Topical Advisory Panel applications are now closed. Please contact the Editorial Office with any queries.
Journal Description
Dermatopathology
Dermatopathology
is an international, peer-reviewed, open access journal on dermatopathology, published quarterly online. It is the official journal of the European Society of Dermatopathology (ESDP).
- Open Access— free for readers, with article processing charges (APC) paid by authors or their institutions.
- High visibility: indexed within ESCI (Web of Science), Scopus, PubMed, PMC, Embase, and other databases.
- Rapid Publication: manuscripts are peer-reviewed and a first decision is provided to authors approximately 32.6 days after submission; acceptance to publication is undertaken in 6.8 days (median values for papers published in this journal in the second half of 2025).
- Recognition of Reviewers: APC discount vouchers, optional signed peer review, and reviewer names published annually in the journal.
Impact Factor:
1.7 (2024);
5-Year Impact Factor:
1.5 (2024)
Latest Articles
Pedunculated Acral Keratotic Papule on an Ischemic Foot
Dermatopathology 2026, 13(2), 18; https://doi.org/10.3390/dermatopathology13020018 - 21 Apr 2026
Abstract
►
Show Figures
An 86-year-old man presented with a slowly enlarging, subject to chronic mechanical irritation, pedunculated keratotic papule on the plantar tip of the right hallux in the setting of severe peripheral arterial disease. Excision was deferred until after endovascular revascularization to reduce the risk
[...] Read more.
An 86-year-old man presented with a slowly enlarging, subject to chronic mechanical irritation, pedunculated keratotic papule on the plantar tip of the right hallux in the setting of severe peripheral arterial disease. Excision was deferred until after endovascular revascularization to reduce the risk of nonhealing and limb complications, after which the lesion was removed without wound sequelae. Histopathology demonstrated a conical papule with a central collagenous core and an overlying cap of compact hyperkeratosis. This case highlights key clinicopathologic features that distinguish acral keratotic tumors and underscores the importance of perfusion optimization when planning elective excision on an ischemic limb.
Full article
Open AccessArticle
Desmosomal-Type Acantholysis—A New Histologic Pattern Related to Mutations of Genes for Desmosomal Proteins
by
Dieter Metze, Kira Süßmuth, Clemens Metze, Vinzenz Oji and Heiko Traupe
Dermatopathology 2026, 13(2), 17; https://doi.org/10.3390/dermatopathology13020017 - 3 Apr 2026
Abstract
Desmosomes are specialized cell–cell junctions that play a crucial role in maintaining the structural integrity of both cornifying and non-cornifying epithelium. Disruption of desmosomal cohesion in autoimmune, infectious, and other diseases is typically associated with acantholysis, often leading to intraepidermal blisters and erosions.
[...] Read more.
Desmosomes are specialized cell–cell junctions that play a crucial role in maintaining the structural integrity of both cornifying and non-cornifying epithelium. Disruption of desmosomal cohesion in autoimmune, infectious, and other diseases is typically associated with acantholysis, often leading to intraepidermal blisters and erosions. In recent decades, genetic mutations have been identified that impair desmosomal integrity to varying degrees, giving rise to a spectrum of genodermatoses. These conditions, which include palmoplantar keratoderma, epidermolysis bullosa, and ichthyoses, can range from mild to severe, with some forms being syndromic and life-threatening. We investigated dermatopathologic changes in patients with mutations in genes encoding desmosomal proteins seen in consultations at our genodermatoses unit. A series of cases, including keratosis palmoplantaris areata et striata (striated palmoplantar keratoderma type 1), Carvajal–Huerta syndrome, severe dermatitis–multiple allergies–metabolic wasting (SAM) syndrome, ectodermal dysplasia–skin fragility syndrome, and inflammatory peeling skin disease, was examined histologically and, when necessary, immunohistochemically. Findings from our cohort were compared with histopathological consultation cases from our dermatopathology laboratory and previously published cases in the literature. Through these observations, we defined a distinct form of acantholysis associated with desmosomal protein mutations, which we term “desmosomal-type acantholysis.” We outline the spectrum of this newly characterized pattern and highlight its differences from conventional forms of acantholysis. Furthermore, for the first time, we describe incidental cases where “desmosomal-type acantholysis” appears sporadically in solitary acanthoma and in association with a melanocytic nevus.
Full article
(This article belongs to the Special Issue New Insights in Paediatric Dermatopathology 2025)
►▼
Show Figures

Figure 1
Open AccessArticle
Bilateral Auricular Blastomycosis-like Pyoderma: A Rare Presentation Histologically Misinterpreted as Squamous Cell Carcinoma
by
Nazario Pesce, Giorgia Di Marco, Giorgio Stabile, Antonio Podo Brunetti, Alessandro Russo, Stefania Guida and Rongioletti Franco
Dermatopathology 2026, 13(2), 16; https://doi.org/10.3390/dermatopathology13020016 - 1 Apr 2026
Abstract
►▼
Show Figures
Blastomycosis-like pyoderma (BLP) is a rare chronic inflammatory dermatosis characterized by exuberant vegetative and verrucous plaques, most frequently associated with bacterial colonization, particularly Staphylococcus aureus. Owing to its striking clinical and histopathological resemblance to squamous cell carcinoma (SCC) and other granulomatous or
[...] Read more.
Blastomycosis-like pyoderma (BLP) is a rare chronic inflammatory dermatosis characterized by exuberant vegetative and verrucous plaques, most frequently associated with bacterial colonization, particularly Staphylococcus aureus. Owing to its striking clinical and histopathological resemblance to squamous cell carcinoma (SCC) and other granulomatous or hyperplastic dermatoses, BLP represents a well-recognized diagnostic pitfall, often leading to delayed diagnosis or unnecessary surgical management. We report an unusual case of bilateral auricular BLP in a 58-year-old apparently immunocompetent woman, initially misdiagnosed as SCC. Comprehensive clinicopathological reassessment revealed pseudoepitheliomatous hyperplasia, intraepidermal neutrophilic microabscesses, and a dense mixed inflammatory infiltrate, findings consistent with a reactive rather than neoplastic process. Microbiological cultures confirmed Staphylococcus aureus, supporting the final diagnosis of BLP and guiding effective antimicrobial therapy. To better contextualize this rare presentation, we reviewed all previously reported cases of BLP, summarizing available clinical, histopathological, microbiological, and therapeutic data. This case further raises the possibility of an association between BLP and systemic inflammatory conditions, as the patient subsequently developed severe colitis, highlighting the potential role of immune dysregulation and the gut–skin axis in disease pathogenesis or a possible temporal association, without allowing causal inference. Beyond inflammatory bowel disease, blastomycosis-like pyoderma has been reported in association with a variety of systemic and immune-mediated conditions, including diabetes mellitus, hematologic malignancies, HIV infection, chronic renal failure, autoimmune disorders, and prolonged immunosuppressive therapies. These associations support the concept that BLP represents a hyperinflammatory reaction pattern occurring in the setting of altered immune surveillance rather than a purely infectious disease. Accurate recognition and management of BLP require careful integration of clinical features, histological findings, and microbiological results. Increased awareness of its diverse presentations is essential to avoid misdiagnosis and to ensure appropriate, conservative treatment.
Full article

Figure 1
Open AccessArticle
Comprehensive Genomic Profiling of Cutaneous Adnexal Carcinomas: A Genomic Landscape Study
by
Maroun Bou Zerdan, Kevin T. Jamouss, Alexandre Maalouf, Rita Moukarzel, Tanishq Chhabra, Daniel J. Zaccarini, Dean Pavlick, Natalie Danziger and Jeffrey Ross
Dermatopathology 2026, 13(2), 15; https://doi.org/10.3390/dermatopathology13020015 - 30 Mar 2026
Abstract
►▼
Show Figures
Cutaneous adnexal carcinomas (CACs) comprise a diverse group of malignant tumors that show morphological differentiation toward one of the four main adnexal structures in normal skin: hair follicles, sebaceous glands, sweat-apocrine glands, and sweat-eccrine glands. These tumors can arise sporadically or may be
[...] Read more.
Cutaneous adnexal carcinomas (CACs) comprise a diverse group of malignant tumors that show morphological differentiation toward one of the four main adnexal structures in normal skin: hair follicles, sebaceous glands, sweat-apocrine glands, and sweat-eccrine glands. These tumors can arise sporadically or may be associated with rare genetic syndromes. A total of 276 CACs cases underwent hybrid capture-based comprehensive genomic profiling (CGP) to assess all classes of genomic alterations (GA). Sequencing data were used to determine microsatellite instability (MSI) status, tumor mutational burden (TMB), genomic loss of heterozygosity (gLOH), genomic ancestry, and COSMIC mutational signatures. PD-L1 expression was evaluated by immunohistochemistry (TPS; Dako 22C3). Statistical analyses were performed using Fisher’s exact test, with false discovery rate correction via the Benjamini–Hochberg method. Sequencing was performed on primary cutaneous tumors in 131 cases (47.4%) and on local recurrence or metastatic site biopsies in 145 cases (52.5%). Across all groups, there was a male predominance (64–81%) and similar mean ages (59–63 years), with apocrine (APO) tumors occurring in older patients than eccrine (ECC) tumors (72 vs. 62 years; p = 0.001). Histologically, 173 tumors (62.7%) were sweat gland-derived (SWT), 55 (19.9%) sebaceous gland-derived (SEB), 14 (5.1%) hair follicle-derived (HRF), and 34 (12.3%) unclassified (UNK). Among SWT tumors, 150 (86.7%) were eccrine and 23 (13.3%) apocrine. SWT tumors included digital papillary adenocarcinomas (DPA, 6.9%), mucinous carcinomas (MC, 6.3%), porocarcinomas (POR, 11.0%), spiradenocarcinomas (SPR, 8.1%), syringoadenocarcinomas (SRNG, 5.8%), and 77 (44.5%) unclassified cases. The number of GA per tumor was highest in SEB compared with SWT tumors (7.9 vs. 4.9; p = 0.005) and lowest in DPA (2.1 vs. 5.0 in non-DPA; p = 0.03). No differences in ancestry distribution were observed. Compared with SWT tumors, SEB tumors exhibited higher frequencies of RB1 (38.2% vs. 8.1%; p < 0.0001) and TP53 alterations (76.4% vs. 43.4%; p = 0.0002), suggesting potential neuroendocrine differentiation. MC tumors showed significantly higher PTCH1 alterations than non-MC tumors (36.4% vs. 1.8%; p = 0.044). MSI-high status was most frequent in SEB tumors compared with all other groups (15.7% vs. 1.2%; p = 0.005), and gLOH > 16% was also more common in SEB than SWT tumors (19.6% vs. 7.2%; p = 0.081). The MMR signature occurred more frequently in SEB than SWT tumors (32.0% vs. 2.1%; p = 0.005). Mean TMB was elevated across most CACs types, ranging from 10.4 mutations/Mb in HRF to 38.8 mutations/Mb in MC, with the exceptions of APO (2.7 mut/Mb; p = 0.001) and DPA (1.4 mut/Mb; p = 0.003). PD-L1 expression was generally low and did not differ significantly between SWT and SEB tumors (37.0% vs. 33.3%; NS). Given the limited data on CAC treatment, this study provides a catalog of commonly observed GA. SEB tumors exhibited the highest frequency of genomic alterations. Prospective clinical trials are needed to determine the prognostic and predictive value of CAC-specific biomarkers for immune checkpoint inhibitor (ICI) response, which is essential for integrating novel therapies into the evolving treatment landscape.
Full article

Figure 1
Open AccessArticle
PRAME Expression in Melanoacanthomas: Expanding the Spectrum of Positive Melanocytes in Sun-Exposed Skin
by
Francesco Fortarezza, Anna Poputchikova, Federica Pezzuto, Christian Ciolfi, Vincenza Guzzardo, Paolo Del Fiore, Gerardo Cazzato, Franco Bassetto, Mauro Alaibac and Angelo Paolo Dei Tos
Dermatopathology 2026, 13(1), 14; https://doi.org/10.3390/dermatopathology13010014 - 23 Mar 2026
Abstract
►▼
Show Figures
PRAME (Preferentially Expressed Antigen in Melanoma) is increasingly used as an immunohistochemical marker in the evaluation of melanocytic lesions; however, its expression in benign melanocytic proliferations remains incompletely characterized. This study investigated PRAME expression in melanoacanthomas, with particular emphasis on its relationship with
[...] Read more.
PRAME (Preferentially Expressed Antigen in Melanoma) is increasingly used as an immunohistochemical marker in the evaluation of melanocytic lesions; however, its expression in benign melanocytic proliferations remains incompletely characterized. This study investigated PRAME expression in melanoacanthomas, with particular emphasis on its relationship with ultraviolet exposure and chronic solar damage. A consecutive series of melanoacanthomas was retrospectively analyzed. Melanocytes were identified and quantified using SOX10 immunohistochemistry, while PRAME-positive melanocytes were counted and graded semiquantitatively according to nuclear staining intensity. PRAME expression was correlated with lesion site (photoexposed versus non-photoexposed skin) and with the degree of solar elastosis. Eighty-four cases were evaluated, of which 25 (29.8%) showed at least focal PRAME positivity in melanocytes. Overall melanocytic density assessed by SOX10 did not differ significantly between photoexposed and non-photoexposed lesions. Similarly, stratification based on total PRAME-positive melanocyte counts, irrespective of staining intensity, revealed no significant association with photoexposure. In contrast, analysis restricted to melanocytes with strong nuclear PRAME expression demonstrated a significant enrichment in photoexposed lesions compared with non-photoexposed sites (p < 0.01). Moreover, high-intensity PRAME expression showed a positive association with increasing grades of solar elastosis. These findings indicate that strong PRAME expression in melanoacanthoma could be associated with chronic sun damage and may reflect non-specific, ultraviolet-related modulation rather than malignant transformation, underscoring the importance of contextual interpretation of PRAME immunohistochemistry in diagnostic practice.
Full article

Figure 1
Open AccessReview
Longitudinal Melanonychia in Children: Clinical and Histopathologic Features and Management with Literature Update
by
Isabelle Moulonguet, Marie Caucanas and Sophie Goettmann
Dermatopathology 2026, 13(1), 13; https://doi.org/10.3390/dermatopathology13010013 - 23 Mar 2026
Abstract
Longitudinal melanonychia (LM) results from the deposition of pigment in the nail plate due to increased melanocytic activity within the nail matrix. Recent publications on this topic have helped clarify the main clinical, histological, and evolutionary characteristics of pediatric LM and provide guidance
[...] Read more.
Longitudinal melanonychia (LM) results from the deposition of pigment in the nail plate due to increased melanocytic activity within the nail matrix. Recent publications on this topic have helped clarify the main clinical, histological, and evolutionary characteristics of pediatric LM and provide guidance for its appropriate management. In this review, we will examine the literature on the subject. LM is far less common in children than in adults and is most often caused by benign nail matrix lesions. Pediatric LM has specific clinical and histopathologic features, and many of the clinical warning signs used in adults are not applicable to children. Pediatric lesions may show atypical cytologic and even architectural features yet still follow a benign clinical course. Spontaneous regression of LM is common in children, with fading and narrowing of the pigmented band, or even complete disappearance. The vast majority of pediatric LM cases can be managed conservatively with regular follow-up, including clinical photography and onychoscopy.
Full article
(This article belongs to the Special Issue New Insights in Paediatric Dermatopathology 2025)
►▼
Show Figures

Figure 1
Open AccessReview
Genital Disorders in Children: What Does a Biopsy Bring?
by
Francoise Plantier and Fiona Lewis
Dermatopathology 2026, 13(1), 12; https://doi.org/10.3390/dermatopathology13010012 - 23 Mar 2026
Abstract
Biopsies are only performed in less than 1% of all consultations dedicated to paediatric genital dermatology. The objectives of this paper are to review and clarify the histopathological features of the conditions most often biopsied: first, lichen sclerosus, which has a peak incidence
[...] Read more.
Biopsies are only performed in less than 1% of all consultations dedicated to paediatric genital dermatology. The objectives of this paper are to review and clarify the histopathological features of the conditions most often biopsied: first, lichen sclerosus, which has a peak incidence in childhood and progresses over years; secondly, pigmented lesions, including atypical genital naevi and common naevi in the context of lichen sclerosus, both histologically differential diagnoses of melanoma, which probably does not present in childhood. And finally, Crohn’s disease, which is a cause of vulval oedema or genital ulceration.
Full article
(This article belongs to the Special Issue New Insights in Paediatric Dermatopathology 2025)
►▼
Show Figures

Figure 1
Open AccessCase Report
Cutaneous Granular Cell Tumor with Overlying Hypertrichosis in an Adult: A Rare Case Report
by
Yara Alhusaini, Abdulaziz Almufadhi, Naif Alzahrani, Nawaf Alqahtani and Ohoud Aljarbou
Dermatopathology 2026, 13(1), 11; https://doi.org/10.3390/dermatopathology13010011 - 20 Mar 2026
Abstract
Granular cell tumors are uncommon neoplasms of neural origin that may involve the skin and often present with nonspecific clinical features, making diagnosis challenging. Cutaneous granular cell tumors rarely exhibit overlying hypertrichosis, a finding that may obscure their clinical recognition. In this report,
[...] Read more.
Granular cell tumors are uncommon neoplasms of neural origin that may involve the skin and often present with nonspecific clinical features, making diagnosis challenging. Cutaneous granular cell tumors rarely exhibit overlying hypertrichosis, a finding that may obscure their clinical recognition. In this report, we describe a rare case of a primary cutaneous granular cell tumor with prominent overlying terminal hair growth in an adult patient. A 27-year-old woman presented with a slowly enlarging, firm, pigmented plaque on the upper back associated with pruritus and increased hair growth. Histopathologic examination revealed sheets of large polygonal cells with abundant granular eosinophilic cytoplasm, and immunohistochemical staining was positive for S100, SOX10, CD68, and calretinin, confirming the diagnosis. The lesion was completely excised with no evidence of malignancy. To our knowledge, this represents the second reported instance of a cutaneous granular cell tumor associated with hypertrichosis and the first described in an adult. It underscores the importance of clinicopathologic correlation in evaluating unusual cutaneous lesions and expands the spectrum of recognized presentations of cutaneous granular cell tumors.
Full article
(This article belongs to the Section Clinico-Pathological Correlation in Dermatopathology)
►▼
Show Figures

Figure 1
Open AccessCase Report
A Case of Recurrent Chromoblastomycosis Treated with Multiple Surgical Management Options
by
Madeleine Kelly, Crystal Williams and Robert Miller
Dermatopathology 2026, 13(1), 10; https://doi.org/10.3390/dermatopathology13010010 - 18 Mar 2026
Abstract
►▼
Show Figures
Chromoblastomycosis is a chronic mycosis of the skin and subcutaneous tissue typically caused by traumatic inoculation of dematiaceous fungi of the Herpotrichiellaceae. A 59-year-old male presented with a 12-month history of an asymmetrical, scaly plaque on the left forearm that has been
[...] Read more.
Chromoblastomycosis is a chronic mycosis of the skin and subcutaneous tissue typically caused by traumatic inoculation of dematiaceous fungi of the Herpotrichiellaceae. A 59-year-old male presented with a 12-month history of an asymmetrical, scaly plaque on the left forearm that has been slowly increasing in size. Past medical history included atrial fibrillation on apixaban, hypertension and a cardiac stent. A 4 mm punch biopsy of the left forearm revealed superficial dermal fibrosis with mild pseudoepitheliomatous hyperplasia and granulomatous inflammation with scattered multinucleate histiocytes. There were giant cells with dark brown, somewhat round, yeast-like structures, some with internal septation exhibiting moderate staining for PAS, compatible with Medlar bodies suggestive of chromoblastomycosis. The patient was on rosuvastatin, rendering itraconazole not a possible treatment option, and instead the patient underwent curettage and cautery with two bouts of cryotherapy freeze and thaw cycles. A twelve-month follow-up noted a crusted area on the distal aspect of the scar. A shave biopsy of this area revealed pigmented organisms suggesting a recurrence of chromoblastomycosis. A further excisional biopsy was performed, with no evidence of chromoblastomycosis. This case highlights multiple surgical options for the management of chromoblastomycosis in patients where medical management is contraindicated. It highlights the therapeutic challenge of this disease due to frequent recurrence of lesions and that repeat biopsy may be efficacious in monitoring for recurrence.
Full article

Figure 1
Open AccessArticle
Defining Histological Patterns in Inherited Ichthyoses: Toward a Diagnostic Algorithm Based on 66 Confirmed Cases
by
Kira Süßmuth, Vinzenz Oji, Jacqueline Bodes, Isabelle Jochum, Florian Muhs, Katalin Komlosi, Ingrid Hausser, Matthias Schmuth, Heiko Traupe, Judith Fischer and Dieter Metze
Dermatopathology 2026, 13(1), 9; https://doi.org/10.3390/dermatopathology13010009 - 28 Feb 2026
Cited by 1
Abstract
Background: Inherited ichthyoses are a heterogeneous group of disorders of cornification caused by mutations in genes encoding epidermal proteins. Clinically, patients with ichthyosis present with erythema, scaling, and occasionally blistering; some subtypes are syndromic. Accurate and timely diagnosis is essential for appropriate management
[...] Read more.
Background: Inherited ichthyoses are a heterogeneous group of disorders of cornification caused by mutations in genes encoding epidermal proteins. Clinically, patients with ichthyosis present with erythema, scaling, and occasionally blistering; some subtypes are syndromic. Accurate and timely diagnosis is essential for appropriate management and genetic counseling. Objectives: Diagnosis of ichthyosis typically relies on a combination of clinical features, histopathological and ultrastructural findings, immunohistochemistry, and molecular genetic testing. Dermatopathology can be particularly valuable in three diagnostic scenarios: (i) when the clinical diagnosis of ichthyosis is evident, but the specific subtype remains unclear; (ii) when differential diagnoses such as inflammatory dermatoses need to be excluded; and (iii) when molecular testing is unavailable or yields variants of uncertain significance. However, definitive classification according to current nomenclature requires molecular confirmation. Methods: Despite being a routine diagnostic tool in dermatology, histopathological criteria for ichthyoses remain ill-defined and diagnostically challenging. In this retrospective study, we systematically assessed histological features in 66 patients with confirmed ichthyosis. Results: Our analysis revealed six distinct histological patterns. Based on these, we propose a pattern-based diagnostic algorithm to support the histological classification of ichthyosis subtypes. Limitations: Although some rare subtypes were underrepresented, this cohort represents the largest and most heterogeneous group of molecularly confirmed ichthyosis cases analyzed histologically to date. Conclusions: Our findings highlight the diagnostic value of skin biopsies in inherited ichthyoses. The delineation of characteristic histological patterns and the development of a diagnostic algorithm may facilitate more accurate subtype identification, particularly in settings where genetic testing is limited or inconclusive.
Full article
(This article belongs to the Section Clinico-Pathological Correlation in Dermatopathology)
►▼
Show Figures

Figure 1
Open AccessCase Report
The Unusual Invader in a Patient with Long-Standing Rheumatoid Arthritis: A Case of Leishmania major Colonization of Rheumatoid Nodules
by
Monia Di Prete, Viviana Lora, Arianna Lamberti, Alessandra Latini and Carlo Cota
Dermatopathology 2026, 13(1), 8; https://doi.org/10.3390/dermatopathology13010008 - 27 Jan 2026
Cited by 1
Abstract
Rheumatoid nodules are the most common extra-articular manifestation of rheumatoid arthritis. Long-term immunomodulatory therapies, including corticosteroids, used in the management of rheumatoid arthritis are associated with a higher risk of infections. Leishmaniasis is a neglected protozoal infection that may arise in these patients.
[...] Read more.
Rheumatoid nodules are the most common extra-articular manifestation of rheumatoid arthritis. Long-term immunomodulatory therapies, including corticosteroids, used in the management of rheumatoid arthritis are associated with a higher risk of infections. Leishmaniasis is a neglected protozoal infection that may arise in these patients. Cutaneous presentation is the most common and is characterized by a wide spectrum of clinical manifestations and courses, depending on the interplay between species involved and the host’s immune response. Here, we report the rare and intriguing case of a patient with long-standing rheumatoid arthritis, chronically treated with systemic prednisone, whose rheumatoid nodules were colonized by Leishmania major. In this context, therapeutic strategies must be tailored to species and patient factors. This report expands the differential diagnosis of rheumatoid nodule, highlighting the importance of considering opportunistic infections in exuberant presentations, particularly in immunosuppressed patients coming from or travelling in endemic regions. Intracellular pathogens may exploit the localized immunological niche represented by the rheumatoid nodule of an immunocompromised host to survive and replicate undisturbed. It also underscores the value of the clinico-pathological correlation and the importance of integrating molecular analyses to identify unexpected microorganisms that can be hidden by concomitant disease, avoiding misdiagnosis, ensuring timely treatment, and improving patients outcomes.
Full article
(This article belongs to the Section Clinico-Pathological Correlation in Dermatopathology)
►▼
Show Figures

Figure 1
Open AccessReview
Behçet-like Syndromes: A Comprehensive Review
by
Gaia Mancuso, Igor Salvadè, Adam Ogna, Brenno Balestra and Helmut Beltraminelli
Dermatopathology 2026, 13(1), 7; https://doi.org/10.3390/dermatopathology13010007 - 16 Jan 2026
Abstract
Background: Behçet-like syndrome (BLS) refers to the presence of Behçet’s disease (BD) features occurring in association with distinct clinical–pathological conditions such as inborn errors of immunity, myeloproliferative disorders, infections, or drug exposure. BLS may differ clinically from BD and is increasingly recognized as
[...] Read more.
Background: Behçet-like syndrome (BLS) refers to the presence of Behçet’s disease (BD) features occurring in association with distinct clinical–pathological conditions such as inborn errors of immunity, myeloproliferative disorders, infections, or drug exposure. BLS may differ clinically from BD and is increasingly recognized as a separate entity. Distinguishing BLS from primary BD is essential for appropriate management, and studying BLS may provide insights into BD pathogenesis. Objectives: To summarize clinical features, treatments, and genetic abnormalities reported in BLS, we reviewed all published cases up to January 2024. Methods: A systematic search of PubMed, Scopus, and Embase was performed using the terms “Behçet-like syndrome”, “Behçet-like disease”, and “Pseudo-Behçet disease”. We included English-language reports of patients > 12 years old with a defined underlying etiology and Behçet-like manifestations, defined by ≥2 ICBD criteria and/or gastrointestinal involvement, mucosal ulcers, thrombosis, or non-recurrent disease. Epidemiological, clinical, laboratory, histological, and treatment data were extracted and analyzed descriptively. Results: Of 679 publications, 53 met inclusion criteria, comprising 100 patients with BLS. The median age was 44 years (IQR 22–52), with a female predominance (1:2). Fifty-three percent were from non-European countries. A genetic disorder was identified in 70% of cases, while HLA-B51 was present in 10%. Frequent manifestations included skin lesions (68%), fever (56%), intestinal involvement (43%), and joint symptoms (43%). Treatments included glucocorticoids (65%), conventional DMARDs (32%), and biologics (22%), mainly anti-TNF agents. Antiviral/antibiotic therapy was used in 9% and chemotherapy in 15%. Two patients with trisomy-8 MDS underwent allogeneic stem cell transplantation. Conclusions: Diverse conditions—including monogenic diseases, immune defects, myeloproliferative disorders, infections, and drug-related reactions—can produce Behçet-like features. Our findings highlight differences in clinical expression and treatment response across BLS etiologies. Recognizing BLS is essential for appropriate management and may contribute to a deeper understanding of BD pathogenesis and future targeted therapies.
Full article
(This article belongs to the Section Clinico-Pathological Correlation in Dermatopathology)
►▼
Show Figures

Figure 1
Open AccessSystematic Review
Tumor Infiltrating Lymphocytes in Cutaneous Squamous Cell Carcinoma—A Systematic Review
by
Li Yang Loo, Shi Huan Tay and Choon Chiat Oh
Dermatopathology 2026, 13(1), 6; https://doi.org/10.3390/dermatopathology13010006 - 13 Jan 2026
Abstract
►▼
Show Figures
Cutaneous squamous cell carcinoma (cSCC) is an immunogenic malignancy with variable immune infiltration and inconsistent responses to checkpoint blockade. Tumor-infiltrating lymphocytes (TILs) influence tumor progression and therapeutic outcome, yet their phenotypic and functional diversity across disease contexts remains incompletely understood. This review systematically
[...] Read more.
Cutaneous squamous cell carcinoma (cSCC) is an immunogenic malignancy with variable immune infiltration and inconsistent responses to checkpoint blockade. Tumor-infiltrating lymphocytes (TILs) influence tumor progression and therapeutic outcome, yet their phenotypic and functional diversity across disease contexts remains incompletely understood. This review systematically characterizes the TIL landscape in human cSCC. Following PRISMA 2020 guidelines, PubMed and Embase were searched up to May 2025 and restricted to studies evaluating tumor-infiltrating lymphocytes in human cSCC, using the modified Newcatle–Ottawa score to assess risk of bias. Data were synthesized qualitatively given methodological heterogeneity. 48 studies met inclusion criteria. cSCCs exhibited dense CD3+ infiltrates composed of cytotoxic (CD8+GzmB+, Ki-67+, CD69+) and regulatory (FOXP3+, CCR4+) subsets. Higher CD8+ activity correlated with smaller tumors and longer disease-free survival, whereas FOXP3+ enrichment and TGF-β2 signaling promoted immune evasion. Immunosuppressed patients demonstrated diminished CD8+ density and clonality. Immune modulation with PD-1/PD-L1 blockade, imiquimod, HPV vaccination, or OX40 stimulation enhanced effector function. The cSCC immune microenvironment reflects a balance between cytotoxic and suppressive factors. Harmonizing multimodal immune profiling and integrating spatial context with systemic immune status may advance both prognostic stratification and therapeutic design.
Full article

Figure 1
Open AccessArticle
The Need for Standardization of PRAME Immunohistochemistry in Melanocytic Neoplasms
by
Calla M. Sullivan, Dominick DiMaio, Scott Lauer, Dinesh Pradhan, Julie Youngs, Kaeli Samson and Corey J. Georgesen
Dermatopathology 2026, 13(1), 5; https://doi.org/10.3390/dermatopathology13010005 - 31 Dec 2025
Abstract
►▼
Show Figures
Accurate diagnosis of melanomas is crucial for proper evaluation and treatment. One immunohistochemical stain frequently utilized is PRAME (PReferentially expressed Antigen in MElanoma), a tumor-associated antigen expressed in most melanomas. This study aims to evaluate the reproducibility of PRAME scoring performed by dermatopathologists
[...] Read more.
Accurate diagnosis of melanomas is crucial for proper evaluation and treatment. One immunohistochemical stain frequently utilized is PRAME (PReferentially expressed Antigen in MElanoma), a tumor-associated antigen expressed in most melanomas. This study aims to evaluate the reproducibility of PRAME scoring performed by dermatopathologists at an academic tertiary referral medical center. A blinded survey was designed featuring 21 melanocytic neoplasms stained with PRAME and H&E. For each case, five dermatopathologists provided a PRAME score from 0–4+, percent PRAME positivity, values for H-score, and a descriptive interpretation. Absolute agreement across raters was assessed using a Kappa statistic for PRAME score and intraclass correlations (ICCs) for H-score and PRAME percentage. Statistical analysis indicated poor inter-rater reliability for PRAME score (Kappa = 0.16), percent PRAME positivity (ICC = 0.31), and H-score (ICC = 0.40). Reporting language varied among pathologists. Our study demonstrated that the interpretation of PRAME immunohistochemistry lacks reproducibility, especially for challenging lesions. This suggests that a more rigorous, defined, and reproducible scoring method should be investigated for equivocal cases. Future studies may explore the utility of artificial intelligence software in the interpretation of PRAME for borderline lesions to improve reliability and standardize scoring.
Full article

Figure 1
Open AccessCase Report
Deeply Pigmented Reticulated Acanthoma with Sebaceous Differentiation Mimicking Cutaneous Malignancy: A Case Report and Review of the Literature
by
Padol Chamninawakul, Xiaotian Wu and Joyce S. S. Lee
Dermatopathology 2026, 13(1), 4; https://doi.org/10.3390/dermatopathology13010004 - 30 Dec 2025
Abstract
►▼
Show Figures
Reticulated acanthoma with sebaceous differentiation (RASD) is a rare, benign cutaneous neoplasm. Its variable clinical presentation frequently mimics both benign and malignant entities, posing a significant diagnostic challenge. We report a case of pigmented RASD in a 78-year-old Malay male of Fitzpatrick skin
[...] Read more.
Reticulated acanthoma with sebaceous differentiation (RASD) is a rare, benign cutaneous neoplasm. Its variable clinical presentation frequently mimics both benign and malignant entities, posing a significant diagnostic challenge. We report a case of pigmented RASD in a 78-year-old Malay male of Fitzpatrick skin type IV who presented with a 5-year history of an 8 × 5 mm deeply pigmented, asymmetrical nodule on the left upper back, with a 2 mm central raised area showing less pigmentation. The lesion was clinically suspicious for malignant melanoma. Histopathological examination revealed characteristic features of RASD: a broad, plate-like, reticulated and pigmented epidermal proliferation with clusters of mature sebocytes at the bases of anastomosing rete ridges. Following biopsy confirmation, the residual lesion is being managed conservatively with observation. This case demonstrates an unusual heavily pigmented clinical presentation that completely obscured the typical yellowish hue associated with sebaceous differentiation, highlighting pigmented RASD as an important diagnostic pitfall in patients with skin of color. In conclusion, RASD should be included in the differential diagnosis of pigmented cutaneous lesions, especially in patients with skin of color. Recognition of this benign entity can prevent unnecessary aggressive surgical intervention.
Full article

Figure 1
Open AccessArticle
Hypothetical Abductive Reasoning in Dermatology and Dermatopathology
by
Carlo Francesco Tomasini and Lorenzo Magnani
Dermatopathology 2026, 13(1), 3; https://doi.org/10.3390/dermatopathology13010003 - 25 Dec 2025
Abstract
►▼
Show Figures
Abductive reasoning, or abduction, is a key process in scientific discovery and medical diagnosis. In everyday dermatology and dermatopathology, however, it functions as the practical engine behind differential diagnosis, clinicopathologic correlation, and disciplined pattern recognition. In this paper, we retain the epistemological
[...] Read more.
Abductive reasoning, or abduction, is a key process in scientific discovery and medical diagnosis. In everyday dermatology and dermatopathology, however, it functions as the practical engine behind differential diagnosis, clinicopathologic correlation, and disciplined pattern recognition. In this paper, we retain the epistemological foundation of abduction but translate it into usable steps for clinicians and dermatopathologists. We distinguish abduction from deduction and induction; separate creative abduction (which generates new concepts) from selective abduction (daily diagnostic choice); and show how both operate within a simple Select-and-Test (ST) Model: select a hypothesis, deduce what else should be true, test against data, and then update. We then reinterpret Ackerman’s algorithmic method of pattern analysis as an operationalization of the ST-Model. Through a couple of concise case vignettes, we illustrate visual and manipulative abduction, nonmonotonic updates, and the role of artifacts (dermoscopy, DIF, stains) as so-called epistemic mediators. Finally, we map contemporary AI tools to selective abduction and propose practical guardrails for fairness, transparency, and accountability. The result is a pragmatic framework that preserves philosophical depth while addressing the daily needs of dermatologists and dermatopathologists in the clinic and at the microscope.
Full article

Figure 1
Open AccessArticle
Increased Expression of Angiopoietin 2 and Tie2 in Rosacea
by
Aysin Kaya, Jean-Hilaire Saurat, Nathalie Satta and Gürkan Kaya
Dermatopathology 2026, 13(1), 2; https://doi.org/10.3390/dermatopathology13010002 - 25 Dec 2025
Abstract
►▼
Show Figures
In this study we evaluated the expression of Angiopoietin 1, Angiopoietin 2, and Tie2 by immunohistochemistry in the skin of 10 patients with erythemato telangiectatic and papulopustular rosacea. Significantly increased expression of Tie2 and Angiopoietin 2 in the endothelial cells of the dermal
[...] Read more.
In this study we evaluated the expression of Angiopoietin 1, Angiopoietin 2, and Tie2 by immunohistochemistry in the skin of 10 patients with erythemato telangiectatic and papulopustular rosacea. Significantly increased expression of Tie2 and Angiopoietin 2 in the endothelial cells of the dermal vessels in rosacea skin vs. non-lesional skin (100% and 33.3% for Tie2, and 100% and 50% for Angiopoietin 2) was observed. There was no difference in the expression of Angiopoietin 1 and phosphorylated Tie2 (pTie2) between the lesional skin of rosacea and non-lesional skin.
Full article

Figure 1
Open AccessArticle
Artificial Intelligence for Lentigo Maligna: Automated Margin Assessment via Sox-10-Based Melanocyte Density Mapping
by
Rieke Löper, Lennart Abels, Daniel Otero Baguer, Felix Bremmer, Michael P. Schön and Christina Mitteldorf
Dermatopathology 2026, 13(1), 1; https://doi.org/10.3390/dermatopathology13010001 - 19 Dec 2025
Abstract
Lentigo maligna (LM) is a melanoma in situ with high cumulative sun damage. Histological evaluation of resection margins is difficult and time-consuming. Melanocyte density (MD) is a suitable, quantifiable, and reproducible diagnostic criterion. In this retrospective single-centre study, we investigated whether an artificial
[...] Read more.
Lentigo maligna (LM) is a melanoma in situ with high cumulative sun damage. Histological evaluation of resection margins is difficult and time-consuming. Melanocyte density (MD) is a suitable, quantifiable, and reproducible diagnostic criterion. In this retrospective single-centre study, we investigated whether an artificial intelligence (AI) tool can support the assessment of LM. Training and evaluation were based on MD in Sox-10-stained digitalised slides. In total, 86 whole slide images (WSIs) from LM patients were annotated and used as a training set. The test set consisted of 177 slides. The tool was trained to detect the epidermis, measure its length, and determine the MD. A cut-off of ≥30 melanocytes per 0.5 mm of epidermis length was defined as positive. Our AI model automatically recognises the epidermis and measures the MD. The model was trained on nuclear immunohistochemical signals and can also be applied to other nuclear stains, such as PRAME or MITF. The WSI is automatically visualised by a three-colour heat map with a subdivision into low, borderline, and high melanocyte density. The cut-offs can be adjusted individually. Compared to manually counted ground truth MD, the AI model achieved high sensitivity (87.84%), specificity (72.82%), and accuracy (79.10%), and an area under the curve (AUC) of 0.818 in the test set. This automated tool can assist (dermato) pathologists by providing a quick overview of the WSI at first glance and making the time-consuming assessment of resection margins more efficient and more reproducible. The AI model can provide significant benefits in the daily routine workflow.
Full article
(This article belongs to the Section Artificial Intelligence in Dermatopathology)
►▼
Show Figures

Figure 1
Open AccessReview
Is Radiotherapy a Risk Factor for Melanoma?
by
Sumeyye Ozer, Priya Agarwal, Noah Musolff, Brendan Plann-Curley, Gizem Cosgun, Helen Yanyu Sun and Babar Rao
Dermatopathology 2025, 12(4), 43; https://doi.org/10.3390/dermatopathology12040043 - 17 Nov 2025
Abstract
Melanoma is a highly aggressive skin cancer primarily linked to ultraviolet (UV) radiation. However, the potential role of ionizing radiation from radiotherapy in melanoma development remains unclear. This review synthesizes data from epidemiologic studies and case reports on melanoma after radiation exposure. Evidence
[...] Read more.
Melanoma is a highly aggressive skin cancer primarily linked to ultraviolet (UV) radiation. However, the potential role of ionizing radiation from radiotherapy in melanoma development remains unclear. This review synthesizes data from epidemiologic studies and case reports on melanoma after radiation exposure. Evidence indicates that childhood radiotherapy, even at low doses, is associated with an increased melanoma risk, plausibly reflecting the heightened radiosensitivity of developing melanocytes. Occupational radiation exposure, particularly in earlier eras with insufficient shielding, also appears to elevate risk. In patients exposed to radiation in adulthood, findings are mixed: large population datasets suggest a modest increase in melanoma following therapeutic radiation, whereas some case–control analyses do not demonstrate a clear dose–response relationship. UV radiation promotes melanomagenesis through direct DNA photoproducts driving characteristic C>T transitions at dipyrimidine sites, alongside oxidative stress and local immune modulation that facilitate malignant transformation. Collectively, individuals with prior radiotherapy, especially those irradiated in childhood, should be considered at increased melanoma risk and may benefit from long-term, targeted surveillance of irradiated fields. Awareness of this association between radiation exposure and melanoma may also support clinicopathologic correlation during the diagnostic evaluation of melanocytic lesions. Future work should define dose–response relationships in contemporary radiotherapy methods, characterize molecular signatures of ionizing radiation-associated melanomas, and establish evidence-based surveillance strategies for high-risk cohorts.
Full article
(This article belongs to the Section Experimental Dermatopathology)
Open AccessReview
Translating Features to Findings: Deep Learning for Melanoma Subtype Prediction
by
Dorra Guermazi, Sarina Khemchandani, Samer Wahood, Cuong Nguyen and Elie Saliba
Dermatopathology 2025, 12(4), 42; https://doi.org/10.3390/dermatopathology12040042 - 12 Nov 2025
Abstract
►▼
Show Figures
Melanoma subtyping plays a vital role in histopathological diagnosis, informing prognosis and, in some cases, guiding targeted therapy. However, conventional histologic classification is constrained by inter-rater reliability, morphologic overlap, and the underrepresentation of rare subtypes. Deep learning (DL)—particularly convolutional neural networks (CNNs)—presents a
[...] Read more.
Melanoma subtyping plays a vital role in histopathological diagnosis, informing prognosis and, in some cases, guiding targeted therapy. However, conventional histologic classification is constrained by inter-rater reliability, morphologic overlap, and the underrepresentation of rare subtypes. Deep learning (DL)—particularly convolutional neural networks (CNNs)—presents a compelling opportunity to enhance diagnostic precision and reproducibility through automated analysis of histopathologic slides. This review examines the clinical importance and diagnostic challenges of melanoma subtyping, outlines core DL methodologies in dermatopathology, and synthesizes current advances in applying DL to subtype classification. Pertinent limitations including dataset imbalance, a lack of interpretability, and domain generalizability are discussed. Additionally, emerging directions such as multimodal integration, synthetic data generation, federated learning, and explainable AI are highlighted as potential solutions. As these technologies mature, DL holds considerable promise in advancing melanoma diagnostics and supporting more personalized, accurate, and equitable patient care.
Full article
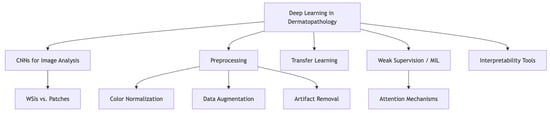
Figure 1
Highly Accessed Articles
Latest Books
E-Mail Alert
News
Topics

Conferences
Special Issues
Special Issue in
Dermatopathology
New Insights in Paediatric Dermatopathology 2025
Guest Editor: Sylvie FraitagDeadline: 31 July 2026
Special Issue in
Dermatopathology
Guidelines for Optimizing Skin Biopsies: Best Practices for Clinicians and Dermatopathologists
Guest Editors: Maria Teresa Fernández Figueras, Angel Fernandez-FloresDeadline: 31 August 2026









