Can Multifrequency Tympanometry Be Used in the Diagnosis of Meniere’s Disease? A Systematic Review and Meta-Analysis
Abstract
1. Introduction
- At least two spontaneous episodes of vertigo with a duration of 20 min to 12 h.
- Pure tone audiogram reveals sensorineural hearing impairment in low and mid frequencies in the affected ear before, during, and/or after one of the episodes.
- Symptoms of hearing loss, tinnitus, and aural fullness in the affected ear present with fluctuation.
- Not better accounted for by other vestibular pathologies [11].
2. Materials and Methods
2.1. Protocol and Registration
2.2. Study Design
2.3. Eligibility Criteria
2.4. Search Strategy
2.5. Data Extraction and Tabulation
2.6. Quality of Evidence Assessment
2.7. Statistical Analysis
3. Results
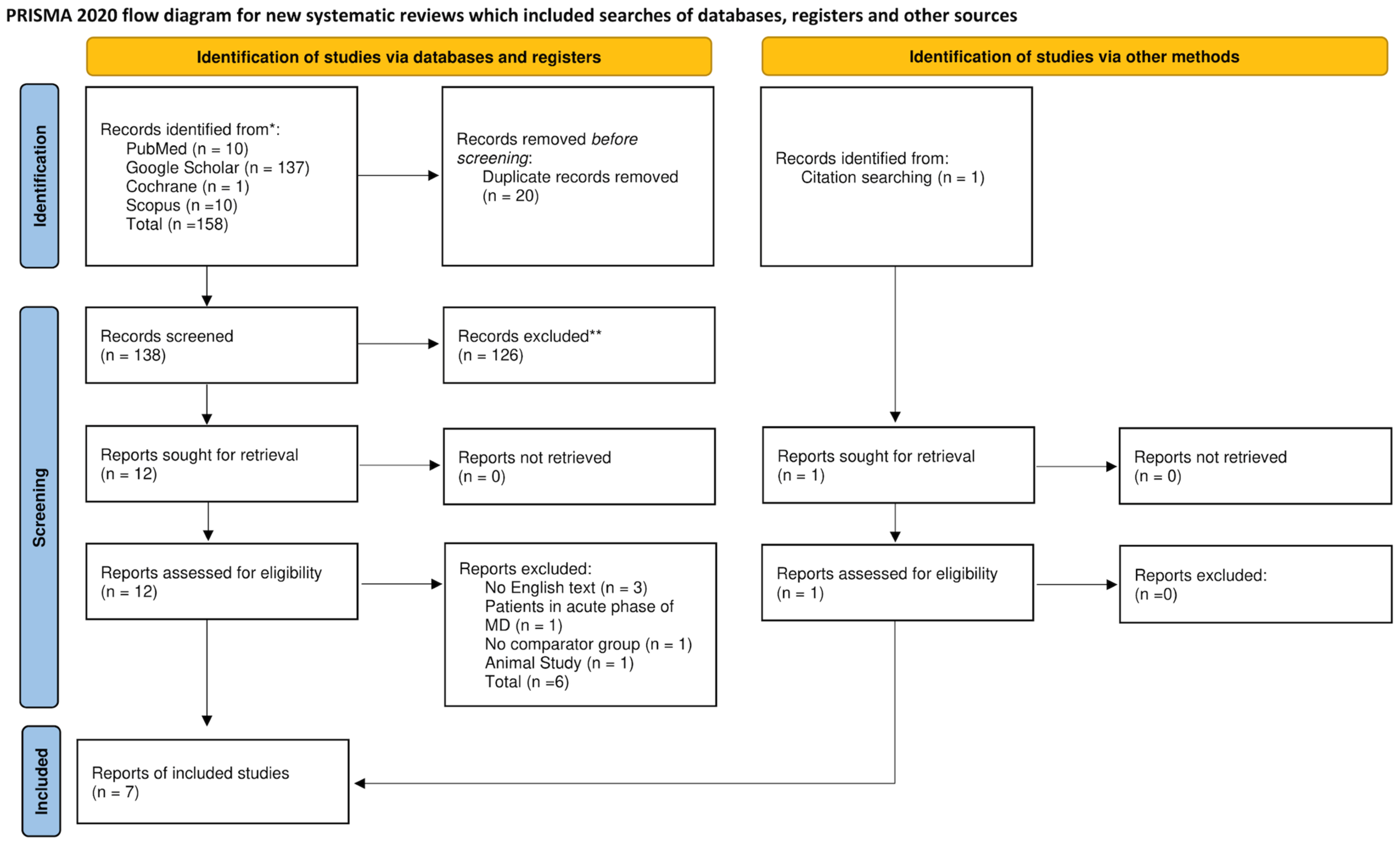
3.1. Study Selection and Baseline Characteristics
3.2. Outcomes
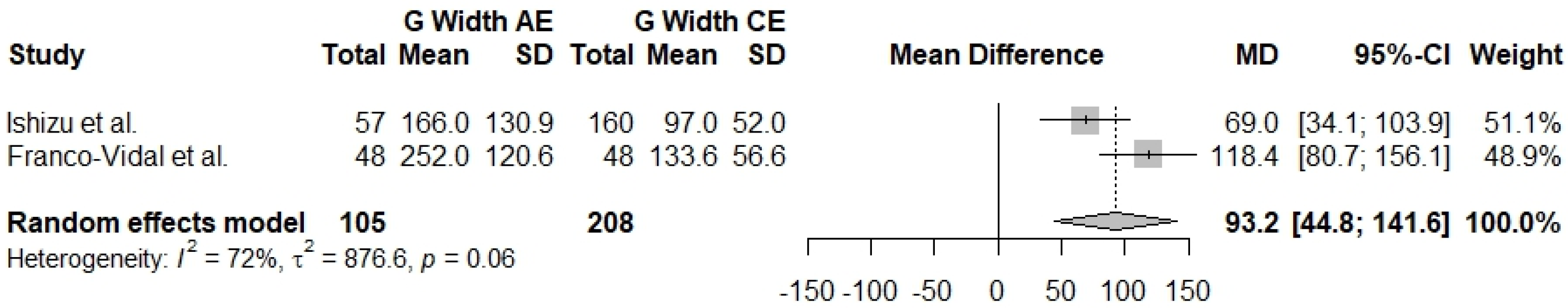
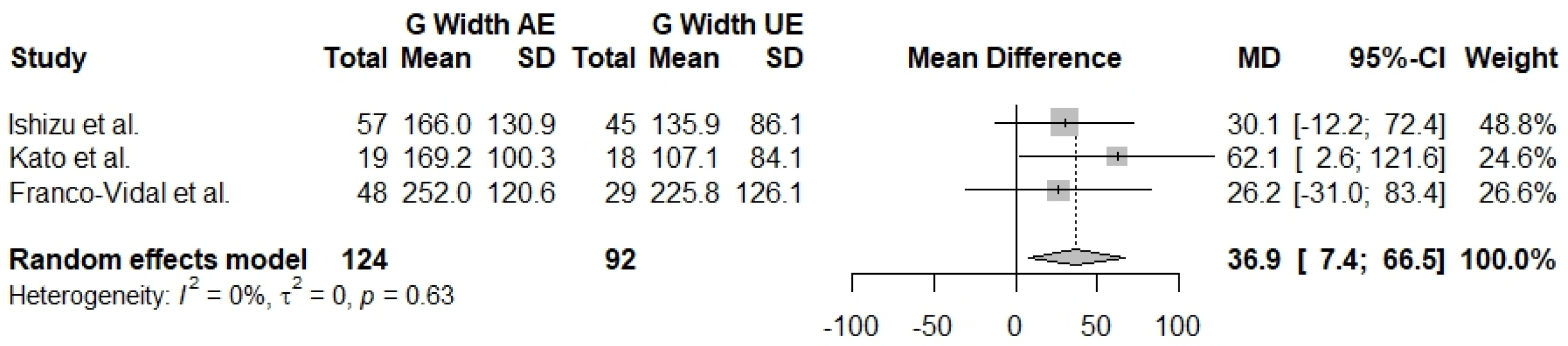
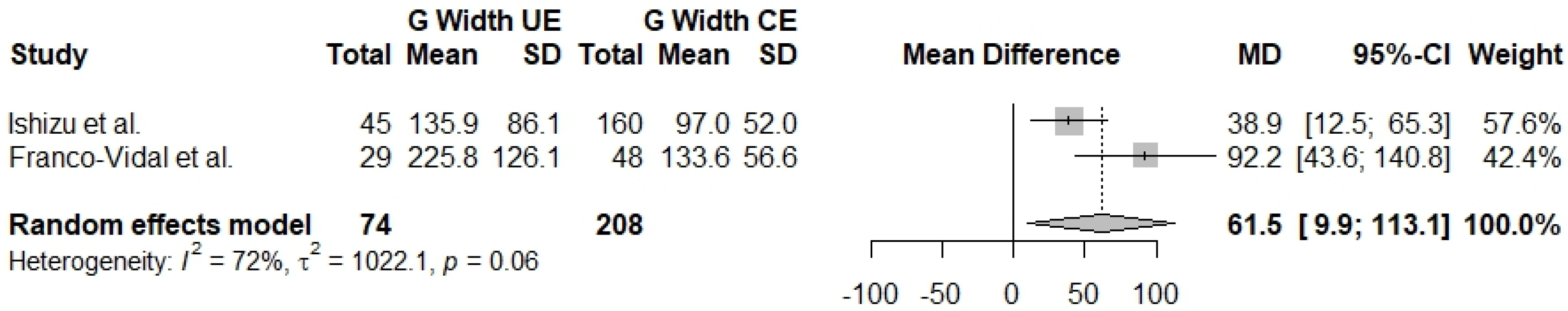
3.2.1. G Width 2 kHz
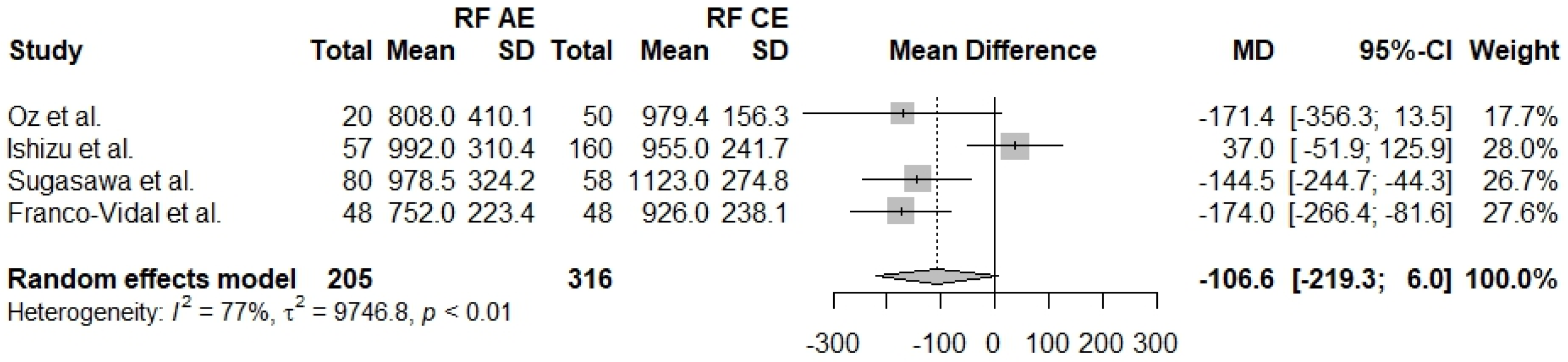
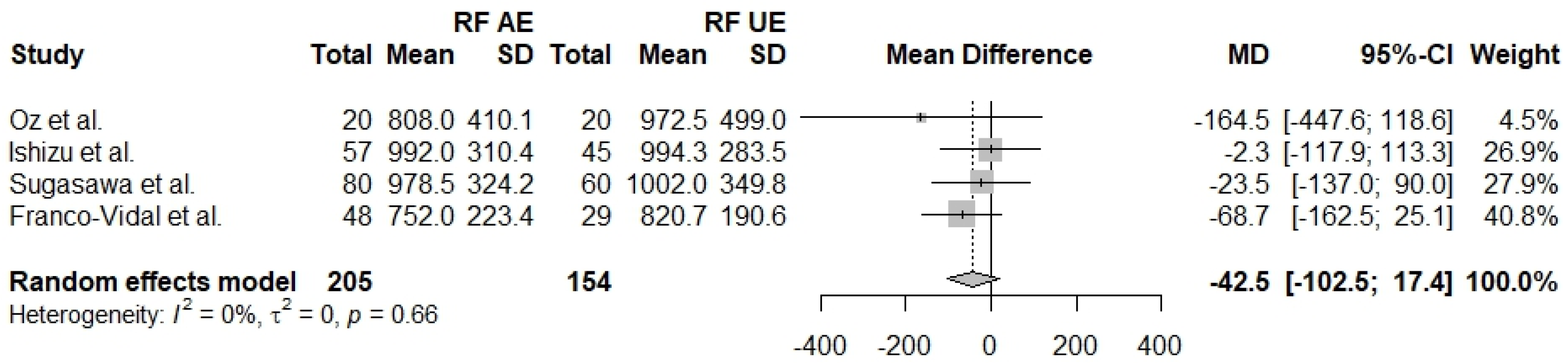
3.2.2. Resonant Frequency (RF)
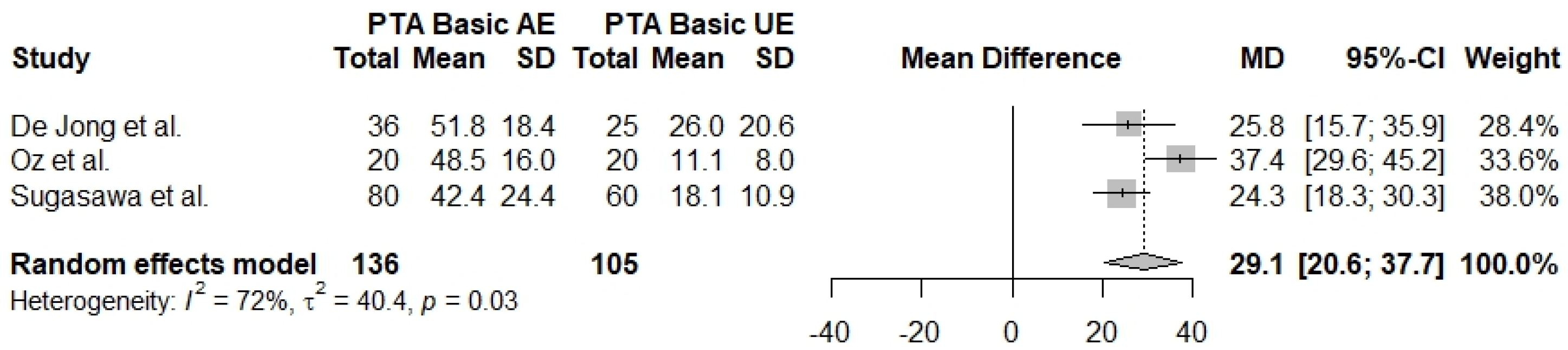
3.2.3. PTA Basic
4. Discussion
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Aibara, R.; Welsh, J.T.; Puria, S.; Goode, R.L. Human middle-ear sound transfer function and cochlear input impedance. Hear. Res. 2001, 152, 100–109. [Google Scholar] [CrossRef]
- Kim, J.; Koo, M. Mass and Stiffness Impact on the Middle Ear and the Cochlear Partition. J. Audiol. Otol. 2015, 19, 1–6. [Google Scholar] [CrossRef]
- Terkildsen, K.; Thomsen, K.A. The influence of pressure variations on the impedance of the human ear drum. A method for objective determination of the middle-ear pressure. J. Laryngol. Otol. 1959, 73, 409–418. [Google Scholar] [CrossRef]
- McCoul, E.D. Unlearning the ABCs of Tympanometry. Otolaryngol. Head Neck Surg. 2021, 165, 491–492. [Google Scholar] [CrossRef]
- Holte, L. Aging effects in multifrequency tympanometry. Ear Hear. 1996, 17, 12–18. [Google Scholar] [CrossRef]
- Lilly, D.J. Multiple frequency, multiple component tympanometry: New approaches to an old diagnostic problem. Ear Hear. 1984, 5, 300–308. [Google Scholar] [CrossRef] [PubMed]
- Iacovou, E.; Vlastarakos, P.V.; Ferekidis, E.; Nikolopoulos, T.P. Multi-frequency tympanometry: Clinical applications for the assessment of the middle ear status. Indian J. Otolaryngol. Head Neck Surg. 2013, 65, 283–287. [Google Scholar] [CrossRef] [PubMed]
- Paparella, M.M.; Djalilian, H.R. Etiology, pathophysiology of symptoms, and pathogenesis of Meniere’s disease. Otolaryngol. Clin. N. Am. 2002, 35, 529–545. [Google Scholar] [CrossRef] [PubMed]
- Basura, G.J.; Adams, M.E.; Monfared, A.; Schwartz, S.R.; Antonelli, P.J.; Burkard, R.; Bush, M.L.; Bykowski, J.; Colandrea, M.; Derebery, J.; et al. Clinical Practice Guideline: Ménière’s Disease. Otolaryngol. Head Neck Surg. 2020, 162 (Suppl. S2), S1–S55. [Google Scholar] [CrossRef] [PubMed]
- Magnan, J.; Özgirgin, O.N.; Trabalzini, F.; Lacour, L.; Escamez, A.L.; Magnusson, M.; Güneri, E.A.; Guyot, J.P.; Nuti, D.; Mandalà, M.; et al. European Position Statement on Diagnosis, and Treatment of Meniere’s Disease. J. Int. Adv. Otol. 2018, 14, 317–321. [Google Scholar] [CrossRef] [PubMed]
- Lopez-Escamez, J.A.; Carey, J.; Chung, W.H.; Goebel, J.A.; Magnusson, M.; Mandalà, M.; Newman-Toker, D.E.; Strupp, M.; Suzuki, M.; Trabalzini, F.; et al. Diagnostic criteria for Menière’s disease. J. Vestib. Res. 2015, 25, 1–7. [Google Scholar] [CrossRef] [PubMed]
- EEggermont, J.J. Ups and Downs in 75 Years of Electrocochleography. Front. Syst. Neurosci. 2017, 11, 2. [Google Scholar] [CrossRef]
- Lin, M.; Timmer, F.C.A.; Oriel, B.S.; Zhou, G.; Guinan, J.J.; Kujawa, S.G.; Herrmann, B.S.; Merchant, S.N.; Rauch, S.D. Vestibular evoked myogenic potentials (VEMP) can detect asymptomatic saccular hydrops. Laryngoscope 2006, 116, 987–992. [Google Scholar] [CrossRef] [PubMed]
- Fukuoka, H.; Takumi, Y.; Tsukada, K.; Miyagawa, M.; Oguchi, T.; Ueda, H.; Kadoya, M.; Usami, S. Comparison of the diagnostic value of 3 T MRI after intratympanic injection of GBCA, electrocochleography, and the glycerol test in patients with Meniere’s disease. Acta Otolaryngol. 2012, 132, 141–145. [Google Scholar] [CrossRef] [PubMed]
- Darrouzet, V.; Dulon, D.; Franco-Vidal, V. Multifrequency immittancemetry in experimentally induced stapes, round window and cochlear lesions. Audiol. Neurootol. 2007, 12, 85–100. [Google Scholar] [CrossRef] [PubMed]
- Page, M.J.; McKenzie, J.E.; Bossuyt, P.M.; Boutron, I.; Hoffmann, T.C.; Mulrow, C.D.; Shamseer, L.; Tetzlaff, J.M.; Akl, E.A.; Brennan, S.E.; et al. The PRISMA 2020 statement: An updated guideline for reporting systematic reviews. BMJ 2021, 10, n71. [Google Scholar] [CrossRef] [PubMed]
- Wohlin, C. Guidelines for snowballing in systematic literature studies and a replication in software engineering. In Proceedings of the 18th International Conference on Evaluation and Assessment in Software Engineering, London, UK, 13–14 May 2014. [Google Scholar]
- Wells, G.A.; Shea, B.; O’Connell, D.; Peterson, J.; Welch, V.; Losos, M.; Tugwell, P. The Newcastle-Ottawa Scale (NOS) for Assessing the Quality of Nonrandomized Studies in Meta-Analyses. Available online: http://www.ohri.ca/programs/clinical_epidemiology/oxford.htm (accessed on 1 February 2009).
- Hozo, S.P.; Djulbegovic, B.; Hozo, I. Estimating the mean and variance from the median, range, and the size of a sample. BMC 2005, 5, 13. [Google Scholar] [CrossRef]
- Bianchedi, M.; Croce, A.; Neri, G.; Moretti, A. La timpanometria multifrequenziale nella malattia di Ménière: Risultati preliminari [Multifrequency tympanometry in Meniere’s disease: Preliminary results]. Acta Otorhinolaryngol. Ital. 1996, 16, 1–5. (In Italian) [Google Scholar]
- Gersdorff, M. Intérêt clinique de la tympanométrie multifréquentielle [Clinical value of multifrequential tympanometry]. Acta Otorhinolaryngol. Belg. 1980, 34, 270–278. (In French) [Google Scholar]
- González, C.; García, M.L.S.; Vilas, C.C.; Varela, A.S.; Lago, P.V.; de la Soledad Santos Pérez, S.M.; Caballero, T.L. Timpanometría de multifrecuencia en el vértigo de Menière unilateral durante las intercrisis. Acta Otorrinolaringol. Gallega 2003, 4, 1–6. [Google Scholar]
- Cakir Cetin, A.; Gurkan, S.; Kirkim, G.; Guneri, E.A. Wide-Band Tympanometry Results during an Acute Episode of Ménière’s Disease. Audiol. Neurootol. 2019, 24, 231–236. [Google Scholar] [CrossRef]
- Franco-Vidal, V.; Bonnard, D.; Bellec, O.; Thomeer, H.; Darrouzet, V. Effects of Body Tilt on Multifrequency Admittance Tympanometry. Otol. Neurotol. 2015, 36, 737–740. [Google Scholar] [CrossRef]
- Darrouzet, V.; Erre, J.P.; Dulon, D.; Camicas van Gout, M.; Aran, J.M.; Poutout, P.A.; Negrevergne, M.; Dauman, R.; Bebear, J.P. Données de l’impédancemétrie multifréquentielle dans les pathologies cochléaires. Approche expérimentale chez le chinchilla et le cobaye [Multi-frequency tympanometry in experimentally-induced cochlear lesions in chinchillas and guinea pigs]. Rev. Laryngol. Otol. Rhinol. 1999, 120, 305–316. (In French) [Google Scholar]
- Yasui, T.; Iwasaki, S.; Sugasawa, K.; Sakamoto, T.; Kashio, A.; Suzuki, M.; Kakigi, A.; Yamasoba, T. Admittance tympanometry with 2-kHz probe tones in patients with low-frequency hearing loss. Laryngoscope 2012, 122, 2252–2255. [Google Scholar] [CrossRef]
- Ishizu, K.; Tamae, A.; Kubo, K.; Yoshida, T.; Matsumoto, N.; Yasui, T.; Nakagawa, T. Diagnosis and following up of Ménière’s disease using multifrequency tympanometry-Cutoff values and temporal changes in measurements. Auris Nasus Larynx. 2018, 45, 81–87. [Google Scholar] [CrossRef] [PubMed]
- Sugasawa, K.; Iwasaki, S.; Fujimoto, C.; Kinoshita, M.; Inoue, A.; Egami, N.; Ushio, M.; Chihara, Y.; Yamasoba, Y. Diagnostic usefulness of multifrequency tympanometry for Ménière’s disease. Audiol. Neurootol. 2013, 18, 152–160. [Google Scholar] [CrossRef] [PubMed]
- Kato, K.; Yoshida, T.; Teranishi, M.; Sano, R.; Otake, H.; Sone, M.; Naganawa, S.; Nakashima, T. Peak width in multifrequency tympanometry and endolymphatic hydrops revealed by magnetic resonance imaging. Otol. Neurotol. 2012, 33, 912–915. [Google Scholar] [CrossRef] [PubMed]
- Franco-Vidal, V.; Legarlantezec, C.; Blanchet, H.; Convert, C.; Torti, F.; Darrouzet, V. Multifrequency admittancemetry in Ménière’s Disease: A preliminary study for a new diagnostic test. Otol. Neurotol. 2005, 26, 723–727. [Google Scholar] [CrossRef] [PubMed]
- Oz, I.; Hizal, E.; Cam, O.H.; Ozluoglu, L.N. Effects of Glycerol Test on Resonance Frequency in Patients with Ménière’s Disease. Audiol. Neurootol. 2019, 24, 285–292. [Google Scholar] [CrossRef] [PubMed]
- de Jong, M.A.; van Esch, B.F.; van Benthem, P.P.G.; van der Zaag-Loonen, H.J.; Bruintjes, T.D.; Thomeer, H.G.X.M. The Diagnostic Value of Multifrequency Tympanometry in Patients with Ménière’s Disease: A Prospective Analysis. Audiol. Neurootol. 2023, 15, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Kontrogianni, A.; Ferekidis, E.; Ntouniadakis, E.; Psarommatis, I.; Apostolopoulos, N.; Adamopoulos, G. Multiple-frequency tympanometry in children with otitis media with effusion. ORL J. Otorhinolaryngol. Relat. Spec. 1996, 58, 78–81. [Google Scholar] [CrossRef]
- Vlachou, S.; Ferekidis, E.; Tsakanikos, M.; Apostolopoulos, N.; Adamopoulos, G. Prognostic value of multiple-frequency tympanometry in acute otitis media. ORL J. Otorhinolaryngol. Relat. Spec. 1999, 61, 195–200. [Google Scholar] [CrossRef]
- Ferekidis, E.; Vlachou, S.; Douniadakis, D.; Apostolopoulos, N.; Adamopoulos, G. Multiple-frequency tympanometry in children with acute otitis media. Otolaryngol. Head Neck Surg. 1999, 121, 797–801. [Google Scholar] [CrossRef]
- Thai-Van, H.; Bounaix, M.J.; Fraysse, B. Menière’s disease: Pathophysiology and treatment. Drugs 2001, 61, 1089–1102. [Google Scholar] [CrossRef] [PubMed]
- Zwislocki, J. An acoustic method for clinical examination of the ear. J. Speech Hear Res. 1963, 6, 303–314. [Google Scholar] [CrossRef] [PubMed]
- Tanno, G.A.Y.; Santos, M.A.O.; Sanches, M.T.D.; Durante, A.S.; Almeida, K.; Gameiro, M.S.; Roque, N.M.C.F.; Sousa Neto, O.M. Analysis of wideband tympanometry in Ménière’s disease. Braz. J. Otorhinolaryngol. 2022, 88, 194–203. [Google Scholar] [CrossRef]
- Camicas van Gout, M. Théorie acoustico-mécanique: Localisation des sources sonores. Rev. Laryngol. Otol. Rhinol. 1994, 115, 13–20. [Google Scholar]
- Camicas van Gout, M.; Negrevergne, M. Impédancemétrie multifréquentielle et exploration des surdités professionnelles. Un nouveau test «le Teflag». Rev. Laryngol. Otol. Rhinol. 1996, 117, 399–407. [Google Scholar]
- Tamae, A.; Ishizu, K.; Yoshida, T.; Kubo, K.; Matsumoto, N.; Yasui, T.; Masutani, K.; Tsuruya, K.; Nakagawa, T.; Clinic, F.I.O. Evaluation of the Effects of Chronic Kidney Disease and Hemodialysis on the Inner Ear Using Multifrequency Tympanometry. J. Int. Adv. Otol. 2018, 14, 447–450. [Google Scholar] [CrossRef]
- Nakashima, T.; Ueda, H.; Furuhashi, A.; Eisuke, S.; Kiyomitsu, A.; Shinji, N.; Reiko, B. Air-bone gap and resonant frequency in large vestibular aqueduct syndrome. Am. J. Otol. 2000, 21, 671Y4. [Google Scholar]
- Paparella, M.M.; Griebie, M.S. Bilaterality of Meniere’s disease. Acta Otolaryngol. 1984, 97, 233–237. [Google Scholar] [CrossRef]
- Ferekidis, E. Microtraumatic stapedotomy. Adv. Otorhinolaryngol. 2007, 65, 164–168. [Google Scholar] [PubMed]
- Mateijsen, D.J.; Van Hengel, P.W.; Van Huffelen, W.M.; Wit, H.P.; Albers, F.W.J. Pure-tone and speech audiometry in patients with Menière’s disease. Clin. Otolaryngol. Allied Sci. 2001, 26, 379–387. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Mucknik, C.; Hildesheimer, M.; Rubinstein, M.; Arenberg, I.K. Low frequency air-bone gap in Meniere’s disease without middle ear pathology. A preliminary report. Am. J. Otol. 1989, 10, 1Y4. [Google Scholar]

| Author | Year | Study Design | Total Ears Examined | Affected/Unaffected/Control Ears | RF, Mean ± SD | PTA Basic, Mean ± SD | G Width (2 KHz), Mean ± SD | Y Width (2 KHz), Mean ± SD |
|---|---|---|---|---|---|---|---|---|
| De Jong et al. [32] | 2023 | Prospective, not matched | 125 | AE: 36 UE: 25 CE: 64 | N/A | AE: 51.8 ± 18.4 UE: 26 ± 20.6 CE: N/A | N/A | AE: 315.6 ± 70.2 UE: 292.3 ± 98.6 CE: 259.4 ± 60.6 |
| Oz et al. [31] | 2019 | Prospective, not matched | 90 | AE: 20 UE:20 CE: 50 | AE: 808 ± 410.1 UE: 972.5 ± 499 CE: 979.4 ± 156.3 | AE: 48.5 ±16 UE: 11.2 ± 8 CE: N/A | N/A | N/A |
| Ishizu et al. [27] | 2018 | Prospective, not matched | 262 | AE: 57 UE: 45 CE: 160 | AE: 992 ± 320.4 UE: 994.3 ± 283.5 CE: 955 ± 241.7 | N/A | AE: 166 ± 130.9 UE: 135.9 ± 86.1 CE: 97 ± 52 | N/A |
| Sugawasa et al. [28] | 2013 | Prospective, not matched | 198 | AE: 80 UE: 60 CE: 58 | AE: 978.5 ± 324.2 UE: 1002 ± 349.8 CE: 1123± 274.8 | AE: 42.4 ± 24.4 UE: 18.1 ± 10.9 CE: N/A | N/A | AE: 256.5 ± 126.1 UE:226.2 ± 138.7 CE: 175.4 ± 66.6 |
| Kato et al. [29] | 2012 | Prospective, not matched | 50 | AE: 19 UE: 18 CE: 13 | AE: 917.4 ± 205.3 UE: 926.9 ± 156.3 CE: N/A | N/A | AE: 169.2 ± 100.3 UE: 107.2 ± 84.1 CE: N/A | N/A |
| Franco-Vidal et al. [30] | 2005 | Prospective, not matched | 125 | AE: 48 UE: 29 CE: 48 | AE: 752 ± 223.4 UE: 820.7 ± 190.6 CE: 926 ± 238.1 | N/A | AE: 252 ± 120.6 UE: 225.8 ± 126.1 CE: 133.6 ± 56.6 | N/A |
| Yasui et al. [26] | 2012 | Prospective, not matched | 49 | AE: 22 UE: N/A CE: 27 | N/A | N/A | N/A | AE: 230 ± 15 UE: 179 ± 9 CE: 157 ± 14 |
| Outcomes | n | Mean Difference [95% CI] | Heterogeneity | |
|---|---|---|---|---|
| I2 | p | |||
| G Width 2 kHz (AE–UE) | 3 | 36.9 [7.4; 66.5] | 0% | 0.63 |
| G Width 2 kHz (AE–CE) | 2 | 93.2 [44.8; 141.6] | 72% | 0.06 |
| G Width 2 kHz (UE–CE) | 2 | 61.5 [9.9; 113.1] | 72% | 0.06 |
| PTA Basic (AE–UE) | 3 | 29.1 [20.6; 37.7] | 72% | 0.03 |
| RF (AE–UE) | 4 | −42.5 [−102.5; 17.4] | 0% | 0.66 |
| RF (AE–CE) | 4 | −106.6 [−219.3; 6.0] | 77% | <0.01 |
| RF (UE–CE) | 5 | −52.4 [−139.9; 35.1] | 55% | 0.09 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Tsilivigkos, C.; Vitkos, E.N.; Ferekidis, E.; Warnecke, A. Can Multifrequency Tympanometry Be Used in the Diagnosis of Meniere’s Disease? A Systematic Review and Meta-Analysis. J. Clin. Med. 2024, 13, 1476. https://doi.org/10.3390/jcm13051476
Tsilivigkos C, Vitkos EN, Ferekidis E, Warnecke A. Can Multifrequency Tympanometry Be Used in the Diagnosis of Meniere’s Disease? A Systematic Review and Meta-Analysis. Journal of Clinical Medicine. 2024; 13(5):1476. https://doi.org/10.3390/jcm13051476
Chicago/Turabian StyleTsilivigkos, Christos, Evangelos N. Vitkos, Eleftherios Ferekidis, and Athanasia Warnecke. 2024. "Can Multifrequency Tympanometry Be Used in the Diagnosis of Meniere’s Disease? A Systematic Review and Meta-Analysis" Journal of Clinical Medicine 13, no. 5: 1476. https://doi.org/10.3390/jcm13051476
APA StyleTsilivigkos, C., Vitkos, E. N., Ferekidis, E., & Warnecke, A. (2024). Can Multifrequency Tympanometry Be Used in the Diagnosis of Meniere’s Disease? A Systematic Review and Meta-Analysis. Journal of Clinical Medicine, 13(5), 1476. https://doi.org/10.3390/jcm13051476