Journal Description
Hearts
Hearts
is an international, peer-reviewed, open access journal on cardiology and cardiac & vascular surgery, published quarterly online by MDPI. The Jordanian Cardiac Society (JCS) is affiliated with Hearts and its members receive a discount on the article processing charges.
- Open Access— free for readers, with article processing charges (APC) paid by authors or their institutions.
- High Visibility: indexed within FSTA, and other databases.
- Rapid Publication: manuscripts are peer-reviewed and a first decision is provided to authors approximately 19.9 days after submission; acceptance to publication is undertaken in 2.8 days (median values for papers published in this journal in the second half of 2025).
- Recognition of Reviewers: APC discount vouchers, optional signed peer review, and reviewer names published annually in the journal.
Latest Articles
The Microvascular–Immune Interface in Cardiovascular Disease: A Stage-Based Framework of Microvascular Failure
Hearts 2026, 7(2), 17; https://doi.org/10.3390/hearts7020017 - 21 May 2026
Abstract
Cardiovascular disease is traditionally interpreted through macrocirculatory parameters such as cardiac output, vascular resistance, and epicardial coronary anatomy. However, clinical outcomes frequently diverge from predictions based solely on these indices, particularly in syndromes such as heart failure with preserved ejection fraction (HFpEF), cardiogenic
[...] Read more.
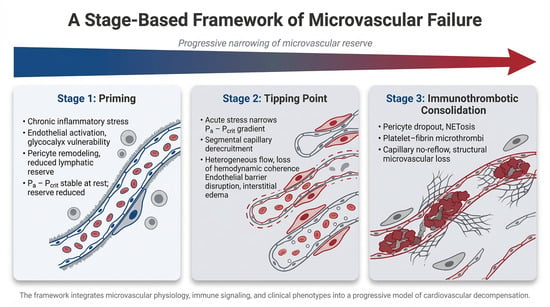
Cardiovascular disease is traditionally interpreted through macrocirculatory parameters such as cardiac output, vascular resistance, and epicardial coronary anatomy. However, clinical outcomes frequently diverge from predictions based solely on these indices, particularly in syndromes such as heart failure with preserved ejection fraction (HFpEF), cardiogenic shock, and sepsis-associated myocardial dysfunction. Increasing evidence suggests that the integrity of the microvascular–immune interface plays a central role in determining tissue perfusion and cardiovascular resilience. This review proposes a staged framework of cardiovascular decompensation centered on progressive failure of this interface. In Stage 1, chronic cardiometabolic and inflammatory stress produces a primed but compensated microvascular state characterized by endothelial activation, glycocalyx vulnerability, pericyte remodeling, platelet sensitization, and reduced lymphatic reserve. Perfusion is preserved at rest, but vasodilatory reserve and microvascular stability are reduced, narrowing the effective perfusion window under physiologic stress. In Stage 2, acute insults such as infection, ischemia, or neurohumoral activation precipitate threshold instability within the microcirculation. Perfusion becomes governed by the arterial pressure–critical closing pressure (Pa − Pcrit) relationship rather than traditional arterial–venous gradients. As this window narrows, segmental capillary derecruitment and heterogeneous flow emerge, producing loss of hemodynamic coherence in which systemic blood pressure and cardiac output may appear preserved despite impaired tissue perfusion. In Stage 3, inflammatory amplification and immunothrombotic processes consolidate microvascular dysfunction. Pericyte contraction, endothelial injury, cytokine escalation, and neutrophil extracellular trap formation promote platelet–fibrin deposition and capillary obstruction, transforming reversible conductance failure into structural microvascular impairment. This framework provides a unifying physiologic lens for diverse cardiovascular syndromes, including Type 2 myocardial infarction, HFpEF decompensation, and cardiogenic shock. It also suggests that therapeutic efficacy may depend less on macrocirculatory normalization alone and more on preserving microvascular integrity before immunothrombotic consolidation occurs. Although this model remains hypothesis-generating, it highlights the microvascular–immune interface as a central determinant of cardiovascular stability and a potential target for future precision hemodynamic and immunomodulatory strategies.
Full article
(This article belongs to the Topic Cardiovascular Disease in Special Populations: From Basic Science to Clinical Practice)
►
Show Figures
Open AccessArticle
Size Your Valve: Sutureless Valve Size Recomendation System Using Machine Learning Algorithm
by
Rafik Margaryan, Giovanni Concistrè, Giacomo Bianchi and Marco Solinas
Hearts 2026, 7(2), 16; https://doi.org/10.3390/hearts7020016 - 7 May 2026
Abstract
Background: Traditional intraoperative sizing for sutureless aortic valves, such as the Corcym Perceval Plus (CPP), often relies on subjective tactile feedback, which can lead to excessive over-sizing. Significant over-sizing is associated with complications like increased trans-prosthetic gradients, valve thrombosis, and conduction disturbances requiring
[...] Read more.
Background: Traditional intraoperative sizing for sutureless aortic valves, such as the Corcym Perceval Plus (CPP), often relies on subjective tactile feedback, which can lead to excessive over-sizing. Significant over-sizing is associated with complications like increased trans-prosthetic gradients, valve thrombosis, and conduction disturbances requiring permanent pacemakers. This study aims to develop an AI-driven predictive recommendation system using Multidetector Computed Tomography (MDCT) data to optimize valve sizing and improve patient outcomes. Methods: Data were collected from 380 consecutive patients who underwent aortic valve replacement with a CPP prosthesis between 2011 and 2026. Two machine learning models were trained using preoperative MDCT features, including annular area, perimeter, and diameters. The first model predicted “normal” clinical labels, while the second used “penalized” labels adjusted for postoperative hemodynamic performance to discourage over-sizing. The dataset was split into training (80%) and testing (20%) subsets. Results: The mean patient age was 77.6 years. The model using normal labels achieved an overall accuracy of 91.84% (68.75% on the test set). The penalized label model showed improved performance with an overall accuracy of 92.89% (72.16% on the test set). MDCT provided highly reproducible objective metrics superior to echocardiography for calculating optimal sizing. Conclusions: The AI-driven recommendation system proves to be a reliable and reproducible tool for preoperative planning. By transitioning from subjective tactile assessment to predictive modeling, surgeons can better select valve sizes that minimize complications, particularly in minimally invasive approaches.
Full article
(This article belongs to the Collection Feature Papers from Hearts Editorial Board Members)
►▼
Show Figures

Figure 1
Open AccessReview
Intraoperative Methadone in Adult and Pediatric Cardiac Surgery: A Narrative Review
by
João Paulo Jordão Pontes, Isabella Rodrigues Reis, Anastácio de Jesus Pereira, Neise Apoliany Martins Pacheco, Celso Eduardo Rezende Borges, Antônio de Pádua Gandra Júnior and Fernando Cássio do Prado Silva
Hearts 2026, 7(2), 15; https://doi.org/10.3390/hearts7020015 - 6 May 2026
Abstract
►▼
Show Figures
Background/Objectives: Intraoperative methadone has emerged as a significant pharmacological strategy in cardiac surgery to improve postoperative analgesic outcomes and reduce the reliance on rescue short-action opioids. This review aims to synthesize evidence regarding the safety and efficacy of intravenous methadone compared to
[...] Read more.
Background/Objectives: Intraoperative methadone has emerged as a significant pharmacological strategy in cardiac surgery to improve postoperative analgesic outcomes and reduce the reliance on rescue short-action opioids. This review aims to synthesize evidence regarding the safety and efficacy of intravenous methadone compared to other strategies for postoperative pain control in adult and pediatric cardiac surgeries. Methods: This narrative review relied on electronic searches in PubMed, Web of Science, Cochrane Library, and EMBASE up to January 2026. From 199 articles retrieved, 41 were included, focusing on analgesic efficacy, safety, pharmacokinetic variations during cardiopulmonary bypass (CPB), and cost-effectiveness. Results: The implementation of methadone results in up to 70% reduction in postoperative opioid requirements. Patients experience significantly lower pain scores from 24 to 72 h and improvement in satisfaction regarding pain management. In pediatric populations (neonates and children), the use of methadone leads to a significant reduction in opioid needs and a high rate of extubation in the operating room. Pharmacokinetically, a 48% drop in methadone concentration occurs during CPB due to hemodilution and sequestration. Safety data confirms that intraoperative use does not prolong mechanical ventilation; however, doses exceeding 0.25 mg/kg are linked to an increased incidence of delirium. Economically, methadone can be cost-effective, resulting in savings of up to $6355 per patient. Conclusions: Intraoperative methadone improves postoperative analgesia, opioid consumption, patient satisfaction, and costs after cardiac surgery. Its opioid-sparing effects make it particularly attractive for ERAS protocols, although vigilance against dose-related delirium and QT prolongation remains essential. Further research, especially in pediatrics, is needed to refine dosages and safety protocols.
Full article

Graphical abstract
Open AccessCorrection
Correction: Kwak et al. The Influence of Body Mass Index on Percutaneous Coronary Intervention Outcomes: A National Inpatient Sample Study. Hearts 2025, 6, 5
by
Eun Seo Kwak, Momin Shah, Abdulmajeed Alharbi, Nahush Bansal, Qutaiba Qafisheh, Shariq Ahmad Wani, Mohanad Qwaider, Ayman Salih, Ahmed El-Rahyel, Hafsa Shah, Omar Sajdeya and Ehab Eltahawy
Hearts 2026, 7(2), 14; https://doi.org/10.3390/hearts7020014 - 27 Apr 2026
Abstract
There was an error in the original publication [...]
Full article
Open AccessArticle
NT-proBNP Discriminates Severe Systolic Dysfunction and Is Associated with Mortality in Advanced Duchenne Muscular Dystrophy: A Retrospective Cohort Study
by
Marcello Marcì, Francesca Macaione and Grazia Crescimanno
Hearts 2026, 7(2), 13; https://doi.org/10.3390/hearts7020013 - 20 Apr 2026
Abstract
►▼
Show Figures
Background: Cardiomyopathy is a major cause of morbidity and mortality in Duchenne muscular dystrophy (DMD). We evaluated whether N-terminal pro–brain natriuretic peptide (NT-proBNP) identifies severe systolic dysfunction and assessed its diagnostic performance. Methods: Male patients with genetically confirmed DMD and established
[...] Read more.
Background: Cardiomyopathy is a major cause of morbidity and mortality in Duchenne muscular dystrophy (DMD). We evaluated whether N-terminal pro–brain natriuretic peptide (NT-proBNP) identifies severe systolic dysfunction and assessed its diagnostic performance. Methods: Male patients with genetically confirmed DMD and established cardiomyopathy were included if NT-proBNP measurement and echocardiographic ejection fraction (EF) were available within one month. Severe systolic dysfunction was defined as EF < 40%. Clinical, cardiac, and respiratory variables were analysed. ROC analysis with bootstrap validation and exploratory logistic regressions was performed. Results: NT-proBNP levels were significantly higher in patients with EF < 40% (median 843 vs. 81 pg/mL). A cut-off >200 pg/mL identified severe systolic dysfunction with 90.5% sensitivity and 90.9% specificity (AUC 0.96, 95% CI 0.88–1.00). During 24 months of follow-up, five deaths occurred. NT-proBNP showed moderate discrimination for mortality (AUC 0.79) and was associated with mortality in exploratory analysis. Conclusions: NT-proBNP was associated with severe systolic dysfunction in Duchenne cardiomyopathy and may complement imaging. Prospective validation is warranted.
Full article

Figure 1
Open AccessCase Report
Paradoxical Coronary Artery Embolism Through a Patent Foramen Ovale in a Young Adult
by
Sumi Singh, Mays Tawayha, Manoj Sharma, Taher Sbitli and Wassim Mosleh
Hearts 2026, 7(2), 12; https://doi.org/10.3390/hearts7020012 - 7 Apr 2026
Abstract
►▼
Show Figures
We describe the case of a 26-year-old man who presented with acute chest pain and was found to have single-vessel coronary occlusion most consistent with probable paradoxical embolism. Coronary angiography demonstrated complete occlusion of the ramus intermedius artery. Aspiration thrombectomy restored flow without
[...] Read more.
We describe the case of a 26-year-old man who presented with acute chest pain and was found to have single-vessel coronary occlusion most consistent with probable paradoxical embolism. Coronary angiography demonstrated complete occlusion of the ramus intermedius artery. Aspiration thrombectomy restored flow without stent implantation. Intravascular ultrasound showed no plaque rupture, atherosclerosis, or coronary dissection, supporting but not definitively confirming an embolic etiology. Transthoracic and transesophageal echocardiography subsequently identified a large patent foramen ovale with bidirectional shunting. Lower-extremity Doppler studies and an extensive hypercoagulable evaluation were negative. The patient later underwent successful percutaneous closure of the patent foramen ovale. This case highlights probable paradoxical coronary embolism as a rare cause of acute myocardial infarction in a young patient without significant atherosclerotic disease and underscores the value of multimodality imaging in supporting the diagnosis and guiding management.
Full article

Figure 1
Open AccessCase Report
Twiddler’s Syndrome: Predictors, Prevention, and Outcomes in a Case Series
by
Cian Murray, Abdullahi Khair and Solomon Asgedom
Hearts 2026, 7(2), 11; https://doi.org/10.3390/hearts7020011 - 30 Mar 2026
Abstract
►▼
Show Figures
Background/Objectives: Twiddler’s syndrome is an uncommon but clinically important complication of implantable cardiac devices, in which generator rotation within the pocket results in lead torsion, lead retraction, and device malfunction. Recurrence can necessitate repeated surgical intervention and may be preventable through early risk
[...] Read more.
Background/Objectives: Twiddler’s syndrome is an uncommon but clinically important complication of implantable cardiac devices, in which generator rotation within the pocket results in lead torsion, lead retraction, and device malfunction. Recurrence can necessitate repeated surgical intervention and may be preventable through early risk identification and procedural strategies. Methods: We describe a single-centre case series of three female patients with pacemaker-associated Twiddler’s syndrome. Clinical presentation, timing of lead retraction, management strategies (including pocket location and fixation approach), recurrence, and follow-up outcomes were reviewed. Results: All patients were older women and developed symptomatic device failure early after implantation, with radiographic confirmation of lead retraction and coiling occurring within three weeks in all cases. Recurrence was observed when enhanced preventive measures were not employed. Notably, in one patient, recurrence occurred after an initial revision in a second prepectoral pocket, prompting subsequent reimplantation in a subpectoral location with reinforced fixation and structured patient and family counselling, after which no further recurrence occurred at one year. In the remaining cases, revision with reinforced generator fixation and counselling was associated with stable lead position and satisfactory device function during follow-up. Conclusions: Twiddler’s syndrome most commonly presents in the first weeks following implantation. Proactive identification of at-risk patients and consideration of reinforced fixation and pocket strategies at the index procedure may reduce recurrence and avoid repeat interventions.
Full article

Figure 1
Open AccessReview
Why and How to Measure Left Ventriculo-Arterial Coupling in Rapidly Altered Hemodynamic States
by
Cosmin Balan, Marina Petersen Saadi, Miguel Ayala Leon, Matteo Cameli and Hatem Soliman Aboumarie
Hearts 2026, 7(1), 10; https://doi.org/10.3390/hearts7010010 - 13 Mar 2026
Abstract
Background: Left ventriculo-arterial coupling (VAC) integrates the interaction between left ventricular contractility and the arterial system, representing a key determinant of cardiovascular efficiency. In rapidly changing hemodynamic states such as septic or cardiogenic shock, conventional indices of pressure or flow alone may
[...] Read more.
Background: Left ventriculo-arterial coupling (VAC) integrates the interaction between left ventricular contractility and the arterial system, representing a key determinant of cardiovascular efficiency. In rapidly changing hemodynamic states such as septic or cardiogenic shock, conventional indices of pressure or flow alone may be misleading. VAC provides a unified physiological framework to assess global cardiovascular performance and guide therapy. Objective: To review the physiological foundations, bedside assessment, and therapeutic applications of VAC in critically ill patients with rapidly fluctuating circulatory conditions. Methods and Content: The article revisits the underlying principles of VAC, expressed as the ratio between arterial elastance (Ea) and end-systolic elastance (Ees), and discusses their derivation from the pressure–volume relationship. Practical echocardiographic methods for bedside estimation, including the non-invasive single-beat approach, are outlined with illustrative figures. The review further examines how VAC patterns evolve in sepsis, cardiogenic shock, and heart failure and how this integrative index clarifies paradoxical responses to vasoactive and inotropic therapies. Specific therapeutic phenotypes are proposed according to Ea/Ees profiles, providing a structured approach to optimise coupling and restore circulatory efficiency. Summary: VAC offers a physiology-based perspective on cardiovascular performance, enabling clinicians to interpret complex hemodynamic changes beyond traditional measures of ejection fraction or mean arterial pressure. Its dynamic tracking may refine the assessment of therapeutic trajectories and improve bedside decision-making. Conclusions: By integrating ventricular and arterial function into a single measure, VAC bridges cardiovascular physiology and clinical practice. Its incorporation into routine critical care monitoring could enhance individualised hemodynamic management and serve as a foundation for future outcome-driven studies. Methodology: This narrative review was conducted using a structured literature search to ensure comprehensive coverage of contemporary evidence regarding ventriculo-arterial coupling (VAC) in critical care and shock states. A systematic search of PubMed/MEDLINE, Embase, and Scopus databases was performed from database inception through October 2025. The following key search terms were used: “ventriculo-arterial coupling”; “arterial elastance”; “end-systolic elastance”; “Ea/Ees”; “pressure–volume loops”; “septic shock”; “cardiogenic shock”; “critical care echocardiography”; “point-of-care ultrasound”; “mechanical circulatory support”. Reference lists of relevant articles, review papers, and consensus documents were also manually screened to identify additional pertinent studies. Only English-language publications were included. Both seminal foundational studies and recent contemporary investigations were reviewed to provide historical context and up-to-date clinical applicability.
Full article
(This article belongs to the Collection Feature Papers from Hearts Editorial Board Members)
►▼
Show Figures

Figure 1
Open AccessArticle
Primary Prevention of Atherosclerotic Cardiovascular Disease Fails in Young Individuals According to Recent Data in The Netherlands
by
Juliette J. Crooijmans, Kayleigh M. van de Wiel, Kun He, Max C. Keuken, Viktor Wottschel, Christine Widrich, Koos A. H. Zwinderman and Sara-Joan Pinto-Sietsma
Hearts 2026, 7(1), 9; https://doi.org/10.3390/hearts7010009 - 6 Mar 2026
Abstract
►▼
Show Figures
Background: Atherosclerotic cardiovascular disease (ASCVD) is one of the most important causes of morbidity worldwide. Registries show an impressive decline in prevalent ASCVD morbidity over the last years. Whether this decline is due to the improvement in treatment options for ASCVD or
[...] Read more.
Background: Atherosclerotic cardiovascular disease (ASCVD) is one of the most important causes of morbidity worldwide. Registries show an impressive decline in prevalent ASCVD morbidity over the last years. Whether this decline is due to the improvement in treatment options for ASCVD or whether we are also able to prevent first ASCVD events is still unknown. Methods: A nationally representative real-world data longitudinal prescription (LRx) database (IQVIA) was used over a period from 2008 to 2019. All patients ≥20 years were included from the moment they had been prescribed ASCVD medication. The primary outcome was the standardized incidence of first ASCVD events among men and women of different age groups. The secondary outcome of this study was to identify comorbidities in the year 2019. Results: The prescription data on 296.050 individuals were analyzed, and the results indicate the standardized cumulative incidence (%) among women of first ASCVD event prescriptions. This rise in incidence was most pronounced for young women (women 20–39 yr: + 109.46%). The comorbidity analysis indicated that, e.g., thyroid hormones were significantly more often prescribed in the young patients with a first ASCVD event than in those patients without ASCVD events. Conclusions: Prescriptions for the first ASCVD event increased over a period of 12 years among young women. This study suggests that although ASCVD as a whole has decreased over time, this does not seem to be the case for first ASCVD events and that young women are particularly affected.
Full article

Figure 1
Open AccessReview
Transcatheter Edge-to-Edge Repair for Mitral Regurgitation: Distinct Interventional Paradigms for Primary and Secondary MR
by
Lucio Giuseppe Granata, Marcello Marchetta, Simona Giubilato, Michele Massimo Gulizia, Giuseppe Massimo Sangiorgi and Giuseppina Maura Francese
Hearts 2026, 7(1), 8; https://doi.org/10.3390/hearts7010008 - 26 Feb 2026
Abstract
►▼
Show Figures
Background/Objectives: Transcatheter edge-to-edge repair (TEER) has become an established therapeutic option for selected patients with mitral regurgitation (MR). However, primary (degenerative) and secondary (functional) MR represent distinct disease entities, characterized by different pathophysiological mechanisms, clinical trajectories, and determinants of benefit. This review aims
[...] Read more.
Background/Objectives: Transcatheter edge-to-edge repair (TEER) has become an established therapeutic option for selected patients with mitral regurgitation (MR). However, primary (degenerative) and secondary (functional) MR represent distinct disease entities, characterized by different pathophysiological mechanisms, clinical trajectories, and determinants of benefit. This review aims to provide an interventional cardiology-oriented synthesis of TEER, emphasizing the fundamental differences between primary and secondary MR and their implications for patient selection, procedural strategy, and outcome interpretation. Methods: A targeted literature search was performed in PubMed and Embase to identify pivotal randomized trials, registries, guideline documents, and high-quality reviews addressing TEER in MR. The available evidence was synthesized narratively, with a focus on mechanistic insights, TEER-specific imaging and procedural endpoints, and clinically relevant outcomes. Results: In primary MR, TEER functions as a valve-centered therapy, with procedural success primarily determined by anatomical suitability and the balance between durable MR reduction and avoidance of elevated transmitral gradients. In secondary MR, TEER should be considered an adjunctive intervention within a comprehensive heart failure strategy, with benefit dependent on patient phenotype, myocardial substrate, optimization of background therapy, and appropriate timing. Emerging phenotypes, such as atrial functional MR, further challenge traditional classification and highlight the need for mechanism-based selection. Across MR subtypes, residual MR and transmitral gradients emerge as key post-procedural endpoints with differential prognostic implications. Conclusions: TEER represents a phenotype-specific intervention rather than a uniform solution for MR. Recognizing the distinct interventional paradigms of primary and secondary MR is essential to optimizing patient selection, procedural decision-making, and clinical outcomes.
Full article

Graphical abstract
Open AccessCase Report
Successful Pregnancy in a Woman with a History of Löffler’s Endomyocarditis and Recurrent Ventricular Thrombosis: A Case Report and Literature Review
by
Noriko Arakaki, Kaoru Kawasaki, Kaori Moriuchi, Iiji Koh, Yoshie Yo and Noriomi Matsumura
Hearts 2026, 7(1), 7; https://doi.org/10.3390/hearts7010007 - 8 Feb 2026
Abstract
►▼
Show Figures
We present the case of a 27-year-old woman diagnosed with Löffler’s endomyocarditis complicated by intraventricular thrombus and cerebral infarction. She was treated with prednisolone and anticoagulation therapy; however, tapering of corticosteroids resulted in recurrence of intraventricular thrombosis. Given disease relapse after medication withdrawal,
[...] Read more.
We present the case of a 27-year-old woman diagnosed with Löffler’s endomyocarditis complicated by intraventricular thrombus and cerebral infarction. She was treated with prednisolone and anticoagulation therapy; however, tapering of corticosteroids resulted in recurrence of intraventricular thrombosis. Given disease relapse after medication withdrawal, lifelong anticoagulation was indicated. At 29 years of age, she sought pregnancy counseling. Conception was permitted after stabilization of prednisolone dosage, with a planned switch from a vitamin K antagonist to therapeutic-dose unfractionated heparin during pregnancy. Following disease stabilization, she conceived via artificial insemination. Serial echocardiography at 22 and 34 weeks of gestation demonstrated preserved cardiac function without thrombus recurrence. She delivered a healthy infant by emergency cesarean section at 39 weeks of gestation due to fetal distress. No thrombus recurrence was observed postpartum, and she remained clinically stable during 13 months of follow-up. This represents the case of a successful pregnancy in a woman with a history of recurrent intraventricular thrombosis due to Löffler’s endomyocarditis, highlighting the importance of early diagnosis, sustained immunosuppression, individualized anticoagulation, and multidisciplinary preconception planning.
Full article

Figure 1
Open AccessCase Report
Percutaneous Retrieval of an Embolized Catheter Fragment in Right Heart Chambers in Pinch-Off Syndrome and Subsequent Reimplantation: Nurse’s Role in Interventional Cardiology—A Case Report
by
Alessandro Faraci, Salvatore Evola, Daniele Adorno, Giuseppe Vadalà, Cristina Madaudo, Giulia Mingoia, Giuseppe Astuti, Vincenzo Sucato and Alfredo Ruggero Galassi
Hearts 2026, 7(1), 6; https://doi.org/10.3390/hearts7010006 - 2 Feb 2026
Abstract
►▼
Show Figures
“Pinch-Off Syndrome,” first described by Hinke, is a mechanical complication of totally implantable central venous catheters inserted via subclavian venous access. It occurs when the catheter is compressed between the clavicle and the first rib. Compression can cause transient catheter obstruction and may
[...] Read more.
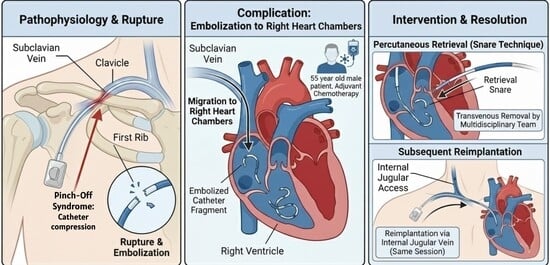
“Pinch-Off Syndrome,” first described by Hinke, is a mechanical complication of totally implantable central venous catheters inserted via subclavian venous access. It occurs when the catheter is compressed between the clavicle and the first rib. Compression can cause transient catheter obstruction and may result in rupture or even complete resection and embolization of the catheter. In this case report, we describe our experience of percutaneous transvenous removal of an embolized port-a-cath fragment within the right heart chambers following a rupture. We used the “retrieval snare” technique and subsequent reimplantation through internal jugular access. The intervention occurred in the same session and involved a multidisciplinary team for a 55-year-old man in need of adjuvant chemotherapy.
Full article
Graphical abstract
Open AccessCase Report
Biventricular Takotsubo Cardiomyopathy Complicated with Cardiogenic Shock: A Postoperative Complication Following Non-Cardiac Surgery
by
Karuna Rayamajhi, Fnu Parul, Mahmoud Khairy, Sumugdha Rayamajhi and Appa Bandi
Hearts 2026, 7(1), 5; https://doi.org/10.3390/hearts7010005 - 11 Jan 2026
Abstract
►▼
Show Figures
Biventricular Takotsubo cardiomyopathy (TCM) is a rare variant characterized by involvement of both the left and right ventricles. This variant is associated with greater hemodynamic instability and longer hospital stays compared to the isolated left ventricular-only variant. We report the case of a
[...] Read more.
Biventricular Takotsubo cardiomyopathy (TCM) is a rare variant characterized by involvement of both the left and right ventricles. This variant is associated with greater hemodynamic instability and longer hospital stays compared to the isolated left ventricular-only variant. We report the case of a 67-year-old female patient who underwent elective resection of a left adrenal adenoma. While her preoperative and intraoperative courses were uneventful, she developed cardiogenic shock postoperatively, necessitating prolonged intensive care unit (ICU) management and vasopressor support. Further evaluation revealed elevated high-sensitivity troponin levels and reduced ejection fraction on echocardiography (30–35%). Hypokinesis was noted in the apical and mid-ventricular segments of both ventricles. A coronary angiogram performed two months prior to admission showed no significant coronary artery disease. Based on these findings, a diagnosis of biventricular TCM was established. The patient was managed supportively and discharged in stable condition with ongoing therapy, including beta-blockers, renin–angiotensin–aldosterone system inhibitors (RAASis), and statins. Follow-up echocardiography showed resolution of regional wall motion abnormalities. Although rare, biventricular TCM is associated with increased severity and a higher risk of complications. Early recognition and timely management are essential to improve outcomes in affected patients.
Full article

Figure 1
Open AccessReview
Contemporary Management of Cardiac Implantable Electronic Devices in the LVAD Era: Evidence, Controversies, and Clinical Implications
by
Giuseppe Sgarito, Francesco Campo, Davide Genovese, Giacomo Mugnai, Francesco Santoro, Pietro Francia, Donatella Ruggiero, Laura Perrotta and Sergio Conti
Hearts 2026, 7(1), 4; https://doi.org/10.3390/hearts7010004 - 8 Jan 2026
Cited by 1
Abstract
►▼
Show Figures
The role of cardiac implantable electronic devices (CIEDs), including implantable cardioverter-defibrillators (ICDs) and cardiac resynchronization therapy (CRT) devices, in patients supported with left ventricular assist devices (LVADs) remains controversial. Although ICDs clearly reduce the risk of sudden cardiac death (SCD) and improve outcomes
[...] Read more.
The role of cardiac implantable electronic devices (CIEDs), including implantable cardioverter-defibrillators (ICDs) and cardiac resynchronization therapy (CRT) devices, in patients supported with left ventricular assist devices (LVADs) remains controversial. Although ICDs clearly reduce the risk of sudden cardiac death (SCD) and improve outcomes in advanced heart failure (HF), their benefit in patients with continuous-flow mechanical circulatory support is less certain. Initial small studies involving LVAD patients, particularly those with older pulsatile devices, suggested that ICDs confer a survival benefit during LVAD support. However, more recent evidence has been inconsistent. Some studies show modest protection against arrhythmic death, whereas others show no improvement in overall mortality. Similarly, CRT does not appear to offer significant additional hemodynamic benefits after LVAD implantation, and current evidence does not strongly support its routine continuation. Device-related complications—including lead failure, infection, electromagnetic interference, and inappropriate shocks—are major clinical concerns that can offset potential benefits. Accordingly, current guidelines recommend maintaining pre-existing ICD or CRT devices in LVAD patients but do not endorse the routine implantation of new devices after LVAD placement. The existing evidence highlights the need for a nuanced and individualized approach to CIED therapy in patients with LVAD. Future research should focus on randomized trials, registry-based analyses, and the exploration of novel technologies such as leadless pacing, subcutaneous ICDs, and advanced programming algorithms. Patient-centered outcomes, particularly quality of life and ethical considerations—such as ICD deactivation in end-of-life scenarios—must be considered in decision-making in this evolving field.
Full article

Graphical abstract
Open AccessArticle
How Online Health Platform Engagement Shapes Atrial Fibrillation Treatment Attitudes: The Role of Psychological Mediators
by
Myrthe F. Kuipers, Joey R. F. N. Snel, Mellanie T. Hills, Bianca J. J. M. Brundel and Umut Konus
Hearts 2026, 7(1), 3; https://doi.org/10.3390/hearts7010003 - 1 Jan 2026
Abstract
Background: This study investigates the impact of engagement with online health platforms (OHPs), perceived treatment effectiveness, and country of residence on patient attitudes toward atrial fibrillation (AF) treatments, mediated by threat perception and behavioral evaluation within an adapted Health Belief Model (HBM). Methods:
[...] Read more.
Background: This study investigates the impact of engagement with online health platforms (OHPs), perceived treatment effectiveness, and country of residence on patient attitudes toward atrial fibrillation (AF) treatments, mediated by threat perception and behavioral evaluation within an adapted Health Belief Model (HBM). Methods: A cross-sectional survey conducted in June 2024 included 589 members of two professionally curated OHPs: the AFIP Foundation (Amsterdam, The Netherlands) and StopAfib.org (Decatur, United States). Data were analyzed using Structural Equation Modeling (SEM) to examine both direct and indirect relationships among engagement behaviors, perceived treatment effectiveness, country of residence, and patient attitudes toward AF treatments (PAAT). Results: Results indicate that higher engagement (i.e., frequency of OHP visits and time spent on the OHP) positively predicts more favorable PAAT, whereas the number of content types consumed showed no significant mediating effect via threat perception or behavioral evaluation. Conclusions: By increasing awareness of AF and reinforcing the perceived effectiveness of treatments, OHPs can serve as effective tools for patient education and support. From a managerial perspective, these findings provide actionable insights for platform operators and healthcare stakeholders on which engagement factors most effectively enhance patient attitudes toward treatment options.
Full article
(This article belongs to the Topic Epidemiology of Atrial Fibrillation: Trends, Insights, and Global Challenges)
►▼
Show Figures
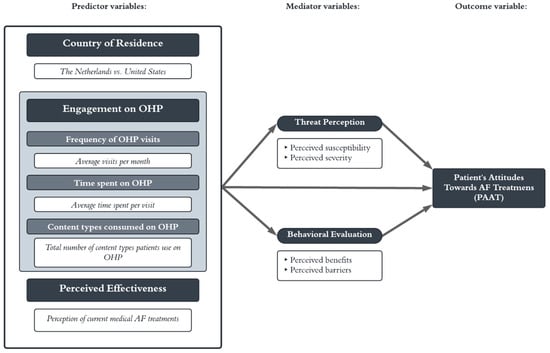
Figure 1
Open AccessReview
Mitral Annular Disjunction: Where Is the Cut-Off Value? Case Series and Literature Review
by
Giovanni Balestrucci, Vitaliano Buffa, Maria Teresa Del Canto, Maria Chiara Brunese, Salvatore Cappabianca and Alfonso Reginelli
Hearts 2026, 7(1), 2; https://doi.org/10.3390/hearts7010002 - 22 Dec 2025
Abstract
►▼
Show Figures
Mitral annular disjunction (MAD) is a structural abnormality of the mitral valve increasingly detected with advanced cardiac imaging, particularly cardiac magnetic resonance (CMR). However, the clinical impact of different degrees of disjunction and the lack of standardized measurement criteria remain controversial. This study
[...] Read more.
Mitral annular disjunction (MAD) is a structural abnormality of the mitral valve increasingly detected with advanced cardiac imaging, particularly cardiac magnetic resonance (CMR). However, the clinical impact of different degrees of disjunction and the lack of standardized measurement criteria remain controversial. This study aimed to describe a series of patients with MAD assessed by CMR and to discuss, in the context of current literature, potential cut-off values that may distinguish physiological from pathological MAD. We retrospectively identified all CMR examinations performed at our institution over a 6-month period in which MAD was visible in at least two cine steady-state free precession (SSFP) projections. For each patient, we recorded MAD extent, presence of mitral valve prolapse/regurgitation, late gadolinium enhancement (LGE) pattern, and main clinical presentation. Nine patients (mean age 57 years; 5 men) were included. Larger MAD distances (>4 mm) were frequently associated with non-ischemic LGE in the basal lateral wall and with valvular abnormalities, whereas smaller disjunctions (≤3 mm) were often observed in patients without significant structural disease. Non-ischemic LGE was present in 6/9 patients, all with MAD > 5 mm. These observations, together with published data, support the hypothesis that small degrees of MAD may represent a frequent anatomical variant, while more extensive disjunction, especially when associated with fibrosis, may indicate a pathological substrate for arrhythmias. Standardized CMR-based criteria and validated MAD cut-off values are needed to improve risk stratification and to incorporate MAD assessment into routine clinical practice.
Full article

Figure 1
Open AccessArticle
No Mismatch and a Lifetime Valve: Surgical Strategy
by
Walid Elmahdy, Brianda Ripoll, Mohamed Sherif, Yama Haqzad, Ahmed Omran, James O’Neill, Christopher Malkin and Dominik Schlosshan
Hearts 2026, 7(1), 1; https://doi.org/10.3390/hearts7010001 - 20 Dec 2025
Abstract
Background: Prosthesis patient mismatch (PPM) is associated with poor outcomes in literature. Prevention of mismatch is crucial in aortic valve replacement, yet there is no current consensus on preventative strategies. Objectives: This study introduces a novel clinical framework, nomenclature, and algorithm for contemporary
[...] Read more.
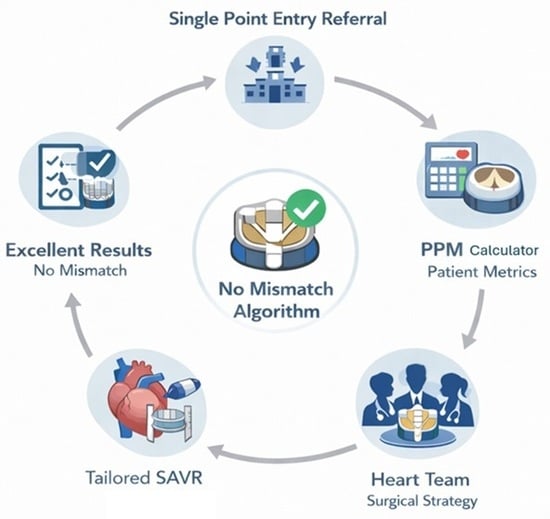
Background: Prosthesis patient mismatch (PPM) is associated with poor outcomes in literature. Prevention of mismatch is crucial in aortic valve replacement, yet there is no current consensus on preventative strategies. Objectives: This study introduces a novel clinical framework, nomenclature, and algorithm for contemporary Heart Team practice, providing a systematic approach for a tailored surgical strategy to anticipate and prevent mismatch. Methods: This was a single-center observational study performing a descriptive analysis of an evolving practice on 100 consecutive patients operated for aortic valve stenosis between 2020 and 2024. A step-by-step No-Mismatch algorithm was designed for the Heart Team to triage, discuss, and decide the surgical strategy prior to the procedure, identifying patients at risk of mismatch, and guiding the surgeon’s plan to prevent PPM and consider a Lifetime Valve Strategy. Results: The algorithm identified 26% of patients at risk of mismatch requiring a No-Mismatch strategy, and 20% at risk of small valve implantation requiring a Lifetime Valve Strategy. This cohort included 51 urgent cases. Valve pathology included 35% congenital, 59% degenerative, 1% rheumatic, and 5% redo operations. Valve implant type: 82% biological, including 29% rapid deployment valve (RDV), and 18% mechanical; 20% of patients required aortic root enlargements (AREs). Pre-, intra-, and post-operative data are presented. Mortality occurred at 1%. All degrees of mismatch were prevented. Conclusions: The surgeon was able to predict mismatch and elected either ARE, RDV, or a mechanical valve as required. Patient selection and a No-Mismatch Heart Team approach are essential to provide a tailored strategy for aortic valve interventions.
Full article
(This article belongs to the Topic Cardiovascular Disease in Special Populations: From Basic Science to Clinical Practice)
►▼
Show Figures
Graphical abstract
Open AccessArticle
Serum Albumin Is Independently Associated with Length of Hospital-Stay and Short-Term Mortality in Elderly Heart Failure Patients: A Real-World Experience
by
Gianluigi Cuomo, Paolo Tirelli, Gabriella Oliva, Domenico Birra, Antonietta De Sena, Fabio Granato Corigliano, Mariavittoria Guerra, Claudio De Luca, Benedetta Tartaglia, Vittoria Gammaldi, Carmine Fierarossa, Pasquale Madonna, Vincenzo Nuzzo and Francesco Giallauria
Hearts 2025, 6(4), 34; https://doi.org/10.3390/hearts6040034 - 18 Dec 2025
Abstract
Background: Serum albumin is a well-known marker of nutritional and inflammatory status and has been associated with adverse outcomes in heart failure (HF). However, its predictive value for length of hospital-stay and short-term mortality in elderly HF patients remains underexplored. Objectives:
[...] Read more.
Background: Serum albumin is a well-known marker of nutritional and inflammatory status and has been associated with adverse outcomes in heart failure (HF). However, its predictive value for length of hospital-stay and short-term mortality in elderly HF patients remains underexplored. Objectives: To investigate the association between serum albumin levels at hospital admission and length of stay, as well as post-admission mortality, in a cohort of elderly patients hospitalized for HF. Methods: We conducted a retrospective analysis of 56 consecutive patients aged ≥65 years admitted for HF. Comorbidities were assessed using the Cumulative Illness Rating Scale for Geriatrics (CIRS-G), and inflammatory status was measured via C-reactive protein (CRP). Negative binomial regression with robust confidence intervals was employed to evaluate the relationship between serum albumin and length of hospital-stay, adjusting for age, comorbidity burden, and CRP. Cox proportional hazards models were used to assess mortality at 6 months and 1 year, adjusting for age, comorbidity, CRP, and HF subtype, with Kaplan–Meier curves illustrating unadjusted survival differences according to albumin levels and HF subtype. Results: Mean age was 78.6 ± 7.5 years, with 69.6% female patients. Mean serum albumin at admission was 3.58 ± 0.60 g/dL, and mean length of stay was 14.8 ± 10.1 days. Each 1 g/dL increase in albumin was associated with a 32% reduction in length of stay (adjusted IRR = 0.68; 95% CI: 0.54–0.85; p = 0.01), independently by age, inflammatory status and comorbidity. Serum albumin was independently associated with reduced risk of death at 6 months (HR 0.30; 95% CI: 0.11–0.82; p = 0.019) and 1 year (HR = 0.41; 95% CI: 0.17–0.96; p = 0.041). Conclusions: Serum albumin at hospital admission independently predicts length of stay and short-term mortality in elderly patients with HF. Albumin measurement, simple, cheap and universally available biomarker, is helpful for early risk stratification and may guide clinical management in this vulnerable population.
Full article
(This article belongs to the Collection Feature Papers from Hearts Editorial Board Members)
►▼
Show Figures

Graphical abstract
Open AccessArticle
Real-Life Measurement of Vasoregulation in Patients with Cyanotic Congenital Heart Disease: A Feasibility Study
by
Reiner Buchhorn and Elisabeth Hofmann
Hearts 2025, 6(4), 33; https://doi.org/10.3390/hearts6040033 - 13 Dec 2025
Abstract
Background: In cardiology, vasoregulation is one of the most important targets of pharmacotherapy. SOMNOtouch™-NIBP (SOMNOmedics AG, Randersacker, Germany) is a cuffless device designed for continuous, non-invasive blood pressure measurements, and it appears to be ready for use in infants and children with congenital
[...] Read more.
Background: In cardiology, vasoregulation is one of the most important targets of pharmacotherapy. SOMNOtouch™-NIBP (SOMNOmedics AG, Randersacker, Germany) is a cuffless device designed for continuous, non-invasive blood pressure measurements, and it appears to be ready for use in infants and children with congenital heart disease. For infants, minor methodological modifications are required due to their small body size. Methods: Using this device, we demonstrate fluctuations in diastolic blood pressure in three patients: an infant with hypoplastic left heart syndrome after Norwood stage 1 and 2 operations; an infant with Tetralogy of Fallot with heart failure due to pulmonary overcirculation after an aorto-pulmonary shunt implantation; and a 13-year-old girl with chronic cyanosis due to a congenitally corrected transposition of the great arteries (ccTGA) with a ventricular septal defect and pulmonary stenosis. The measurement procedures are completely non-invasive and feasible in an outpatient setting. Results: The results demonstrate strong correlations between blood pressure and oxygen saturation levels as well as heart rate variability. We discuss our results in relation to current concepts of hypoxic pulmonary/systemic vasoconstriction and hypoxemia-related pathways. Conclusions: The cuffless device for continuous, non-invasive blood pressure measurement seems to be useful for infants with and without congenital heart defects who receive pharmacotherapies that modulate vasoregulation. These patients should also be non-invasively monitored for safety reasons and for a better understanding of their pathophysiology.
Full article
(This article belongs to the Topic Adult Congenital Heart Disease: Advances in Diagnosis, Surgery, and Lifelong Care)
►▼
Show Figures

Figure 1
Open AccessReview
A Review of Systemic Hypertension in the Cardiac Transplant Population: Pathophysiology, Management, and Future Directions
by
Eman R. Rashed, Swethika Sundaravel and Juan M. Ortega-Legaspi
Hearts 2025, 6(4), 32; https://doi.org/10.3390/hearts6040032 - 8 Dec 2025
Cited by 1
Abstract
►▼
Show Figures
Heart transplantation is the gold standard in patients with end stage heart failure, offering vastly improved survival, mortality and quality of life. However, hypertension occurring after cardiac transplantation is a serious issue, with the incidence ranging from 50 to 80% of patients. The
[...] Read more.
Heart transplantation is the gold standard in patients with end stage heart failure, offering vastly improved survival, mortality and quality of life. However, hypertension occurring after cardiac transplantation is a serious issue, with the incidence ranging from 50 to 80% of patients. The pathophysiology of the hypertension encompasses a more varied and unique set of causes than those identified in non-organ transplant patients, particularly related to the use of calcineurin inhibitors (CNIs) especially cyclosporine. An in-depth understanding of hypertension after heart transplantation remains a critical issue that necessitates further clarification, due to its deleterious long-term consequence such as impaired graft survival, cardiac allograft vasculopathy (CAV), and overall survival. This article provides a comprehensive review of the prevalence, risk factors, etiology, complications, and management of hypertension after heart transplantation.
Full article

Figure 1
Highly Accessed Articles
Latest Books
E-Mail Alert
News
Topics
Topic in
Cardiogenetics, Hearts, JCDD, JCM
Adult Congenital Heart Disease: Advances in Diagnosis, Surgery, and Lifelong Care
Topic Editors: Satoshi Akagi, Jin Young SongDeadline: 30 June 2026
Topic in
Diagnostics, JCM, JCDD, Hearts, JVD
Mechanical Circulatory Support in Heart Failure—Second Edition
Topic Editors: Anton Sabashnikov, Fernando Riesgo Gil, Aron-Frederik Popov, Evgenij V. Potapov, Ihor KrasivskyiDeadline: 31 December 2026
Topic in
Antioxidants, Biomedicines, Disabilities, JCDD, Hearts, JCRM
Cardiovascular Disease in Special Populations: From Basic Science to Clinical Practice
Topic Editors: Song-Young Park, Gwenael LayecDeadline: 31 January 2027
Topic in
Hearts, JCDD, JCM
Epidemiology of Atrial Fibrillation: Trends, Insights, and Global Challenges
Topic Editors: Tomer Ziv-Baran, Moshe KatzDeadline: 30 April 2027

Special Issues
Topical Collections
Topical Collection in
Hearts
Feature Papers from Hearts Editorial Board Members
Collection Editor: Matthias Thielmann