Journal Description
Infectious Disease Reports
Infectious Disease Reports
is an international, peer-reviewed, open access journal on infectious diseases published bimonthly online by MDPI (since Volume 12, Issue 3 - 2020).
- Open Access— free for readers, with article processing charges (APC) paid by authors or their institutions.
- High Visibility: indexed within Scopus, ESCI (Web of Science), PubMed, PMC, Embase, and other databases.
- Rapid Publication: manuscripts are peer-reviewed and a first decision is provided to authors approximately 34.1 days after submission; acceptance to publication is undertaken in 5.1 days (median values for papers published in this journal in the second half of 2025).
- Journal Rank: CiteScore - Q2 (Infectious Diseases)
- Recognition of Reviewers: APC discount vouchers, optional signed peer review, and reviewer names published annually in the journal.
- Benefits of Publishing: We aim to be a leading journal on infectious diseases and to be in the top 20 journals listed in the Journal Citation Report (JCR) in this specific category in the near future.
Impact Factor:
2.4 (2024);
5-Year Impact Factor:
2.2 (2024)
Latest Articles
Superficial Fungal Infection Associations with Comorbid Diseases and Risk Factors: An Analysis of Global Burden of Disease 2023
Infect. Dis. Rep. 2026, 18(3), 46; https://doi.org/10.3390/idr18030046 (registering DOI) - 12 May 2026
Abstract
Background: Superficial fungal infections caused by dermatophyte and non-dermatophyte species are increasing globally. While several comorbid diseases and risk factors have been associated with fungal infections at the individual level, their epidemiological relationships at the population level remains poorly characterized. Objective: We aimed
[...] Read more.
Background: Superficial fungal infections caused by dermatophyte and non-dermatophyte species are increasing globally. While several comorbid diseases and risk factors have been associated with fungal infections at the individual level, their epidemiological relationships at the population level remains poorly characterized. Objective: We aimed to examine population-level associations between the burden of superficial fungal infections and selected comorbid conditions and risk factors, stratified by age, sex and country. Methods: We obtained years lived with disability (YLDs) for superficial fungal infections, diabetes, psoriasis, and atopic dermatitis and summary exposure values (SEVs) for high body mass index (BMI) and high alcohol intake from Global Burden of Disease Study 2023. Data were obtained for Australia, Brazil, the United Kingdom and the United States for males and females younger than 20 years, 20 to 54 years and 55+ years old. Pearson correlation coefficients were calculated between fungal infection YLDs and each comorbid condition (YLDs) and risk factor (SEVs). Results: Significant positive correlations were observed between superficial fungal infection burden and diabetes (R = 0.6–0.98), high BMI (R = 0.75–0.95), psoriasis (R = 0.59–0.96), and atopic dermatitis (R = 0.51–0.93) in older adults (55 years+). Correlations with high alcohol consumption were more variable across regions and sex. In young–middle-aged adults (20–54 years), moderate-to-strong correlations (R ~ 0.8–0.9) were observed, although patterns were less consistent across countries. In individuals < 20 years, associations were generally weaker, with some positive correlations observed for atopic dermatitis (R = 0.4–0.7) in select countries. Conclusions: The findings demonstrate population-level associations between superficial fungal infections and metabolic, inflammatory, and behavioural risk factors, with stronger correlations observed in older age groups. These patterns may reflect shared demographic, epidemiologic, and clinical patterns across conditions.
Full article
(This article belongs to the Section Fungal Infections)
►
Show Figures
Open AccessArticle
Facility-Level Access Drives Disparities in Influenza and Pneumococcal Vaccination in Long-Term Care Facilities in Southern Poland
by
Zofia Gniadek, Estera Jachowicz-Matczak, Cezary Kapturkiewicz, Izabella Bylica, Dorota Romaniszyn and Jadwiga Wójkowska-Mach
Infect. Dis. Rep. 2026, 18(3), 45; https://doi.org/10.3390/idr18030045 (registering DOI) - 12 May 2026
Abstract
►▼
Show Figures
Background: Vaccinations prevent severe respiratory infections in older adults, yet uptake in Polish long-term care facilities (LTCFs) remains poorly characterized. We assessed influenza and pneumococcal vaccination coverage and factors associated with uptake, including the influence of local government financing. Methods: In this prospective
[...] Read more.
Background: Vaccinations prevent severe respiratory infections in older adults, yet uptake in Polish long-term care facilities (LTCFs) remains poorly characterized. We assessed influenza and pneumococcal vaccination coverage and factors associated with uptake, including the influence of local government financing. Methods: In this prospective observational study (January–June 2022), residents aged ≥65 years from eight LTCFs in southern Poland (four public, four private) were evaluated. Clinical data and geriatric assessments (Barthel Index, ADL, FRAIL-NH) were obtained from medical records and questionnaires. Comparative analyses were limited to residents living in facilities where vaccination activities were implemented and for whom complete data were available. Results: Overall, 429 residents were assessed: 136 (31.7%) received influenza vaccination and 77 (17.9%) received pneumococcal vaccination. Three of the eight LTCFs administered neither influenza nor pneumococcal vaccines, highlighting a facility-level access gap. For individual-level comparisons, 260 residents with complete data from LTCFs offering vaccination were analyzed (245 for pneumococcal outcomes). Influenza vaccination was not associated with most comorbidities or functional measures, but was more common among residents with dementia. Pneumococcal vaccine recipients were younger, had better functional status, and exhibited a lower burden of comorbidities than unvaccinated residents, suggesting preferential vaccination of fitter individuals. Municipality-level data showed low uptake of publicly funded pneumococcal programs (6.1% in Kraków; 3.6% in Wilkowice). Conclusions: Vaccination coverage among LTCF residents was low and strongly influenced by structural access at the facility level. Simplifying costs, reducing out-of-pocket costs and addressing potential age-related biases are essential to improving equitable immunization in Polish LTCFs.
Full article

Figure 1
Open AccessReview
A Risk-Based Isolation Strategy for MDR-Endemic Facilities with Limited Resources
by
Zeynep Ture and Emine Alp
Infect. Dis. Rep. 2026, 18(3), 44; https://doi.org/10.3390/idr18030044 - 9 May 2026
Abstract
Background/Objectives: The increasing burden of multidrug-resistant (MDR) microorganisms and limited resources in healthcare settings are making traditional strategies based on routine isolation of all carriers unsustainable. Methods: A clinical narrative review was conducted by searching PubMed, Web of Science, and Google Scholar for
[...] Read more.
Background/Objectives: The increasing burden of multidrug-resistant (MDR) microorganisms and limited resources in healthcare settings are making traditional strategies based on routine isolation of all carriers unsustainable. Methods: A clinical narrative review was conducted by searching PubMed, Web of Science, and Google Scholar for studies published between 2011 and 2025. International guidelines were analyzed to synthesize a sustainable infection control strategy. Results: High-quality evidence, including cluster-randomized trials, indicates that routine contact isolation for endemic ESBL-producing Enterobacterales (IRR: 0.99) and VRE (RR: 0.93) provides no additional benefit over standard precautions. In contrast, strict isolation remains vital for high-threat pathogens such as Carbapenem-Resistant Enterobacterales (CRE), Acinetobacter baumannii (CRAB), and Candidozyma auris due to their high environmental resilience and limited treatment options. Prioritization should be guided by pathogen biology, patient-specific transmission traits (e.g., diarrhea), and facility infrastructure. Conclusions: Traditional one-size-fits-all infection control is increasingly unsustainable under resource constraints. A risk-based approach prioritizing horizontal measures for low-risk pathogens enables a more balanced allocation of limited resources toward high-threat containment.
Full article
(This article belongs to the Special Issue Prevention, Diagnosis and Treatment of Healthcare-Associated Infections)
►▼
Show Figures

Figure 1
Open AccessArticle
A Real-World Pharmacovigilance Analysis of the Safety Profiles Associated with Anti-MRSA Agents Using the Japanese Adverse Drug Event Report (JADER) Database
by
Yuki Hanai, Shusuke Uekusa, Mizuki Mori, Kohei Shimoyama, Hayato Ohashi, Koji Nishimura, Sachiko Yanagino, Takahiro Matsumoto and Kazuhiro Matsuo
Infect. Dis. Rep. 2026, 18(3), 43; https://doi.org/10.3390/idr18030043 - 2 May 2026
Abstract
Background: Anti-MRSA agents are essential for treating severe infections, yet their use is constrained by distinct toxicity profiles. However, comparative real-world data remain scarce. Methods: This nationwide pharmacovigilance study used the Japanese Adverse Drug Event Report (JADER) database (2004–2025). Disproportionality analyses (proportional reporting
[...] Read more.
Background: Anti-MRSA agents are essential for treating severe infections, yet their use is constrained by distinct toxicity profiles. However, comparative real-world data remain scarce. Methods: This nationwide pharmacovigilance study used the Japanese Adverse Drug Event Report (JADER) database (2004–2025). Disproportionality analyses (proportional reporting ratio [PRR]) were performed at the Standardized MedDRA Query and Preferred Term levels, complemented by Weibull-based time-to-onset modeling, to characterize AE patterns associated with vancomycin (VCM), teicoplanin (TEIC), arbekacin (ABK), daptomycin (DAP), linezolid (LZD), and tedizolid (TZD). Results: Distinct agent-specific AE profiles were observed. VCM showed disproportionate reporting of acute renal failure (PRR 6.66) and severe cutaneous reactions. TEIC displayed fewer renal signals but relatively higher reporting of hematologic events (PRR 3.51). ABK demonstrated high disproportionality in acute and chronic renal failure, reflecting aminoglycoside nephrotoxicity. DAP showed a high reporting signal for eosinophilic pneumonia (PRR 23.30), interstitial lung disease, and creatine kinase elevation/rhabdomyolysis, with wear-out hazard patterns suggesting a possible time-dependent reporting tendency. LZD exhibited hematopoietic signals (PRR 6.13) and additional associations with hyponatremia, lactic acidosis, and optic neuropathy, consistent with marrow suppression and mitochondrial toxicity. Weibull analysis indicated cumulative “wear-out” risks for renal, hepatic, and hematologic events, whereas hypersensitivity and many pulmonary events followed random-failure patterns. Conclusions: This large-scale JADER analysis delineated the distinct safety profiles of the six anti-MRSA agents. The key findings included DAP pulmonary and muscle toxicities, LZD hematological events, and VCM nephrotoxicity. Time-to-onset modeling indicates potential cumulative versus random risk patterns, suggesting the need for individualized monitoring and cross-validation.
Full article
(This article belongs to the Section Bacterial Diseases)
Open AccessArticle
Chromosomal Mechanisms of Colistin Resistance in Clinical Isolates of Carbapenem-Resistant Klebsiella pneumoniae from a Tunisian Tertiary-Care Hospital
by
Zaineb Hamzaoui, Hajer Kilani, Alain Ocampo-Sosa, Sana Ferjani, Elaa Maamar, Lamia Kanzari, Ahmed Fakhfakh, Amel Rehaiem, Luis Martínez-Martínez and Ilhem Boutiba Ben Boubaker
Infect. Dis. Rep. 2026, 18(3), 42; https://doi.org/10.3390/idr18030042 - 1 May 2026
Abstract
Background/Objectives: Carbapenem-resistant Klebsiella pneumoniae (CRKP) is a major nosocomial pathogen. Although newer agents have reduced colistin use in high-income countries, this polymyxin remains important in many low- and middle-income settings. Colistin resistance in K. pneumoniae is most commonly associated with chromosomal alterations affecting
[...] Read more.
Background/Objectives: Carbapenem-resistant Klebsiella pneumoniae (CRKP) is a major nosocomial pathogen. Although newer agents have reduced colistin use in high-income countries, this polymyxin remains important in many low- and middle-income settings. Colistin resistance in K. pneumoniae is most commonly associated with chromosomal alterations affecting the MgrB–PhoPQ pathway, or with plasmid-mediated mcr genes. This study aimed to investigate chromosomally mediated colistin resistance in CRKP clinical isolates from a Tunisian tertiary hospital. Methods: Between 2010 and 2015, 317 non-duplicate CRKP isolates were collected at Charles Nicolle Hospital, Tunis. Colistin MICs were determined by broth microdilution. Phenotypic tests and PCR characterized carbapenemases, extended-spectrum β-lactamases, AmpC, plasmid-mediated quinolone resistance, mcr and virulence genes. Porins (OmpK35/OmpK36) and the mgrB, phoP and phoQ loci were analyzed by SDS-PAGE and sequencing. Clonal relatedness was assessed by ERIC-PCR and multilocus sequence typing. We additionally compared colistin-resistant isolates with a panel of colistin-susceptible CRKP controls and assessed phenotypic stability after serial passages without colistin. Results: Five isolates (1.6%) were colistin-resistant. All were multidrug-resistant, produced OXA-48, and two also carried NDM-1. The isolates belonged to five distinct sequence types, including high-risk clones (ST11, ST101, ST147). No mcr genes were detected. Four isolates carried disruptive mutations in mgrB, and the remaining strain harbored inactivating mutations in both phoP and phoQ with an intact mgrB. Truncating alterations in PhoP/PhoQ and frequent loss or truncation of OmpK35/OmpK36 were observed. No mgrB/phoP/phoQ alterations were detected among colistin-susceptible controls, and colistin MICs remained stable after 7 days of drug-free passaging. Conclusions: In Tunisian CRKP, colistin resistance was associated with chromosomal alterations, predominantly involving disruption of the MgrB–PhoPQ pathway, in the absence of mcr genes. These mechanisms in both high-risk and emerging sequence types underscore the adaptability of CRKP and the need for surveillance where colistin remains an important therapeutic option.
Full article
(This article belongs to the Section Antimicrobial Stewardship and Resistance)
►▼
Show Figures

Figure 1
Open AccessReview
Non-Albicans Candida Peritonitis in Peritoneal Dialysis: Species Distribution, Management, and Outcomes—A Systematic Case-Based Review
by
John Dotis, Athina Papadopoulou, Maria Fourikou, Marianna Papakonstantinou, Ioustini Kalaitzopoulou and Charalampos Antachopoulos
Infect. Dis. Rep. 2026, 18(3), 41; https://doi.org/10.3390/idr18030041 - 27 Apr 2026
Abstract
Background/Objectives: Fungal peritonitis is a severe complication of peritoneal dialysis (PD) associated with catheter removal, technique failure, and increased mortality. Although Candida albicans was traditionally the predominant pathogen, non-albicans Candida (NAC) species are increasingly reported. This review summarizes the epidemiology and outcomes of
[...] Read more.
Background/Objectives: Fungal peritonitis is a severe complication of peritoneal dialysis (PD) associated with catheter removal, technique failure, and increased mortality. Although Candida albicans was traditionally the predominant pathogen, non-albicans Candida (NAC) species are increasingly reported. This review summarizes the epidemiology and outcomes of PD-associated NAC peritonitis. Methods: A systematic review was performed following PRISMA guidelines. PubMed/MEDLINE, Scopus, and Google Scholar were searched (January 1990–March 2026) for NAC peritonitis studies. Case reports and series with species-level identification were included. Results: 31 studies met the inclusion criteria, comprising 25 individual case reports and 6 case series, totaling 89 NAC isolates. Candida parapsilosis was the most frequently reported species (n = 50), followed by Candida tropicalis (n = 15). Other pathogens included Candida glabrata, Candida guilliermondii, and several rare NAC species. Fluconazole was the most commonly used initial antifungal therapy. Catheter removal was performed in most cases, with the majority of patients requiring transition to hemodialysis. Overall mortality was 20% among individual case reports vs. 24% across case series. Species-specific differences were observed: C. parapsilosis and C. guilliermondii were generally associated with favorable outcomes, whereas infections involving C. glabrata and other emerging NAC species more frequently required treatment escalation and were linked to poorer outcomes. Conclusions: NAC species are an important cause of fungal peritonitis in PD patients and show considerable heterogeneity in clinical outcomes and antifungal susceptibility. Early species-level identification and prompt catheter removal remain essential for optimal management.
Full article
(This article belongs to the Section Fungal Infections)
Open AccessEditor’s ChoiceReview
Cardiovascular Manifestations Documented in Patients with Lyme Disease: Clinical Presentation, Management Strategies, and Outcomes
by
Luis Antonio Cortes Islas, Priscila Mishelle Bartolo Gomez, Nora Denice Cuevas Obispo, Ayelen Xicohtencatl Muñoz, Lao Yuling Lopez Lucero and Juan Pablo Ramirez Hinojosa
Infect. Dis. Rep. 2026, 18(3), 40; https://doi.org/10.3390/idr18030040 - 27 Apr 2026
Abstract
Background/Objectives: Lyme disease is a tick-borne zoonosis caused by Borrelia burgdorferi that can affect multiple organ systems. Although cardiovascular involvement is considered uncommon, it may lead to severe and potentially life-threatening complications, particularly conduction disturbances and inflammatory cardiac conditions. This review aims to
[...] Read more.
Background/Objectives: Lyme disease is a tick-borne zoonosis caused by Borrelia burgdorferi that can affect multiple organ systems. Although cardiovascular involvement is considered uncommon, it may lead to severe and potentially life-threatening complications, particularly conduction disturbances and inflammatory cardiac conditions. This review aims to describe the spectrum of cardiovascular manifestations documented in patients with Lyme disease, focusing on clinical presentation, diagnostic approaches, management strategies, and reported outcomes. Methods: A narrative literature review was performed using PubMed, MEDLINE, and Google Scholar. Articles published between January 2000 and July 2025 in English or Spanish were screened. Eligible studies included original research articles, systematic and narrative reviews, case series, and case reports describing confirmed Lyme disease with cardiovascular involvement. A total of 30 studies were included. The available evidence was predominantly based on case reports and small case series, with considerable heterogeneity in study design, patient populations, and reported outcomes. Data on clinical manifestations, diagnostic methods, treatment strategies, and outcomes were extracted and synthesized. Results: Atrioventricular conduction disturbances were the most frequently reported cardiovascular manifestation, ranging from first-degree block to complete heart block, often presenting abruptly with syncope or bradycardia. Other reported manifestations included atrial and ventricular arrhythmias, myocarditis, pericarditis, myopericarditis, valvular endocarditis, aortitis, and vasculitis. Diagnosis relied on a combination of clinical suspicion, epidemiologic exposure, serologic testing, electrocardiographic monitoring, and cardiac imaging. Most patients were treated with antimicrobial therapy, commonly intravenous ceftriaxone followed by oral doxycycline, with temporary pacemaker support required in selected cases. Overall, clinical outcomes were favorable when treatment was initiated promptly. Conclusions: Cardiovascular involvement in Lyme disease, although infrequent, encompasses a broad clinical spectrum with potentially serious consequences. Early recognition, appropriate diagnostic evaluation, and timely antimicrobial therapy are essential to ensure reversibility of cardiac manifestations and favorable outcomes. However, the available evidence is limited by heterogeneity and the predominance of low-level-evidence studies.
Full article
(This article belongs to the Section Bacterial Diseases)
►▼
Show Figures

Figure 1
Open AccessCase Report
Spontaneous Pneumomediastinum, Subcutaneous Emphysema, and Pneumoperitoneum in RT-PCR-Confirmed Measles: A Pediatric Case Report
by
Roberto Miguel Damián-Negrete, Alondra Denisse Hernández-Luna, Rocío Guadalupe Cano-Arias, Antonio Durán-Plaza, Judith Carolina De Arcos-Jiménez, Kathya Analí Rodríguez-González, Braulio Dazahel González-Flores, Pedro Iván Navarro-González and Jaime Briseno-Ramírez
Infect. Dis. Rep. 2026, 18(3), 39; https://doi.org/10.3390/idr18030039 - 24 Apr 2026
Abstract
Measles remains a major global public health challenge as declining vaccination coverage fuels outbreaks worldwide. Although pneumonia is the most recognized respiratory complication, spontaneous air leak syndrome—including pneumomediastinum, subcutaneous emphysema, and pneumoperitoneum—is rarely documented. We report the case of a 9-year-old previously healthy
[...] Read more.
Measles remains a major global public health challenge as declining vaccination coverage fuels outbreaks worldwide. Although pneumonia is the most recognized respiratory complication, spontaneous air leak syndrome—including pneumomediastinum, subcutaneous emphysema, and pneumoperitoneum—is rarely documented. We report the case of a 9-year-old previously healthy girl with no documented measles–rubella vaccination who presented with fever, maculopapular exanthem, Koplik spots, and persistent cough. Measles was confirmed by both immunoglobulin M enzyme-linked immunosorbent assay and real-time reverse transcription polymerase chain reaction. She developed sudden cervicothoracic swelling and chest pain. Chest radiography revealed pneumomediastinum and subcutaneous emphysema; computed tomography confirmed extensive air leak including pneumoperitoneum. Flexible bronchoscopy and upper gastrointestinal endoscopy excluded structural airway and esophageal injury. Laboratory evaluation revealed elevated hepatic transaminases, gamma-glutamyl transferase, lactate dehydrogenase, and D-dimer. Conservative management with high-flow supplemental oxygen and clinical surveillance led to progressive resolution. The patient was discharged on hospital day three, asymptomatic and breathing room air. This case highlights the spectrum of air leak complications in measles and supports conservative management in hemodynamically stable pediatric patients when structural injury has been excluded.
Full article
(This article belongs to the Special Issue Viral Infectious Diseases: Epidemiology and Prevention Through Vaccination)
►▼
Show Figures

Figure 1
Open AccessReview
HBV and the Microbiome—PubMed Database Literature Review
by
Anna Marija Prince, Indra Zeltiņa, Aigars Reinis, Olga Valciņa and Angelika Krūmiņa
Infect. Dis. Rep. 2026, 18(3), 38; https://doi.org/10.3390/idr18030038 - 22 Apr 2026
Abstract
Objective: Hepatitis B virus (HBV) is a globally distributed infectious disease affecting the liver. This literature review aims to summarize all available relevant information on the PubMed database about HBV’s connection to the microbiome and to consider possible treatment adjuncts. Materials and methods:
[...] Read more.
Objective: Hepatitis B virus (HBV) is a globally distributed infectious disease affecting the liver. This literature review aims to summarize all available relevant information on the PubMed database about HBV’s connection to the microbiome and to consider possible treatment adjuncts. Materials and methods: Database used: PubMed. Keywords used: “HBV”, “Hepatitis B”, “microbiome”. In the PubMed database, 179 research publications were identified using these keywords; 69 studies were excluded as they were irrelevant or retracted. Of the remaining, 110 were analyzed in this literature review, and four additional literature sources were used to supply background information and context. Information was summarized. The analysed studies in total included 14,814 participants (excluding animal studies), of whom 8564 were HBV-infected individuals. Results: Results characterizing abundance or decrease in specific bacterial, viral, and fungal species are heterogeneous; multiple studies support that the HBV patient oral and fecal microbiome is different from that in healthy controls (HCs) and varies throughout disease progression. The HBV seems to transform the microbiome negatively, leading to dysbiosis and decreased microbial diversity in most studies. Evidence links HBV microbiome changes with influence on HbeAg seroconversion, HBV-DNA load, metabolic pathways, liver cirrhosis, and hepatocellular carcinoma. The research proposes that members of microbiota could potentially promote or protect against liver injury in HBV. Four studies proposed that the plasma virome in HBV patients was primarily composed of members of the Anelloviridae. One study researched a parasite (Entamoeba gingivalis) in HBV patients. Two studies analyzed HBV patients’ fungal profiles. Conclusions: Microbiota research, although promising, at the present moment is heterogeneous. HBV patients’ microbiota is distinguishable from HCs, and multiple studies have tried to identify the HBV characteristic microbiome; however, more precise information is needed to draw conclusions. Fecal microbiota transplantation and probiotics have the potential to be therapy adjuncts for HBV patients, but more research is needed.
Full article
(This article belongs to the Section Viral Infections)
►▼
Show Figures

Figure 1
Open AccessArticle
Influenza A(H3N2) Subclade K (J.2.4.1): Molecular Characterization, Antigenic Divergence, and Global Spread During the 2025/26 Season
by
Francesco Branda, Nicola Petrosillo, Giancarlo Ceccarelli, Fabio Scarpa, Marta Giovanetti and Massimo Ciccozzi
Infect. Dis. Rep. 2026, 18(2), 37; https://doi.org/10.3390/idr18020037 - 14 Apr 2026
Cited by 1
Abstract
►▼
Show Figures
Background: Influenza A(H3N2) continues to evolve rapidly, frequently eroding population immunity and challenging seasonal vaccine strain selection. During the 2025/26 season, the A(H3N2) subclade K (J.2.4.1) expanded quickly across multiple regions and showed evidence of antigenic divergence in standard assays. Methods: In this
[...] Read more.
Background: Influenza A(H3N2) continues to evolve rapidly, frequently eroding population immunity and challenging seasonal vaccine strain selection. During the 2025/26 season, the A(H3N2) subclade K (J.2.4.1) expanded quickly across multiple regions and showed evidence of antigenic divergence in standard assays. Methods: In this study, we combined phylogenetic analyses of hemagglutinin (HA) and neuraminidase (NA) sequences with a systematic synthesis of recent peer-reviewed studies and official surveillance reports to comprehensively define the molecular profile and early epidemiological dynamics of subclade K. Results: Our phylogenetic reconstructions of HA and NA genes confirmed the emergence of a coherent and recently diversified lineage characterized by coordinated evolution of surface glycoproteins and broad geographic representation during 2025. Integration of molecular, temporal, and surveillance evidence further supported rapid expansion with limited early regional structuring. Antigenic analyses reported in peer-reviewed studies described reduced haemagglutination inhibition reactivity to vaccine reference antisera for many subclade K viruses, whereas vaccine effectiveness (VE) estimates from multiple settings remained moderate. Conclusions: Overall, the available genetic, antigenic, and epidemiological evidence indicates that subclade K represents a recently diversified A(H3N2) lineage associated with rapid international spread during the 2025/26 season, highlighting the importance of integrated HA/NA genomic surveillance and timely antigenic characterization to support evidence-based vaccine strain selection.
Full article

Figure 1
Open AccessEditor’s ChoiceArticle
Trends in Outpatient Antibiotic Prescriptions Issued in Croatian Primary Healthcare, 2015–2024
by
Anamaria Jurčević, Jelena Dimnjaković and Rok Čivljak
Infect. Dis. Rep. 2026, 18(2), 36; https://doi.org/10.3390/idr18020036 - 14 Apr 2026
Abstract
Objectives: Outpatient antibiotic prescribing is a major driver of antimicrobial resistance, yet detailed long-term analyses of prescribing patterns in Croatia remain limited. This study aimed to analyze trends in outpatient antibiotic prescriptions issued in Croatian primary healthcare from 2015 to 2024, stratified by
[...] Read more.
Objectives: Outpatient antibiotic prescribing is a major driver of antimicrobial resistance, yet detailed long-term analyses of prescribing patterns in Croatia remain limited. This study aimed to analyze trends in outpatient antibiotic prescriptions issued in Croatian primary healthcare from 2015 to 2024, stratified by antibiotic class, substance, and the WHO AWaRe classification. Methods: A retrospective analysis of nationwide data on antibiotic prescriptions issued in primary care outpatient settings was conducted using the data from the Central Health Information System of the Republic of Croatia. All prescriptions for ATC group J01 antibiotics issued between 1 January 2015 and 31 December 2024 were included. The primary outcome was the annual number of issued outpatient antibiotic prescriptions, described overall and by substance. Annual counts were additionally expressed as a percentage of the 2015 baseline (index year = 100%) to enable the comparison across substances with different prescribing volumes. The prescriptions were classified according to the WHO AWaRe framework. Results: A total of 31,048,414 outpatient antibiotic prescriptions were issued between 2015 and 2024. Overall prescribing declined by 5.6% from 2015 to 2019, followed by a marked decrease of 21.0% in 2020, and subsequently rebounded to 3,338,235 prescriptions by 2024, a number virtually identical to pre-pandemic levels. Co-amoxiclav and azithromycin together accounted for 49.5% of all prescriptions. By 2024, prescribing third-generation cephalosporins increased by 281.9% compared to the 2015 levels, while prescribing amoxicillin decreased by 43.6% over the same period. The proportion of Access antibiotics declined from 64.7% in 2015 to 57.9% in 2024. Conclusions: The main challenge for antimicrobial stewardship in Croatia lies not only in overall prescribing volume but in prescribing composition. Targeted interventions are needed to reduce reliance on broad-spectrum agents and promote the use of narrower-spectrum first-line alternatives.
Full article
(This article belongs to the Section Antimicrobial Stewardship and Resistance)
►▼
Show Figures

Figure 1
Open AccessArticle
Prevalence of Mycoplasma genitalium and Co-Infections with Chlamydia trachomatis and Neisseria gonorrhoeae Among Japanese Women: A Cross-Sectional Study
by
Hiroshige Mikamo, Yuka Yamagishi and Daisuke Sakanashi
Infect. Dis. Rep. 2026, 18(2), 35; https://doi.org/10.3390/idr18020035 - 13 Apr 2026
Abstract
Background/Objectives: Mycoplasma genitalium is an emerging cause of sexually transmitted infections (STIs) and is increasingly recognized for its association with cervicitis and pelvic inflammatory disease. However, prevalence data in specific Japanese subpopulations, particularly comparing pregnant and non-pregnant women, remains limited. This study
[...] Read more.
Background/Objectives: Mycoplasma genitalium is an emerging cause of sexually transmitted infections (STIs) and is increasingly recognized for its association with cervicitis and pelvic inflammatory disease. However, prevalence data in specific Japanese subpopulations, particularly comparing pregnant and non-pregnant women, remains limited. This study aimed to determine the prevalence of M. genitalium and its co-infection rates with Chlamydia trachomatis and Neisseria gonorrhoeae among Japanese women. Methods: A cross-sectional study was conducted using vaginal swab specimens collected between April 2021 and November 2022 from patients visiting two clinics in Gifu, Japan. The study population comprised 2138 non-pregnant women presenting with urogenital symptoms or sexual contact history, and 236 pregnant women undergoing routine antenatal screening. Detection was performed using real-time polymerase chain reaction assays on the cobas® 8800 system (Roche Diagnostics). Results: Among non-pregnant women, the overall prevalence was 3.8% (82/2138) for M. genitalium, 3.4% (72/2138) for C. trachomatis, and 0.4% (9/2138) for N. gonorrhoeae. Co-infection rates were low; M. genitalium and C. trachomatis co-infection was observed in 0.2% of cases. Among pregnant women, the prevalence was 3.8% (9/236) for both M. genitalium and C. trachomatis, and 0.4% (1/236) for N. gonorrhoeae. No statistically significant differences in prevalence were observed between pregnant and non-pregnant women for any pathogen. Conclusions: The prevalence of M. genitalium in this Japanese cohort was comparable to that of C. trachomatis in both pregnant and non-pregnant women, highlighting its significance as a major STI pathogen. These findings underscore the importance of including M. genitalium in routine STI screening panels for symptomatic women and antenatal care to prevent reproductive health complications. Given the high rates of antimicrobial resistance documented in Japanese M. genitalium strains, specific diagnostic testing is essential to enable targeted, resistance-guided therapy.
Full article
(This article belongs to the Section Sexually Transmitted Diseases)
Open AccessReview
Newer Therapeutics to Selectively Kill Clostridioides difficile and Restore the Microbiome
by
Guido Granata and Nicola Petrosillo
Infect. Dis. Rep. 2026, 18(2), 34; https://doi.org/10.3390/idr18020034 - 11 Apr 2026
Abstract
Background: The antibiotic ibezapolstat and the live biotherapeutic product live-JSLM are promising future approaches for treating Clostridioides difficile infection. Ibezapostat is a highly specific antibiotic for Clostridioides difficile, with minimal impact on the intestinal flora. Live-JSLM is designed to restore healthy intestinal
[...] Read more.
Background: The antibiotic ibezapolstat and the live biotherapeutic product live-JSLM are promising future approaches for treating Clostridioides difficile infection. Ibezapostat is a highly specific antibiotic for Clostridioides difficile, with minimal impact on the intestinal flora. Live-JSLM is designed to restore healthy intestinal microbiota, thus preventing recurrence of Clostridioides difficile infection. In this narrative review, we reviewed available data on ibezapostat and live-JSLM, considering that they are prototypes of two distinct, unique mechanisms of action against Clostridioides difficile. Methods: Data sources: PubMed and SCOPUS databases were searched from 1 January 2012 to 15 November 2025. Original articles reporting data on ibezapolstat and live-JSLM were included. Results: 31 studies were included. When compared to conventional anti-Clostridioides difficile antibiotics, ibezapolstat had a similar level of effectiveness and minimal impact on the gut microbiota. The available data confirm live-JSLM safety and efficacy in restoring the gut microbiota following the conclusion of the standard anti-Clostridioides difficile antibiotic regimen. Conclusions: The results on ibezapolstat efficacy are promising, but require confirmation in larger patient populations through double-blind, randomised phase III trials. In the near future, an integrated approach may enhance the management of Clostridioides difficile infection: starting with highly specific antibiotics, i.e., ibezapolstat, followed by microbiome-based therapies such as live-JSLM.
Full article
(This article belongs to the Section Bacterial Diseases)
Open AccessEditor’s ChoiceCase Report
Progressive Multifocal Leukoencephalopathy in AIDS: The Diagnostic Role of PET Imaging
by
Virginia Donini, Riccardo Paggi, Alberto Farese, Costanza Malcontenti, Enrico Tagliaferri, Claudio Caroselli, Spartaco Sani, Maria Matteini, Alessandro Bartoloni and Lorenzo Zammarchi
Infect. Dis. Rep. 2026, 18(2), 33; https://doi.org/10.3390/idr18020033 - 8 Apr 2026
Abstract
►▼
Show Figures
Introduction: The majority of progressive multifocal leukoencephalopathy (PML) cases is still represented by patients affected by acquired immunodeficiency syndrome (AIDS). Diagnosis of PML relies on histopathological findings or by the combination of clinical signs, radiological evidence, and molecular positivity of the JC virus
[...] Read more.
Introduction: The majority of progressive multifocal leukoencephalopathy (PML) cases is still represented by patients affected by acquired immunodeficiency syndrome (AIDS). Diagnosis of PML relies on histopathological findings or by the combination of clinical signs, radiological evidence, and molecular positivity of the JC virus in cerebrospinal fluid. However, AIDS status predisposes to various diseases involving the brain, testing the diagnostic ability of the clinician. Case description: We describe a PML case in a patient with AIDS, in whom lumbar puncture was initially impossible for severe thrombocytopenia and magnetic resonance showed an hyperintense lesion and was unable to distinguish between PML and lymphoma. In this case, [18F]-fluorodeoxyglucose (FDG)-PET imaging showing a hypometabolism of the lesion helped to initially orient toward PML, as diagnosis was later confirmed by lumbar puncture. We collected 21 cases in the literature in which [18F]-FDG-PET was helpful in cases of PML. Discussion and Conclusions: PET imaging is not considered a standard diagnostic tool for PML. However, in selected cases, it may provide valuable information to direct the diagnosis towards PML.
Full article
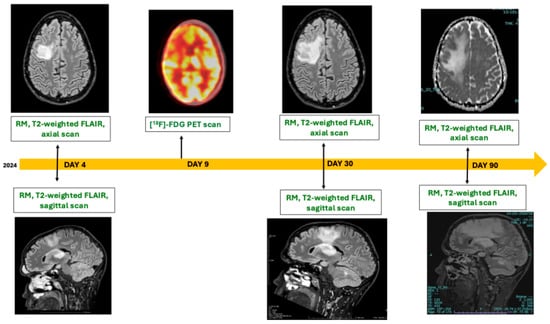
Figure 1
Open AccessCase Report
Brucella anthropi Endocarditis: An Unusual Pathogen
by
Fernando Baires, Erin Arias, María José Díaz, Cesar Burgos, Carlos A. Umaña Mejia, Justice Cruz, Joanne Cordero Guerra, Helen Hoffman, Jack Bordovsky, Jana Radwanski, Miguel Sierra-Hoffman and Amy C. Madril
Infect. Dis. Rep. 2026, 18(2), 32; https://doi.org/10.3390/idr18020032 - 8 Apr 2026
Abstract
►▼
Show Figures
Background: The genus Brucella has expanded considerably in the 21st century. With the advent of advanced phylogenetic analyses, a close genetic relationship between Brucella and Ochrobactrum has been identified, leading to reclassification of Ochrobactrum species within the genus Brucella. Among these, Brucella
[...] Read more.
Background: The genus Brucella has expanded considerably in the 21st century. With the advent of advanced phylogenetic analyses, a close genetic relationship between Brucella and Ochrobactrum has been identified, leading to reclassification of Ochrobactrum species within the genus Brucella. Among these, Brucella anthropi (formerly Ochrobactrum anthropi) is increasingly recognized as a rare cause of invasive human infection. We report a clinically significant case of B. anthropi infective endocarditis and review the available literature. Methods: We report a case of B. anthropi infective endocarditis and conducted a narrative review of the English-language medical literature through 2025. Cases were analyzed for demographics, clinical presentation, antimicrobial susceptibility, and outcomes. Results: A 75-year-old man with a prosthetic aortic valve and prior endocarditis presented with fever of unknown origin, weight loss, and prior transient ischemic attacks. Blood cultures grew B. anthropi after prolonged incubation. Transesophageal echocardiography demonstrated vegetations involving both the aortic and tricuspid valves, and the patient required targeted combination antimicrobial therapy due to persistent bacteremia. Seven additional cases of B. anthropi infective endocarditis were identified on review of the literature. Most patients had underlying valvular disease or prosthetic material. Reported lethality approached 25%. Antimicrobial susceptibility patterns were variable, underscoring the importance of targeted individualized therapy. Conclusion: Consistent with other Gram-negative bacilli, B. anthropi is a rare but established cause of acute bacterial endocarditis. Despite its rarity, it may represent an under-recognized cause of invasive disease. This case highlights the importance of prolonged culture incubation, careful microbiologic interpretation, and susceptibility-guided therapy.
Full article

Figure 1
Open AccessReview
Therapeutic Management of Septic Venous Thrombosis: A Narrative Review
by
Anabel Franco-Moreno, Ana Bustamante-Fermosel, Juan Torres-Macho and Belén Comeche-Fernández
Infect. Dis. Rep. 2026, 18(2), 31; https://doi.org/10.3390/idr18020031 - 3 Apr 2026
Abstract
Background/Objectives: Septic venous thrombosis is an uncommon complication but clinically significant due to its high morbidity and mortality and the complexity of therapeutic decision-making. The lack of standardized guidelines and the scarcity of high-quality studies complicate clinical management, as most available evidence derives
[...] Read more.
Background/Objectives: Septic venous thrombosis is an uncommon complication but clinically significant due to its high morbidity and mortality and the complexity of therapeutic decision-making. The lack of standardized guidelines and the scarcity of high-quality studies complicate clinical management, as most available evidence derives from highly heterogeneous case series and retrospective studies. In this context, a comprehensive overview is essential to guide real-world practice. Methods: This manuscritp provides an in-depth review of the treatment of septic venous thrombosis at its most frequent sites, including the portal vein and its branches, the pelvic veins, catheter-associated events, the internal jugular vein, and dural venous sinus thrombosis. Results: Across all scenarios, early initiation of appropriate antibiotic therapy is the cornerstone of treatment and must be tailored to the suspected source of infection and the patient’s clinical course. In parallel, although the role of anticoagulation remains debated, several observational studies suggest potential benefits in terms of recanalization and complication prevention, particularly in selected patients. Conclusions: However, the decision to anticoagulate should be carefully individualized within a multidisciplinary framework. Despite the recent progress, many clinical uncertainties remain. Therefore, well-designed clinical trials are needed to define optimal therapeutic strategies for this condition.
Full article
(This article belongs to the Special Issue Review on Infectious Diseases)
►▼
Show Figures

Figure 1
Open AccessCase Report
Non-Typhoidal Salmonella enterica Bacteremia Complicated by Native Shoulder Septic Arthritis in a Patient with Sickle Cell Disease Following Foodborne Exposure: A Case Report and Literature Review
by
Gabriel A. Godart, Vidit Yadav, Joseph M. Bestic, Bradley S. Schoch, Bryan D. Springer, Ravi V. Durvasula, Sammer M. Elwasila and Justin M. Oring
Infect. Dis. Rep. 2026, 18(2), 30; https://doi.org/10.3390/idr18020030 - 2 Apr 2026
Abstract
Background/Objectives: Non-typhoidal Salmonella (NTS) species are well-recognized causes of invasive infection in patients with sickle cell disease (SCD), with a particular predilection for the musculoskeletal system. Although Salmonella osteomyelitis is well described in this population, septic arthritis is uncommon, especially involving the shoulder
[...] Read more.
Background/Objectives: Non-typhoidal Salmonella (NTS) species are well-recognized causes of invasive infection in patients with sickle cell disease (SCD), with a particular predilection for the musculoskeletal system. Although Salmonella osteomyelitis is well described in this population, septic arthritis is uncommon, especially involving the shoulder joint. We describe a case of NTS bacteremia complicated by native shoulder septic arthritis in a patient with SCD and review its clinical implications. Methods: We report the clinical course, diagnostic evaluation, microbiologic findings, imaging studies, and management of a 22-year-old man with homozygous SCD who presented with a vaso-occlusive pain crisis and subsequently developed severe sepsis with persistent Salmonella enterica bacteremia following ingestion of undercooked poultry. Persistent bacteremia prompted further evaluation for metastatic infection using advanced imaging and diagnostic arthrocentesis. Results: Whole-body imaging identified septic arthritis of the native right shoulder, which was confirmed by synovial fluid cultures growing Salmonella species. The patient underwent arthroscopic irrigation and debridement for source control. Antimicrobial therapy was narrowed to intravenous ceftriaxone based on susceptibility data and continued for six weeks. The patient demonstrated clinical improvement with resolution of bacteremia and was discharged to rehabilitation to complete therapy. Conclusions: This case highlights the importance of a careful exposure history, including foodborne sources, in patients with SCD presenting with invasive Salmonella infection. Persistent bacteremia should prompt early investigation for metastatic foci, and timely surgical source control combined with targeted antimicrobial therapy is essential for optimal outcomes in this population.
Full article
(This article belongs to the Section Bacterial Diseases)
►▼
Show Figures

Figure 1
Open AccessArticle
A Blood-Based Interferon Viral Score Defines Acute RSV Bronchiolitis in Infants
by
Ilaria Galliano, Stefania Alfonsina Liguori, Anna Pau, Paola Montanari, Cristina Calvi, Anna Clemente, Anna Massobrio, Claudia Linari, Stefano Gambarino, Alessandra Conio and Massimiliano Bergallo
Infect. Dis. Rep. 2026, 18(2), 29; https://doi.org/10.3390/idr18020029 - 1 Apr 2026
Abstract
►▼
Show Figures
Background: Respiratory syncytial virus (RSV) is the leading cause of bronchiolitis and hospitalization in infancy. Reliable biomarkers reflecting host antiviral responses and disease dynamics are still lacking. Methods: We evaluated the expression of the interferon-stimulated genes IFI44L, IFI27, and RSAD2 in peripheral blood
[...] Read more.
Background: Respiratory syncytial virus (RSV) is the leading cause of bronchiolitis and hospitalization in infancy. Reliable biomarkers reflecting host antiviral responses and disease dynamics are still lacking. Methods: We evaluated the expression of the interferon-stimulated genes IFI44L, IFI27, and RSAD2 in peripheral blood of infants hospitalized with RSV bronchiolitis at admission and discharge, and in healthy controls, using multiplex RT-qPCR. A composite interferon-based Viral Score was derived from coordinated ISG expression. Results: All three ISGs and the Viral Score were markedly elevated during acute RSV infection at hospital admission compared with discharge and healthy controls. Following clinical recovery, ISG expression and Viral Score declined significantly and approached baseline levels. The Viral Score clearly discriminated acute infection from recovery and healthy states, reflecting dynamic systemic interferon activation. Conclusions: A Viral Score based on IFI44L, IFI27, and RSAD2 captures systemic antiviral immune responses in infants with RSV bronchiolitis and declines with disease resolution. This interferon-based host-response signature represents a promising biomarker for defining viral infection status and monitoring disease dynamics in pediatric respiratory infections.
Full article

Figure 1
Open AccessEditor’s ChoiceArticle
Heart Failure Incidence and Risk Factors in U.S. Adults Receiving Bezlotoxumab: A Large Database Analysis
by
Chia-Yu Chiu, Daniel B. Chastain, Joseph Sassine and Andrés F. Henao-Martínez
Infect. Dis. Rep. 2026, 18(2), 28; https://doi.org/10.3390/idr18020028 - 31 Mar 2026
Abstract
Background: Bezlotoxumab is used to prevent recurrent Clostridioides difficile infection. Although well tolerated, heart failure (HF) exacerbations have been reported as adverse events in clinical trials. This study evaluates the incidence and predictors of HF exacerbation following bezlotoxumab. Methods: We used the TriNetX
[...] Read more.
Background: Bezlotoxumab is used to prevent recurrent Clostridioides difficile infection. Although well tolerated, heart failure (HF) exacerbations have been reported as adverse events in clinical trials. This study evaluates the incidence and predictors of HF exacerbation following bezlotoxumab. Methods: We used the TriNetX research database to identify U.S. adults who received bezlotoxumab and stratified them into three groups based on HF history: no HF, HF with preserved ejection fraction (HFpEF), and HF with reduced ejection fraction (HFrEF). The 90-day cumulative incidence of HF events and mortality were assessed. Cox proportional hazard models identified predictors of HF events. Results: Among 2515 patients, 89% had no HF history, 4% had HFpEF, and 7% had HFrEF. The 90-day HF event rates were 1%, 29%, and 52% for the no HF, HFpEF, and HFrEF groups, respectively (p < 0.001). The 90-day all-cause mortality was 0.9%. Corresponding 90-day all-cause mortality rates were 0.04%, 4%, and 11%, respectively (p < 0.001). Independent positive predictors of HF events included HFrEF (aHR 19.400), HFpEF (adjusted hazard ratio [aHR] 8.632), heart transplant (aHR 7.485), hyperlipidemia (aHR 3.184), valvular heart disease (aHR 2.267), chronic kidney disease stage ≥ 3 (aHR 1.715), and ischemic heart disease (aHR 1.987). Protective factors included non-cardiac solid organ transplant (aHR 0.333). Conclusions: Bezlotoxumab appears safe in patients without HF history but is associated with a significantly increased risk of HF exacerbation in those with pre-existing HF, especially HFrEF.
Full article
(This article belongs to the Section Bacterial Diseases)
►▼
Show Figures

Figure 1
Open AccessArticle
Matrix-Dependent Sensitivity of Two Pan-Trematode PCR Assays for Detecting Schistosoma spp. in Clinical Human Samples
by
Hagen Frickmann, Andreas Hahn, Kirsten Alexandra Eberhardt, Ulrike Loderstädt, Norbert Georg Schwarz and Ralf Matthias Hagen
Infect. Dis. Rep. 2026, 18(2), 27; https://doi.org/10.3390/idr18020027 - 27 Mar 2026
Abstract
Background: Schistosoma spp. are trematodes occurring in tropical endemic areas but can be imported to non-endemic regions as causes of travel-associated infections. In this study, two pan-trematode-specific real-time PCR assays were evaluated for their diagnostic sensitivity in detecting Schistosoma spp. DNA in diagnostic
[...] Read more.
Background: Schistosoma spp. are trematodes occurring in tropical endemic areas but can be imported to non-endemic regions as causes of travel-associated infections. In this study, two pan-trematode-specific real-time PCR assays were evaluated for their diagnostic sensitivity in detecting Schistosoma spp. DNA in diagnostic human samples. Methods: Two previously described pan-trematode-specific real-time PCR assays were comparatively assessed using diagnostic samples containing DNA of either the S. haematobium complex or the S. mansoni complex, as confirmed by Schistosoma species complex-specific real-time PCR. Results: Out of a total of 655 samples containing Schistosoma spp. DNA, positive signals in at least one of the two pan-trematode real-time PCR assays were recorded for 17 (2.6%) nucleic acid extractions. Although sensitivity was in the >90% range for stool samples, only a few individual blood plasma and serum samples, and none of the Schistosoma spp. DNA-containing tissue or urine samples, tested positive by pan-trematode PCR. The lower sensitivity of pan-trematode PCR compared with Schistosoma spp.-specific PCR was semi-quantitatively confirmed by higher cycle threshold (Ct) values in the former. When comparing samples with concordant versus discordant positive results for Schistosoma spp.-specific and pan-trematode PCR, Ct values of the Schistosoma spp.-specific PCR were lower in concordantly positive samples than in discordantly positive samples. Conclusions: While the assessed pan-trematode PCR assays showed insufficient sensitivity as screening tools for blood plasma, blood serum, tissue, and urine samples from individuals with suspected schistosomiasis, they were sufficiently sensitive when applied to stool samples, in which substantial amounts of target DNA, as indicated by low Ct values in the Schistosoma species complex-specific real-time PCR assays, can be expected. For screening for Schistosoma spp. DNA in sample materials other than stool, the use of highly sensitive target-specific PCR remains necessary.
Full article
Highly Accessed Articles
Latest Books
E-Mail Alert
News
Topics
Topic in
Infectious Disease Reports, Insects, IJERPH, Pathogens, TropicalMed, Zoonotic Diseases
Vector-Borne Disease Spatial Epidemiology, Disease Ecology, and Zoonoses
Topic Editors: Chad L. Cross, Louisa Alexandra MessengerDeadline: 31 December 2026
Topic in
IJERPH, TropicalMed, Microorganisms, Infectious Disease Reports, Pathogens
Genetic, Environmental, and Climatic Drivers of Emerging Arboviruses and Public Health Implications
Topic Editors: André Ricardo Ribas Freitas, Pedro María Alarcón-Elbal, Luciano Pamplona de Góes CavalcantiDeadline: 20 January 2027
Topic in
Diseases, Epidemiologia, Infectious Disease Reports, Medicina, TropicalMed
Surveillance Systems and Predictive Analytics for Epidemics
Topic Editors: Georgia Kourlaba, Elisavet StavropoulouDeadline: 31 January 2027

Special Issues
Special Issue in
Infectious Disease Reports
Prevention, Diagnosis and Treatment of Healthcare-Associated Infections
Guest Editor: Emine Alp MeşeDeadline: 31 May 2026
Special Issue in
Infectious Disease Reports
Challenges in the Management of Onychomycosis and Other Superficial Fungal Infections
Guest Editor: Aditya K. GuptaDeadline: 30 June 2026
Special Issue in
Infectious Disease Reports
Infections in Vulnerable Populations
Guest Editors: Botond Lakatos, Francesco Di GennaroDeadline: 30 June 2026
Special Issue in
Infectious Disease Reports
Review on Infectious Diseases
Guest Editor: Carlo TasciniDeadline: 1 July 2026










