Training for Pediatric Sepsis—A Medical Education Perspective and Potential Role of Artificial Intelligence
Abstract
1. Introduction
2. Methods
- Lectures;
- Seminars;
- E-learning;
- Hybrid learning;
- Technology-enhanced learning (gamification, virtual reality (VR) and augmented reality (AR) simulation;
- Artificial intelligence;
- Barriers to implementation of artificial intelligence in sepsis education.Pediatric sepsis definitions vary across different studies:
3. Results
3.1. Lectures and Seminars
3.2. Lectures
3.3. Seminars
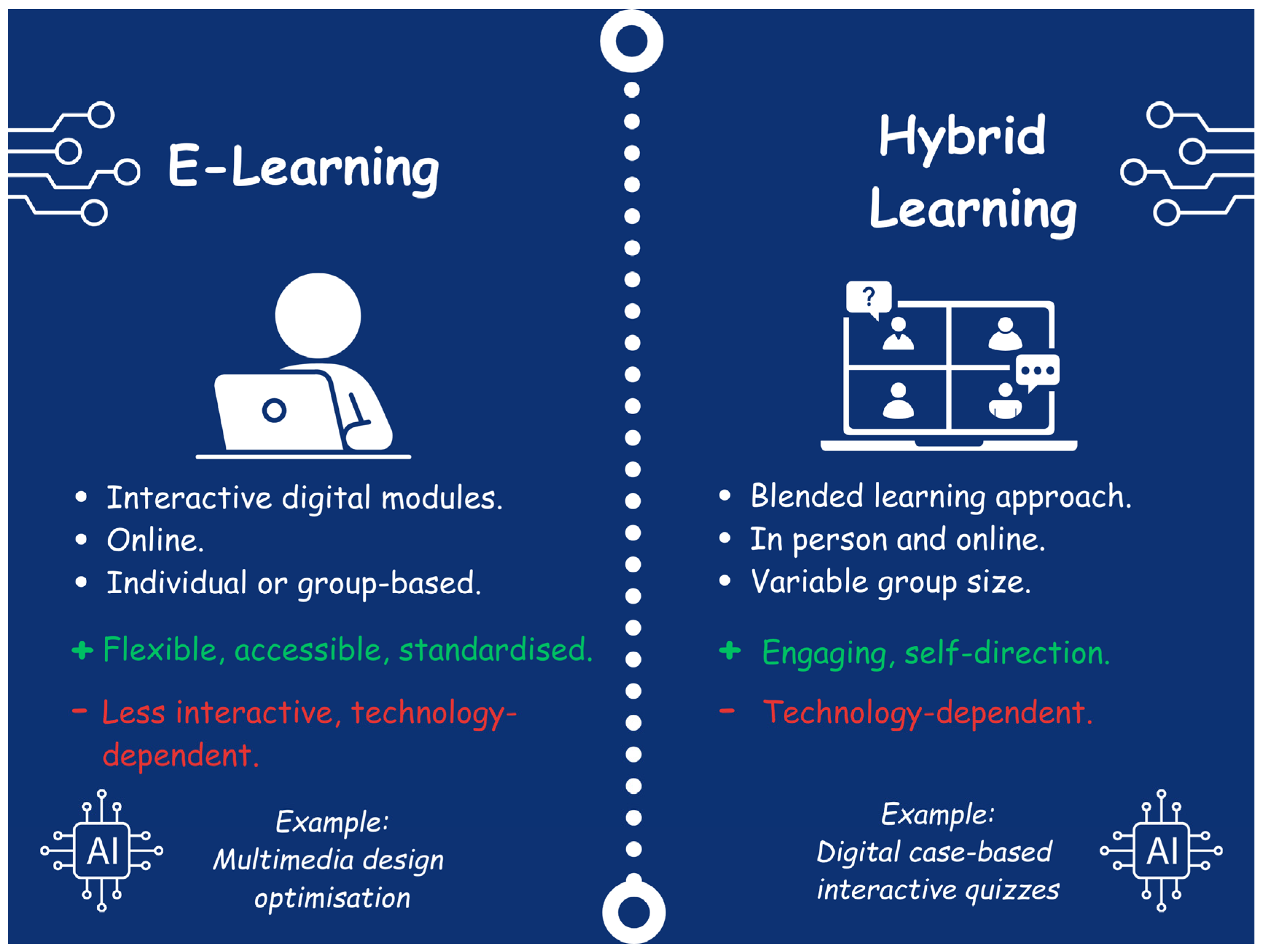
3.4. E-Learning and Hybrid Learning
3.5. E-Learning
3.6. Hybrid Learning
3.7. Technology-Enhanced Learning and AI
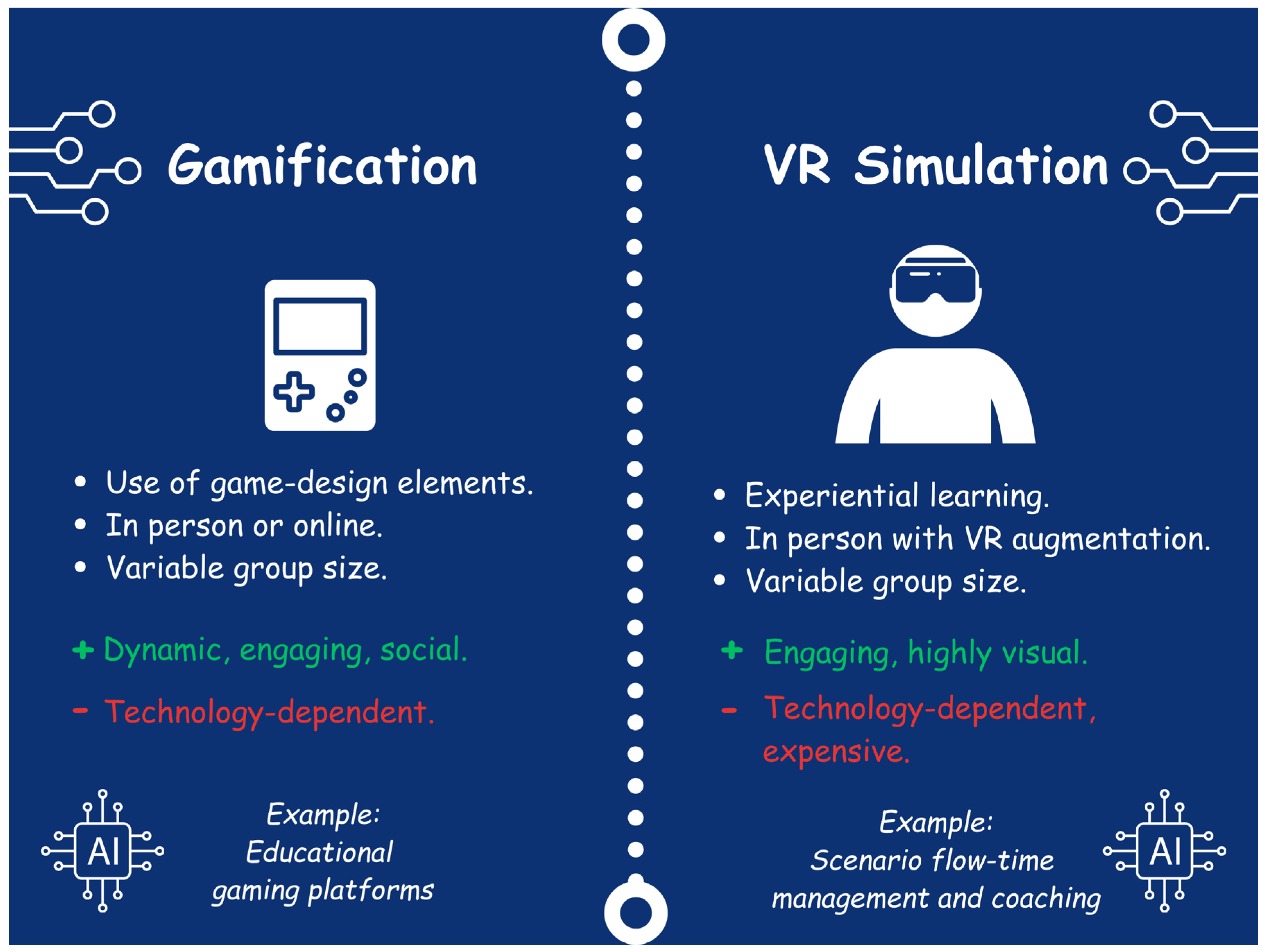
3.8. Gamification
3.9. Simulation
3.10. Virtual and Augmented Reality Simulation
3.11. Barriers to the Implementation of AI in Sepsis Education
3.12. Limitations
4. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| ED | Emergency Department |
| AI | Artificial Intelligence |
| IV | Intravenous |
| CI | Confidence Interval |
| PALS | Pediatric Advanced Life Support |
| QI | Quality Improvement |
| OR | Odds Ratio |
| LMIC | Low- and Middle-Income Countries |
| PEAK | Pediatric Education and Advocacy Kit |
| EMSC | Emergency Medical Services for Children |
| SIRS | Systemic Inflammatory Response Syndrome |
| SOAR | Strengths, Opportunities, Aspirations, Results |
| VR/AR | Virtual Reality/Augmented Reality |
References
- Miranda, M.; Nadel, S. Pediatric Sepsis: A Summary of Current Definitions and Management Recommendations. Curr. Pediatr. Rep. 2023, 11, 29–39. [Google Scholar] [CrossRef] [PubMed]
- Hibberd, O.; Karageorgos, S.; Ranaweera, M.; Mullally, P.J.W.; Athanasiou, D.; Roland, D. Recognising and Managing Sepsis in Children’s Emergency Care: A Clinical Practice Review. Pediatr. Med. 2025, 8, 11. [Google Scholar] [CrossRef]
- Paul, R.; Melendez, E.; Wathen, B.; Larsen, G.; Chapman, L.; Wheeler, D.S.; Wakefield, T.; Macias, C.G. A Quality Improvement Collaborative for Pediatric Sepsis: Lessons Learned. Pediatr. Qual. Saf. 2018, 3, e051. [Google Scholar] [CrossRef] [PubMed]
- Depinet, H.; Macias, C.G.; Balamuth, F.; Lane, R.D.; Luria, J.; Melendez, E.; Myers, S.R.; Patel, B.; Richardson, T.; Zaniletti, I.; et al. Pediatric Septic Shock Collaborative Improves Emergency Department Sepsis Care in Children. Pediatrics 2022, 149, e2020007369. [Google Scholar] [CrossRef]
- Woods, J.M.; Scott, H.F.; Zaveri, P.P. Creating Consensus Educational Goals for Pediatric Sepsis via Multicenter Modified Delphi. AEM Educ. Train. 2018, 2, 254–258. [Google Scholar] [CrossRef]
- Ahmed, S.K.; Mohammed, R.A.; Nashwan, A.J.; Ibrahim, R.H.; Abdalla, A.Q.; Ameen, B.M.M.; Khdhir, R.M. Using Thematic Analysis in Qualitative Research. J. Med. Surg. Public Health 2025, 6, 100198. [Google Scholar] [CrossRef]
- Choy, C.L.; Liaw, S.Y.; Goh, E.L.; See, K.C.; Chua, W.L. Impact of Sepsis Education for Healthcare Professionals and Students on Learning and Patient Outcomes: A Systematic Review. J. Hosp. Infect. 2022, 122, 84–95. [Google Scholar] [CrossRef]
- Zeng, H.L.; Chen, D.X.; Li, Q.; Wang, X.Y. Effects of Seminar Teaching Method versus Lecture-Based Learning in Medical Education: A Meta-Analysis of Randomized Controlled Trials. Med. Teach. 2020, 42, 1343–1349. [Google Scholar] [CrossRef]
- Huggett, K.N.; Smith, G.A.; Hsieh, P.H.; Ownby, A.R. Experience of Medical School Faculty in the Transition from Lectures to Active Learning: A Phenomenographic Study. Acad. Med. J. Assoc. Am. Med. Coll. 2025, 100, 621–627. [Google Scholar] [CrossRef]
- Prabu Kumar, A.; Omprakash, A.; Chokkalingam Mani, P.K.; Kuppusamy, M.; Wael, D.; Sathiyasekaran, B.W.C.; Vijayaraghavan, P.V.; Ramasamy, P. E-Learning and E-Modules in Medical Education-A SOAR Analysis Using Perception of Undergraduate Students. PLoS ONE 2023, 18, e0284882. [Google Scholar] [CrossRef] [PubMed]
- Abid, T.; Zahid, G.; Shahid, N.; Bukhari, M. Online Teaching Experience during the COVID-19 in Pakistan: Pedagogy–Technology Balance and Student Engagement. Fudan J. Humanit. Soc. Sci. 2021, 14, 367–391. [Google Scholar] [CrossRef]
- Abbas, U.; Parveen, M.; Sahito, F.S.; Hussain, N.; Munir, S. E-Learning in Medical Education: A Perspective of Pre-Clinical Medical Students from a Lower-Middle Income Country. BMC Med. Educ. 2024, 24, 162. [Google Scholar] [CrossRef]
- Pew, S. Andragogy and Pedagogy as Foundational Theory for Student Motivation in Higher Education. InSight J. Sch. Teach. 2007, 2, 14–25. [Google Scholar] [CrossRef]
- Tang, B.; Coret, A.; Qureshi, A.; Barron, H.; Ayala, A.P.; Law, M. Online Lectures in Undergraduate Medical Education: Scoping Review. JMIR Med. Educ. 2018, 4, e11. [Google Scholar] [CrossRef]
- Datta, R.; Di Tanna, G.L.; Youssef, M.; Harley, A.; Schlapbach, L.J.; Nunnink, L.; Venkatesh, B. An Assessment of Knowledge and Education about Sepsis among Medical Students: A Multi-University Survey. Crit. Care Resusc. J. Australas. Acad. Crit. Care Med. 2021, 23, 117–118. [Google Scholar] [CrossRef]
- Delungahawatta, T.; Dunne, S.S.; Hyde, S.; Halpenny, L.; McGrath, D.; O’Regan, A.; Dunne, C.P. Advances in E-Learning in Undergraduate Clinical Medicine: A Systematic Review. BMC Med. Educ. 2022, 22, 711. [Google Scholar] [CrossRef] [PubMed]
- Lewis, K.O.; Cidon, M.J.; Seto, T.L.; Chen, H.; Mahan, J.D. Leveraging E-Learning in Medical Education. Curr. Probl. Pediatr. Adolesc. Health Care 2014, 44, 150–163. [Google Scholar] [CrossRef] [PubMed]
- Goldie, J.G.S. Connectivism: A Knowledge Learning Theory for the Digital Age? Med. Teach. 2016, 38, 1064–1069. [Google Scholar] [CrossRef] [PubMed]
- Shabila, N.P.; Alkhateeb, N.E.; Dauod, A.S.; Al-Dabbagh, A. Exploring the Perspectives of Medical Students on Application of E-Learning in Medical Education during the COVID-19 Pandemic. Work Read. Mass 2021, 70, 751–762. [Google Scholar] [CrossRef]
- Knowles, M.S. Andragogy: Adult Learning Theory in Perspective. Community Coll. Rev. 1978, 5, 9–20. [Google Scholar] [CrossRef]
- Kolb, D.A. Experiential Learning: Experience as the Source of Learning and Development, 2nd ed.; Pearson Education, Inc.: Upper Saddle River, NJ, USA, 2015; ISBN 978-0-13-389240-6. [Google Scholar]
- Schon, D.A.; DeSanctis, V. The Reflective Practitioner: How Professionals Think in Action. J. Contin. High. Educ. 1986, 34, 29–30. [Google Scholar] [CrossRef]
- Saurabh, M.K.; Patel, T.; Bhabhor, P.; Patel, P.; Kumar, S. Students’ Perception on Online Teaching and Learning during COVID-19 Pandemic in Medical Education. Maedica 2021, 16, 439–444. [Google Scholar] [CrossRef]
- Hameed, T.; Husain, M.; Jain, S.K.; Singh, C.B.; Khan, S. Online Medical Teaching in COVID-19 Era: Experience and Perception of Undergraduate Students. Maedica 2020, 15, 440–444. [Google Scholar] [CrossRef]
- Dost, S.; Hossain, A.; Shehab, M.; Abdelwahed, A.; Al-Nusair, L. Perceptions of Medical Students towards Online Teaching during the COVID-19 Pandemic: A National Cross-Sectional Survey of 2721 UK Medical Students. BMJ Open 2020, 10, e042378. [Google Scholar] [CrossRef] [PubMed]
- Mayer, R.E. Multimedia Learning. In Psychology of Learning and Motivation; Elsevier: Amsterdam, The Netherlands, 2002; Volume 41, pp. 85–139. ISBN 978-0-12-543341-9. [Google Scholar]
- Bernacchio, C.; Mullen, M. Universal Design for Learning. Psychiatr. Rehabil. J. 2007, 31, 167–169. [Google Scholar] [CrossRef] [PubMed]
- Vallée, A.; Blacher, J.; Cariou, A.; Sorbets, E. Blended Learning Compared to Traditional Learning in Medical Education: Systematic Review and Meta-Analysis. J. Med. Internet Res. 2020, 22, e16504. [Google Scholar] [CrossRef]
- Prober, C.G.; Heath, C. Lecture Halls without Lectures—A Proposal for Medical Education. N. Engl. J. Med. 2012, 366, 1657–1659. [Google Scholar] [CrossRef]
- Pediatric Education and Advocacy Kit (PEAK): Sepsis. Available online: https://emscimprovement.center/education-and-resources/peak/peak-sepsis/ (accessed on 20 August 2025).
- SIRS. Sepsis and Shock Module—Don’t Forget the Bubbles. Available online: https://dontforgetthebubbles.com/sirs-sepsis-and-shock-module/ (accessed on 20 August 2025).
- Van Gaalen, A.E.J.; Brouwer, J.; Schönrock-Adema, J.; Bouwkamp-Timmer, T.; Jaarsma, A.D.C.; Georgiadis, J.R. Gamification of Health Professions Education: A Systematic Review. Adv. Health Sci. Educ. 2021, 26, 683–711. [Google Scholar] [CrossRef] [PubMed]
- Evans, K.H.; Daines, W.; Tsui, J.; Strehlow, M.; Maggio, P.; Shieh, L. Septris: A Novel, Mobile, Online, Simulation Game That Improves Sepsis Recognition and Management. Acad. Med. 2015, 90, 180–184. [Google Scholar] [CrossRef]
- Dugan, M.C.; McCracken, C.E.; Hebbar, K.B. Does Simulation Improve Recognition and Management of Pediatric Septic Shock, and If One Simulation Is Good, Is More Simulation Better? Pediatr. Crit. Care Med. 2016, 17, 605–614. [Google Scholar] [CrossRef]
- Harder, N. Advancing Healthcare Simulation Through Artificial Intelligence and Machine Learning: Exploring Innovations. Clin. Simul. Nurs. 2023, 83, 101456. [Google Scholar] [CrossRef]
- Zhao, L.; Wu, C.; Su, J.; Bai, H.; Xia, Q.; Ma, W.; Wang, R. Integration of Mind Mapping and In-Situ Simulation Training to Enhance the Implementation of Sepsis Hour-1 Bundle Treatment. BMC Med. Educ. 2025, 25, 331. [Google Scholar] [CrossRef] [PubMed]
- Wu, Q.; Wang, Y.; Lu, L.; Chen, Y.; Long, H.; Wang, J. Virtual Simulation in Undergraduate Medical Education: A Scoping Review of Recent Practice. Front. Med. 2022, 9, 855403. [Google Scholar] [CrossRef]
- Toto, R.L.; Vorel, E.S.; Tay, K.-Y.E.; Good, G.L.; Berdinka, J.M.; Peled, A.; Leary, M.; Chang, T.P.; Weiss, A.K.; Balamuth, F.B. Augmented Reality in Pediatric Septic Shock Simulation: Randomized Controlled Feasibility Trial. JMIR Med. Educ. 2021, 7, e29899. [Google Scholar] [CrossRef]
- Liaw, S.Y.; Tan, J.Z.; Lim, S.; Zhou, W.; Yap, J.; Ratan, R.; Ooi, S.L.; Wong, S.J.; Seah, B.; Chua, W.L. Artificial Intelligence in Virtual Reality Simulation for Interprofessional Communication Training: Mixed Method Study. Nurse Educ. Today 2023, 122, 105718. [Google Scholar] [CrossRef]
- Rincón, E.H.H.; Jimenez, D.; Aguilar, L.A.C.; Flórez, J.M.P.; Tapia, Á.E.R.; Peñuela, C.L.J. Mapping the Use of Artificial Intelligence in Medical Education: A Scoping Review. BMC Med. Educ. 2025, 25, 526. [Google Scholar] [CrossRef]
- Hippe, D.S.; Umoren, R.A.; McGee, A.; Bucher, S.L.; Bresnahan, B.W. A Targeted Systematic Review of Cost Analyses for Implementation of Simulation-Based Education in Healthcare. SAGE Open Med. 2020, 8, 2050312120913451. [Google Scholar] [CrossRef] [PubMed]
- Ferreira, J.M.G.; Generoso, J.R.; Marra, A.R.; Deliberato, R.O.; Dewan, M.; Loeb, D.; Real, F.; Collins, K.; Ely, K.; Zackoff, M.; et al. Effectiveness of Low-Cost, Technology-Enhanced Simulation Training for Healthcare Training in Low—And Middle-Income Countries (LMICs): A Systematic Literature Review. J. Gen. Intern. Med. 2025; Online ahead of print. [Google Scholar] [CrossRef]
- Aslan, A.T.; Permana, B.; Harris, P.N.A.; Naidoo, K.D.; Pienaar, M.A.; Irwin, A.D. The Opportunities and Challenges for Artificial Intelligence to Improve Sepsis Outcomes in the Paediatric Intensive Care Unit. Curr. Infect. Dis. Rep. 2023, 25, 243–253. [Google Scholar] [CrossRef]
- Abdulnour, R.-E.E.; Gin, B.; Boscardin, C.K. Educational Strategies for Clinical Supervision of Artificial Intelligence Use. N. Engl. J. Med. 2025, 393, 786–797. [Google Scholar] [CrossRef] [PubMed]
- Weidener, L.; Fischer, M. Teaching AI Ethics in Medical Education: A Scoping Review of Current Literature and Practices. Perspect. Med. Educ. 2023, 12, 399–410. [Google Scholar] [CrossRef]
- Truhn, D.; Müller-Franzes, G.; Kather, J.N. The Ecological Footprint of Medical AI. Eur. Radiol. 2023, 34, 1176–1178. [Google Scholar] [CrossRef] [PubMed]

| 1. Recognize possible septic shock signs: tachycardia, abnormal capillary refill, abnormal mental status, systolic hypotension, widened pulse pressure, elevated lactate |
| 2. Initiate early IV access, with large diameter and short length preferred |
| 3. Initiate IV fluid resuscitation with the appropriate agent and volume |
| 4. Deliver IV fluids rapidly using rapid delivery system and specifically not with an IV pump |
| 5. Deliver appropriate antibiotics within 180 min of sepsis recognition |
| 6. Recognize appropriate responses to fluid therapy by normalization of or improvement in heart rate, blood pressure, capillary refill time, lactate, and/or urine output |
| 7. Continue fluid resuscitation and prepare for potential vasoactive agent requirement when septic shock persists despite appropriate initial rapid fluid resuscitation |
| 8. Recognize fluid overload during resuscitation and appropriately choose adjunctive therapy |
| 9. Initiate vasoactive infusion through any access available when hypotension is present despite appropriate rapid fluid resuscitation |
| 10. Obtain blood culture prior to giving antibiotics |
| 11. Recognize and correct hypoglycemia |
| 12. Appropriate pressor choice |
| 13. Consider corticosteroids in catecholamine-resistant shock. Treat and test appropriately |
| 14. Recognize and correct hypocalcemia |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Karageorgos, S.; Hibberd, O.; Ren, D.; Hornsby, Y.; Roland, D.; Koutroulis, I. Training for Pediatric Sepsis—A Medical Education Perspective and Potential Role of Artificial Intelligence. Children 2025, 12, 1542. https://doi.org/10.3390/children12111542
Karageorgos S, Hibberd O, Ren D, Hornsby Y, Roland D, Koutroulis I. Training for Pediatric Sepsis—A Medical Education Perspective and Potential Role of Artificial Intelligence. Children. 2025; 12(11):1542. https://doi.org/10.3390/children12111542
Chicago/Turabian StyleKarageorgos, Spyridon, Owen Hibberd, Dennis Ren, Yasmin Hornsby, Damian Roland, and Ioannis Koutroulis. 2025. "Training for Pediatric Sepsis—A Medical Education Perspective and Potential Role of Artificial Intelligence" Children 12, no. 11: 1542. https://doi.org/10.3390/children12111542
APA StyleKarageorgos, S., Hibberd, O., Ren, D., Hornsby, Y., Roland, D., & Koutroulis, I. (2025). Training for Pediatric Sepsis—A Medical Education Perspective and Potential Role of Artificial Intelligence. Children, 12(11), 1542. https://doi.org/10.3390/children12111542







