Association Between SGLT2 Inhibitor Therapy and the Incidence of Tinnitus in Patients with Type 2 Diabetes: A Retrospective Cohort Study
Abstract
1. Introduction
2. Material and Methods
2.1. Data Source
2.2. Statistical Analyses
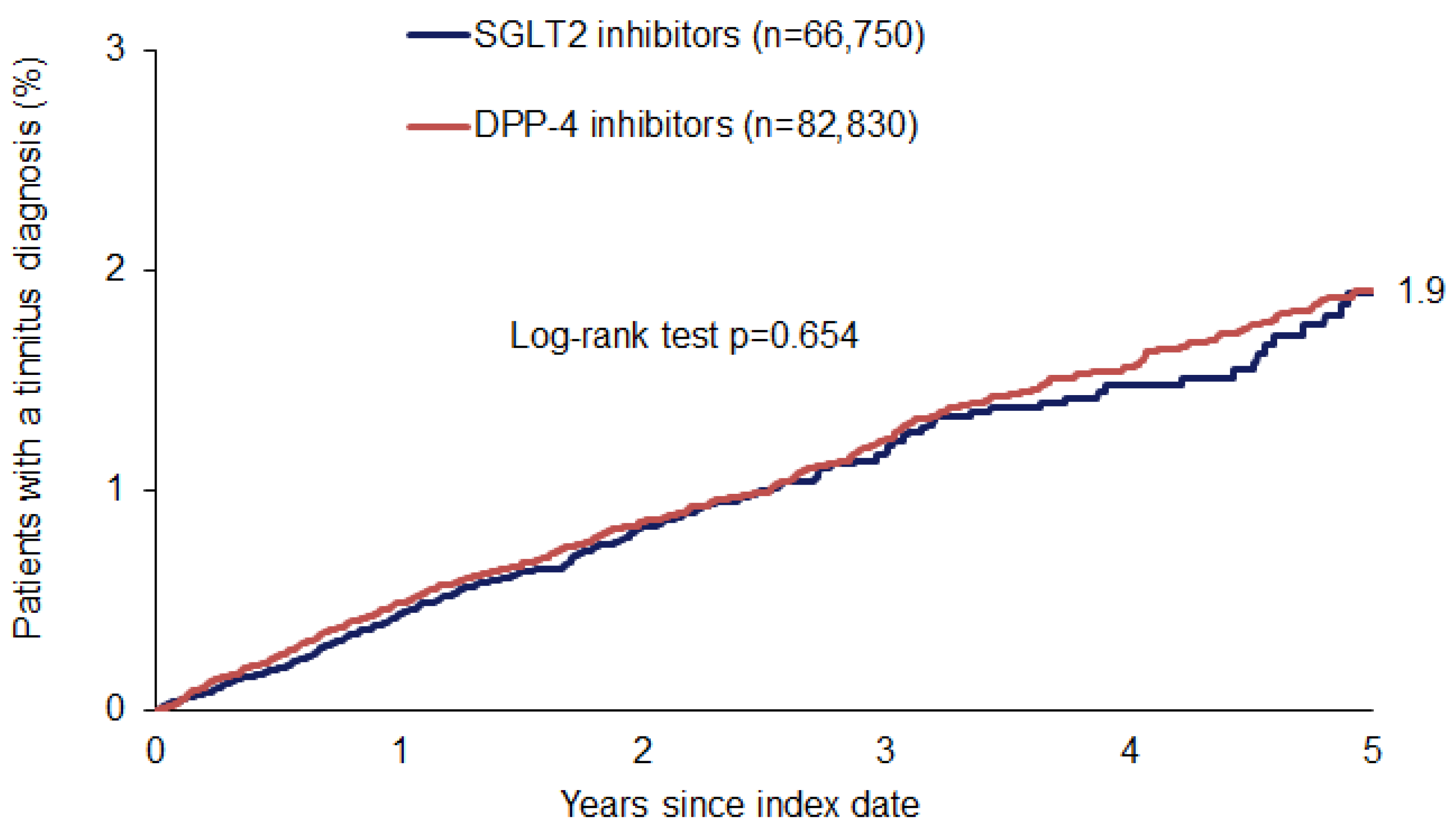
3. Results
4. Discussion
4.1. Considerations Regarding the Study Design
4.2. Tinnitus Incidence and Demografic Data
4.3. Possible Confounders
4.4. Interpretation of the Results
4.5. Strengths and Limitations of the Study
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Jarach, C.M.; Lugo, A.; Scala, M.; van den Brandt, P.A.; Cederroth, C.R.; Odone, A.; Garavello, W.; Schlee, W.; Langguth, B.; Gallus, S. Global Prevalence and Incidence of Tinnitus: A Systematic Review and Meta-analysis. JAMA Neurol. 2022, 79, 888–900. [Google Scholar] [CrossRef]
- Tan, C.J.W.; Koh, J.W.T.; Tan, B.K.J.; Woon, C.Y.; Teo, Y.H.; Ng, L.S.; Loh, W.S. Association Between Hearing Loss and Cardiovascular Disease: A Meta-analysis. Otolaryngol.-Head Neck Surg. 2024, 170, 694–707. [Google Scholar] [CrossRef]
- Zhang, Y.P.; Gao, Q.Y.; Gao, J.W.; Liang, X.T.; Guo, D.C.; Chen, Z.T.; Wang, J.F.; Tang, D.M.; Zhang, H.F. The association between tinnitus and risk of cardiovascular events and all-cause mortality: Insight from the UK Biobank. Acta Cardiol. 2024, 79, 374–382. [Google Scholar] [CrossRef]
- Jiang, Y.; Liu, Q.; Ding, Y.; Sun, Y. Systematic review and meta-analysis of the correlation between tinnitus and mental health. Am. J. Otolaryngol.-Head Neck Med. Surg. 2025, 46, 104611. [Google Scholar] [CrossRef] [PubMed]
- Patel, S.D.; Patel, S.; Finberg, A.; Shah, V.N.; Mittal, R.; Eshraghi, A.A. Association between Tinnitus and Hypertension: A Cross-Sectional Analysis of the National Health and Nutrition Examination Survey. Otol. Neurotol. 2022, 43, 766–772. [Google Scholar] [CrossRef] [PubMed]
- Yüksel, F.; Karataş, D.; Türkdoğan, F.T.; Yüksel, Ö. Increased Atherosclerosis Correlates with Subjective Tinnitus Severity. Indian J. Otolaryngol. Head Neck Surg. 2018, 70, 119–124. [Google Scholar] [CrossRef] [PubMed]
- Lee, H.J.; Lee, D.C.; Kim, C.O. The Association between Serum Lipid Levels and Tinnitus Prevalence and Severity in Korean Elderly: A Nationwide Population-Based Cross-Sectional Study. Yonsei Med. J. 2024, 65, 156. [Google Scholar] [CrossRef]
- Kostev, K.; Alymova, S.; Kössl, M.; Jacob, L. Risk Factors for Tinnitus in 37,692 Patients Followed in General Practices in Germany. Otol. Neurotol. 2019, 40, 436–440. [Google Scholar] [CrossRef]
- Biswas, R.; Genitsaridi, E.; Trpchevska, N.; Lugo, A.; Schlee, W.; Cederroth, C.R.; Gallus, S.; Hall, D.A. Low Evidence for Tinnitus Risk Factors: A Systematic Review and Meta-analysis. JARO-J. Assoc. Res. Otolaryngol. 2023, 24, 81–94. [Google Scholar] [CrossRef]
- Gupta, S.; Eavey, R.D.; Wang, M.; Curhan, S.G.; Curhan, G.C. Type 2 diabetes and the risk of incident hearing loss. Diabetologia 2019, 62, 281–285. [Google Scholar] [CrossRef]
- Kakarlapudi, V.; Sawyer, R.; Staecker, H. The effect of diabetes on sensorineural hearing loss. Otol. Neurotol. 2003, 24, 382–386. [Google Scholar] [CrossRef]
- Verma, S.; McMurray, J.J. SGLT2 inhibitors and mechanisms of cardiovascular benefit: A state-of-the-art review. Diabetologia 2018, 61, 2108–2117. [Google Scholar] [CrossRef]
- Drake, T.; Landsteiner, A.; Langsetmo, L.; MacDonald, R.; Anthony, M.; Kalinowski, C.; Ullman, K.; Billington, C.J.; Kaka, A.; Sultan, S.; et al. Newer Pharmacologic Treatments in Adults with Type 2 Diabetes: A Systematic Review and Network Meta-analysis for the American College of Physicians. Ann. Intern. Med. 2024, 177, 618–632. [Google Scholar] [CrossRef]
- Neuen, B.L.; Young, T.; Heerspink, H.J.; Neal, B.; Perkovic, V.; Billot, L.; Mahaffey, K.W.; Charytan, D.M.; Wheeler, D.C.; Arnott, C.; et al. SGLT2 inhibitors for the prevention of kidney failure in patients with type 2 diabetes: A systematic review and meta-analysis. Lancet Diabetes Endocrinol. 2019, 7, 845–854. [Google Scholar] [CrossRef]
- Rieg, T.; Liu, R.; Staruschenko, A. Gliflozins in Hypertension: Basic Mechanisms and Clinical Insights. Am. J. Physiol.-Ren. Physiol. 2025, 329, F32–F45. [Google Scholar] [CrossRef]
- Rathmann, W.; Bongaerts, B.; Carius, H.J.; Kruppert, S.; Kostev, K. Basic characteristics and representativeness of the German Disease Analyzer database. Int. J. Clin. Pharmacol. Ther. 2018, 56, 459–466. [Google Scholar] [CrossRef] [PubMed]
- Hare, D.L.; Toukhsati, S.R.; Johansson, P.; Jaarsma, T. Depression and cardiovascular disease: A clinical review. Eur. Heart J. 2014, 35, 1365–1372. [Google Scholar] [CrossRef] [PubMed]
- Oussoren, F.K.; Poulsen, L.N.; Kardux, J.J.; Schermer, T.R.; Bruintjes, T.D.; van Leeuwen, R.B. Cerebral Small Vessel Disease in Elderly Patients with Vestibular Neuritis. Front. Neurol. 2022, 13, 818533. [Google Scholar] [CrossRef]
- Pâris, P.; Charpiot, A.; Veillon, F.; Severac, F.; Djennaoui, I. Prevalence of cardiovascular risk factors in superior vestibular neuritis: A cross-sectional study following STROBE guidelines. Eur. Ann. Otorhinolaryngol. Head Neck Dis. 2022, 139, 194–197. [Google Scholar] [CrossRef] [PubMed]
- Oron, Y.; Shemesh, S.; Shushan, S.; Cinamon, U.; Goldfarb, A.; Dabby, R.; Ovnat Tamir, S. Cardiovascular Risk Factors among Patients with Vestibular Neuritis. Ann. Otol. Rhinol. Laryngol. 2017, 126, 597–601. [Google Scholar] [CrossRef]
- Coronel-Touma, G.S.; Monopoli-Roca, C.; Almeida-Ayerve, C.N.; Marcos-Alonso, S.; Gómez de la Torre-Morales, D.; Serradilla-López, J.; Cruz-Ruiz, S.S.; Batuecas-Caletrío, Á.; Sánchez-Gómez, H. Influence of Age and Cardiovascular Risk Factors in Vestibular Neuritis: Retrospective Cohort Study. J. Clin. Med. 2023, 12, 6544. [Google Scholar] [CrossRef] [PubMed]
- Zannad, F.; Ferreira, J.P.; Pocock, S.J.; Anker, S.D.; Butler, J.; Filippatos, G.; Brueckmann, M.; Ofstad, A.P.; Pfarr, E.; Jamal, W.; et al. SGLT2 inhibitors in patients with heart failure with reduced ejection fraction: A meta-analysis of the EMPEROR-Reduced and DAPA-HF trials. Lancet 2020, 396, 819–829. [Google Scholar] [CrossRef]
- Siao, W.Z.; Lin, T.K.; Huang, J.Y.; Tsai, C.F.; Jong, G.P. The association between sodium-glucose cotransporter 2 inhibitors and incident dementia: A nationwide population-based longitudinal cohort study. Diabetes Vasc. Dis. Res. 2022, 19, 14791641221098168. [Google Scholar] [CrossRef] [PubMed]
- Hu, J.C.; Shao, S.C.; Hsiang-Te Tsai, D.; Chuang, A.T.M.; Liu, K.H.; Lai, E.C.C. Use of SGLT2 Inhibitors vs GLP-1 RAs and Anemia in Patients with Diabetes and CKD. JAMA Netw. Open 2024, 7, e240946. [Google Scholar] [CrossRef] [PubMed]

| Variable | SGLT2 Patients | DPP4 Patients | p Values |
| Number of patients | 66,750 | 82,830 | |
| Age mean (SD) | 68.4 (13.3) | 68.1 (13.0) | <0.001 |
| ≤60 years | 18,515 (27.7) | 23,469 (28.4) | <0.001 |
| 61–70 years | 17,388 (26.1) | 21,546 (26.0) | |
| 71–80 years | 16,305 (24.4) | 21,480 (25.9) | |
| >80 years | 14,542 (21.8) | 16,335 (19.7) | |
| Sex: female | 25,749 (45.7) | 37,837 (38.6) | <0.001 |
| Sex: male | 41,001 (54.3) | 44,993 (61.4) | |
| Start of therapy: 2016–2018 | 8164 (12.2) | 33,317 (40.2) | <0.001 |
| Start of therapy: 2019–2021 | 18,486 (27.7) | 32,840 (39.7) | |
| Start of therapy: 2022–2023 | 40,100 (60.1) | 16,673 (20.1) | |
| Disorders of vestibular function | 2359 (3.5) | 2025 (2.4) | <0.001 |
| All-cause hearing loss | 3728 (5.6) | 3438 (4.2) | <0.001 |
| Hypertension | 44,916 (67.3) | 49,097 (59.3) | <0.001 |
| Atherosclerosis | 5453 (8.2) | 4394 (5.3) | <0.001 |
| Dyslipidemia | 29,609 (44.4) | 29,584 (35.7) | <0.001 |
| COPD | 9500 (14.2) | 8403 (10.1) | <0.001 |
| Depression | 13,346 (20.0) | 13,800 (16.7) | <0.001 |
| HbA1c in % mean (SD) | 7.7 (1.7) | 7.9 (1.6) | <0.001 |
| Diabetes duration median (IQR) | 1.0 (5.2) | 1.0 (5.2) | <0.001 |
| Subgroup | Adjusted HR (95% CI) * | p Value |
| Total cohort | 1.04 (0.89–1.21) | 0.641 |
| Patients aged ≤60 years | 1.09 (0.86–1.39) | 0.479 |
| Patients 61–70 years | 1.05 (0.80–1.38) | 0.732 |
| Patients 71–80 years | 1.00 (0.69.–1.46) | 0.996 |
| Patients >80 years | 0.95 (0.58–1.58) | 0.086 |
| Female patients | 1.24 (0.97–1.59) | 0.087 |
| Male patients | 0.93 (0.76–1.13) | 0.439 |
| Start of therapy: 2016–2018 | 1.22 (0.95–1.58) | 0.125 |
| Start of therapy: 2019–2021 | 0.89 (0.70–1.14) | 0359 |
| Start of therapy: 2022–2023 | 0.99 (0.72–1.37) | 0.971 |
| Patients with hypertension | 0.99 (0.82–1.20) | 0.936 |
| Patients with atherosclerosis | 1.01 (0.54–1.90) | 0.969 |
| Patients with ischemic heart disease | 1.16 (0.85–1.59) | 0.356 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Seidel, D.U.; Bode, S.; Kostev, K. Association Between SGLT2 Inhibitor Therapy and the Incidence of Tinnitus in Patients with Type 2 Diabetes: A Retrospective Cohort Study. Audiol. Res. 2025, 15, 102. https://doi.org/10.3390/audiolres15040102
Seidel DU, Bode S, Kostev K. Association Between SGLT2 Inhibitor Therapy and the Incidence of Tinnitus in Patients with Type 2 Diabetes: A Retrospective Cohort Study. Audiology Research. 2025; 15(4):102. https://doi.org/10.3390/audiolres15040102
Chicago/Turabian StyleSeidel, David Ulrich, Simon Bode, and Karel Kostev. 2025. "Association Between SGLT2 Inhibitor Therapy and the Incidence of Tinnitus in Patients with Type 2 Diabetes: A Retrospective Cohort Study" Audiology Research 15, no. 4: 102. https://doi.org/10.3390/audiolres15040102
APA StyleSeidel, D. U., Bode, S., & Kostev, K. (2025). Association Between SGLT2 Inhibitor Therapy and the Incidence of Tinnitus in Patients with Type 2 Diabetes: A Retrospective Cohort Study. Audiology Research, 15(4), 102. https://doi.org/10.3390/audiolres15040102







