Salmonella, Food Safety and Food Handling Practices
Abstract
1. Introduction
2. Salmonella
2.1. Occurrence of Salmonella
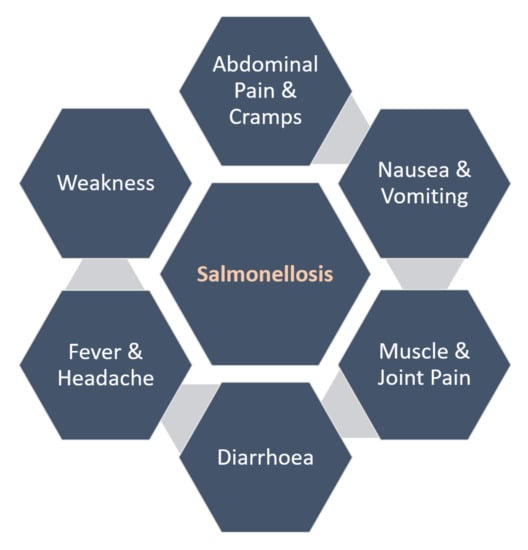
2.2. Epidemiology and Pathogenicity
2.3. Food Products Associated with Salmonella
2.4. Salmonella and Vegetable Produce
3. Global Burden of Salmonellosis
4. Control of Salmonellosis
4.1. Food Hygiene Practices
4.2. Food Handler Effects
Hygienic Meat Handling Practices
4.3. Ready-to-Eat (RTE) Foods and Processed Foods with Needed Control
4.4. Knowledge vs. Behavioural Training Models
5. Future Perspective and Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Callejón, R.M.; Rodríguez-Naranjo, M.I.; Ubeda, C.; Hornedo-Ortega, R.; Garcia-Parrilla, M.C.; Troncoso, A.M. Reported foodborne outbreaks due to fresh produce in the United States and European Union: Trends and causes. Foodborne Pathog. Dis. 2015, 12, 32–38. [Google Scholar] [CrossRef]
- Myintzaw, P.; Moran, F.; Jaiswal, A.K. Campylobacteriosis, consumer’s risk perception, and knowledge associated with domestic poultry handling in Ireland. J. Food Saf. 2020, 40, e12799. [Google Scholar] [CrossRef]
- ECDC. Salmonella the Most Common Cause of Foodborne Outbreaks in the European Union. 2020. Available online: https://www.ecdc.europa.eu/en/news-events/salmonella-most-common-cause-foodborne-outbreaks-european-union (accessed on 2 March 2020).
- Munck, N.; Smith, J.; Bates, J.; Glass, K.; Hald, T.; Kirk, M.D. Source attribution of Salmonella in Macadamia nuts to animal and environmental reservoirs in Queensland, Australia. Foodborne Pathog. Dis. 2020, 17, 357–364. [Google Scholar] [CrossRef] [PubMed]
- Zweifel, C.; Stephan, R. Spices and Herbs as Source of Salmonella-Related Foodborne Diseases. Food Res. Int. 2012, 45, 765–769. [Google Scholar] [CrossRef]
- HPSC. Annual Epidemiological Report. Salmonella Infection in Ireland (2018). 2019. Available online: https://www.hpsc.ie/a-z/gastroenteric/salmonellosis/publications/annualreportsonsalmonellosisinireland/Salmonella%202018%20Annual%20report.pdf (accessed on 31 March 2020).
- Eng, S.-K.; Pusparajah, P.; Ab Mutalib, N.-S.; Ser, H.-L.; Chan, K.-G.; Lee, L.-H. Salmonella: A review on pathogenesis, epidemiology and antibiotic resistance. Front. Life Sci. 2015, 8, 284–293. [Google Scholar] [CrossRef]
- Podolak, R.; Enache, E.; Stone, W.; Black, D.G.; Elliott, P.H. Sources and risk factors for contamination, survival, persistence, and heat resistance of Salmonella in low-moisture foods. J. Food Prot. 2010, 73, 1919–1936. [Google Scholar] [CrossRef]
- Zwietering, M.H.; Jacxsens, L.; Membré, J.-M.; Nauta, M.; Peterz, M. Relevance of microbial finished product testing in food safety management. Food Cont. 2016, 60, 31–43. [Google Scholar] [CrossRef]
- Ray, B.; Jezeski, J.; Busta, F. Isolation of Salmonellae from naturally contaminated dried milk products: Iii. Influence of pre-enrichment conditions. J. Milk Food Technol. 1972, 35, 607–614. [Google Scholar] [CrossRef]
- Gruzdev, N.; Pinto, R.; Sela, S. Persistence of Salmonella enterica during dehydration and subsequent cold storage. Food Microbiol. 2012, 32, 415–422. [Google Scholar] [CrossRef]
- Rayman, M.; D’AOUST, J.-Y.; Aris, B.; Maishment, C.; Wasik, R. Survival of microorganisms in stored pasta. J. Food Prot. 1979, 42, 330–334. [Google Scholar] [CrossRef]
- Tamminga, S.; Beumer, R.; Kampelmacher, E.; Van Leusden, F. Survival of Salmonella east bourne and Salmonella typhimurium in chocolate. Epidemiol. Infect. 1976, 76, 41–47. [Google Scholar] [CrossRef]
- Kotzekidou, P. Microbial stability and fate of Salmonella Enteritidis in halva, a low-moisture confection. J. Food Prot. 1998, 61, 181–185. [Google Scholar] [CrossRef] [PubMed]
- Kozak, G.; MacDonald, D.; Landry, L.; Farber, J. Foodborne outbreaks in Canada linked to produce: 2001 through 2009. J. Food Prot. 2013, 76, 173–183. [Google Scholar] [CrossRef] [PubMed]
- Burnett, S.; Gehm, E.; Weissinger, W.; Beuchat, L. Survival of Salmonella in peanut butter and peanut butter spread. J. Appl. Microbiol. 2000, 89, 472–477. [Google Scholar] [CrossRef] [PubMed]
- Ray, B.; Jezeski, J.; Busta, F. Isolation of Salmonellae from naturally contaminated dried milk products: Ii. Influence of storage time on the isolation of Salmonellae. J. Milk Food Technol. 1971, 34, 423–427. [Google Scholar] [CrossRef]
- De Jong, B.; Ekdahl, K. The comparative burden of salmonellosis in the European Union member states, associated and candidate countries. Bmc Public Health 2006, 6, 1–9. [Google Scholar] [CrossRef]
- Obukhovska, O. The natural reservoirs of Salmonella Enteritidis in populations of wild birds. Online J. Public Health Inf. 2013, 5. [Google Scholar] [CrossRef]
- PFMA.org.uk. Pet Population 2019. Available online: https://www.pfma.org.uk/pet-population-2019 (accessed on 14 March 2020).
- Finlay, F.; Furnell, C.; Ridley, P. Salmonella in pets the risk to children. Community Pract. 2015, 88, 27–29. [Google Scholar]
- Bjelland, A.M.; Sandvik, L.M.; Skarstein, M.M.; Svendal, L.; Debenham, J.J. Prevalence of Salmonella serovars isolated from reptiles in Norwegian zoos. Acta Vet. Scand. 2020, 62, 1–9. [Google Scholar] [CrossRef]
- CFSPH. Reptile-Associated Salmonellosis. 2013. Available online: http://www.cfsph.iastate.edu/Factsheets/pdfs/reptile_associated_salmonellosis.pdf (accessed on 19 August 2020).
- Simpson, K.M.; Hill-Cawthorne, G.A.; Ward, M.P.; Mor, S.M. Diversity of Salmonella serotypes from humans, food, domestic animals and wildlife in New South Wales, Australia. BMC Infect. Dis. 2018, 18, 1–11. [Google Scholar] [CrossRef]
- CDC. Outbreaks Involving Salmonella. 2020. Available online: https://www.cdc.gov/Salmonella/outbreaks.html (accessed on 10 March 2020).
- CDC. Outbreak of Salmonella Infections Linked to Small Pet Turtles. 2020. Available online: https://www.cdc.gov/Salmonella/typhimurium-1-20/index.html (accessed on 12 August 2020).
- CDC. Outbreak of Multidrug-Resistant Salmonella Infections Linked to Contact with Pig Ear Pet Treats. 2019. Available online: https://www.cdc.gov/Salmonella/pet-treats-07-19/index.html (accessed on 12 August 2020).
- CDC. Outbreaks of Salmonella Infections Linked to Backyard Poultry. 2019. Available online: https://www.cdc.gov/Salmonella/backyardpoultry-05-19/index.html (accessed on 12 August 2020).
- CDC. Multistate Outbreaks of Human Salmonella Infections Linked to live Poultry in Backyard Flocks. 2017. Available online: https://www.cdc.gov/Salmonella/live-poultry-06-17/index.html (accessed on 12 August 2020).
- FDA. FDA Investigates Outbreak of Salmonella Infections Linked To Pet Food. 2018. Available online: https://www.fda.gov/animal-veterinary/outbreaks-and-advisories/fda-investigates-outbreak-Salmonella-infections-linked-raws-paws-ground-turkey-food-pets (accessed on 12 August 2020).
- HPSC. Reptiles and Risks of Infectious Diseases-Health Protection Surveillance Centre. 2013. Available online: https://www.hpsc.ie/a-z/zoonotic/reptilesandrisksofinfectiousdiseases/ (accessed on 13 March 2021).
- Turgeon, P.; Ng, V.; Murray, R.; Nesbitt, A. Forecasting the incidence of salmonellosis in seniors in Canada: A trend analysis and the potential impact of the demographic shift. PLoS ONE 2018, 13, e0208124. [Google Scholar] [CrossRef]
- Kurtz, J.R.; Goggins, J.A.; McLachlan, J.B. Salmonella infection: Interplay between the bacteria and host immune system. Immunol. Let. 2017, 190, 42–50. [Google Scholar] [CrossRef]
- Schempp, C.M.; Schauer, F.; Huhn, C.K.; Venhoff, N.; Finzel, S. Skin inflammation associated with arthritis, synovitis and enthesitis. Part 2: Rheumatoid arthritis, reactive arthritis, Reiter’s syndrome, Lyme borreliosis, dermatomyositis and lupus erythematosus. J. Dtsch. Dermaltol. 2019, 17, 167–181. [Google Scholar] [CrossRef]
- Ajene, A.N.; Walker, C.L.F.; Black, R.E. Enteric pathogens and reactive arthritis: A systematic review of Campylobacter, Salmonella and Shigella-associated reactive arthritis. J. Health Popul. Nutr. 2013, 31, 299–307. [Google Scholar] [CrossRef]
- Townes, J.M.; Deodhar, A.A.; Laine, E.S.; Smith, K.; Krug, H.E.; Barkhuizen, A.; Thompson, M.E.; Cieslak, P.R.; Sobel, J. Reactive arthritis following culture-confirmed infections with bacterial enteric pathogens in Minnesota and Oregon: A population-based study. Ann. Rheum. Dis. 2008, 67, 1689–1696. [Google Scholar] [CrossRef]
- EFSA. Multi-Country Outbreak of Salmonella Agona Infections Possibly Linked to Ready-to-Eat Food. 2018. Available online: https://www.efsa.europa.eu/en/supporting/pub/en-1465 (accessed on 27 August 2020).
- FDA. Salmonella (Salmonellosis). 2019. Available online: https://www.fda.gov/food/foodborne-pathogens/Salmonella-salmonellosis (accessed on 11 April 2021).
- FDA. Outbreaks of Foodborne Illness. 2021. Available online: https://www.fda.gov/food/recalls-outbreaks-emergencies/outbreaks-foodborne-illness (accessed on 11 April 2021).
- CDC. Outbreak of Salmonella Infections Linked to Cavi Brand Whole, Fresh Papayas. 2019. Available online: https://www.cdc.gov/Salmonella/uganda-06-19/index.html (accessed on 11 August 2020).
- CDC. Cost of Illness. 2021. Available online: https://www.cdc.gov/policy/polaris/economics/cost-of-illness.html (accessed on 11 April 2021).
- CDC. Reports of Selected Salmonella Outbreak Investigations. 2021. Available online: https://www.cdc.gov/Salmonella/outbreaks.html (accessed on 11 April 2021).
- FDA. Outbreak Investigation of Salmonella Uganda: Fresh Papayas (June 2019). 2020. Available online: https://www.fda.gov/food/outbreaks-foodborne-illness/outbreak-investigation-Salmonella-uganda-fresh-papayas-june-2019 (accessed on 11 August 2020).
- Ung, A.; Baidjoe, A.Y.; Van Cauteren, D.; Fawal, N.; Fabre, L.; Guerrisi, C.; Danis, K.; Morand, A.; Donguy, M.-P.; Lucas, E.; et al. Disentangling a complex nationwide Salmonella Dublin outbreak associated with raw-milk cheese consumption, France, 2015 to 2016. Eurosurveillance 2019, 24, 1700703. [Google Scholar] [CrossRef]
- Jourdan-da Silva, N.; Fabre, L.; Robinson, E.; Fournet, N.; Nisavanh, A.; Bruyand, M.; Mailles, A.; Serre, E.; Ravel, M.; Guibert, V.; et al. Ongoing nationwide outbreak of Salmonella Agona associated with internationally distributed infant milk products, France, December 2017. Eurosurveillance 2018, 23, 17–00852. [Google Scholar] [CrossRef] [PubMed]
- CDC. Outbreak of Multidrug-Resistant Salmonella Infections Linked to Raw Chicken Products. 2019. Available online: https://www.cdc.gov/Salmonella/infantis-10-18/index.html (accessed on 11 August 2020).
- Brandwagt, D.; van den Wijngaard, C.; Tulen, A.D.; Mulder, A.C.; Hofhuis, A.; Jacobs, R.; Heck, M.; Verbruggen, A.; van den Kerkhof, H.; Slegers-Fitz-James, I.; et al. Outbreak of Salmonella Bovismorbificans associated with the consumption of uncooked ham products, the Netherlands, 2016 to 2017. Eurosurveillance 2018, 23, 17–00335. [Google Scholar] [CrossRef] [PubMed]
- CDC. Food Safety. 2021. Available online: https://www.cdc.gov/foodsafety/ (accessed on 14 March 2021).
- England, P.H. Outbreak Report Outbreak of Salmonella Enteritidis Phage Type 14B, May-September 2014. Available online: https://assets.publishing.service.gov.uk/government/uploads/system/uploads/attachment_data/file/432637/S_Enteritidis_PT14B_outbreak_report_gateway__2_pdf (accessed on 11 August 2020).
- EFSA. Salmonella Cases No Longer Falling in the EU. 2017. Available online: https://www.efsa.europa.eu/en/press/news/171212 (accessed on 18 June 2020).
- Bennington-Castro, J. What Is Salmonella? Symptoms, Causes, Diagnosis, Treatment, and Prevention. Available online: https://www.everydayhealth.com/Salmonella/guide/ (accessed on 10 March 2021).
- Lenzi, A.; Marvasi, M.; Baldi, A. Agronomic practices to limit pre-and post-harvest contamination and proliferation of human pathogenic Enterobacteriaceae in vegetable produce. Food Cont. 2020, 107486. [Google Scholar]
- Abbott, D.W.; Boraston, A.B. Structural biology of pectin degradation by Enterobacteriaceae. Microbiol. Mole. Biol. Rev. 2008, 72, 301–316. [Google Scholar] [CrossRef] [PubMed]
- Jacob, C.; Melotto, M. Human pathogen colonization of lettuce dependent upon plant genotype and defense response activation. Front. Plant Sci. 2020, 10, 1769. [Google Scholar] [CrossRef] [PubMed]
- Rai, P.K.; Tripathi, B. Microbial contamination in vegetables due to irrigation with partially treated municipal wastewater in a tropical city. Int. J. Environ. Health Res. 2007, 17, 389–395. [Google Scholar] [CrossRef]
- Critzer, F.J.; Doyle, M.P. Microbial ecology of foodborne pathogens associated with produce. Cur. Opi. Biotechnol. 2010, 21, 125–130. [Google Scholar] [CrossRef] [PubMed]
- Barak, J.D.; Schroeder, B.K. Interrelationships of food safety and plant pathology: The life cycle of human pathogens on plants. Ann. Rev. Phytopathol. 2012, 50, 241–266. [Google Scholar] [CrossRef] [PubMed]
- FoodSafety.gov. 4 Steps to Food Safety. 2020. Available online: https://www.foodsafety.gov/keep-food-safe/4-steps-to-food-safety (accessed on 28 August 2020).
- Bartz, J.A.; Marvasi, M.; Teplitski, M. Salmonella and tomatoes. In The Produce Contamination Problem: Causes and Solution Matthews, K.R., Sapers, G.M., Gerba, C.P., Eds.; Elsevier: Amsterdam, The Netherlands, 2014; pp. 269–289. [Google Scholar]
- Holden, N.J. Plants as reservoirs for human enteric pathogens. Ani. Sci. Rev. 2010, 5, 185. [Google Scholar] [CrossRef]
- Ibenyassine, K.; Mhand, R.A.; Karamoko, Y.; Anajjar, B.; Chouibani, M.; Ennaji, M. Bacterial pathogens recovered from vegetables irrigated by wastewater in Morocco. J. Environ.Environ. Health 2007, 69, 47–51. [Google Scholar]
- Iwu, C.D.; Okoh, A.I. Preharvest transmission routes of fresh produce associated bacterial pathogens with outbreak potentials: A review. Int. J. Environ. Res. Public Health 2019, 16, 4407. [Google Scholar] [CrossRef]
- Luna-Guevara, J.J.; Arenas-Hernandez, M.M.; Martínez de la Peña, C.; Silva, J.L.; Luna-Guevara, M.L. The role of pathogenic E. coli in fresh vegetables: Behavior, contamination factors, and preventive measures. Int. J. Microb. 2019, 2019. [Google Scholar] [CrossRef]
- Park, S.; Navratil, S.; Gregory, A.; Bauer, A.; Srinath, I.; Jun, M.; Szonyi, B.; Nightingale, K.; Anciso, J.; Ivanek, R. Generic Escherichia coli contamination of spinach at the preharvest stage: Effects of farm management and environmental factors. Appl. Environ. Microbiol. 2013, 79, 4347–4358. [Google Scholar] [CrossRef]
- Jung, Y.; Jang, H.; Matthews, K.R. Effect of the food production chain from farm practices to vegetable processing on outbreak incidence. Microb. Biotechnol. 2014, 7, 517–527. [Google Scholar] [CrossRef]
- Dos Santos, S.F.; Cardoso, R.D.C.V.; Borges, Í.M.P.; Almeida, A.C.; Andrade, E.S.; Ferreira, I.O.; do Carmo Ramos, L. Post-harvest losses of fruits and vegetables in supply centers in Salvador, Brazil: Analysis of determinants, volumes and reduction strategies. Waste Manag. 2020, 101, 161–170. [Google Scholar] [CrossRef]
- Gould, L.H.; Walsh, K.A.; Vieira, A.R.; Herman, K.; Williams, I.T.; Hall, A.J.; Cole, D. Surveillance for foodborne disease outbreaks—United States, 1998–2008. Morb. Mortal. Wkly. Rep. Surveill. Summ. 2013, 62, 1–34. [Google Scholar]
- Mandrell, R.E. Enteric human pathogens associated with fresh produce: Sources, transport and ecology. In Microbial Safety of Fresh Produce; Blackwell Publishing: Hoboken, NJ, USA, 2009; pp. 5–41. [Google Scholar]
- Bennett, S.; Littrell, K.; Hill, T.; Mahovic, M.; Behravesh, C.B. Multistate foodborne disease outbreaks associated with raw tomatoes, United States, 1990–2010: A recurring public health problem. Epidemiol. Inf. 2015, 143, 1352–1359. [Google Scholar] [CrossRef] [PubMed]
- Devleesschauwer, B.; Marvasi, M.; Giurcanu, M.C.; Hochmuth, G.J.; Speybroeck, N.; Havelaar, A.H.; Teplitski, M. High relative humidity pre-harvest reduces post-harvest proliferation of Salmonella in tomatoes. Food Microbiol. 2017, 66, 55–63. [Google Scholar] [CrossRef] [PubMed]
- Stanaway, J.D.; Parisi, A.; Sarkar, K.; Blacker, B.F.; Reiner, R.C.; Hay, S.I.; Nixon, M.R.; Dolecek, C.; James, S.L.; Mokdad, A.H.; et al. The global burden of non-typhoidal Salmonella invasive disease: A systematic analysis for the Global Burden of Disease Study 2017. Lancet Infect. Dis. 2019, 19, 1312–1324. [Google Scholar] [CrossRef]
- WHO. WHO Estimates of the Global Burden of Foodborne Diseases: Foodborne Disease Burden Epidemiology Reference Group 2007–2015; World Health Organization: Geneva, Switzerland, 2015; Available online: https://apps.who.int/iris/handle/10665/199350 (accessed on 21 June 2020).
- Kirk, M.D.; Pires, S.M.; Black, R.E.; Caipo, M.; Crump, J.A.; Devleesschauwer, B.; Döpfer, D.; Fazil, A.; Fischer-Walker, C.L.; Hald, T. World Health Organization estimates of the global and regional disease burden of 22 foodborne bacterial, protozoal, and viral diseases, 2010: A data synthesis. PLoS Med. 2015, 12, e1001921. [Google Scholar]
- Majowicz, S.E.; Scallan, E.; Jones-Bitton, A.; Sargeant, J.M.; Stapleton, J.; Angulo, F.J.; Yeung, D.H.; Kirk, M.D. Global incidence of human Shiga toxin–producing Escherichia coli infections and deaths: A systematic review and knowledge synthesis. Foodborne Pathog. Dis. 2014, 11, 447–455. [Google Scholar] [CrossRef] [PubMed]
- Van Cauteren, D.; Le Strat, Y.; Sommen, C.; Bruyand, M.; Tourdjman, M.; Da Silva, N.J.; Couturier, E.; Fournet, N.; de Valk, H.; Desenclos, J.-C. Estimated annual numbers of foodborne pathogen–associated illnesses, hospitalizations, and deaths, France, 2008–2013. Emerg. Infect. Dis. 2017, 23, 1486. [Google Scholar] [CrossRef]
- EFSA. Salmonella . 2021. Available online: https://www.efsa.europa.eu/en/topics/topic/Salmonella (accessed on 22 March 2021).
- USDA. Cost Estimates of Foodborne Illnesses. 2021. Available online: https://www.ers.usda.gov/data-products/cost-estimates-of-foodborne-illnesses.aspx (accessed on 21 June 2020).
- Agency, F.S. The Burden of Foodborne Disease in the UK 2018. Available online: https://www.food.gov.uk/research/research-projects/the-burden-of-foodborne-disease-in-the-uk-2018 (accessed on 19 June 2020).
- Sundström, K. Cost of illness for five major foodborne illnesses and sequelae in Sweden. Appl. Health Econ. Health Policy 2018, 16, 243–257. [Google Scholar] [CrossRef]
- Ford, L.; Haywood, P.; Kirk, M.D.; Lancsar, E.; Williamson, D.A.; Glass, K. Cost of Salmonella Infections in Australia, 2015. J. Food Prot. 2019, 82, 1607–1614. [Google Scholar] [CrossRef]
- Jain, S.; Mukhopadhyay, K.; Thomassin, P.J. An economic analysis of Salmonella detection in fresh produce, poultry, and eggs using whole genome sequencing technology in Canada. Food Res. Int. 2019, 116, 802–809. [Google Scholar] [CrossRef]
- Suijkerbuijk, A.W.; Bouwknegt, M.; Mangen, M.-J.J.; de Wit, G.A.; van Pelt, W.; Bijkerk, P.; Friesema, I.H. The economic burden of a Salmonella Thompson outbreak caused by smoked salmon in the Netherlands, 2012–2013. Eur. J. Public Health 2017, 27, 325–330. [Google Scholar]
- EC. Control of Salmonella. 2020. Available online: https://ec.europa.eu/food/safety/biosafety/food_borne_diseases/Salmonella_en (accessed on 14 August 2020).
- Food.gov.uk. Meat Industry Guide- Microbiological Criteria. Available online: https://www.food.gov.uk/sites/default/files/media/document/Chapter13-Microbiological-criteria.pdf (accessed on 25 August 2020).
- WHO. Salmonella (non-typhoidal).2020. Available online: https://www.who.int/news-room/fact-sheets/detail/Salmonella-(non-typhoidal) (accessed on 21 March 2020).
- WHO. Promoting Safe Food Handling. 2019. Available online: https://www.who.int/foodsafety/areas_work/food-hygiene/en/ (accessed on 27 August 2020).
- CCOHS. Food and Kitchen Hygiene: OSH Answers. 2017. Available online: https://www.ccohs.ca/oshanswers/prevention/kitchen_hygiene.html (accessed on 27 August 2020).
- Adesokan, H.K.; Akinseye, V.O.; Adesokan, G.A. Food safety training is associated with improved knowledge and behaviours among foodservice establishments’ workers. Int. J. Food Sci. 2015, 2015. [Google Scholar] [CrossRef]
- CDC. Vital signs: Incidence and trends of infection with pathogens transmitted commonly through food--foodborne diseases active surveillance network, 10 US sites, 1996–2010. Mmwr. Morb. Mortal. Wkly. Rep. 2011, 60, 749–755. [Google Scholar]
- Almanza, B.A.; Nesmith, M.S. Food safety certification regulations in the United States. J. Environ. Health 2004, 66, 10. [Google Scholar]
- Yu, H.; Neal, J.; Dawson, M.; Madera, J.M. Implementation of behavior-based training can improve food service employees’ handwashing frequencies, duration, and effectiveness. Cornell Hosp. Q. 2018, 59, 70–77. [Google Scholar] [CrossRef]
- McFarland, P.; Checinska Sielaff, A.; Rasco, B.; Smith, S. Efficacy of food safety training in commercial food service. J. Food Sci. 2019, 84, 1239–1246. [Google Scholar] [CrossRef] [PubMed]
- National Restaurant Association. Restaurant Industry Facts at a Glance. 2019. Available online: https://www.restaurant.org/research/restaurant-statistics/restaurant-industry-facts-at-a-glance (accessed on 17 August 2020).
- CIoF. Why Food Safety Training Is Important. 2020. Available online: https://www.foodsafety.ca/blog/why-food-safety-training-important (accessed on 27 August 2020).
- FAO. Food Handlers: Manual • Instructor. 2017. Available online: http://www.fao.org/3/i5896e/i5896e.pdf (accessed on 21 June 2020).
- Mama, M.; Alemu, G. Prevalence, antimicrobial susceptibility patterns and associated risk factors of Shigella and Salmonella among food handlers in Arba Minch University, South Ethiopia. BMC Infect. Dis. 2016, 16, 1–7. [Google Scholar] [CrossRef]
- Solomon, F.B.; Wada, F.W.; Anjulo, A.A.; Koyra, H.C.; Tufa, E.G. Burden of intestinal pathogens and associated factors among asymptomatic food handlers in South Ethiopia: Emphasis on salmonellosis. Bmc Res. Notes 2018, 11, 1–6. [Google Scholar] [CrossRef] [PubMed]
- Europe Commission. Regulation (EC) No 853/2004. Specific Hygiene Rules for Food of Animal Origin. Available online: https://www.fsai.ie/uploadedFiles/Consol_Reg853_2004(1).pdf (accessed on 28 March 2020).
- Teffo, L.A.; Tabit, F.T. An assessment of the food safety knowledge and attitudes of food handlers in hospitals. BMC Public Health 2020, 20, 1–12. [Google Scholar] [CrossRef] [PubMed]
- Nkhebenyane, J.S.; Lues, R. The knowledge, attitude, and practices of food handlers in central South African hospices. Food Sci. Nut. 2020, 8, 2598–2607. [Google Scholar] [CrossRef] [PubMed]
- Moreb, N.A.; Priyadarshini, A.; Jaiswal, A.K. Knowledge of food safety and food handling practices amongst food handlers in the Republic of Ireland. Food Cont. 2017, 80, 341–349. [Google Scholar] [CrossRef]
- Yenealem, D.G.; Yallew, W.W.; Abdulmajid, S. Food Safety Practice and Associated Factors among Meat Handlers in Gondar Town: A Cross-Sectional Study. J. Environ. Public Health 2020, 2020. [Google Scholar] [CrossRef] [PubMed]
- Alvseike, O.; Røssvoll, E.; Røtterud, O.-J.; Nesbakken, T.; Skjerve, E.; Prieto, M.; Sandberg, M.; Johannessen, G.; Økland, M.; Urdahl, A.M. Slaughter hygiene in European cattle and sheep abattoirs assessed by microbiological testing and Hygiene Performance Rating. Food Cont. 2019, 101, 233–240. [Google Scholar] [CrossRef]
- Afreen, A.; Ahmed, Z.; Ahmad, H.; Khalid, N. Estimates and burden of foodborne pathogens in RTE beverages in relation to vending practices. Food Qual. Saf. 2019, 3, 107–115. [Google Scholar] [CrossRef]
- Gizaw, Z. Public health risks related to food safety issues in the food market: A systematic literature review. Environ. Health Prev. Med. 2019, 24, 1–21. [Google Scholar] [CrossRef] [PubMed]
- SafeFood. How to Cook Meat Safely. Available online: https://www.safefood.net/food-safety/cooking-meat (accessed on 28 March 2020).
- NHS. Eating Processed Foods. 2020. Available online: https://www.nhs.uk/live-well/eat-well/what-are-processed-foods/ (accessed on 17 August 2020).
- Huang, L.; Hwang, C.A. In-package pasteurization of ready-to-eat meat and poultry products. In Advances in Meat, Poultry and Seafood Packaging; Elsevier: Amsterdam, The Netherlands, 2012; pp. 437–450. [Google Scholar]
- Vestrheim, D.; Lange, H.; Nygård, K.; Borgen, K.; Wester, A.; Kvarme, M.; Vold, L. Are ready-to-eat salads ready to eat? An outbreak of Salmonella Coeln linked to imported, mixed, pre-washed and bagged salad, Norway, November 2013. Epidemiol. Infect. 2016, 144, 1756–1760. [Google Scholar] [CrossRef] [PubMed]
- Akbar, A.; Anal, A.K. Isolation of Salmonella from ready-to-eat poultry meat and evaluation of its survival at low temperature, microwaving and simulated gastric fluids. J. Food Sci. Technol. 2015, 52, 3051–3057. [Google Scholar] [CrossRef]
- Jongenburger, I.; Den Besten, H.; Zwietering, M. Statistical aspects of food safety sampling. Annu. Rev. Food Sci. Technol. 2015, 6, 479–503. [Google Scholar] [CrossRef]
- Husain, N.R.N.; Muda, W.M.W.; Jamil, N.I.N.; Hanafi, N.N.N.; Rahman, R.A. Effect of food safety training on food handlers’ knowledge and practices. Br. Food J. 2016, 118, 795–808. [Google Scholar] [CrossRef]
- Richard, A.; Brown, J.; Radhakrishna, R.; Yoder, E.; Nieto-Montenegro, S.; Cutter, C. Development and Implementation of a “Counter-Top”. Food Prot. Trends 2013, 33, 10–19. [Google Scholar]
- Schiellerup, P.; Krogfelt, K.A.; Locht, H. A comparison of self-reported joint symptoms following infection with different enteric pathogens: Effect of HLA-B27. J. Rheumatol. 2008, 35, 480–487. [Google Scholar] [PubMed]
- Tokuç, B.; Ekuklu, G.; Berberoğlu, U.; Bilge, E.; Dedeler, H. Knowledge, attitudes and self-reported practices of food service staff regarding food hygiene in Edirne, Turkey. Food Cont. 2009, 20, 565–568. [Google Scholar] [CrossRef]
| Food | Salmonella Serotypes | Survival Times | Reference |
|---|---|---|---|
| Dried milk products | S. Infantis, S. Typhimurium, S. Eastbourne | ≤10 months | [10] |
| Desiccated plastic surface Pasta | S. Typhimurium SL 1344, S. Infantis, S. Typhimurium, S. Eastbourne | <100 weeks | [11] |
| ≤12 months | [12] | ||
| Milk chocolate | S. Infantis, S. Typhimurium, S. Eastbourne | >9 months at 20 °C | [13] |
| Bitter chocolate | S. Eastbourne | ≤9 months at 20 °C | [13] |
| Halva | S. Enteritidis | >8 months at refrigeration temp | [14] |
| Peanut butter | S. Agona, S. Enteritidis, S. Michigan, S. Montevideo, S. Typhimurium | ≤24 weeks at 5 °C ≤6 weeks at 21 °C | [15,16] |
| Paprika powder | multiple serotypes | >8 months | [17] |
| Salmonella Strains | Pet/Pet Food Product | Cases | Locations Affected | References |
|---|---|---|---|---|
| S. Typhimurium | Small Pet Turtles | 34 reported cases and 11 Hospitalizations | 9 | [25] |
| S. Oranienburg | Small Pet Turtles | 26 reported cases and 8 Hospitalizations | 14 | [26] |
| S. Cerro S. Derby S. London S. Infantis S. Newport S. Rissen | Pig Ear Pet Treats | 154 reported cases and 35 hospitalizations | 35 | [27] |
| Salmonella spp. | Backyard Poultry | 1134 reported cases, 219 hospitalizations and 2 deaths | 49 | [28] |
| Salmonella spp. | Poultry in Backyard Flocks | 1120 reported cases, 249 hospitalizations and 1 death | 48 | [29] |
| S. Reading | Paws Ground Turkey Food for Pets | 90 reported cases | 26 | [30] |
| Salmonella spp. | Reptiles | 449 hospitalizations | Ireland | [31] |
| Salmonella Strain | Food Product | Cases | Locations Affected | References |
|---|---|---|---|---|
| S. Javiana | Pre-cut fruits | 165 reported cases and 73 hospitalizations | 14 | [25] |
| S. Newport | Red Onions | 640 reported cases and 85 hospitalizations | 43 | [38] |
| S. Javiana | Fruit Mix | 165 reported cases and 73 hospitalizations | 14 | [39] |
| S. Uganda | Cavi Brand Whole, Fresh Papayas | 81 reported cases and 27 hospitalizations | 9 | [40] |
| S. Newport | Frozen Raw Tuna | 15 reported cases and 2 hospitalizations | 8 | [41] |
| S. Carrau | Pre-Cut Melons | 137 reported cases and 38 hospitalizations | 10 | [42] |
| S. Uganda | Fresh Papayas | 81 reported cases and 27 hospitalizations | 9 | [43] |
| S. Dublin | Reblochon (bovine raw-milk cheese) | 83 reported cases and 41 hospitalizations and 10b deaths | France | [44] |
| S. Agona | infant milk products | 37 case and 18 were hospitalized | France | [45] |
| S. Infantis | Raw chicken products | 129 reported cases and 25 hospitalizations | 32 | [46] |
| S. Bovismorbificans | uncooked ham products | 57 cases and 15 hospitalizations | Netherlands | [47] |
| S. Mbandaka | Kellogg’s Honey Smacks Cereal | 135 reported cases and 34 hospitalizations | 36 | [48] |
| S. Enteritidis PT14b* | Egg and chicken products | 287 reported cases and 78 hospitalizations | North West and South of England | [49] |
| Salmonella Serovars | Illnesses | Deaths | References |
|---|---|---|---|
| S. enterica, non-typhoidal | 153,097,991 | 56,969 | [72] |
| Invasive non-typhoidal S. enterica | 596,824 | 63,312 | [72] |
| Invasive non-typhoidal S. enterica | 535,000 | 77,500 | [71] |
| S. enterica Paratyphi A | 4,826,477 | 33,325 | [73] |
| S. enterica Typhi | 20,984,683 | 144,890 | [73] |
| Country | Year (S) | Cost | Reference |
|---|---|---|---|
| UK | 2018 | £0.21 billion | [78] |
| Sweden | 2018 | €25.6 million | [79] |
| Australia | 2015 | AUD 146.8 million | [80] |
| Canada | 2000–2015 | CAD 287.78 million | [81] |
| Netherlands | 2012 | €6.8 million | [82] |
| USA | 2011 | USD 394 million | [41] |
| Organization | Regulations/Policies | Objective |
|---|---|---|
| European Commission | Regulation (EC) No 1177/2006 | Overall implement acts on application of antimicrobial agents and vaccines for poultry birds |
| Regulation (EC) No 2008/798/EC | Overall implement acts for importing live birds and eggs | |
| Regulation (EC) No 517/2011 | Reduction in flocks of laying hens | |
| Regulation (EC) No 200/2010 | Standard sampling and monitoring of Gallus gallus to reduce Salmonella among breeding stocks | |
| Decision (EC) No 1237/2007 | Strict requirement mandating all eggs meant for trade must follow national control programs across the chain | |
| Regulation (EC) No 200/2012 | Standard sampling and monitoring for reduction of Salmonella in broilers | |
| Regulation (EC) No 1190/2012 | Standard sampling and monitoring for reduction of Salmonella in fattening and breeding turkeys | |
| World Health Organization | Global Foodborne Infections Network (GFN) | Ensuring efficient oversight of antimicrobial-resistant Salmonella strains across the food chain; acquiring and testing samples along with data analysis |
| WHO Advisory Group on Integrated Surveillance of Antimicrobial Resistance (AGISAR) | Working with FAO in prompt detection and response to food outbreaks by supporting national competent authorities at such periods | |
| International Network of Food Safety Authorities (INFOSAN) | Provides risk assessment data that serve as guidelines for international standards and recommendations through the Codex Alimentarius Commission |
| Recommendations | Objectives |
|---|---|
| Prevention methods | Prevention steps should be applied at all stages of the food chain: from primary production, processing, distribution, sales and consumption. |
| Salmonella prevention steps recommended in the food handlers handbook should be followed. | |
| The contact between children and domesticated animals require supervision. | |
| The public is advised to follow national and regional surveillance systems on foodborne diseases to be aware, detect and respond rapidly to salmonellosis outbreaks early and halt the spread. | |
| Recommendations for the public and travellers | Food must always be cooked properly and served hot |
| Only pasteurized milk and its products should be consumed | |
| Fruits and vegetables should be washed adequately before consumption | |
| Hands should be washed adequately after contacting animals or using the restroom. | |
| Ice meant for consumption must be made from potable water | |
| Recommendations for food handlers | Food handlers should observe ingredients and follow hygienic food preparation rules. |
| Provision of Five keys to safer food which provides a basis for food safety training courses both for professionals and consumers. They centre on: keeping clean, separating raw from cooked foods, cooking adequately, storing at correct temperatures and use of potable water | |
| Recommendations for producers of fruits and vegetables | Practice good personal hygiene. |
| Faecal pollution should be avoided | |
| Only treated faecal waste is permitted | |
| Irrigation water should be treated and well managed. | |
| Recommendations for producers of aquaculture products | Practice good personal hygiene. |
| Pond environment should be clean | |
| Water quality should be managed. | |
| Harvest equipment should be hygienic | |
| Ensure fish is healthy. |
| Region | Study Type | Issues | References |
|---|---|---|---|
| South Africa (Hospital) | Interview using questionnaire | 29% of all food handlers never had a food safety training course. More than 60% of the hospital staff had either good or satisfactory Food Safety Knowledge (FSK) but these did not contribute to better Food Safety Outcomes. | [99] |
| South Africa (Hospices) | Semi-structured questionnaire | 68% had not taken basic food safety training. There was no knowledge of appropriate temperatures for refrigeration and hot RTE foods. | [100] |
| Ireland (Public) | Survey | Knowledge of food handling was below 10.8% and food poisoning below 20.1%—both were critically low. | [101] |
| Ethiopia | Survey | Unsatisfactory meet handling practice especially after smoking, sneezing, and coughing. | [102] |
| Norway, Denmark, Germany, Spain and the UK | Microbiological testing and Hygiene Performance Rating audits | Hygiene is a major issue in Slaughter Operational issues | [103] |
| Pakistan | Cross-tabulations, chi-square, and correlation tests. | Unhygienic vending practices for ready-to-eat foods | [104] |
| Global | Analysis of 81 full-text articles | Internalisation of food products across several countries increases risks for poor handling and food safety | [105] |
| Country | Training Method | Study Type | Behaviour | Conclusion | Reference |
|---|---|---|---|---|---|
| USA | Knowledge and behaviour-based online training video | Seven question quiz from Servy Safe coursebook | Observation by researcher | Behaviour-based training improves handwashing better than knowledge-based training especially during peak hours | [91] |
| Malaysia | Food safety training course based on regulations and behaviour training | 31 questions | Self-reported questionnaire and researcher observations | Behaviour-based training performed better in certain areas than the control group | [112] |
| USA | Two hours ServSave training | Questionnaire | Self-reported | Volunteers reported a significant increase in food safety knowledge, but behaviour is unchanged. Self-reported data is unreliable | [36] |
| USA | Customized lessons using ServSafe | Questionnaire | Researcher Observation | Significant improvement in Food safety knowledge | [113] |
| Korea | Lecture and demonstrations | Questionnaire | Self-reported questionnaire and researcher observations | Increase in knowledge was statistically significant Intervention did not produce a change in behaviour | [64] |
| USA | Four hours ServSafe class and behaviour training | Questionnaire | Researcher Observation | Hand washing knowledge and behaviour significantly Improved but these did not improve general compliance behaviour | [114] |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Ehuwa, O.; Jaiswal, A.K.; Jaiswal, S. Salmonella, Food Safety and Food Handling Practices. Foods 2021, 10, 907. https://doi.org/10.3390/foods10050907
Ehuwa O, Jaiswal AK, Jaiswal S. Salmonella, Food Safety and Food Handling Practices. Foods. 2021; 10(5):907. https://doi.org/10.3390/foods10050907
Chicago/Turabian StyleEhuwa, Olugbenga, Amit K. Jaiswal, and Swarna Jaiswal. 2021. "Salmonella, Food Safety and Food Handling Practices" Foods 10, no. 5: 907. https://doi.org/10.3390/foods10050907
APA StyleEhuwa, O., Jaiswal, A. K., & Jaiswal, S. (2021). Salmonella, Food Safety and Food Handling Practices. Foods, 10(5), 907. https://doi.org/10.3390/foods10050907