Journal Description
Journal of Cardiovascular Development and Disease
Journal of Cardiovascular Development and Disease
(JCDD) is an international, peer-reviewed, open access journal on cardiovascular medicine, published monthly online by MDPI.
- Open Access— free for readers, with article processing charges (APC) paid by authors or their institutions.
- High Visibility: indexed within Scopus, SCIE (Web of Science), PubMed, PMC, Embase, CAPlus / SciFinder, and other databases.
- Journal Rank: JCR - Q2 (Cardiac and Cardiovascular Systems) / CiteScore - Q2 (General Pharmacology, Toxicology and Pharmaceutics )
- Rapid Publication: manuscripts are peer-reviewed and a first decision is provided to authors approximately 24.7 days after submission; acceptance to publication is undertaken in 3.6 days (median values for papers published in this journal in the second half of 2025).
- Recognition of Reviewers: reviewers who provide timely, thorough peer-review reports receive vouchers entitling them to a discount on the APC of their next publication in any MDPI journal, in appreciation of the work done.
Impact Factor:
2.3 (2024);
5-Year Impact Factor:
2.7 (2024)
Latest Articles
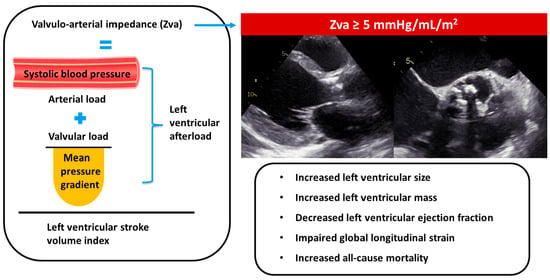
Valvulo-Arterial Impedance in Patients with Severe Aortic Stenosis and Bicuspid Aortic Valve
J. Cardiovasc. Dev. Dis. 2026, 13(4), 163; https://doi.org/10.3390/jcdd13040163 (registering DOI) - 9 Apr 2026
Abstract
Background: Risk stratification in patients with bicuspid aortic valve (BAV) and severe aortic stenosis (AS) remains challenging. Valvulo-arterial impedance (Zva), an integrated marker of global left ventricular (LV) afterload, has shown prognostic value in tricuspid AS; however, data in BAV are limited. This
[...] Read more.
Background: Risk stratification in patients with bicuspid aortic valve (BAV) and severe aortic stenosis (AS) remains challenging. Valvulo-arterial impedance (Zva), an integrated marker of global left ventricular (LV) afterload, has shown prognostic value in tricuspid AS; however, data in BAV are limited. This study aimed to evaluate the association of Zva with LV remodeling, symptoms, and all-cause death in patients with BAV and severe AS. Methods: In this retrospective, two-center cohort study, 147 patients with severe AS and BAV were included. Zva was calculated at the time of the first echocardiographic diagnosis of severe AS. The study endpoint was all-cause mortality. Results: Over a median follow-up of 9.8 years, 24 patients (16%) died. A Zva threshold of 5 mmHg/mL/m2 was identified as optimal by ROC analysis. Patients with Zva ≥ 5 mmHg/mL/m2 showed higher mortality rates (29% vs. 10%; p = 0.003), more advanced symptoms (NYHA III-IV: 41% vs. 9%; p < 0.001), adverse LV remodeling, lower LVEF (60% (IQR 36–66) vs. 66% (IQR 61–71); p = 0.001), and worse LV global longitudinal strain (14.8% ± 2.7 vs. 16.5% ± 3.0; p = 0.016). Zva ≥ 5 mmHg/mL/m2 was independently associated with worse long-term survival after adjustment (HR 2.885; 95% CI 1.119–7.438; p = 0.028). Conclusions: Among patients with BAV and severe AS, an increased Zva was associated with more advanced symptoms, adverse LV remodeling, impaired LV systolic function, and worse long-term survival, and might therefore help in risk stratification of these patients.
Full article
(This article belongs to the Special Issue The Role of Echocardiography in Cardiovascular Diseases)
►
Show Figures
Open AccessCase Report
A Diagnostic Dilemma of Arrhythmogenic Cardiomyopathy Masquerading as Recurrent Myocarditis in a Pediatric Patient with a DES Gene Variant: A Case Report
by
Qi Meng, Wei Li, Wenhong Ding, Hui Wang, Dong Chen, Ling Han, Yifei Li and Chencheng Dai
J. Cardiovasc. Dev. Dis. 2026, 13(4), 162; https://doi.org/10.3390/jcdd13040162 - 8 Apr 2026
Abstract
Background: Arrhythmogenic cardiomyopathy (ACM) is an inherited disorder characterized by fibrofatty replacement of cardiomyocytes. The inflammatory episodes of ACM, known as the “hot phase”, can mimic acute myocarditis. It was seldom observed in a DES-associated ACM as a “hot-phase” presentation. Case Presentation:
[...] Read more.
Background: Arrhythmogenic cardiomyopathy (ACM) is an inherited disorder characterized by fibrofatty replacement of cardiomyocytes. The inflammatory episodes of ACM, known as the “hot phase”, can mimic acute myocarditis. It was seldom observed in a DES-associated ACM as a “hot-phase” presentation. Case Presentation: The proband, a 13-year-old female, initially presented with a series of clinical manifestations of fulminant myocarditis. Although recommendation-guided anti-immunotherapy had been provided, this patient still developed into an aggressive cardiomyopathy with biventricular dilation and severe systolic heart failure. Additionally, cardiac magnetic resonance demonstrated circumferential late gadolinium enhancement in left ventricular myocardium with diffuse fibrosis. Whole-exon sequencing identified a de novo missense variant, as c.335T>A (p.L112Q) of the DES gene, resulting in protein dysfunction. And a diagnosis of ACM due to a DES variant had been identified. Finally, this patient received heart transplantation, and biventricular fibrofatty infiltration was confirmed by pathological analysis. Conclusions: This case presented a de novo genetic variant that can induce severe and aggressive heart failure. This finding emphasizes the importance of comprehensive genetic analysis in patients suspected of having fulminant myocarditis, which would greatly benefit the precise clinical management and outcomes.
Full article
(This article belongs to the Topic Molecular and Cellular Mechanisms of Heart Disease)
►▼
Show Figures
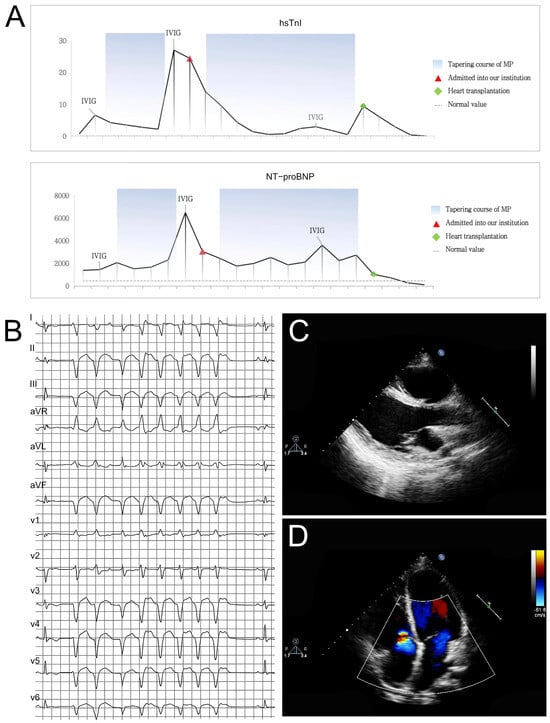
Figure 1
Open AccessArticle
Standardized Beating-Heart Aortic Arch Reconstruction with Simultaneous Cerebral and Coronary Perfusion in Neonates and Infants: A Single-Center Cardiovascular Cohort Study
by
Shiraslan Bakhshaliyev and Ergin Arslanoglu
J. Cardiovasc. Dev. Dis. 2026, 13(4), 161; https://doi.org/10.3390/jcdd13040161 - 7 Apr 2026
Abstract
Background: Neonatal and infant aortic arch reconstruction remains a high-risk cardiovascular procedure requiring effective cerebral and myocardial protection. Variability in perfusion strategies may influence early hemodynamic stability and postoperative recovery. This study aimed to evaluate the early and short-term cardiovascular outcomes of a
[...] Read more.
Background: Neonatal and infant aortic arch reconstruction remains a high-risk cardiovascular procedure requiring effective cerebral and myocardial protection. Variability in perfusion strategies may influence early hemodynamic stability and postoperative recovery. This study aimed to evaluate the early and short-term cardiovascular outcomes of a standardized beating-heart aortic arch reconstruction strategy incorporating simultaneous antegrade selective cerebral and continuous coronary perfusion. Methods: In this retrospective single-center cohort study, 31 consecutive neonates and infants undergoing aortic arch reconstruction between November 2022 and December 2025 were analyzed. A standardized surgical protocol was applied, consisting of extensive ductal tissue resection, interdigitating posterior end-to-end anastomosis, anterior autologous pericardial patch augmentation, and moderate hypothermic antegrade selective cerebral perfusion combined with continuous coronary perfusion via innominate artery cannulation. Early postoperative outcomes and short-term echocardiographic follow-up results were assessed. Results: The cohort included 31 patients, 22.6% of whom had complex associated cardiac anomalies requiring concomitant procedures. Median cardiopulmonary bypass and aortic cross-clamp times were 119 and 64 min, respectively. There was no in-hospital mortality. Major complications were infrequent, and median intensive care unit stay was 5 days. During a median follow-up of 6.8 months, one patient (3.2%) developed recoarctation requiring reintervention. No late mortality was observed. Conclusions: A fully standardized beating-heart aortic arch reconstruction strategy incorporating simultaneous cerebral and coronary perfusion demonstrated favorable early cardiovascular and short-term outcomes, even in anatomically complex cases. Preservation of continuous coronary perfusion may be associated with improved myocardial stability and early postoperative recovery; however, these findings should be interpreted as observational and hypothesis-generating given the absence of a control group. Larger multicenter studies with longer follow-up are warranted to confirm these findings.
Full article
(This article belongs to the Section Pediatric Cardiology and Congenital Heart Disease)
Open AccessArticle
Effect of SGLT2 Inhibitors on the Efficacy of First-Time Pulmonary Vein Isolation and Clinical Course of Patients with Heart Failure with Preserved Ejection Fraction and Atrial Fibrillation
by
Magdalena Balwierz-Podgórna, Bartosz Gruchlik, Katarzyna Mizia-Stec, Adriana Filak, Anna Hejmej, Piotr Paździora, Mikołaj Gołda, Aleksandra Spirkowicz, Karina Dzięcioł and Maciej Wybraniec
J. Cardiovasc. Dev. Dis. 2026, 13(4), 160; https://doi.org/10.3390/jcdd13040160 - 6 Apr 2026
Abstract
Background/Objectives: SGLT2 inhibitors (SGLT2i) became a cornerstone of heart failure with preserved ejection fraction (HFpEF) pharmacotherapy in the recent years However, their actual influence on pulmonary veins isolation (PVI) efficacy in this population remains unclear. The aim of the study was to
[...] Read more.
Background/Objectives: SGLT2 inhibitors (SGLT2i) became a cornerstone of heart failure with preserved ejection fraction (HFpEF) pharmacotherapy in the recent years However, their actual influence on pulmonary veins isolation (PVI) efficacy in this population remains unclear. The aim of the study was to evaluate an impact of SGLT2i on one-year first-time PVI efficacy and clinical course of patients with HFpEF and atrial fibrillation (AF). Methods: This is a single-center retrospective study including 105 HFpEF and AF individuals, who underwent the first-time PVI (51 (48.6%) males; mean age at PVI: 65.2 ± 9.5 years). 53 patients treated with SGLT2i (hospitalized for PVI since 2023) and 52 patients without such a treatment (2020-mid-2023) were assessed according to the clinical presentation and hard endpoints. The primary endpoint was arrhythmia recurrence rate. The secondary endpoint was a composite of major adverse cardiovascular and cerebrovascular events (MACCE). Results: SGLT2i therapy was associated with greater symptom reduction after PVI (90.6% vs. 62.7%; p < 0.001). There was a statistical trend toward reduced all-cause mortality in SGLT2i (0% vs. 5.8%; p = 0.076). Although overall AF recurrence rates were similar between subgroups, Kaplan–Meier analysis showed a non-significant trend toward lower recurrence in the SGLT2i group (p = 0.096). The analysis did not reveal significant differences in terms of cardiovascular hospitalizations, stroke/transient ischemic attack (TIA) and MACCE incidence between the subgroups. Non-vitamin K antagonist oral anticoagulants (NOACs) administration was associated with a lower risk of AF recurrence (OR 0.27; 95% CI 0.096 to 0.77; p = 0.014). MACCE occurrence was predicted by higher CHA2DS2-VA (Congestive heart failure, Hypertension, Age ≥ 75, Diabetes, Stroke, Vascular disease, Age 65–74) (OR 5.63; 95% CI 1.57–20.12; p = 0.008), lower left ventricular ejection fraction (LVEF) (OR 0.74; 95% CI 0.57–0.99; p = 0.028) and (vitamin K antagonists) VKA use (OR 97.44; 95% CI 3.2–2962.57; p = 0.009). Conclusions: SGLT2i pharmacotherapy in the study population was linked to higher efficacy in symptom reduction, with a probability of AF recurrence and all-cause mortality reduction, which may suggest a potential beneficial role of SGLT2i in this cohort.
Full article
(This article belongs to the Section Electrophysiology and Cardiovascular Physiology)
►▼
Show Figures

Figure 1
Open AccessArticle
Protective Role of Hesperidin Against Deltamethrin-Induced Cardiovascular Structural Damage: Involvement of Caspase-3-Driven Apoptosis and Fibrosis Suppression in Rats
by
Burcu Gültekin, Halime Tuba Canbaz, Hasan Basri Savaş, Gökhan Cüce and Sabiha Serpil Kalkan
J. Cardiovasc. Dev. Dis. 2026, 13(4), 159; https://doi.org/10.3390/jcdd13040159 - 3 Apr 2026
Abstract
►▼
Show Figures
Background and Objectives: Deltamethrin (DLM), a widely used pyrethroid insecticide, has been linked to cardiotoxic effects in non-target organisms. Hesperidin (HSP), a dietary bioflavonoid with antioxidant and cardioprotective properties, may counteract these effects. This study investigated the protective role of HSP against DLM-induced
[...] Read more.
Background and Objectives: Deltamethrin (DLM), a widely used pyrethroid insecticide, has been linked to cardiotoxic effects in non-target organisms. Hesperidin (HSP), a dietary bioflavonoid with antioxidant and cardioprotective properties, may counteract these effects. This study investigated the protective role of HSP against DLM-induced cardiotoxicity in male Wistar Albino rats. Materials and Methods: Thirty-two rats were divided into four groups: Control, DLM, DLM + HSP 100, and DLM + HSP 300. At the end of the experiment, serum ischemia-modified albumin (IMA), glucose, cholesterol, triglyceride, and HDL levels were analyzed. Cardiac and aortic tissues were assessed histopathologically. Masson’s trichrome staining evaluated cardiac fibrosis, Verhoeff–Van Gieson staining examined elastin and tunica media thickness, and caspase-3 expression in the aorta was determined immunohistochemically. Results: DLM administration caused cardiac and aortic damage by increasing IMA, glucose, caspase 3 activities, and tunica media thickness. HSP treatment, particularly at 300 mg/kg, reduced IMA (0.28 ± 0.02 vs. 0.60 ± 0.03 AU), glucose (141.12 ± 11.70 vs. 207.06 ± 9.85 mg/dL), cardiac histopathological damage score (2.17 ± 0.41 vs. 9.02 ± 1.35), tunica media thickness (95.29 ± 4.29 vs. 114.95 ± 17.20 µm), and caspase-3 expression score (0.62 ± 0.74 vs. 2.87 ± 0.35). All results showed significance at the p < 0.05 level. Conclusions: HSP exhibited dose-dependent protective effects against DLM-induced oxidative stress, apoptosis, and cardiovascular injury, suggesting its potential as a therapeutic candidate against pesticide-related cardiotoxicity.
Full article
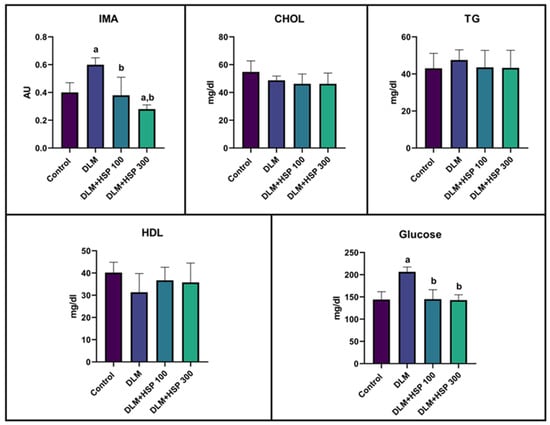
Figure 1
Open AccessReview
Acute Aortic Dissection in Women: A Comprehensive Review of Sex-Specific Differences, Clinical Management, and Outcomes
by
Vasiliki Androutsopoulou, Dimitrios E. Magouliotis, Andrew Xanthopoulos, Kalliopi Keramida, Metaxia Bareka, Konstantinos Stamoulis, Kosmas Tsakiridis, Thanos Athanasiou and John Skoularigis
J. Cardiovasc. Dev. Dis. 2026, 13(4), 158; https://doi.org/10.3390/jcdd13040158 - 3 Apr 2026
Abstract
Acute aortic dissection (AAD) is a life-threatening cardiovascular emergency characterized by important sex-related differences in presentation, management, and outcomes. Although women account for a smaller proportion of cases, they typically present at older ages and more frequently exhibit atypical symptoms, hemodynamic instability, and
[...] Read more.
Acute aortic dissection (AAD) is a life-threatening cardiovascular emergency characterized by important sex-related differences in presentation, management, and outcomes. Although women account for a smaller proportion of cases, they typically present at older ages and more frequently exhibit atypical symptoms, hemodynamic instability, and complications such as pericardial effusion or tamponade, contributing to diagnostic delays and higher pre-hospital mortality. Beyond clinical factors, biological differences may influence disease expression in women. Menopause-associated vascular aging, hormonal modulation of extracellular matrix remodeling, and pregnancy-related hemodynamic and connective tissue changes may alter aortic wall integrity and susceptibility to dissection. Notably, women often experience dissection at smaller absolute aortic diameters, highlighting the potential importance of body-size indexing in risk stratification and surgical thresholds. In type A AAD, women are less likely to undergo extensive surgical repair in some cohorts, and although contemporary in-hospital mortality differences are narrowing, long-term survival disparities may persist. In type B AAD, women are more frequently managed conservatively, while outcomes following thoracic endovascular aortic repair appear broadly comparable between sexes. Pregnancy and the postpartum period represent particularly vulnerable windows, especially among patients with underlying heritable aortopathies. Greater awareness of sex-specific biological and clinical characteristics, incorporation of indexed aortic dimensions, and improved multidisciplinary management strategies are essential to optimize outcomes for women with acute aortic dissection.
Full article
(This article belongs to the Special Issue Aortic Disease: Pathophysiology, Surgical Management, and Long-Term Outcomes)
►▼
Show Figures

Figure 1
Open AccessArticle
Nocturnal Cardiac Arrhythmias in Sleep Apnoea After Acute Myocardial Infarction and the Effect of Adaptive Servo-Ventilation: An Ancillary Study of the TEAM-ASV I Trial
by
Jan Pec, Marek Nigl, Henrik Fox, Stefan Stadler, Michael Kohn, Sarah Driendl, Olaf Oldenburg, Florian Zeman, Stefan Buchner and Michael Arzt
J. Cardiovasc. Dev. Dis. 2026, 13(4), 157; https://doi.org/10.3390/jcdd13040157 - 2 Apr 2026
Abstract
►▼
Show Figures
(1) Background: Early treatment of sleep-disordered breathing (SDB) with adaptive servo-ventilation (ASV) after acute myocardial infarction (AMI) has been shown to improve myocardial salvage. This analysis evaluates nocturnal electrocardiogram (ECG) Holter data, derived from polygraphy in a randomised clinical trial (NCT02093377), to assess
[...] Read more.
(1) Background: Early treatment of sleep-disordered breathing (SDB) with adaptive servo-ventilation (ASV) after acute myocardial infarction (AMI) has been shown to improve myocardial salvage. This analysis evaluates nocturnal electrocardiogram (ECG) Holter data, derived from polygraphy in a randomised clinical trial (NCT02093377), to assess the occurrence of nocturnal cardiac arrhythmias in patients with SDB and to explore the effect of ASV therapy. (2) Methods: In the TEAM-ASV I trial, patients were stratified by the presence/absence of SDB, defined by an apnoea–hypopnoea index (AHI) ≥15 events/h assessed with polygraphy. Those with SDB were subsequently randomised to receive ASV in addition to standard AMI care. Guideline-conforming semi-automated ECG analysis of nocturnal cardiac arrhythmias was conducted via Holter–ECG software (custo diagnostic, version 5.4). (3) Results: Patients with SDB had an increased incidence of non-sustained ventricular tachycardia (NSVT) (SDB: n = 8 (16%) vs. no SDB: n = 1 (2%); p = 0.024) and premature atrial contractions (PAC) (SDB: 1.2/h [0.3, 3.4] vs. no SDB: 0.3/h [0.1, 1.2]; p = 0.017). In patients with SDB who were randomised to ASV treatment early after AMI, we found no reduction in cardiac arrhythmias when ASV was added to standard care. (4) Conclusions: After AMI, SDB was linked to increased NSVT and PAC. ASV treatment demonstrated neither a harmful nor a beneficial effect on the occurrence of nocturnal cardiac arrhythmias. Further trials are warranted to confirm these findings.
Full article

Figure 1
Open AccessReview
Cardiogenic Shock: Clinical Management, Outcomes and Future Directions
by
Aaqil Ahmad Aubdool, Andrew J. Sullivan, Daniel A. Jones, Anthony Mathur, Alastair Proudfoot and Krishnaraj S. Rathod
J. Cardiovasc. Dev. Dis. 2026, 13(4), 156; https://doi.org/10.3390/jcdd13040156 - 31 Mar 2026
Abstract
Cardiogenic shock is a life-threatening condition caused by the heart’s sudden inability to pump sufficient blood to maintain adequate tissue perfusion, most commonly occurring following a myocardial infarction or acute decompensated heart failure. The resultant hypoperfusion can quickly progress to end-organ failure and
[...] Read more.
Cardiogenic shock is a life-threatening condition caused by the heart’s sudden inability to pump sufficient blood to maintain adequate tissue perfusion, most commonly occurring following a myocardial infarction or acute decompensated heart failure. The resultant hypoperfusion can quickly progress to end-organ failure and ultimately death if not treated urgently. This review explores the management of cardiogenic shock, highlighting current treatments, their effectiveness, and the challenges faced by healthcare providers. It looks at both pharmacological therapies and devices used for cardiac support, including mechanical circulatory support and emergency revascularisation procedures to restore blood flow. We also examine how different stages of shock affect survival and how new technologies including artificial intelligence and wearable monitors could help detect and treat this condition earlier. In addition, this review discusses the significant pressure that cardiogenic shock places on healthcare provision, including the typical financial cost of treatment in the UK, resource utilisation and regional disparities. Finally, we outline future directions for trial design, better prevention, more rapid diagnosis and improved treatments that could improve morbidity and mortality.
Full article
(This article belongs to the Special Issue Feature Review Papers in Cardiovascular Clinical Research)
►▼
Show Figures
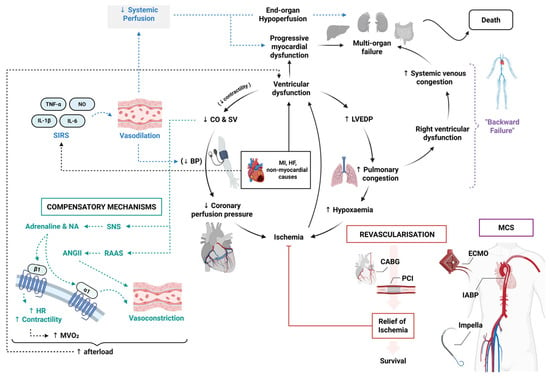
Figure 1
Open AccessReview
Current Management of Infective Endocarditis: A Narrative Review Focused on Unmet Clinical Needs and the Multidisciplinary Approach
by
Luca Di Vito, Giuseppina D’Amato, Riccardo Pascucci, Antonella D’Antonio, Giancarla Scalone, Mariavirginia Boni, Brunella Rossi, Ilaria Cimaroli, Claudia Acciarri, Marida Andreucci, Andrea Romandini, Simona Silenzi, Procolo Marchese and Pierfrancesco Grossi
J. Cardiovasc. Dev. Dis. 2026, 13(4), 155; https://doi.org/10.3390/jcdd13040155 - 30 Mar 2026
Abstract
►▼
Show Figures
Infective endocarditis (IE) is a severe infectious disease affecting cardiac valves (either native or prosthetic) or implantable cardiac devices, and it is associated with high rates of morbidity and mortality. Recent data from the Global Burden of Disease study have shown a significant
[...] Read more.
Infective endocarditis (IE) is a severe infectious disease affecting cardiac valves (either native or prosthetic) or implantable cardiac devices, and it is associated with high rates of morbidity and mortality. Recent data from the Global Burden of Disease study have shown a significant increase in both the incidence and mortality of IE. One-year mortality following diagnosis can reach up to 30%. IE can present with a wide range of clinical manifestations, and its course may be complicated by systemic embolic events or intracardiac complications such as abscess formation or prosthetic valve dehiscence. Echocardiography remains the first-line imaging modality; however, an integrated multimodality imaging approach is increasingly adopted in contemporary practice, incorporating both cardiac computed tomography and positron emission tomography. A multidisciplinary approach involving cardiologists, cardiac surgeons, internists, infectious disease specialists, and nuclear medicine physicians is often required to ensure accurate diagnosis and effective treatment of IE. The prognosis of infective endocarditis depends on early diagnosis, appropriate antimicrobial therapy, and timely surgical intervention when indicated. This review aims to summarize the current knowledge on IE, from pathophysiological insights to surgical strategies. It also focuses on practical recommendations to address the most pressing unmet clinical needs through a multidisciplinary approach.
Full article
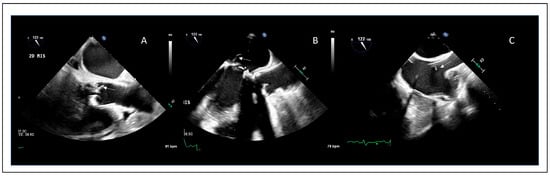
Figure 1
Open AccessReview
Isometric Handgrip Training and Cardiovascular Risk Modulation: State of the Art
by
Calogero Geraci, Francesca La Rocca, Salvatore Massimo Petrina, Agostino Buonauro, Giulio Geraci, Valentina Morello and Roberta Esposito
J. Cardiovasc. Dev. Dis. 2026, 13(4), 154; https://doi.org/10.3390/jcdd13040154 - 30 Mar 2026
Abstract
►▼
Show Figures
Cardiometabolic diseases remain the leading cause of morbidity and mortality worldwide, despite major advances in pharmacological and lifestyle interventions. Exercise training is a cornerstone of prevention and treatment; however, adherence to traditional aerobic programs remains suboptimal. Isometric handgrip (IHG) training has emerged as
[...] Read more.
Cardiometabolic diseases remain the leading cause of morbidity and mortality worldwide, despite major advances in pharmacological and lifestyle interventions. Exercise training is a cornerstone of prevention and treatment; however, adherence to traditional aerobic programs remains suboptimal. Isometric handgrip (IHG) training has emerged as a simple, time-efficient, and potentially effective strategy for improving cardiovascular and metabolic outcomes. This state-of-the-art review synthesizes current evidence on the physiological mechanisms underlying IHG training, including autonomic modulation, vascular function improvement, endothelial adaptation, and metabolic regulation. We summarize clinical data regarding its effects on blood pressure, arterial stiffness, endothelial function, insulin sensitivity, and inflammatory markers. Special attention is given to its applicability in specific populations, including hypertensive patients, individuals with metabolic syndrome, heart failure patients, and cancer survivors. We also discuss methodological heterogeneity across studies, safety considerations, and knowledge gaps. Finally, we outline future research directions needed to define optimal protocols and clarify long-term cardiometabolic benefits. IHG training represents a promising adjunctive strategy within cardiometabolic prevention and rehabilitation programs.
Full article
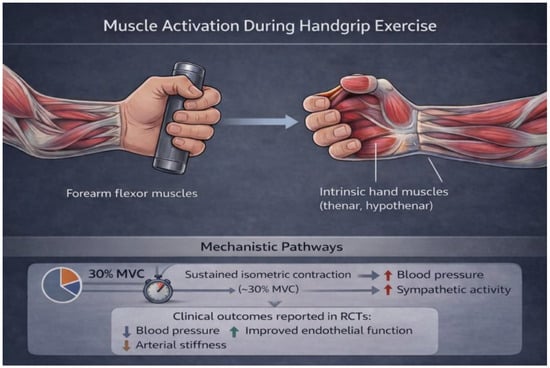
Figure 1
Open AccessReview
Obesity and Heart Failure: Introducing the Theme
by
Francesco Monitillo, Paolo Basile and Giuseppe Lisco
J. Cardiovasc. Dev. Dis. 2026, 13(4), 153; https://doi.org/10.3390/jcdd13040153 - 30 Mar 2026
Abstract
Obesity is a chronic, highly prevalent disease affecting nearly one-third of the global population and represents a major independent risk factor for heart failure (HF), particularly heart failure with preserved ejection fraction (HFpEF). Excess adiposity—especially visceral and epicardial adipose tissue (EAT)—acts as an
[...] Read more.
Obesity is a chronic, highly prevalent disease affecting nearly one-third of the global population and represents a major independent risk factor for heart failure (HF), particularly heart failure with preserved ejection fraction (HFpEF). Excess adiposity—especially visceral and epicardial adipose tissue (EAT)—acts as an active endocrine and immune organ, promoting chronic low-grade inflammation, oxidative stress, endothelial dysfunction, and adverse myocardial remodeling. Expanded EAT exerts both paracrine inflammatory effects and mechanical constraint on the myocardium, contributing to diastolic dysfunction, microvascular impairment, atrial arrhythmogenesis, and elevated filling pressures despite preserved systolic function. Evidence demonstrates a dose–response relationship between increasing body mass index and incident HF. Clinically, obesity-related HFpEF is characterized by concentric left ventricular hypertrophy, impaired relaxation, increased plasma volume, reduced exercise tolerance, and relatively low natriuretic peptide levels, complicating diagnosis. HF management includes traditional treatment with diuretics, renin-angiotensin system inhibitors, β-blockers, mineralocorticoid receptor antagonists, and angiotensin receptor-neprilysin inhibitors. These agents widely remain foundational as they primarily target hemodynamic and neurohormonal pathways in HF. In contrast, sodium–glucose cotransporter 2 inhibitors consistently reduce HF hospitalizations across the ejection fraction spectrum, while glucagon-like peptide-1 receptor agonists and dual incretin therapies (e.g., tirzepatide) promote substantial weight loss, improve symptoms, and demonstrate promising anti-remodeling effects in obesity-related HFpEF. Recognizing obesity-driven HF as a distinct cardiometabolic entity supports an integrated therapeutic strategy combining structured weight reduction with guideline-directed HF polypharmacotherapy to address both hemodynamic burden and upstream adiposity-related mechanisms.
Full article
(This article belongs to the Special Issue Obesity and Heart Failure)
►▼
Show Figures

Graphical abstract
Open AccessReview
Multimodal Imaging for Monitoring of Disease Progression in Cardiac Amyloidosis: Advances and Gaps in Evidence
by
Claudia Meier, Roja Soutodeh and Stephan Gielen
J. Cardiovasc. Dev. Dis. 2026, 13(4), 152; https://doi.org/10.3390/jcdd13040152 - 30 Mar 2026
Abstract
►▼
Show Figures
Among cardiac storage diseases, amyloidosis has emerged as a common cause of heart failure (HF), particularly in older people: it is diagnosed in up to 13–19% of patients with heart failure and preserved ejection fraction. Current treatments for transthyretin amyloidosis (ATTR) focus on
[...] Read more.
Among cardiac storage diseases, amyloidosis has emerged as a common cause of heart failure (HF), particularly in older people: it is diagnosed in up to 13–19% of patients with heart failure and preserved ejection fraction. Current treatments for transthyretin amyloidosis (ATTR) focus on stopping the misfolding of the TTR protein or reducing TTR production and treating the symptoms with cardiac medication, while systemic chemotherapy is the focus for light-chain amyloidosis (AL). New fibril clearance agents and gene therapies are currently in development. In addition to clinical and laboratory observations, multimodal imaging is essential for the monitoring of the effects of treatment on the progression of heart disease, but it is not yet included in established staging systems. This narrative review collects current multimodal imaging parameters that have been evaluated in clinical trials to assess the progression of cardiac amyloidosis and used in phase III intervention studies. These evolving findings are compared with current consensus recommendations to identify gaps in knowledge for specific imaging modalities, particularly cardiac MRI. Ultimately, the goal should be to standardize imaging of disease progression in cardiac amyloidosis so that the therapeutic effects of new pharmacological treatment options can be compared with the current standard of care.
Full article

Figure 1
Open AccessArticle
Prognostic Value of the RVFWLS/PASP Ratio in Pulmonary Arterial Hypertension
by
Hongjie Bian, Qinhua Zhao, Fengling Ju, Lan Wang, Yupei Han, Hongling Qiu, Cijun Luo, Pei Gang, Ke Li and Xumeng Ding
J. Cardiovasc. Dev. Dis. 2026, 13(4), 151; https://doi.org/10.3390/jcdd13040151 - 30 Mar 2026
Abstract
Background: The right ventricular free wall longitudinal strain to pulmonary arterial systolic pressure (RVFWLS/PASP) ratio is an emerging echocardiographic index for evaluating right ventricular–pulmonary artery (RV-PA) coupling. This study aimed to evaluate its prognostic significance and incremental value in risk stratification for patients
[...] Read more.
Background: The right ventricular free wall longitudinal strain to pulmonary arterial systolic pressure (RVFWLS/PASP) ratio is an emerging echocardiographic index for evaluating right ventricular–pulmonary artery (RV-PA) coupling. This study aimed to evaluate its prognostic significance and incremental value in risk stratification for patients with pulmonary arterial hypertension (PAH). Methods: We conducted a retrospective–prospective cohort study of 149 adult PAH patients (87 idiopathic PAH and 62 connective tissue disease-associated PAH). RVFWLS was measured via speckle tracking echocardiography, and PASP was estimated using Doppler. The primary endpoint was event-free survival, defined as the first occurrence of all-cause mortality, lung transplantation, or rehospitalization for right heart failure. Kaplan–Meier and multivariate Cox regression analyses were performed to identify independent predictors. Results: During a median follow-up of 32 months, 78 primary events occurred. Patients in the lower RVFWLS/PASP group (<0.246%/mmHg) exhibited significantly worse exercise capacity, higher NT-proBNP levels, and poorer hemodynamics compared with the higher group (≥0.246%/mmHg) (all p < 0.001). The event-free survival rate for the composite endpoint was significantly lower in the group with reduced RVFWLS/PASP compared with that observed in the higher RVFWLS/PASP group (log-rank p < 0.05). Multivariate Cox regression analysis demonstrated RVFWLS/PASP ≥ 0.246%/mmHg was independently predictive of reduced risk for the primary endpoint (HR = 0.46, 95%CI 0.23–0.93, p < 0.05). Moreover, RVFWLS/PASP facilitated additional risk stratification among patients classified as low risk based on established models (FPHN, COMPERA 2.0, and REVEAL Lite 2). Conclusions: RVFWLS/PASP is a robust, independent determinant of long-term prognosis in patients with PAH. As a noninvasive measure of RV-PA coupling, it provides significant incremental value for clinical risk assessment and treatment monitoring.
Full article
(This article belongs to the Special Issue Pulmonary Hypertension: Far from a Rare Disease—a Journey from Diagnosis to Treatment)
►▼
Show Figures

Figure 1
Open AccessReview
State-of-the-Art Definitive Femoropopliteal Lesion Treatment: A Case-Based Systematic Approach
by
Grigorios Korosoglou, Nasser Malyar, Andrej Schmidt, Michael Lichtenberg, Gerd Grözinger, Dittmar Böckler, Christian A. Behrendt, Erwin Blessing, Ralf Langhoff, Thomas Zeller and Christos Rammos
J. Cardiovasc. Dev. Dis. 2026, 13(4), 150; https://doi.org/10.3390/jcdd13040150 - 28 Mar 2026
Abstract
After vessel preparation, using different strategies such as balloon angioplasty, specialty balloons, atherectomy or intravascular lithotripsy, definitive treatment has emerged as a key feature in endovascular treatment strategies. Based on current guidelines, endovascular treatment is the most common treatment option in patients with
[...] Read more.
After vessel preparation, using different strategies such as balloon angioplasty, specialty balloons, atherectomy or intravascular lithotripsy, definitive treatment has emerged as a key feature in endovascular treatment strategies. Based on current guidelines, endovascular treatment is the most common treatment option in patients with claudication. In patients with chronic limb-threatening ischemia (CLTI), on the other hand, the best treatment modality, including bypass surgery and endovascular revascularization, needs to be selected by an interdisciplinary team, focusing on individual anatomic and patient-specific characteristics, on the availability of a vein graft and on cardiovascular and other comorbidities of the patients. With endovascular therapy, currently, a plethora of options are available for the treatment of femoropopliteal lesions, which are increasingly gaining in complexity. Therefore, a practical systematic case-based approach, entailing contemporary treatment options, like drug-coated balloon (DCB) angioplasty tools, self-expanding bare-metal stents (BMSs), drug-eluting stents (DESs), interwoven stents and covered stents, is crucial. Generally, most endovascular operators adhere to the ‘leave nothing behind’ concept, meaning that, after proper lesion preparation, lesions can be treated with DCBs, avoiding the implantation of permanent metallic implants. However, in the case of severe dissections or significant recoil, stent implantation becomes necessary to achieve adequate limb perfusion. The selection between long versus spot stenting and the different stent options depends on the current scientific evidence, guidelines and expert opinion statements. An interdisciplinary expert consensus was recently compiled on how these modalities should be used in specific lesions and patients in the femoropopliteal segment. Herein we present a practical case-based approach, which is based on this algorithm and aims at harmonization of endovascular treatment strategies in daily practice and ultimately at further improvements in limb and patient outcomes.
Full article
(This article belongs to the Section Cardiovascular Clinical Research)
►▼
Show Figures

Figure 1
Open AccessArticle
Estimated Pulse Wave Velocity as a Marker of Blood-Pressure-Dependent Arterial Load and Ventricular–Vascular Interaction in Severe Aortic Stenosis Before and After Transcatheter Aortic Valve Replacement
by
Simina Mariana Moroz, Alina Gabriela Negru, Mirela Baba, Silvia Luca, Mihaela Valcovici, Alina Maria Lupu, Darius Buriman, Daniel-Dumitru Nișulescu, Ana Lascu, Daniel Florin Lighezan and Ioana Mozos
J. Cardiovasc. Dev. Dis. 2026, 13(4), 149; https://doi.org/10.3390/jcdd13040149 - 25 Mar 2026
Abstract
Background: Severe aortic stenosis (AS) increases left ventricular afterload and disrupts ventricular–vascular coupling. Transcatheter aortic valve replacement (TAVR) promptly relieves valvular obstruction, but its immediate effects on blood pressure-dependent arterial load and ventricular–vascular interactions are not fully clarified. Estimated pulse wave velocity (ePWV),
[...] Read more.
Background: Severe aortic stenosis (AS) increases left ventricular afterload and disrupts ventricular–vascular coupling. Transcatheter aortic valve replacement (TAVR) promptly relieves valvular obstruction, but its immediate effects on blood pressure-dependent arterial load and ventricular–vascular interactions are not fully clarified. Estimated pulse wave velocity (ePWV), derived from age and mean arterial pressure, is a convenient surrogate of global arterial load. The study aimed to assess ePWV before and after TAVR and its relationship with ventricular function and inflammatory biomarkers. Methods: In this retrospective observational study, 100 elderly patients with severe AS undergoing TAVR underwent detailed clinical, laboratory, and echocardiographic assessments before and after the procedure. Arterial stiffness was quantified using ePWV, while left ventricular geometry and systolic function were evaluated by standard echocardiography. Post-procedural reassessment was performed at hospital discharge (median 8 days after TAVR). Results: TAVR led to a modest but significant reduction in ePWV (from 12.79 ± 1.54 to 12.39 ± 1.54 m/s, p < 0.01) and improvement in left ventricular ejection fraction (LVEF) (from 44.89 ± 9.2% to 46.7 ± 7.95%, p < 0.01). Higher baseline ePWV correlated with unfavorable left ventricular remodeling and systolic dysfunction, and post-procedural ePWV remained linked to right ventricular performance. Before TAVR, ePWV and LVEF were both associated with inflammatory biomarkers, relationships that disappeared after intervention. Conclusions: Overall, ePWV functioned as an integrated measure of ventricular–vascular interaction and global hemodynamic load, though its interpretation post-TAVR requires caution due to direct blood pressure dependence and confounding by acute procedural inflammation.
Full article
(This article belongs to the Special Issue Transcatheter and Surgical Approaches to Complications of Transcatheter Procedures: Current Trends and Future Challenges, 2nd Edition)
►▼
Show Figures

Figure 1
Open AccessReview
Between a Rock and a Hard Place: Balancing Embolic Stroke and Intracerebral Hemorrhage Risk in Left Atrial Appendage Occlusion
by
Juan Felipe Daza-Ovalle, Johanna Seiden, Daniel Labovitz, Erick Daniel Martinez, Deepti Athreya and Charles Esenwa
J. Cardiovasc. Dev. Dis. 2026, 13(3), 148; https://doi.org/10.3390/jcdd13030148 - 23 Mar 2026
Abstract
Patients with atrial fibrillation (AF) who are not candidates for long-term anticoagulation present a complex therapeutic dilemma due to competing risks of cardioembolic stroke and intracerebral hemorrhage (ICH). This challenge is particularly pronounced in neurologically vulnerable individuals, including those with prior ICH, cerebral
[...] Read more.
Patients with atrial fibrillation (AF) who are not candidates for long-term anticoagulation present a complex therapeutic dilemma due to competing risks of cardioembolic stroke and intracerebral hemorrhage (ICH). This challenge is particularly pronounced in neurologically vulnerable individuals, including those with prior ICH, cerebral amyloid angiopathy (CAA), or neuroimaging markers of cerebral small vessel disease (SVD). Left atrial appendage occlusion (LAAO) has emerged as an alternative stroke prevention strategy for patients with contraindications to anticoagulation; however, optimal patient selection and post-procedural antithrombotic management remain uncertain, largely because existing bleeding risk scores inadequately capture ICH risk. Most hemorrhagic risk scores were designed to estimate systemic bleeding and demonstrate limited ability to predict ICH, as they do not incorporate hemorrhage etiology or neuroimaging features. Importantly, ICH recurrence risk varies substantially by subtype, with the highest risk observed in CAA-related hemorrhage, the lowest in hypertensive SVD, and intermediate risk in mixed or secondary etiologies. These distinctions have direct implications for anticoagulation decisions and consideration of LAAO. Finally, we synthesize contemporary evidence on ICH risk stratification, neuroimaging biomarkers, and antithrombotic strategies following LAAO. We propose a multidisciplinary, evidence-based decision-making framework integrating clinical risk scores, neuroimaging findings, and hemorrhage phenotype to support individualized stroke prevention strategies in high-risk patients with AF.
Full article
(This article belongs to the Special Issue Controversies in Stroke and Cerebrovascular Disease)
►▼
Show Figures

Figure 1
Open AccessArticle
Vertical Right Axillary Thoracotomy for Repair of Ventricular Septal Defects in Infants and Children: Experience with 50 Consecutive Cases
by
Yasin Essa, Ali H. Mashadi, Joseph Giamelli, Alexander Mittnacht, Mahmoud I. Salem and Sameh M. Said
J. Cardiovasc. Dev. Dis. 2026, 13(3), 147; https://doi.org/10.3390/jcdd13030147 - 23 Mar 2026
Abstract
Objectives: Recently, there has been a growing interest in repairing congenital heart defects in children via right axillary thoracotomy. We sought to review our experience with ventricular septal defect closure through this approach. Patients and Methods: This is a retrospective single-center analysis of
[...] Read more.
Objectives: Recently, there has been a growing interest in repairing congenital heart defects in children via right axillary thoracotomy. We sought to review our experience with ventricular septal defect closure through this approach. Patients and Methods: This is a retrospective single-center analysis of 50 children who underwent closure of ventricular septal defects via vertical right axillary thoracotomy between March 2018 and February 2024. We reviewed the patients’ characteristics, perioperative and follow-up data. Results: The study included 26 (52%) girls with a median age of 7 (1–132) months. All patients underwent vertical right axillary thoracotomy with no conversion to sternotomy. Membranous ventricular septal defect was the most common diagnosis and was present in 43 (89%) patients. The median cardiopulmonary bypass and aortic cross clamp times were 96.5 (47–157) and 73 (30–114) min, respectively. In 45 (90%) of the patients, a patch was used. No early or late mortality. All patients were extubated in the operating room, and the median length of hospital stay was 2 (1–321) days. One early reoperation for bleeding, and one patient needed a permanent pacemaker. No late reoperations and all patients/parents were pleased with the incision. Conclusions: The outcomes of the right axillary thoracotomy for repairing ventricular septal defects in children are excellent. The approach is safe and is associated with superior cosmetic results and very short hospital stay. It should be strongly considered as an alternate to sternotomy for closure of ventricular septal defects.
Full article
(This article belongs to the Section Cardiac Surgery)
►▼
Show Figures

Figure 1
Open AccessArticle
Out-of-Hospital Cardiac Arrest in Southern Italy: A Retrospective Analysis of 11,653 Cases
by
Luca Gregorio Giaccari, Pasquale Sansone, Nicola D’Angelo, Daniele Antonaci, Eva Epifani, Luciana Mascia, Maria Caterina Pace, Vincenzo Pota and Gaetano Tammaro
J. Cardiovasc. Dev. Dis. 2026, 13(3), 146; https://doi.org/10.3390/jcdd13030146 - 23 Mar 2026
Abstract
(1) Background: Out-of-hospital cardiac arrest (OHCA) remains a major public health issue, with survival largely determined by the initial rhythm and timeliness of resuscitation. Comprehensive population-based data are essential for guiding prevention, emergency medical services (EMS) planning, and improving outcomes. (2) Methods: We
[...] Read more.
(1) Background: Out-of-hospital cardiac arrest (OHCA) remains a major public health issue, with survival largely determined by the initial rhythm and timeliness of resuscitation. Comprehensive population-based data are essential for guiding prevention, emergency medical services (EMS) planning, and improving outcomes. (2) Methods: We performed a retrospective observational study of all adult OHCA cases managed by EMS in Lecce (Italy) between January 2013 and March 2025. Demographics, arrest circumstances, initial rhythm, time intervals, and return of spontaneous circulation (ROSC) were analyzed across age, sex, temporal, and pandemic-related strata. Rhythm classification followed European Resuscitation Council guidelines. (3) Results: A total of 11,653 cases were analyzed (mean age 76.8 ± 15.5 years, 56.6% male). Asystole (AS) was the predominant rhythm (88.7%), followed by ventricular fibrillation (VF, 7.6%), pulseless electrical activity (PEA, 1.3%), and pulseless ventricular tachycardia (pVT, 0.08%). VF was more common in younger and male patients, while AS increased with age. Hour-level analysis revealed circadian peaks: VF in late afternoon and AS in early morning. Pandemic analysis showed reduced VF and increased AS during COVID-19, with partial recovery post-pandemic. ROSC occurred in 3.47% overall, strongly associated with shockable rhythms. EMS response times were stable across day–night and pandemic phases. (4) Conclusions: AS dominates OHCA presentations, especially among the elderly, whereas VF remains the strongest predictor of ROSC. Circadian variation at the hourly level suggests potential for EMS optimization. Pandemic-related shifts in rhythm highlight the vulnerability of the chain of survival to societal disruptions. Strengthening bystander CPR, expanding AED availability, and tailoring EMS strategies remain key priorities for improving OHCA outcomes.
Full article
(This article belongs to the Section Epidemiology, Lifestyle, and Cardiovascular Health)
►▼
Show Figures

Figure 1
Open AccessReview
Mechanical Circulatory Support in the Very Elderly Undergoing Complex High-Risk Indicated Procedures: A Case Report and Literature Review
by
Giuseppe Giacchi and Antonino Nicosia
J. Cardiovasc. Dev. Dis. 2026, 13(3), 145; https://doi.org/10.3390/jcdd13030145 - 20 Mar 2026
Abstract
Interventional treatment of very elderly patients with severe coronary artery disease is currently one of the central topics in interventional cardiology. Technological progress and increased life expectancy have made these patients appropriate candidates for contemporary standards of care, especially those with an active
[...] Read more.
Interventional treatment of very elderly patients with severe coronary artery disease is currently one of the central topics in interventional cardiology. Technological progress and increased life expectancy have made these patients appropriate candidates for contemporary standards of care, especially those with an active lifestyle. We hereby report the case of a 95-year-old patient hospitalized for acute myocardial infarction, who underwent a complex percutaneous coronary intervention with mechanical circulatory support. A literature review on mechanical circulatory support devices in older adults is also provided.
Full article
(This article belongs to the Special Issue Coronary Artery Disease: Risk Stratification and Optimization of Intervention Strategies)
►▼
Show Figures

Figure 1
Open AccessArticle
Single-Site Experience in the ONSET–OFFSET Study Demonstrates Pharmacodynamic and Pharmacokinetic Advantages of Ticagrelor over Clopidogrel in Patients with Chronic Coronary Syndromes
by
Heather M. Judge, William A. E. Parker and Robert F. Storey
J. Cardiovasc. Dev. Dis. 2026, 13(3), 144; https://doi.org/10.3390/jcdd13030144 - 20 Mar 2026
Abstract
The ONSET–OFFSET study was a multicentre study assessing the pharmacodynamic responses to ticagrelor and clopidogrel in aspirin-treated patients with chronic coronary syndromes. Recent concerns have been raised about the study methodology, including at the single United Kingdom (UK) site in Sheffield. Here, we
[...] Read more.
The ONSET–OFFSET study was a multicentre study assessing the pharmacodynamic responses to ticagrelor and clopidogrel in aspirin-treated patients with chronic coronary syndromes. Recent concerns have been raised about the study methodology, including at the single United Kingdom (UK) site in Sheffield. Here, we report data generated at this site along with additional analyses. The UK site recruited 40 out of 123 of the study participants. Platelet P2Y12 receptor inhibition was assessed using light transmission aggregometry and whole-blood methodologies. Samples were obtained during the onset and offset dosing periods. Percentage inhibition of platelet aggregation (%IPA) was calculated with (pre-specified) and without (post hoc) truncation of values [0, 100]. Study conduct was monitored by an external contract research organisation. The results from the UK site were concordant with the main study findings. %IPA at 2 h after ticagrelor loading: main study 88%, UK site 91% (truncated), UK site 91% (untruncated). %IPA correlated with other measures of P2Y12 inhibition (VerifyNow: p < 0.0001; VASP phosphorylation assay: p < 0.0001). One patient treated with ticagrelor had >2 h delay in the onset of platelet inhibition associated with co-administration of metformin. The primary endpoint for the offset period was also similar to the main study findings. The UK site data confirm the more rapid onset and offset of inhibitory effects and greater mean levels of platelet inhibition with ticagrelor compared with clopidogrel, regardless of the mode of %IPA data analysis. Study conduct was rigorously monitored in order to demonstrate the integrity and validity of the results. Metformin may delay the onset of action of a ticagrelor loading dose.
Full article
(This article belongs to the Section Acquired Cardiovascular Disease)
►▼
Show Figures

Graphical abstract

Journal Menu
► ▼ Journal Menu-
- JCDD Home
- Aims & Scope
- Editorial Board
- Reviewer Board
- Topical Advisory Panel
- Instructions for Authors
- Special Issues
- Topics
- Sections & Collections
- Article Processing Charge
- Indexing & Archiving
- Editor’s Choice Articles
- Most Cited & Viewed
- Journal Statistics
- Journal History
- Journal Awards
- Conferences
- Editorial Office
Journal Browser
► ▼ Journal BrowserHighly Accessed Articles
Latest Books
E-Mail Alert
News
Topics
Topic in
Cardiogenetics, Hearts, JCDD, JCM
Adult Congenital Heart Disease: Advances in Diagnosis, Surgery, and Lifelong Care
Topic Editors: Satoshi Akagi, Jin Young SongDeadline: 30 June 2026
Topic in
CIMB, IJMS, JCDD, Organoids, Biomedicines
Molecular and Cellular Mechanisms of Heart Disease
Topic Editors: Pasi Tavi, Ebru Arioglu-InanDeadline: 31 December 2026
Topic in
Antioxidants, Biomedicines, Disabilities, JCDD, Hearts, JCRM
Cardiovascular Disease in Special Populations: From Basic Science to Clinical Practice
Topic Editors: Song-Young Park, Gwenael LayecDeadline: 31 January 2027
Topic in
Biomedicines, CIMB, IJMS, IJTM, JCDD
Future Directions in Cardiology: How the Clinic Will Change in the Coming Years, the Laboratory Always Standing
Topic Editors: Cristina Vassalle, Melania GagginiDeadline: 28 February 2027

Conferences
Special Issues
Special Issue in
JCDD
Regenerative Medicine in Congenital Heart Disease—Current Status and Future Challenges
Guest Editor: Beatrijs BarteldsDeadline: 15 April 2026
Special Issue in
JCDD
Advances in Diagnosis and Interventional Therapy of Coronary Artery Disease
Guest Editors: Dario Buccheri, Stefano CangemiDeadline: 15 April 2026
Special Issue in
JCDD
Arrhythmic Risk Stratification, 2nd EditionGuest Editors: Marisa Varrenti, Patrizio MazzoneDeadline: 15 April 2026
Special Issue in
JCDD
Cardiovascular Disease and Nutrition
Guest Editor: Aivars LejnieksDeadline: 20 April 2026
Topical Collections
Topical Collection in
JCDD
Current Challenges in Heart Failure and Cardiac Transplantation
Collection Editors: Rasmus Rivinius, Daniel Oehler, Andreas J. Rieth, Andreas Doesch