Boron- and Boric Acid-Treated Titanium Implant Surfaces in Sheep Tibia: A Histologic, Histomorphometric and Mechanical Study
Abstract
1. Introduction
2. Materials and Methods
2.1. Power Analysis
2.2. Surface Preparation
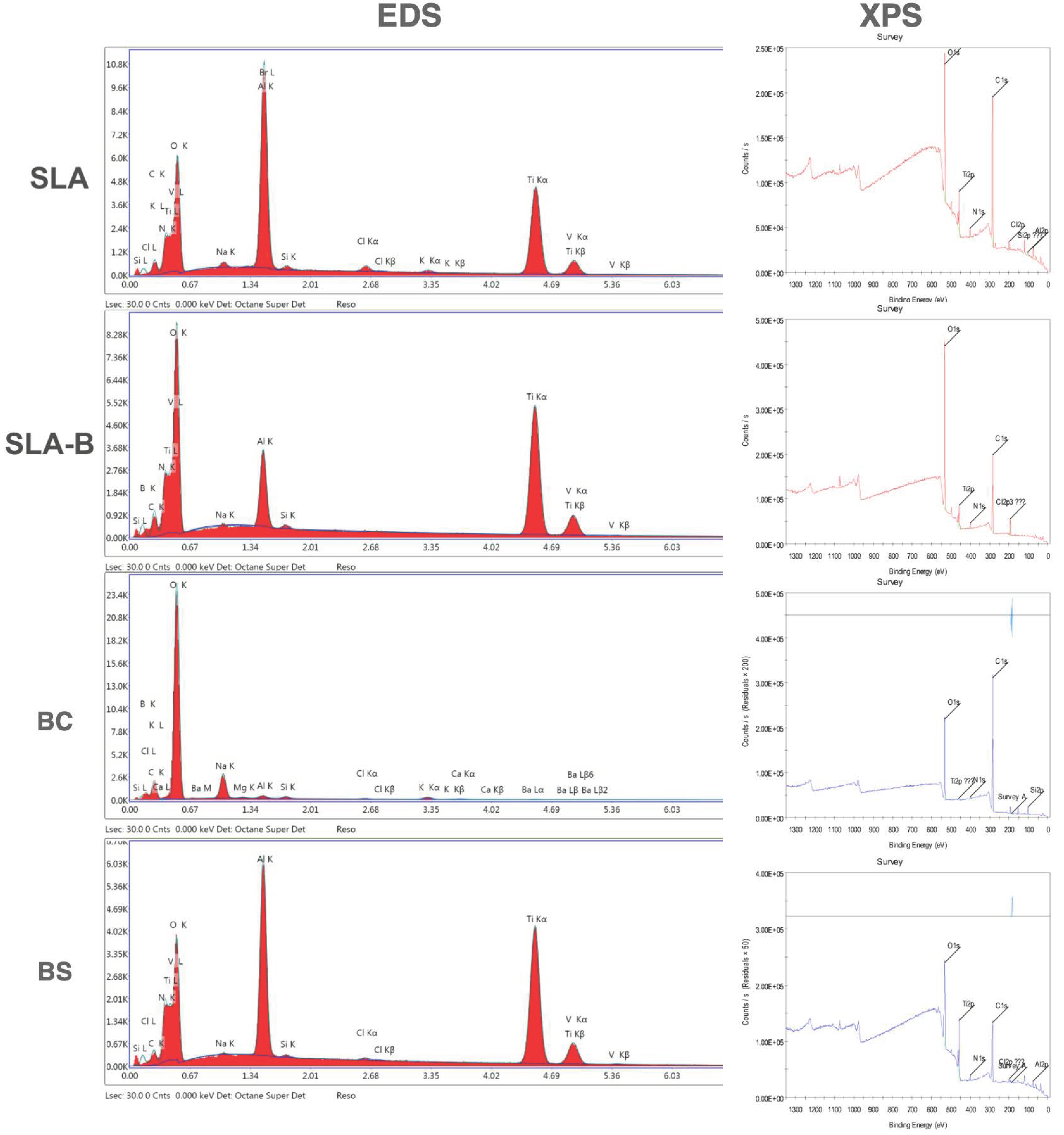
2.3. Surface Characterization
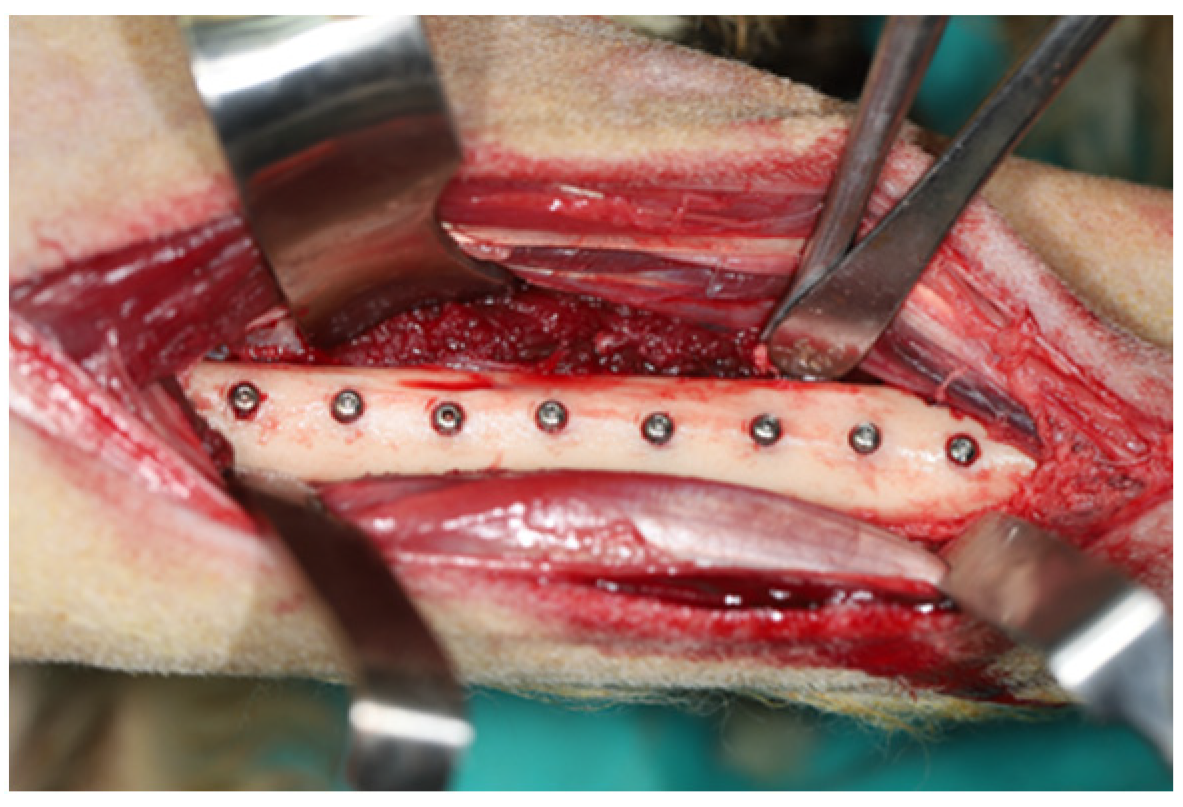
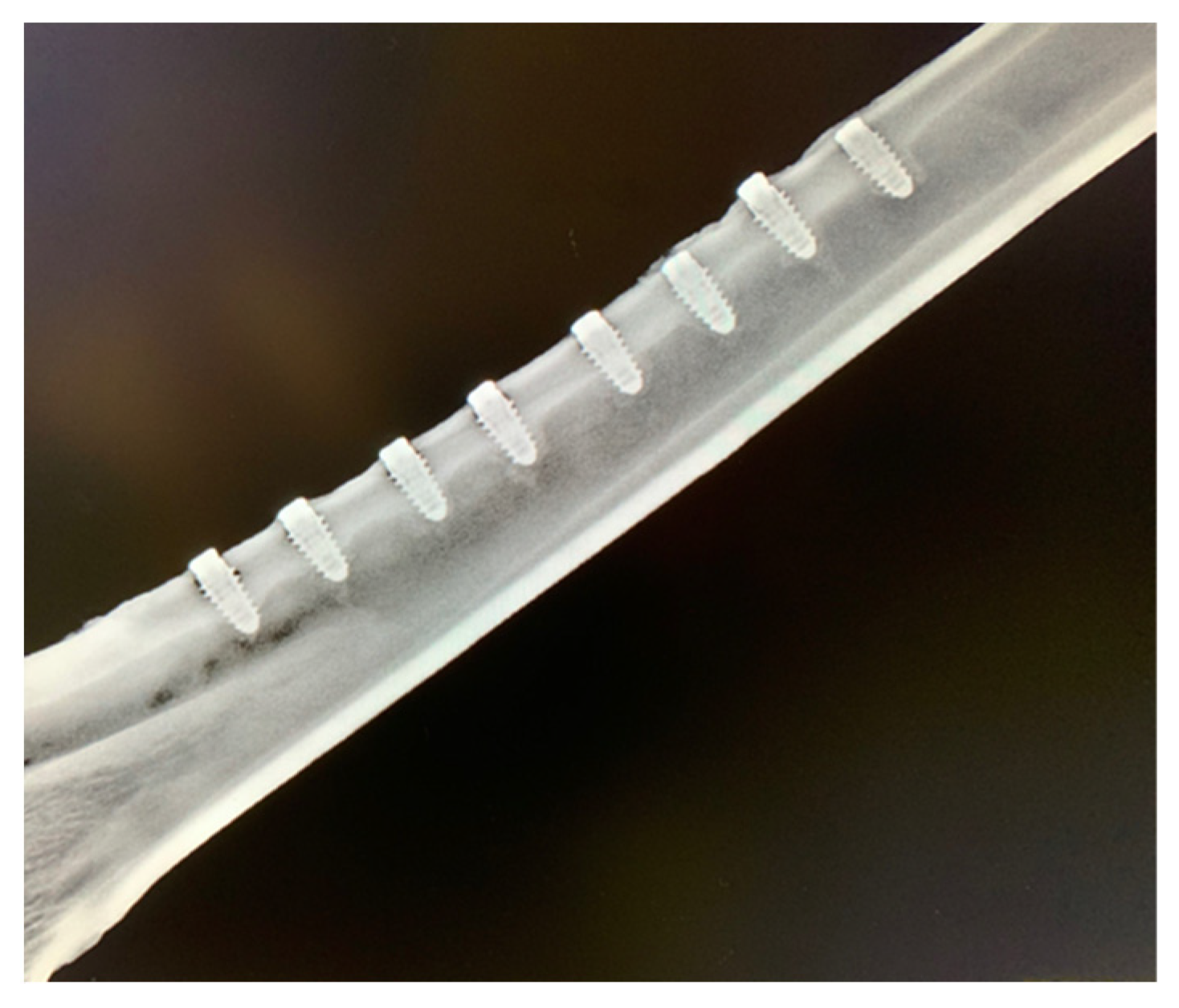
2.4. Animal Experiment
2.5. Fluorochrome Labeling
2.6. Sacrifice and RTV Measurement
2.7. Histologic and Histomorphometric Evaluation
2.8. Statistical Analysis
3. Results
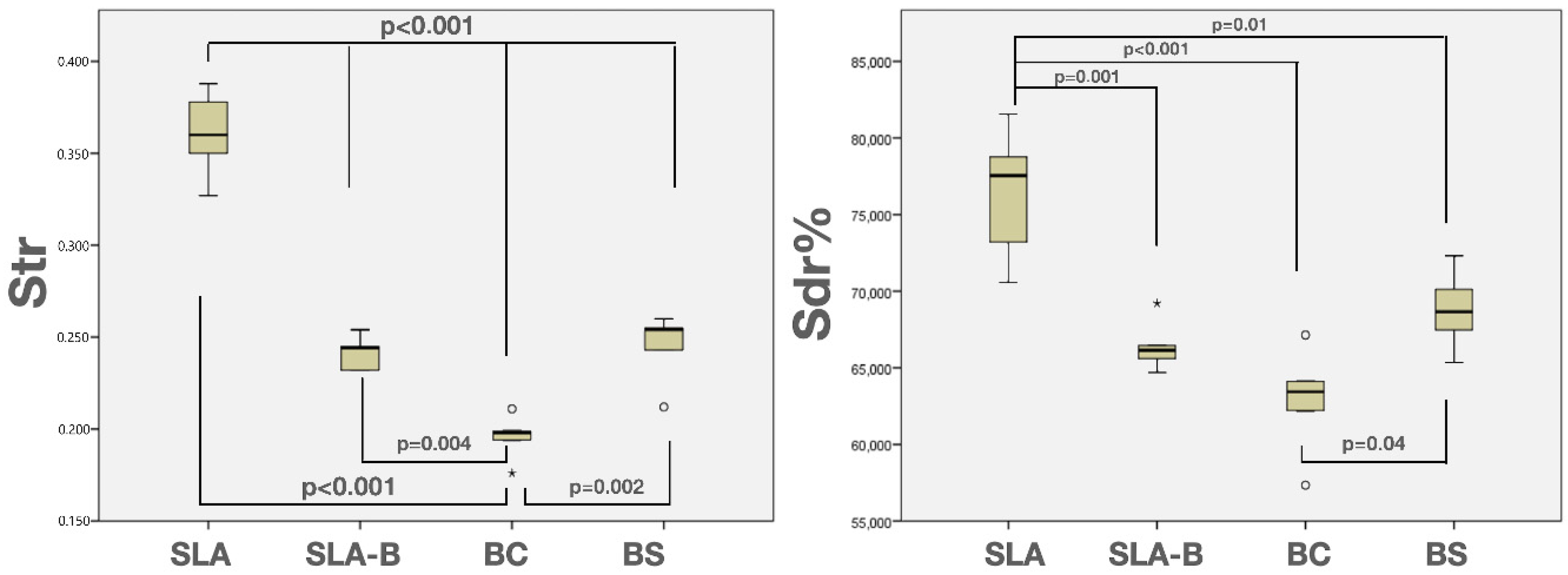
3.1. In Vitro Findings
3.2. In Vivo Findings
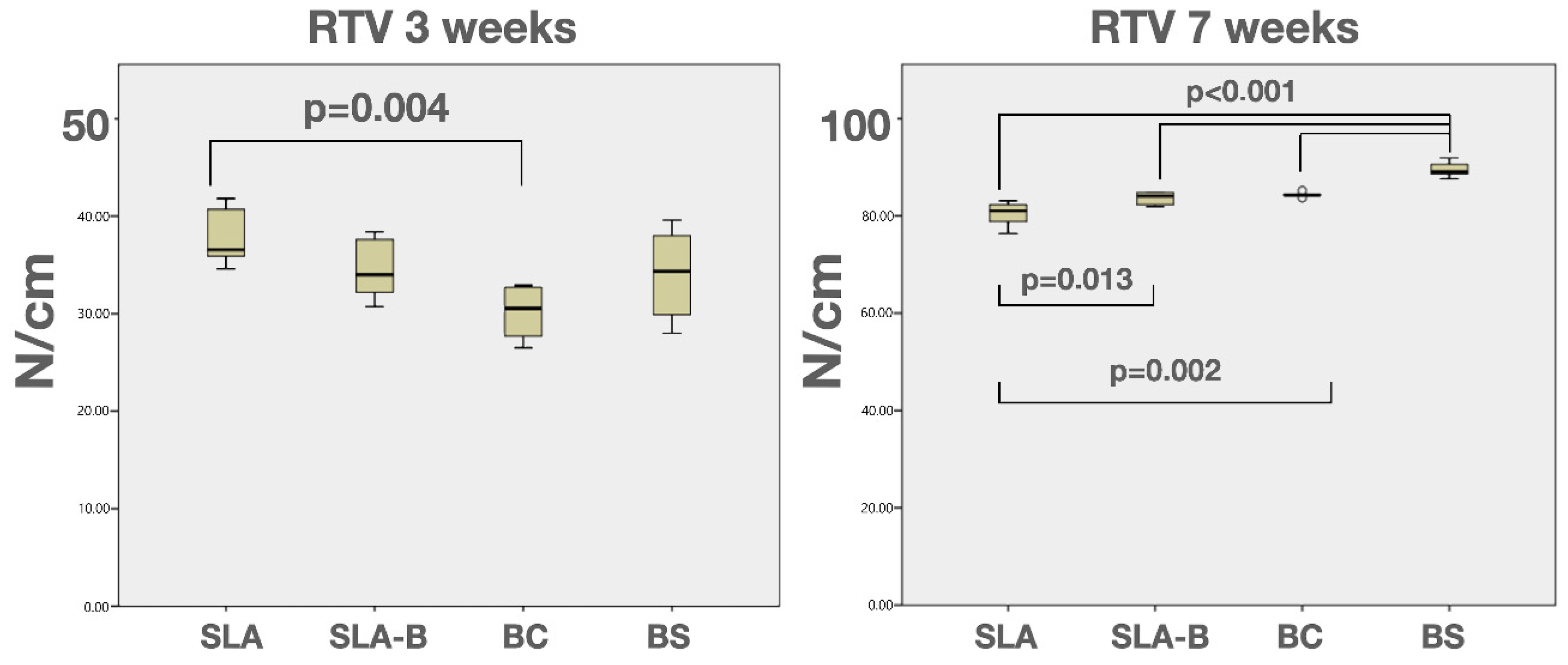
Mechanical Test Results
3.3. Histology and Histomorphometry
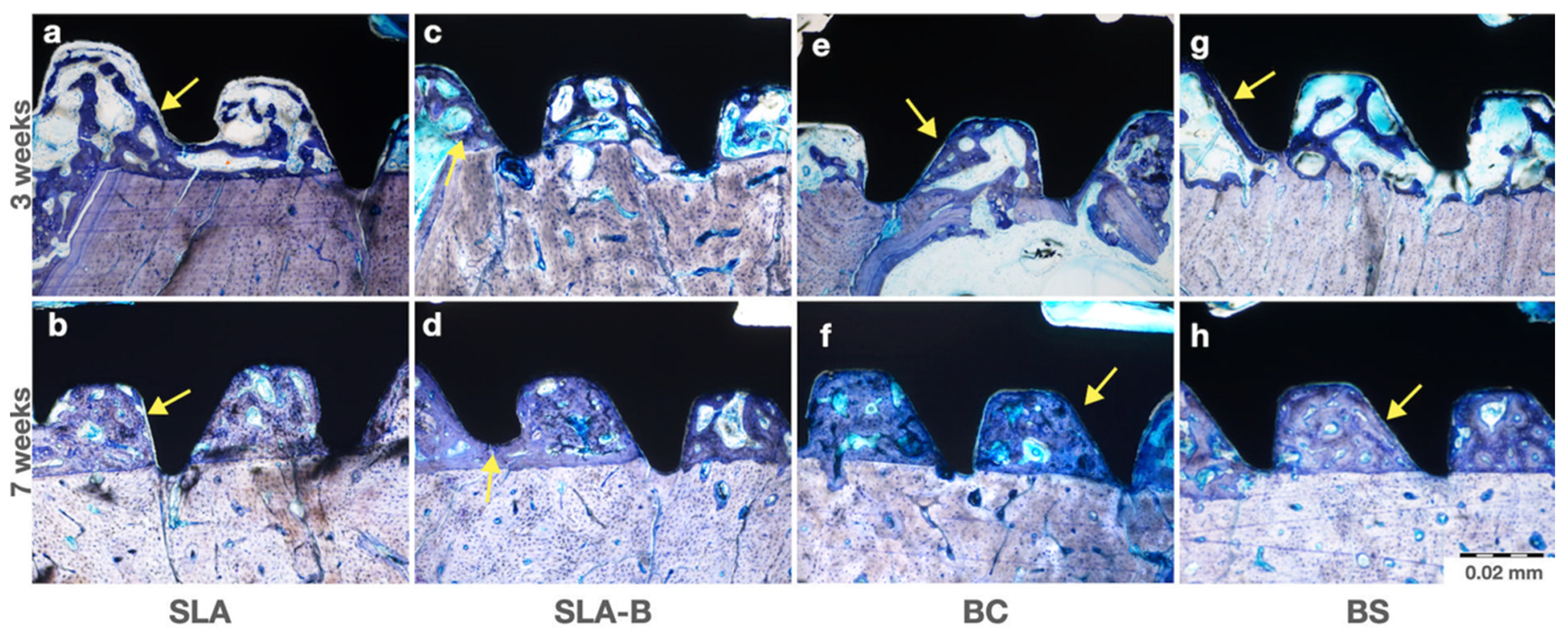
3.3.1. Light Microscopic Observations
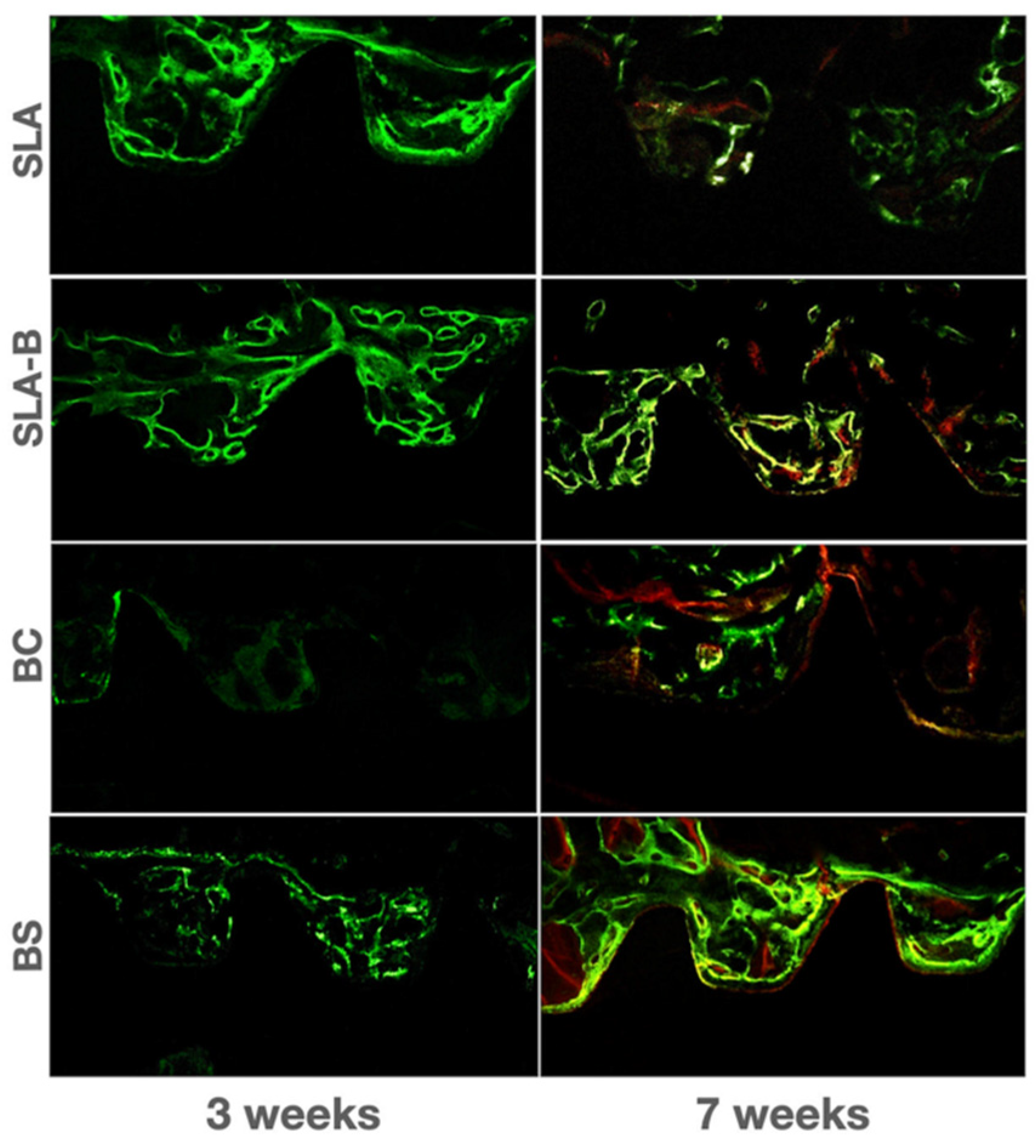
3.3.2. Fluorescence Microscopic Observations
3.3.3. Bone Histomorphometry
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Albrektsson, T.; Wennerberg, A. On osseointegration in relation to implant surfaces. Clin. Implant. Dent. Relat. Res. 2019, 21, 4–7. [Google Scholar] [CrossRef]
- Wennerberg, A.; Albrektsson, T. Effects of titanium surface topography on bone integration: A systematic review. Clin. Oral Implant. Res. 2009, 20 (Suppl. 4), 172–184. [Google Scholar] [CrossRef]
- Guglielmotti, M.B.; Olmedo, D.G.; Cabrini, R.L. Research on implants and osseointegration. Periodontology 2000 2019, 79, 178–189. [Google Scholar] [CrossRef] [PubMed]
- Nicolau, P.; Guerra, F.; Reis, R.; Krafft, T.; Benz, K.; Jackowski, J. 10-year outcomes with immediate and early loaded implants with a chemically modified SLA surface. Quintessence Int. 2019, 50, 114–124. [Google Scholar] [CrossRef] [PubMed]
- Messias, A.; Nicolau, P.; Guerra, F. Titanium Dental Implants with Different Collar Design and Surface Modifications: A Systematic Review on Survival Rates and Marginal Bone Levels. Clin. Oral Implant. Res. 2019, 30, 20–48. [Google Scholar] [CrossRef]
- Wennerberg, A.; Albrektsson, T. Suggested guidelines for the topographic evaluation of implant surfaces. Int. J. Oral. Maxillofac. Implant. 2000, 15, 331–344. [Google Scholar]
- Rupp, F.; Liang, L.; Geis-Gerstorfer, J.; Scheideler, L.; Hüttig, F. Surface characteristics of dental implants: A review. Dent. Mater. 2018, 34, 40–57. [Google Scholar] [CrossRef]
- Jemat, A.; Ghazali, M.J.; Razali, M.; Otsuka, Y. Surface modifications and their effects on titanium dental implants. BioMed Res. Int. 2015, 2015, 791725. [Google Scholar] [CrossRef]
- Nielsen, F.H. Micronutrients in Parenteral Nutrition: Boron, Silicon, and Fluoride. Gastroenterology 2009, 137 (Suppl. 5), S55–S60. [Google Scholar] [CrossRef] [PubMed]
- Uluisik, I.; Karakaya, H.C.; Koc, A. The importance of boron in biological systems. J. Trace Elem. Med. Biol. 2018, 45, 156–162. [Google Scholar] [CrossRef]
- Gorustovich, A.A.; Steimetz, T.; Nielsen, F.H.; Guglielmotti, M.B. Histomorphometric study of alveolar bone healing in rats fed a boron-deficient diet. Anat. Rec. 2008, 291, 441–447. [Google Scholar] [CrossRef] [PubMed]
- Adriztina, I.; Adenin, L.I.; Lubis, Y.M. Efficacy of boric acid as a treatment of choice for chronic suppurative otitis media and its ototoxicity. Korean J. Fam. Med. 2018, 39, 2–9. [Google Scholar] [CrossRef] [PubMed]
- Ulu, M.; Kütük, N.; Cıcık, M.F.; Bilge, S.; Akçay, H.; Saygılı, S.; Tuğlu, M.İ.; Alkan, A. Effects of boric acid on bone formation after maxillary sinus floor augmentation in rabbits. Oral Maxillofac. Surg. 2018, 22, 443–450. [Google Scholar] [CrossRef] [PubMed]
- Çakal, G.; Gökmenoğlu, C.; Kaftanoğlu, B.; Özmeriç, N. Surface Characterization and Corrosion Resistance of Boron Nitride Coated Titanium Dental Implants. Prot. Met. Phys. Chem. Surf. 2019, 55, 608–614. [Google Scholar] [CrossRef]
- Lukasz, W.; Jonathan, M.; Michelle, B.; Nick, T.; Christopher, D.L.; Roumiana, S.P. Assessing osseointegration of metallic implants with boronized surface treatment. Med. Oral Patol. Oral Cir. Bucal 2020, 25, e311–e317. [Google Scholar] [CrossRef]
- Zboun, M.; Arısan, V.; Topcuoglu, N.; Kuruoglu, F.; Sener, L.T.; Sarcan, F. In vitro comparison of titanium surface conditioning via boron-compounds and sand-blasting acid-etching. Surf. Interf. 2020, 21, 100703. [Google Scholar] [CrossRef]
- Guarnieri, R.; Miccoli, G.; Reda, R.; Mazzoni, A.; Di Nardo, D.; Testarelli, L. Sulcus fluid volume, IL-6, and Il-1b concentrations in periodontal and peri-implant tissues comparing machined and laser-microtextured collar/abutment surfaces during 12 weeks of healing: A split-mouth RCT. Clin. Oral Implant. Res. 2022, 33, 94–104. [Google Scholar] [CrossRef]
- Qamheya, A.H.A.; Arısan, V.; Mutlu, Z.; Karabaglı, M.; Soluk Tekkeşin, M.; Kara, K.; Erol, A.; Ersanlı, S. Thermal oxidation and hydrofluoric acid treatment on the sandblasted implant surface: A histologic histomorphometric and biomechanical study. Clin. Oral Implant. Res. 2018, 29, 741–755. [Google Scholar] [CrossRef]
- Ou, K.L.; Hsu, H.J.; Yang, T.S.; Lin, Y.H.; Chen, C.S.; Peng, P.W. Osseointegration of titanium implants with SLAffinity treatment: A histological and biomechanical study in miniature pigs. Clin. Oral Investig. 2016, 20, 1515–1524. [Google Scholar] [CrossRef]
- Van Gaalen, S.M.; Kruyt, M.C.; Geuze, R.E.; de Bruijn, J.D.; Alblas, J.; Dhert, W.J.A. Use of fluorochrome labels in in vivo bone tissue engineering research. Tissue Eng. Part B Rev. 2010, 16, 209–217. [Google Scholar] [CrossRef]
- Wu, J.Z.; Yun, S.H.; Dibos, A.; Kim, D.K.; Tidrow, M. Fabrication and characterization of boron-related nanowires. Microelectron. J. 2003, 34, 463–470. [Google Scholar] [CrossRef]
- Huang, Q.; Yang, X.; Zhang, R.; Liu, X.; Shen, Z.; Feng, Q. Enhanced hydrophilicity and in vitro bioactivity of porous TiO2 film through the incorporation of boron. Ceram. Int. 2015, 41, 4452–4459. [Google Scholar] [CrossRef]
- Lioubavina-Hack, N.; Lang, N.P.; Karring, T. Significance of primary stability for osseointegration of dental implants. Clin. Oral Implant. Res. 2006, 17, 244–250. [Google Scholar] [CrossRef] [PubMed]
- Abdel-Haq, J.; Karabuda, C.Z.; Arisan, V.; Mutlu, Z.; Kürkçü, M. Osseointegration and stability of a modified sand-blasted acid-etched implant: An experimental pilot study in sheep. Clin. Oral Implant. Res. 2011, 22, 265–274. [Google Scholar] [CrossRef] [PubMed]
- Buser, D.; Nydegger, T.; Oxland, T.; Cochran, D.L.; Schenk, R.K.; Hirt, H.P.; Snétivy, D.; Nolte, L.P. Interface shear strength of titanium implants with a sandblasted and acid-etched surface: A biomechanical study in the maxilla of miniature pigs. J. Biomed. Mater. Res. 1999, 45, 75–83. [Google Scholar] [CrossRef]
- Klokkevold, P.R.; Johnson, P.; Dadgostari, S.; Caputo, A.; Davies, J.E.; Nishimura, R.D. Early endosseous integration enhanced by dual acid etching of titanium: A torque removal study in the rabbit. Clin. Oral Implant. Res. 2001, 12, 350–357. [Google Scholar] [CrossRef] [PubMed]
- Devirian, T.A.; Volpe, S.L. The Physiological Effects of Dietary Boron. Crit. Rev. Food Sci. Nutr. 2003, 43, 219–231. [Google Scholar] [CrossRef]
- Mangano, F.G.; Pires, J.T.; Shibli, J.A.; Mijiritsky, E.; Iezzi, G.; Piattelli, A.; Mangano, C. Early Bone Response to Dual Acid-Etched and Machined Dental Implants Placed in the Posterior Maxilla: A Histologic and Histomorphometric Human Study. Implant Dent. 2017, 26, 24–29. [Google Scholar] [CrossRef]
- Sennerby, L. A Morphometric and Biomechanic Comparison of Titanium Implants Inserted in Rabbit Cortical and Cancellous Bone. Int. J. Oral Maxillofac. Implant. 1992, 7, 62–70. [Google Scholar]
- Pearce, A.I.; Pearce, S.G.; Schwieger, K.; Milz, S.; Schneider, E.; Archer, C.W.; Richards, R.G. Effect of surface topography on removal of cortical bone screws in a novel sheep model. J. Orthop. Res. 2008, 26, 1377–1383. [Google Scholar] [CrossRef]
- Cordioli, G.; Majzoub, Z.; Piattelli, A.; Scarano, A. Removal torque and histomorphometric investigation of 4 different titanium surfaces: An experimental study in the rabbit tibia. Int. J. Oral Maxillofac. Implant. 2000, 15, 668–674. [Google Scholar]
- Ding, Z.; Peng, Q.; Zuo, J.; Wang, Y.; Zhou, H.; Tang, Z. Osteogenesis Performance of Boronized Ti6Al4V/HA Composites Prepared by Microwave Sintering: In Vitro and In Vivo Studies. Materials 2022, 15, 4985. [Google Scholar] [CrossRef] [PubMed]
- Kaczmarek, M.; Jurczyk, M.U.; Miklaszewski, A.; Paszel-Jaworska, A.; Romaniuk, A.; Lipińska, N.; Żurawski, J.; Urbaniak, P.; Jurczyk, K. In vitro biocompatibility of titanium after plasma surface alloying with boron. Mater. Sci. Eng. C 2016, 69, 1240–1247. [Google Scholar] [CrossRef] [PubMed]
- Ying, X.; Cheng, S.; Wang, W.; Lin, Z.; Chen, Q.; Zhang, W.; Kou, D.; Shen, Y.; Cheng, X.; Rompis, F.A.; et al. Effect of boron on osteogenic differentiation of human bone marrow stromal cells. Biol. Trace Elem. Res. 2011, 144, 306–315. [Google Scholar] [CrossRef] [PubMed]
- Kotsakis, G.A. Minimizing risk of bias in clinical implant research study design. Periodontology 2000 2019, 81, 18–28. [Google Scholar] [CrossRef] [PubMed]
- Ito, Y.; Sato, D.; Yoneda, S.; Ito, D.; Kondo, H.; Kasugai, S. Relevance of resonance frequency analysis to evaluate dental implant stability: Simulation and histomorphometrical animal experiments. Clin. Oral Implant. Res. 2008, 19, 9–14. [Google Scholar] [CrossRef]
- Tanaka, K.; Sailer, I.; Iwama, R.; Yamauchi, K.; Nogami, S.; Yoda, N.; Takahashi, T. Relationship between cortical bone thickness and implant stability at the time of surgery and secondary stability after osseointegration measured using resonance frequency analysis. J. Periodontal Implant. Sci. 2018, 48, 360–372. [Google Scholar] [CrossRef]

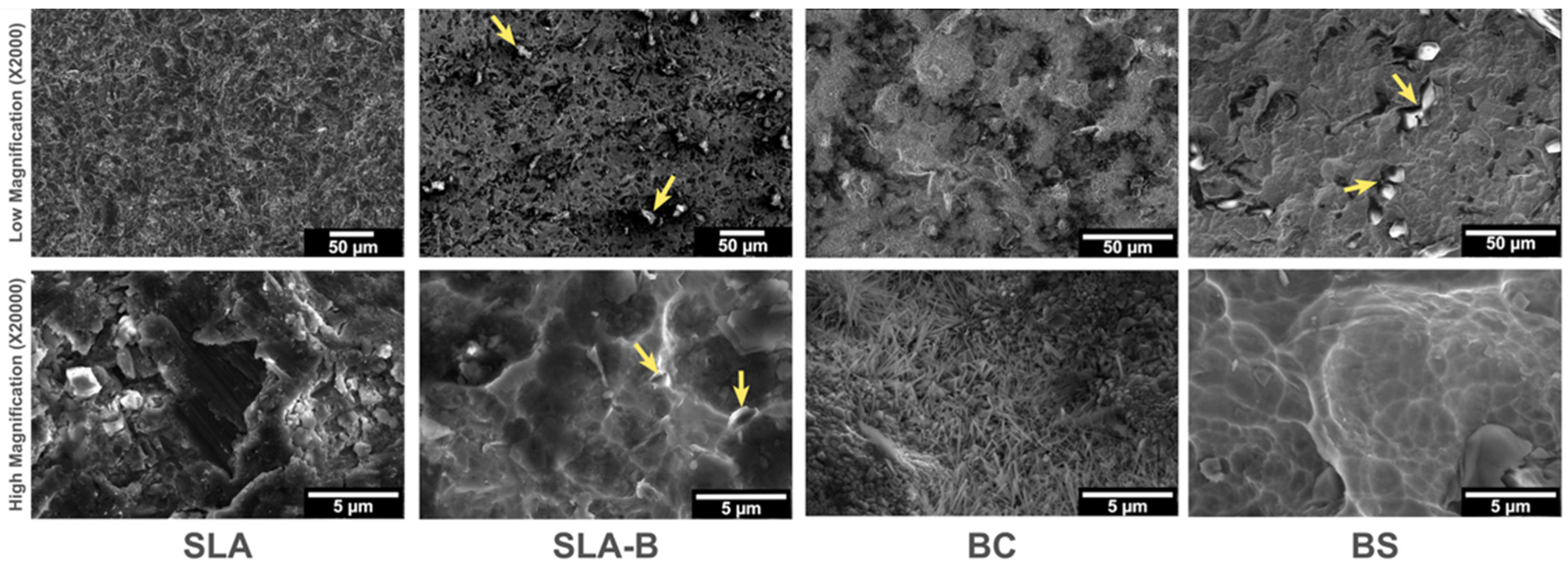

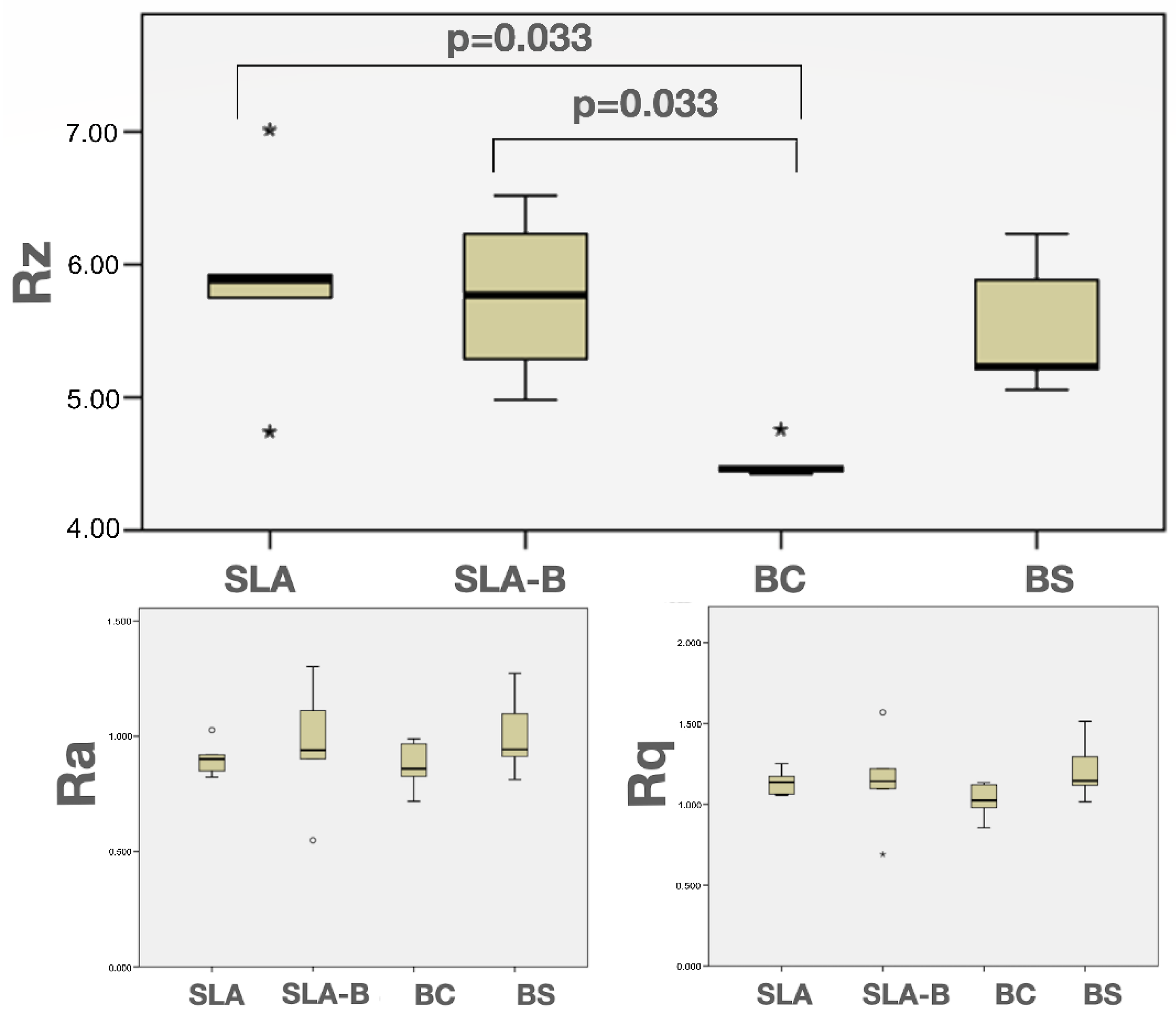
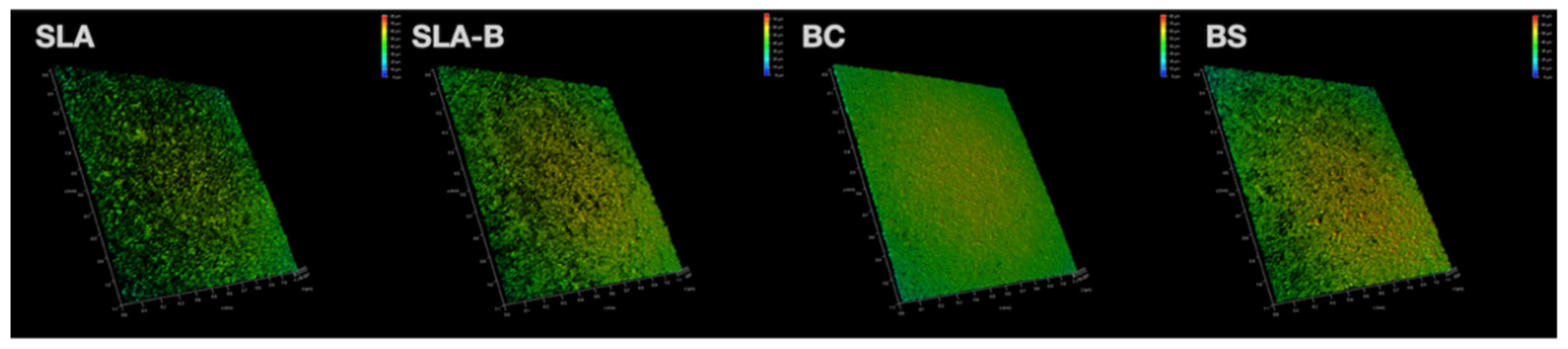
| Modifications/Surface Groups | SLA | SLA-B | BC | BS |
|---|---|---|---|---|
| Sandblasting | Al2O3 | Al2O3 + H3BO3 | Al2O3 + H3BO3 | Al2O3 |
| Acid-etching | HCl + H2SO4 | HCl + H2SO4 | HCl + H2SO4 | HCl + H2SO4 |
| Additional treatment | - | - | B coating | H3BO3 in saline solution |
| Surface Groups | Mean (SD) | Ra (μm) | Rz * (μm) | Rq (μm) |
|---|---|---|---|---|
| Median (IQR) | ||||
| 95% CI | ||||
| SLA | Mean (SD) | 0.90 (0.79) | 5.86 (0.80) a | 1.13 (0.08) |
| Median (IQR) | 0.90 (0.13) | 5.89 (1.22) | 1.13 (0.15) | |
| 95% CI | 0.80–1.00 | 4.85–6.86 | 1.03–1.23 | |
| SLA-B | Mean (SD) | 0.96 (0.27) | 5.75 (0.64) b | 1.14 (0.31) |
| Median (IQR) | 0.94 (0.75) | 5.77 (1.25) | 1.14 (0.50) | |
| 95% CI | 0.61–1.30 | 4.95–6.55 | 0.75–1.53 | |
| BC | Mean (SD) | 0.87 (0.11) | 4.51 (0.13) a,b | 1.02 (0.11) |
| Median (IQR) | 0.85 (0.20) | 4.45 (0.18) | 1.02 (0.21) | |
| 95% CI | 0.73–1.00 | 4.33–4.68 | 0.88–1.16 | |
| BS | Mean (SD) | 1.007 (0.18) | 5.52 (0.50) | 1.21 (0.19) |
| Median (IQR) | 0.94 (0.32) | 5.23 (0.92) | 1.14 (0.33) | |
| 95% CI | 0.78–1.23 | 4.89–6.15 | 0.97–1.45 |
| Surface Groups | Texture Aspect Ratio (Str) * | Developed Interfacial Area Ratio (Sdr%) * | |
|---|---|---|---|
| SLA | Mean (SD) | 0.36 (0.02) a,b,c,d | 76.32 (4.41) x,y,z |
| Median (IQR) | 0.36 (0.04) | 77.54 (8.28) | |
| 95% CI | 0.33–0.39 | 70.84–81.80 | |
| SLA-B | Mean (SD) | 0.24 (0.009) a,e | 66.42 (1.69) x |
| Median (IQR) | 0.24 (0.01) | 66.14 (2.68) | |
| 95% CI | 0.22 –0.25 | 64.31–68.52 | |
| BC | Mean (SD) | 0.19 (0.01) b,d,e,f | 62.84 (3.57) y,t |
| Median (IQR) | 0.19 (0.03) | 63.43 (5.86) | |
| 95% CI | 0.17–0.21 | 58.40–67.28 | |
| BS | Mean (SD) | 0.24 (0.01) c,f | 68.78 (2.64) z,t |
| Median (IQR) | 0.25 (0.03) | 68.66 (4.81) | |
| 95% CI | 0.22–0.26 | 65.50–72.06 | |
| SLA | SLA-B | BC | BS | ||
|---|---|---|---|---|---|
| ITV | Mean (SD) | 42.37 (13.39) | 39.05 (8.45) | 42.44 (10.48) | 41.63 (11.18) |
| Median (IQR) | 40.45 (10.15) | 38.65 (7.75) | 40.45 (11.01) | 41.85 (17.40) | |
| Min–Max | 27–66 | 18.3–69.7 | 29.7–68 | 20.9–53.2 | |
| 95% CI | 36.72–48.03 | 35.47–42.62 | 38.01–46.87 | 36.98–46.28 | |
| RTV 3 weeks | Mean (SD) | 37.68 (2.87) a | 34.48 (3.00) | 30.15 (2.60) a | 34.03 (4.48) |
| Median (IQR) | 36.55 (5.40) | 34.00 (5.47) | 30.55 (5.35) | 34.25 (8.98) | |
| Min–Max | 34.6–41.8 | 30.7–38.4 | 27.7–32.9 | 28–39.6 | |
| 95% CI | 34.66–40.70 | 31.32–37.63 | 27.42–32.87 | 29.32–38.73 | |
| RTV 7 weeks | Mean (SD) | 80.45 (2.46) b,c,d,e | 83.65 (1.30) b,f | 84.35 (0.49) c,g | 89.46 (1.53) d,e,f,g |
| Median (IQR) | 81.05 (4.30) | 84.05 (2.60) | 84.25 (0.60) | 89.05 (2.58) | |
| Min–Max | 76.4–83.1 | 81.9–84.8 | 83.7–85.2 | 87.6–91.9 | |
| 95% CI | 77.86–83.03 | 82.28–85.01 | 83.83–84.86 | 87.85–91.08 | |
| BIC% | SLA | SLA-B | BC | BS | |
|---|---|---|---|---|---|
| 3 weeks | Mean (SD) | 25.82 (5.31) | 23.13 (7.11) | 25.95 (10.37) | 33.0 (5.86) |
| Median (IQR) | 24.82 (5.38) | 24.77 (12.61) | 25.59 (18.61) | 35.29 (7.74) | |
| Min–Max | 20.19–35.94 | 11.35–29.56 | 11.28–38.97 | 21.76–37.38 | |
| 95% CI | 20.24–31.39 | 15.67–30.60 | 15.07–36.84 | 26.85–39.15 | |
| 7 weeks | Mean (SD) | 52.49 (11.51) | 68.58 (11.76) | 61.34 (12.07) | 64.02 (9.64) |
| Median (IQR) | 49.37 (20.38) | 64.96 (12.23) | 61.43 (16.91) | 65.20 (16.42) | |
| Min–Max | 36.84–67.79 | 57.18–91.26 | 46.91–82.30 | 49.32–74.54 | |
| 95% CI | 40.40–64.57 | 56.23–80.92 | 48.67–74.01 | 53.89–74.14 | |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Ayşeşek, N.; Arısan, V.; Balcıoğlu, N.B.; Erol, A.; Kuruoğlu, F.; Tekkeşin, M.S.; Ersanlı, S. Boron- and Boric Acid-Treated Titanium Implant Surfaces in Sheep Tibia: A Histologic, Histomorphometric and Mechanical Study. Bioengineering 2022, 9, 705. https://doi.org/10.3390/bioengineering9110705
Ayşeşek N, Arısan V, Balcıoğlu NB, Erol A, Kuruoğlu F, Tekkeşin MS, Ersanlı S. Boron- and Boric Acid-Treated Titanium Implant Surfaces in Sheep Tibia: A Histologic, Histomorphometric and Mechanical Study. Bioengineering. 2022; 9(11):705. https://doi.org/10.3390/bioengineering9110705
Chicago/Turabian StyleAyşeşek, Nazlı, Volkan Arısan, Nilüfer Bölükbaşı Balcıoğlu, Ayşe Erol, Furkan Kuruoğlu, Merva Soluk Tekkeşin, and Selim Ersanlı. 2022. "Boron- and Boric Acid-Treated Titanium Implant Surfaces in Sheep Tibia: A Histologic, Histomorphometric and Mechanical Study" Bioengineering 9, no. 11: 705. https://doi.org/10.3390/bioengineering9110705
APA StyleAyşeşek, N., Arısan, V., Balcıoğlu, N. B., Erol, A., Kuruoğlu, F., Tekkeşin, M. S., & Ersanlı, S. (2022). Boron- and Boric Acid-Treated Titanium Implant Surfaces in Sheep Tibia: A Histologic, Histomorphometric and Mechanical Study. Bioengineering, 9(11), 705. https://doi.org/10.3390/bioengineering9110705








