Smartphone-Based Maternal Education for the Complementary Feeding of Undernourished Children Under 3 Years of Age in Food-Secure Communities: Randomised Controlled Trial in Urmia, Iran
Abstract
1. Introduction
2. Materials and Methods
3. Results
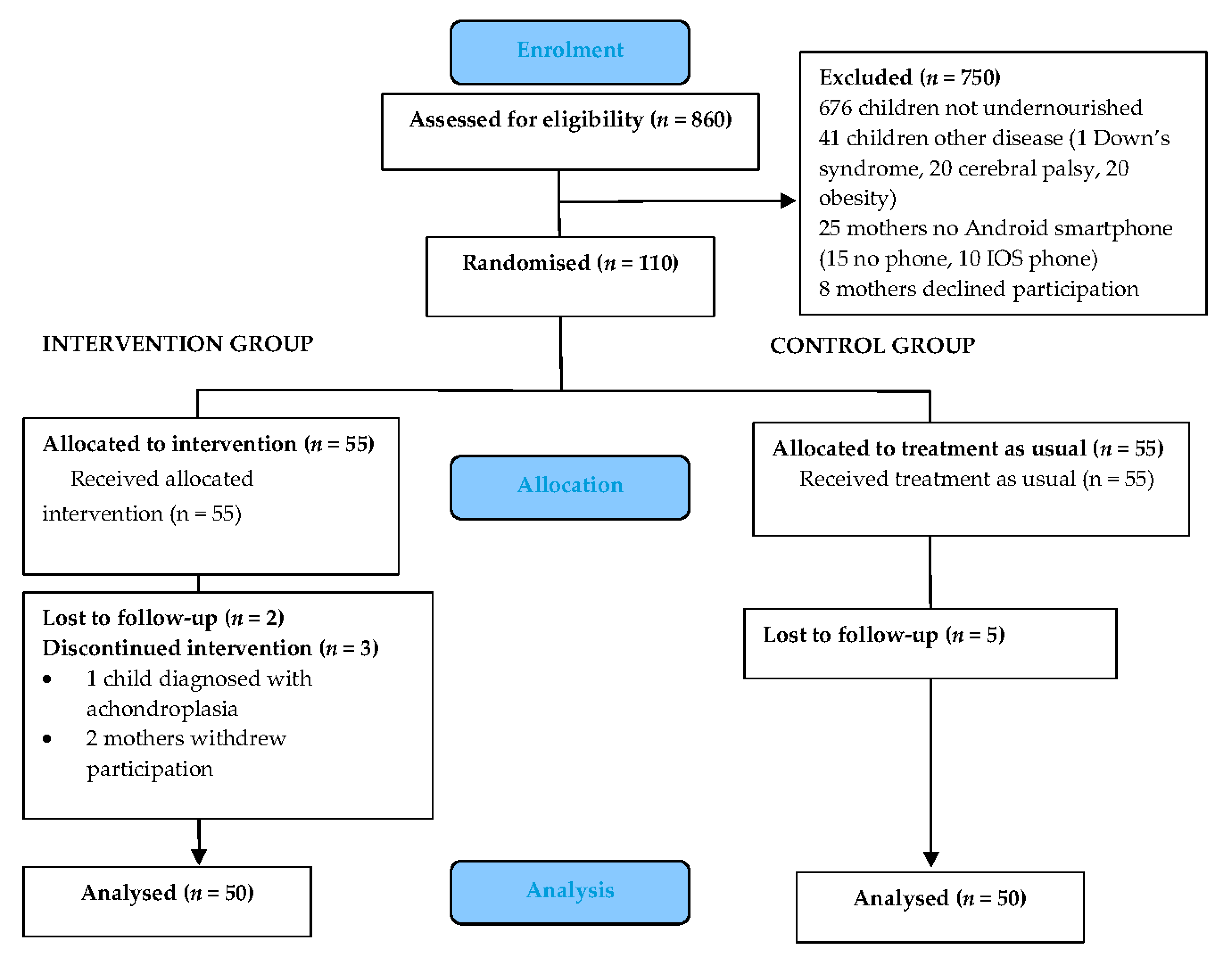
3.1. Participant Flow
3.2. Mothers’ Nutritional Literacy
3.3. Child Undernourishment
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
Appendix A
References
- The MALEDNI. The MAL-ED Study: A Multinational and Multidisciplinary Approach to Understand the Relationship Between Enteric Pathogens, Malnutrition, Gut Physiology, Physical Growth, Cognitive Development, and Immune Responses in Infants and Children Up to 2 Years of Age in Resource-Poor Environments. Clin. Infect. Dis. 2014, 59, S193–S206. [Google Scholar]
- World Health Organization. Guiding Principles for Feeding Non-Breastfed Children 6–24 Months of Age; WHO: Geneva, Switzerland, 2005. [Google Scholar]
- World Health Organization. Indicators for the Global Monitoring Framework on Maternal, Infant and Young Child Nutrition; World Health Organization: Geneva, Switzerland, 2014; Available online: http://www.who.int/nutrition/topics/indicators_monitoringframework_miycn_background.pdf (accessed on 7 June 2019).
- Dewey, K.G.; Begum, K. Long-term consequences of stunting in early life. Matern. Child Nutr. 2011, 7, 5–18. [Google Scholar] [CrossRef] [PubMed]
- Simons, D.; De Bourdeaudhuij, I.; Clarys, P.; De Cocker, K.; Vandelanotte, C.; Deforche, B. A smartphone app to promote an active lifestyle in lower-educated working young adults: Development, usability, acceptability, and feasibility study. JMIR Mhealth. Uhealth. 2018, 6, 2. [Google Scholar] [CrossRef]
- Black, R.E.; Victora, C.G.; Walker, S.P.; Bhutta, Z.A.; Christian, P.; De Onis, M.; Ezzati, M.; Grantham-McGregor, S.; ScD, J.K.; Martorell, R.; et al. Maternal and child undernutrition and overweight in low-income and middle-income countries. Lancet 2013, 382, 427–451. [Google Scholar] [CrossRef]
- Institute IFPR. 2015 Annual Report; International Food Policy Research Institute (IFPRI): Washington, DC, USA, 2006; Available online: http://ebrary.ifpri.org/cdm/ref/collection/p15738coll2/id/130442 (accessed on 26 July 2019).
- Days, T. Reaching the Global Target to Reduce Stunting: How Much Will It Cost and How Can We Pay for It. Washington, DC. 2015. Available online: http://pubdocs.worldbank.org/en/460861439997767818/Stunting-Costing-and-Financing-Overview-Brief.pdf (accessed on 22 August 2018).
- Hien, N.N.; Kam, S. Nutritional status and the characteristics related to malnutrition in children under five years of age in Nghean, Vietnam. J. Prev. Med. Public Health 2008, 41, 232–240. [Google Scholar] [CrossRef] [PubMed]
- Saito, K.; Korzenik, J.; Jekel, J.F.; Bhattacharji, S. A case-control study of maternal knowledge of malnutrition and health-care-seeking attitudes in rural South India. Yale J. Biol. Med. 1997, 70, 149. [Google Scholar] [PubMed]
- Imdad, A.; Yakoob, M.Y.; Bhutta, Z.A. Impact of maternal education about complementary feeding and provision of complementary foods on child growth in developing countries. BMC Public Health 2011, 11, S25. [Google Scholar] [CrossRef] [PubMed]
- Bhavsar, S.; Hemant, M.; Kulkarni, R. Maternal and environmental factors affecting the nutritional status of children in Mumbai urban slum. Int. J. Sci. Res. Publ. 2012, 2, 1–9. [Google Scholar]
- Gupta, M.C.; Mehrotra, M.; Arora, S.; Saran, M. Relation of childhood malnutrition to parental education and mothers’ nutrition related KAP. Indian J. Pediatr. 1991, 58, 269–274. [Google Scholar] [CrossRef]
- Panjwani, A.; Heidkamp, R. Complementary feeding interventions have a small but significant impact on linear and ponderal growth of children in low-and middle-income countries: A systematic review and meta-analysis. J. Nutr. 2017, 147, 2169S–2178S. [Google Scholar] [CrossRef]
- Lassi, Z.S.; Das, J.K.; Zahid, G.; Imdad, A.; Bhutta, Z.A. Impact of education and provision of complementary feeding on growth and morbidity in children less than 2 years of age in developing countries: A systematic review. BMC Public Health 2013, 13, S13. [Google Scholar] [CrossRef] [PubMed]
- Dewey, K.G.; Adu-Afarwuah, S. Systematic review of the efficacy and effectiveness of complementary feeding interventions in developing countries. Matern. Child Nutr. 2008, 4, 24–85. [Google Scholar] [CrossRef] [PubMed]
- Yabancı, N.; Kısaç, I.; Karakuş, S.Ş. The effects of mother’s nutritional knowledge on attitudes and behaviors of children about nutrition. Procedia Soc. Behav. Sci. 2014, 116, 4477–4481. [Google Scholar] [CrossRef]
- Kao, C.-K.; Liebovitz, D.S.M. Consumer mobile health apps: Current state, barriers, and future directions. PMR 2017, 9, S106–S115. [Google Scholar] [CrossRef] [PubMed]
- Ormel, H.L.; van der Schoot, G.G.; Westerink, N.-D.L.; Sluiter, W.J.; Gietema, J.A.; Walenkamp, A.M. Self-monitoring physical activity with a smartphone application in cancer patients: A randomized feasibility study (SMART-trial). Support Care Cancer 2018, 26, 3915–3923. [Google Scholar] [CrossRef] [PubMed]
- Ek, A.; Alexandrou, C.; Nyström, C.D.; Direito, A.; Eriksson, U.; Hammar, U.; Henriksson, P.; Maddison, R.; Lagerros, Y.T.; Löf, M. The Smart City Active Mobile Phone Intervention (SCAMPI) study to promote physical activity through active transportation in healthy adults: A study protocol for a randomised controlled trial. BMC Public Health 2018, 18, 880. [Google Scholar] [CrossRef]
- Nadri, H.; Rahimi, B.; Timpka, T.; Sedghi, S. The top 100 articles in the medical informatics: A bibliometric analysis. J. Med. Syst. 2017, 41, 150. [Google Scholar] [CrossRef]
- Bachiri, M.; Idri, A.; Fernández-Alemán, J.L.; Toval, A. Mobile personal health records for pregnancy monitoring functionalities: Analysis and potential. Comput. Methods Programs Biomed. 2016, 134, 121–135. [Google Scholar] [CrossRef]
- Handel, M.J. mHealth (mobile health)—Using apps for health and wellness. Explore (NY) 2011, 7, 256–261. [Google Scholar] [CrossRef]
- Nyumbeka, D., Wesson, J., Eds.; Using mobile computing to support malnutrition management in South Africa. In Proceedings of the Southern African Institute for Computer Scientist and Information Technologists Annual Conference 2014 on SAICSIT 2014 Empowered by Technology 2014, Baltimore, MD, USA, 12–14 May 2014. [Google Scholar]
- Lee, W.; Chae, Y.M.; Kim, S.; Ho, S.H.; Choi, I. Evaluation of a mobile phone-based diet game for weight control. J. Telemed. Telecare 2010, 16, 270–275. [Google Scholar] [CrossRef] [PubMed]
- Nyström, C.D.; Sandin, S.; Henriksson, P.; Henriksson, H.; Trolle-Lagerros, Y.; Larsson, C.; Maddison, R.; Ortega, F.B.; Pomeroy, J.; Ruiz, J.R.; et al. Mobile-based intervention intended to stop obesity in preschool-aged children: The MINISTOP randomized controlled trial. Am. J. Clin. Nutr. 2017, 105, 1327–1335. [Google Scholar]
- Farrokh Eslamlou, H.; Oshnouei, S.; Ahmadi, N.; Babaei, F. Geographical distribution of nutrition deficiency among children under five years old in the west Azerbaijan province, Iran. Urmia. Med. J. 2013, 24, 201–209. [Google Scholar]
- Tadele, N.; Habta, F.; Akmel, D.; Deges, E. Knowledge, attitude and practice towards exclusive breastfeeding among lactating mothers in Mizan Aman town, Southwestern Ethiopia: Descriptive cross-sectional study. Int. Breastfeed. J. 2016, 11, 3. [Google Scholar] [CrossRef] [PubMed]
- Ayed, A. Knowledge, attitude and practice regarding exclusive breastfeeding among mothers attending primary health care centers in Abha city. Int. J. Med. Sci. Public Health 2014, 3, 1355–1363. [Google Scholar] [CrossRef]
- Alina, T.; Ismail, T.; Sulaiman, Z. Reliability and validity of a Malay-version questionnaire assessing knowledge of breastfeeding. Malaysian J. Med. Sci. 2010, 17, 32–39. [Google Scholar]
- Olatona, F.A.; Adenihun, J.O.; Aderibigbe, S.A.; Adeniyi, O.F. Complementary feeding knowledge, practices, and dietary diversity among mothers of under-five children in an urban community in Lagos State, Nigeria. Int. J. MCH AIDS 2017, 6, 46. [Google Scholar] [CrossRef]
- Gessese, D.; Bolka, H.; Alemu Abajobir, A.; Tegabu, D. The practice of complementary feeding and associated factors among mothers of children 6-23 months of age in Enemay district, Northwest Ethiopia. Nutr. Food Sci. 2014, 44, 230–240. [Google Scholar] [CrossRef]
- IMoH. Maternity Guidelines for Maternal and Child Health Services; Iranian Ministry of Health: Teheran, Iran, 2017. Available online: http://file.qums.ac.ir/repository/vch/family/1395/96Boklet.rar (accessed on 4 February 2019).
- Kia, A.A.; Rezapour, A.; Khosravi, A.; Abarghouei, V.A. Socioeconomic inequality in malnutrition in under-5 children in Iran: Evidence from the multiple indicator demographic and health survey, 2010. J. Prev. Med. Public Health 2017, 50, 201. [Google Scholar]
- Rahimi, B.; Nadri, H.; Afshar, H.L.; Timpka, T. A systematic review of the technology acceptance model in health informatics. Appl. Clin. Inform. 2018, 9, 604–634. [Google Scholar] [CrossRef]
- Norman, D. The Design of Everyday Things; Revised and Expanded Edition; Basic Books: New York, NY, USA, 2013. [Google Scholar]
- Glanz, K.; Rimer, B.K.; Viswanath, K. Health Behavior and Health Education: Theory, Research, and Practice; John Wiley & Sons: New York, NY, USA, 2008. [Google Scholar]
- Kamal, N.; Fels, S.; Fergusson, M. Online social networks for health behaviour change: Designing to increase socialization. Comput. Hum. Behav. 2014, 41, 444–453. [Google Scholar] [CrossRef]
- Tang, J.; Abraham, C.; Stamp, E.; Greaves, C. How can weight-loss app designers’ best engage and support users? A qualitative investigation. Br. J. Health Psychol. 2015, 20, 151–171. [Google Scholar] [CrossRef] [PubMed]
- Burrows, T.; Hutchesson, M.; Chai, L.K.; Rollo, M.; Skinner, G.; Collins, C. Nutrition interventions for prevention and management of childhood obesity: What do parents want from an eHealth program? Nutrients 2015, 7, 10469–10479. [Google Scholar] [CrossRef] [PubMed]
- Azar, K.M.; Lesser, L.I.; Laing, B.Y.; Stephens, J.; Aurora, M.S.; Burke, L.E.; Palaniappan, L.P. Mobile applications for weight management: Theory-based content analysis. Am. J. Prev. Med. 2013, 45, 583–589. [Google Scholar] [CrossRef] [PubMed]
- Direito, A.; Dale, L.P.; Shields, E.; Dobson, R.; Whittaker, R.; Maddison, R. Do physical activity and dietary smartphone applications incorporate evidence-based behaviour change techniques? BMC Public Health 2014, 14, 646. [Google Scholar] [CrossRef]
- Ammaniti, M.; Ambruzzi, A.M.; Lucarelli, L.; Cimino, S.; D’Olimpio, F. Malnutrition and dysfunctional mother-child feeding interactions: Clinical assessment and research implications. J. Am. Coll. Nutr. 2004, 23, 259–271. [Google Scholar] [CrossRef]
- Silverman, A.H.; Lukens, C.T. Systematic review of psychological interventions for pediatric feeding problems. J. Pediatr. Psychol. 2014, 39, 903–917. [Google Scholar]
- Petzoldt, J.; Wittchen, H.U.; Einsle, F.; Martini, J. Maternal anxiety versus depressive disorders: Specific relations to infants’ crying, feeding and sleeping problems. Child Care Health Dev. 2016, 42, 231–245. [Google Scholar] [CrossRef]
- Rybak, A. Organic and nonorganic feeding disorders. Ann. Nutr. Metab. 2015, 66, 16–22. [Google Scholar] [CrossRef]
- Budd, K.S.; McGraw, T.E.; Farbisz, R.; Murphy, T.B.; Hawkins, D.; Heilman, N.; Werle, M. Psychosocial concomitants of children’s feeding disorders. J. Pediatr. Psychol. 1992, 17, 81–94. [Google Scholar] [CrossRef]
- Seyyedi, N.; Rahimi, B.; Farrokh Eslamlou, H.R.; Timpka, T.; Lotfnezhad Afshar, H. Mobile phone applications to overcome malnutrition among preschoolers: A systematic review. BMC Med. Inform. Decis. Mak. 2019, 19, 83. [Google Scholar] [CrossRef]
- Ngwira, A.; Munthali, E.C.; Vwalika, K.D. Analysis on the association among stunting, wasting and underweight in Malawi: An application of a log-linear model for the three-way table. J. Public Health Afr. 2017, 8, 620. [Google Scholar] [CrossRef] [PubMed]
- Addelyan Rasi, H.; Moula, A.; Puddephatt, A.J.; Timpka, T. Empowering single mothers in Iran: Applying a problem-solving model in learning groups to develop participants’ capacity to improve their lives. Br. J. Soc. Work 2012, 43, 833–852. [Google Scholar] [CrossRef]
- McDonald, C.; Olofin, I.; Flaxman, S.; Fawzi, W.; Spiegelman, D.; Caulfield, L.E.; Black, R.E.; Ezzati, M.; Danaei, G.; Nutrition Impact Model Study. The effect of multiple anthropometric deficits on child mortality: Meta-analysis of individual data in 10 prospective studies from developing countries. Am. J. Clin. Nutr. 2013, 97, 896–901. [Google Scholar] [CrossRef] [PubMed]
| Study Group $ | |||
|---|---|---|---|
| Smartphone | Control | ||
| n = 50 | n = 50 | p Value | |
| Formal education | |||
| Elementary or high school | 30 (60) | 38 (76) | p = 0.086 |
| Academic | 20 (40) | 12 (24) | |
| Employment status | |||
| Stay-at-home parent | 43 (86) | 45 (90) | p = 0.538 |
| Employed with salary | 7 (14) | 5 (10) | |
| Residency | |||
| City | 16 (32) | 24 (48) | p = 0.102 |
| Village or suburb | 34 (68) | 26 (52) | |
| Home ownership | |||
| Yes | 15 (30) | 13 (26) | p = 0.656 |
| No | 35 (70) | 37 (74) | |
| Home size | |||
| 3 rooms or fewer | 48 (96) | 50 (100) | p = 0.495 |
| > 3 rooms | 2 (4) | 0 (0) | |
| Car ownership | |||
| Yes | 21 (42) | 17 (34) | p = 0.410 |
| No | 29 (58) | 33 (66) | |
| Study Group | |||
|---|---|---|---|
| Child Age (Months) | Smartphone | Control | Total |
| 0–6 | 4 (8) | 9 (18) | 13 (13) |
| 7–12 | 18 (36) | 12 (24) | 30 (30) |
| 13–24 | 17 (34) | 17 (34) | 34 (34) |
| 25–36 | 11 (22) | 12 (24) | 23 (23) |
| Total | 50 (100) | 50 (100) | 100 (100) |
| Mothers’ Nutritional Literacy Scores (Mean (95% CI)) | ||||||
|---|---|---|---|---|---|---|
| Baseline Score | Score Change at Follow-Up | |||||
| Smartphone Group n = 50 | TAU Group n = 50 | Smartphone Group n = 50 | TAU Group n = 50 | Between-Group Difference | p | |
| Critical knowledge | 19.94 ± 0.83 | 19.94 ± 0.71 | 5.56 ± 0.78 | −0.94 ± 0.59 | 6.50 ± 0.98 | <0.001 |
| Feeding attitudes | 68.78 ± 1.85 | 67.98 ± 2.23 | 7.52 ± 1.36 | −1.86 ± 1.02 | 9.38 ± 1.70 | <0.001 |
| Nutrition practice | 84.64 ± 2.77 | 82.40 ± 2.92 | 3.16 ± 1.02 | 1.04 ± 0.75 | 2.12 ± 1.27 | 0.001 |
| Nutritional literacy | 173.36 ± 3.83 | 170.32 ± 3.66 | 16.24 ± 1.97 | −1.76 ± 1.58 | 18.00 ± 2.53 | <0.001 |
| Children’s Undernourishment Indicator Status (Mean (95% CI)) | ||||||
|---|---|---|---|---|---|---|
| Baseline Indicator Status | Indicator Status Change at Follow-Up | |||||
| Smartphone Group n = 50 | TAU Group n = 50 | Smartphone Group n = 50 | TAU Group n = 50 | Between-Group Difference | p | |
| Wasting | −1.82 ± 0.21 | −1.80 ± 0.23 | 0.65 ± 0.16 | 0.31 ± 0.21 | 0.34 ± 0.26 | 0.011 |
| Underweight | −1.89 ± 0.18 | −1.81 ± 0.17 | 0.50 ± 0.15 | 0.15 ± 0.13 | 0.35 ± 0.20 | 0.001 |
| Stunting | −1.48 ± 0.22 | −1.37 ± 0.32 | 0.26 ± 0.15 | −0.09 ± 0.14 | 0.34 ± 0.21 | 0.002 |
| Children’s Undernourishment Caseness (n (Percent)) | |||||
|---|---|---|---|---|---|
| Baseline Caseness | Caseness Change at Follow-Up | ||||
| Smartphone Group n = 50 | TAU Group n = 50 | Smartphone Group n = 50 | TAU Group n = 50 | p | |
| Wasting | 29 (58) | 33 (66) | 26 (90) | 17 (52) | 0.001 |
| Underweight | 22 (44) | 20 (40) | 15 (68) | 4 (20) | 0.002 |
| Stunting | 17 (34) | 15 (30) | 6 (35) | 1 (7) | 0.088 * |
| Any caseness | 50 (100) | 50 (100) | 33 (66) | 19 (38) | 0.005 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Seyyedi, N.; Rahimi, B.; Eslamlou, H.R.F.; Afshar, H.L.; Spreco, A.; Timpka, T. Smartphone-Based Maternal Education for the Complementary Feeding of Undernourished Children Under 3 Years of Age in Food-Secure Communities: Randomised Controlled Trial in Urmia, Iran. Nutrients 2020, 12, 587. https://doi.org/10.3390/nu12020587
Seyyedi N, Rahimi B, Eslamlou HRF, Afshar HL, Spreco A, Timpka T. Smartphone-Based Maternal Education for the Complementary Feeding of Undernourished Children Under 3 Years of Age in Food-Secure Communities: Randomised Controlled Trial in Urmia, Iran. Nutrients. 2020; 12(2):587. https://doi.org/10.3390/nu12020587
Chicago/Turabian StyleSeyyedi, Navisa, Bahlol Rahimi, Hamid Reza Farrokh Eslamlou, Hadi Lotfnezhad Afshar, Armin Spreco, and Toomas Timpka. 2020. "Smartphone-Based Maternal Education for the Complementary Feeding of Undernourished Children Under 3 Years of Age in Food-Secure Communities: Randomised Controlled Trial in Urmia, Iran" Nutrients 12, no. 2: 587. https://doi.org/10.3390/nu12020587
APA StyleSeyyedi, N., Rahimi, B., Eslamlou, H. R. F., Afshar, H. L., Spreco, A., & Timpka, T. (2020). Smartphone-Based Maternal Education for the Complementary Feeding of Undernourished Children Under 3 Years of Age in Food-Secure Communities: Randomised Controlled Trial in Urmia, Iran. Nutrients, 12(2), 587. https://doi.org/10.3390/nu12020587







