Abstract
Recent advancements in biomimetic dentistry have introduced innovative materials designed to better simulate natural dentin. One such material is Ribbond®, long polyethylene fiber. It is particularly effective in absorbing and redistributing masticatory forces in teeth with substantial dentin loss. This review aims to analyze the literature on the biomimetic restorative technique using long polyethylene fiber and assess its benefits and indications relative to traditional cusp coverage restorations. Methods: A search was conducted in the PubMed database until March 2024. The authors selected in vitro studies that studied long polyethylene fiber as a dentin reinforcement. Results: From 247 potentially relevant articles, eighteen studies were included in the review. A detailed analysis of the reviewed literature was summarized into three principal sections involving the use of long polyethylene fiber in restorative dentistry. Conclusions: Long polyethylene fibers improve fracture resistance and promote favorable fracture modes, helping to mitigate the shrinkage forces in composite restorations. However, their clinical significance over traditional cusp coverage is unclear.
1. Introduction
Restorative dentistry has advanced significantly from basic mechanical retention to sophisticated adhesive techniques, driven by innovations in materials and adhesives [1,2]. Biomimetic dentistry represents a notable advancement, focusing on restoring a tooth’s original biomechanical integrity through materials that closely replicate the physical and mechanical properties of natural tissues. This approach ensures that restorative materials mimic the behavior of natural teeth under various conditions, such as thermal expansion and tensile strength, thereby preserving the integrity of dental tissues [3]. Key factors in restoring structurally compromised teeth include matching the elastic modulus and surface hardness of natural tissues to ensure even stress distribution and reduce fracture risk [3,4]. In that context, mimicking the amelodentinal junction is essential for harmonious load transfer and preventing the propagation of enamel cracks into the dentin [4].
The prognosis of restorations is significantly affected by the amount of remaining dental tissue, with structural factors, such as interaxial dentin, pulp chamber roof, marginal ridges, non-undermined cusps, and pericervical dentin thickness, serving as predictors of restoration success [5,6,7]. Greater structural compromise correlates with a higher risk of future catastrophic fractures due to reduced residual enamel and dentin, underscoring the importance of replicating natural interfaces to enhance the durability and effectiveness of dental restorations [8,9].
While fiberglass posts have traditionally been used to reinforce root canal-treated teeth, their effectiveness remains debated, and evidence is mixed [1,10]. Recent advancements in materials and adhesive systems aim to enhance the bonding strength of composite resins to dentin, improving adhesion to compromised dental structures. To address or redistribute tensile loads on composite restorations in teeth with substantial hard tissue loss, the incorporation of reinforcing fibers, especially glass and polyethylene fibers, has been proposed as a promising approach [11,12,13].
A leno-woven ultra-high molecular weight polyethylene (LWUHMW) fiber has been utilized to strengthen structurally compromised teeth. One commercially available example is the non-impregnated polyethylene fiber known as Ribbond. (RB), which undergoes cold gas plasma treatment to improve its chemical bonding with restorative materials. The classical use of these fibers includes periodontal splinting, Maryland direct bridges, endodontic posts and cores, stabilization of avulsed teeth, orthodontic retainers, and maintaining diastema closures [12]. Long polyethylene fibers (RB) are not new to the market; their increased use has been primarily driven by biomimetic restorative dentists.
In vitro studies have demonstrated that incorporating long polyethylene fibers can significantly improve the fracture resistance of heavily restored teeth and endodontically treated by acting as stress-absorbing layers that internally splint the tooth and reinforce the composite in multiple directions, effectively redistributing occlusal forces and preventing crack propagation [14,15]. Some authors denote the effectiveness in reducing adhesive stresses during polymerization and minimizing marginal microleakage, all without compromising the aesthetic results. Additionally, long polyethylene fibers possess a fail-safe mechanism that prevents catastrophic failure, allowing for a repairable tooth structure. However, several potential drawbacks have also been identified in studies, including the presence of porosities, adhesive failures, longer clinical application times, and handling difficulties [16,17,18,19]. Furthermore, there remains a lack of studies evaluating the effectiveness of polyethylene fibers in sclerotic or carious dentin, which, from a clinical standpoint, represents one of the most reasonable indications for their use, given that reinforcement is typically recommended for highly compromised teeth.
Overall, each material should be viewed as an additional tool in the clinician’s arsenal rather than a necessity. Clinicians should prioritize adhesion and strive to simplify procedures without compromising the quality or longevity of treatments.
The purpose of our narrative review is to provide clinicians with a comprehensive overview of the advantages offered by long polyethylene fiber reinforcement, contrasting these benefits with those of conventional protocols and trying to answer the arising question: does the integration of long polyethylene fibers into adhesive protocols used as a dentin reinforcement provide sufficient advantages to warrant its consideration as a new clinical approach?
2. Materials and Methods
The study protocol was registered on 1 October 2024 on the Open Science Framework (OSF) database (https://doi.org/10.17605/OSF.IO/QJ74A) under number CRD42021295212. The guidelines of the PRISMA-ScR 2018 statement were used to guide the reporting of this narrative review. Only in vitro studies were considered for this review.
2.1. Search Strategy
A thorough electronic literature search was performed on PubMed up to March 2024. Additionally, during the review process, the relevant literature was further gathered from the reference sections of the retrieved articles to supplement the information. The search utilized the following MeSH terms as keywords: “composite resin”, “biomimetics”, “fiber-reinforced” and “ribbond”. The final search was conducted using the following combination of keywords: “Composite resin AND Biomimetics AND fiber-reinforced OR ribbond”.
2.2. Eligibility Criteria
Scientific papers eligible for inclusion in the present review were published in English, peer-reviewed, and dated from 2019 to 2024. To present the most up-to-date and comprehensive evidence, this study incorporates the latest findings and recent advancements in the field. The selected articles were required to include the search terms in either the title or abstract. Preference was given to full-text published articles. Systematic reviews, meta-analyses, unpublished works, personal communications, background information, and advertisements were excluded from consideration.
2.3. Selection Process
Two investigators independently searched and screened the results using the agreed inclusion criteria: (a) in vitro laboratory studies; (b) related to long polyethylene fiber material; (c) comparison between properties of long polyethylene fiber and conventional particulate filler composite (PFC) resins; (d) published in a peer-reviewed journal; (e) reported manufacturer information; and (f) published in English.
Whenever it was not possible to make this determination, the full-text article was examined. Subsequently, all relevant articles were obtained, and those not meeting the inclusion criteria were excluded from the review.The selection and screening process was made using Microsoft Excel (16.93 version).
2.4. Data Synthesis
After omitting the duplicates/repetitive articles, a total of 18 full-text articles were studied and concluded for review, for that purpose EndNote 20.4 was used. For each article, the authors’ names, study setup, main results, and conclusion were reported (Table 1). Additionally, main findings, limitations, and controversies were summarized (Table 2).

Table 1.
Details of the included publications.

Table 2.
Summary of main findings, limitations, and controversies.
3. Results
A total of 247 relevant articles were identified and screened by evaluating their titles and abstracts. Following a thorough assessment, 225 articles were excluded due to not meeting the inclusion criteria or being duplicates. Consequently, 22 articles were selected for their relevance to this review. After a full-text screening of text articles, three further studies were excluded due to methodological issues. Finally, 18 articles were included in our review for full-text analysis. Figure 1 shows the screening and selection process in a PRISMA flow diagram.
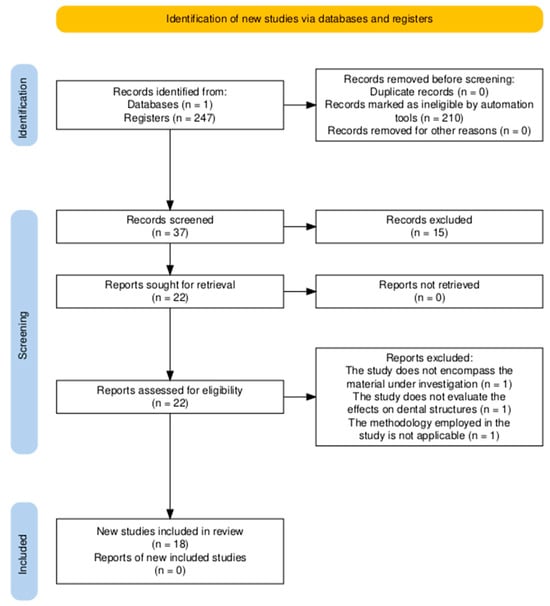
Figure 1.
PRISMA flow diagram of the screening and selection process.
Nine studies evaluated the influence of fiber and/or different restorative modalities of structurally compromised posterior teeth; four articles analyzed the effect of fiber and gap formation and stress distribution; and five studies aborded restoration of anterior teeth with fibers (Figure 2). Seventeen included publications investigated the effect of fiber on extracted teeth, twelve on posterior premolars and molar teeth, five on anterior, and one study analyzed the effect of fiber reinforcement on resin composite molds.

Figure 2.
Summary of key points from each section analyzed in the results.
4. Discussion
This comprehensive review aims to equip clinicians with an in-depth understanding of biomimetic restoration techniques utilizing long polyethylene fibers and to offer a clinical rationale for their application. A detailed analysis of the reviewed literature categorizes the examined characteristics into three principal sections. Each section provides a summary of current evidence on the topic, addresses existing limitations, and outlines potential directions for future research.
4.1. Influence of Fiber Placement on Mechanical Performance in Structurally Compromised Posterior Teeth
The loss of dental structure and the compromise of the remaining structure directly affect tooth strength [35]. Research shows that the involvement of marginal ridges is associated with structural compromise and weakening of the tooth [36]. In this context, most studies assess the design of MOD [5,14,22,26,28,30,32,33] and Class II [21,31] cavities to replicate compromised situations, frequently in combination with endodontic treatment [14,22,28,32]. However, the study by Sfeikos, Dionysopoulos, Kouros, Naka, and Tolidis [2] analyzed the situation in Class I cavities.
Most authors agree that fiber incorporation improves fracture resistance in restorations [5,21,22,26,28,32], cuspid deflection [30], and fatigue resistance [14]. However, some authors argue that its effectiveness may depend on the amount of remaining tooth structure [5].
Some researchers had explored the effectiveness of fibers when cusp coverage is incorporated [14,23], denoting that fiber incorporation and overall resistance benefits from cusp coverage [7], while Fildisi and Eliguzeloglu Dalkilic [23] found no significant changes when fibers were added to overlay or endocrown restorations. Moreover, polyethylene fibers were found to outperform glass fiber posts in terms of enhancing restoration strength and longevity [7].
Furthermore, authors such as Agrawal, Shah, and Kapoor [26] and Fildisi and Eliguzeloglu Dalkilic [23] observed that the incorporation of fibers reduces the frequency of irreparable fractures and favors the preservation of the dental structure. This implies that RB can play a pivotal role in maintaining the structural integrity of restorations.
Some authors also noted that the incorporation of short fibers improves mechanical properties, outperforming long fibers [14,22,33]. Soto-Cadena, Zavala-Alonso, Cerda-Cristerna, and Ortiz-Magdaleno [22] found that combining RB and EverX Posterior significantly enhances fracture resistance compared to using RB alone. This suggests that while RB can contribute to reinforcement, it may not be sufficient as a standalone material, emphasizing the importance of combining materials to achieve optimal results.
Recent studies evaluating the fracture resistance and failure modes of polyethylene fiber-reinforced restorations have not demonstrated significant improvements in the fracture resistance of teeth restored with these fibers. Surprisingly, a notable finding was the increased occurrence of adhesive failures at the tooth–restoration interface. Furthermore, the studies reported a concerning presence of porosities and defects at the fiber–resin interface, which could serve as potential sites for water accumulation and material degradation. These observations highlight critical challenges in the performance and resistance of teeth [17].
4.2. Impact of Fiber Reinforcement on Microleakage and Gap Formation in Dental Restorations
In studies, the predominant fiber placement orientation was horizontal. However, several authors specifically studied fiber orientation and found a correlation between fiber positioning relative to the cavity and the outcomes achieved. Albar and Khayat [33] observed that fibers oriented along the axial and gingival walls exhibited better fracture resistance results. Similarly, Agrawal, Shah, and Kapoor [26] noted that fibers placed horizontally on the gingival and pulpal floors showed improved fracture resistance, outperforming restorations without fibers. This suggests that horizontal fiber orientation is beneficial due to reinforcement when fibers are perpendicular to applied forces.
Conversely, Sfeikos, Dionysopoulos, Kouros, Naka, and Tolidis [2] observed that vertically placed fibers reduced microleakage, although no comparison was made with horizontal placement, and the cavity design was Class I. In contrast, Hasija, Meena, Wadhwa, and Aggarwal [31] found that fiber incorporation did not improve adaptation in compromised caries-affected dentin.
One of the challenges in restorative dentistry is minimizing the stress caused by polymerization shrinkage. Recently, bulk-fill composites, designed to be placed in a single increment of 4 mm thickness, have been introduced as a potential solution to streamline the restorative process and reduce polymerization shrinkage stress.
Several authors have studied the relationship between fiber placement and bulk-fill restorative materials. Sfeikos, Dionysopoulos, Kouros, Naka, and Tolidis [2] found that the addition of fibers reduces marginal microleakage regardless of the bulk-fill material or the application protocol. Similarly, Sadr, Bakhtiari, Hayashi, Luong, Chen, Chyz, Chan, and Tagami [27] demonstrated that the incorporation of fibers significantly reduces gap formation in the deepest areas of the cavity, also acting as a shrinkage stress breaker and protecting the bonded interface in deep dentin. Conversely, Deger, Ozduman, Oglakci, and Eliguzeloglu Dalkilic [30] found that fiber incorporation exhibited greater gap formation. Recently, another interesting study concluded that the placement of fibers on the pulpal floor or axial wall to minimize stress does not offer benefits over classical alternatives with conventional composite resin [33].
4.3. Analysis of Fiber Reinforcement and Fracture Resistance in Anterior Dental Restoration
Studies on fiber reinforcement in anterior dental restorations reveal varying effects on mechanical performance and fracture resistance. Some authors compared fiber reinforcement with fiberglass posts in anterior restorations [25,29]. Sreen, Abraham, Gupta, Singh, Aggarwal, Chauhan, Jala, and Mehta [29] observed that restorations with fiberglass posts required more force to fracture compared to those with RB, which demonstrated less resistance. This is consistent with findings that restorations with fiberglass posts exhibited greater fracture resistance than those with RB, regardless of fracture type [25]. Both studies suggest that traditional fiberglass posts may provide superior mechanical support compared to long polyethylene fibers in enhancing the strength of anterior restorations.
In contrast, other authors found positive results for polyethylene fibers in anterior restorations [20,34]. Jadhav, Mittal, Shinde, Al-Qarni, Al-Obaid, Abullais, Cicciu, and Minervini [34] demonstrated that composites with a single palatal polyethylene fiber achieved higher load resistance and primarily fractured in the remaining tooth structure, indicating reduced stress at the interface and improved bonding. Similar research observed that composites reinforced with polyethylene fibers mostly exhibited cohesive fractures in incisal and mesioincisal restorations, suggesting enhanced fracture resistance [20]. Both studies support the efficacy of polyethylene fibers in improving the mechanical performance and durability of anterior restorations compared to traditional reinforcement methods.
4.4. Potential Barriers to Clinical Adoption of Long Polyethylene Fibers
Another important aspect to consider is the potential barriers to the clinical adoption of polyethylene fibers. Some studies have reported that the complex application techniques and restoration designs involving RB fiber did not result in significant improvements in clinical outcomes but instead introduced notable handling difficulties [16,18]. The most recent randomized clinical trials addressing this issue have concluded that the application of RB-reinforced resin composite restorations can be both expensive and time-consuming, particularly in cases of moderate tooth loss [19].
5. Limitations and Recommendations for Future Research
The main limitation of this review is that it is based solely on in vitro studies and mainly on mechanical performance. In our opinion, these in vitro studies are necessary to provide information to clinicians and industries about the expected clinical behavior of a material, and it is the previous necessary step for a clinical trial of a material. However, we acknowledge the importance and necessity of clinical trials with long-term follow-up to evaluate the potential benefits of polyethylene fiber-reinforced restorations over traditional cusp-coverage restorations. These trials are essential to assess the challenges associated with handling procedures, time management, and the cost-benefit of incorporating polyethylene fibers into routine clinical practice.
6. Conclusions
Within the limitations of this review, long polyethylene fibers appear to enhance overall fracture resistance and promote favorable fracture modes. However, their clinical significance compared to traditional cusp coverage methods remains uncertain. Long polyethylene fibers seem to offer protection to the hybrid layer by mitigating polymerization shrinkage, especially from low-filled resin composites; however, they can incorporate porosities and defects at the fiber–resin interface. Conversely, short fiber-reinforced composites have shown promising results when compared with long polyethylene fibers. The learning curve and reproducibility remain potential drawbacks for clinicians to incorporate long polyethylene fibers, The above findings do not support the systematic integration of long polyethylene fibers into adhesive protocols, highlighting the need for further studies to fully elucidate the potential advantages of polyethylene fiber-reinforced restorations over conventional approaches in direct restorative dentistry and to comprehensively evaluate the cost-benefit of incorporating fibers into clinical practice.
Author Contributions
Conceptualization, Á.F.C. and A.A.M.; methodology, A.A.M., R.A.-P., S.S. and A.L.; writing—original draft preparation Á.F.C., A.A.M. and S.S.; writing—review and editing C.M.C.-P., R.F.C. and R.H. All authors have read and agreed to the published version of the manuscript.
Funding
This research received no external funding.
Institutional Review Board Statement
Not applicable.
Informed Consent Statement
Not applicable.
Data Availability Statement
No new data were created or analyzed in this study. Data sharing is not applicable to this article.
Acknowledgments
We appreciate José Eduardo Maté-Sánchez de Val’s help in reviewing this paper.
Conflicts of Interest
The authors declare no conflicts of interest.
References
- Magne, P.; Lazari, P.C.; Carvalho, M.A.; Johnson, T.; Del Bel Cury, A.A. Ferrule-Effect Dominates Over Use of a Fiber Post When Restoring Endodontically Treated Incisors: An In Vitro Study. Oper. Dent. 2017, 42, 396–406. [Google Scholar] [CrossRef] [PubMed]
- Sfeikos, T.; Dionysopoulos, D.; Kouros, P.; Naka, O.; Tolidis, K. Effect of a fiber-reinforcing technique for direct composite restorations of structurally compromised teeth on marginal microleakage. J. Esthet. Restor. Dent. 2022, 34, 650–660. [Google Scholar] [CrossRef]
- Singer, L.; Fouda, A.; Bourauel, C. Biomimetic approaches and materials in restorative and regenerative dentistry: Review article. BMC Oral Health 2023, 23, 105. [Google Scholar] [CrossRef]
- Zafar, M.S.; Amin, F.; Fareed, M.A.; Ghabbani, H.; Riaz, S.; Khurshid, Z.; Kumar, N. Biomimetic Aspects of Restorative Dentistry Biomaterials. Biomimetics 2020, 5, 34. [Google Scholar] [CrossRef] [PubMed]
- Zotti, F.; Hu, J.; Zangani, A.; Albanese, M.; Paganelli, C. Fracture strength and ribbond fibers: In vitro analysis of mod restorations. J. Clin. Exp. Dent. 2023, 15, e318–e323. [Google Scholar] [CrossRef] [PubMed]
- Deliperi, S.; Alleman, D.; Rudo, D. Stress-reduced Direct Composites for the Restoration of Structurally Compromised Teeth: Fiber Design According to the “Wallpapering” Technique. Oper. Dent. 2017, 42, 233–243. [Google Scholar] [CrossRef] [PubMed]
- Volom, A.; Vincze-Bandi, E.; Sary, T.; Alleman, D.; Forster, A.; Jakab, A.; Braunitzer, G.; Garoushi, S.; Frater, M. Fatigue performance of endodontically treated molars reinforced with different fiber systems. Clin. Oral. Investig. 2023, 27, 3211–3220. [Google Scholar] [CrossRef]
- Abdelfattah, R.A.; Nawar, N.N.; Kataia, E.M.; Saber, S.M. How loss of tooth structure impacts the biomechanical behavior of a single-rooted maxillary premolar: FEA. Odontology 2024, 112, 279–286. [Google Scholar] [CrossRef]
- Al-Nuaimi, N.; Patel, S.; Austin, R.S.; Mannocci, F. A prospective study assessing the effect of coronal tooth structure loss on the outcome of root canal retreatment. Int. Endod. J. 2017, 50, 1143–1157. [Google Scholar] [CrossRef] [PubMed]
- Lazari, P.C.; de Carvalho, M.A.; Del Bel Cury, A.A.; Magne, P. Survival of extensively damaged endodontically treated incisors restored with different types of posts-and-core foundation restoration material. J. Prosthet. Dent. 2018, 119, 769–776. [Google Scholar] [CrossRef] [PubMed]
- Shah, E.H.; Shetty, P.; Aggarwal, S.; Sawant, S.; Shinde, R.; Bhol, R. Effect of fibre-reinforced composite as a post-obturation restorative material on fracture resistance of endodontically treated teeth: A systematic review. Saudi Dent. J. 2021, 33, 363–369. [Google Scholar] [CrossRef] [PubMed]
- Scribante, A.; Vallittu, P.K.; Ozcan, M. Fiber-Reinforced Composites for Dental Applications. Biomed. Res. Int. 2018, 2018, 4734986. [Google Scholar] [CrossRef] [PubMed]
- Gurel, M.A.; Helvacioglu Kivanc, B.; Ekici, A.; Alacam, T. Fracture Resistance of Premolars Restored Either with Short Fiber or Polyethylene Woven Fiber-Reinforced Composite. J. Esthet. Restor. Dent. 2016, 28, 412–418. [Google Scholar] [CrossRef]
- Jakab, A.; Volom, A.; Sary, T.; Vincze-Bandi, E.; Braunitzer, G.; Alleman, D.; Garoushi, S.; Frater, M. Mechanical Performance of Direct Restorative Techniques Utilizing Long Fibers for “Horizontal Splinting” to Reinforce Deep MOD Cavities—An Updated Literature Review. Polymers 2022, 14, 1438. [Google Scholar] [CrossRef] [PubMed]
- Mangoush, E.; Garoushi, S.; Lassila, L.; Vallittu, P.K.; Sailynoja, E. Effect of Fiber Reinforcement Type on the Performance of Large Posterior Restorations: A Review of In Vitro Studies. Polymers 2021, 13, 3682. [Google Scholar] [CrossRef] [PubMed]
- Bijelic-Donova, J.; Bath, A.K.; Rocca, G.T.; Bella, E.D.; Saratti, C.M. Can Fiber-reinforced Composites Increase the Fracture Resistance of Direct Composite Restorations in Structurally Compromised Teeth? A Systematic Review and Meta-analysis of Laboratory Studies. Oper. Dent. 2025, 50, E1–E29. [Google Scholar] [CrossRef] [PubMed]
- Canobra, L.F.; Parra-Gatica, E.; Sanhueza, V.; Medina, C.; Wendler, M. Fracture Resistance and Failure Mode of Polyethylene Fiber-reinforced Resin-based Restorations in Structurally Compromised Premolars: An in Vitro Study. Oper. Dent. 2024, 49, 455–464. [Google Scholar] [CrossRef]
- Sary, T.; Garoushi, S.; Braunitzer, G.; Alleman, D.; Volom, A.; Frater, M. Fracture behaviour of MOD restorations reinforced by various fibre-reinforced techniques—An in vitro study. J. Mech. Behav. Biomed. Mater. 2019, 98, 348–356. [Google Scholar] [CrossRef]
- Metwaly, A.A.; Elzoghby, A.F.; Abd ElAziz, R.H. Clinical performance of polyethylenefiber reinforced resin composite restorations in endodontically treated teeth: (A randomized controlled clinical trial). BMC Oral Health 2024, 24, 1285. [Google Scholar] [CrossRef] [PubMed]
- Patnana, A.K.; Vanga, N.R.V.; Vabbalareddy, R.; Chandrabhatla, S.K. Evaluating the fracture resistance of fiber reinforced composite restorations—An in vitro analysis. Indian J. Dent. Res. 2020, 31, 138–144. [Google Scholar] [CrossRef] [PubMed]
- Albar, N.H.M.; Khayat, W.F. Evaluation of Fracture Strength of Fiber-Reinforced Direct Composite Resin Restorations: An In Vitro Study. Polymers 2022, 14, 4339. [Google Scholar] [CrossRef] [PubMed]
- Soto-Cadena, S.L.; Zavala-Alonso, N.V.; Cerda-Cristerna, B.I.; Ortiz-Magdaleno, M. Effect of short fiber-reinforced composite combined with polyethylene fibers on fracture resistance of endodontically treated premolars. J. Prosthet. Dent. 2023, 129, 598.e1–598.e10. [Google Scholar] [CrossRef] [PubMed]
- Fildisi, M.A.; Eliguzeloglu Dalkilic, E. The effect of fiber insertion on fracture strength and fracture modes in endocrown and overlay restorations. Microsc. Res. Tech. 2022, 85, 1799–1807. [Google Scholar] [CrossRef] [PubMed]
- Kinikoglu, I.; Turkoglu Kayaci, S.; Arslan, H. Short fiber reinforced composite on fracture strength of immature permanent anterior teeth with simulated regenerative endodontic procedures: An in vitro study. J. Clin. Pediatr. Dent. 2023, 47, 171–177. [Google Scholar] [CrossRef] [PubMed]
- Khurana, D.; Prasad, A.B.; Raisingani, D.; Srivastava, H.; Mital, P.; Somani, N. Comparison of Ribbond and Everstick Post in Reinforcing the Re-attached Maxillary Incisors Having Two Oblique Fracture Patterns: An In Vitro Study. Int. J. Clin. Pediatr. Dent. 2021, 14, 689–692. [Google Scholar] [CrossRef]
- Agrawal, V.S.; Shah, A.; Kapoor, S. Effect of fiber orientation and placement on fracture resistance of large class II mesio-occluso-distal cavities in maxillary premolars: An in vitro study. J. Conserv. Dent. 2022, 25, 122–127. [Google Scholar] [CrossRef]
- Sadr, A.; Bakhtiari, B.; Hayashi, J.; Luong, M.N.; Chen, Y.W.; Chyz, G.; Chan, D.; Tagami, J. Effects of fiber reinforcement on adaptation and bond strength of a bulk-fill composite in deep preparations. Dent. Mater. 2020, 36, 527–534. [Google Scholar] [CrossRef]
- Verma, V.; Bansal, A.; Kukreja, N.; Kaur, S.; Varsha, P.; Zanjad, S.R. Evaluation of fracture resistance in class II tooth cavity using different techniques. Bioinformation 2022, 18, 858–861. [Google Scholar] [CrossRef]
- Sreen, D.; Abraham, D.; Gupta, A.; Singh, A.; Aggarwal, V.; Chauhan, N.; Jala, S.; Mehta, N. Comparative evaluation of the force required to fracture coronal segments reattached using different methods. Dent. Traumatol. 2022, 38, 143–148. [Google Scholar] [CrossRef]
- Deger, C.; Ozduman, Z.C.; Oglakci, B.; Eliguzeloglu Dalkilic, E. The Effect of Different Intermediary Layer Materials Under Resin Composite Restorations on Volumetric Cuspal Deflection, Gap Formation, and Fracture Strength. Oper. Dent. 2023, 48, 108–116. [Google Scholar] [CrossRef]
- Hasija, M.K.; Meena, B.; Wadhwa, D.; Aggarwal, V. Effect of adding ribbond fibres on marginal adaptation in class II composite restorations in teeth with affected dentine. J. Oral. Biol. Craniofacial Res. 2020, 10, 203–205. [Google Scholar] [CrossRef] [PubMed]
- Balkaya, H.; Topcuoglu, H.S.; Demirbuga, S.; Kafdag, O.; Topcuoglu, G. Effect of different coronal restorations on the fracture resistance of teeth with simulated regenerative endodontic treatment: An in vitro study. Aust. Endod. J. 2022, 48, 331–337. [Google Scholar] [CrossRef] [PubMed]
- Albar, N.; Khayat, W. Fracture Load of Mesio-Occluso-Distal Composite Restorations Performed with Different Reinforcement Techniques: An In Vitro Study. Polymers 2023, 15, 1358. [Google Scholar] [CrossRef] [PubMed]
- Jadhav, G.R.; Mittal, P.; Shinde, S.; Al-Qarni, M.A.; Al-Obaid, M.; Abullais, S.S.; Cicciu, M.; Minervini, G. Biomimetic approach to strengthen the incisal fracture composite build-up: An in vitro study. BMC Oral Health 2024, 24, 42. [Google Scholar] [CrossRef] [PubMed]
- Ibrahim, A.M.; Richards, L.C.; Berekally, T.L. Effect of remaining tooth structure on the fracture resistance of endodontically-treated maxillary premolars: An in vitro study. J. Prosthet. Dent. 2016, 115, 290–295. [Google Scholar] [CrossRef]
- Shahrbaf, S.; Mirzakouchaki, B.; Oskoui, S.S.; Kahnamoui, M.A. The effect of marginal ridge thickness on the fracture resistance of endodontically-treated, composite restored maxillary premolars. Oper. Dent. 2007, 32, 285–290. [Google Scholar] [CrossRef] [PubMed]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).