Journal Description
Pediatric Reports
Pediatric Reports
is an international, peer-reviewed, open access journal on all aspects of pediatrics, and is published bimonthly online by MDPI (since Volume 12, Issue 3 - 2020). The Italian Society of Pediatric Psychology (SIPPed) is affiliated with Pediatric Reports and its members receive discounts on the article processing charges.
- Open Access— free for readers, with article processing charges (APC) paid by authors or their institutions.
- High Visibility: indexed within Scopus, ESCI (Web of Science), PubMed, PMC, Embase, and other databases.
- Rapid Publication: manuscripts are peer-reviewed and a first decision is provided to authors approximately 31.7 days after submission; acceptance to publication is undertaken in 4.9 days (median values for papers published in this journal in the second half of 2025).
- Recognition of Reviewers: APC discount vouchers, optional signed peer review, and reviewer names published annually in the journal.
Impact Factor:
1.4 (2024);
5-Year Impact Factor:
1.2 (2024)
Latest Articles
Modified Tal (M-Tal) Score as a Predictor of Outcomes in Infants with Bronchiolitis: A Prospective Study
Pediatr. Rep. 2026, 18(3), 69; https://doi.org/10.3390/pediatric18030069 - 17 May 2026
Abstract
Background/Objectives: Bronchiolitis is the leading cause of hospitalization among infants, and early prediction of disease severity and clinical outcomes remains challenging. The Modified Tal (M-Tal) score is a clinical tool used to assess severity; however, its utility in predicting outcomes requires further validation.
[...] Read more.
Background/Objectives: Bronchiolitis is the leading cause of hospitalization among infants, and early prediction of disease severity and clinical outcomes remains challenging. The Modified Tal (M-Tal) score is a clinical tool used to assess severity; however, its utility in predicting outcomes requires further validation. Methods: This prospective study was conducted over a 2-year period at a tertiary care teaching hospital. Infants aged 1–12 months diagnosed with moderate-to-severe bronchiolitis were enrolled. Demographic, clinical, management, and outcome data were recorded. Results: A total of 120 infants were included (mean age 7.7 months; 61.7% males). Moderate bronchiolitis accounted for 81.7% of cases. The mean duration of illness at admission was 4.1 days. Severe bronchiolitis was associated with significantly longer duration of oxygen therapy (p = 0.034) and hospital stay (p = 0.028). Each one-point increase in M-Tal score was associated with an increase of 0.69 days in hospital stay (p = 0.012), 9.8 h in oxygen requirement (p < 0.01), and 0.32 days in PICU stay (p = 0.04). Conclusions: The M-Tal score at admission is a useful predictor of clinical outcomes in infants with moderate-to-severe bronchiolitis. Higher scores are associated with increased need for respiratory support and prolonged hospitalization, supporting its role in early risk stratification and management planning.
Full article
(This article belongs to the Special Issue Infectious Diseases in Children and Adolescents)
►
Show Figures
Open AccessArticle
Sleep Difficulties, Sleep Duration, and Sleeping Place in Early Childhood: A Longitudinal Study on Stability and Inter-Relations from 1 to 5 Years
by
Tanja Poulain, Juliane Ludwig, Nico Grafe, Andreas Merkenschlager and Wieland Kiess
Pediatr. Rep. 2026, 18(3), 68; https://doi.org/10.3390/pediatric18030068 - 14 May 2026
Abstract
Background/Objectives: This longitudinal study examined the association between sleep duration, sleep difficulties, and sleeping place at one year (t1) and corresponding characteristics at 4/5 years of age (t2). Methods: Data were collected from 2018 to 2021 (t1) and from 2021 to 2024 (t2)
[...] Read more.
Background/Objectives: This longitudinal study examined the association between sleep duration, sleep difficulties, and sleeping place at one year (t1) and corresponding characteristics at 4/5 years of age (t2). Methods: Data were collected from 2018 to 2021 (t1) and from 2021 to 2024 (t2) in the LIFE Child cohort study conducted in Leipzig, Germany. Parents completed the Brief Infant Sleep Questionnaire at t1 and the Child Sleep Habits Questionnaire at t2. Associations between sleep characteristics at t1 and t2 were estimated using linear and logistic regression models. All associations were adjusted for child sex, age at t2, and maternal education. Results: The analyses showed significant associations between shorter sleep durations, later sleep onset times, more frequent nightly awakenings and bed sharing and room sharing at t1 and more sleep difficulties at t2. A shorter sleep duration at t2 was predicted by shorter sleep and more parent-perceived sleep difficulties at t1. Bed sharing and room sharing at t1 were significantly associated with a lower probability of sleeping alone at t2. Conclusions: These results indicate that sleep duration, sleep difficulties, and sleeping places are already stable in early childhood.
Full article
(This article belongs to the Section Pediatric Psychology)
►▼
Show Figures

Figure 1
Open AccessArticle
Predictors of Length of Hospital Stay Among Under-Five Children with Clinical Pneumonia at a Rural Tertiary Hospital Setting in South Africa
by
Sanelisiwe Rosemary Mkhize, Olufunmilayo Olukemi Akapo, Siyonela Mlonyeni and Mirabel Kah-Keh Nanjoh
Pediatr. Rep. 2026, 18(3), 67; https://doi.org/10.3390/pediatric18030067 - 13 May 2026
Abstract
►▼
Show Figures
Background: Pneumonia of viral and polymicrobial origin predominates the pathological profile of clinical childhood pneumonia, with high admissions rates in recent times. Identifying factors associated with prolonged hospital stay may aid in developing risk reduction strategies for improved admission outcomes. Methods: A facility-based
[...] Read more.
Background: Pneumonia of viral and polymicrobial origin predominates the pathological profile of clinical childhood pneumonia, with high admissions rates in recent times. Identifying factors associated with prolonged hospital stay may aid in developing risk reduction strategies for improved admission outcomes. Methods: A facility-based historical cross-sectional study was conducted with a random selection of 186 medical records from January 2020 to December 2024 of children aged 0 to 5 with clinical pneumonia at a tertiary Hospital in Mthatha. Results: Over the five-year study period, clinical pneumonia accounted for 10.4% (95% CI: 9.8–11.1%, n = 950/9098) of the total under-five admissions. The median age was 108.5 (interquartile range (IQR) = 48.0–345.5) days, mainly comprising males (51.1%) and infants (65.2%), with viral (91.6%) and mild (88.0%) forms of pneumonia. The median length of hospital stay was 5 (IQR = 3.3–8) days, and 91 (49.5%) of the children had a prolonged hospital stay. In modified Poisson regression, infants [(relative risk (RR) = 2.7, 95% confidence interval (CI): 1.6–4.3), p < 0.001]; neonates (RR = 2.3, 95% CI: 1.2–4.6, p = 0.013); bacterial pneumonia (RR = 1.7, 95% CI: 1.2–2.6, p = 0.007); being hypoxic (RR = 2.2, 95% CI: 1.3–3.6, p = 0.003); absence of other respiratory tract infections (RR = 1.6, 95% CI: 1.2–2.1, p = 0.003), incomplete vaccination (RR = 1.5, 95% CI: 1.0–2.2, p = 0.038), non-usage of herbal medications (RR = 1.7, 95% CI: 1.3–2.2, p < 0.001), difficult breathing (RR = 1.7, 95% CI: 1.1–2.6, p = 0.028), current breastfeeding (RR = 0.6, 95% CI: 0.4–1.0, p = 0.048), other morbidities (RR = 0.7, 95% CI: 0.5–0.9, p = 0.002) were associated with prolonged length of hospital stay. Conclusion: Stratification of under-five children at admission according to age, type of pneumonia, vaccination status, and presence of other morbidities are needed to enhance monitoring and timely medical interventions.
Full article

Figure 1
Open AccessReview
Acquired Platelet Dysfunction with Eosinophilia: A Narrative Review
by
Anselm Chi-Wai Lee
Pediatr. Rep. 2026, 18(3), 66; https://doi.org/10.3390/pediatric18030066 - 7 May 2026
Abstract
Background. Acquired platelet dysfunction with eosinophilia (APDE) is a transient bleeding disorder initially thought to occur exclusively in Southeast Asia. There are no uniformly agreed diagnostic criteria, and its full clinical features have not been defined. Methods. A literature search was
[...] Read more.
Background. Acquired platelet dysfunction with eosinophilia (APDE) is a transient bleeding disorder initially thought to occur exclusively in Southeast Asia. There are no uniformly agreed diagnostic criteria, and its full clinical features have not been defined. Methods. A literature search was conducted through MEDLINE, EMBASE, and Google Scholar for publications on APDE in order to explore patient demography, epidemiology, diagnostic criteria, and laboratory findings of the disease. Results. Ten retrospective, observational studies, five case series, and 21 case reports were identified with a total of 431 patients. Diagnostic criteria varied, with a two-tier approach for the diagnosis of impaired platelet function. In recent years, cases of APDE have been reported extensively outside of the Malay peninsula. Male patients (243/390, 62.3%) predominated. Their ages ranged from 11 months to 30 years, with only 40 (9.3%) subjects aged 18 years or older. Eosinophilia was absent in 10 to 33% of subjects in a few observational studies. Thrombocytopenia was present in 42 (9.7%) subjects. Parasitic infestation was less common in the new millennium. Spontaneous recovery within six months was the trend, and serious complications were extremely rare. Conclusions. APDE is no longer restricted to Southeast Asia. A uniform set of diagnostic criteria is needed. Clinician awareness followed by reliable but easily available laboratory tests is essential to confirm diagnosis. It is proposed that rapid diagnosis can be accomplished by screening the blood smear for grey platelets by a trained examiner followed by confirmatory platelet aggregometry. National or international collaboration and prospective studies are required to delineate the core and variable clinical and laboratory features of APDE.
Full article
(This article belongs to the Collection Recent Advances and Critical Issues in Pediatrics: a Collection of Feature Papers)
►▼
Show Figures

Figure 1
Open AccessCase Report
Severe Macular Commotio Retinae Following a Fall from a Horse in a Pediatric Patient
by
Bogumiła Wójcik-Niklewska, Zofia Oliwa, Karina Dzięcioł and Adrian Smędowski
Pediatr. Rep. 2026, 18(3), 65; https://doi.org/10.3390/pediatric18030065 - 2 May 2026
Abstract
►▼
Show Figures
Background and Clinical Significance: Blunt ocular trauma is a significant but often underestimated cause of visual impairment, particularly among adolescents involved in high-risk activities such as horseback riding. While most equestrian injuries affect the head and extremities, ocular trauma, especially commotio retinae, can
[...] Read more.
Background and Clinical Significance: Blunt ocular trauma is a significant but often underestimated cause of visual impairment, particularly among adolescents involved in high-risk activities such as horseback riding. While most equestrian injuries affect the head and extremities, ocular trauma, especially commotio retinae, can result in severe visual complications. Case Presentation: We report the case of a 15-year-old girl who sustained blunt ocular trauma to the left eye following a fall from a horse and presented with decreased visual acuity. Multimodal imaging revealed outer retinal abnormalities on spectral-domain optical coherence tomography (OCT), including ellipsoid zone irregularities. Early-phase fluorescein angiography showed central hypofluorescence in the foveal region with surrounding mild mottled hyperfluorescence, without clear vascular abnormalities. Fundus photography demonstrated subtle macular changes. Visual acuity improved significantly following treatment, with partial resolution of macular changes, although mild outer retinal irregularities persisted on follow-up imaging. Conclusions: These findings underscore the importance of early ophthalmic evaluation and advanced retinal imaging in blunt ocular trauma. Given the high risk of visual injury during equestrian activities, especially in pediatric and adolescent populations, preventive strategies such as mandatory helmet use and rider education are essential. Implementation of standardized follow-up protocols is also recommended to monitor long-term retinal changes in patients with traumatic maculopathy.
Full article

Figure 1
Open AccessArticle
Mind the Gap: Exploring Parental Intentions, Actual Engagement, and Associated Outcomes in Tailored Digital Parent Training
by
Or Brandes, Chen R. Saar, Orly Sapir-Budnero and Amit Baumel
Pediatr. Rep. 2026, 18(3), 64; https://doi.org/10.3390/pediatric18030064 - 1 May 2026
Abstract
Background/Objectives: Digital parent training (DPT) programs offer scalable solutions for childhood disruptive behaviors but face significant engagement challenges. Although content tailoring may enhance outcomes, its clinical impact remains under-examined. This study aimed to (a) describe the correspondence between program recommendations, parental choices and
[...] Read more.
Background/Objectives: Digital parent training (DPT) programs offer scalable solutions for childhood disruptive behaviors but face significant engagement challenges. Although content tailoring may enhance outcomes, its clinical impact remains under-examined. This study aimed to (a) describe the correspondence between program recommendations, parental choices and engagement, and (b) examine how initial decisions are associated with subsequent engagement and therapeutic outcomes. Methods: A secondary analysis of three randomized trials included 151 parents of children (ages 3–7) with disruptive behaviors. Participants were classified as ‘Recommendation-Adherent’ (n = 63) or ‘Beyond-Recommendation’ (n = 88) based on whether initial content selections matched or exceeded program recommendations. Clinical outcomes (child behavior, parenting styles) and objective usage metrics were assessed at baseline and post intervention. Results: Many parents chose to expand the intervention scope beyond clinical recommendations (e.g., 91.5% selected the non-recommended Emotion Regulation module). However, this proactive initial intention did not increase objective engagement; groups did not differ significantly in total usage time, login days, or module completion rates. Although both groups showed comparable improvements in child behavior, intending to adhere to the recommended pathway was associated with significantly greater reductions in permissive parenting (laxness; p = 0.029) after adjusting for baseline differences. Conclusions: The findings highlight a discrepancy between parents’ intent to expand intervention scope and their actual engagement capacity. While the decision to adhere to a tailored pathway was associated with specific improvements in permissive parenting, the observational nature of the study precludes causal claims. Nevertheless, the results suggest that guided tailoring may serve as a protective function against choice overload. Aligning program demands with the practical realities of parental effort could help families focus finite energy on essential clinical targets.
Full article
(This article belongs to the Section Pediatric Psychology)
►▼
Show Figures

Figure 1
Open AccessBrief Report
Point-of-Care Ultrasound Detects Rapid Muscle Loss in Pediatric ECMO Patients—A Secondary Analysis Paper
by
Mohammad Sabobeh, Elizabeth Seewer, William Hunt Stafford, Nicolas Chiriboga, Thomas Spentzas, Shyam Popat, Alyssa Clark, David B. Kantor, Hitesh S. Sandhu and Saad Ghafoor
Pediatr. Rep. 2026, 18(3), 63; https://doi.org/10.3390/pediatric18030063 - 1 May 2026
Abstract
Background: Critically ill children requiring extracorporeal membrane oxygenation (ECMO) support are at high risk of immobility, deconditioning, and muscle loss. There is a lack of screening and diagnostic tools to quantify muscle loss in this population. Objective: This study aims to evaluate the
[...] Read more.
Background: Critically ill children requiring extracorporeal membrane oxygenation (ECMO) support are at high risk of immobility, deconditioning, and muscle loss. There is a lack of screening and diagnostic tools to quantify muscle loss in this population. Objective: This study aims to evaluate the use of bedside ultrasound as a practical and effective method for detecting muscle loss in this high-risk group. Materials and Methods: This is a secondary analysis of a prospective observational clinical study conducted between January 2024 and January 2025 that used ultrasound to describe muscle loss in critically ill children aged 2 to 18 years. Results: The primary study enrolled 35 patients, five of whom required ECMO support. All patients who required ECMO showed significant muscle loss (>10%) in the quadriceps femoris, as measured by muscle thickness and cross-sectional area, compared with baseline measurements obtained before ECMO cannulation. Conclusions: Point-of-care muscle ultrasound could be a reliable, cost-effective tool for assessing muscle loss in pediatric patients on ECMO.
Full article
(This article belongs to the Collection Recent Advances and Critical Issues in Pediatrics: a Collection of Feature Papers)
►▼
Show Figures

Figure 1
Open AccessArticle
Fractional Exhaled Nitric Oxide in Children with Non-Cystic Fibrosis Bronchiectasis: Associations with Etiology, Lung Function, and CT Extent
by
Taner Adiguzel and Bulent Karadag
Pediatr. Rep. 2026, 18(3), 62; https://doi.org/10.3390/pediatric18030062 - 1 May 2026
Abstract
Background/Objectives: Childhood non-cystic fibrosis (non-CF) bronchiectasis is clinically heterogeneous. We aimed to describe fractional exhaled nitric oxide (FeNO) levels in affected children and examine associations with etiology, spirometry, and CT-defined disease extent. Methods: This single-center prospective observational study included 100 clinically stable children
[...] Read more.
Background/Objectives: Childhood non-cystic fibrosis (non-CF) bronchiectasis is clinically heterogeneous. We aimed to describe fractional exhaled nitric oxide (FeNO) levels in affected children and examine associations with etiology, spirometry, and CT-defined disease extent. Methods: This single-center prospective observational study included 100 clinically stable children aged 6–18 years with CT-confirmed non-CF bronchiectasis evaluated between September 2014 and December 2015. FeNO was measured before spirometry using an online single-breath electrochemical technique. Chest CT was reviewed at the lobar level, with the lingula counted separately, and disease extent was summarized by the number of involved lobar regions. Associations were assessed using Spearman correlation and non-parametric tests. Results: Mean age was 14.9 ± 2.0 years, 55% were male, and mean FeNO was 20.9 ± 14.0 ppb. FeNO correlated positively with FEV1 (% predicted), FVC (% predicted), and FEF25–75 (% predicted) (all p < 0.01). FeNO was higher in males and adolescents than in females and younger children, respectively. FeNO did not differ by CT-defined lobar extent. It was lower in primary ciliary dyskinesia than in asthma overlap. Overall, 82% of the cohort received an ICS-containing maintenance regimen and household tobacco smoke exposure was present in 58%. Conclusions: FeNO was associated with selected functional indices and etiologic subgroups, but not with CT-defined structural extent, suggesting a greater role in clinical phenotyping than in reflecting radiologic burden. Rather than reflecting overall disease severity, FeNO may be more relevant as a marker of T2-leaning airway inflammatory phenotype in selected children with non-CF bronchiectasis. These findings should be interpreted as exploratory and hypothesis-generating, particularly for etiologic subgroup comparisons and for FeNO interpretation in the setting of treatment and environmental confounding.
Full article
Open AccessArticle
Evaluation of Parental Knowledge and Practices in Pediatric Fever Management Among Iranian Families: A Cross-Sectional Study
by
Tarlan Soumei, Sara Hamideh Kerdar, David D. Martin, Parviz Rafiezadeh and Ekkehart Jenetzky
Pediatr. Rep. 2026, 18(3), 61; https://doi.org/10.3390/pediatric18030061 - 22 Apr 2026
Abstract
►▼
Show Figures
Background/Objectives: Fever is a common concern among parents, often leading to heightened anxiety and misconceptions about its management. While fever phobia has been extensively studied in Western countries, data from the Middle East—particularly Iran—remain limited. Understanding parental knowledge and anxiety in this
[...] Read more.
Background/Objectives: Fever is a common concern among parents, often leading to heightened anxiety and misconceptions about its management. While fever phobia has been extensively studied in Western countries, data from the Middle East—particularly Iran—remain limited. Understanding parental knowledge and anxiety in this cultural context is essential for developing targeted educational interventions. This study aims to assess parental knowledge, behavior, and anxiety regarding fever in children and to identify factors associated with higher levels of anxiety among Iranian parents, thereby contributing culturally specific evidence to the international literature on pediatric fever management. Methods: A cross-sectional study was conducted involving 552 parents from Tehran, Iran, recruited through convenience sampling. Data were collected using self-administered questionnaires assessing demographic characteristics, knowledge about fever, treatment practices, and anxiety levels using a 10-point Likert scale. Principal component analysis (PCA) was performed to examine the underlying factors influencing parents’ decisions to reduce fever. Univariate and multivariate linear regression analyses on standardized z-values were conducted to determine the predictors of fever-related anxiety. Results: Results showed that 67.4% of parents experienced anxiety when managing their child’s fever, with 65.6% perceiving fever as harmful. Fear of febrile seizures (77.4%) and brain damage were significant concerns motivating parents to reduce fever. Female parental sex (β = 0.336, p = 0.004) and the perception of fever as harmful (β = 0.058, p < 0.001) were the strongest predictors of fever-related anxiety. The PCA identified two key factors influencing fever management behavior: well-being protection and medical risk prevention. Parents commonly treated fever using combinations with either Paracetamol or Ibuprofen (47.6%). Conclusions: Parental anxiety about fever in Iran is largely driven by misconceptions, especially regarding febrile seizures and brain damage. Culturally tailored education and clear communication from healthcare providers are essential to reduce these fears, improve fever management, and decrease unnecessary antipyretic use.
Full article

Figure 1
Open AccessArticle
The Predictive Power of Early Socio-Emotional Skills on Behavioral Outcomes in Very Preterm Preschoolers: A Longitudinal Study
by
Chiara Ionio, Caterina Colombo, Francesco Cavigioli, Francesca Sala, Rachele Cantella, Marina Balestriero, Giovanna Cardile, Giulia Ciuffo and Gianluca Lista
Pediatr. Rep. 2026, 18(2), 60; https://doi.org/10.3390/pediatric18020060 - 20 Apr 2026
Abstract
Background: Preterm birth increases the risk of socio-emotional difficulties and later behavioral problems. Early identification is essential, but the predictive value of socio-emotional assessments at different ages remains uncertain. Aim: This study sought to examine whether socio-emotional skills at 1, 2, and 3
[...] Read more.
Background: Preterm birth increases the risk of socio-emotional difficulties and later behavioral problems. Early identification is essential, but the predictive value of socio-emotional assessments at different ages remains uncertain. Aim: This study sought to examine whether socio-emotional skills at 1, 2, and 3 years predict behavioral outcomes at 4 years in very preterm children. Methods: Fifty-seven preterm children were assessed longitudinally with the Bayley-III Socio-Emotional scale at 1, 2, and 3 years, and with the CBCL 1.5–5 at 4 years. Analyses included correlations, repeated-measures ANOVA, and regression models. Results: Mean socio-emotional scores were within the normative range at all ages, with a modest increase by age 3. Associations were observed between socio-emotional skills at 1 year and behavioral outcomes at 4 years, particularly internalizing and total problems. These associations were weaker at 2 years and not evident at 3 years. Regression analyses indicated that only 1-year socio-emotional scores were significantly associated with later outcomes, although models were unadjusted. Conclusions: Socio-emotional competencies at 1 year were associated with later behavioral outcomes in this sample of very preterm children. These findings suggest that early assessments may contribute to identifying children who could benefit from closer developmental monitoring, although further research with adjusted models is needed.
Full article
(This article belongs to the Special Issue The Developing Child: Integrating Emotional and Physical Health)
Open AccessArticle
Prevalence of Glucose-6-Phosphate Dehydrogenase (G6PD) Deficiency and Risk of Hyperbilirubinemia Among Newborns: A Tertiary Center Experience from Western Saudi Arabia
by
Rogaya AlShugair, Mansour Al-Qurashi, Ahmad Mustafa, Mohammad Y. Alhindi, Abrar Ahmed, Hend AlNajjar, Mona AlDabbagh, Ashraf Sahafi, Hashim Almarzouki, Nabila A. AlRashdi, Eman A. AlThobaiti and Syed Sameer Aga
Pediatr. Rep. 2026, 18(2), 59; https://doi.org/10.3390/pediatric18020059 - 15 Apr 2026
Abstract
Background: Glucose-6-phosphate dehydrogenase (G6PD) deficiency is among the most common inherited enzymatic disorders worldwide and is an important risk factor for neonatal hyperbilirubinemia. Regional data from Western Saudi Arabia based on universal newborn screening remain limited. Objectives: To determine the prevalence of G6PD
[...] Read more.
Background: Glucose-6-phosphate dehydrogenase (G6PD) deficiency is among the most common inherited enzymatic disorders worldwide and is an important risk factor for neonatal hyperbilirubinemia. Regional data from Western Saudi Arabia based on universal newborn screening remain limited. Objectives: To determine the prevalence of G6PD deficiency among newborns delivered at a tertiary center in Jeddah, Saudi Arabia, and to evaluate its association with clinically relevant outcomes, including early-onset jaundice (<24 h), need for phototherapy, admission for hyperbilirubinemia management, and readmission after discharge. Methods: We conducted a retrospective cohort study at King Abdulaziz Medical City, Western Region, Jeddah, Saudi Arabia, between January 2020 and May 2025. Cord blood samples from live-born infants were screened using a qualitative fluorescent spot test. Demographic variables (sex, gestational age, birth weight) and jaundice-related outcomes were extracted from the electronic medical record. Categorical variables were compared using chi-square testing, with p < 0.05 considered statistically significant. Results: Among 14,964 screened newborns, 489 were identified as G6PD deficient, yielding a prevalence of 3.3%. Prevalence was higher in males than in females (5.6% vs. 0.9%). Among the G6PD-deficient infants, early-onset jaundice occurred in 17.2%, phototherapy was required in 36.0%, and 16.5% were admitted for hyperbilirubinemia management. Readmission for worsening jaundice requiring phototherapy occurred in 11.0%, and no exchange transfusions were required. Compared with term infants, late preterm infants had higher rates of early-onset jaundice (11/49, 22.4% vs. 73/440, 16.6%) and phototherapy use (22/49, 45.0% vs. 154/440, 35.0%) (p < 0.01). Conclusions: G6PD deficiency was identified in a substantial proportion of newborns in this large screened cohort and was associated with clinically significant jaundice-related outcomes, particularly among late preterm infants. These findings underscore the importance of universal screening and structured postnatal follow-up to reduce the risk of severe hyperbilirubinemia and its complications. Early identification of G6PD-deficient infants should be accompanied by careful bilirubin monitoring, clear discharge planning, and timely post-discharge follow-up, especially for those born late preterm.
Full article
(This article belongs to the Special Issue Global Neonatal Screening: Expanding Horizons in Diagnostic Technologies)
►▼
Show Figures

Figure 1
Open AccessReview
Admission Criteria to Paediatric Intensive Care for Oncology Haematology Patients: Updates and Evidence-Based Clinical Recommendations
by
Ivonne Portaccio, Enzo Picconi, Tony Christian Morena, Giorgio Conti and Marco Piastra
Pediatr. Rep. 2026, 18(2), 58; https://doi.org/10.3390/pediatric18020058 - 14 Apr 2026
Abstract
Background: The landscape of paediatric oncology has undergone a remarkable transformation over recent decades. Advances in both oncological and supportive therapies have dramatically improved survival in children with haematological malignancies and solid tumours, with current survival rates exceeding 80% for many childhood cancers.
[...] Read more.
Background: The landscape of paediatric oncology has undergone a remarkable transformation over recent decades. Advances in both oncological and supportive therapies have dramatically improved survival in children with haematological malignancies and solid tumours, with current survival rates exceeding 80% for many childhood cancers. However, this therapeutic success has brought with it an unexpected consequence: the intensification of treatment protocols has led to a parallel increase in life-threatening complications requiring intensive care support. Current evidence indicates that up to 40% of paediatric oncology patients will require admission to a Paediatric Intensive Care Unit (PICU) at some point during their disease trajectory. Objectives: This comprehensive review synthesises current evidence to provide an updated framework for PICU admission decision-making in oncology haematology patients. We have integrated the most recently published international guidelines, including the groundbreaking Phoenix 2024 sepsis criteria and the updated PALICC-2 2023 recommendations for paediatric acute respiratory distress syndrome. Beyond establishing admission criteria, we critically analyse the efficacy of advanced support strategies and examine emerging therapeutic approaches in this uniquely vulnerable population. Methods: Our methodology encompassed a systematic review of the literature published between 2011 and 2024, complemented by a detailed analysis of current international guidelines and expert consensus statements. We included randomised controlled trials, observational studies, meta-analyses, and consensus conference proceedings specifically addressing the intensive care management of paediatric patients with oncological or haematological conditions. Main Results: Several key findings emerge from our analysis. The Phoenix 2024 criteria represent a fundamental reconceptualisation of paediatric sepsis diagnosis, validated through an unprecedented dataset encompassing more than 3 million paediatric encounters. In the realm of respiratory support, early implementation of non-invasive ventilation (NIV) or continuous positive airway pressure (CPAP) has demonstrated remarkable efficacy, reducing the need for invasive mechanical ventilation by 45% (RR 0.45, 95% CI 0.26–0.78) when applied to appropriately selected patients. Extracorporeal membrane oxygenation (ECMO), whilst increasingly utilised, shows survival to decannulation ranging from 52% to 64%, though survival to hospital discharge remains less encouraging at 36–42%. Continuous renal replacement therapy (CRRT) has proven highly effective for tumour lysis syndrome, achieving metabolic correction in 90% of severe cases. Perhaps most promisingly, emerging biomarkers—particularly interleukin-6, interleukin-10, and procalcitonin—have substantially enhanced our ability to stratify infection risk, demonstrating sensitivity exceeding 85% for bacteraemia detection. Conclusions: The evidence unequivocally supports several core principles for optimising outcomes in this population. Early identification of deterioration through validated scoring systems enables timely intervention before irreversible organ failure develops. Prompt implementation of non-invasive respiratory support, when appropriately applied, can obviate the need for mechanical ventilation with its attendant complications. Perhaps most critically, centralisation of care in centres with dedicated expertise and comprehensive support capabilities fundamentally improves survival. These findings argue compellingly for the establishment of a formal national network of reference centres, implementing standardised protocols and structured care pathways specifically designed for critically ill paediatric oncology haematology patients.
Full article
Open AccessCase Report
A Case Report of Vitamin C Deficiency Mimicking Osteomyelitis
by
Akash Daswaney, Nirali Borad, Anhthu Trinh, Stephanie Thompson and Youmna Mousattat
Pediatr. Rep. 2026, 18(2), 57; https://doi.org/10.3390/pediatric18020057 - 14 Apr 2026
Abstract
►▼
Show Figures
Vitamin C, also known as ascorbic acid, plays a pivotal role in forming blood vessels, cartilage, muscles, and collagen in bones. We report a 6-year-old non-verbal female with global developmental delay who presented with complaints of lower limb pain and inability to bear
[...] Read more.
Vitamin C, also known as ascorbic acid, plays a pivotal role in forming blood vessels, cartilage, muscles, and collagen in bones. We report a 6-year-old non-verbal female with global developmental delay who presented with complaints of lower limb pain and inability to bear weight. Symptoms started five weeks prior to presentation and had progressed from decreased activity to complete loss of weight-bearing. Physical examination showed gingival hyperplasia, perifollicular petechiae, lower limb edema, and corkscrew hair. Initial radiologic findings raised concerns of osteomyelitis, showing bone marrow edema, periosteal reaction, and cortical irregularity. However, correlation with dietary history limited to flavored milk and yogurt and lacking fruits and vegetables, in conjunction with clinical presentation, suggested vitamin C deficiency, and she was started on ascorbic acid. Vitamin C deficiency was later confirmed on day 7 by a low C deficiency level (<0.1 mg/dL). Treatment with ascorbic acid, multivitamins, and supportive therapy led to gradual recovery, and gastrostomy tube placement facilitated supplementation. This case highlights the importance of detailed dietary history and recognition of clinical signs of vitamin C deficiency. Early dietary assessment and clinical correlation can prevent unnecessary invasive procedures and prolonged antibiotic therapy. Early identification enables timely intervention, reducing morbidity and improving quality of life.
Full article

Figure 1
Open AccessArticle
Comparison of Postoperative Outcomes of Duhamel and Transanal Endorectal Pull-Through in Hirschsprung Disease: A Propensity Score Study
by
Jiraporn Khorana, Juthamas Jenyongsak, Kanokkan Tepmalai and Sireekarn Chantakhow
Pediatr. Rep. 2026, 18(2), 56; https://doi.org/10.3390/pediatric18020056 - 13 Apr 2026
Abstract
►▼
Show Figures
Background/Objectives: Hirschsprung disease (HSCR) is a congenital condition characterized by absence of ganglion cells in the distal bowel. The principle of surgical treatment is resection of the aganglionic bowel with restoration of intestinal continuity. Several operative techniques have been developed. This study aimed
[...] Read more.
Background/Objectives: Hirschsprung disease (HSCR) is a congenital condition characterized by absence of ganglion cells in the distal bowel. The principle of surgical treatment is resection of the aganglionic bowel with restoration of intestinal continuity. Several operative techniques have been developed. This study aimed to compare outcomes between the Duhamel procedure and transanal endorectal pull-through (TERPT) in Hirschsprung disease using propensity score-based methods. Methods: Hirschsprung patients who underwent Duhamel or TERPT from January 2006 to December 2021 were included. The primary outcome was a composite endpoint at 6 months comprising obstructive symptoms, fecal soiling, or Hirschsprung-associated enterocolitis. Propensity scores were estimated via logistic regression incorporating eight preoperative covariates. The primary analysis employed overlap weighting (ATO), with multiple sensitivity analyses performed to assess robustness. Results: A total of 239 patients were included (TERPT, n = 181; Duhamel, n = 58). Before weighting, seven of eight covariates demonstrated meaningful imbalance (SMD > 0.10); ATO weighting achieved satisfactory balance across all covariates (all SMD < 0.10). A good composite outcome was achieved in 51.9% of TERPT and 53.4% of Duhamel patients, with no significant difference in the primary ATO-weighted analysis (OR 0.94, 95% CI 0.39–2.28; p = 0.897). No significant differences were observed in individual outcome components. Findings were consistent across all sensitivity analyses. TERPT was associated with significantly shorter operative time, lower estimated blood loss, and shorter hospital stay (all p < 0.001). Conclusions: No statistically significant differences were detected in 6-month postoperative functional outcomes between TERPT and the Duhamel operation. TERPT was associated with improved perioperative outcomes. However, these findings should be interpreted with caution due to limited statistical power and baseline differences between groups. Prospective multicenter studies with standardized outcome definitions and longer follow-up are warranted.
Full article

Figure 1
Open AccessCase Report
Candida dubliniensis as a Cause of Chronic Meningitis in a 3-Year-Old Boy with Acute Lymphoblastic Leukemia
by
Adrianna Ćwiertnia, Laura Chuchla and Tomasz Ociepa
Pediatr. Rep. 2026, 18(2), 55; https://doi.org/10.3390/pediatric18020055 - 12 Apr 2026
Abstract
►▼
Show Figures
Candida dubliniensis is an opportunistic yeast closely related to Candida albicans and an uncommon cause of central nervous system (CNS) infection. While isolates are often susceptible to azoles, reduced susceptibility or acquired resistance may occur, making species identification and antifungal susceptibility testing clinically
[...] Read more.
Candida dubliniensis is an opportunistic yeast closely related to Candida albicans and an uncommon cause of central nervous system (CNS) infection. While isolates are often susceptible to azoles, reduced susceptibility or acquired resistance may occur, making species identification and antifungal susceptibility testing clinically relevant. We report a 3-year-old boy with Philadelphia chromosome-positive B-cell precursor acute lymphoblastic leukemia (ALL) in hematologic remission who developed chronic meningitis during maintenance chemotherapy. The initial presentation was non-specific (marked somnolence without fever or meningeal signs) and lumbar puncture performed to exclude CNS relapse revealed neutrophil-predominant pleocytosis and elevated protein; the cerebrospinal fluid (CSF) culture grew C. dubliniensis. Treatment with intravenous liposomal amphotericin B followed by prolonged fluconazole led to clinical improvement and sterile CSF. Six months later, progressive gait disturbance, limb pain, and episodic severe headaches recurred; repeat CSF cultures again yielded C. dubliniensis, with a changed susceptibility profile. Spine MRI demonstrated leptomeningeal enhancement involving the cauda equina nerve roots. Intravenous voriconazole with therapeutic drug monitoring was initiated and combined with intrathecal liposomal amphotericin B (seven doses, dose-escalated up to 3 mg), which was well tolerated and associated with rapid neurologic improvement, CSF sterilization, and radiologic resolution. At 12 months of follow-up, the patient remained infection-free and in leukemia remission. This case highlights that C. dubliniensis chronic meningitis may present subtly yet progress, requiring repeated CSF cultures with susceptibility testing; intrathecal liposomal amphotericin B can be a safe and effective adjunct to systemic therapy in refractory or recurrent disease.
Full article

Figure 1
Open AccessCase Report
Pediatric Autoimmune Sclerosing Cholangitis: Diagnostic and Therapeutic Challenges
by
Raisa-Maria Sucaciu, Alina Grama, Alexandra Mititelu, Bianca Raluca Mariș, Ioana Filimon, Bobe Petrushev, Daniel Cristian Popescu, Gabriel Benţa and Tudor Lucian Pop
Pediatr. Rep. 2026, 18(2), 54; https://doi.org/10.3390/pediatric18020054 - 8 Apr 2026
Cited by 1
Abstract
Background. Autoimmune sclerosing cholangitis (ASC) is a rare clinical entity characterized by overlapping features of autoimmune hepatitis and primary sclerosing cholangitis. It predominantly affects pediatric patients. Therapeutic management is often complex, requiring a multidisciplinary and individualized approach, especially in the context of associated
[...] Read more.
Background. Autoimmune sclerosing cholangitis (ASC) is a rare clinical entity characterized by overlapping features of autoimmune hepatitis and primary sclerosing cholangitis. It predominantly affects pediatric patients. Therapeutic management is often complex, requiring a multidisciplinary and individualized approach, especially in the context of associated autoimmune diseases. Case presentation. We present the case of a female patient diagnosed at the age of 10 with ASC, for which immunosuppressive therapy with prednisone, azathioprine (AZA), and ursodeoxycholic acid (UDCA) was initiated, with an initially favorable course. One year later, following a Severe Acute Respiratory Syndrome Coronavirus-2 (SARS-CoV-2) infection, the patient experienced reactivation of liver disease and subsequently developed ulcerative pancolitis (UC), for which 5-aminosalicylic acid (5-ASA) therapy was initiated. Due to repeated hepatic flares and/or colitis relapses, therapy was escalated successively to mycophenolate mofetil, tacrolimus, and eventually infliximab (IFX). Despite treatment, the liver disease progressed, culminating in liver cirrhosis. Our patient developed portal hypertension and esophageal varices, with two episodes of upper gastrointestinal bleeding requiring endoscopic band ligation. At the age of 14, the patient developed recurrent episodes of non-infectious ulcerative stomatitis. Biopsy of the lesions revealed non-specific chronic inflammation, unrelated to colitis activity (confirmed microscopic remission of UC). By exclusion, an adverse drug reaction was suspected, with AZA being the most likely cause. Following its discontinuation, the lesions resolved. Beyond the physiological and therapeutic aspects, the patient displays marked emotional fragility due to prolonged and repeated hospitalizations (18 out of 60 months), which have impacted treatment adherence. Conclusions. This case highlights the complexity of managing pediatric patients with multiple autoimmune diseases. The necessary combination of immunosuppressive therapies may lead to significant adverse effects and further complicate disease progression. Moreover, psychological components play a crucial role in treatment compliance and therapeutic success, emphasizing the need for an integrated approach that includes specialized psychological support.
Full article
(This article belongs to the Special Issue Advanced Diagnostic and Treatment Approach in Pediatric Hepatology)
►▼
Show Figures
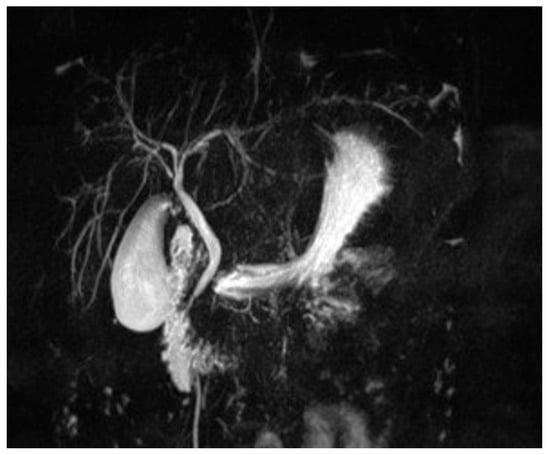
Figure 1
Open AccessArticle
Internet Gaming Disorder and Internet Addiction: Comparing Italian and Migrant Children and Adolescents
by
Giovanni Giulio Valtolina, Diego Boerchi and Luca Milani
Pediatr. Rep. 2026, 18(2), 53; https://doi.org/10.3390/pediatric18020053 - 7 Apr 2026
Abstract
Background: research suggests that adolescents with a migrant background may be particularly vulnerable to behavioral addictions, including problematic gaming and Internet use. Methods: we compared Italian (ITA) and non-Italian (WIC) students on Internet Gaming Disorder (IGD) and Internet Addiction (IA) and examined whether
[...] Read more.
Background: research suggests that adolescents with a migrant background may be particularly vulnerable to behavioral addictions, including problematic gaming and Internet use. Methods: we compared Italian (ITA) and non-Italian (WIC) students on Internet Gaming Disorder (IGD) and Internet Addiction (IA) and examined whether coping strategies and interpersonal-relationship quality were associated with these outcomes, using robust linear models estimated with the GENLIN procedure in IBM SPSS Statistics 31 and regression-based models on observed variables. A total of 535 students (64.5% female; aged 9–18) completed the Video Games Addiction Questionnaire (VGA), the Internet Addiction Test (IAT), the Children’s Coping Strategies Checklist–Revised (CCSC), and the Assessment of Interpersonal Relations (AIR). Results: robust generalized linear models showed that WIC adolescents reported significantly higher IGD levels than their Italian peers, while no differences emerged for IA. Gender differences were evident only in unadjusted models, with males reporting higher IGD and females higher IA; however, these effects were not significant once age and nationality were considered simultaneously. Age was positively associated with IA but not with IGD. Avoidance coping was associated with higher levels of both IGD and IA, whereas active coping was negatively associated with IGD. Relationship quality was not associated with IGD but showed protective effects for IA: better relationships with mothers and with both male and female peers were associated with lower IA scores. Overall, the findings highlight that IGD and IA follow partially distinct developmental patterns. Migrant background emerged as a specific vulnerability factor for IGD, while IA appears more closely linked to age-related processes, coping styles, and interpersonal-relationship quality. Conclusions: the results call for differentiated prevention and intervention approaches targeting the distinct etiological mechanisms of each problematic behavior, focusing on coping and migration-related stress and belonging for IGD, and on strengthening coping repertoires and relational resources for IA.
Full article
(This article belongs to the Section Pediatric Psychology)
Open AccessArticle
The Secure Base in the Storm: How Parent–Child Bonds Shape Coping in Pediatric Cancer Caregiving
by
Damiano Rizzi, Lavinia Barone, Alessandra Balestra, Maria Montanaro, Francesca Nichelli, Emanuela Schivalocchi, Giulia Rampoldi, Marco Spinelli, Giulia Ciuffo, Letizia Pomponia Brescia, Valerio Cecinati, Marco Zecca, Claudia Greco, Francesca Lionetti, Jessica Rotella, Giulia Gambini, Catherine Klersy and Chiara Ionio
Pediatr. Rep. 2026, 18(2), 52; https://doi.org/10.3390/pediatric18020052 - 2 Apr 2026
Abstract
Background: A paediatric cancer diagnosis is a profound stressor for the entire family system. Although coping strategies are well-studied, their link to the quality of the parent–child attachment relationship remains less explored. In this study, we investigated whether dyadic attachment dynamics—specifically closeness and
[...] Read more.
Background: A paediatric cancer diagnosis is a profound stressor for the entire family system. Although coping strategies are well-studied, their link to the quality of the parent–child attachment relationship remains less explored. In this study, we investigated whether dyadic attachment dynamics—specifically closeness and conflict between parent and child—are associated with the use of adaptive or maladaptive coping strategies in caregivers of children undergoing active treatment for oncohaematological diseases. Methods: We conducted a multicentre, cross-sectional study across three Italian paediatric oncohaematology centres. A total of 165 caregivers of 91 paediatric patients aged 3–17 years completed self-report measures assessing parent–child relationship quality (Child–Parent Relationship Scale-CPRS), coping strategies (COPE-NVI), perceived social support (MSPSS), and resilience (RS-14). We tested whether the quality of the parent–child attachment relationship is associated with caregivers’ coping strategies. We hypothesised that Attachment Closeness would be associated with adaptive coping (Positive Attitude, Social Support, Problem Orientation), whereas Attachment Conflict would be associated with maladaptive coping (Avoidance). We conducted multiple linear regression models, adjusted for key covariates and with robust standard errors clustered at the family level, to test these hypotheses. Results: Higher levels of emotional closeness (CPRS) were significantly associated with greater use of adaptive coping strategies, specifically Positive Attitude (β = 0.20, p = 0.049) and Problem Orientation (β = 0.26, p = 0.002), even after controlling for sociodemographic factors, social support, and resilience. Conversely, higher levels of relational conflict were significantly associated with greater use of the maladaptive Avoidance strategy (β = 0.14, p = 0.015). The hypothesis linking closeness to Social Support seeking was not supported. Conclusions: The findings suggest that the parent–child attachment relationship is a significant correlate of caregiver coping strategies in caregivers of children with cancer. Interventions aimed at supporting the caregiver–child dyad by fostering emotional closeness and reducing conflict may promote more adaptive parental coping mechanisms, thereby enhancing family resilience and psychological adjustment throughout the treatment journey.
Full article
(This article belongs to the Section Pediatric Psychology)
Open AccessCase Report
Pneumococcal Sepsis Revealing Pediatric Systemic Lupus Erythematosus with Sjögren’s Syndrome Overlap: A Case Report
by
Francesco Accomando, Vittorio Albertazzi, Francesco Girelli, Michela Biscarini, Melodie O. Aricò and Enrico Valletta
Pediatr. Rep. 2026, 18(2), 51; https://doi.org/10.3390/pediatric18020051 - 2 Apr 2026
Abstract
Background: Systemic lupus erythematosus (SLE) may present with heterogeneous clinical manifestations in pediatric patients. Although infections are a major cause of morbidity and mortality in SLE, severe bacterial infections rarely represent the presenting clinical event leading to diagnosis. Case description: We report the
[...] Read more.
Background: Systemic lupus erythematosus (SLE) may present with heterogeneous clinical manifestations in pediatric patients. Although infections are a major cause of morbidity and mortality in SLE, severe bacterial infections rarely represent the presenting clinical event leading to diagnosis. Case description: We report the case of a 13-year-old boy diagnosed with SLE with Sjögren’s syndrome overlap who presented with pneumococcal sepsis. The patient was admitted with high-grade fever and facial swelling, and blood cultures grew Streptococcus pneumoniae. Although an initial clinical response to antibiotic therapy was observed, fever subsequently recurred, accompanied by persistent systemic symptoms and progressive laboratory abnormalities. Further investigations revealed hematologic abnormalities, serosal involvement, renal disease, and a characteristic autoantibody profile. The patient fulfilled the 2019 ACR/EULAR classification criteria for SLE after comprehensive autoimmune evaluation. The overlap with Sjögren’s syndrome was supported by the autoantibody profile and imaging findings involving the parotid glands. Following treatment with intravenous methylprednisolone pulses, oral prednisone, hydroxychloroquine, and mycophenolate mofetil, the patient showed rapid clinical improvement and sustained remission. Conclusions: This case highlights that severe invasive bacterial infection may occasionally be the clinical circumstance that leads to the diagnosis of pediatric systemic lupus erythematosus. Persistent systemic inflammation or evolving multisystem involvement despite appropriate antimicrobial therapy should prompt consideration of an underlying autoimmune disease, even in patients without a prior history of immune dysfunction.
Full article
(This article belongs to the Special Issue Infectious Diseases in Children and Adolescents)
►▼
Show Figures
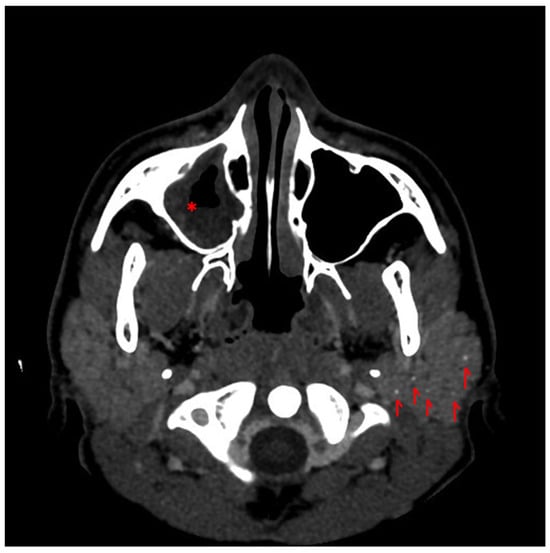
Figure 1
Open AccessArticle
Long-Term Outcomes After Childhood Stroke
by
Kerttu Kivisikk, Pilvi Ilves, Mairi Männamaa, Eve Õiglane-Shlik, Nigul Ilves, Norman Ilves, Inga Talvik, Dagmar Loorits, Pille Kool and Rael Laugesaar
Pediatr. Rep. 2026, 18(2), 50; https://doi.org/10.3390/pediatric18020050 - 1 Apr 2026
Abstract
►▼
Show Figures
The aim of this study was to assess long-term outcomes in patients with different vascular types of childhood stroke. Methods: Data for children with childhood stroke (aged 29 days to 18 years) were collected from the Estonian Pediatric Stroke Database. Outcomes (death, recurrent
[...] Read more.
The aim of this study was to assess long-term outcomes in patients with different vascular types of childhood stroke. Methods: Data for children with childhood stroke (aged 29 days to 18 years) were collected from the Estonian Pediatric Stroke Database. Outcomes (death, recurrent stroke, epilepsy, neurodevelopmental outcome by pediatric stroke outcome measure (PSOM)) were assessed at a minimum of two years after stroke. Results: Long-term outcome data were available for 44 patients with childhood stroke (including three patients who died of stroke). According to the PSOM, based on gender, age, location of stroke and epilepsy, there were no differences in outcomes, but patients with a Pediatric NIH Stroke Scale (PedNIHSS) score of ≥6 had worse outcomes compared to patients with a score of <6. Children with arterial hemorrhagic stroke (AHS) were more likely to die, suffer from epilepsy and develop problems in the cognition/behavior PSOM subscale compared to children with arterial ischemic stroke (AIS). Combined poor outcomes (epilepsy, PSOM ≥ 1, recurrent stroke, mortality) occurred in 75% (33/44) of all patients with long-term outcome data. Conclusions: Combined poor outcomes occurred in 75% of the patients with childhood stroke. Patients with AHS showed higher mortality and worse long-term outcomes compared to patients with AIS in certain neurodevelopmental domains.
Full article
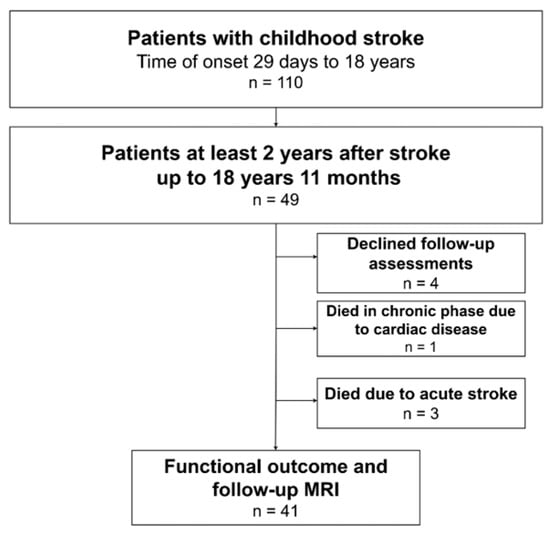
Figure 1

Journal Menu
► ▼ Journal Menu-
- Pediatric Reports Home
- Aims & Scope
- Editorial Board
- Topical Advisory Panel
- Instructions for Authors
- Special Issues
- Topics
- Sections & Collections
- Article Processing Charge
- Indexing & Archiving
- Most Cited & Viewed
- Journal Statistics
- Journal History
- Journal Awards
- Society Collaborations
- Conferences
- Editorial Office
Journal Browser
► ▼ Journal BrowserHighly Accessed Articles
Latest Books
E-Mail Alert
News
Topics

Conferences
Special Issues
Special Issue in
Pediatric Reports
Diagnosis and Treatment of the Maxillofacial Region in Pediatric Patients
Guest Editors: Maciej Chęciński, Maciej SikoraDeadline: 30 June 2026
Special Issue in
Pediatric Reports
Infectious Diseases in Children and Adolescents
Guest Editors: Désirée Caselli, Melodie Olivia Loredana Rosa AricòDeadline: 15 August 2026
Special Issue in
Pediatric Reports
Advanced Diagnostic and Treatment Approach in Pediatric Hepatology
Guest Editor: Tudor PopDeadline: 30 September 2026
Special Issue in
Pediatric Reports
The Developing Child: Integrating Emotional and Physical Health
Guest Editor: Chiara IonioDeadline: 31 October 2026
Topical Collections
Topical Collection in
Pediatric Reports
Recent Advances and Critical Issues in Pediatrics: a Collection of Feature Papers
Collection Editors: Maurizio Aricò, Claudia Mandato, Pietro Vajro








