-
 Planetary Health Diet Adherence and Medication Use in Older Adults with Chronic Kidney Disease: A Cross-Sectional Study
Planetary Health Diet Adherence and Medication Use in Older Adults with Chronic Kidney Disease: A Cross-Sectional Study -
 Late-Onset Depression in an Aging World: A Multidimensional Perspective on Risks, Mechanisms, and Treatment
Late-Onset Depression in an Aging World: A Multidimensional Perspective on Risks, Mechanisms, and Treatment -
 Effect of Yoga Practices on Postural Stability, Fall Risk, and Psychological Wellbeing in Older Adults
Effect of Yoga Practices on Postural Stability, Fall Risk, and Psychological Wellbeing in Older Adults -
 Assessing Ageist Attitudes: Psychometric Properties of the Fraboni Scale of Ageism in a Population-Based Sample
Assessing Ageist Attitudes: Psychometric Properties of the Fraboni Scale of Ageism in a Population-Based Sample -
 Effects of a Community-Based Multi-Component Intervention on Subjective Well-Being in Older Adults: The Chofu–Digital–Choju Project in Japan
Effects of a Community-Based Multi-Component Intervention on Subjective Well-Being in Older Adults: The Chofu–Digital–Choju Project in Japan
Journal Description
Geriatrics
Geriatrics
is an international, peer-reviewed, scientific open access journal on geriatric medicine published bimonthly online by MDPI.
- Open Access— free for readers, with article processing charges (APC) paid by authors or their institutions.
- High Visibility: indexed within Scopus, ESCI (Web of Science), PubMed, PMC, and other databases.
- Journal Rank: CiteScore - Q2 (Health (Social Science))
- Rapid Publication: manuscripts are peer-reviewed and a first decision is provided to authors approximately 27.3 days after submission; acceptance to publication is undertaken in 3.7 days (median values for papers published in this journal in the second half of 2025).
- Recognition of Reviewers: reviewers who provide timely, thorough peer-review reports receive vouchers entitling them to a discount on the APC of their next publication in any MDPI journal, in appreciation of the work done.
- Testimonials: See what our editors and authors say about Geriatrics.
- Journal Cluster of Healthcare Sciences and Services: Geriatrics, Journal of Ageing and Longevity, Healthcare, Hospitals, Hygiene, International Journal of Environmental Research and Public Health and Nursing Reports.
Impact Factor:
2.1 (2024);
5-Year Impact Factor:
2.5 (2024)
Latest Articles
Patient-Centred Care for Older Patients Considering Surgery: An Evaluation of the Perioperative Care of Older Patients Service at an Australian Tertiary Hospital
Geriatrics 2026, 11(3), 55; https://doi.org/10.3390/geriatrics11030055 - 28 Apr 2026
Abstract
Background/Objectives: As mounting numbers of older people consider surgery, the importance of aligning treatments with patient values and goals is paramount. This has led to the growth of POPS (Perioperative care of Older Patients) services internationally and across Australia. An observational pilot
[...] Read more.
Background/Objectives: As mounting numbers of older people consider surgery, the importance of aligning treatments with patient values and goals is paramount. This has led to the growth of POPS (Perioperative care of Older Patients) services internationally and across Australia. An observational pilot evaluation of the Melbourne Health POPS service was conducted throughout 2022, with the aims of describing the population, measuring patient-reported outcomes and comparing postoperative outcomes to a matched historical cohort. Methods: Data were sourced from clinical review, electronic medical records and health intelligence. Patients who pursued surgery were matched 2:1 with a 2020 control cohort on up to 10 characteristics ranked on clinical judgement. Patient-reported outcomes were collected at 3 months post-surgery or at the clinic in consenting participants. Results: There were 128 participants, of whom 64 (50%) pursued non-surgical management. Participants were older (median 79 [13] years), frail (median CFS 5 [2]), and multimorbid (median CCI 5 [2.25]). Despite increased perioperative risk amongst the POPS surgical group (ASA-4 23.4% vs. 5.5%, p < 0.001), increased incidence of postoperative delirium (15% vs. 5.8%, p = 0.042) and ICU admission (21.7% vs. 7.5%, p = 0.006) compared to the control group, median length of stay was similar (4.3 [6.7] vs. 4.3 [5.1] days, p = 0.537). Patient-reported outcomes were similar between surgical and non-surgical POPS groups (90.7% vs. 88.1% would make the same surgical decision, p = 0.697). Conclusions: Patients attending POPS were multimorbid with geriatric syndromes and elevated perioperative risk. A high proportion pursued non-operative care. Patient-reported feedback was high with low decisional regret.
Full article
(This article belongs to the Special Issue Comprehensive Geriatric Assessment of Older Surgical Patients)
►
Show Figures
Open AccessReview
Day Surgery in Older Adults: Safety, Effectiveness, and Best Practices for Patient Selection and Perioperative Care—A Narrative Review
by
Judit Groman, Zsolt Viktor Göböl, Andrea Virág, Gyula Domján and Klara Gadó
Geriatrics 2026, 11(3), 54; https://doi.org/10.3390/geriatrics11030054 - 28 Apr 2026
Abstract
►▼
Show Figures
Background: The growing number of older adults undergoing surgical procedures requires care models that minimise hospital exposure, optimise safety, and support rapid recovery. Day surgery has become an increasingly attractive option for selected older patients, provided their medical, functional and psychosocial needs are
[...] Read more.
Background: The growing number of older adults undergoing surgical procedures requires care models that minimise hospital exposure, optimise safety, and support rapid recovery. Day surgery has become an increasingly attractive option for selected older patients, provided their medical, functional and psychosocial needs are carefully assessed. Recent developments in prehabilitation, geriatric-focused perioperative pathways and enhanced post-discharge follow-up have further expanded its potential. This narrative review aims not only to synthesise current evidence, but also to provide a clinically oriented framework for patient selection, perioperative optimisation, and safe implementation of day surgery pathways in older adults. Main findings: Evidence from the past decade indicates that day surgery can be safe and effective for adults aged ≥65 when supported by structured preoperative assessment, targeted optimisation, and clear discharge criteria. Older patients benefit particularly from reduced risks of hospital-acquired complications, including infection, delirium, immobility and functional decline. Prehabilitation programmes focusing on nutrition, strength, balance and medication review are associated with improved postoperative stability and faster return to baseline function. Multidisciplinary teamwork, integrating surgeons, anaesthetists, geriatricians, nurses, physiotherapists, dietitians and caregivers, play a key role in identifying modifiable risks and ensuring continuity of care. Studies also highlight the value of post-discharge telephone follow-up, caregiver engagement and close collaboration with primary care in preventing readmissions. Conclusions: Day surgery is a viable and patient-centred option for many older adults when careful selection and preparation are combined with age-sensitive perioperative care. Most adverse outcomes can be mitigated through systematic prehabilitation, thoughtful anaesthetic planning, early mobilisation and structured follow-up. The evidence suggests that older patients may benefit from reduced hospital stay, less exposure to harm, and faster functional recovery. Implications for practice: The findings support broader integration of geriatric day surgery into routine care pathways, especially within health systems facing capacity constraints. Clinicians should consider implementing standardised geriatric assessment, multidisciplinary optimisation strategies, and robust discharge and follow-up protocols to enhance safety and effectiveness. With appropriate preparation and coordinated teamwork, day surgery can contribute meaningfully to safer, more efficient and more patient-centred surgical care for older adults.
Full article

Graphical abstract
Open AccessArticle
Effects of Dual Tasking on Intersegmental Coordination During Walking in People with Parkinson’s Disease: A Cross-Sectional Case–Control Study
by
Valéria Feijó Martins, Edilson Fernando de Borba, Lucas de Liz Alves, Leonardo A. Peyré-Tartaruga and Flávia Gomes Martinez
Geriatrics 2026, 11(3), 53; https://doi.org/10.3390/geriatrics11030053 - 28 Apr 2026
Abstract
Background: In dual-task (DT) conditions, individuals must walk while simultaneously engaging in cognitive or motor tasks, which impacts gait performance, especially in older adults and individuals with Parkinson’s disease (PD). Gait impairments in PD under DT conditions have implications for intersegmental coordination. Research
[...] Read more.
Background: In dual-task (DT) conditions, individuals must walk while simultaneously engaging in cognitive or motor tasks, which impacts gait performance, especially in older adults and individuals with Parkinson’s disease (PD). Gait impairments in PD under DT conditions have implications for intersegmental coordination. Research question: Intersegmental coordination and gait biomechanics during the DTs were compared between people with PD and older adults. Methods: Thirty-two individuals (16 PD, H&Y 1–3; and 16 older adults) participated in this study and were asked to walk under the following self-selected conditions: single task, DT with a math component, and texting on a cell phone. Spatiotemporal, angular, and intersegmental coordination data were collected using a markerless motion analysis system (OpenCap). Results: Dual-task conditions significantly affected spatiotemporal and kinematic variables, as well as intersegmental coordination. A significant task effect was observed for thigh–shank coordination, whereas no significant group effect was found for the main coordination outcomes. Significance: Significant task effects were observed for intersegmental coordination (thigh–shank CRP), with no significant group differences. The concurrent demands of processing visual and motor information for texting and walking lead to significant reductions in gait speed and lower limb movement, as well as altered intersegmental coordination, with task demands rather than disease status being the primary driver of coordination changes.
Full article
(This article belongs to the Topic AI-Driven Smart Elderly Care: Innovations and Solutions)
►▼
Show Figures

Figure 1
Open AccessArticle
Two Months of Active Video Game Training Improves Selected Lipid Profile Markers in Older Adults: A Preliminary Study
by
Agali Y. López-Miguel, Ángel E. Brizuela-Araujo, Omar A. López-López, Juan J. Calleja-Núñez, Roberto Espinoza-Gutiérrez, Elena C. Guzmán-Gutiérrez, Aracely Serrano-Medina, José Moncada-Jiménez and Jorge A. Aburto-Corona
Geriatrics 2026, 11(3), 52; https://doi.org/10.3390/geriatrics11030052 - 23 Apr 2026
Abstract
Background: The purpose of this study was to compare the effects of two months of exergaming, conventional resistance exercise training, and no exercise on body composition and cardiometabolic risk factors in physically inactive older adults. Methods: For the preliminary study, twenty-four
[...] Read more.
Background: The purpose of this study was to compare the effects of two months of exergaming, conventional resistance exercise training, and no exercise on body composition and cardiometabolic risk factors in physically inactive older adults. Methods: For the preliminary study, twenty-four physically inactive adults aged 60–74 yrs. were allocated to an active video game training group (AVG n = 8), a conventional exercise group (CEG n = 7), or a non-exercising control group (CON n = 9). The AVG and CEG completed 24 supervised exercise training sessions over two months (three sessions per week) at self-selected, predominantly moderate-to-vigorous intensity, while the CON maintained usual daily activities. Body weight, skeletal muscle mass, body fat percentage, phase angle, and fasting blood biomarkers (glucose, total cholesterol, LDL, HDL, VLDL, and triglycerides) were assessed before and after the intervention. Results: No significant interactions were observed for body composition variables. Body weight decreased significantly following exercise training in both the AVG and CEG (p < 0.05). Significant interactions were found for total cholesterol (p = 0.001) and LDL cholesterol (p = 0.009). The AVG demonstrated significant reductions in fasting glucose, total cholesterol, and LDL cholesterol (p < 0.05), whereas the CEG showed a significant reduction only in total cholesterol. In contrast, the CON exhibited a significant increase in total cholesterol over the same period (p < 0.05). Conclusions: Two months of exergaming-based exercise training may lead to greater improvements in lipid-related cardiometabolic risk factors compared with conventional resistance exercise training in physically inactive older adults. These findings suggest that exergaming could be a promising exercise modality for supporting cardiometabolic health in aging populations.
Full article
(This article belongs to the Topic Exercise and Human Aging: Physiological and Psychological Functions)
Open AccessArticle
Sarcopenia Severity and the Accumulation of Geriatric Syndromes Among Older Adults: A Cross-Sectional Study from Vietnam
by
Huong Thi Thu Nguyen, Vasi Naganathan, Thanh Xuan Nguyen, Tam Ngoc Nguyen, Thu Thi Hoai Nguyen, Huyen Thi Thanh Vu, Anh Lan Nguyen, Vien Chi Le, Narelle Warren, Hoa Lan Nguyen, Robert J. Goldberg and Anh Trung Nguyen
Geriatrics 2026, 11(3), 51; https://doi.org/10.3390/geriatrics11030051 - 23 Apr 2026
Abstract
►▼
Show Figures
Background/Objectives: Sarcopenia frequently coexists with other geriatric syndromes, and its severity may influence their clinical manifestation. This study examines the prevalence of geriatric syndromes in older adults with non-severe and severe sarcopenia and explores the associations between sarcopenia severity and individual geriatric syndromes
[...] Read more.
Background/Objectives: Sarcopenia frequently coexists with other geriatric syndromes, and its severity may influence their clinical manifestation. This study examines the prevalence of geriatric syndromes in older adults with non-severe and severe sarcopenia and explores the associations between sarcopenia severity and individual geriatric syndromes in Vietnam. Methods: A cross-sectional study was conducted among 726 older outpatients with sarcopenia. Non-severe and severe sarcopenia were diagnosed according to the Asian Working Group for Sarcopenia algorithm. Fifteen geriatric conditions spanning physical and psychological health, functional status, and social circumstances were assessed using components of the Comprehensive Geriatric Assessment. Logistic regression models were used to examine associations between sarcopenia severity and geriatric syndromes. Results: A total of 726 older patients with sarcopenia (mean age 74.4 years, 77.4% females) were included, of whom 53.4% had severe sarcopenia. A significantly higher prevalence of geriatric syndromes was observed in patients with severe compared with non-severe sarcopenia, including sleep disturbances (79.4% vs. 67.5%), frailty (71.4% vs. 54.7%), malnourishment/risk of malnutrition (61.9% vs. 50.0%), depression (54.9% vs. 34.9%), polypharmacy (49.5% vs. 42.0%), impairment in activities of daily living (52.8% vs. 32.5%), and impairment in instrumental activities of daily living (58.2% vs. 39.3%). After adjustment for potential confounders, severe sarcopenia remained associated with sleep disturbance (adjusted OR 1.49, 95%CI 1.02–2.18, p = 0.046), depression (adjusted OR 1.90, 95%CI 1.36–2.66, p < 0.001), and mobility impairment (adjusted OR 3.01, 95%CI 2.12–4.27, p < 0.001). Conclusions: Older Vietnamese adults with sarcopenia had a high burden of geriatric syndromes, particularly among those with severe disease. Severe sarcopenia was independently associated with sleep disturbance, depression, and impaired mobility—clinically relevant and potentially modifiable conditions. These findings highlight the importance of evaluating sarcopenia within a broader geriatric framework and may inform early identification and prioritization of coexisting geriatric syndromes, especially in resource-limited settings.
Full article

Figure 1
Open AccessArticle
Appropriateness and Outcome of a Statin Deprescription Intervention in Hospitalized Frail Older Adults: A Retrospective Study
by
Giuseppe Castiglia, Nicola Veronese, Gianluca Gortan Cappellari, Erica Voinovich, Paolo De Colle and Michela Zanetti
Geriatrics 2026, 11(2), 50; https://doi.org/10.3390/geriatrics11020050 - 20 Apr 2026
Abstract
Background/Objectives: The appropriateness of statin treatment in frail older adults is controversial because of insufficient evidence on its efficacy. The aim of this study was to assess the appropriateness of statin prescription at admission and discharge from hospital and the association of
[...] Read more.
Background/Objectives: The appropriateness of statin treatment in frail older adults is controversial because of insufficient evidence on its efficacy. The aim of this study was to assess the appropriateness of statin prescription at admission and discharge from hospital and the association of deprescription with one-year mortality in a cohort of older patients. Methods: Monocentric retrospective observational study of older (≥65 year) adults admitted to a Geriatric Unit. Patients underwent comprehensive geriatric assessment and prevalence of statin prescription at admission and discharge was recorded. Appropriateness of prescription was determined using the Medication Appropriateness Index (MAI), multidimensional frailty using the Multidimensional Prognostic Index (MPI). Mortality at 12 months was recorded. Results: Among 528 consecutively admitted patients, 112 (mean age 83.6 ± 6.2 years) were treated with statins and were included in the study. In addition, 87.5% of patients showed at least one inappropriate criterion for statin prescription at admission and 91.7% at discharge. Deprescription occurred in 46.4% of patients at discharge, particularly in those who were older and in MPI high mortality risk class. Mean MAI did not differ between admission and discharge in the whole study cohort, but it decreased in patients at highest mortality risk (from 3.2 ± 4.0 to 2.0 ± 1.2). In multivariate analysis, compared with patients who continued statins after discharge, those who were deprescribed did not show increased one-year mortality risk. Conclusions: Inappropriate statin prescription is common at hospital admission in frail older patients and deprescription does not affect one-year residual survival. Therefore, rigorous assessment of mortality risk and medication appropriateness should be encouraged.
Full article
(This article belongs to the Section Cardiogeriatrics)
►▼
Show Figures

Figure 1
Open AccessArticle
Screening for Pre-Frailty Using Phase Angle Derived from Bioelectrical Impedance Analysis in Community-Dwelling Older Adults
by
Masayuki Hoshi, Tomoka Ogata, Maaya Chiguchi, Ayane Nakamaru, Tatsuya Nakanowatari, Akihiko Asao, Natsumi Kimura, Maki Ogasawara, Yuko Horikoshi, Rie Sakuraba-Hirata, Akiomi Yoshihisa, Hiroshi Hayashi, Toshimasa Sone and Yoshitaka Shiba
Geriatrics 2026, 11(2), 49; https://doi.org/10.3390/geriatrics11020049 - 20 Apr 2026
Abstract
►▼
Show Figures
Background/Objectives: To evaluate the utility of phase angle (PhA) derived from bioelectrical impedance analysis as a screening indicator for pre-frailty in community-dwelling older adults. Methods: This cross-sectional study included 171 participants (36 men and 135 women) in Japan in 2023. PhA at 50
[...] Read more.
Background/Objectives: To evaluate the utility of phase angle (PhA) derived from bioelectrical impedance analysis as a screening indicator for pre-frailty in community-dwelling older adults. Methods: This cross-sectional study included 171 participants (36 men and 135 women) in Japan in 2023. PhA at 50 kHz was measured using bioelectrical impedance analysis and evaluated as a potential screening indicator for pre-frailty. Assessments included body composition, physical function tests (maximum walking speed, Timed Up and Go (TUG), grip strength, knee extension strength, and one-leg stance time with eyes open), cognitive function (MoCA-J), and the Motor Fitness Scale (MFS), a questionnaire assessing physical function, along with the Kihon Checklist (KCL). Frailty status was defined using KCL scores (4–7: pre-frailty; ≥8: frailty), and participants were classified into robust and pre-frail/frail groups. Results: PhA was significantly correlated with physical function measures, including grip strength (r = 0.54, p < 0.01), MFS (r = 0.36, p < 0.01), maximum walking speed (r = 0.20, p < 0.05), knee extension strength (r = 0.16, p < 0.05), and TUG (r = −0.17, p < 0.05). In women, logistic regression analysis showed that PhA was independently associated with pre-frailty (age-adjusted odds ratio: 2.38; 95% CI: 1.08–5.23; p < 0.05). ROC analysis yielded an area under the curve of 0.65 (95% CI: 0.56–0.74), indicating modest discriminative ability. Age-adjusted cutoff values of PhA were 4.19° and 4.74°, corresponding to points prioritizing sensitivity and specificity, respectively. Conclusions: PhA is associated with physical function and may serve as a simple, non-invasive indicator for identifying pre-frailty in community settings. However, given its modest discriminative ability, PhA alone may not be sufficient as a standalone screening tool and should be used in combination with other clinical indicators for clinical application.
Full article

Figure 1
Open AccessArticle
Effects of Intraoperative Prone Versus Supine Positioning on Postoperative Delirium
by
Theresa E. Hering, Maria Wittmann, Vera Guttenthaler, Robert Pflugmacher and Rudolf Hering
Geriatrics 2026, 11(2), 48; https://doi.org/10.3390/geriatrics11020048 - 19 Apr 2026
Abstract
►▼
Show Figures
Background: Postoperative delirium (POD) is a common complication in geriatric patients. This prospective cohort study evaluated a possible influence of intraoperative positioning on the occurrence of POD, as intraoperative prone positioning could affect cerebral perfusion. Methods: We included 760 patients of ≥60
[...] Read more.
Background: Postoperative delirium (POD) is a common complication in geriatric patients. This prospective cohort study evaluated a possible influence of intraoperative positioning on the occurrence of POD, as intraoperative prone positioning could affect cerebral perfusion. Methods: We included 760 patients of ≥60 years scheduled for elective surgery in prone or supine positions. The primary outcome was POD incidence on the first five days after surgery, assessed via 3D-Confusion Assessment Method (3-D CAM) or Confusion Assessment Method for Intensive Care Units (CAM-ICU). Preoperative assessments included the American Society of Anesthesiologists (ASA) and New York Heart Association (NYHA) classifications as well as short screenings for the cognitive (modified Montreal Cognitive Assessment (MoCA)) and self-care status of the patient. Secondary outcomes were length of hospital stay (LOS) and mortality rates. Results: Postoperative delirium rates were similar in prone and supine patients (7.6% vs. 5.5%; p = 0.31), and logistic regression analysis revealed no association of intraoperative prone positioning with POD (odds ratio 1.42 (95% CI 0.68–2.92; p = 0.342)). The overall incidence of POD was 6.1% and was associated with older age (81.5 (CI 76.2–84.8) vs. 72.0 (CI 67.0–79.0) years; p < 0.01), higher ASA and NHYA classifications, lower preoperative modified MoCA, reduced independence in self-care (p < 0.001, respectively), and longer incision-to-suture times (107.0 (CI 73.0–173.0) vs. 85.0 (CI 60.0–130.0) minutes; p < 0.01). Postoperative delirium resulted in longer LOS (14.5 (CI 9.0–27.0) vs. 7.0 (CI 4.0–9.0) days; p < 0.001), and increased mortality (13.0% vs. 1.7%; p < 0.001). Conclusions: Intraoperative prone positioning was not associated with POD in patients aged 60 years or older (OR 1.42; CI 0.68–2.92; p < 0.340), and LOS and mortality as secondary outcome parameters were also similar in patients after prone and supine surgery. Future studies assessing additional and possible confounding factors and intraoperative systemic and regional hemodynamics and oxygenation are needed to verify this result and to evaluate cerebral hypoperfusion as a possible mechanism of POD.
Full article

Graphical abstract
Open AccessReview
Constipation in Older Adults: Pathophysiology, Clinical Impact, and Management Strategies
by
Shima Mimura, Asahiro Morishita, Atsuo Kitaoka, Kota Sasaki, Hiroki Tai, Rie Yano, Mai Nakahara, Kyoko Oura, Tomoko Tadokoro, Koji Fujita, Joji Tani, Takashi Himoto and Hideki Kobara
Geriatrics 2026, 11(2), 47; https://doi.org/10.3390/geriatrics11020047 - 16 Apr 2026
Abstract
►▼
Show Figures
Background/Objectives: Constipation is a common gastrointestinal problem in older adults and is associated with reduced quality of life, functional decline, frailty, and an increased risk of delirium and cognitive impairment. Its pathogenesis is multifactorial, involving age-related changes in gastrointestinal motility, neural regulation, comorbidities,
[...] Read more.
Background/Objectives: Constipation is a common gastrointestinal problem in older adults and is associated with reduced quality of life, functional decline, frailty, and an increased risk of delirium and cognitive impairment. Its pathogenesis is multifactorial, involving age-related changes in gastrointestinal motility, neural regulation, comorbidities, and polypharmacy. However, this condition has traditionally been regarded as a localized gastrointestinal disorder, which may not fully reflect its systemic clinical significance in older populations. While prior narrative reviews have described multifactorial contributors to constipation, none have formally applied a geriatric syndrome framework to integrate these dimensions. This review proposes a three-criterion operational definition—multifactorial pathogenesis, association with functional decline and frailty, and contribution to adverse systemic outcomes—to characterize constipation in older adults as a “systemic geriatric syndrome,” and evaluates available evidence against each criterion. Methods: A narrative literature search was conducted using PubMed to identify relevant studies published between 1 January 2023, and 31 December 2025. MeSH terms included “Constipation” [Major Topic] and “Aged” [MeSH Terms]. Eligible articles included English-language original studies, systematic reviews, and clinical or epidemiological studies involving individuals aged ≥65 years. Results: Diagnosis in older adults is often complicated by secondary causes, including medications and neurological disorders, as well as atypical symptom presentations in individuals with cognitive impairment. Key pathophysiological mechanisms include reductions in interstitial cells of Cajal, impaired smooth muscle contractility, dysfunction of the enteric and autonomic nervous systems, and gut microbiota dysbiosis, which may promote chronic low-grade inflammation. Major contributing factors include physical inactivity, sarcopenia, dehydration, inappropriate defecation posture, and polypharmacy, particularly opioids and anticholinergic agents. Importantly, these factors interact through the brain–gut–microbiota axis, contributing not only to gastrointestinal dysfunction but also to systemic outcomes such as frailty, cognitive decline, and increased healthcare burden, thereby supporting a multidimensional disease framework. Conclusions: The available evidence collectively supports the plausibility of framing constipation in older adults as a systemic geriatric syndrome, though formal validation of this classification requires further longitudinal and mechanistic research. Comprehensive and individualized management strategies, extending beyond simple laxative use, are essential to reduce complications and preserve functional health in aging populations. Further studies are required to validate this framework.
Full article

Figure 1
Open AccessArticle
Clinical Utility of Gait Speed Indices for Identifying Sarcopenia in Older Adults with Type 2 Diabetes
by
Kensaku Kashima, Rie Nishimura, Hisashi Sugano and Shimpei Fujimoto
Geriatrics 2026, 11(2), 46; https://doi.org/10.3390/geriatrics11020046 - 14 Apr 2026
Abstract
►▼
Show Figures
Background/Objectives: This study aimed to compare the diagnostic performance of usual gait speed (UGS), maximal gait speed (MGS), and gait speed reserve (GSR) for identifying sarcopenia in older adults with type 2 diabetes (T2D), and to examine whether combining gait indices improves
[...] Read more.
Background/Objectives: This study aimed to compare the diagnostic performance of usual gait speed (UGS), maximal gait speed (MGS), and gait speed reserve (GSR) for identifying sarcopenia in older adults with type 2 diabetes (T2D), and to examine whether combining gait indices improves diagnostic performance. Methods: This cross-sectional study included 117 older adults with T2D hospitalized for glycemic control. UGS and MGS were measured in the central 10-m section of a 16-m course, which included 3-m acceleration and deceleration zones on either side. GSR was calculated as the difference between MGS and UGS. Sarcopenia was diagnosed according to the AWGS 2025 criteria. Multivariable logistic regression was used to examine the associations between each gait index and sarcopenia. Diagnostic performance was evaluated using receiver operating characteristic (ROC) curve analysis, and the usefulness of a combined criterion based on UGS and GSR was also assessed. Results: Sarcopenia was identified in 32 participants (27.4%). UGS, MGS, and GSR were each associated with sarcopenia independently of clinical factors. UGS showed the highest sensitivity (90.6%), suggesting its potential usefulness as a screening measure, whereas GSR showed the highest specificity (83.5%), suggesting its potential usefulness in reducing false positives when identifying sarcopenia. In the ROC analysis of the three gait-related indices, the area under the curve (AUC) for MGS was the highest (0.79), but it was not significantly different from the AUC for UGS. The combined criterion of UGS < 1.07 m/s and GSR < 0.21 m/s improved specificity and yielded a high positive likelihood ratio (PLR = 6.5). Conclusions: UGS, MGS, and GSR each exhibit distinct diagnostic characteristics for sarcopenia. UGS may be useful for screening, whereas GSR may help improve specificity. In particular, combining UGS and GSR may provide complementary diagnostic information for identifying sarcopenia in older adults with T2D.
Full article

Graphical abstract
Open AccessReview
Cognitive Testing in Spanish Older Adults: A Scoping Review
by
Lucía Sáez-González, Luis A. Martínez, Gema Blázquez-Abellán, José Antonio Carbajal de Lara, Rosa M. Martinez-Garcia and Lucía Castro-Vázquez
Geriatrics 2026, 11(2), 45; https://doi.org/10.3390/geriatrics11020045 - 10 Apr 2026
Abstract
Background/Objectives: Cognitive impairment is a major concern in aging populations. Early detection through validated neuropsychological tests is essential for dementia risk stratification and preventive interventions. This scoping review (PRISMA-ScR, 2013–2023, registration protocol: 10.17605/OSF.IO/8NHJF) evaluated cognitive testing trends in aging research and identified the
[...] Read more.
Background/Objectives: Cognitive impairment is a major concern in aging populations. Early detection through validated neuropsychological tests is essential for dementia risk stratification and preventive interventions. This scoping review (PRISMA-ScR, 2013–2023, registration protocol: 10.17605/OSF.IO/8NHJF) evaluated cognitive testing trends in aging research and identified the most frequently used neuropsychological screening tests in Spanish populations. Methods: Searches in PubMed and Web of Science (March 2024) yielded 730 records; 156 were reviewed in full, and 15 met inclusion criteria for Spanish adults ≥65 years. Results: The Mini-Mental State Examination was the most-used test, followed by verbal fluency and Trail Making Test. No test covered all six DSM-5 cognitive domains, and social cognition was never assessed in any of the studies. The Montreal Cognitive Assessment was underused despite its superior sensitivity. Conclusions: Findings support developing a tailored, multidomain battery combining global and domain-specific tests. Social cognition assessments should be included to ensure a complete cognitive domain coverage.
Full article
(This article belongs to the Special Issue Current Issues in Cognitive Testing of Older Adults)
►▼
Show Figures

Graphical abstract
Open AccessArticle
Comparison of Physical Performance and Muscle Thickness Between Older Women with High and Low Fall Risk: A Bayesian Approach
by
Claudineia Matos de Araujo, Rafael Pereira, Joanderson Felipe Soares Silva, Cláudia Thais Pereira Pinto, Alinne Alves Oliveira, Luciano Magno de Almeida Faria, Ludmila Schettino, Mikhail Santos Cerqueira and Marcos Henrique Fernandes
Geriatrics 2026, 11(2), 44; https://doi.org/10.3390/geriatrics11020044 - 10 Apr 2026
Abstract
►▼
Show Figures
Objective: The present study aimed to compare muscle thickness and physical performance in different functional tests predicting falls between older adults with low and high fall risk. Methods: Seventy-one community-dwelling older women (74.5 ± 8.5 years old) volunteered for this study. The Berg
[...] Read more.
Objective: The present study aimed to compare muscle thickness and physical performance in different functional tests predicting falls between older adults with low and high fall risk. Methods: Seventy-one community-dwelling older women (74.5 ± 8.5 years old) volunteered for this study. The Berg Balance Scale (BBS) was used to stratify the sample as low and high risk for fall (BBS cutoff = ≥ 50 points). The performance in the Timed Up and Go Test (TUGT), 5-repetition sit-to-stand test (5xSST), 3 m walk test (3mWT), and 3 m backward walk test (3mBWT) was assessed. The elbow flexor and knee extensor muscle thickness were obtained by ultrasound (USD). A linear mixed model analysis was used to determine between-group differences in functional mobility and muscle thickness, and Bayesian analysis was applied to check the probability to replicate the same results (i.e., the magnitude of the evidence). Results: The low-fall-risk group exhibited significantly better performance only in 3mWT (mean difference = 0.84 s [95% CI: 0.40 to 1.29 s]; p = 0.001) and 3mBWT (mean difference = 1.54 s [95% CI: 0.21 to 2.85 s]; p = 0.024). The Bayes Factor (BF) for performance on the 3mWT and 3mBWT shows that the low-fall-risk group has a probability of 98.7% (BF10 = 77.3) and 99.7% (BF10 = 368), respectively, of performing better than the high-fall-risk group. Conclusions: Based on inferential and Bayesian analysis, the performance in 3mWT and that in 3mBWT were classified as very strong to excellent instruments, respectively, for differentiating older women with high fall risk.
Full article

Figure 1
Open AccessArticle
Exploring the Interplay Between Core Stability, Pulmonary Function, and Cardiorespiratory Fitness in Older Adults: A Randomized Controlled Trial of an 8-Week Mat Pilates Intervention
by
Bulin Jirapongsatorn, Decha Chinaksorn, Kanapot Pengked, Wannaporn Tongtako and Timothy Mickleborough
Geriatrics 2026, 11(2), 43; https://doi.org/10.3390/geriatrics11020043 - 9 Apr 2026
Abstract
Background: Identifying multimodal interventions to counteract age-related physiological decline is a critical public health priority. This study investigated the impact of an 8-week Mat Pilates intervention (MPT) on the interplay between core stability, pulmonary function, and cardiorespiratory fitness in older adults, specifically examining
[...] Read more.
Background: Identifying multimodal interventions to counteract age-related physiological decline is a critical public health priority. This study investigated the impact of an 8-week Mat Pilates intervention (MPT) on the interplay between core stability, pulmonary function, and cardiorespiratory fitness in older adults, specifically examining the mechanistic link between trunk stabilization and respiratory mechanics. Methods: Twenty older adults (18 females, 2 males; age 60—77 years) were randomized (stratified by sex, age, and baseline stability) into an MPT group (n = 10; 60-min sessions, 3×/week) or a control group (CON, n = 10). Primary outcomes included core stability (plank test), functional flexibility (sit-and-reach; back-scratch), pulmonary function (FVC, FEV1, FEV1/FVC, FEF25–75%, MVV), and cardiorespiratory fitness (6-min walk test; 6MWT). Results: Post-intervention, the MPT group demonstrated significant improvements in core stability, flexibility, and all pulmonary variables (FVC, FEV1, FEF25–75%, MVV) compared to the CON group (p < 0.001). A significant reduction in body weight was also observed (p < 0.001). Notably, MPT participants achieved superior 6MWT distances and reduced perceived exertion (p = 0.006). Correlation analysis revealed strong positive associations between core stability gains and pulmonary function (r = 0.892, p < 0.01), supporting the mechanistic link between trunk stabilization, enhanced ventilatory mechanics, and functional aerobic capacity. Conclusions: Mat Pilates is a potent intervention for older adults, facilitating a physiological synergy where core strengthening optimizes pulmonary function and cardiorespiratory endurance. These findings suggest MPT is a comprehensive modality for maintaining musculoskeletal and respiratory health, proving superior to habitual activity alone in promoting functional independence.
Full article
(This article belongs to the Special Issue Exercise Interventions for Healthy Aging)
►▼
Show Figures

Figure 1
Open AccessArticle
Impact of Inflammation and Muscle Mass on Prognosis in Hospitalized Patients with Suspected Dysphagia at a Tertiary Hospital
by
Mario Alfredo Saavedra-Vásquez, Juan José López-Gómez, Beatriz Ramos-Bachiller, Olatz Izaola-Jauregui, Eva López-Andrés, Isabel Pérez-Mellén, Sara Cuenca-Becerril, María Jesús Villameriel-Galván, Jaime González-Gutiérrez, Lucia Estevez-Asensio, María Ángeles Castro-Lozano and Daniel Antonio De Luis-Román
Geriatrics 2026, 11(2), 42; https://doi.org/10.3390/geriatrics11020042 - 9 Apr 2026
Abstract
Background/Objectives: Dysphagia is associated with an increased risk of in-hospital complications and adverse outcomes. Prognosis in frail hospitalized populations is influenced by systemic inflammation and reduced muscle mass. Calf circumference (CC) and an estimated appendicular skeletal muscle index (ASMI) can serve as
[...] Read more.
Background/Objectives: Dysphagia is associated with an increased risk of in-hospital complications and adverse outcomes. Prognosis in frail hospitalized populations is influenced by systemic inflammation and reduced muscle mass. Calf circumference (CC) and an estimated appendicular skeletal muscle index (ASMI) can serve as indirect measures of muscle mass, while inflammatory status may be captured by C-reactive protein (CRP), albumin, and the CRP/albumin ratio. This study aimed to evaluate the prognostic value of indirect biomarkers of inflammation and muscle mass to predict prognosis in hospitalized patients with suspected dysphagia. Methods: A retrospective observational study was conducted at a tertiary hospital and included patients admitted with suspected dysphagia between April 2015 and October 2024. On admission, demographic variables (sex and age), anthropometry (weight, height, and CC), EAT-10 (Eating Assessment Tool) score, and serum laboratory parameters (CRP, albumin) were collected. ASMI was estimated using the formula −10.427 + (CC × 0.768) − (age × 0.029) + (sex × 7.523)/(height2). Outcomes were in-hospital mortality and length of hospital stay. Comparisons were performed between survivors and non-survivors, and multivariable models adjusted for age and sex were used to identify independent associations with mortality. Results: A total of 4241 patients were included (51.2% women), with a median age of 85 (Interquartile range [IQR] 14) years and a mean EAT-10 score of 15.98 (SD 7.79). In-hospital mortality was 18.13% (n = 769). Non-survivors were older (86 [IQR 11] vs. 84 [IQR 14] years; p < 0.001) and displayed a more inflammatory profile, with higher CRP (78.1 [IQR 114.28] vs. 44 [IQR 96] mg/L) and CRP/albumin ratio (27.27 [IQR 43.04] vs. 13.64 [IQR 31.77]; p < 0.001), and lower albumin (3 [IQR 0.8] vs. 3.3 [IQR 0.8] g/dL; p < 0.001). They also had lower muscle mass, with reduced CC and lower ASMI in both sexes. In multivariable analysis, a higher CRP/albumin ratio was independently associated with increased odds of death (OR 1.011; 95% CI 1.008–1.014; p < 0.001), whereas a higher ASMI was protective (OR 0.885; 95% CI 0.801–0.978; p = 0.017). Higher CRP/albumin ratios were also associated with longer hospital stays and lower albumin, CC, and ASMI values. Conclusions: In hospitalized patients with suspected dysphagia, systemic inflammation and lower muscle mass were associated with worse clinical outcomes. The CRP/albumin ratio independently predicted higher in-hospital mortality and prolonged hospitalization, whereas higher estimated ASMI was associated with lower mortality risk, supporting the combined prognostic value of inflammatory and muscle-mass indicators in this population.
Full article
(This article belongs to the Section Dysphagia)
►▼
Show Figures

Graphical abstract
Open AccessArticle
Association Between the Color Kanji Pick-Out Test App Performance and Cognitive Frailty as a Potential Early Screening Marker for Cognitive Decline
by
Akio Goda, Hideki Nakano, Yuki Kikuchi, Tsuyoshi Katsurasako, Kohei Mori, Atsuko Kubo, Kayoko Nonaka, Kohei Iwamoto, Nozomi Mitsumaru, Takaki Shimura and Shin Murata
Geriatrics 2026, 11(2), 41; https://doi.org/10.3390/geriatrics11020041 - 9 Apr 2026
Abstract
Background/Objective: Cognitive frailty, the coexistence of physical frailty and cognitive impairment, is a potentially reversible and high-risk state for dementia. This study examined the association between Color Kanji Pick-out Test (CKPT) app performance and cognitive frailty independent of Mini-Mental State Examination (MMSE)
[...] Read more.
Background/Objective: Cognitive frailty, the coexistence of physical frailty and cognitive impairment, is a potentially reversible and high-risk state for dementia. This study examined the association between Color Kanji Pick-out Test (CKPT) app performance and cognitive frailty independent of Mini-Mental State Examination (MMSE) scores in community-dwelling older women. Methods: In this cross-sectional study, the participants were 102 community-dwelling older women without dementia and with MMSE scores ≥ 27 (73.6 ± 6.0 years). Reversible cognitive frailty was defined as subjective cognitive decline (≥1 point in the cognitive domain of the Kihon Checklist) plus physical frailty or prefrailty, according to the Japanese Cardiovascular Health Study (J-CHS) criteria. Firth’s penalized logistic regression using three prespecified models, adjusted for age and education, was used to examine the independent associations between CKPT app performance and MMSE scores with reversible cognitive frailty. Results: Fourteen participants (13.7%) met the criteria for cognitive frailty. In separate models, higher CKPT app and MMSE scores were significantly associated with lower odds of cognitive frailty (CKPT: odds ratio [OR] 0.470, p = 0.019; MMSE: OR 0.548, p = 0.020). In a multivariable model including both measures, the CKPT app (OR 0.499, p = 0.031) and MMSE scores (OR 0.553, p = 0.031) remained independently associated with cognitive frailty, and this model had the lowest Akaike information criterion. Conclusions: The CKPT app performance was independently associated with cognitive frailty beyond global cognition. The CKPT app may detect subtle executive and attentional vulnerabilities not captured by the MMSE, supporting practical, objective, early screening and risk stratification of cognitive frailty.
Full article
(This article belongs to the Section Geriatric Psychiatry and Psychology)
►▼
Show Figures

Figure 1
Open AccessReview
Personalized Hemodialysis Approaches in Frail Older Individuals
by
Guido Gembillo, Luca Soraci, Matteo Floris, Lorenzo Lo Cicero, Claudia Lo Re, Elvira Filicetti, Michela Calderone, Carmelo Giorgio Benenati, Andrea Corsonello and Domenico Santoro
Geriatrics 2026, 11(2), 40; https://doi.org/10.3390/geriatrics11020040 - 7 Apr 2026
Abstract
►▼
Show Figures
The hemodialysis population has progressively aged over the past two decades; in several settings, adults aged ≥75 years represent one of the fastest-growing populations receiving dialysis. Frailty, characterized by reduced physiological reserve and heightened vulnerability to stressors, has emerged as a critical determinant
[...] Read more.
The hemodialysis population has progressively aged over the past two decades; in several settings, adults aged ≥75 years represent one of the fastest-growing populations receiving dialysis. Frailty, characterized by reduced physiological reserve and heightened vulnerability to stressors, has emerged as a critical determinant of outcomes and is commonly assessed using validated instruments such as the Fried Frailty Phenotype or the Clinical Frailty Scale (CFS). Reported frailty prevalence in hemodialysis varies widely (approximately 20% to >80%), largely depending on the assessment instrument and the population studied, with consistently higher prevalence in older cohorts. It is consistently associated with older age, female sex, diabetes, lower serum albumin, cardiovascular disease, longer dialysis vintage, and lower physical activity. Compared with non-frail patients, frail hemodialysis patients have a substantially higher risk of death (approximately two-fold in pooled analyses). Seminal trials and large observational programs that shaped hemodialysis targets underrepresented very old, frail, and highly comorbid patients, limiting generalizability. In frail older adults with limited life expectancy and substantial comorbidity burden, standard thrice-weekly schedules, higher ultrafiltration intensity, and a uniform ‘fistula-first’ approach may increase treatment burden without clear proportional gains in patient-centered outcomes. This review examines evidence supporting individualized hemodialysis strategies in frail older adults. As the dialysis population continues to age, proficiency in goal-concordant, personalized prescribing is increasingly important for nephrologists and dialysis teams.
Full article

Figure 1
Open AccessProject Report
Impact of Comprehensive Geriatric Assessments on Dementia Care
by
Shazia Durrani, Minhal Mussawar and Mariam Alaverdashvili
Geriatrics 2026, 11(2), 39; https://doi.org/10.3390/geriatrics11020039 - 1 Apr 2026
Abstract
Introduction: According to the Alzheimer Society of Canada, over 770,000 people in Canada are living with dementia. This number is expected to rise to nearly 1 million people by 2030. Although the provision of team-based interprofessional assessment in gerontological care is critical for
[...] Read more.
Introduction: According to the Alzheimer Society of Canada, over 770,000 people in Canada are living with dementia. This number is expected to rise to nearly 1 million people by 2030. Although the provision of team-based interprofessional assessment in gerontological care is critical for the early detection and prevention of dementia, its planning and delivery can be a challenge. In Saskatchewan, previous assessments have identified significant gaps between actual and best practices in dealing with this medical condition. The emergence of Geriatric Services Resource Teams (GSRTs), which apply an innovative, team-based model to improve the diagnosis and care of older adults with complex health practices, can be proven beneficial in this regard. The purpose of this study is to compare the efficacy of the care provision process between a GSRT and a traditional medical care channel (i.e., primary health) with respect to dementia patients. Methods: A retrospective patient chart review was conducted by collecting data from a large Primary Care practice (n = 90) and the GSRT in Regina (n = 75). Collected data included information on patient demographics and treatment, and the diagnosis process itself. Results: While demographic characteristics between patient groups were similar, significant differences (p < 0.05) were found in the involvement of pharmacy and other healthcare professionals, prescriptions for memory loss, and in who made the diagnosis. Moreover, although the dementia diagnosis was usually made first in Primary Care, further clarification of the type of dementia, counseling of diagnosis, review of medication, and assessment of functions and social supports were better managed in the GSRT group. Discussion: The use of Geriatric Services Resource Teams is a relatively new concept in Saskatchewan. As these teams are established, initial results show that their role in complex care management has beneficial outcomes for dementia patients.
Full article
Open AccessSystematic Review
The Need for Standardized Data Collection to Improve Harmonization and Pooling of Information About Modifiable Risk Factors for Alzheimer’s Diseases in Italian Clinical Studies: A Systematic Review
by
Patrizio Allegra, Manuela Lodico, Claudia Migliazzo, Domenico Tarantino, Tommaso Piccoli, Nicola Vanacore, Giuseppe Salemi, Laura Maniscalco and Domenica Matranga
Geriatrics 2026, 11(2), 38; https://doi.org/10.3390/geriatrics11020038 - 31 Mar 2026
Abstract
►▼
Show Figures
Background/Objectives: At the international level, harmonized networks of dementia clinical studies are available, but Italian participation remains limited. This systematic review aims to define harmonization rules to facilitate the inclusion of Italian clinical studies in existing networks and to propose standardized data collection
[...] Read more.
Background/Objectives: At the international level, harmonized networks of dementia clinical studies are available, but Italian participation remains limited. This systematic review aims to define harmonization rules to facilitate the inclusion of Italian clinical studies in existing networks and to propose standardized data collection methods to enable comparison of the study results. Methods: A systematic review was conducted (January 2019–December 2024) to identify Italian clinical studies evaluating Alzheimer’s disease and other dementias as outcomes. Eight modifiable risk factors were extracted: BMI, arterial hypertension, diabetes, dietary patterns, alcohol consumption, smoking habits, depressive symptomatology, and physical activity. WHO definitions and internationally accepted criteria were used as reference standards. Variable harmonization potential was assessed using the DataSHaPER methodology and classified as complete, partial, or impossible, considering information loss across studies. Results: Of 365 records identified, 18 studies met the inclusion criteria. Obesity assessed via BMI showed the highest harmonization potential (44% complete, 33% partial), along with dietary habits measured by food frequency questionnaires (44% complete). Diabetes and physical inactivity followed (33% complete), assessed through fasting glucose or pharmacological treatment and the IPAQ, respectively. Smoking habits classified as current, former, or never smokers were reported in 28% of studies. Depression (assessed by GDS or CES-D) and hypertension (blood pressure measurement or antihypertensive treatment) showed complete harmonization in only 22% of studies. Conclusions: Italian studies show substantial limitations in the harmonization of modifiable risk factor data for Alzheimer’s disease, mainly due to heterogeneous and non-standardized data collection methods, highlighting the need for uniform research protocols.
Full article
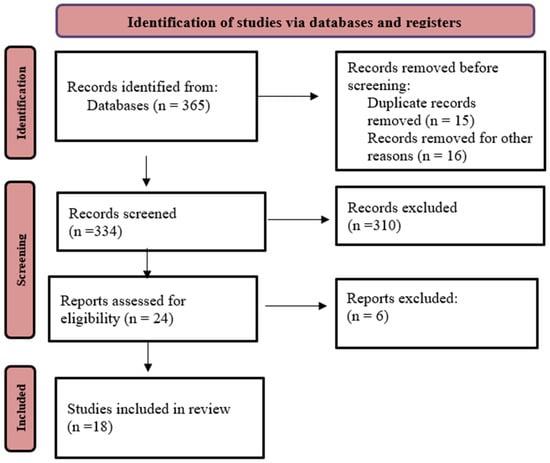
Figure 1
Open AccessCommentary
Prescribing Cascade as a Therapeutic Error: A Danger for Geriatric Patients with Multimorbidity
by
Adrian Bryła, Jarosław Woroń, Miłosz Miedziaszczyk, Barbara Lorkowska-Zawicka, Beata Bujak-Giżycka, Daniel Orzechowski, Paulina Połetek and Wojciech Pałys
Geriatrics 2026, 11(2), 37; https://doi.org/10.3390/geriatrics11020037 - 31 Mar 2026
Abstract
►▼
Show Figures
The aging of the population and the increasing prevalence of multimorbidity contribute to the widespread use of polypharmacotherapy, which in turn elevates the risk of adverse drug reactions and clinically significant drug–drug interactions. One of the key yet frequently underestimated issues in clinical
[...] Read more.
The aging of the population and the increasing prevalence of multimorbidity contribute to the widespread use of polypharmacotherapy, which in turn elevates the risk of adverse drug reactions and clinically significant drug–drug interactions. One of the key yet frequently underestimated issues in clinical practice is the prescribing cascade, which occurs when an adverse drug reaction is misinterpreted as a new medical condition, leading to the initiation of an additional medication. This phenomenon is particularly relevant in the older population, in whom altered pharmacokinetics and pharmacodynamics, together with reduced organ reserve, increase susceptibility to adverse drug events, including nephrotoxicity (renal impairment is used throughout the review as a clinically relevant example of organ-specific harm resulting from prescribing cascades, rather than as the sole focus of the analysis). This article discusses the mechanisms and clinical consequences of the prescribing cascade—with particular emphasis on renal function deterioration—as well as strategies for its prevention in the geriatric population. Analysis of the literature indicates that prescribing cascades remain insufficiently recognized in clinical practice, despite the availability of pharmacotherapy assessment tools such as The American Geriatrics Society (AGS) Beers Criteria and the STOPP/START criteria. Documented prescribing cascades have been shown to contribute to deterioration in health status and quality of life, an increased frequency of hospitalizations, and a greater burden on healthcare systems. Particularly concerning are cascades involving cardiovascular, neurological, and analgesic medications, which may induce or exacerbate renal injury, ultimately leading to chronic kidney disease and organ failure. Prescribing cascades represent a significant yet frequently underestimated threat to the efficacy and safety of pharmacotherapy in older adults. Their consequences may extend beyond reduced quality of life and increased treatment costs to include serious complications such as the development of renal failure. Enhancing clinicians’ awareness, conducting systematic medication reviews, and employing validated assessment tools are essential for the identification and prevention of prescribing cascades, thereby reducing the risk of renal injury and improving clinical outcomes.
Full article
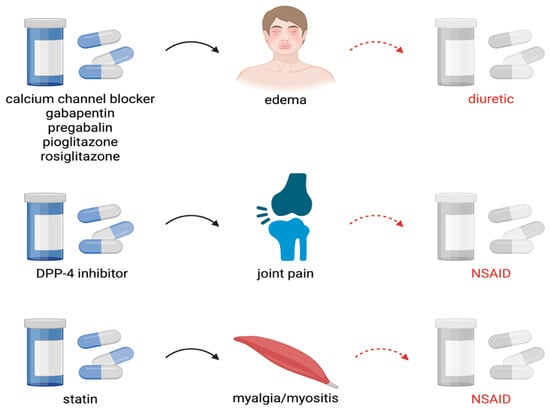
Figure 1
Open AccessArticle
Emergency Ventral Hernia Management in Older Adults: A Retrospective Cohort Study and Structured Review of the Literature
by
Ivan Tomasi, Jeremy Samuel, Eimante Raupelyte, Antonia Elizabeth Loizou, Angela Wang Yihui, Lilian Chioma Ujunwa Nwosu, Sneha Mehrotra, Mariia Druziagina, Kenneth Wing Ngai Law and Magda Sbai
Geriatrics 2026, 11(2), 36; https://doi.org/10.3390/geriatrics11020036 - 27 Mar 2026
Abstract
►▼
Show Figures
Background/Objectives: Older adults frequently present with emergency ventral hernias, a situation that carries significant physiological risks and often requires challenging clinical decisions. Despite the prevalence of these cases, there is a lack of robust evidence to inform emergency care in this demographic,
[...] Read more.
Background/Objectives: Older adults frequently present with emergency ventral hernias, a situation that carries significant physiological risks and often requires challenging clinical decisions. Despite the prevalence of these cases, there is a lack of robust evidence to inform emergency care in this demographic, as most existing research centres on short-term mortality rates and operative variables. Key aspects such as the impact of frailty and the course of recovery following surgery are insufficiently addressed in the literature. This study aimed to describe management strategies, frailty burden and postoperative outcomes in older adults presenting with emergency ventral hernias. Methods: This study retrospectively examined patients aged 65 and older who were admitted to a UK tertiary centre with emergency ventral hernias from February 2016 to July 2024. Data, including patient demographics, comorbid conditions, frailty status (as measured by the Clinical Frailty Scale), management approach, healthcare resource use, and clinical outcomes, were analysed descriptively. Additionally, a structured literature review was conducted in accordance with PRISMA guidelines to identify research on emergency ventral hernia treatment outcomes in adults aged 60 years and older. Results: A total of 67 patients met the inclusion criteria for the cohort. High rates of frailty and multiple coexisting health conditions were observed. While surgical intervention was the predominant management strategy, a subset of patients received conservative or palliative care. Greater degrees of frailty correlated with longer hospital stays and an increased need for critical care, even though six-month mortality remained comparatively low. Traditional risk assessment tools tended to overpredict mortality risk and failed to reflect the true postoperative burden or the recovery process. The systematic review yielded 7 studies, most of which documented mortality and complication rates, but few addressed frailty or provided detailed postoperative recovery data. Conclusions: The management of emergency ventral hernias in older adults is highly variable, with a significant postoperative impact that extends beyond mortality statistics. Assessing frailty appears to provide additional information that may support clinical decision-making and help anticipate recovery after surgery. Integrating frailty evaluation into emergency hernia care could enhance multidisciplinary collaboration and help ensure that treatment plans are better tailored to patient vulnerability and individual care goals.
Full article

Graphical abstract

Journal Menu
► ▼ Journal Menu-
- Geriatrics Home
- Aims & Scope
- Editorial Board
- Reviewer Board
- Topical Advisory Panel
- Instructions for Authors
- Special Issues
- Topics
- Sections & Collections
- Article Processing Charge
- Indexing & Archiving
- Most Cited & Viewed
- Journal Statistics
- Journal History
- Journal Awards
- Conferences
- Editorial Office
- 10th Anniversary
Journal Browser
► ▼ Journal BrowserHighly Accessed Articles
Latest Books
E-Mail Alert
News
Topics
Topic in
IJERPH, Medicina, Hospitals, Healthcare, Safety, Geriatrics
The Imperative of Patient Safety and Safety Culture in Contemporary Healthcare
Topic Editors: Hana Brborović, Ognjen Brborovic, Reinhard StrametzDeadline: 8 July 2026
Topic in
Geriatrics, IJMS, Life, Sports, Neurology International, Obesities
Exercise and Human Aging: Physiological and Psychological Functions
Topic Editors: Samuel Da Silva Aguiar, Ismael Perez-SuarezDeadline: 20 September 2026
Topic in
IJMS, Cells, Biomolecules, Geriatrics, Immuno
Inflammaging: The Immunology of Aging, 2nd Edition
Topic Editors: Brianna Cyr, Juan Pablo de Rivero VaccariDeadline: 15 February 2027
Topic in
Behavioral Sciences, Brain Sciences, Geriatrics
Psychopathology and Developmental Trajectories
Topic Editors: Donatella Rita Petretto, Carmelo Masala, Stefan BogaertsDeadline: 31 March 2027

Conferences
Special Issues
Special Issue in
Geriatrics
Healthy Ageing and Lifestyle Medicine: Current Knowledge and Future Direction (2nd Edition)
Guest Editors: Alice Masini, Massimiliano PanellaDeadline: 10 May 2026
Special Issue in
Geriatrics
Oral Health Care in Older Adults
Guest Editor: Alice Kit Ying ChanDeadline: 20 May 2026
Special Issue in
Geriatrics
Digital Health Equity: Bridging the Gap for Elderly People and People with Disabilities
Guest Editors: Donatella Rita Petretto, Roberto Pili, Luca GavianoDeadline: 31 May 2026
Special Issue in
Geriatrics
Quality of Life in Older Adults with Musculoskeletal or Neuromuscular Disorders: Assessment and Intervention Strategies
Guest Editor: Tatsunori IkemotoDeadline: 20 June 2026
Topical Collections
Topical Collection in
Geriatrics
Joint Arthroplasty in the Oldest People
Collection Editors: Juan F. Blanco, Carmen da Casa
Topical Collection in
Geriatrics
Ageism, the Black Sheep of the Decade of Healthy Ageing
Collection Editor: Lydia Gimenez Llort
Topical Collection in
Geriatrics
Responding to the Pandemic: Geriatric Care Models
Collection Editor: James Powers







