-
 Primary Multi-Systemic Metastases in Osteosarcoma: Presentation, Treatment, and Survival of 83 Patients of the Cooperative Osteosarcoma Study Group
Primary Multi-Systemic Metastases in Osteosarcoma: Presentation, Treatment, and Survival of 83 Patients of the Cooperative Osteosarcoma Study Group -
 Addressing Genetic Tumor Heterogeneity, Post-Therapy Metastatic Spread, Cancer Repopulation, and Development of Acquired Tumor Cell Resistance
Addressing Genetic Tumor Heterogeneity, Post-Therapy Metastatic Spread, Cancer Repopulation, and Development of Acquired Tumor Cell Resistance -
 The Role of Macrophages in Sarcoma Tumor Microenvironment and Treatment
The Role of Macrophages in Sarcoma Tumor Microenvironment and Treatment -
 Synergistic Sensitization of High-Grade Serous Ovarian Cancer Cells Lacking Caspase-8 Expression to Chemotherapeutics Using Combinations of Small-Molecule BRD4 and CDK9 Inhibitors
Synergistic Sensitization of High-Grade Serous Ovarian Cancer Cells Lacking Caspase-8 Expression to Chemotherapeutics Using Combinations of Small-Molecule BRD4 and CDK9 Inhibitors
Journal Description
Cancers
Cancers
is a peer-reviewed, open access journal of oncology, published semimonthly online by MDPI. The Irish Association for Cancer Research (IACR), Spanish Association for Cancer Research (ASEICA), Biomedical Research Centre (CIBM), British Neuro-Oncology Society (BNOS) and Spanish Group for Cancer Immuno-Biotherapy (GÉTICA) are affiliated with Cancers and their members receive a discount on the article processing charges.
- Open Access— free for readers, with article processing charges (APC) paid by authors or their institutions.
- High Visibility: indexed within Scopus, SCIE (Web of Science), PubMed, PMC, Embase, CAPlus / SciFinder, and other databases.
- Journal Rank: JCR - Q2 (Oncology) / CiteScore - Q1 (Oncology)
- Rapid Publication: manuscripts are peer-reviewed and a first decision is provided to authors approximately 17.9 days after submission; acceptance to publication is undertaken in 2.8 days (median values for papers published in this journal in the second half of 2023).
- Recognition of Reviewers: reviewers who provide timely, thorough peer-review reports receive vouchers entitling them to a discount on the APC of their next publication in any MDPI journal, in appreciation of the work done.
- Sections: published in 18 topical sections.
- Companion journals for Cancers include: Radiation and Onco.
Impact Factor:
5.2 (2022);
5-Year Impact Factor:
5.6 (2022)
Latest Articles
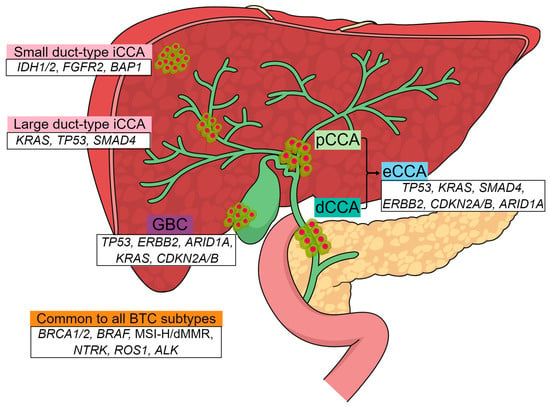
Recent Advancement in Diagnosis of Biliary Tract Cancer through Pathological and Molecular Classifications
Cancers 2024, 16(9), 1761; https://doi.org/10.3390/cancers16091761 (registering DOI) - 01 May 2024
Abstract
Biliary tract cancers (BTCs), including intrahepatic, perihilar, and distal cholangiocarcinomas, as well as gallbladder cancer, are a diverse group of cancers that exhibit unique molecular characteristics in each of their anatomic and pathological subtypes. The pathological classification of BTCs compromises distinct growth patterns,
[...] Read more.
Biliary tract cancers (BTCs), including intrahepatic, perihilar, and distal cholangiocarcinomas, as well as gallbladder cancer, are a diverse group of cancers that exhibit unique molecular characteristics in each of their anatomic and pathological subtypes. The pathological classification of BTCs compromises distinct growth patterns, including mass forming, periductal infiltrating, and intraductal growing types, which can be identified through gross examination. The small-duct and large-duct types of intrahepatic cholangiocarcinoma have been recently introduced into the WHO classification. The presentation of typical clinical symptoms, as well as the extensive utilization of radiological, endoscopic, and molecular diagnostic methods, is thoroughly detailed in the description. To overcome the limitations of traditional tissue acquisition methods, new diagnostic modalities are being explored. The treatment landscape is also rapidly evolving owing to the emergence of distinct subgroups with unique molecular alterations and corresponding targeted therapies. Furthermore, we emphasize the crucial aspects of diagnosing BTC in practical clinical settings.
Full article
(This article belongs to the Special Issue Current Epidemiologic, Diagnostic, and Therapeutic Aspects of Cholangiocarcinoma (CCA))
►
Show Figures
Open AccessArticle
Real-World Data Analysis of CDK4/6 Inhibitor Therapy—A Patient-Centric Single Center Study
by
Isabell Ge, Kai Berner, Marlene Mathis, Catherine Hensgen, Sebastian Mayer, Thalia Erbes, Ingolf Juhasz-Böss and Jasmin Asberger
Cancers 2024, 16(9), 1760; https://doi.org/10.3390/cancers16091760 (registering DOI) - 01 May 2024
Abstract
Background: The quest to comprehend the real-world efficacy of CDK4/6 inhibitors (CDKis) in breast cancer continues, as patient responses vary significantly. Methods: This single-center retrospective study evaluated CDKi use outside the trial condition from November 2016 to May 2020. Progression-free survival (PFS), time-to-treatment
[...] Read more.
Background: The quest to comprehend the real-world efficacy of CDK4/6 inhibitors (CDKis) in breast cancer continues, as patient responses vary significantly. Methods: This single-center retrospective study evaluated CDKi use outside the trial condition from November 2016 to May 2020. Progression-free survival (PFS), time-to-treatment failure (TTF), short-term and prolonged treatment benefit (≥4 and ≥10 months), as well as prognostic and predictive markers were assessed with Kaplan–Meier and multivariate regression analyses. Results: Out of 86 identified patients, 58 (67.4%) had treatment failure of which 40 (46.5%) were due to progression. Median PFS and TTF were 12 and 8.5 months, respectively. A total of 57 (66.3%) and 42 (48.8%) patients experienced short-term and prolonged treatment benefit. Independent, significant predictors for PFS were progesterone receptor expression (HR: 0.88), multiple metastatic sites (HR: 2.56), and hepatic metastasis (HR: 2.01). Significant predictors for TTF were PR expression (HR: 0.86), multiple sites (HR: 3.29), adverse events (HR: 2.35), and diabetes (HR: 2.88). Aside from tumor biology and adverse events, treatment modifications like pausing and switching of CDKi were predictive for short-term (OR: 6.73) and prolonged (OR: 14.27) therapeutic benefit, respectively. Conclusions: These findings emphasize the importance of tailored treatment strategies, highlighting the role of PR expression, metastatic burden, and therapeutic adjustments in optimizing patient outcomes in real-world breast cancer management.
Full article
(This article belongs to the Special Issue CDK4/6 Inhibitors in Breast Cancer)
►▼
Show Figures
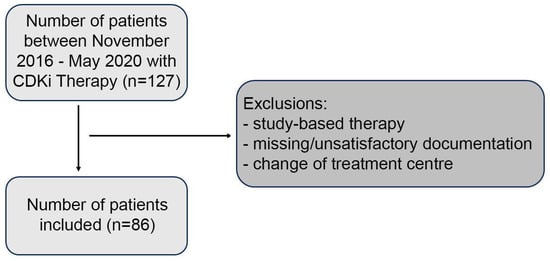
Figure 1
Open AccessArticle
Kinetics of IFNγ-Induced Cytokines and Development of Immune-Related Adverse Events in Patients Receiving PD-(L)1 Inhibitors
by
Leticia Alserawan, Maria Mulet, Geòrgia Anguera, Mariona Riudavets, Carlos Zamora, Rubén Osuna-Gómez, Jorgina Serra-López, Andrés Barba Joaquín, Ivana Sullivan, Margarita Majem and Silvia Vidal
Cancers 2024, 16(9), 1759; https://doi.org/10.3390/cancers16091759 (registering DOI) - 01 May 2024
Abstract
Immune checkpoint inhibitors (ICI) have the potential to trigger unpredictable immune-related adverse events (irAEs), which can be severe. The underlying mechanisms of these events are not fully understood. As PD-L1 is upregulated by IFN, the heightened immune activation resulting from PD-1/PD-L1 inhibition may
[...] Read more.
Immune checkpoint inhibitors (ICI) have the potential to trigger unpredictable immune-related adverse events (irAEs), which can be severe. The underlying mechanisms of these events are not fully understood. As PD-L1 is upregulated by IFN, the heightened immune activation resulting from PD-1/PD-L1 inhibition may enhance the IFN response, triggering the expression of IFN-inducible genes and contributing to irAE development and its severity. In this study, we investigated the interplay between irAEs and the expression of IFN-inducible chemokines and cytokines in 134 consecutive patients with solid tumours treated with PD-(L)1 inhibitors as monotherapy or in combination with chemotherapy or other immunotherapy agents. We compared the plasma levels of IFN-associated cytokines (CXCL9/10/11, IL-18, IL-10, IL-6 and TGFβ) at various time points (at baseline, at the onset of irAE and previous to irAE onset) in three patient groups categorized by irAE development and severity: patients with serious irAEs, mild irAEs and without irAEs after PD-(L)1 inhibitors. No differences were observed between groups at baseline. However, patients with serious irAEs exhibited significant increases in CXCL9/10/11, IL-18 and IL-10 levels at the onset of the irAE compared to baseline. A network analysis and correlation patterns highlighted a robust relationship among these chemokines and cytokines at serious-irAE onset. Combining all of the analysed proteins in a cluster analysis, we identified a subgroup of patients with a higher incidence of serious irAEs affecting different organs or systems. Finally, an ROC analysis and a decision tree model proposed IL-18 levels ≥ 807 pg/mL and TGFβ levels ≤ 114 pg/mL as predictors for serious irAEs in 90% of cases. In conclusion, our study elucidates the dynamic changes in cytokine profiles associated with serious irAE development during treatment with PD-(L)1 inhibitors. The study’s findings offer valuable insights into the intricate IFN-induced immune responses associated with irAEs and propose potential predictive markers for their severity.
Full article
(This article belongs to the Section Cancer Immunology and Immunotherapy)
►▼
Show Figures
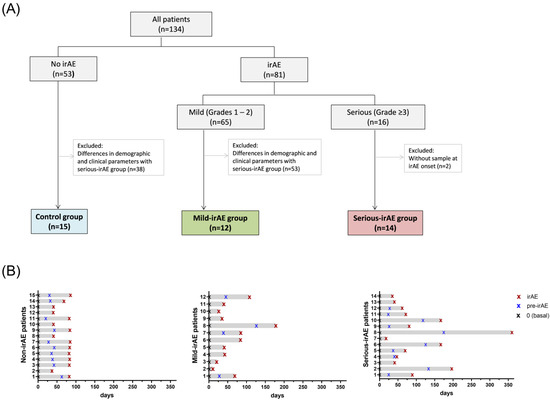
Figure 1
Open AccessArticle
Building a Bridge to Community: A Pragmatic Randomized Trial Examining a Combined Physical Therapy and Resistance Exercise Intervention for People after Head and Neck Cancer
by
Margaret L. McNeely, K. Ming Chan, Ryan A. Spychka, Joni Nedeljak, Brock Debenham, Naresh Jha and Hadi Seikaly
Cancers 2024, 16(9), 1758; https://doi.org/10.3390/cancers16091758 (registering DOI) - 01 May 2024
Abstract
Background: Established barriers to general exercise and physical activity among individuals with head and neck cancer include dry mouth, difficulty eating, weight loss, fear of injury, comorbidities, and treatment-related symptoms of pain and fatigue. Methods/Design: A 12-week pragmatic randomized controlled trial was conducted
[...] Read more.
Background: Established barriers to general exercise and physical activity among individuals with head and neck cancer include dry mouth, difficulty eating, weight loss, fear of injury, comorbidities, and treatment-related symptoms of pain and fatigue. Methods/Design: A 12-week pragmatic randomized controlled trial was conducted followed by an optional supported exercise transition phase. Eligible participants were individuals with head and neck cancers who had undergone surgery and/or radiation therapy to lymph node regions in the neck. Participants were randomized to a comparison group involving a shoulder and neck physiotherapeutic exercise protocol, or to a combined experimental group comprising the shoulder and neck physiotherapeutic exercise protocol and lower-body resistance exercise training. The primary outcome of this study was fatigue-related quality of life. Results: Sixty-one participants enrolled, 59 (97%) completed the randomized trial phase, 55 (90%) completed the 24-week follow-up, and 52 (85%) completed the one-year follow-up. Statistically significant between-group differences were found in favor of the combined experimental group for the fatigue-related quality of life, fitness outcomes, and overall physical activity. Paired comparisons confirmed significant within-group improvements for both groups from baseline to one-year follow-up across most outcomes. Discussion: A group-based combined physiotherapeutic and lower-body resistance exercise program was feasible and effective. Findings are limited to individuals who had undergone a surgical neck dissection procedure. Given the complexity of head and neck cancer, further pragmatic interdisciplinary research is warranted.
Full article
(This article belongs to the Special Issue 2nd Edition: Targeting Head and Neck Cancer)
►▼
Show Figures
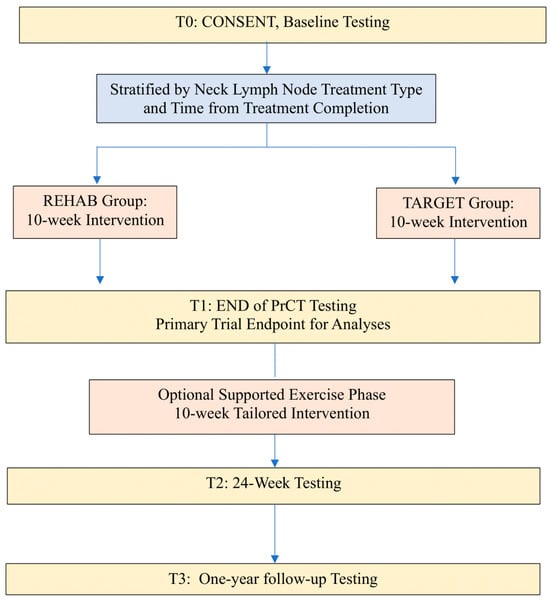
Figure 1
Open AccessArticle
snRNAs from Radical Prostatectomy Specimens Have the Potential to Serve as Prognostic Factors for Clinical Recurrence after Biochemical Recurrence in Patients with High-Risk Prostate Cancer
by
Hikaru Mikami, Syunya Noguchi, Jun Akatsuka, Hiroya Hasegawa, Kotaro Obayashi, Hayato Takeda, Yuki Endo, Yuka Toyama, Hiroyuki Takei, Go Kimura, Yukihiro Kondo and Toshihiro Takizawa
Cancers 2024, 16(9), 1757; https://doi.org/10.3390/cancers16091757 (registering DOI) - 01 May 2024
Abstract
In patients with high-risk prostate cancer (HRPC) after radical prostatectomy (RP), biochemical recurrence (BCR) increases the risk of distant metastasis. Accordingly, additional prognostic biomarkers are required to identify the subpopulation of patients with HRPC who develop clinical recurrence (CR) after BCR. The objective
[...] Read more.
In patients with high-risk prostate cancer (HRPC) after radical prostatectomy (RP), biochemical recurrence (BCR) increases the risk of distant metastasis. Accordingly, additional prognostic biomarkers are required to identify the subpopulation of patients with HRPC who develop clinical recurrence (CR) after BCR. The objective of this study was to identify biomarkers in formalin-fixed paraffin-embedded (FFPE) RP samples that are prognostic for CR in patients with HRPC who experience BCR after RP (post-RP BCR). First, we performed a preliminary RNA sequencing analysis to comprehensively profile RNA expression in FFPE RP samples obtained from patients with HRPC who developed CR after post-RP BCR and found that many snRNAs were very abundant in preserved FFPE samples. Subsequently, we used quantitative polymerase chain reaction (qPCR) to compare the expression levels of highly abundant snRNAs in FFPE RP samples from patients with HRPC with and without CR after post-RP BCR (21 CR patients and 46 non-CR patients who had more than 5 years of follow-up after BCR). The qPCR analysis revealed that the expression levels of snRNA RNU1-1/1-2 and RNU4-1 were significantly higher in patients with CR than in patients without CR. These snRNAs were significantly correlated with clinical recurrence-free survival (RFS) in patients with HRPC who experienced post-RP BCR. Furthermore, snRNA RNU1-1/1-2 could serve as an independent prognostic factor for clinical RFS in post-RP BCR of HRPC cases where known prognostic factors (e.g., Gleason score) cannot distinguish between CR and non-CR patients. Our findings provide new insights into the involvement of snRNAs in prostate cancer progression.
Full article
(This article belongs to the Special Issue Biomarkers in Prostate Cancers)
►▼
Show Figures
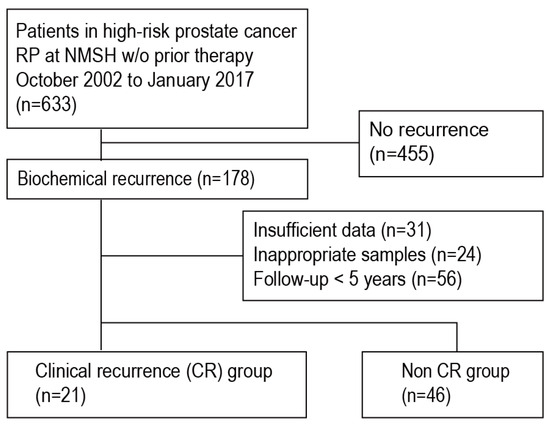
Figure 1
Open AccessArticle
Interventional Treatments of Colorectal Liver Metastases Using Thermal Ablation and Transarterial Chemoembolization: A Single-Center Experience over 26 Years
by
Thomas J. Vogl, Jason Freichel, Tatjana Gruber-Rouh, Nour-Eldin Abdelrehim Nour-Eldin, Wolf-Otto Bechstein, Stefan Zeuzem, Nagy N. N. Naguib, Ulrich Stefenelli and Hamzah Adwan
Cancers 2024, 16(9), 1756; https://doi.org/10.3390/cancers16091756 (registering DOI) - 30 Apr 2024
Abstract
The aim of this study was to analyze the long-term results of different locoregional treatments for colorectal cancer liver metastases (CRLM), including transarterial chemoembolization (TACE), laser-induced thermotherapy (LITT) and microwave ablation (MWA). A total of 2140 patients with CRLM treated at our department
[...] Read more.
The aim of this study was to analyze the long-term results of different locoregional treatments for colorectal cancer liver metastases (CRLM), including transarterial chemoembolization (TACE), laser-induced thermotherapy (LITT) and microwave ablation (MWA). A total of 2140 patients with CRLM treated at our department between 1993 and 2020 were included in this retrospective study. The patients were divided into the following groups: LITT (573 patients; median age: 62 years), TACE + LITT (346 patients; median age: 62 years), MWA (67 patients; median age: 59 years), TACE + MWA (152 patients; median age: 65 years), and TACE (1002 patients; median age: 62 years). Median survival was 1.9 years in the LITT group and 1.7 years in the TACE + LITT group. The median survival times in the MWA group and TACE + MWA group were 3.1 years and 2.1 years, respectively. The median survival in the TACE group was 0.8 years. The 1-, 3-, and 5-year survival rates were 77%, 27%, and 9% in the LITT group and 74%, 18%, and 5% in the TACE + LITT group, respectively. The corresponding survival rates were 80%, 55%, and 33% in the MWA group, 74%, 36%, and 20% in the TACE + MWA group and 37%, 3%, and 0% in the TACE group, respectively. The long-term results of this study demonstrate the efficacy of locoregional treatments in treating patients with CRLM. The longest survival was found in the MWA group, followed by the combination therapy of TACE and MWA.
Full article
(This article belongs to the Section Cancer Epidemiology and Prevention)
►▼
Show Figures

Figure 1
Open AccessArticle
Activation of the Anaphase Promoting Complex Restores Impaired Mitotic Progression and Chemosensitivity in Multiple Drug-Resistant Human Breast Cancer
by
Mathew Lubachowski, Cordell VanGenderen, Sarah Valentine, Zach Belak, Gerald Floyd Davies, Terra Gayle Arnason and Troy Anthony Alan Harkness
Cancers 2024, 16(9), 1755; https://doi.org/10.3390/cancers16091755 - 30 Apr 2024
Abstract
The development of multiple-drug-resistant (MDR) cancer all too often signals the need for alternative toxic therapy or palliative care. Our recent in vivo and in vitro studies using canine MDR lymphoma cancer cells demonstrate that the Anaphase Promoting Complex (APC) is impaired in
[...] Read more.
The development of multiple-drug-resistant (MDR) cancer all too often signals the need for alternative toxic therapy or palliative care. Our recent in vivo and in vitro studies using canine MDR lymphoma cancer cells demonstrate that the Anaphase Promoting Complex (APC) is impaired in MDR cells compared to normal canine control and drug-sensitive cancer cells. Here, we sought to establish whether this phenomena is a generalizable mechanism independent of species, malignancy type, or chemotherapy regime. To test the association of blunted APC activity with MDR cancer behavior, we used matched parental and MDR MCF7 human breast cancer cells, and a patient-derived xenograft (PDX) model of human triple-negative breast cancer. We show that APC activating mechanisms, such as APC subunit 1 (APC1) phosphorylation and CDC27/CDC20 protein associations, are reduced in MCF7 MDR cells when compared to chemo-sensitive matched cell lines. Consistent with impaired APC function in MDR cells, APC substrate proteins failed to be effectively degraded. Similar to our previous observations in canine MDR lymphoma cells, chemical activation of the APC using Mad2 Inhibitor-1 (M2I-1) in MCF7 MDR cells enhanced APC substrate degradation and resensitized MDR cells in vitro to the cytotoxic effects of the alkylating chemotherapeutic agent, doxorubicin (DOX). Using cell cycle arrest/release experiments, we show that mitosis is delayed in MDR cells with elevated substrate levels. When pretreated with M2I-1, MDR cells progress through mitosis at a faster rate that coincides with reduced levels of APC substrates. In our PDX model, mice growing a clinically MDR human triple-negative breast cancer tumor show significantly reduced tumor growth when treated with M2I-1, with evidence of increased DNA damage and apoptosis. Thus, our results strongly support the hypothesis that APC impairment is a driver of aggressive tumor development and that targeting the APC for activation has the potential for meaningful clinical benefits in treating recurrent cases of MDR malignancy.
Full article
(This article belongs to the Special Issue Molecular Insights into Drug Resistance in Cancer)
►▼
Show Figures
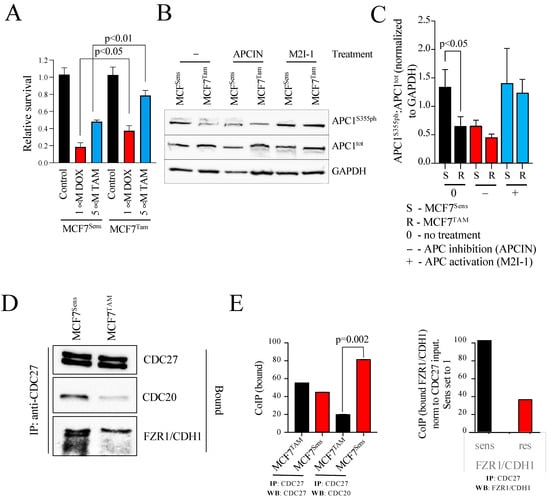
Figure 1
Open AccessArticle
Antiretroviral Drug Repositioning for Glioblastoma
by
Sarah R. Rivas, Mynor J. Mendez Valdez, Jay S. Chandar, Jelisah F. Desgraves, Victor M. Lu, Leo Ampie, Eric B. Singh, Deepa Seetharam, Christian K. Ramsoomair, Anna Hudson, Shreya M. Ingle, Vaidya Govindarajan, Tara T. Doucet-O’Hare, Catherine DeMarino, John D. Heiss, Avindra Nath and Ashish H. Shah
Cancers 2024, 16(9), 1754; https://doi.org/10.3390/cancers16091754 - 30 Apr 2024
Abstract
Outcomes for glioblastoma (GBM) remain poor despite standard-of-care treatments including surgical resection, radiation, and chemotherapy. Intratumoral heterogeneity contributes to treatment resistance and poor prognosis, thus demanding novel therapeutic approaches. Drug repositioning studies on antiretroviral therapy (ART) have shown promising potent antineoplastic effects in
[...] Read more.
Outcomes for glioblastoma (GBM) remain poor despite standard-of-care treatments including surgical resection, radiation, and chemotherapy. Intratumoral heterogeneity contributes to treatment resistance and poor prognosis, thus demanding novel therapeutic approaches. Drug repositioning studies on antiretroviral therapy (ART) have shown promising potent antineoplastic effects in multiple cancers; however, its efficacy in GBM remains unclear. To better understand the pleiotropic anticancer effects of ART on GBM, we conducted a comprehensive drug repurposing analysis of ART in GBM to highlight its utility in translational neuro-oncology. To uncover the anticancer role of ART in GBM, we conducted a comprehensive bioinformatic and in vitro screen of antiretrovirals against glioblastoma. Using the DepMap repository and reversal of gene expression score, we conducted an unbiased screen of 16 antiretrovirals in 40 glioma cell lines to identify promising candidates for GBM drug repositioning. We utilized patient-derived neurospheres and glioma cell lines to assess neurosphere viability, proliferation, and stemness. Our in silico screen revealed that several ART drugs including reverse transcriptase inhibitors (RTIs) and protease inhibitors (PIs) demonstrated marked anti-glioma activity with the capability of reversing the GBM disease signature. RTIs effectively decreased cell viability, GBM stem cell markers, and proliferation. Our study provides mechanistic and functional insight into the utility of ART repurposing for malignant gliomas, which supports the current literature. Given their safety profile, preclinical efficacy, and neuropenetrance, ARTs may be a promising adjuvant treatment for GBM.
Full article
(This article belongs to the Special Issue Glioblastoma: Advances in Molecular Insights and Therapeutic Strategies)
►▼
Show Figures
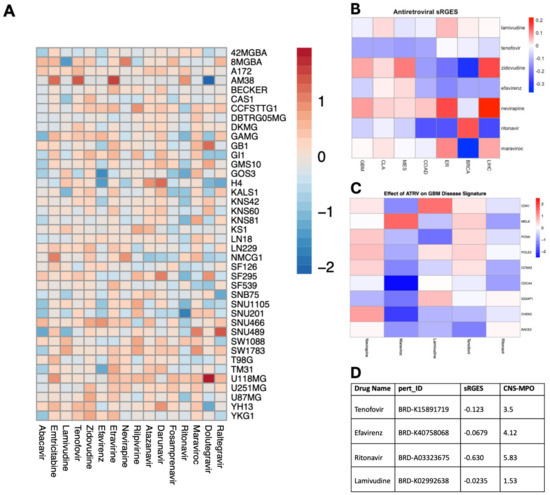
Figure 1
Open AccessReview
The Evolving Classification of Meningiomas: Integration of Molecular Discoveries to Inform Patient Care
by
S. Joy Trybula, Mark W. Youngblood, Constantine L. Karras, Nikhil K. Murthy, Amy B. Heimberger, Rimas V. Lukas, Sean Sachdev, John A. Kalapurakal, James P. Chandler, Daniel J. Brat, Craig M. Horbinski and Stephen T. Magill
Cancers 2024, 16(9), 1753; https://doi.org/10.3390/cancers16091753 - 30 Apr 2024
Abstract
Meningioma classification and treatment have evolved over the past eight decades. Since Bailey, Cushing, and Eisenhart’s description of meningiomas in the 1920s and 1930s, there have been continual advances in clinical stratification by histopathology, radiography and, most recently, molecular profiling, to improve prognostication
[...] Read more.
Meningioma classification and treatment have evolved over the past eight decades. Since Bailey, Cushing, and Eisenhart’s description of meningiomas in the 1920s and 1930s, there have been continual advances in clinical stratification by histopathology, radiography and, most recently, molecular profiling, to improve prognostication and predict response to therapy. Precise and accurate classification is essential to optimizing management for patients with meningioma, which involves surveillance imaging, surgery, primary or adjuvant radiotherapy, and consideration for clinical trials. Currently, the World Health Organization (WHO) grade, extent of resection (EOR), and patient characteristics are used to guide management. While these have demonstrated reliability, a substantial number of seemingly benign lesions recur, suggesting opportunities for improvement of risk stratification. Furthermore, the role of adjuvant radiotherapy for grade 1 and 2 meningioma remains controversial. Over the last decade, numerous studies investigating the molecular drivers of clinical aggressiveness have been reported, with the identification of molecular markers that carry clinical implications as well as biomarkers of radiotherapy response. Here, we review the historical context of current practices, highlight recent molecular discoveries, and discuss the challenges of translating these findings into clinical practice.
Full article
(This article belongs to the Special Issue Molecular Pathology of Brain Tumors)
►▼
Show Figures
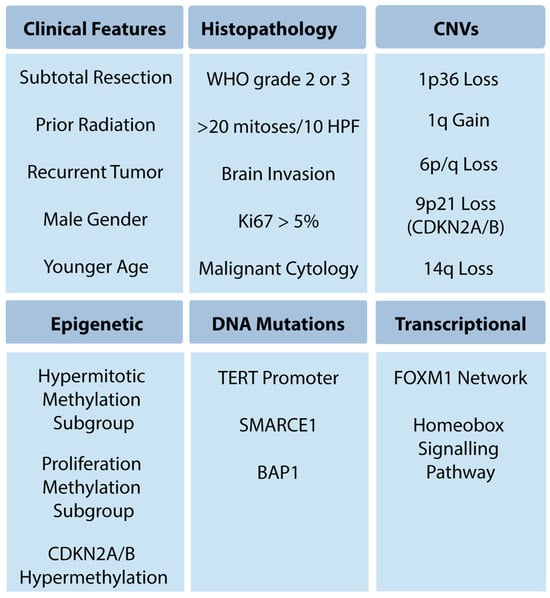
Figure 1
Open AccessReview
Drivers Underlying Metastasis and Relapse in Medulloblastoma and Targeting Strategies
by
Karl O. Holmberg, Anna Borgenvik, Miao Zhao, Géraldine Giraud and Fredrik J. Swartling
Cancers 2024, 16(9), 1752; https://doi.org/10.3390/cancers16091752 - 30 Apr 2024
Abstract
Medulloblastomas comprise a molecularly diverse set of malignant pediatric brain tumors in which patients are stratified according to different prognostic risk groups that span from very good to very poor. Metastasis at diagnosis is most often a marker of poor prognosis and the
[...] Read more.
Medulloblastomas comprise a molecularly diverse set of malignant pediatric brain tumors in which patients are stratified according to different prognostic risk groups that span from very good to very poor. Metastasis at diagnosis is most often a marker of poor prognosis and the relapse incidence is higher in these children. Medulloblastoma relapse is almost always fatal and recurring cells have, apart from resistance to standard of care, acquired genetic and epigenetic changes that correlate with an increased dormancy state, cell state reprogramming and immune escape. Here, we review means to carefully study metastasis and relapse in preclinical models, in light of recently described molecular subgroups. We will exemplify how therapy resistance develops at the cellular level, in a specific niche or from therapy-induced secondary mutations. We further describe underlying molecular mechanisms on how tumors acquire the ability to promote leptomeningeal dissemination and discuss how they can establish therapy-resistant cell clones. Finally, we describe some of the ongoing clinical trials of high-risk medulloblastoma and suggest or discuss more individualized treatments that could be of benefit to specific subgroups.
Full article
(This article belongs to the Special Issue The Biological Diversity and Therapeutic Implications of Medulloblastoma Metastases and Recurrence)
►▼
Show Figures
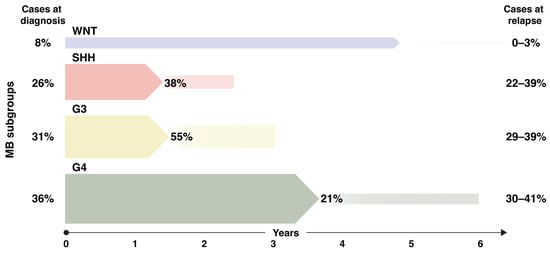
Figure 1
Open AccessReview
Challenges and Opportunities in Breast Cancer Care in Low-Resourced Countries, Jordan as An Example
by
Hikmat Abdel-Razeq and Asem Mansour
Cancers 2024, 16(9), 1751; https://doi.org/10.3390/cancers16091751 - 30 Apr 2024
Abstract
Jordan is a relatively small country with a rapidly growing population and a challenged economy. Breast cancer is the most diagnosed cancer among women worldwide and also in Jordan. Though the age-standardized rate (ASR) of breast cancer incidence is still lower than that
[...] Read more.
Jordan is a relatively small country with a rapidly growing population and a challenged economy. Breast cancer is the most diagnosed cancer among women worldwide and also in Jordan. Though the age-standardized rate (ASR) of breast cancer incidence is still lower than that in Western societies, the number of newly diagnosed cases continues to increase, involving younger women, and new cases are usually detected at more advanced stages. Improvements in breast cancer care across the health care continuum, including early detection, prevention, treatment, and survivorship and palliative care, have become very visible, but may not match the magnitude of the problem. More organized, goal-oriented work is urgently needed to downstage the disease and improve awareness of, access to, and participation in early detection programs. The cost of recently introduced anti-cancer therapies poses a great challenge, but the impact of these therapies on treatment outcomes, including overall survival, is becoming very noticeable. Though the concept of a multidisciplinary approach to breast cancer treatment is often used at most health care facilities, its implementation in real practice varies significantly. The availability of breast reconstruction procedures, survivorship programs, germline genetic testing, counselling, and palliative care is improving, but these are not widely practiced. In this manuscript, we review the status of breast cancer in Jordan and highlight some of the existing challenges and opportunities.
Full article
(This article belongs to the Special Issue Health Services Research in Cancer Care)
►▼
Show Figures
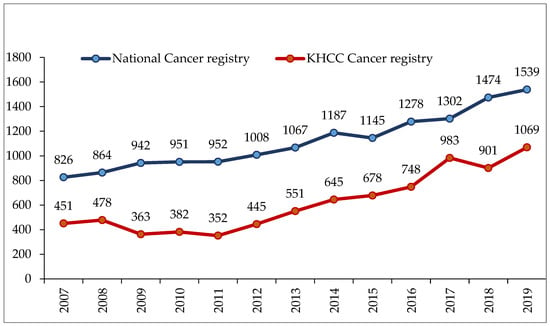
Figure 1
Open AccessArticle
Anticancer Activity of Encapsulated Pearl Millet Polyphenol-Rich Extract against Proliferating and Non-Proliferating Breast Cancer Cells In Vitro
by
Latifa Hajri, Anna Lewińska, Iwona Rzeszutek, Bernadetta Oklejewicz, Renata Wojnarowska-Nowak, Agnieszka Krogul-Sobczak, Ewa Szpyrka, Alfredo Aires, Soumaya Ghodbane, Mohamed Ammari and Maciej Wnuk
Cancers 2024, 16(9), 1750; https://doi.org/10.3390/cancers16091750 - 30 Apr 2024
Abstract
Plant-derived polyphenols are bioactive compounds with potential health-promoting properties including antioxidant, anti-inflammatory, and anticancer activity. However, their beneficial effects and biomedical applications may be limited due to their low bioavailability. In the present study, we have considered a microencapsulation-based drug delivery system to
[...] Read more.
Plant-derived polyphenols are bioactive compounds with potential health-promoting properties including antioxidant, anti-inflammatory, and anticancer activity. However, their beneficial effects and biomedical applications may be limited due to their low bioavailability. In the present study, we have considered a microencapsulation-based drug delivery system to investigate the anticancer effects of polyphenol-rich (apigenin, caffeic acid, and luteolin) fractions, extracted from a cereal crop pearl millet (Pennisetum glaucum), using three phenotypically different cellular models of breast cancer in vitro, namely triple negative HCC1806, ER-positive HCC1428, and HER2-positive AU565 cells. Encapsulated polyphenolic extract induced apoptotic cell death in breast cancer cells with different receptor status, whereas it was ineffective against non-tumorigenic MCF10F cells. Encapsulated polyphenolic extract was also found to be cytotoxic against drug-resistant doxorubicin-induced senescent breast cancer cells that were accompanied by increased levels of apoptotic and necrotic markers, cell cycle inhibitor p21 and proinflammatory cytokine IL8. Furthermore, diverse responses to the stimulation with encapsulated polyphenolic extract in senescent breast cancer cells were observed, as in the encapsulated polyphenolic extract-treated non-proliferating AU565 cells, the autophagic pathway, here cytotoxic autophagy, was also induced, as judged by elevated levels of beclin-1 and LC3b. We show for the first time the anti-breast cancer activity of encapsulated polyphenolic extract of pearl millet and postulate that microencapsulation may be a useful approach for potentiating the anticancer effects of phytochemicals with limited bioavailability.
Full article
(This article belongs to the Section Cancer Drug Development)
►▼
Show Figures
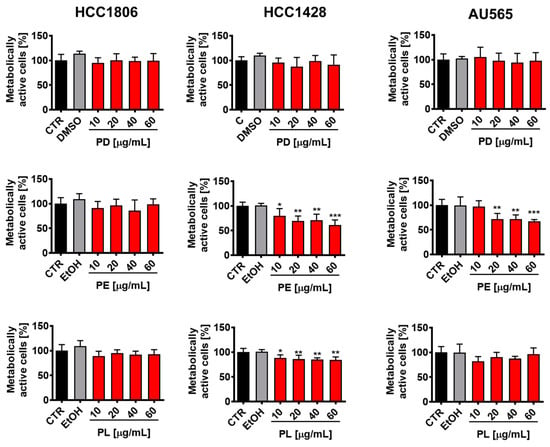
Figure 1
Open AccessArticle
Real-World Experience among Elderly Metastatic Breast Cancer Patients Treated with CDK4/6 Inhibitor-Based Therapy
by
Thomas N. O’Connor, Emily Schultz, Jianxin Wang, Tracey O’Connor, Ellis Levine, Erik S. Knudsen and Agnieszka K. Witkiewicz
Cancers 2024, 16(9), 1749; https://doi.org/10.3390/cancers16091749 - 30 Apr 2024
Abstract
The largest portion of breast cancer patients diagnosed after 70 years of age present with hormone receptor-positive (HR+) breast cancer subtypes. Cyclin-dependent kinase (CDK) 4/6 inhibitor treatment, in conjunction with endocrine therapy, has become standard-of-care for metastatic HR+ breast cancer. In total, 320
[...] Read more.
The largest portion of breast cancer patients diagnosed after 70 years of age present with hormone receptor-positive (HR+) breast cancer subtypes. Cyclin-dependent kinase (CDK) 4/6 inhibitor treatment, in conjunction with endocrine therapy, has become standard-of-care for metastatic HR+ breast cancer. In total, 320 patients with metastatic breast cancer receiving CDK4/6 inhibitor combined with fulvestrant or an aromatase inhibitor were enrolled in an ongoing observational study or were included in an IRB-approved retrospective study. All patients receiving CDK4/6 inhibitor-based therapy that were ≥70 years of age (n = 111) displayed prolonged progression-free survival (27.6 months) as compared to patients <70 years of age (n = 209, 21.1 months, HR = 1.38, p < 0.05). Specifically, patients receiving a CDK4/6 inhibitor with an aromatase inhibitor who were ≥70 years of age (n = 79) displayed exceptionally prolonged progression-free survival (46.0 months) as compared to patients receiving the same treatment who were <70 years of age (n = 161, 21.8 months, HR = 1.71, p < 0.01). However, patients ≥70 years of age also experienced more frequent adverse responses to CDK4/6 inhibitor-based treatment leading to dose reduction, hold, or discontinuation than the younger cohort (69% and 53%, respectively). Treatment strategies that may decrease toxicity without affecting efficacy (such as dose titration) are worth further exploration.
Full article
(This article belongs to the Special Issue The Long Reach of the Retinoblastoma Tumor Suppressor Pathway)
►▼
Show Figures
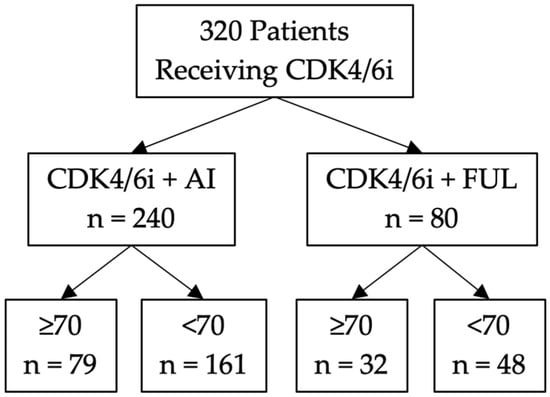
Figure 1
Open AccessArticle
Programmed Death Ligand-1 and Tumor Burden Score Dictate Treatment Responses in Patients with Recurrent or Metastatic Head and Neck Squamous Cell Carcinoma
by
Ming-Yu Lien, Chih-Chun Wang, Tzer-Zen Hwang, Ching-Yun Hsieh, Chuan-Chien Yang, Chien-Chung Wang, Ching-Feng Lien, Yu-Chen Shih, Shyh-An Yeh and Meng-Che Hsieh
Cancers 2024, 16(9), 1748; https://doi.org/10.3390/cancers16091748 - 30 Apr 2024
Abstract
Background: The significance of tumor burden for survival is unknown for patients with recurrent or metastatic head and neck squamous cell carcinoma (R/M HNSCC). The purpose of our study was to evaluate the prognostic impact of programmed death ligand-1 (PD-L1) and tumor burden
[...] Read more.
Background: The significance of tumor burden for survival is unknown for patients with recurrent or metastatic head and neck squamous cell carcinoma (R/M HNSCC). The purpose of our study was to evaluate the prognostic impact of programmed death ligand-1 (PD-L1) and tumor burden score (TBS) in patients with R/M HNSCC. Patients and Methods: R/M HNSCC patients who were treated with cisplatin, 5-fluorouracil plus cetuximab (EPF) or pembrolizumab (PPF) as first-line treatment were included in our study. PD-L1 and TBS were estimated and correlated with treatment responses. Kaplan–Meier curves were plotted for outcomes estimation. Results: A total of 252 R/M HNSCC patients were included, with 126 high tumor burden (HTB) and 126 low tumor burden (LTB) patients. Median progression-free survival (PFS) was 7.1 months in LTB and 3.9 months in HTB (p < 0.001) and median overall survival (OS) was 14.2 months in LTB and 9.2 months in HTB (p = 0.001). Patients with LTB had better PFS and OS than those with HTB independent of PD-L1 status. Subgroup analysis showed HTB patients treated with EPF had better survival than those treated with PPF, regardless of PD-L1 expression. For LTB PD-L1 positive patients, there was a longer survival with PPF than EPF, while for LTB PD-L1 negative patients, survival was similar between PPF and EPF. Multivariate analysis exhibited that tumor burden was significantly correlated with OS. Conclusions: Tumor burden is significantly correlated with survival in patients with R/M HNSCC. PD-L1 and TBS should be taken into consideration to determine first-line treatment.
Full article
(This article belongs to the Special Issue Head and Neck Cancers—Novel Approaches and Future Outlook)
►▼
Show Figures
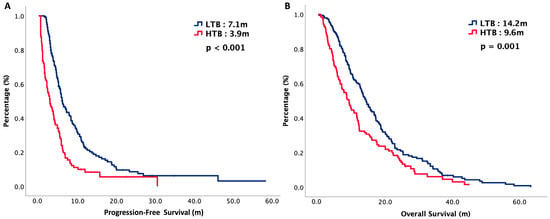
Figure 1
Open AccessReview
Recent Progress in Treatment for HER2-Positive Advanced Gastric Cancer
by
Takeshi Kawakami and Kentaro Yamazaki
Cancers 2024, 16(9), 1747; https://doi.org/10.3390/cancers16091747 - 30 Apr 2024
Abstract
Human epidermal receptor (HER) 2-positive advanced gastric cancer is one of the major subtypes of gastric cancer, accounting for ~20% of all cases. Although combination therapy with trastuzumab and chemotherapy provides meaningful survival benefit, clinical trials targeting HER2 have failed to demonstrate clinical
[...] Read more.
Human epidermal receptor (HER) 2-positive advanced gastric cancer is one of the major subtypes of gastric cancer, accounting for ~20% of all cases. Although combination therapy with trastuzumab and chemotherapy provides meaningful survival benefit, clinical trials targeting HER2 have failed to demonstrate clinical benefits in first- or subsequent-line treatment. Trastuzumab deruxtecan, an antibody–drug conjugate, has shown positive results even in later-line treatment and has become new standard treatment. In first-line therapy, combination therapy with pembrolizumab and trastuzumab plus chemotherapy demonstrated a dramatic response rate. Therefore, the FDA rapidly approved it without waiting for the results of survival time. The emergence of combination therapy including immunotherapy with HER2-targeting agents and the development of HER2 targeting agents with or without immunotherapy have been advancing for treating HER2-positive gastric cancer. In this review, we will discuss the current status of treatment development and future perspectives for HER2-positive gastric cancer.
Full article
(This article belongs to the Special Issue Feature Review Papers on Advanced Gastric Cancer)
►▼
Show Figures
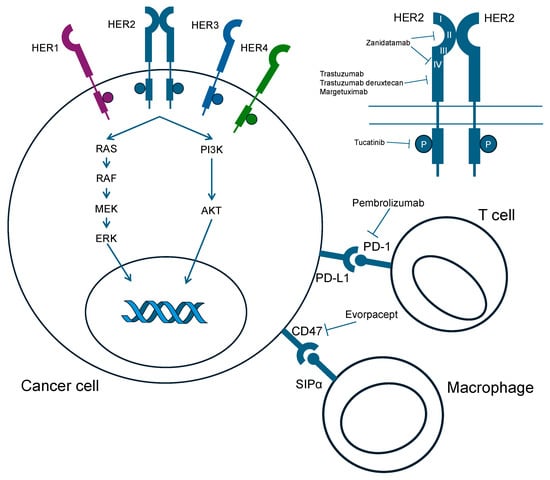
Figure 1
Open AccessArticle
Bovine Meat and Milk Factor-like Sequences Are Frequently Detected in Renal Cell Carcinoma Tissues
by
Ghalib Mobaraki, Shuai Shi, Kim M. Smits, Kim Severens, Kim Lommen, Dorit Rennspiess, Emil Chteinberg, Véronique Winnepenninckx, Iryna Samarska, Faisal Klufah and Axel zur Hausen
Cancers 2024, 16(9), 1746; https://doi.org/10.3390/cancers16091746 - 29 Apr 2024
Abstract
Previous studies have indicated a potential role of diet in the pathogenesis of renal cell carcinoma (RCC). Recently, circular bovine meat and milk factor (BMMF) DNAs have been identified in peritumoral tissues of human colon and breast cancers. Here, we investigated the prevalence
[...] Read more.
Previous studies have indicated a potential role of diet in the pathogenesis of renal cell carcinoma (RCC). Recently, circular bovine meat and milk factor (BMMF) DNAs have been identified in peritumoral tissues of human colon and breast cancers. Here, we investigated the prevalence of the DNA of these novel human pathogenic infectious agents in RCC and adjacent peritumoral renal tissues. DNA was extracted from formalin-fixed and paraffin-embedded (FFPE) RCC and peritumoral kidney tissues, including a test (n = 11) and a validation (n = 152) collection. BMMF1 and BMMF2 consensus primers were designed to screen for the presence of BMMF1- and BMMF2-like DNA. In addition, BMMF-specific PCR was performed on selected cases to test for the presence of additional regions of BMMF1 and BMMF2 genomes. A reference collection of hepatocellular carcinomas (HCCs; n = 60) and adjacent peritumoral liver tissues (n = 50) was also included. Our results demonstrated that BMMF1 and BMMF2 DNAs are frequently found in human RCC tissues and are particularly more prevalent in peritumoral kidney tissues. Of note, BMMF1 and BMMF2 genotype heterogeneity was higher in peritumoral kidney tissues compared to RCC tissues. This is the first study to directly test human FFPE tissues for BMMF1- and BMMF2-like DNA using consensus PCR and demonstrate BMMF DNA in neoplastic and peritumoral kidney tissues. The findings are in line with the recently proposed indirect etiopathogenetic role of BMMFs in, e.g., colorectal carcinogenesis. Follow-up studies are needed to explore the potential role of BMMFs in the etiopathogenesis of RCC.
Full article
(This article belongs to the Section Methods and Technologies Development)
Open AccessArticle
Incident Cancer Risk in Patients with Incident Type 2 Diabetes Mellitus in Hungary (Part 1)
by
Zsolt Abonyi-Tóth, György Rokszin, Ibolya Fábián, Zoltán Kiss, György Jermendy, Péter Kempler, Csaba Lengyel, István Wittmann, Gergő A. Molnár and Gábor Sütő
Cancers 2024, 16(9), 1745; https://doi.org/10.3390/cancers16091745 - 29 Apr 2024
Abstract
(1) Background: Patients with type 2 diabetes mellitus (T2DM) are at higher risk of cancer but how these two diseases associate is still debated. The goal of this study was the assessment of the overall incidence of cancer among patients with newly diagnosed
[...] Read more.
(1) Background: Patients with type 2 diabetes mellitus (T2DM) are at higher risk of cancer but how these two diseases associate is still debated. The goal of this study was the assessment of the overall incidence of cancer among patients with newly diagnosed T2DM in Hungary. (2) Methods: A nationwide, retrospective, longitudinal study was performed using a Hungarian database. After exclusion of cases of age < 18 years, with gestational diabetes, with polycystic ovary syndrome, and with type 1 and prevalent type 2 diabetes mellitus, the incident T2DM (approx. 50,000 cases yearly) and for comparison, the diabetes-free Hungarian adult population (approx. 7,000,000 cases yearly) was included in the study. The primary endpoints were the overall and site-specific incidence and annual percentage change of the incidence of cancer in both populations. (3) Results: The overall incidence of cancer in patients amounted to 29.4/1000 and 6.6/1000 with or without T2DM, respectively, and the OR (95%CI) of cancer of the T2DM group was 4.32 (4.14–4.53), p < 0.0001. The risk of having cancer was age dependent. The incidence of cancer was declining in the non-diabetic but was unchanged in the T2DM population. The average lag time of diagnosing cancer after the detection of T2DM was 3.86 months. (4) Conclusions: Incident T2DM is associated with a significantly higher overall risk of incident cancer, with a reverse correlation of age. Newly registered T2DM patients were suggested to be screened for cancer within 6 months.
Full article
(This article belongs to the Special Issue Cancer and Diabetes: What Connections Lie between Them?)
Open AccessArticle
Evolution of Complexity of Palliative Care Needs and Patient Profiles According to the PALCOM Scale (Part Two): Pooled Analysis of the Cohorts for the Development and Validation of the PALCOM Scale in Advanced Cancer Patients
by
Albert Tuca, Margarita Viladot, Gemma Carrera, Lucia Llavata, Carmen Barrera, Manoli Chicote, Javier Marco-Hernández, Joan Padrosa, Carles Zamora-Martínez, Ignacio Grafia, Anais Pascual, Carme Font and Elena Font
Cancers 2024, 16(9), 1744; https://doi.org/10.3390/cancers16091744 - 29 Apr 2024
Abstract
Introduction: Identifying the complexity of palliative care needs is a key aspect of referral to specialized multidisciplinary early palliative care (EPC) teams. The PALCOM scale is an instrument consisting of five multidimensional assessment domains developed in 2018 and validated in 2023 to identify
[...] Read more.
Introduction: Identifying the complexity of palliative care needs is a key aspect of referral to specialized multidisciplinary early palliative care (EPC) teams. The PALCOM scale is an instrument consisting of five multidimensional assessment domains developed in 2018 and validated in 2023 to identify the level of complexity in patients with advanced cancer. (1) Objectives: The main objective of this study was to determine the degree of instability (likelihood of level change or death), health resource consumption and the survival of patients according to the level of palliative complexity assigned at the baseline visit during a 6-month follow-up. (2) Method: An observational, prospective, multicenter study was conducted using pooled data from the development and validation cohort of the PALCOM scale. The main outcome variables were as follows: (a) instability ratio (IR), defined as the probability of level change or death; (b) emergency department visits; (c) days of hospitalization; (d) hospital death; (e) survival. All the variables were analyzed monthly according to the level of complexity assigned at the baseline visit. (3) Results: A total of 607 patients with advanced cancer were enrolled. According to the PALCOM scale, 20% of patients were classified as low complexity, 50% as medium and 30% as high complexity. The overall IR was 45% in the low complexity group, 68% in the medium complexity group and 78% in the high complexity group (p < 0.001). No significant differences in mean monthly emergency department visits (0.2 visits/ patient/month) were observed between the different levels of complexity. The mean number of days spent in hospital per month was 1.5 in the low complexity group, 1.8 in the medium complexity group and 3.2 in the high complexity group (p < 0.001). The likelihood of in-hospital death was significantly higher in the high complexity group (29%) compared to the medium (16%) and low (8%) complexity groups (p < 0.001). Six-month survival was significantly lower in the high complexity group (24%) compared to the medium (37%) and low (57%) complexity groups (p < 0.001). Conclusion: According to the PALCOM scale, more complex cases are associated with greater instability and use of hospital resources and lower survival. The data also confirm that the PALCOM scale is a consistent and useful tool for describing complexity profiles, targeting referrals to the EPC and managing the intensity of shared care.
Full article
(This article belongs to the Section Cancer Survivorship and Quality of Life)
Open AccessArticle
Quantitative Assessment of Tumor Contact with Neurogenic Zones and Its Effects on Survival: Insights beyond Traditional Predictors
by
Kirsten Jung, Johanna Kempter, Georg Prokop, Tim Herrmann, Michael Griessmair, Su-Hwan Kim, Claire Delbridge, Bernhard Meyer, Denise Bernhardt, Stephanie E. Combs, Claus Zimmer, Benedikt Wiestler, Friederike Schmidt-Graf and Marie-Christin Metz
Cancers 2024, 16(9), 1743; https://doi.org/10.3390/cancers16091743 - 29 Apr 2024
Abstract
So far, the cellular origin of glioblastoma (GBM) needs to be determined, with prevalent theories suggesting emergence from transformed endogenous stem cells. Adult neurogenesis primarily occurs in two brain regions: the subventricular zone (SVZ) and the subgranular zone (SGZ) of the hippocampal dentate
[...] Read more.
So far, the cellular origin of glioblastoma (GBM) needs to be determined, with prevalent theories suggesting emergence from transformed endogenous stem cells. Adult neurogenesis primarily occurs in two brain regions: the subventricular zone (SVZ) and the subgranular zone (SGZ) of the hippocampal dentate gyrus. Whether the proximity of GBM to these neurogenic niches affects patient outcome remains uncertain. Previous studies often rely on subjective assessments, limiting the reliability of those results. In this study, we assessed the impact of GBM’s relationship with the cortex, SVZ and SGZ on clinical variables using fully automated segmentation methods. In 177 glioblastoma patients, we calculated optimal cutpoints of minimal distances to the SVZ and SGZ to distinguish poor from favorable survival. The impact of tumor contact with neurogenic zones on clinical parameters, such as overall survival, multifocality, MGMT promotor methylation, Ki-67 and KPS score was also examined by multivariable regression analysis, chi-square test and Mann–Whitney-U. The analysis confirmed shorter survival in tumors contacting the SVZ with an optimal cutpoint of 14 mm distance to the SVZ, separating poor from more favorable survival. In contrast, tumor contact with the SGZ did not negatively affect survival. We did not find significant correlations with multifocality or MGMT promotor methylation in tumors contacting the SVZ, as previous studies discussed. These findings suggest that the spatial relationship between GBM and neurogenic niches needs to be assessed differently. Objective measurements disprove prior assumptions, warranting further research on this topic.
Full article
(This article belongs to the Section Cancer Survivorship and Quality of Life)
Open AccessArticle
Long-Term Results of Stereotactic Radiotherapy in Patients with at Least 10 Brain Metastases at Diagnosis
by
Rémy Kinj, Andreas Felix Hottinger, Till Tobias Böhlen, Mahmut Ozsahin, Véronique Vallet, Vincent Dunet, Hasna Bouchaab, Solange Peters, Constantin Tuleasca, Jean Bourhis and Luis Schiappacasse
Cancers 2024, 16(9), 1742; https://doi.org/10.3390/cancers16091742 - 29 Apr 2024
Abstract
Purpose: to evaluate an SRT approach in patients with at least 10 lesions at the time of BM initial diagnosis. Methods: This is a monocentric prospective cohort of patients treated by SRT, followed by a brain MRI every two months. Subsequent SRT could
[...] Read more.
Purpose: to evaluate an SRT approach in patients with at least 10 lesions at the time of BM initial diagnosis. Methods: This is a monocentric prospective cohort of patients treated by SRT, followed by a brain MRI every two months. Subsequent SRT could be delivered in cases of new BMs during follow-up. The main endpoints were local control rate (LCR), overall survival (OS), and strategy success rate (SSR). Acute and late toxicity were evaluated. Results: Seventy patients were included from October 2014 to January 2019, and the most frequent primary diagnosis was non-small-cell lung cancer (N = 36, 51.4%). A total of 1174 BMs were treated at first treatment, corresponding to a median number of 14 BMs per patient. Most of the patients (N = 51, 72.6%) received a single fraction of 20–24 Gy. At 1 year, OS was 62.3%, with a median OS of 19.2 months, and SSR was 77.8%. A cumulative number of 1537 BM were treated over time, corresponding to a median cumulative number of 16 BM per patient. At 1-year, the LCR was 97.3%, with a cumulative incidence of radio-necrosis of 2.1% per lesion. Three patients (4.3%) presented Grade 2 toxicity, and there was no Grade ≥ 3 toxicity. The number of treated BMs and the treatment volume did not influence OS or SSR (p > 0.05). Conclusions: SRT was highly efficient in controlling the BM, with minimal side effects. In this setting, an SRT treatment should be proposed even in patients with ≥10 BMs at diagnosis.
Full article
(This article belongs to the Special Issue Stereotactic Radiotherapy in Tumor Ablation (Volume II))

Journal Menu
► ▼ Journal Menu-
- Cancers Home
- Aims & Scope
- Editorial Board
- Reviewer Board
- Topical Advisory Panel
- Instructions for Authors
- Special Issues
- Topics
- Sections & Collections
- Article Processing Charge
- Indexing & Archiving
- Editor’s Choice Articles
- Most Cited & Viewed
- Journal Statistics
- Journal History
- Journal Awards
- Society Collaborations
- Conferences
- Editorial Office
Journal Browser
► ▼ Journal BrowserHighly Accessed Articles
Latest Books
E-Mail Alert
News
Topics
Topic in
Bioengineering, Biomolecules, Cancers, Diseases, Nanomaterials, Pharmaceutics
Dynamic Nano-Biomaterials in Tissue Regeneration and Cancer Therapies
Topic Editors: Ramar Thangam, Heemin Kang, Bibin G. Anand, Ramachandran Vijayan, Venugopal KrishnanDeadline: 15 May 2024
Topic in
Biomedicines, Cancers, JFB, Nanomaterials, Polymers
Advanced Functional Materials for Regenerative Medicine
Topic Editors: Antonino Morabito, Luca ValentiniDeadline: 6 June 2024
Topic in
Biology, Cancers, Current Oncology, Diseases, JCM, Pathogens
Pathogenetic, Diagnostic and Therapeutic Perspectives in Head and Neck Cancer
Topic Editors: Shun-Fa Yang, Ming-Hsien ChienDeadline: 20 June 2024
Topic in
Cancers, Cells, JCM, Radiation, Pharmaceutics, Applied Sciences, Nanomaterials, Current Oncology
Innovative Radiation Therapies
Topic Editors: Gérard Baldacchino, Eric Deutsch, Marie Dutreix, Sandrine Lacombe, Erika Porcel, Charlotte Robert, Emmanuelle Bourneuf, João Santos Sousa, Aurélien de la LandeDeadline: 30 June 2024

Conferences
Special Issues
Special Issue in
Cancers
Differential Scanning Calorimetry and Related Thermal Analysis Techniques as Complementary Approaches for Cancer Diagnosis, Prognosis, Monitoring and Assessment of Treatment Response
Guest Editor: Nichola C. GarbettDeadline: 1 May 2024
Special Issue in
Cancers
Molecular and Cellular Heterogeneity in an Evolving Tumor Landscape: When Diversity Gives Rise to Aggressive and Drug Resistant Cells
Guest Editor: Michelle R. DawsonDeadline: 20 May 2024
Special Issue in
Cancers
Innovations in Soft Tissue Sarcoma Diagnosis and Treatment
Guest Editors: Erlinda M. Gordon, Sant P. Chawla, Frederick L. HallDeadline: 30 May 2024
Special Issue in
Cancers
Perioperative Care and Pain Management in Cancer Patients: From Basic Science to Clinical Practice
Guest Editors: Dario Bugada, Juan P. CataDeadline: 20 June 2024
Topical Collections
Topical Collection in
Cancers
Drug Resistance and Novel Therapies in Cancers
Collection Editor: Zhixiang Wang