Journal Description
Allergies
Allergies
is an international, peer-reviewed, open access journal on allergy and immunology published quarterly online by MDPI.
- Open Access— free for readers, with article processing charges (APC) paid by authors or their institutions.
- High Visibility: indexed within Scopus, Embase, and other databases.
- Rapid Publication: manuscripts are peer-reviewed and a first decision is provided to authors approximately 29.4 days after submission; acceptance to publication is undertaken in 6.2 days (median values for papers published in this journal in the second half of 2025).
- Recognition of Reviewers: APC discount vouchers, optional signed peer review, and reviewer names published annually in the journal.
Latest Articles
Cross-Kingdom Network Analysis of Bacterial and Fungal Communities in Allergic Rhinitis, Asthma, and Healthy Controls
Allergies 2026, 6(2), 17; https://doi.org/10.3390/allergies6020017 - 5 May 2026
Abstract
Bacterial and fungal airway communities play a critical role in allergic respiratory diseases, yet they are often studied independently despite evidence of cross-kingdom ecological interactions. We investigated bacterial–fungal interactions across allergic rhinitis (AR), asthma (AS), allergic rhinitis with asthma comorbidity (ARAS), and healthy
[...] Read more.
Bacterial and fungal airway communities play a critical role in allergic respiratory diseases, yet they are often studied independently despite evidence of cross-kingdom ecological interactions. We investigated bacterial–fungal interactions across allergic rhinitis (AR), asthma (AS), allergic rhinitis with asthma comorbidity (ARAS), and healthy controls (HC) in a cohort of 286 participants (531 samples) using network analysis. Buccal and nasal samples were sequenced for 16S rRNA and ITS amplicons and networks constructed using sparse inverse covariance estimation for ecological association and statistical inference. Inferred bacterial–fungal connections comprised approximately one-third of the network edges. Taxonomic analyses of cross-kingdom-associated ASVs from the bacterial genera Dolosigranulum, Gamella, Haemophilus, Lawsonella, and Moraxella and the fungal genus Cladosporium revealed significant (p < 0.05) differences in mean relative abundance between the disease groups and healthy controls. Network topology analysis further identified distinct high-weight and high-degree microbial hubs, predominantly comprising fungal ASVs (Aleurina, Cladosporium, Malassezia, and Vishniacozyma) acting as putative keystone taxa and with disease-specific patterns. Together, these findings demonstrate that allergic airway diseases in this cohort are characterized by altered cross-kingdom network structure and disease-specific reorganization of microbial interaction patterns; this highlights the importance of integrated bacteriome–mycobiome analyses in understanding airway dysbiosis.
Full article
(This article belongs to the Special Issue Molecular Mechanisms of Allergy and Asthma: 4th Edition)
Open AccessReview
Atopic Dermatitis: Contemporary Concepts in Epidemiology, Pathogenesis, Assessment, and Targeted Treatment
by
Caijun Jin, Zhiyuan Ding, Pham Ngoc Chien and Chan Yeong Heo
Allergies 2026, 6(2), 16; https://doi.org/10.3390/allergies6020016 - 5 May 2026
Abstract
Atopic dermatitis (AD) is a chronic, relapsing inflammatory dermatosis characterized by pruritus, eczematous lesions, and a fluctuating course. It imposes substantial quality-of-life and economic burdens through sleep disturbance, pain, psychosocial distress, and frequent healthcare utilization. Recent global estimates suggest AD affects hundreds of
[...] Read more.
Atopic dermatitis (AD) is a chronic, relapsing inflammatory dermatosis characterized by pruritus, eczematous lesions, and a fluctuating course. It imposes substantial quality-of-life and economic burdens through sleep disturbance, pain, psychosocial distress, and frequent healthcare utilization. Recent global estimates suggest AD affects hundreds of millions worldwide, with meaningful prevalence in both children and adults. AD pathogenesis is multifactorial, reflecting the interaction of genetic predisposition, immune dysregulation dominated by type 2 inflammation, epidermal barrier impairment, neuroimmune itch pathways, and microbial dysbiosis. Clinical diagnosis remains primarily clinical, supported by classic criteria emphasizing pruritus, typical morphology, chronicity, and atopic history. Disease severity and treatment response are commonly quantified using validated measures such as EASI and SCORAD, enabling standardized monitoring and evidence-based escalation. Management has shifted from broad immunosuppression to a stepwise, endotype-aware approach integrating barrier repair, anti-inflammatory topical therapy, phototherapy, conventional systemic agents, and rapidly expanding targeted options. Recent guidelines and approvals highlight increasing roles for biologics and JAK pathway inhibition, alongside newer nonsteroidal topicals. This review summarizes current concepts and practical treatment integration, with emphasis on safety, monitoring, and future research directions.
Full article
(This article belongs to the Section Dermatology)
►▼
Show Figures

Figure 1
Open AccessArticle
Formula Modification and Clinical Outcomes in Infants with Atopic Dermatitis and Suspected Non–IgE–Mediated Cow’s Milk Protein Allergy: A Real-World Comparative Cohort Study
by
Zainab Al Alawi, Rabab Abbas Majzoub and Ossama M. Zakaria
Allergies 2026, 6(2), 15; https://doi.org/10.3390/allergies6020015 - 16 Apr 2026
Abstract
Background: Cow’s milk protein allergy (CMPA) is a common cause of gastrointestinal and dermatologic symptoms in infancy. In clinical practice, infants with atopic dermatitis (AD) and suspected non-IgE-mediated CMPA are frequently managed with formula modification, although real-world comparative data across different formula strategies
[...] Read more.
Background: Cow’s milk protein allergy (CMPA) is a common cause of gastrointestinal and dermatologic symptoms in infancy. In clinical practice, infants with atopic dermatitis (AD) and suspected non-IgE-mediated CMPA are frequently managed with formula modification, although real-world comparative data across different formula strategies remain limited. Aim: To evaluate gastrointestinal symptom resolution, improvement in AD, and growth outcomes following formula modification in infants with AD and suspected non-IgE-mediated CMPA. Methods: This retrospective comparative cohort study included 107 infants aged ≤12 months with documented AD and suspected non-IgE-mediated CMPA evaluated at a tertiary academic center between January 2024 and December 2025. Infants were categorized according to initial management strategy: switch to extensively hydrolyzed formula (eHF; n = 63), switch to amino acid formula (AAF; n = 29), or continued standard cow’s milk-based formula (n = 15). The primary outcome was resolution of gastrointestinal symptoms within 2–4 weeks. Secondary outcomes included improvement in AD, weight gain, and need for further formula escalation. Multivariable logistic regression was performed to adjust for potential confounders. Results: Overall, gastrointestinal symptom resolution occurred in 74 of 107 infants (69.2%). Resolution rates were 71.4% in the eHF group, 79.3% in the AAF group, and 40% in the standard formula group (p = 0.01). In adjusted analysis, switching to eHF (aOR 2.8; 95% CI 1.1–7.3; p = 0.03) and AAF (aOR 4.1; 95% CI 1.3–12.5; p = 0.01) was independently associated with higher odds of symptom resolution compared with continued standard formula. Improvement in AD was observed in 57.9% of infants overall and differed significantly across groups (p = 0.04). Mean weight gain during follow-up did not differ significantly between groups (p = 0.63). Subsequent formula escalation was more frequent in the standard formula group (46.7%) compared with eHF (17.5%) and AAF (13.8%) groups (p = 0.004). Conclusions: In infants with AD and suspected non-IgE-mediated CMPA, substitution with extensively hydrolyzed or amino acid formula was independently associated with greater gastrointestinal symptom resolution and improvement in dermatitis compared with continued standard formula, without evidence of compromised growth. These findings provide supportive real-world evidence consistent with current international guidelines; however, given the observational design and potential for residual confounding, they should be interpreted as hypothesis-generating rather than confirmatory evidence of causal treatment effects.
Full article
(This article belongs to the Section Pediatric Allergy)
Open AccessReview
Allergic Chronic Rhinosinusitis: Myth, Misnomer, or Missing Endotype?
by
George N. Konstantinou and Konstantinos Petalas
Allergies 2026, 6(2), 14; https://doi.org/10.3390/allergies6020014 - 14 Apr 2026
Abstract
Chronic rhinosinusitis (CRS) is a heterogeneous inflammatory syndrome of the sinonasal mucosa that is imperfectly captured by phenotypes with or without nasal polyps. Since allergic rhinitis (AR) and atopy often occur alongside CRS, the term “allergic CRS” is commonly used. However, it is
[...] Read more.
Chronic rhinosinusitis (CRS) is a heterogeneous inflammatory syndrome of the sinonasal mucosa that is imperfectly captured by phenotypes with or without nasal polyps. Since allergic rhinitis (AR) and atopy often occur alongside CRS, the term “allergic CRS” is commonly used. However, it is uncertain whether this term indicates a specific allergen-related, IgE-mediated endotype or merely represents a clinical overlap. We synthesize epidemiologic data, mucosal immunobiology, epithelial barrier dysfunction, and host–microbe interactions that can generate IgE-rich type 2 inflammation in CRS. We propose an operational entity test (objective CRS; clinically relevant allergy; evidence of IgE relevance in target tissue; exposure–response patterns; and differential response to allergy-directed interventions) to guide hypothesis testing rather than diagnosis. Using this framework, allergic fungal rhinosinusitis and central compartment atopic disease emerge as the clearest clinical prototypes where allergen contact patterns and IgE relevance plausibly contribute to disease expression. In contrast, microbial superantigens and other non-allergen stimuli can drive local IgE amplification, limiting the specificity of systemic sensitization as a causal marker. We discuss therapeutic implications, including biologics targeting type 2 pathways and epithelial alarmin blockade, and outline research priorities for endotype-resolved cohorts and mechanism-informed trials to test whether allergic CRS should evolve from a heuristic descriptor into a validated endotype.
Full article
(This article belongs to the Section Rhinology/Allergic Rhinitis)
►▼
Show Figures

Figure 1
Open AccessArticle
High Dietary Salt Exposure During Sensitization Is Associated with Increased Severity of Allergic Contact Dermatitis in Mice
by
Yukihiro Yoshimura and Aya Fujii
Allergies 2026, 6(2), 13; https://doi.org/10.3390/allergies6020013 - 13 Apr 2026
Abstract
Background: High dietary salt intake has been implicated in immune-mediated inflammatory diseases; however, its impact on allergic contact dermatitis (ACD) remains unclear. This study examined whether dietary salt exposure during the sensitization phase influences the severity of DNFB-induced ACD in mice. Methods: Female
[...] Read more.
Background: High dietary salt intake has been implicated in immune-mediated inflammatory diseases; however, its impact on allergic contact dermatitis (ACD) remains unclear. This study examined whether dietary salt exposure during the sensitization phase influences the severity of DNFB-induced ACD in mice. Methods: Female C57BL/6N mice were fed a normal diet (ND) or an 8% high-salt diet (HSD). In a subset, salt intake was normalized prior to sensitization (HSD → ND). ACD was induced using a DNFB sensitization and challenge protocol. Ear swelling was quantified using incremental area under the curve (iAUC). Histological analyses and measurements of plasma and skin sodium were performed. Results: HSD-fed mice showed greater ear swelling and higher iAUC than ND controls, accompanied by enhanced inflammatory cell infiltration. Skin sodium concentration differed among groups, with a higher concentration in HSD-fed mice compared that in the HSD → ND group. Normalization of salt intake prior to sensitization attenuated disease severity. Spearman analyses indicated that total sodium intake and plasma potassium concentration were associated with inflammatory severity. Conclusions: Dietary salt exposure during immune sensitization exacerbated experimental ACD and was associated with systemic electrolyte alterations. These findings suggest that sodium exposure during immune activation may influence allergic skin inflammation.
Full article
(This article belongs to the Section Dermatology)
►▼
Show Figures

Figure 1
Open AccessCorrection
Correction: Tharakan et al. D-2-Hydroxyglutarate Attenuates Sinonasal Inflammation in Murine Allergic Rhinitis. Allergies 2025, 5, 13
by
Anuj Tharakan, Ankit Kumar, Carmen Camarena, Daniel H. Conrad and Rebecca K. Martin
Allergies 2026, 6(2), 12; https://doi.org/10.3390/allergies6020012 - 9 Apr 2026
Abstract
There was an error in the original publication [...]
Full article
Open AccessReview
Chronic Spontaneous Urticaria: Pathophysiological Mechanisms, Emerging Biomarkers, and Therapeutic Advances
by
Maykon Jhuly Martins de Paiva, Livia Cavalcante de Araújo, Maressa de Oliveira Marinho, Renata Ferreira Diogo de Paiva, Vitória Pires dos Santos Costa, Gabriela Pires Santomé de Faria, Guilherme Silva de Souza, Sávia Denise Silva Carlotto Herrera, Iangla Araújo de Melo Damasceno, Taides Tavares dos Santos, Juliane Farinelli Panontin and Walmirton Bezerra D’Alessandro
Allergies 2026, 6(2), 11; https://doi.org/10.3390/allergies6020011 - 2 Apr 2026
Abstract
Chronic urticaria (CU) is a mast cell-driven inflammatory skin disorder characterized by recurrent wheals, angioedema, or both lasting more than six weeks, often resulting in significant impairment of quality of life. Although CU has traditionally been regarded as a predominantly histamine-mediated condition, evidence
[...] Read more.
Chronic urticaria (CU) is a mast cell-driven inflammatory skin disorder characterized by recurrent wheals, angioedema, or both lasting more than six weeks, often resulting in significant impairment of quality of life. Although CU has traditionally been regarded as a predominantly histamine-mediated condition, evidence accumulated over the past decade has redefined chronic spontaneous urticaria (CSU) as a complex immune-mediated disease with marked biological heterogeneity. Distinct pathogenic mechanisms involving autoimmune pathways, dysregulated mast cell activation, and chronic inflammatory networks have been identified, providing a mechanistic basis for disease persistence, variable severity, and therapeutic refractoriness. This review synthesizes current concepts in CSU pathophysiology, with emphasis on mast cell biology, autoimmune endotypes, and inflammatory amplification mechanisms. We further discuss emerging biomarkers with potential relevance for disease stratification and treatment prediction, as well as established and novel therapeutic strategies targeting key pathogenic pathways. By integrating mechanistic insights with clinical implications, this review highlights the transition toward endotype-driven and biomarker-guided management of chronic urticaria.
Full article
(This article belongs to the Special Issue Feature Papers 2025)
►▼
Show Figures

Figure 1
Open AccessReview
Cardiovascular Safety of Dupilumab: Current Evidence and Emerging Concerns
by
Giulia Laterra, Federica Giammona Indaco, Simone Bongiorno, Antonino Maniaci, Salvatore Maira, Mariangela Lodato, Carmelo Battaglia, Marco Barbanti and Cosimo Galletti
Allergies 2026, 6(1), 10; https://doi.org/10.3390/allergies6010010 - 13 Mar 2026
Abstract
Chronic rhinosinusitis with nasal polyps (CRSwNP) is a type 2 inflammatory disease effectively treated with dupilumab, a monoclonal antibody that inhibits IL-4 and IL-13 signaling. Dupilumab is an effective treatment for type 2 inflammatory diseases such as CRSwNP. Although efficacy of dupilumab in
[...] Read more.
Chronic rhinosinusitis with nasal polyps (CRSwNP) is a type 2 inflammatory disease effectively treated with dupilumab, a monoclonal antibody that inhibits IL-4 and IL-13 signaling. Dupilumab is an effective treatment for type 2 inflammatory diseases such as CRSwNP. Although efficacy of dupilumab in controlling upper airway inflammation is well established, concerns have emerged regarding its potential cardiovascular effects. Emerging evidence suggests that IL-4/IL-13 signaling plays a protective role in post-myocardial infarction remodeling by promoting anti-inflammatory macrophage polarization, angiogenesis, and controlled fibrosis, especially during the early healing phase. Pharmacological blockade of the IL-4/IL-13 signaling pathway, such as that induced by dupilumab, may theoretically impair myocardial repair mechanisms, particularly in male patients who appear more responsive to these cytokines. Although rare, dupilumab-associated hypereosinophilia and myocarditis have been reported. In patients with pre-existing ischemic heart disease or heart failure, a multidisciplinary risk–benefit evaluation should be considered. Concomitant use of cardioprotective agents such as sacubitril/valsartan or SGLT2 inhibitors may help mitigate potential cardiac risks. Future studies are needed to clarify the safety and therapeutic implications of combining dupilumab with cardiovascular therapies in patients with coexisting CRSwNP and heart disease. This review critically evaluates emerging evidence of potential interference with post-infarction myocardial repair and highlights the importance of a multidisciplinary approach in managing patients with coexisting inflammatory and cardiovascular diseases. The aim of this review is to explore the available data on the cardiovascular impact of dupilumab and to provide possible future perspectives.
Full article
(This article belongs to the Section Rhinology/Allergic Rhinitis)
►▼
Show Figures

Figure 1
Open AccessArticle
Recommended Age of Introduction on Commercial Baby Food Labels: Alignment with Allergy Prevention Guidelines
by
Lara Barros, Diana Arantes, Leonor Nora and Inês Pádua
Allergies 2026, 6(1), 9; https://doi.org/10.3390/allergies6010009 - 11 Mar 2026
Abstract
Background: Current recommendations for infant weaning suggest the early introduction of solid and diverse foods. Although homemade meals are advisable, there is a demand for commercially available complementary foods (CACFs), and the information present on their labeling influences caregivers’ choices. The aim of
[...] Read more.
Background: Current recommendations for infant weaning suggest the early introduction of solid and diverse foods. Although homemade meals are advisable, there is a demand for commercially available complementary foods (CACFs), and the information present on their labeling influences caregivers’ choices. The aim of this study was to evaluate recommended-age-of-introduction labeling of CACFs in the Portuguese market, in light of current guidelines for complementary feeding. Methods: Between November and December 2025, labels of all CACFs found in infant feeding sections of 13 Portuguese grocery retailers were analyzed. Milk formulas, powders, products for children over 15 months, and those for children with food allergies or intolerances were excluded. Results: Of the 539 products analyzed, 458 showed a recommended age for introduction, ranging from 4 to 12 months, with significant variability being observed between food categories. Significant variability was also observed in the recommended age for introduction depending on whether major allergens were present. Conclusions: The results of our study identified an age-segmented approach to complementary feeding recommendations in CACF labeling, not reflecting current infant feeding guidelines that support complementary feeding. Our results reinforce the need for more support from scientific evidence and health guidelines in food availability and marketing.
Full article
(This article belongs to the Special Issue Feature Papers 2025)
Open AccessArticle
Tolerability, Efficacy, and Quality of Life Outcomes of Allerspray-G Nasal Spray in Adults with Allergic Rhinitis: Real-World Post-Marketing Clinical Trial
by
Marine Delmas, Manon D’Almeida, Séverine Dameron-Puech, Nicolas Macian, Gisèle Pickering and Rémi Shrivastava
Allergies 2026, 6(1), 8; https://doi.org/10.3390/allergies6010008 - 2 Mar 2026
Abstract
(1) Allergic rhinitis (AR) is a chronic inflammatory condition of nasal mucosa that impairs quality of life (QOL). Beyond pharmacological treatments, some patients seek non-pharmacological options due to side effects or incomplete symptom control. Allerspray-G (AAG) is a barrier-forming Class IIa medical device
[...] Read more.
(1) Allergic rhinitis (AR) is a chronic inflammatory condition of nasal mucosa that impairs quality of life (QOL). Beyond pharmacological treatments, some patients seek non-pharmacological options due to side effects or incomplete symptom control. Allerspray-G (AAG) is a barrier-forming Class IIa medical device (Medical Device Regulation (MDR) 2017/745) designed to reduce allergen contact and alleviate AR symptoms. This study evaluated the safety and efficacy of AAG in adults with AR in a real-life post-marketing setting through an open-label, single-center investigation using a two-stage Fleming design. (2) Tolerance was the primary outcome, assessed through the monitoring of adverse events. Secondary outcomes included efficacy measures, evaluated using the Total Nasal Symptom Score (TNSS) and patient-reported QOL outcomes. (3) In total, 20% reported a possible or probable event related to AAG, with all being mild. The TNSS decreased significantly from baseline (mean change: −1.94, p < 0.001), and 73.3% achieved a ≥30% reduction. Significant improvements were also observed across all QOL domains (p < 0.05). (4) AAG was safe, well tolerated, and improved nasal symptoms and QOL, supporting its use as a non-pharmacological option for symptom relief in allergic rhinitis. These findings are consistent with and further reinforce results from the initial 2017 clinical study.
Full article
(This article belongs to the Section Rhinology/Allergic Rhinitis)
►▼
Show Figures

Figure 1
Open AccessReview
Urticaria and Urticaria-like Dermatoses in Pregnancy: Clinical Spectrum, Differential Diagnosis and Management
by
Federica Trovato, Antonio Di Guardo, Maria Elisabetta Greco, Giovanni Grossi, Annunziata Dattola, Steven Paul Nisticò and Giovanni Pellacani
Allergies 2026, 6(1), 7; https://doi.org/10.3390/allergies6010007 - 25 Feb 2026
Abstract
Urticaria is a mast cell-mediated disorder commonly encountered in women of reproductive age, making its interaction with pregnancy clinically relevant. Gestation induces profound hormonal and immunologic adaptations—including shifts between Th1/Th17 and Th2/Treg responses and sustained exposure to sex steroids and placental hormones—that can
[...] Read more.
Urticaria is a mast cell-mediated disorder commonly encountered in women of reproductive age, making its interaction with pregnancy clinically relevant. Gestation induces profound hormonal and immunologic adaptations—including shifts between Th1/Th17 and Th2/Treg responses and sustained exposure to sex steroids and placental hormones—that can modulate mast cell reactivity. As a result, chronic urticaria (CU) shows heterogeneous behavior during pregnancy: approximately half of patients improve, one third worsen, and the remainder remain stable. Pregnancy also presents several urticaria-like dermatoses, notably polymorphic eruption of pregnancy (PEP/PUPPP), atopic eruption of pregnancy (AEP) and pemphigoid gestationis (PG), as well as rare hormone-induced hypersensitivity reactions. Additionally, systemic disorders such as intrahepatic cholestasis of pregnancy (ICP), chronic kidney disease–associated pruritus and urticarial vasculitis may mimic urticaria but differ markedly in prognosis, maternal–fetal risk and management. Given this complexity, accurate diagnosis requires integration of temporal pattern, lesion morphology and duration, distribution, systemic features and targeted investigations, as outlined in the diagnostic algorithm proposed. Most pregnancy-specific eruptions are benign, whereas PG, ICP and urticarial vasculitis warrant prompt recognition due to potential fetal implications. Management of CU in pregnancy generally follows standard guidelines, with second-generation H1-antihistamines as first-line therapy and omalizumab reserved for severe refractory cases.
Full article
(This article belongs to the Section Dermatology)
►▼
Show Figures

Figure 1
Open AccessSystematic Review
The Potential Link Between Food Allergies and the Insurgence of Allergic and Rheumatoid Arthritis: A Systematic Review
by
Luigi Cofone and Marise Sabato
Allergies 2026, 6(1), 6; https://doi.org/10.3390/allergies6010006 - 14 Feb 2026
Abstract
Introduction: The potential role of food hypersensitivity in the insurgence of inflammatory activity in arthritis such as Rheumatoid Arthritis (RA) has received intermittent attention, also supported by theoretical links involving mucosal immunity, mast-cell activation, and microbiome–immune interactions. Despite biological plausibility, the clinical significance
[...] Read more.
Introduction: The potential role of food hypersensitivity in the insurgence of inflammatory activity in arthritis such as Rheumatoid Arthritis (RA) has received intermittent attention, also supported by theoretical links involving mucosal immunity, mast-cell activation, and microbiome–immune interactions. Despite biological plausibility, the clinical significance of dietary antigens in RA remains uncertain. Methods: A systematic review was conducted following the PRISMA guidelines. Searches using PubMed, Scopus, and Web of Science identified studies exploring dietary interventions or food hypersensitivity in RA. Eligible articles included clinical trials, case reports, and observational studies, in English or Italian, up to the 10 December 2025. Data extraction and quality assessment were performed using the Newcastle–Ottawa Scale. Results: Eight studies met the inclusion criteria. Findings indicate that elimination or elemental diets occasionally yielded subjective improvements—such as a reduction in pain, morning stiffness, and functional improvements—yet objective inflammatory markers rarely changed. Small, highly selected, cohorts demonstrated immuno-histological alterations, including reduced mast-cell density, while long-term diets (e.g., gluten-free or vegan) have reduced specific IgG levels without altering radiographic progression. Conclusions: Evidence suggests that dietary interventions may offer symptomatic relief only in a minority of RA patients. Due to methodological constraints, inconsistent outcomes, and limited applicability to contemporary treatments, dietary approaches need further exploration and investigation. Rigorous trials in modern cohorts are warranted to clarify whether food hypersensitivity meaningfully influences RA pathophysiology.
Full article
(This article belongs to the Special Issue Feature Papers 2025)
►▼
Show Figures

Figure 1
Open AccessArticle
Scope, Features, and Utility of Australian Penicillin Allergy Delabelling Protocols: A Descriptive Analysis
by
Claire Chitty, Lerato Obadimeji, Rafah Mahmood, Amy Skett, Catherine J. Hornung, Rani Scott Farmer, Sandra Vale, Jennifer J. Koplin, Michaela Lucas, James Yun and Sandra M. Salter
Allergies 2026, 6(1), 5; https://doi.org/10.3390/allergies6010005 - 9 Feb 2026
Abstract
Penicillin allergy delabelling improves patient outcomes, reduces healthcare costs, and supports antimicrobial stewardship. While PADL protocols (PADL-P) are increasingly used in clinical practice, the consistency of Australian PADL-Ps and their alignment with established guidance remain unclear. A cross-sectional study (from June to August
[...] Read more.
Penicillin allergy delabelling improves patient outcomes, reduces healthcare costs, and supports antimicrobial stewardship. While PADL protocols (PADL-P) are increasingly used in clinical practice, the consistency of Australian PADL-Ps and their alignment with established guidance remain unclear. A cross-sectional study (from June to August 2025) identified Australian PADL-Ps through organisational and professional outreach, the literature, and structured internet searches. Protocol features were extracted iteratively and deductively. Citation counts and overlap were determined using the Graphical Representation of Overlap for OVErviews (GROOVE) methodology. Protocols were applied to 20 validated penicillin allergy scenarios, and the Australasian Society for Clinical Immunology and Allergy (ASCIA) Consensus Statement for the Management of Suspected Penicillin Allergy and risk alignment were compared. Fifteen Australian PADL-Ps were identified. They shared similar features; however, differences were observed in the no/low-risk criteria and subsequent delabelling actions. Protocols cited a mean of nine references (mean of 4.7 (43.9%) unique), with one protocol citing no references. When applied to clinical scenarios, protocol-assigned risk did not consistently align with the ASCIA risk classification (54.6% of adult and 77.8% of paediatric protocols assigned scenarios to the same risk level). Adult protocol alignment was lowest for no-risk (31.9%) and low-risk (50.0%) scenarios and highest for moderate-risk scenarios (78.8%), whereas paediatric protocol alignment was 33.3% for moderate risk and 100% for low and high-risk scenarios. Although Australian PADL-Ps shared core structural features, incongruencies in risk criteria and alignment with established guidelines may result in different clinical outcomes for patients with similar penicillin allergy histories. These findings emphasise the complexity of clinical decision-making around penicillin allergy and suggest a need for standardisation of PADL-Ps to maximise delabelling benefits and safety across Australian healthcare settings.
Full article
(This article belongs to the Section Drug Allergy)
►▼
Show Figures

Figure 1
Open AccessReview
A False Allergic Contact Dermatitis? A Review of Earlobe Eczema Beyond Nickel Allergy: Irritant Mechanisms and Psoriatic Diathesis
by
Ramon Grimalt
Allergies 2026, 6(1), 4; https://doi.org/10.3390/allergies6010004 - 27 Jan 2026
Abstract
Background: Dermatitis affecting the earlobe is a highly frequent clinical presentation, predominantly attributed to Allergic Contact Dermatitis (ACD) caused by metallic ions like nickel from earrings. However, a significant subset of patients presents with recurrent eczematous lesions highly suggestive of ACD but with
[...] Read more.
Background: Dermatitis affecting the earlobe is a highly frequent clinical presentation, predominantly attributed to Allergic Contact Dermatitis (ACD) caused by metallic ions like nickel from earrings. However, a significant subset of patients presents with recurrent eczematous lesions highly suggestive of ACD but with inconclusive or negative patch test results, posing a profound diagnostic and therapeutic dilemma. Objective: This comprehensive review critically evaluates the differential diagnosis of earlobe eczema in the context of negative patch tests. Drawing from a representative case of a 30-year-old female with recurrent earlobe eczema and a strong family history of psoriasis, we explore alternative non-immunological and endogenous mechanisms, specifically Irritant Contact Dermatitis (ICD) and the Koebner Phenomenon on a background of Psoriatic Diathesis. Methods: We performed an extensive review of the current literature focusing on the epidemiology and pathogenesis of metal ACD, non-allergic mechanisms of jewelry-induced dermatitis (ICD), the molecular basis of the Koebner phenomenon, and the clinical overlap between eczema and psoriasis (Eczematous Psoriasis). Results: The localized nature of the inflammation, coupled with the absence of generalized nickel sensitivity, strongly suggests that the mechanical and occlusive trauma from earrings can induce a purely irritant reaction. Crucially, the presence of a familial psoriatic diathesis supports the hypothesis that this local irritation acts as a Koebner phenomenon trigger, leading to an eczematous manifestation of an underlying psoriatic tendency. Conclusions: Not all recurrent eczematous lesions at common contact sites are caused by ACD. Clinicians must adopt an integrated diagnostic approach, factoring in personal and family history alongside patch test results, to differentiate true allergy from ICD and the Koebner phenomenon. This nuanced perspective is vital for providing appropriate counseling (strict jewelry avoidance) and targeted, often steroid-sparing, management (e.g., topical calcineurin inhibitors) for a durable therapeutic outcome.
Full article
(This article belongs to the Section Dermatology)
Open AccessReview
Diagnosis of Food Allergy: Which Tests Truly Have Clinical Value?
by
Katarzyna Napiorkowska-Baran, Alicja Gruszka-Koselska, Karolina Osinska, Gary Andrew Margossian, Carla Liana Margossian, Aleksandra Wojtkiewicz, Pawel Treichel and Jozef Slawatycki
Allergies 2026, 6(1), 3; https://doi.org/10.3390/allergies6010003 - 27 Jan 2026
Abstract
Food allergy diagnosis remains challenging due to the difficulty of distinguishing true clinical allergy from asymptomatic sensitization. Inaccurate diagnosis may result in unnecessary dietary restrictions, reduced quality of life, or, conversely, failure to identify individuals at risk of severe allergic reactions. This review
[...] Read more.
Food allergy diagnosis remains challenging due to the difficulty of distinguishing true clinical allergy from asymptomatic sensitization. Inaccurate diagnosis may result in unnecessary dietary restrictions, reduced quality of life, or, conversely, failure to identify individuals at risk of severe allergic reactions. This review critically analyzes the efficacy, limitations, and clinical utility of currently available diagnostic tests for food allergy, with particular emphasis on their ability to predict true clinical reactivity. A comprehensive literature review was conducted to evaluate the sensitivity, specificity, and predictive values of both traditional and emerging diagnostic modalities. English-language guidelines, systematic reviews, and key clinical studies published primarily within the past 15 years (up to 2025) were identified through PubMed and Google Scholar. Classic diagnostic tools, including skin prick testing (SPT) and serum-specific IgE (sIgE), were assessed alongside novel approaches such as component-resolved diagnostics (CRD), basophil activation test (BAT), mast cell activation test (MAT), atopy patch testing (APT), cytokine profiling, and omics-based diagnostics. Particular attention was given to how these tests compare with the oral food challenge (OFC), which remains the diagnostic gold standard. The findings demonstrate that while conventional tests offer high sensitivity and are valuable for initial risk assessment, their limited specificity often leads to overdiagnosis. Emerging molecular and cellular assays show improved specificity and functional relevance, especially in complex cases involving polysensitization or unclear clinical histories and may reduce reliance on OFCs in the future. However, accessibility, cost, and lack of standardization currently limit their widespread clinical application. Advances in artificial intelligence and data integration hold promise for improving diagnostic accuracy through enhanced interpretation of complex immunological data. Based on the synthesized evidence, this review proposes an evidence-based, stepwise, and individualized diagnostic algorithm for food allergy. Integrating clinical history, targeted testing, and selective use of OFCs can improve diagnostic certainty, enhance food safety, minimize unnecessary dietary avoidance, and optimize patient outcomes. The review underscores the need for continued research, standardization, and validation of novel diagnostic tools to support personalized and precise food allergy management.
Full article
(This article belongs to the Section Food Allergy)
Open AccessArticle
Specific IgE/IgG in Umbilical Cord Blood and Maternal Blood in Mothers with Eosinophilia
by
Diana Mitkova Hristova, Martin Vladimirov, Bozhidar Karamishev, Anatoli Kolev, Daria Koleva, Liliya Koleva, Victoria Spasova, Svetlana Shumarova and Vesela Karamisheva
Allergies 2026, 6(1), 2; https://doi.org/10.3390/allergies6010002 - 19 Jan 2026
Abstract
Background: Presence of milk, fruits, eggs, fish, nuts and wheat antigens in the amniotic fluid is described in the literature. Studies show a contradictory relationship between maternal exposure to allergens and early sensitization of the fetus to allergens. Hemochorionic type of the human
[...] Read more.
Background: Presence of milk, fruits, eggs, fish, nuts and wheat antigens in the amniotic fluid is described in the literature. Studies show a contradictory relationship between maternal exposure to allergens and early sensitization of the fetus to allergens. Hemochorionic type of the human placenta allows for easier transfer of nutrients and antibodies from the mother’s blood to the fetal circulation through the direct contact of maternal blood with the fetal chorion. During the third trimester of pregnancy, immunoglobulin G (IgG) is actively transferred through the placenta into the fetal via neonatal FcRN receptor (FcRN). In addition, monomeric immunoglobulin E (IgE) cannot cross the placenta Aim: The objective of our study is to track intrauterine sensitization to essential food proteins at birth in umbilical cord blood in mothers with established peripheral blood eosinophilia and in their infants using allergen-specific IgE and IgG. Methods: An observational study was carried out in a cohort of 22 mothers with eosinophilia and their babies. Differences in expression between groups were assessed. Blood samples were collected to determine serum IgE and IgG specific to a set of inhalant and food allergens. Results: We did not find a significant correlation between specific IgE to cow’s milk (p = 0.857), egg white (p = 0.926) and egg yolk (p = 0.096) in umbilical cord blood and maternal blood samples taken immediately before birth. Spearman’s correlation of the specific IgE and IgG in umbilical cord blood showed no dependence between the two variables. In contrast, statistical analysis showed that maternal eosinophilia in peripheral blood could be a risk factor for the development of allergy in the offspring (χ2, p = 0.0347). However, given the small number of patients, this claim needs to be confirmed with further studies. Conclusions: Due to the functional immaturity of the developing immune system of the fetus, the generation and maintenance of an independent immune response to allergens are incomplete. Maternal IgG (specific) passes to the baby and high maternal IG to a specific allergen reduces babies IgE production. In addition, low maternal specific IgG may promote IgE production in the baby under the influence of microenvironmental factors (cytokine background). The main limitation of our study is the small number of patients. Further research is needed in this direction to clarify the mechanisms and risk factors for early sensitization in newborns.
Full article
(This article belongs to the Section Physiopathology)
►▼
Show Figures

Figure 1
Open AccessEditor’s ChoiceArticle
Development and Optimization of a LAMP Assay for Lupin Detection in Foods
by
Marta Trujillo, Beatriz Beroiz, Carmen Cuadrado, Rosario Linacero and Isabel Ballesteros
Allergies 2026, 6(1), 1; https://doi.org/10.3390/allergies6010001 - 28 Dec 2025
Abstract
Lupin (Lupinus spp.) is increasingly incorporated into processed foods as a gluten-free ingredient and alternative protein source, but it is also a regulated allergen in the European Union due to cross-reactivity with other legumes, especially peanut. Reliable methods for detecting undeclared lupin
[...] Read more.
Lupin (Lupinus spp.) is increasingly incorporated into processed foods as a gluten-free ingredient and alternative protein source, but it is also a regulated allergen in the European Union due to cross-reactivity with other legumes, especially peanut. Reliable methods for detecting undeclared lupin traces in complex food matrices are therefore essential for consumer protection. In this study, a loop-mediated isothermal amplification (LAMP) assay was developed for rapid and sensitive detection of lupin DNA. Several nuclear and chloroplast regions were evaluated for primer design, and gene encoding the Lup a 1 allergen was selected as the optimal target. Amplification was monitored by real-time fluorescence, agarose gel electrophoresis, and visual colorimetry. The selected primer set achieved a detection limit of 25 pg of lupin DNA and consistently detected lupin in binary mixtures down to 10 mg/kg, with no cross-reactivity against closely related legumes or tree nuts. Application to processed foods confirmed detection in products declaring lupin and revealed potential undeclared presence in some commercial samples. Colorimetric detection provided reliable results comparable to real-time monitoring, enabling simple readouts without specialized equipment. Overall, the developed LAMP assay represents a rapid, specific, and sensitive alternative to PCR-based methods for allergen monitoring and food safety management.
Full article
(This article belongs to the Special Issue Feature Papers 2025)
►▼
Show Figures

Graphical abstract
Open AccessReview
Shellfish Allergy Immunotherapy: Are We Moving Forward?
by
Lucio H. T. Fung, Ho Lam Yeung, Chun Wai Lim, Shan Jiang, Nicki Y. H. Leung, Patrick S. C. Leung, Ting Fan Leung and Christine Y. Y. Wai
Allergies 2025, 5(4), 44; https://doi.org/10.3390/allergies5040044 - 12 Dec 2025
Cited by 1
Abstract
Shellfish allergy is among the most common food allergies (FAs) worldwide and represents a severe immunoglobulin E (IgE)-mediated FA with tropomyosin functioning as the predominant pan-allergen. Current management of shellfish allergies is strictly palliative with allergen avoidance, underscoring the critical need for disease-modifying
[...] Read more.
Shellfish allergy is among the most common food allergies (FAs) worldwide and represents a severe immunoglobulin E (IgE)-mediated FA with tropomyosin functioning as the predominant pan-allergen. Current management of shellfish allergies is strictly palliative with allergen avoidance, underscoring the critical need for disease-modifying therapies. While conventional allergen-specific immunotherapy (AIT) approaches, namely oral and sublingual immunotherapies, demonstrate capacity for desensitization, more clinical applications are needed in the potential safety concerns and prolonged treatment durations. Innovative treatments, such as the design of modified shellfish allergens, DNA vaccine technologies, and nanoparticle-based delivery platforms such as virus-like particles (VLP), show efficacy and potential in inducing protective antibodies while promoting antigen-specific immune tolerance with reduced allergenic risks. These innovative approaches hint at a promising pathway in achieving safe, effective, and long-lasting clinical tolerance for shellfish allergy. This review describes the current perspectives on allergen immunotherapy regarding shellfish allergy and analyzes emerging therapeutic strategies poised to overcome these limitations.
Full article
(This article belongs to the Section Food Allergy)
►▼
Show Figures
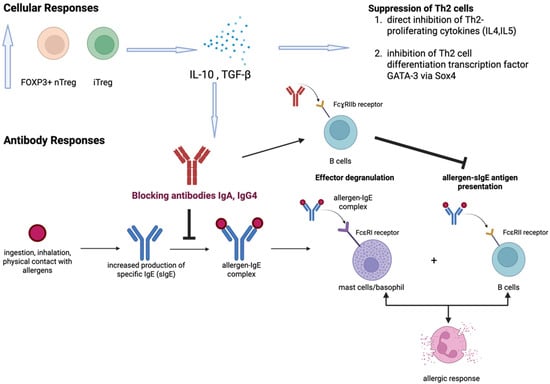
Figure 1
Open AccessEditor’s ChoiceReview
Multiple Nut Allergies and Anaphylaxis Risk in Children: A Narrative Review
by
Aleksandra Ossowska, Adrian T. De Jager, Kasith Abdul Cader and Danusha Sanchez
Allergies 2025, 5(4), 43; https://doi.org/10.3390/allergies5040043 - 12 Dec 2025
Cited by 1
Abstract
Pediatric food allergies are an escalating public health concern, with nut allergies representing a primary cause of persistent hypersensitivity and anaphylaxis. New data suggests that pediatric populations with multiple nut allergies (MNA) may be at higher anaphylaxis risk than their counterparts with single
[...] Read more.
Pediatric food allergies are an escalating public health concern, with nut allergies representing a primary cause of persistent hypersensitivity and anaphylaxis. New data suggests that pediatric populations with multiple nut allergies (MNA) may be at higher anaphylaxis risk than their counterparts with single nut allergies. Despite this, there is an absence of literature posing multiple nut allergies against singular nut allergy cases. The majority of the research in this topic is directed towards singular nut allergy, without any differentiation between children with one versus multiple sensitivities. Epidemiological evidence indicates that multiple nut allergies are associated with lifelong sensitization, high cross-reactivity potential and increased risk and severity of reactions. Compounding clinical risk factors reinforce the already high risk associated with MNA and indicate that these children require careful monitoring and individual management. Diagnostic tools, including component-resolved diagnostics and oral food challenges, enable differentiation between true multi-nut sensitization and cross-reactivity, guiding targeted interventions. Management strategies must therefore be multifaceted, encompassing selective allergen avoidance, emergency preparedness with epinephrine auto-injectors, asthma control, nutritional support, and psychosocial care. Recognizing MNA as a distinct, high-risk phenotype highlights the necessity of precision-based, biomarker-driven clinical approaches to optimize safety, reduce morbidity, and improve quality of life for affected pediatric populations.
Full article
(This article belongs to the Section Pediatric Allergy)
►▼
Show Figures

Figure 1
Open AccessReview
Alpha-Gal Syndrome: A Concise Review
by
Prashant Kaushik, Faryal S. Bhatti, Tanmay Bangale and Creticus P. Marak
Allergies 2025, 5(4), 42; https://doi.org/10.3390/allergies5040042 - 1 Dec 2025
Abstract
Alpha-gal syndrome (AGS) is an emerging, relatively newly recognized allergic disorder with clinical manifestations that occur as a result of hypersensitivity reactions to oligosaccharide galactose-α-1,3-galactose (α-gal), a carbohydrate present in lower-mammalian meat, dairy products, and some biopharmaceutical products. These reactions are delayed with
[...] Read more.
Alpha-gal syndrome (AGS) is an emerging, relatively newly recognized allergic disorder with clinical manifestations that occur as a result of hypersensitivity reactions to oligosaccharide galactose-α-1,3-galactose (α-gal), a carbohydrate present in lower-mammalian meat, dairy products, and some biopharmaceutical products. These reactions are delayed with oral ingestion of the antigen but can be immediate with intravascular or other parenteral antigenic exposure. Over the past 15 years, many revelations have occurred in the realm of AGS. However, there is still a huge unmet need related to its pathophysiology, diagnostics, timely recognition, and management. This article is geared towards providing a review of AGS for healthcare providers (HCPs) from all realms of medicine. It is a universal challenge, with cases being recognized from various parts of the world. Hence, it is critically important for HCPs planet-wide to pay heed to the prompt recognition of AGS and educate their patients. This can prevent morbidity as well as potentially fatal complications like severe anaphylaxis. It is a narrative clinical review. The PubMed database was searched from 2009 to 2025. Alpha-gal syndrome and related topics were included in the search engine.
Full article
(This article belongs to the Section Diagnosis and Therapeutics)
►▼
Show Figures
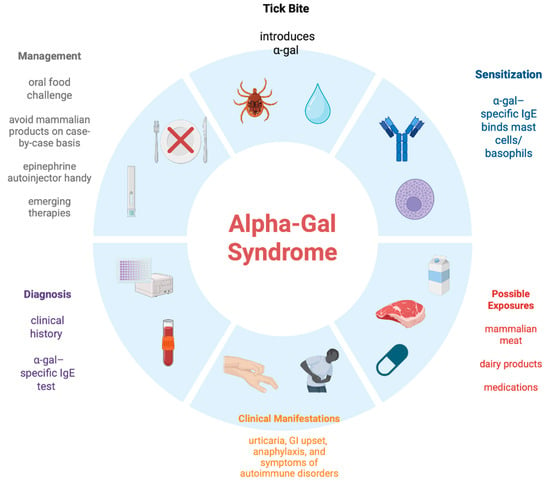
Figure 1
Highly Accessed Articles
Latest Books
E-Mail Alert
News
Topics
Topic in
Cells, Immuno, IJMS, JCM, Allergies, Dermato
Skin Barrier Function and Immune Mediators as Key Therapeutic Targets of Main Inflammatory Diseases
Topic Editors: Marco Manfredini, Carlo PincelliDeadline: 31 August 2026
Topic in
Biomedicines, Cancers, Cells, JCM, Pharmaceutics, Reports, Allergies
The Tumor Microenvironment, Immuno-Oncology, and Immune Checkpoint: Implications for Current and Emergent Immunotherapies, 2nd Edition
Topic Editors: Joaquim Carreras, Luis J. Castro-VegaDeadline: 31 December 2026

Conferences
Special Issues
Special Issue in
Allergies
Molecular Mechanisms of Allergy and Asthma: 4th Edition
Guest Editor: Daniel P. PotaczekDeadline: 31 October 2026





