A Preliminary Assessment of Compassion Fatigue in Chimpanzee Caregivers
Abstract
Simple Summary
Abstract
1. Introduction
2. Materials and Methods
3. Results
4. Discussion
4.1. Comparison with Other Occupations
4.1.1. Compassion Satisfaction
4.1.2. Burnout
4.1.3. Secondary Traumatic Stress
4.1.4. The Interaction of Subscales
4.2. Years of Experience
4.3. Compassion Fatigue Impacts on Quality of Care
4.4. Trauma
4.5. Processes to Mitigate Compassion Fatigue
4.6. Future Directions
5. Conclusions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Appendix A
References
- Stamm, B.H. The Concise ProQOL Manual, 2nd ed.; ProQOL.org: Pocatello, ID, USA, 2010. [Google Scholar]
- Potter, P.; Deshields, T.; Divanbeigi, J.; Berger, J.; Cipriano, D.; Norris, L. Compassion fatigue and burnout: Prevalence among oncology nurses. Clin. J Oncol. Nurs. 2010, 14, E56–E62. [Google Scholar] [CrossRef] [PubMed]
- Blough, J.A. To Save a Starfish; A Compassion-Fatigue Workbook for the Animal-Welfare Warrior; Deepwater Books: New Boston, MI, USA, 2016. [Google Scholar]
- Joinson, C. Coping with compassion fatigue. Nursing 1992, 22, 116–120. [Google Scholar]
- Koenig, A.; Rodger, S.; Specht, J. Educator burnout and compassion fatigue: A pilot study. Can. J. Sch. Psych. 2018, 33, 259–278. [Google Scholar] [CrossRef]
- Bride, B.E.; Figley, C.R. The fatigue of compassionate social workers: An introduction to the special issue on compassion fatigue. Clin. Soc. Work J. 2007, 35, 151–153. [Google Scholar] [CrossRef]
- Franza, F.; Del Buono, G.; Pellegrino, F. Psychiatric caregiver stress: Clinical implications of compassion fatigue. Psychiatr. Danub. 2015, 27 (Suppl. S1), S321–S327. [Google Scholar]
- Xie, W.; Chen, L.; Feng, F.; Okoli, C.T.; Tang, P.; Zeng, L.; Jin, M.; Zhang, Y.; Wang, J. The prevalence of compassion satisfaction and compassion fatigue among nurses: A systematic review and meta-analysis. Int. J. Nurs. Std. 2021, 120, 103973. [Google Scholar] [CrossRef] [PubMed]
- Hooper, C.; Craig, J.; Janvrin, D.R.; Wetsel, M.A.; Reimels, E. Compassion satisfaction, burnout and compassion fatigue among emergency nurses compared with nurses in other selected inpatient specialties. J. Emerg. Nurs. 2010, 36, 420–427. [Google Scholar] [CrossRef] [PubMed]
- Hill, E.M.; LaLonde, C.M.; Reese, L.A. Compassion fatigue in animal care workers. Traumatology 2019, 26, 96–108. [Google Scholar] [CrossRef]
- Rank, M.G.; Zaparanick, T.L.; Gentry, J.E. Nonhuman-animal care compassion fatigue. Best Pract. Ment. Health 2009, 5, 40–61. [Google Scholar]
- Scotney, R.L.; McLaughlin, D.; Keates, H.L. An investigation of the prevalence of compassion fatigue, compassion satisfaction and burnout in those working in animal-related occupations using the Professional Quality of Life (ProQoL) Scale. Vet. Nurse 2019, 10, 276–284. [Google Scholar] [CrossRef]
- Rudolph, J.M.; Stamm, B.H.; Stamm, H.E. Compassion fatigue: A concern for mental health policy, providers, & administration. In Proceedings of the International Society for Traumatic Stress Studies, Montreal, QC, Canada, 6–10 November 1997. [Google Scholar]
- Sorenson, C.; Bolick, B.; Wright, K.; Hamilton, R. Understanding compassion fatigue in healthcare providers: A review of current literature. J. Nurs. Sch. 2016, 48, 456–465. [Google Scholar] [CrossRef] [PubMed]
- Vahey, D.C.; Aiken, L.H.; Sloane, D.M.; Clarke, S.P.; Vargas, D. Nurse burnout and patient satisfaction. Med. Care 2004, 24, II57–II66. [Google Scholar] [CrossRef] [PubMed]
- Leiter, M.; Harvie, P.; Frizzell, C. The correspondence of patient satisfaction and nurse burnout. Soc. Sci. Med. 1998, 47, 1611–1617. [Google Scholar] [CrossRef] [PubMed]
- Zajac, L.M.; Moran, K.J.; Groh, C.J. Confronting compassion fatigue: Assessment and intervention in inpatient oncology. Clin. J. Oncol. Nurs. 2017, 21, 446–453. [Google Scholar]
- Figley, C.R.; Roop, R.G. Compassion Fatigue in the Animal-Care Community; Humane Society Press: Washington, DC, USA, 2006. [Google Scholar]
- Rohlf, V.I.; Scotney, R.; Monaghan, H.; Bennett, P. Predictors of professional quality of life in veterinary professionals. J. Vet. Med. Ed. 2022, 49, 372–381. [Google Scholar] [CrossRef]
- Rantala, M.; Gabriel, K.I.; Lipton, J.; Mulcahy, J.B. Compassion fatigue and satisfaction within sanctuary-based primate husbandry. Soc. Anim. 2022. (Under review). [Google Scholar]
- Thurston, S.E.; Chan, G.; Burlingame, L.A.; Jones, J.A.; Lester, P.A.; Martin, T.L. Compassion fatigue in laboratory animal personnel during the COVID-19 pandemic. J. Am. Assoc. Lab. Anim. Sci. 2021, 60, 646–654. [Google Scholar] [CrossRef]
- Monaghan, H.; Rohlf, V.; Scotney, R.; Bennett, P. Compassion fatigue in people who care for animals: An investigation of risk and protective factors. Traumatology 2020. [Google Scholar] [CrossRef]
- LaFollette, M.R.; Riley, M.C.; Cloutier, S.; Brady, C.M.; O’Haire, M.E.; Gaskill, B.N. Laboratory animal welfare meets human welfare: A cross-sectional study of professional quality of life, including compassion fatigue in laboratory animal personnel. Front. Vet. Sci. 2020, 7, 114. [Google Scholar] [CrossRef]
- Schlanser, T.V.; Rabinowitz, P.M.; Thompson-Iritani, S. Compassion fatigue and Satisfaction in US Army laboratory animal medicine personnel. J. Am. Assoc. Lab. Anim. Sci. 2021, 60, 422–430. [Google Scholar] [CrossRef]
- ChimpCARE. Available online: https://chimpcare.org/ (accessed on 14 June 2022).
- Hirata, S.; Morimura, N.; Watanuki, K.; Ross, S.R. The establishment of sanctuaries for former laboratory chimpanzees: Challenges, successes, and cross-cultural context. In Chimpanzees in Context; Hopper, L.M., Ross, S.R., Eds.; University of Chicago Press: Chicago, IL, USA, 2020; pp. 208–230. [Google Scholar]
- Bride, B.E.; Radey, M.; Figley, C.R. Measuring compassion fatigue. Clin. Soc. Work J. 2007, 35, 155–163. [Google Scholar] [CrossRef]
- Tremoleda, J.L.; Kerton, A. Creating space to build emotional resilience in the animal research community. Lab Anim. 2020, 49, 275–277. [Google Scholar] [CrossRef] [PubMed]
- Cavanagh, N.; Cockett, G.; Heinrich, C.; Doig, L.; Fiest, K.; Guichon, J.R.; Page, S.; Mitchell, I.; Doig, C.J. Compassion fatigue in healthcare providers: A systematic review and meta-analysis. Nurs. Ethics 2020, 27, 639–665. [Google Scholar] [CrossRef] [PubMed]
- Bowens, A.N.; Amamoo, M.A.; Blake, D.D.; Clark, B. Assessment of professional quality of life in the Alabama physical therapy workforce. Phys. Ther. 2021, 101, pzab089. [Google Scholar] [CrossRef] [PubMed]
- Kim, S. Compassion fatigue in liver and kidney transplant nurse coordinators: A descriptive research study. Prog. Transpl. 2013, 23, 329–335. [Google Scholar] [CrossRef]
- Hinderer, K.A.; VonRueden, K.T.; Friedmann, E.; McQuillan, K.A.; Gilmore, R.; Kramer, B.; Murray, M. Burnout, compassion fatigue, compassion satisfaction, and secondary traumatic stress in trauma nurses. J. Trauma. Nurs. 2014, 21, 160–169. [Google Scholar] [CrossRef]
- Bellolio, M.F.; Cabrera, D.; Sadosty, A.T.; Hess, E.P.; Campbell, R.L.; Lohse, C.M.; Sunga, K.L. Compassion fatigue is similar in emergency medicine residents compared to other medical and surgical specialties. West J. Emerg. Med. 2014, 15, 629–635. [Google Scholar]
- Klein, C.J.; Riggenbach-Hays, J.J.; Sollenberger, L.M.; Harney, D.M.; McGarvey, J.S. Quality of life and compassion satisfaction in clinicians: A pilot intervention study for reducing compassion fatigue. Am. J. Hosp. Palliat. Med. 2017, 35, 882–888. [Google Scholar] [CrossRef]
- Goodall, J. The Chimpanzees of Gombe; Belknap Press of Harvard University: Cambridge, MA, USA, 1986. [Google Scholar]
- Bartram, D.J.; Baldwin, D.S. Veterinary surgeons and suicide: A structured review of possible influences on increased risk. Vet. Rec. 2010, 166, 388–397. [Google Scholar] [CrossRef] [PubMed]
- Wu, D.; Gross, B.; Rittenhouse, K.; Harnish, C.; Mooney, C.; Rogers, F.B. A preliminary analysis of compassion fatigue in a surgeon population: Are female surgeons at heightened risk? Am. Surg. 2017, 83, 1302–1307. [Google Scholar] [CrossRef]
- Austin, C.L.; Saylor, R.; Finley, P.J. Moral distress in physicians and nurses: Impact on professional quality of life and turnover. Psychol. Trauma. 2016, 9, 399–406. [Google Scholar] [CrossRef] [PubMed]
- Murray, J.; Bauer, C.; Vilminot, N.; Turner, P.V. Strengthening workplace well-being in research animal facilities. Front. Vet. Sci. 2020, 7, 573106. [Google Scholar] [CrossRef] [PubMed]
- Ferrara, F.; Hiebl, B.; Kunzmann, P.; Hutter, F.; Afkham, F.; LaFollette, M.; Gruber, C. Culture of care in animal research–Expanding the 3Rs to include people. Lab. Anim. 2022, 56, 511–518. [Google Scholar] [CrossRef] [PubMed]
- Fluery, E. Personal Communication; North American Primate Sanctuary Alliance: Los Angeles, CA, USA, 2022. [Google Scholar]
- Wei, H.; Wei, T.; Brown, K.J.; Buck, S.H.; Mill, M.R. Parents’ perception of caring characteristics of physicians and nurses. Int. J. Hum. Caring 2018, 22, 49–55. [Google Scholar] [CrossRef]
- Lyn, H.; Russell, J.L.; Hopkins, W.D. The impact of environment on the comprehension of declarative communication in apes. Psychol. Sci. 2010, 21, 360–365. [Google Scholar] [CrossRef]
- Beran, M.J.; Heimbauer, L.A. A longitudinal assessment of vocabulary retention in symbol-competent chimpanzees (Pan troglodytes). PLoS ONE 2015, 10, e0118408. [Google Scholar] [CrossRef] [PubMed]
- Ross, S.R. Captive chimpanzees. In The Ethics of Captivity; Gruen, L., Ed.; Oxford University Press: New York, NY, USA, 2014; pp. 57–76. [Google Scholar]
- Fultz, A. A guide for modern sanctuaries with examples from a captive chimpanzee sanctuary. Anim. Stud. J. 2017, 6, 9–29. [Google Scholar]
- Kurtycz, L.M.; Wagner, K.E.; Ross, S.R. Outdoor access affects great ape behaviour. J. App. Anim. Welf. Sci. 2014, 17, 185–197. [Google Scholar] [CrossRef]
- Perry, B. Why exemplary oncology nurses seem to avoid compassion fatigue. Can. Onclo. Nurs. J. 2008, 18, 87–92. [Google Scholar] [CrossRef]
- Funkhouser, J.A.; Mayhew, J.A.; Mulcahy, J.B. Social network and dominance hierarchy analyses at Chimpanzee Sanctuary Northwest. PLoS ONE 2018, 13, e0191898. [Google Scholar] [CrossRef]
- Malone, N.; Vaughan, L.; Fuentes, A. The role of human caregivers in the post-conflict interactions of captive chimpanzees (Pan troglodytes). Lab. Primate Newsl. 2000, 39, 1–3. [Google Scholar]
- Jensvold, M.L. Relationships between caregivers and chimpanzee sanctuary residents. In Chimpanzee Behavior: Recent Understandings from Captivity and the Forest; Jensvold, M.L., Ed.; Nova Science Publisher: New York, NY, USA, 2019; pp. 175–198. [Google Scholar]
- Jensvold, M.L. Chimpanzee (Pan troglodytes) responses to caregiver use of chimpanzee behaviors. Zoo Biol. 2008, 27, 345–359. [Google Scholar] [CrossRef] [PubMed]
- Jensvold, M.L.; Buckner, J.; Stadtner, G. Caregiver-chimpanzee interactions with species-specific behaviors. Interact. Stud. 2010, 11, 396–409. [Google Scholar] [CrossRef]
- Hemsworth, P.H.; Barnett, J.L.; Hansen, C. The influence of inconsistent handling by humans on the behaviour, growth and corticosteroids of young pigs. Appl. Anim. Behav. Sci. 1987, 17, 245–252. [Google Scholar] [CrossRef]
- Seabrook, M.F. The psychological interaction between the stockman and his animals and its influence on performance of pigs and dairy cows. Vet. Rec. 1984, 115, 84–87. [Google Scholar] [CrossRef]
- Waitt, C.; Buchanan-Smith, H.M.; Morris, K. The effects of caretaker-primate relationships on primates in the laboratory. J. Appl. Anim. Welf. Sci. 2002, 5, 309–319. [Google Scholar] [CrossRef]
- Baker, K.C. Benefits of positive human interaction for socially housed chimpanzees. Anim. Welf. 2004, 13, 239–245. [Google Scholar]
- Bloomsmith, M.A.; Baker, K.; Ross, S.; Lambeth, S. Comparing animal training to non-training human interaction as environmental enrichment for chimpanzees. Am. J. Primatol. 1999, 49, 35–36. [Google Scholar]
- Serpell, J.A. Factors influencing human attitudes to animals and their welfare. Anim. Welf. 2004, 13, 145–151. [Google Scholar]
- Kleber, R.J. Trauma and public mental health: A focused review. Front. Psychiatry 2019, 10, 451–457. [Google Scholar] [CrossRef]
- Ferdowsian, H.; Merskin, D. Parallels in sources of trauma, pain, distress, and suffering in humans and nonhuman animals. J. Trauma Dissoc. 2012, 13, 448–468. [Google Scholar] [CrossRef] [PubMed]
- Bradshaw, G.A.; Capaldo, T.; Linder, L.; Grow, G. Building an inner sanctuary: Complex PTSD in chimpanzees. Trauma Dissoc. 2008, 9, 9–34. [Google Scholar] [CrossRef] [PubMed]
- Bloomsmith, M.A.; Clay, A.W.; Lambeth, S.P.; Lutz, C.K.; Breaux, S.D.; Lammey, M.L.; Franklin, A.N.; Neu, K.A.; Perlman, J.E.; Reamer, L.A.; et al. Survey of behavioral indices of welfare in research chimpanzees (Pan troglodytes) in the United States. J. Am. Assoc. Lab. Anim. Sci. 2019, 58, 160–177. [Google Scholar] [CrossRef]
- Bloomsmith, M.A.; Clay, A.W.; Ross, S.R.; Lambeth, S.P.; Lutz, C.K.; Breaux, S.D.; Pietsch, R.; Fultz, A.; Lammey, M.L.; Jacobson, S.L.; et al. Chimpanzees in US zoos, sanctuaries, and research facilities: A survey-based comparison of atypical behaviors. In Chimpanzees in Context; Hopper, L.M., Ross, S.R., Eds.; University of Chicago Press: Chicago, IL, USA, 2020; pp. 481–508. [Google Scholar]
- Serafini, G.; Canepa, G.; Adavastro, G.; Nebbia, J.; Belvederi Murri, M.; Erbuto, D.; Pocai, B.; Fiorillo, A.; Pompili, M.; Flouri, E.; et al. The relationship between childhood maltreatment and non-suicidal self-injury: A systematic review. Front. Psychiatry 2017, 8, 149. [Google Scholar] [CrossRef]
- Brüne, M.; Brüne-Cohrs, U.; McGrew, W.C.; Preuschoft, S. Psychopathology in great apes: Concepts, treatment options and possible homologies to human psychiatric disorders. Neurosci. Biobehav. Rev. 2006, 30, 1246–1259. [Google Scholar] [CrossRef] [PubMed]
- Lopresti-Goodman, S.M.; Bezner, J.; Ritter, C. Psychological distress in chimpanzees rescued from laboratories. J. Trauma Dissoc. 2015, 16, 349–366. [Google Scholar] [CrossRef] [PubMed]
- Rohlf, V.I. Interventions for occupational stress and compassion fatigue in animal care professionals—A systematic review. Traumatology 2018, 24, 186–192. [Google Scholar] [CrossRef]
- ProQOL Professional Quality of Life. Available online: https://proqol.org/self-care-tools-1 (accessed on 17 July 2022).
- The Trauma Stewardship Institute. Available online: https://traumastewardship.com/purchase/ (accessed on 17 July 2022).
- The Compassion Fatigue Awareness Project. Available online: https://compassionfatigue.org/index.html (accessed on 17 July 2022).
- How to Manage Compassion Fatigue in Caregiving|Patricia Smith|TEDxSanJuanIsland. Available online: https://youtu.be/7keppA8Xras (accessed on 17 July 2022).
- Jarrad, R.A.; Hammad, S. Oncology nurses’ compassion fatigue, burnout and compassion satisfaction. Annls. Gen. Psychiatry 2020, 19, 1–8. [Google Scholar] [CrossRef]
- Emmons, R.A.; McCullough, M.E. Counting blessings versus burdens: An experimental investigation of gratitude and subjective well-being in daily life. J. Personal. Soc. Psychol. 2003, 84, 377. [Google Scholar] [CrossRef]
- 13 Most Popular Gratuity Exercises. Available online: https://positivepsychology.com/gratitude-exercises/ (accessed on 17 July 2022).
- Lomas, T.; Medina, J.C.; Ivtzan, I.; Rupprecht, S.; Eiroa-Orosa, F.J. A systematic review of the impact of mindfulness on the well-being of healthcare professionals. J. Clin. Psychol. 2018, 74, 319–355. [Google Scholar] [CrossRef]
- Kabat-Zinn, J. Wherever You Go, There You Are: Mindfulness Meditation in Everyday Life; Hachette Books: Boston, MA, USA, 2005. [Google Scholar]
- Zaccaro, A.; Piarulli, A.; Laurino, M.; Garbella, E.; Menicucci, D.; Neri, B.; Gemignani, A. How breath-control can change your life: A systematic review on psycho-physiological correlates of slow breathing. Front. Hum. Neurosci. 2018, 12, 353. [Google Scholar] [CrossRef] [PubMed]
- Jerath, R.; Barnes, V.A. Augmentation of mind-body therapy and role of deep slow breathing. J. Complement. Integr. Med. 2009, 6, 1–7. [Google Scholar] [CrossRef]
- Jerath, R.; Crawford, M.W.; Barnes, V.A.; Harden, K. Self-regulation of breathing as a primary treatment for anxiety. Appl. Psychophysiol. Biofeedback 2015, 40, 107–115. [Google Scholar] [CrossRef] [PubMed]
- Bach, D.; Groesbeck, G.; Stapleton, P.; Sims, R.; Blickheuser, K.; Church, D. Clinical EFT (Emotional Freedom Techniques) improves multiple physiological markers of health. J. Evid. Based Integr. Med. 2019, 24, 2515690X18823691. [Google Scholar] [CrossRef]
- Ross, A.; Thomas, S. The health benefits of yoga and exercise: A review of comparison studies. J. Alt. Complement. Med. 2010, 16, 3–12. [Google Scholar] [CrossRef]
- Pascoe, M.C.; de Manincor, M.J.; Hallgren, M.; Baldwin, P.A.; Tseberja, J.; Parker, A.G. Psychobiological mechanisms underlying the mental health benefits of yoga-based interventions: A narrative review. Mindfulness 2021, 12, 2877–2889. [Google Scholar] [CrossRef]
- Yilmaz, G.; Üstün, B. Professional quality of life in nurses: Compassion satisfaction and compassion fatigue. J. Psychol. Nurs. 2018, 9, 205–211. [Google Scholar] [CrossRef]
- Zwack, J.; Schweitzer, J. If every fifth physician is affected by burnout, what about the other four? Resilience strategies of experienced physicians. Acad. Med. 2013, 88, 382–389. [Google Scholar] [CrossRef]
- Dowling, T. Compassion does not fatigue! Can. Vet. J. 2018, 59, 749. [Google Scholar]
- Singer, T.; Seymour, B.; O’Doherty, J.; Kaube, H.; Dolan, R.J.; Frith, C.D. Empathy for pain involves the affective but not sensory components of pain. Science 2004, 303, 1157–1162. [Google Scholar] [CrossRef]
- de Vignemont, F.; Singer, T. The empathic brain: How, when and why? Trends Cog. Sci. 2006, 10, 435–441. [Google Scholar] [CrossRef] [PubMed]
- Bloom, P. Against Empathy: The Case for Rational Compassion; Random House: New York, NY, USA, 2017. [Google Scholar]
- Mascaro, J.S.; Rilling, J.K.; Tenzin Negi, L.; Raison, C.L. Compassion meditation enhances empathic accuracy and related neural activity. Soc. Cogn. Aff. Neurosci. 2013, 8, 48–55. [Google Scholar] [CrossRef] [PubMed]
- Shonin, E.; Van Gordon, W.; Compare, A.; Zangeneh, M.; Griffiths, M.D. Buddhist-derived loving-kindness and compassion meditation for the treatment of psychopathology: A systematic review. Mindfulness 2015, 6, 1161–1180. [Google Scholar] [CrossRef]
- Weng, H.Y.; Fox, A.S.; Shackman, A.J.; Stodola, D.E.; Caldwell, J.Z.K.; Olson, M.C.; Roges, G.M.; Davidson, R.J. Compassion training alters altruism and neural responses to suffering. Psychol. Sci. 2013, 24, 1171–1180. [Google Scholar] [CrossRef] [PubMed]
- Leiberg, S.; Klimecki, O.; Singer, T. Short-term compassion training increases prosocial behavior in a newly developed prosocial game. PLoS ONE 2011, 6, e17798. [Google Scholar] [CrossRef] [PubMed]
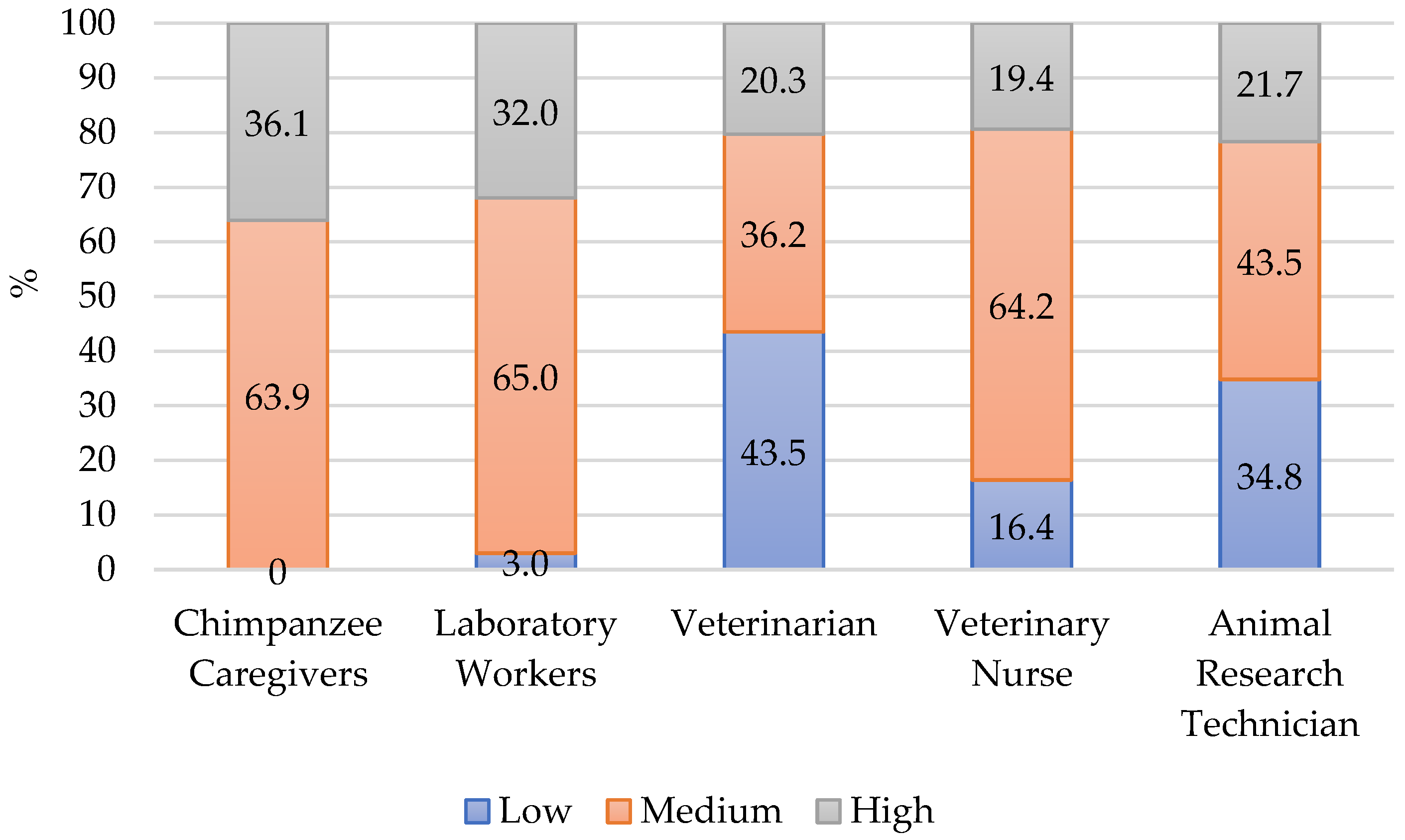
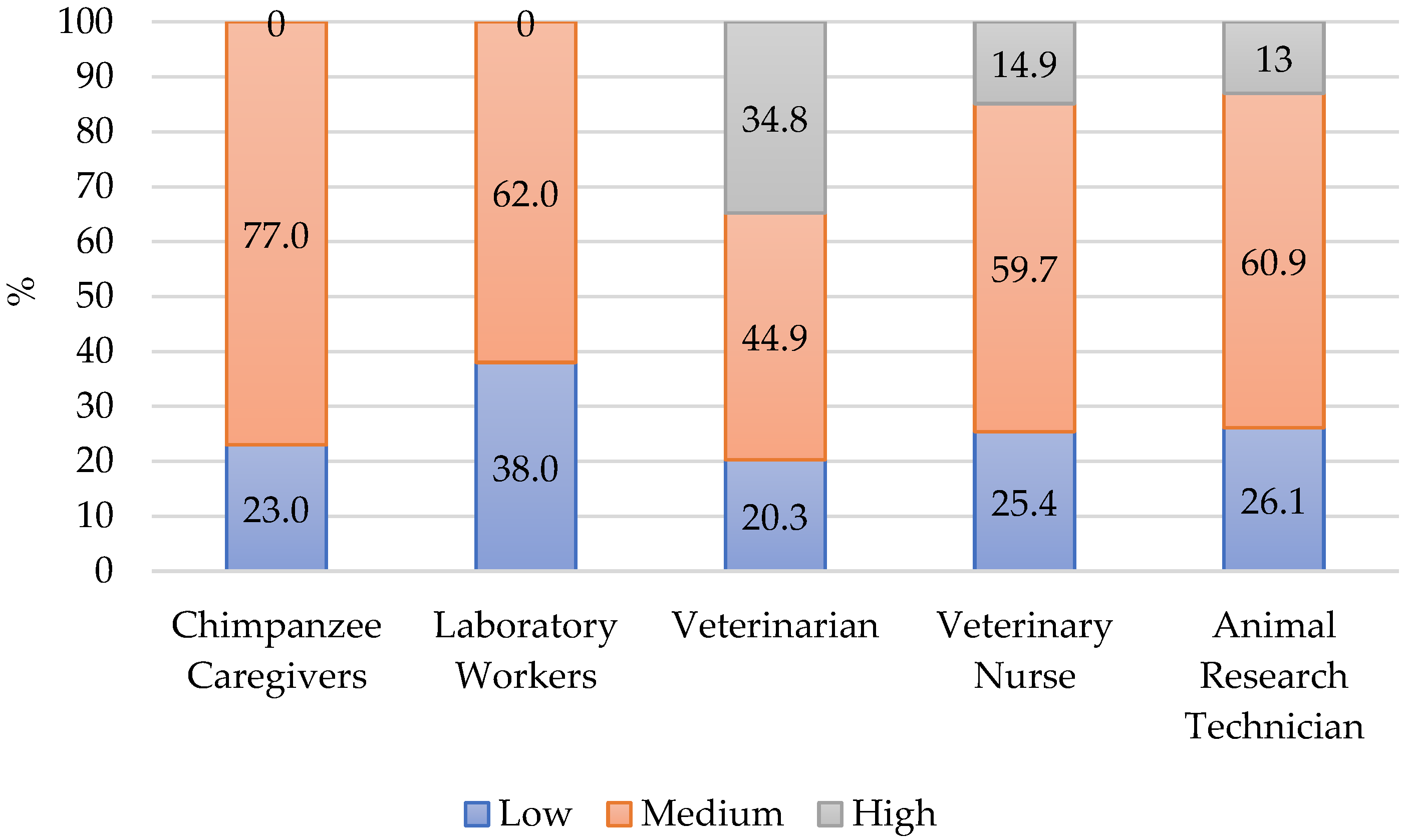
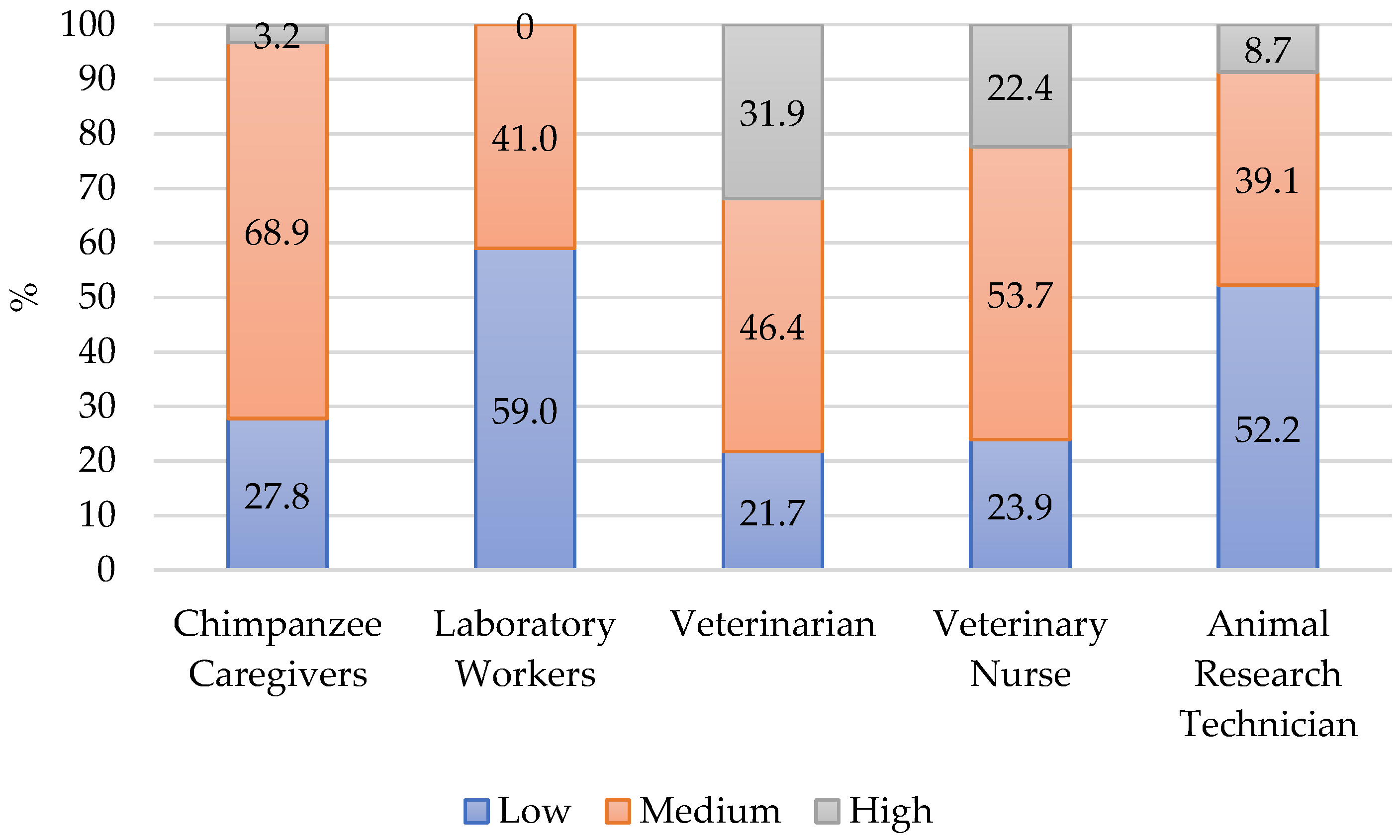
| CS | BO | STS | |
|---|---|---|---|
| Range raw | 25–50 | 10–40 | 15–43 |
| Mean raw | 39.26 | 27.46 | 27.56 |
| SD raw | 6.50 | 6.76 | 6.81 |
| Range t-scores | 27.88–66.66 | 22.92–69.45 | 31.27–73.02 |
| Mean t-score | 50.0 | 50.0 | 50.0 |
| SD t score | 10.08 | 10.49 | 10.15 |
| CS | BO | STS | |
|---|---|---|---|
| n (%) | n (%) | n (%) | |
| Low | 0 | 14 (23.0) | 17 (27.9) |
| Medium | 39 (63.9) | 47 (77.0) | 42 (68.9) |
| High | 22 (36.1) | 0 | 2 (3.3) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the author. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Jensvold, M.L. A Preliminary Assessment of Compassion Fatigue in Chimpanzee Caregivers. Animals 2022, 12, 3506. https://doi.org/10.3390/ani12243506
Jensvold ML. A Preliminary Assessment of Compassion Fatigue in Chimpanzee Caregivers. Animals. 2022; 12(24):3506. https://doi.org/10.3390/ani12243506
Chicago/Turabian StyleJensvold, Mary Lee. 2022. "A Preliminary Assessment of Compassion Fatigue in Chimpanzee Caregivers" Animals 12, no. 24: 3506. https://doi.org/10.3390/ani12243506
APA StyleJensvold, M. L. (2022). A Preliminary Assessment of Compassion Fatigue in Chimpanzee Caregivers. Animals, 12(24), 3506. https://doi.org/10.3390/ani12243506




