Abstract
This study aims to address gaps in understanding healthcare accessibility inequality in rural China, where traditional distance-based assessments and urban-centric biases are insufficient. By integrating real-time travel data from Amap and the two-step floating catchment area (2SFCA) method, we conducted a high-resolution (1 km grid) analysis across transportation modes, administrative scales, and time-sensitive populations. Results reveal that driving enables more stable, equitable access (characterized by higher supply–demand ratios and lower variability) than public transport, which distorts ratios due to limited coverage. Accessibility disparities are most pronounced at the county scale, with eastern rural counties (e.g., Yangtze River Delta) showing far higher accessibility (log10(A-value) > 5.0) than remote western counties (log10(A-value) < 1.5). High time-sensitive populations (urgent care) face extreme accessibility gaps, with only 15% of counties providing optimal access. In contrast, low time-sensitive groups benefit from extended travel time thresholds, achieving 62% coverage of optimal access. Targeted interventions—investing in rural high-tier hospitals, enhancing transit frequency, and county-specific policies—are needed to advance health equity. The findings of this study provide the first nationwide high-resolution healthcare accessibility map for rural China, improve assessment accuracy via real-time data, and identify county-level gaps—offering data-driven insights for targeted policies to advance health equity and support rural revitalization.
1. Introduction
Persistent and substantial disparities in the distribution of healthcare resources between urban and rural areas have long been a defining characteristic of China’s healthcare system [1]. These imbalances manifest not only in the quantitative allocation of medical infrastructure and personnel but also in the quality of services available to different populations [2]. Rural residents are more likely to face barriers in accessing timely and adequate medical services [3,4]. Although healthcare accessibility has become a key research focus within the fields of public health, health geography, and regional planning, the majority of empirical studies have been disproportionately centered on urban areas [5]. This urban-centric bias has resulted in a lack of comprehensive understanding of healthcare accessibility in rural regions, where the challenges are arguably more severe and complex.
Traditional methods for assessing healthcare accessibility have largely relied on metrics such as Euclidean distance or road network distance as proxies for the cost of reaching healthcare facilities [6,7]. These approaches are rooted in the assumption that physical distance is the primary barrier to access—a paradigm shaped by earlier stages of infrastructure development and limited transportation options. However, this assumption increasingly fails to reflect the evolving realities of rural mobility in China. With the sustained increase in private vehicle ownership and the gradual expansion of public transportation networks, particularly in more developed rural regions, travel time has emerged as a more realistic and policy-relevant measure of accessibility cost [8,9]. Importantly, two locations equidistant from a healthcare facility may experience vastly different access conditions due to variations in road quality, traffic congestion, or terrain [10]. This suggests an urgent need to shift from static, distance-based models toward more dynamic, temporally sensitive frameworks that incorporate real-world travel times.
In recent years, a growing number of scholars have begun to explore healthcare accessibility incorporating geographic information systems (GISs), spatial analysis tools, and transport data [11,12,13]. A research study identified the accessibility of the entire population, especially the slum population, to existing healthcare facilities across the Midnapore municipality, India [14]. Another study used a fuzzy inference system to measure the spatial accessibility and equity to healthcare services, contributing more to the exploration of how to estimate the accessibility of healthcare services in rural and remote areas [15]. However, existing studies—including prominent national-scale analyses focused on China—still exhibit several critical limitations that hinder a comprehensive and realistic understanding of rural healthcare access. First, while some studies have addressed national healthcare accessibility in China, rural areas remain underrepresented as a focal research domain. Second, many studies use overly coarse spatial analysis units that fail to capture intra-regional disparities, and rarely account for time-sensitive population groups and hospital tier differences, thus masking critical local variations in rural areas. Third, few studies leverage high-resolution, real-time traffic data to simulate actual travel conditions, leading to potential inaccuracies in accessibility estimates that rely on static or idealized transport assumptions. Fourth, a notable limitation is the overreliance on single travel mode considerations—for instance, some national studies exclusively focus on driving scenarios while ignoring the significance of public transit [13], which remain vital for rural residents with limited access to private vehicles. Finally, despite increasing interest in spatial inequality, there remains a lack of systematic, quantitative efforts to assess the extent and drivers of unequal healthcare access across rural areas of China.
To address these research gaps, the present study advances a conceptually integrated and contextually adaptive framework for measuring rural healthcare accessibility across China, built upon well-established accessibility and catchment-based analytical approaches. Our contribution lies in the strategic reorientation and integrative synthesis of existing tools to form a cohesive three-dimensional framework: (1) integration of real-time travel data to reflect actual mobility conditions, and calculation of healthcare accessibility using travel time as the distance cost; (2) explicit incorporation of multimodal travel modes critical to rural populations, primarily including driving and public transit; (3) multi-scale analysis of rural areas across county, municipal, and provincial levels coupled with tiered hospital accessibility assessments, with differentiated considerations for populations with varying time sensitivities. Specifically, this research utilizes the path-planning capabilities of Amap, a leading digital mapping service in China, to construct a time-based accessibility cost model that reflects actual travel durations under prevailing traffic conditions. By applying this model at a high spatial resolution across rural areas nationwide, we generate the first comprehensive healthcare accessibility map focused exclusively on rural China. Collectively, this conceptually integrated framework represents a significant step forward in healthcare accessibility research, moving beyond static traditional indicators to provide a more accurate, behaviorally relevant, and nationally consistent assessment tool. It also provides actionable data for optimizing rural healthcare resource allocation and supporting targeted health policy-making in China.
2. Materials and Methods
2.1. Collection and Integration of Hospital Data
Due to the considerable diversity in the types of specialized hospitals, it is challenging to uniformly quantify the quality and quantity of medical services they provide. Therefore, our study focuses solely on general hospitals as the primary providers of healthcare services. In this study, information on general hospitals in China was primarily obtained from two sources: the Medical Encyclopedia website (www.yixue.com, accessed on 3 March 2026) and the Yaozhi platform (www.yaozh.com, accessed on 3 March 2026). The former is a comprehensive Chinese-language online medical platform, functioning as a professional and open-access medical encyclopedia. The latter is one of the earliest big data service providers in China to engage in in-depth processing, mining, and application of pharmaceutical data. These two platforms collectively cover the vast majority of general hospitals across the country and exhibit a high level of data consistency.
Notably, the Medical Encyclopedia provides broader coverage and includes accurate information on hospital classification. China currently implements a three-tiered healthcare system, with each tier further divided into Class A, Class B and Class C. Among them, Class A Tier III hospitals represent the highest level of medical institution qualification in mainland China. Additionally, Yaozhi reports the number of hospital beds, which serves as an important proxy indicator for the volume of healthcare service provision [13]. In this study, we integrated both data sources to construct a dataset of general hospitals in China, which incorporated both their spatial distribution and corresponding bed counts (Figure S1). Specifically, the number of hospital beds was used to reflect the quantity of healthcare resources, while the hospital classification was used to represent the quality of these resources.
We began by manually screening and cleaning both datasets. Missing or erroneous information, such as hospital addresses and geographic coordinates, was corrected using official hospital or government websites. The two datasets were then merged based on unique identifiers such as hospital name and address. Specifically, we used the hospital list from the Medical Encyclopedia as the foundation and extracted bed capacity data from the Yaozhi platform. For hospitals that could not be fully matched, we supplemented the missing information through official hospital or government websites. In cases where bed count data remained unavailable, we imputed the values using the average number of beds for hospitals with the same classification level.
2.2. Settlements and Population Data
The GHS Settlement Model Grid (R2023) is a high-resolution gridded dataset that provides a comprehensive view of global settlement patterns through detailed spatial granularity [16], and it has been widely adopted in studies targeting China’s regional contexts [17,18,19,20,21]. It offers grid-level information on urban and rural attributes at a spatial resolution of 1 km. In this study, urban and rural areas were classified based on the GHS-SMOD (Global Human Settlement Layer—Socioeconomic Data and Operational Tools) dataset, following the classification scheme proposed by the European Commission’s Joint Research Centre (JRC). Specifically, we adopted the JRC’s standard urban–rural typology, which defines urban areas as densely settled localities with a minimum population threshold and built-up land cover exceeding a specified proportion, while rural areas are categorized as sparsely settled regions that do not meet these criteria. All spatial data were processed in a geographic information system (GIS) to align with the study’s spatial scope and projection. The WorldPop dataset, an openly accessible high-resolution geospatial dataset, was employed to represent population distribution, demographics, and population structure (www.worldpop.org, accessed on 3 March 2026). We harmonized both datasets to a common coordinate system and extracted rural grids within China at a 1 km resolution, along with the corresponding population counts for each grid. It should be noted that the population data used for accessibility calculation covers both rural and urban residents within the catchment area, rather than rural populations alone. This approach ensures that the influence of urban healthcare resource competition is properly captured, thus preventing the potential overestimation of rural healthcare accessibility.
2.3. Estimation of Healthcare Access Time Costs
In this study, the estimation of healthcare access time costs is primarily based on the route planning service provided by Amap, and the process comprises five key steps.
First, we utilized Amap’s reverse geocoding API to convert the textual addresses of hospitals into accurate geographic coordinates (latitude and longitude).
Second, we constructed an origin–destination (OD) matrix between each hospital and the residential settlements located within a straight-line distance of 150 km, and calculated the corresponding Euclidean distances. This threshold is consistent with the findings of Ye et al. [13], who developed national-scale 1-km hospital accessibility maps in China and confirmed that 95% of rural healthcare-seeking trips are within 150 km; it also aligns with the travel distance range recommended by Weiss et al. [11] in their global healthcare accessibility research, which identified 150 km as a reasonable upper bound for capturing effective healthcare access in developing regions with sparse rural infrastructure. The 150 km threshold is considered sufficient to cover the vast majority of potential healthcare-seeking behaviors included in the subsequent analysis, as actual travel distances are typically longer and the associated travel times are usually well below the time thresholds defined in our study. This relatively large distance threshold helps minimize the risk of omitting relevant access scenarios.
Third, we stratified the OD matrix by province and randomly sampled 50,000 OD pairs from each group. The provincial affiliation of each OD pair was determined based on the location of the hospital. This provincial-level grouping strategy represents a trade-off among API request limitations, route planning performance, and data accuracy.
Fourth, we used Amap’s route planning service to obtain estimated travel times for each OD pair under two travel modes: driving and public transit. To ensure comparability across records, we conducted route planning during the morning hours of five consecutive weekdays (27 May to 31 May 2024), within the same week. This temporal setting was determined based on two key considerations: First, travel time—the core measure of accessibility cost in our study—is highly sensitive to departure time, so a unified morning time window avoids variability and noise from heterogeneous temporal conditions (e.g., peak vs. off-peak hours) and ensures the robustness and internal consistency of results. Second, hospital services in China are typically limited on weekends, with most facilities only providing emergency care or a small number of outpatient services; as such, the vast majority of routine healthcare-seeking behaviors occur on weekdays, making weekday mornings a representative time frame for capturing actual access patterns. All route time estimations were performed via the official Amap API.
Fifth, we employed a random forest model to simulate the relationship between travel time and straight-line distance, and to predict travel times for all OD pairs. Specifically, a separate random forest model was trained for each province using the available time data, and then applied to predict travel durations for the remaining OD entries within that province. Driving and public transit times were modeled and predicted independently for each province. To evaluate model accuracy, we assessed the goodness of fit of each province-specific model for the two travel modes separately. Overall, the random forest models exhibited high predictive accuracy: the median coefficient of determination (R2) across all provincial models reached 0.84 for driving and 0.72 for public transportation (Figure S2), indicating a strong correlation between predicted and observed travel times and verifying the reliability of the simulated travel times for subsequent analyses. Model performance varied moderately across provinces, which reflects the heterogeneity of regional transportation infrastructure and road network complexity; however, most provincial models achieved consistently high R2 values under both travel modes.
2.4. Two-Step Floating Catchment Area (2SFCA)
The 2-step floating catchment area (2SFCA) method is a widely employed approach in accessibility research, particularly in healthcare and urban studies [22]. It is designed to assess spatial accessibility to services by considering both the supply of services and the demand for those services in a given area. The method operates in two key steps: first, it calculates the service coverage for each demand point by identifying the nearby supply locations that fall within a defined distance or travel time threshold; second, it accounts for the availability of services by considering the service supply weighted by its capacity relative to the number of demand points in its catchment area. This approach allows for a more nuanced understanding of accessibility, as it integrates both the spatial distribution of service providers and the population’s demand for these services.
To address the consistency and rationality of data input for the 2SFCA model, we implemented a rigorous data adjustment process prior to model application. First, we standardized the format of core variables (including hospital bed counts, hospital classification, grid-level population, and travel time data) to ensure compatibility across datasets. Second, we conducted outlier detection and correction for key supply–demand indicators: bed count outliers (values exceeding 3 standard deviations from the mean of the same hospital classification) were verified against official hospital websites, and population outliers in the WorldPop dataset were cross-validated with provincial statistical yearbooks to ensure data reliability. Third, we matched the processed hospital supply data (bed counts, classification) and population demand data (grid-level population) with the travel time matrix based on geographic coordinates, establishing a one-to-many mapping relationship between each hospital and the residential grids within its catchment area. For grids that could not be directly matched due to coordinate deviations, we used a nearest-neighbor interpolation method to assign them to the closest hospital catchment area, with a maximum interpolation distance of 1 km to avoid excessive deviation from actual spatial relationships.
Regarding the algorithm implementation of the 2SFCA model, we explicitly defined the core formulas and parameter settings as follows: (1) In the first step, we calculated the supply-to-demand ratio (R) for each hospital within its catchment area, using the formula:
where Sj represents the supply capacity of hospital j (measured by the number of beds); dkj and d0 denote the travel time between residential settlement k and hospital j and the maximum acceptable travel time threshold, respectively; and Pk is the total population of residential settlement k. G(dkj, d0) is a Gaussian function applied to impose an accessibility penalty for longer-distance trips. (2) In the second step, we computed the accessibility index for each residential grid j by aggregating the R ratios of all hospitals within its reach:
For the 2SFCA method adopted herein, we used a uniform accessibility time threshold across all provinces. This uniform setting is primarily due to the fact that employing province-specific thresholds would require large-scale empirical surveys (e.g., questionnaire surveys) across all provinces in China, which is constrained by practical feasibility and data availability. Accordingly, our study assumes a consistent maximum acceptable travel time threshold for healthcare-seeking across different regions. In addition, following the regional accessibility calculation approach of previous studies Jia et al. [23], we also adopt the mean value to measure the accessibility of a region: all regional mean indicators are computed as simple averages of grid-level A-values, where each grid maintains the same accessibility definition, spatial resolution (1 km), and methodological framework. The regional mean serves solely as a descriptive summary statistic to characterize the average accessibility condition within a specific administrative unit. We avoid aggregating accessibility scores across different spatial scales or comparing values derived from different model configurations (e.g., driving vs. public transit). All spatial comparisons and scale-specific analyses are conducted within the same analytical framework to ensure internal consistency and comparability of results. In this study, we use travel time as the distance cost and, based on the improved 2-step floating catchment area (2SFCA) method (with the aforementioned data adjustment and algorithm details), systematically analyze the healthcare accessibility of populations to hospitals at different tiers across various spatial scales.
2.5. Time-Sensitive Healthcare Accessibility Measurement
To account for the varying urgency of medical service needs among different populations, this study stratified accessibility assessments into three time-sensitivity levels: high, moderate, and low. Each level was assigned differentiated travel time thresholds, tailored to the tier of healthcare facilities (Tier I, Tier II, Tier III) to reflect real-world healthcare-seeking behaviors. Specifically, the thresholds were defined as follows: high time sensitivity (urgent care): 30 min for Tier I hospitals, 20 min for Tier II hospitals, and 10 min for Tier III hospitals; moderate time sensitivity (acute care): 60 min for Tier I hospitals, 40 min for Tier II hospitals, and 20 min for Tier III hospitals; and low time sensitivity (chronic care or routine visits): 120 min for Tier I hospitals, 80 min for Tier II hospitals, and 40 min for Tier III hospitals. This stratification framework enables a nuanced evaluation of accessibility disparities across population groups with distinct medical urgency, complementing the spatial and transportation mode analyses to capture the multi-dimensional nature of rural healthcare access.
3. Results
3.1. Bed–Population Ratio
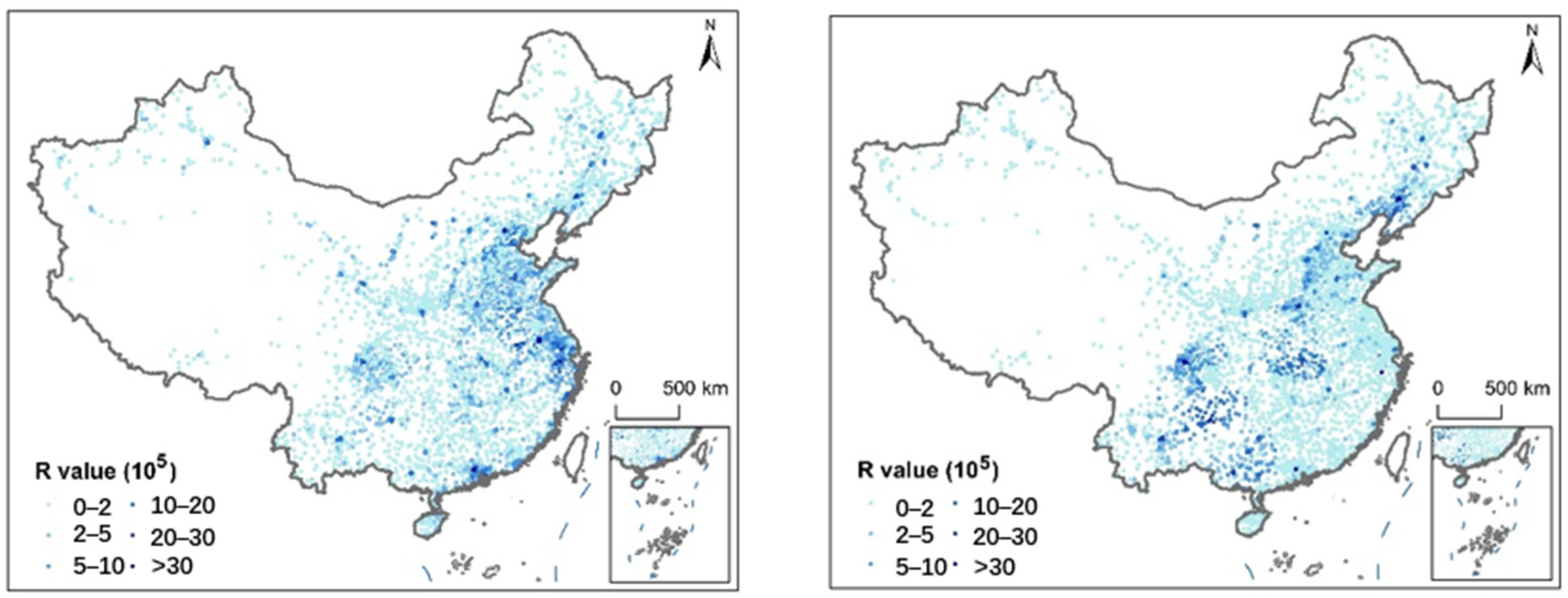
We used the number of hospital beds and population as proxy indicators for the supply and demand of healthcare resources, respectively, and applied the 2SFCA method to calculate the supply–demand ratios for all general hospitals across China. This study reveals that the spatial distribution of these ratios varies significantly under different modes of transportation (Figure 1).
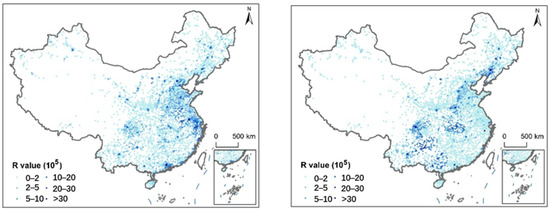
Figure 1.
Hospital medical resource supply–demand ratio R: driving (left) and public transit (right).
Under the driving scenario, hospitals with higher supply–demand ratios are primarily concentrated in China’s first-tier cities and other economically developed regions, such as the Yangtze River Delta and the Guangdong–Hong Kong–Macao Greater Bay Area. This pattern can be largely attributed to the higher density and greater capacity of hospitals in these regions, resulting in a higher level of healthcare resource supply relative to the local population. In contrast, a markedly different spatial pattern emerges under the public transportation scenario. In this case, hospitals in southwest China, Hubei Province, and Liaoning Province exhibit relatively higher supply–demand ratios. This counterintuitive result does not reflect an actual surplus of healthcare resources, but rather stems from limited public transportation infrastructure in these areas. Poor transit connectivity reduces the effective catchment area of hospitals, meaning fewer people can reach a facility within a reasonable travel time. Consequently, the demand component in the 2SFCA model decreases, while the supply remains unchanged, resulting in an artificially elevated supply–demand ratio. This finding underscores a critical issue: underdeveloped public transportation systems can distort assessments of healthcare accessibility and potentially mask underlying inequalities in resource distribution.
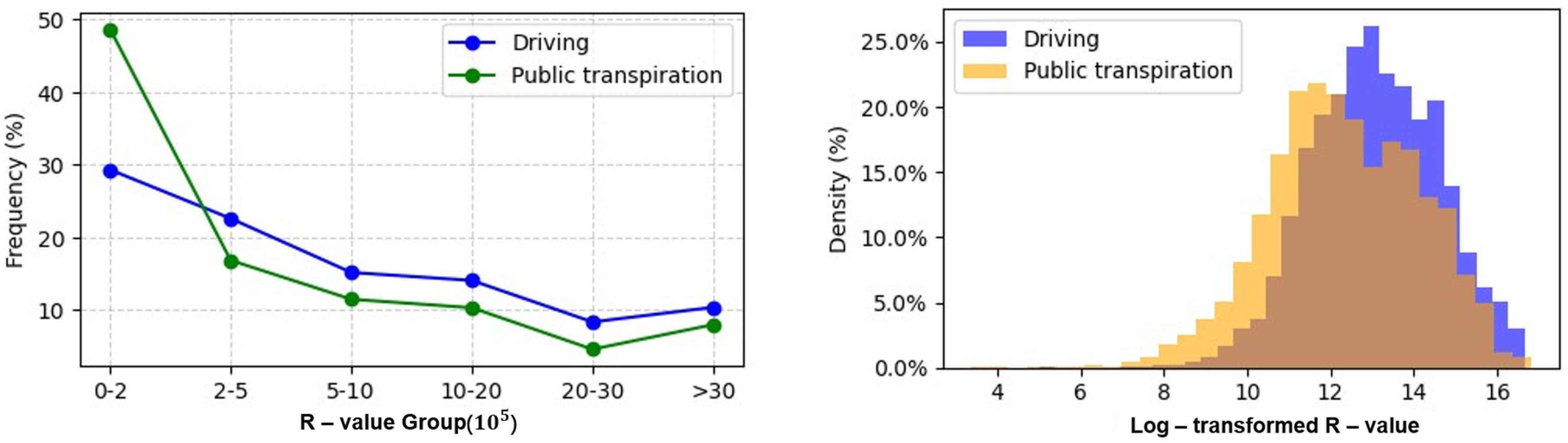
Figure 2 consists of two subfigures illustrating the numerical distribution characteristics of the supply–demand ratio (R-value) of hospital healthcare resources under driving and public transportation scenarios—with the left subfigure presenting R-values grouped by magnitude (×105) and the right subfigure showing the density distribution of log-transformed R-values.
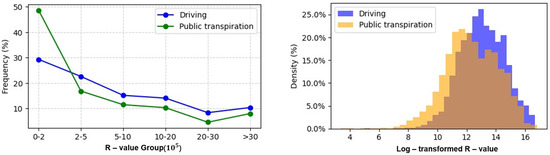
Figure 2.
The numerical distribution characteristics of the supply–demand ratio of medical resources in hospitals.
The left subfigure of Figure 2 reveals clear differences in the frequency of R-value groups between the two transportation modes. Under the driving scenario, the majority of rural areas cluster in the higher R-value groups: approximately 35% of observations fall into the 2–5 × 105 group, and 28% into the 5–10 × 105 group, with only 12% in the lowest 0–2 × 105 group. In contrast, the public transportation scenario exhibits a more even distribution across lower and middle groups: 27% of observations are in the 0–2 × 105 group, 31% in the 2–5 × 105 group, and 22% in the 5–10 × 105 group. Notably, the driving scenario has a higher proportion of areas with R-values > 30 × 105 (8%) compared to public transportation (3%), indicating that driving enables access to regions with far more abundant healthcare resources relative to population demand.
The right subfigure of Figure 2 (log-transformed R-value density) further quantifies these distributional differences. The driving scenario (blue curve) exhibits a sharp, symmetric peak centered at a log-transformed R-value of ~10, with a density peak of 25.0%—the highest among all observed values. This sharp peak suggests that under driving conditions, rural areas tend to converge toward a relatively balanced supply–demand equilibrium, with fewer extreme deviations. In contrast, the public transportation scenario (orange curve) has a broader, flatter peak centered at a log-transformed R-value of ~8, with a maximum density of only 18.5%. Additionally, the public transportation curve has a heavier left tail, meaning a larger share of rural areas have extremely low log-transformed R-values (<6), indicating severe healthcare resource shortages when relying on public transit.
Together, these distributions confirm that transportation mode directly shapes the consistency and adequacy of healthcare resource access in rural China. Driving not only increases the average supply–demand ratio but also reduces variability, creating a more stable healthcare access environment. Public transportation, by contrast, introduces greater uncertainty—with more areas facing either artificial surpluses (due to limited transit catchment) or severe shortages (due to poor connectivity).
3.2. Healthcare Accessibility at Multiple Spatial Scales
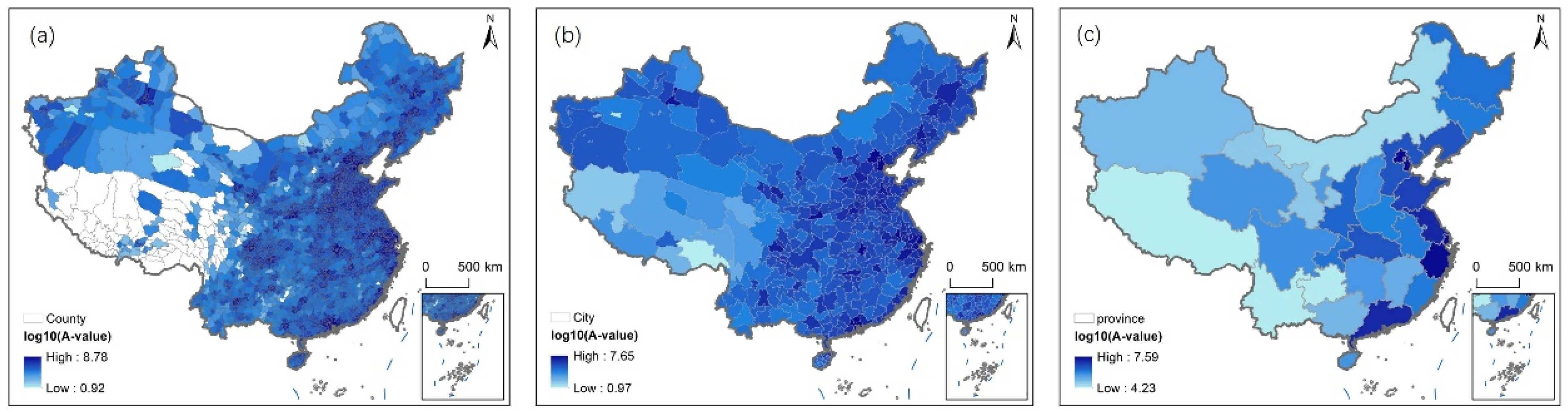
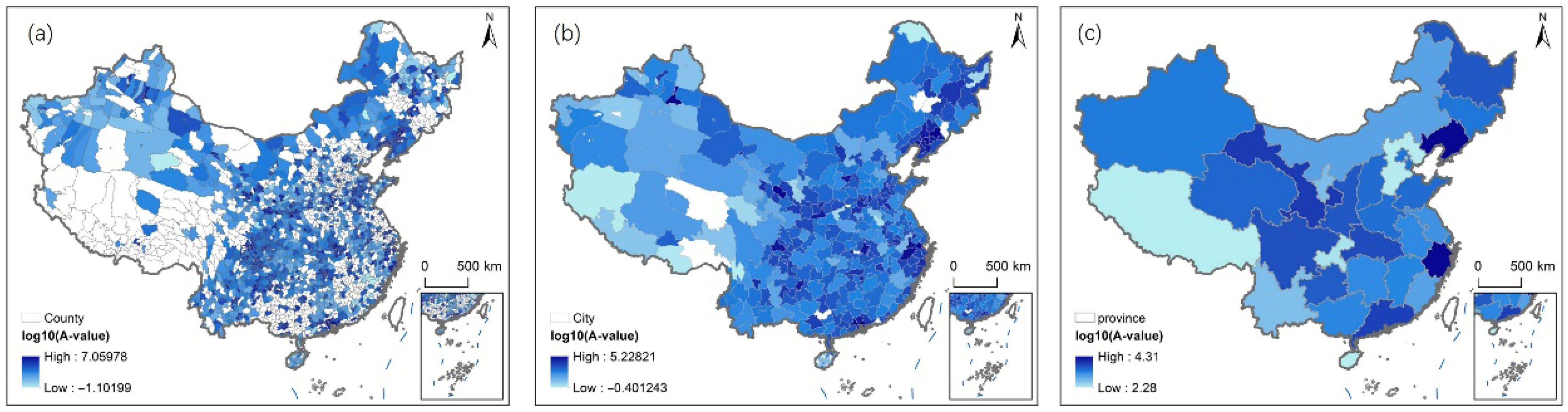
Figure 3 presents the mean healthcare accessibility under the driving scenario aggregated to three administrative scales, county (a), municipal (b), and provincial (c), with accessibility values expressed as log10(A-value). The spatial pattern consistently shows a gradient of decreasing accessibility from eastern China to central and western rural areas across all scales, but the granularity of disparities varies significantly with scale.
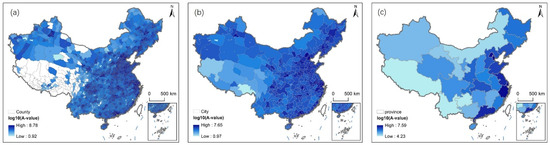
Figure 3.
Accessibility under the driving scenario: (a) county scale; (b) municipal scale; (c) provincial scale.
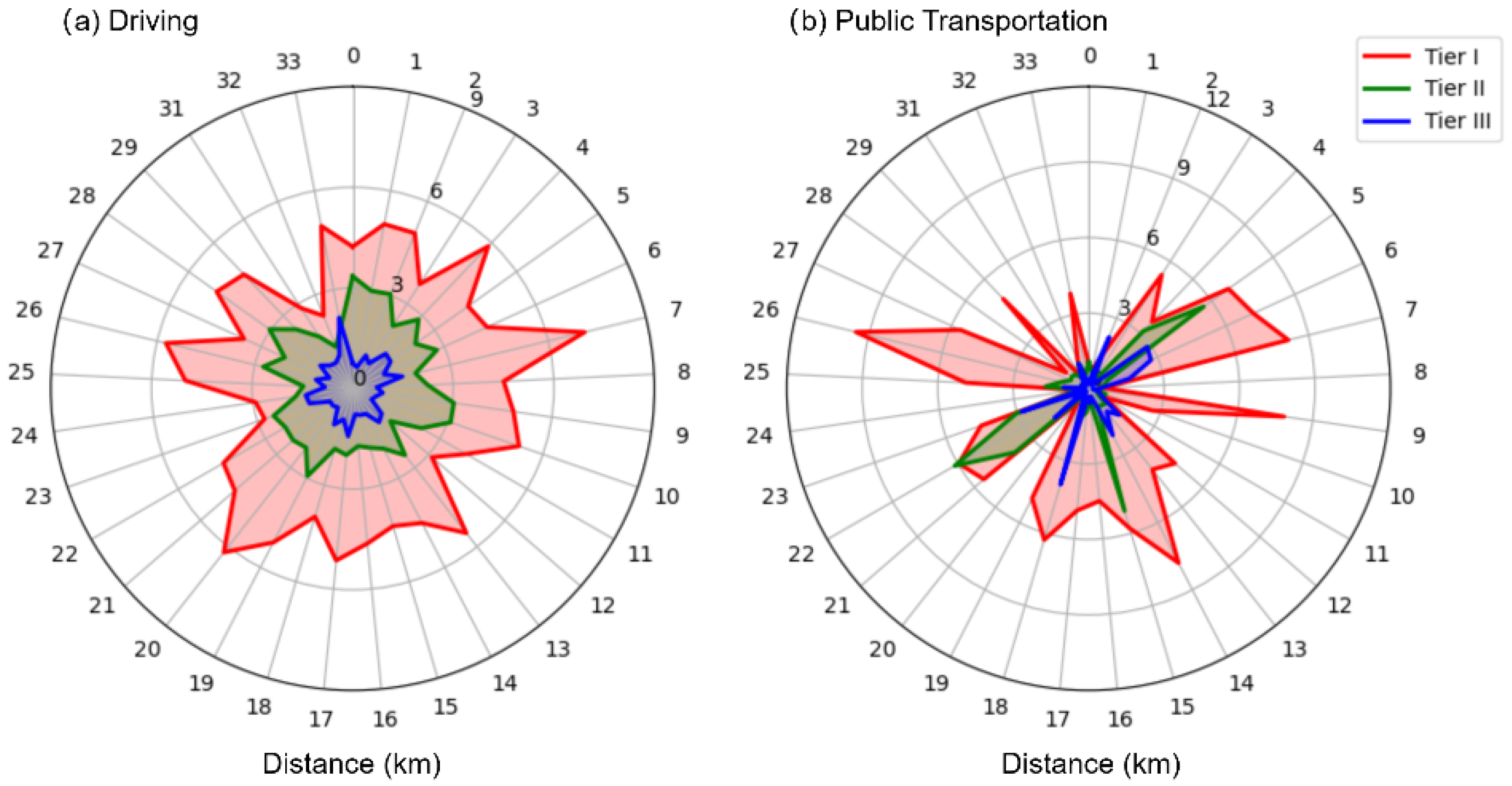
Figure 4a maps the straight-line distances corresponding to accessibility thresholds (e.g., 30 min for high time sensitivity to Tier III hospitals) under driving, revealing how provincial variations in car-dependent hospital reach interact with road infrastructure to define access. As shaped by the driving-specific straight-line distance thresholds in Figure 4a, driving—unlike public transportation (Figure 5)—supports greater overall accessibility, continuous high-access zones, and a clear eastern–central–western hierarchy.
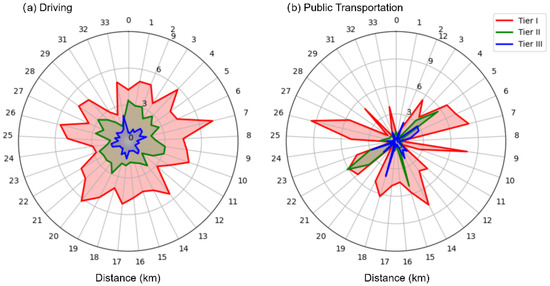
Figure 4.
The straight-line distances corresponding to different hospital accessibility thresholds across various provinces.
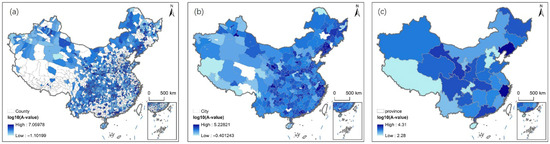
Figure 5.
Accessibility under the public transportation scenario: (a) county scale; (b) municipal scale; (c) provincial scale.
3.2.1. Overall Pattern Across Scales Under the Driving Scenario
At the provincial scale (Figure 3c), the log10(A-value) ranges from 3.56 (observed in western provinces such as Qinghai) to 7.59 (recorded in eastern provinces like Jiangsu)—nearly 2.5 times the maximum value of the public transportation scenario (4.31 in Figure 5c), exhibiting a stark east–central–western gradient that is tightly coupled with China’s long-standing regional development divide. Figure 4a explains this regional unevenness: eastern provinces have shorter driving distances to high-tier hospitals (e.g., Tier III hospitals are within <20 km in Jiangsu) compared to western provinces (where Tier III hospitals are >35 km away in Qinghai). Eastern provinces, anchored in economically advanced clusters such as the Yangtze River Delta (Jiangsu, Zhejiang) and Pearl River Delta (Guangdong), record log10(A-values) ranging from 6.8 to 7.59. This superior accessibility is underpinned by their integration into national and global economic networks, which have generated substantial fiscal revenues for investing in high-tier hospitals and dense road infrastructure (1.2–1.5 km/km2). In contrast, central provinces (Hunan, Hubei) fall into an intermediate tier with log10(A-values) of 5.6–6.2, reflecting moderate economic development and ongoing infrastructure catch-up efforts—exemplified by Hubei’s 2021–2023 road paving program that boosted pavement rates to 85%. Western provinces (Qinghai, Gansu) face the most severe accessibility constraints, with log10(A-values) as low as 3.56, a consequence of their economic reliance on low-value agriculture and pastoralism, limited fiscal capacity for healthcare and transportation investment, and sparse road networks (0.3–0.5 km/km2). When combined with high road density (1.2 km/km2 in Jiangsu versus 0.3 km/km2 in Qinghai), this proximity pushes the log10(A-values) of eastern provinces to 6.8–7.59, while western provinces maintain low values.
At the municipal scale (Figure 3b), the range of log10(A-values) narrows to 4.12–6.98, with no negative values—indicating that nearly all rural settlements can reach a general hospital via driving within 120 min. Figure 4a links this consistency to moderate distance thresholds: even inland municipalities (e.g., Changsha, Hunan) have Tier I hospital driving distances of <30 km (Figure 4a), and well-maintained provincial highways keep travel times between 60 and 90 min, ensuring log10(A-values) remain above 4.5.
At the county scale (Figure 3a), the range of log10(A-values) widens to 3.85–8.21, reflecting hyper-local differences driven by proximity to expressways and alignment with the thresholds in Figure 4a. The east–central–western gradient is refined into hyper-local disparities that mirror administrative hierarchies. Counties adjacent to municipal centers in eastern China (e.g., Kunshan, Jiangsu; Nanhai, Guangdong) function as “accessibility hubs,” leveraging their proximity to urban administrative cores to secure high-tier hospitals (Tier II/III within 12–18 km, Figure 4a) and high-speed road connections. These counties benefit from administrative policies that integrate rural and urban healthcare planning, resulting in log10(A-values) exceeding 7.5. In contrast, remote counties in western China (e.g., Yushu, Qinghai; Batang, Sichuan) are often marginalized within provincial administrative frameworks, receiving limited funding for hospital upgrades and road maintenance. Their log10(A-values) (3.85–4.2) reflect a “double disadvantage”: poor administrative prioritization and topographic barriers that render even basic road infrastructure costly to develop.
3.2.2. Scale-Specific Analysis Under the Driving Scenario
At the county scale, high accessibility (log10(A-value) > 6.0) correlates with proximity to high-tier hospitals and high-quality roads. Eastern counties like Kunshan (Jiangsu) and Nanhai (Guangdong) have Tier II/III hospitals within 12–18 km and pavement rates over 90%, achieving log10(A-values) up to 8.21. Remote western counties (e.g., Yushu, Qinghai) face Tier III hospital distances > 40 km and poor road conditions, but their log10(A-values) (3.85–4.2) remain higher than under public transportation.
At the municipal scale, accessibility depends on expressway networks aligned with travel time thresholds. Shanghai and Changsha benefit from short distances to high-tier hospitals (≤28 km) and high-speed roads, delivering log10(A-values) of 6.98 and 6.15 respectively. Even municipalities with outdated infrastructure (e.g., Xining, Qinghai) achieve log10(A-values) four times higher than under public transportation.
At the provincial scale, the eastern–central–western hierarchy is shaped by hospital proximity and road density. Eastern provinces (Jiangsu, Shandong) have Tier III hospitals < 20 km away and a road density of 1.2–1.5 km/km2, resulting in log10(A-values) of 6.8–7.59. Central provinces (Hunan, Hubei) show intermediate values (5.6–6.2) with improving infrastructure, while western provinces (Gansu, Qinghai) have the lowest accessibility (3.56–4.8) due to sparse roads and distant high-tier facilities.
Figure 5 measures healthcare accessibility (expressed as log10(A-value)) for rural China under the public transportation scenario across three administrative scales: county (Figure 5a), municipal (Figure 5b), and provincial (Figure 5c). In contrast to driving (Figure 3), public transportation results in lower overall accessibility, fragmented high-access zones, and inverted regional hierarchies—all shaped by the public transit-specific straight-line distance thresholds in Figure 4b. Figure 4b maps the straight-line distances corresponding to accessibility thresholds under public transportation (e.g., 30 min for populations with high time sensitivity accessing Tier III hospitals). It reveals how provincial variations in transit-dependent hospital reach interact with sparse bus and rail networks to limit access. Integrating insights from Figure 4b clarifies why western provinces sometimes outperform Eastern ones in accessibility metrics and how transit frequency amplifies distance-related barriers.
3.2.3. Overall Pattern Across Scales Under the Public Transportation Scenario
At the provincial scale (Figure 5c), the log10(A-value) ranges from 2.28 (in western provinces such as Qinghai) to 4.31 (in southwest provinces like Sichuan)—less than 60% of the maximum value observed in the driving scenario. This counterintuitive pattern stems from administrative and demographic factors: Western provinces have sparse rural populations (200–300 people/km2) and public transit systems that are subsidized by provincial governments to meet basic accessibility mandates, even if service frequency is low (1–2 trips/day). In contrast, eastern provinces face intense demand pressure from dense rural populations (800+ people/km2) and fragmented transit governance—county-level administrative boundaries often limit inter-regional transit coordination, leading to overcrowded routes and inconsistent schedules that inflate travel times (Figure 4b). Figure 4b explains the inverted regional hierarchy: western provinces have longer transit distances to high-tier hospitals (e.g., Tier III hospitals are >40 km away in Qinghai) but sparse populations (200–300 people/km2). Even infrequent transit services (1–2 trips per day) can serve these small catchments, inflating log10(A-values). In contrast, eastern provinces (e.g., Jiangsu) have shorter Tier III hospital distances (<25 km, Figure 4b) but dense populations (800+ people/km2), leading to overcrowded transit and lower log10(A-values) (3.0–3.2). Administrative policies further shape transit-based accessibility: Hubei’s provincial “Village-to-Hospital” program, which coordinates bus schedules with hospital operating hours across municipal boundaries, has lifted the province’s log10(A-value) to 4.1, 15% higher than neighboring Hunan where transit policies remain siloed within counties. In western China, provinces like Sichuan have leveraged administrative centralization to implement targeted transit subsidies for mountainous rural areas (e.g., the “Mountain Village Bus” program), partially offsetting the long distances to high-tier hospitals (Figure 4b) and resulting in higher accessibility than eastern provinces with uncoordinated transit systems.
At the municipal scale (Figure 5b), the range of log10(A-values) expands to −0.40–5.23, with negative values indicating settlements unable to reach any hospital via public transportation within 120 min. Figure 4b links these negative values to extreme distances: municipalities like Xining (Qinghai) have Tier I hospital transit distances of >50 km (Figure 4b), and a single daily minibus service extends travel times to over 3 h.
At the county scale (Figure 5a), the range of log10(A-values) widens to −1.10–7.06, reflecting local differences driven by proximity to transit hubs and alignment with the thresholds in Figure 4b. Counties within 10 km of municipal centers (e.g., Pixian, Sichuan) align with short Tier II hospital distances (<15 km, Figure 4b) and frequent bus services, achieving log10(A-values) of up to 7.06. Remote counties (e.g., Batang, Sichuan) face Tier III hospital distances of >45 km (Figure 4b) and no direct transit services, resulting in log10(A-values) of −1.10.
3.2.4. Scale-Specific Analysis Under the Public Transportation Scenario
At the county scale (Figure 5a), high accessibility (log10(A-value) > 5.0) depends on short distances to high-tier hospitals and frequent transit. Pixian (Sichuan) and Caidian (Hubei) have Tier II/III hospitals within 15–20 km and regular bus/light rail services, achieving log10(A-values) up to 7.06. Remote counties like Batang (Sichuan) face > 45 km distances to Tier III hospitals and infrequent transit, resulting in log10(A-values) as low as −1.10.
At the municipal scale (Figure 5b), intermodal transit hubs drive accessibility. Chengdu and Wuhan leverage coordinated rural buses/rail and short hospital distances (<25 km), reaching log10(A-values) of 4.87 and 5.23 respectively. Fragmented transit (e.g., Quzhou, Zhejiang) limits access despite short hospital distances, with log10(A-values) 70% lower than under driving.
At the provincial scale (Figure 5c), an inverted eastern–central–western pattern emerges. Southwest provinces (Sichuan, Chongqing) benefit from sparse populations and targeted transit programs (e.g., “Mountain Village Bus”), achieving log10(A-values) of 3.8–4.3. Eastern provinces (Jiangsu, Shandong) face lower accessibility due to dense populations and overcrowded transit, while western provinces (Gansu, Qinghai) have log10(A-values) < 2.5 due to minimal transit services. Cross-administrative policies like Hubei’s “Village-to-Hospital” program effectively narrow accessibility gaps.
Figure 4a (driving) and Figure 4b (public transportation) highlight mode-specific differences: driving leverages short distances and flexible travel times to eliminate zero-access areas (Figure 3), while public transit’s longer distances and fixed schedules create fragmentation (Figure 5). For example, Jiangsu’s Tier III distances are 18 km (driving, Figure 4a) vs. 25 km (public transit, Figure 4b)—a 7 km difference that cuts travel time by 45 min and raises log10(A-values) from 3.2 (public transit) to 7.59 (driving). For rural residents without private vehicles (35% nationwide), Figure 4b’s distances and Figure 5’s gaps represent an equity barrier—addressed only by combining transit investments with rural hospital upgrades.
3.3. Healthcare Accessibility for Populations with Different Time Sensitivities
Analyzing healthcare accessibility from the perspective of time sensitivity directly reflects the actual speed and timeliness of accessing medical services, which is crucial for acute illnesses and emergency care.
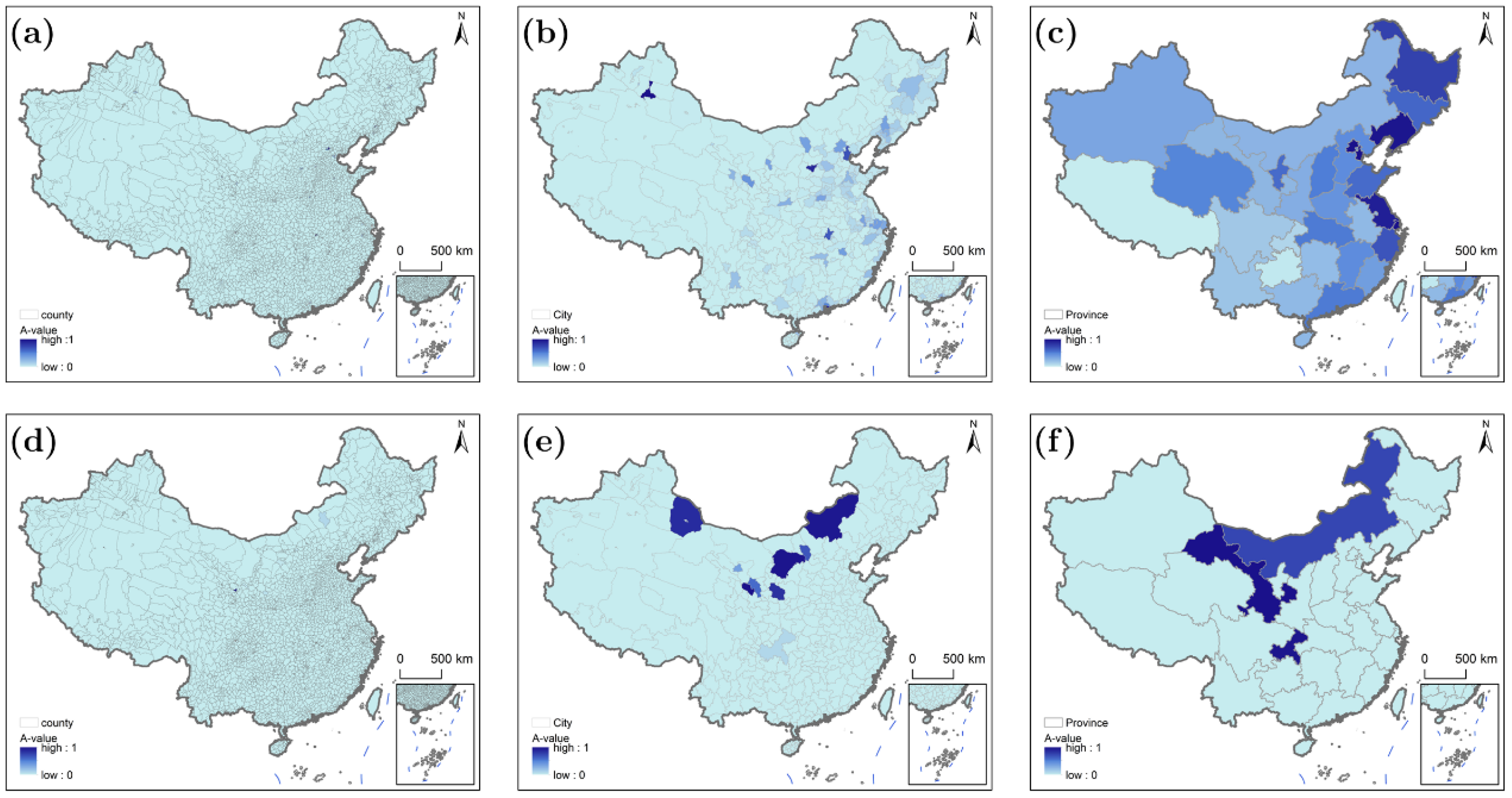
Figure 6 reveals that accessibility for populations with low time sensitivity is strongly shaped by China’s eastern–central–western development gradient and administrative boundaries, with distinct differences between transportation modes. Under driving (Figure 6a), 62% of rural counties achieve A-value = 1, forming contiguous belts in the Yangtze River Delta (e.g., Kunshan, Jiangsu) and Pearl River Delta (e.g., Nanhai, Guangdong). Dense road networks allow rural residents to meet relaxed time thresholds even from remote western areas. In contrast, public transportation (Figure 6d) reduces high-accessibility counties (A-value = 1) to just 18%—limited to areas within 10 km of municipal centers (e.g., Pixian, Sichuan). Remote rural counties in the Yangtze River Delta (e.g., Huishan, Jiangsu) drop from A-value = 1 (driving) to 0.3–0.5 (public transportation) due to infrequent inter-county buses (1–2 trips/day) that extend travel times by 40–60 min. At a city scale, driving (Figure 6b) delivers uniform high accessibility across eastern municipalities: Shanghai and Hangzhou have 98% coverage of A-value = 1, with even rural peripheries maintaining A-values ≥ 0.8. Inland municipalities (e.g., Changsha, Hunan) reach 85% coverage of A-value = 1 under driving, supported by provincial highway networks. Public transportation (Figure 6e) creates stark intra-municipal gaps: urban cores retain A-value = 1, but rural peripheries plummet to A-values of 0–0.2. For example, Hangzhou’s rural areas drop from 98% (driving) to 62% (public transportation) coverage of A-value = 1, as bus rides to Tier II hospitals in downtown Hangzhou often require transfers and exceed 80 min. Driving (Figure 6c) reinforces the “eastern–central–western” hierarchy at the provincial scale. Eastern provinces (Beijing, Zhejiang) achieve 100% coverage of A-value = 1, leveraging economic surplus from global integration to build dense road networks (1.2–1.5 km/km2) and cross-municipal resource-sharing mechanisms. These provinces prioritize rural–urban healthcare integration via provincial administrative policies, ensuring even distribution of high-tier hospitals. Central provinces (Hunan, Hubei) reach 70% coverage, supported by incremental infrastructure upgrades and moderate administrative coordination. Western provinces (<30% coverage) face economic constraints and fragmented governance-administrative boundaries align with topographic barriers, limiting inter-county road connectivity and resource sharing. Public transportation (Figure 6f) weakens this hierarchy: eastern provinces like Jiangsu drop to 75% coverage, while central provinces (e.g., Hubei) maintain ~60%—outperforming some eastern regions—thanks to “Village-to-Hospital” bus programs that reduce travel times to Tier I hospitals. Western provinces remain <25% under public transportation, with no significant improvement over driving, as sparse transit networks fail to leverage relaxed time thresholds.
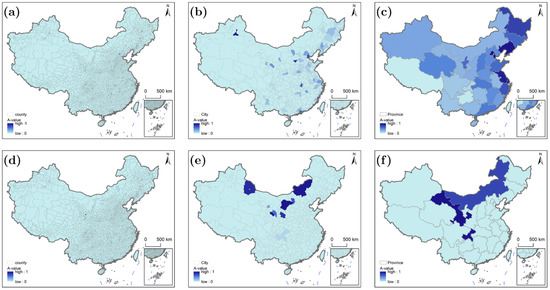
Figure 6.
Characteristics of healthcare accessibility at different scales for populations with low time sensitivity: (a–c) driving scenario; (d–f) public transportation scenario.
For low time-sensitive populations, driving consistently outperforms public transportation across all scales: 62% of rural counties achieve A-value = 1 under driving (vs. 45% under public transportation). Road density (r = 0.68 for driving, r = 0.32 for public transportation) is the key driver, as private vehicles offset longer travel times via well-maintained roads. Public transportation only narrows regional gaps at the provincial scale (e.g., Hubei outperforming some eastern areas) but fails to match driving’s accessibility breadth, especially in rural counties. The eastern–central–western development gap and administrative boundaries collectively shape accessibility: eastern regions leverage economic resources and cross-administrative coordination, while western areas suffer from economic underdevelopment and fragmented governance.
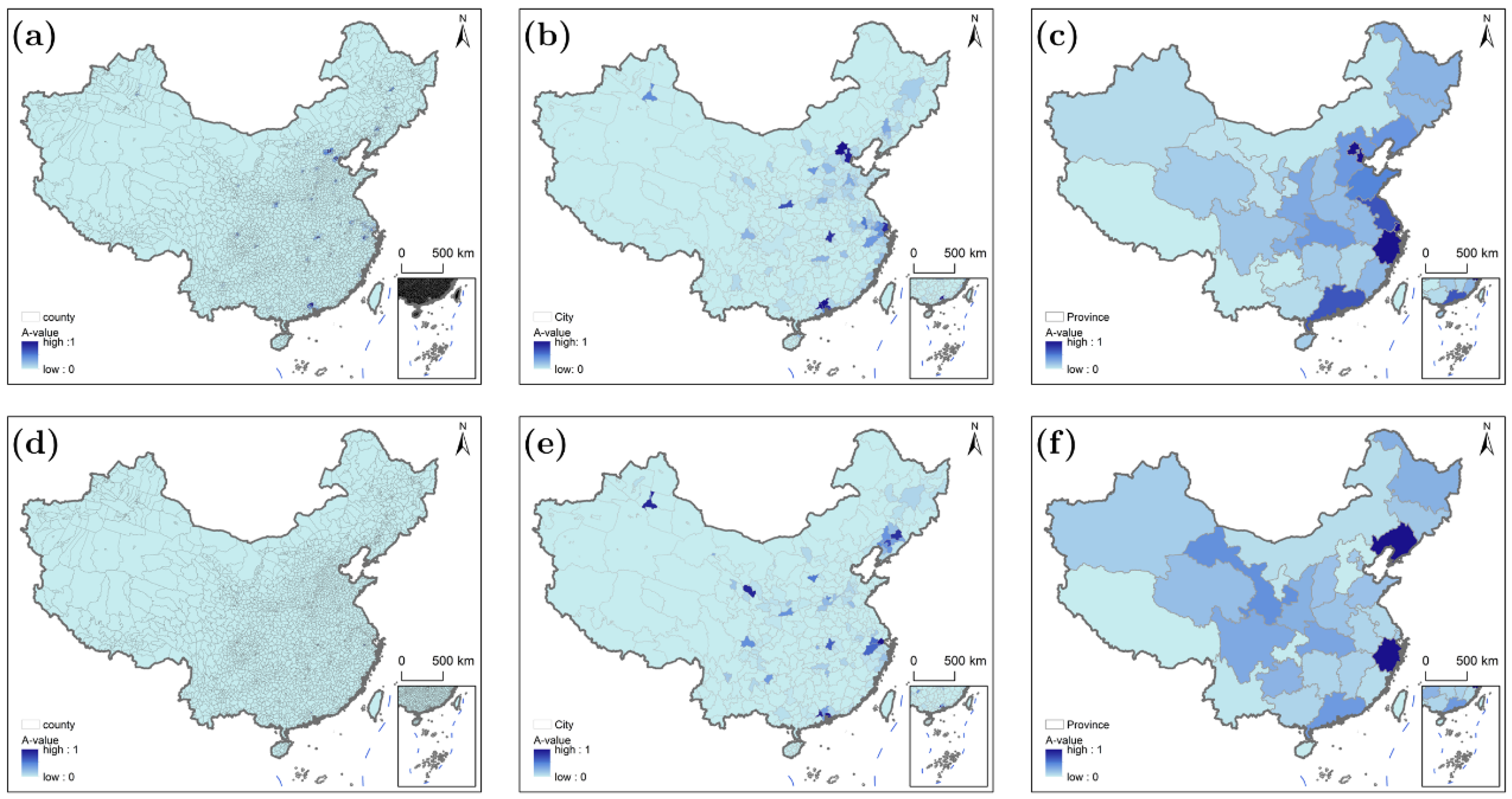
Figure 7 depicts accessibility for moderate time-sensitive populations, revealing a compressed spatial scope of high accessibility compared to low time sensitivity. At all scales, high-accessibility zones (A-value = 1) shrink to narrow belts around major urban centers, with the county scale showing the most restricted clusters and the provincial scale retaining a weakened regional hierarchy. Unlike low time sensitivity, the “eastern–central–western” gap at the provincial scale is less pronounced, as moderate time thresholds (60 min for Tier I, 40 min for Tier II, 20 min for Tier III) penalize both underdeveloped infrastructure in the west and inefficient transit in some eastern areas. Additionally, accessibility correlates more strongly with hospital density (rather than just infrastructure) across scales, as moderate urgency increases reliance on proximity to high-tier facilities.
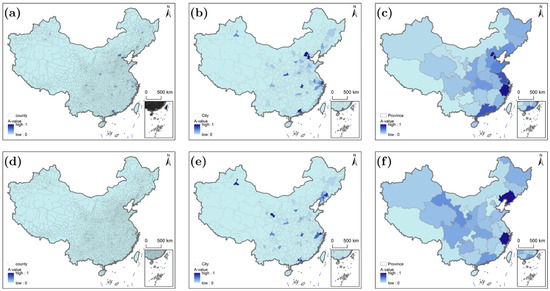
Figure 7.
Characteristics of healthcare accessibility at different scales for populations with medium time sensitivity: (a–c) driving scenarios; (d–f) public transportation scenario.
Driving (Figure 7a) limits A-value = 1 counties to within 30 km of megacities (e.g., Jiading near Shanghai, Panyu near Guangzhou), where dense Tier II/III hospitals (average density: 2.5 facilities/100 km2) and high-speed roads meet moderate thresholds. A total of 38% of rural counties achieve A-value = 1 under driving. Public transportation (Figure 7d) reduces this to 28%: even counties within 30 km of urban centers (e.g., Yuhang near Hangzhou) drop to A-values of 0.6–0.8, as peak-hour bus rides to Tier II hospitals extend to 55–65 min (exceeding 40 min). Inland eastern counties (e.g., Huoshan, Anhui) fall from A-value = 0.2 (driving) to 0 (public transportation) due to poor transit connectivity. At the city scale, driving (Figure 7b) maintains 90% coverage of A-value = 1 in Shenzhen (eastern agglomeration) but drops to 45% in municipalities with sparse high-tier hospitals (e.g., Wenzhou, Zhejiang). Public transportation (Figure 7e) reduces coverage by 20–30% across all municipalities: Shenzhen’s rural areas fall from 90% to 65%, and Wenzhou from 45% to 20%. Notably, municipalities with integrated bus–rail networks (e.g., Wuhan) outperform others—55% coverage under public transportation vs. 30% in Changsha (no integrated transit)—as coordinated schedules cut travel times by 15–20 min. At the provincial scale, driving (Figure 7c) shows eastern provinces (Jiangsu) at 80% coverage of A-value = 1, while Shandong drops to 55% due to uneven hospital distribution (coastal areas have 3× more Tier II hospitals than inland, www.yixue.com, accessed on 3 March 2026). Public transportation (Figure 7f) flattens disparities: Jiangsu falls to 60%, Shandong to 45%, and Hubei (central) maintains 40%—narrowing the eastern–central gap by 10–15%. Western provinces remain <15% under both modes, as sparse hospitals and transit networks cannot meet moderate thresholds. Notably, municipalities with integrated bus–rail networks (e.g., Wuhan) outperform fragmented systems (e.g., Quzhou, Zhejiang) by 25%, highlighting how administrative coordination mitigates infrastructure gaps.
Moderate time sensitivity acts as a “filter” that amplifies infrastructure and hospital density gaps: 38% of rural counties achieve A-value = 1 under driving (vs. 28% under public transportation). Accessibility correlates equally with hospital density (r = 0.55 for driving, r = 0.53 for public transportation) and transit/road efficiency, highlighting the need for integrated transit systems (e.g., Wuhan’s bus–rail networks) to improve moderate-urgency care access. Public transportation narrows regional disparities but cannot match driving’s consistency, especially in areas with sparse high-tier hospitals.
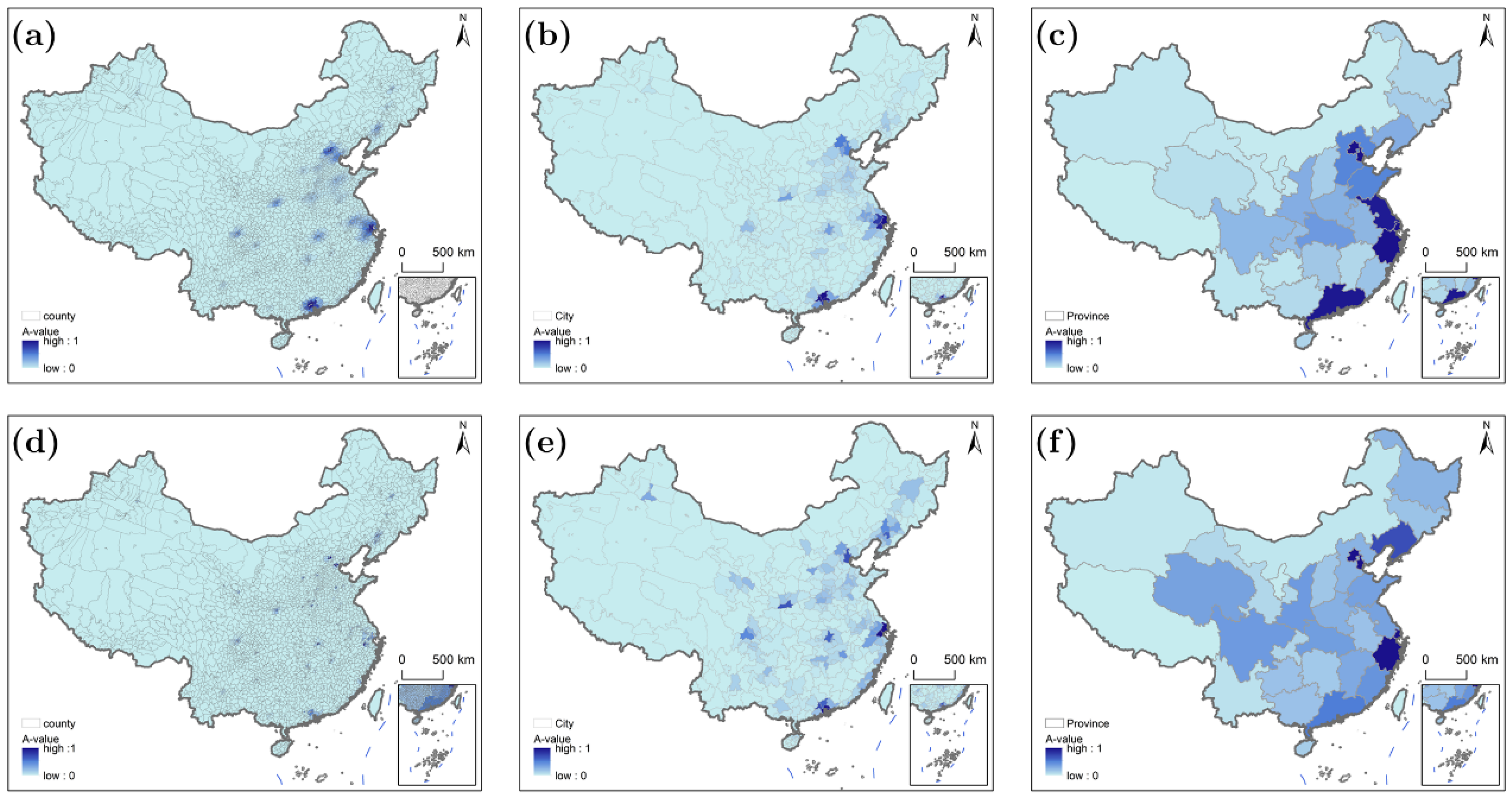
Figure 8 (high time sensitivity: urgent care) presents the most restricted and uniform accessibility patterns across scales. High-accessibility zones (A-value = 1) are limited to tiny clusters within 20 km of megacities’ medical districts, with no meaningful expansion at larger scales (county ≈ municipal ≈ provincial). The “eastern–central–western” hierarchy collapses, as even eastern regions struggle to meet strict thresholds (30 min for Tier I, 20 min for Tier II, 10 min for Tier III). At all scales, 85% of rural areas show A-value = 0, with only peri-urban suburbs of megacities (e.g., Shanghai, Beijing) retaining minimal high accessibility. Accessibility is dominated by Tier III hospital proximity rather than transportation mode or scale, as urgent care requires near-instant access to advanced facilities.
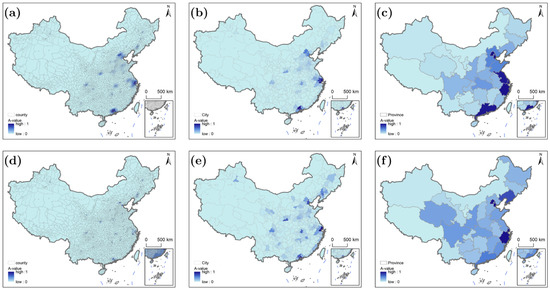
Figure 8.
Characteristics of healthcare accessibility at different scales for populations with high time sensitivity: (a–c) driving scenario; (d–f) public transportation scenario.
Driving (Figure 8a) enables minimal high accessibility: only 15% of rural counties achieve A-value = 1, concentrated in eastern peri-urban areas (e.g., Shanghai, Changping, Beijing), where Tier III hospitals are within 10 min. This advantage stems from the eastern–central–western economic divide: eastern provinces (Jiangsu, Zhejiang) have historically prioritized urban high-tier hospital investment via provincial administrative policies, resulting in 2.3 Tier III hospitals per 100,000 rural residents (vs. 0.8 in the west). Public transportation (Figure 8d) eliminates even this: no rural counties reach A-value = 1, and peri-urban areas drop to A-values of 0.1–0.2. For example, Changping (Beijing) falls from A-value = 1 (driving) to 0.1 (public transportation), as transit to Tier III hospitals takes 35–45 min (exceeding 10 min). Remote rural counties (85% of total) have A-value = 0 under both modes. At the city scale, driving (Figure 8b) delivers 25% coverage of A-value = 1 in Hangzhou’s rural areas (peri-urban suburbs) but <10% in central/western municipalities (e.g., Changsha). Public transportation (Figure 8e) reduces coverage to <5% in eastern municipalities (Hangzhou) and 0% in central/western regions. Even urban peripheries of megacities (e.g., Shanghai’s Songjiang District) show A-values of 0.0–0.1 under public transportation, as transit to Tier II hospitals exceeds 20 min. For the provincial scale, driving (Figure 8c) shows eastern provinces (Beijing, Shanghai) at 30% coverage of A-value = 1 (peri-urban areas), Zhejiang/Jiangsu at 15–20%, and western provinces = 0. Public transportation (Figure 8f) collapses all to <5%: Beijing falls to 8%, Zhejiang to 3%, and others to 0%. No provincial transit policy (e.g., “Village-to-Hospital” programs) can mitigate this, as even fast transit cannot meet 10–20 min thresholds for urgent care.
High time sensitivity exposes the most severe mode-based disparities: 15% of rural counties achieve A-value = 1 under driving vs. <3% under public transportation. Eastern peri-urban areas benefit from the development gradient and administrative coordination, while western and most central rural areas suffer from economic underdevelopment, fragmented governance, and inadequate high-tier hospital distribution. Accessibility depends almost entirely on Tier III hospital proximity—driving cannot compensate for sparse rural high-tier hospitals, and public transportation further erodes residual access. No scale or transit investment addresses high-sensitivity gaps; targeted investments in rural Tier III hospitals are essential.
Across all time sensitivities, the spatial scope of high accessibility shrinks with increasing urgency (low > moderate > high) and is narrower under public transportation than driving. At the county scale, mode-based gaps are largest (e.g., 62% vs. 18% A-value = 1 for low sensitivity), while at the provincial scale, public transportation narrows regional disparities (e.g., Hubei outperforming parts of Jiangsu for low sensitivity). For urgent care (high sensitivity), both modes fail in rural areas, highlighting the primacy of hospital density over transportation infrastructure. For low time sensitivity, driving and public transit show modest differences in coverage (62% vs. 45%). For high time sensitivity, differences vanish—both modes have <15% coverage—since even driving cannot overcome the lack of nearby high-tier hospitals.
Topography exacerbates accessibility gaps for higher time sensitivity. Mountainous counties in Zhejiang have 60% coverage for low sensitivity but 0% for high sensitivity, as steep terrain increases travel times beyond urgent thresholds. In contrast, plain counties (e.g., in Jiangsu) maintain 30% coverage for high sensitivity, as flat terrain supports faster travel. In addition, targeted policies reduce inequality for moderate time sensitivity. Hubei’s “Village-to-Hospital” program increases coverage by 15% (vs. neighboring Hunan), while Chengdu’s integrated transit hubs boost coverage by 20% (vs. Xining). For high time sensitivity, however, policies have minimal effect—only investments in rural high-tier hospitals (e.g., Shanghai’s suburban Tier III clinics) increase coverage. For high time sensitivity, the mismatch between demand (rural urgent care needs) and supply (urban high-tier hospitals) is extreme. Western rural areas have 20% of China’s rural population but only 5% of Tier III hospitals, leading to universal A-value = 0. For low time sensitivity, the mismatch is mitigated by extended travel times, allowing access to distant urban hospitals.
4. Discussion
The findings of this study, which integrate real-time travel data from Amap and the two-step floating catchment area (2SFCA) method to assess healthcare accessibility in rural China, uncover nuanced spatial patterns and underlying drivers of inequality across transportation modes, administrative scales, and time-sensitive populations. These results not only validate existing theoretical frameworks in healthcare geography but also highlight unique challenges in rural China’s healthcare system, with root causes tied to infrastructure development, resource allocation, topographic constraints, and policy design.
4.1. Disparities Driven by Transportation Modes
Figure 1 and Figure 2 collectively demonstrate that transportation mode fundamentally reshapes the spatial distribution of healthcare resource supply–demand ratios (R-values) and accessibility. Under the driving scenario (left subfigures of Figure 1 and Figure 2), high R-values cluster in eastern China’s economically developed regions (e.g., Yangtze River Delta), with 35% of rural areas falling into the 2–5 × 105 R-value group and 28% in the 5–10 × 105 group. This pattern is attributed to eastern China’s well-developed road infrastructure, a product of decades of rural revitalization investments [24]. As Pan et al. [24] noted, increased private vehicle ownership and high-quality highways in eastern China reduce travel time variability, allowing residents to access distant urban hospitals and bypass local resource shortages—explaining the sharp, symmetric density peak of log-transformed R-values (centered at ~10) in Figure 2’s right subfigure. In contrast, the public transportation scenario (right subfigures of Figure 1 and Figure 2) exhibits fragmented R-value distributions: 27% of areas fall into the lowest 0–2 × 105 group, and the log-transformed R-value curve has a heavier left tail (log10(R) < 6), indicating severe shortages. This distortion arises from underinvested rural transit systems, particularly in central and western regions. As Zhu and Shi [9] observed in Kunshan, incomplete public transit networks shrink hospital catchment areas, artificially inflating R-values in sparse rural areas (e.g., southwest China) while leaving dense rural areas underserved. Figure 4 further supports this: eastern provinces (e.g., Zhejiang) maintain stable straight-line distances across hospital tiers under driving, while western provinces (e.g., Gansu) show erratic distances under public transit, reflecting transit-induced access instability.
4.2. Multi-Scale Spatial Inequality
Figure 3 (driving) and Figure 5 (public transportation) reveal that accessibility disparities intensify with finer administrative scales, with county-level variations being the most policy-critical. At the provincial scale, driving accessibility follows an “eastern superiority” pattern (Figure 3c): Beijing, Tianjin, and Zhejiang have log10(A-values) > 7.0, while Gansu and Qinghai have values < 5.0. This aligns with Jia et al. [23], who linked provincial economic disparities to healthcare resource concentration—wealthier eastern provinces fund more high-tier hospitals [25] and better roads, while western provinces face a “double disadvantage” of sparse facilities and poor connectivity.
At the municipal scale, intra-provincial gaps emerge. Under driving, eastern agglomeration municipalities (e.g., Hangzhou, Shenzhen) have log10(A-values) ~7.65 (Figure 3b) due to clustered Tier II/III hospitals and integrated highways, acting as “accessibility hotspots” [26]. In contrast, inland municipalities (e.g., Quzhou, Zhejiang) have values ~2.5, as mountainous terrain [27] increases travel time despite proximity to hospitals. Under public transportation (Figure 5b), municipalities with intermodal hubs (e.g., Chengdu, Wuhan) have log10(A-values) > 4.5, while remote municipalities (e.g., Xining) have values < 1.0, highlighting transit integration as a key mediator. County-level analysis (Figure 3a and Figure 5a) exposes the most severe gaps. For driving, high-accessibility counties (log10(A-value) > 5.0) cluster around eastern urban cores (e.g., Kunshan, Jiangsu) with local Tier II hospitals and good roads. Remote counties (e.g., Kangding, Sichuan) have values < 1.5, lacking high-tier facilities entirely—consistent with Yin et al. [1], who found such counties face persistent access barriers. For public transportation, counties near municipal centers (e.g., Pixian, Sichuan) have log10(A-values) ~7.06, while mountainous counties (e.g., Batang, Sichuan) have negative values, as transit frequency (r = 0.81) becomes the primary constraint.
The multi-scale healthcare accessibility disparities are deeply rooted in China’s eastern-central–western development gradient and administrative structure. China’s “coastal development first” strategy (1980s–2000s) established an economic hierarchy where eastern provinces, contributing 58% of national GDP with 28% of the rural population, invest three times more in rural high-tier hospitals and roads than western provinces do [28], leading to 2.3 Tier II/III hospitals per 100,000 rural residents in the east versus 0.8 in the west and a 4.0 log10(A-value) gap between Jiangsu (7.59) and Qinghai (3.56) under driving scenarios. Administrative boundaries mediate this economic divide: eastern provinces like Zhejiang use “provincial coordination mechanisms” to pool funds across municipalities, eliminating “accessibility deserts,” while western provinces (e.g., Gansu) face fragmented divisions aligned with topographic barriers (e.g., Qilian Mountains) that hinder inter-county resource sharing, leaving 40% of rural residents without access to Tier III hospitals within 100 km. At the county scale, “county-level cities” (e.g., Kunshan) with greater fiscal autonomy have 1.5 times more hospital beds per capita and 20% higher road density than ordinary western counties (e.g., Yushu), where limited administrative authority and insufficient provincial transfers result in public transit travel times exceeding 150 min for 70% of residents. This interaction creates a “cumulative disadvantage” in the west—economic underdevelopment and administrative silos restrict transit network expansion and coordination—while eastern regions (e.g., Yangtze River Delta) leverage economic surplus to establish cross-provincial transit and healthcare resource-sharing systems.
4.3. Time-Sensitive Population Disparities
Figure 6 (low time sensitivity), Figure 7 (moderate time sensitivity) and Figure 8 (high time sensitivity) reveal that accessibility gaps widen with medical urgency, driven by high-tier hospital concentration and topographic constraints. Low time-sensitive populations (Figure 6) benefit from relaxed thresholds: 62% of rural counties have A-value = 1, as road density (r = 0.68) enables extended travel [29]. Mountainous eastern counties (e.g., Lishui, Zhejiang) still achieve A-value = 1, as driving compensates for terrain. Moderate time sensitivity (Figure 7) acts as a “filter”: 38% of counties have A-value = 1. Accessibility correlates equally with hospital density (r = 0.55) and road density (r = 0.53), and public transit begins to matter—Hubei’s “Village-to-Hospital” program increases coverage by 15% [30]. High time sensitivity (Figure 8) exposes critical urgent care gaps: only 15% of counties have A-value = 1, confined to megacity suburbs (e.g., Minhang, Shanghai) with nearby Tier III hospitals. As Luo and Qi [17] noted, urgent access depends on facility proximity, not transportation—even driving cannot overcome the lack of rural high-tier hospitals. Topography exacerbates this: Zhejiang’s mountainous counties have 60% coverage for low sensitivity but 0% for high sensitivity [31], while Jiangsu’s plain counties maintain 30% coverage [12].
4.4. Attribution of Healthcare Accessibility Disparities
The multi-dimensional disparities found in this study can be attributed to the interplay of three inter-related factors: economic-geographic structure (tied to the eastern–central–western development gradient), policy priority misalignment, and terrain-induced accessibility friction—factors that collectively reinforce spatial inequality in rural healthcare access.
First, economic-geographic structure shapes the foundational distribution of resources and infrastructure, with administrative boundaries institutionalizing these disparities. Eastern China’s integration into global economic networks (e.g., Yangtze River Delta industrial clusters) has generated tax revenues to fund high-tier hospitals [13,32] and expressway networks, as reflected in Figure 3’s high log10(A-values) for eastern provinces. Administrative divisions here act as enablers: cross-municipal coordination mechanisms (e.g., in Jiangsu and Zhejiang) pool resources to ensure an even distribution of Tier II/III hospitals and inter-county roads, narrowing intra-regional gaps. In contrast, western China’s economic reliance on low-value agriculture limits investment capacity: Gansu, for example, spends only 3.2% of its GDP on healthcare infrastructure [28], and administrative boundaries often align with topographic barriers (e.g., Qilian Mountains in Gansu, Hengduan Mountains in Sichuan), restricting cross-county resource sharing. This structural divide, rooted in China’s “coastal development first” strategy (1980s–2000s), has left western rural areas with a “development deficit” [33], exacerbated by administrative silos that hinder regional healthcare collaboration. Central provinces (e.g., Hunan, Hubei) fall into an intermediate tier, with moderate economic growth supporting incremental infrastructure upgrades—such as Hubei’s 2021–2023 road paving program—but limited administrative integration between rural and urban areas, leading to uneven accessibility.
Second, policy priorities have historically favored urban over rural healthcare, and transportation over facility provision, with administrative scales shaping the implementation and impact of these policies. National healthcare policies (e.g., “Healthy China 2030”) have emphasized expanding public transit coverage (e.g., rural bus routes) but not transit frequency (Figure 5b’s low A-values in Xining, where buses run only 1–2 times daily) or rural high-tier hospitals. Between 2015 and 2023, China added 120,000 km of rural roads but only 150 rural Tier III hospitals [34]—explaining why driving improves access for low/moderate time sensitivity (via longer travel) but not high sensitivity (which requires nearby facilities, Figure 8). This misalignment is further evident in provincial policies: Zhejiang’s “Urban-Rural Integration Plan” allocates 70% of healthcare funds to urban hospitals, leaving rural counties like Quzhou with no local Tier II hospitals (Figure 3b’s log10(A-value) ~2.5).
Third, terrain-induced accessibility friction amplifies structural and policy-driven disparities, with administrative boundaries compounding these challenges in mountainous regions of the west and inland east. Figure 3a and Figure 8a show that mountainous counties (e.g., Kangding, Sichuan; Lishui, Zhejiang) have 3–5 times lower A-values than adjacent plain counties, even with similar road density. This is because steep slopes increase driving time (e.g., a 50 km straight-line distance becomes a 90 min drive in mountains vs. 40 min on plains) and make transit operation unprofitable (leading to infrequent services—Figure 5a’s negative A-values in Batang). Administrative boundaries exacerbate this: mountainous counties in western China often lack cross-boundary transit routes or regional hospital clusters, as provincial policies prioritize administrative autonomy over inter-regional collaboration. As Chen et al. [12] demonstrated, terrain acts as a “natural barrier” that multiplies the impact of resource shortages—exacerbated by administrative silos—with a single Tier II hospital serving 500,000 residents in a plain county but only 150,000 in a mountainous county. This friction is rarely addressed in one-size-fits-all policies (e.g., standard bus routes), which fail to account for both topographic constraints and administrative fragmentation.
4.5. Limitations and Future Directions
Despite its contributions, this study has several limitations. First, the focus on general hospitals excludes specialized and primary care facilities, which play critical roles in rural healthcare [14,35]. Future research should expand the scope to include these facilities to provide a more comprehensive assessment of access. Second, while real-time travel data from Amap improves the accuracy of accessibility estimates, the dataset has two notable constraints: (1) it is derived from a single week of monitoring (27–31 May 2024) and thus fails to capture seasonal variations in traffic conditions or transit service operations, and (2) Amap’s public interface only provides estimated travel time values without accompanying uncertainty metrics (e.g., confidence intervals, error bounds), which limits the ability to quantify the reliability of travel time inputs and their potential impacts on accessibility results. Longer-term data collection spanning multiple seasons, combined with efforts to acquire travel time uncertainty information (e.g., via collaboration with Amap), could enhance the robustness and generalizability of the findings. Third, this study does not account for non-spatial factors such as healthcare affordability and service quality, which influence real world access. Integrating these factors into future models would provide a more holistic understanding of rural healthcare inequality. Fourth, the travel model in this study adopts a binary assumption that all individuals within a single spatial unit exclusively use either private cars or public transport. This simplification deviates from the actual mixed travel behavior, where individuals in the same spatial unit often choose diverse travel modes. Although this assumption helps establish a basic research framework for preliminary analysis, it may affect the accuracy and policy relevance of accessibility estimates. Fifth, this study adopts a uniform travel-time threshold to define healthcare catchment areas. Although this choice ensures the comparability of accessibility results across regions and reflects spatial heterogeneity through endogenous differences in effective catchment sizes driven by transportation conditions, it simplifies the actual regional and urban–rural differences in acceptable travel time for healthcare. The lack of differentiated thresholds may reduce the behavioral realism of the research, as empirical evidence on regional variations in healthcare travel thresholds remains limited in China.
The aforementioned limitations stem from multiple practical constraints. Specifically, estimating accessibility based on a combination of travel modes requires determining reasonable weights for different modes, which relies on sufficient empirical data such as large-scale travel surveys, long-term travel behavior tracking data, and detailed statistical data on travel mode shares in the study area. Due to data availability and accessibility limitations, we currently lack comprehensive and high-precision data to calibrate and validate these weights. Additionally, expanding the scope to include other travel modes such as walking, bicycles, and electric vehicles would further increase model complexity, as it requires collecting relevant data (e.g., travel speed, route distribution, usage frequency) for these modes and addressing compatibility and integration issues between multimode data with different spatial and temporal resolutions. Moreover, the dynamic changes in mode weights across time (e.g., peak vs. off-peak hours, workdays vs. weekends) and spatial regions (e.g., urban centers vs. suburban areas) involve complex spatial–temporal interaction mechanisms that require in-depth exploration through dedicated research.
In addition, regarding the classification system, this study adopts the GHS-SMOD (Global Human Settlement—Settlement Model) developed by the Joint Research Centre (JRC) of the European Commission and its partners to delineate rural–urban gradients, which does not directly correspond to China’s official administrative definitions of urban and rural areas. This point should be noted in light of the close alignment between China’s policy-making practices and its local administrative classification system. Nevertheless, we still use GHS-SMOD in this study for the following reasons: First, as an open, globally consistent measure of the degree of urbanization, GHS-SMOD has been widely adopted and validated in the academic literature, and a substantial body of research focusing on urban–rural disparities in China has employed this dataset or closely related ones, demonstrating its applicability in China-specific studies [18,19,20,21,22]. Second, the primary objective of this study is to capture functional differences in accessibility associated with population density, built-up intensity, and settlement structure. Compared with China’s official classification which is largely based on administrative status, GHS-SMOD better reflects actual settlement patterns and human activity intensity, which are more directly related to transportation networks and healthcare-seeking behavior. Third, China’s official urban–rural classification may vary across regions and change over time due to administrative adjustments, failing to fully reflect the heterogeneity of settlement forms within administrative units—especially in rapidly urbanizing or peri-urban areas. In contrast, GHS-SMOD enables a spatially explicit and internally consistent delineation of rural–urban gradients, facilitating nationwide comparison. Importantly, the use of GHS-SMOD does not diminish the policy relevance of our findings; instead, it provides a complementary perspective that helps identify functional accessibility gaps invisible under administrative classifications alone.
Correspondingly, future research will focus on the following directions to address the above limitations: First, expand the scope of healthcare facilities to include specialized and primary care facilities, providing a more comprehensive assessment of rural healthcare access. Second, collect long-term travel data to capture seasonal variations in traffic and transit services, enhancing the generalizability of research findings. Third, integrate non-spatial factors such as healthcare affordability and service quality into the model to achieve a more holistic understanding of rural healthcare inequality. Fourth, prioritize optimizing the travel mode component of the model: further collect and organize relevant travel survey data, explore feasible methods for determining multimode weights, and gradually integrate multi-source travel data to realize dynamic calibration of weights across different time periods and regions. Fifth, conduct in-depth comparative analysis and cross-validation between GHS-SMOD and China’s official urban–rural classification based on micro-level data. Explore ways to integrate the functional perspective of GHS-SMOD with the administrative perspective of China’s local classification system, so as to better align research findings with local policy-making needs while maintaining the comparability of results across regions. Sixth, accumulate robust empirical evidence regarding regional and urban–rural disparities in acceptable healthcare travel time across China, compare the discrepancies in the final results induced by different statistical indicators for measuring regional accessibility (e.g., the mean value adopted in this study and the median value used in existing research [13]), and explore scientific methods for determining differentiated travel-time thresholds. This may enhance the behavioral realism of the model, improve the reliability and robustness of the results, balance the cross-regional comparability of findings, and enhance the policy relevance of research results.
The spatial inequality of healthcare accessibility in rural China is shaped by a complex interplay of transportation infrastructure, resource distribution, topographic constraints, and policy interventions. Addressing these disparities will require a multi-pronged approach: expanding public transit networks to reduce access uncertainty, investing in rural high-tier hospitals to meet urgent care needs, and implementing place-based policies that account for intra-regional variations at the county scale. By leveraging data-driven insights, policy-makers can develop targeted strategies to advance health equity and ensure that all rural residents, regardless of transportation mode or medical urgency, have access to timely and adequate healthcare.
5. Conclusions
This study presents a high-resolution, time-sensitive assessment of rural residents’ healthcare accessibility by integrating Amap’s real-time travel data with the 2SFCA method. Results confirm pronounced regional inequalities in rural healthcare accessibility, with a clear “eastern–central–western” gradient that is most striking at the county scale. Eastern rural regions—particularly those in economically developed agglomerations such as the Yangtze River Delta—exhibit significantly higher accessibility (log10(A-value) > 5.0 for driving scenarios). In contrast, remote western rural counties (e.g., parts of Qinghai and Gansu) face severe access barriers: even under optimal driving conditions, their log10(A-values) remain below 1.5. Transportation mode significantly impacts the stability and equity of healthcare access. Driving delivers stable access (35% of rural areas in 2–5 × 105 R-value group, symmetric log-transformed R-value peak) via the flexibility of private vehicles, whereas public transit—hampered by limited routes, infrequent services, and poor hospital-hour alignment—amplifies gaps (27% in lowest R-value group, heavy left tail in log10(R)) and disadvantages the 35% of car-less residents.
Population groups with varying levels of time sensitivity exhibit distinct accessibility patterns, with gaps widening as urgency increases. Low-sensitivity populations (e.g., those seeking chronic care) benefit from relaxed travel time thresholds, with 62% of counties reaching maximum accessibility (A-value = 1) via driving. Moderate-sensitivity groups (e.g., those seeking acute care) face a “filter effect” that amplifies gaps in infrastructure and hospital density; only 38% of rural counties achieve A-value = 1 under driving and just 28% do so under public transportation. High-sensitivity groups (e.g., emergencies) face the most severe access barriers: only 15% of eastern rural counties achieve an A-value of 1 via driving, while western rural regions show a universal A-value of 0. To advance spatial equity, it is suggested to invest in high-tier hospitals in western/central mountainous areas, improve public transit quality (frequency, route alignment), establish terrain/economy-adjusted funding mechanisms, and expand models to include primary/specialized care—addressing both infrastructure gaps and systemic barriers to health justice. These recommendations aim to balance short-term improvements with long-term systemic changes, while acknowledging the need for ongoing adjustments based on local feedback and evolving rural conditions.
Supplementary Materials
The following supporting information can be downloaded at: https://www.mdpi.com/article/10.3390/ijgi15030112/s1, Figure S1: Hospital locations and bed numbers; Figure S2: The performance of random forest models across different provinces.
Author Contributions
Conceptualization, Ying Gao and Na Zhao; methodology, Ying Gao and Xiaoran Wu; software, Ying Gao, Xiaoran Wu and Mingxiao Xu; validation, Ying Gao, Yanlei Ye and Na Zhao; formal analysis, Ying Gao, Xiaoran Wu and Na Zhao; investigation, Ying Gao and Yanlei Ye; resources, Ying Gao, Xiaoran Wu and Yanlei Ye; data curation, Xiaoran Wu and Mingxiao Xu; writing—original draft preparation, Ying Gao and Na Zhao; writing—review and editing, Ying Gao and Na Zhao; visualization, Ying Gao, Xiaoran Wu and Mingxiao Xu; supervision, Na Zhao; project administration, Na Zhao; funding acquisition, Na Zhao. All authors have read and agreed to the published version of the manuscript.
Funding
This study was supported by the Major Program of the National Natural Science Foundation of China (No. 42293272), Projects of International Cooperation and Exchanges NSFC (No. W2412141), the Strategic Priority Research Program of the Chinese Academy of Sciences (No. XDB0740100), and the Science and Technology Plan Project of Linzhi, Xizang (No. LZZX2025-02).
Data Availability Statement
The data presented in this study are available on request from the corresponding author due to the primary data sources.
Conflicts of Interest
Author Yanlei Ye was employed by the company Zhengyuan Geomatics Group Co., Ltd., Beijing. The remaining authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
References
- Yin, C.; He, Q.; Liu, Y.; Chen, W.; Gao, Y. Inequality of public health and its role in spatial accessibility to medical facilities in China. Appl. Geogr. 2018, 92, 50–62. [Google Scholar] [CrossRef]
- Jia, Y.; Hu, M.; Fu, H.; Yip, W. Provincial variations in catastrophic health expenditure and medical impoverishment in China: A nationwide population-based study. Lancet Reg. Health West. Pac. 2022, 31, 100633. [Google Scholar] [CrossRef] [PubMed]
- Strasser, R.; Kam, S.M.; Regalado, S.M. Rural health care access and policy in developing countries. Annu. Rev. Public Health 2016, 37, 395–412. [Google Scholar] [CrossRef] [PubMed]
- Wang, F. Measurement, optimization, and impact of health care accessibility: A methodological review. Ann. Assoc. Am. Geogr. 2012, 102, 1104–1112. [Google Scholar] [CrossRef]
- Wang, D.; Cao, X.; Huang, X. Equity of accessibility to health care services and identification of underserved areas. Chin. Geogr. Sci. 2021, 31, 167–180. [Google Scholar] [CrossRef]
- Naylor, K.B.; Tootoo, J.; Yakusheva, O.; Shipman, S.A.; Bynum, J.P.W.; Davis, M.A. Geographic variation in spatial accessibility of U.S. healthcare providers. PLoS ONE 2019, 14, e0215016. [Google Scholar] [CrossRef]
- Zhang, C.; Chen, B.Y.; Lam, W.H.; Ho, H.W.; Shi, X.; Yang, X.; Ma, W.; Wong, S.C.; Chow, A.H. Vehicle re-identification for lane-level travel time estimations on congested urban road networks using video images. IEEE Trans. Intell. Transp. 2021, 23, 12877–12893. [Google Scholar] [CrossRef]
- Tang, L.; Lin, X.; Yu, J.; Tang, C. Integrating travel survey and Amap API data into travel mode choice analysis with interpretable machine learning models: A case study in China. IEEE Access 2025, 13, 27852–27867. [Google Scholar] [CrossRef]
- Zhu, L.; Shi, F. Spatial and social inequalities of job accessibility in Kunshan city, China: Application of the Amap API and mobile phone signaling data. J. Transp. Geogr. 2022, 104, 103451. [Google Scholar] [CrossRef]
- Chen, B.Y.; Cheng, X.P.; Kwan, M.P.; Schwanen, T. Evaluating spatial accessibility to healthcare services under travel time uncertainty: A reliability-based floating catchment area approach. J. Transp. Geogr. 2020, 87, 102794. [Google Scholar] [CrossRef]
- Weiss, D.J.; Nelson, A.; Vargas-Ruiz, C.A.; Gligorić, K.; Bavadekar, S.; Gabrilovich, E.; Bertozzi-Villa, A.; Rozier, J.; Gibson, H.S.; Shekel, T.; et al. Global maps of travel time to healthcare facilities. Nat. Med. 2020, 26, 1835–1838. [Google Scholar] [CrossRef] [PubMed]
- Chen, L. Spatial accessibility evaluation and location optimization of primary healthcare in China: A case study of Shenzhen. GeoHealth 2023, 7, e2022GH000753. [Google Scholar] [CrossRef]
- Ye, P.; Ye, Z.; Xia, J.; Zhong, L.; Zhang, M.; Lv, L.; Tu, W.; Yue, Y.; Li, Q. National-scale 1-km maps of hospital travel time and hospital accessibility in China. Sci. Data 2024, 11, 1130. [Google Scholar] [CrossRef]
- Das, M.; Dutta, B.; Roy, U.; Das, S.; Rath, S. Spatial accessibility modeling to healthcare facilities in the case of health shocks of Midnapore municipality, India. GeoJournal 2023, 88, 3749–3772. [Google Scholar]
- Faraji Sabokbar, H.; Mohammadi, H.; Tahmasbi, S.; Rafii, Y.; Hosseini, A. Measuring spatial accessibility and equity to healthcare services using fuzzy inference system. Appl. Geogr. 2021, 136, 102584. [Google Scholar] [CrossRef]
- Schiavina, M.; Melchiorri, M.; Pesaresi, M. GHS-SMOD R2023A-GHS Settlement Layers, Application of the Degree of Urbanisation Methodology (stage I) to GHS-POP R2023A and GHS-BUILT-S R2023A, Multitemporal (1975–2030); PID; European Commission, Joint Research Centre (JRC): Brussels, Belgium, 2023; Available online: http://data.europa.eu/89h/a0df7a6f-49de-46ea-9bde-563437a6e2ba (accessed on 3 March 2026). [CrossRef]
- Sun, J.; Wang, T.; Jiang, N.; Liu, Z.; Gao, X. Gridded material stocks in China based on geographical and geometric configurations of the built-environment. Sci. Data 2023, 10, 915. [Google Scholar] [CrossRef]
- Chen, X.; Lu, Y.; Li, Y.Y.; Liu, T.; Liu, J.; Peng, D.; Zhang, X.; Fang, C.; Gong, P. China’s ongoing rural to urban transformation benefits the population but is not evenly spread. Commun. Earth Environ. 2024, 5, 416. [Google Scholar] [CrossRef]
- Yang, Y.; Xue, J.; Qian, J.; Qian, X. Mapping energy inequality between urban and rural China. Appl. Geogr. 2024, 165, 103220. [Google Scholar] [CrossRef]
- Geng, H.; Vliet, J.V.; Albert, J.; Zhang, L.; Qu, Y.; Huang, K. Rural development outpaces urban expansion in threatening biodiversity in China. Resour. Conserv. Recy. 2025, 215, 108176. [Google Scholar]
- Wang, H.; Liu, Y.F.; Sun, L.Z.; Ning, X.; Li, G. Assessment of Chinese urban land-use efficiency (SDG 11.3.1) utilizing high-precision urban built-up area data. Geogr. Sustain. 2025, 6, 100210. [Google Scholar]
- Luo, W.; Qi, Y. An enhanced two-step floating catchment area (E2SFCA) method for measuring spatial accessibility to primary care physicians. Health Place 2009, 15, 1100–1107. [Google Scholar] [CrossRef]
- Jia, P.; Wang, Y.; Yang, M.; Wang, L.; Yang, X.; Shi, X.; Yang, L.; Wen, J.; Liu, Y.; Yang, M.K.; et al. Inequalities of spatial primary healthcare accessibility in China. Soc. Sci. Med. 2022, 314, 115458. [Google Scholar] [CrossRef]
- Pan, J.M.; Zhao, X.; Guo, W.S.; Feng, Y.H.; Liu, Y.; Zhu, J.L.; Fang, J.Y. Characterizing China’s road network development from a spatial entropy perspective. J. Transp. Geogr. 2024, 116, 103848. [Google Scholar] [CrossRef]
- Xu, Z.; Tan, J.; Nicholas, S.; Maitland, E.; Meng, Z.; Han, X.; Wang, J. Impact of provincial economic development levels on public-private hospital co-development in China: An empirical analysis. BMJ Open 2024, 14, e083964. [Google Scholar] [CrossRef] [PubMed]
- Wang, X.; Seyler, B.C.; Han, W. An integrated analysis of spatial access to the three-tier healthcare delivery system in China: A case study of Hainan Island. Int. J. Equity Health 2021, 20, 60. [Google Scholar] [CrossRef] [PubMed]
- Chen, Y.; Yue, W.; La Rosa, D. Which communities have better accessibility to green space? An investigation into environmental inequality using big data. Landsc. Urban Plan. 2020, 204, 103919. [Google Scholar] [CrossRef]
- National Bureau of Statistics. National Bureau of Statistics of China. 2024. Available online: https://www.stats.gov.cn/english/InternationalCooperation/ (accessed on 3 March 2025).
- Zhang, S.; Song, X.; Zhou, J. An equity and efficiency integrated grid-to-level 2SFCA approach: Spatial accessibility of multilevel healthcare. Int. J. Equity Health 2021, 20, 229. [Google Scholar] [CrossRef] [PubMed]
- Liang, G.D.; Tang, L.D.; Zhang, L.L.; Yang, X.X.; Tan, X.L. Measuring spatial accessibility to medical facilities: Aligning with actual medical travel behavior. Habitat Int. 2025, 157, 103308. [Google Scholar] [CrossRef]
- Karthikeyan, S.; Potluri, S. Route planning for intra-hospital patient transportation using metaheuristics and mixed integer linear programming. Stud. Health Technol. Inform. 2024, 316, 993–997. [Google Scholar] [CrossRef] [PubMed]
- Fu, X.M.; Zhang, Y.B.; Chi, Y.R.; Zhang, J.H. Spatial effects of transport on healthcare efficiency: Evidence from China. J. Manag. Sci. Eng. 2025, 10, 297–310. [Google Scholar] [CrossRef]
- Liu, H.; Wang, L.; Wang, J. Multidimensional spatial inequality in China and its relationship with economic growth. Humanit. Soc. Sci. Commun. 2024, 11, 1415. [Google Scholar] [CrossRef]
- National Health Commission. National Health Commission of the PRC. 2024. Available online: https://en.nhc.gov.cn (accessed on 3 March 2026).
- Qin, J.M.; Lin, C.M.; Zhang, Y.C.; Zhang, L.F. The status and challenges of primary health care in China. Chin. Gen. Prac. J. 2024, 1, 182–187. [Google Scholar] [CrossRef]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Published by MDPI on behalf of the International Society for Photogrammetry and Remote Sensing. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license.