-
 Addressing the Shortage of GLP-1 RA and Dual GIP/GLP-1 RA-Based Therapies—A Systematic Review
Addressing the Shortage of GLP-1 RA and Dual GIP/GLP-1 RA-Based Therapies—A Systematic Review -
 The Intricate Relationship Between Thyroid Disorders and Type 2 Diabetes—A Narrative Review
The Intricate Relationship Between Thyroid Disorders and Type 2 Diabetes—A Narrative Review -
 Medication Adherence and Glycemic Control in Older Adults with Type 2 Diabetes: A Cross-Sectional Study in a Community Setting
Medication Adherence and Glycemic Control in Older Adults with Type 2 Diabetes: A Cross-Sectional Study in a Community Setting -
 The Relationship Between Quality of Life, Diabetes Distress, and Metabolic Control in Hungarian Type 1 Diabetic Patients: A Cross-Sectional Study
The Relationship Between Quality of Life, Diabetes Distress, and Metabolic Control in Hungarian Type 1 Diabetic Patients: A Cross-Sectional Study -
 The Role of Vitamin C in Wound Healing in Surgically Managed Diabetic Foot Disease
The Role of Vitamin C in Wound Healing in Surgically Managed Diabetic Foot Disease
Journal Description
Diabetology
Diabetology
is an international, peer-reviewed, open access journal on diabetes research published monthly online by MDPI.
- Open Access— free for readers, with article processing charges (APC) paid by authors or their institutions.
- High Visibility: indexed within ESCI (Web of Science), Scopus, EBSCO, and other databases.
- Rapid Publication: manuscripts are peer-reviewed and a first decision is provided to authors approximately 24.4 days after submission; acceptance to publication is undertaken in 8.9 days (median values for papers published in this journal in the second half of 2025).
- Journal Rank: CiteScore - Q2 (Medicine (miscellaneous))
- Recognition of Reviewers: APC discount vouchers, optional signed peer review, and reviewer names published annually in the journal.
Impact Factor:
2.2 (2024);
5-Year Impact Factor:
2.5 (2024)
Latest Articles
QSAR Insights into Antidiabetic Activity of Natural Sulfur-Containing Compounds
Diabetology 2026, 7(4), 81; https://doi.org/10.3390/diabetology7040081 - 20 Apr 2026
Abstract
►
Show Figures
Plants of the genus Salacia (Celastraceae) have long been used in traditional medical systems of South and Southeast Asia for the management of diabetes and related metabolic disorders. Modern phytochemical and pharmacological studies have confirmed the antidiabetic potential of several Salacia species, leading
[...] Read more.
Plants of the genus Salacia (Celastraceae) have long been used in traditional medical systems of South and Southeast Asia for the management of diabetes and related metabolic disorders. Modern phytochemical and pharmacological studies have confirmed the antidiabetic potential of several Salacia species, leading to the identification of a distinctive group of sulfur-containing sugars as their principal bioactive constituents. Salacinol, neosalacinol, kotalanol, neokotalanol, and related analogues represent a novel class of thiosugar sulfonium compounds that act as potent and selective α-glucosidase inhibitors, providing a clear mechanistic basis for their glucose-lowering effects. Simpler thiosugars, such as 5-thiomannose, further contribute to the overall metabolic activity of Salacia extracts and may serve as biosynthetic or functional precursors. Beyond Salacia, sulfur-containing natural products are widespread in nature and perform diverse biological roles. In particular, the genus Allium is well known for producing organosulfur compounds, including thioethers and polysulfides, which exhibit antidiabetic, hypolipidemic, antioxidant, and cardioprotective activities. In a different context, sulfur-containing hopanes have been identified in sediments and petroleum as products of early diagenetic sulfurization of bacterial hopanoids. Although these compounds have been studied primarily as geochemical biomarkers, recent QSAR/PASS analyses suggest that sulfur hopanes may also possess biologically relevant activities, particularly related to metabolic and cardiovascular regulation. Recent PASS-based QSAR evaluations of Salacia-derived thiosugars and sulfur hopanes predict significant antidiabetic activity, including potential type 2 diabetes-related pharmacological effects, supported by predicted α-glucosidase inhibitory, hypoglycemic, hepatic, and gastrointestinal activities. Collectively, these findings highlight sulfur-containing natural products from both plant and sedimentary sources as chemically diverse yet functionally convergent scaffolds with promising potential for the development of functional foods and therapeutic agents targeting metabolic disorders.
Full article
Open AccessArticle
A Thematic Analysis of Sleep Behavior Self-Regulation in Young Adults with Type 1 Diabetes
by
Madeline Long, Dayna A. Johnson, Youjeong Kang and Stephanie Alisha Griggs
Diabetology 2026, 7(4), 80; https://doi.org/10.3390/diabetology7040080 - 14 Apr 2026
Abstract
Background/Objectives: Sleep is critical for young adults, particularly those with type 1 diabetes (T1D), who face unique challenges in achieving recommended sleep and diabetes health targets. The purpose of this study guided by the theoretical framework of self-regulation theory is to explore
[...] Read more.
Background/Objectives: Sleep is critical for young adults, particularly those with type 1 diabetes (T1D), who face unique challenges in achieving recommended sleep and diabetes health targets. The purpose of this study guided by the theoretical framework of self-regulation theory is to explore how these individuals navigate self-regulatory processes in their sleep behaviors through mechanisms of self-monitoring, self-judgment, and self-evaluation. Methods: A qualitative descriptive design was implemented using semi-structured interviews with 34 young adults (ages 18–30) living with T1D. Data were collected through focused interviews, sleep diaries, actigraphy, and continuous glucose monitoring, followed by thematic analysis to identify sleep behavior self-regulation patterns. Results: Three primary themes were identified: (1) Sleep Behavior Self-Monitoring—highlighting participants’ awareness of their sleep habits and the diabetes-related impacts on these habits; (2) Sleep Behavior Self-Judgment—reflecting how personal and societal standards inform their evaluation of sleep health; (3) Sleep Behavior Self-Evaluation—showing emotional responses associated with sleep out-comes, where good sleep led to positive feelings and motivation, while poor sleep resulted in frustration. Conclusions: Understanding sleep behavior self-regulation among young adults with T1D is crucial for improving sleep health and diabetes management. Targeted interventions incorporating sleep education and self-regulatory strategies may enhance both perceived sleep quality and overall well-being in this population.
Full article
(This article belongs to the Special Issue Advances in Sleep Disorders in Patients with Diabetes)
►▼
Show Figures

Graphical abstract
Open AccessArticle
Trabecular and Cortical Bone and Ossified Vessel Analysis in Rat Tibiae and Femora in a Polygenic Rat Model for Type 2 Diabetes Mellitus
by
Jason McIntire, Hope Oyeyemi, Michelle L. Harrison, Suchit Chidurala, Richard K. McCuller, Milena Samora, Yu Huo, Ann-Katrin Grotle, Audrey J. Stone, Kimber L. Stanhope, Peter J. Havel and Rhonda D. Prisby
Diabetology 2026, 7(4), 79; https://doi.org/10.3390/diabetology7040079 - 14 Apr 2026
Abstract
►▼
Show Figures
Background: In type 2 diabetes mellitus (T2DM), bone and microvascular complications may be linked. Methods: The University of California Davis (UCD) polygenic T2DM and Sprague Dawley healthy control (CTL) rats (N = 48) were divided equally into diabetic and age-matched groups: (1) pre-diabetes,
[...] Read more.
Background: In type 2 diabetes mellitus (T2DM), bone and microvascular complications may be linked. Methods: The University of California Davis (UCD) polygenic T2DM and Sprague Dawley healthy control (CTL) rats (N = 48) were divided equally into diabetic and age-matched groups: (1) pre-diabetes, (2) diabetes onset, (3) early-stage T2DM, and (4) late-stage T2DM. Body mass, HbA1c, fasted blood glucose and femoral and tibial lengths were measured. Bones were scanned (μCT; 15 µm) to assess trabecular microarchitecture and density and mid-shaft cortical thickness (Ct.Th, µm), density and porosity. Ossified vessel volume (OsVV, %) and thickness (OsV.Th, µm) were also analyzed. A GLM determined significance at p < 0.05. Body mass and HbA1c were higher (p < 0.05) in all T2DM groups and blood glucose became elevated (p < 0.05) in early-stage T2DM and late-stage T2DM. Results: Tibiae and femora were longer (p < 0.05) with diabetes. Tibial bone volume was lower (p < 0.05) in pre-diabetes (4 ± 1% vs. CTL, 9 ± 2%) and late-stage T2DM (5 ± 2% vs. CTL, 8 ± 2%), and femoral bone volume was lower (p < 0.05) in pre-diabetes (7 ± 1% vs. 12 ± 4%). Cortical density (tibia) was lower (p < 0.05) in pre-diabetes and early-stage T2DM. Trabecular density in the femur was lower (p < 0.05) in all T2DM groups and cortical density was reduced (p < 0.05) in pre-diabetes, diabetes onset, and late-stage T2DM. OsVV in both bones were lower (p < 0.05) during early-stage T2DM. Tibial OsV.Th was higher (p < 0.05) in pre-diabetes (69 ± 14 µm vs. CTL, 56 ± 13 µm) and late-stage T2DM (80 ± 10 µm vs. CTL, 59 ± 13 µm) and higher (p < 0.05) in the femur at diabetes onset (58 ± 14 µm vs. CTL, 40 ± 10 µm). Conclusions: Trabecular and cortical bone varied as diabetes progressed, and the thicker ossified vessels may represent microangiopathy.
Full article

Figure 1
Open AccessArticle
Long-Term Hyperglycemia Affects the Expression of Diaph1 and Its Cytoskeleton Ligands in the Epidermis of Diabetic Patients—A Quantitative Study
by
Bernard Kordas, Wojciech Matuszewski, Robert Modzelewski, Jarosław Szuszkiewicz, Michał Załęcki, Joanna Wojtkiewicz and Judyta Juranek
Diabetology 2026, 7(4), 78; https://doi.org/10.3390/diabetology7040078 - 10 Apr 2026
Abstract
►▼
Show Figures
Background/Objectives: Diabetic small fiber neuropathy and related sensory and epidermal problems affect up to 70% of all patients with diabetes. Long-term hyperglycemia disrupts cytoskeletal organization and axonal transport; however, molecular changes within human diabetic epidermis remain understudied. Diaph1 and its cytoskeletal ligands,
[...] Read more.
Background/Objectives: Diabetic small fiber neuropathy and related sensory and epidermal problems affect up to 70% of all patients with diabetes. Long-term hyperglycemia disrupts cytoskeletal organization and axonal transport; however, molecular changes within human diabetic epidermis remain understudied. Diaph1 and its cytoskeletal ligands, including β-Actin and Profilin, are key regulators of cytoskeletal dynamics and may be associated with diabetes-related alterations in skin structure and innervation. Methods: Sixteen patients with type 2 diabetes, aged 43.3 ± 9.6 years (disease duration 18.9 ± 8.7 years), and twelve non-diabetic controls, aged 43.9 ± 8.9 years, were enrolled in the study. All participants provided informed consent. Skin punch biopsies were obtained under local anesthesia and processed for staining of PGP 9.5, Diaph1, β-Actin, and Profilin. Quantitative image analysis was performed to assess stained area fraction, signal intensity, and intraepidermal nerve fiber density. Statistical comparisons and Spearman’s rank correlation analyses were used to evaluate group differences and associations between staining parameters. Results: Diabetic skin samples exhibited a significant reduction in PGP 9.5-positive intraepidermal nerve fibers, indicating reduced cutaneous innervation. In contrast, Diaph1 and Profilin showed broader and more diffuse epidermal staining, while β-Actin displayed altered staining patterns and intensity. Significant correlations between Diaph1- and β-Actin-related staining measures indicated an association consistent with altered cytoskeletal organization under chronic hyperglycemic conditions. Conclusions: Long-standing type 2 diabetes was associated with reduced PGP 9.5-positive intraepidermal nerve fibers, together with altered epidermal staining patterns of Diaph1, Profilin and β-Actin. These findings indicate coexisting cutaneous denervation and cytoskeletal alterations in diabetic skin.
Full article

Graphical abstract
Open AccessArticle
Sexual Dimorphism in the Association Between Vitamin D and Depressive Symptoms in Diabetic Patients and the Mediating Role of BMI: A Cross-Sectional Study
by
Miriam Hernández-López, Rafael Ramírez-Carracedo, Mónica Grande-Alonso, Alba Sebastián-Martín and Rafael Moreno-Gómez-Toledano
Diabetology 2026, 7(4), 77; https://doi.org/10.3390/diabetology7040077 - 9 Apr 2026
Abstract
►▼
Show Figures
Background: The interplay between vitamin D deficiency, obesity, and depressive symptoms in type 2 diabetes remains poorly understood. Potential sex-specific differences in these associations have not been fully explored. Methods: We conducted a cross-sectional analysis of patients with type 2 diabetes
[...] Read more.
Background: The interplay between vitamin D deficiency, obesity, and depressive symptoms in type 2 diabetes remains poorly understood. Potential sex-specific differences in these associations have not been fully explored. Methods: We conducted a cross-sectional analysis of patients with type 2 diabetes (N = 917) from the NHANES 2017–2018 cycle. Restricted cubic spline models were used to assess potential non-linear associations between serum 25-hydroxyvitamin D3 and PHQ-9 depression scores. Regression-based mediation analysis was performed to estimate total, direct, and indirect associations, with body mass index (BMI) considered as a potential mediator. Models were adjusted for relevant demographic and cardiometabolic covariates. Results: In the overall diabetic cohort, higher vitamin D levels were modestly associated with lower depressive symptom scores. Mediation analysis suggested that this association was statistically accounted for by BMI. In sex-stratified analyses, significant total and indirect associations were observed among men, with a remaining direct association after adjustment for BMI, whereas no statistically significant associations were detected among women. Formal interaction testing supported differential association patterns by sex. Conclusions: Among adults with type 2 diabetes, serum vitamin D levels were inversely associated with depressive symptoms, with evidence suggesting sex-specific association patterns. These findings warrant further investigation in prospective studies to clarify potential underlying mechanisms and clinical implications.
Full article

Figure 1
Open AccessArticle
Identifying Risk Factors Associated with the Severity of Foot Ulcers in Type 2 Diabetic Patients: Evidence from a Hospital-Based Study in Rajshahi, Bangladesh
by
Shah Tanzen Jahan, Durga H. Kutal, Anicha Akter, Md. Selim Reza, Md. Kabirul Islam and Md. Monimul Huq
Diabetology 2026, 7(4), 76; https://doi.org/10.3390/diabetology7040076 - 8 Apr 2026
Abstract
►▼
Show Figures
Background: Diabetic foot ulcer (DFU) is a major complication of type 2 diabetes (T2D), frequently resulting in disability, lower-limb amputation, and substantial healthcare burden. Early identification of patients at high risk of progressing to severe DFU is essential for timely intervention, yet evidence
[...] Read more.
Background: Diabetic foot ulcer (DFU) is a major complication of type 2 diabetes (T2D), frequently resulting in disability, lower-limb amputation, and substantial healthcare burden. Early identification of patients at high risk of progressing to severe DFU is essential for timely intervention, yet evidence on associated risk factors remains limited in Bangladesh. This study aims to identify demographic, clinical, and behavioral predictors of severe DFU to support early management strategies. Methods: A cross-sectional study was conducted among 159 DFU patients attending the Rajshahi Diabetic Association General Hospital, Bangladesh. Data on demographic characteristics, clinical variables, and behavioral factors were obtained through structured questionnaires and standardized examinations. Severe DFU was defined as Wagner grades 3–5, while grades 0–2 were considered non-severe. Firth’s penalized logistic regression was used to identify determinants of severe DFU. Model performance was assessed using ROC analysis, calibration belt analysis, and decision curve analysis (DCA). Results: Among the 159 participants, 101 (63.5%) presented with severe DFU. Patients with severe DFU had significantly higher BMI (26.1 vs. 23.7 kg/m2), treatment costs (50,000 vs. 20,000 BDT), and were older (57 vs. 54 years). Severe DFU was also associated with higher prevalence of peripheral arterial disease (PAD) (29.7% vs. 3.4%), prior amputation (31.7% vs. 3.4%), peripheral neuropathy (PN) (86.1% vs. 58.6%), and poor glycemic control (71.3% vs. 30.7%) (all p < 0.05). Firth’s regression identified older age (aOR 1.08), poor glycemic control (aOR 3.90), PN (aOR 3.41), PAD (aOR 7.54), and previous amputation (aOR 13.67) as independent predictors of severe DFU. Conclusions: Older age, uncontrolled glycemia, PN, PAD, and prior amputation were significantly associated with severe stages of DFU. Early detection and targeted management of these factors are critical to reducing complications and lowering the healthcare burden.
Full article
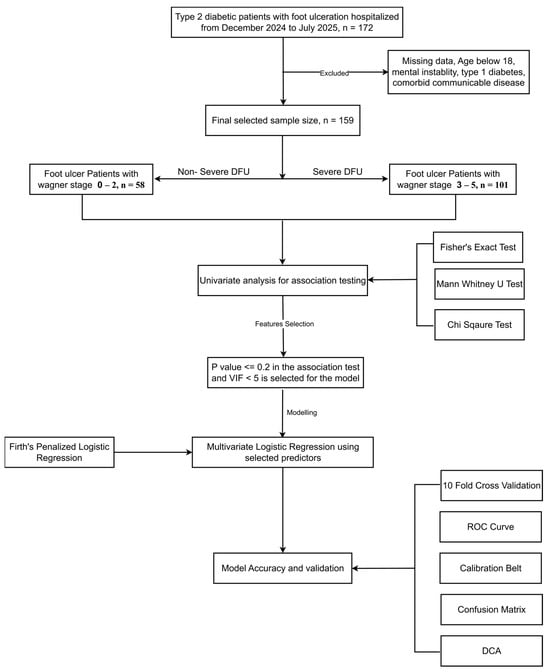
Figure 1
Open AccessArticle
Effect of Metformin on Sleep Architecture in Patients with Comorbid Diabetes and Sleep Apnea
by
Kristen Masada, Daniel Nguyen and Madhu Varma
Diabetology 2026, 7(4), 75; https://doi.org/10.3390/diabetology7040075 - 7 Apr 2026
Abstract
Background/Objectives: Patients with poor sleep are at high risk of developing type II diabetes mellitus (T2DM). Since T2DM is linked to increased risk of obstructive sleep apnea (OSA), and Metformin is commonly used to treat T2DM, we examined how Metformin affects sleep stages
[...] Read more.
Background/Objectives: Patients with poor sleep are at high risk of developing type II diabetes mellitus (T2DM). Since T2DM is linked to increased risk of obstructive sleep apnea (OSA), and Metformin is commonly used to treat T2DM, we examined how Metformin affects sleep stages in patients with concurrent T2DM and OSA-related symptoms of snoring and fatigue. Patients with T2DM on Metformin progressively develop increased insulin resistance associated with sleep disturbances and poor glycemic control. We therefore explored sleep pattern changes in patients with OSA symptoms and T2DM on Metformin, with a special focus on whether Metformin affects sleep architecture. Methods: Polysomnogram (PSG) data from patients with T2DM on Metformin was evaluated along with data on age, body-mass index (BMI), and biological sex. Data analysis included mean ± standard deviation, t-test with p < 0.05 taken as significant, and linear regression. Results: Patients with a BMI of less than 30 (non-obese) and taking Metformin exhibited a significantly shorter rapid eye movement sleep stage (REM) duration than patients on alternative therapies (p = 0.036). No such difference in REM was found for patients with a BMI of 30 or greater (obese) taking Metformin. While there was also no significant difference in slow-wave sleep stage (N3) duration with Metformin use, linear regression identified a moderate negative correlation between N3 and age in patients taking non-Metformin therapies (R2 = 0.4555). No significant correlations between sleep stage duration and patient sex, smoking status, or BMI greater than 30 were identified. Conclusions: Overall, patients with OSA and T2DM on Metformin had lower mean quantities of N3, and REM sleep compared to those not on Metformin. Non-obese patients with T2DM and OSA being treated with Metformin were observed to have less REM sleep, regardless of sex or smoking history. N3 and REM sleep are needed for the timely secretion of growth hormone and memory consolidation. Since Metformin is correlated with differences in N3 and REM sleep, it may contribute to the development of insulin resistance. Future studies are needed to explore potential causes for this relationship and how it may affect the treatment of T2DM.
Full article
(This article belongs to the Special Issue Advances in Sleep Disorders in Patients with Diabetes)
►▼
Show Figures

Figure 1
Open AccessArticle
Effect of Glycemic Management on Severity of Functional Impairment in Elderly Individuals with Type 2 Diabetes
by
Kohei Ueda, Rie Saito, Akiko Matsunaga, Takayuki Sonoda, Misako Kawaguchi, Saori Kaeriyama, Satsuki Sato, Yasuo Zenimaru, Masamichi Ikawa and Norio Harada
Diabetology 2026, 7(4), 74; https://doi.org/10.3390/diabetology7040074 - 3 Apr 2026
Abstract
Background/Objectives: Diabetes threatens independent living among elderly individuals. However, the effects of glycemic management on the severity of functional impairment are unclear. This study aimed to elucidate the relationship between glycemic management and functional impairment severity in elderly individuals with type 2 diabetes
[...] Read more.
Background/Objectives: Diabetes threatens independent living among elderly individuals. However, the effects of glycemic management on the severity of functional impairment are unclear. This study aimed to elucidate the relationship between glycemic management and functional impairment severity in elderly individuals with type 2 diabetes (T2D). Methods: We used data from the Japanese National Health Insurance Database from 2017 to 2024. The database included 11,411 elderly individuals (≥65 years) with Long-Term Care Insurance evaluations. Functional status was classified into three categories based on independence—Group A (non-mild impairment), Group B (moderate impairment), and Group C (severe impairment). The factors associated with the severity of functional impairment in patients with T2D were elucidated. Results: The severity of functional impairment was significantly greater in patients with T2D than in those without T2D. In participants with T2D, low glycated hemoglobin (HbA1c) levels were associated with the severity of functional impairment (odds ratio [OR]: 0.78; p < 0.001). In contrast, the use of antidiabetic drugs that could induce severe hypoglycemia (high-risk drugs) was positively associated with the severity of functional impairment (Group A vs. B/C: OR: 1.42; p < 0.001; Group C vs. A/B: OR: 1.90; p < 0.001). The frequency of high-risk drug use increased as functional impairment increased. Conclusions: The use of high-risk drugs is associated with the severity of functional impairment in elderly individuals with T2D. Elucidating the factors associated with the severity of functional impairment in elderly individuals with T2D may contribute to maintaining their quality of life and reducing the economic burden on healthcare and long-term care systems.
Full article
(This article belongs to the Special Issue Advances in Diabetes: Prevalence, Risk Factors, Complications, Costs and Disparities)
►▼
Show Figures

Graphical abstract
Open AccessArticle
Adipose Tissue Grafting: A New Paradigm in Diabetic Foot Treatment
by
Roberto Da Ros, Roberta Assaloni, Andrea Michelli, Barbara Brunato, Enrica Barro, Marta Nardi, Giovanni Papa and Cesare Miranda
Diabetology 2026, 7(4), 73; https://doi.org/10.3390/diabetology7040073 - 3 Apr 2026
Abstract
►▼
Show Figures
Background: Adipose tissue grafting is a regenerative medicine approach based on the use of autologous adipose tissue showing significant potential for the treatment of diabetic foot lesions. In subjects with diabetes, impaired wound healing, peripheral neuropathy, and vascular insufficiency contribute to the development
[...] Read more.
Background: Adipose tissue grafting is a regenerative medicine approach based on the use of autologous adipose tissue showing significant potential for the treatment of diabetic foot lesions. In subjects with diabetes, impaired wound healing, peripheral neuropathy, and vascular insufficiency contribute to the development of chronic ulcers and osteomyelitis, complicating traditional treatment strategies. Materials and Methods: We conducted a retrospective analysis of our center’s database, including all subjects treated for chronic diabetic foot ulcers who underwent adipose grafting with a follow-up of at least six months. For the control group, we included patients who received artificial dermis grafts rather than adipose grafts. Results: We identified 45 patients in the adipose group and 39 in the control group. Baseline characteristics were similar between the two groups for: mean age, diabetes duration, creatinine level, HbA1c, peripheral neuropathy, peripheral vascular disease and osteomyelitis. Coronary artery disease was prevalent in the control group. Wound location demonstrates a prevalent heel involvement for the adipose group. No patients experienced severe complications due to adipose graft: four patients (9%) developed a hematoma at the adipose tissue harvesting site, which was resolved spontaneously. At a mean follow-up of 12 ± 5 months, 30 (67%) patients achieved healing with a mean healing time of 202 ± 82 days, without requiring further surgical interventions. The control group achieved 51% of healing (p = 0.04), with a mean healing time longer than in the adipose graft group: 275 ± 132 days (p = 0.02). Moreover adipose graft permitted the best performance in rearfoot lesions. Conclusions: Adipose grafting is a safe and minimally invasive procedure with no major adverse events. Our data demonstrate its efficacy in promoting healing, even in chronic lesions with osteomyelitis and those located on the heel. Efficacy was found to be superior to that of the artificial dermis graft group.
Full article

Graphical abstract
Open AccessReview
Lipoprotein (a) and Apolipoproteins in Diabetes and Atherosclerotic Cardiovascular Disease: A Comprehensive Review of the Current Evidence
by
Albion Luzha, Michael Y. Henein, Guxim Bytyçi, Rina Tafarshiku, Gani Bajraktari and Venera Berisha-Muharremi
Diabetology 2026, 7(4), 72; https://doi.org/10.3390/diabetology7040072 - 3 Apr 2026
Abstract
Atherosclerosis, manifesting as acute myocardial infarction, stroke and peripheral artery disease, is the main cause of death worldwide. Conventional risk factors contributing to the development and progression of atherosclerosis are well established, including diabetes mellitus, hypertension, hypercholesterolemia, smoking and obesity. In recent decades,
[...] Read more.
Atherosclerosis, manifesting as acute myocardial infarction, stroke and peripheral artery disease, is the main cause of death worldwide. Conventional risk factors contributing to the development and progression of atherosclerosis are well established, including diabetes mellitus, hypertension, hypercholesterolemia, smoking and obesity. In recent decades, other lipid molecules have been identified as risk factors for atherosclerosis and arterial calcification, including lipoprotein (a) and apolipoproteins. Despite the available evidence for the association between those biomarkers and atherosclerosis in the general population, their impact on diabetic patients is incompletely characterized. This review aims to summarize the current evidence on the relationship between lipoprotein (a), apolipoproteins and atherosclerotic cardiovascular disease in diabetic patients. By integrating genetic, epidemiological, and mechanistic data, this review highlights the dual and context-dependent associations of lipoprotein (a) with incident type 2 diabetes and atherosclerotic cardiovascular risk, supporting more nuanced interpretation of Lp(a) in diabetes-related risk assessment.
Full article
(This article belongs to the Special Issue Precision Medicine for Diabetes: From Screening to Personalized Management)
►▼
Show Figures

Figure 1
Open AccessArticle
Diabetes-Related β-Cell Dysfunction Across COVID-19 and Metabolic Syndrome Is More Closely Associated with Chronic Oxidative Stress than with Transient Hypoxia
by
Victoria Tsvetkova, Malvina Todorova, Milena Atanasova, Irena Gencheva and Katya Todorova
Diabetology 2026, 7(4), 71; https://doi.org/10.3390/diabetology7040071 - 2 Apr 2026
Abstract
Aims/hypothesis: Hypoxia and oxidative stress have been implicated in both metabolic syndrome and COVID-19-associated dysglycaemia, yet it remains unclear whether shared or distinct mechanisms underlie β-cell dysfunction across these conditions. We investigated hypoxia- and oxidative stress-related pathways in relation to β-cell function
[...] Read more.
Aims/hypothesis: Hypoxia and oxidative stress have been implicated in both metabolic syndrome and COVID-19-associated dysglycaemia, yet it remains unclear whether shared or distinct mechanisms underlie β-cell dysfunction across these conditions. We investigated hypoxia- and oxidative stress-related pathways in relation to β-cell function during acute COVID-19, post-COVID metabolic states, and COVID-negative metabolic syndrome. Methods: In this prospective observational study, 100 adults were stratified into three groups: active COVID-19 (n = 32), post-COVID with newly diagnosed carbohydrate metabolism disorders (n = 35), and COVID-negative individuals with metabolic syndrome (n = 33). Circulating markers of hypoxia (HIF-1α), oxidative stress (8-epi-prostaglandin F2α), and antioxidant response (NFE2L2) were measured alongside α- and β-cell functional markers, including C-peptide, proinsulin, glucagon, and derived indices of β-cell processing and secretory efficiency. Non-parametric statistical analyses were applied. Results: Circulating HIF-1α levels differed significantly across study groups (p < 0.001), with the highest concentrations observed during active COVID-19, intermediate levels in COVID-negative individuals with metabolic syndrome, and the lowest levels in the post-COVID group. In contrast, oxidative stress, assessed by 8-epi-prostaglandin F2α, differed significantly across groups (p < 0.001), increasing from acute COVID-19 to post-COVID and reaching the highest levels in metabolic syndrome; however, the difference between the post-COVID and metabolic syndrome groups did not remain significant after correction for multiple testing. NFE2L2 concentrations did not differ significantly between groups. Marked β-cell dysfunction was observed predominantly in COVID-negative individuals with metabolic syndrome, characterized by reduced C-peptide levels, elevated glucagon concentrations, increased proinsulin/C-peptide ratios, and reduced C-peptide/glucose ratios (all overall group comparisons p < 0.001). In contrast, β-cell secretory indices were relatively preserved during acute and post-COVID states despite pronounced alterations in hypoxia and oxidative stress markers. Conclusions/interpretation: Hypoxia- and oxidative stress-related pathways exhibit distinct, context-dependent patterns across acute COVID-19, post-COVID dysglycaemia, and metabolic syndrome. Acute COVID-19 is characterized by pronounced hypoxia signalling with relative preservation of β-cell function, whereas chronic metabolic syndrome is associated with sustained oxidative stress and impaired β-cell processing and secretory efficiency. These findings suggest that diabetes-related β-cell dysfunction is more closely associated with chronic oxidative and metabolic stress than with transient infection-related hypoxia during SARS-CoV-2 infection.
Full article
(This article belongs to the Special Issue Beta-Cell Failure and Death: A Cornerstone in Diabetes Pathogenesis)
►▼
Show Figures

Graphical abstract
Open AccessArticle
Cost-Effectiveness of Pressure-Guided-Offloading-Improved Custom-Made Footwear for People with Diabetes at High Risk of Plantar Foot Ulceration
by
Sicco A. Bus, Jaap J. van Netten, Diekje R. Schouten and Marcel G. W. Dijkgraaf
Diabetology 2026, 7(4), 70; https://doi.org/10.3390/diabetology7040070 - 2 Apr 2026
Abstract
Background: Custom-made footwear that improves offloading using in-shoe pressure-guided techniques, when worn as recommended, reduces the risk of diabetic foot ulcer recurrence. We aimed to assess the cost-effectiveness of this approach, as it requires extra investments in equipment and personnel, and implementation is
[...] Read more.
Background: Custom-made footwear that improves offloading using in-shoe pressure-guided techniques, when worn as recommended, reduces the risk of diabetic foot ulcer recurrence. We aimed to assess the cost-effectiveness of this approach, as it requires extra investments in equipment and personnel, and implementation is not yet widespread. Methods: We conducted an economic evaluation using data from the DIAFOS RCT that randomized 171 participants at high ulcer risk to either pressure-guided-offloading-improved (intervention) or non-pressure-guided (usual care) custom-made footwear. The clinical outcome was the 18-month ulcer recurrence incidence, available from the RCT. Costs were modeled from a partial healthcare perspective using bottom-up unit cost calculation, with ulcer treatment costs obtained from reference data. Univariable regression analyses were executed to obtain incremental cost-effectiveness ratios (ICERs). Bootstrapping techniques accounted for uncertainty. Results: For the intervention, costs for ulcer recurrence were non-significantly lower (€−436; 95% CI: €−1434; €563) than for usual care. The ICER was €−8124 (i.e., costs saved to prevent one extra participant from having an ulcer), and the maximum probability for cost-effectiveness was 0.81. In the subgroup of participants who were adherent to wearing their prescribed footwear, costs for the intervention were non-significantly lower at €−1170 (95% CI: €−2595; €254), with ICER of €−5317, and a maximum probability for cost-effectiveness of 0.94. Conclusions: The use of in-shoe pressure-guided-offloading-improved custom-made footwear to help prevent diabetic foot ulcer recurrence is cost-effective with high probability when ulcer treatment costs are considered. Probability further increases when users adhere to their footwear. Future economic analyses should consider a full healthcare and societal perspective and use prospectively collected data on ulcer treatment costs.
Full article
(This article belongs to the Special Issue Prevention and Care of Diabetic Foot Ulcers)
►▼
Show Figures

Graphical abstract
Open AccessReview
Evaluation of the Present Perspective on Diabetic Foot Syndrome and Health Education and Analysis of the Impact of Educational Interventions: A Systematic Review and Meta-Analysis
by
Sol Tejeda-Ramírez, José Luis Lázaro-Martínez, Esther García-Morales, Sara García-Oreja, Laura Palacios-Abril and Aroa Tardáguila-García
Diabetology 2026, 7(4), 69; https://doi.org/10.3390/diabetology7040069 - 2 Apr 2026
Abstract
Aims: To evaluate the effectiveness of preventive educational interventions in individuals with diabetic foot syndrome (DFS) and to summarise current evidence on knowledge, self-care and health-education strategies related to this complication. Materials and methods: A systematic review and meta-analysis was conducted
[...] Read more.
Aims: To evaluate the effectiveness of preventive educational interventions in individuals with diabetic foot syndrome (DFS) and to summarise current evidence on knowledge, self-care and health-education strategies related to this complication. Materials and methods: A systematic review and meta-analysis was conducted in accordance with PRISMA guidelines. Risk of bias was evaluated using the Cochrane Handbook recommendations. Analyses were performed with Review Manager v5.4.1. Results: Educational interventions produced a significant improvement in patient knowledge and self-care practices compared with usual care. Despite some heterogeneity across studies, the overall effect favoured structured education as a preventive strategy for DFS-related complications. Conclusions: Preventive educational interventions enhance knowledge and self-care among individuals with DFS. Implementing structured education programs may help reduce complications and improve clinical outcomes.
Full article
(This article belongs to the Special Issue Prevention and Care of Diabetic Foot Ulcers)
►▼
Show Figures

Figure 1
Open AccessReview
G Protein-Coupled Receptors in Pancreatic β-Cells: From Trafficking and Localization to Insulin Secretion and Diabetes
by
Ramona M. Tecucianu, Sorin Tunaru and Stefana M. Petrescu
Diabetology 2026, 7(4), 68; https://doi.org/10.3390/diabetology7040068 - 2 Apr 2026
Abstract
►▼
Show Figures
G protein-coupled receptors (GPCRs) constitute the largest family of membrane receptors and are critical regulators of β-cell physiology. Nearly 300 GPCRs are expressed in human islets, where they integrate metabolic, hormonal, neuronal, and inflammatory cues to control insulin secretion, proliferation, and survival. Altered
[...] Read more.
G protein-coupled receptors (GPCRs) constitute the largest family of membrane receptors and are critical regulators of β-cell physiology. Nearly 300 GPCRs are expressed in human islets, where they integrate metabolic, hormonal, neuronal, and inflammatory cues to control insulin secretion, proliferation, and survival. Altered GPCR signaling contributes to β-cell dysfunction and the pathogenesis of both type 1 and type 2 diabetes. This review provides an overview of GPCR functions in β-cell biology, highlighting receptors that stimulate or inhibit glucose-stimulated insulin secretion, as well as those influencing β-cell fate. We also examine GPCR biosynthesis, trafficking, and subcellular localization—processes that shape receptor availability and signaling specificity. Aberrant folding, retention, or misrouting of GPCRs can disrupt β-cell function and contribute to metabolic disease. Thus, beyond receptor pharmacology, understanding the molecular mechanisms governing GPCR biogenesis and spatial distribution is essential for designing targeted strategies to preserve β-cell function and improve glucose homeostasis.
Full article

Figure 1
Open AccessArticle
Spinal Cord Lipid and ATPase Changes in Zucker Diabetic Fatty (ZDF) Rats, a Model of Type 2 Diabetes
by
Lenka Nemcová, Janka Kubincová, Mária Chomová, Katarína Orešanská and Monika Ďurfinová
Diabetology 2026, 7(4), 67; https://doi.org/10.3390/diabetology7040067 - 1 Apr 2026
Abstract
►▼
Show Figures
Background/Objectives: Altered lipid metabolism is a key feature of type 2 diabetes mellitus (T2DM), yet its impact on early spinal cord involvement remains poorly understood. Distinguishing between pathological lipid accumulation and adaptive metabolic responses is essential for interpreting initial stages of neural alteration
[...] Read more.
Background/Objectives: Altered lipid metabolism is a key feature of type 2 diabetes mellitus (T2DM), yet its impact on early spinal cord involvement remains poorly understood. Distinguishing between pathological lipid accumulation and adaptive metabolic responses is essential for interpreting initial stages of neural alteration in T2DM. This study aimed to characterize spinal cord lipid composition and ATPase activities in a rat model of T2DM. Methods: Zucker diabetic fatty (ZDF) rats were used as a model of T2DM and divided into diabetic and obese groups, with lean Zucker rats as controls. ATPase activities in spinal cord tissue were measured spectrophotometrically, and lipid profiling was performed using gas chromatography with flame-ionization detection. Indices of stearoyl-CoA desaturase-1 (SCD1) and delta-5 desaturase activity (D5D) were calculated from specific fatty acid ratios as estimates of enzyme-related activity. Results: Diabetic rats exhibited significantly higher levels of free monounsaturated fatty acids (MUFAs) compared with controls, while the obese group showed a moderate increase. Elevated SCD1 indices were indicative of increased estimated MUFA synthesis. Levels of free polyunsaturated fatty acids (PUFAs), including those crucial for myelin stability, as well as ATPase activities, remained unchanged, suggesting preserved basal membrane-associated enzyme function. Conclusions: This study identifies lipid alterations in the spinal cord preceding overt neurodegenerative changes in T2DM, characterized by increased free MUFA abundance, without evidence of altered ATPase activities. These findings support the interpretation that lipid changes observed at this stage are more consistent with adaptive metabolic remodeling than with overt structural or functional neural impairment.
Full article

Graphical abstract
Open AccessArticle
Association Between Adaptive Coping and Medication Adherence Among Patients with Type 2 Diabetes Mellitus
by
María Alicia Mejía-Blanquel, Ricardo Castrejón-Salgado, Miguel Trujillo-Martínez, María G. Ortiz-López, Gabriela Monserrat Huitzil-Juárez, Marco Antonio León-Mazón, Edith Araceli Cano-Estrada and José Ángel Hernández-Mariano
Diabetology 2026, 7(4), 66; https://doi.org/10.3390/diabetology7040066 - 1 Apr 2026
Abstract
►▼
Show Figures
Background/Objectives: Previous evidence suggests that psychosocial factors may play an important role in shaping medication adherence among individuals with chronic diseases; however, the relationship between adaptive coping and medication adherence in adults with type 2 diabetes (T2D) remains inconsistent, and evidence from
[...] Read more.
Background/Objectives: Previous evidence suggests that psychosocial factors may play an important role in shaping medication adherence among individuals with chronic diseases; however, the relationship between adaptive coping and medication adherence in adults with type 2 diabetes (T2D) remains inconsistent, and evidence from low- and middle-income settings, including Mexico, is limited. Given the high burden of T2D and the persistently high prevalence of medication non-adherence in this population, understanding potentially modifiable psychosocial determinants is particularly relevant. Hence, we aimed to evaluate the association between adaptive coping and medication adherence among Mexican adults with T2D. Methods: We conducted an analytical cross-sectional study among 564 adults attending two primary care health centers in Hidalgo, Mexico. Adaptive coping was assessed using the Coping and Adaptation Processing Scale, and medication adherence was measured with the four-item Morisky–Green–Levine Medication Adherence Scale. Associations of interest were evaluated using Poisson regression models to estimate prevalence ratios and 95% confidence intervals, adjusting for confounders. Results: The prevalence of medication non-adherence was 81.4%. Each 20-point increase in adaptive coping was associated with a 4.8% lower prevalence of non-adherence in adjusted models (PR = 0.95; 95% CI: 0.92–0.98), with no significant effect modification by sex or educational level. Conclusions: Lower adaptive coping was associated with a higher prevalence of medication non-adherence in adults with T2D. These findings contribute to the literature describing psychosocial factors in the context of diabetes care and situate coping among the psychosocial characteristics reported in individuals managing type 2 diabetes in primary care settings.
Full article

Figure 1
Open AccessArticle
Impact of Vascular Risk Factors on Longitudinal Changes in Diabetic Macular Edema After Intravitreal Therapy
by
Carmen Alba-Linero, José Coín Ruiz, Marta Mérida Luque, Javier Espíldora-Hernández and Mario Gutiérrez Bedmar
Diabetology 2026, 7(4), 65; https://doi.org/10.3390/diabetology7040065 - 1 Apr 2026
Abstract
Objectives: The aim of this study was to analyze the association between cardiovascular risk factors such as glycated hemoglobin (HbA1c), low-density lipoprotein cholesterol (LDL-C), hypertension, overweight, and smoking and longitudinal anatomical and functional changes in diabetic macular edema (DME) during intravitreal therapy. Materials
[...] Read more.
Objectives: The aim of this study was to analyze the association between cardiovascular risk factors such as glycated hemoglobin (HbA1c), low-density lipoprotein cholesterol (LDL-C), hypertension, overweight, and smoking and longitudinal anatomical and functional changes in diabetic macular edema (DME) during intravitreal therapy. Materials and Methods: This is a retrospective, observational, descriptive study conducted on a sample of 318 patients with DME associated with some degree of diabetic retinopathy (DR). They were treated with aflibercept, ranibizumab, and/or dexamethasone, assessing anatomical and functional outcomes through visual acuity, retinal thickness, and macular volume. Simultaneously, serum HbA1c and LDL-C levels, blood pressure, body mass index (BMI) and tobacco use were measured at baseline, 6, and 12 months to determine their association with treatment response using linear mixed models. Results: Of the variables analyzed in this study, HbA1c and degree of retinopathy were significantly associated with greater retinal thickness over time. Likewise, we found that, compared with aflibercept, dexamethasone intravitreal treatment was associated with greater retinal thickness over time. Concerning visual acuity, we found an inverse relationship with age, tobacco use and degree of retinopathy. Associations between outcomes and the initial intravitreal agent were observed; however, these findings should be interpreted cautiously. Conclusions: This study was consistent with previous research suggesting an association between glycemic control and DME response and progression. It also highlighted the importance of degree of retinopathy and intravitreal treatment in diabetic macular edema progression. Treatment-related findings represent exploratory associations and should not be interpreted as evidence of comparative effectiveness.
Full article
Open AccessArticle
Voluntary Exercise Delays Type 1 Diabetes Onset Independent of Splenic T Cell Subsets and Inflammatory Cytokines in NOD Mice
by
Marina Cetkovic-Cvrlje, Hans Addo, Mohammad A. Nimer, Sunny S. K. Chan and Gengyun Le-Chan
Diabetology 2026, 7(4), 64; https://doi.org/10.3390/diabetology7040064 - 1 Apr 2026
Abstract
Objectives: This study aimed to assess the effects of voluntary exercise on type 1 diabetes mellitus (T1D) development and splenic immunological profiles in non-obese diabetic (NOD) mice, a spontaneous model of human T1D. Methods: Prediabetic female NOD mice were randomly assigned to sedentary
[...] Read more.
Objectives: This study aimed to assess the effects of voluntary exercise on type 1 diabetes mellitus (T1D) development and splenic immunological profiles in non-obese diabetic (NOD) mice, a spontaneous model of human T1D. Methods: Prediabetic female NOD mice were randomly assigned to sedentary or exercise groups, with mice in the exercise group given 10-week wheel access and sedentary mice receiving none. Late-time mice were monitored to diabetes onset or 24 weeks of age; early-time mice were analyzed immediately post-intervention. Blood glucose, food intake, water consumption, and body mass were monitored weekly. At the endpoints, splenocyte counts, T and B cell subsets, and mitogen-stimulated cytokine production were analyzed using flow cytometry. Results: Mice in the exercise group ran an average of 20.76 ± 0.22 km/day. By the late-time endpoint, 75% of mice in the exercise group remained non-diabetic versus 35% of sedentary mice (p = 0.006). Mice in the exercise group demonstrated lower blood glucose (p = 0.015), visceral fat mass (p = 0.035), and water intake (p < 0.001) but higher food intake (p = 0.001), with no difference in body mass (p = 0.389) compared to sedentary mice. No differences were observed in splenocyte counts or Th, Tc, Treg, or B cell populations at either time point (p ≥ 0.185). Early-time point cytokines also did not differ between groups (p ≥ 0.08). Conclusions: Voluntary exercise reduces T1D incidence and mitigates hyperglycemia in NOD mice, suggesting a protective effect against disease progression. Despite the benefits, physical activity did not alter splenic Tcell subsets or inflammatory cytokines, demonstrating systemic immunomodulation may not be the primary driver of benefit. Our results indicate that voluntary exercise protects against T1D through tissue-specific or metabolic mechanisms, which warrant further mechanistic investigation.
Full article
(This article belongs to the Special Issue Exercise as Medicine: Exploring the Prevention and Management of Diabetes)
►▼
Show Figures

Figure 1
Open AccessArticle
Autonomic Dysfunction and Ocular Complications: The Role of Sudoscan in Diabetic Retinopathy Screening
by
Andra-Elena Nica, Emilia Rusu, Carmen Dobjanschi, Florin Rusu, Claudia Sivu, Oana Andreea Parliteanu, Ioana Verde, Andreea Andrita and Gabriela Radulian
Diabetology 2026, 7(4), 63; https://doi.org/10.3390/diabetology7040063 - 30 Mar 2026
Abstract
Background: Diabetic retinopathy (DR) remains one of the most frequent and severe complications in patients with type 2 diabetes (T2DM), with significant implications for vision and quality of life. While classical screening methods are effective, they are not always accessible or systematically used.
[...] Read more.
Background: Diabetic retinopathy (DR) remains one of the most frequent and severe complications in patients with type 2 diabetes (T2DM), with significant implications for vision and quality of life. While classical screening methods are effective, they are not always accessible or systematically used. Sudoscan, a device that evaluates sweat gland function by measuring electrochemical skin conductance (ESC)—an indicator of chloride ion flow through sweat glands and a marker of peripheral autonomic nerve function—has recently attracted attention as a potential adjunct tool for risk assessment of microvascular complications. Objectives: In this cross-sectional study, we investigated its utility in identifying DR among 271 adults with T2DM. DR was diagnosed in 35.8% of patients, and those affected showed lower Sudoscan scores in the lower limbs and higher scores indicating cardiovascular autonomic neuropathy. Methods: Statistical analyses, including ROC curve evaluation and multiple linear regression, revealed moderate diagnostic accuracy and significant correlations between Sudoscan parameters and DR severity. Results: Our results suggest that Sudoscan could serve as a fast, painless, and informative screening tool, particularly valuable in settings with limited access to ophthalmologic services. Conclusions: Although it does not replace fundus examination, it may offer complementary insights and help stratify patients by risk level, guiding more targeted monitoring and intervention strategies.
Full article
(This article belongs to the Special Issue New Perspectives and Future Challenges in Diabetic Retinopathy)
►▼
Show Figures

Figure 1
Open AccessArticle
Absence of Tendon Reflexes as a Predictor of Diabetic Retinopathy: A Retrospective Cohort Study in Japan
by
Taichi Muramatsu, Ayaka Sugiura, Daisuke Yamamuro, Ryosuke Kumazawa, Manabu Akazawa, Akifumi Kushiyama and Takako Kikuchi
Diabetology 2026, 7(4), 62; https://doi.org/10.3390/diabetology7040062 - 25 Mar 2026
Abstract
Background/Objective: This study investigated the association between tendon reflexes (Achilles and patellar) and the development of diabetic retinopathy (DR) in patients with type 2 diabetes (T2D). Methods: This single-center retrospective cohort study enrolled patients with T2D. The primary outcome was the
[...] Read more.
Background/Objective: This study investigated the association between tendon reflexes (Achilles and patellar) and the development of diabetic retinopathy (DR) in patients with type 2 diabetes (T2D). Methods: This single-center retrospective cohort study enrolled patients with T2D. The primary outcome was the development of DR. Tendon reflex findings were classified into four groups (normal, decreased, absent, and not examined). A regression analysis using a Cox proportional hazard model was performed to evaluate the association between tendon reflex findings and the outcome. Results: A total of 1172 patients were included in the primary outcome analysis. The median follow-up period was 4.3 years, and 271 experienced DR development. In the multivariate analysis, an absent Achilles tendon reflex (hazard ratio [HR], 1.52; 95% confidence interval [CI]: 1.01–2.27) and an absent patellar tendon reflex (HR: 1.89, 95% CI: 1.18–3.03) were independently associated with DR development. Conclusions: The absence of the Achilles and patellar tendon reflexes may serve as risk markers for DR development. Clinical Practice Implications: Non-invasive assessment of tendon reflexes may serve as an adjunctive tool to identify patients with T2D at high risk for future DR, enabling timely ophthalmologic referral and targeted management.
Full article
(This article belongs to the Special Issue New Perspectives and Future Challenges in Diabetic Retinopathy)
►▼
Show Figures

Figure 1
Highly Accessed Articles
Latest Books
E-Mail Alert
News
Topics
Topic in
Biomolecules, Diabetology, IJMS, JCM, Metabolites, Nutrients
Diabetes and Obesity Under Environmental Stressors: Mechanisms and Clinical Implications
Topic Editors: Ioanna Eleftheriadou, Dimitris KounatidisDeadline: 31 March 2027
Topic in
Antibiotics, Diabetology, JAPMA, JCM, Medicina
Diabetic Foot Disease: Current Challenges, Emerging Concepts and Future Directions
Topic Editors: José Luis Lázaro-Martínez, Marco Meloni, Prashanth VasDeadline: 31 March 2028

Special Issues
Special Issue in
Diabetology
Beta-Cell Failure and Death: A Cornerstone in Diabetes Pathogenesis
Guest Editor: Mourad FerdaoussiDeadline: 29 April 2026
Special Issue in
Diabetology
Insulin Therapy: New Technologies and Future Perspectives
Guest Editor: Betul HatipogluDeadline: 20 May 2026
Special Issue in
Diabetology
Treatment of Type 1 Diabetes: Transplantation of Insulin Producing Cells
Guest Editor: Naoaki SakataDeadline: 20 May 2026
Special Issue in
Diabetology
Advances in Sleep Disorders in Patients with Diabetes
Guest Editor: Stephanie A. GriggsDeadline: 20 May 2026









