Dissecting Polygenic Etiology of Ischemic Stroke in the Era of Precision Medicine
Abstract
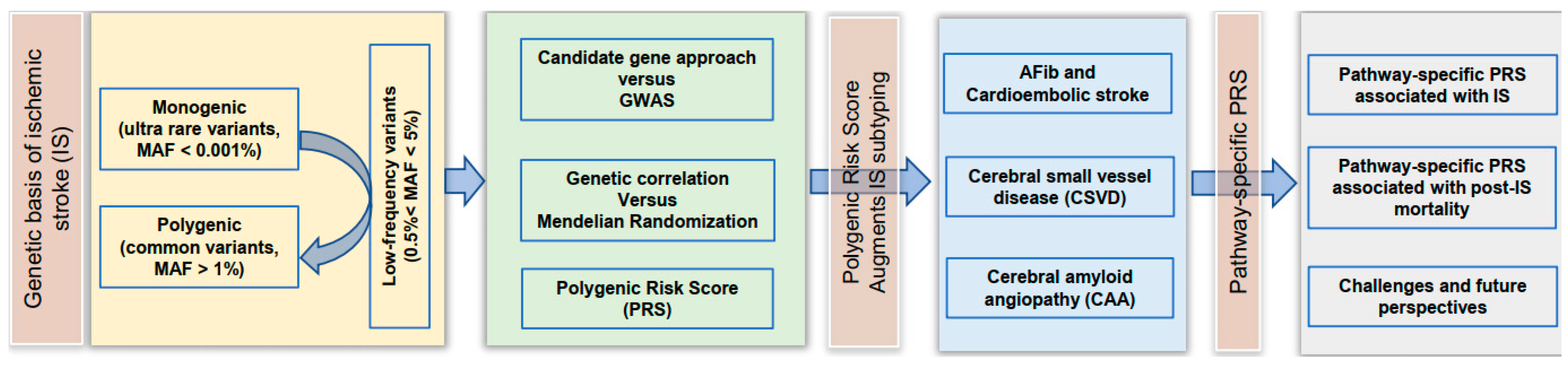
1. Polygenic Nature of Ischemic Stroke
1.1. Pioneer Studies on Monogenetic Disease
1.2. Genome-Wide Association Studies (GWAS)
1.3. Polygenic Risk Score (PRS) Construction
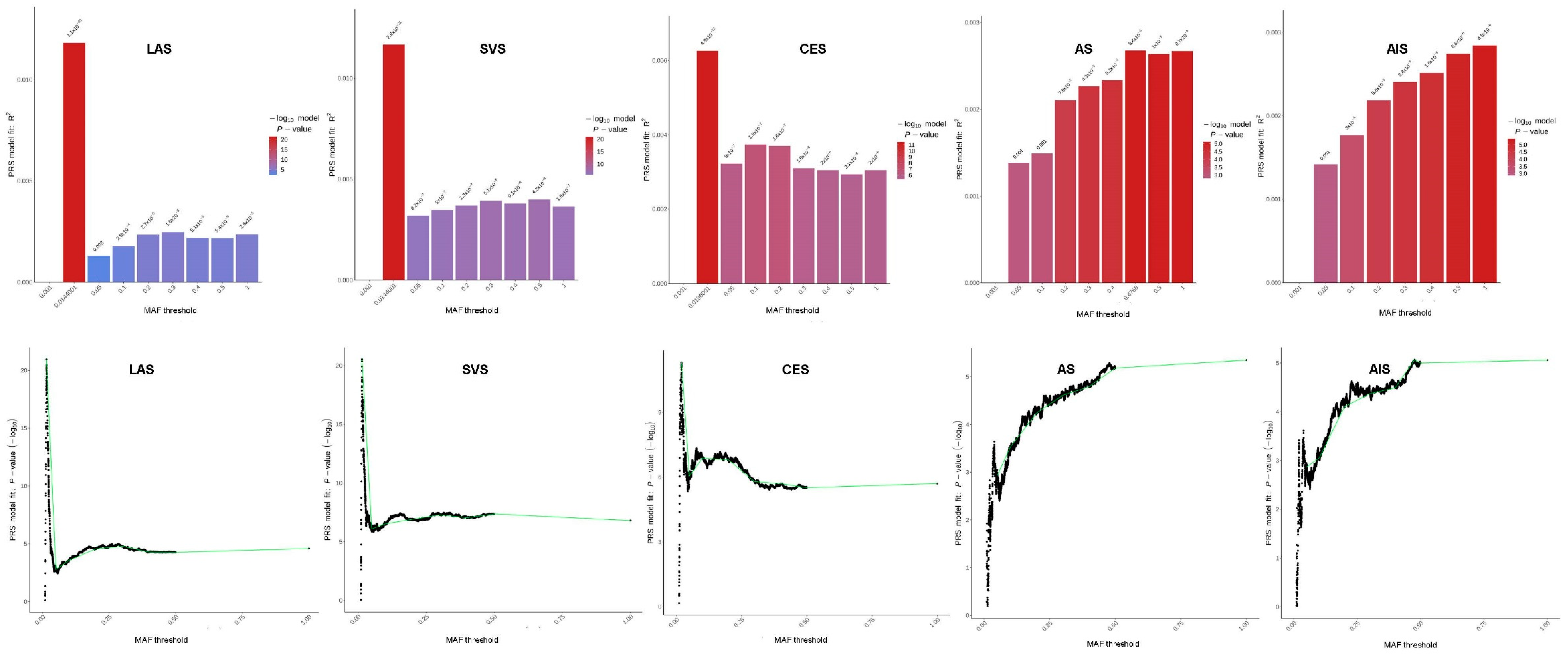
1.4. Low-Frequency Variants Explain More Phenotypic Variation
2. Polygenic Risk for Cardiovascular Disease May Also Contribute to the Risk for Sporadic IS
2.1. Candidate Gene Approach
2.2. Genetic Correlation between Cardiometabolic Risk Factors and IS
2.3. Mendelian Randomization for Causal Inference
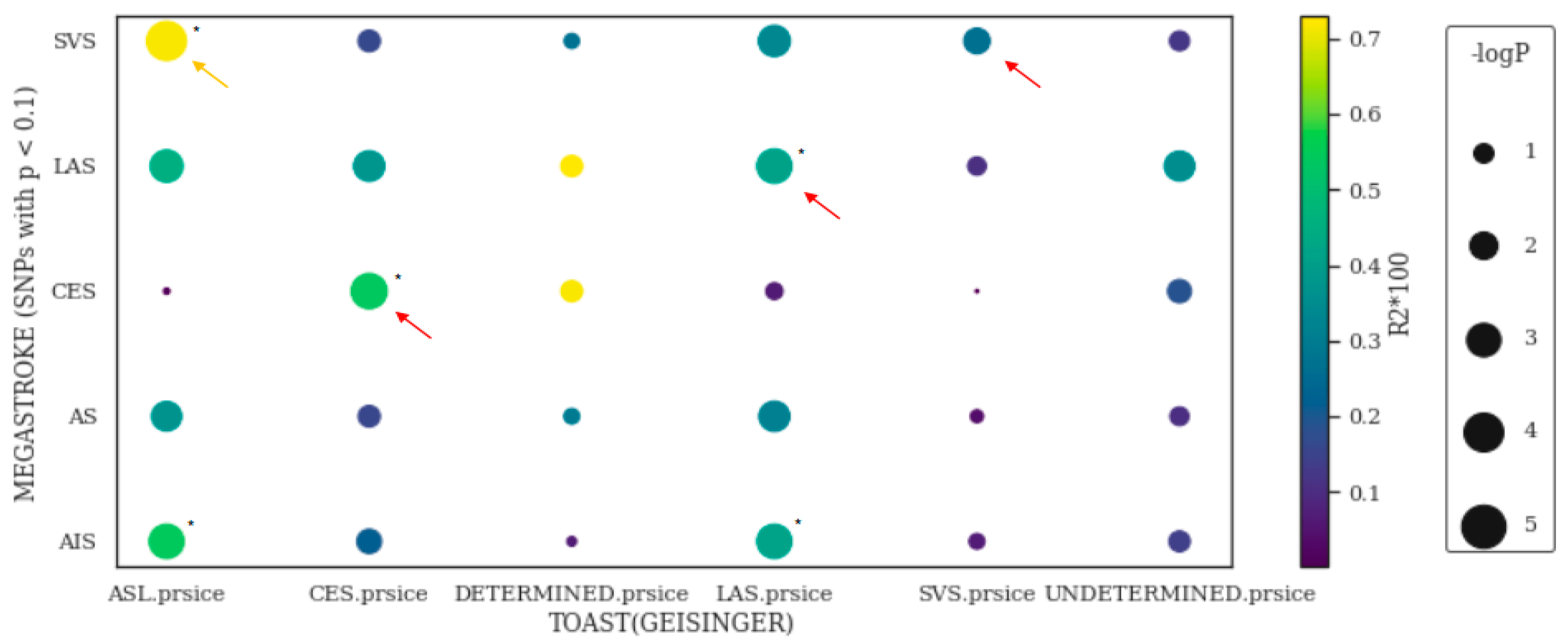
3. Polygenic Risk Scores (PRSs) Augment IS Subtyping
4. Genetic Basis of Cardioembolic Stroke
5. Genetic Basis of Sporadic Cerebral Small Vessel Disease (CSVD)
5.1. Heritability of CSVD
5.2. Genetic Variants from Extracellular Matrix (ECM) Genes May Contribute to the Risk for Sporadic CSVD
5.3. Genes Associated with Blood–Brain Barrier (BBB) Integrity May Contribute to the Risk for CSVD
5.4. Genetic Basis of Sporadic Cerebral Amyloid Angiopathy
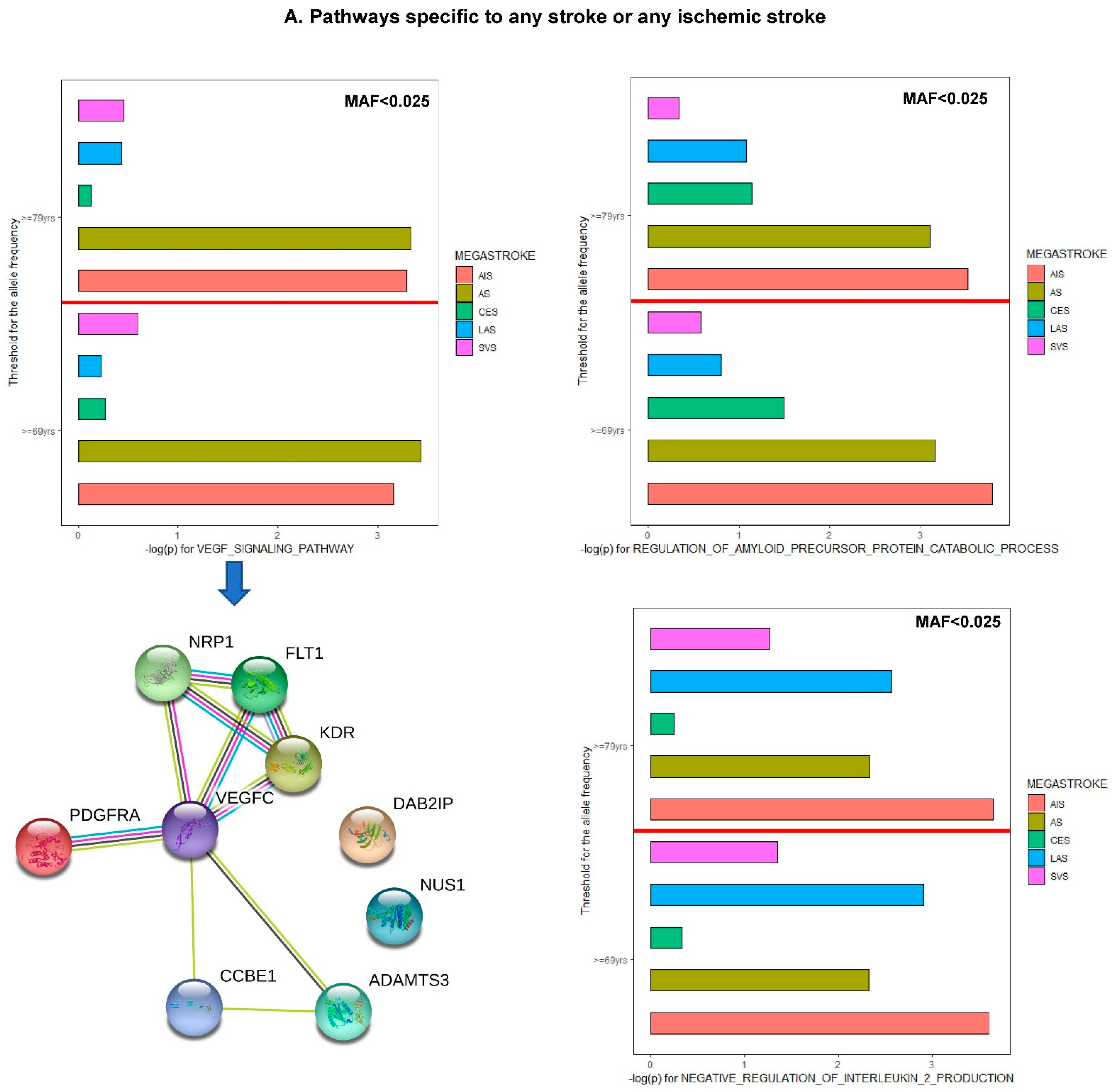
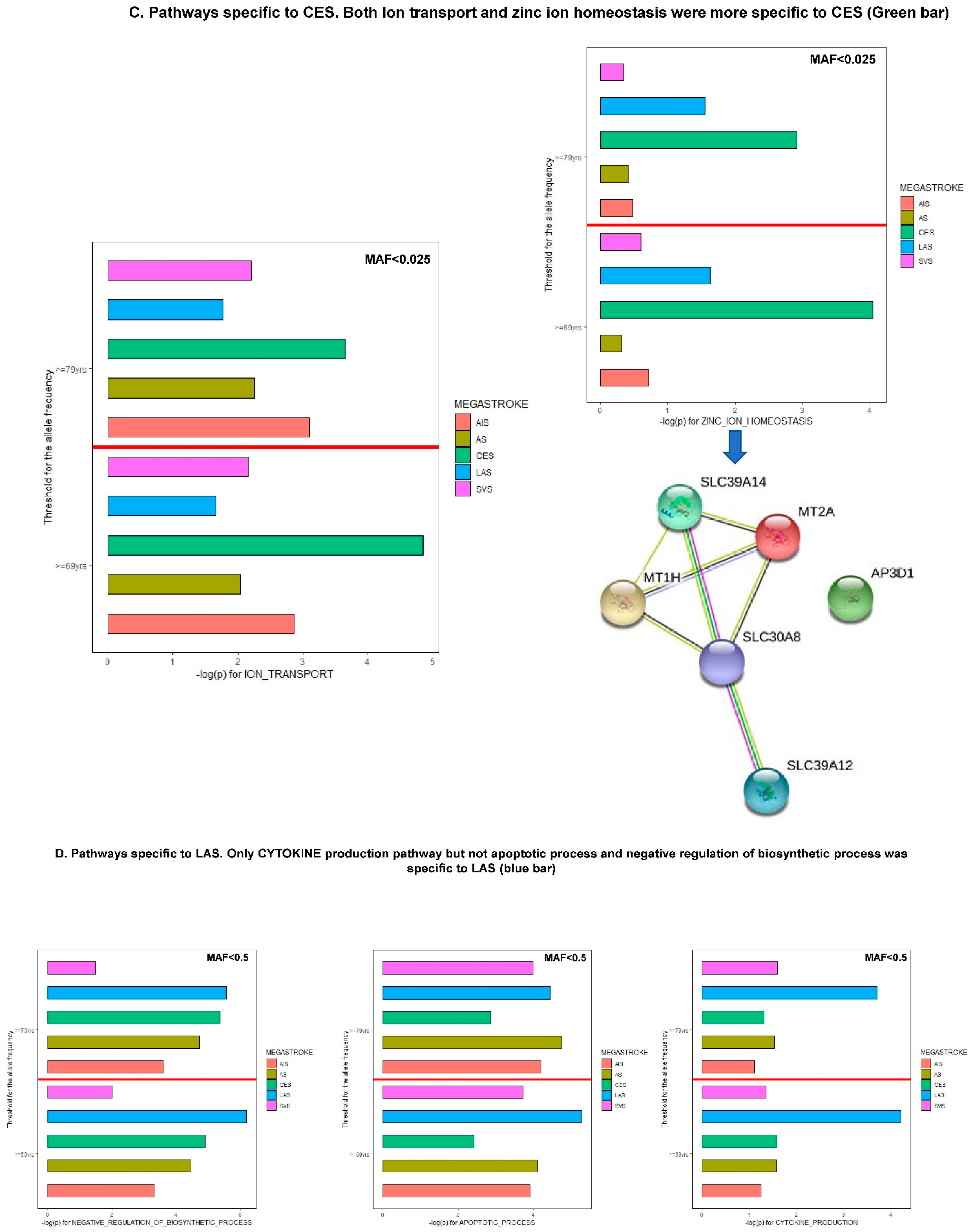
6. Pathway-Specific PRS Analysis for IS
6.1. Pathway-Specific PRS Construction
6.2. A Modified Paradigm of IS Risk Stratification beyond TOAST Subtyping
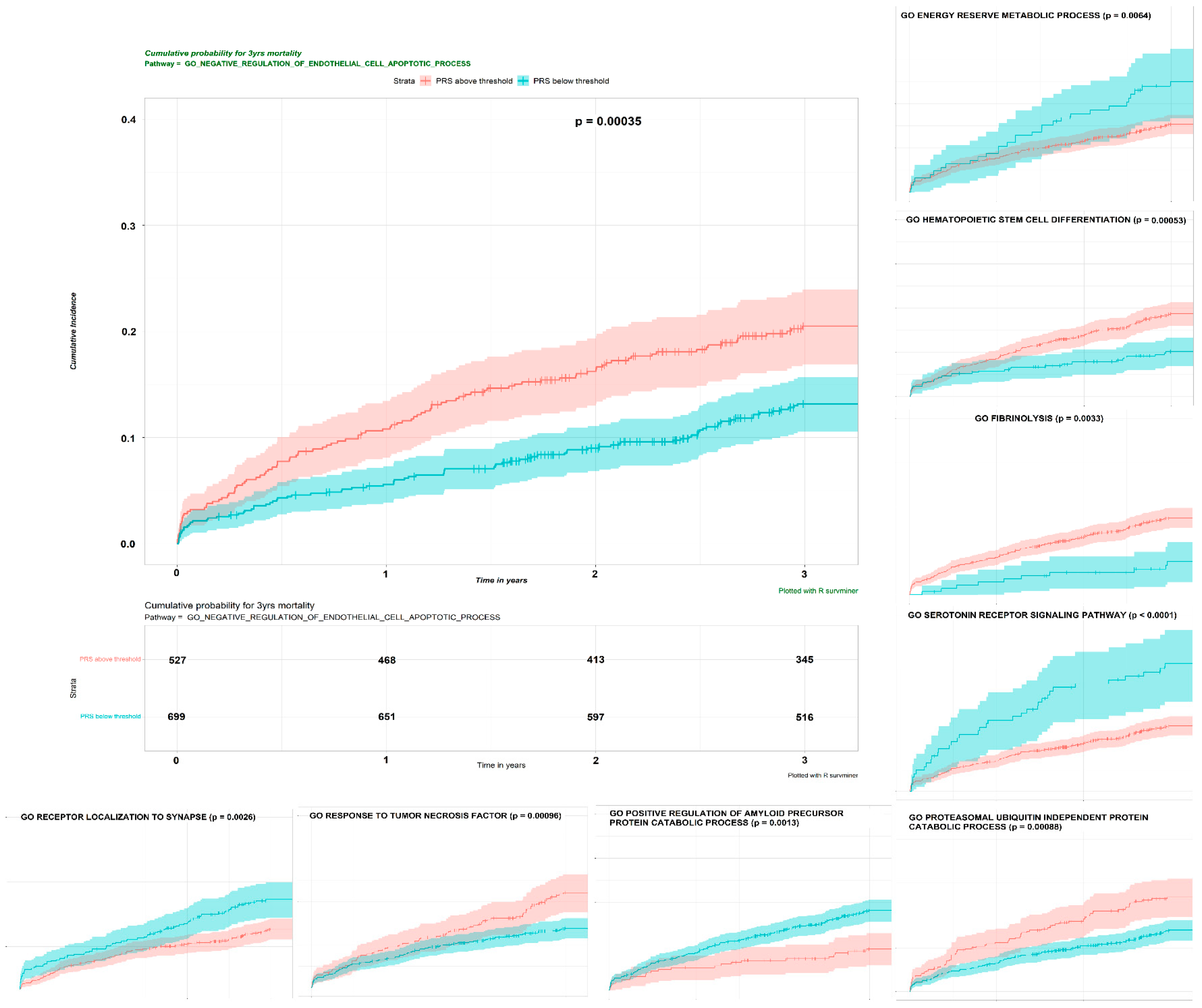
7. Pathway-Specific PRS Analysis of Post-IS Mortality
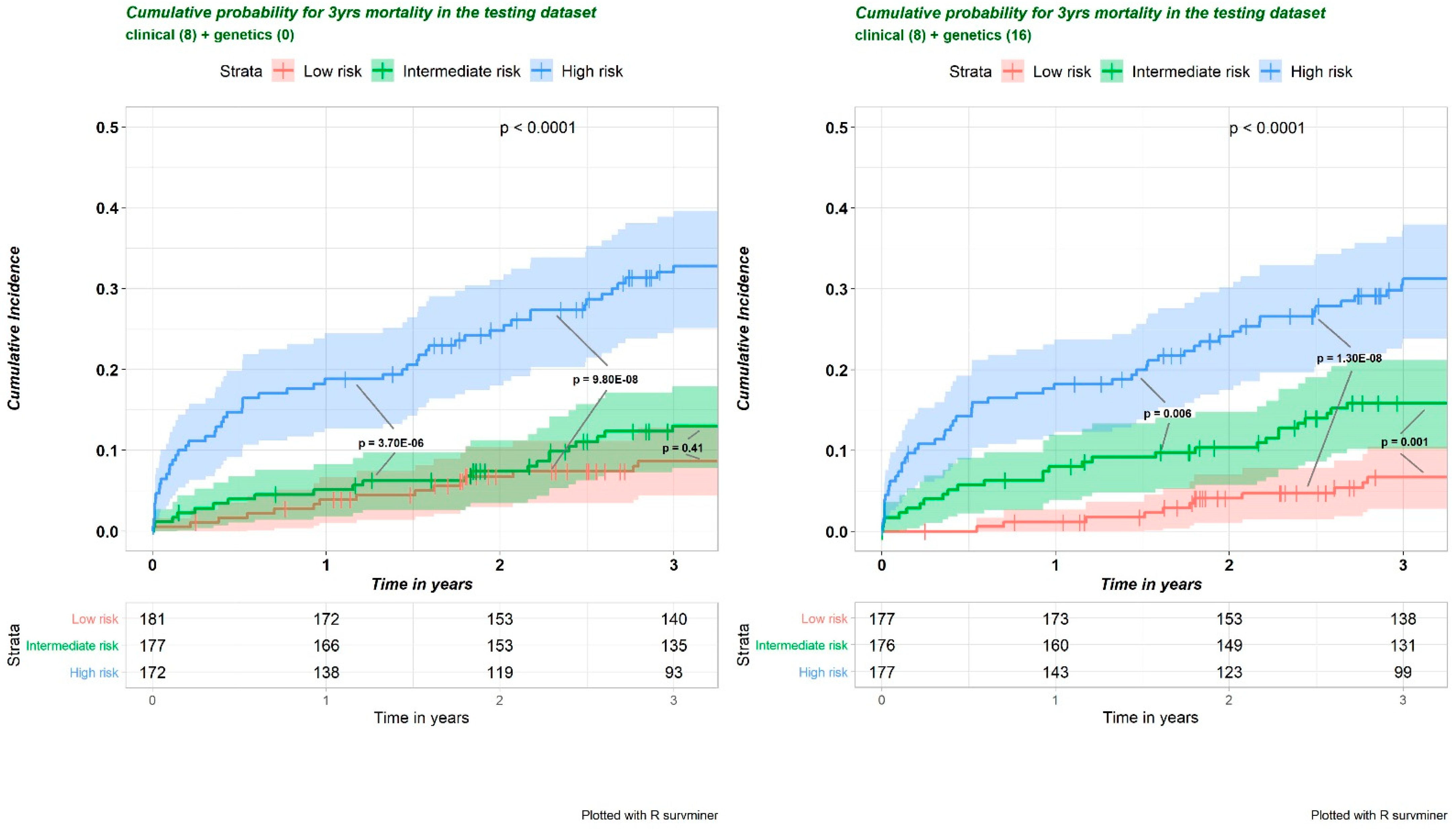
7.1. Pathway-Specific PRSs Augment Etiologic Subtyping of IS and Outcome Prediction
7.2. Improved Predictability of Pathway-Specific PRS for Post-IS Mortality Using an Integrated Cox Proportional Hazards Model
7.3. Validation of Exiting Etiologies and Drug-Targeting Pathways
8. Future Perspectives
8.1. The Utility of PRS in Mixed or Underrepresented Populations
8.2. The Challenges of Integrating PRS into Clinical Decision Support Systems and Risk Stratification Procedures
9. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Available Statement
Conflicts of Interest
Abbreviations
References
- Bevan, S.; Traylor, M.; Adib-Samii, P.; Malik, R.; Paul, N.L.M.; Jackson, C.; Farrall, M.; Rothwell, P.M.; Sudlow, C.; Dichgans, M.; et al. Genetic heritability of ischemic stroke and the contribution of previously reported candidate gene and genomewide associations. Stroke 2012, 43, 3161–3167. [Google Scholar] [CrossRef] [PubMed]
- Arsava, E.M.; Helenius, J.; Avery, R.; Sorgun, M.H.; Kim, G.M.; Pontes-Neto, O.M.; Park, K.Y.; Rosand, J.; Vangel, M.; Ay, H. Assessment of the Predictive Validity of Etiologic Stroke Classification. JAMA Neurol. 2017, 74, 419–426. [Google Scholar] [CrossRef] [PubMed]
- Unlu, M.; de Lange, R.P.; de Silva, R.; Kalaria, R.; St Clair, D. Detection of complement factor B in the cerebrospinal fluid of patients with cerebral autosomal dominant arteriopathy with subcortical infarcts and leukoencephalopathy disease using two-dimensional gel electrophoresis and mass spectrometry. Neurosci. Lett. 2000, 282, 149–152. [Google Scholar] [CrossRef]
- Joutel, A.; Vahedi, K.; Corpechot, C.; Troesch, A.; Chabriat, H.; Vayssiere, C.; Cruaud, C.; Maciazek, J.; Weissenbach, J.; Bousser, M.G.; et al. Strong clustering and stereotyped nature of Notch3 mutations in CADASIL patients. Lancet 1997, 350, 1511–1515. [Google Scholar] [CrossRef]
- Hack, R.J.; Rutten, J.W.; Person, T.N.; Li, J.; Khan, A.; Griessenauer, C.J.; Regeneron Genetics, C.; Abedi, V.; Lesnik Oberstein, S.A.J.; Zand, R. Cysteine-Altering NOTCH3 Variants Are a Risk Factor for Stroke in the Elderly Population. Stroke 2020, 51, 3562–3569. [Google Scholar] [CrossRef]
- Hara, K.; Shiga, A.; Fukutake, T.; Nozaki, H.; Miyashita, A.; Yokoseki, A.; Kawata, H.; Koyama, A.; Arima, K.; Takahashi, T.; et al. Association of HTRA1 mutations and familial ischemic cerebral small-vessel disease. N. Engl. J. Med. 2009, 360, 1729–1739. [Google Scholar] [CrossRef]
- Zhou, C.; Huang, J.; Cui, G.; Zeng, H.; Wang, D.W.; Zhou, Q. Identification of a novel loss-of-function mutation of the GLA gene in a Chinese Han family with Fabry disease. BMC Med. Genet. 2018, 19, 219. [Google Scholar] [CrossRef]
- Germain, D.P. Fabry disease. Orphanet. J. Rare Dis. 2010, 5, 30. [Google Scholar] [CrossRef]
- Richards, A.; van den Maagdenberg, A.M.; Jen, J.C.; Kavanagh, D.; Bertram, P.; Spitzer, D.; Liszewski, M.K.; Barilla-Labarca, M.L.; Terwindt, G.M.; Kasai, Y.; et al. C-terminal truncations in human 3′–5′ DNA exonuclease TREX1 cause autosomal dominant retinal vasculopathy with cerebral leukodystrophy. Nat. Genet. 2007, 39, 1068–1070. [Google Scholar] [CrossRef]
- Yamada, M. Cerebral amyloid angiopathy: An overview. Neuropathology 2000, 20, 8–22. [Google Scholar] [CrossRef]
- Traylor, M.; Persyn, E.; Tomppo, L.; Klasson, S.; Abedi, V.; Bakker, M.K.; Torres, N.; Li, L.; Bell, S.; Rutten-Jacobs, L.; et al. Genetic basis of lacunar stroke: A pooled analysis of individual patient data and genome-wide association studies. Lancet Neurol. 2021, 20, 351–361. [Google Scholar] [CrossRef]
- Li, J.; Abedi, V.; Regeneron Genetic, C.; Zand, R.; Griessenauer, C.J. Replication of Top Loci From COL4A1/2 Associated with White Matter Hyperintensity Burden in Patients with Ischemic Stroke. Stroke 2020, 51, 3751–3755. [Google Scholar] [CrossRef] [PubMed]
- Rannikmae, K.; Davies, G.; Thomson, P.A.; Bevan, S.; Devan, W.J.; Falcone, G.J.; Traylor, M.; Anderson, C.D.; Battey, T.W.; Radmanesh, F.; et al. Common variation in COL4A1/COL4A2 is associated with sporadic cerebral small vessel disease. Neurology 2015, 84, 918–926. [Google Scholar] [CrossRef]
- Persyn, E.; Hanscombe, K.B.; Howson, J.M.M.; Lewis, C.M.; Traylor, M.; Markus, H.S. Genome-wide association study of MRI markers of cerebral small vessel disease in 42,310 participants. Nat. Commun. 2020, 11, 2175. [Google Scholar] [CrossRef] [PubMed]
- Sargurupremraj, M.; Suzuki, H.; Jian, X.; Sarnowski, C.; Evans, T.E.; Bis, J.C.; Eiriksdottir, G.; Sakaue, S.; Terzikhan, N.; Habes, M.; et al. Cerebral small vessel disease genomics and its implications across the lifespan. Nat. Commun. 2020, 11, 6285. [Google Scholar] [CrossRef]
- Malik, R.; Chauhan, G.; Traylor, M.; Sargurupremraj, M.; Okada, Y.; Mishra, A.; Rutten-Jacobs, L.; Giese, A.K.; van der Laan, S.W.; Gretarsdottir, S.; et al. Multiancestry genome-wide association study of 520,000 subjects identifies 32 loci associated with stroke and stroke subtypes. Nat. Genet. 2018, 50, 524–537. [Google Scholar] [CrossRef] [PubMed]
- Neurology Working Group of the Cohorts for Heart and Aging Research in Genomic Epidemiology (CHARGE) Consortium; the Stroke Genetics Network (SiGN); the International Stroke Genetics Consortium (ISGC). Identification of additional risk loci for stroke and small vessel disease: A meta-analysis of genome-wide association studies. Lancet Neurol. 2016, 15, 695–707. [Google Scholar] [CrossRef]
- Ibrahim-Verbaas, C.A.; Fornage, M.; Bis, J.C.; Choi, S.H.; Psaty, B.M.; Meigs, J.B.; Rao, M.; Nalls, M.; Fontes, J.D.; O’Donnell, C.J.; et al. Predicting stroke through genetic risk functions: The CHARGE Risk Score Project. Stroke 2014, 45, 403–412. [Google Scholar] [CrossRef]
- Malik, R.; Bevan, S.; Nalls, M.A.; Holliday, E.G.; Devan, W.J.; Cheng, Y.C.; Ibrahim-Verbaas, C.A.; Verhaaren, B.F.; Bis, J.C.; Joon, A.Y.; et al. Multilocus genetic risk score associates with ischemic stroke in case-control and prospective cohort studies. Stroke 2014, 45, 394–402. [Google Scholar] [CrossRef]
- Tada, H.; Shiffman, D.; Smith, J.G.; Sjogren, M.; Lubitz, S.A.; Ellinor, P.T.; Louie, J.Z.; Catanese, J.J.; Engstrom, G.; Devlin, J.J.; et al. Twelve-single nucleotide polymorphism genetic risk score identifies individuals at increased risk for future atrial fibrillation and stroke. Stroke 2014, 45, 2856–2862. [Google Scholar] [CrossRef]
- Hachiya, T.; Kamatani, Y.; Takahashi, A.; Hata, J.; Furukawa, R.; Shiwa, Y.; Yamaji, T.; Hara, M.; Tanno, K.; Ohmomo, H.; et al. Genetic Predisposition to Ischemic Stroke: A Polygenic Risk Score. Stroke 2017, 48, 253–258. [Google Scholar] [CrossRef] [PubMed]
- Igo, R.P., Jr.; Kinzy, T.G.; Cooke Bailey, J.N. Genetic Risk Scores. Curr. Protoc. Hum. Genet. 2019, 104, e95. [Google Scholar] [CrossRef] [PubMed]
- Choi, S.W.; O’Reilly, P.F. PRSice-2: Polygenic Risk Score software for biobank-scale data. Gigascience 2019, 8, giz082. [Google Scholar] [CrossRef] [PubMed]
- Li, J.; Chaudhary, D.P.; Khan, A.; Griessenauer, C.; Carey, D.J.; Zand, R.; Abedi, V. Polygenic Risk Scores Augment Stroke Subtyping. Neurol. Genet. 2021, 7, e560. [Google Scholar] [CrossRef]
- Zhang, Q.; Prive, F.; Vilhjalmsson, B.; Speed, D. Improved genetic prediction of complex traits from individual-level data or summary statistics. Nat. Commun. 2021, 12, 4192. [Google Scholar] [CrossRef]
- Vilhjalmsson, B.J.; Yang, J.; Finucane, H.K.; Gusev, A.; Lindstrom, S.; Ripke, S.; Genovese, G.; Loh, P.R.; Bhatia, G.; Do, R.; et al. Modeling Linkage Disequilibrium Increases Accuracy of Polygenic Risk Scores. Am. J. Hum. Genet. 2015, 97, 576–592. [Google Scholar] [CrossRef]
- Ge, T.; Chen, C.Y.; Ni, Y.; Feng, Y.A.; Smoller, J.W. Polygenic prediction via Bayesian regression and continuous shrinkage priors. Nat. Commun. 2019, 10, 1776. [Google Scholar] [CrossRef]
- Mak, T.S.H.; Porsch, R.M.; Choi, S.W.; Zhou, X.; Sham, P.C. Polygenic scores via penalized regression on summary statistics. Genet. Epidemiol. 2017, 41, 469–480. [Google Scholar] [CrossRef]
- Rutten-Jacobs, L.C.; Larsson, S.C.; Malik, R.; Rannikmae, K.; MEGASTROKE Consortium; International Stroke Genetics Consortium; Sudlow, C.L.; Dichgans, M.; Markus, H.S.; Traylor, M. Genetic risk, incident stroke, and the benefits of adhering to a healthy lifestyle: Cohort study of 306 473 UK Biobank participants. BMJ 2018, 363, k4168. [Google Scholar] [CrossRef]
- Ibanez, L.; Heitsch, L.; Dube, U.; Farias, F.H.G.; Budde, J.; Bergmann, K.; Davenport, R.; Bradley, J.; Carrera, C.; Kinnunen, J.; et al. Overlap in the Genetic Architecture of Stroke Risk, Early Neurological Changes, and Cardiovascular Risk Factors. Stroke 2019, 50, 1339–1345. [Google Scholar] [CrossRef]
- Malik, R.; Traylor, M.; Pulit, S.L.; Bevan, S.; Hopewell, J.C.; Holliday, E.G.; Zhao, W.; Abrantes, P.; Amouyel, P.; Attia, J.R.; et al. Low-frequency and common genetic variation in ischemic stroke: The METASTROKE collaboration. Neurology 2016, 86, 1217–1226. [Google Scholar] [CrossRef] [PubMed]
- Wray, N.R.; Yang, J.; Hayes, B.J.; Price, A.L.; Goddard, M.E.; Visscher, P.M. Pitfalls of predicting complex traits from SNPs. Nat. Rev. Genet. 2013, 14, 507–515. [Google Scholar] [CrossRef] [PubMed]
- Gazal, S.; Loh, P.R.; Finucane, H.K.; Ganna, A.; Schoech, A.; Sunyaev, S.; Price, A.L. Functional architecture of low-frequency variants highlights strength of negative selection across coding and non-coding annotations. Nat. Genet. 2018, 50, 1600–1607. [Google Scholar] [CrossRef] [PubMed]
- Byars, S.G.; Huang, Q.Q.; Gray, L.A.; Bakshi, A.; Ripatti, S.; Abraham, G.; Stearns, S.C.; Inouye, M. Genetic loci associated with coronary artery disease harbor evidence of selection and antagonistic pleiotropy. PLoS Genet. 2017, 13, e1006328. [Google Scholar] [CrossRef]
- Bersano, A.; Ballabio, E.; Bresolin, N.; Candelise, L. Genetic polymorphisms for the study of multifactorial stroke. Hum. Mutat. 2008, 29, 776–795. [Google Scholar] [CrossRef]
- Zhang, Z.; Xu, G.; Liu, D.; Fan, X.; Zhu, W.; Liu, X. Angiotensin-converting enzyme insertion/deletion polymorphism contributes to ischemic stroke risk: A meta-analysis of 50 case-control studies. PLoS ONE 2012, 7, e46495. [Google Scholar] [CrossRef]
- Rao, R.; Tah, V.; Casas, J.P.; Hingorani, A.; Whittaker, J.; Smeeth, L.; Sharma, P. Ischaemic stroke subtypes and their genetic basis: A comprehensive meta-analysis of small and large vessel stroke. Eur. Neurol. 2009, 61, 76–86. [Google Scholar] [CrossRef]
- Bulik-Sullivan, B.K.; Loh, P.R.; Finucane, H.K.; Ripke, S.; Yang, J.; Schizophrenia Working Group of the Psychiatric Genomics Consortium; Patterson, N.; Daly, M.J.; Price, A.L.; Neale, B.M. LD Score regression distinguishes confounding from polygenicity in genome-wide association studies. Nat. Genet. 2015, 47, 291–295. [Google Scholar] [CrossRef]
- Pickrell, J.K.; Berisa, T.; Liu, J.Z.; Segurel, L.; Tung, J.Y.; Hinds, D.A. Detection and interpretation of shared genetic influences on 42 human traits. Nat. Genet. 2016, 48, 709–717. [Google Scholar] [CrossRef]
- Shi, H.; Mancuso, N.; Spendlove, S.; Pasaniuc, B. Local Genetic Correlation Gives Insights into the Shared Genetic Architecture of Complex Traits. Am. J. Hum. Genet. 2017, 101, 737–751. [Google Scholar] [CrossRef]
- Fedak, K.M.; Bernal, A.; Capshaw, Z.A.; Gross, S. Applying the Bradford Hill criteria in the 21st century: How data integration has changed causal inference in molecular epidemiology. Emerg. Epidemiol. 2015, 12, 14. [Google Scholar] [CrossRef] [PubMed]
- Dai, J.Y.; Peters, U.; Wang, X.; Kocarnik, J.; Chang-Claude, J.; Slattery, M.L.; Chan, A.; Lemire, M.; Berndt, S.I.; Casey, G.; et al. Diagnostics for Pleiotropy in Mendelian Randomization Studies: Global and Individual Tests for Direct Effects. Am. J. Epidemiol. 2018, 187, 2672–2680. [Google Scholar] [CrossRef] [PubMed]
- Davies, N.M.; Holmes, M.V.; Davey Smith, G. Reading Mendelian randomisation studies: A guide, glossary, and checklist for clinicians. BMJ 2018, 362, k601. [Google Scholar] [CrossRef] [PubMed]
- Hindy, G.; Engstrom, G.; Larsson, S.C.; Traylor, M.; Markus, H.S.; Melander, O.; Orho-Melander, M.; Stroke Genetics, N. Role of Blood Lipids in the Development of Ischemic Stroke and its Subtypes: A Mendelian Randomization Study. Stroke 2018, 49, 820–827. [Google Scholar] [CrossRef]
- Dichgans, M.; Pulit, S.L.; Rosand, J. Stroke genetics: Discovery, biology, and clinical applications. Lancet Neurol. 2019, 18, 587–599. [Google Scholar] [CrossRef]
- Pulit, S.L.; Weng, L.C.; McArdle, P.F.; Trinquart, L.; Choi, S.H.; Mitchell, B.D.; Rosand, J.; de Bakker, P.I.W.; Benjamin, E.J.; Ellinor, P.T.; et al. Atrial fibrillation genetic risk differentiates cardioembolic stroke from other stroke subtypes. Neurol. Genet. 2018, 4, e293. [Google Scholar] [CrossRef]
- Wolf, P.A.; Abbott, R.D.; Kannel, W.B. Atrial fibrillation as an independent risk factor for stroke: The Framingham Study. Stroke 1991, 22, 983–988. [Google Scholar] [CrossRef]
- Feigin, V.L.; Lawes, C.M.; Bennett, D.A.; Barker-Collo, S.L.; Parag, V. Worldwide stroke incidence and early case fatality reported in 56 population-based studies: A systematic review. Lancet Neurol. 2009, 8, 355–369. [Google Scholar] [CrossRef]
- Diaz, J.; Koza, E.; Chaudhary, D.; Shahjouei, S.; Naved, M.M.A.; Malik, M.T.; Li, J.; Adibuzzaman, M.; Griffin, P.; Abedi, V.; et al. Adherence to anticoagulant guideline for atrial fibrillation: A large care gap among stroke patients in a rural population. J. Neurol. Sci. 2021, 424, 117410. [Google Scholar] [CrossRef]
- Gudbjartsson, D.F.; Arnar, D.O.; Helgadottir, A.; Gretarsdottir, S.; Holm, H.; Sigurdsson, A.; Jonasdottir, A.; Baker, A.; Thorleifsson, G.; Kristjansson, K.; et al. Variants conferring risk of atrial fibrillation on chromosome 4q25. Nature 2007, 448, 353–357. [Google Scholar] [CrossRef]
- Gretarsdottir, S.; Thorleifsson, G.; Manolescu, A.; Styrkarsdottir, U.; Helgadottir, A.; Gschwendtner, A.; Kostulas, K.; Kuhlenbaumer, G.; Bevan, S.; Jonsdottir, T.; et al. Risk variants for atrial fibrillation on chromosome 4q25 associate with ischemic stroke. Ann. Neurol. 2008, 64, 402–409. [Google Scholar] [CrossRef]
- Gudbjartsson, D.F.; Holm, H.; Gretarsdottir, S.; Thorleifsson, G.; Walters, G.B.; Thorgeirsson, G.; Gulcher, J.; Mathiesen, E.B.; Njolstad, I.; Nyrnes, A.; et al. A sequence variant in ZFHX3 on 16q22 associates with atrial fibrillation and ischemic stroke. Nat. Genet. 2009, 41, 876–878. [Google Scholar] [CrossRef] [PubMed]
- Christophersen, I.E.; Rienstra, M.; Roselli, C.; Yin, X.; Geelhoed, B.; Barnard, J.; Lin, H.; Arking, D.E.; Smith, A.V.; Albert, C.M.; et al. Large-scale analyses of common and rare variants identify 12 new loci associated with atrial fibrillation. Nat. Genet. 2017, 49, 946–952. [Google Scholar] [CrossRef] [PubMed]
- Marston, N.A.; Patel, P.N.; Kamanu, F.K.; Nordio, F.; Melloni, G.M.; Roselli, C.; Gurmu, Y.; Weng, L.C.; Bonaca, M.P.; Giugliano, R.P.; et al. Clinical Application of a Novel Genetic Risk Score for Ischemic Stroke in Patients with Cardiometabolic Disease. Circulation 2021, 143, 470–478. [Google Scholar] [CrossRef]
- O’Sullivan, J.W.; Shcherbina, A.; Justesen, J.M.; Turakhia, M.; Perez, M.; Wand, H.; Tcheandjieu, C.; Clarke, S.L.; Rivas, M.A.; Ashley, E.A. Combining Clinical and Polygenic Risk Improves Stroke Prediction Among Individuals with Atrial Fibrillation. Circ. Genom. Precis. Med. 2021, 14, e003168. [Google Scholar] [CrossRef]
- Pantoni, L. Cerebral small vessel disease: From pathogenesis and clinical characteristics to therapeutic challenges. Lancet Neurol. 2010, 9, 689–701. [Google Scholar] [CrossRef]
- Caplan, L.R. Lacunar infarction and small vessel disease: Pathology and pathophysiology. J. Stroke 2015, 17, 2–6. [Google Scholar] [CrossRef]
- Ogata, J.; Yamanishi, H.; Ishibashi-Ueda, H. Cerebral small vessel disease: The pathological features of cerebral amyloid angiopathy. Brain Nerve 2013, 65, 879–885. [Google Scholar]
- Pantoni, L.; Gorelick, P. Advances in vascular cognitive impairment 2010. Stroke 2011, 42, 291–293. [Google Scholar] [CrossRef]
- Lau, K.K.; Li, L.; Simoni, M.; Mehta, Z.; Kuker, W.; Rothwell, P.M.; Oxford Vascular, S. Long-Term Premorbid Blood Pressure and Cerebral Small Vessel Disease Burden on Imaging in Transient Ischemic Attack and Ischemic Stroke. Stroke 2018, 49, 2053–2060. [Google Scholar] [CrossRef]
- Wardlaw, J.M.; Smith, E.E.; Biessels, G.J.; Cordonnier, C.; Fazekas, F.; Frayne, R.; Lindley, R.I.; O’Brien, J.T.; Barkhof, F.; Benavente, O.R.; et al. Neuroimaging standards for research into small vessel disease and its contribution to ageing and neurodegeneration. Lancet Neurol. 2013, 12, 822–838. [Google Scholar] [CrossRef]
- Atwood, L.D.; Wolf, P.A.; Heard-Costa, N.L.; Massaro, J.M.; Beiser, A.; D’Agostino, R.B.; DeCarli, C. Genetic variation in white matter hyperintensity volume in the Framingham Study. Stroke 2004, 35, 1609–1613. [Google Scholar] [CrossRef] [PubMed]
- Turner, S.T.; Jack, C.R.; Fornage, M.; Mosley, T.H.; Boerwinkle, E.; de Andrade, M. Heritability of leukoaraiosis in hypertensive sibships. Hypertension 2004, 43, 483–487. [Google Scholar] [CrossRef] [PubMed]
- Kochunov, P.; Glahn, D.; Winkler, A.; Duggirala, R.; Olvera, R.L.; Cole, S.; Dyer, T.D.; Almasy, L.; Fox, P.T.; Blangero, J. Analysis of genetic variability and whole genome linkage of whole-brain, subcortical, and ependymal hyperintense white matter volume. Stroke 2009, 40, 3685–3690. [Google Scholar] [CrossRef]
- Carmelli, D.; DeCarli, C.; Swan, G.E.; Jack, L.M.; Reed, T.; Wolf, P.A.; Miller, B.L. Evidence for genetic variance in white matter hyperintensity volume in normal elderly male twins. Stroke 1998, 29, 1177–1181. [Google Scholar] [CrossRef]
- Haffner, C.; Malik, R.; Dichgans, M. Genetic factors in cerebral small vessel disease and their impact on stroke and dementia. J. Cereb. Blood Flow Metab. 2016, 36, 158–171. [Google Scholar] [CrossRef]
- Kubo, M.; Hata, J.; Ninomiya, T.; Matsuda, K.; Yonemoto, K.; Nakano, T.; Matsushita, T.; Yamazaki, K.; Ohnishi, Y.; Saito, S.; et al. A nonsynonymous SNP in PRKCH (protein kinase C eta) increases the risk of cerebral infarction. Nat. Genet. 2007, 39, 212–217. [Google Scholar] [CrossRef]
- Wu, L.; Shen, Y.; Liu, X.; Ma, X.; Xi, B.; Mi, J.; Lindpaintner, K.; Tan, X.; Wang, X. The 1425G/A SNP in PRKCH is associated with ischemic stroke and cerebral hemorrhage in a Chinese population. Stroke 2009, 40, 2973–2976. [Google Scholar] [CrossRef]
- Paternoster, L.; Chen, W.; Sudlow, C.L. Genetic determinants of white matter hyperintensities on brain scans: A systematic assessment of 19 candidate gene polymorphisms in 46 studies in 19,000 subjects. Stroke 2009, 40, 2020–2026. [Google Scholar] [CrossRef]
- Fornage, M.; Debette, S.; Bis, J.C.; Schmidt, H.; Ikram, M.A.; Dufouil, C.; Sigurdsson, S.; Lumley, T.; DeStefano, A.L.; Fazekas, F.; et al. Genome-wide association studies of cerebral white matter lesion burden: The CHARGE consortium. Ann. Neurol. 2011, 69, 928–939. [Google Scholar] [CrossRef]
- Woo, D.; Falcone, G.J.; Devan, W.J.; Brown, W.M.; Biffi, A.; Howard, T.D.; Anderson, C.D.; Brouwers, H.B.; Valant, V.; Battey, T.W.; et al. Meta-analysis of genome-wide association studies identifies 1q22 as a susceptibility locus for intracerebral hemorrhage. Am. J. Hum. Genet. 2014, 94, 511–521. [Google Scholar] [CrossRef] [PubMed]
- Verhaaren, B.F.; Debette, S.; Bis, J.C.; Smith, J.A.; Ikram, M.K.; Adams, H.H.; Beecham, A.H.; Rajan, K.B.; Lopez, L.M.; Barral, S.; et al. Multiethnic genome-wide association study of cerebral white matter hyperintensities on MRI. Circ. Cardiovasc. Genet. 2015, 8, 398–409. [Google Scholar] [CrossRef] [PubMed]
- Traylor, M.; Zhang, C.R.; Adib-Samii, P.; Devan, W.J.; Parsons, O.E.; Lanfranconi, S.; Gregory, S.; Cloonan, L.; Falcone, G.J.; Radmanesh, F.; et al. Genome-wide meta-analysis of cerebral white matter hyperintensities in patients with stroke. Neurology 2016, 86, 146–153. [Google Scholar] [CrossRef] [PubMed]
- Network, N.S.G.; International Stroke Genetics, C. Loci associated with ischaemic stroke and its subtypes (SiGN): A genome-wide association study. Lancet Neurol. 2016, 15, 174–184. [Google Scholar] [CrossRef]
- Traylor, M.; Malik, R.; Nalls, M.A.; Cotlarciuc, I.; Radmanesh, F.; Thorleifsson, G.; Hanscombe, K.B.; Langefeld, C.; Saleheen, D.; Rost, N.S.; et al. Genetic variation at 16q24.2 is associated with small vessel stroke. Ann. Neurol. 2017, 81, 383–394. [Google Scholar] [CrossRef]
- Rutten-Jacobs, L.C.A.; Tozer, D.J.; Duering, M.; Malik, R.; Dichgans, M.; Markus, H.S.; Traylor, M. Genetic Study of White Matter Integrity in UK Biobank (N = 8448) and the Overlap with Stroke, Depression, and Dementia. Stroke 2018, 49, 1340–1347. [Google Scholar] [CrossRef]
- Traylor, M.; Tozer, D.J.; Croall, I.D.; Lisiecka Ford, D.M.; Olorunda, A.O.; Boncoraglio, G.; Dichgans, M.; Lemmens, R.; Rosand, J.; Rost, N.S.; et al. Genetic variation in PLEKHG1 is associated with white matter hyperintensities (n = 11,226). Neurology 2019, 92, e749–e757. [Google Scholar] [CrossRef]
- Schmidt, H.; Zeginigg, M.; Wiltgen, M.; Freudenberger, P.; Petrovic, K.; Cavalieri, M.; Gider, P.; Enzinger, C.; Fornage, M.; Debette, S.; et al. Genetic variants of the NOTCH3 gene in the elderly and magnetic resonance imaging correlates of age-related cerebral small vessel disease. Brain 2011, 134, 3384–3397. [Google Scholar] [CrossRef]
- Wight, T.N. Versican: A versatile extracellular matrix proteoglycan in cell biology. Curr. Opin. Cell Biol. 2002, 14, 617–623. [Google Scholar] [CrossRef]
- Naba, A.; Clauser, K.R.; Hoersch, S.; Liu, H.; Carr, S.A.; Hynes, R.O. The matrisome: In silico definition and in vivo characterization by proteomics of normal and tumor extracellular matrices. Mol. Cell Proteom. 2012, 11, M111.014647. [Google Scholar] [CrossRef]
- Reyahi, A.; Nik, A.M.; Ghiami, M.; Gritli-Linde, A.; Ponten, F.; Johansson, B.R.; Carlsson, P. Foxf2 Is Required for Brain Pericyte Differentiation and Development and Maintenance of the Blood-Brain Barrier. Dev. Cell 2015, 34, 19–32. [Google Scholar] [CrossRef] [PubMed]
- Sweeney, M.D.; Ayyadurai, S.; Zlokovic, B.V. Pericytes of the neurovascular unit: Key functions and signaling pathways. Nat. Neurosci. 2016, 19, 771–783. [Google Scholar] [CrossRef] [PubMed]
- Siegenthaler, J.A.; Choe, Y.; Patterson, K.P.; Hsieh, I.; Li, D.; Jaminet, S.C.; Daneman, R.; Kume, T.; Huang, E.J.; Pleasure, S.J. Foxc1 is required by pericytes during fetal brain angiogenesis. Biol. Open 2013, 2, 647–659. [Google Scholar] [CrossRef] [PubMed]
- Tumer, Z.; Bach-Holm, D. Axenfeld-Rieger syndrome and spectrum of PITX2 and FOXC1 mutations. Eur. J. Hum. Genet. 2009, 17, 1527–1539. [Google Scholar] [CrossRef]
- Boulouis, G.; Charidimou, A.; Jessel, M.J.; Xiong, L.; Roongpiboonsopit, D.; Fotiadis, P.; Pasi, M.; Ayres, A.; Merrill, M.E.; Schwab, K.M.; et al. Small vessel disease burden in cerebral amyloid angiopathy without symptomatic hemorrhage. Neurology 2017, 88, 878–884. [Google Scholar] [CrossRef]
- Charidimou, A.; Boulouis, G.; Gurol, M.E.; Ayata, C.; Bacskai, B.J.; Frosch, M.P.; Viswanathan, A.; Greenberg, S.M. Emerging concepts in sporadic cerebral amyloid angiopathy. Brain 2017, 140, 1829–1850. [Google Scholar] [CrossRef]
- Bugiani, O.; Giaccone, G.; Rossi, G.; Mangieri, M.; Capobianco, R.; Morbin, M.; Mazzoleni, G.; Cupidi, C.; Marcon, G.; Giovagnoli, A.; et al. Hereditary cerebral hemorrhage with amyloidosis associated with the E693K mutation of APP. Arch. Neurol. 2010, 67, 987–995. [Google Scholar] [CrossRef]
- Kadowaki, H.; Nishitoh, H.; Urano, F.; Sadamitsu, C.; Matsuzawa, A.; Takeda, K.; Masutani, H.; Yodoi, J.; Urano, Y.; Nagano, T.; et al. Amyloid beta induces neuronal cell death through ROS-mediated ASK1 activation. Cell Death Differ. 2005, 12, 19–24. [Google Scholar] [CrossRef]
- Cajamarca, S.A.; Norris, E.H.; van der Weerd, L.; Strickland, S.; Ahn, H.J. Cerebral amyloid angiopathy-linked beta-amyloid mutations promote cerebral fibrin deposits via increased binding affinity for fibrinogen. Proc. Natl. Acad. Sci. USA 2020, 117, 14482–14492. [Google Scholar] [CrossRef]
- Rozemuller, A.J.; Roos, R.A.; Bots, G.T.; Kamphorst, W.; Eikelenboom, P.; Van Nostrand, W.E. Distribution of beta/A4 protein and amyloid precursor protein in hereditary cerebral hemorrhage with amyloidosis-Dutch type and Alzheimer’s disease. Am. J. Pathol. 1993, 142, 1449–1457. [Google Scholar]
- Wattendorff, A.R.; Bots, G.T.; Went, L.N.; Endtz, L.J. Familial cerebral amyloid angiopathy presenting as recurrent cerebral haemorrhage. J. Neurol. Sci. 1982, 55, 121–135. [Google Scholar] [CrossRef]
- Levy, E.; Carman, M.D.; Fernandez-Madrid, I.J.; Power, M.D.; Lieberburg, I.; van Duinen, S.G.; Bots, G.T.; Luyendijk, W.; Frangione, B. Mutation of the Alzheimer’s disease amyloid gene in hereditary cerebral hemorrhage, Dutch type. Science 1990, 248, 1124–1126. [Google Scholar] [CrossRef] [PubMed]
- Nochlin, D.; Bird, T.D.; Nemens, E.J.; Ball, M.J.; Sumi, S.M. Amyloid angiopathy in a Volga German family with Alzheimer’s disease and a presenilin-2 mutation (N141I). Ann. Neurol. 1998, 43, 131–135. [Google Scholar] [CrossRef] [PubMed]
- Van Nostrand, W.E. The influence of the amyloid ss-protein and its precursor in modulating cerebral hemostasis. Biochim. Biophys. Acta 2016, 1862, 1018–1026. [Google Scholar] [CrossRef] [PubMed]
- Li, J.; Chaudhary, D.; Griessenauer, C.J.; Carey, D.J.; Zand, R.; Abedi, V. Predicting mortality among ischemic stroke patients using pathways-derived polygenic risk scores. Sci. Rep. 2022, 12, 12358. [Google Scholar] [CrossRef]
- Gamazon, E.R.; Wheeler, H.E.; Shah, K.P.; Mozaffari, S.V.; Aquino-Michaels, K.; Carroll, R.J.; Eyler, A.E.; Denny, J.C.; Consortium, G.T.; Nicolae, D.L.; et al. A gene-based association method for mapping traits using reference transcriptome data. Nat. Genet. 2015, 47, 1091–1098. [Google Scholar] [CrossRef]
- Lee, S.; Emond, M.J.; Bamshad, M.J.; Barnes, K.C.; Rieder, M.J.; Nickerson, D.A.; Team, N.G.E.S.P.-E.L.P.; Christiani, D.C.; Wurfel, M.M.; Lin, X. Optimal unified approach for rare-variant association testing with application to small-sample case-control whole-exome sequencing studies. Am. J. Hum. Genet. 2012, 91, 224–237. [Google Scholar] [CrossRef]
- Grossman, S.R.; Andersen, K.G.; Shlyakhter, I.; Tabrizi, S.; Winnicki, S.; Yen, A.; Park, D.J.; Griesemer, D.; Karlsson, E.K.; Wong, S.H.; et al. Identifying recent adaptations in large-scale genomic data. Cell 2013, 152, 703–713. [Google Scholar] [CrossRef]
- Culman, J.; Zhao, Y.; Gohlke, P.; Herdegen, T. PPAR-gamma: Therapeutic target for ischemic stroke. Trends. Pharm. Sci. 2007, 28, 244–249. [Google Scholar] [CrossRef]
- Huang, C.X.; Zhang, Y.L. The target of regulating the ATP-binding cassette A1 protein (ABCA1): Promoting ABCA1-mediated cholesterol efflux in different cells. Curr. Pharm. Biotechnol. 2013, 14, 623–631. [Google Scholar] [CrossRef][Green Version]
- Iwamoto, N.; Abe-Dohmae, S.; Ayaori, M.; Tanaka, N.; Kusuhara, M.; Ohsuzu, F.; Yokoyama, S. ATP-binding cassette transporter A1 gene transcription is downregulated by activator protein 2alpha. Doxazosin inhibits activator protein 2alpha and increases high-density lipoprotein biogenesis independent of alpha1-adrenoceptor blockade. Circ. Res. 2007, 101, 156–165. [Google Scholar] [CrossRef]
- Klimentidis, Y.C.; Arora, A.; Newell, M.; Zhou, J.; Ordovas, J.M.; Renquist, B.J.; Wood, A.C. Phenotypic and Genetic Characterization of Lower LDL Cholesterol and Increased Type 2 Diabetes Risk in the UK Biobank. Diabetes 2020, 69, 2194–2205. [Google Scholar] [CrossRef] [PubMed]
- Park, J.H.; Hong, K.S.; Lee, E.J.; Lee, J.; Kim, D.E. High levels of apolipoprotein B/AI ratio are associated with intracranial atherosclerotic stenosis. Stroke 2011, 42, 3040–3046. [Google Scholar] [CrossRef] [PubMed]
- Debette, S.; Seshadri, S. Genetics of atherothrombotic and lacunar stroke. Circ. Cardiovasc. Genet. 2009, 2, 191–198. [Google Scholar] [CrossRef] [PubMed]
- Lange, C.; Storkebaum, E.; de Almodovar, C.R.; Dewerchin, M.; Carmeliet, P. Vascular endothelial growth factor: A neurovascular target in neurological diseases. Nat. Rev. Neurol. 2016, 12, 439–454. [Google Scholar] [CrossRef]
- Sun, B.B.; Maranville, J.C.; Peters, J.E.; Stacey, D.; Staley, J.R.; Blackshaw, J.; Burgess, S.; Jiang, T.; Paige, E.; Surendran, P.; et al. Genomic atlas of the human plasma proteome. Nature 2018, 558, 73–79. [Google Scholar] [CrossRef]
- Bushnell, C.D.; Goldstein, L.B. Diagnostic testing for coagulopathies in patients with ischemic stroke. Stroke 2000, 31, 3067–3078. [Google Scholar] [CrossRef]
- Bushnell, C.; Siddiqi, Z.; Morgenlander, J.C.; Goldstein, L.B. Use of specialized coagulation testing in the evaluation of patients with acute ischemic stroke. Neurology 2001, 56, 624–627. [Google Scholar] [CrossRef]
- Waddy, S.P. Disorders of coagulation in stroke. Semin. Neurol. 2006, 26, 57–64. [Google Scholar] [CrossRef]
- Ay, H.; Furie, K.L.; Singhal, A.; Smith, W.S.; Sorensen, A.G.; Koroshetz, W.J. An evidence-based causative classification system for acute ischemic stroke. Ann. Neurol. 2005, 58, 688–697. [Google Scholar] [CrossRef]
- Ay, H.; Benner, T.; Arsava, E.M.; Furie, K.L.; Singhal, A.B.; Jensen, M.B.; Ayata, C.; Towfighi, A.; Smith, E.E.; Chong, J.Y.; et al. A computerized algorithm for etiologic classification of ischemic stroke: The Causative Classification of Stroke System. Stroke 2007, 38, 2979–2984. [Google Scholar] [CrossRef] [PubMed]
- Abraham, G.; Malik, R.; Yonova-Doing, E.; Salim, A.; Wang, T.; Danesh, J.; Butterworth, A.S.; Howson, J.M.M.; Inouye, M.; Dichgans, M. Genomic risk score offers predictive performance comparable to clinical risk factors for ischaemic stroke. Nat. Commun. 2019, 10, 5819. [Google Scholar] [CrossRef] [PubMed]
- Abedi, V.; Avula, V.; Razavi, S.M.; Bavishi, S.; Chaudhary, D.; Shahjouei, S.; Wang, M.; Griessenauer, C.J.; Li, J.; Zand, R. Predicting short and long-term mortality after acute ischemic stroke using EHR. J. Neurol. Sci. 2021, 427, 117560. [Google Scholar] [CrossRef]
- Abedi, V.; Avula, V.; Chaudhary, D.; Shahjouei, S.; Khan, A.; Griessenauer, C.J.; Li, J.; Zand, R. Prediction of Long-Term Stroke Recurrence Using Machine Learning Models. J. Clin. Med. 2021, 10, 1286. [Google Scholar] [CrossRef]
- Spooner, A.; Chen, E.; Sowmya, A.; Sachdev, P.; Kochan, N.A.; Trollor, J.; Brodaty, H. A comparison of machine learning methods for survival analysis of high-dimensional clinical data for dementia prediction. Sci. Rep. 2020, 10, 20410. [Google Scholar] [CrossRef] [PubMed]
- Smith, E.E.; Charidimou, A.; Ayata, C.; Werring, D.J.; Greenberg, S.M. Cerebral Amyloid Angiopathy-Related Transient Focal Neurologic Episodes. Neurology 2021, 97, 231–238. [Google Scholar] [CrossRef]
- Bak, S.; Gaist, D.; Sindrup, S.H.; Skytthe, A.; Christensen, K. Genetic liability in stroke: A long-term follow-up study of Danish twins. Stroke 2002, 33, 769–774. [Google Scholar] [CrossRef]
- Tibshirani, R. The lasso method for variable selection in the Cox model. Stat. Med. 1997, 16, 385–395. [Google Scholar] [CrossRef]
- Chavakis, E.; Dimmeler, S. Regulation of endothelial cell survival and apoptosis during angiogenesis. Arter. Thromb. Vasc. Biol. 2002, 22, 887–893. [Google Scholar] [CrossRef]
- Scarabelli, T.; Stephanou, A.; Rayment, N.; Pasini, E.; Comini, L.; Curello, S.; Ferrari, R.; Knight, R.; Latchman, D. Apoptosis of endothelial cells precedes myocyte cell apoptosis in ischemia/reperfusion injury. Circulation 2001, 104, 253–256. [Google Scholar] [CrossRef]
- Poller, W.C.; Nahrendorf, M.; Swirski, F.K. Hematopoiesis and Cardiovascular Disease. Circ. Res. 2020, 126, 1061–1085. [Google Scholar] [CrossRef] [PubMed]
- Sobowale, O.A.; Parry-Jones, A.R.; Smith, C.J.; Tyrrell, P.J.; Rothwell, N.J.; Allan, S.M. Interleukin-1 in Stroke: From Bench to Bedside. Stroke 2016, 47, 2160–2167. [Google Scholar] [CrossRef] [PubMed]
- Emsley, H.C.; Smith, C.J.; Georgiou, R.F.; Vail, A.; Hopkins, S.J.; Rothwell, N.J.; Tyrrell, P.J.; Acute Stroke, I. A randomised phase II study of interleukin-1 receptor antagonist in acute stroke patients. J. Neurol. Neurosurg. Psychiatry 2005, 76, 1366–1372. [Google Scholar] [CrossRef] [PubMed]
- Smith, C.J.; Emsley, H.C.; Udeh, C.T.; Vail, A.; Hoadley, M.E.; Rothwell, N.J.; Tyrrell, P.J.; Hopkins, S.J. Interleukin-1 receptor antagonist reverses stroke-associated peripheral immune suppression. Cytokine 2012, 58, 384–389. [Google Scholar] [CrossRef]
- Singh, N.; Hopkins, S.J.; Hulme, S.; Galea, J.P.; Hoadley, M.; Vail, A.; Hutchinson, P.J.; Grainger, S.; Rothwell, N.J.; King, A.T.; et al. The effect of intravenous interleukin-1 receptor antagonist on inflammatory mediators in cerebrospinal fluid after subarachnoid haemorrhage: A phase II randomised controlled trial. J. Neuroinflamm. 2014, 11, 1. [Google Scholar] [CrossRef]
- Barone, F.C.; Arvin, B.; White, R.F.; Miller, A.; Webb, C.L.; Willette, R.N.; Lysko, P.G.; Feuerstein, G.Z. Tumor necrosis factor-alpha. A mediator of focal ischemic brain injury. Stroke 1997, 28, 1233–1244. [Google Scholar] [CrossRef]
- Bonetti, N.R.; Diaz-Canestro, C.; Liberale, L.; Crucet, M.; Akhmedov, A.; Merlini, M.; Reiner, M.F.; Gobbato, S.; Stivala, S.; Kollias, G.; et al. Tumour Necrosis Factor-alpha Inhibition Improves Stroke Outcome in a Mouse Model of Rheumatoid Arthritis. Sci. Rep. 2019, 9, 2173. [Google Scholar] [CrossRef]
- Bush, L.R.; Campbell, W.B.; Kern, K.; Tilton, G.D.; Apprill, P.; Ashton, J.; Schmitz, J.; Buja, L.M.; Willerson, J.T. The effects of alpha 2-adrenergic and serotonergic receptor antagonists on cyclic blood flow alterations in stenosed canine coronary arteries. Circ. Res. 1984, 55, 642–652. [Google Scholar] [CrossRef]
- Ashton, J.H.; Benedict, C.R.; Fitzgerald, C.; Raheja, S.; Taylor, A.; Campbell, W.B.; Buja, L.M.; Willerson, J.T. Serotonin as a mediator of cyclic flow variations in stenosed canine coronary arteries. Circulation 1986, 73, 572–578. [Google Scholar] [CrossRef]
- Vikenes, K.; Farstad, M.; Nordrehaug, J.E. Serotonin is associated with coronary artery disease and cardiac events. Circulation 1999, 100, 483–489. [Google Scholar] [CrossRef]
- Eidt, J.F.; Ashton, J.; Golino, P.; McNatt, J.; Buja, L.M.; Willerson, J.T. Thromboxane A2 and serotonin mediate coronary blood flow reductions in unsedated dogs. Am. J. Physiol. 1989, 257, H873–H882. [Google Scholar] [CrossRef] [PubMed]
- Fanburg, B.L.; Lee, S.L. A new role for an old molecule: Serotonin as a mitogen. Am. J. Physiol. 1997, 272, L795–L806. [Google Scholar] [CrossRef] [PubMed]
- De Clerck, F. The role of serotonin in thrombogenesis. Clin. Physiol. Biochem. 1990, 8 (Suppl. 3), 40–49. [Google Scholar]
- Willerson, J.T.; Yao, S.K.; McNatt, J.; Benedict, C.R.; Anderson, H.V.; Golino, P.; Murphree, S.S.; Buja, L.M. Frequency and severity of cyclic flow alternations and platelet aggregation predict the severity of neointimal proliferation following experimental coronary stenosis and endothelial injury. Proc. Natl. Acad. Sci. USA 1991, 88, 10624–10628. [Google Scholar] [CrossRef] [PubMed]
- Pakala, R.; Willerson, J.T.; Benedict, C.R. Mitogenic effect of serotonin on vascular endothelial cells. Circulation 1994, 90, 1919–1926. [Google Scholar] [CrossRef]
- Jorge, R.E.; Acion, L.; Moser, D.; Adams, H.P., Jr.; Robinson, R.G. Escitalopram and enhancement of cognitive recovery following stroke. Arch. Gen. Psychiatry 2010, 67, 187–196. [Google Scholar] [CrossRef]
- Globus, M.Y.; Wester, P.; Busto, R.; Dietrich, W.D. Ischemia-induced extracellular release of serotonin plays a role in CA1 neuronal cell death in rats. Stroke 1992, 23, 1595–1601. [Google Scholar] [CrossRef]
- Dimyan, M.A.; Cohen, L.G. Neuroplasticity in the context of motor rehabilitation after stroke. Nat. Rev. Neurol. 2011, 7, 76–85. [Google Scholar] [CrossRef]
- Gulati, T.; Won, S.J.; Ramanathan, D.S.; Wong, C.C.; Bodepudi, A.; Swanson, R.A.; Ganguly, K. Robust neuroprosthetic control from the stroke perilesional cortex. J. Neurosci. 2015, 35, 8653–8661. [Google Scholar] [CrossRef]
- Wathen, C.A.; Frizon, L.A.; Maiti, T.K.; Baker, K.B.; Machado, A.G. Deep brain stimulation of the cerebellum for poststroke motor rehabilitation: From laboratory to clinical trial. Neurosurg. Focus 2018, 45, E13. [Google Scholar] [CrossRef]
- Andersen, K.K.; Olsen, T.S. The obesity paradox in stroke: Lower mortality and lower risk of readmission for recurrent stroke in obese stroke patients. Int. J. Stroke 2015, 10, 99–104. [Google Scholar] [CrossRef] [PubMed]
- Chaudhary, D.; Khan, A.; Gupta, M.; Hu, Y.; Li, J.; Abedi, V.; Zand, R. Obesity and mortality after the first ischemic stroke: Is obesity paradox real? PLoS ONE 2021, 16, e0246877. [Google Scholar] [CrossRef] [PubMed]
- Bomba, L.; Walter, K.; Soranzo, N. The impact of rare and low-frequency genetic variants in common disease. Genome Biol. 2017, 18, 77. [Google Scholar] [CrossRef] [PubMed]
- Malik, R.; Dichgans, M. Challenges and opportunities in stroke genetics. Cardiovasc. Res. 2018, 114, 1226–1240. [Google Scholar] [CrossRef]
- Li, J.; Zhang, Y.; Jilg, A.L.; Wolk, D.M.; Khara, H.S.; Kolinovsky, A.; Rolston, D.D.K.; Hontecillas, R.; Bassaganya-Riera, J.; Williams, M.S.; et al. Variants at the MHC Region Associate with Susceptibility to Clostridioides difficile Infection: A Genome-Wide Association Study Using Comprehensive Electronic Health Records. Front. Immunol. 2021, 12, 638913. [Google Scholar] [CrossRef]
- Williams, J.S.; Walker, R.J.; Egede, L.E. Achieving Equity in an Evolving Healthcare System: Opportunities and Challenges. Am. J. Med. Sci. 2016, 351, 33–43. [Google Scholar] [CrossRef]
- Duncan, L.; Shen, H.; Gelaye, B.; Meijsen, J.; Ressler, K.; Feldman, M.; Peterson, R.; Domingue, B. Analysis of polygenic risk score usage and performance in diverse human populations. Nat. Commun. 2019, 10, 3328. [Google Scholar] [CrossRef]
- Martin, A.R.; Kanai, M.; Kamatani, Y.; Okada, Y.; Neale, B.M.; Daly, M.J. Clinical use of current polygenic risk scores may exacerbate health disparities. Nat. Genet. 2019, 51, 584–591. [Google Scholar] [CrossRef]
- Mudd-Martin, G.; Cirino, A.L.; Barcelona, V.; Fox, K.; Hudson, M.; Sun, Y.V.; Taylor, J.Y.; Cameron, V.A.; on behalf of the American Heart Association Council on Genomic and Precision Medicine; Council on Cardiovascular and Stroke Nursing; et al. Considerations for Cardiovascular Genetic and Genomic Research with Marginalized Racial and Ethnic Groups and Indigenous Peoples: A Scientific Statement from the American Heart Association. Circ. Genom. Precis. Med. 2021, 14, e000084. [Google Scholar] [CrossRef]
- Mars, N.; Koskela, J.T.; Ripatti, P.; Kiiskinen, T.T.J.; Havulinna, A.S.; Lindbohm, J.V.; Ahola-Olli, A.; Kurki, M.; Karjalainen, J.; Palta, P.; et al. Polygenic and clinical risk scores and their impact on age at onset and prediction of cardiometabolic diseases and common cancers. Nat. Med. 2020, 26, 549–557. [Google Scholar] [CrossRef]
- Vuckovic, D.; Bao, E.L.; Akbari, P.; Lareau, C.A.; Mousas, A.; Jiang, T.; Chen, M.H.; Raffield, L.M.; Tardaguila, M.; Huffman, J.E.; et al. The Polygenic and Monogenic Basis of Blood Traits and Diseases. Cell 2020, 182, 1214–1231.e1211. [Google Scholar] [CrossRef] [PubMed]
- Wray, N.R.; Wijmenga, C.; Sullivan, P.F.; Yang, J.; Visscher, P.M. Common Disease Is More Complex Than Implied by the Core Gene Omnigenic Model. Cell 2018, 173, 1573–1580. [Google Scholar] [CrossRef] [PubMed]
- Giudicessi, J.R.; Ackerman, M.J. Determinants of incomplete penetrance and variable expressivity in heritable cardiac arrhythmia syndromes. Transl. Res. 2013, 161, 1–14. [Google Scholar] [CrossRef] [PubMed]



| SNP | Locus | Gene | Phenotype | p-Value | Reference |
|---|---|---|---|---|---|
| rs2230500 | 14q22-q23 | PRKCH | Lacunar infarct | 5.1 × 10−7 | [67] |
| rs2230500 | 14q22-q23 | PRKCH | ICH | 5.4 × 10−3 | [68] |
| rs4646994 | 17q23 | ACE | WMH | NA | [69] |
| rs1055129 | 17q25 | TRIM47 | WMH | 4.1 × 10−8 | [70] |
| rs3744028 | 17q25 | TRIM65 | WMH | 4.0 × 10−9 | |
| rs4646994 | 17q23 | ACE | Lacunar infarct | 6.0 × 10−3 | [36] |
| rs2984613 | 1q22 | PMF1 SLC25A44 | Non-lobar ICH | 1.6 × 10−8 | [71] |
| rs72848980 | 17q25.1 | NEURL1 | WMH | 2.7 × 10−19 | [72] |
| rs7894407 | 10q24.33 | PDCD11 | WMH | 2.7 × 10−19 | |
| rs12357919, rs7909791 | 10q24 | SH3PXD2A | WMH | 1.6 × 10−9 | |
| rs78857879 | 2p16.1 | EFEMP1 | WMH | 1.5 × 10−8 | [72] |
| rs11679640 | 2p21 | HAAO | WMH | 4.4 × 10−8 | |
| rs72934505 | 2q33.2 | NBEAL1 | WMH | 2.2 × 10−8 | [73] |
| rs941898 | 14q32.2 | EVL | WMH | 4.0 × 10−8 | |
| rs962888 | 17q21.31 | C1QL1 | WMH | 1.1 × 10−8 | |
| rs9515201 | 13q34 | COL4A2 | WMH | 6.9 × 10−9 | |
| rs10744777 | 12 | ALDH2 | Small artery stroke | 2.92 × 10−9 | [74] |
| rs12204590 | 6p25 | FOXF2 | WMH | 2.17 × 10−6 | [17] |
| rs12445022 | 16q24 | ZCCHC14 | WMH | 5.3 × 10−5 | [75] |
| rs13164785, rs67827860 | 5q14.3 | VCAN | MD, FA | 3.7 × 10−18 1.3 × 10−14 | [76] |
| rs275350 | 6q25.1 | PLEKHG1 | WMH | 1.6 × 10−8 | [77] |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Li, J.; Abedi, V.; Zand, R. Dissecting Polygenic Etiology of Ischemic Stroke in the Era of Precision Medicine. J. Clin. Med. 2022, 11, 5980. https://doi.org/10.3390/jcm11205980
Li J, Abedi V, Zand R. Dissecting Polygenic Etiology of Ischemic Stroke in the Era of Precision Medicine. Journal of Clinical Medicine. 2022; 11(20):5980. https://doi.org/10.3390/jcm11205980
Chicago/Turabian StyleLi, Jiang, Vida Abedi, and Ramin Zand. 2022. "Dissecting Polygenic Etiology of Ischemic Stroke in the Era of Precision Medicine" Journal of Clinical Medicine 11, no. 20: 5980. https://doi.org/10.3390/jcm11205980
APA StyleLi, J., Abedi, V., & Zand, R. (2022). Dissecting Polygenic Etiology of Ischemic Stroke in the Era of Precision Medicine. Journal of Clinical Medicine, 11(20), 5980. https://doi.org/10.3390/jcm11205980








