Journal Description
Neurology International
Neurology International
is an international, peer-reviewed, open access journal which provides an advanced forum for studies related to all aspects of neurology and neuroscience, published monthly online by MDPI (since Volume 12, Issue 3 - 2020). The Panhellenic Federation of Alzheimer's Disease and Related Disorders (PFADRD) is affiliated with Neurology International and its members receive discounts on the article processing charges.
- Open Access— free for readers, with article processing charges (APC) paid by authors or their institutions.
- High Visibility: indexed within Scopus, ESCI (Web of Science), PubMed, PMC, Embase, and other databases.
- Journal Rank: JCR - Q2 (Clinical Neurology)
- Rapid Publication: manuscripts are peer-reviewed and a first decision is provided to authors approximately 21.5 days after submission; acceptance to publication is undertaken in 3.6 days (median values for papers published in this journal in the second half of 2025).
- Recognition of Reviewers: APC discount vouchers, optional signed peer review, and reviewer names published annually in the journal.
- Journal Cluster of Neurosciences: Brain Sciences, Neurology International, NeuroSci, Clinical and Translational Neuroscience, Neuroimaging, Neuroglia, Psychiatry International, Clocks & Sleep and Journal of Dementia and Alzheimer's Disease.
Impact Factor:
3.0 (2024);
5-Year Impact Factor:
3.3 (2024)
Latest Articles
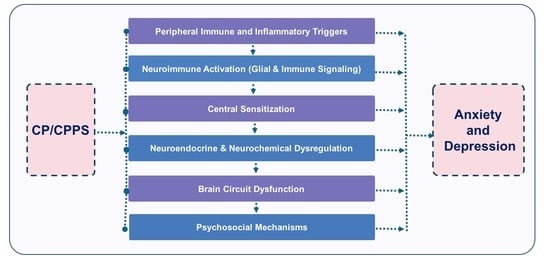
Neurobiology of Anxiety and Depression in CP/CPPS: A Narrative Review of Underlying Mechanisms
Neurol. Int. 2026, 18(4), 69; https://doi.org/10.3390/neurolint18040069 - 13 Apr 2026
Abstract
►
Show Figures
Chronic prostatitis/chronic pelvic pain syndrome (CP/CPPS) is a prevalent urological disorder characterized by persistent pelvic pain, urinary symptoms, and significant impact on quality of life. In addition to its clinical symptoms, CP/CPPS is frequently associated with psychiatric comorbidities, such as anxiety and depression,
[...] Read more.
Chronic prostatitis/chronic pelvic pain syndrome (CP/CPPS) is a prevalent urological disorder characterized by persistent pelvic pain, urinary symptoms, and significant impact on quality of life. In addition to its clinical symptoms, CP/CPPS is frequently associated with psychiatric comorbidities, such as anxiety and depression, indicating complex neurobiological mechanisms. This review explores the mechanisms linking CP/CPPS with affective disorders, emphasizing central nervous system alterations, dysregulation of the hypothalamic–pituitary–adrenal (HPA) axis, and neuroimmune interactions. Evidence in-dicates that central sensitization, microglial and astrocytic activation, and elevated proinflammatory cytokines (IL-1β, IL-6, TNF-α) contribute to maladaptive painemotion network interactions. Additionally, dysregulation of hormones and neurotransmitters may exacerbate both pain perception and mood disorders. Psychosocial factors, including stress, coping strategies, and cognitive-emotional processes, further modulate symptom severity and treatment outcomes, highlighting the importance of a biopsychosocial approach. Gaining a deeper understanding of the neurobiological and psychosocial mechanisms behind anxiety and depression in CP/CPPS can lead to more effective, multidimensional management strategies and enhance patient-centered care.
Full article
Open AccessArticle
Temporal Patterns of Fever Onset as an Indicator of Etiology in Intracerebral Hemorrhage
by
Felix Hess, Enayatullah Baki, Julian McGinnis, Tun Wiltgen, Hannah Scholz, Kathleen Bernkopf, Gerhard Schneider, Jan Kirschke, Dominik Sepp, Bernhard Hemmer, Silke Wunderlich and Mark Mühlau
Neurol. Int. 2026, 18(4), 68; https://doi.org/10.3390/neurolint18040068 - 3 Apr 2026
Abstract
Background: Fever occurs frequently in patients with intracerebral hemorrhage (ICH) and is associated with worse functional outcomes. Rapid identification of the fever’s cause is crucial for guiding diagnostics and treatment. Data on the distribution of different fever causes in ICH are limited, and
[...] Read more.
Background: Fever occurs frequently in patients with intracerebral hemorrhage (ICH) and is associated with worse functional outcomes. Rapid identification of the fever’s cause is crucial for guiding diagnostics and treatment. Data on the distribution of different fever causes in ICH are limited, and the diagnostic value of the day of fever onset remains uncertain. This study aimed to assess the distribution of fever causes in a large cohort of ICH patients and to evaluate whether temporal patterns of fever onset are associated with its underlying cause in a clinically meaningful manner. Methods: This retrospective single-center study included 547 patients with spontaneous ICH. Fever was defined as a body temperature exceeding 38.3 °C for at least two consecutive days. Fever causes were evaluated by two blinded investigators and categorized as infectious, central, or other causes. Infectious fever causes were further specified. Results: Fever occurred in 213 patients (39%) and was associated with longer hospital and ICU stays (both p < 0.01) and poor functional outcome (odds ratio 2.0, 95% CI 1.1–3.6). The three most frequent fever etiologies (>90% of cases) were pneumonia, central fever, and catheter-associated infections (i.e., urethral tract infections, ventriculitis, and central line-associated bloodstream infections). Median onset day differed across etiologies (overall p < 0.001): central fever developed earliest (2 [IQR 1–3] days), followed by pneumonia (5 [IQR 4–7] days) and catheter-associated infections (8 [IQR 5–12] days). Conclusions: In ICH, the day of fever onset may provide a useful clue to its etiology and could support clinical decision-making, but prospective validation is needed.
Full article
(This article belongs to the Topic Neurological Updates in Neurocritical Care)
►▼
Show Figures
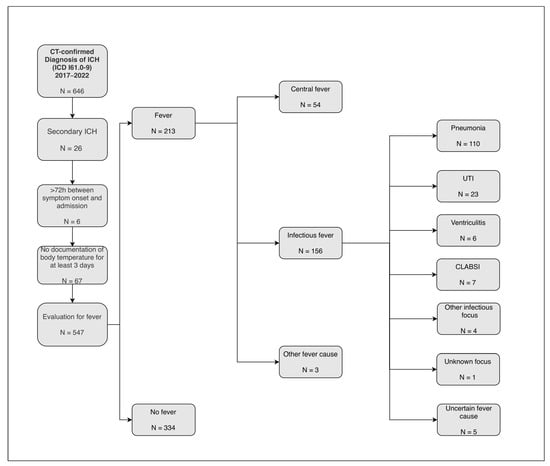
Figure 1
Open AccessArticle
Comparing the Efficacy and Safety of Anti-CGRP Monoclonal Antibodies Versus Topiramate for Migraine Prophylaxis: Six-Month, Real-World, Intention-to-Treat Retrospective Evidence from the GRASP Study Group
by
Michail Vikelis, Dimitrios Rikos, Andreas A. Argyriou, Panagiotis Soldatos, Christos Tsironis, Emmanouil Giakoumakis, Georgia Xiromerisiou, Maria Chondrogianni, Aikaterini Foska, Maria Koutsokera, Konstantinos Notas, Eleni Mavraki and Emmanouil V. Dermitzakis
Neurol. Int. 2026, 18(4), 67; https://doi.org/10.3390/neurolint18040067 - 1 Apr 2026
Abstract
Objective: This retrospective, intention-to-treat real-world study, designed by the Greek Research Alliance for the Study of headache and Pain (GRASP) sought to compare the effectiveness and safety of anti-CGRP monoclonal antibodies (anti-CGRP Mabs) to topiramate in preventing migraine. Patients and methods:
[...] Read more.
Objective: This retrospective, intention-to-treat real-world study, designed by the Greek Research Alliance for the Study of headache and Pain (GRASP) sought to compare the effectiveness and safety of anti-CGRP monoclonal antibodies (anti-CGRP Mabs) to topiramate in preventing migraine. Patients and methods: Patients received either fremanezumab, erenumab, galcanezumab, eptinezumab, or topiramate for at least six months. Outcomes included reductions in monthly headache days (MHDs), ≥50% and ≥75% responder rates, monthly acute medication intake (MAI), MHDs with peak headache intensity ≥5 on VAS, migraine-related disability (MIDAS, HIT-6), quality of life (EQ-VAS), discontinuation rates and safety. Results: We included 409 migraine patients (median age 45.2 years), predominantly female (80%) and mostly with long-standing disease and high baseline burden. After six months, all treatments reduced MHDs. Mean MHDs decreased by −7.8 days with anti-CGRP Mabs versus −3.8 days with topiramate (p < 0.001). Higher ≥50% and ≥75% responder rates were observed across all anti-CGRP agents, compared to topiramate. Anti-CGRP Mabs also achieved greater reductions in moderate/severe MHDs, MAI, disability metrics, and superior QOL gains. Among the CGRP-targeted therapies, slight differences in effectiveness outcomes were present, though failing to demonstrate any specific superiority. Safety was favorable for anti-CGRP Mabs, whereas topiramate showed substantially higher adverse events and discontinuations. Conclusions: Anti-CGRP Mabs were more effective, produced greater reductions in disability and higher improvements quality-of-life metrics and were better tolerated than topiramate. Differences among individual anti-CGRP agents were modest and unlikely to represent a clinically meaningful superiority, supporting a class-wide benefit vs. topiramate in migraine prevention both in terms of effectiveness and safety.
Full article
(This article belongs to the Section Pain Research)
►▼
Show Figures

Figure 1
Open AccessArticle
The Added Value of Endoscopic Micro-Inspection in Microvascular Decompression for Trigeminal Neuralgia and Hemifacial Spasm: Literature Review and Single-Center Experience
by
Alexandra Mihaela Pătrășcan, Felix Mircea Brehar, Radu Mircea Gorgan and Viorel Mihai Prună
Neurol. Int. 2026, 18(4), 66; https://doi.org/10.3390/neurolint18040066 - 31 Mar 2026
Abstract
Background: In the last few decades, microvascular decompression has been proven to be one of the best therapeutic options in the management of neurovascular compression syndromes, especially trigeminal neuralgia, hemifacial spasm, and glossopharyngeal neuralgia. However, higher rates of recurrences and morbidities have been
[...] Read more.
Background: In the last few decades, microvascular decompression has been proven to be one of the best therapeutic options in the management of neurovascular compression syndromes, especially trigeminal neuralgia, hemifacial spasm, and glossopharyngeal neuralgia. However, higher rates of recurrences and morbidities have been recorded postoperatively. In the thorough search for better solutions, the option of adjuvant QEVO® endoscopy has arisen as a very promising alternative. Methods: In this study, a retrospective single-center observational analysis was conducted, comprising patients who underwent microvascular decompression for trigeminal neuralgia, hemifacial spasm, and glossopharyngeal neuralgia at our institution, between January 2020 and November 2025. Demographical data and outcomes of therapeutic management were statistically analyzed and presented accordingly. Results: A total of 40 patients diagnosed with neurovascular compression syndromes were neurosurgically treated in our center, and the most common diagnosis was represented by trigeminal neuralgia, identified in 32 patients (80%). Another five (12.5%) patients underwent microvascular decompression for hemifacial spasm, two (5%) patients were treated for combined trigeminal neuralgia and hemifacial spasm, and one patient (2.5%) for glossopharyngeal neuralgia. Arterial conflict was the triggering factor in the majority of cases, and no postoperative mortality was recorded. In patients treated using adjuvant QEVO endoscopy, the identification of hidden conflicts may be facilitated. Furthermore, the use of the QEVO endoscope allowed the identification of additional neurovascular conflicts and influenced intraoperative management in a subset of patients. Conclusions: Notwithstanding the medical literature suggesting that the main influential factor for therapeutic success is the vessel type and the pattern of compression, many authors identified the cornerstone of favorable outcomes as being endoscopic assistance. Nevertheless, this adjuvant factor has had a positive impact on the majority of patients.
Full article
(This article belongs to the Section Pain Research)
►▼
Show Figures
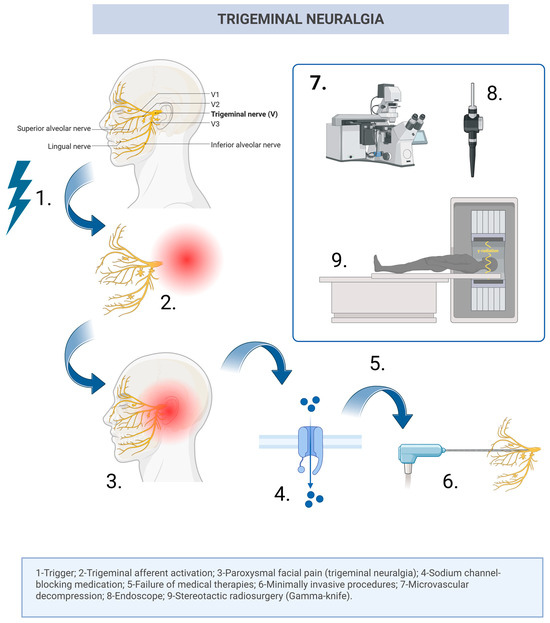
Figure 1
Open AccessReview
Seizure and Status Epilepticus in Human Organophosphate Poisoning: A Narrative Review
by
Giuseppe Magro, Oreste Marsico, Federico Tosto, Concetta Lobianco, Laura Rapisarda, Giovanni Mastroianni and Angelo Pascarella
Neurol. Int. 2026, 18(4), 65; https://doi.org/10.3390/neurolint18040065 - 30 Mar 2026
Abstract
Organophosphate (OP) exposure can trigger seizures within minutes and can rapidly evolve into status epilepticus (SE). Early seizure generation is plausibly driven by acetylcholinesterase inhibition, leading to central cholinergic overstimulation. With increasing seizure duration, experimental data are consistent with a time-dependent shift toward
[...] Read more.
Organophosphate (OP) exposure can trigger seizures within minutes and can rapidly evolve into status epilepticus (SE). Early seizure generation is plausibly driven by acetylcholinesterase inhibition, leading to central cholinergic overstimulation. With increasing seizure duration, experimental data are consistent with a time-dependent shift toward glutamatergic maintenance (NMDA/AMPA), oxidative stress, neuroinflammation, and progressive failure of GABAergic inhibition. This framework predicts a narrow window in which benzodiazepine (BDZ) monotherapy is most effective and a rising probability of BDZ non-response when seizures are prolonged, while anti-glutamatergic strategies may retain relative efficacy later in the course. This narrative review integrates clinical phenomenology, diagnostic limitations, and mechanistic evidence to propose an operational approach for OP-related seizures and SE in emergency settings. We discuss a pragmatic “Stage 1 Plus” framing for patients presenting after prolonged seizures or in non-convulsive SE with coma. Human evidence remains limited and heterogeneous, and inference is constrained by confounding due to delayed recognition, variable decontamination/resuscitation pathways, sparse EEG confirmation, and selection bias in mass-casualty reporting.
Full article
(This article belongs to the Special Issue Drug Treatment of Epilepsy)
►▼
Show Figures

Graphical abstract
Open AccessReview
Alpha-Lipoic Acid and Biotin in Neurodegenerative Diseases: Convergent Mechanistic Insights from Preclinical Models to Clinical Perspectives
by
Asdrubal Aguilera-Méndez, Karel Aguilera-Manuel, Alfredo Saavedra-Molina, Patricia Ríos-Chávez, Santiago Villafaña, Renato Nieto-Aguilar, Daniel Godínez-Hernández, Daniel Ortega-Cuellar, Zoraya Palomera-Sanchez and Marcia Gauthereau-Torres
Neurol. Int. 2026, 18(4), 64; https://doi.org/10.3390/neurolint18040064 - 26 Mar 2026
Abstract
Background: Neurodegenerative diseases, including Alzheimer’s disease, Parkinson’s disease, multiple sclerosis, and amyotrophic lateral sclerosis, represent a major global health burden and share convergent pathogenic mechanisms, such as mitochondrial dysfunction, oxidative stress, neuroinflammation, calcium imbalance, and neuronal loss. Despite advances in symptomatic management, effective
[...] Read more.
Background: Neurodegenerative diseases, including Alzheimer’s disease, Parkinson’s disease, multiple sclerosis, and amyotrophic lateral sclerosis, represent a major global health burden and share convergent pathogenic mechanisms, such as mitochondrial dysfunction, oxidative stress, neuroinflammation, calcium imbalance, and neuronal loss. Despite advances in symptomatic management, effective disease-modifying therapies remain limited. Objectives: This review aims to critically synthesize mechanistic, preclinical, and clinical evidence on α-lipoic acid and biotin as candidate neuroprotective agents in neurodegenerative diseases, with emphasis on shared signaling pathways, therapeutic potential, generally favorable safety profiles, and translational limitations. Methods: A narrative and integrative review was conducted, encompassing mechanistic studies, preclinical experimental models, and clinical trials and observational studies evaluating ALA and biotin in neurodegenerative diseases. The evidence was qualitatively analyzed with attention to biological plausibility, consistency across models, and clinical relevance. Results: ALA and biotin modulate key cellular pathways implicated in neurodegeneration, including mitochondrial metabolism, redox homeostasis, inflammatory signaling, and neurovascular function. Preclinical studies consistently report beneficial effects on mitochondrial efficiency, oxidative stress, and neuroinflammatory markers. In contrast, clinical evidence remains heterogeneous, with more extensive evaluation of biotin in progressive multiple sclerosis and more limited or exploratory findings for ALA across neurodegenerative disorders. Conclusions: ALA and biotin exhibit mechanistic convergence across pathways relevant to neurodegeneration and generally favorable safety profiles. Although current evidence supports their biological plausibility as adjunctive or exploratory therapeutic strategies, clinical outcomes remain inconsistent and appear to be influenced by dosing regimens, disease stage at intervention, and endpoint selection. Well-designed clinical studies are required to define their efficacy, optimal dosing, and disease-specific applicability.
Full article
(This article belongs to the Special Issue Molecular and Cellular Research of Neuroprotection and Neurodegeneration)
►▼
Show Figures
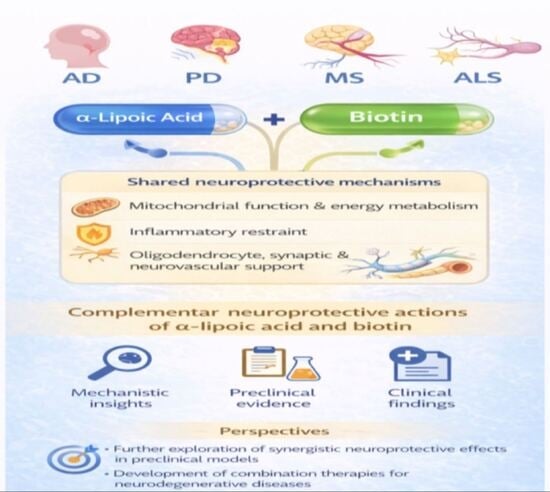
Graphical abstract
Open AccessArticle
Reversal of Endogenous Bioelectrical Network Collapse in Advanced Childhood Cerebral X-Linked Adrenoleukodystrophy
by
Salvatore Rinaldi, Arianna Rinaldi and Vania Fontani
Neurol. Int. 2026, 18(4), 63; https://doi.org/10.3390/neurolint18040063 - 24 Mar 2026
Abstract
Background/Objectives: Advanced childhood cerebral X-linked adrenoleukodystrophy (cALD) is traditionally regarded as an irreversible terminal phase of neurodegeneration driven by inflammatory demyelination and axonal loss. Experimental evidence indicates that endogenous bioelectrical fields regulate central nervous system organisation, raising the possibility that functional network collapse
[...] Read more.
Background/Objectives: Advanced childhood cerebral X-linked adrenoleukodystrophy (cALD) is traditionally regarded as an irreversible terminal phase of neurodegeneration driven by inflammatory demyelination and axonal loss. Experimental evidence indicates that endogenous bioelectrical fields regulate central nervous system organisation, raising the possibility that functional network collapse in cALD may be biologically modifiable, even in the presence of persistent structural damage. This study examined whether longitudinal modulation of endogenous bioelectrical network organisation is associated with sustained clinical and neurophysiological stabilisation in advanced cALD. Methods: We performed a longitudinal observational analysis of two paediatric patients with advanced childhood cerebral X-linked adrenoleukodystrophy undergoing repeated neuroregenerative treatment cycles. Standardised scalp electroencephalography was recorded during spontaneous wakefulness and repeated over months under comparable vigilance conditions. Multimodal analysis included conventional EEG, quantitative EEG, independent component analysis, and standardised low-resolution electromagnetic tomography (sLORETA). Clinical function was assessed using validated measures of consciousness, swallowing, and voluntary motor behaviour. Results: Across patients, longitudinal recordings demonstrated sustained stabilisation of consciousness, swallowing, and voluntary motor function, accompanied by reproducible reorganisation of pathological brain rhythms. Delta and theta oscillations showed a consistent topographical redistribution from limbic–frontoinsular networks towards sensorimotor and parietal integrative cortices. These changes were observed across modalities and timepoints and are unlikely to reflect spontaneous fluctuation, delayed effects of haematopoietic stem cell transplantation, or state-dependent EEG variation. Conclusions: Advanced childhood cerebral X-linked adrenoleukodystrophy is associated with disorganisation of endogenous bioelectrical network activity. In this longitudinal analysis, large-scale network reorganisation was temporally associated with sustained clinical stabilisation, supporting a view of late-stage cALD as a dynamic disorder of network-level vulnerability, rather than a fixed terminal state.
Full article
(This article belongs to the Section Movement Disorders and Neurodegenerative Diseases)
►▼
Show Figures

Figure 1
Open AccessArticle
Cognition and Health-Related Quality of Life After aSAH: The Role of Objective and Subjective Impairment
by
Angelka Pešterac-Kujundžić, Una Nedeljković, Ivana Sretenović, Aleksandar Milosavljević, Dragoslav Nestorović, Vojislav Bogosavljević and Ivan Vukašinović
Neurol. Int. 2026, 18(3), 62; https://doi.org/10.3390/neurolint18030062 - 23 Mar 2026
Abstract
Objectives: Survivors of mild-grade aneurysmal subarachnoid hemorrhage (aSAH) often achieve favorable neurological recovery, yet many continue to experience cognitive difficulties and reduced health-related quality of life (HRQoL). The relative contribution of objectively measured cognition and subjective cognitive complaints to long-term HRQoL in this
[...] Read more.
Objectives: Survivors of mild-grade aneurysmal subarachnoid hemorrhage (aSAH) often achieve favorable neurological recovery, yet many continue to experience cognitive difficulties and reduced health-related quality of life (HRQoL). The relative contribution of objectively measured cognition and subjective cognitive complaints to long-term HRQoL in this population remains insufficiently clarified. Methods: This prospective cohort study assessed objective and subjective cognitive functioning one year after mild-grade aSAH (Hunt & Hess I–II) and examined their unique contributions to HRQoL. Forty endovascularly treated aSAH survivors and 80 neurologically healthy controls, matched for sex, age, and educational level, were assessed 12–14 months post-ictus using the Montreal Cognitive Assessment (MoCA), Cognitive Failures Questionnaire (CFQ), and SF-36. Results: Compared with controls, patients demonstrated significantly lower MoCA scores, with cognitive impairment present in 42.5% of cases, as well as reduced HRQoL. In multivariate regression analyses adjusted for demographic, clinical, and affective covariates, subjective cognitive complaints (CFQ) remained independently associated with the mental component summary score of the SF-36 (β = −0.47, p = 0.002). Objective cognitive performance (MoCA) was not associated with the SF-36 component summary scores but showed weaker, domain-specific associations in exploratory analyses. The correlation between MoCA and CFQ was weak (ρ = −0.33), indicating a dissociation between these two measures. Conclusions: One year after mild-grade aSAH, subjective cognitive complaints contribute to mental HRQoL above and beyond the influence of affective symptoms. These findings highlight a clinically relevant dissociation between perceived and objectively measured cognition and support the importance of incorporating patient-reported cognitive difficulties into long-term outcome assessment and rehabilitation planning.
Full article
(This article belongs to the Section Aging Neuroscience)
►▼
Show Figures

Figure 1
Open AccessArticle
Posterior Communicating Artery Configuration and Laterality of Thalamic and Lenticulostriate Infarction
by
Junpei Nagasawa, Masamichi Hozumi, Tatsuhiro Yokoyama, Makiko Ogawa, Junya Ebina, Mari Shibukawa, Takehisa Hirayama and Osamu Kano
Neurol. Int. 2026, 18(3), 61; https://doi.org/10.3390/neurolint18030061 - 22 Mar 2026
Abstract
Background: Anatomical variations in the posterior communicating artery (PCoA) are common, but their association with ischemic stroke remains unclear. In this study, we investigated the relationship between PCoA configuration and the localization of perforator infarction. Methods: We conducted a single-center, retrospective observational study
[...] Read more.
Background: Anatomical variations in the posterior communicating artery (PCoA) are common, but their association with ischemic stroke remains unclear. In this study, we investigated the relationship between PCoA configuration and the localization of perforator infarction. Methods: We conducted a single-center, retrospective observational study of consecutive patients admitted with acute ischemic stroke between April 2016 and July 2023. Patients with a single, unilateral lacunar infarction confined to the thalamic or lenticulostriate artery (LSA) territory were included. PCoA configuration was assessed using time-of-flight magnetic resonance angiography and dichotomized as present (normal PCoA or fetal-type posterior cerebral artery) or absent (hypoplastic or aplastic PCoA). Using a within-patient, hemisphere-based approach, the presence of PCoA on the infarcted side was directly compared with that on the contralateral side. McNemar’s test with continuity correction was used for laterality analysis. Results: A total of 64 patients met the inclusion criteria, including 45 with LSA infarction and 19 with thalamic infarction. The prevalence of PCoA presence on the infarcted hemisphere was 20.0% in the LSA group and 26.3% in the thalamic group, identical to that observed on the contralateral hemisphere in each group. Within-patient comparisons revealed no significant difference in PCoA presence between infarcted and non-infarcted hemispheres in either territory (all p > 0.05). Conclusions: In patients with unilateral perforator infarction involving the thalamic or LSA territories, PCoA configuration was not associated with infarct laterality. These findings suggest that variations in PCoA anatomy have a limited influence on hemispheric vulnerability to perforator infarction, supporting the predominant role of local small-vessel pathology rather than proximal collateral anatomy in the development of lacunar stroke.
Full article
(This article belongs to the Special Issue Cerebrovascular Disease: Update on Diagnosis and Treatment)
►▼
Show Figures
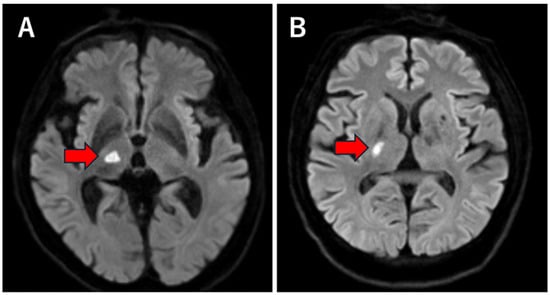
Figure 1
Open AccessReview
Duropathies as Unifying Concept—Part Two: A Narrative Overview of Clinical and Neuroradiological Features
by
Marialuisa Zedde, Luigi Cirillo, Elisa Francesca Maria Ciceri, Nicola Limbucci, Mario Muto, Mauro Bergui, Francesco Causin and Rosario Pascarella
Neurol. Int. 2026, 18(3), 60; https://doi.org/10.3390/neurolint18030060 - 20 Mar 2026
Abstract
Duropathies represent a spectrum of disorders associated with spinal dural tears and cerebrospinal fluid (CSF) leaks. Diagnosis and treatment is often complicated by overlapping clinical manifestations. This review aims to synthesize current literature on duropathies, focusing on their clinical, neuroradiological, and pathophysiological features.
[...] Read more.
Duropathies represent a spectrum of disorders associated with spinal dural tears and cerebrospinal fluid (CSF) leaks. Diagnosis and treatment is often complicated by overlapping clinical manifestations. This review aims to synthesize current literature on duropathies, focusing on their clinical, neuroradiological, and pathophysiological features. A comprehensive literature review was conducted, analyzing various conditions classified as duropathies, including spontaneous intracranial hypotension (SIH), superficial siderosis (SS), spinal cord herniation, and, as added issue, arachnoid webs. The review emphasized the importance of imaging techniques such as MRI and CT myelography in diagnosing these conditions. Duropathies can arise from congenital anomalies, trauma, and degenerative changes, with SIH being characterized by orthostatic headaches and neurological deficits. Imaging typically reveals specific patterns, such as a widened dorsal subarachnoid space and ventral displacement of the spinal cord. Syringomyelia was frequently associated with arachnoid webs, and complications like SS and bibrachial amyotrophy were noted in patients with persistent ventral spinal CSF leaks. The unifying concept of duropathies is proposed, emphasizing the need for timely intervention to mitigate long-term neurological consequences. Enhanced diagnostic strategies are crucial for improving patient outcomes, and a multidisciplinary approach is recommended for the management of these complex disorders. Further research is warranted to clarify the pathophysiological mechanisms underlying duropathies and to establish standardized treatment protocols.
Full article
(This article belongs to the Collection Exclusive Papers from the Editorial Board Members (EBMs) of Neurology International)
►▼
Show Figures

Figure 1
Open AccessReview
No New Relevant Treatment Options for L-DOPA-Induced Dyskinesia from a Clinician’s Point of View
by
Thomas Müller
Neurol. Int. 2026, 18(3), 59; https://doi.org/10.3390/neurolint18030059 - 20 Mar 2026
Abstract
Background: The term dyskinesia describes involuntary movements of the face, body and extremities. Frequently, they appear following and in relation with prior oral long-lasting and high-dose levodopa therapy in Parkinson’s disease patients. Onset of these motion sequences causes patient distress and caregiver embarrassment
[...] Read more.
Background: The term dyskinesia describes involuntary movements of the face, body and extremities. Frequently, they appear following and in relation with prior oral long-lasting and high-dose levodopa therapy in Parkinson’s disease patients. Onset of these motion sequences causes patient distress and caregiver embarrassment with declined quality of life. Continuity of nigrostriatal postsynaptic dopamine receptor stimulation delays occurrence of dyskinesia. A pulsatile pattern with temporary too high dopamine receptor excitation promotes manifestation of dyskinesia. Methods: This narrative review describes past pharmacologic approaches for therapy of dyskinesia, such as the principle of continuous dopamine receptor stimulation. Discussion and Conclusions: Novel concepts were tested. They influenced neurotransmission of serotonin and altered stimulation of dopamine receptor subtypes. The translation of successful experimental research outcomes into valuable clinical trial results with consecutive approval of drugs with a new mode of action under the indication “antidyskinetic” repeatedly failed. An exception is the open-channel blocker of the N-methyl-D-aspartate receptor and dopamine reuptake inhibitor amantadine with its moderate dyskinesia-reducing effects, particularly in its extended-release formulation. This antiviral compound also improves impaired motor behavior and reduces “OFF” intervals. Therefore, amantadine is currently experiencing a certain resurgence in regions where its extended-release formulations are marketed for therapy of levodopa-induced dyskinesia.
Full article
(This article belongs to the Collection Exclusive Papers from the Editorial Board Members (EBMs) of Neurology International)
►▼
Show Figures

Figure 1
Open AccessArticle
Delta Power in SLC6A1-Related Neurodevelopmental Disorder: Operationalizing Quantitative EEG Metrics for Biomarker Development
by
Hamza Dahshi, Marie Varnet, Kimberly Goodspeed, Jacob Tiller, Dallas Armstrong and Deepa Sirsi
Neurol. Int. 2026, 18(3), 58; https://doi.org/10.3390/neurolint18030058 - 18 Mar 2026
Abstract
Introduction: SLC6A1-related neurodevelopmental disorder (SLC6A1-NDD) is an epileptic encephalopathy linked to mutations in the SLC6A1 gene and is characterized by early-onset seizures and developmental delays. Despite the growing recognition of SLC6A1 as a major cause of early-onset epilepsy, the electrophysiological changes associated with
[...] Read more.
Introduction: SLC6A1-related neurodevelopmental disorder (SLC6A1-NDD) is an epileptic encephalopathy linked to mutations in the SLC6A1 gene and is characterized by early-onset seizures and developmental delays. Despite the growing recognition of SLC6A1 as a major cause of early-onset epilepsy, the electrophysiological changes associated with the disorder remain inadequately characterized. This study aims to identify electrophysiological biomarkers of SLC6A1-NDD by characterizing EEG delta power using automated tools, EEGLAB (v2023.1) and Persyst 13, exploring age- and state-related effects. Methods: We analyzed EEG recordings from 20 patients with SLC6A1-NDD and 20 neurotypical age- and sex-matched controls using EEGLAB and Persyst, quantifying delta power and related metrics. The Wilcoxon signed-rank method tested for differences between patients and controls, area under the curve (AUC) values evaluated patient classifier models, and Pearson’s correlation assessed concordance between EEGLAB and Persyst. Results: Patients with SLC6A1-NDD exhibited significantly elevated delta power (19.4 ± 4.1) compared to controls (14.2 ± 3.0; p < 0.001). The mean delta power showed an age-dependent increasing trend in patients (b = 0.5), contrasting with a decline in controls (b = −1.0; p < 0.001). In Persyst, the frequency of delta activity above an optimized threshold best differentiated patients from controls in wake epochs (AUC = 0.93). Concordance between EEGLAB and Persyst was one-to-one but with moderate variability (R2 = 0.644; p < 0.001). Conclusions: Elevated delta power is a notable feature of SLC6A1-NDD. Cross-platform comparison demonstrates the feasibility of quantitative EEG analysis, while imperfect concordance highlights the need for pipeline standardization. Future work should validate these findings in larger cohorts and, as suitable reference data emerge, benchmark delta power metrics against age-matched children with other developmental and epileptic encephalopathies.
Full article
(This article belongs to the Special Issue The Evolving Role of EEG in Neurological Disorders: Advanced Techniques and Future Directions)
►▼
Show Figures

Figure 1
Open AccessCase Report
Ischemic Stroke as the First Manifestation of Takayasu Arteritis: A Case Report
by
Dominika Jakubowicz-Lachowska, Magdalena Sarnowska, Monika Chorąży and Alina Kułakowska
Neurol. Int. 2026, 18(3), 57; https://doi.org/10.3390/neurolint18030057 - 18 Mar 2026
Abstract
Introduction: Ischemic stroke in young adults is uncommon and is frequently associated with rare etiologies, including autoimmune diseases and vasculitis. Takayasu arteritis (TA) is a chronic inflammatory large-vessel arteriopathy involving the aorta and its major branches and may result in cerebral ischemia due
[...] Read more.
Introduction: Ischemic stroke in young adults is uncommon and is frequently associated with rare etiologies, including autoimmune diseases and vasculitis. Takayasu arteritis (TA) is a chronic inflammatory large-vessel arteriopathy involving the aorta and its major branches and may result in cerebral ischemia due to arterial stenosis or thrombosis. Case Presentation: We report the case of a 26-year-old woman with a history of suspected rheumatoid arthritis and Lyme disease who presented with acute left-sided hemiparesis and dysarthria. At admission, large-vessel vasculitis had not yet been suspected, and the patient was treated according to standard acute stroke protocols. Computed tomography angiography (CTA) revealed occlusion of the right middle cerebral artery bifurcation and the right common carotid artery, with inflammatory changes involving the brachiocephalic trunk and subclavian arteries. Intravenous thrombolysis (iv rtPA) was followed by mechanical thrombectomy (MT), resulting in neurological improvement. Outcome: Further diagnostic work-up confirmed TA, and immunosuppressive therapy with cyclophosphamide and infliximab was initiated. Conclusion: This case underscores the importance of considering inflammatory large-vessel disease in young patients presenting with acute ischemic stroke and illustrates that endovascular reperfusion may be feasible in this clinical setting.
Full article
(This article belongs to the Special Issue Cerebrovascular Disease: Update on Diagnosis and Treatment)
►▼
Show Figures

Figure 1
Open AccessArticle
Post-Transplant Tremor: Characteristics and Differences Based on Sex and Post-Transplant Therapy
by
Srdjana Telarovic, Maja Vrdoljak Pazur, Nikolina Zupancic, Anamarija Strajduhar and Irma Telarovic
Neurol. Int. 2026, 18(3), 56; https://doi.org/10.3390/neurolint18030056 - 17 Mar 2026
Abstract
Background/Objectives: Kidney transplantation is the standard of care for the majority of patients with end-stage kidney disease. Neurological complications are common, and among them, tremor is very frequent and usually attributed to immunosuppressive drug toxicity. Methods: In this retrospective study, we
[...] Read more.
Background/Objectives: Kidney transplantation is the standard of care for the majority of patients with end-stage kidney disease. Neurological complications are common, and among them, tremor is very frequent and usually attributed to immunosuppressive drug toxicity. Methods: In this retrospective study, we investigate the incidence and characteristics of tremor in kidney transplant patients and analyze its occurrence with respect to a multitude of demographic and clinical parameters, thereby aiming to confirm the role of calcineurin inhibitor-induced neurotoxicity and to identify other putative predictive factors. Furthermore, we characterize post-transplant tremor with the goal of identifying its clinical features and determining the impact on quality of life. Results: A total of 129 kidney transplant recipients were screened; six patients were excluded due to a history of movement disorders prior to kidney transplantation. In total, 123 patients were included in the final analysis—69 male (56%) and 54 female patients (44%), with a median age of 50. A total of 36% (46 patients) developed tremor in the post-transplant period. Using both univariable and multivariable analyses, we found that female sex and tacrolimus use were independently associated with the development of post-transplant tremor. In addition, multivariable analysis identified an association between younger age and post-transplant tremor. Furthermore, we observed a trend in the duration of symptoms in relation to the calcineurin inhibitor choice. Conclusions: Despite a relatively high prevalence (36%), post-transplant tremor does not significantly impact the QoL and spontaneously resolves within 1 year in adult kidney transplant recipients. Female sex and tacrolimus were identified as independent predictors of post-transplant tremor in renal transplant recipients.
Full article
(This article belongs to the Section Movement Disorders and Neurodegenerative Diseases)
►▼
Show Figures

Graphical abstract
Open AccessSystematic Review
Effectiveness of Physiotherapy Interventions on Executive Function in Patients with Chronic Pain: A Systematic Review
by
Aser Donado-Bermejo, Silvia Di-Bonaventura, Pablo Barrenechea-Leal, Francisco Mercado-Romero, Marisa Fernández-Sánchez and Raúl Ferrer-Peña
Neurol. Int. 2026, 18(3), 55; https://doi.org/10.3390/neurolint18030055 - 16 Mar 2026
Abstract
Background: Chronic pain is a prevalent and disabling condition that affects physical health but also cognitive domains. Executive functions, including inhibitory control, cognitive flexibility, and working memory, essentials for self-regulation, treatment adherence, and coping with symptoms, are particularly compromised. Physiotherapy interventions, traditionally aimed
[...] Read more.
Background: Chronic pain is a prevalent and disabling condition that affects physical health but also cognitive domains. Executive functions, including inhibitory control, cognitive flexibility, and working memory, essentials for self-regulation, treatment adherence, and coping with symptoms, are particularly compromised. Physiotherapy interventions, traditionally aimed at physical outcomes, may also influence executive functions; however, their impact remains unclear. Objective: This review aimed to synthesize current evidence regarding the effects of physiotherapy-related interventions on executive function in adults with chronic pain. Methods: The review followed the Cochrane Handbook and Preferred Reporting Items for Systematic Reviews (PRISMA) guidelines, and the protocol was registered in PROSPERO (CRD42024611800). A comprehensive search was performed. Randomized controlled trials (RCTs) included adults with chronic pain (≥3 months) whose executive function outcomes were evaluated after physiotherapy-based interventions. Results: Out of 12,391 records, 10 randomized controlled trials were included. Populations primarily had fibromyalgia, chronic low back pain, and chronic musculoskeletal pain. Interventions encompassed transcranial direct current stimulation (tDCS), transcranial magnetic stimulation (rTMS), neurofeedback, structured exercise, and multimodal physical-cognitive-mindfulness training. Intervention durations ranged from one session to 16 weeks. Executive function was assessed with diverse neuropsychological tests. tDCS improved attention, inhibitory control, cognitive flexibility, and working memory. Exercise interventions showed benefits in working memory and inhibitory control. Conclusions: Preliminary evidence suggests that physiotherapy interventions, particularly anodal tDCS and structured exercise, may improve executive functions in individuals with chronic pain. Future trials should incorporate long-term follow-up. Integrating cognitive targets into physiotherapy may enhance the multidimensional management of chronic pain.
Full article
(This article belongs to the Special Issue Non-Invasive Neuromodulation in Treatment of Chronic Pain)
►▼
Show Figures

Graphical abstract
Open AccessArticle
EEG in the Emergency Department: When the Neurophysiological Test Can Be Avoided in Emergency Diagnostic Workups? The EMINENCE Study
by
Maenia Scarpino, Antonello Grippo, Federica Barraco, Benedetta Piccardi, Laura Betti, Peiman Nazerian, Arianna Fabbri, Roberto Fratangelo, Cristina Mei and Andrea Nencioni
Neurol. Int. 2026, 18(3), 54; https://doi.org/10.3390/neurolint18030054 - 16 Mar 2026
Abstract
►▼
Show Figures
Introduction: This study was conducted to determine whether specific emergency physician (EP) diagnoses and/or neurological signs/symptoms upon admission to the Emergency Department (ED) were associated with normal/non-informative emergency electroencephalogram (emEEG). Methods: Data from consecutive patients admitted to the ED of our tertiary
[...] Read more.
Introduction: This study was conducted to determine whether specific emergency physician (EP) diagnoses and/or neurological signs/symptoms upon admission to the Emergency Department (ED) were associated with normal/non-informative emergency electroencephalogram (emEEG). Methods: Data from consecutive patients admitted to the ED of our tertiary hospital over a two-year period (1 January 2023–31 December 2024) were analyzed retrospectively. We evaluated the correlation between normal/non-specific emEEGs and EP admission diagnoses and neurological signs/symptoms on admission. Epileptic discharges and sharp waves with triphasic morphology were considered specific patterns. Results: A total of 2008 patients underwent emEEG recording during the study period. EmEEGs were considered non-informative in 100% of global amnesia diagnoses, 100% of cases of mild head trauma, 100% of cases of migraine with aura, 98.3% of transient ischemic attacks (TIAs), 95.6% of transient losses of consciousness (TLCs) when seizure was not the primary suspected diagnosis, and in 92.7% of falls of unknown dynamics. Epileptic patterns were detected in 4% of patients presenting with TLC and in 2.4% of those with falls of unknown dynamics, with approximately half of these patients having a pre-existing diagnosis of epilepsy. Triphasic waves were detected in 4.9% patients with falls of unknown dynamics, in 1.7% with TIA, and in 0.4% with TLC. All of these patients had fever/sepsis or metabolic/electrolyte disorders. Overall, across all clinical scenarios, emEEGs were considered non-informative in 385 (19.1%) tested patients. Conclusions: emEEGs are almost non-informative in the diagnostic pathway for patients with global amnesia, mild head trauma, and migraine with aura, and in patients with TIA, TLC, or falls of unknown dynamics. EPs can safely consider avoiding emEEGs in the absence of previous epilepsy diagnosis, fever/sepsis, metabolic/electrolyte disturbances, or drug abuse.
Full article
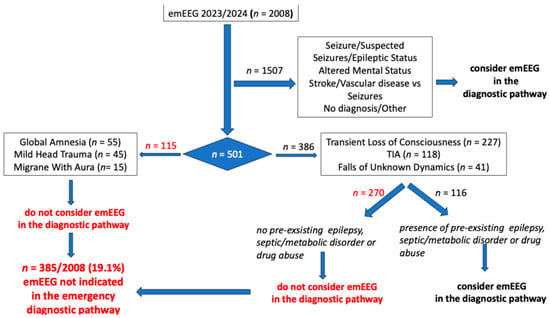
Figure 1
Open AccessReview
Treating the Patient, Not Only the Amyloid: Symptomatic Management in Transthyretin Amyloidosis
by
Christian Messina
Neurol. Int. 2026, 18(3), 53; https://doi.org/10.3390/neurolint18030053 - 13 Mar 2026
Abstract
Transthyretin amyloidosis (ATTR) is a progressive multisystem disorder characterized by extracellular deposition of misfolded transthyretin fibrils, leading to neurological, cardiac, gastrointestinal, urogenital, sexual, and ophthalmological involvement. While disease-modifying therapies have significantly improved survival and slowed disease progression, a substantial proportion of patients continue
[...] Read more.
Transthyretin amyloidosis (ATTR) is a progressive multisystem disorder characterized by extracellular deposition of misfolded transthyretin fibrils, leading to neurological, cardiac, gastrointestinal, urogenital, sexual, and ophthalmological involvement. While disease-modifying therapies have significantly improved survival and slowed disease progression, a substantial proportion of patients continue to experience a high symptomatic burden that markedly impairs quality of life. Symptomatic manifestations often occur early, may precede the diagnosis, and frequently persist despite etiological treatment. This review provides a comprehensive overview of the symptomatic management of ATTR, with particular emphasis on autonomic dysfunction and its systemic consequences. We discuss current therapeutic strategies for orthostatic hypotension, gastrointestinal dysmotility, nutritional impairment, sexual dysfunction, lower urinary tract dysfunction, and ophthalmological involvement, highlighting both pharmacological and non-pharmacological approaches. Special attention is given to treatment limitations related to cardiac involvement, autonomic failure, and drug tolerability. Despite the clinical relevance of symptom control in ATTR, evidence-based recommendations remain scarce, and no dedicated guidelines currently exist. Most therapeutic approaches are derived from observational studies, expert opinion, and clinical experience. Improved awareness of symptomatic manifestations, early intervention, and a multidisciplinary, individualized approach are essential to optimize patient outcomes. Future research should focus on prospective studies and the development of structured symptomatic treatment algorithms to complement disease-modifying therapies and enhance patient-centered care in ATTR.
Full article
(This article belongs to the Topic Dysautonomia in Neurological Disorders)
Open AccessCase Report
Middle Meningeal Artery Embolization as Standalone Therapy for Chronic Subdural Hematoma with Radiological Herniation Features: A Case Report
by
Gamaliel Wibowo Soetanto and Elvan Wiyarta
Neurol. Int. 2026, 18(3), 52; https://doi.org/10.3390/neurolint18030052 - 5 Mar 2026
Abstract
Background: Chronic subdural hematoma is commonly managed with surgical evacuation when significant mass effect or herniation features are present. Although middle meningeal artery embolization has emerged as an effective adjunctive therapy, evidence supporting its use as standalone treatment in patients with radiological herniation
[...] Read more.
Background: Chronic subdural hematoma is commonly managed with surgical evacuation when significant mass effect or herniation features are present. Although middle meningeal artery embolization has emerged as an effective adjunctive therapy, evidence supporting its use as standalone treatment in patients with radiological herniation remains limited. Case Presentation: We report a 51-year-old man who presented with a three-week history of progressive headache, intermittent confusion, and mild left-sided weakness. Magnetic resonance imaging demonstrated a right-sided chronic subdural hematoma with marked cortical compression and subfalcine herniation. Despite radiological severity, the patient remained neurologically stable. After multidisciplinary discussion, middle meningeal artery embolization was performed as sole therapy via right radial access using a liquid embolic agent. Selective angiography demonstrated pathological neovascular supply from the right middle meningeal artery, which was completely obliterated following embolization without procedural complications. The post-procedural course was uneventful, with progressive clinical improvement. Follow-up non-contrast computed tomography at eight months demonstrated near-complete resolution of the hematoma with normalization of midline structures, and no surgical evacuation was required. Conclusions: Standalone middle meningeal artery embolization may represent a feasible therapeutic option in carefully selected clinically stable patients with chronic subdural hematoma and radiological herniation features, though further studies are required to define optimal selection criteria and long-term outcomes.
Full article
(This article belongs to the Section Brain Tumor and Brain Injury)
►▼
Show Figures
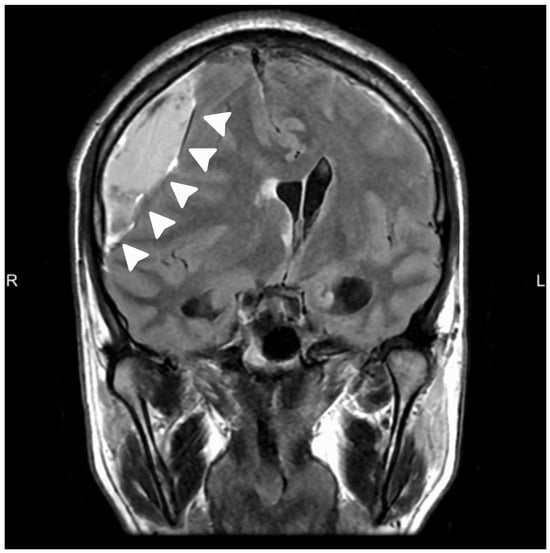
Figure 1
Open AccessArticle
Neurotrophins Plasma Levels Kinetics in Ischemic Stroke Patients—Potential Relation to Outcomes
by
Radosław Opiła, Karolina Łuczkowska, Edyta Paczkowska, Przemysław Nowacki, Jarosław Peregud-Pogorzelski and Bogusław Machaliński
Neurol. Int. 2026, 18(3), 51; https://doi.org/10.3390/neurolint18030051 - 4 Mar 2026
Abstract
Background/Objectives: Neurotrophins are a family of structurally related growth factors known to play an important role in the physiology and pathophysiology of the central nervous system. In ischemic stroke, lower blood concentrations of brain-derived neurotrophic factor (BDNF) have been linked to worse
[...] Read more.
Background/Objectives: Neurotrophins are a family of structurally related growth factors known to play an important role in the physiology and pathophysiology of the central nervous system. In ischemic stroke, lower blood concentrations of brain-derived neurotrophic factor (BDNF) have been linked to worse outcomes. However, data regarding blood levels of other neurotrophins remain limited. Methods: Plasma levels of BDNF, NGF, NT-3 and NT-4 of 93 patients with ischemic stroke were measured using Luminex immunoassay at two time points: within 24 h from onset and on the seventh day. Clinical data regarding co-existing risk factors, National Institutes of Health Stroke Scale (NIHSS) score and mortality were collected and analyzed in relation to analytes. Results: BDNF levels at both time points were lower in patients with severe stroke and correlated negatively with NIHSS scores. No such associations were observed for NGF and NT-3. Patients who died had lower baseline BDNF, NT-4 and higher NT-3. Conclusions: A lower BDNF level, but no other neurotrophins, is associated with worse outcomes in ischemic stroke patients. NT-3 and NT-4 levels change in response to ischemic stroke.
Full article
(This article belongs to the Collection Biomarkers in Stroke Prognosis)
►▼
Show Figures

Figure 1
Open AccessReview
Genetic Architecture of Cognitive Resilience in Alzheimer’s Disease: Mechanisms, Pathways, and Therapeutic Implications
by
Gabriel Burdman, Juliet Akkaoui, Natalia Colon, Andres Perez and Madepalli K. Lakshmana
Neurol. Int. 2026, 18(3), 50; https://doi.org/10.3390/neurolint18030050 - 3 Mar 2026
Abstract
Background/Objectives: Alzheimer’s disease (AD) is defined by amyloid-β plaques and tau neurofibrillary tangles and is typically associated with progressive cognitive decline. However, a substantial subset of individuals remains cognitively intact despite intermediate-to-high AD pathology, a phenomenon termed cognitive resilience. This review aims
[...] Read more.
Background/Objectives: Alzheimer’s disease (AD) is defined by amyloid-β plaques and tau neurofibrillary tangles and is typically associated with progressive cognitive decline. However, a substantial subset of individuals remains cognitively intact despite intermediate-to-high AD pathology, a phenomenon termed cognitive resilience. This review aims to synthesize genetic variants and biological pathways associated with preserved cognition in the presence of AD neuropathology. Methods: We performed a narrative thematic synthesis of human genetic studies (GWAS, sequencing, biomarker-informed cohorts) and extreme resilience case reports. Variants were prioritized by replication, mechanistic plausibility, and relevance to clinicopathologic dissociation, and were organized by shared biological pathways. When applicable, cognitive resilience was operationalized using residual-based approaches modeling cognitive performance after adjustment for neuropathological burden, age, sex, and education or cognitive reserve proxies reported by each cohort. Results: Recurrent resilience-associated variants include APOE ε2, APOE3-Christchurch, RELN-COLBOS, ATP8B1, RAB10, PLCG2, PICALM, CLU, FN1, and synapse-linked markers such as NPTX2. These variants converge on lipid metabolism, synaptic function and neuroplasticity, tau regulation and proteostasis, immune and inflammatory signaling, vascular/BBB resilience, and RNA regulation. Conclusions: Genetic determinants of cognitive resilience highlight mechanisms that preserve neural integrity independent of pathological load. Targeting resilience pathways may enable precision therapies designed to maintain cognitive function in AD.
Full article
(This article belongs to the Special Issue Molecular and Cellular Research of Neuroprotection and Neurodegeneration)
►▼
Show Figures

Graphical abstract

Journal Menu
► ▼ Journal Menu-
- Neurology International Home
- Aims & Scope
- Editorial Board
- Instructions for Authors
- Special Issues
- Topics
- Sections & Collections
- Article Processing Charge
- Indexing & Archiving
- Editor’s Choice Articles
- Most Cited & Viewed
- Journal Statistics
- Journal History
- Journal Awards
- Society Collaborations
- Conferences
- Editorial Office
Journal Browser
► ▼ Journal BrowserHighly Accessed Articles
Latest Books
E-Mail Alert
News
Topics
Topic in
Brain Sciences, Neurology International, NeuroSci, JDAD
Impacts of Sex Hormones on Memory and Aging
Topic Editors: Carolina Villada, Vanesa Hidalgo, Caroline GurvichDeadline: 25 May 2026
Topic in
Biomedicines, IJMS, JCM, Medicina, Neurology International
Advances in Exercise-Induced Neurogenesis, Neuronal and Functional Adaptations in Neurorehabilitation
Topic Editors: Carlos Bernal-Utrera, Cleofas Rodriguez-Blanco, Maria Livia Carrascal MorenoDeadline: 29 June 2026
Topic in
Geriatrics, IJMS, Life, Sports, Neurology International, Obesities
Exercise and Human Aging: Physiological and Psychological Functions
Topic Editors: Samuel Da Silva Aguiar, Ismael Perez-SuarezDeadline: 20 September 2026
Topic in
Brain Sciences, Clocks & Sleep, Neurology International, NeuroSci
Translational Advances in Neurodegenerative Dementias, Second Edition
Topic Editors: Francesco Di Lorenzo, Annibale AntonioniDeadline: 30 September 2026

Conferences
Special Issues
Special Issue in
Neurology International
Mechanism and Treatment for Psychiatric and Neurological Disorders
Guest Editor: Rakesh KumarDeadline: 30 April 2026
Special Issue in
Neurology International
Towards an All-Inclusive Paradigm for Acute Stroke Treatment—Challenges and Innovations
Guest Editors: Riwaj Bhagat, Ekokobe FonkemDeadline: 30 April 2026
Special Issue in
Neurology International
Advances in Molecular Mechanisms of Neurodegenerative Diseases
Guest Editors: Pravin Hivare, Joshna Gadhavi, Cristoforo ComiDeadline: 30 April 2026
Special Issue in
Neurology International
Cerebrovascular Disease: Update on Diagnosis and Treatment
Guest Editors: Marialuisa Zedde, Rosario PascarellaDeadline: 31 May 2026
Topical Collections
Topical Collection in
Neurology International
Advances in Neurodegenerative Diseases
Collection Editors: Vasileios Siokas, Efthimios Dardiotis
Topical Collection in
Neurology International
Biomarkers in Stroke Prognosis
Collection Editors: Dimitrios Tsiptsios, Konstantinos Vadikolias
Topical Collection in
Neurology International
Exclusive Papers from the Editorial Board Members (EBMs) of Neurology InternationalCollection Editor: Junji Yamauchi
Topical Collection in
Neurology International
Feature Papers in Movement Disorders and Neurodegenerative Diseases
Collection Editors: Tibor Hortobágyi, Cristoforo Comi