Enhancing COVID-19 Vaccines Acceptance: Results from a Survey on Vaccine Hesitancy in Northern Italy
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Design and Data Collection
2.2. Questionnaire
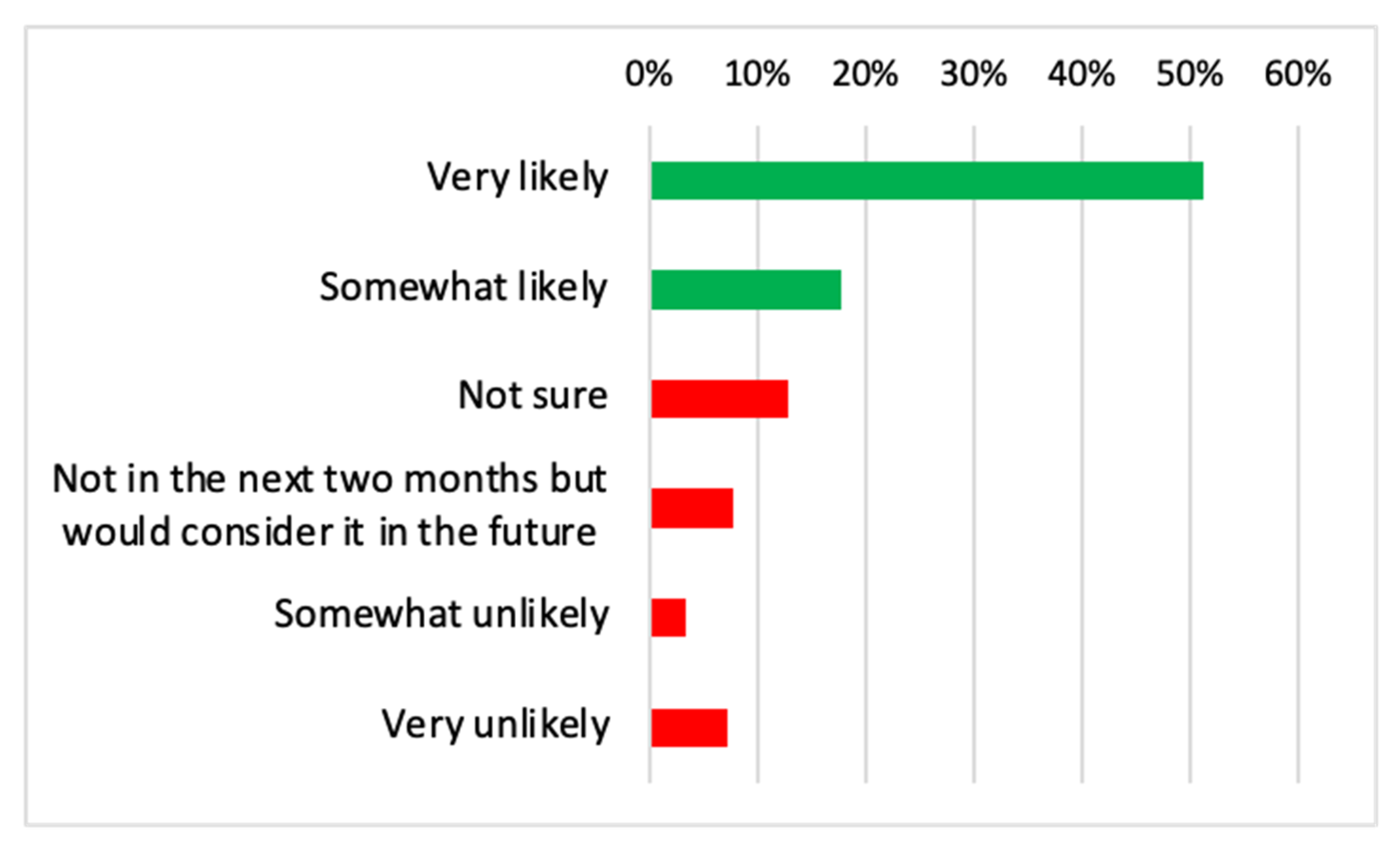
2.3. Vaccine Hesitancy (Dependent Variable)
2.4. Putative Predictors of Vaccine Hesitancy (Independent Variables)
2.5. Statistical Analysis
3. Results
3.1. Sample Characteristics
3.2. Risk of Infection Perception
3.3. Predictors of Vaccine Hesitancy
3.4. Specific Reasons for Past Refusal
3.5. Motivations Needed to Increase Confidence in COVID-19 Vaccine in Hesitant Respondents
3.6. Classification Tree Analysis
4. Discussion
5. Limitations and Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- EU Vaccination Days. Available online: http://www.politicheeuropee.gov.it/en/communication/news/european-vaccination-days-against-covid-19/ (accessed on 3 March 2021).
- COVID-19 Vaccines: Development, Evaluation, Approval and Monitoring. Available online: https://www.ema.europa.eu/en/human-regulatory/overview/public-health-threats/coronavirus-disease-covid-19/treatments-vaccines/vaccines-covid-19/covid-19-vaccines-development-evaluation-approval-monitoring (accessed on 3 March 2021).
- COVID-19 Vaccines: Key Facts. Available online: https://www.ema.europa.eu/en/human-regulatory/overview/public-health-threats/coronavirus-disease-covid-19/treatments-vaccines/vaccines-covid-19/covid-19-vaccines-key-facts (accessed on 3 March 2021).
- Coronavirus Vaccines Strategy. Available online: https://ec.europa.eu/info/live-work-travel-eu/coronavirus-response/public-health/coronavirus-vaccines-strategy_en (accessed on 12 March 2021).
- Lazarus, J.V.; Ratzan, S.C.; Palayew, A.; Gostin, L.O.; Larson, H.J.; Rabin, K.; Kimball, S.; El-Mohandes, A. A Global Survey of Potential Acceptance of a COVID-19 Vaccine. Nat. Med. 2021, 27, 225–228. [Google Scholar] [CrossRef] [PubMed]
- MacDonald, N.E. SAGE Working Group on Vaccine Hesitancy Vaccine Hesitancy: Definition, Scope and Determinants. Vaccine 2015, 33, 4161–4164. [Google Scholar] [CrossRef]
- COVID-19 Vaccination Intent Is Decreasing Globally. Available online: https://www.ipsos.com/en/global-attitudes-covid-19-vaccine-october-2020 (accessed on 3 March 2021).
- Lewis, J.R. What Is Driving the Decline in People’s Willingness to Take the COVID-19 Vaccine in the United States? JAMA Health Forum 2020, 1, e201393. [Google Scholar] [CrossRef]
- Savoia, E.; Piltch-Loeb, R.; Goldberg, B.; Miller-Idriss, C.; Hughes, B.; Montrond, A.; Kayyem, J.; Testa, M. Predictors of COVID-19 Vaccine Hesitancy: Socio-Demographics, Co-Morbidity and Past Experience of Racial Discrimination. medRxiv 2021. [Google Scholar] [CrossRef]
- Piltch-Loeb, R.; Savoia, E.; Goldberg, B.; Hughes, B.; Verhey, T.; Kayyem, J.; Miller-Idriss, C.; Testa, M. Examining the Effect of Information Channel on COVID-19 Vaccine Acceptance. medRxiv 2021. [Google Scholar] [CrossRef]
- Malik, A.A.; McFadden, S.M.; Elharake, J.; Omer, S.B. Determinants of COVID-19 Vaccine Acceptance in the US. EClinicalMedicine 2020, 26, 100495. [Google Scholar] [CrossRef] [PubMed]
- Graffigna, G.; Palamenghi, L.; Boccia, S.; Barello, S. Relationship between Citizens’ Health Engagement and Intention to Take the COVID-19 Vaccine in Italy: A Mediation Analysis. Vaccines 2020, 8, 576. [Google Scholar] [CrossRef] [PubMed]
- Catalogue of Interventions Addressing Vaccine Hesitancy. Available online: https://www.ecdc.europa.eu/en/publications-data/catalogue-interventions-addressing-vaccine-hesitancy (accessed on 3 March 2021).
- Ten Health Issues WHO Will Tackle This Year. Available online: https://www.who.int/news-room/spotlight/ten-threats-to-global-health-in-2019 (accessed on 3 March 2021).
- Vaccine Hesitancy Is a Global Public Health Threat. Are We Doing Enough about It? Available online: https://www.elsevier.com/connect/vaccine-hesitancy-is-a-global-public-health-threat-are-we-doing-enough-about-it (accessed on 4 March 2021).
- Rapid Literature Review on Motivating Hesitant Population Groups in Europe to Vaccinate. Available online: https://www.ecdc.europa.eu/en/publications-data/rapid-literature-review-motivating-hesitant-population-groups-europe-vaccinate (accessed on 3 March 2021).
- Neumann-Böhme, S.; Varghese, N.E.; Sabat, I.; Barros, P.P.; Brouwer, W.; van Exel, J.; Schreyögg, J.; Stargardt, T. Once We Have It, Will We Use It? A European Survey on Willingness to Be Vaccinated against COVID-19. Eur. J. Health Econ. 2020, 21, 977–982. [Google Scholar] [CrossRef] [PubMed]
- Fisher, K.A.; Bloomstone, S.J.; Walder, J.; Crawford, S.; Fouayzi, H.; Mazor, K.M. Attitudes Toward a Potential SARS-CoV-2 Vaccine: A Survey of U.S. Adults. Ann. Intern. Med. 2020, 173, 964–973. [Google Scholar] [CrossRef]
- Taylor, S.; Landry, C.A.; Paluszek, M.M.; Groenewoud, R.; Rachor, G.S.; Asmundson, G.J.G. A Proactive Approach for Managing COVID-19: The Importance of Understanding the Motivational Roots of Vaccination Hesitancy for SARS-CoV2. Front. Psychol. 2020, 11, 575950. [Google Scholar] [CrossRef]
- Reiter, P.L.; Pennell, M.L.; Katz, M.L. Acceptability of a COVID-19 Vaccine among Adults in the United States: How Many People Would Get Vaccinated? Vaccine 2020, 38, 6500–6507. [Google Scholar] [CrossRef]
- Caserotti, M.; Girardi, P.; Rubaltelli, E.; Tasso, A.; Lotto, L.; Gavaruzzi, T. Associations of COVID-19 Risk Perception with Vaccine Hesitancy over Time for Italian Residents. Soc. Sci. Med. 2021, 272, 113688. [Google Scholar] [CrossRef]
- Ruiz, J.B.; Bell, R.A. Predictors of Intention to Vaccinate against COVID-19: Results of a Nationwide Survey. Vaccine 2021, 39, 1080–1086. [Google Scholar] [CrossRef]
- SteelFisher, G.K.; Blendon, R.J.; Caporello, H. An Uncertain Public—Encouraging Acceptance of Covid-19 Vaccines. N. Engl. J. Med. 2021. [Google Scholar] [CrossRef] [PubMed]
- Dror, A.A.; Eisenbach, N.; Taiber, S.; Morozov, N.G.; Mizrachi, M.; Zigron, A.; Srouji, S.; Sela, E. Vaccine Hesitancy: The next Challenge in the Fight against COVID-19. Eur. J. Epidemiol. 2020, 35, 775–779. [Google Scholar] [CrossRef] [PubMed]
- Machida, M.; Nakamura, I.; Kojima, T.; Saito, R.; Nakaya, T.; Hanibuchi, T.; Takamiya, T.; Odagiri, Y.; Fukushima, N.; Kikuchi, H.; et al. Acceptance of a COVID-19 Vaccine in Japan during the COVID-19 Pandemic. Vaccines 2021, 9, 210. [Google Scholar] [CrossRef] [PubMed]
- Schwarzinger, M.; Watson, V.; Arwidson, P.; Alla, F.; Luchini, S. COVID-19 Vaccine Hesitancy in a Representative Working-Age Population in France: A Survey Experiment Based on Vaccine Characteristics. Lancet Public Health 2021. [Google Scholar] [CrossRef]
- Verger, P.; Peretti-Watel, P. Understanding the Determinants of Acceptance of COVID-19 Vaccines: A Challenge in a Fast-Moving Situation. Lancet Public Health 2021. [Google Scholar] [CrossRef]
- Carpiano, R.M.; Polonijo, A.N.; Gilbert, N.; Cantin, L.; Dubé, E. Socioeconomic Status Differences in Parental Immunization Attitudes and Child Immunization in Canada: Findings from the 2013 Childhood National Immunization Coverage Survey (CNICS). Prev. Med. 2019, 123, 278–287. [Google Scholar] [CrossRef]
- Kempe, A.; Saville, A.W.; Albertin, C.; Zimet, G.; Breck, A.; Helmkamp, L.; Vangala, S.; Dickinson, L.M.; Rand, C.; Humiston, S.; et al. Parental Hesitancy about Routine Childhood and Influenza Vaccinations: A National Survey. Pediatrics 2020, 146, e20193852. [Google Scholar] [CrossRef]
- Silveira, M.F.; Buffarini, R.; Bertoldi, A.D.; Santos, I.S.; Barros, A.J.D.; Matijasevich, A.; Menezes, A.M.B.; Gonçalves, H.; Horta, B.L.; Barros, F.C.; et al. The Emergence of Vaccine Hesitancy among Upper-Class Brazilians: Results from Four Birth Cohorts, 1982–2015. Vaccine 2020, 38, 482–488. [Google Scholar] [CrossRef] [PubMed]
- De Cata-Preta, B.O.; Wehrmeister, F.C.; Santos, T.M.; Barros, A.J.D.; Victora, C.G. Patterns in Wealth-Related Inequalities in 86 Low- and Middle-Income Countries: Global Evidence on the Emergence of Vaccine Hesitancy. Am. J. Prev. Med. 2021, 60, S24–S33. [Google Scholar] [CrossRef] [PubMed]
- Lin, C.; Tu, P.; Beitsch, L.M. Confidence and Receptivity for COVID-19 Vaccines: A Rapid Systematic Review. Vaccines 2021, 9, 16. [Google Scholar] [CrossRef] [PubMed]
- Bert, F.; Olivero, E.; Rossello, P.; Gualano, M.R.; Castaldi, S.; Damiani, G.; D’Errico, M.M.; Di Giovanni, P.; Fantini, M.P.; Fabiani, L.; et al. Knowledge and Beliefs on Vaccines among a Sample of Italian Pregnant Women: Results from the NAVIDAD Study. Eur. J. Public Health 2020, 30, 286–292. [Google Scholar] [CrossRef]
- Salmon, D.A.; Dudley, M.Z.; Glanz, J.M.; Omer, S.B. Vaccine Hesitancy: Causes, Consequences, and a Call to Action. Am. J. Prev. Med. 2015, 49, S391–S398. [Google Scholar] [CrossRef] [PubMed]
- Sallam, M.; Dababseh, D.; Eid, H.; Al-Mahzoum, K.; Al-Haidar, A.; Taim, D.; Yaseen, A.; Ababneh, N.A.; Bakri, F.G.; Mahafzah, A. High Rates of COVID-19 Vaccine Hesitancy and Its Association with Conspiracy Beliefs: A Study in Jordan and Kuwait among Other Arab Countries. Vaccines 2021, 9, 42. [Google Scholar] [CrossRef]
- Jarrett, C.; Wilson, R.; O’Leary, M.; Eckersberger, E.; Larson, H.J. Strategies for Addressing Vaccine Hesitancy—A Systematic Review. Vaccine 2015, 33, 4180–4190. [Google Scholar] [CrossRef]
- How Can We Address Covid-19 Vaccine Hesitancy and Improve Vaccine Acceptance? Available online: https://blogs.bmj.com/bmj/2021/02/19/how-can-we-address-covid-19-vaccine-hesitancy-and-improve-vaccine-acceptance/ (accessed on 3 March 2021).
- Alley, S.J.; Stanton, R.; Browne, M.; To, Q.G.; Khalesi, S.; Williams, S.L.; Thwaite, T.L.; Fenning, A.S.; Vandelanotte, C. As the Pandemic Progresses, How Does Willingness to Vaccinate against COVID-19 Evolve? Int. J. Environ. Res. Public Health 2021, 18, 797. [Google Scholar] [CrossRef]
- Wang, K.; Wong, E.L.; Ho, K.F.; Cheung, A.W.; Yau, P.S.; Dong, D.; Wong, S.Y.; Yeoh, E.K. Change of Willingness to Accept COVID-19 Vaccine and Reasons of Vaccine Hesitancy of Working People at Different Waves of Local Epidemic in Hong Kong, China: Repeated Cross-Sectional Surveys. Vaccines 2021, 9, 62. [Google Scholar] [CrossRef]
| Characteristics | Overall | Confident | Hesitant | p-Value |
|---|---|---|---|---|
| (N = 1011) | (N = 697) | (N = 314) | ||
| N (%) | N (%) | N (%) | ||
| Age (years) | 0.002 | |||
| 18–34 | 154 (15.2) | 117 (16.8) | 37 (11.8) | |
| 35–44 | 271 (26.8) | 167 (24.0) | 104 (33.1) | |
| 45–54 | 314 (31.1) | 211 (30.3) | 103 (32.8) | |
| ≥55 | 272 (26.9) | 202 (29.0) | 70 (22.3) | |
| Gender | 0.235 | |||
| Male | 453(44.8) | 321 (46.1) | 132 (42.0) | |
| Female | 558 (55.2) | 376 (53.9) | 182 (58.0) | |
| Education | 0.013 | |||
| High school or lower degree | 642 (63.5) | 425 (61.0) | 217 (69.1) | |
| Bachelor’s or higher degree | 369 (36.5) | 272 (39.0) | 97 (30.9) | |
| Employment status | 0.028 | |||
| Paid employed | 592 (58.5) | 414 (59.4) | 178 (56.7) | |
| Self-employed | 129 (12.8) | 76 (10.9) | 53 (17.9) | |
| Other | 290 (28.7) | 207 (29.7) | 83 (26.4) | |
| Family income | 0.001 | |||
| Higher than average | 104 (10.3) | 81 (11.6) | 23 (7.3) | |
| On average | 591 (58.5) | 421 (60.4) | 170 (54.1) | |
| Lower than average | 316 (31.3) | 195 (28.0) | 121 (38.5) | |
| Number of family members | 0.413 | |||
| 1 | 112 (11.1) | 72 (10.3) | 40 (12.7) | |
| 2 | 306 (30.3) | 221 (31.7) | 85 (27.1) | |
| 3 | 318 (31.5) | 222 (31.9) | 96 (30.6) | |
| 4 | 214 (21.2) | 143 (20.5) | 71 (22.6) | |
| ≥5 | 61 (6.0) | 39 (5.6) | 22 (7.0) | |
| Old family member (>70y) | 0.061 | |||
| No | 278 (27.5) | 199 (28.5) | 72 (22.9) | |
| Yes, not living together | 544 (53.8) | 381 (54.7) | 163 (51.9) | |
| Yes, living together | 189 (18.7) | 117 (16.8) | 79 (25.2) | |
| Comorbidities | <0.001 | |||
| No | 724 (71.6) | 476 (68.3) | 248 (79.0) | |
| One or more | 287 (28.4) | 221 (31.7) | 66 (21.0) | |
| Past vaccination refusal | <0.001 | |||
| No | 853 (84.4) | 644 (92.4) | 209 (66.6) | |
| Yes | 158 (15.6) | 53 (7.6) | 105 (33.4) | |
| COVID-19 diagnosis | 0.604 | |||
| No | 918 (90.8) | 637 (91.4) | 281 (89.5) | |
| Yes | 58 (5.7) | 38 (5.4) | 20 (6.4) | |
| Not sure | 35 (3.5) | 22 (3.2) | 13 (4.1) | |
| Income reduction due to pandemic | 0.041 | |||
| No | 716 (70.8) | 508 (72.9) | 208 (66.2) | |
| Yes because of quarantine | 59 (5.8) | 42 (6.0) | 17 (5.4) | |
| Yes because of containment measures | 236 (23.3) | 147 (21.1) | 89 (28.3) | |
| Perceived risk of infection | <0.001 | |||
| High risk | 345 (34.1) | 267 (38.3) | 78 (24.8) | |
| Medium risk | 479 (47.4) | 333 (47.8) | 146 (46.5) | |
| Low risk | 187 (18.5) | 97 (13.9) | 90 (28.7) |
| Multivariable Model | |||
|---|---|---|---|
| OR | 95% CI | p-Value | |
| Age (years) | 1 | - | <0.001 |
| ≥55 (Reference category) | 1.58 | 1.05–2.38 | |
| 45–54 | 2.31 | 1.51–3.54 | |
| 35–44 | 1.19 | 0.70–2.00 | |
| 18–34 | |||
| Female | 1.39 | 1.02–1.89 | 0.038 |
| High school or lower degree | 1.52 | 1.10–2.11 | 0.011 |
| Family income | 1 | - | 0.044 |
| Higher than average (Reference catetgory) | 1.58 | 0.90–2.76 | |
| On average | 2.04 | 1.13–3.67 | |
| Lower than average | |||
| Absence of comorbidities | 1.95 | 1.36–2.80 | <0.001 |
| Past vaccination refusal | 7.52 | 5.02–11.3 | <0.001 |
| Risk perception | 1 | - | <0.001 |
| High risk (Reference category) | 1.47 | 1.04–2.08 | |
| Medium risk | 3.74 | 2.43–5.73 | |
| Low risk | |||
| Reasons for Past Vaccine Refusal | Overall (N = 158) | Confident (N = 53) | Hesitant (N = 105) | |
|---|---|---|---|---|
| N (%) | N (%) | N (%) | p-Value | |
| I did not think it was needed | 59 (37.3) | 25 (47.2) | 34 (32.4) | 0.070 |
| I did not have enough information on the vaccine | 37 (23.4) | 4 (7.6) | 33 (31.4) | 0.001 |
| I did not think the vaccine was effective | 22 (13.9) | 6 (11.3) | 16 (15.2) | 0.502 |
| I did not think the vaccine was safe | 31 (19.6) | 4 (7.6) | 27 (25.7) | 0.007 |
| I was worried about side effects | 56 (35.4) | 15 (28.3) | 41 (39.1) | 0.182 |
| I had a bad experience with a previous vaccination | 22 (13.9) | 6 (11.3) | 16 (15.2) | 0.502 |
| Logistical issues | 14 (8.9) | 2 (3.8) | 12 (11.4) | 0.110 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Reno, C.; Maietti, E.; Fantini, M.P.; Savoia, E.; Manzoli, L.; Montalti, M.; Gori, D. Enhancing COVID-19 Vaccines Acceptance: Results from a Survey on Vaccine Hesitancy in Northern Italy. Vaccines 2021, 9, 378. https://doi.org/10.3390/vaccines9040378
Reno C, Maietti E, Fantini MP, Savoia E, Manzoli L, Montalti M, Gori D. Enhancing COVID-19 Vaccines Acceptance: Results from a Survey on Vaccine Hesitancy in Northern Italy. Vaccines. 2021; 9(4):378. https://doi.org/10.3390/vaccines9040378
Chicago/Turabian StyleReno, Chiara, Elisa Maietti, Maria Pia Fantini, Elena Savoia, Lamberto Manzoli, Marco Montalti, and Davide Gori. 2021. "Enhancing COVID-19 Vaccines Acceptance: Results from a Survey on Vaccine Hesitancy in Northern Italy" Vaccines 9, no. 4: 378. https://doi.org/10.3390/vaccines9040378
APA StyleReno, C., Maietti, E., Fantini, M. P., Savoia, E., Manzoli, L., Montalti, M., & Gori, D. (2021). Enhancing COVID-19 Vaccines Acceptance: Results from a Survey on Vaccine Hesitancy in Northern Italy. Vaccines, 9(4), 378. https://doi.org/10.3390/vaccines9040378









