- Article
Safety of Perineural Lidocaine in Cervical Nerve Root Injections: A Retrospective Case–Control Study
- Kevin E. Salinas,
- Samir Ghandour and
- Zachary E. Stewart
- + 2 authors
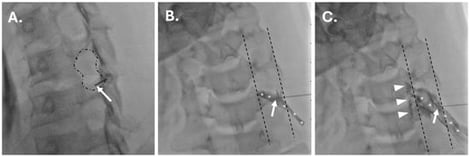
Background/Objectives: Fluoroscopically guided cervical nerve root corticosteroid injections are used for the treatment and diagnosis of radicular pain. Including a local anesthetic with the injected corticosteroid may decrease the pain associated with the procedure and add immediate diagnostic value. However, little is known about the safety of including a local anesthetic with a corticosteroid in these injections. Methods: A total of 299 consecutive cervical nerve root injections, performed between 2016 and 2024, were reviewed. Demographic and injection information (level/laterality and inclusion/exclusion of 1% preservative-free lidocaine with dexamethasone injectate) were documented. Charts were reviewed for major complications and increased pain post-procedure. Categorical data were compared between groups using Fisher’s exact test or Chi-square testing. Results: Injections were performed with 10 mg of dexamethasone only in 263 cases and with a mixture of 10 mg of dexamethasone and 1 mL of 1% lidocaine in 36 cases. There was no statistically significant difference in the incidence of major complications (p ≈ 1) or immediately increased pain post-procedure (p = 0.799). Conclusions: With proper technique, there is no evidence from this case–control study or in the available literature to suggest that including lidocaine with corticosteroid increases risks associated with cervical nerve root injections. However, serious adverse events are theoretically possible with injection of local anesthetic into a radicular artery, the vertebral artery, or subdural space. Given that such risks are not associated with the use of non-particulate steroids alone, large multi-institutional studies are needed to draw confident conclusions on the risks and benefits of the inclusion of local anesthetics with non-particulate corticosteroids for cervical transforaminal epidural steroid injection to inform clinical practice.
6 February 2026