-
 Diffusion Tensor Imaging and Advanced Diffusion Imaging in Post-Stroke Aphasia Recovery
Diffusion Tensor Imaging and Advanced Diffusion Imaging in Post-Stroke Aphasia Recovery -
 Cancer-Associated Fibroblasts: Clinical Applications in Imaging and Therapy
Cancer-Associated Fibroblasts: Clinical Applications in Imaging and Therapy -
 Overestimation of the Apparent Diffusion Coefficient in Diffusion-Weighted Imaging Due to Residual Fat Signal and Out-of-Phase Conditions
Overestimation of the Apparent Diffusion Coefficient in Diffusion-Weighted Imaging Due to Residual Fat Signal and Out-of-Phase Conditions -
 Quantitative Magnetic Resonance Imaging of the Forearm in Myotonic Dystrophy Type 1
Quantitative Magnetic Resonance Imaging of the Forearm in Myotonic Dystrophy Type 1
Journal Description
Tomography
Tomography
is an international, peer-reviewed open access journal on imaging technologies published monthly online by MDPI (from Volume 7, Issue 1 - 2021).
- Open Access— free for readers, with article processing charges (APC) paid by authors or their institutions.
- High Visibility: indexed within Scopus, SCIE (Web of Science), PubMed, MEDLINE, PMC, and other databases.
- Journal Rank: JCR - Q2 (Radiology, Nuclear Medicine and Medical Imaging)
- Rapid Publication: manuscripts are peer-reviewed and a first decision is provided to authors approximately 26.3 days after submission; acceptance to publication is undertaken in 4.1 days (median values for papers published in this journal in the second half of 2025).
- Recognition of Reviewers: APC discount vouchers, optional signed peer review, and reviewer names published annually in the journal.
Impact Factor:
2.2 (2024);
5-Year Impact Factor:
2.2 (2024)
Latest Articles
Association Between Regional Cardiac Radiation Dose and Magnetic Resonance Imaging Myocardial Contractility Parameters: A Prospective Pilot Study
Tomography 2026, 12(5), 70; https://doi.org/10.3390/tomography12050070 (registering DOI) - 12 May 2026
Abstract
Background/Objectives: Magnetic resonance imaging (MRI) provides a non-invasive means for a comprehensive assessment of the effect of radiation therapy (RT) on heart function. This study aims to determine RT induced cardiotoxicity in thoracic cancer patients using cardiac MRI. Methods: Cardiac MRI was performed
[...] Read more.
Background/Objectives: Magnetic resonance imaging (MRI) provides a non-invasive means for a comprehensive assessment of the effect of radiation therapy (RT) on heart function. This study aims to determine RT induced cardiotoxicity in thoracic cancer patients using cardiac MRI. Methods: Cardiac MRI was performed at baseline and at six months post-treatment in patients undergoing standard-of-care RT for lung or esophageal cancers at a single institution. Parameters included regional myocardial strain in the longitudinal, circumferential, and radial directions as well as myocardium T1, T2, and extracellular-volume (ECV) maps. Cardiac segmental doses were extracted from the RT planning scans. The relationship between changes in segmental MRI parameters at six months and segmental heart RT dose were investigated. Results: Twelve patients underwent baseline MRI and four completed the follow-up MRI. Five of the segmental strain parameters showed notable changes between baseline and six-month follow-up. Increased doses in the heart base and apex were associated with moderate-to-large and mild deteriorations, respectively, in strain for all regions. Increased doses in the mid-ventricular regions were associated with improved strain in all regions. The segmental analysis revealed that myocardial regions nurtured by the left coronary artery are more negatively affected by radiation compared to those nurtured by the right coronary artery. Conclusions: Alterations in regional tissue and strain parameters on MRI vary according to local myocardial RT dose, suggesting there may be heterogeneity of radiation sensitivity for the heart substructures and regions. Changes in segmental strain parameters may reflect post-RT cardiac remodeling, but larger confirmatory studies are required.
Full article
(This article belongs to the Section Cardiovascular Imaging)
Open AccessReview
Beyond Angiography: Cardiac CT for Planning Complex PCI in Calcified Coronary Lesions
by
Kenji Sadamatsu, Kazumasa Kurogi, Yasuhiro Nakano and Takashi Kajiya
Tomography 2026, 12(5), 69; https://doi.org/10.3390/tomography12050069 (registering DOI) - 12 May 2026
Abstract
Coronary artery calcification, present in 20–30% of percutaneous coronary interventions (PCI), significantly impairs procedural success. Conventional angiography detects calcification in fewer than half of affected cases, while intravascular imaging—though precise—requires lesion crossability that cannot be guaranteed in up to 20% of severely calcified
[...] Read more.
Coronary artery calcification, present in 20–30% of percutaneous coronary interventions (PCI), significantly impairs procedural success. Conventional angiography detects calcification in fewer than half of affected cases, while intravascular imaging—though precise—requires lesion crossability that cannot be guaranteed in up to 20% of severely calcified lesions. Cardiac CT (CCT) addresses both constraints by providing comprehensive, three-dimensional calcium characterization before the procedure begins, independent of wire crossability. This review details how specific CCT-derived parameters translate into procedural decisions. Calcium arc, depth, density, and longitudinal distribution each carry distinct implications for device selection: superficial high-density calcium favors atherectomy, while deep concentric patterns are better addressed by intravascular lithotripsy. Validated scoring systems—including the ABCD score—enable objective pre-procedural risk stratification. For chronic total occlusions, bifurcation lesions, ostial stenoses, and very long calcified segments, CCT provides lesion-specific information that supports stepwise strategy selection, equipment preparation, and anticipation of combined modification approaches. Importantly, CCT also identifies anatomical configurations—such as left main bifurcations or tortuous calcified segments—where specific device-related risks warrant particular caution. CCT and intravascular imaging serve complementary roles: CCT defines the strategic framework before the procedure, while intravascular imaging guides real-time execution and optimization. Limitations include operator-dependent interpretation, the absence of standardized protocols for translating calcium morphology into device selection, and the need to validate established Hounsfield unit thresholds in emerging photon-counting CT systems. Prospective randomized evidence comparing CCT-guided and intravascular imaging-guided strategies remains limited but is anticipated from ongoing trials.
Full article
(This article belongs to the Special Issue Celebrate the 10th Anniversary of Tomography)
►▼
Show Figures
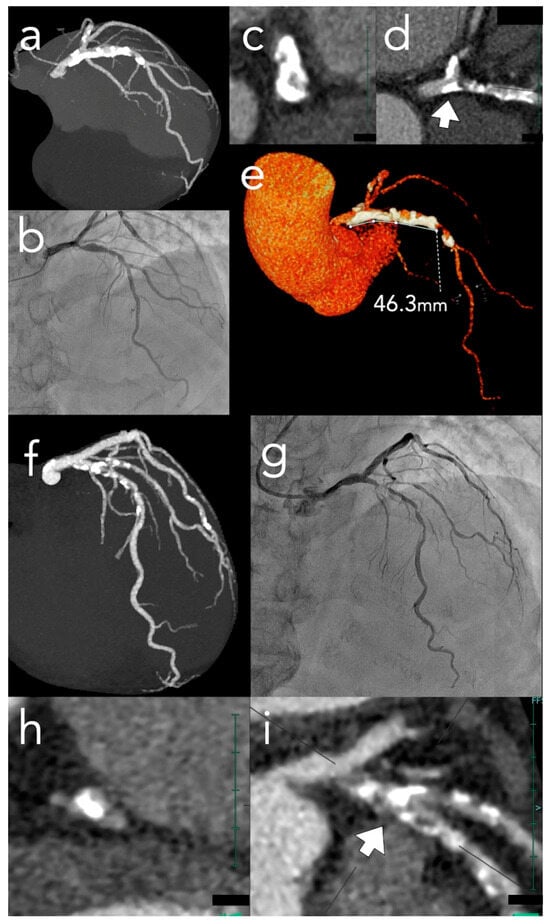
Figure 1
Open AccessArticle
Differentiation of Adrenal Adenomas from Non-Adenomatous Lesions: Diagnostic Value of Unenhanced Spectral CT
by
Tommasa Catania, Grazia Morabito, Simone Barbera, Massimo Venturini, Federico Fontana, Eduardo Maccarrone, Grazia Maria Arillotta, Velio Ascenti, Silvio Mazziotti, Thomas Joseph Vogl, Giovanni Foti, Tommaso D’Angelo and Giorgio Ascenti
Tomography 2026, 12(5), 68; https://doi.org/10.3390/tomography12050068 (registering DOI) - 12 May 2026
Abstract
►▼
Show Figures
Background: Differentiating adrenal adenomas from non-adenomatous lesions remains a critical challenge in the management of adrenal incidentalomas. Conventional unenhanced CT relies on attenuation thresholds of 10 HU and 20 HU, which present trade-offs between sensitivity and specificity. Objectives: To evaluate the diagnostic performance
[...] Read more.
Background: Differentiating adrenal adenomas from non-adenomatous lesions remains a critical challenge in the management of adrenal incidentalomas. Conventional unenhanced CT relies on attenuation thresholds of 10 HU and 20 HU, which present trade-offs between sensitivity and specificity. Objectives: To evaluate the diagnostic performance of unenhanced Spectral CT using the attenuation difference between 40 keV and 140 keV virtual monoenergetic images for differentiating adrenal adenomas from non-adenomatous lesions. Methods: In this retrospective single-center study, 60 patients with adrenal lesions who underwent unenhanced dual-energy CT were included. Mean attenuation values were measured on conventional images and on virtual monoenergetic images at 40 keV and 140 keV. The spectral attenuation difference (Δ40–140 keV) was calculated. ROC analysis was performed to determine the optimal threshold and diagnostic performance. Additional analyses included DeLong comparison of correlated ROC curves and bootstrap resampling to estimate 95% confidence intervals for the area under the curve. Results: Forty-nine lesions were adenomas and eleven were non-adenomatous. The optimal threshold for Δ40–140 keV was −17 HU. When evaluated as a continuous variable, Δ40–140 keV yielded an area under the curve of 0.940 (95% confidence interval: 0.851–1.000), compared with 0.939 (95% confidence interval: 0.870–0.992) for conventional unenhanced attenuation. DeLong comparison showed no statistically significant difference between the two curves (p = 0.980). Diagnostic performance was as follows: HU ≤ 10 (AUC 0.816, diagnostic accuracy 0.70), HU ≤ 20 (AUC 0.883, diagnostic accuracy 0.87), and Δ40–140 keV ≤ −17 HU (AUC 0.940, diagnostic accuracy 0.90). The spectral attenuation difference demonstrated the highest overall diagnostic accuracy. Conclusions: Unenhanced Spectral CT using Δ40–140 keV improves discrimination between adrenal adenomas and non-adenomatous lesions compared with conventional attenuation thresholds. This technique may reduce indeterminate findings and limit the need for additional imaging.
Full article
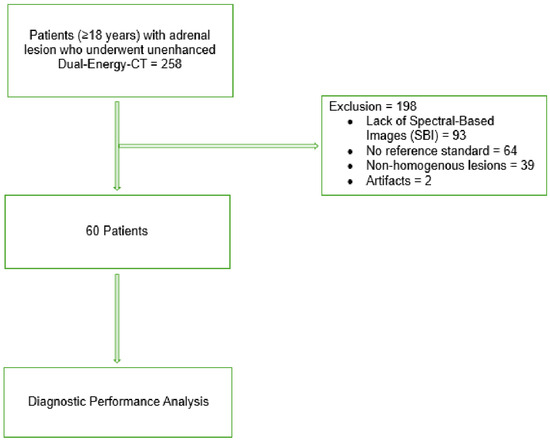
Figure 1
Open AccessArticle
Computed Tomography Versus Pathologic Tumor Size in Resected Lung Tumors: High Correlation, Limited Agreement, and the Impact of Ground-Glass Opacity
by
Omer Yavuz, Reyhan Ertan, Muhammet Kertmen and Mehlika Iscan
Tomography 2026, 12(5), 67; https://doi.org/10.3390/tomography12050067 (registering DOI) - 11 May 2026
Abstract
Background: Computed tomography (CT) is routinely used to estimate tumor size before lung resection, whereas pathologic examination provides the reference tissue-based measurement after surgery. This study aimed to compare CT-derived and pathologic tumor size and to evaluate correlation, agreement, proportional bias, clinically defined
[...] Read more.
Background: Computed tomography (CT) is routinely used to estimate tumor size before lung resection, whereas pathologic examination provides the reference tissue-based measurement after surgery. This study aimed to compare CT-derived and pathologic tumor size and to evaluate correlation, agreement, proportional bias, clinically defined accuracy, and size-based T-category concordance, with particular attention to the effect of ground-glass opacity (GGO). Methods: This retrospective single-center study included 96 patients who underwent lung resection between January 2023 and December 2025 and had complete preoperative CT and pathologic tumor measurements. Maximum tumor diameter was defined as the largest of three orthogonal measurements for each modality. Correlation was assessed using Spearman’s rank correlation coefficient, reliability using the intraclass correlation coefficient (ICC), and agreement using Bland–Altman analysis. Proportional bias was evaluated by regression of the paired difference on the paired mean. Subgroup, size category, regression and size-based T-category concordance analyses were also performed. Results: CT and pathologic maximum diameters showed strong correlation (Spearman’s ρ = 0.952, p < 0.0001) and excellent reliability (ICC = 0.959, 95% CI, 0.939–0.973). The paired comparison was not statistically significant (p = 0.175), and the mean bias was −0.76 mm. However, the 95% limits of agreement ranged from −13.66 mm to +12.13 mm. Significant proportional bias was observed, with increasing CT underestimation as tumor size increased (slope = −0.093, p = 0.0014). In tumors with GGO, CT pathology differences shifted toward overestimation (+8.91 ± 7.30 mm vs. −1.64 ± 5.80 mm without GGO; p = 0.0003). Accuracy within ±5 mm and ±10 mm was 68.8% and 88.5%, respectively, but was lower in the GGO subgroup. CT-derived and pathology-derived size-based T-categories were concordant in 60 patients (62.5%), while pathology-based upstaging occurred in 23 patients (24.0%) and pathology-based downstaging in 13 patients (13.5%). Conclusions: CT-based tumor size showed strong overall correlation with pathologic measurements, but agreement at the individual patient level was more limited than correlation metrics alone would suggest. GGO and tumor size appeared to be important modifiers of measurement performance; however, the GGO-related findings should be interpreted cautiously because of the small subgroup size. These findings support cautious interpretation of CT-derived whole-lesion diameter, particularly in subsolid tumors and larger lesions.
Full article
(This article belongs to the Special Issue Imaging in Cancer Diagnosis)
Open AccessReview
Fluoroscopy-Guided Motion Management in Particle Therapy: Evolution, Challenges, and AI-Enabled Opportunities
by
Feifei Li, Keith M. Furutani and Chris J. Beltran
Tomography 2026, 12(5), 66; https://doi.org/10.3390/tomography12050066 (registering DOI) - 9 May 2026
Abstract
The sharp dose gradients that underpin the dosimetric advantage of particle therapy over photon therapy can be undermined by the interplay effects due to intra-fraction motion in modern pencil beam scanning systems. Fluoroscopy-Guided Particle Therapy (FGPT) offers a promising path to improved motion
[...] Read more.
The sharp dose gradients that underpin the dosimetric advantage of particle therapy over photon therapy can be undermined by the interplay effects due to intra-fraction motion in modern pencil beam scanning systems. Fluoroscopy-Guided Particle Therapy (FGPT) offers a promising path to improved motion management through real-time tracking of tumors or surrogate signals. The advent of flat-panel detector (FPD)-based technology has enabled tighter integration of fluoroscopy/fluorography into treatment units and accelerated clinical adoption and research, with commercial systems such as Hitachi’s Real-time Gated Particle Therapy (RGPT) now available. However, the need for implanted fiducial markers, with the associated invasiveness and risk of complications, limits the utility of RGPT to a few anatomic sites in selected patients. The full potential of FGPT, therefore, depends on reliable marker-less tumor tracking, which remains challenging because soft-tissue targets are obscured by overlapping anatomy along the X-ray path, leading to reduced reliability of traditional image-registration algorithms in the projection domain. Recent advances in deep learning and AI-driven image registration have renewed hope for overcoming these barriers, enabling real-time marker-less tracking for particle therapy. This review outlines the evolution of fluoroscopy technology from image intensifier (II) to FPD-based systems, summarizes historical and recent vendor-supported FGPT strategies, and surveys emerging AI-based algorithms in the literature. A general review of machine learning-based image registration is provided, challenges in generalizability and interpretability are highlighted, and potential paths toward reliable, clinically deployable FGPT are discussed.
Full article
(This article belongs to the Special Issue Progress in the Use of Advanced Imaging for Radiation Oncology)
Open AccessSystematic Review
Quantitative Consistency of Amide Proton Transfer-Weighted MRI for Brain Tumor Differentiation: Systematic Review of Clinical Evidence
by
Julius Juhyun Chung, Tianwen Ma, Phaethon Philbrook, Toby Zhou, Adam Ezra Goldman-Yassen and Phillip Zhe Sun
Tomography 2026, 12(5), 65; https://doi.org/10.3390/tomography12050065 - 6 May 2026
Abstract
Background/Objectives: Accurate grading of brain gliomas is important, and amide proton transfer-weighted (APTw) MRI shows promise for non-invasive tumor differentiation. This study aimed to perform a comprehensive review and meta-analyses to demonstrate heterogeneity in both the diagnostic accuracy and quantitative consistency of APTw
[...] Read more.
Background/Objectives: Accurate grading of brain gliomas is important, and amide proton transfer-weighted (APTw) MRI shows promise for non-invasive tumor differentiation. This study aimed to perform a comprehensive review and meta-analyses to demonstrate heterogeneity in both the diagnostic accuracy and quantitative consistency of APTw MRI in distinguishing high-grade gliomas (HGGs) from low-grade gliomas (LGGs), highlight issues with reporting standards and identify sources of heterogeneity through meta-regression. Methods: A systematic literature search was conducted between 1 January 2013 and 18 January 2026, following PRISMA guidelines. Peer-reviewed articles in English reporting diagnostic accuracy/contrast values of APTw MRI and study parameters were included. Principal component analysis (PCA) was used to extract the principal components (PCs) of the chemical exchange saturation transfer (CEST) contrast mechanism. Random-effects meta-analyses and univariate meta-regression models using individual CEST parameters and three PCs were performed. Forest plots with pooled estimates were generated. Leave-one-out meta-analysis (LOOMA) and complete case analysis were performed to examine the effects of outliers and missing data, respectively. Results: A total of 31 studies were included. Meta-analyses of the AUC and mean difference demonstrated significant heterogeneity across the studies (I2 = 73.9% & 78.2%, p < 0.001). The mean difference was moderated by one SD within the mean of the readout PC (p = 0.034) and the total PC (p = 0.02). The heterogeneity for the AUC and group mean difference was not substantially reduced by moderating nor LOOMA. The results of the meta-regression using all the data were similar to those using only data with no missing parameters. Conclusions: While APTw MRI shows promise for non-invasively distinguishing glioma grades, substantial heterogeneity in the study parameters limits generalizability. To improve consistency and comparability across studies, full reports of imaging parameters and standardization of APTw protocols are essential.
Full article
(This article belongs to the Special Issue Celebrate the 10th Anniversary of Tomography)
Open AccessSystematic Review
Conditional Diffusion Models for CT Image Synthesis from CBCT: A Systematic Review
by
Alzahra Altalib, Chunhui Li and Alessandro Perelli
Tomography 2026, 12(5), 64; https://doi.org/10.3390/tomography12050064 - 6 May 2026
Abstract
Background: Cone Beam Computed Tomography (CBCT) is widely used in image-guided radiotherapy because it provides on-board volumetric imaging at relatively low doses, but its clinical utility for synthetic CT (sCT) generation remains limited by noise, scatter, artifacts, and reduced Hounsfield Unit (HU) fidelity.
[...] Read more.
Background: Cone Beam Computed Tomography (CBCT) is widely used in image-guided radiotherapy because it provides on-board volumetric imaging at relatively low doses, but its clinical utility for synthetic CT (sCT) generation remains limited by noise, scatter, artifacts, and reduced Hounsfield Unit (HU) fidelity. Conditional diffusion models (CDMs) have recently emerged as a promising alternative to earlier deep learning approaches because their iterative denoising process may better preserve anatomical structure and model uncertainty. Objective: This systematic review evaluates the use of conditional diffusion models for CBCT-to-CT synthesis, with particular attention to architectural strategies, reported quantitative outcomes, and potential clinical relevance. A systematic search was conducted in PubMed, Web of Science, Scopus, IEEE Xplore, and Google Scholar for studies published between 2013 and 2024. Eleven studies met the eligibility criteria and were analyzed to address three questions: (1) Which conditional diffusion strategies have been used? (2) What outcomes have been reported? and (3) What clinical implications have been discussed? Results: Across the included studies, CDMs frequently showed promising image quality performance, especially when incorporating anatomical priors, spatial-frequency guidance, hierarchical refinement, or latent representations. However, the evidence base remains small and highly heterogeneous with respect to anatomy, dimensionality, supervision strategy, and evaluation metrics, limiting the strength of direct comparative claims. The reviewed literature suggests that conditional diffusion models are a promising direction for CBCT-to-CT synthesis, but stronger dose-aware validation, standardized reporting, and broader multicenter evaluation are still needed before routine clinical deployment. This review has been registered with the International Prospective Register of Systematic Reviews (PROSPERO), under registration number CRD42024619240.
Full article
(This article belongs to the Special Issue Celebrate the 10th Anniversary of Tomography)
►▼
Show Figures

Graphical abstract
Open AccessReview
Advances and Challenges in Pharmacokinetic Modeling for PET Imaging: Compartment Models, Input Functions, and Quantitative Techniques
by
James Hao Wang, Meltem Uyanik, Xue Li, Weijie Chen, Zhijin He, Caitlin Randell and Alan McMillan
Tomography 2026, 12(5), 63; https://doi.org/10.3390/tomography12050063 - 28 Apr 2026
Abstract
►▼
Show Figures
Pharmacokinetic modeling in Positron Emission Tomography (PET) imaging has become a cornerstone in cancer research, offering insights into tumor development and progression. These models facilitate the quantification of radiotracer distribution and metabolism, enabling precise measurement of physiological parameters essential for cancer diagnosis, staging,
[...] Read more.
Pharmacokinetic modeling in Positron Emission Tomography (PET) imaging has become a cornerstone in cancer research, offering insights into tumor development and progression. These models facilitate the quantification of radiotracer distribution and metabolism, enabling precise measurement of physiological parameters essential for cancer diagnosis, staging, and treatment monitoring. However, accurate pharmacokinetic modeling depends on reliable input function acquisition and partial volume correction techniques to minimize biases in quantitative PET metrics. This review provides a comprehensive overview of current methodologies and advancements in pharmacokinetic modeling for PET oncology imaging. We discuss techniques for acquiring input functions, including arterial, venous, and image-derived input functions (IDIFs), along with population-based input functions (PBIFs). Their strengths, limitations, and clinical applications are critically evaluated. Additionally, we examine quantitative methods such as partial volume correction (PVC) that mitigate the spatial resolution limitations of PET, improving radiotracer quantification in small or heterogeneous tumors. Furthermore, we explore advanced kinetic modeling techniques, including compartmental models, graphical approaches, and data-driven methods, highlighting recent innovations such as machine learning and Bayesian modeling. Key areas for future research in PET pharmacokinetic modeling include integrating hybrid imaging modalities, developing robust patient-specific input functions, and leveraging machine learning to streamline modeling processes. These advancements aim to enhance the precision and clinical utility of PET imaging in oncology, leading to more personalized cancer treatment strategies.
Full article

Figure 1
Open AccessSystematic Review
The Role of Artificial Intelligence in the Characterization and Outcome Prediction of Prostate Cancer: A Systematic Review
by
Shahd Aljoudi, Aasiya Khan, Iman Dajani, Minatullah Al-Ani, Michael Mina, Dounia Baroudi, Sama Al-Saffar, Souha Aouadi, Tarraf Torfeh, Rabih Hammoud, Noora Al Hammadi and Mohammad S. Yousef
Tomography 2026, 12(5), 62; https://doi.org/10.3390/tomography12050062 - 28 Apr 2026
Abstract
Background/Objectives: Prostate cancer (PCa) is the second most commonly diagnosed cancer in men globally. Radiation oncologists often find PCa tumor characterization and outcome prediction challenging. Therefore, the potential for artificial intelligence (AI) implementation in radiation oncology has increased in recent years. This systematic
[...] Read more.
Background/Objectives: Prostate cancer (PCa) is the second most commonly diagnosed cancer in men globally. Radiation oncologists often find PCa tumor characterization and outcome prediction challenging. Therefore, the potential for artificial intelligence (AI) implementation in radiation oncology has increased in recent years. This systematic review aims to evaluate the efficacy of AI algorithms in characterizing PCa tumors and predicting post-therapy outcomes. Methods: A total of 2055 studies were identified through a comprehensive search across PubMed and Scopus, then exported to Covidence. Inclusion criteria focused on prospective and retrospective cohort studies as well as randomized clinical trials (RCTs) published between 2015 and 2024 that explored the implementation of AI in tumor characterization and outcome prediction of PCa. Two independent reviewers evaluated each paper, and evaluation metrics such as specificity, sensitivity, accuracy, and area under the curve (AUC) were analyzed. The Risk of Bias in Non-randomized Studies of Interventions, Version 2 (ROBINS-I V2) tool was used to assess the risk of bias (ROB). Results: Across the 19 studies analyzed, there was no significant difference in model performance between machine learning (ML) and deep learning (DL) models. AI models using multi-input strategies (e.g., radiomics with clinical markers) generally performed better than single-input models. Of the imaging modalities used for radiomic feature extraction, multiparametric MRI (mpMRI)-trained AI models consistently achieved the highest performance. Conclusions: AI displays considerable potential for integration into clinical workflows for PCa management. However, further studies utilizing larger datasets and external cohorts independent of the sample population are needed to validate clinical utility and improve model transparency for reliable implementation.
Full article
(This article belongs to the Section Artificial Intelligence in Medical Imaging)
►▼
Show Figures

Figure 1
Open AccessArticle
AI-Driven Prediction of Chest CT Radiation Doses: Establishing BMI-Based Diagnostic Reference Levels and Patient–Factor Correlations for Machine-Learning Models
by
Zuhal Y. Hamd, Mohamed Abuzaid, Mohamed Alharbi, Nissren Tamam, Amal I. Alorainy, Lena Alrujaee, Najla Almutairi and Aljouharah Abdullah Alyagoub
Tomography 2026, 12(5), 61; https://doi.org/10.3390/tomography12050061 - 28 Apr 2026
Abstract
Background and aim: Chest CT is a major contributor to population radiation exposure. Conventional, pooled diagnostic reference levels (DRLs) do not account for inter-individual variability in body habitus and are typically used retrospectively. We evaluated dose behavior in adult chest CT, derived BMI-stratified
[...] Read more.
Background and aim: Chest CT is a major contributor to population radiation exposure. Conventional, pooled diagnostic reference levels (DRLs) do not account for inter-individual variability in body habitus and are typically used retrospectively. We evaluated dose behavior in adult chest CT, derived BMI-stratified local DRLs, and developed models to enable AI-assisted, prescan dose prediction. Methods: Consecutive adult chest CT examinations from a single center were analyzed. Dose indices (CTDIvol, DLP) and patient factors (BMI, weight, height, age, sex; scan length and planned technical parameters where available) were extracted. DRLs were defined as the 75th percentile overall and within BMI categories (underweight, normal, overweight, and obese). Group differences were assessed using non-parametric tests; associations were examined using correlation analysis. Supervised learning (e.g., Random Forest, Gradient Boosting) was trained to predict CTDIvol and DLP from routinely available variables. Results: BMI-stratified DRLs increased monotonically with habitus: underweight 444.95 mGy·cm/9.60 mGy; normal 513.00/11.55; overweight 756.08/14.65; obese 931.60/20.25 (DLP/CTDIvol). Differences across BMI groups were significant for DLP (H = 31.53, p < 0.001) and CTDIvol (H = 33.61, p < 0.001). DLP correlated moderately with weight and BMI (r ≈ 0.54–0.56, p < 0.001), with a weaker association for age; height was not a meaningful predictor. No sex-based differences in CTDIvol or DLP were observed. Predictive models estimated CTDIvol and DLP with high performance (R2 up to ~0.79 and ~0.77, respectively), enabling comparison of predicted dose against BMI-matched DRLs before acquisition. Conclusions: Size-aware, BMI-stratified DRLs provide clinically interpretable investigation levels that avoid pitfalls of pooled benchmarks. Coupled with robust prediction of individualized dose from routine variables, this framework supports a shift from retrospective audit to prospective, point-of-care dose governance and protocol optimization in chest CT.
Full article
(This article belongs to the Special Issue Cutting-Edge Applications: Artificial Intelligence and Deep Learning Revolutionizing CT and MRI)
►▼
Show Figures

Figure 1
Open AccessArticle
Imaging of Artificial Tumor Models in an Anatomical Breast Phantom with a Single-Sided Magnetic Particle Imaging Scanner
by
Christopher McDonough, John Chrisekos, Matthew Jurj, Alycen Wiacek and Alexey Tonyushkin
Tomography 2026, 12(5), 60; https://doi.org/10.3390/tomography12050060 - 24 Apr 2026
Abstract
Background: Magnetic Particle Imaging (MPI) is an emerging biomedical imaging modality that detects superparamagnetic iron oxide nanoparticles (SPIONs), providing high contrast, sensitivity, and quantification capabilities without ionizing radiation, making it particularly suitable for cancer diagnostics. Considerable engineering efforts are underway to translate MPI
[...] Read more.
Background: Magnetic Particle Imaging (MPI) is an emerging biomedical imaging modality that detects superparamagnetic iron oxide nanoparticles (SPIONs), providing high contrast, sensitivity, and quantification capabilities without ionizing radiation, making it particularly suitable for cancer diagnostics. Considerable engineering efforts are underway to translate MPI technology to clinical settings. Most of these MPI scanners feature a cylindrical bore geometry similar to that of other clinical imaging modalities, which limits their potential application primarily to head scanning. Methods: We have developed a single-sided MPI scanner designed to expand the modality’s applicability to other regions of the human body through a unique hardware design developed in our previous work. Imaging experiments were performed on an anatomical breast phantom containing implanted SPION point sources placed at anatomically plausible locations for breast tumors. These point sources served as artificial tumors for evaluating the system’s suitability for breast imaging applications. Results: The scanner successfully detected and clearly resolved the implanted SPION tumors in two orthogonal imaging planes. Tumor positioning was independently validated by ultrasound imaging, confirming MPI’s accurate localization. In addition, sensitivity measurements demonstrated a detection limit of 4.0
(This article belongs to the Section Cancer Imaging)
►▼
Show Figures

Figure 1
Open AccessArticle
Feasibility and Reliability of an Automated Muscle Segmentation Pipeline Linking Thoracic Supine Kyphosis and Trunk Muscle–Fat% on CT
by
Tianxi Liang, Rian Atri, Sarah Joseph, Yiyuan Shao, Zhitong Zou, Adrian J. Villanueva, Aida Y. Prince, Renke Deng, Kurt Teichman, Xinzi He and Martin R. Prince
Tomography 2026, 12(5), 59; https://doi.org/10.3390/tomography12050059 (registering DOI) - 23 Apr 2026
Abstract
Background: As muscles atrophy, myocytes are replaced by fat and muscle strength diminishes, increasing thoracic supine kyphosis. Here, we investigate the relationship between muscle fat percentage (muscle–fat%) and thoracic supine kyphosis on CT. Methods: Thoracic Cobb angle was measured on supine CT scans
[...] Read more.
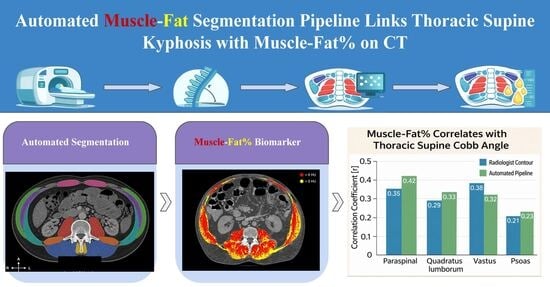
Background: As muscles atrophy, myocytes are replaced by fat and muscle strength diminishes, increasing thoracic supine kyphosis. Here, we investigate the relationship between muscle fat percentage (muscle–fat%) and thoracic supine kyphosis on CT. Methods: Thoracic Cobb angle was measured on supine CT scans from the AtlasDataset by four observers (
(This article belongs to the Section Artificial Intelligence in Medical Imaging)
►▼
Show Figures
Graphical abstract
Open AccessArticle
Utility of Native T1 Mapping for the Evaluation of Myocardial Iron Overload in Patients with Thalassemia Major
by
Antonio Matteo Amadu, Alessio Contena, Alberto Dessì, Leandra Piscopo, Emma Solinas, Davide Turilli, Salvatore Claudio Fanni, Mariano Scaglione and Salvatore Masala
Tomography 2026, 12(4), 58; https://doi.org/10.3390/tomography12040058 - 14 Apr 2026
Abstract
►▼
Show Figures
Purpose: This study aimed to assess the utility of native T1 mapping for the evaluation of myocardial iron overload in patients with Thalassemia Major. T1 was compared to T2*, which represents the gold standard for iron quantification in the heart and liver.
[...] Read more.
Purpose: This study aimed to assess the utility of native T1 mapping for the evaluation of myocardial iron overload in patients with Thalassemia Major. T1 was compared to T2*, which represents the gold standard for iron quantification in the heart and liver. Methods: Consecutive patients with Thalassemia Major who performed cardiac MRI at the University Hospital of Sassari between 2022 and 2024 were prospectively included. All patients underwent a 1.5 T MRI with the same scanner (Philips Ingenia). T2* and native T1 mapping (MOLLI) sequences were performed in all patients on a mid-ventricular single 8 mm short-axis slice of the left ventricle. A region of interest was manually drawn in the septal wall. A T2* value < 20 ms was considered indicative of significant myocardial iron overload. A normal lower limit value of 990 ms was adopted for native T1 mapping. Results: In total, 100 patients with Thalassemia Major were included (median age, 45 [range, 7–80] years; 55% were male). The median myocardial T2* value was 31.4 (range, 5.1–47) and median T1 was 941 ms (range, 557–1131). A total of 12 patients (12%) exhibited T2* values < 20 ms; the T1 values in these patients (median, 733.8 ms [range, 557–975]) were significantly lower compared to those with a T2* of 20 ms or greater (median, 961 ms [range, 820–1131]), p < 0.001. No patient with T2* < 20 ms had a T1 value greater than or equal to 990 ms. Among the 88 patients with T2* ≥ 20 ms, 56 (64%) had T1 < 990 ms (median, 939.2 ms [range, 820–986]). Using a T1 threshold of 990 ms, the sensitivity was 100%, but the specificity was only 36%. ROC analysis identified an optimal T1 value of 895.5 ms, corresponding to 92% sensitivity and 100% specificity. Conclusions: Native T1 mapping is highly sensitive for detecting myocardial iron overload in Thalassemia Major, but the standard 990 ms threshold generates many false-positive results. In our cohort, adopting an ROC-optimized threshold of 895.5 ms markedly improved specificity while preserving excellent sensitivity.
Full article

Figure 1
Open AccessReview
Acute Traumatic Aortic Injury: What the Radiologist Needs to Know
by
Kristina Ramirez-Garcia, Catalina Jaramillo, Emma Ferguson, Jason Au, Erika Odisio, Gustavo S. Oderich, Daniel Ocazionez, Cihan Duran and Thanila Macedo
Tomography 2026, 12(4), 57; https://doi.org/10.3390/tomography12040057 - 13 Apr 2026
Abstract
Acute traumatic aortic injury (ATAI) is a rare but life-threatening consequence of blunt trauma that requires prompt diagnosis and accurate imaging assessment. This review presents an imaging-based approach to ATAI, with emphasis on computed tomography angiography (CTA) as the first-line modality for diagnosis,
[...] Read more.
Acute traumatic aortic injury (ATAI) is a rare but life-threatening consequence of blunt trauma that requires prompt diagnosis and accurate imaging assessment. This review presents an imaging-based approach to ATAI, with emphasis on computed tomography angiography (CTA) as the first-line modality for diagnosis, grading, treatment planning, and follow-up. CTA enables the detection of both direct and indirect signs while also allowing for the assessment of lesion severity, extent, and associated findings that may influence management. Familiarity with common mimics and anatomic variants improves diagnostic confidence and helps avoid false positive interpretations. Careful protocol optimization, including multiphasic acquisition, bolus timing, and postprocessing reconstructions, can further enhance image quality and diagnostic performance. Recognition of patient-related and technical CTA artifacts, along with strategies to reduce them, including the selective use of ECG-gated CTA, may further decrease diagnostic uncertainty. We also discuss the complementary roles of emerging CT technologies and magnetic resonance angiography in selected patients. Finally, we review current classification systems, imaging-guided management, post-treatment surveillance, and potential complications. Awareness of ATAI imaging findings, protocol optimization, and diagnostic pitfalls is essential for accurate interpretation and effective multidisciplinary care.
Full article
(This article belongs to the Special Issue Celebrate the 10th Anniversary of Tomography)
►▼
Show Figures

Figure 1
Open AccessArticle
Double Boosting Strategy for Low-Iodine-Dose Dual-Source DECT Follow-Up CT After Intervention with Raw DICOM-Level Deep Learning Iodine Boosting and Low-keV Dual-Energy-Derived Images
by
Tae Young Lee, Jong Hwa Lee, Hoonsub So and Ho Min Jang
Tomography 2026, 12(4), 56; https://doi.org/10.3390/tomography12040056 - 13 Apr 2026
Abstract
Background/Objectives: We aim to evaluate whether digital imaging and communications in medicine (DICOM)-level deep learning-based iodine-boosting applied to dual-source dual-energy computed tomography (DECT) source DICOM improves image quality in low-iodine-dose abdominal DECT in adults undergoing post-procedure follow-up computed tomography (CT). Methods:
[...] Read more.
Background/Objectives: We aim to evaluate whether digital imaging and communications in medicine (DICOM)-level deep learning-based iodine-boosting applied to dual-source dual-energy computed tomography (DECT) source DICOM improves image quality in low-iodine-dose abdominal DECT in adults undergoing post-procedure follow-up computed tomography (CT). Methods: This retrospective study included 43 adults (April–September 2025) who underwent dynamic dual-source DECT using a low-iodine protocol. Three CT reconstructions were compared: mixed images, conventional 50-keV virtual monoenergetic images (VMIs), and 50-keV VMIs generated after applying DICOM-based deep learning iodine-boosting/denoising to the tube-specific dual-energy source DICOM series prior to VMI/iodine-map reconstruction (deep learning-based reconstruction [DLR]-VMI). Iodine material density (IMD) images were compared between the conventional and DLR-processed datasets. Quantitative attenuation and signal-to-noise ratio (SNR) were assessed using paired and repeated-measures tests. Image quality was scored by two readers using a five-point Likert scale. Results: Attenuation varied across CT reconstructions for all regions of interest in both phases (all overall p < 0.001). Liver attenuation increased from 94.9 ± 22.0 Hounsfield units (HU) (VMI) to 114.5 ± 34.6 HU (DLR-VMI) during the arterial phase and from 127.6 ± 25.6 HU to 166.6 ± 39.9 HU during the portal venous phase (both p < 0.001). Liver SNR improved with DLR-VMI compared to VMI (arterial: 9.11 ± 3.62 vs. 6.06 ± 1.90; portal: 12.74 ± 3.56 vs. 7.90 ± 1.82; both p < 0.001). On IMD images, DLR increased HU-equivalent values and liver SNR (arterial: 5.20 ± 2.89 vs. 2.61 ± 1.39; portal: 9.22 ± 2.81 vs. 4.48 ± 1.28; both p < 0.001). Qualitatively, DLR-VMI yielded the highest overall image-quality scores for both reviewers in both phases (Reviewer 1, arterial/portal: 4 (4–5)/5 (4–5); Reviewer 2, arterial/portal: 4 (3–4)/4 (4–4)). DLR also improved the overall image quality of IMD images for both reviewers (all p < 0.001). Conclusions: Raw DICOM-level iodine-boosting DLR applied to dual-source DECT-source DICOM enabled enhanced image quality and improved quantitative and qualitative metrics in low-iodine-dose abdominal DECT.
Full article
(This article belongs to the Section Abdominal Imaging)
►▼
Show Figures

Figure 1
Open AccessArticle
Pericoronary Fat Attenuation Index and MRI-Derived Coronary Flow Reserve: A Comparative Study in Suspected Versus Known Coronary Artery Disease
by
Ryoya Takizawa, Shingo Kato, Sho Kodama, Kazuki Fukui, Ryusuke Sekii, Naofumi Yasuda, Shungo Sawamura, Tae Iwasawa and Daisuke Utsunomiya
Tomography 2026, 12(4), 55; https://doi.org/10.3390/tomography12040055 - 13 Apr 2026
Abstract
Background: The fat attenuation index (FAI) derived from coronary computed tomography angiography (CTA) is an emerging imaging biomarker of perivascular inflammation. Coronary flow reserve (CFR), assessed by phase-contrast (PC) cine cardiac magnetic resonance (CMR) of the coronary sinus, reflects coronary microvascular function. Although
[...] Read more.
Background: The fat attenuation index (FAI) derived from coronary computed tomography angiography (CTA) is an emerging imaging biomarker of perivascular inflammation. Coronary flow reserve (CFR), assessed by phase-contrast (PC) cine cardiac magnetic resonance (CMR) of the coronary sinus, reflects coronary microvascular function. Although FAI has been linked to adverse outcomes in coronary artery disease (CAD), its relationship with CFR across different CAD stages is not well defined. Methods: We retrospectively evaluated 241 patients (mean age 73.4 ± 10.8 years; 149 men [61.8%]) who underwent both coronary CTA and CMR (122 with known CAD and 119 with suspected CAD). FAI was measured in the proximal left anterior descending (LAD), left circumflex (LCX), and right coronary (RCA) arteries. Impaired CFR was defined as <2.0. Univariable and multivariable logistic regression analyses were performed to identify factors associated with impaired CFR. Results: Impaired CFR was observed in 38 of 122 patients (31.1%) with known CAD and 26 of 119 (21.8%) with suspected CAD. Higher LAD-FAI was associated with impaired CFR in both groups: OR 1.06 (95% CI 1.01–1.11; p = 0.018) in known CAD and OR 1.08 (95% CI 1.02–1.15; p = 0.017) in suspected CAD. Correlation analysis also demonstrated an inverse relationship between LAD-FAI and CFR (p < 0.001), and the strength of association was comparable between the two groups. Conclusions: LAD-FAI was associated with impaired CFR in both suspected and known CAD, with comparable strength of association across the two groups. These findings indicate that perivascular inflammation, reflected by FAI, may relate to coronary microvascular dysfunction in different stages of CAD.
Full article
(This article belongs to the Section Cardiovascular Imaging)
►▼
Show Figures

Figure 1
Open AccessArticle
Baseline Body Composition Characteristics and Overall Survival in Young Women with Breast Cancer: Matched Case–Control Study Nested Within a Cohort
by
Aynur Aktas, Diptasree Mukherjee, Danielle Boselli, Brandon N. VanderVeen, Lejla Hadzikadic-Gusic, Rebecca S. Greiner, Michelle L. Wallander, Declan Walsh and Kunal C. Kadakia
Tomography 2026, 12(4), 54; https://doi.org/10.3390/tomography12040054 - 8 Apr 2026
Abstract
Background/Objectives: Young women with breast cancer (aged ≤ 40 years) have distinct prognostic characteristics, yet little is known about how modifiable body composition factors influence outcomes in this age group. This study examined whether CT-derived body composition measures could identify thresholds that predict
[...] Read more.
Background/Objectives: Young women with breast cancer (aged ≤ 40 years) have distinct prognostic characteristics, yet little is known about how modifiable body composition factors influence outcomes in this age group. This study examined whether CT-derived body composition measures could identify thresholds that predict overall survival (OS). Methods: This was a single-center, 10-year, matched case–control study nested within a cohort, utilizing retrospectively collected data. Using an institutional database (2009–2018) and the initial cohort of 112 patients, we performed a subset analysis of patients with stage I–III breast cancer at diagnosis who had available pretreatment CT scans to estimate associations with body composition metrics and OS. The final analytic dataset included 89 individuals (49 survivors and 40 deceased). CT scans at the L3 level were analyzed using Slice-O-Matic software to quantify visceral (VAT), subcutaneous (SAT), intermuscular (IMAT), total adipose tissue (TAT), skeletal muscle density (SMD), skeletal muscle gauge (SMG), and skeletal muscle index (SMI). Cox proportional hazard models determined optimal cutpoints for OS. Multivariable models included adjustments for disease stage and hormone receptor status. Results: The median age was 35 (IQR, 32–38); 47% were White and 37% were Black. The majority (78%) were not Hispanic or Latina. Most (67%) were overweight/obese. Specific thresholds for IMAT index (>2.57), VAT (>31.38), and SMG (<2419.89) were associated with worse survival (all p < 0.05), while no cutpoints were identified for other variables. Conclusions: These findings show that muscle fat infiltration and reduced muscle quality have important prognostic value in young women with breast cancer. Exploratory cutpoints derived from routine staging CT scans may help inform risk stratification and generate hypotheses for targeted nutritional or exercise interventions, but require validation in larger, independent cohorts before clinical application.
Full article
(This article belongs to the Section Cancer Imaging)
►▼
Show Figures

Figure 1
Open AccessArticle
MRI-Based Evaluation of Lumbar Epidural Space Depth and Its Correlation with Anthropometric Factors in Saudi Adults
by
Ilhaam Alsaati, Khaleel Alyahya, Mohammed Alharbi, Zuhal Y. Hamd and Shaden Alhegail
Tomography 2026, 12(4), 53; https://doi.org/10.3390/tomography12040053 - 8 Apr 2026
Abstract
Background: Epidural procedures benefit from a pre-procedural informed estimation of epidural depth, as anticipating the approximate distance can support safer needle placement and reduce technical difficulties during analgesia or anesthesia procedures. The influence of ethnicity has been established across different populations worldwide;
[...] Read more.
Background: Epidural procedures benefit from a pre-procedural informed estimation of epidural depth, as anticipating the approximate distance can support safer needle placement and reduce technical difficulties during analgesia or anesthesia procedures. The influence of ethnicity has been established across different populations worldwide; however, there is a lack of Saudi-specific MRI data on epidural depth among the adult population. Aim of this Study: To measure the skin to epidural space distance (SED) at the lumbar interspaces L3–L4 and L4–L5 in the Saudi adult population using magnetic resonance imaging (MRI) and to examine its correlations with age, sex, height, weight, and body mass index (BMI). Methods: In this retrospective cross-sectional study, sagittal T1-weighted lumbar MRI images of the spine of 169 adult Saudi patients were studied. The age group ranged from 20 to 70 years, with an equal distribution of males and females. The skin to epidural space distance (SED) was measured at the L3–L4 and L4–L5 interspaces, and its correlations with age, sex, height, weight, and BMI were analyzed. Results: The average measurement of skin to epidural space distance (SED) was 59.08 mm in L3–L4, and 63.21 in L4–L5. BMI and weight showed strong positive correlations with SED across both levels. Female sex was associated with longer SED values at L4–L5. There was no significant correlation between SED and age or height of the patients. Conclusions: MRI-based assessment of SED revealed strong correlations with weight and BMI, but no correlation with height, age, and sex. These findings support the individualized estimation of epidural depth and needle length selection to enhance procedural safety and reduce complications.
Full article
(This article belongs to the Special Issue Orthopaedic Radiology: Clinical Diagnosis and Application)
►▼
Show Figures

Figure 1
Open AccessArticle
Radiographic Evaluation of Spinopelvic Sagittal Alignment Anatomy in Juvenile and Adolescent Idiopathic Scoliosis Patients
by
Ozden Bedre Duygu, Figen Govsa, Anil Murat Ozturk and Gokhan Gokmen
Tomography 2026, 12(4), 52; https://doi.org/10.3390/tomography12040052 - 7 Apr 2026
Abstract
Background and Objectives: The association between spinal and pelvic alignment significantly impacts sagittal balance in adults. This study, that is retrospective, aims to investigate sagittal alignment anatomy of the pelvis and spine in juvenile idiopathic scoliosis (JIS) and adolescent idiopathic scoliosis (AIS)
[...] Read more.
Background and Objectives: The association between spinal and pelvic alignment significantly impacts sagittal balance in adults. This study, that is retrospective, aims to investigate sagittal alignment anatomy of the pelvis and spine in juvenile idiopathic scoliosis (JIS) and adolescent idiopathic scoliosis (AIS) patients. Materials and Methods: We evaluated nine sagittal parameters from lateral radiographs of 100 JIS and AIS patients, including thoracic kyphosis (TKA), lumbar lordosis (LLA), pelvic tilt (PTA), pelvic incidence (PIA), spinosacral (SSA), sacral slope (SSLA), C7 tilt angles (C7-TA), sagittal vertical axis length (SVAL), and odontoid process hip axis angle (OPHAA) using the ImageJ program. Participants were classified based on their coronal curve group. Analysis of variance compared parameters between curve groups, and Pearson coefficients assessed the relationship between all parameters (p < 0.05). Results: Female participants had an average age of 13.4, and male participants had an average age of 13.0. Female participants had an average scoliosis degree of 19.3, while male participants had 15.2. PIA, PTA, SSLA, and SSA values were significantly higher in women participants than in men participants (p < 0.05). Additionally, PIA, PTA, SSLA, SSA, and OPHAA values were significantly lower in participants with a lower scoliosis degree (p < 0.05). We observed a moderately positive association between LLA and TKA, PIA, SSA, and C7-TA. There was also a moderate positive association between spinopelvic alignment parameters and the degree of scoliosis in participants. Conclusions: Easily measured values such as PIA, PTA, SSLA, SSA, and OPHAA may be related to severity of vertebral column deformities in patients, making them valuable for monitoring scoliosis patients.
Full article
(This article belongs to the Special Issue Orthopaedic Radiology: Establishing Radiologic Measurements as Diagnostic Tools and Criteria for Treatment)
►▼
Show Figures

Figure 1
Open AccessArticle
Anatomical Variations in Major Abdominal Aortic Branches and Sex-Related Differences: A Large-Scale Analysis of 1174 Patients
by
Oguzhan Tokur and Koray Bingol
Tomography 2026, 12(4), 51; https://doi.org/10.3390/tomography12040051 - 6 Apr 2026
Abstract
Background: This study aims to evaluate the prevalence, spectrum, and coexistence of anatomical variations in the major branches of the abdominal aorta using Multidetector Computed Tomography (MDCT) angiography, with a specific emphasis on analyzing sex-related differences in a large-scale cohort. Methods: A retrospective
[...] Read more.
Background: This study aims to evaluate the prevalence, spectrum, and coexistence of anatomical variations in the major branches of the abdominal aorta using Multidetector Computed Tomography (MDCT) angiography, with a specific emphasis on analyzing sex-related differences in a large-scale cohort. Methods: A retrospective analysis was conducted on 1174 patients (63.8% male, 36.2% female; mean age 60.54) who underwent abdominal CT angiography between January 2023 and June 2024. Images were acquired using a 128-slice MDCT scanner and reconstructed for detailed vascular assessment. Statistical comparisons between genders were performed using Chi-square and Fisher–Freeman–Halton tests, with p < 0.05 considered significant. Results: The celiac trunk (93.3%), superior mesenteric artery (SMA) (97.1%), and inferior mesenteric artery (IMA) (98.5%) predominantly showed classical patterns. However, significant sex-related differences were identified. Females exhibited significantly higher rates of classical patterns for the celiac trunk (96.2% vs. 91.7%), IMA (99.1% vs. 98.1%), right hepatic artery (RHA) (91.5% vs. 82.6%), and left hepatic artery (LHA) (95.8% vs. 85.4%). Conversely, males showed a higher prevalence of complex variations, including replaced/accessory hepatic arteries and the absence of the common hepatic artery. The number of right and left renal arteries was similar between sexes and did not show a significant difference, while horseshoe kidney was detected only in males. Conclusions: Abdominal vascular structures adhere to classical anatomy more frequently in females, while males exhibit greater morphological variability. These findings emphasize the necessity of gender-specific preoperative vascular mapping to optimize surgical outcomes and reduce morbidity.
Full article
(This article belongs to the Section Cardiovascular Imaging)
►▼
Show Figures

Figure 1

Journal Menu
► ▼ Journal Menu-
- Tomography Home
- Aims & Scope
- Editorial Board
- Reviewer Board
- Topical Advisory Panel
- Instructions for Authors
- Special Issues
- Topics
- Sections
- Article Processing Charge
- Indexing & Archiving
- Editor’s Choice Articles
- Most Cited & Viewed
- Journal Statistics
- Journal History
- Journal Awards
- Conferences
- Editorial Office
Journal Browser
► ▼ Journal BrowserHighly Accessed Articles
Latest Books
E-Mail Alert
News
Topics
Topic in
Anatomia, Biomedicines, IJMS, Medicina, Tomography
Human Anatomy and Pathophysiology, 3rd Edition
Topic Editors: Francesco Cappello, Mugurel Constantin RusuDeadline: 31 May 2026
Topic in
Cancers, Radiation, Tomography, Physics, QuBS
Innovations in Physics and Radiobiology Studies of Particle Therapy
Topic Editors: Yidong Yang, Francesco Giuseppe Cordoni, Fada GuanDeadline: 31 August 2026

Conferences
Special Issues
Special Issue in
Tomography
Medical Image Analysis in CT Imaging
Guest Editor: Martin PichotkaDeadline: 31 August 2026
Special Issue in
Tomography
Advances in Low-Dose Tomography
Guest Editor: Tony SvahnDeadline: 21 October 2026
Special Issue in
Tomography
Imaging in Vascular Interventional Radiology
Guest Editors: Mohammad Ghasemi Rad, David Leon, Mohadese AhmadzadeDeadline: 31 December 2026
Special Issue in
Tomography
Orthopaedic Radiology: Establishing Radiologic Measurements as Diagnostic Tools and Criteria for Treatment
Guest Editor: Olumide A. DanisaDeadline: 31 December 2026







