as a preservation approach that enables metabolic and ischemic injury assessment and may facilitate broader use of deceased donor uteri for transplantation.
Full article
(This article belongs to the Special Issue New Advances in Uterus and Ovarian Transplantation: 2nd Edition)
►▼
Show Figures
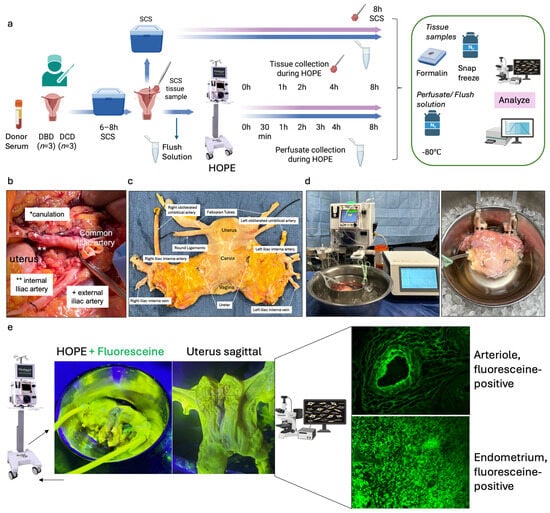
Figure 1

Journal Menu
► ▼ Journal Menu-
- JCM Home
- Aims & Scope
- Editorial Board
- Reviewer Board
- Topical Advisory Panel
- Instructions for Authors
- Special Issues
- Topics
- Sections & Collections
- Article Processing Charge
- Indexing & Archiving
- Editor’s Choice Articles
- Most Cited & Viewed
- Journal Statistics
- Journal History
- Journal Awards
- Society Collaborations
- Conferences
- Editorial Office
Journal Browser
► ▼ Journal BrowserHighly Accessed Articles
Latest Books
E-Mail Alert
News
Topics
Topic in
Applied Sciences, Children, Dentistry Journal, JCM
Preventive Dentistry and Public Health
Topic Editors: Denis Bourgeois, Elena BardelliniDeadline: 30 April 2026
Topic in
Biology, JCM, Diagnostics, Dentistry Journal
Assessment of Craniofacial Morphology: Traditional Methods and Innovative Approaches
Topic Editors: Nikolaos Gkantidis, Carlalberta VernaDeadline: 1 June 2026
Topic in
Cells, JCM, Organoids, JMP
Novel Discoveries in Oncology 2nd Edition
Topic Editors: Michela Campolo, Giovanna Casili, Alessia Filippone, Marika LanzaDeadline: 20 June 2026
Topic in
Biomedicines, IJMS, JCM, Medicina, Neurology International
Advances in Exercise-Induced Neurogenesis, Neuronal and Functional Adaptations in Neurorehabilitation
Topic Editors: Carlos Bernal-Utrera, Cleofas Rodriguez-Blanco, Maria Livia Carrascal MorenoDeadline: 29 June 2026

Conferences
Special Issues
Special Issue in
JCM
Neurosurgery and Spine Surgery: From Up-to-Date Practitioners, 2nd Edition
Guest Editor: Massimiliano VisocchiDeadline: 10 April 2026
Special Issue in
JCM
Advances in Diagnosis and Treatment for Thymic Pathology
Guest Editor: Charalambos ZisisDeadline: 10 April 2026
Special Issue in
JCM
Cesarean Section Versus Vaginal Delivery
Guest Editors: Demetra Gabriela Socolov, Angela Vinturache, Liana PlesDeadline: 10 April 2026
Special Issue in
JCM
Oral and Maxillofacial Surgery: Recent Clinical Advances and Future Directions
Guest Editors: Funda Göker, Gianluca M. Tartaglia, Massimo Del FabbroDeadline: 10 April 2026
Topical Collections
Topical Collection in
JCM
Pediatric and Adolescent Gynecology
Collection Editor: Panagiotis Christopoulos