Journal Description
Tropical Medicine and Infectious Disease
Tropical Medicine and Infectious Disease
(TropicalMed) is an international, peer-reviewed, open access journal of tropical medicine and infectious disease, and is published monthly online. The Australasian College of Tropical Medicine (ACTM) and its joint Faculties of Travel Medicine and Expedition and Wilderness Medicine are affiliated with the journal, serving as their official journal. College members receive discounts on the article processing charges.
- Open Access— free for readers, with article processing charges (APC) paid by authors or their institutions.
- High Visibility: indexed within Scopus, SCIE (Web of Science), PubMed, PMC, Embase, Informit, and other databases.
- Journal Rank: JCR - Q1 (Tropical Medicine) / CiteScore - Q2 (Public Health, Environmental and Occupational Health)
- Rapid Publication: manuscripts are peer-reviewed and a first decision is provided to authors approximately 22.2 days after submission; acceptance to publication is undertaken in 3.8 days (median values for papers published in this journal in the second half of 2025).
- Recognition of Reviewers: reviewers who provide timely, thorough peer-review reports receive vouchers entitling them to a discount on the APC of their next publication in any MDPI journal, in appreciation of the work done.
Impact Factor:
2.6 (2024);
5-Year Impact Factor:
2.8 (2024)
Latest Articles
Serological Susceptibility to Measles Among International Students in South Korea After a Cluster of Cases: A Cross-Sectional Study
Trop. Med. Infect. Dis. 2026, 11(6), 150; https://doi.org/10.3390/tropicalmed11060150 (registering DOI) - 30 May 2026
Abstract
Background: Even though South Korea had eliminated measles in 2006, a localized cluster of measles occurred in a university dormitory in Gyeongsangbuk-do, South Korea, in 2024, involving 22 international students. This study aims to explore measles transmission and to inform future preventive measures.
[...] Read more.
Background: Even though South Korea had eliminated measles in 2006, a localized cluster of measles occurred in a university dormitory in Gyeongsangbuk-do, South Korea, in 2024, involving 22 international students. This study aims to explore measles transmission and to inform future preventive measures. Methods: In a cross-sectional study, 299 international students from two local universities underwent a self-reported questionnaire survey and targeted serological testing by enzyme-linked immunosorbent assay two months after the cluster of measles cases. Statistical analysis used Pearson’s chi-square test, Fisher’s exact test, multivariate logistic regression, and Firth’s penalized logistic regression. Results: The overall seropositivity was 79.6%, and 78.0% among participants aged ≤ 30 years. Among multivariate analyses, nationality was independently associated with seropositivity (aOR up to 8.35 for Chinese students). Conclusions: These findings underscore the immunity gaps among international students, with seropositivity remaining below the 95% threshold required for herd immunity. Targeted serological screening and catch-up vaccination may help to improve immunity in mobile populations.
Full article
(This article belongs to the Section Infectious Diseases)
Open AccessArticle
Knowledge, Attitudes, Practices, and Information Pathways Related to Brucellosis Among Adults in Najran City, Saudi Arabia: A Stratified Time–Location Cross-Sectional Study
by
Abdullateef Abdullah Alshehri, Mohammad Y. Alqahtani, Osman AE. Elnoubi, Mohsen A. Qahtani, Dehiyyan E. Alyami, Meshal M. Alabbas, Mosa M. Bahnass, Abdullah Alshehari, Mohammed A. Alshehri and Mohammed A. Alshahrani
Trop. Med. Infect. Dis. 2026, 11(6), 149; https://doi.org/10.3390/tropicalmed11060149 - 29 May 2026
Abstract
Brucellosis remains an important zoonotic disease in southern Saudi Arabia; however, community-level knowledge, risk-related practices, and information pathways in Najran City are insufficiently characterized. This study assessed brucellosis-related knowledge, attitudes, practices, and information pathways among adults in Najran City to inform locally relevant
[...] Read more.
Brucellosis remains an important zoonotic disease in southern Saudi Arabia; however, community-level knowledge, risk-related practices, and information pathways in Najran City are insufficiently characterized. This study assessed brucellosis-related knowledge, attitudes, practices, and information pathways among adults in Najran City to inform locally relevant One Health interventions. In this cross-sectional survey, adults were recruited using stratified time–location (venue-based) sampling across community and exposure-relevant sites in Najran City. A total of 608 adults completed a structured interviewer-administered questionnaire. Composite scores were calculated for knowledge (0–21), attitude (0–22), practice (0–64), and information-source breadth (0–6). Descriptive statistics, group comparisons, correlation analyses, and multivariable linear regressions were performed. The findings suggest that participants more commonly relied on interpersonal social networks, especially family and friends, for information related to brucellosis (53.9%), whereas formal sources were less commonly reported, including health professionals (7.9%), media (4.6%), internet sources (3.3%), educational institutions (2.0%), and agricultural or veterinary organizations (1.3%). Mean knowledge scores were moderate (10.7/21), attitudes were generally favorable (19.5/22), and practice scores were moderate (36.6/64). Exposure-related behaviors remained common, particularly the consumption of unpasteurized milk or dairy products (56.6%). The breadth of information sources showed a moderate positive correlation with knowledge (rho = 0.561), whereas attitude showed only small positive correlations with knowledge and practice. Finally, knowledge was weakly and inversely correlated with practice. Among adults recruited in this venue-based sample, favorable attitudes did not consistently correspond to safer practices. These findings support practical One Health interventions, including coordinated veterinary–public health messaging on animal abortion events, safe-dairy guidance at points of sale and community venues, workplace-based training for livestock-contact groups, and referral pathways linking suspected animal cases with veterinary services and human care-seeking. Because recruitment was venue-based and non-probability, the results should be interpreted as descriptive and hypothesis-generating rather than population-representative; however, they still identify practical communication and service-delivery priorities for future intervention studies in Najran.
Full article
(This article belongs to the Special Issue Advances in Brucella Infections)
Open AccessBrief Report
Schistosoma japonicum Worms Alter the miRNA Expression Profile of Hepatic Stellate Cells with Potential Implications for Liver Fibrosis and Hepatocellular Carcinoma
by
Haoran Zhong, Bowen Dong, Danlin Zhu, Ruiting Zhang, Yuanzhao Sun, Junhan Xiong, Liu Gao, Ke Lu, Hao Li, Zhiqiang Fu, Jinming Liu and Yamei Jin
Trop. Med. Infect. Dis. 2026, 11(6), 148; https://doi.org/10.3390/tropicalmed11060148 - 28 May 2026
Abstract
Although schistosome eggs are widely recognized as the principal drivers of hepatic granulomatous inflammation and fibrosis, the independent effects of adult worms may be masked by strong egg antigen-mediated responses. This study aimed to investigate whether adult Schistosoma japonicum worms alter the miRNA
[...] Read more.
Although schistosome eggs are widely recognized as the principal drivers of hepatic granulomatous inflammation and fibrosis, the independent effects of adult worms may be masked by strong egg antigen-mediated responses. This study aimed to investigate whether adult Schistosoma japonicum worms alter the miRNA expression profile of hepatic stellate cells and to explore the potential relevance of these changes to liver fibrosis and hepatocellular carcinoma-related processes. A non-contact Transwell co-culture system was established using paired Schistosoma japonicum worms or male worms and hepatic stellate cells. Male worms were additionally included to further assess worm-derived effects independent of egg production–related influences. Untreated hepatic stellate cells served as controls. Total RNA was extracted for miRNA sequencing, and differentially expressed miRNAs were identified. Target gene prediction, Kyoto Encyclopedia of Genes and Genomes pathway enrichment analysis, and validation using The Cancer Genome Atlas database were subsequently performed. Both paired worms and male worms significantly altered the miRNA expression profile of hepatic stellate cells. Several differentially expressed miRNAs were identified, among which hsa-miR-103a-3p showed relatively stable changes. Pathway enrichment analysis suggested that the potential target genes of hsa-miR-103a-3p were mainly enriched in AMP-activated protein kinase, mechanistic target of rapamycin, tumor necrosis factor, insulin signaling, and cellular senescence pathways. Further analysis using The Cancer Genome Atlas database showed that hsa-miR-103a-3p had diagnostic value in hepatocellular carcinoma and was associated with alpha-fetoprotein level, albumin level, Ishak fibrosis score, pathological stage, histological type, and tumor status. These findings suggest that adult S. japonicum worms may alter the miRNA expression profile of hepatic stellate cells, and that hsa-miR-103a-3p may be associated with fibrogenic responses and may have potential relevance to hepatocellular carcinoma-related processes. However, this inference is based on correlative TCGA data and does not imply a causal role in schistosomiasis-associated hepatocarcinogenesis.
Full article
(This article belongs to the Special Issue Research Advances and New Perspectives on Helminthic Diseases)
►▼
Show Figures

Figure 1
Open AccessArticle
Residual Human Intestinal Nematode Infections Following Discontinuation of Mass Drug Administration in a Rural South Asian Setting: Implications for Deworming Surveillance
by
Nalini Jayakody, Catherine A. Gordon, Anjana Silva, Nuwan Wickramasinghe, Susiji Wickramasinghe, Natasha Collinson, Asela Wijayasekara, Chanaka Karunarathne, Nilanthi de Silva and Kosala Weerakoon
Trop. Med. Infect. Dis. 2026, 11(6), 147; https://doi.org/10.3390/tropicalmed11060147 - 27 May 2026
Abstract
Prevalence of soil-transmitted helminth (STH) infections in Sri Lanka has declined from 73.3% in 1954 to <1% in 2017, leading to revised deworming policies and discontinuation of routine deworming in three districts, including Anuradhapura, in 2019. As countries approach elimination, this study assessed
[...] Read more.
Prevalence of soil-transmitted helminth (STH) infections in Sri Lanka has declined from 73.3% in 1954 to <1% in 2017, leading to revised deworming policies and discontinuation of routine deworming in three districts, including Anuradhapura, in 2019. As countries approach elimination, this study assessed human intestinal nematode infection (HINI) prevalence in Anuradhapura, a low-endemic setting, using microscopic and molecular methods. From January to November 2023, 967 primary school children were recruited and screened for HINI using direct smears, Kato–Katz, formalin ether concentration, agar plate culture, scotch tape, and qPCR. Combined microscopy and molecular prevalence was 41.2% for STH and 54.1% for HINI. The most prevalent HINI was Enterobius vermicularis (191, 24.5%), followed by Strongyloides stercoralis (120, 19.2%), Ascaris lumbricoides (113, 18.1%), Trichuris trichiura (40, 6.4%), and hookworm (43, 6.9%). Against the composite reference standard, qPCR demonstrated superior diagnostic performance across all species, achieving sensitivities of 86.7% for Ascaris, 85.0% for Trichuris, and 97.7% for hookworm, consistently exceeding those of microscopy-based methods. Correspondingly, qPCR also identified the highest infection prevalences, detecting Ascaris, Trichuris, and hookworm infections in 15.7%, 5.4%, and 6.7% of participants, respectively. All infections were low-intensity as determined by Kato–Katz. Microscopy significantly underestimates STH prevalence. In post-deworming settings, integrated surveillance including molecular diagnostics is essential. The high prevalence of S. stercoralis and E. vermicularis highlights the need for expanded surveillance and targeted interventions to support sustainable control.
Full article
(This article belongs to the Section Neglected and Emerging Tropical Diseases)
►▼
Show Figures
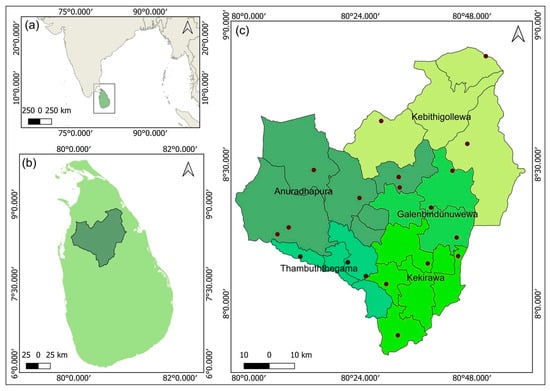
Figure 1
Open AccessArticle
Localization of the Complement C1q-Binding Site on Echinococcus multilocularis Calreticulin Identified by Peptide Mapping
by
Yinghui Song, Meng Xia, Haoran Zong, Wenjie Dong, Qiang Wang, Qin Yang, Bin Zhan, Yanhai Wang and Limei Zhao
Trop. Med. Infect. Dis. 2026, 11(6), 146; https://doi.org/10.3390/tropicalmed11060146 - 26 May 2026
Abstract
Alveolar echinococcosis is a life-threatening zoonotic parasitic disease caused by infection of Echinococcus multilocularis larvae. To survive within the host’s immune milieu, E. multilocularis has evolved sophisticated immune evasion strategies, including the expression of immunomodulatory proteins that regulate the host immune response. Our
[...] Read more.
Alveolar echinococcosis is a life-threatening zoonotic parasitic disease caused by infection of Echinococcus multilocularis larvae. To survive within the host’s immune milieu, E. multilocularis has evolved sophisticated immune evasion strategies, including the expression of immunomodulatory proteins that regulate the host immune response. Our previous studies have demonstrated that E. multilocularis calreticulin (EmCRT) possessed strong binding ability to human complement component C1q to inhibit C1q-initiated complement activation and biological functions. To further elucidate the mechanism by which EmCRT mediates C1q inactivation and immune evasion, the precise C1q-binding site on EmCRT was identified and analyzed in this study through expression of overlapping fragments and synthesis of overlapping peptides covering the identified functional fragment. The fragment expression and functional assay narrowed down the C1q-binding site to the EmCRT-S1 fragment located between amino acids 140 and 204 of EmCRT. The precise binding site was further pinpointed to the P5 peptide (EmCRT160–174 aa) by testing the synthetic peptides covering this region. The binding of peptide P5 to C1q markedly suppressed the activation of the C1q-mediated classical complement pathway and C1q-induced neutrophil chemotaxis, production of reactive oxygen species, cathepsin G, and myeloperoxidase. These findings suggest that the C1q-binding P5 peptide of EmCRT may serve as a potential target for the development of vaccines against echinococcosis or therapeutic drugs for complement-associated inflammatory or autoimmune diseases.
Full article
(This article belongs to the Special Issue Research Advances and New Perspectives on Helminthic Diseases)
►▼
Show Figures

Figure 1
Open AccessBrief Report
High Positivity Rate for Leptospira Infection in Symptomatic Urban Owned Dogs in Guayaquil, Ecuador
by
Solon Alberto Orlando, Naomi Mora Jaramillo, Ariana Montenegro Pesántez, Melissa Joseth Carvajal-Capa, Jose Julián Zuñiga-Velarde, Silvia Tafur and Miguel Angel Garcia-Bereguiain
Trop. Med. Infect. Dis. 2026, 11(6), 145; https://doi.org/10.3390/tropicalmed11060145 - 26 May 2026
Abstract
Leptospirosis is a zoonotic disease caused by spirochete bacteria of the genus Leptospira, with a wide global distribution. In Ecuador, leptospirosis is endemic, particularly in low-resource tropical areas, and multiple animal reservoirs have been identified either in rural or urban areas, including
[...] Read more.
Leptospirosis is a zoonotic disease caused by spirochete bacteria of the genus Leptospira, with a wide global distribution. In Ecuador, leptospirosis is endemic, particularly in low-resource tropical areas, and multiple animal reservoirs have been identified either in rural or urban areas, including stray dogs. In this study, a total of 81 domestic dogs presenting clinical manifestations compatible with leptospirosis were recruited at the Municipal Center for Animal Welfare in Guayaquil, Ecuador, in 2023. A survey regarding clinical, demographic, and environmental risk factors was filled in by every dog’s owner; urine and blood samples were collected for pathogenic Leptospira diagnosis by qPCR for lipL32, rrs, and secY gene targets. A very high (62.96%) positivity rate for Leptospira infection was found. Almost 90% of the dogs were not vaccinated against Leptospira. Although the animals exhibited multiple clinical signs, none showed a statistically significant association with Leptospira positivity, confirming the nonspecific presentation of the disease and its potential for misdiagnosis. The consumption of bulk food emerged as a significant environmental risk factor only in the multivariate logistic regression and not in the univariate analysis, suggesting the need for improved food safety practices. Moreover, we reported very frequent close-contact behaviors between owners and dogs. Overall, our study underscores the potential role of owned urban dogs as reservoirs of Leptospira in the city of Guayaquil in Ecuador, emphasizing the need for public health policies to increase awareness and improve diagnosis in domestic animals under a comprehensive One Health vision.
Full article
(This article belongs to the Special Issue Leptospirosis and One Health)
►▼
Show Figures

Figure 1
Open AccessArticle
Zoonotic Spillover of a Canine-like Rotavirus A G3P[3] Strain in a Brazilian Child
by
Vanessa Cristina Martins Silva, Lais Sampaio Azevedo, Raquel Guiducci and Adriana Luchs
Trop. Med. Infect. Dis. 2026, 11(6), 144; https://doi.org/10.3390/tropicalmed11060144 - 26 May 2026
Abstract
Rotavirus A (RVA) G3P[3] genotype is widely reported in dogs and less frequently in cats, with only sporadic human cases worldwide. All reported human infections have occurred in children, suggesting increased susceptibility likely linked to close contact with pets and age-related hygiene practices.
[...] Read more.
Rotavirus A (RVA) G3P[3] genotype is widely reported in dogs and less frequently in cats, with only sporadic human cases worldwide. All reported human infections have occurred in children, suggesting increased susceptibility likely linked to close contact with pets and age-related hygiene practices. The identification of a novel genotype constellation in Brazilian canine G3P[3] strains in 2017 prompted full-genotype characterization of the historical RVA/Human-wt/BRA/IAL-R451/2011/G3P[3] strain, previously sequenced only for VP7 and VP4, to define its genomic constellation and relatedness to canine strains. All 11 segments were analyzed by RT-PCR, sequencing and phylogenetics. The rare genotype–lineage constellation G3.III-P[3]-I2.XX-R3.II-C2.V-M3.II-A9-N2.XXIV-T3.II-E3.II-H6.I, shared with Brazilian canine strains, was identified, supporting a potential common origin. RVA/Human-wt/BRA/IAL-R451/2011/G3P[3] strain showed high genetic similarity (93.2–99%) with canine, feline and canine/feline-like human strains worldwide, with six genes (VP1, VP6 and NSP2–NSP5) closely related to Brazilian dog isolates (97.6–99%), indicating its canine origin. NSP2 clustered with strains from domestic (bovine), synanthropic (rat) and human hosts, while VP7 and VP4 were associated with wildlife (bat; raccoon dog) and environmental (sewage; river water) strains, supporting interhost reassortment and highlighting aquatic environments as reservoirs for interspecies transmission. Identification of new lineages (VP1, VP3 and NSP2) within the AU-1-like backbone reflects its underexplored diversity. This novel constellation likely circulated in dogs and may spill over to humans via close contact, reinforcing a One Health approach to understand RVA zoonotic risk, especially in hotspot regions like Brazil.
Full article
(This article belongs to the Special Issue Viral Enteropathogens in Pediatric Populations)
►▼
Show Figures

Figure 1
Open AccessArticle
Anthropophagy and Ecological Bridges: Blood-Meal Patterns of Invasive Aedes albopictus (Skuse, 1894) and Native Aedes aegypti Linnaeus, 1762 and Their Implications for Arbovirus Emergence in Central Africa
by
Armel N. Tedjou, Christophe R. Keumeni, Aurélie P. Yougang, Flobert Njiokou, Jo Lines, Sian E. Clarke, Charles S. Wondji and Basile Kamgang
Trop. Med. Infect. Dis. 2026, 11(6), 143; https://doi.org/10.3390/tropicalmed11060143 - 25 May 2026
Abstract
Aedes (Ae.) aegypti and Ae. albopictus are important vectors of arboviruses. Yet their blood-feeding pattern remains poorly characterised in Africa, including Cameroon. In this study, we characterised the blood-meal sources in both species collected from vegetation, household surroundings, and animal cages across four
[...] Read more.
Aedes (Ae.) aegypti and Ae. albopictus are important vectors of arboviruses. Yet their blood-feeding pattern remains poorly characterised in Africa, including Cameroon. In this study, we characterised the blood-meal sources in both species collected from vegetation, household surroundings, and animal cages across four urban sites, one rural site, and a zoo-botanical garden where humans and animals in captivity are the main hosts. Overall, Aedes mosquitoes represented about half of 10,054 female mosquitoes collected, with Ae. albopictus strongly dominating Ae. aegypti among 5001 Aedes females, and only 5.95% of females visibly blood-fed. Sequencing a 748 base pairs (bp) fragment of the cytochrome oxidase I gene from 156 blood-fed abdomens yielded 126 high-confidence host assignments, of which 98.25% were humans, indicating a strong anthropophagic pattern in both species. Unpredictably, two Ae. albopictus individuals had fed on a baboon (Papio anubis) and a frugivorous bat (Pteropodidae), as confirmed by bio informatic analyses, highlighting the species’ opportunistic blood-feeding nature and providing preliminary molecular evidence consistent with a potential bridge-vector role in this setting. Despite the extreme anthropophagy of both species observed, results indicate that Ae. albopictus could also serve as a bridge vector enabling spillover of enzootic viruses to humans, including urbanised settings where wild animals are present. These findings emphasise the urgent need for enhanced arbovirus surveillance in Central Africa using a One Health approach.
Full article
(This article belongs to the Topic Vector-Borne Disease Spatial Epidemiology, Disease Ecology, and Zoonoses)
►▼
Show Figures

Figure 1
Open AccessArticle
Evaluating the Usability, Durability, and Effectiveness of Permethrin-Treated Uniforms and Metofluthrin Spatial Repellent in Preventing Mosquito Bites in the Laos Military
by
Parat Boonyarangka, Pheutsapha Sonthilath, Sidhartha Chaudhury, Virasack Banouvong, Worachet Kuntawunginn, Siriporn Sornsakrin, Bounor Taobouathong, Thavone Sinhthapaseuth, Utaiwan Srichairatanakul, Montri Arsanok, Chanthalone Khamkong, Latsamee Lattavong, Raweewan Srisawat, Tharinee Saleepochn, Witcha Imaram, Alyssa Mann, Erica J. Lindroth, Bouasy Hongvanthong, James Jones and Krisada Jongsakul
Trop. Med. Infect. Dis. 2026, 11(5), 142; https://doi.org/10.3390/tropicalmed11050142 - 19 May 2026
Abstract
While vector control methods have successfully reduced malaria rates worldwide, such methods are not always suitable for military use. We evaluated the usability, durability, and effectiveness of permethrin-treated uniforms and metofluthrin spatial repellent in preventing mosquito bites among soldiers in the Laos People’s
[...] Read more.
While vector control methods have successfully reduced malaria rates worldwide, such methods are not always suitable for military use. We evaluated the usability, durability, and effectiveness of permethrin-treated uniforms and metofluthrin spatial repellent in preventing mosquito bites among soldiers in the Laos People’s Army that were deployed on a 12-week field exercise. The study enrolled 173 subjects into four different groups: (1) metofluthrin-only, (2) permethrin-treated uniforms, (3) metofluthrin with permethrin-treated uniforms, and (4) a control group. We measured efficacy through self-reported survey responses and a serological test for antibodies to Anopheles salivary antigens and assessed the durability of permethrin treatment over the 12-week exercise. We found that soldiers given metofluthrin and permethrin-treated uniforms were 72% and 46% more likely to report decreased mosquito bites compared to those in the control group and that soldiers with permethrin-treated uniforms had significantly lower (p < 0.05) antibody levels to the Anopheles SG6 salivary antigen. Mass spectrometry analysis revealed that treated uniforms still contained a significant permethrin concentration that showed 50 to 100% mosquito mortality. Overall, our findings show that both metofluthrin and permethrin-treated uniforms were well-tolerated and led to significantly fewer reported mosquito bites, and that permethrin, in particular, was found to be durable throughout the 12-week field exercise and effective in reducing mosquito bite exposure, underscoring its value in military applications.
Full article
(This article belongs to the Special Issue Military Medicine: An Everlasting War against Tropical and Infectious Diseases)
►▼
Show Figures
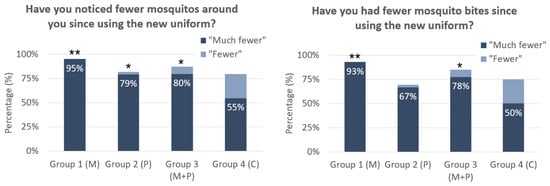
Figure 1
Open AccessPerspective
Tafenoquine: A Breakthrough Option for Babesiosis Treatment
by
Dongxue Ma, Mo Zhou, Shinuo Cao, Eloiza May Galon-Bedonia, Zhiqiang Xu, Chenghui Li, Xu Gao, Shujiang Xue and Shengwei Ji
Trop. Med. Infect. Dis. 2026, 11(5), 141; https://doi.org/10.3390/tropicalmed11050141 - 19 May 2026
Abstract
Babesiosis is a zoonosis caused by protozoan parasites of the genus Babesia. It has a worldwide distribution and affects many kinds of mammals, principally domestic animals and humans. Because there are no safe and effective vaccines available, the treatment and control for
[...] Read more.
Babesiosis is a zoonosis caused by protozoan parasites of the genus Babesia. It has a worldwide distribution and affects many kinds of mammals, principally domestic animals and humans. Because there are no safe and effective vaccines available, the treatment and control for babesiosis continues to involve the use of chemotherapeutics. For years, only a few drugs have been used for clinical treatment, namely atovaquone plus azithromycin or clindamycin plus quinine for human, and imidocarb dipropionate and diminazene aceturate for domestic animals. Although screening and developing alternative drugs are continuously pursued, only a few drugs have been prospected to have clinical applications. Of these, tafenoquine has shown wide and potent antibabesial activity, offering a new option to control babesiosis. This article aims to present the current clinical therapeutic strategies for babesiosis and their limitations, as well as the prospect of tafenoquine as a promising drug to treat babesiosis.
Full article
(This article belongs to the Special Issue New Strategies for the Diagnosis, Treatment and Risk Assessment of Parasitic Disease)
►▼
Show Figures

Figure 1
Open AccessArticle
Unveiling Clinical Phenotypes in Chronic Chikungunya Disease: Insights from a Brazilian Observational Study
by
Karen Santos Lima, Adriane Paz Rocha, Alice Lanna Damásio Castro, Anna Carolina Faria Moreira Gomes Tavares, Flávia Patrícia Sena Teixeira Santos, Gilda Aparecida Ferrreira, Livia Barbara Cordeiro Alves, Josiane Lino dos Santos Frattari, Juliana Froeseler Fittipaldi, Lucas Borba Paulino Coelho, Maria Fernanda Brandão de Resende Guimarães, Pedro Ribeiro de Jesus Almeida, Último Libânio Costa, Cristina Costa Duarte Lanna, Gustavo Gomes Resende and Mauro Martins Teixeira
Trop. Med. Infect. Dis. 2026, 11(5), 140; https://doi.org/10.3390/tropicalmed11050140 - 19 May 2026
Abstract
Chronic chikungunya disease (CCD) affects approximately 30–50% of infected individuals and is associated with persistent inflammatory arthritis, chronic pain, and long-term functional disability. We conducted a prospective observational cohort study including 584 patients with laboratory-confirmed chikungunya infection, evaluated between 3 and 12 months
[...] Read more.
Chronic chikungunya disease (CCD) affects approximately 30–50% of infected individuals and is associated with persistent inflammatory arthritis, chronic pain, and long-term functional disability. We conducted a prospective observational cohort study including 584 patients with laboratory-confirmed chikungunya infection, evaluated between 3 and 12 months after acute infection, to better understand the natural history, risk factors, clinical presentation, and treatment patterns of CCD. Here, we present a cross-sectional analysis derived from this cohort. Older age, female sex, and higher body mass index were identified as major risk factors for CCD. Four distinct clinical phenotypes were identified: Axial (12.2%), defined by inflammatory axial pain regardless of peripheral manifestations; Oligoarthritis (18.1%), defined by fewer than four swollen joints; Polyarthritis (10.6%), defined by four or more swollen joints; and Pain without Swelling (70.4%), characterized by myalgia and/or arthralgia in the absence of objective inflammatory findings on physical examination. The axial phenotype could overlap with peripheral phenotypes, whereas oligoarthritis, polyarthritis, and pain without swelling were mutually exclusive categories. These phenotypes differed substantially in symptom burden and clinical impact. Patients with the Pain without Swelling phenotype had longer symptom duration, whereas Axial and Polyarthritis phenotypes were associated with greater functional impairment and higher disease burden. These findings reinforce the clinical heterogeneity of CCD and support the potential value of phenotype-based approaches for clinical management and future therapeutic research.
Full article
(This article belongs to the Special Issue Arboviral Infections: Pathogenesis and Immunity)
►▼
Show Figures
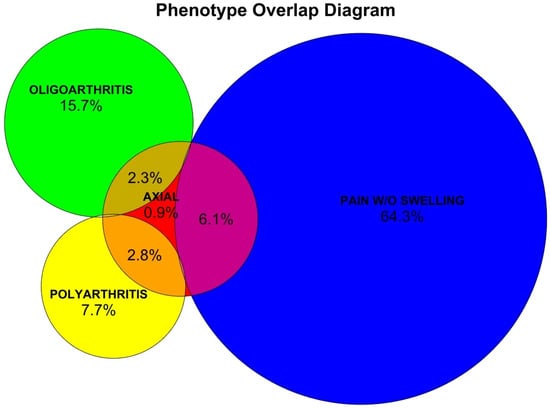
Figure 1
Open AccessEditorial
Biomarkers and Diagnostic and Therapeutic Approaches for Mycobacterial Diseases
by
Arshad Rizvi and Yash Gupta
Trop. Med. Infect. Dis. 2026, 11(5), 139; https://doi.org/10.3390/tropicalmed11050139 - 19 May 2026
Abstract
Mycobacterial diseases, particularly tuberculosis (TB), continue to impose a substantial global health burden, disproportionately affecting populations in low- and middle-income countries [...]
Full article
(This article belongs to the Special Issue Biomarkers, Diagnostic, and Therapeutic Approaches for Mycobacterial Diseases)
Open AccessCase Report
First Usutu Virus Infection in an Asymptomatic Blood Donor in Greece
by
Anna Papa, Katerina Tsioka, Styliani Pappa, Danai Pervanidou, Constantina Politis, Kostas Stamoulis and Vassiliki Bakaloudi
Trop. Med. Infect. Dis. 2026, 11(5), 138; https://doi.org/10.3390/tropicalmed11050138 - 18 May 2026
Abstract
►▼
Show Figures
Usutu virus (USUV) is a mosquito-borne flavivirus, widely distributed in Central Europe, where it causes avian outbreaks with large-scale mortality. Although most human infections are asymptomatic or mild, the reports of USUV neurologic infections are increasing, especially among immunocompromised patients. Cross-reactivity in serological
[...] Read more.
Usutu virus (USUV) is a mosquito-borne flavivirus, widely distributed in Central Europe, where it causes avian outbreaks with large-scale mortality. Although most human infections are asymptomatic or mild, the reports of USUV neurologic infections are increasing, especially among immunocompromised patients. Cross-reactivity in serological and molecular assays is often seen between USUV and the genetically and antigenically related West Nile virus (WNV). Here, we report the first USUV infection in Greece in an asymptomatic blood donor who tested positive in the automated nucleic acid test during screening for WNV, which is endemic in the country. Following the blood donation surveillance plan, a serum sample taken two weeks post-donation was tested for WNV IgM and IgG antibodies. The borderline index of the IgM antibodies, combined with negative result for IgG antibodies, raised the suspicion of molecular cross-reactivity with USUV. Although the USUV-specific PCR in donor’s plasma was negative, its result was positive following amplification of the virus in cell culture, as USUV RNA was detected in the culture supernatant confirming the USUV infection. Whole genome sequence was taken using an Ion Torrent next-generation sequencing platform. Phylogenetic analysis showed that the Greek strain clusters within the USUV Europe 2A genetic lineage. The detection of USUV human infection in Greece prompts for surveillance studies to elucidate its epidemiology and ecology in the country.
Full article

Figure 1
Open AccessArticle
Impact of Insecticide-Treated Nets on Plasmodium falciparum Infection Rates: A Meta-Analysis
by
Nevra Karaca Biçakçi, Ayşe Çalmaz, Merve Ayyildiz Akin, Ching Siang Tan, Jayanthi Barasarathi, Babatunji E. Oyinloye, Annaev Umidjon, Kuvonchbek Egamberdiyev and Intizor Avazmetova
Trop. Med. Infect. Dis. 2026, 11(5), 137; https://doi.org/10.3390/tropicalmed11050137 - 18 May 2026
Abstract
Insecticide-treated nets (ITNs), particularly long-lasting insecticide-treated nets (LLINs), are important for malaria control; however, the rise of insecticide resistance, behavioral adaptations in mosquito vectors, and diminishing net durability may affect their efficacy. The objective of this systematic literature review and meta-analysis to synthesize
[...] Read more.
Insecticide-treated nets (ITNs), particularly long-lasting insecticide-treated nets (LLINs), are important for malaria control; however, the rise of insecticide resistance, behavioral adaptations in mosquito vectors, and diminishing net durability may affect their efficacy. The objective of this systematic literature review and meta-analysis to synthesize recent epidemiological evidence (2021–2025) on the correlation between ITN/LLIN use and Plasmodium falciparum infection prevalence and to explore sources of heterogeneity across populations, settings, and type of nets. Searches across PubMed, Scopus, and Web of Science yielded 3151 records, of which 10 met the inclusion criteria. Two separate meta-analyses were performed for crude and adjusted effect estimates using random-effects models. The crude-effects meta-analysis included six studies comprising 7466 participants and yielded a pooled odds ratio of 0.67 (95% CI: 0.42–1.07; p = 0.078), indicating no statistically significant association between ITN/LLIN use and P. falciparum infection. Significant heterogeneity was observed (I2 = 79.8%), which was partially explained by population type (59.3%) and study design (36.1%). Subgroup analysis revealed comparable infection prevalence–based associations for ITNs (OR = 0.72) and LLINs (OR = 0.59) use. Assessment of publication bias indicated slight asymmetry; however, the trim-and-fill adjustment did not significantly change the conclusions. The adjusted-effects meta-analysis, comprising nine studies, yielded a non-significant pooled effect (aOR = 0.88; 95% CI: 0.42–1.86; p = 0.71) with substantial heterogeneity (I2 = 88.7%). Meta-regression analyses indicated that effect estimates varied by population group and country, with statistically significant modifiers observed for children under five years (p = 0.0098) and for studies conducted in Uganda (p = 0.0378). The type of net contributed to variation between studies, with insecticide-treated nets (ITNs) exhibiting lower pooled odds than long-lasting insecticide-treated nets (LLINs) (p = 0.0415). Overall, this meta-analysis found no conclusive evidence of a statistically significant association between ITN/LLIN use and P. falciparum infection in contemporary epidemiological studies. The substantial heterogeneity across settings underscores the context-dependent nature of observed associations and highlights the need for integrated vector-control strategies and continued evaluation of net technologies under conditions of increasing resistance.
Full article
(This article belongs to the Special Issue The Global Burden of Malaria and Control Strategies, 2nd Edition)
►▼
Show Figures

Figure 1
Open AccessArticle
Knowledge, Attitudes and Practices Regarding Rift Valley Fever Among Livestock Traders in the Alaotra Mangoro Region, Madagascar
by
Félix Alain, Botovola Miraimila, Véronique Chevalier and Peter N. Thompson
Trop. Med. Infect. Dis. 2026, 11(5), 136; https://doi.org/10.3390/tropicalmed11050136 - 16 May 2026
Abstract
Rift Valley fever (RVF) is a viral zoonosis endemic in Madagascar, threatening human and animal health as well as the economy. Trade-related livestock movements are a major factor in the spread of RVF virus. While previous RVF research in Madagascar has focused on
[...] Read more.
Rift Valley fever (RVF) is a viral zoonosis endemic in Madagascar, threatening human and animal health as well as the economy. Trade-related livestock movements are a major factor in the spread of RVF virus. While previous RVF research in Madagascar has focused on farmers or general ecology, this study is the first to specifically target livestock traders, the primary drivers for long-distance viral spread, in the Alaotra Mangoro endemic hotspot. This study aimed to assess the level of knowledge, prevailing attitudes and current practices regarding RVF among people engaged in livestock trade in the Alaotra Mangoro region, as well as the factors associated with these KAPs. A descriptive and analytical cross-sectional survey was conducted among 406 livestock traders in five districts of the Alaotra Mangoro region, using a structured questionnaire. A multi-stage sampling approach was employed, utilising purposive selection of markets followed by snowball sampling to reach informal traders often missed by traditional surveys. Generalised linear mixed models were used to analyse factors associated with KAPs regarding RVF. Awareness of RVF was very low (only 18.5% respondents had heard of it), with significant regional disparities (0% in Anosibe An’Ala versus 51.6% in Moramanga). Veterinarians (15.5%), family (12.8%), radio (9.6%) and neighbours (9.6%) were the main sources of information. Understanding of symptoms and modes of transmission (particularly mosquito bites) was limited. Higher levels of education (OR = 181.6; 95% CI: 29.9–1123.7; p < 0.001) and older age (50–60 years) were associated with better knowledge. Proactive attitudes were scarce (21.4%), although more than half (53.4%) believed that RVF is a real disease. Perception of personal risk and the contribution of livestock trade to the spread of the disease was low. However, confidence in animal vaccination was relatively high (60.3%). Preventive practices were highly inadequate. The majority did not wear protective equipment when handling sick animals (94.6%) and rarely avoided touching aborted foetuses (12.6%). Less than half (48.3%) expressed a willingness to report sick or dead animals, and nearly half admitted to having sold or purchased sick livestock (49.5%). Cooking meat (95.1%) and using mosquito nets (74.1%) were the only well-established practices. More than half of respondents (57.9%) lived more than 5 km from veterinary services, and cost was the most frequently cited barrier to consultation. Participation in awareness campaigns was virtually non-existent (5.4%). Results revealed critical gaps in KAP that may contribute to the persistence of RVF. A “One Health” approach is imperative, integrating human, animal and environmental health.
Full article
(This article belongs to the Section One Health)
►▼
Show Figures

Figure 1
Open AccessArticle
Human Metapneumovirus G Protein Immunogenicity and Safety Explored via Carrier Protein Fusion
by
Tian Ren, Kailun Ma, Xinmiao Lai, Jizheng Chen and Changgui Li
Trop. Med. Infect. Dis. 2026, 11(5), 135; https://doi.org/10.3390/tropicalmed11050135 - 15 May 2026
Abstract
Human metapneumovirus (HPMV) is a significant pathogen that causes lower respiratory tract infections. Given the weak immunogenicity thereof, and the few relevant studies, the utility of the viral membrane protein G as a vaccine remains controversial. In this study, the G extracellular domain
[...] Read more.
Human metapneumovirus (HPMV) is a significant pathogen that causes lower respiratory tract infections. Given the weak immunogenicity thereof, and the few relevant studies, the utility of the viral membrane protein G as a vaccine remains controversial. In this study, the G extracellular domain (RMG) of HMPV was expressed either alone or fused with the cholera toxin B subunit (CTB) and “cross-reacting material 197” (CRM197) carrier proteins (giving G-CTB/G and CRM197), to enhance immunogenicity. The non-glycosylated G protein (REG) expressed in Escherichia coli served as a control. SDS-PAGE and anti-His tag Western blotting verified that each protein was successfully expressed and correctly identified. BALB/c mice were immunized with each protein and subjected to challenge with HMPV. The results showed that, although immunization with RMG alone failed to induce potent neutralizing antibodies, it modestly reduced viral loads in the lungs of mice. However, the pathological damage caused by lung inflammation was more aggravated than that of the control challenge group. The level of specific IgG antibody induced by the recombinant G-CTB was significantly higher than that elicited by RMG. Compared to the RMG group, the viral load in the lungs of the G-CTB group tended to be reduced. Also, the damage caused by lung inflammation was significantly alleviated. Our study proves that HMPV G may be a valuable antigen in terms of HMPV vaccine development and offers a promising strategy for modulating the immunogenicity and safety thereof.
Full article
(This article belongs to the Special Issue Immune Responses in Respiratory Infections)
►▼
Show Figures

Figure 1
Open AccessArticle
Oviposition Deterrent and Larvicidal Activity of Salvia munzii Essential Oil Against Susceptible and Insecticide-Resistant Aedes aegypti
by
Selene M. Gutierrez-Rodriguez, Ivan Cordova-Guerreo, Laura Diaz-Rubio, Jesus A. Davila-Barboza, Iram P. Rodriguez-Sanchez, Beatriz Lopez-Monroy, Sergio A. Galindo-Rodriguez and Adriana E. Flores
Trop. Med. Infect. Dis. 2026, 11(5), 134; https://doi.org/10.3390/tropicalmed11050134 - 15 May 2026
Abstract
The increasing prevalence of insecticide resistance in Aedes aegypti threatens the effectiveness of chemical vector control and highlights the need for alternative approaches targeting mosquito behavior. This study evaluated the oviposition deterrent and larvicidal activity of Salvia munzii essential oil against insecticide-susceptible (New
[...] Read more.
The increasing prevalence of insecticide resistance in Aedes aegypti threatens the effectiveness of chemical vector control and highlights the need for alternative approaches targeting mosquito behavior. This study evaluated the oviposition deterrent and larvicidal activity of Salvia munzii essential oil against insecticide-susceptible (New Orleans; NO) and insecticide-resistant (Escobedo) Ae. aegypti strains. The essential oil, dominated by camphor (29.6%), 1,8-cineole (20.8%), and limonene (16.7%), was assessed through laboratory and semi-field bioassays. Larvicidal activity yielded LC50 values of 184.38 µg mL−1 for the susceptible strain and 305.04 µg mL−1 for the resistant strain, with a resistance ratio of 1.65, indicating susceptibility. Oviposition deterrence was quantified using the Oviposition Activity Index (OAI), and median repellent concentrations (RC50) were estimated. Under laboratory conditions, RC50 values were 1.65 µg mL−1 for the NO strain and 1.73 µg mL−1 for the Escobedo strain. Under semi-field conditions, the RC50 for the Escobedo strain decreased to 0.62 µg mL−1. Deterrent activity increased with concentration and persisted for up to 40 days, particularly at higher doses. These results demonstrate that S. munzii essential oil exhibits both larvicidal and oviposition deterrent activity against Ae. aegypti, including a pyrethroid-resistant population, under laboratory and semi-field conditions. The findings support further evaluation of S. munzii essential oil as a potential complementary tool for integrated vector management strategies.
Full article
(This article belongs to the Special Issue Insecticide Resistance and Vector Control, 2nd Edition)
►▼
Show Figures

Figure 1
Open AccessCase Report
Strongyloides stercoralis Hyperinfection Presenting as Diffuse Alveolar Hemorrhage in an Endemic Region: A Case Report
by
Juan Camilo Motta, Manuel Alejandro Delgado and Jacqueline Mugnier-Quijano
Trop. Med. Infect. Dis. 2026, 11(5), 133; https://doi.org/10.3390/tropicalmed11050133 - 14 May 2026
Abstract
Background: Strongyloides stercoralis is a soil-transmitted helminth capable of establishing chronic infection through an autoinfective cycle, with the potential to progress to life-threatening hyperinfection, particularly in immunocompromised individuals. Case Presentation: We report the case of a 70-year-old man from an endemic region in
[...] Read more.
Background: Strongyloides stercoralis is a soil-transmitted helminth capable of establishing chronic infection through an autoinfective cycle, with the potential to progress to life-threatening hyperinfection, particularly in immunocompromised individuals. Case Presentation: We report the case of a 70-year-old man from an endemic region in Colombia with metastatic urothelial carcinoma who developed hyperinfection syndrome following corticosteroid therapy for spinal cord compression. The patient presented with progressive respiratory failure and diffuse alveolar hemorrhage. Chest imaging showed bilateral ground glass opacities, and bronchoalveolar lavage revealed numerous larvae consistent with S. stercoralis, confirming the diagnosis. Despite supportive care and broad-spectrum antimicrobial therapy, the patient experienced rapid clinical deterioration and died. Conclusions: This case highlights the importance of considering strongyloidiasis in the differential diagnosis of diffuse alveolar hemorrhage in endemic settings, particularly in patients receiving corticosteroids. Early recognition and timely treatment are essential to reduce the high associated mortality. Preventive strategies, including targeted screening or empiric ivermectin administration prior to immunosuppression, should be considered in high-risk populations.
Full article
(This article belongs to the Special Issue Advances in Strongyloidiasis: Celebrating the Tenth Anniversary of Tropical Medicine and Infectious Disease and a Special Tribute in Memory of Professor Rick Speare (1946–2016))
►▼
Show Figures

Figure 1
Open AccessCase Report
Clinical Experience of Therapeutic Plasma Exchange (TPE) in Severe Leptospirosis: A Case Series from Sri Lanka
by
Manana Dewage Sankani Vishvara Kularathna and Senanayake Abeysinghe Mudiyanselage Kularatne
Trop. Med. Infect. Dis. 2026, 11(5), 132; https://doi.org/10.3390/tropicalmed11050132 - 12 May 2026
Abstract
Background: Leptospirosis is a globally prevalent zoonosis with significant morbidity and mortality, especially in tropical regions like South Asia. In its severe form, the disease often leads to multiorgan dysfunction, with pulmonary haemorrhage being a major cause of death. Evidence supporting specific treatments
[...] Read more.
Background: Leptospirosis is a globally prevalent zoonosis with significant morbidity and mortality, especially in tropical regions like South Asia. In its severe form, the disease often leads to multiorgan dysfunction, with pulmonary haemorrhage being a major cause of death. Evidence supporting specific treatments for severe leptospirosis with pulmonary involvement remains limited. Recent studies suggest that immunomodulatory therapies, such as therapeutic plasma exchange (TPE), may offer survival benefits. This case series explores the application and outcomes of TPE in patients with severe leptospirosis at a tertiary care hospital in Sri Lanka. Methods: We studied a case series involving nine patients with confirmed severe leptospirosis and multiorgan involvement from September 2021 to October 2022. All patients received standard care, including intravenous antibiotics and methylprednisolone. TPE was initiated in all nine patients based on clinical severity, particularly in the presence of pulmonary haemorrhage. Clinical, laboratory, and radiological data were collected from patient records and follow-up. Leptospirosis diagnosis was confirmed through ELISA IgM testing. TPE decisions were made by a multidisciplinary team. Results: Of the nine patients who received TPE, seven survived (78%). Pulmonary haemorrhage was the primary indication for TPE in all cases. All patients had multiorgan involvement: renal failure (89%), hepatic dysfunction (55%), and myocarditis (67%). Mortality was associated with inotropic-dependent myocarditis and mechanical ventilation at TPE initiation. Patients requiring intubation had a 50% mortality rate, compared to 14% in those who were not intubated. Non-survivors also had significantly elevated lactate levels (>4 mmol/L) and worsening acid–base status. Four patients required dialysis: three survived. Conclusions: Early initiation of TPE may be safe and beneficial in severe leptospirosis, and future randomised controlled studies are necessary to examine its benefits further. These findings are hypothesis-generating for further research, particularly on patient selection for TPE.
Full article
(This article belongs to the Section Infectious Diseases)
Open AccessSystematic Review
Spatiotemporal Patterns and Historical Overview of Aedes Mosquitoes in Iran: A Systematic Review
by
Jalil Nejati, Abedin Saghafipour, Mahsa Sarvi and Rubén Bueno-Marí
Trop. Med. Infect. Dis. 2026, 11(5), 131; https://doi.org/10.3390/tropicalmed11050131 - 12 May 2026
Abstract
Aedes mosquitoes are among the most important vectors of arboviral diseases such as dengue, Zika, and chikungunya. Mapping their geographic and temporal patterns is essential for understanding disease risk and guiding vector control. This systematic review provides an updated synthesis of the spatial
[...] Read more.
Aedes mosquitoes are among the most important vectors of arboviral diseases such as dengue, Zika, and chikungunya. Mapping their geographic and temporal patterns is essential for understanding disease risk and guiding vector control. This systematic review provides an updated synthesis of the spatial and temporal distribution of Aedes species across Iran. A comprehensive search of international (PubMed, Scopus, Web of Science) and national (SID, IranMedex, Magiran) databases was performed for studies published between 1980 and 2025. Eligible publications reporting the occurrence or distribution of Aedes mosquitoes were screened according to PRISMA guidelines. Data were extracted and analyzed descriptively to identify long-term spatial and temporal trends. Sixty-six studies met the inclusion criteria, covering more than 20 provinces and examining over 390,000 mosquito specimens. Aedes caspius was the dominant species nationwide, reflecting its high ecological adaptability. Invasive vectors, Ae. aegypti and Ae. albopictus, were recorded mainly in southern coastal provinces and, more recently, in the humid northern regions. Over time, surveys have evolved from scattered faunistic reports to systematic nationwide monitoring, revealing clear patterns of ecological expansion driven by climatic and environmental factors. Increasing reports, broader geographic distribution, and adaptability to diverse ecological settings indicate an ongoing expansion of Aedes mosquitoes in Iran. While these developments reflect successful entomological surveillance and public health efforts, enhanced preparedness and continuous monitoring are essential to manage potential Aedes-borne outbreaks effectively.
Full article
(This article belongs to the Special Issue Global Perspectives on the Role of Invasive Mosquito Species and Emerging Vector-Borne Diseases)
►▼
Show Figures

Figure 1

Journal Menu
► ▼ Journal Menu-
- TropicalMed Home
- Aims & Scope
- Editorial Board
- Topical Advisory Panel
- Instructions for Authors
- Special Issues
- Topics
- Sections & Collections
- Article Processing Charge
- Indexing & Archiving
- Editor’s Choice Articles
- Most Cited & Viewed
- Journal Statistics
- Journal History
- Journal Awards
- Society Collaborations
- Conferences
- Editorial Office
- 10th Anniversary
Journal Browser
► ▼ Journal BrowserHighly Accessed Articles
Latest Books
E-Mail Alert
News
26 May 2026
Meet Us at the 18th World Congress on Public Health, 6–8 September 2026, Cape Town, South Africa
Meet Us at the 18th World Congress on Public Health, 6–8 September 2026, Cape Town, South Africa

21 May 2026
Meet Us at the Northern European Conference on Travel Medicine (NECTM10), 3–5 June 2026, Belfast, UK
Meet Us at the Northern European Conference on Travel Medicine (NECTM10), 3–5 June 2026, Belfast, UK

Topics
Topic in
Infectious Disease Reports, Insects, IJERPH, Pathogens, TropicalMed, Zoonotic Diseases
Vector-Borne Disease Spatial Epidemiology, Disease Ecology, and Zoonoses
Topic Editors: Chad L. Cross, Louisa Alexandra MessengerDeadline: 31 December 2026
Topic in
IJERPH, TropicalMed, Microorganisms, Infectious Disease Reports, Pathogens
Genetic, Environmental, and Climatic Drivers of Emerging Arboviruses and Public Health Implications
Topic Editors: André Ricardo Ribas Freitas, Pedro María Alarcón-Elbal, Luciano Pamplona de Góes CavalcantiDeadline: 20 January 2027
Topic in
Diseases, Epidemiologia, Infectious Disease Reports, Medicina, TropicalMed
Surveillance Systems and Predictive Analytics for Epidemics
Topic Editors: Georgia Kourlaba, Elisavet StavropoulouDeadline: 31 January 2027

Conferences
Special Issues
Special Issue in
TropicalMed
Burden of Tuberculosis in Different Countries, 2nd Edition
Guest Editors: Mareli Claassens, Cari van Schalkwyk, Graeme HoddinottDeadline: 31 May 2026
Special Issue in
TropicalMed
Filarial Infections in Humans: Advances in Epidemiology and Immunological Insights
Guest Editor: Manuel RitterDeadline: 31 May 2026
Special Issue in
TropicalMed
Integrating Data-Driven Insights into Mathematical Modeling of Infectious Diseases
Guest Editors: Adejimi Adeniji, Kayode Oshinubi, Allan KomakechDeadline: 31 May 2026
Special Issue in
TropicalMed
HIV Testing, Prevention and Care Interventions, 2nd Edition
Guest Editors: Ricardo Izurieta, Enrique TeránDeadline: 31 May 2026
Topical Collections
Topical Collection in
TropicalMed
Infection Prevention and Control: Practical and Educational Advances
Collection Editors: Constantinos Tsioutis, Spyridon Karageorgos, Carlos Palos








