Abstract
Objective: Fluoride is widely recognized for its preventive role against secondary caries. This systematic review aimed to evaluate how environmental and material factors influence fluoride ion release from metal-reinforced glass ionomer cements. Methods: A structured literature search was performed in March 2025 across PubMed, Scopus, and Web of Science databases. Search terms included combinations of fluoride release AND glass ionomer AND silver OR zinc OR strontium OR copper. The study selection process followed PRISMA 2020 guidelines and was organized using the PICO framework. Out of 281 initially identified records, 153 were screened based on titles and abstracts. After applying predefined eligibility criteria, 23 studies met the inclusion requirements and were included in the qualitative analysis. Results: Among the 23 included publications, 12 involved glass ionomers modified with silver, and 6 of these reported an increase in fluoride release. Seven studies focused on zinc-modified cements, and four examined materials reinforced with strontium. Conclusions: The addition of strontium, titanium oxide, silver nanoparticles, or zirconium oxide increases the release of fluoride ions, while sintered silver reduces it. There is a great discrepancy among researchers regarding the effect of the addition of zinc oxide and its appropriate amount in the glass ionomer material.
Keywords:
fluoride release; glass-ionomer; metal-modified glass ionomer; silver; zinc; strontium; copper 1. Introduction
Fluoride release from dental materials plays a critical role in caries prevention and the long-term success of restorative treatments. Among various materials, metal-modified glass-ionomer cements (M-GICs) have attracted attention due to their ability to release fluoride over time, contributing to remineralization of adjacent tooth structures and inhibition of bacterial growth [1,2,3]. This ion-exchange mechanism helps protect the enamel and dentin, especially in patients at high caries risk. Fluoride ions can reduce demineralization by enhancing the formation of fluorapatite, which is more resistant to acid attacks [4,5,6]. Furthermore, fluoride possesses antibacterial properties, disrupting bacterial metabolism and reducing acid production [7,8]. However, the effectiveness of fluoride release depends on both material composition and environmental conditions, such as pH, temperature, and storage medium [9,10,11]. Recent studies have also explored the impact of surface coatings and nanomodifications on fluoride release profiles [12,13,14,15,16]. Variability in fluoride release among M-GICs has prompted interest in evaluating how different formulations and clinical factors influence this process [17,18]. Understanding these interactions is essential for optimizing material selection and enhancing therapeutic outcomes.
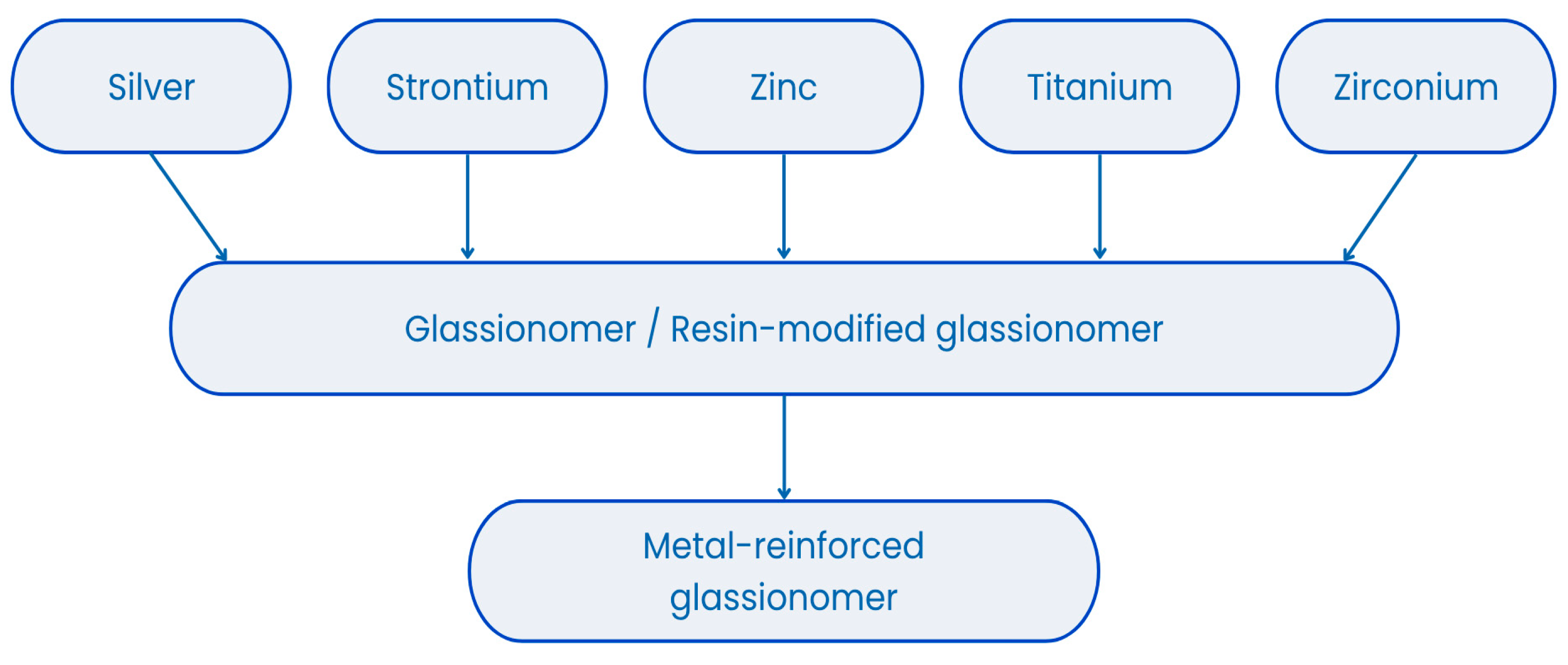
Metal-modified glass-ionomer cements (M-GICs) are hybrid dental materials developed to enhance the mechanical properties of glass-ionomer cements (GICs) [17,19]. They are composed of fluoroaluminosilicate glass powder and polyacrylic acid, with the addition of metal particles such as silver, titanium, or stainless steel (see Figure 1) to improve wear resistance, compressive strength, and radiopacity [20,21,22]. M-GICs maintain the essential features of traditional GICs, including chemical bonding to tooth structures, fluoride ion release, and biocompatibility, which contribute to caries prevention and enamel remineralization [20,23]. Their reinforced composition makes them suitable for use in stress-bearing areas, core build-ups, and atraumatic restorative treatment (ART) techniques, especially in pediatric and community dentistry [20,24,25]. The presence of metal may influence fluoride ion exchange and long-term release, which are key factors in their preventive function [12,26]. However, these materials may present esthetic limitations due to their opacity or metallic color, making them less ideal for anterior restorations [27]. Despite this, their durability, therapeutic ion release, and antimicrobial activity have made them valuable for clinical use [28]. Ongoing research explores nanomodifications and formulation adjustments to improve their physical, biological, and esthetic performance for broader indications [29,30,31,32,33,34,35].
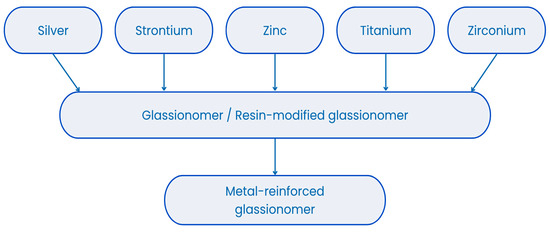
Figure 1.
Metals present in metal-reinforced glass ionomers.
The release of fluoride from dental materials used for tooth restoration plays a significant role in preventing and inhibiting the recurrence of caries [36,37,38]. The amount and dynamics of fluoride release are influenced by several factors. One of the most important of these is the pH of the environment in which the material is located. It has been proven that a decrease in pH increases the amount of fluoride ions released. This relationship is beneficial because increased activity of cariogenic bacteria triggers mechanisms that lead to the inhibition of their metabolism [39,40]. Another important factor is the medium in which the material is stored. Studies have shown that a greater amount of fluoride is released into deionized water than into artificial saliva. This is due to the influence of other ions on the solubility of dental materials [41,42]. Other important factors include the composition of the material and the concentration of the fluoride-containing substance. In the case of GIC-type materials, other factors include the porosity of the surface and the ability to charge fluoride, as well as the acid-base reaction at which a sudden release of large amounts of fluoride occurs due to its loose binding to cement [42,43]. In the case of resin-modified GICs and composite materials, fluoride release is influenced by the presence of the resin matrix, its hydrophilicity, the temperature at which the material is located, the size and amount of filler particles, and even the surface finishing technique of the filling [41,44,45,46].
While the release of fluoride ions from restorative dental materials is widely considered beneficial due to its cariostatic and antibacterial properties, it is equally important to take into account the potential risks associated with prolonged or excessive fluoride exposure. Although fluoride enhances remineralization and inhibits bacterial metabolism, excessive systemic intake may have adverse biological consequences. Elevated levels of fluoride have been shown to disrupt the mineralization of hard dental tissues, including both enamel and dentin, particularly during tooth development. This may result in dental fluorosis, which manifests as enamel hypomineralization and structural alterations in both enamel and dentin layers [47].
To ensure clinical safety, fluoride release from restorative materials should be carefully controlled and maintained within a therapeutic range that offers effective local action without contributing to systemic accumulation. Although glass ionomer cements typically exhibit an initial burst of fluoride release followed by a gradual decline, their long-term release patterns must be considered, especially in treatments involving young patients or those with multiple restorations [48]. These factors highlight the need for designing materials with predictable, sustained, and clinically appropriate fluoride release to balance caries prevention with overall biological safety.
This review aims to assess the influence of environmental and material factors on the release of fluoride from metal-modified glass ionomer cements. Having reviewed studies on this topic, we concluded that a comprehensive systematic review is needed. No such review was found in the literature. A detailed analysis of the factors responsible for the amount and mode of fluoride release is essential in order to understand the specificity of the type of glass ionomer cement being studied. This will help clinicians to select and use the material most efficiently in a clinical setting.
2. Materials and Methods
2.1. Focused Question
The systematic review followed the PICO framework [49] as follows. In the case of metal-modified glass ionomer cements (population), will exposure to various environmental and material factors (investigated condition) cause a change in fluoride release (outcome) compared to conditions without such influencing factors or compared to conventional glass ionomer cements (comparison condition)?
2.2. Protocol
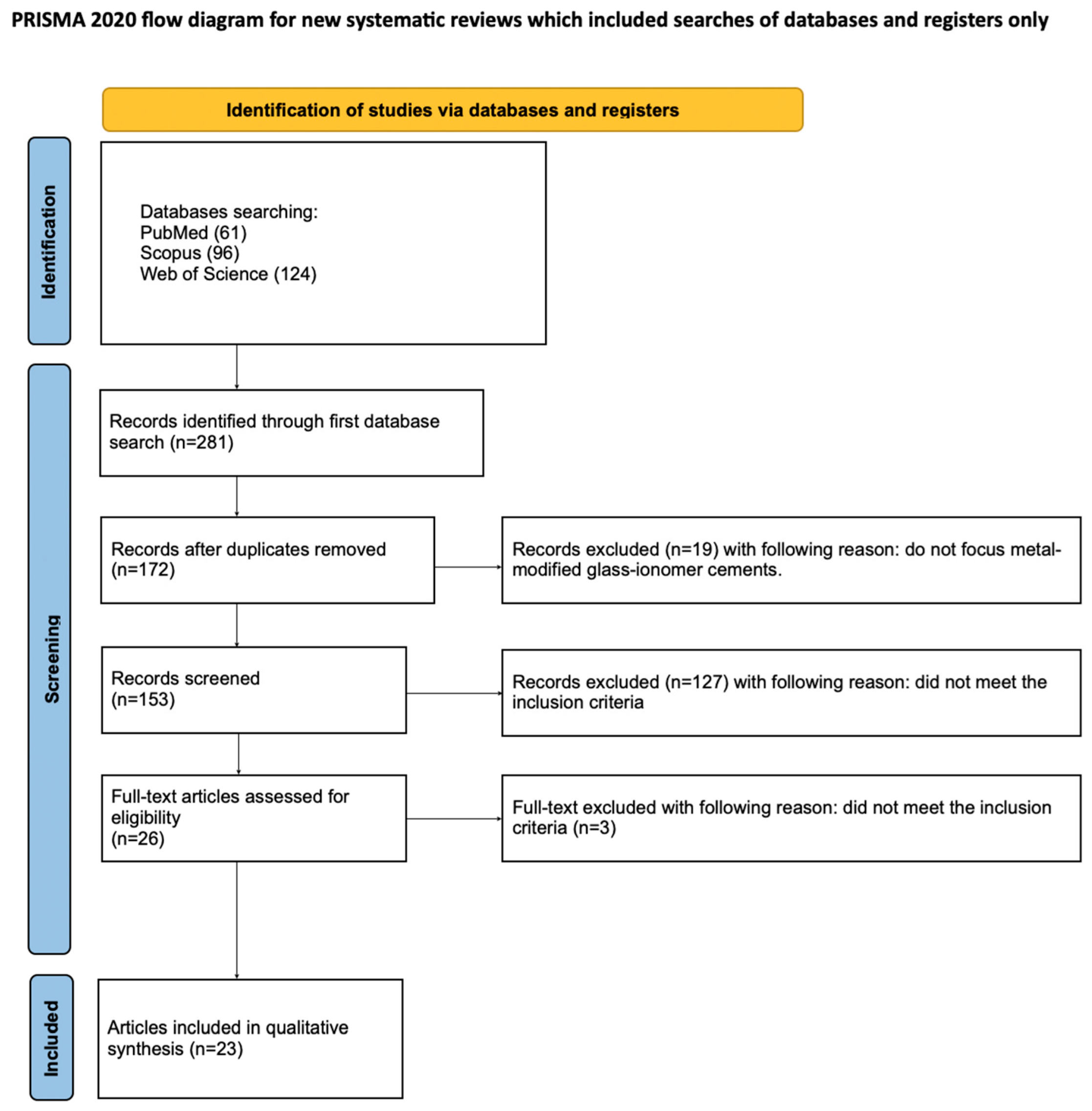
The selection process for articles in the systematic review was carefully outlined following the PRISMA flow diagram [50] (see Figure 2). The systematic review was registered on the Open Science Framework under the following link: http://osf.io/7t5be (accessed on 26 May 2025). The completed checklist is provided in the Supplementary Materials (see Supplementary Table S1).
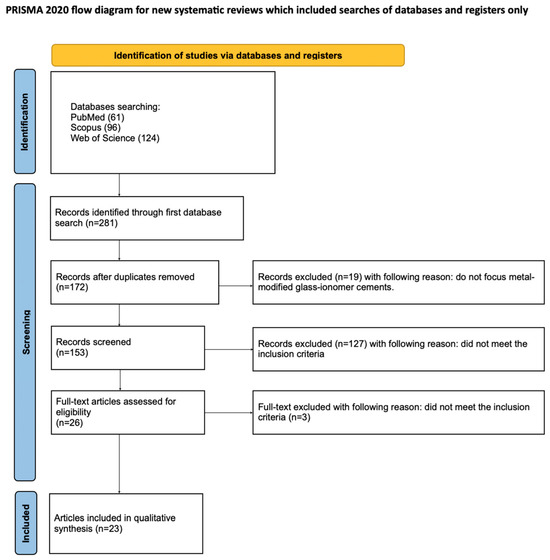
Figure 2.
The PRISMA 2020 flow diagram.
2.3. Eligibility Criteria
Studies were considered acceptable for inclusion in the review if they met the following criteria:
- Studies involving the examination of metal-modified glass-ionomer cements;
- Studies evaluating fluoride release;
- In vitro studies;
- Full-text articles
- Studies in English;
The exclusion criteria the reviewers agreed upon were as follows:
- Studies not focusing on glass-ionomers modified with metal/metal particles;
- Measurement of other properties than fluoride release;
- Non-English paper;
- Systematic review papers;
- Review articles;
- No full text accessible;
- Duplicated publications.
No restrictions were applied with regard to the year of publication.
2.4. Information Sources, Search Strategy, and Study Selection
Up to March 2025, an extensive literature search was performed using the PubMed, Scopus, and Web of Science (WoS) databases to identify studies that met the predefined inclusion criteria. The search was focused on exploring factors affecting fluoride content in tea infusions and was limited to titles and abstracts containing the keywords: (fluoride release AND glass ionomer) AND (silver OR zinc OR strontium OR copper). Articles were screened according to established eligibility criteria, and only studies with available full-text access were included in the final analysis.
2.5. Data Collection Process and Data Items
Six independent reviewers (S.K., J.K., A.K., J.K., S.K., and M.M.) independently screened and selected articles that fulfilled the inclusion criteria. Key data extracted from each study included the first author’s name, year of publication, study design, article title, metal type used to modify glass-ionomer cement, and measured fluoride content. All extracted information was systematically documented using a standardized Excel spreadsheet (Microsoft Excel 365, Version 2505, Build 16.0.18827.20102, 64-bit).
2.6. Risk of Bias and Quality Assessment
In the initial stage of study selection, all reviewers independently assessed titles and abstracts to minimize selection bias. Cohen’s kappa coefficient was used to evaluate the consistency of agreement between reviewers. Any discrepancies concerning the inclusion or exclusion of articles were resolved through group discussion among the authors [51].
2.7. Quality Assessment
The methodological quality of each included study was independently evaluated by two blinded reviewers (J.M. and M.D.) using the Joanna Briggs Institute (JBI) checklist for quasi-experimental studies (nonrandomized designs). The authors selected this tool because it fits the type of studies assessed, enables a reliable quality assessment, is methodologically recognized, enhances transparency and repeatability, and is consistent with international standards. This assessment tool consists of nine targeted questions, such as:
- Is it clear in the study what is the ‘cause’ and what is the ‘effect’?
- Were the participants included in any similar comparisons?
- Were the participants included in any comparisons receiving similar treatment/care, other than the exposure or intervention of interest? Was there a control group?
- Were there multiple measurements of the outcome both before and after the intervention/exposure?
- Was a follow-up completed, and if not, were differences between groups in terms of their follow-up adequately described and analyzed? Were the outcomes of participants included in any comparisons measured in the same way?
- Were the outcomes measured in a reliable way?
- Was an appropriate statistical analysis used?
Reviewers responded to each item using one of four options: “yes”, “no”, “unclear”, or “not applicable”. Any differing judgments were discussed until a mutual agreement was reached. To evaluate the consistency between raters, Cohen’s kappa was calculated using MedCalc (version 23.1.7, MedCalc Software Ltd., Ostend, Belgium). The resulting kappa coefficient was 0.84 (p < 0.001), signifying a very high level of agreement and reliability across reviewers.
3. Results
3.1. Study Selection
A total of 281 potentially relevant articles were identified through an initial search of PubMed, Scopus, and Web of Science. After duplicate removal, 172 records were retained for screening. An evaluation of titles and abstracts led to the exclusion of 146 articles that were unrelated to fluoride release from metal-reinforced glass ionomers. Of the 26 full-text articles assessed for eligibility, 3 were excluded for not meeting the inclusion criteria [33,52,53]. Consequently, 23 studies were included in the qualitative synthesis [54,55,56,57,58,59,60,61,62,63,64,65,66,67,68,69,70,71,72,73,74,75,76]. The high degree of variability among these studies precluded the possibility of conducting a meta-analysis.
3.2. General Characteristics of the Included Studies
Among the qualified works, the most frequently added and tested metal to glass ionomers was silver. Its compounds appeared in 12 publications [54,55,56,57,59,61,62,63,72,73,75,76]; in 7 studies, zinc compounds were used [59,61,64,65,66,67,74], and in 4, strontium [58,60,68,71]. Saxena et al. [70] studied the Zirconomer material in which zirconium oxide is present, and Cibim et al. [69] and Wassel et al. [62] experimentally added titanium oxide nanotubes to glass ionomer. Deionized water was standardly used as the sample storage environment [54,55,56,57,58,59,60,61,62,63,65,66,67,68,72,73,75,76]; four authors decided to use artificial saliva [64,70,74,76]; Shahid et al. [71] used acetic acid solution at pH 4; and Cibim et al. [69] used demineralizing and remineralizing solutions. The most frequently chosen measurement method was the use of an ion-selective electrode. It was used in 19 works [54,56,58,60,61,62,63,64,65,66,68,69,70,71,72,73,74,75,76]; in 2 studies, high performance liquid chromatography (HPLC) was used [57,59]; Guo et al. [55] used an ion chromatograph (IC); and Putri et al. [67] used a spectrophotometer. Some researchers decided to measure the release of other ions, apart from fluorine, and so in four works the level of zinc [64,65,66,74] was checked; in six, calcium [57,58,60,66,68,71]; in five, aluminum [57,58,60,66,71]; in two, silicon [60,66]; in three, strontium [58,66,71], in two, sodium [57,66], in three, phosphorus [57,58,66], and in two, silver [54,57]. Pardi et al. [54] additionally studied the release of vanadium, and Bahammam et al. [66] the release of oxygen, magnesium, sulfur, and zirconium (see Table 1).

Table 1.
General characteristics of studies.
3.3. Main Study Outcomes
3.3.1. Influence of Silver Additions on Fluoride Release
Four publications investigated the Ketac Silver material from GC, which contains sintered silver [72,73,75,76]. Three of these reported lower fluoride release compared to glass ionomers without silver [72,75,76]. Hattab et al. [76] even observed a fourfold decrease. In contrast, Xu et al. [73] reported higher fluoride release, although accompanied by poorer mechanical properties. In studies where silver nanoparticles were used, five authors reported an increase in fluoride release [54,56,59,61,62]. However, in AlMatar et al. [59], this effect was observed in combination with ZnO, and Wassel et al. [62] combined silver with TiO2. Pardi et al. [54] and Raghimi et al. [56] found increased fluoride only at specific concentrations. Conversely, Guo et al. [55], Alshehri et al. [63], and Qasim et al. [57] did not observe improvement or reported reduced fluoride release.
3.3.2. Influence of Zinc Oxide and Its Compounds
Studies by Gunay et al. [61] and Bahammam et al. [66] showed that zinc addition decreases fluoride release. Malekhoseini et al. [65] confirmed this at 3% ZnO, while 2% led to increased release. Putri et al. [67] observed an increase at 10% ZnO, with no further effect at higher levels. Osinaga et al. [74] found no effect of ZnSO4 on fluoride release, though antibacterial properties improved. Kohno et al. [64] concluded that the fluoride level was insufficient for bacterial inhibition.
3.3.3. Influence of Strontium Additions
All studies involving strontium-modified glass ionomers consistently reported increased fluoride release [58,60,68,71]. For example, Karimi et al. [68] observed higher fluoride levels with increased concentrations of strontium-containing ACP nanoparticles. Shahid et al. [71] measured fluoride release across various combinations of SrO and SrF2 and found a clear trend: groups with 1.5% SrF2 and 1% SrO showed the highest cumulative fluoride values (2.61 mequiv/g). Thongsri et al. [60] also demonstrated that materials with 1% bioactive strontium glass had improved fluoride rerelease and better compressive strength than the control group. Overall, strontium-modified GICs showed consistent improvements in fluoride release across multiple studies and conditions.
3.3.4. Influence of Titanium Dioxide
Cibim et al. [69] examined the effect of TiO2 nanotube additions (3%, 5%, and 7%) in both demineralizing and remineralizing solutions. They found that fluoride release increased at 3% and 7% concentrations, but not at 5%. In demineralizing solution, the 3% group reached 1.172 ppm on day 15, the highest recorded in their experiment. Surface hardness also improved in the 5% group (118.25 ± 4.21 HV). Wassel et al. [62] tested a GIC modified with 5% TiO2 and reported slightly reduced cumulative fluoride release (0.047 mg/cm2) compared to the AgNP-modified version (0.065 mg/cm2), but compressive strength was significantly higher (166.31 ± 15.08 MPa). These results suggest that TiO2 may enhance mechanical properties while having a variable effect on fluoride release depending on concentration and experimental conditions.
3.3.5. Influence of Zirconium Dioxide
Only one study by Saxena et al. [70] investigated GIC modified with zirconium oxide (Zirconomer). The fluoride release was significantly higher at all time points compared to Fuji IX. For instance, on day 7, Zirconomer released 35.65 ppm versus 15.46 ppm from Fuji IX. The material also showed greater antibacterial activity against Streptococcus mutans and Lactobacillus casei. However, no data on mechanical properties were provided. Given that this is a single study, the promising results should be interpreted cautiously until validated by further research.
3.3.6. Comparative Summary
The studies suggest that the addition of metals may either enhance or reduce fluoride release, depending on their type, form, and concentration. The most consistent positive effect was seen with strontium, which reliably increased fluoride release across all studies. Titanium dioxide also showed promise, particularly when used at specific concentrations. Zirconium oxide demonstrated the highest fluoride release among compared materials in a single study. In contrast, the effects of silver and zinc varied significantly depending on their chemical form and concentration. These results highlight the importance of selecting additives based on both the desired fluoride release profile and the mechanical performance of the final material. The findings summarized here are supported by a wide range of studies covering various metal modifications and testing conditions, including those by Pardi et al. [54], Guo et al. [55], Raghimi et al. [56], Qasim et al. [57], Potiprapanpong et al. [58], AlMatar et al. [59], Thongsri et al. [60], Gunay et al. [61], Wassel et al. [62], Alshehri et al. [63], Kohno et al. [64], Malekhoseini et al. [65], Bahammam et al. [66], Putri et al. [67], Karimi et al. [68], Cibim et al. [69], Saxena et al. [70], Shahid et al. [71], Selimovic-Dragas et al. [72], Xu et al. [73], Osinaga et al. [74], Helvatjoglu-Antoniades et al. [75], and Hattab et al. [76] (see Table 2).

Table 2.
Detailed characteristics of included studies.
3.4. Quality Assessment
For all of the 9 questions, there were 2 papers that scored maximum points and received a positive answer to 9 of them [54,70] and the remaining 21 papers received a positive answer to 8 of them [55,56,57,58,59,60,61,62,63,64,65,66,67,68,69,71,72,73,74,75,76] (see Table 3).

Table 3.
Quality assessment—JBI checklist for quasi-experimental studies (nonrandomized experimental studies).
4. Discussion
This study aims to assess how both the material composition and external environmental conditions influence the fluoride release behavior of metal-reinforced glass ionomer cements (MGICs). Our synthesis of 23 studies demonstrated that the impact of metal incorporation is highly dependent on the type, form, and concentration of additives [54,55,56,57,58,59,60,61,62,63,64,65,66,67,68,69,70,71,72,73,74,75,76]. The data suggest that while certain modifications, such as optimal levels of silver or titanium nanoparticles, may promote fluoride release [54,56,69], others, like sintered silver or excessive strontium content, may reduce it [68,72,75,76]. Both Pardi et al. [54] and Hattab et al. [76] reported early peaks in fluoride release, with Pardi observing a maximum on day 7 and Hattab noting high initial values that stabilized after two weeks. This behavior suggests that short-term efficacy may be overestimated if cumulative release profiles are not taken into account. The synthesis highlights dose- and formulation-dependent patterns across diverse experimental settings, such as distilled water, artificial saliva, or acidic environments [54,55,56,57,58,59,60,61,62,63,64,65,66,67,68,69,70,71,72,73,74,75,76]. Differences in ion release behavior observed under deionized water versus artificial saliva further illustrate the complexity of translating lab data to clinical conditions [76]. Overall, the findings underscore that fluoride release cannot be attributed to metal addition alone, but to its integration into specific glass matrices, setting mechanisms, and environmental exposures.
Our analysis showed that cermet cements containing sintered silver consistently exhibit reduced fluoride release compared to other glass ionomers. In three studies, Ketac Silver demonstrated notably lower cumulative fluoride values [72,75,76]. Hattab et al. [76] reported a fourfold decrease in release versus Ketac-Fil and Fuji II in deionized water, while Helvatjoglu-Antoniades et al. [75] observed only 3.1 µg/mm2 from Ketac Silver compared to 8.3 and 11.7 µg/mm2 in Fuji III and Miracle Mix, respectively. Xu et al. [73] found a relatively higher release (318 µg/cm2—cumulative fluoride release in 21 days), yet still below Miracle Mix and coupled with reduced compressive strength. These results, consistent across durations and media, suggest that cermets may underperform in fluoride-based prevention. Similarly, Yip et al. [77] also reported that the cermet Ketac Silver released less fluoride than other glass ionomer cements, a finding supported by Wandera et al. [78], who observed lower fluoride release from Ketac Silver compared to Ketac-Fil in both distilled water and artificial saliva. Originally developed for improved strength, sintered silver cermets may offer limited caries-inhibitory benefits and should be reconsidered for high-risk patients due to low fluoride release and poor recharge capacity.
The current synthesis establishes that additive effects on fluoride release are not uniform and depend on chemical formulation and dosing. Silver nanoparticles appear to enhance fluoride release primarily within specific concentration ranges, as shown in materials modified with AgVO3 or Ag/HA/Si [54,56]. In Pardi et al.’s study [54], fluoride release peaked at day 7 in the 1% and 2.5% groups, then declined. In contrast, Raghimi et al. [56] demonstrated statistically significant improvements at 1% and 2%, with plateauing at higher doses. However, combinations involving zinc oxide or titanium dioxide did not always result in further increases [59,62]; in fact, AlMatar et al. [59] found that the simultaneous addition of 5% ZnONP and 5% AgNP reversed the fluoride gain achieved by 5% AgNP alone. According to the findings of Wasel et al. [62], although the addition of 5% Ag-NP did not lead to a statistically significant increase in fluoride release compared to the control group, a significantly higher fluoride release was observed in comparison with the TiO2-NP group. Zinc showed a threshold-dependent trend: 2% ZnO increased fluoride release, whereas 3% caused a marked decline [65]. Putri et al. [67] reported similar results with ZnO at 10% enhancing, but 15% reducing fluoride release. Titanium dioxide was effective at 3% and 7% but not 5% [69]. Strontium compounds varied: while Shahid et al. [71] reported a large increase at specific SrF2/SrO ratios (1.5%/1%), Karimi et al. [68] found a decrease in fluoride with increasing Sr content. The study by Saxena et al. [70] showed that GIC containing ZrO2 (Zirconomer) released higher amounts of fluoride compared to the conventional GIC (Fuji IX) at all time points. This indicates that the incorporation of ZrO2 enhances fluoride ion release and prolongs its availability over time.
Notably, the findings contextualize fluoride release in relation to potential antibacterial and remineralizing functions. Based on the study by Malekhoseini et al. [65], the addition of 2% ZnO to RMGI cement provided the strongest antibacterial effect and the highest fluoride release. Increasing the concentration to 3% did not enhance antibacterial activity and reduced fluoride release, indicating a threshold beyond which performance may decline. Guo et al. [55] demonstrated reduced biofilm formation with AgNW-modified GICs despite unchanged fluoride levels. Osinaga et al. [74] reported that ZnSO4-modified GICs showed improved antibacterial properties without observable negative effects on overall fluoride release patterns. Zirconomer exhibits stronger antibacterial effects against Streptococcus mutans and Lactobacillus casei, along with a higher level of fluoride release [70]. According to Cibim et al. [69], incorporating 5% TiO2 into GIC enhanced its fluoride ion release capacity. Alshehri et al. [63] further showed that silver-modified GICs did not enhance fluoride recharging or remineralization potential. Kohno et al. [64] confirmed that fluoride concentrations in Zn-containing GICs were insufficient to inhibit biofilm growth. According to the study by Wassel et al. [62], glass ionomers modified with Ag and TiO2 exhibited greater antibacterial activity, as evidenced by larger inhibition zones compared to conventional GICs. In the study by Gunay et al. [61], Riva Silver and ChemFil Rock showed markedly stronger antibacterial activity than the conventional glass ionomer Ketac Molar Easymix. Importantly, the evidence underscores that while fluoride plays a significant role, it cannot serve as the sole predictor of clinical benefit. Therefore, interpreting biological effects should include considerations of ion release synergy, local pH, and material structure.
Numerous studies have confirmed that the incorporation of nanoparticles into glass ionomer cements (GICs) can significantly alter their mechanical properties, often in a trade-off-dependent manner. Guo et al. [55] observed that silver nanowires and nanoparticles decreased both compressive strength and microhardness at all tested concentrations. AlMatar et al. [59] reported that combining AgNP and ZnONP enhanced fluoride release but lowered microhardness compared to the control. Cibim et al. [69] found that TiO2 at 3–5% increased surface hardness, but 7% reduced it; surface roughness showed an increasing trend with higher TiO2 concentrations, though the relationship was not linear. In the study by Raghimi et al. [56], compressive strength improved up to 1% Ag/HA/Si but dropped at 2%. Similarly, Karimi et al. [68] reported that increasing Sr content enhanced compressive strength up to a point, but this coincided with reduced fluoride release at higher doses. Wassel et al. [62] showed that TiO2NP addition increased compressive strength without drastically changing fluoride output. Meanwhile, Potiprapanpong et al. [58] demonstrated that Sr/F-BGNPs improved fluoride release, but the formulation with the highest release (H5S10) had the lowest biaxial flexural strength. Finally, Osinaga et al. [74] showed slight decreases in flexural strength with ZnSO4-modified GICs. Collectively, these findings highlight the need to balance mechanical enhancement with functional efficacy when designing nanoparticle-modified GICs.
Based on the reviewed studies, several modified glass ionomer cements appear promising for future clinical use due to their enhanced fluoride release and favorable supplementary properties. RMGICs modified with strontium/fluoride-containing bioactive glass nanoparticles and HEMA demonstrated high fluoride release and good biocompatibility [58]. Although the formulation with 10% Sr/F-BGNPs released slightly more fluoride, the 5% Sr/F-BGNPs variant offered a better balance between ion release and mechanical strength. Given its comparable fluoride performance and superior flexural properties, the latter may be more appropriate for patients with parafunctional habits, high occlusal loads, or advanced tooth wear. Similarly, the addition of Ag/HA/Si hybrid nanoparticles [56] or 2% ZnO nanoparticles [65] to RMGICs significantly increased fluoride ion release; however, the 2% Ag/HA/Si concentration slightly reduced compressive strength compared to the unmodified control, suggesting that lower concentrations—1% may offer a better balance between mechanical integrity and fluoride release. GICs modified with 5% TiO2 nanoparticles showed enhanced surface hardness and fluoride release [69], and Zirconomer displayed strong antibacterial effects along with sustained fluoride release [70]. Additionally, GICs containing silver nanowires effectively reduced biofilm adherence while maintaining stable fluoride profiles [55]. These findings suggest that such formulations may offer improved therapeutic potential, particularly in high-caries-risk patients, individuals with poor oral hygiene, or pediatric patients. Their properties also make them a promising option for managing cases with multiple restorations or a history of recurrent caries.
This systematic review included studies conducted in vitro, which do not fully reflect the complex dynamics of the oral environment, including factors such as temperature fluctuations, enzymes, bacterial biofilm, and variable pH. The effect of fluoride in the oral cavity is more distributed over time and is subject to fluctuations due to the medium of saliva containing proteins and ions. Its composition and quantity change over time, which affects the solubility and diffusion of fluoride. In addition, in vitro studies of dental materials neglect long-term factors such as microcracks, abrasion, bacterial infiltration, and thermal cycling. The heterogeneity of experimental protocols, including variations in storage media, measurement intervals, and fluoride detection methods, complicates direct comparisons between studies. Moreover, many articles assessed only short-term fluoride release (up to 15 days) [55,59,60,64,65,66,67,69,71,72], which may not accurately represent long-term clinical performance. The influence of biofilm presence on fluoride release remains insufficiently explored. Therefore, it is imperative that future studies include in situ models or are conducted in clinical settings, taking into account bacterial biofilm, pH, and storage media to better mimic oral conditions. Additionally, employing multi-species biofilm models instead of single-strain bacterial cultures could improve the understanding of antimicrobial behavior in more realistic conditions. Furthermore, it is recommended to use long-term observations and standardized measurement methods. Investigating the relationship between fluoride release, mechanical durability, and antibacterial activity over time would be particularly valuable for the development of optimized metal-modified glass ionomer cements (MGIC). Such approaches would help reduce discrepancies between in vitro results and actual clinical outcomes, ultimately supporting the development of more effective restorative materials.
5. Conclusions
The analysis of the studies showed that adding silver in the form of nanoparticles in the amount of 2–2.5% by weight to the glass ionomer increases fluoride secretion, but sintered silver has the opposite effect. Even more fluoride can be obtained by adding titanium oxide together with silver nanoparticles, but this may have a negative effect on the mechanical parameters of the material. In turn, the addition of zinc oxide, in addition to increasing fluoride secretion, may bring additional benefits in the form of antibacterial action, but further research is necessary in this area due to large discrepancies between studies regarding the appropriate proportions, and it has been proven that the incorrect amount of zinc oxide can have exactly the opposite effect. The most reliable additives in terms of positive effects in clinical practice seem to be strontium, titanium oxide, and zirconium oxide. The effect of strontium is confirmed by numerous studies, but further analyses of the effect of titanium oxide and zirconium oxide are necessary due to the insufficient number of publications in this area.
Supplementary Materials
The following supporting information can be downloaded at: https://www.mdpi.com/article/10.3390/ma18133187/s1, Table S1: PRISMA 2020 Checklist.
Author Contributions
Conceptualization, S.K. (Sylwia Klimas), J.M. and M.D.; methodology, S.K. (Sylwia Klimas), S.K. (Sylwia Kiryk) and J.K. (Julia Kensy); software, S.K. (Sylwia Klimas); validation, J.M., Z.R. and M.D.; formal analysis, S.K. (Sylwia Klimas), J.M. and Z.R.; investigation, S.K. (Sylwia Klimas), S.K. (Sylwia Kiryk), J.K. (Jan Kiryk), A.K., J.K. (Julia Kensy) and M.M.; resources, S.K. (Sylwia Klimas), S.K. (Sylwia Kiryk), J.K. (Jan Kiryk), A.K., J.K. (Julia Kensy) and M.M.; data curation, S.K. (Sylwia Klimas), S.K. (Sylwia Kiryk), J.K. (Jan Kiryk), A.K., J.K. (Julia Kensy) and M.M.; writing—original draft preparation, S.K. (Sylwia Klimas), S.K. (Sylwia Kiryk), J.K. (Jan Kiryk), J.K. (Julia Kensy) and M.M.; writing—review and editing, J.M. and S.K. (Sylwia Klimas); visualization, J.K. (Jan Kiryk) and Z.R.; supervision, J.M.; project administration, J.M. and M.D.; funding acquisition, M.D. All authors have read and agreed to the published version of the manuscript.
Funding
This work was financed by a subsidy from Wroclaw Medical University.
Institutional Review Board Statement
Not applicable.
Informed Consent Statement
Not applicable.
Data Availability Statement
No new data were created or analyzed in this study. Data sharing is not applicable to this article.
Conflicts of Interest
The authors declare no conflicts of interest.
References
- Brenes-Alvarado, A.; Cury, J.A.; Brenes-Alvarado, A.; Cury, J.A. Fluoride Release from Glass Ionomer Cement and Resin-modified Glass Ionomer Cement Materials under Conditions Mimicking the Caries Process. Oper. Dent. 2021, 46, 457–466. [Google Scholar] [CrossRef]
- el Mallakh, B.F.; Sarkar, N.K. Fluoride release from glass-ionomer cements in de-ionized water and artificial saliva. Dent. Mater. 1990, 6, 118–122. [Google Scholar] [CrossRef] [PubMed]
- Aguilar-Perez, D.; Vargas-Coronado, R.; Cervantes-Uc, J.M.; Rodriguez-Fuentes, N.; Aparicio, C.; Covarrubias, C.; Alvarez-Perez, M.; Garcia-Perez, V.; Martinez-Hernandez, M.; Cauich-Rodriguez, J.V. Antibacterial activity of a glass ionomer cement doped with copper nanoparticles. Dent. Mater. J. 2020, 39, 389–396. [Google Scholar] [CrossRef] [PubMed]
- Simmer, J.P.; Hardy, N.C.; Chinoy, A.F.; Bartlett, J.D.; Hu, J.C.-C. How Fluoride Protects Dental Enamel from Demineralization. J. Int. Soc. Prev. Community Dent. 2020, 10, 134–141. [Google Scholar] [CrossRef]
- Cochrane, N.J.; Cai, F.; Huq, N.L.; Burrow, M.F.; Reynolds, E.C. New approaches to enhanced remineralization of tooth enamel. J. Dent. Res. 2010, 89, 1187–1197. [Google Scholar] [CrossRef] [PubMed]
- Piszko, P.J.; Piszko, A.; Kiryk, J.; Lubojański, A.; Dobrzyński, W.; Wiglusz, R.J.; Matys, J.; Dobrzyński, M. The Influence of Fluoride Gels on the Physicochemical Properties of Tooth Tissues and Dental Materials—A Systematic Review. Gels 2024, 10, 98. [Google Scholar] [CrossRef]
- ten Cate, J.M.; van Loveren, C. Fluoride mechanisms. Dent. Clin. N. Am. 1999, 43, 713–742. [Google Scholar] [CrossRef]
- Marquis, R.E. Antimicrobial actions of fluoride for oral bacteria. Can. J. Microbiol. 1995, 41, 955–964. [Google Scholar] [CrossRef]
- Di Lauro, A.; Di Duca, F.; Montuori, P.; Dal Piva AMde, O.; Tribst, J.P.M.; Borges, A.L.S.; Ausiello, P. Fluoride and Calcium Release from Alkasite and Glass Ionomer Restorative Dental Materials: In Vitro Study. J. Funct. Biomater. 2023, 14, 109. [Google Scholar] [CrossRef]
- Aliberti, A.; Di Duca, F.; Triassi, M.; Montuori, P.; Scippa, S.; Piscopo, M.; Ausiello, P. The Effect of Different pH and Temperature Values on Ca2+, F−, PO43−, OH−, Si, and Sr2+ Release from Different Bioactive Restorative Dental Materials: An In Vitro Study. Polymers 2025, 17, 640. [Google Scholar] [CrossRef]
- Piszko, P.J.; Kulus, M.; Piszko, A.; Kiryk, J.; Kiryk, S.; Kensy, J.; Małyszek, A.; Michalak, M.; Dobrzyński, W.; Matys, J.; et al. The Influence of Calcium Ions and pH on Fluoride Release from Commercial Fluoride Gels in an In Vitro Study. Gels 2025, 11, 486. [Google Scholar] [CrossRef]
- Morales-Valenzuela, A.A.; Scougall-Vilchis, R.J.; Lara-Carrillo, E.; Garcia-Contreras, R.; Hegazy-Hassan, W.; Toral-Rizo, V.H.; Salmerón-Valdés, E.N. Enhancement of fluoride release in glass ionomer cements modified with titanium dioxide nanoparticles. Medicine 2022, 101, e31434. [Google Scholar] [CrossRef] [PubMed]
- Tokarczuk, D.; Tokarczuk, O.; Kiryk, J.; Kensy, J.; Szablińska, M.; Dyl, T.; Dobrzyński, W.; Matys, J.; Dobrzyński, M. Fluoride Release by Restorative Materials after the Application of Surface Coating Agents: A Systematic Review. Appl. Sci. 2024, 14, 4956. [Google Scholar] [CrossRef]
- Tiwari, S.; Nandlal, B. Effect of nano-filled surface coating agent on fluoride release from conventional glass ionomer cement: An in vitro trial. J. Indian Soc. Pedod. Prev. Dent. 2013, 31, 91–95. [Google Scholar] [CrossRef]
- Herman, K.; Wujczyk, M.; Dobrzynski, M.; Diakowska, D.; Wiglusz, K.; Wiglusz, R.J. In Vitro Assessment of Long-Term Fluoride Ion Release from Nanofluorapatite. Materials 2021, 14, 3747. [Google Scholar] [CrossRef]
- Shalaby, H.A.; Soliman, N.K.; Al-Saudi, K.W. Antibacterial and preventive effects of newly developed modified nano-chitosan/glass-ionomer restoration on simulated initial enamel caries lesions: An in vitro study. Dent. Med. Probl. 2024, 61, 353–362. [Google Scholar] [CrossRef] [PubMed]
- Williams, J.A.; Billington, R.W.; Pearson, G.J. A long term study of fluoride release from metal-containing conventional and resin-modified glass-ionomer cements. J. Oral Rehabil. 2001, 28, 41–47. [Google Scholar] [CrossRef]
- Karantakis, P.; Helvatjoglou-Antoniades, M.; Theodoridou-Pahini, S.; Papadogiannis, Y. Fluoride release from three glass ionomers, a compomer, and a composite resin in water, artificial saliva, and lactic acid. Oper. Dent. 2000, 25, 20–25. [Google Scholar]
- Mitra, S.B.; Kedrowski, B.L. Long-term mechanical properties of glass ionomers. Dent. Mater. 1994, 10, 78–82. [Google Scholar] [CrossRef]
- Sarkar, N.K. Metal–matrix interface in reinforced glass ionomers. Dent. Mater. 1999, 15, 421–425. [Google Scholar] [CrossRef]
- Walls, A.W.G.; Adamson, J.; McCabe, J.F.; Murray, J.J. The properties of a glass polyalkenoate (ionomer) cement incorporating sintered metallic particles. Dent. Mater. 1987, 3, 113–116. [Google Scholar] [CrossRef]
- Lubojanski, A.; Dobrzynski, M.; Nowak, N.; Rewak-Soroczynska, J.; Sztyler, K.; Zakrzewski, W.; Dobrzynski, W.; Szymonowicz, M.; Rybak, Z.; Wiglusz, K.; et al. Application of Selected Nanomaterials and Ozone in Modern Clinical Dentistry. Nanomaterials 2021, 11, 259. [Google Scholar] [CrossRef] [PubMed]
- Cvjeticanin, M.; Ramic, B.; Milanović, M.; Veljović, D.; Andjelkovic, A.; Maletic, S.; Jevrosimov, I.; Bajkin, B.; Guduric, V. Cell viability assessment and ion release profiles of GICs modified with TiO2- and Mg-doped hydroxyapatite nanoparticles. J. Dent. 2024, 145, 105015. [Google Scholar] [CrossRef]
- Gloria D’costa, V.; Singhal, D.K.; Acharya, S. Efficacy of GC Gold Label 9 and GC Miracle Mix ® Restorations Efficacy of GC Gold Label 9 and GC Miracle Mix® Restorations using Atraumatic Restorative Treatment (ART) in Rural Settings: A Randomized Controlled Trial. J. Clin. Pediatr. Dent. 2020, 44, 148–153. [Google Scholar] [CrossRef]
- Sztyler, K.; Wiglusz, R.J.; Dobrzynski, M. Review on Preformed Crowns in Pediatric Dentistry—The Composition and Application. Materials 2022, 15, 2081. [Google Scholar] [CrossRef]
- Williams, J.A.; Billington, R.W.; Pearson, G. Silver and fluoride ion release from metal-reinforced glass-ionomer filling materials. J. Oral Rehabil. 1997, 24, 369–375. [Google Scholar] [CrossRef] [PubMed]
- Almuhaiza, M. Glass-ionomer cements in restorative dentistry: A critical appraisal. J. Contemp. Dent. Pract. 2016, 17, 331–336. [Google Scholar] [CrossRef]
- Zheng, L.; Li, K.; Ning, C.; Sun, J. Study on antibacterial and fluoride-releasing properties of a novel composite resin with fluorine-doped nano-zirconia fillers. J. Dent. 2021, 113, 103772. [Google Scholar] [CrossRef]
- Najeeb, S.; Khurshid, Z.; Zafar, M.S.; Khan, A.S.; Zohaib, S.; Martí, J.M.N.; Sauro, S.; Matinlinna, J.P.; Rehman, I.U. Modifications in Glass Ionomer Cements: Nano-Sized Fillers and Bioactive Nanoceramics. Int. J. Mol. Sci. 2016, 17, 1134. [Google Scholar] [CrossRef]
- Gu, Y.W.; Yap, A.U.J.; Cheang, P.; Khor, K.A. Effects of incorporation of HA/ZrO2 into glass ionomer cement (GIC). Biomaterials 2005, 26, 713–720. [Google Scholar] [CrossRef]
- Alaohali, A.; Brauer, D.S.; Gentleman, E.; Sharpe, P.T. A modified glass ionomer cement to mediate dentine repair. Dent. Mater. 2021, 37, 1307–1315. [Google Scholar] [CrossRef]
- Guo, T.; Yang, M.; Wang, D.; Zheng, J.; Gao, S.S. Antibiofilm and mechanical properties of silver nanowire-modified glass ionomer cement. J. Dent. 2023, 135, 104569. [Google Scholar] [CrossRef]
- Tjan, A.H.L.; Morgan, D.L. Metal-reinforced glass ionomers: Their flexural and bond strengths to tooth substrates. J. Prosthet. Dent. 1988, 59, 137–141. [Google Scholar] [CrossRef]
- Chungk, H. The properties of metal-reinforced glass ionomer materials. J. Oral Rehabil. 1993, 20, 79–87. [Google Scholar] [CrossRef] [PubMed]
- Biglar, N.; Chaychi Raghimi, E.; Sadighian, S.; Karamitanha, F.; Zajkani, E.; Nourian, A. Effect of incorporating silica-hydroxyapatite-silver hybrid nanoparticles into the resin-modified glass ionomer on the adhesive remnant index score and shear bond strength of orthodontic metal brackets: An in vitro study. Int. Orthod. 2023, 21, 100761. [Google Scholar] [CrossRef] [PubMed]
- Olczak-Kowalczyk, D.; Mielczarek, A.; Jackowska, T.; Mielnik-Błaszczak, M.; Turska-Szybka, A.; Opydo-Szymaczek, J.; Jurczak, A.; Kaczmarek, U. Fluoride agents in the prevention and treatment of dental caries and erosion in children, adolescents and adults—Recommendations of Polish Experts. Update of recommendations: Individual fluoride prevention in children and adolescents—Recommendations of Polish Experts. Nowa Stomatol. 2022, 27. [Google Scholar] [CrossRef]
- Kosior, P.; Dobrzyński, M.; Korczyński, M.; Herman, K.; Czajczyńska-Waszkiewicz, A.; Kowalczyk-Zając, M.; Piesiak-Pańczyszyn, D.; Fita, K.; Janeczek, M. Long-term release of fluoride from fissure sealants—In vitro study. J. Trace Elem. Med. Biol. 2017, 41, 107–110. [Google Scholar] [CrossRef]
- Iranparvar, P.; Ghasemi, A.; Iranparvar, P. Adhesion of glass ionomer cements to primary dentin using a universal adhesive. Dent. Med. Probl. 2024, 61, 93–98. [Google Scholar] [CrossRef]
- Garcez, R.M.V.D.B.; Buzalaf, M.A.R.; De Araújo, P.A. Fluoride release of six restorative materials in water and pH-cycling solutions. J. Appl. Oral Sci. 2007, 15, 406. [Google Scholar] [CrossRef]
- Bahadure, R.N.; Pandey, R.K.; Kumar, R.; Gopal, K.; Singh, R.K. An estimation of fluoride release from various dental restorative materials at different pH: In vitro study. J. Indian Soc. Pedod. Prev. Dent. 2012, 30, 122–126. [Google Scholar] [CrossRef]
- Nigam, A.G.; Jaiswal, J.; Murthy, R.; Pandey, R. Estimation of Fluoride Release from Various Dental Materials in Different Media—An In Vitro Study. Int. J. Clin. Pediatr. Dent. 2009, 2, 1. [Google Scholar] [CrossRef]
- Kumari, P.D.; Khijmatgar, S.; Chowdhury, A.; Lynch, E.; Chowdhury, C.R. Factors influencing fluoride release in atraumatic restorative treatment (ART) materials: A review. J. Oral Biol. Craniofac. Res. 2019, 9, 315. [Google Scholar] [CrossRef] [PubMed]
- Jingarwar, M.M.; Pathak, A.; Bajwa, N.K.; Sidhu, H.S. Quantitative Assessment of Fluoride Release and Recharge Ability of Different Restorative Materials in Different Media: An In Vitro Study. J. Clin. Diagn. Res. 2014, 8, ZC31. [Google Scholar] [CrossRef]
- Elfakhri, F.; Alkahtani, R.; Li, C.; Khaliq, J. Influence of filler characteristics on the performance of dental composites: A comprehensive review. Ceram. Int. 2022, 48, 27280–27294. [Google Scholar] [CrossRef]
- Oleniacz-Trawińska, M.; Kotela, A.; Kensy, J.; Kiryk, S.; Dobrzyński, W.; Kiryk, J.; Gerber, H.; Fast, M.; Matys, J.; Dobrzyński, M. Evaluation of Factors Affecting Fluoride Release from Compomer Restorative Materials: A Systematic Review. Materials 2025, 18, 1627. [Google Scholar] [CrossRef] [PubMed]
- Morawska-Wilk, A.; Kensy, J.; Kiryk, S.; Kotela, A.; Kiryk, J.; Michalak, M.; Grychowska, N.; Fast, M.; Matys, J.; Dobrzyński, M. Evaluation of Factors Influencing Fluoride Release from Dental Nanocomposite Materials: A Systematic Review. Nanomaterials 2025, 15, 651. [Google Scholar] [CrossRef] [PubMed]
- Okamoto, M.; Yamashita, S.; Mendonca, M.; Brueckner, S.; Achong-Bowe, R.; Thompson, J.; Kuriki, N.; Mizuhira, M.; Benjamin, Y.; Duncan, H.F.; et al. Ultrastructural evaluation of adverse effects on dentine formation from systemic fluoride application in an experimental mouse model. Int. Endod. J. 2025, 58, 128–140. [Google Scholar] [CrossRef]
- Forsten, L. Fluoride release and uptake by glass-ionomers and related materials and its clinical effect. Biomaterials 1998, 19, 503–508. [Google Scholar] [CrossRef]
- Huang, X.; Lin, J.; Demner-Fushman, D. Evaluation of PICO as a knowledge representation for clinical questions. AMIA Annu. Symp. Proc. 2006, 2006, 359–363. [Google Scholar]
- Page, M.J.; McKenzie, J.E.; Bossuyt, P.M.; Boutron, I.; Hoffmann, T.C.; Mulrow, C.D.; Shamseer, L.; Tetzlaff, J.M.; Akl, E.A.; Brennan, S.E.; et al. The PRISMA 2020 statement: An updated guideline for reporting systematic reviews. BMJ 2021, 372, 71. [Google Scholar] [CrossRef]
- Watson, P.F.; Petrie, A. Method agreement analysis: A review of correct methodology. Theriogenology 2010, 73, 1167–1179. [Google Scholar] [CrossRef] [PubMed]
- Kanjevac, T.; Milovanovic, M.; Volarevic, V.; Lukic, M.L.; Arsenijevic, N.; Markovic, D.; Zdravkovic, N.; Tesic, Z.; Lukic, A. Cytotoxic Effects of Glass Ionomer Cements on Human Dental Pulp Stem Cells Correlate with Fluoride Release. Med. Chem. 2012, 8, 40–45. [Google Scholar] [CrossRef]
- Guida, A.; Towler, M.R.; Wall, J.G.; Hill, R.G.; Eramo, S. Preliminary work on the antibacterial effect of strontium in glass ionomer cements. J. Mater. Sci. Lett. 2003, 22, 1401–1403. [Google Scholar] [CrossRef]
- Pardi, M.; Ribeiro, K.L.G.; Marques, M.B.E.S.; Costa, C.R.; de Brito Silva, E.B.; Schiavon, M.A.; dos Reis, A.C.; Lepri, C.P.; de Castro, D.T. Incorporation of AgVO3 into Glass Ionomer Cement: Ionic Release. Pesqui. Bras. Odontopediatria Clin. Integr. 2025, 25, e240015. [Google Scholar] [CrossRef]
- Guo, T.; Wang, D.; Gao, S.S. The antibiofilm effect and mechanism of silver nanowire-modified glass ionomer cement against multi-species oral biofilm. BMC Oral Health 2025, 25, 160. [Google Scholar] [CrossRef]
- Raghimi, E.C.; Biglar, N.; Sadighian, S.; Karamitanha, F.; Nouri, A.; Nourian, A. Compressive strength and fluoride release profile of a glass ionomer cement reinforced with silver-hydroxyapatite-silica hybrid nanoparticles: An in vitro study. Int. Orthod. 2024, 22, 100871. [Google Scholar] [CrossRef]
- Saad Bin Qasim, S.; Bmuajdad, A. The effect of mesoporous silica doped with silver nanoparticles on glass ionomer cements; physiochemical, mechanical and ion release analysis. BMC Oral Health 2024, 24, 1269. [Google Scholar] [CrossRef]
- Potiprapanpong, W.; Naruphontjirakul, P.; Khamsuk, C.; Channasanon, S.; Toneluck, A.; Tanodekaew, S.; Monmaturapoj, N.; Young, A.M.; Panpisut, P. Assessment of Mechanical/Chemical Properties and Cytotoxicity of Resin-Modified Glass Ionomer Cements Containing Sr/F-Bioactive Glass Nanoparticles and Methacrylate Functionalized Polyacids. Int. J. Mol. Sci. 2023, 24, 10231. [Google Scholar] [CrossRef]
- AlMatar, D.; AlSanousi, S.; Ahmed, J.; Saad Bin Qasim, S. The In-Vitro Effect of Silver and Zinc Oxide Nanoparticles on Fluoride Release and Microhardness of a Resin-Modified Glass Ionomer Cement. J. Inorg. Organomet. Polym. Mater. 2023, 33, 1507–1516. [Google Scholar] [CrossRef]
- Thongsri, O.; Srisuwan, S.; Thaitalay, P.; Dangwiriyakul, R.; Chanlek, N.; Talabnin, C.; Rattanachan, S.T. Fluoride release and uptake characteristics of the sol-gel derived glass ionomer cement modified with fluoride containing strontium-based bioactive glass nanoparticles. J. Solgel Sci. Technol. 2023, 105, 857–870. [Google Scholar] [CrossRef]
- Gunay, A.; Celenk, S.; Adiguzel, O.; Cangul, S.; Ozcan, N.; Cakmakoglu, E.E. Comparison of Antibacterial Activity, Cytotoxicity, and Fluoride Release of Glass Ionomer Restorative Dental Cements in Dentistry. Med. Sci. Monit. 2022, 28, e939065. [Google Scholar] [CrossRef] [PubMed]
- Wassel, M.O.; Allam, G.G. Anti-Bacterial Effect, Fluoride Release, and Compressive Strength of a Glass Ionomer Containing Silver and Titanium Nanoparticles. Indian J. Dent. Res. 2022, 33, 75–79. [Google Scholar] [CrossRef]
- Alshehri, T.D.; Kotha, S.B.; Abed, F.M.; Barry, M.J.; Alasmari, A.; Mallineni, S.K. Effect of the Addition of Varying Concentrations of Silver Nanoparticles on the Fluoride Uptake and Recharge of Glass Ionomer Cement. Nanomaterials 2022, 12, 1971. [Google Scholar] [CrossRef]
- Kohno, T.; Liu, Y.; Tsuboi, R.; Kitagawa, H.; Imazato, S. Evaluation of ion release and the recharge ability of glass-ionomer cement containing BioUnion filler using an in vitro saliva-drop setting assembly. Dent. Mater. 2021, 37, 882–893. [Google Scholar] [CrossRef]
- Malekhoseini, Z.; Rezvani, M.B.; Niakan, M.; Atai, M.; Mohammadi Bassir, M.; Alizade, H.S.; Siabani, S. Effect of zinc oxide nanoparticles on physical and antimicrobial properties of resin-modified glass ionomer cement. Dent. Res. J. 2021, 18, 73. [Google Scholar] [CrossRef] [PubMed]
- Bahammam, S.; Nathanson, D.; Fan Medina, Y. Assessing the release of the fluoride ion in four restorative glass ionomer cements. Fluoride 2020, 53, 611–620. [Google Scholar]
- Putri, L.K.; Rianti, D.; Harijanto, E. Release of fluoride to the addition of nanoparticle zinc oxide with glass ionomer cements. Int. J. Pharm. Res. 2020, 12, 1530–1533. [Google Scholar] [CrossRef]
- Karimi, M.; Hesaraki, S.; Alizadeh, M.; Kazemzadeh, A. Effect of synthetic amorphous calcium phosphate nanoparticles on the physicochemical and biological properties of resin-modified glass ionomer cements. Mater. Sci. Eng. C 2019, 98, 227–240. [Google Scholar] [CrossRef]
- Cibim, D.D.; Saito, M.T.; Giovani, P.A.; Borges, A.F.S.; Pecorari, V.G.A.; Gomes, O.P.; Lisboa-Filho, P.N.; Nociti-Junior, F.H.; Puppin-Rontani, R.M.; Kantovitz, K.R. Novel nanotechnology of TiO2 improves physical-chemical and biological properties of glass ionomer cement. Int. J. Biomater. 2017, 2017, 7123919. [Google Scholar] [CrossRef]
- Saxena, S.; Tiwari, S. Energy dispersive X-ray microanalysis, fluoride release, and antimicrobial properties of glass ionomer cements indicated for atraumatic restorative treatment. J. Int. Soc. Prev. Community Dent. 2016, 6, 366–372. [Google Scholar] [CrossRef]
- Shahid, S.; Hassan, U.; Billington, R.W.; Hill, R.G.; Anderson, P. Glass ionomer cements: Effect of strontium substitution on esthetics, radiopacity and fluoride release. Dent. Mater. 2014, 30, 308–313. [Google Scholar] [CrossRef] [PubMed]
- Selimović-Dragaš, M.; Hasić-Branković, L.; Korać, F.; Đapo, N.; Huseinbegović, A.; Kobašlija, S.; Lekić, M.; Hatibović-Kofman, Š. In vitro fluoride release from a different kind of conventional and resin modified glass-ionomer cements. Bosn. J. Basic Med. Sci. 2013, 13, 197. [Google Scholar] [CrossRef] [PubMed]
- Xu, X.; Burgess, J.O. Compressive strength, fluoride release and recharge of fluoride-releasing materials. Biomaterials 2003, 24, 2451–2461. [Google Scholar] [CrossRef]
- Osinaga, P.W.; Helena Grande, R.M.; Ballester, R.Y.; Regina Simionato, M.L.; Âlia Regina Delgado Rodrigues, C.M.; Muench, A. Zinc sulfate addition to glass-ionomer-based cements: Influence on physical and antibacterial properties, zinc and fluoride release. Dent. Mater. 2003, 19, 212–217. [Google Scholar] [CrossRef] [PubMed]
- Helvatjoglu-Antoniades, M.; Karantakis, P.; Papadogiannis, Y.; Kapetanios, H. Fluoride release from restorative materials and a luting cement. J. Prosthet. Dent. 2001, 86, 156–164. [Google Scholar] [CrossRef]
- Hattab, F.N.; Amin, W.M. Fluoride release from glass ionomer restorative materials and the effects of surface coating. Biomaterials 2001, 22, 1449–1458. [Google Scholar] [CrossRef]
- Yip, H.K.; Lam, W.T.C.; Smales, R.J. Fluoride release, weight loss and erosive wear of modern aesthetic restoratives. Br. Dent. J. 1999, 187, 265–270. [Google Scholar] [CrossRef]
- Wandera, A.; Spencer, P.; Bohaty, B. In vitro comparative fluoride release, and weight and volume change in light-curing and self-curing glass ionomer materials. Pediatr. Dent. 1996, 18, 210–214. [Google Scholar]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).