Atrial Septal Defects: From Embryology to Pediatric Pulmonary Hypertension
Abstract
1. Introduction
2. Embryology and Genetic Predispositions to ASD
2.1. ASD Development
2.2. Genetic Predispositions to ASD
3. Pathophysiology and Classification of ASD
3.1. Types of ASD
3.2. Left-to-Right Shunt Dynamics
3.3. Hemodynamic Consequences
4. ASD and Pulmonary Hypertension
4.1. Definition
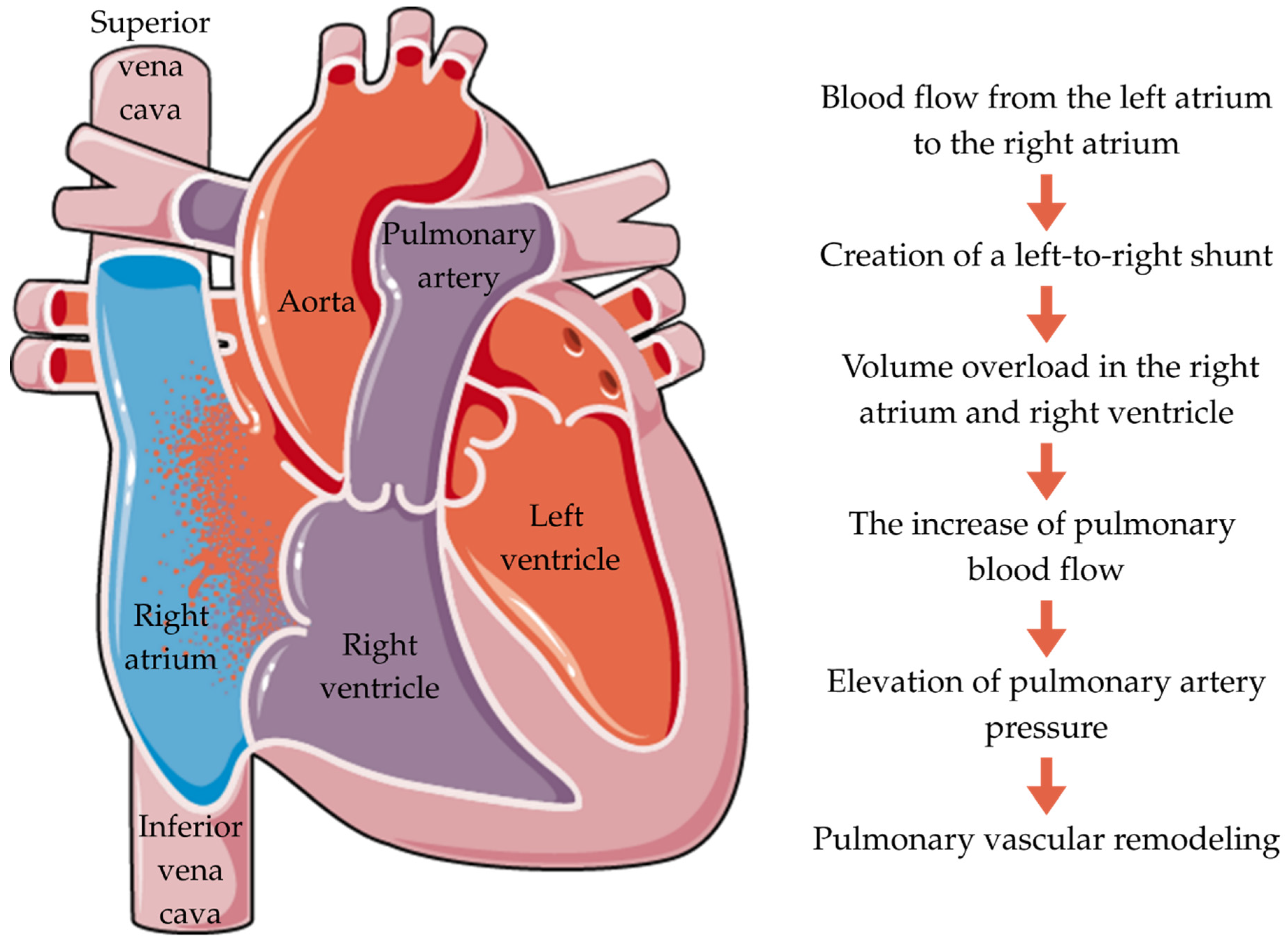
4.2. Mechanism of Disease Progression
4.3. Comparative Risk of PAH in Ostium Primum and Secundum ASDs
4.4. Eisenmenger Syndrome
5. Clinical Presentation and Diagnosis
5.1. Symptoms
5.2. Diagnostic Tests
5.3. Clinical Presentation
6. Managing Atrial Septal Defect and Pulmonary Hypertension in Children
6.1. Watchful Waiting for Minor ASDs
6.2. When and How to Close ASDs
- Very large size (diameter greater than 36–40 mm);
- Inadequate margins for device anchorage;
- Potential device interference with atrioventricular valve function;
6.3. Treating ASD and PAH
6.4. Outlook and Long-Term Care
7. Discussion
Author Contributions
Funding
Conflicts of Interest
References
- Kashyap, T.; Sanusi, M.; Momin, E.S.; Khan, A.A.; Mannan, V.; Pervaiz, M.A.; Akram, A.; Elshaikh, A.O. Transcatheter Occluder Devices for the Closure of Atrial Septal Defect in Children: How Safe and Effective Are They? A Systematic Review. Cureus 2022, 14, e25402. [Google Scholar] [CrossRef]
- Isolated Atrial Septal Defects (ASDs) in Children: Classification, Clinical Features, and Diagnosis—UpToDate. Available online: https://www.uptodate.com/contents/isolated-atrial-septal-defects-asds-in-children-classification-clinical-features-and-diagnosis. (accessed on 30 July 2025).
- Therrien, J.; Webb, G. Clinical update on adults with congenital heart disease. Lancet 2003, 362, 1305–1313. [Google Scholar] [CrossRef] [PubMed]
- Sjöberg, P.; Clausen, H.; Arheden, H.; Liuba, P.; Hedström, E. Atrial septal defect closure in children at young age is beneficial for left ventricular function. Eur. Heart J. Imaging Methods Pract. 2024, 2, qyae058. [Google Scholar] [CrossRef] [PubMed]
- Menillo, A.M.; Alahmadi, M.H.; Pearson-Shaver, A.L. Atrial Septal Defect. In Nadas’ Pediatric Cardiology; Elsevier: Amsterdam, The Netherlands, 2025; pp. 285–295. [Google Scholar] [CrossRef]
- Torres, A.J. Hemodynamic assessment of atrial septal defects. J. Thorac. Dis. 2018, 10, S2882–S2889. [Google Scholar] [CrossRef] [PubMed]
- Grygier, M.; Sabiniewicz, R.; Smolka, G.; Demkow, M.; Araszkiewicz, A.; Sorysz, D.; Kusa, J.; Huczek, Z.; Komar, M.; Przewłocki, T.; et al. Percutaneous closure of atrial septal defect A consensus document of the joint group of experts from the Association of Cardiovascular Interventions and the Grown-Up Congenital Heart Disease Section of the Polish Cardiac Society. Kardiol. Pol. 2020, 78, 1066–1083. [Google Scholar] [CrossRef]
- Sabri, M.R.; Mahdavi, C.; Bigdelian, H.; Ahmadi, A.R.; Ghaderian, M.; Dehghan, B. A case series of pulmonary hypertension in small infants with atrial septal defect. ARYA Atheroscler. 2020, 16, 208–210. [Google Scholar] [CrossRef]
- Eisenmenger Syndrome: Background, Pathophysiology, Etiology. Available online: https://emedicine.medscape.com/article/154555-overview (accessed on 31 July 2025).
- Brida, M.; Chessa, M.; Celermajer, D.; Li, W.; Geva, T.; Khairy, P.; Griselli, M.; Baumgartner, H.; A Gatzoulis, M. Atrial septal defect in adulthood: A new paradigm for congenital heart disease. Eur. Heart J. 2022, 43, 2660–2671. [Google Scholar] [CrossRef]
- Jain, S.; Dalvi, B. Atrial septal defect with pulmonary hypertension: When/how can we consider closure? J. Thorac. Dis. 2018, 10, S2890. [Google Scholar] [CrossRef]
- Takaya, Y.; Akagi, T.; Sakamoto, I.; Kanazawa, H.; Nakazawa, G.; Murakami, T.; Yao, A.; Nanasato, M.; Saji, M.; Hirokami, M.; et al. Efficacy of treat-and-repair strategy for atrial septal defect with pulmonary arterial hypertension. Heart 2022, 108, 382–387. [Google Scholar] [CrossRef]
- Kozlik-Feldmann, R.; Hansmann, G.; Bonnet, D.; Schranz, D.; Apitz, C.; Michel-Behnke, I. Pulmonary hypertension in children with congenital heart disease (PAH-CHD, PPHVD-CHD). Expert consensus statement on the diagnosis and treatment of paediatric pulmonary hypertension. The European Paediatric Pulmonary Vascular Disease Network, endorsed by ISHLT and DGPK. Heart 2016, 102, II42–II48. [Google Scholar] [CrossRef]
- Wittenberg, R.E.; Gauvreau, K.; Desocio, M.B.; Du, X.; Jayasankar, J.P.; Sandoval, N.; Jenkins, K.J. Associations with Adverse Postoperative Outcomes in Children Undergoing Atrial Septal Defect Closure in Lower-Resource Settings. JACC Adv. 2024, 3, 101332. [Google Scholar] [CrossRef]
- Kim, N.K.; Park, S.J.; Choi, J.Y. Transcatheter Closure of Atrial Septal Defect: Does Age Matter? Korean Circ. J. 2011, 41, 633. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Le Gloan, L.; Legendre, A.; Iserin, L.; Ladouceur, M. Pathophysiology and natural history of atrial septal defect. J. Thorac. Dis. 2018, 10, S2854–S2863. [Google Scholar] [CrossRef]
- Eisenmenger Syndrome—StatPearls—NCBI Bookshelf. Available online: https://www.ncbi.nlm.nih.gov/books/NBK507800/ (accessed on 28 July 2025).
- Arvanitaki, A.; Giannakoulas, G.; Baumgartner, H.; Lammers, A.E. Eisenmenger syndrome: Diagnosis, prognosis and clinical management. Heart 2020, 106, 1638–1645. [Google Scholar] [CrossRef]
- Ostium Primum Atrial Septal Defect—GPnotebook. Available online: https://gpnotebook.com/pages/cardiovascular-medicine/ostium-primum-atrial-septal-defect (accessed on 31 July 2025).
- Faletra, F.F.; Saric, M.; Saw, J.; Lempereur, M.; Hanke, T.; Vannan, M.A. Imaging for Patient’s Selection and Guidance of LAA and ASD Percutaneous and Surgical Closure. JACC Cardiovasc. Imaging 2021, 14, 3–21. [Google Scholar] [CrossRef] [PubMed]
- Principles of Developmental Genetics|ScienceDirect. Available online: https://www.sciencedirect.com/book/9780124059450/principles-of-developmental-genetics (accessed on 31 July 2025).
- Marty, M.; Lui, F. Embryology, Fetal Circulation; StatPearls: Treasure Island, FL, USA, 2023. [Google Scholar]
- White, H.J.; Helwany, M.; Biknevicius, A.R.; Peterson, D.C. Anatomy, Head and Neck, Ear Organ of Corti; StatPearls: Treasure Island, FL, USA, 2023. [Google Scholar]
- Klimek-Piotrowska, W.; Hołda, M.K.; Koziej, M.; Piątek, K.; Hołda, J. Anatomy of the true interatrial septum for transseptal access to the left atrium. Ann. Anat. 2016, 205, 60–64. [Google Scholar] [CrossRef]
- Lammers, A.E.; Stegger, J.; Koerten, M.A.; Helm, P.C.; Bauer, U.M.; Baumgartner, H.; Uebing, A.S. Secundum Type Atrial Septal Defect in Patients with Trisomy 21—Therapeutic Strategies, Outcome, and Survival: A Nationwide Study of the German National Registry for Congenital Heart Defects. J. Clin. Med. 2021, 10, 3807. [Google Scholar] [CrossRef] [PubMed]
- Atrial Septal Defects and Patent Foramen Ovale: Current Data Update—Cardiac Interventions Today. Available online: https://citoday.com/articles/2022-jan-feb/atrial-septal-defects-and-patent-foramen-ovale-current-data-update (accessed on 17 August 2025).
- McMahon, C.J.; Feltes, T.F.; Fraley, J.K.; Bricker, J.T.; Grifka, R.G.; A Tortoriello, T.; Blake, R.; I Bezold, L. Natural history of growth of secundum atrial septal defects and implications for transcatheter closure. Heart 2002, 87, 256–259. [Google Scholar] [CrossRef]
- Atrial Septal Defect (ASD)—Pediatrics—Merck Manual Professional Edition. Available online: https://www.merckmanuals.com/professional/pediatrics/congenital-cardiovascular-anomalies/atrial-septal-defect-asd (accessed on 31 July 2025).
- Aoki, H.; Horie, M. Electrical disorders in atrial septal defect: Genetics and heritability. J. Thorac. Dis. 2018, 10, S2848–S2853. [Google Scholar] [CrossRef]
- Hoffman, J.I.E.; Kaplan, S. The incidence of congenital heart disease. J. Am. Coll. Cardiol. 2002, 39, 1890–1900. [Google Scholar] [CrossRef]
- Cervantes-Salazar, J.L.; Pérez-Hernández, N.; Calderón-Colmenero, J.; Rodríguez-Pérez, J.M.; González-Pacheco, M.G.; Villamil-Castañeda, C.; Rosas-Tlaque, A.A.; Ortega-Zhindón, D.B. Genetic Insights into Congenital Cardiac Septal Defects—A Narrative Review. Biology 2024, 13, 911. [Google Scholar] [CrossRef]
- Loser, H.; Majewski, F. Type and frequency of cardiac defects in embryofetal alcohol syndrome report of 16 cases. Heart 1977, 39, 1374–1379. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Kheiwa, A.; Hari, P.; Madabhushi, P.; Varadarajan, P. Patent foramen ovale and atrial septal defect. Echocardiography 2020, 37, 2172–2184. [Google Scholar] [CrossRef]
- Nashat, H.; Montanaro, C.; Li, W.; Kempny, A.; Wort, S.J.; Dimopoulos, K.; Gatzoulis, M.A.; Babu-Narayan, S.V. Atrial septal defects and pulmonary arterial hypertension. J. Thorac. Dis. 2018, 10, S2953–S2965. [Google Scholar] [CrossRef]
- Bradley, E.A.; Zaidi, A.N. Atrial Septal Defect. Cardiol. Clin. 2020, 38, 317–324. [Google Scholar] [CrossRef]
- Alkashkari, W.; Albugami, S.; Hijazi, Z.M. Current practice in atrial septal defect occlusion in children and adults. Expert. Rev. Cardiovasc. Ther. 2020, 18, 315–329. [Google Scholar] [CrossRef] [PubMed]
- Humbert, M.; Kovacs, G.; Hoeper, M.M.; Badagliacca, R.; Berger, R.M.; Brida, M.; Carlsen, J.; Coats, A.J.; Escribano-Subias, P.; Ferrari, P.; et al. 2022 ESC/ERS Guidelines for the diagnosis and treatment of pulmonary hypertension. Eur. Respir. J. 2023, 61, 2200879. [Google Scholar] [CrossRef] [PubMed]
- Sławek-Szmyt, S.L.; Araszkiewicz, A.; Grygier, M. Komu i dlaczego zamykać ubytek przegrody międzyprzedsionkowej z użyciem fenestrowanego okludera? Kardiol. Inwazyjna 2020, 15, 33–37. [Google Scholar]
- Liu, X.; Gao, Y.; Wang, Z.; Shi, R.; Qian, W.L.; Shen, M.T.; Sun, Y.-S.; Yang, Z.-G. Effect of concomitant atrial septal defect on left ventricular function in adult patients with unrepaired Ebstein’s anomaly: A cardiovascular magnetic resonance imaging study. J. Cardiovasc. Magn. Reson. 2023, 25, 75. [Google Scholar] [CrossRef]
- Ostium Primum Atrial Septal Defects: Background, Pathophysiology, Etiology. Available online: https://emedicine.medscape.com/article/890880-overview?utm_source=chatgpt.com&form=fpf (accessed on 16 August 2025).
- Çelik, M.; Yılmaz, Y.; Küp, A.; Kahyaoğlu, M.; Karagöz, A.; Özdemir, N.; Kaymaz, C.; Kırali, M.K. Predictors of pulmonary hypertension after atrial septal defect closure: Impact of atrial fibrillation. Turk. J. Thorac. Cardiovasc. Surg. 2022, 30, 344–353. [Google Scholar] [CrossRef]
- Campbell, A.; Kanodia, A.K.; Gingles, C.R.; Chandrashekar, H. Antiphospholipid syndrome leading to paradoxical embolus and stroke via secundum atrial septal defect. BMJ Case Rep. 2021, 14, e239674. [Google Scholar] [CrossRef]
- Opotowsky, A.R.; Cedars, A.; Kutty, S. Atrial septal defects and pulmonary hemodynamics: A time for holey reflection. Am. J. Physiol. Heart Circ. Physiol. 2020, 318, H1159–H1161. [Google Scholar] [CrossRef]
- Maier, O.; Hellhammer, K.; Horn, P.; Afzal, S.; Jung, C.; Westenfeld, R.; Zeus, T.; Kelm, M.; Veulemans, V. Iatrogenic atrial septal defect persistence after percutaneous mitral valve repair: A meta-analysis. Acta Cardiol. 2022, 77, 166–175. [Google Scholar] [CrossRef]
- Wang, F.; Wang, W.; Wu, Q.; Cao, Y.; Huang, H.; Tao, E.; Fang, Q.; Tang, L.; Wan, L. Summary of the Experiences and Results of Transesophageal Ultrasound-Guided Ventricular Septal Defect and Atrial Septal Defect Closure Operation. Heart Surg. Forum 2022, 25, E638–E644. [Google Scholar] [CrossRef]
- Kovacs, G.; Bartolome, S.; Denton, C.P.; Gatzoulis, M.A.; Gu, S.; Khanna, D.; Badesch, D.; Montani, D. Definition, classification and diagnosis of pulmonary hypertension. Eur. Respir. J. 2024, 64, 2401324. [Google Scholar] [CrossRef] [PubMed]
- Mukherjee, D.; Konduri, G.G. Pediatric Pulmonary Hypertension: Definitions, Mechanisms, Diagnosis, and Treatment. Compr. Physiol. 2021, 11, 2135–2190. [Google Scholar] [CrossRef] [PubMed]
- D’Alto, M.; Mahadevan, V.S. Pulmonary arterial hypertension associated with congenital heart disease. Eur. Respir. Rev. 2012, 21, 328–337. [Google Scholar] [CrossRef] [PubMed]
- Briosa, A.; Ferreira, F.; Santos, J.; Alegria, S.; Loureiro, M.J.; Repolho, D.; Pereira, H. Severe and Apparently Irreversible Pulmonary Arterial Hypertension in a Patient with Ostium Secundum Atrial Septal Defect—A Successful Case of Treat and Close Strategy. Clin. Med. Insights Circ. Respir. Pulm. Med. 2022, 16, 11795484221141298. [Google Scholar] [CrossRef]
- Martin, S.S.; Shapiro, E.P.; Mukherjee, M. Atrial septal defects—Clinical manifestations, echo assessment, and intervention. Clin. Med. Insights Cardiol. 2015, 8, 93–98. [Google Scholar] [CrossRef]
- Zhu, X.; Li, W.; Gao, J.; Shen, J.; Xu, Y.; Zhang, C.; Qian, C. RUNX3 improves CAR-T cell phenotype and reduces cytokine release while maintaining CAR-T function. Med. Oncol. 2023, 40, 89. [Google Scholar] [CrossRef]
- Faultersack, J.; Johnstad, C.M.; Zhang, X.; Greco, M.; Hokanson, J.S. Follow-Up of Secundum ASD, Muscular VSD, or PDA Diagnosed During Neonatal Hospitalization. Pediatr. Cardiol. 2025, 46, 1211–1217. [Google Scholar] [CrossRef]
- Diller, G.P.; Körten, M.A.; Bauer, U.M.M.; Miera, O.; Tutarel, O.; Kaemmerer, H.; Berger, F.; Baumgartner, H. Current therapy and outcome of Eisenmenger syndrome: Data of the German National Register for congenital heart defects. Eur. Heart J. 2016, 37, 1449–1455. [Google Scholar] [CrossRef] [PubMed]
- Arvanitaki, A.; Gatzoulis, M.A.; Opotowsky, A.R.; Khairy, P.; Dimopoulos, K.; Diller, G.-P.; Giannakoulas, G.; Brida, M.; Griselli, M.; Grünig, E.; et al. Eisenmenger Syndrome: JACC State-of-the-Art Review. J. Am. Coll. Cardiol. 2022, 79, 1183–1198. [Google Scholar] [CrossRef]
- Muroke, V.; Jalanko, M.; Haukka, J.; Sinisalo, J. Cause-Specific Mortality of Patients with Atrial Septal Defect and Up to 50 Years of Follow-Up. J. Am. Heart Assoc. 2023, 12, 2. [Google Scholar] [CrossRef] [PubMed]
- Latson, L.; Briston, D. Atrial Septal Defect: Transcatheter Closure Is Not Bad, But There Is More to the Story. JACC Cardiovasc. Interv. 2021, 14, 576–577. [Google Scholar] [CrossRef] [PubMed]
- Hardman, G.; Zacharias, J. Minimal-Access Atrial Septal Defect (ASD) Closure. J. Cardiovasc. Dev. Dis. 2023, 10, 206. [Google Scholar] [CrossRef]
- Syamasundar, R.P. Role of Echocardiography in the Diagnosis and Interventional Management of Atrial Septal Defects. Diagnostics 2022, 12, 1494. [Google Scholar] [CrossRef]
- Hong, W.; Sheng, Q.; Dong, B.; Wu, L.; Chen, L.; Zhao, L.; Liu, Y.; Zhu, J.; Liu, Y.; Xie, Y.; et al. Automatic Detection of Secundum Atrial Septal Defect in Children Based on Color Doppler Echocardiographic Images Using Convolutional Neural Networks. Front. Cardiovasc. Med. 2022, 9, 834285. [Google Scholar] [CrossRef]
- Satoh, A.; Katayama, K.; Hiro, T.; Yano, M.; Miura, T.; Kohno, M.; Fujii, T.; Matsuzaki, M. Effect of right ventricular volume overload on left ventricular diastolic function in patients with atrial septal defect. Jpn. Circ. J. 1996, 60, 758–766. [Google Scholar] [CrossRef][Green Version]
- Tanghöj, G.; Liuba, P.; Sjöberg, G.; Naumburg, E. Predictors of the Need for an Atrial Septal Defect Closure at Very Young Age. Front. Cardiovasc. Med. 2020, 6, 185. [Google Scholar] [CrossRef]
- Callegari, A.; Quandt, D.; Nordmeyer, J.; Schubert, S.; Kramer, P.; Knirsch, W.; Kretschmar, O. Transcatheter Closure of Atrial Septal Defect with Carag Bioresorbable Septal OccluderTM: First-in-Child Experience with 12-MonthFollow-Up. Genet. Res. 2022, 2022, 3476398. [Google Scholar] [CrossRef]
- Chinawa, J.M.; Chinawa, A.T.; Ossai, E.N.; Duru, C.O. Predictors of pulmonary hypertension among children with atrial septal defects (ASD). Libyan J. Med. 2022, 17, 2007603. [Google Scholar] [CrossRef]
- Raja, S.G.; Lammers, A.; Hess, J. Atrial septal defect in infancy: To close or not to close? J. Thorac. Cardiovasc. Surg. 2005, 130, 1483. [Google Scholar] [CrossRef][Green Version]
- Atrial Septal Defect (ASD)—Pediatrics—MSD Manual Professional Edition. Available online: https://www.msdmanuals.com/professional/pediatrics/congenital-cardiovascular-anomalies/atrial-septal-defect-asd (accessed on 17 August 2025).
- Behjati-Ardakani, M.; Golshan, M.; Akhavan-Karbasi, S.; Hosseini, S.M.; Behjati-Ardakani, M.A.; Sarebanhassanabadi, M. The clinical course of patients with atrial septal defects. Iran J. Pediatr. 2016, 26, e4649. [Google Scholar] [CrossRef]
- Liava’a, M.; Kalfa, D. Surgical closure of atrial septal defects. J. Thorac. Dis. 2018, 10, S2931–S2939. [Google Scholar] [CrossRef] [PubMed]
- Rao, P.S.; Harris, A.D. Recent advances in managing septal defects: Atrial septal defects. F1000Research 2017, 6, 2042. [Google Scholar] [CrossRef]
- Meier, B. Percutaneous atrial septal defect closure: Pushing the envelope but pushing it gently. Editorial comment. Catheter. Cardiovasc. Interv. 2005, 66, 397–399. [Google Scholar] [CrossRef] [PubMed]
- Marie Valente, A.; Rhodes, J.F. Current indications and contraindications for transcatheter atrial septal defect and patent foramen ovale device closure. Am. Heart J. 2007, 153, 81–84. [Google Scholar] [CrossRef] [PubMed]
- Manning, P.B. Repair of primum ASD with cleft mitral valve. Oper. Tech. Thorac. Cardiovasc. Surg. 2004, 9, 240–246. [Google Scholar] [CrossRef][Green Version]
- Tadros, V.X.; Asgar, A.W. Atrial septal defect closure with left ventricular dysfunction. EuroIntervention 2016, 12 (Suppl. X), X13–X17. [Google Scholar] [CrossRef]
- Alexandre, A.; Luz, A.; de Frias, A.D.; Santos, R.B.; Brochado, B.; Oliveira, F.; Silveira, J.; Torres, S. Temporary atrial septal defect balloon occlusion test as a must in the elderly. BMC Cardiovasc. Disord. 2023, 23, 15. [Google Scholar] [CrossRef]
- Omar Shebani, S.; Skinner, G.J.; Duke, C. ASD closure under pressure. BMJ Case. Rep. 2014, 2014, bcr2014205493. [Google Scholar] [CrossRef]
- Akagi, T. Current concept of transcatheter closure of atrial septal defect in adults. J. Cardiol. 2015, 65, 17–25. [Google Scholar] [CrossRef] [PubMed]
- Faccini, A.; Butera, G. Atrial septal defect (ASD) device trans-catheter closure: Limitations. J. Thorac. Dis. 2018, 10, S2923–S2930. [Google Scholar] [CrossRef] [PubMed]
- Hofmann, M.; Dave, H.H.; Schmiady, M.O.; Hübler, M. Warden procedure for correction of sinus venosus atrial septal defect and partial anomalous pulmonary venous connection. Multimed. Man. Cardiothorac. Surg. 2016, 2016. [Google Scholar] [CrossRef]
- Stewart, R.D.; Bailliard, F.; Kelle, A.M.; Backer, C.L.; Young, L.; Mavroudis, C. Evolving Surgical Strategy for Sinus Venosus Atrial Septal Defect: Effect on Sinus Node Function and Late Venous Obstruction. Ann. Thorac. Surg. 2007, 84, 1651–1655. [Google Scholar] [CrossRef]
- Warden, H.E.; Gustafson, R.A.; Tarnay, T.J.; Neal, W.A. An Alternative Method for Repair of Partial Anomalous Pulmonary Venous Connection to the Superior Vena Cava. Ann. Thorac. Surg. 1984, 38, 601–605. [Google Scholar] [CrossRef] [PubMed]
- Prochownik, P.; Przewłocki, T.; Podolec, P.; Wilkołek, P.; Sobień, B.; Gancarczyk, U.; Podolec, N.; Komar, M. Improvement of physical capacity in patients undergoing transcatheter closure of atrial septal defects. Postepy Kardiol. Interwencyjnej 2018, 14, 90–94. [Google Scholar] [CrossRef]
- Ivy, D.D.; Frank, B.S. Treat and Repair for Congenital Heart Disease and Pulmonary Hypertension: Not a Panacea. JACC Adv. 2024, 3, 100891. [Google Scholar] [CrossRef]
- Ferrero, P.; Constantine, A.; Chessa, M.; Dimopoulos, K. Pulmonary arterial hypertension related to congenital heart disease with a left-to-right shunt: Phenotypic spectrum and approach to management. Front. Cardiovasc. Med. 2024, 11, 1360555. [Google Scholar] [CrossRef]
- Wang, X.; Wang, S.; Lu, Z.; Wang, W.; Wang, X. Therapeutic effects of treat and repair strategy in pediatric patients with pulmonary arterial hypertension and simple congenital heart defects. Pulm. Circ. 2024, 14, e12387. [Google Scholar] [CrossRef]
- McDonagh, T.A.; Metra, M.; Adamo, M.; Gardner, R.S.; Baumbach, A.; Böhm, M.; Burri, H.; Butler, J.; Čelutkienė, J.; Chioncel, O.; et al. 2021 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure. Eur. Heart J. 2021, 42, 3599–3726. [Google Scholar] [CrossRef]
- Tsuda, T.; Davies, R.R.; Radtke, W.; Pizarro, C.; Bhat, A.M. Early Surgical Closure of Atrial Septal Defect Improves Clinical Status of Symptomatic Young Children with Underlying Pulmonary Abnormalities. Pediatr. Cardiol. 2020, 41, 1115–1124. [Google Scholar] [CrossRef]
- Wiegand, J.L.; Thompson, J.A.; Landeck, B.F.; Fierstein, J.L.; Ashour, D.; Machry, J.S.; Kiskaddon, A.L.; Betensky, M.; Freire, G.A. Pulmonary Hypertension Outcomes After Closure of Atrial Septal Defect in Infants with Developmental Lung Disease. Pulm. Circ. 2025, 15, e70164. [Google Scholar] [CrossRef]
- Lammers, A.E.; Bauer, L.J.; Diller, G.P.; Helm, P.C.; Abdul-Khaliq, H.; Bauer, U.M.; Baumgartner, H. Pulmonary hypertension after shunt closure in patients with simple congenital heart defects. Int. J. Cardiol. 2020, 308, 28–32. [Google Scholar] [CrossRef] [PubMed]
- Muroke, V.; Jalanko, M.; Haukka, J.; Hartikainen, J.; Tahvanainen, A.; Ukkonen, H.; Ylitalo, K.; Pihkala, J.; Sinisalo, J. Outcome of transcatheter atrial septal defect closure in a nationwide cohort. Ann. Med. 2023, 55, 615–623. [Google Scholar] [CrossRef] [PubMed]
- Kazmi, T.; Sadiq, M.; Hyder, N.; Latif, F. Intermediate and long term outcome of patients after device closure of ASD with special reference to complications. J. Ayub Med. Coll. Abbottabad 2009, 21, 117–121. [Google Scholar] [PubMed]


| Type of ASD | Developmental Defect | Location | Associated Features |
|---|---|---|---|
| Primum ASD | Incomplete formation of the inferior limb of the septum secundum. | Lower part of the atrial septum. | Often linked with a cleft anterior mitral leaflet; considered a partial atrioventricular septal defect (AVSD). |
| Secundum ASD | Defect in septum primum (fossa ovalis) or upper septum secundum. | Central part (fossa ovalis region). | May be single or fenestrated (multiple small defects). |
| Sinus Venosus ASD | Abnormal development near venous entry points; deficiency of tissue separating pulmonary veins and vena cava. | Near the superior vena cava and inferior vena cava. | Frequently associated with abnormal pulmonary venous return. |
| Coronary Sinus ASD | Unroofing or absence of the coronary sinus. | Area of the coronary sinus ostium. | Can lead to communication between the atria through the coronary sinus. |
| Drug Type | Active Substances | Goal | Notes |
|---|---|---|---|
| Angiotensin Converting Enzyme (ACE) Inhibitors | Ramipril, Enalapril, Lisinopril | Reduction in afterload and halted LV remodelling. | Use in case of LV dysfunction or hypertension; caution with excessive afterload reduction. |
| Angiotensin Receptor Blockers (ARBs) | Losartan, Valsartan | Alternative to ACE-I. | Use when ACE-I is not tolerated. |
| Angiotensin Receptor Neprilysin Inhibitors (ARNI) | Sacubitril + Valsartan | Newer alternative to ACE-I/ARB. | For HFrEF or post-closure LV dysfunction, avoid if unstable BP. |
| Beta-blockers | Bisoprolol, Carvedilol, Metoprolol succinate | HR reduction, survival improvement, tachycardia prevention. | Start low in low-output or preload-dependent ASD; avoid bradycardia. |
| Mineralocorticoid Receptor Antagonists | Spironolactone, Eplerenone | Halted remodelling. | Use in chronic HF phenotype; avoid if K+ > 5 or eGFR < 30. |
| SGLT-2 Inhibitors | Empagliflozin, Dapagliflozin | Reduced hospitalizations and mortality. | Adjust if eGFR < 30; watch for dehydration. |
| Loop Diuretics | Furosemide, Torasemide, Bumetanide | Congestion and fluid overload decompression. | Avoid overdiuresis. |
| If-channel Inhibitor | Ivabradine | HR reduction in sinus rhythm when HR ≥ 70 bpm despite a beta-blocker. | Only if sinus rhythm and symptomatic; avoid in AF. |
| Hydralazine + ISDN | Hydralazine + Isosorbide dinitrate | Alternative/add-on vasodilator in intolerance to RAAS blockers. | Use with caution in ASD (hemodynamic shifts); watch BP. |
| Digoxin | Digoxin | Rate control in AF, mild inotropy in LV dysfunction. | High toxicity risk. |
| Monitoring Domain | Key Assessment Parameters |
|---|---|
| Clinical Evaluation | Exercise tolerance, dyspnea, syncope, palpitations |
| Cardiac Rhythm | ECG, Holter monitoring |
| Echocardiography | RV size and function, Tricuspid Regurgitation (TR) velocity, residual shunts |
| Radiology | Cardiac MRI |
| Biomarkers | NT-proBNP |
| Functional Testing | CPET, 6-min walk test |
| Hemodynamic Assessment | Right Heart Catheterization (RHC) |
| Hematology | Oxygen saturation (SpO2), Complete Blood Count (CBC) |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Bartoszewska, E.; Chrapkowska, A.; Zielińska, O.; Mordalska, M.; Lizon, J.; Zalewska, Z.; Wasicionek, M. Atrial Septal Defects: From Embryology to Pediatric Pulmonary Hypertension. J. Clin. Med. 2025, 14, 7698. https://doi.org/10.3390/jcm14217698
Bartoszewska E, Chrapkowska A, Zielińska O, Mordalska M, Lizon J, Zalewska Z, Wasicionek M. Atrial Septal Defects: From Embryology to Pediatric Pulmonary Hypertension. Journal of Clinical Medicine. 2025; 14(21):7698. https://doi.org/10.3390/jcm14217698
Chicago/Turabian StyleBartoszewska, Elżbieta, Anna Chrapkowska, Oliwia Zielińska, Maria Mordalska, Julia Lizon, Zuzanna Zalewska, and Marek Wasicionek. 2025. "Atrial Septal Defects: From Embryology to Pediatric Pulmonary Hypertension" Journal of Clinical Medicine 14, no. 21: 7698. https://doi.org/10.3390/jcm14217698
APA StyleBartoszewska, E., Chrapkowska, A., Zielińska, O., Mordalska, M., Lizon, J., Zalewska, Z., & Wasicionek, M. (2025). Atrial Septal Defects: From Embryology to Pediatric Pulmonary Hypertension. Journal of Clinical Medicine, 14(21), 7698. https://doi.org/10.3390/jcm14217698





