Prevalence and Predictors of Food Insecurity among Adults with Type 1 Diabetes: Observational Findings from the 2022 Behavioral Risk Factor Surveillance System
Abstract
1. Introduction
2. Materials and Methods
2.1. Measures
2.2. Statistical Analysis
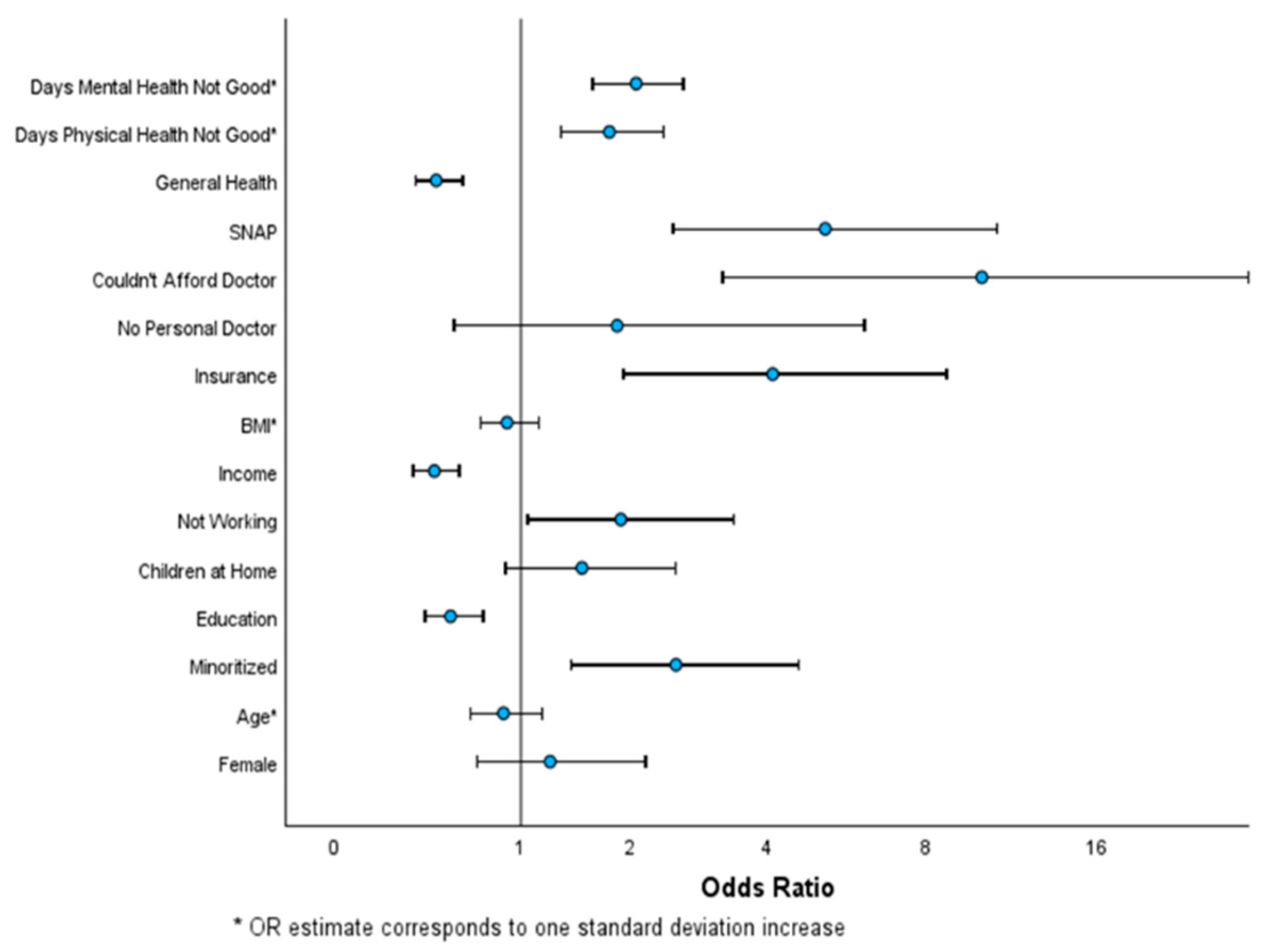
3. Results
4. Discussion
4.1. Limitations
4.2. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Data Availability Statement
Conflicts of Interest
References
- American Diabetes Association. Available online: https://diabetes.org/about-diabetes/statistics/about-diabetes (accessed on 13 May 2024).
- Anderson, S.E. Core indicators of nutritional state for difficult-to-sample populations. J. Nutr. 1990, 120, 1557–1660. [Google Scholar] [CrossRef] [PubMed]
- Mendoza, J.A.; Haaland, W.; D’Agostino, R.B.; Martini, L.; Pihoker, C.; Frongillo, E.A.; Mayer-Davis, E.J.; Liu, L.L.; Dabelea, D.; Lawrence, J.M.; et al. Food insecurity is associated with high risk glycemic control and higher health care utilization among youth and young adults with type 1 diabetes. Diabetes Res. Clin. Pract. 2018, 138, 128–137. [Google Scholar] [CrossRef] [PubMed]
- Malik, F.S.; Liese, A.D.; Ellyson, A.; Reid, L.A.; Reboussin, B.A.; Sauder, K.A.; Frongillo, E.A.; Pihoker, C.; Dabelea, D.; Reynolds, K.; et al. Household food insecurity and associations with hemoglobin A(1c) and acute diabetes-related complications in youth and young adults with type 1 diabetes: The SEARCH for diabetes in youth study. Diabetes Res. Clin. Pract. 2024, 212, 111608. [Google Scholar] [CrossRef] [PubMed]
- Ratzki-Leewing, A.A.; Black, J.E.; Ryan, B.L.; Zou, G.; Klar, N.; Webster-Bogaert, S.; Timcevska, K.; Harris, S.B. Development and validation of a real-world model to predict 1-year Level 3 (severe) hypoglycaemia risk in adults with diabetes (the iNPHORM study, United States). Diabetes Obes. Metab. 2023, 25, 2910–2927. [Google Scholar] [CrossRef] [PubMed]
- Eitel, K.B.; Roberts, A.J.; D’Agostino, R., Jr.; Barrett, C.E.; Bell, R.A.; Bellatorre, A.; Cristello, A.; Dabelea, D.; Dolan, L.M.; Jensen, E.T.; et al. Diabetes stigma and psychosocial outcomes in adolescents and young adults: The SEARCH for diabetes in youth study. Diabetes Care 2024, 47, 290–294. [Google Scholar] [CrossRef] [PubMed]
- Reid, L.A.; Zheng, S.; Mendoza, J.A.; Reboussin, B.A.; Roberts, A.J.; Sauder, K.A.; Lawrence, J.M.; Jensen, E.; Henkin, L.; Flory, K.; et al. Household food insecurity and fear of hypoglycemia in adolescents and young adults with diabetes and parents of youth with diabetes. Diabetes Care 2023, 46, 262–269. [Google Scholar] [CrossRef] [PubMed]
- Centers for Disease Control and Prevention. Available online: https://www.cdc.gov/brfss/questionnaires/modules/category2022.htm (accessed on 22 July 2024).
- Cohen, A.J.; Dosa, D.M.; Rudolph, J.L.; Halladay, C.W.; Heisler, M.; Thomas, K.S. Risk factors for Veteran food insecurity: Findings from a national US Department of Veterans Affairs Food Insecurity Screener. Public Health Nutr. 2022, 25, 819–828. [Google Scholar] [CrossRef] [PubMed]
- Bickel, G.M.N.C.P.W.H.; John, C. Guide to Measuring Household Food Security, Revised 2000; U.S. Department of Agriculture, Food and Nutrition Service: Alexandria, VA, USA, 2000.
- Cook, J.T.; Black, M.; Chilton, M.; Cutts, D.; Ettinger de Cuba, S.; Heeren, T.C.; Rose-Jacobs, R.; Sandel, M.; Casey, P.H.; Coleman, S.; et al. Are food insecurity’s health impacts underestimated in the U.S. population? Marginal food security also predicts adverse health outcomes in young U.S. children and mothers. Adv. Nutr. 2013, 4, 51–61. [Google Scholar] [CrossRef] [PubMed]
- Bermúdez-Millán, A.; Damio, G.; Cruz, J.; D’Angelo, K.; Segura-Pérez, S.; Hromi-Fiedler, A.; Pérez-Escamilla, R. Stress and the social determinants of maternal health among Puerto Rican women: A CBPR approach. J. Health Care Poor Underserved 2011, 22, 1315–1330. [Google Scholar] [CrossRef] [PubMed]
- Liese, A.D.; Brown, A.D.; Frongillo, E.A.; Julceus, E.F.; Sauder, K.A.; Reboussin, B.A.; Bellatorre, A.; Dolan, L.M.; Reynolds, K.; Pihoker, C.; et al. Properties of the Household Food Security Survey Module scale in young adults with diabetes. J. Nutr. 2024, 154, 1050–1057. [Google Scholar] [CrossRef] [PubMed]
- Essien, U.R.; Shahid, N.N.; Berkowitz, S.A. Food insecurity and diabetes in developed societies. Curr. Diab Rep. 2016, 16, 79. [Google Scholar] [CrossRef] [PubMed]
- Drown, L.; Adler, A.J.; Schwartz, L.N.; Sichali, J.; Valeta, F.; Boudreaux, C.; Trujillo, C.; Ruderman, T.; Bukhman, G. Living with type 1 diabetes in Neno, Malawi: A qualitative study of self-management and experiences in care. BMC Health Serv. Res. 2023, 23, 595. [Google Scholar] [CrossRef] [PubMed]
- Adler, A.J.; Trujillo, C.; Schwartz, L.; Drown, L.; Pierre, J.; Noble, C.; Allison, T.; Cook, R.; Randolph, C.; Bukhman, G. Experience of living with type 1 diabetes in a low-income country: A qualitative study from Liberia. BMJ Open 2021, 11, e049738. [Google Scholar] [CrossRef] [PubMed]
- Carruth, L.; Mendenhall, E. “Wasting away”: Diabetes, food insecurity, and medical insecurity in the Somali Region of Ethiopia. Soc. Sci. Med. 2019, 228, 155–163. [Google Scholar] [CrossRef] [PubMed]
- Khan, Y.; Albache, N.; Almasri, I.; Gabbay, R.A. The management of diabetes in conflict settings: Focus on the Syrian crisis. Diabetes Spectr. 2019, 32, 264–269. [Google Scholar] [CrossRef] [PubMed]
- Hilliard, M.E.; Yi-Frazier, J.P.; Hessler, D.; Butler, A.M.; Anderson, B.J.; Jaser, S. Stress and A1c among people with diabetes across the lifespan. Curr. Diab Rep. 2016, 16, 67. [Google Scholar] [CrossRef]
- Keith-Jennings, B. Introduction to Puerto Rico’s Nutrition Assistance Program; Center on Budget and Policy Priorities: Washington, DC, USA, 2020. [Google Scholar]
- Cumba-Avilés, E.; Sáez-Santiago, E. Research program on type 1 diabetes and youth depression in Puerto Rico. Rev. Puertorriquena Psicol. 2016, 27, 44–60. [Google Scholar]
| Demographic | Unweighted Count | Weighted Percentage | Percentage with Positive Screen for FI | Odds Ratio | 95% CI | p-Value |
|---|---|---|---|---|---|---|
| Sex | ||||||
| Female | 226 | 45.3 | 28.5 | 1.23 | 0.70–2.18 | 0.473 |
| Male | 243 | 54.7 | 24.5 | reference | ||
| Age | ||||||
| Mean ± SE, Coefficient B | 49.4 ± 1.3 | B = −0.008 | 0.99 | 0.98–1.01 | 0.360 | |
| Race | ||||||
| Minoritized * | 88 | 26.0 | 44.1 | 2.56 | 1.41–4.62 | 0.002 |
| White/Non-Hispanic | 364 | 74.0 | 21.8 | reference | ||
| Education | ||||||
| Less than high school | 38 | 12.7 | 49.1 | 8.05 | 2.85–22.71 | <0.001 |
| High school | 115 | 26.2 | 32.0 | 3.93 | 1.77–8.72 | |
| Attended college | 136 | 33.4 | 26.4 | 2.99 | 1.18–7.59 | |
| Graduated college | 178 | 27.1 | 10.7 | reference | ||
| DK/Refused | 2 | 0.6 | ||||
| Linear Predictor Coefficient B ^ | B = −0.615 | 0.54 | 0.40–0.74 | <0.001 | ||
| Children in Household | ||||||
| Children | 99 | 27.2 | 32.4 | 1.51 | 0.89–2.56 | 0.125 |
| No children | 368 | 72.8 | 24.1 | reference | ||
| Employment | ||||||
| Not working | 286 | 52.4 | 32.3 | 1.90 | 1.05–3.42 | 0.033 |
| Working | 181 | 46.9 | 20.1 | reference | ||
| Refused | 2 | 0.7 | ||||
| Income | ||||||
| <25 k | 96 | 20.6 | 46.7 | 23.78 | 2.95–191.53 | <0.001 |
| 25–50 k | 98 | 17.4 | 43.4 | 20.81 | 2.55–169.9 | |
| 50–100 k | 127 | 28.3 | 23.2 | 8.19 | 0.90–74.37 | |
| 100–200 k | 57 | 13.4 | 0.5 | 0.14 | 0.0–74.37 | |
| >200 k | 18 | 5.8 | 3.6 | reference | ||
| DK/Refused | 73 | 14.5 | ||||
| Linear Predictor Coefficient B ^ | B = −0.797 | 0.45 | 0.34–0.59 | <0.001 | ||
| Health Insurance | ||||||
| Government | 261 | 45.8 | 40.0 | 4.10 | 1.93–8.73 | 0.001 |
| None | 10 | 2.7 | 28.5 | 2.45 | 0.30–20.41 | |
| Private | 188 | 47.8 | 14.0 | reference | ||
| DK/Refused | 10 | 3.6 | ||||
| Received SNAP | ||||||
| Yes | 57 | 11.2 | 59.9 | 5.20 | 2.52–10.73 | <0.001 |
| No | 408 | 88.0 | 22.3 | reference | ||
| DK/Refused | 4 | 0.8 | ||||
| Have Personal Doctor | ||||||
| No | 17 | 4.5 | 39.2 | 1.86 | 0.56–6.17 | 0.313 |
| Yes | 449 | 95.1 | 25.8 | reference | ||
| DK/Refused | 3 | 0.3 | ||||
| Couldn’t Afford to See Doctor | ||||||
| Yes | 35 | 9.7 | 73.1 | 10.10 | 3.23–31.63 | <0.001 |
| No | 431 | 90.2 | 21.2 | reference | ||
| DK/Refused | 3 | 0.1 | ||||
| General Health | ||||||
| Poor | 65 | 13.6 | 56.3 | 16.78 | 2.77–101.83 | <0.001 |
| Fair | 117 | 25.4 | 31.7 | 6.05 | 1.03–35.41 | |
| Good | 177 | 38.6 | 22.1 | 3.68 | 0.58–23.57 | |
| Very good | 95 | 19.3 | 8.3 | 1.18 | 0.17–8.33 | |
| Excellent | 14 | 2.9 | 7.1 | reference | ||
| DK/Refused | 1 | 0.3 | <0.001 | |||
| Linear Predictor Coefficient B ^ | B = −0.779 | 0.46 | 0.35–0.61 | |||
| Days Physical Health Not Good | ||||||
| Mean ± SE, Coefficient B | 7.9 ± 0.7 | B = 0.046 | 1.05 | 1.01–1.08 | 0.008 | |
| Days Mental Health Not Good | ||||||
| Mean ± SE, Coefficient B | 6.6 ± 0.6 | B = 0.069 | 1.07 | 1.04–1.11 | <0.001 | |
| BMI | ||||||
| Underweight | 7 | 1.3 | 35.2 | 1.21 | 0.17–8.32 | 0.599 |
| Normal | 134 | 31.2 | 31 | reference | ||
| Overweight | 156 | 35.1 | 22.3 | 0.64 | 0.32–1.28 | |
| Obese | 156 | 32.3 | 25.8 | 0.77 | 0.39–1.55 | |
| Mean ± SE | 29.2 ± 0.6 | |||||
| Linear Predictor Coefficient B ^ | B = −0.139 | 0.870 | 0.62–1.22 | 0.413 |
| Demographic | Odds Ratio | 95% CI | p-Value |
|---|---|---|---|
| Age | |||
| One year increase | 0.98 | 0.95–1.00 | 0.019 |
| Income | |||
| One category increase | 0.57 | 0.43–0.77 | <0.001 |
| Health Insurance | |||
| Government | 5.25 | 2.07–13.30 | 0.003 |
| None | 3.34 | 0.37–30.39 | |
| Private | reference | ||
| Couldn’t Afford to See Doctor | |||
| Yes | 11.21 | 3.11–40.42 | <0.001 |
| No | reference | ||
| Days Mental Health Not Good | |||
| One day increase | 1.05 | 1.02–1.09 | <0.001 |
| Fit Statistics | |||
| Nagelkerke R-square | 0.447 | ||
| Correct Classification | |||
| Food Secure | 86.9% | ||
| Food Insecure | 34.0% | ||
| Overall | 72.0% |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Wagner, J.A.; Bermúdez-Millán, A.; Feinn, R.S. Prevalence and Predictors of Food Insecurity among Adults with Type 1 Diabetes: Observational Findings from the 2022 Behavioral Risk Factor Surveillance System. Nutrients 2024, 16, 2406. https://doi.org/10.3390/nu16152406
Wagner JA, Bermúdez-Millán A, Feinn RS. Prevalence and Predictors of Food Insecurity among Adults with Type 1 Diabetes: Observational Findings from the 2022 Behavioral Risk Factor Surveillance System. Nutrients. 2024; 16(15):2406. https://doi.org/10.3390/nu16152406
Chicago/Turabian StyleWagner, Julie Ann, Angela Bermúdez-Millán, and Richard S. Feinn. 2024. "Prevalence and Predictors of Food Insecurity among Adults with Type 1 Diabetes: Observational Findings from the 2022 Behavioral Risk Factor Surveillance System" Nutrients 16, no. 15: 2406. https://doi.org/10.3390/nu16152406
APA StyleWagner, J. A., Bermúdez-Millán, A., & Feinn, R. S. (2024). Prevalence and Predictors of Food Insecurity among Adults with Type 1 Diabetes: Observational Findings from the 2022 Behavioral Risk Factor Surveillance System. Nutrients, 16(15), 2406. https://doi.org/10.3390/nu16152406





