- Systematic Review
Advancing Nasopharyngeal Carcinoma Diagnosis: A Systematic Review of AI-Driven Machine Learning Techniques for CT, MRI, and WSI Imaging in Bioengineering
- Muhammad Kabir Abdullahi,
- Arbab Sufyan Wadood and
- Mohammad Faizal Ahmad Fauzi
- + 2 authors
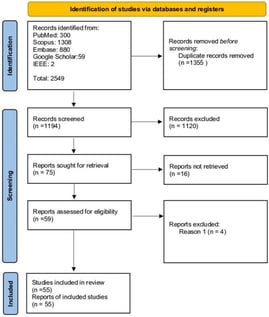
Background: Nasopharyngeal carcinoma (NPC) presents significant diagnostic and therapeutic challenges, often due to late-stage detection and its complex anatomical location. The increasing integration of artificial intelligence (AI) into oncology offers potential opportunities to enhance the precision of NPC management. This systematic review aims to synthesise the current evidence of AI applications in NPC diagnosis, prognostication, and treatment planning. Methods: A systematic literature search was conducted following PRISMA guidelines across multiple databases (PubMed, Scopus, Embase, Google Scholar, IEEE Xplore) for studies published up to June 2025. From an initial pool of 2549 articles, 55 studies meeting the inclusion criteria were selected for qualitative analysis. The review focuses on AI models applied to key diagnostic modalities: computed tomography (CT), magnetic resonance imaging (MRI), and histopathological whole-slide images (WSI). Results: AI, particularly deep learning (DL), shows promising performance in automating critical tasks across all modalities. For CT and MRI, models have been reported to achieve accurate tumor and organ-at-risk segmentation, potentially supporting radiotherapy planning, and show strong performance in predicting survival outcomes and treatment toxicity. In digital pathology, AI enables automated diagnosis and facilitates the extraction of prognostic “pathomic” features from WSIs, with some studies suggesting performance comparable to or exceeding traditional radiomics. The most significant advances are seen in multimodal AI systems that integrate radiological, pathological, and clinical data, which, in some studies, show modest improvements in prognostic performance compared to single-modality approaches. However, these findings are preliminary, as none of the reviewed multimodal models underwent rigorous external validation in large, multi-center cohorts. Reported performance varies considerably across studies, and claims of superiority should be interpreted with caution.
25 May 2026