Pectin-Lyase-Modified Ginseng Extract and Ginsenoside Rd Inhibits High Glucose-Induced ROS Production in Mesangial Cells and Prevents Renal Dysfunction in db/db Mice
Abstract
1. Introduction
2. Results
2.1. GE-E3D and Ginsenoside Rd Alleviates ROS Generation in High-Glucose-Exposed MMCs
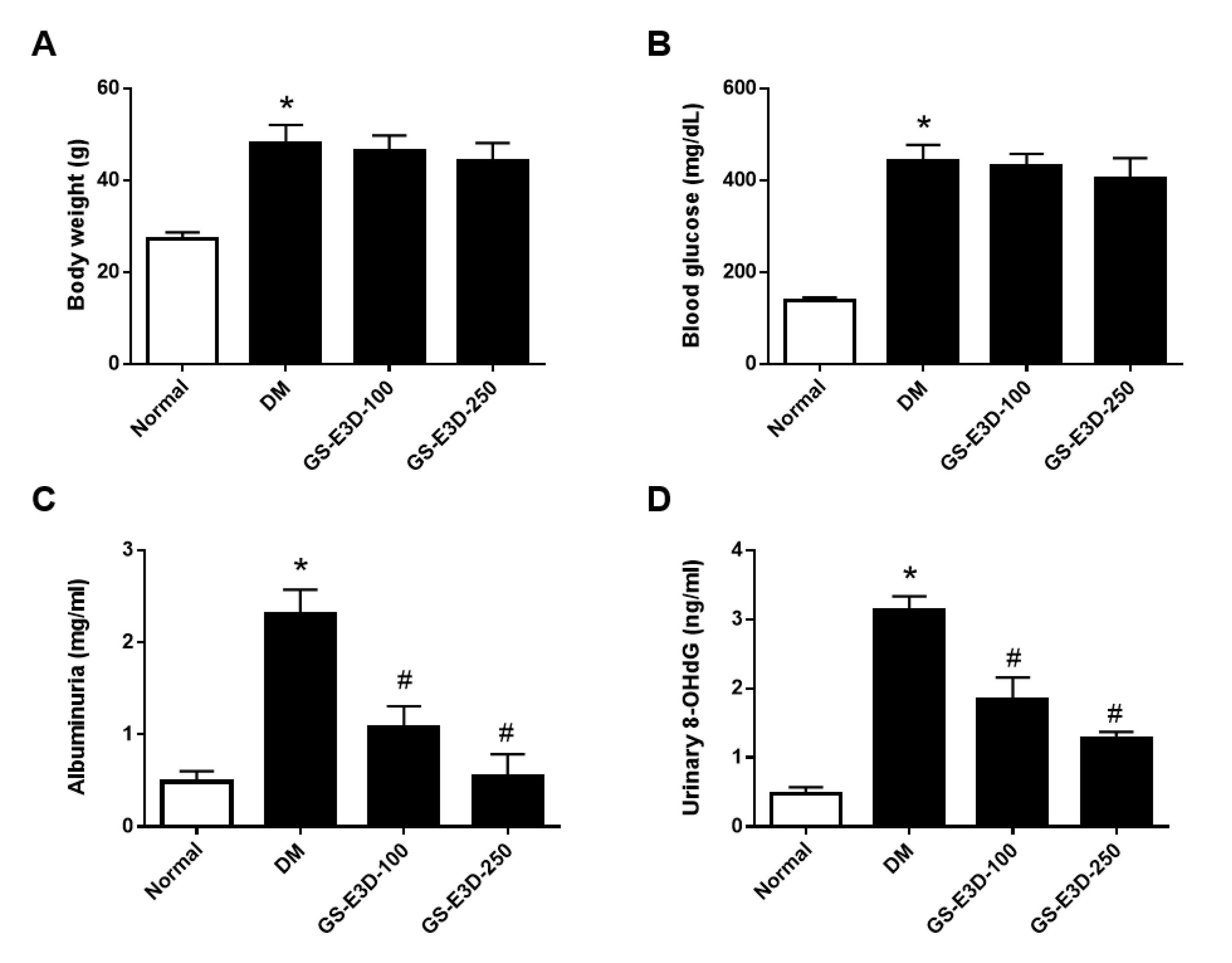
2.2. GS-E3D Improves Renal Dysfunction in Db/Db Mice
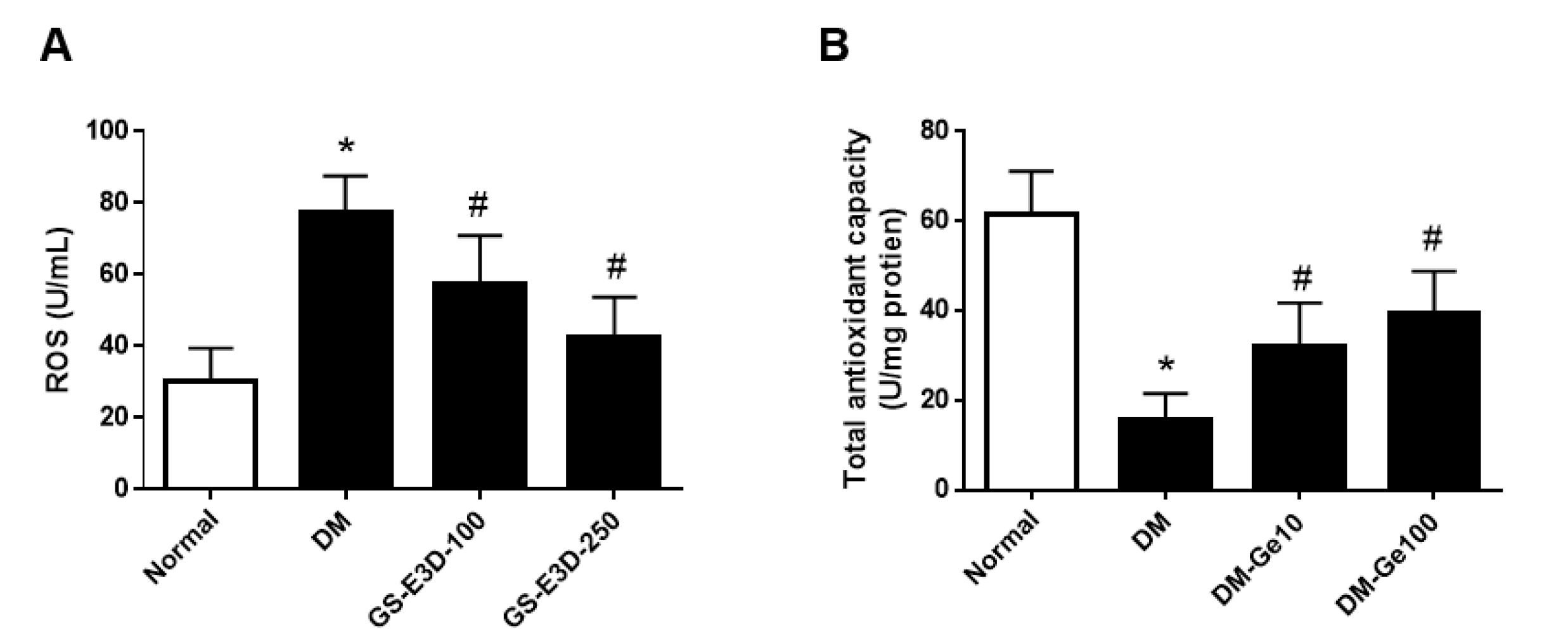
2.3. GS-E3D Decreased ROS Production in Renal Tissues in Db/Db Mice
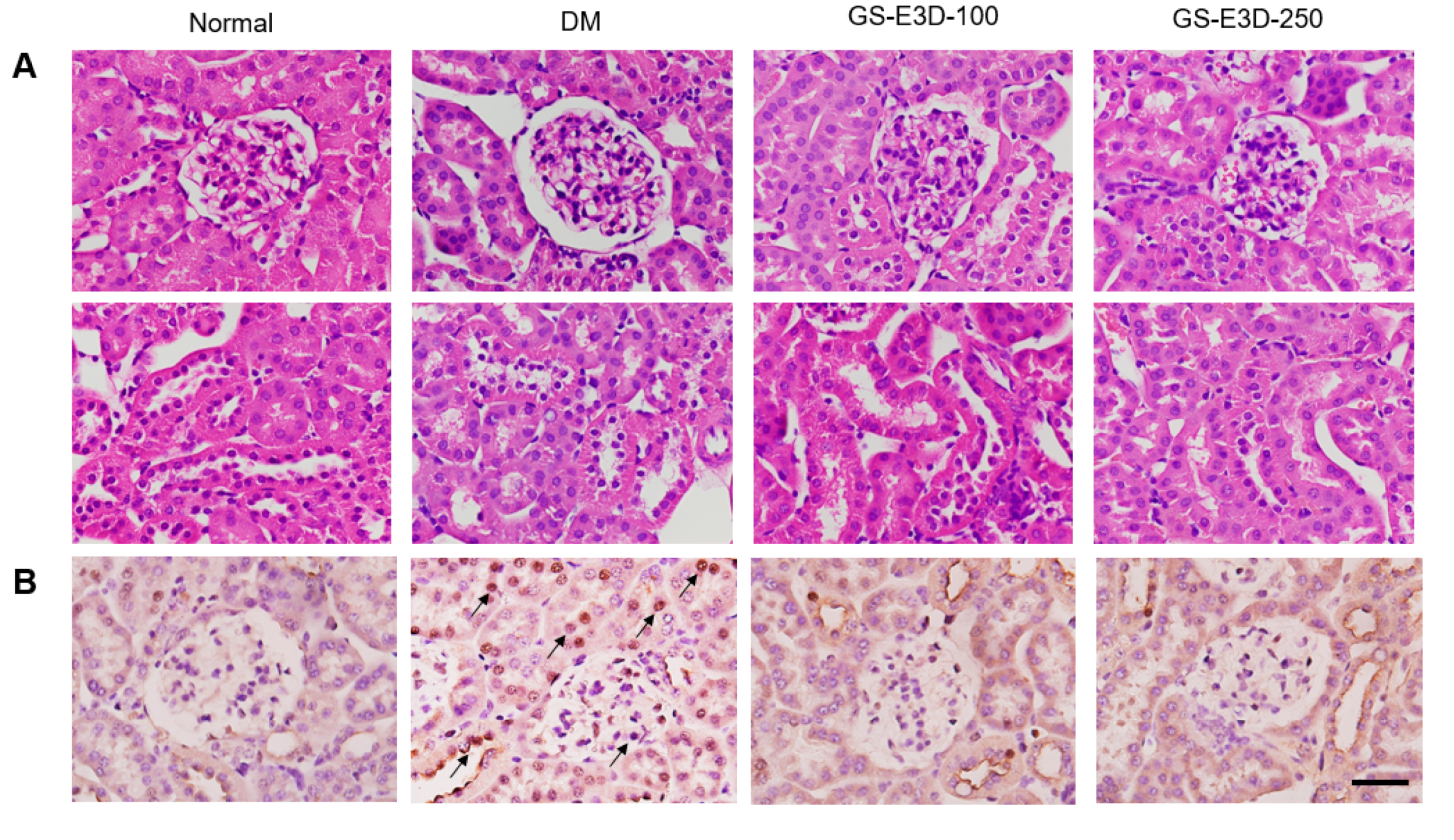
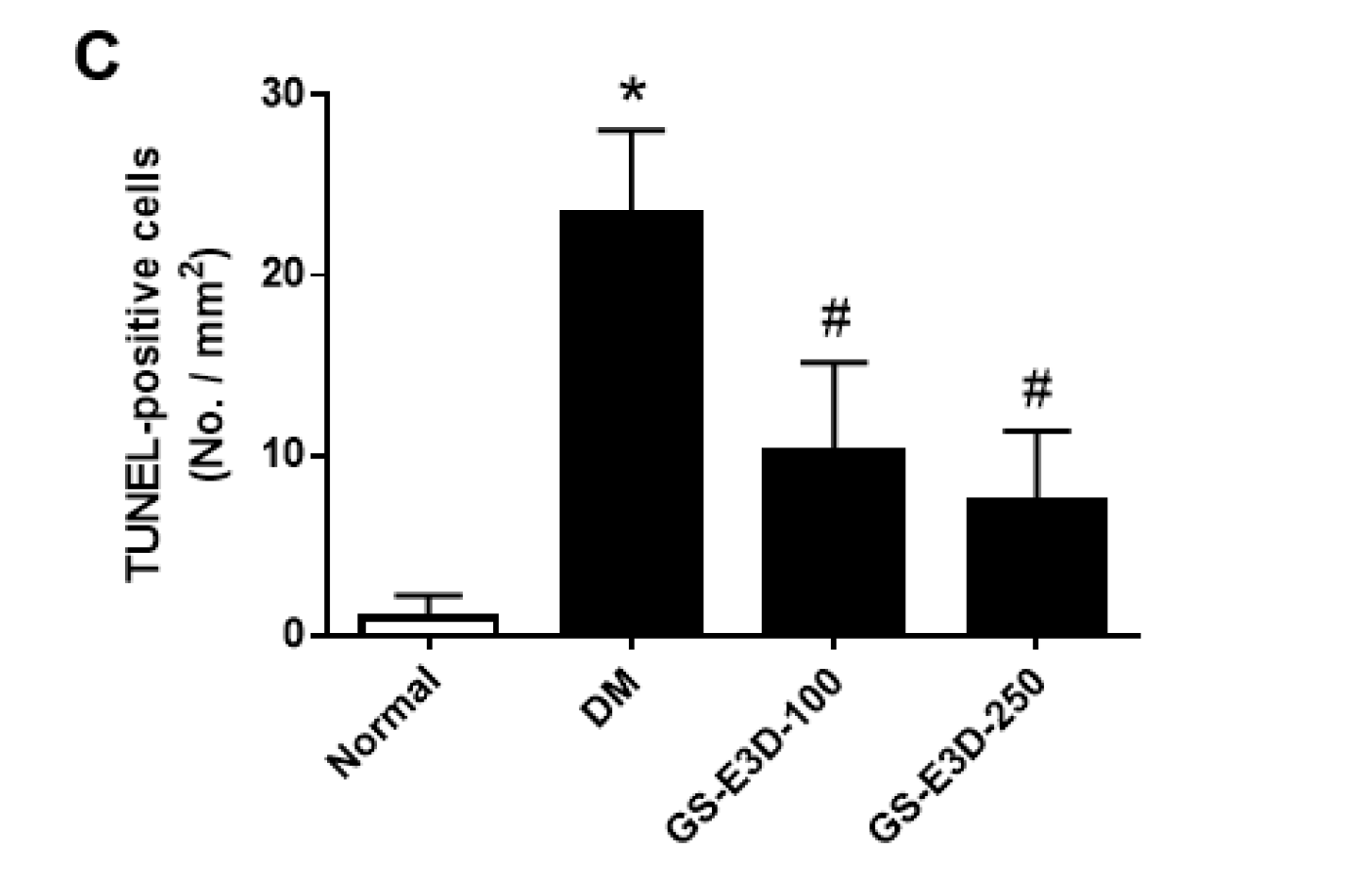
2.4. GS-E3D Prevents Histopathological Changes and Apoptosis in Renal Tissues
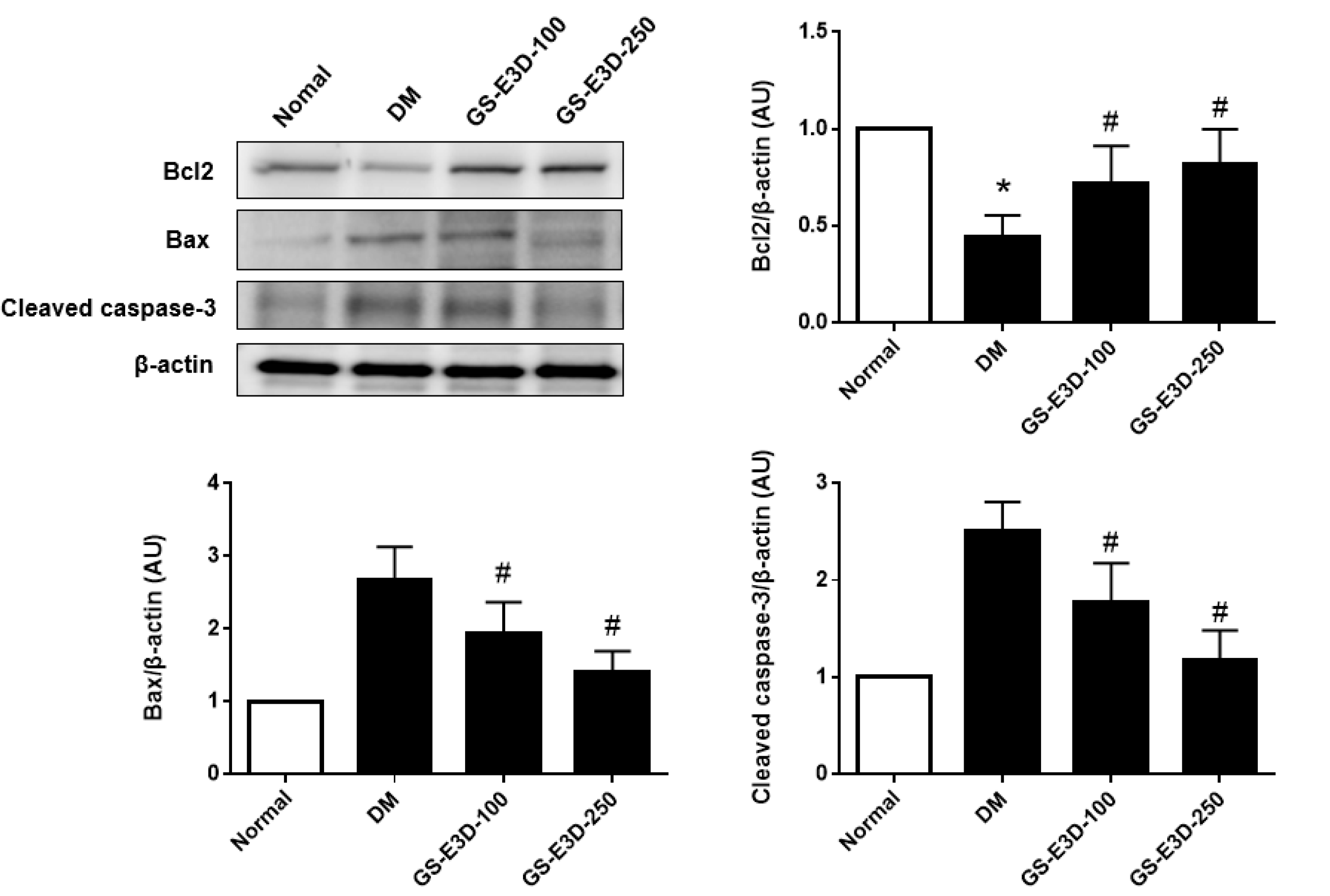
2.5. Protective Effects of GS-E3D on Renal Tissues in Diabetes Were Dependent on Inhibition of Apoptosis-Related Protein Expression
3. Discussion
4. Materials and Methods
4.1. Preparation of Pectin-Lyase-Modified Ginseng
4.2. Cell Culture
4.3. Oxidative Stress Assay in MMCs
4.4. Animals
4.5. Bioassay of Urine
4.6. Oxidative Stress Assay on Kidneys
4.7. Hematoxylin and Eosin Staining
4.8. TUNEL Staining
4.9. Western Blot Assay
4.10. Statistical Analysis
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Sample Availability
References
- White, K.E.; Bilous, R.W. Type 2 diabetic patients with nephropathy show structural-functional relationships that are similar to type 1 disease. J. Am. Soc. Nephrol. 2000, 11, 1667–1673. [Google Scholar] [PubMed]
- Furukawa, M.; Gohda, T.; Tanimoto, M.; Tomino, Y. Pathogenesis and novel treatment from the mouse model of type 2 diabetic nephropathy. Sci. World J. 2013, 2013, 928197. [Google Scholar] [CrossRef] [PubMed]
- Dounousi, E.; Duni, A.; Leivaditis, K.; Vaios, V.; Eleftheriadis, T.; Liakopoulos, V. Improvements in the Management of Diabetic Nephropathy. Rev. Diabet Stud. 2015, 12, 119–133. [Google Scholar] [CrossRef] [PubMed]
- Aldukhayel, A. Prevalence of diabetic nephropathy among Type 2 diabetic patients in some of the Arab countries. Int. J. Health Sci. (Qassim) 2017, 11, 1–4. [Google Scholar]
- Piccoli, G.B.; Grassi, G.; Cabiddu, G.; Nazha, M.; Roggero, S.; Capizzi, I.; De Pascale, A.; Priola, A.M.; Di Vico, C.; Maxia, S.; et al. Diabetic Kidney Disease: A Syndrome Rather Than a Single Disease. Rev. Diabet Stud. 2015, 12, 87–109. [Google Scholar] [CrossRef]
- Furuichi, K.; Shimizu, M.; Okada, H.; Narita, I.; Wada, T. Clinico-pathological features of kidney disease in diabetic cases. Clin. Exp. Nephrol. 2018, 22, 1046–1051. [Google Scholar]
- Kim, C.S.; Jo, K.; Kim, J.S.; Pyo, M.K.; Kim, J. GS-E3D, a new pectin lyase-modified red ginseng extract, inhibited diabetes-related renal dysfunction in streptozotocin-induced diabetic rats. BMC Complement. Altern. Med. 2017, 17, 430. [Google Scholar]
- Shukla, R.; Banerjee, S.; Tripathi, Y.B. Antioxidant and Antiapoptotic effect of aqueous extract of Pueraria tuberosa (Roxb. Ex Willd.) DC. On streptozotocin-induced diabetic nephropathy in rats. BMC Complement. Altern. Med. 2018, 18, 156. [Google Scholar]
- Tchamgoue, A.D.; Tchokouaha, L.R.Y.; Tsabang, N.; Tarkang, P.A.; Kuiate, J.R.; Agbor, G.A. Costus afer Protects Cardio-, Hepato-, and Reno-Antioxidant Status in Streptozotocin-Intoxicated Wistar Rats. Biomed Res. Int. 2018, 2018, 4907648. [Google Scholar] [CrossRef]
- Nishikawa, T.; Edelstein, D.; Du, X.L.; Yamagishi, S.-i.; Matsumura, T.; Kaneda, Y.; Yorek, M.A.; Beebe, D.; Oates, P.J.; Hammes, H.-P. Normalizing mitochondrial superoxide production blocks three pathways of hyperglycaemic damage. Nature 2000, 404, 787. [Google Scholar] [CrossRef]
- Cameron, N.; Cotter, M.; Maxfield, E. Anti-oxidant treatment prevents the development of peripheral nerve dysfunction in streptozotocin-diabetic rats. Diabetologia 1993, 36, 299–304. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Mekiňová, D.; Chorvathova, V.; Volkovova, K.; Staruchova, M.; Graňičová, E.; Klvanova, J.; Ondreič, R. Effect of intake of exogenous vitamins C, E and β-carotene on the antioxidative status in kidneys of rats with streptozotocin-induced diabetes. Food/Nahrung 1995, 39, 257–261. [Google Scholar] [CrossRef] [PubMed]
- Ido, Y.; Kilo, C.; Williamson, J. Cytosolic NADH/NAD+, free radicals, and vascular dysfunction in early diabetes mellitus. Diabetologia 1997, 40, S115–S117. [Google Scholar] [CrossRef] [PubMed]
- Kaul, N.; Siveski-Iliskovic, N.; Hill, M.; Khaper, N.; Seneviratne, C.; Singal, P. Probucol treatment reverses antioxidant and functional deficit in diabetic cardiomyopathy. Mol. Cell. Biochem. 1996, 160, 283–288. [Google Scholar]
- Song, Y.; Cook, N.R.; Albert, C.M.; Van Denburgh, M.; Manson, J.E. Effects of vitamins C and E and β-carotene on the risk of type 2 diabetes in women at high risk of cardiovascular disease: A randomized controlled trial. Am. J. Clin. Nutr. 2009, 90, 429–437. [Google Scholar] [CrossRef]
- Ghamarian, A.; Abdollahi, M.; Su, X.; Amiri, A.; Ahadi, A.; Nowrouzi, A. Effect of chicory seed extract on glucose tolerance test (GTT) and metabolic profile in early and late stage diabetic rats. DARU J. Pharm. Sci. 2012, 20, 56. [Google Scholar] [CrossRef]
- Miller, E.R.; Pastor-Barriuso, R.; Dalal, D.; Riemersma, R.A.; Appel, L.J.; Guallar, E. Meta-analysis: High-dosage vitamin E supplementation may increase all-cause mortality. Ann. Intern. Med. 2005, 142, 37–46. [Google Scholar] [CrossRef]
- Kim, P.; Park, J.H.; Kwon, K.J.; Kim, K.C.; Kim, H.J.; Lee, J.M.; Kim, H.Y.; Han, S.H.; Shin, C.Y. Effects of Korean red ginseng extracts on neural tube defects and impairment of social interaction induced by prenatal exposure to valproic acid. Food Chem. Toxicol. 2013, 51, 288–296. [Google Scholar]
- Park, H.M.; Kim, S.J.; Mun, A.R.; Go, H.K.; Kim, G.B.; Kim, S.Z.; Jang, S.I.; Lee, S.J.; Kim, J.S.; Kang, H.S. Korean red ginseng and its primary ginsenosides inhibit ethanol-induced oxidative injury by suppression of the MAPK pathway in TIB-73 cells. J. Ethnopharmacol. 2012, 141, 1071–1076. [Google Scholar] [CrossRef]
- Paul, S.; Shin, H.S.; Kang, S.C. Inhibition of inflammations and macrophage activation by ginsenoside-Re isolated from Korean ginseng (Panax ginseng C.A. Meyer). Food Chem. Toxicol. 2012, 50, 1354–1361. [Google Scholar] [CrossRef]
- Vuksan, V.; Sung, M.K.; Sievenpiper, J.L.; Stavro, P.M.; Jenkins, A.L.; Di Buono, M.; Lee, K.S.; Leiter, L.A.; Nam, K.Y.; Arnason, J.T.; et al. Korean red ginseng (Panax ginseng) improves glucose and insulin regulation in well-controlled, type 2 diabetes: Results of a randomized, double-blind, placebo-controlled study of efficacy and safety. Nutr. Metab. Cardiovasc. Dis. 2008, 18, 46–56. [Google Scholar] [CrossRef] [PubMed]
- Yokozawa, T.; Liu, Z.W.; Dong, E. A study of ginsenoside-Rd in a renal ischemia-reperfusion model. Nephron 1998, 78, 201–206. [Google Scholar] [CrossRef]
- Yokozawa, T.; Owada, S. Effect of ginsenoside-Rd in cephaloridine-induced renal disorder. Nephron 1999, 81, 200–207. [Google Scholar] [CrossRef] [PubMed]
- Yokozawa, T.; Liu, Z.W. The role of ginsenoside-Rd in cisplatin-induced acute renal failure. Ren. Fail. 2000, 22, 115–127. [Google Scholar] [CrossRef]
- Jung, E.; Kim, C.S.; Jung, W.; Park, S.B.; Pyo, M.K.; Kim, J. Ginseng Extract Modified by Pectin Lyase Inhibits Retinal Vascular Injury and Blood-Retinal Barrier Breakage in a Rat Model of Diabetes. J. Med. Food 2019, 22, 337–343. [Google Scholar] [CrossRef]
- Lee, H.Y.; Park, K.H.; Park, Y.M.; Moon, D.I.; Oh, H.G.; Kwon, D.Y.; Yang, H.J.; Kim, O.; Kim, D.W.; Yoo, J.H.; et al. Effects of pectin lyase-modified red ginseng extracts in high-fat diet-fed obese mice. Lab Anim. Res. 2014, 30, 151–160. [Google Scholar] [CrossRef][Green Version]
- Kim, C.S.; Jo, K.; Pyo, M.K.; Kim, J.S.; Kim, J. Pectin lyase-modified red ginseng extract exhibits potent anti-glycation effects in vitro and in vivo. J. Exerc. Nutr. Biochem. 2017, 21, 56–62. [Google Scholar] [CrossRef]
- Kim, G.W.; Pyo, M.K.; Chung, S.H. Pectin lyase-modified red ginseng extract improves glucose homeostasis in high fat diet-fed mice. J. Ethnopharmacol. 2020, 249, 112384. [Google Scholar] [CrossRef]
- Lee, J.Y.; Park, C.S.; Choi, H.Y.; Yune, T.Y. Ginseng Extracts, GS-KG9 and GS-E3D, Prevent Blood-Brain Barrier Disruption and Thereby Inhibit Apoptotic Cell Death of Hippocampal Neurons in Streptozotocin-Induced Diabetic Rats. Nutrients 2020, 12, 2383. [Google Scholar] [CrossRef]
- Mason, A.L.; Xu, L.; Guo, L.; Garry, R.F. Retroviruses in autoimmune liver disease: Genetic or environmental agents? Arch. Immunol. Ther. Exp. 1999, 47, 289–297. [Google Scholar]
- Van, J.A.; Scholey, J.W.; Konvalinka, A. Insights into Diabetic Kidney Disease Using Urinary Proteomics and Bioinformatics. J. Am. Soc. Nephrol. 2017, 28, 1050–1061. [Google Scholar] [CrossRef] [PubMed]
- Yu, S.M.; Bonventre, J.V. Acute Kidney Injury and Progression of Diabetic Kidney Disease. Adv. Chronic. Kidney Dis. 2018, 25, 166–180. [Google Scholar] [CrossRef] [PubMed]
- Hong, Y.J.; Kim, N.; Lee, K.; Hee Sonn, C.; Eun Lee, J.; Tae Kim, S.; Ho Baeg, I.; Lee, K.M. Korean red ginseng (Panax ginseng) ameliorates type 1 diabetes and restores immune cell compartments. J. Ethnopharmacol. 2012, 144, 225–233. [Google Scholar] [CrossRef] [PubMed]
- Hong, S.H.; Suk, K.T.; Choi, S.H.; Lee, J.W.; Sung, H.T.; Kim, C.H.; Kim, E.J.; Kim, M.J.; Han, S.H.; Kim, M.Y.; et al. Anti-oxidant and natural killer cell activity of Korean red ginseng (Panax ginseng) and urushiol (Rhus vernicifera Stokes) on non-alcoholic fatty liver disease of rat. Food Chem. Toxicol. 2013, 55, 586–591. [Google Scholar] [CrossRef] [PubMed]
- Yang, H.; Lee, S.E.; Jeong, S.I.; Park, C.S.; Jin, Y.H.; Park, Y.S. Up-regulation of Heme Oxygenase-1 by Korean Red Ginseng Water Extract as a Cytoprotective Effect in Human Endothelial Cells. J. Ginseng Res. 2011, 35, 352–359. [Google Scholar] [CrossRef] [PubMed]
- Luo, Z.F.; Feng, B.; Mu, J.; Qi, W.; Zeng, W.; Guo, Y.H.; Pang, Q.; Ye, Z.L.; Liu, L.; Yuan, F.H. Effects of 4-phenylbutyric acid on the process and development of diabetic nephropathy induced in rats by streptozotocin: Regulation of endoplasmic reticulum stress-oxidative activation. Toxicol. Appl. Pharmacol. 2010, 246, 49–57. [Google Scholar] [CrossRef]
- Li, H.; Wang, F.; Zhang, L.; Cao, Y.; Liu, W.; Hao, J.; Liu, Q.; Duan, H. Modulation of Nrf2 expression alters high glucose-induced oxidative stress and antioxidant gene expression in mouse mesangial cells. Cell Signal 2011, 23, 1625–1632. [Google Scholar] [CrossRef]
- Schafer, S.; Linz, W.; Bube, A.; Gerl, M.; Huber, J.; Kurzel, G.U.; Bleich, M.; Schmidts, H.L.; Busch, A.E.; Rutten, H. Vasopeptidase inhibition prevents nephropathy in Zucker diabetic fatty rats. Cardiovasc. Res. 2003, 60, 447–454. [Google Scholar] [CrossRef]
- Kim, J.; Shon, E.; Kim, C.S.; Kim, J.S. Renal podocyte injury in a rat model of type 2 diabetes is prevented by metformin. Exp. Diabetes Res. 2012, 2012, 210821. [Google Scholar] [CrossRef]
- Susztak, K.; Raff, A.C.; Schiffer, M.; Bottinger, E.P. Glucose-induced reactive oxygen species cause apoptosis of podocytes and podocyte depletion at the onset of diabetic nephropathy. Diabetes 2006, 55, 225–233. [Google Scholar] [CrossRef]
- Gorin, Y.; Block, K.; Hernandez, J.; Bhandari, B.; Wagner, B.; Barnes, J.L.; Abboud, H.E. Nox4 NAD(P)H oxidase mediates hypertrophy and fibronectin expression in the diabetic kidney. J. Biol. Chem. 2005, 280, 39616–39626. [Google Scholar] [CrossRef] [PubMed]
- Oltvai, Z.N.; Milliman, C.L.; Korsmeyer, S.J. Bcl-2 heterodimerizes in vivo with a conserved homolog, Bax, that accelerates programmed cell death. Cell 1993, 74, 609–619. [Google Scholar] [CrossRef]
- Allen, D.A.; Yaqoob, M.M.; Harwood, S.M. Mechanisms of high glucose-induced apoptosis and its relationship to diabetic complications. J. Nutr. Biochem. 2005, 16, 705–713. [Google Scholar] [CrossRef]
- Desagher, S.; Martinou, J.C. Mitochondria as the central control point of apoptosis. Trends Cell Biol. 2000, 10, 369–377. [Google Scholar] [CrossRef]
- Quan, H.Y.; Kim, D.Y.; Chung, S.H. Korean red ginseng extract alleviates advanced glycation end product-mediated renal injury. J. Ginseng Res. 2013, 37, 187–193. [Google Scholar] [CrossRef]
- Yokozawa, T.; Iwano, M.; Dohi, K.; Hattori, M.; Oura, H. Inhibitory effects of ginseng on proliferation of cultured mouse mesangial cells. Nihon Jinzo Gakkai Shi 1994, 36, 13–18. [Google Scholar]
- Park, C.R.; Pyo, M.K.; Lee, H.; Hong, S.Y.; Kim, S.H.; Park, C.B.; Oh, S.M. Acute and genetic toxicity of GS-E3D, a new pectin lyase-modified red ginseng extract. Regul. Toxicol. Pharmacol. 2019, 104, 157–162. [Google Scholar]

Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Jung, E.; Pyo, M.-k.; Kim, J. Pectin-Lyase-Modified Ginseng Extract and Ginsenoside Rd Inhibits High Glucose-Induced ROS Production in Mesangial Cells and Prevents Renal Dysfunction in db/db Mice. Molecules 2021, 26, 367. https://doi.org/10.3390/molecules26020367
Jung E, Pyo M-k, Kim J. Pectin-Lyase-Modified Ginseng Extract and Ginsenoside Rd Inhibits High Glucose-Induced ROS Production in Mesangial Cells and Prevents Renal Dysfunction in db/db Mice. Molecules. 2021; 26(2):367. https://doi.org/10.3390/molecules26020367
Chicago/Turabian StyleJung, Eunsoo, Mi-kyung Pyo, and Junghyun Kim. 2021. "Pectin-Lyase-Modified Ginseng Extract and Ginsenoside Rd Inhibits High Glucose-Induced ROS Production in Mesangial Cells and Prevents Renal Dysfunction in db/db Mice" Molecules 26, no. 2: 367. https://doi.org/10.3390/molecules26020367
APA StyleJung, E., Pyo, M.-k., & Kim, J. (2021). Pectin-Lyase-Modified Ginseng Extract and Ginsenoside Rd Inhibits High Glucose-Induced ROS Production in Mesangial Cells and Prevents Renal Dysfunction in db/db Mice. Molecules, 26(2), 367. https://doi.org/10.3390/molecules26020367






