Acute Myeloid Leukemia: Current Progress and Future Directions
A special issue of Journal of Personalized Medicine (ISSN 2075-4426). This special issue belongs to the section "Personalized Therapy in Clinical Medicine".
Deadline for manuscript submissions: 15 October 2026 | Viewed by 4915
Special Issue Editors
Interests: myeloid malignancies; bone marrow failure syndromes; RNA splicing
Special Issues, Collections and Topics in MDPI journals
Interests: acute myeloid leukemia; myelodysplastic syndromes; myeloproliferative neoplasms; acute promyelocytic leukemia
Special Issues, Collections and Topics in MDPI journals
Special Issue Information
Dear Colleagues,
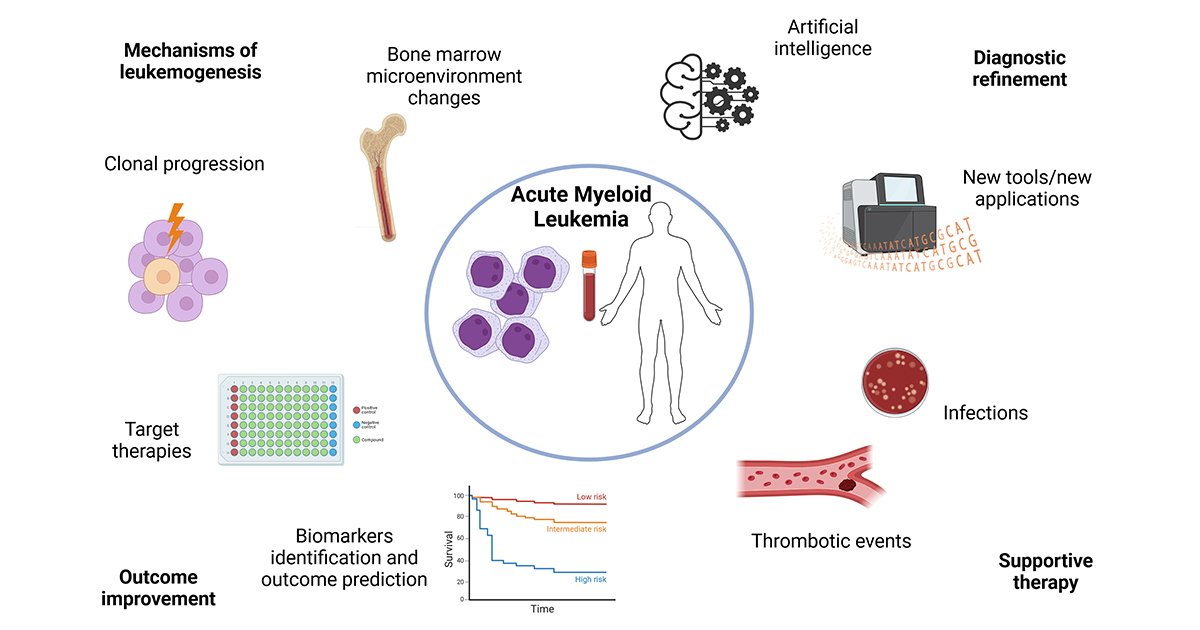
Acute myeloid leukemia (AML) is an aggressive malignancy spanning heterogenous clinical and molecular phenotypes. In recent years, huge advances in our understanding of the disease’s biology have led us to gain deeper insight into the genetic features and the bone marrow microenvironment changes underpinning the process of leukemogenesis, paving the way to targeted treatments. Therefore, paired with these findings, there has been a rise in attention toward support therapies and careful assessments of patients’ wellbeing. All in all, these novelties have manifested in the investigation and successful introduction of target therapies in clinical practice; more precise risk stratification; and AML management tailored to both the disease’s biological features and patients’ characteristics. Thus, this Special Issue will focus on the recent advances concerning all facets of personalized AML management, including both treatment investigations and translational research, as well as the bench-side management of complications and all-day practice. Moreover, current and future risk disease stratifications, prognostic markers and models, and applications of novel techniques regarding the disease’s multimodal nature will be considered. We will highly appreciate and welcome the submissions of original papers and reviews in line with the aim of this Special Issue.
Dr. Valeria Visconte
Dr. Luca Guarnera
Guest Editors
Manuscript Submission Information
Manuscripts should be submitted online at www.mdpi.com by registering and logging in to this website. Once you are registered, click here to go to the submission form. Manuscripts can be submitted until the deadline. All submissions that pass pre-check are peer-reviewed. Accepted papers will be published continuously in the journal (as soon as accepted) and will be listed together on the special issue website. Research articles, review articles as well as short communications are invited. For planned papers, a title and short abstract (about 250 words) can be sent to the Editorial Office for assessment.
Submitted manuscripts should not have been published previously, nor be under consideration for publication elsewhere (except conference proceedings papers). All manuscripts are thoroughly refereed through a single-blind peer-review process. A guide for authors and other relevant information for submission of manuscripts is available on the Instructions for Authors page. Journal of Personalized Medicine is an international peer-reviewed open access monthly journal published by MDPI.
Please visit the Instructions for Authors page before submitting a manuscript. The Article Processing Charge (APC) for publication in this open access journal is 2600 CHF (Swiss Francs). Submitted papers should be well formatted and use good English. Authors may use MDPI's English editing service prior to publication or during author revisions.
Benefits of Publishing in a Special Issue
- Ease of navigation: Grouping papers by topic helps scholars navigate broad scope journals more efficiently.
- Greater discoverability: Special Issues support the reach and impact of scientific research. Articles in Special Issues are more discoverable and cited more frequently.
- Expansion of research network: Special Issues facilitate connections among authors, fostering scientific collaborations.
- External promotion: Articles in Special Issues are often promoted through the journal's social media, increasing their visibility.
- Reprint: MDPI Books provides the opportunity to republish successful Special Issues in book format, both online and in print.
Further information on MDPI's Special Issue policies can be found here.






