Abstract
Human immunodeficiency virus-1 (HIV-1) persists as a global health concern, with an incidence rate of approximately 2 million, and estimated global prevalence of over 35 million. Combination antiretroviral treatment is highly effective, but HIV-1 patients that have been treated still suffer from chronic inflammation and residual viral replication. It is therefore paramount to identify therapeutically efficacious strategies to eradicate viral reservoirs and ultimately develop a cure for HIV-1. It has been long accepted that the restriction factor tripartite motif protein 5 isoform alpha (TRIM5α) restricts HIV-1 infection in a species-specific manner, with rhesus macaque TRIM5α strongly restricting HIV-1, and human TRIM5α having a minimal restriction capacity. However, several recent studies underscore human TRIM5α as a cell-dependent HIV-1 restriction factor. Here, we present an overview of the latest research on human TRIM5α and propose a novel conceptualization of TRIM5α as a restriction factor with a varied portfolio of antiviral functions, including mediating HIV-1 degradation through autophagy- and proteasome-mediated mechanisms, and acting as a viral sensor and effector of antiviral signaling. We have also expanded on the protective antiviral roles of autophagy and outline the therapeutic potential of autophagy modulation to intervene in chronic HIV-1 infection.
2. TRIM5α-Mediated HIV-1 Restriction Across Species
2.1. TRIM5α of Old World Monkeys: The Case of Rhesus Macaques
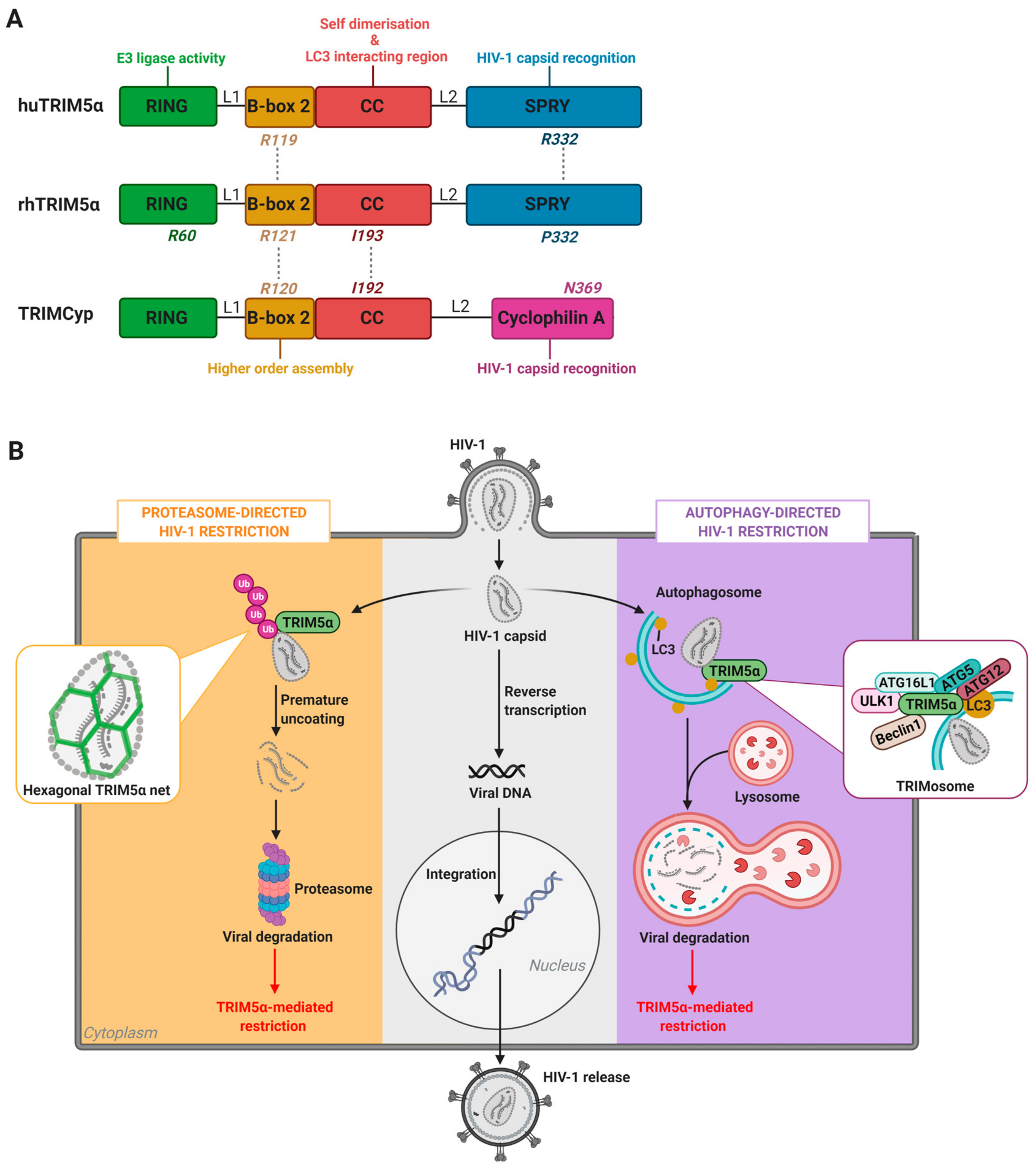
rhTRIM5α is an approximately 500-amino-acid-long protein that exists as either a free cytoplasmic protein or localized within highly mobile cytoplasmic clusters termed cytoplasmic bodies [50]. It is a member of the extensive TRIM (tripartite motif) protein family, so named for their inclusion of three characteristic domains: an amino-terminal RING (really interesting new gene) domain, a B-box, and a coiled-coil (CC) region [67]. The RING and B-box domains are connected via the linker region 1 (L1). This TRIM motif is connected to a carboxyl-terminal SPRY (also known as B30.2) domain via the flexible linker region 2 (L2). The SPRY domain, and in particular its variable sequence 1 (v1), one of three variable peptide sequences in the SPRY domain, mediates TRIM5α interaction with retroviral capsids (Figure 1A) [68,69].
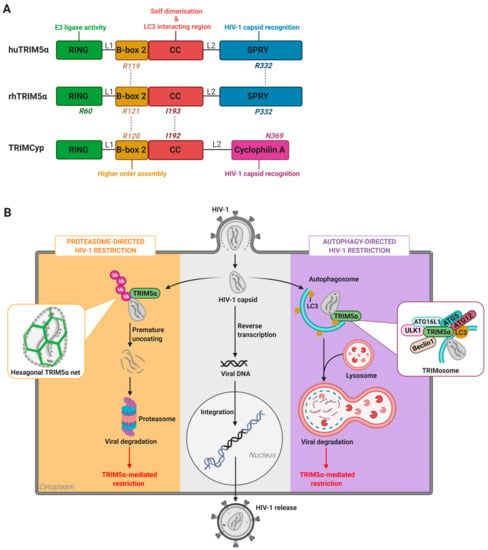
Figure 1.
Structure and functions of TRIM5α. (A) Rhesus (rh)TRIM5α, human (hu)TRIM5α, and TRIMCyp protein domain organization and associated functions. Key amino acid residues impacting antiviral functions per protein domain are depicted. (B) Schematic overview of the main steps of HIV-1 virus replication cycle (center panel, in grey), and the proteasome-directed (left panel, in orange) and autophagy-directed (right panel, in purple) TRIM5α-mediated mechanisms of HIV-1 restriction. RING: really interesting new gene, CC: coiled-coil, LC3: microtubule-associated protein 1A/1B-light chain 3, ULK1: Unc-51 like autophagy activating kinase 1, ATG: autophagy related, Ub: ubiquitin, L1: linker 1, L2: linker 2.
Studies conducted using purified rhTRIM5α protein preparations or in human (HeLa) or canine (Cf2Th) cell lines stably transfected with rhTRIM5α have found that the RING, SPRY, CC, and B-box domains of rhTRIM5α all contribute to the HIV-1 restriction process. The CC and B-box domains facilitate the initial dimerization and subsequent multimerization of rhTRIM5α, promoting its aggregation into cytoplasmic bodies and, upon HIV-1 infection, formation of hexagonal rhTRIM5α nets around target virus capsid proteins [58,59,60]. In vitro mutations of the B-box residue R121 inhibit the formation of hexagonal structures on the surface of HIV-1 capsid, and thereby abrogated rhTRIM5α-mediated HIV-1 restriction (Figure 1A) [58,59,70]. In addition, an I193A mutation within the CC-domain of a rhTRIM5α fusion protein resulted in loss of restriction in HeLa cells and a slight instability of the rhTRIM5α dimer [71]. Structural modeling indicated that residue I193 is likely important for the correct packaging of the CC/L2/SPRY domains, and that the I193A mutation may alter the positioning of the SPRY domain relative to the CC-domain, which is associated with defective binding to the viral capsid [71].
Cryogenic electron microscopy studies with purified rhTRIM5α protein preparations have demonstrated that binding of the SPRY domain to the virus capsid promotes formation of hexagonal rhTRIM5α nets that physically mirror the viral capsid surface lattice, thus compensating for the low affinity of the SPRY domain for the viral capsid by increasing binding avidity, and reinforcing rhTRIM5α binding efficiency [60,72,73]. In HeLa and 293T cell lines transfected with rhTRIM5α, interaction of rhTRIM5α with viral capsid cylinders leads to structural disruption of the HIV-1 capsid proteins, driving premature uncoating of the virus and thereby inhibiting viral genome translocation to the nucleus and retroviral integration [50,74,75].
The E3 ubiquitin ligase activity of the RING domain of rhTRIM5α is key in directing rhTRIM5α-mediated degradation of the HIV-1 capsid. Demonstrative of this, the R60A mutation within the rhTRIM5α RING domain, which abolishes its E3 ubiquitin ligase activity, interferes with retroviral restriction (Figure 1A) [76,77]. The rhTRIM5α RING domain normally directs the elongation of N-terminally anchored K63-linked ubiquitin chains to the viral capsid, which tags the incoming virus for destruction. These ubiquitin-tagged rhTRIM5α-HIV-1 complexes are then directed to the proteasome for subsequent degradation [56,78,79,80].
It has been reported that proteasome inhibition with small-molecule inhibitor MG132 or deletion of the RING domain limits but does not completely abrogate rhTRIM5α-mediated HIV-1 restriction [78,81]. Proteasome inhibition or introduction of RING domain mutations C15A or C18A in rhTRIM5α alters the intracellular localization of rhTRIM5α, causing it to accumulate in relatively large cytoplasmic or (peri)nuclear bodies, respectively, and resulting in decreased availability of rhTRIM5α to restrict HIV-1 [78,81]. Furthermore, disrupting proteasome function permitted the generation of HIV-1 late reverse transcription products, although infection with a single cycle R7ΔEnvGFP reporter HIV-1 virus, as measured by GFP+ cells, remained impaired. Taken together, these data underline that rhTRIM5α acts soon after entry of the retroviral capsid into the cytoplasm, prior to reverse transcription, and together with the proteasome system prevents reverse transcription of HIV-1 and drives proteasomal degradation of rhTRIM5α-HIV-1 complexes.
2.2. TRIM5α of New World Monkeys: The Case of TRIMCyp
It is common amongst Old World monkeys such as Rhesus macaques to exhibit TRIM5α-mediated post-entry restriction of HIV-1, but this phenotype is less common amongst New World monkeys. Owl monkeys specifically exhibit a distinct pattern of HIV-1 restriction not detected in the other New World monkeys such as squirrel monkeys, golden-headed lion tamarins, or black-tailed marmosets [51]. The protein responsible for HIV-1 restriction in owl monkeys was identified to be a fusion protein in which the SPRY domain of TRIM5α has been replaced by the coding sequence of Cyclophilin A (CypA) due to a historical Long Interspersed Element 1 (LINE-1) retrotransposition event [82]. CypA is a host chaperone prolyl isomerase that has interacted with prehistoric lentivirus capsids related to HIV-1 throughout evolution via an exposed peptide loop on the viral capsid lattice [83,84]. The resultant fusion protein, termed TRIMCyp, is a potent inhibitor of lentiviruses, including of HIV-1 by owl monkeys [60,82,85,86]. In addition, CypA has been implicated in MxB-mediated HIV-1 restriction, although the molecular details of this interaction are not yet fully elucidated [87,88].
Owl monkey TRIMCyp-mediated HIV-1 restriction relies on multimeric binding to incoming virus, with the CypA domain (replacing the SPRY domain of rhTRIM5α) binding the HIV-1 capsid [89,90]. Recent studies have highlighted that, similar to rhTRIM5α, the TRIMCyp CC and B-box domains facilitate its dimerization and subsequent multimerization, thereby promoting aggregation into cytoplasmic bodies and, upon HIV-1 infection, formation of hexagonal TRIMCyp nets around target virus capsid proteins [60,91]. Higher-order assembly of TRIMCyp may serve an analogous function of coupling capsid binding and ubiquitination to promote HIV-1 degradation, as with rhTRIM5α.
Like rhTRIM5α, mutating amino acid residue R120 within the TRIMCyp B-box domain abrogates HIV-1 restriction by TRIMCyp (Figure 1A) [70]. In contrast to the rhesus orthologue, mutation of the TRIMCyp CC-domain residue I192 did not result in the abrogation of HIV-1 restriction [71].
With regard to capsid binding, N369 within the CypA domain of TRIMCyp is a key residue for HIV-1 capsid recognition (Figure 1A) [92]. Correspondingly, treatment of HIV-1-GFP-infected HeLa cells with cyclosporine A, which binds the CypA domain, completely abrogated TRIMCyp restriction, indicating that viral capsid binding by the CypA domain is essential for the TRIMCyp’s HIV-1 inhibitory function [91,93].
2.3. Human TRIM5α
Akin to its rhesus macaque orthologue, the huTRIM5α structure contains the characteristic RING, B-box, CC region, and SPRY domains. Exogenous huTRIM5α is able to restrict some lentiviruses, such as N-tropic murine leukemia viruses (N-MLV) in human and mouse cell lines [94]. Unlike rhTRIM5α, huTRIM5α does not efficiently restrict HIV-1 in cell lines [50]. For example, huTRIM5α stably expressed in HeLa cells only slightly inhibits HIV-1-GFP (recombinant HIV-1 expressing GFP pseudotyped with VSV-G glycoprotein) when compared to HeLa-cells expressing rhTRIM5α [50]. Likewise, huTRIM5α expressed in the feline cell line CRFK weakly restricts HIV-1, while rhTRIM5a completely blocks infection [95]. It has previously been suggested that the differing patterns of retrovirus restriction by rhTRIM5α versus huTRIM5α observed in cell lines is due to variation in the SPRY v1 sequence between the two orthologues, in line with the long-standing belief that HIV-1 restriction by rhTRIM5α is species-specific [96,97].
The apparent decreased ability of huTRIM5α to restrict HIV-1 in cell lines has been associated to low affinity for the viral core and instability of the protein [98]. In support of this, a single amino acid substitution on position 332 from arginine to proline (R322P), mimicking the sequence in rhTRIM5α, conferred the ability of huTRIM5α to restrict HIV-1, though ten times less efficient than rhTRIM5α [99]. Furthermore, a R332/R335 double mutation in the SPRY domain provided HIV-1 resistance similar to rhTRIM5α in a T-cell line (SUP-T1) and in primary human T-cells [97,98]. In addition, stabilization of huTRIM5α via fusion to mCherry resulted in robust restriction of HIV-1 strains SF162 and BK132 [98]. This indicated that huTRIM5α is able to bind HIV-1 but that the increased degradation of the human orthologue as compared to rhTRIM5α hampers the HIV-1 restrictive capabilities of huTRIM5α. Furthermore, it has also been demonstrated that the huTRIM5α B-box residue R119, similar to its orthologues rhTRIM5α (R121) and TRIMCyp (R120), is essential for hexagonal structure formation and viral restriction [70]. huTRIM5α R119E and R119D mutants lost antiretroviral activity against non-human viruses such as N-MLV (Figure 1A) [70].
Notably, Ribeiro and colleagues were the first to show that huTRIM5α is a potent HIV-1 restriction factor in specific primary human cells [64]. However, it functions via a distinct mechanism to rhTRIM5α, which relies on HIV-1 uptake via specific cell surface receptors and on an alternative cellular degradation system in human primary immune cells [64]. Recent literature support these findings and further demonstrated the capacity of huTRIM5α to bind the HIV-1 capsid and efficiently restrict HIV-1 infection in human primary immune cells using alternative host proteins and cellular degradations pathways [65,66,100].
4. HIV-1 Escapes huTRIM5α-Mediated Restriction in Submucosal DC-SIGN+ Dendritic Cells and CD4+ T Cells
4.1. Submucosal Dendritic Cells
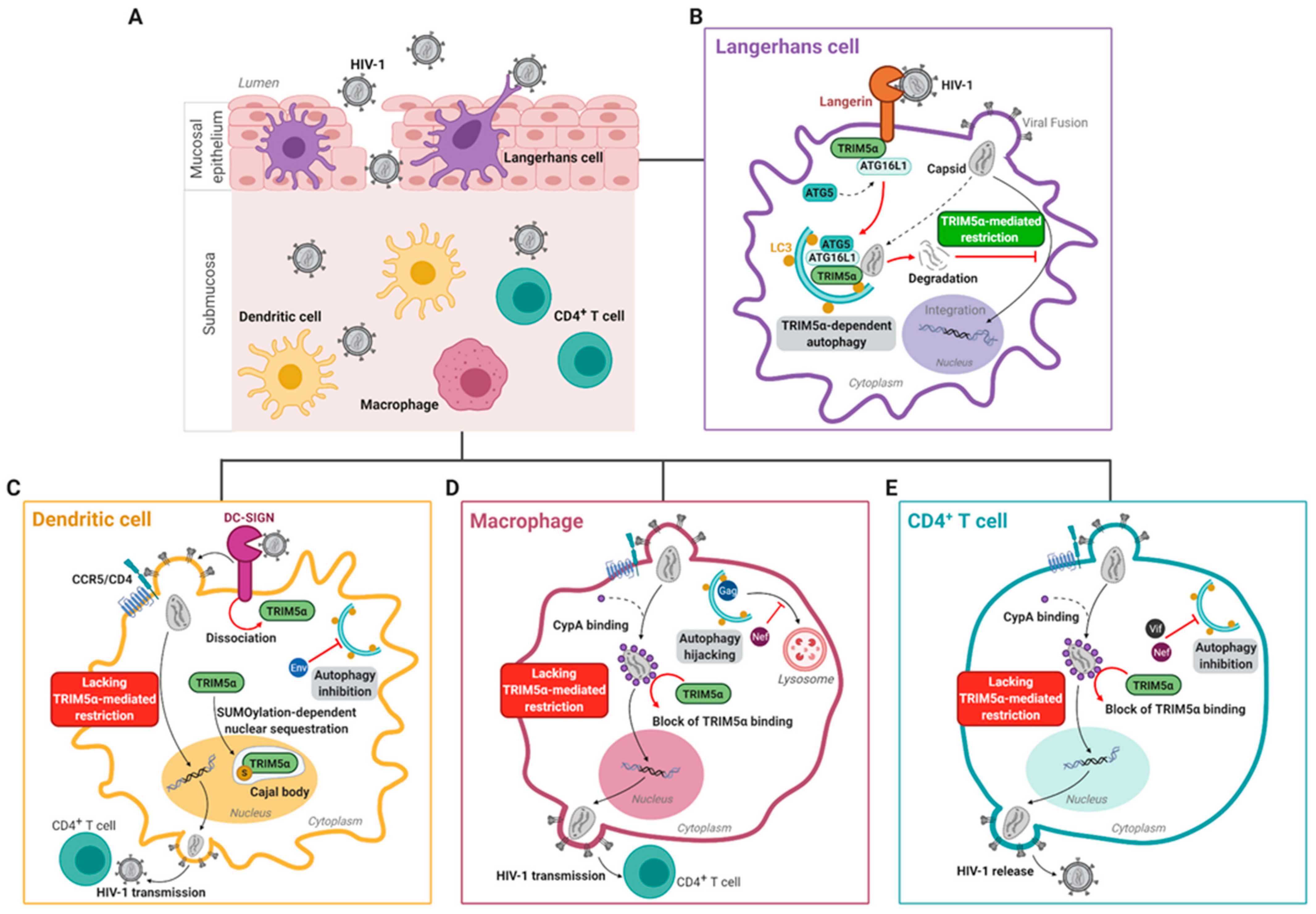
Although huTRIM5α has been demonstrated to restrict HIV-1 in an autophagy-dependent manner in primary human LCs, several groups have independently shown that huTRIM5α is unable to restrict HIV-1 in other primary targets such as submucosal DCs [64,153]. An important receptor for HIV-1 transmission is the highly expressed surface receptor DC-SIGN [152]. Normally, upon binding to a ligand, DC-SIGN facilitates receptor-mediated endocytosis to initiate antigen-processing [158]. In addition, DC-SIGN facilitates interaction of DCs with CD4+ T-cells via the immunological synapse [152]. Several studies have also shown that submucosal DCs are able to facilitate HIV-1 transmission via a mechanism termed trans-infection [152,159,160]. During this mechanism, DCs capture the virus and transmit it to CD4+ T-cells via a virological synapse, without replication of the virus within the DCs. Several independent studies have also reported productive HIV-1 infection of submucosal DCs, with active replication prior to transmission to other cells (termed cis-infection), although productive infection of DCs compared to CD4+ T-cells is 10- to 100-fold lower [150,151,161]. In the case of productive infection, DC-SIGN strongly binds the HIV-1 envelope glycoprotein gp120 and together with other PRRs is essential for viral replication in DCs [151,162,163]. In particular, DC-SIGN-mediated signaling, which is induced upon binding of the HIV-1 envelope glycoprotein gp120, is necessary for eventual generation of full-length virus transcripts [151]. In addition, HIV-1 envelope protein Env activates mammalian target of rapamycin (mTOR), thereby downregulating autophagy, which prevents autophagy-mediated viral degradation. In support of this, treatment with the mTOR inhibitors everolimus or rapamycin results in induction of autophagy, leading to a reduction in productive HIV-1 infection of tissue-derived DCs, and a decrease in transmission of HIV-1 by human DCs to CD4+ T-cells [153,164].
Notably, at steady-state conditions, huTRIM5α forms a complex with DC-SIGN, in a manner similar to that with Langerin as described in Section 3.3 [64]. However, upon binding of HIV-1 to DC-SIGN, huTRIM5α dissociated from the DC-SIGN signalosome [64] (Figure 2C). In concurrence with this data, silencing of huTRIM5α in DC-SIGN+ DCs had no effect on HIV-1 integration or infection [64]. This highlights that multiple C-type lectin receptors, including DC-SIGN and Langerin, can form complexes with huTRIM5α, but that the HIV-1 restriction properties of huTRIM5α are cell-specific and receptor-dependent.
Recently, new light was shed on the lack of HIV-1 restriction by huTRIM5α in primary human monocyte-derived DCs [62,144]. In human DCs, huTRIM5α is sequestered in Cajal bodies, a subset of membrane-less nuclear bodies consisting mostly of proteins and RNA, and other nuclear bodies via a small ubiquitin-like modifier (SUMO)ylation-dependent manner. Nuclear sequestration of huTRIM5α makes room for innate immune sensing of retroviral genetic material by the DNA sensor cGAS in the cytosol, leading to potent induction of type I IFN responses that are key for promoting an antiviral state [62,144]. Strikingly, overexpression of huTRIM5α in human DCs, or treatment with an inhibitor of SUMOylation, restored cytoplasmic huTRIM5α expression and efficient huTRIM5α-mediated HIV-1 restriction [62]. These results suggest the potentiality of huTRIM5α to restrict HIV-1 in other DC subsets in addition to LCs.
Furthermore, a recent study demonstrated the potential role for CypA in abrogating huTRIM5α-mediated HIV-1 restriction in DCs [165]. Infection of primary human monocyte-derived DCs with single round VSV-G pseudotyped HIV-1 viruses bearing capsid mutation P90A, which prevents CypA from interacting with the capsid, was less efficient as compared to infection with viruses lacking the P90A mutation [66,166,167]. HIV-1 infection by HIV-1 P90A was restored upon depletion of huTRIM5α in the DCs, which further highlights the capacity of huTRIM5α to inhibit HIV-1 in DCs [165]. It is important to note here that VSV-G-pseudotyped HIV-1 largely bypasses the DC-SIGN uptake route, and that the observed huTRIM5α-mediated restriction of VSV-G pseudotyped HIV-1 P90A in DCs upon CypA depletion is yet to be confirmed with HIV-1 bearing the viral glycoprotein gp120 [165,168].
Notably, it was also recently demonstrated that rhTRIM5α does not restrict HIV-1 in primary rhesus macaque monocyte-derived DCs, unlike in other rhesus macaque primary cells or cell lines, or in human cell lines ectopically expressing rhTRIM5α [50,169]. Rather, rhTRIM5α was SUMOylated and sequestered in the nucleus of rhesus macaque DCs following the same mechanism described in human DCs. Strikingly, this lack of restriction by rhTRIM5α was also demonstrated in cynomolgus and pigtailed macaque DCs, as well as in African green monkey DCs, indicating that lack of TRIM5α-mediated restriction is prevalent in humans and other primate DCs [62].
This lack of TRIM5α-mediated restriction in DCs is thus conserved throughout evolution, possibly as a tradeoff for viral sensing and induction of type I IFN responses. Restoration of huTRIM5α-mediated restriction in DCs by blocking host pathways such as CypA binding and SUMOylation provides insight into novel therapeutic possibilities.
4.2. Macrophages
Macrophages are myeloid lineage cells that are resident in subepithelial tissues throughout the body. They can originate from self-renewing tissue-resident macrophages or infiltrating blood-derived monocytes [170,171]. As antigen-presenting cells, macrophages are important for bridging innate and adaptive immunity by phagocytosing extracellular pathogens, and presenting pathogen-derived antigens to CD4+ T cells [172]. As macrophages express the HIV-1 entry receptor CD4 and co-receptors CCR5 and CXCR4, they are themselves susceptible to HIV-1 infection [13]. In addition, HIV-1 infected macrophages can transmit virus to CD4+ T cells via a viral synapse, i.e., cell-to-cell contact, in a manner similar to that of DCs (Figure 2D) [173,174,175].
In macrophages, HIV-1 hijacks the early non-degradative stages of autophagy. Research using primary human macrophages, as well as THP-1 and U937 monocyte-derived macrophages, has demonstrated that the induction of autophagy with rapamycin increased extracellular HIV-1 yields [176]. In addition, inhibition of autophagy via treatment with 3MA or knock-out of Beclin1 and ATG7 resulted in a reduction in the extracellular release of infectious virus as compared to untreated cells, indicating that autophagy promotes HIV-1 maturation or release in macrophages [176]. This is in contrast with other immune cell types, as induction of autophagy in LCs, DCs, and CD4+ T cells results in a decrease in production of mature virions [64,164,177].
In macrophages, the interaction of toll-like receptor 8 (TLR8) and HIV-1 induces autophagy by Beclin 1-dependent dephosphorylation of transcription factor EB (TFEB) and subsequently its nuclear translocation during the initial stages of HIV-1 infection [178,179]. Upon the induction of autophagy, HIV-1 Gag proteins co-localize with autophagy-related protein LC3 and subsequently promote Gag processing [176].
The HIV-1 Nef protein plays an important role in manipulation of host autophagy, and thereby immune evasion, in macrophages. Several studies have indicated that, by inhibiting Beclin 1 association with class III PI 3-kinase (PI3KC3) complex II, which plays a key role in autophagosome-lysosome fusion, HIV-1 Nef blocks autophagosome maturation [176,180]. Interestingly, recent studies have also indicated that Nef additionally blocks autophagy at its early initiation stages [176,178,180,181].
In addition to evading host antiviral mechanisms in macrophages, HIV-1 also exploits host proteins to evade restriction. Recent studies have demonstrated that multimeric binding of host CypA proteins to the viral capsid prevents interaction of huTRIM5α with the viral core, thereby blocking huTRIM5α-mediated restriction [165,182]. Correspondingly, HIV-1 viruses bearing capsid mutation P90A, which prevents CypA from interacting with the capsid, were restricted by huTRIM5α in macrophages, as was also demonstrated in DCs [66,165,166,167]. Likewise, a construct generated by fusion of CypA to huTRIM5α (hT5Cyp), inspired by the New World monkey TRIMCyp as described in Section 2.2, was able to block HIV-1 infection in human primary macrophages [19].
4.3. T Cells
CD4+ T cells are key HIV-1 target cells that can be infected directly within the mucosal environment, or following transmission from DCs (Figure 2E) [144]. In addition, HIV-1 can latently persist in long-lived CD4+ T cells in PLWH [6,148,183]. As in DCs, HIV-1 infection inhibits autophagy in human CD4+ T cells, via HIV-1 Vif interactions with LC3, and a HIV-1 Nef-dependent block in autophagy flux resulting in accumulation of endosomes and lysosomes [184,185]. Moreover, as in macrophages, multimeric binding of host CypA to the incoming viral capsid blocks the interaction of huTRIM5α with the viral core, thereby preventing huTRIM5α-mediated restriction during CD4+ T cell infection. In addition, it was demonstrated recently that endogenous huTRIM5α in primary human CD4+ T cells is able to bind the HIV-1 capsid post-fusion, in the absence of CypA, and thereby restrict HIV-1 [66]. In addition, HIV-1 viruses bearing capsid mutations such as P90A and G89V, which prevent CypA interacting with the capsid, were unable to infect primary human CD4+ T cells [66,166,167]. Similar to in submucosal DCs and macrophages, infection by HIV-1-P90A was restored upon depletion of huTRIM5α in primary human CD4+ T cells or in Jurkat cells [66,165]. However, it is still unclear whether autophagy machinery plays a role in the huTRIM5α-mediated HIV-1 restriction in CD4+ T cells.
An additional IFNα-dependent mechanism for huTRIM5α-directed control of HIV-1 infection in human cell lines and primary human CD4+ T cells was recently demonstrated [65]. In primary human CD4+ T cells and in U87-MG.CD4+CXCR4+ cells transduced to ectopically express huTRIM5α, HIV-1 infection was efficiently inhibited in the presence of IFNα, in a manner dependent on SPRY domain-mediated recognition of the viral capsid [65]. The presence of IFNα stimulated activation of the immunoproteasome, a proteasome isoform primarily present in immune cells, and selectively promoted ubiquitination of huTRIM5α, thereby accelerating its proteolytic turnover, indicating that, in the presence of IFNα, the immunoproteasome may facilitate degradation of huTRIM5α-HIV-1 capsid complexes [65].
Prior to these findings, huTRIM5α had long been considered to be a poor HIV-1 restrictor in a variety of cell lines. We have shown for the first time that huTRIM5α is a potent restriction factor in human LCs, and that this restriction is dependent on autophagy mechanisms and cell-surface receptor usage by HIV-1. These recent studies further underline the capacity of huTRIM5α to potentially restrict HIV-1 in other relevant human target cells such as DCs, CD4+ T cells, and macrophages. Thus, efficient huTRIM5α restriction likely depends on TRIM5α subcellular localization (e.g., nucleus versus cytosol) within specific cell or tissue types, but also on the ability to induce autophagy- and immunoproteasome-facilitated degradation pathways, the presence of additional cellular factors that facilitate the action of huTRIM5α (e.g., Langerin), and the absence or inhibition of cellular factors that block huTRIM5α recognition of the viral capsid (e.g., CypA) [62,64,65,186].
4.4. Cell-Specific and Autophagy-Dependent Restriction of HIV-1 by Additional Restriction Factors
Cell-specific restriction is not exclusive to TRIM5α. For example, it has been suggested that differential SAMHD1 degradation may be an underlying contributor to the reduced permissiveness to HIV-1 in human macrophages and DCs as compared to activated CD4+ T cells. In support of this, pre-treatment with Vpx, a known inducer of SAMHD1 degradation during HIV-2 or SIV infection but absent in HIV-1, promoted degradation of SAMHD1 and enhanced susceptibility of macrophages and DCs to HIV-1 [35]. However, another study showed that SAMHD1 also protects resting CD4+ T cells in a similar manner to macrophages and DCs [187].
The restriction factor MARCH8 also shows cell-specific activity. MARCH8 mRNA levels have been demonstrated to be 5 to 8 times higher in primary human terminally differentiated myeloid cells versus CD4+ T cells and monocytes [25]. These expression levels aligned with decreased infection in differentiated myeloid cells versus high infection in CD4+ T cells. Taken together, these recent data suggest that in primary cells, HIV-1 restriction by different host antiviral factors is likely cell-specific, and modulated by the presence or absence, and expression or degradation levels of the restriction factors in question.
In recent years, several reports have also indicated that autophagy is involved in the activity of multiple HIV-1 restriction factors in addition to huTRIM5α. For example, tetherin has been shown to interact with autophagy via multiple different pathways. In the context of HIV-1 infection, HIV-1 Vpu has been reported to downregulate tetherin expression on the cell surface by promoting its ubiquitination and subsequent intracellular sequestration and/or degradation within autophagosomes or lysosomes, thus potentially hijacking the autophagy pathway for the benefit of the virus [188,189]. Strikingly, breast cancer-associated gene 2 (BCA2, also known as Rabring7, ZNF364, or RNF115), a RING-type E3 ubiquitin ligase, was shown to interact with tetherin to promote HIV-1 packaging into CD63+ endosomes, with the end result being lysosomal degradation of HIV-1 virions and tetherin in a manner reminiscent of tetherin-dependent autophagic degradation of damaged mitochondria in uninfected cells [190,191].
On the other hand, tetherin has been demonstrated to recruit a second restriction factor, MARCH8, in order to prevent type I IFN signaling in an autophagy-dependent manner [192]. MARCH8 was recently identified as a novel antiretroviral restriction factor in terminally differentiated myeloid cells, such as macrophages and DCs, and is recruited by tetherin to ubiquitinate the RLR MAVS, leading to NDP52-dependent autophagic degradation of MAVS and, as a result, inhibition of MAVS-dependent type I IFN signaling [25,192]. The restrictive action of MARCH8 may also be autophagy-dependent, as MARCH-8-directed degradation of VSV-G is not affected by treatment with a proteasome inhibitor, but was blocked upon treatment with lysosomal protease inhibitors [25]. Next to MARCH8, the closely related MARCH2 protein has a similar mechanism of virus restriction and potential role for autophagy [43]. It would therefore be interesting to investigate if pharmacological autophagy enhancement could promote MARCH8-or MARCH2-mediated HIV-1 restriction.
5. TRIM5 as An Innate Immune Sensor
By definition, restriction factors must recognize pathogen-associated molecular patterns (PAMPs) to exert their functions and interfere with the replication cycles of viruses. Recent literature highlights that restriction factors can utilize this function not only to prevent viral replication, but also to act as sensors to initiate innate immune signaling pathways to prevent infection [45,46,47,48,49].
The restriction factor huTRIM5α is upregulated by IFNα signaling, as demonstrated by an increase in TRIM5α mRNA expression levels upon IFN treatment, thereby intensifying blocks in HIV-1 infection [63]. However, huTRIM5α is now understood to act not only as a retroviral restriction factor, but also as a PRR for sensing of incoming retroviral capsids (Figure 3) [49].
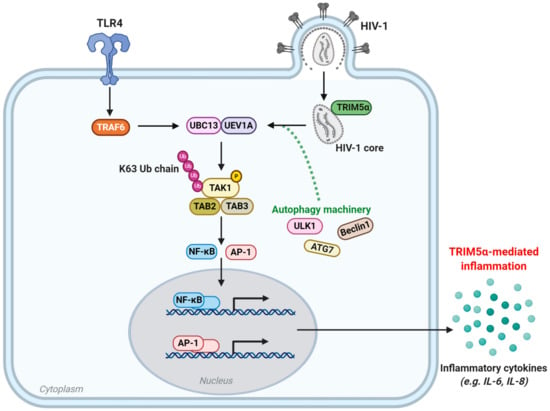
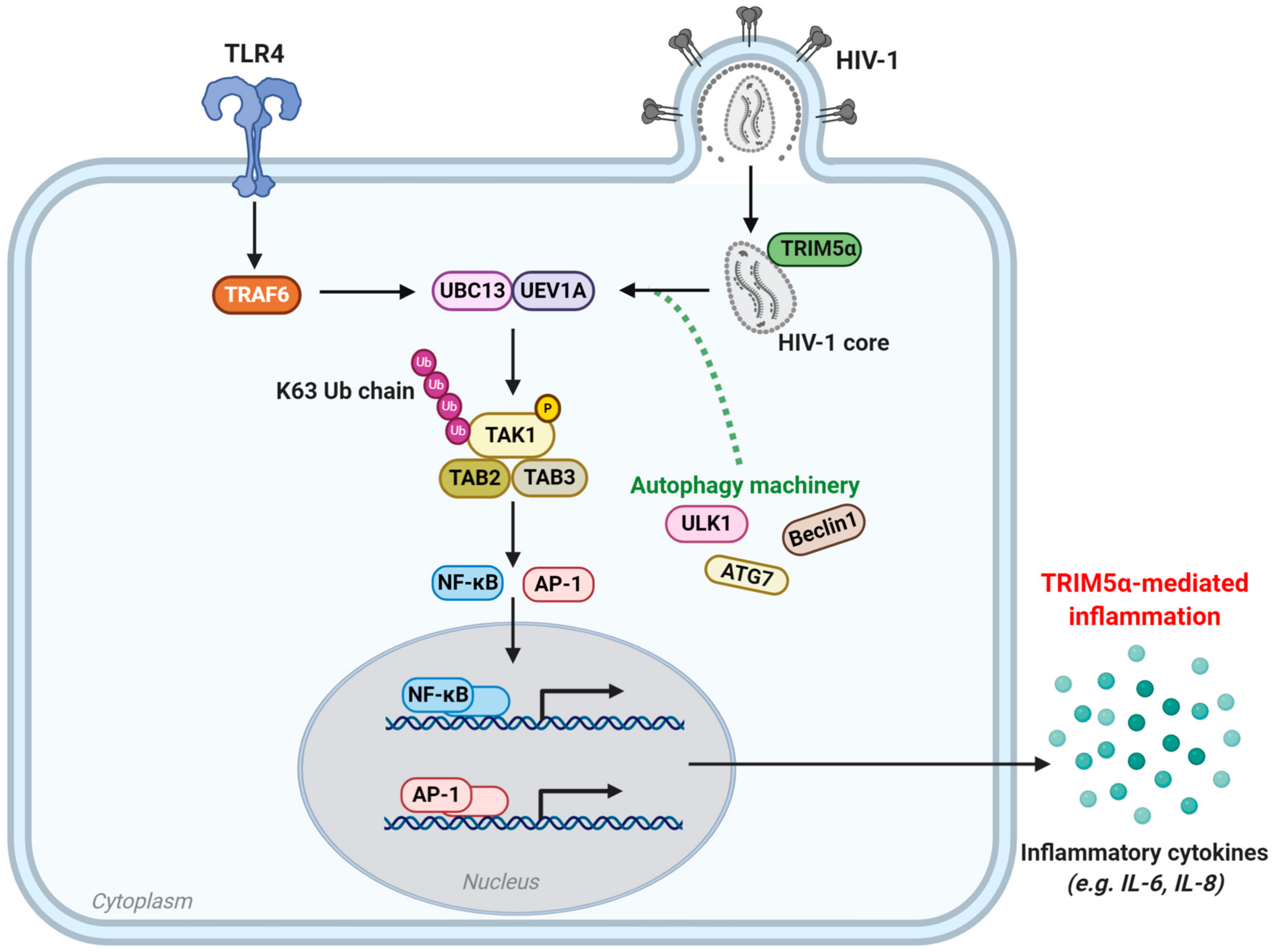
Figure 3.
TRIM5α-mediated regulation of innate immune signaling and molecular inflammation. The TAK1 signaling pathway is activated upon TLR4 stimulation, or upon sensing of viral capsid by TRIM5α. Subsequently, the E3 ligase activity of TRAF6 is activated and, together with the E2 ubiquitin conjugating enzyme complex UEV1A-UBC13, promotes K63-chain linked ubiquitination and autophosphorylation of the TAK1-TAB complex. In the context of HIV-1 infection, sensing of the viral capsid by TRIM5α initiates its E3 ligase activity resulting in K63-chain linked ubiquitination and autophosphorylation of the TAK1-TAB complex. Subsequently, the TAK1-TAB complex activates the transcription factors NF-kB and AP-1, leading to the transcription and ultimately secretion of pro-inflammatory cytokines such as IL-6 and IL-8. The autophagy-related proteins ULK1, Beclin1 and ATG7 are essential for TRIM5α to function as an innate immune sensor. However, precisely how they contribute to the TRIM5α-mediated inflammation is as yet uncertain. TLR4: toll-like receptor 4, TAK1: transforming growth factor-β-activated kinase 1, TAB: TAK1-binding protein, UEV1A: ubiquitin-conjugating enzyme E2 variant 1A, UBC13: ubiquitin-conjugating enzyme E2 13, AP-1: activating protein 1, NF-κB: nuclear factor κB, Ub: ubiquitin, P: phosphate, IL: interleukin.
When huTRIM5α is overexpressed, or recognizes a retroviral capsid, its RING domain recruits E2 ubiquitin-conjugating enzymes, thereby inducing ubiquitin-dependent signaling [49]. The multimerization of huTRIM5α upon binding the retroviral N-MLV capsid results in a unique trimeric RING domain arrangement that specifically promotes polymerization of K63-linked ubiquitin chains at its N-terminus, as demonstrated in feline (CrFK) and human (TE671) cell lines [80]. This polyubiquitination of huTRIM5α subsequently activates the TAK1 (also known as MAP3K7) kinase complex, and later the AP-1 and NF-κB signaling pathways [49]. This ultimately results in activation of the transcription factors AP-1 and NF-κB, which promote transcription of inflammatory mediators such as CXCL9, CXCL10, CCL8, IL-6, IL-8, and COX2, as shown in primary monocyte-derived DCs and macrophages, THP-1 monocytes and macrophages, and owl monkey kidney (OMK) cells upon recognition of the N-MLV capsid [49]. In addition, OMK cells challenged with VSV-G-pseudotyped HIV-1 upregulated secretion of IL8, CCL2, CCL4, and CSCL10 [49]. Alternatively, in 293T cells, huTRIM5α has also been demonstrated to negatively regulate NF-κB activation, via huTRIM5α-directed degradation of TAK-1 binding protein (TAB)-2, in a dose-dependent manner [193]. The use of proteasomal inhibitors showed that this mechanism is independent of E3 ubiquitin ligase activity, suggesting a role for an alternative degradative pathway. Altogether, this underlines huTRIM5α as a key PRR and regulator of AP-1 and NF-κB and AP-1 and NF-κB-responsive inflammatory mediators, in response to sensing retroviral capsids.
Strikingly, recent data highlight a role for autophagy in huTRIM5α’s functioning as an innate sensor. Genetic depletion of key autophagy proteins such as Beclin 1, ATG7, and ULK1 was required for huTRIM5α-based activation of AP-1 and NF-κB, and thereby of AP-1 and NF-κB-responsive genes [194]. In primary immune cells, induction of IFN-β expression in response to huTRIM5α-restricted recognition of HIV-1 capsid mutant (P90A) was dependent on Beclin 1, ATG7, and ULK1. Furthermore, in autophagy deficient cells, huTRIM5α-driven TAK1 activation, which is also Beclin 1 and ATG7-dependent, was attenuated [194]. Taken together, these data underline that autophagy contributes not only to huTRIM5α-mediated HIV-1 restriction, but also to the role of huTRIM5α as an innate immune sensor of incoming retroviral capsids.
Notably, in primary human DCs, which are a key cell type for linking innate and adaptive immune responses, endogenous huTRIM5α has been demonstrated to negatively regulate induction of type I IFN responses, as well as to positively regulate AP-1 and NF-κB-responsive inflammatory mediators, upon HIV-1 infection [49,62]. Type I IFN suppresses viral replication by upregulating IFN-stimulated genes (ISGs) that can target and inhibit HIV-1 at various steps of the viral life cycle [24,38,144,195]. Activation of IFNα upregulates transcription of ISGs including APOBEC3G, tetherin, and TRIM5α itself, as well as other members of the TRIM family that participate in anti-HIV-1 immune responses such as TRIM22 [44,196,197]. Recent data indicate that upregulation of IFNα is also required for huTRIM5α-mediated HIV-1 restriction in the typically HIV-1 permissive U87-MG.CD4+CXCR4+ cell line and in primary human CD4+ T cells [65]. Altogether, these findings further underline that huTRIM5α plays important intracellular roles in antiretroviral immunity and possesses the capacity for retroviral restriction; however, additional host factors or cytoplasmic counterparts are required to elicit such huTRIM5α-mediated HIV-1 restriction.
In addition to huTRIM5α sensing of exogenous retroviruses such as HIV-1, recent data suggest that the hypothesis that TRIM5α evolution was driven by retroelements, or endogenous retroviruses, is well-founded [186,198,199]. Notably, huTRIM5α was shown to both sense and restrict LINE-1 transposable elements, the only known autonomously active transposable element in humans, in HEK 293T cells [186]. Functional SPRY and B-box domains were essential for huTRIM5α-mediated inhibition of LINE-1 replication and insertion into the host genome. Cytoplasmic co-localization of huTRIM5α and LINE-1 ribonucleoproteins (RNPs), in either cytoplasmic bodies or in a more diffuse pattern, was necessary for huTRIM5α-mediated LINE-1 restriction. In addition, upon sensing LINE-1 RNPs, huTRIM5α activated the TAK1 kinase complex, leading to subsequent activation of the AP-1 and NF-κB pathways [186]. Furthermore, rhTRIMCyp also inhibited LINE-1 retrotransposition, suggesting that, as with the SPRY domain of huTRIM5α, CypA may also bind LINE-1 RNPs leading to retroelement restriction. Altogether, these findings indicate that the intrinsic ability of huTRIM5α to restrict LINE-1 elements is reminiscent of the potency of huTRIM5α to restrict exogenous retroviral capsids.
6. In Vivo Relevancy of TRIM5α and Autophagy in HIV-1 Infections
6.1. Impact of huTRIM5α Polymorphisms on Disease Progression
To further define the roles of huTRIM5α and its relevance as a therapeutic target to treat HIV-1 infection, it is enlightening to examine the presence of single nucleotide polymorphisms (SNPs) in the huTRIM5α gene, and their association with clinical outcomes and disease progression. Several epidemiological genetic studies have demonstrated a relationship between SNPs of huTRIM5α and HIV-1 susceptibility, disease progression and innate and adaptive immunity, as summarized in Table 1.

Table 1.
Association between huTRIM5 SNPs and HIV-1 susceptibility, disease progression, and immunity.
With regard to HIV-1 susceptibility and disease progression, two SNPs that have been extensively studied are the arginine to glutamine mutation at gene position 136 (R136Q; TRIM5 rs10838525), and the histidine to tyrosine mutation at position 43 (H43Y; TRIM5 rs3740996). The former, TRIM5 R136Q, is located within the CC domain of huTRIM5α and has been demonstrated to have a protective effect on HIV-1 susceptibility in diverse cohorts [200,201,202]. In concordance, in vitro studies using Cf2TH cells expressing wild-type (wt) or mutant huTRIM5α and incubated with GFP-reporter HIV-1 have demonstrated that the 136Q variant of huTRIM5α showed superior effects in restricting HIV-1 over wild-type 136R huTRIM5α [200].
Likewise, TRIM5 H43Y, located in the RING domain, has been shown to have a protective effect on HIV-1 susceptibility, although there are discrepancies in the demonstrated efficacy of this SNP depending on the ethnicity of participants [200,203,204,205]. Thus, it may be that the protective effect of TRIM5 H43Y on HIV-1 susceptibility depends to some extent on interactions with other polymorphic genes that differ across genetically different populations. Contrastingly, the homozygous TRIM5 H43Y genotype was found to be predictive for an accelerated disease progression in vivo, and deleterious in vitro in CRFK cells stably transduced with H43Y huTRIM5α [95,206]. However, this may be explained by the fact that the RING domain is involved not only in ubiquitination of huTRIM5α-HIV-1 complexes but also in self-ubiquitination of huTRIM5α, which is important for homeostatic cycling of the host factor [127]. Thus, in uninfected individuals, mutations such as H43Y in the RING domain of huTRIM5α may result in impaired self-ubiquitination and increased levels of huTRIM5α in the cytoplasm, leading to increased antiretroviral activity against incoming HIV-1 virions and hence an increased protective effect against HIV-1 infection. On the other hand, the E3 ligase activity of the RING domain has also been shown to be involved in the innate immune response against HIV-1 [49]. Therefore, in infected individuals, mutations in the RING domain of huTRIM5α may be associated with decreased control of HIV-1 infection by the innate immune system, thus explaining the association of SNP H43Y with accelerated disease progression.
More recently, several SNPs in huTRIM5α have been demonstrated to be more prevalent in HIV-1 infected patients as compared to healthy controls, indicating a detrimental effect of these polymorphisms on HIV-1 susceptibility. For example, expression of a G249D allele of huTRIM5α SNP rs11038628 was found to be significantly higher in HIV-infected patients as compared to healthy subjects in an Indian population, and to attenuate HIV-1 restricting activity of huTRIM5α in vitro [207]. The same tendency, though weaker and non-significant, was also observed in a Japanese population [207].
Similarly, a huTRIM5α variant with the G110R SNP in the B-box domain, which is more frequent in Japanese HIV-1 infected patients than controls, also showed a decreased ability to control HIV-1 in vitro [204]. Interestingly, the same study also identified a truncated G176del huTRIM5α variant found only in Japanese populations, which enhanced antiviral activity of co-expressed full-length huTRIM5α. This may be due to the G176del huTRIM5α variant’s enhanced functioning as an activator of innate immune responses, in line with the alternative functioning of huTRIM5α as a PRR as discussed above in Section 5 [204]. Finally, a polymorphic variant of huTRIM5α rs904375, located in intron 4, has been described to affect susceptibility to HIV-1 infection, likely by impacting transcription factor-binding sites and thereby TRIM5 transcriptional activity [208].
To our knowledge, no studies specifically aiming to determine a correlation between huTRIM5α SNPs and the anti-HIV-1 adaptive immune responses in PLWH have thus far been conducted. However, it has been demonstrated that the synonymous SNPs, TRIM5 rs3824949 and TRIM5 rs7122620, correlated with increased levels of rubella- and measles-specific antibodies in humans upon vaccination against these pathogens [209,210]. Notably, patients possessing TRIM5 rs3824949 who were treated for chronic hepatitis C virus (HCV) were also more likely to reach rapid virologic response (RVR), early virologic response (EVR) and sustained virologic response (SVR) as compared to wt control patients [211]. The beneficial effect of TRIM5 rs3824949 in achieving SVR to HCV was also observed in HIV/HCV co-infected patients [212]. Moreover, the presence of SNPs TRIM5 rs7122620 and TRIM5 rs11820502 correlated, respectively, with increased IL-2 and IL-6 secretion upon measles vaccination [210].
These data illustrate the associations of human TRIM5 SNPs to differing HIV-1 susceptibility and disease progression underline the in vivo relevancy of huTRIM5α. Further underlining the importance of huTRIM5α in vivo, higher expression levels of huTRIM5α, as well as TRIM22 and TRIM28, was demonstrated in PLWH who initiated cART treatment early, versus in those who initiated ART treatment during chronic infection phase [213]. However, no relationship between latent HIV-1 reservoir size and huTRIM5α expression in cART-treated patients was demonstrated, although a second study demonstrated increased expression of huTRIM5α, as well as other restriction factors, over time in HIV-1 infected, untreated patients [213,214].
Taken together, these results illustrate that polymorphisms and differential expression of the huTRIM5α gene may impact HIV-1 susceptibility and influence HIV-1 disease progression. Expression of the huTRIM5α gene and its polymorphisms can serve as a predictive biomarker to determine susceptibility to HIV-1 by HIV-1 negative individuals, as well as function as a prognostic biomarker to predict disease progression in PLWH. This utilization of TRIM5 as a biomarker may assist in the design of optimal treatment regimens and prevention of HIV-1 in the future.
6.2. TRIM5α-Based Therapeutic Strategies for HIV-1
In accordance with the long-accepted hypothesis that only rhTRIM5α is able to restrict HIV-1, attempts have been made to genetically engineer rhTRIM5α-expressing human cells. In terms of HIV-1 therapies, the high potential of TRIM-based gene therapy strategies has been extensively reviewed [17]. One potential strategy has been to develop human mimics of TRIMCyp fusion proteins, which restrict HIV-1 when expressed in cell lines or in primary T cells and macrophages [19,85]. Interestingly, a fusion protein of TRIM21 and CypA, TRIM21Cyp, was also effective in preventing HIV-1 reverse transcription in human cell lines and human primary peripheral blood mononuclear cells (PBMCs) [85]. TRIM21Cyp restriction was only partially inhibited by treatment with the protease inhibitor MG132, which may be explained by TRIM21 also being a recruiter of key autophagy machinery upon binding its target proteins, including ULK1, Beclin1, ATG16L1, and GABARAP [85,215]. This could result in autophagic degradation of TRIM21Cyp-HIV-1 complexes. Fusions of CypA with TRIM1, TRIM18, and TRIM19 were also able to restrict HIV-1, with TRIM1Cyp being particularly potent, perhaps because TRIM1 is also an autophagy regulator [129,216].
The potential of mutant huTRIM5α proteins and chimeric rh/huTRIM5α proteins has also been explored. Transduction of CD34+ human hematopoietic stem cells (HSCs) with a chimeric rh/huTRIM5α, in combination with a CCR5 short hairpin RNA (shRNA) and a TAR decoy, was shown to be effective in protecting against HIV-1 challenge and providing a selective survival advantage in human CD4+ T cells upon infection in a humanized mouse model [217]. A rh/huTRIM5α chimeric variant was also demonstrated to efficiently restrict HIV-1 in HSC-derived macrophages in vitro and T-cells in vivo in a humanized mouse model transplanted with human fetal tissue [218]. Besides chimeric variants, single amino acid changes at positions 332 and 335 of the huTRIM5α SPRY domain to more closely mimic the rhTRIM5α v1 sequence were also shown to prevent the spread of HIV-1 infection by 20- to 50-fold in TE671 fibroblasts and in the human T-cell line SUP-T1 [97].
However, gene therapy with such variants of TRIM5α has significant downsides. For one, it is possible that huTRIM5α mutants or human mimics of TRIMCyp fusion proteins could disrupt endogenous huTRIM5α function, for example, in innate immune signaling [85]. Furthermore, delivery of these treatment options would entail either transduction and re-infusion of differentiated autologous cells, which would require life-long therapy, or stem-cell based approaches that would necessitate invasive and relatively high-risk preparative ablative chemotherapy [17,219]. Alternatively, targeting TRIM5α-directed cellular mechanisms such as proteasomal activity, autophagy-mediated degradation, and antiviral inflammatory signaling may represent innovative and relevant approaches to capitalize on TRIM5α-mediated antiviral functions.
6.3. Impact of Autophagy on HIV-1 Disease Progression and Comorbidities
As outlined above in Section 4, HIV-1 has been demonstrated to evade autophagy in several different cell types in vitro, including DCs, macrophages, and CD4+ T cells via viral molecules such as Vif and Nef [64,153,184,185]. In vivo and ex vivo studies have further underlined the importance of autophagy in anti-HIV-1 immunity. Ex vivo studies using PBMCs derived from PLWH have shown that long-term non-progressor PLWH contain more specialized autophagy vesicles than those from normal progressors [220]. Notably, viral production and viral load in ex vivo PBMCs derived from PLWH were reduced upon treatment with the autophagy-enhancing drug rapamycin [220]. In line with this finding, enhancement of autophagy in monocyte-derived DCs and macrophages and CD4+ T cells in vitro has shown similar successes in controlling HIV-1 infection or promoting autophagy-dependent apoptosis of HIV-1 infected cells [164,221,222]. Successful control of HIV-1 infection is likely dependent on the level of induced autophagy. Productive HIV-1 infection has been detected in T cell lines and primary human monocyte-derived macrophages with moderate amounts of autophagosomes present, whereas strong autophagy induction inhibits viral replication and infection [223]. This indicates that intrinsic autophagy mechanisms, and, more importantly, pharmaceutical enhancement of autophagy, can control HIV-1 infection.
Furthermore, autophagy dysfunction has been associated with increased risk for HIV-1 associated comorbidities in cART-treated HIV-1 patients and animal models [224,225]. Cardiovascular disease is a leading comorbidity for PLWH, even in those who are cART-treated [226]. The HIV-1 Nef protein, which is thought to be released extracellularly by HIV-1 infected CD4+ T cells and is detectable in the serum of HIV-1-positive patients, accumulates in cardiomyocytes where it dysregulates autophagy leading to cardiomyocyte cytotoxicity and death. Strikingly, this effect could be reversed in vitro by treatment with the autophagy-inducing drug rapamycin [225]. Nef is not the only HIV-1 protein affecting cardiomyocytes; the HIV-1 protein Tat also has a profound impact on these cells. Recent research has shown that transduction of cardiomyocytes with adenoviral-Tat impaired mitochondrial Ca2+ uptake and the electrophysiological activity of the cardiomyocytes. In addition, Tat impaired the protein clearance function of autophagy under hypoxic conditions, due to a reduction in ubiquitination and dysregulation of autophagy proteins p62 and LC3-ll [227]. As well as Nef and Tat, the HIV-1 proteins Env, Gag, Vif, and p24 have all been shown to impact autophagy pathways or serve as specific substrates for autophagy, depending on the cell type, and thereby evade and dysregulate the autophagy machinery as reviewed in [228].
The central nervous system is also an important target of HIV-1, and neurological impairment ranging from severe HIV-1 associated dementia in untreated PLWH to minor cognitive disorders in cART-treated PLWH have been described [229,230]. In post-mortem brains from HIV-1 patients with encephalitis, levels of autophagy proteins such as Beclin 1, ATG5, ATG7, and LC3-II were significantly increased, as compared to the brains from HIV-1 positive patients without HIV-1 encephalitis or uninfected controls [224]. In line with this finding, in vitro studies showed that adding the supernatant from HIV-1 infected primary macrophages to human fetal neurons resulted in the increase in autophagy-proteins Beclin-1 and ATG5, but no LC3-ll formation was detected [231]. This suggests that while the early steps of autophagy were promoted in neurons, HIV-1 inhibits the later degradative steps of autophagy leading to protein accumulation and thereby neuronal toxicity. Strikingly, the same study showed that autophagy-inducing rapamycin treatment of neurons resulted in protection against HIV-1 toxicity [231]. Taken together, these data are illustrative of widespread autophagy dysregulation during HIV-1 disease progression. Nevertheless, the in vivo relevancy of autophagy in non-progressor PLWH and the beneficial effects of autophagy inducers in vitro showcase the protective role of autophagy mechanisms in HIV-1 disease progression and comorbidity development, and the therapeutic potential to harness autophagy for HIV-1 management.
6.4. Harnessing Autophagy for HIV-1 Management
As demonstrated by several in vitro and ex vivo studies, boosting autophagy in HIV-1 target cells may be an economically feasible and therapeutically effective way to treat HIV-1 infection. Indeed, autophagy-targeting drugs have already proved effective in intervening in HIV-1 infection in human macrophages, DCs, PBMCs, and CD4+ T cells [164,220,221,222,232]. For example, TLR8-induced autophagy inhibits HIV-1 release by infected human monocyte-derived macrophages via a vitamin-D dependent mechanism, and treatment of human monocyte-derived macrophages with vitamin D promoted autophagy-mediated inhibition of HIV-1 replication [221,233]. Treatment with the autophagy-enhancing peptide Tat-vFLIP-α2 could also initiate autophagy-dependent cell death in HIV-1 infected human macrophages [232]. Similarly, treatment with a Tat-Beclin 1 peptide also induced autophagy and had a protective effect against HIV-1 infection of human monocyte-derived macrophages [234]. Comparable effects have been demonstrated in ex vivo PBMCs and CD4+ T cells derived from HIV-infected individuals, where treatment with the autophagy enhancing drug rapamycin or DIABLO/SMAC mimetics, respectively, reduced HIV-1 replication, or selectively induced killing of latently infected CD4+ T cells [220,222]. Likewise, rapamycin treatment could also reverse the HIV-1 Nef-induced block in autophagosome maturation in cardiomyocytes [225].
Strikingly, we have recently demonstrated that treatment with autophagy-enhancing drugs limits HIV-1 acquisition and suppresses ongoing HIV-1 replication in ex vivo human tissue-derived CD11c+ DCs and CD4+ T cells [164]. These data were also corroborated in vaginal and intestinal tissues. Prophylactic treatment with autophagy-enhancing drugs carbamazepine or everolimus significantly reduced HIV-1 acquisition by subepithelial CD11c+ DCs and CD4+ T cells. Notably, a cell-specific effect of post-infection treatment with autophagy drugs was observed. Treatment with carbamazepine, everolimus, or rapamycin reduced HIV-1 replication in infected ex vivo CD4+ T cells, while only therapeutic rapamycin administration intervened in ongoing HIV-1 infection in CD11c+ DCs. Taken together, these data support harnessing autophagy as a relevant emerging target for HIV-1 therapies [164].
Such autophagy-enhancing drugs may circumvent HIV-1-mediated down-regulation of the autophagy system in distinct HIV-1 target cells without usurping alternative signaling roles of the endogenous proteins. This could permit not only more efficient huTRIM5α-mediated HIV-1 restriction in immune cells such as LCs, which possess an intrinsic capacity for such restriction, but also promote huTRIM5α-mediated HIV-1 restriction in permissive immune cells such as DCs and CD4+ T cells, in which HIV-1 likely circumvents huTRIM5α-mediated restriction by blocking autophagy. Finally, autophagic degradation of non-self peptides is well-established to promote antigen presentation [235,236]. Thus, degradation of HIV-1 via autophagy could potentially promote presentation of HIV-1 specific antigens by DCs, enhancing the HIV-1 specific T-cell adaptive immune response. In summary, the use of autophagy enhancers in combination with current cART therapies may have the potential to both reboot the restrictive capacities of host restriction factors for HIV-1 in primary human immune cells and maximize the antiviral immune response mediated by huTRIM5α, as well as other autophagy-interacting restriction factors.
7. Conclusions and Outlook
To reiterate previous reviews, a silver-bullet strategy for HIV-1 cure is unlikely to work, given the hypervariability of the retrovirus and its many adaptations to evade host immune responses and establish viral reservoirs [17,237]. Rather, we should hedge our bets on exploiting a panel of strategies to eradicate HIV-1, including leveraging natural restriction factors, such as TRIM5α, and harnessing the power of protective host pathways, such as autophagy and the immunoproteasome, to prevent infection and promote innate immune responses. Here, we have provided an overview of the multifaceted functions of TRIM5α, which span from virus sensing and restriction to induction of innate immune responses. We have also outlined the impact of TRIM5α genetic polymorphisms on HIV-1 susceptibility and HIV-1 disease progression and comorbidities of PLWH. We propose a novel conceptualization of TRIM5α-mediated HIV-1 restriction. Until recently, TRIM5α-mediated HIV-1 restriction has primarily been considered to be limited to the rhesus orthologue, which relies on early disintegration of the HIV-1 capsid and subsequently proteasomal degradation to exert its protective function. The demonstrated functionalities of huTRIM5α to prevent LINE-1 retrotransposition, restrict HIV-1 in primary human LCs and in DCs treated with SUMOylation inhibitor, and mediate immunoproteasome-dependent restriction of HIV-1 in CD4+ T cells underpin the intrinsic ability of the human huTRIM5α orthologue to restrict HIV-1 infection [62,64,65,186].
Based on this recent literature, we propose that TRIM5α should be conceptualized as a cell-specific restriction factor with a varied portfolio of protective functions, including functionality as an autophagic effector, innate immune retroviral sensor, promoter of viral degradation, and potentially a linker of innate antiviral and adaptive immunity. We have also expanded on the roles of autophagy in the context of HIV-1, and propose that pharmacological modulation of autophagy mechanisms may be a financially and therapeutically efficacious treatment option in combination with current ART.
Author Contributions
Conceptualization, A.P.M.C. and C.M.S.R.; writing—original draft preparation, A.P.M.C., B.C., and C.M.S.R.; writing—review and editing, A.G.R., A.P.M.C., and C.M.S.R.; supervision, C.M.S.R. All authors have read and agreed to the published version of the manuscript.
Funding
This work was funded by an AMC PhD Scholarship (A.P.M.C.), AMC PhD grant (A.G.R.) and Dutch Research Council (NWO-ZonMw) VIDI grant 91718331 (C.M.S.R.).
Institutional Review Board Statement
Not applicable.
Informed Consent Statement
Not applicable.
Data Availability Statement
No new data were created or analyzed in this study. Data sharing is not applicable to this article.
Acknowledgments
We would like to acknowledge BioRender.com, for providing the software in which figures were constructed. We would also like to acknowledge the valuable input from and discussions with members of the Autophagy-directed Immunity, Host Defense, and Laboratory for Viral Immune Pathogenesis groups from the Department of Experimental Immunology.
Conflicts of Interest
The authors declare no conflict of interest.
References
- World Health Organization. HIV/AIDS Factsheets. Available online: https://www.who.int/news-room/fact-sheets/detail/hiv-aids (accessed on 19 October 2020).
- HIV CAUSAL Collaboration; Ray, M.; Logan, R.; Sterne, J.A.C.; Hernández-Díaz, S.; Robins, J.M.; Sabin, C.; Bansi, L.; van Sighem, A.; de Wolf, F.; et al. The effect of combined antiretroviral therapy on the overall mortality of HIV-infected individuals. AIDS 2010, 24, 123–137. [Google Scholar]
- Jean, M.J.; Fiches, G.; Hayashi, T.; Zhu, J.; Fiches, G. Current strategies for elimination of HIV-1 latent reservoirs using chemical compounds targeting host and viral factors. AIDS Res. Hum. Retrovir. 2019, 35, 1–24. [Google Scholar] [CrossRef]
- Hammer, S.M.; Katzenstein, D.A.; Hughes, M.D.; Gundacker, H.; Schooley, R.T.; Haubrich, R.H.; Henry, W.K.; Lederman, M.M.; Phair, J.P.; Niu, M.T.; et al. A trial comparing nucleoside monotherapy with combination therapy in HIV-infected adults with CD4 cell counts from 200 to 500 per cubic millimeter. N. Engl. J. Med. 1996, 335, 1081–1090. [Google Scholar] [CrossRef]
- Egger, M.; Hirschel, B.; Francioli, P.; Sudre, P.; Wirz, M.; Flepp, M.; Rickenbach, M.; Malinverni, R.; Vernazza, P.; Battegay, M. Impact of new antiretroviral combination therapies in HIV infected patients in Switzerland: Prospective multicentre study. Swiss HIV cohort study. BMJ 1997, 315, 1194–1199. [Google Scholar] [CrossRef] [PubMed]
- Chun, T.; Nickle, D.C.; Justement, J.S.; Meyers, J.H.; Roby, G.; Hallahan, C.W.; Kottilil, S.; Moir, S.; Mican, J.M.; Mullins, J.I.; et al. Persistence of HIV in gut-associated lymphoid tissue despite long-term antiretroviral therapy. J. Infect. Dis. 2008, 197, 714–720. [Google Scholar] [CrossRef] [PubMed]
- Popov, S.; Chenine, A.-L.; Gruber, A.; Li, P.-L.; Ruprecht, R.M. Long-term productive human immunodeficiency virus infection of CD1a-sorted myeloid dendritic cells. J. Virol. 2005, 79, 602–608. [Google Scholar] [CrossRef]
- Finzi, D.; Blankson, J.N.; Siliciano, J.D.; Margolick, J.B.; Chadwick, K.; Pierson, T.C.; Smith, K.; Lisziewicz, J.; Lori, F.; Flexner, C.; et al. Latent infection of CD4+ T cells provides a mechanism for lifelong persistence of HIV-1, even in patients on effective combination therapy. Nat. Med. 1999, 5, 512–517. [Google Scholar] [CrossRef]
- Bruner, K.M.; Hosmane, N.N.; Siliciano, R.F. Towards an HIV-1 cre: Measuring the latent reservoir. Trends Microbiol. 2015, 23, 192–203. [Google Scholar] [CrossRef]
- Mait-Kaufman, J.; Fakioglu, E.; Mesquita, P.M.; Elliott, J.; Lo, Y.; Madan, R.P. Chronic HIV infection is associated with upregulation of proinflammatory cytokine and chemokine and alpha defensin gene expression in colorectal mucosa. AIDS Res. Hum. Retrovir. 2015, 31, 615–622. [Google Scholar] [CrossRef] [PubMed]
- Guaraldi, G.; Orlando, G.; Zona, S.; Menozzi, M.; Carli, F.; Garlassi, E.; Berti, A.; Rossi, E.; Roverato, A.; Palella, F. Premature age-related comorbidities among HIV-infected persons compared with the general population. Clin. Infect. Dis. 2011, 53, 1120–1126. [Google Scholar] [CrossRef]
- Klatt, N.R.; Chomont, N.; Douek, D.C.; Deeks, S.G. Immune activation and HIV persistence: Implications for curative approaches to HIV infection. Immunol. Rev. 2013, 254, 326–342. [Google Scholar] [CrossRef]
- Kruize, Z.; Kootstra, N.A. The role of macrophages in HIV-1 persistence and pathogenesis. Front. Microbiol. 2019, 10, 2828. [Google Scholar] [CrossRef] [PubMed]
- Notario-Pérez, F.; Ruiz-Caro, R.; Veiga-Ochoa, M.-D. Historical development of vaginal microbicides to prevent sexual transmission of HIV in women: From past failures to future hopes. Drug Des. Dev. Ther. 2017, 11, 1767–1787. [Google Scholar] [CrossRef]
- McKinnon, L.R.; Liebenberg, L.J.; Yende-Zuma, N.; Archary, D.; Ngcapu, S.; Sivro, A.; Nagelkerke, N.; Lerma, J.G.G.; Kashuba, A.D.; Masson, L.; et al. Genital inflammation undermines the effectiveness of tenofovir gel in preventing HIV acquisition in women. Nat. Med. 2018, 24, 491–496. [Google Scholar] [CrossRef] [PubMed]
- Klatt, N.R.; Cheu, R.; Birse, K.; Zevin, A.S.; Perner, M.; Noël-Romas, L.; Grobler, A.; Westmacott, G.; Xie, I.Y.; Butler, J.; et al. Vaginal bacteria modify HIV tenofovir microbicide efficacy in African women. Science 2017, 356, 938–945. [Google Scholar] [CrossRef] [PubMed]
- Chan, E.; Towers, G.J.; Qasim, W. Gene therapy strategies to exploit TRIM derived restriction factors against HIV-1. Viruses 2014, 6, 243–263. [Google Scholar] [CrossRef]
- Besnard, E.; Hakre, S.; Kampmann, M.; Lim, H.W.; Hosmane, N.N.; Martin, A.; Bassik, M.C.; Verschueren, E.; Battivelli, E.; Chan, J.; et al. The mTOR Complex Controls HIV Latency. Cell Host Microbe 2016, 20, 785–797. [Google Scholar] [CrossRef] [PubMed]
- Neagu, M.R.; Ziegler, P.; Pertel, T.; Strambio-De-Castillia, C.; Grütter, C.; Martinetti, G.; Mazzucchelli, L.; Grütter, M.; Manz, M.G.; Luban, J. Potent inhibition of HIV-1 by TRIM5-cyclophilin fusion proteins engineered from human components. J. Clin. Investig. 2009, 119, 3035–3047. [Google Scholar] [CrossRef]
- Kaufmann, S.H.E.; Dorhoi, A.; Hotchkiss, R.S.; Bartenschlager, R. Host-directed therapies for bacterial and viral infections. Nat. Rev. Drug Discov. 2018, 17, 35–56. [Google Scholar] [CrossRef]
- Colomer-Lluch, M.; Ruiz, A.; Moris, A.; Prado, J.G. Restriction factors: From intrinsic viral restriction to shaping cellular immunity against HIV-1. Front. Immunol. 2018, 9, 2876. [Google Scholar] [CrossRef]
- Yu, J.; Li, M.; Wilkins, J.; Ding, S.; Swartz, T.H.; Esposito, A.M.; Zheng, Y.-M.; Freed, E.O.; Liang, C.; Chen, B.K.; et al. IFITM proteins restrict HIV-1 infection by antagonizing the envelope glycoprotein. Cell Rep. 2015, 13, 145–156. [Google Scholar] [CrossRef] [PubMed]
- Perez-Caballero, D.; Zang, T.; Ebrahimi, A.; McNatt, M.W.; Gregory, D.A.; Johnson, M.C.; Bieniasz, P.D. Tetherin inhibits HIV-1 release by directly tethering virions to cells. Cell 2009, 139, 499–511. [Google Scholar] [CrossRef] [PubMed]
- Malim, M.H.; Bieniasz, P.D. HIV restriction factors and mechanisms of evasion. Cold Spring Harb. Perspect. Med. 2012, 2, a006940. [Google Scholar] [CrossRef]
- Tada, T.; Zhang, Y.; Koyama, T.; Tobiume, M.; Tsunetsugu-Yokota, Y.; Yamaoka, S.; Fujita, H.; Tokunaga, K. MARCH8 inhibits HIV-1 infection by reducing virion incorporation of envelope glycoproteins. Nat. Med. 2015, 21, 1502–1507. [Google Scholar] [CrossRef]
- O’Connor, C.; Pertel, T.; Gray, S.; Robia, S.L.; Bakowska, J.C.; Luban, J.; Campbell, E.M. p62/Sequestosome-1 associates with and sustains the expression of retroviral restriction factor TRIM5α. J. Virol. 2010, 84, 5997–6006. [Google Scholar] [CrossRef]
- Simon, V.; Bloch, N.; Landau, N.R. Intrinsic host restrictions to HIV-1 and mechanisms of viral escape. Nat. Immunol. 2015, 16, 546–553. [Google Scholar] [CrossRef] [PubMed]
- Briggs, J.A.; Kräusslich, H.-G. The molecular architecture of HIV. J. Mol. Biol. 2011, 410, 491–500. [Google Scholar] [CrossRef] [PubMed]
- Engelman, A.; Cherepanov, P. The structural biology of HIV-1: Mechanistic and therapeutic insights. Nat. Rev. Genet. 2012, 10, 279–290. [Google Scholar] [CrossRef]
- Usami, Y.; Wu, Y.; Göttlinger, H.G. SERINC3 and SERINC5 restrict HIV-1 infectivity and are counteracted by Nef. Nature 2015, 526, 218–223. [Google Scholar] [CrossRef] [PubMed]
- Compton, A.A.; Bruel, T.; Porrot, F.; Mallet, A.; Sachse, M.; Euvrard, M.; Liang, C.; Casartelli, N.; Schwartz, O. IFITM proteins incorporated into HIV-1 virions impair viral fusion and spread. Cell Host Microbe 2014, 16, 736–747. [Google Scholar] [CrossRef]
- Lu, J.; Pan, Q.; Rong, L.; Liu, S.-L.; Liang, C. The IFITM proteins inhibit HIV-1 infection. J. Virol. 2011, 85, 2126–2137. [Google Scholar] [CrossRef]
- Tartour, K.; Appourchaux, R.; Gaillard, J.; Nguyen, X.-N.; Durand, S.; Turpin, J.; Beaumont, E.; Roch, E.; Berger, G.; Mahieux, R.; et al. IFITM proteins are incorporated onto HIV-1 virion particles and negatively imprint their infectivity. Retrovirology 2014, 11, 1–14. [Google Scholar] [CrossRef] [PubMed]
- Hultquist, J.F.; Harris, R.S. Leveraging APOBEC3 proteins to alter the HIV mutation rate and combat AIDS. Future Virol. 2009, 4, 605–619. [Google Scholar] [CrossRef]
- Laguette, N.; Sobhian, B.; Casartelli, N.; Ringeard, M.; Chable-Bessia, C.; Ségéral, E.; Yatim, A.; Emiliani, S.; Schwartz, O.; Benkirane, M. SAMHD1 is the dendritic- and myeloid-cell-specific HIV-1 restriction factor counteracted by Vpx. Nature 2011, 474, 654–657. [Google Scholar] [CrossRef]
- Wu, L. SAMHD1: A new contributor to HIV-1 restriction in resting CD4+T-cells. Retrovirology 2012, 9, 1–5. [Google Scholar] [CrossRef]
- Lahouassa, H.; Daddacha, W.; Hofmann, H.; Ayinde, D.; Logue, E.C.; Dragin, L.; Bloch, N.; Maudet, C.; Bertrand, M.; Gramberg, T.; et al. SAMHD1 restricts the replication of human immunodeficiency virus type 1 by depleting the intracellular pool of deoxynucleoside triphosphates. Nat. Immunol. 2012, 13, 223–228. [Google Scholar] [CrossRef] [PubMed]
- Goujon, C.; Malim, M.H. Characterization of the alpha interferon-induced postentry block to HIV-1 infection in primary human macrophages and T cells. J. Virol. 2010, 84, 9254–9266. [Google Scholar] [CrossRef] [PubMed]
- Fricke, T.; White, T.E.; Schulte, B.; Vieira, D.A.D.S.A.; Dharan, A.; Campbell, E.M.; Brandariz-Nuñez, A.; Diaz-Griffero, F. MxB binds to the HIV-1 core and prevents the uncoating process of HIV-1. Retrovirology 2014, 11, 1–14. [Google Scholar] [CrossRef] [PubMed]
- Li, M.; Kao, E.; Gao, X.; Sandig, H.; Limmer, K.; Pavon-Eternod, M.; Jones, T.E.; Landry, S.; Pan, T.; Weitzman, M.D.; et al. Codon-usage-based inhibition of HIV protein synthesis by human schlafen 11. Nature 2012, 491, 125–128. [Google Scholar] [CrossRef]
- Hotter, D.; Sauter, D.; Kirchhoff, F. Guanylate binding protein 5: Impairing virion infectivity by targeting retroviral envelope glycoproteins. Small GTPases 2017, 8, 31–37. [Google Scholar] [CrossRef] [PubMed]
- Krapp, C.; Hotter, D.; Gawanbacht, A.; McLaren, P.J.; Kluge, S.F.; Stürzel, C.M.; Mack, K.; Reith, E.; Engelhart, S.; Ciuffi, A.; et al. Guanylate binding protein (GBP) 5 is an interferon-inducible inhibitor of HIV-1 infectivity. Cell Host Microbe 2016, 19, 504–514. [Google Scholar] [CrossRef] [PubMed]
- Zhang, Y.; Lu, J.; Liu, X. MARCH2 is upregulated in HIV-1 infection and inhibits HIV-1 production through envelope protein translocation or degradation. Virology 2018, 518, 293–300. [Google Scholar] [CrossRef] [PubMed]
- Van Damme, N.; Goff, D.; Katsura, C.; Jorgenson, R.L.; Mitchell, R.S.; Johnson, M.C.; Stephens, E.B.; Guatelli, J.C. The interferon-induced protein BST-2 restricts HIV-1 release and is downregulated from the cell surface by the viral VPU protein. Cell Host Microbe 2008, 3, 245–252. [Google Scholar] [CrossRef]
- Casartelli, N.; Guivel-Benhassine, F.; Bouziat, R.; Brandler, S.; Schwartz, O.; Moris, A. The antiviral factor APOBEC3G improves CTL recognition of cultured HIV-infected T cells. J. Exp. Med. 2010, 207, 39–49. [Google Scholar] [CrossRef] [PubMed]
- Galão, R.P.; Le Tortorec, A.; Pickering, S.; Kueck, T.; Neil, S.J.D. Innate sensing of HIV-1 assembly by tetherin induces NFκB-dependent proinflammatory responses. Cell Host Microbe 2012, 12, 633–644. [Google Scholar] [CrossRef]
- Ayinde, D.; Bruel, T.; Cardinaud, S.; Porrot, F.; Prado, J.G.; Moris, A.; Schwartz, O. SAMHD1 limits HIV-1 antigen presentation by monocyte-derived dendritic cells. J. Virol. 2015, 89, 6994–7006. [Google Scholar] [CrossRef] [PubMed]
- Li, S.X.; Barrett, B.S.; Guo, K.; Kassiotis, G.; Hasenkrug, K.J.; Dittmer, U.; Gibbert, K.; Santiago, M.L. Tetherin/BST-2 promotes dendritic cell activation and function during acute retrovirus infection. Sci. Rep. 2016, 6, 1–12. [Google Scholar] [CrossRef]
- Pertel, T.; Hausmann, S.; Morger, D.; Züger, S.; Guerra, J.; Lascano, J.; Reinhard, C.; Santoni, F.A.; Uchil, P.D.; Chatel, L.; et al. TRIM5 is an innate immune sensor for the retrovirus capsid lattice. Nature 2011, 472, 361–365. [Google Scholar] [CrossRef]
- Stremlau, M.; Owens, C.M.; Perron, M.J.; Kiessling, M.K.H.; Autissier, P.; Sodroski, J. The cytoplasmic body component TRIM5α restricts HIV-1 infection in Old World monkeys. Nature 2004, 427, 848–853. [Google Scholar] [CrossRef] [PubMed]
- Hofmann, W.; Schubert, D.; LaBonte, J.; Munson, L.; Gibson, S.; Scammell, J.; Ferrigno, P.; Sodroski, J. Species-Specific, Postentry Barriers to Primate Immunodeficiency Virus Infection. J. Virol. 1999, 73, 10020–10028. [Google Scholar] [CrossRef] [PubMed]
- Himathongkham, S.; Luciw, P.A. Restriction of HIV-1 (subtype B) replication at the entry step in rhesus macaque cells. Virology 1996, 219, 485–488. [Google Scholar] [CrossRef]
- Shibata, R.; Sakai, H.; Kawamura, M.; Tokunaga, K.; Adachi, A. Early replication block of human immunodeficiency virus type 1 in monkey cells. J. Gen. Virol. 1995, 76, 2723–2730. [Google Scholar] [CrossRef] [PubMed]
- Owens, C.M.; Yang, P.C.; Göttlinger, H.; Sodroski, J. Human and simian immunodeficiency virus capsid proteins are major viral determinants of early, postentry replication blocks in simian cells. J. Virol. 2003, 77, 726–731. [Google Scholar] [CrossRef]
- Münk, C.; Brandt, S.M.; Lucero, G.; Landau, N.R. A dominant block to HIV-1 replication at reverse transcription in simian cells. Proc. Natl. Acad. Sci. USA 2002, 99, 13843–13848. [Google Scholar] [CrossRef] [PubMed]
- Anderson, J.L.; Campbell, E.M.; Wu, X.; Vandegraaff, N.; Engelman, A.; Hope, T.J. Proteasome inhibition reveals that a functional preintegration complex intermediate can be generated during restriction by diverse TRIM5 proteins. J. Virol. 2006, 80, 9754–9760. [Google Scholar] [CrossRef]
- Danielson, C.M.; Cianci, G.C.; Hope, T.J. Recruitment and dynamics of proteasome association with rhTRIM5α cytoplasmic complexes during HIV-1 infection. Traffic 2012, 13, 1206–1217. [Google Scholar] [CrossRef] [PubMed]
- Diaz-Griffero, F.; Qin, X.-R.; Hayashi, F.; Kigawa, T.; Finzi, A.; Sarnak, Z.; Lienlaf, M.; Yokoyama, S.; Sodroski, J. A B-box 2 surface patch important for TRIM5α self-association, capsid binding avidity, and retrovirus restriction. J. Virol. 2009, 83, 10737–10751. [Google Scholar] [CrossRef] [PubMed]
- Li, X.; Sodroski, J. The TRIM5α B-box 2 domain promotes cooperative binding to the retroviral capsid by mediating higher-order self-association. J. Virol. 2008, 82, 11495–11502. [Google Scholar] [CrossRef]
- Li, Y.-L.; Chandrasekaran, V.; Carter, S.D.; Woodward, C.L.; Christensen, D.E.; Dryden, K.A.; Pornillos, O.; Yeager, M.; Ganser-Pornillos, B.K.; Jensen, G.J.; et al. Primate TRIM5 proteins form hexagonal nets on HIV-1 capsids. eLife 2016, 5, e16269. [Google Scholar] [CrossRef]
- Carthagena, L.; Parise, M.C.; Ringeard, M.; Chelbi-Alix, M.K.; Hazan, U.; Nisole, S. Implication of TRIM alpha and TRIMCyp in interferon-induced anti-retroviral restriction activities. Retrovirology 2008, 5, 59. [Google Scholar] [CrossRef]
- Portilho, D.M.; Fernandez, J.; Ringeard, M.; Machado, A.K.; Boulay, A.; Mayer, M.; Mullertrutwin, M.C.; Beignon, A.-S.; Kirchhoff, F.; Nisole, S.; et al. Endogenous TRIM5α function is regulated by SUMOylation and nuclear sequestration for efficient innate sensing in dendritic cells. Cell Rep. 2016, 14, 355–369. [Google Scholar] [CrossRef]
- Asaoka, K.; Ikeda, K.; Hishinuma, T.; Horie-Inoue, K.; Takeda, S.; Inoue, S. A retrovirus restriction factor TRIM5α is transcriptionally regulated by interferons. Biochem. Biophys. Res. Commun. 2005, 338, 1950–1956. [Google Scholar] [CrossRef]
- Ribeiro, C.M.S.; Sarrami-Forooshani, R.; Setiawan, L.C.; Zijlstra-Willems, E.M.; Van Hamme, J.L.; Tigchelaar, W.; Van Der Wel, N.N.; Kootstra, N.A.; Gringhuis, S.I.; Geijtenbeek, T.B.H. Receptor usage dictates HIV-1 restriction by human TRIM5α in dendritic cell subsets. Nature 2016, 540, 448–452. [Google Scholar] [CrossRef]
- Jimenez-Guardeño, J.M.; Apolonia, L.; Betancor, G.; Malim, M.H. Immunoproteasome activation enables human TRIM5α restriction of HIV-1. Nat. Microbiol. 2019, 4, 933–940. [Google Scholar] [CrossRef]
- Selyutina, A.; Persaud, M.; Simons, L.M.; Bulnes-Ramos, A.; Buffone, C.; Martinez-Lopez, A.; Scoca, V.; Di Nunzio, F.; Hiatt, J.; Marson, A.; et al. Cyclophilin A prevents HIV-1 restriction in lymphocytes by blocking human TRIM5α binding to the viral core. Cell Rep. 2020, 30, 3766–3777.e6. [Google Scholar] [CrossRef]
- Nisole, S.; Stoye, J.P.; Saïb, A. TRIM family proteins: Retroviral restriction and antiviral defence. Nat. Rev. Genet. 2005, 3, 799–808. [Google Scholar] [CrossRef] [PubMed]
- Stremlau, M.; Perron, M.; Welikala, S.; Sodroski, J. Species-specific variation in the B30.2(SPRY) domain of TRIM5α determines the potency of human immunodeficiency virus restriction. J. Virol. 2005, 79, 3139–3145. [Google Scholar] [CrossRef]
- Perez-Caballero, D.; Hatziioannou, T.; Yang, A.; Cowan, S.; Bieniasz, P.D. Human tripartite motif 5α domains responsible for retrovirus restriction activity and specificity. J. Virol. 2005, 79, 8969–8978. [Google Scholar] [CrossRef] [PubMed]
- Diaz-Griffero, F.; Kar, A.; Perron, M.; Xiang, S.-H.; Javanbakht, H.; Li, X.; Sodroski, J. Modulation of retroviral restriction and proteasome inhibitor-resistant turnover by changes in the TRIM5α B-Box 2 domain. J. Virol. 2007, 81, 10362–10378. [Google Scholar] [CrossRef] [PubMed]
- Roganowicz, M.D.; Komurlu, S.; Mukherjee, S.; Plewka, J.; Alam, S.L.; Skorupka, K.A.; Wan, Y.; Dawidowski, D.; Cafiso, D.S.; Ganser-Pornillos, B.K.; et al. TRIM5α SPRY/coiled-coil interactions optimize avid retroviral capsid recognition. PLoS Pathog. 2017, 13, e1006686. [Google Scholar] [CrossRef]
- Ganser-Pornillos, B.K.; Chandrasekaran, V.; Pornillos, O.; Sodroski, J.G.; Sundquist, W.I.; Yeager, M. Hexagonal assembly of a restricting TRIM5 protein. Proc. Natl. Acad. Sci. USA 2010, 108, 534–539. [Google Scholar] [CrossRef] [PubMed]
- Yu, A.; Skorupka, K.A.; Pak, A.J.; Ganser-Pornillos, B.K.; Pornillos, O.; Voth, G.A. TRIM5α self-assembly and compartmentalization of the HIV-1 viral capsid. Nat. Commun. 2020, 11, 1–10. [Google Scholar] [CrossRef] [PubMed]
- Black, L.R.; Aiken, C. TRIM5α Disrupts the structure of assembled HIV-1 capsid complexes in vitro. J. Virol. 2010, 84, 6564–6569. [Google Scholar] [CrossRef] [PubMed]
- Stremlau, M.; Perron, M.; Lee, M.; Li, Y.; Song, B.; Javanbakht, H.; Diaz-Griffero, F.; Anderson, D.J.; Sundquist, W.I.; Sodroski, J. Specific recognition and accelerated uncoating of retroviral capsids by the TRIM5 restriction factor. Proc. Natl. Acad. Sci. USA 2006, 103, 5514–5519. [Google Scholar] [CrossRef] [PubMed]
- Yudina, Z.; Roa, A.; Johnson, R.; Biris, N.; Vieira, D.A.D.S.A.; Tsiperson, V.; Reszka, N.; Taylor, A.B.; Hart, P.J.; Demeler, B.; et al. RING dimerization links higher-order assembly of TRIM5α to synthesis of K63-linked polyubiquitin. Cell Rep. 2015, 12, 788–797. [Google Scholar] [CrossRef]
- Lienlaf, M.; Hayashi, F.; Di Nunzio, F.; Tochio, N.; Kigawa, T.; Yokoyama, S.; Diaz-Griffero, F. Contribution of E3-ubiquitin ligase activity to HIV-1 restriction by TRIM5 rh: Structure of the RING domain of TRIM. J. Virol. 2011, 85, 8725–8737. [Google Scholar] [CrossRef]
- Wu, X.; Anderson, J.L.; Campbell, E.M.; Joseph, A.M.; Hope, T.J. Proteasome inhibitors uncouple rhesus TRIM5 restriction of HIV-1 reverse transcription and infection. Proc. Natl. Acad. Sci. USA 2006, 103, 7465–7470. [Google Scholar] [CrossRef]
- Rold, C.J.; Aiken, C. Proteasomal degradation of TRIM5α during retrovirus restriction. PLoS Pathog. 2008, 4, e1000074. [Google Scholar] [CrossRef]
- Fletcher, A.J.; Vaysburd, M.; Maslen, S.; Zeng, J.; Skehel, J.M.; Towers, G.J.; James, L.C. Trivalent RING assembly on retroviral capsids activates TRIM5 ubiquitination and innate immune signaling. Cell Host Microbe 2018, 24, 761–775.e6. [Google Scholar] [CrossRef]
- Javanbakht, H.; Diaz-Griffero, F.; Stremlau, M.; Si, Z.; Sodroski, J. The contribution of RING and B-box 2 domains to retroviral restriction mediated by monkey TRIM5α. J. Biol. Chem. 2005, 280, 26933–26940. [Google Scholar] [CrossRef] [PubMed]
- Sayah, D.M.; Sokolskaja, E.; Berthoux, L.; Luban, J. Cyclophilin A retrotransposition into TRIM5 explains owl monkey resistance to HIV 1. Nature 2004, 430, 569–573. [Google Scholar] [CrossRef]
- Luban, J.; Bossolt, K.L.; Franke, E.K.; Kalpana, G.V.; Goff, S.P. Human immunodeficiency virus type 1 Gag protein binds to cyclophilins A and B. Cell 1993, 73, 1067–1078. [Google Scholar] [CrossRef]
- Goldstone, D.C.; Yap, M.W.; Robertson, L.E.; Haire, L.F.; Taylor, W.R.; Katzourakis, A.; Stoye, J.P.; Taylor, I.A. Structural and functional analysis of prehistoric lentiviruses uncovers an ancient molecular interface. Cell Host Microbe 2010, 8, 248–259. [Google Scholar] [CrossRef] [PubMed]
- Chan, E.; Schaller, T.; Eddaoudi, A.; Zhan, H.; Tan, C.P.; Jacobsen, M.; Thrasher, A.J.; Towers, G.J.; Qasim, W. Lentiviral gene therapy against human immunodeficiency virus type 1, using a novel human TRIM21-cyclophilin A restriction factor. Hum. Gene Ther. 2012, 23, 1176–1185. [Google Scholar] [CrossRef]
- Newman, R.M.; Hall, L.; Kirmaier, A.; Pozzi, L.-A.; Pery, E.; Farzan, M.; O’Neil, S.P.; Johnson, W. Evolution of a TRIM5-CypA splice isoform in old world monkeys. PLoS Pathog. 2008, 4, e1000003. [Google Scholar] [CrossRef] [PubMed]
- Liu, Z.; Pan, Q.; Liang, Z.; Qiao, W.; Cen, S.; Liang, C. The highly polymorphic cyclophilin A-binding loop in HIV-1 capsid modulates viral resistance to MxB. Retrovirology 2015, 12, 1–6. [Google Scholar] [CrossRef] [PubMed]
- Liu, Z.; Pan, Q.; Ding, S.; Qian, J.; Xu, F.; Zhou, J.; Cen, S.; Guo, F.; Liang, C. The interferon-inducible MxB protein inhibits HIV-1 infection. Cell Host Microbe 2013, 14, 398–410. [Google Scholar] [CrossRef]
- Javanbakht, H.; Diaz-Griffero, F.; Yuan, W.; Yeung, D.F.; Li, X.; Song, B.; Sodroski, J. The ability of multimerized cyclophilin A to restrict retrovirus infection. Virology 2007, 367, 19–29. [Google Scholar] [CrossRef]
- Yoo, S.; Myszka, D.G.; Yeh, C.-Y.; McMurray, M.; Hill, C.P.; Sundquist, W.I. Molecular recognition in the HIV-1 capsid/cyclophilin A complex. J. Mol. Biol. 1997, 269, 780–795. [Google Scholar] [CrossRef]
- Wagner, J.M.; Christensen, D.E.; Bhattacharya, A.; Dawidziak, D.M.; Roganowicz, M.D.; Wan, Y.; Pumroy, R.A.; Demeler, B.; Ivanov, D.N.; Ganser-Pornillos, B.K.; et al. A general model for retroviral capsid pattern recognition by TRIM5 proteins. J. Virol. 2018, 92, e01563-17. [Google Scholar] [CrossRef]
- Price, A.J.; Marzetta, F.; Lammers, M.; Ylinen, L.M.J.; Schaller, T.; Wilson, S.J.; Towers, G.J.; James, L.C. Active site remodeling switches HIV specificity of antiretroviral TRIMCyp. Nat. Struct. Mol. Biol. 2009, 16, 1036–1042. [Google Scholar] [CrossRef]
- Ganser-Pornillos, B.K.; Pornillos, O. Restriction of HIV-1 and other retroviruses by TRIM5. Nat. Rev. Genet. 2019, 17, 546–556. [Google Scholar] [CrossRef]
- Perron, M.J.; Stremlau, M.; Song, B.; Ulm, W.; Mulligan, R.C.; Sodorski, J. TRIM5α mediates the postentry block to N-tropic murine leukemia viruses in human cells. Proc. Natl. Acad. Sci. USA 2004, 101, 11827–11832. [Google Scholar] [CrossRef] [PubMed]
- Sawyer, S.L.; Wu, L.I.; Akey, J.M.; Emerman, M.; Malik, H.S. High-frequency persistence of an impaired allele of the retroviral defense gene TRIM5α in humans. Curr. Biol. 2006, 16, 95–100. [Google Scholar] [CrossRef] [PubMed]
- Ohkura, S.; Yap, M.W.; Sheldon, T.; Stoye, J.P. All three variable regions of the TRIM5α B30.2 domain can contribute to the specificity of retrovirus restriction. J. Virol. 2006, 80, 8554–8565. [Google Scholar] [CrossRef] [PubMed]
- Pham, Q.T.; Bouchard, A.; Grütter, M.G.; Berthoux, L. Generation of human TRIM5α mutants with high HIV-1 restriction activity. Gene Ther. 2010, 17, 859–871. [Google Scholar] [CrossRef] [PubMed]
- Richardson, M.W.; Guo, L.; Xin, F.; Yang, X.; Riley, J.L. Stabilized human TRIM5α protects human T cells from HIV-1 infection. Mol. Ther. 2014, 22, 1084–1095. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Li, Y.; Li, X.; Stremlau, M.; Lee, M.; Sodroski, J. Removal of arginine 332 allows human TRIM5α to bind human immunodeficiency virus capsids and to restrict infection. J. Virol. 2006, 80, 6738–6744. [Google Scholar] [CrossRef]
- OhAinle, M.; Helms, L.; Vermeire, J.; Roesch, F.; Humes, D.; Basom, R.; Delrow, J.J.; Overbaugh, J.; Emerman, M. A virus-packageable CRISPR screen identifies host factors mediating interferon inhibition of HIV. eLife 2018, 7. [Google Scholar] [CrossRef]
- Lu, K.; den Brave, F.; Jentsch, S. Receptor oligomerization guides pathway choice between proteasomal and autophagic degradation. Nat. Cell Biol. 2017, 19, 732–739. [Google Scholar] [CrossRef]
- Shaid, S.; Brandts, C.H.; Serve, H.; Dikic, I. Ubiquitination and selective autophagy. Cell Death Differ. 2012, 20, 21–30. [Google Scholar] [CrossRef]
- Rajalingam, K.; Dikic, I. Expanding the ubiquitin code. Cell 2016, 164, 1074–1074.e1. [Google Scholar] [CrossRef] [PubMed]
- Li, X.; Elmira, E.; Rohondia, S.; Wang, J.; Liu, J.; Dou, Q.P. A patent review of the ubiquitin ligase system: 2015–2018. Expert Opin. Ther. Patents 2018, 28, 919–937. [Google Scholar] [CrossRef]
- Seissler, T.; Marquet, R.; Paillart, J.C. Hijacking of the ubiquitin/proteasome pathway by the hiv auxiliary proteins. Viruses 2017, 9, 322. [Google Scholar] [CrossRef] [PubMed]
- Metzger, M.B.; Pruneda, J.N.; Klevit, R.E.; Weissman, A.M. RING-type E3 ligases: Master manipulators of E2 ubiquitin-conjugating enzymes and ubiquitination. Biochim. Biophys. Acta (BBA) Bioenerg. 2014, 1843, 47–60. [Google Scholar] [CrossRef]
- Tai, H.-C.; Schuman, E.M. Ubiquitin, the proteasome and protein degradation in neuronal function and dysfunction. Nat. Rev. Neurosci. 2008, 9, 826–838. [Google Scholar] [CrossRef] [PubMed]
- Ghosh, R.; Vinod, V.; Simons, J.D.; Boudina, S. Protein and mitochondria quality control mechanisms and cardiac aging. Cells 2020, 9, 933. [Google Scholar] [CrossRef]
- Rojas, V.K.; Park, I.-W. Role of the ubiquitin proteasome system (UPS) in the HIV-1 life cycle. Int. J. Mol. Sci. 2019, 20, 2984. [Google Scholar] [CrossRef] [PubMed]
- Lennemann, N.J.; Coyne, C.B. Catch me if you can: The link between autophagy and viruses. PLoS Pathog. 2015, 11, e1004685. [Google Scholar] [CrossRef]
- Dikic, I. Proteasomal and autophagic degradation systems. Annu. Rev. Biochem. 2017, 86, 193–224. [Google Scholar] [CrossRef]
- Russell, R.C.; Tian, Y.; Yuan, H.; Park, H.W.; Chang, Y.-Y.; Kim, J.; Kim, H.; Neufeld, T.P.; Dillin, A.; Guan, K.-L. ULK1 induces autophagy by phosphorylating Beclin-1 and activating VPS34 lipid kinase. Nat. Cell Biol. 2013, 15, 741–750. [Google Scholar] [CrossRef]
- Kim, J.; Kundu, M.; Viollet, B.; Guan, K.-L. AMPK and mTOR regulate autophagy through direct phosphorylation of Ulk1. Nat. Cell Biol. 2011, 13, 132–141. [Google Scholar] [CrossRef]
- Agrotis, A.; Ketteler, R. On ATG4B as drug target for treatment of solid tumours—The knowns and the unknowns. Cells 2019, 9, 53. [Google Scholar] [CrossRef] [PubMed]
- Hanada, T.; Noda, N.N.; Satomi, Y.; Ichimura, Y.; Fujioka, Y.; Takao, T.; Inagaki, F.; Ohsumi, Y. The Atg12-Atg5 conjugate has a novel E3-like activity for protein lipidation in autophagy. J. Biol. Chem. 2007, 282, 37298–37302. [Google Scholar] [CrossRef]
- Noda, N.N.; Fujioka, Y.; Hanada, T.; Ohsumi, Y.; Inagaki, F. Structure of the Atg12-Atg5 conjugate reveals a platform for stimulating Atg8-PE conjugation. EMBO Rep. 2013, 14, 206–211. [Google Scholar] [CrossRef] [PubMed]
- Kimura, T.; Jia, J.; Claude-Taupin, A.; Kumar, S.; Choi, S.W.; Gu, Y.; Mudd, M.; Dupont, N.; Jiang, S.; Peters, R.; et al. Cellular and molecular mechanism for secretory autophagy. Autophagy 2017, 13, 1084–1085. [Google Scholar] [CrossRef]
- He, C.; Klionsky, D.J. Regulation mechanisms and signaling pathways of autophagy. Annu. Rev. Genet. 2009, 43, 67–93. [Google Scholar] [CrossRef]
- Deretic, V.; Saitoh, T.; Akira, S. Autophagy in infection, inflammation and immunity. Nat. Rev. Immunol. 2013, 13, 722–737. [Google Scholar] [CrossRef] [PubMed]
- Gump, J.M.; Thorburn, A. Sorting cells for basal and induced autophagic flux by quantitative ratiometric flow cytometry. Autophagy 2014, 10, 1327–1334. [Google Scholar] [CrossRef]
- Svenning, S.; Johansen, T. Selective autophagy. Essays Biochem. 2013, 55, 79–92. [Google Scholar] [CrossRef]
- Szalai, P.; Hagen, L.K.; Sætre, F.; Luhr, M.; Sponheim, M.; Øverbye, A.; Mills, I.G.; Seglen, P.O.; Engedal, N. Autophagic bulk sequestration of cytosolic cargo is independent of LC3, but requires GABARAPs. Exp. Cell Res. 2015, 333, 21–38. [Google Scholar] [CrossRef] [PubMed]
- Pankiv, S.; Clausen, T.H.; Lamark, T.; Brech, A.; Bruun, J.-A.; Outzen, H.; Øvervatn, A.; Bjørkøy, G.; Johansen, T. p62/SQSTM1 binds directly to Atg8/LC3 to facilitate degradation of ubiquitinated protein aggregates by autophagy. J. Biol. Chem. 2007, 282, 24131–24145. [Google Scholar] [CrossRef] [PubMed]
- Keown, J.R.; Black, M.M.; Ferron, A.; Yap, M.W.; Barnett, M.J.; Pearce, F.G.; Stoye, J.P.; Goldstone, D.C. A helical LC3-interacting region mediates the interaction between the retroviral restriction factor Trim5α and mammalian autophagy-related ATG8 proteins. J. Biol. Chem. 2018, 293, 18378–18386. [Google Scholar] [CrossRef] [PubMed]
- Kimura, T.; Mandell, M.; Deretic, V. Precision autophagy directed by receptor regulators—Emerging examples within the TRIM family. J. Cell Sci. 2016, 129, 881–891. [Google Scholar] [CrossRef]
- Fletcher, A.J.; Christensen, D.E.; Nelson, C.; Tan, C.P.; Schaller, T.; Lehner, P.J.; Sundquist, W.I.; Towers, G.J. TRIM 5α requires Ube2W to anchor Lys63-linked ubiquitin chains and restrict reverse transcription. EMBO J. 2015, 34, 2078–2095. [Google Scholar] [CrossRef]
- Yamauchi, K.; Wada, K.; Tanji, K.; Tanaka, M.; Kamitani, T. Ubiquitination of E3 ubiquitin ligase TRIM5α and its potential role. FEBS J. 2008, 275, 1540–1555. [Google Scholar] [CrossRef]
- Perez-Caballero, D.; Hatziioannou, T.; Zhang, F.; Cowan, S.; Bieniasz, P.D. Restriction of human immunodeficiency virus type 1 by TRIM-CypA occurs with rapid kinetics and independently of cytoplasmic bodies, ubiquitin, and proteasome activity. J. Virol. 2005, 79, 15567–15572. [Google Scholar] [CrossRef]
- Mandell, M.A.; Jain, A.; Arko-Mensah, J.; Chauhan, S.; Kimura, T.; Dinkins, C.; Silvestri, G.; Münch, J.; Kirchhoff, F.; Simonsen, A.; et al. TRIM proteins regulate autophagy and can target autophagic substrates by direct recognition. Dev. Cell 2014, 30, 394–409. [Google Scholar] [CrossRef]
- Lebovitz, C.B.; DeVorkin, L.; Bosc, D.G.; Rothe, K.; Singh, J.; Bally, M.B.; Jiang, X.; Young, R.N.; Lum, J.J.; Gorski, S.M. Precision autophagy: Will the next wave of selective autophagy markers and specific autophagy inhibitors feed clinical pipelines? Autophagy 2015, 11, 1949–1952. [Google Scholar] [CrossRef]
- Di Rienzo, M.; Romagnoli, A.; Antonioli, M.; Piacentini, M.; Fimia, G.M. TRIM proteins in autophagy: Selective sensors in cell damage and innate immune responses. Cell Death Differ. 2020, 27, 887–902. [Google Scholar] [CrossRef] [PubMed]
- Kimura, T.; Jain, A.; Choi, S.W.; Mandell, M.A.; Schroder, K.; Johansen, T.; Deretic, V. TRIM-mediated precision autophagy targets cytoplasmic regulators of innate immunity. J. Cell Biol. 2015, 210, 973–989. [Google Scholar] [CrossRef]
- Imam, S.; Talley, S.; Nelson, R.S.; Dharan, A.; O’Connor, C.; Hope, T.J.; Campbell, E.M. TRIM5α degradation via autophagy is not required for retroviral restriction. J. Virol. 2016, 90, 3400–3410. [Google Scholar] [CrossRef] [PubMed]
- Carter, S.D.; Mamede, J.I.; Hope, T.J.; Jensen, G.J. Correlated cryogenic fluorescence microscopy and electron cryo-tomography shows that exogenous TRIM5α can form hexagonal lattices or autophagy aggregates in vivo. Proc. Natl. Acad. Sci. USA 2020, 117, 29702–29711. [Google Scholar] [CrossRef] [PubMed]
- Sardiello, M.; Cairo, S.; Fontanella, B.; Ballabio, A.; Meroni, G. Genomic analysis of the TRIM family reveals two groups of genes with distinct evolutionary properties. BMC Evol. Biol. 2008, 8, 225. [Google Scholar] [CrossRef] [PubMed]
- De Witte, L.; Nabatov, A.; Pion, M.; Fluitsma, D.; De Jong, M.A.W.P.; De Gruijl, T.; Piguet, V.; Van Kooyk, Y.; Geijtenbeek, T.B.H. Langerin is a natural barrier to HIV-1 transmission by Langerhans cells. Nat. Med. 2007, 13, 367–371. [Google Scholar] [CrossRef]
- Ribeiro, C.M.S.; Sarrami-Forooshani, R.; Geijtenbeek, T.B.H. HIV-1 border patrols: Langerhans cells control antiviral responses and viral transmission. Future Virol. 2015, 10, 1231–1243. [Google Scholar] [CrossRef]
- Hladik, F.; Sakchalathorn, P.; Ballweber, L.; Lentz, G.; Fialkow, M.; Eschenbach, D.; McElrath, M.J. Initial events in establishing vaginal entry and infection by human immunodeficiency virus type-1. Immunology 2007, 26, 257–270. [Google Scholar] [CrossRef] [PubMed]
- Kawamura, T.; Qualbani, M.; Thomas, E.K.; Orenstein, J.M.; Blauvelt, A. Low levels of productive HIV infection in Langerhans cell-like dendritic cells differentiated in the presence of TGF-β1 and increased viral replication with CD40 ligand-induced maturation. Eur. J. Immunol. 2001, 31, 360–368. [Google Scholar] [CrossRef]
- Valladeau, J.; Ravel, O.; Dezutter-Dambuyant, C.; Moore, K.; Kleijmeer, M.; Liu, Y.; Duvert-Frances, V.; Vincent, C.; Schmitt, D.; Davoust, J.; et al. Langerin, a novel C-type lectin specific to Langerhans cells, is an endocytic receptor that induces the formation of Birbeck granules. Immunity 2000, 12, 71–81. [Google Scholar] [CrossRef]
- Van Der Vlist, M.; Geijtenbeek, T.B.H. Langerin functions as an antiviral receptor on Langerhans cells. Immunol. Cell Biol. 2010, 88, 410–415. [Google Scholar] [CrossRef]
- Berg, L.M.V.D.; Ribeiro, C.M.S.; Zijlstra-Willems, E.M.; De Witte, L.; Fluitsma, D.; Tigchelaar, W.; Everts, V.; Geijtenbeek, T.B.H. Caveolin-1 mediated uptake via langerin restricts HIV-1 infection in human Langerhans cells. Retrovirology 2014, 11, 1–9. [Google Scholar] [CrossRef]
- Czubala, M.A.; Finsterbusch, K.; Ivory, M.O.; Mitchell, J.P.; Ahmed, Z.; Shimauchi, T.; Karoo, R.O.; Coulman, S.A.; Gateley, C.; Birchall, J.C.; et al. TGFβ Induces a SAMHD1-independent post-entry restriction to HIV-1 infection of human epithelial langerhans cells. J. Investig. Dermatol. 2016, 136, 1981–1989. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Hertoghs, N.; Geijtenbeek, T.B.H.; Ribeiro, C.M.S. Interplay between HIV-1 innate sensing and restriction in mucosal dendritic cells: Balancing defense and viral transmission. Curr. Opin. Virol. 2017, 22, 112–119. [Google Scholar] [CrossRef] [PubMed]
- Sakoh-Nakatogawa, M.; Matoba, K.; Asai, E.; Kirisako, H.; Ishii, J.; Noda, N.N.; Inagaki, F.; Nakatogawa, H.; Ohsumi, Y. Atg12–Atg5 conjugate enhances E2 activity of Atg3 by rearranging its catalytic site. Nat. Struct. Mol. Biol. 2013, 20, 433–439. [Google Scholar] [CrossRef]
- Walczak, M.; Martens, S. Dissecting the role of the Atg12-Atg5-Atg16 complex during autophagosome formation. Autophagy 2013, 9, 424–425. [Google Scholar] [CrossRef]
- Gramberg, T.; Soilleux, E.; Fisch, T.; Lalor, P.F.; Hofmann, H.; Wheeldon, S.; Cotterill, A.; Wegele, A.; Winkler, T.; Adams, D.H.; et al. Interactions of LSECtin and DC-SIGN/DC-SIGNR with viral ligands: Differential pH dependence, internalization and virion binding. Virology 2008, 373, 189–201. [Google Scholar] [CrossRef]
- Trifonova, R.T.; Bollman, B.; Barteneva, N.S.; Lieberman, J. Myeloid cells in intact human cervical explants capture HIV and can transmit it to CD4 T cells. Front. Immunol. 2018, 9, 2719. [Google Scholar] [CrossRef]
- Bertram, K.M.; Botting, R.A.; Baharlou, H.; Rhodes, J.W.; Rana, H.; Graham, J.D.; Patrick, E.; Fletcher, J.; Plasto, T.M.; Truong, N.R.; et al. Identification of HIV transmitting CD11c+ human epidermal dendritic cells. Nat. Commun. 2019, 10, 1–15. [Google Scholar] [CrossRef]
- McIlroy, D.; Autran, B.; Cheynier, R.; Wain-Hobson, S.; Clauvel, J.P.; Oksenhendler, E.; Debré, P.; Hosmalin, A. Infection frequency of dendritic cells and CD4+ T lymphocytes in spleens of human immunodeficiency virus-positive patients. J. Virol. 1995, 69, 4737–4745. [Google Scholar] [CrossRef] [PubMed]
- Gringhuis, S.I.; Van Der Vlist, M.; Berg, L.M.V.D.; Dunnen, J.D.; Litjens, M.; Geijtenbeek, T.B.H. HIV-1 exploits innate signaling by TLR8 and DC-SIGN for productive infection of dendritic cells. Nat. Immunol. 2010, 11, 419–426. [Google Scholar] [CrossRef]
- Geijtenbeek, T.B.; Kwon, D.S.; Torensma, R.; Van Vliet, S.J.; Van Duijnhoven, G.C.; Middel, J.; Cornelissen, I.L.; Nottet, H.S.; KewalRamani, V.N.; Littman, D.R.; et al. DC-SIGN, a dendritic cell-specific HIV-1-binding protein that enhances trans-infection of T cells. Cell 2000, 100, 587–597. [Google Scholar] [CrossRef]
- Blanchet, F.P.; Moris, A.; Nikolic, D.S.; Lehmann, M.; Cardinaud, S.; Stalder, R.; Garcia, E.; Dinkins, C.; Leuba, F.; Wu, L.; et al. Human immunodeficiency virus-1 inhibition of immunoamphisomes in dendritic cells impairs early innate and adaptive immune responses. Immunity 2010, 32, 654–669. [Google Scholar] [CrossRef] [PubMed]
- Hertoghs, N.; Nijmeijer, B.M.; Van Teijlingen, N.H.; Fenton-May, A.E.; Kaptein, T.M.; Van Hamme, J.L.; Kappes, J.C.; Kootstra, N.A.; Hahn, B.H.; Borrow, P.; et al. Sexually transmitted founder HIV-1 viruses are relatively resistant to Langerhans cell-mediated restriction. PLoS ONE 2019, 14, e0226651. [Google Scholar] [CrossRef]
- De Jong, M.A.; de Witte, L.; Oudhoff, M.J.; Gringhuis, S.I.; Gallay, P.; Geijtenbeek, T.B. TNF-α and TLR agonists increase susceptibility to HIV-1 transmission by human Langerhans cells ex vivo. J. Clin. Investig. 2008, 118, 3440–3452. [Google Scholar] [CrossRef]
- Hester, R.A.; Kennedy, S.B. Candida infection as a risk factor for HIV transmission. J. Women’s Health 2003, 12, 487–494. [Google Scholar] [CrossRef]
- Fleming, D.T.; Wasserheit, J.N. From epidemiological synergy to public health policy and practice: The contribution of other sexually transmitted diseases to sexual transmission of HIV infection. Sex. Transm. Infect. 1999, 75, 3–17. [Google Scholar] [CrossRef]
- Engering, A.; Geijtenbeek, T.B.; van Vliet, S.J.; Wijers, M.; van Liempt, E.; Demaurex, N.; Lanzavecchia, A.; Fransen, J.; Figdor, C.G.; Piguet, V.; et al. The dendritic cell-specific adhesion receptor DC-SIGN internalizes antigen for fresentation to T cells. J. Immunol. 2002, 168, 2118–2126. [Google Scholar] [CrossRef] [PubMed]
- Cameron, P.U.; Freudenthal, P.S.; Barker, J.M.; Gezelter, S.; Inaba, K.; Steinman, R.M. Dendritic cells exposed to human immunodeficiency virus type-1 transmit a vigorous cytopathic infection to CD4+ T cells. Science 1992, 257, 383–387. [Google Scholar] [CrossRef] [PubMed]
- Pope, M.; Betjes, M.; Romani, N.; Hirmand, H.; Cameron, P.; Hoffman, L.; Gezelter, S.; Schuler, G.; Steinman, R. Conjugates of dendritic cells and memory T lymphocytes from skin facilitate productive infection with HIV-1. Cell 1994, 78, 389–398. [Google Scholar] [CrossRef]
- Smed-Sörensen, A.; Loré, K.; Vasudevan, J.; Louder, M.K.; Andersson, J.; Mascola, J.R.; Spetz, A.-L.; Koup, R.A. Differential susceptibility to human immunodeficiency virus type 1 infection of myeloid and plasmacytoid dendritic cells. J. Virol. 2005, 79, 8861–8869. [Google Scholar] [CrossRef]
- Gringhuis, S.I.; den Dunnen, J.; Litjens, M.; van Het Hof, B.; van Kooyk, Y.; Geijtenbeek, T.B. C-type lectin DC-SIGN modulates toll-like receptor signaling via Raf-1 kinase-dependent acetylation of transcription factor NF-κB. Immunity 2007, 26, 605–616. [Google Scholar] [CrossRef]
- Gringhuis, S.I.; Dunnen, J.D.; Litjens, M.; Van Der Vlist, M.; Geijtenbeek, T.B.H. Carbohydrate-specific signaling through the DC-SIGN signalosome tailors immunity to Mycobacterium tuberculosis, HIV-1 and Helicobacter pylori. Nat. Immunol. 2009, 10, 1081–1088. [Google Scholar] [CrossRef]
- Cloherty, A.P.M.; van Teijlingen, N.H.; Eisden, T.T.H.D.; van Hamme, J.L.; Rader, A.G.; Geijtenbeek, T.B.H.; Schreurs, R.R.C.E.; Ribeiro, C.M.S. Autophagy-enhancing drugs limit mucosal HIV-1 acquisition and suppress viral replication ex vivo. Sci. Rep. 2021, 11, 4767. [Google Scholar] [CrossRef] [PubMed]
- Kim, K.; Dauphin, A.; Komurlu, S.; McCauley, S.M.; Yurkovetskiy, L.; Carbone, C.; Diehl, W.E.; Strambio-De-Castillia, C.; Campbell, E.M.; Luban, J. Cyclophilin A protects HIV-1 from restriction by human TRIM5α. Nat. Microbiol. 2019, 4, 2044–2051. [Google Scholar] [CrossRef] [PubMed]
- Thali, M.; Bukovsky, A.A.; Kondo, E.; Rosenwlrth, B.; Walsh, C.T.; Sodroski, J.; Göttlinger, H.G. Functional association of cyclophilin A with HIV-1 virions. Nature 1994, 372, 363–365. [Google Scholar] [CrossRef]
- Gamble, T.R.; Vajdos, F.F.; Yoo, S.; Worthylake, D.K.; Houseweart, M.; Sundquist, W.I.; Hill, C.P. Crystal structure of human cyclophilin A bound to the amino-terminal domain of HIV-1 capsid. Cell 1996, 87, 1285–1294. [Google Scholar] [CrossRef]
- Jin, C.; Li, J.; Cheng, L.; Liu, F.; Wu, N. Gp120 binding with DC-SIGN induces reactivation of HIV-1 provirus via the NF-κB signaling pathway. Acta Biochim. Biophys. Sin. 2015, 48, 275–281. [Google Scholar] [CrossRef]
- Arhel, N.J.; Nisole, S.; Carthagena, L.; Coutant, F.; Souque, P.; Brussel, A.; Estaquier, J.; Charneau, P. Lack of endogenous TRIM5α-mediated restriction in rhesus macaque dendritic cells. Blood 2008, 112, 3772–3776. [Google Scholar] [CrossRef]
- Sattentau, Q.J.; Stevenson, M. Macrophages and HIV-1: An unhealthy constellation. Cell Host Microbe 2016, 19, 304–310. [Google Scholar] [CrossRef]
- Haldar, M.; Murphy, K.M. Origin, development, and homeostasis of tissue-resident macrophages. Immunol. Rev. 2014, 262, 25–35. [Google Scholar] [CrossRef] [PubMed]
- Hirayama, D.; Iida, T.; Nakase, H. The phagocytic function of macrophage-enforcing innate immunity and tissue homeostasis. Int. J. Mol. Sci. 2017, 19, 92. [Google Scholar] [CrossRef]
- Lopez, P.; Koh, W.H.; Hnatiuk, R.; Murooka, T.T. HIV infection stabilizes macrophage-T cell interactions to promote cell-cell HIV spread. J. Virol. 2019, 93, 805–819. [Google Scholar] [CrossRef]
- Carr, J.; Hocking, H.; Li, P.; Burrell, C. Rapid and efficient cell-to-cell transmission of human immunodeficiency virus infection from monocyte-derived macrophages to peripheral blood lymphocytes. Virology 1999, 265, 319–329. [Google Scholar] [CrossRef]
- Duncan, C.J.A.; Russell, R.A.; Sattentau, Q.J. High multiplicity HIV-1 cell-to-cell transmission from macrophages to CD4+ T cells limits antiretroviral efficacy. AIDS 2013, 27, 2201–2206. [Google Scholar] [CrossRef]
- Kyei, G.B.; Dinkins, C.; Davis, A.S.; Roberts, E.; Singh, S.B.; Dong, C.; Wu, L.; Kominami, E.; Ueno, T.; Yamamoto, A.; et al. Autophagy pathway intersects with HIV-1 biosynthesis and regulates viral yields in macrophages. J. Cell Biol. 2009, 186, 255–268. [Google Scholar] [CrossRef] [PubMed]
- Sagnier, S.; Daussy, C.F.; Borel, S.; Robert-Hebmann, V.; Faure, M.; Blanchet, F.P.; Beaumelle, B.; Biard-Piechaczyk, M.; Espert, L. Autophagy restricts HIV-1 infection by selectively degrading TAT in CD4+T lymphocytes. J. Virol. 2015, 89, 615–625. [Google Scholar] [CrossRef]
- Campbell, G.R.; Rawat, P.; Bruckman, R.S.; Spector, S.A. Human immunodeficiency virus type 1 Nef inhibits autophagy through transcription factor EB sequestration. PLoS Pathog. 2015, 11, e1005018. [Google Scholar] [CrossRef] [PubMed]
- Di Malta, C.; Cinque, L.; Settembre, C. Transcriptional regulation of autophagy: Mechanisms and diseases. Front. Cell Dev. Biol. 2019, 7, 114. [Google Scholar] [CrossRef] [PubMed]
- Chang, C.; Young, L.N.; Morris, K.L.; Von Bülow, S.; Schöneberg, J.; Yamamoto-Imoto, H.; Oe, Y.; Yamamoto, K.; Nakamura, S.; Stjepanovic, G.; et al. Bidirectional control of autophagy by BECN1 BARA domain dynamics. Mol. Cell 2019, 73, 339–353.e6. [Google Scholar] [CrossRef] [PubMed]
- Castro-Gonzalez, S.; Shi, Y.; Colomer-Lluch, M.; Song, Y.; Mowery, K.; Almodovar, S.; Bansal, A.; Kirchhoff, F.; Sparrer, K.; Liang, C.; et al. HIV-1 Nef counteracts autophagy restriction by enhancing the association between BECN1 and its inhibitor BCL2 in a PRKN-dependent manner. Autophagy 2020, 1–25. [Google Scholar] [CrossRef]
- Veillette, M.; Bichel, K.; Pawlica, P.; Freund, S.M.V.; Plourde, M.B.; Pham, Q.T.; Reyes-Moreno, C.; James, L.C.; Berthoux, L. The V86M mutation in HIV-1 capsid confers resistance to TRIM5α by abrogation of cyclophilin a-dependent restriction and enhancement of viral nuclear import. Retrovirology 2013, 10, 25. [Google Scholar] [CrossRef]
- Trifonova, R.T.; Lieberman, J.; Van Baarle, D. Distribution of immune cells in the human cervix and implications for HIV transmission. Am. J. Reprod. Immunol. 2014, 71, 252–264. [Google Scholar] [CrossRef]
- Borel, S.; Robert-Hebmann, V.; AlFaisal, J.; Jain, A.; Faure, M.; Espert, L.; Chaloin, L.; Paillart, J.-C.; Johansen, T.; Biard-Piechaczyk, M. HIV-1 viral infectivity factor interacts with microtubule-associated protein light chain 3 and inhibits autophagy. AIDS 2015, 29, 275–286. [Google Scholar] [CrossRef]
- Sanfridson, A.; Hester, S.; Doyle, C. Nef proteins encoded by human and simian immunodeficiency viruses induce the accumulation of endosomes and lysosomes in human T cells. Proc. Natl. Acad. Sci. USA 1997, 94, 873–878. [Google Scholar] [CrossRef] [PubMed]
- Volkmann, B.; Wittmann, S.; Lagisquet, J.; Deutschmann, J.; Eissmann, K.; Ross, J.J.; Biesinger, B.; Gramberg, T. Human TRIM5α senses and restricts LINE-1 elements. Proc. Natl. Acad. Sci. USA 2020, 117, 17965–17976. [Google Scholar] [CrossRef] [PubMed]
- Baldauf, H.-M.; Pan, X.; Erikson, E.; Schmidt, S.; Daddacha, W.; Burggraf, M.; Schenkova, K.; Ambiel, I.; Wabnitz, G.H.; Gramberg, T.; et al. SAMHD1 restricts HIV-1 infection in resting CD4+ T cells. Nat. Med. 2012, 18, 1682–1688. [Google Scholar] [CrossRef] [PubMed]
- Waheed, A.A.; Swiderski, M.; Khan, A.; Gitzen, A.; Majadly, A.; Freed, E.O. The viral protein U (VPU)-interacting host protein ATP6V0C down-regulates cell-surface expression of tetherin and thereby contributes to HIV-1 release. J. Biol. Chem. 2020, 295, 7327–7340. [Google Scholar] [CrossRef]
- Blanchet, F.P.; Mitchell, J.P.; Piguet, V. Beta-TrCP dependency of HIV-1 VPU-induced downregulation of CD4 and BST-2/Tetherin. Curr. HIV Res. 2012, 10, 307–314. [Google Scholar] [CrossRef]
- Miyakawa, K.; Ryo, A.; Murakami, T.; Ohba, K.; Yamaoka, S.; Fukuda, M.; Guatelli, J.; Yamamoto, N. BCA2/Rabring7 promotes tetherin-dependent HIV-1 restriction. PLoS Pathog. 2009, 5, e1000700. [Google Scholar] [CrossRef] [PubMed]
- Zou, J.; Li, W.; Misra, A.; Yue, F.; Song, K.; Chen, Q.; Guo, G.; Yi, J.; Kimata, J.T.; Liu, L. The viral restriction factor tetherin prevents leucine-rich pentatricopeptide repeat-containing protein (LRPPRC) from association with beclin 1 and B-cell CLL/lymphoma 2 (Bcl-2) and enhances autophagy and mitophagy. J. Biol. Chem. 2015, 290, 7269–7279. [Google Scholar] [CrossRef]
- Jin, S.; Tian, S.; Luo, M.; Xie, W.; Liu, T.; Duan, T.; Wu, Y.; Cui, J. Tetherin suppresses type I interferon signaling by targeting MAVS for NDP52-mediated selective autophagic degradation in human cells. Mol. Cell 2017, 68, 308–322.e4. [Google Scholar] [CrossRef]
- Tareen, S.U.; Emerman, M. Human Trim5α has additional activities that are uncoupled from retroviral capsid recognition. Virology 2011, 409, 113–120. [Google Scholar] [CrossRef] [PubMed]
- Saha, B.; Chisholm, D.; Kell, A.M.; Mandell, M.A. A non-canonical role for the autophagy machinery in anti-retroviral signaling mediated by TRIM5α. PLoS Pathog. 2020, 16, e1009017. [Google Scholar] [CrossRef]
- Cheney, K.M.; McKnight, Á. Interferon-alpha mediates restriction of human immunodeficiency virus type-1 replication in primary human macrophages at an early stage of replication. PLoS ONE 2010, 5, e13521. [Google Scholar] [CrossRef] [PubMed]
- Barr, S.D.; Smiley, J.R.; Bushman, F.D. The interferon response inhibits HIV particle production by induction of TRIM22. PLoS Pathog. 2008, 4, e1000007. [Google Scholar] [CrossRef] [PubMed]
- Chen, K.; Huang, J.; Zhang, C.; Huang, S.; Nunnari, G.; Wang, F.-X.; Tong, X.; Gao, L.; Nikisher, K.; Zhang, H. Alpha interferon potently enhances the anti-human immunodeficiency virus type 1 activity of APOBEC3G in resting primary CD4 T Cells. J. Virol. 2006, 80, 7645–7657. [Google Scholar] [CrossRef]
- Iwasaki, A. Innate immune recognition of HIV-1. Immunity 2012, 37, 389–398. [Google Scholar] [CrossRef]
- Lascano, J.; Uchil, P.D.; Mothes, W.; Luban, J. TRIM5 retroviral restriction activity correlates with the ability to induce innate immune signaling. J. Virol. 2015, 90, 308–316. [Google Scholar] [CrossRef] [PubMed]
- Javanbakht, H.; An, P.; Gold, B.; Petersen, D.C.; O’Huigin, C.; Nelson, G.W.; O’Brien, S.J.; Kirk, G.D.; Detels, R.; Buchbinder, S.; et al. Effects of human TRIM5α polymorphisms on antiretroviral function and susceptibility to human immunodeficiency virus infection. Virology 2006, 354, 15–27. [Google Scholar] [CrossRef] [PubMed]
- Price, H.; Lacap, P.; Tuff, J.; Wachihi, C.; Kimani, J.; Ball, T.B.; Luo, M.; Plummer, F.A. A TRIM5α exon 2 polymorphism is associated with protection from HIV-1 infection in the Pumwani sex worker cohort. AIDS 2010, 24, 1813–1821. [Google Scholar] [CrossRef] [PubMed]
- Da Silva, R.C.; Coelho, A.V.C.; Arraes, L.C.; Brandão, L.A.C.; Crovella, S.; Guimarães, R.L. TRIM5 gene polymorphisms in HIV-1-infected patients and healthy controls from Northeastern Brazil. Immunol. Res. 2016, 64, 1237–1242. [Google Scholar] [CrossRef]
- Speelmon, E.C.; Livingston-Rosanoff, D.; Li, S.S.; Vu, Q.; Bui, J.; Geraghty, D.E.; Zhao, L.P.; McElrath, M.J. Genetic association of the antiviral restriction factor TRIM5α with human immunodeficiency virus type 1 infection. J. Virol. 2006, 80, 2463–2471. [Google Scholar] [CrossRef]
- Nakajima, T.; Nakayama, E.E.; Kaur, G.; Terunuma, H.; Mimaya, J.-I.; Ohtani, H.; Mehra, N.; Shioda, T.; Kimura, A. Impact of novel TRIM5α variants, Gly110Arg and G176del, on the anti-HIV-1 activity and the susceptibility to HIV-1 infection. AIDS 2009, 23, 2091–2100. [Google Scholar] [CrossRef]
- Liu, F.-L.; Qiu, Y.-Q.; Li, H.; Kuang, Y.-Q.; Tang, X.; Cao, G.; Tang, N.L.S.; Zheng, Y.-T. An HIV-1 resistance polymorphism in TRIM5α gene among chinese intravenous drug users. J. Acquir. Immune Defic. Syndr. (JAIDS) 2011, 56, 306–311. [Google Scholar] [CrossRef]
- Van Manen, D.; Rits, M.A.N.; Beugeling, C.; Van Dort, K.; Schuitemaker, H.; Kootstra, N.A. The effect of Trim5 polymorphisms on the clinical course of HIV-1 infection. PLoS Pathog. 2008, 4, e18. [Google Scholar] [CrossRef]
- Nakayama, E.E.; Nakajima, T.; Kaur, G.; Mimaya, J.-I.; Terunuma, H.; Mehra, N.; Kimura, A.; Shioda, T. A naturally occurring single amino acid substitution in human TRIM5α linker region affects its anti-HIV type 1 activity and susceptibility to HIV type 1 infection. AIDS Res. Hum. Retrovir. 2013, 29, 919–924. [Google Scholar] [CrossRef] [PubMed]
- Singh, H.; Samani, D.; Ghate, M.V.; Gangakhedkar, R.R. Impact of cellular restriction gene (TRIM5α, BST-2) polymorphisms on the acquisition of HIV-1 and disease progression. J. Gene Med. 2018, 20, e3004. [Google Scholar] [CrossRef]
- Ovsyannikova, I.G.; Haralambieva, I.H.; Dhiman, N.; O’Byrne, M.M.; Pankratz, V.S.; Jacobson, R.M.; Poland, G.A. Polymorphisms in the vitamin A receptor and innate immunity genes influence the antibody response to rubella vaccination. J. Infect. Dis. 2010, 201, 207–213. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Ovsyannikova, I.G.; Haralambieva, I.H.; Vierkant, R.A.; O’Byrne, M.M.; Poland, G.A. Associations between polymorphisms in the antiviral TRIM genes and measles vaccine immunity. Hum. Immunol. 2013, 74, 768–774. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Mobasheri, S.; Irani, N.; Sepahi, A.A.; Sakhaee, F.; Jamnani, F.R.; Vaziri, F.; Siadat, S.D.; Fateh, A. Evaluation of TRIM5 and TRIM22 polymorphisms on treatment responses in Iranian patients with chronic hepatitis C virus infection. Gene 2018, 676, 95–100. [Google Scholar] [CrossRef]
- Medrano, L.M.; Rallón, N.; Berenguer, J.; Jiménez-Sousa, M.Á.; Soriano, V.; Aldámiz-Echevarria, T.; Fernández-Rodríguez, A.; García, M.; Tejerina, F.; Martinez, I.; et al. Relationship of TRIM5 and TRIM22 polymorphisms with liver disease and HCV clearance after antiviral therapy in HIV/HCV coinfected patients. J. Transl. Med. 2016, 14, 257. [Google Scholar] [CrossRef]
- Abdel-Mohsen, M.; Wang, C.; Strain, M.C.; Lada, S.M.; Deng, X.; Cockerham, L.R.; Pilcher, C.D.; Hecht, F.M.; Liegler, T.; Richman, D.D.; et al. Select host restriction factors are associated with HIV persistence during antiretroviral therapy. AIDS 2015, 29, 411–420. [Google Scholar] [CrossRef]
- Raposo, R.A.S.; Abdel-Mohsen, M.; Deng, X.; Hecht, F.M.; Pilcher, C.D.; Pillai, S.K.; Nixon, D.F. Dynamic regulation of host restriction factor expression over the course of HIV-1 infection in vivo. J. Virol. 2014, 88, 11624–11629. [Google Scholar] [CrossRef] [PubMed]
- Kimura, T.; Jain, A.; Choi, S.W.; Mandell, M.A.; Johansen, T.; Deretic, V. TRIM-directed selective autophagy regulates immune activation. Autophagy 2017, 13, 989–990. [Google Scholar] [CrossRef]
- Yap, M.W.; Dodding, M.P.; Stoye, J.P. Trim-cyclophilin A fusion proteins can restrict human immunodeficiency virus type 1 infection at two distinct phases in the viral life cycle. J. Virol. 2006, 80, 4061–4067. [Google Scholar] [CrossRef]
- Walker, J.E.; Chen, R.X.; McGee, J.; Nacey, C.; Pollard, R.B.; Abedi, M.; Bauer, G.; Nolta, J.A.; Anderson, J.S. Generation of an HIV-1-resistant immune system with CD34+ hematopoietic stem cells transduced with a triple-combination anti-HIV lentiviral vector. J. Virol. 2012, 86, 5719–5729. [Google Scholar] [CrossRef]
- Anderson, J.; Akkina, R. Human immunodeficiency virus type 1 restriction by human—Rhesus chimeric tripartite motif 5α (TRIM5α) in CD34+ cell-derived macrophages in vitro and in T cells in vivo in severe combined immunodeficient (SCID-hu) mice transplanted with human fetal tissue. Hum. Gene Ther. 2008, 19, 217–228. [Google Scholar] [CrossRef]
- Morgan, R.A.; Gray, D.; Lomova, A.; Kohn, D.B. Hematopoietic stem cell gene therapy: Progress and lessons learned. Cell Stem Cell 2017, 21, 574–590. [Google Scholar] [CrossRef] [PubMed]
- Nardacci, R.; Amendola, A.; Ciccosanti, F.; Corazzari, M.; Esposito, V.; Vlassi, C.; Taibi, C.; Fimia, G.M.; Del Nonno, F.; Ippolito, G.; et al. Autophagy plays an important role in the containment of HIV-1 in nonprogressor-infected patients. Autophagy 2014, 10, 1167–1178. [Google Scholar] [CrossRef]
- Campbell, G.R.; Spector, S.A. Vitamin D inhibits human immunodeficiency virus type 1 and mycobacterium tuberculosis infection in macrophages through the induction of autophagy. PLoS Pathog. 2012, 8, e1002689. [Google Scholar] [CrossRef] [PubMed]
- Campbell, G.R.; Bruckman, R.S.; Chu, Y.-L.; Trout, R.N.; Spector, S.A. SMAC mimetics induce autophagy-dependent apoptosis of HIV-1-infected resting memory CD4+ T Cells. Cell Host Microbe 2018, 24, 689–702.e7. [Google Scholar] [CrossRef]
- Espert, L.; Varbanov, M.; Robert-Hebmann, V.; Sagnier, S.; Robbins, I.; Sanchez, F.; Lafont, V.; Biard-Piechaczyk, M. Differential role of autophagy in CD4 T cells and macrophages during X4 and R5 HIV-1 infection. PLoS ONE 2009, 4, e5787. [Google Scholar] [CrossRef] [PubMed]
- Zhou, D.; Masliah, E.; Spector, S.A. Autophagy is increased in postmortem brains of persons with HIV-1-associated encephalitis. J. Infect. Dis. 2011, 203, 1647–1657. [Google Scholar] [CrossRef] [PubMed]
- Gupta, M.K.; Kaminski, R.; Mullen, B.; Gordon, J.; Burdo, T.H.; Cheung, J.Y.; Feldman, A.M.; Madesh, M.; Khalili, K. HIV-1 Nef-induced cardiotoxicity through dysregulation of autophagy. Sci. Rep. 2017, 7, 1–15. [Google Scholar] [CrossRef] [PubMed]
- Remick, J.; Georgiopoulou, V.; Marti, C.; Ofotokun, I.; Kalogeropoulos, A.; Lewis, W.; Butler, J. Heart failure in patients with human immunodeficiency virus infection: Epidemiology, pathophysiology, treatment, and future research. Circulation 2014, 129, 1781–1789. [Google Scholar] [CrossRef]
- Tahrir, F.G.; Shanmughapriya, S.; Ahooyi, T.M.; Knezevic, T.; Gupta, M.K.; Kontos, C.D.; McClung, J.M.; Madesh, M.; Gordon, J.; Feldman, A.M.; et al. Dysregulation of mitochondrial bioenergetics and quality control by HIV-1 Tat in cardiomyocytes. J. Cell. Physiol. 2018, 233, 748–758. [Google Scholar] [CrossRef] [PubMed]
- Nardacci, R.; Ciccosanti, F.; Marsella, C.; Ippolito, G.; Piacentini, M.; Fimia, G.M. Role of autophagy in HIV infection and pathogenesis. J. Intern. Med. 2017, 281, 422–432. [Google Scholar] [CrossRef]
- Brew, B.J.; Chan, P. Update on HIV dementia and HIV-associated neurocognitive disorders. Curr. Neurol. Neurosci. Rep. 2014, 14, 468. [Google Scholar] [CrossRef]
- Clifford, D.B.; Ances, B.M. HIV-associated neurocognitive disorder. Lancet Infect. Dis. 2013, 13, 976–986. [Google Scholar] [CrossRef]
- Mehla, R.; Chauhan, A. HIV-1 differentially modulates autophagy in neurons and astrocytes. J. Neuroimmunol. 2015, 285, 106–118. [Google Scholar] [CrossRef]
- Zhang, G.; Luk, B.T.; Hamidy, M.; Zhang, L.; Spector, S.A. Induction of a Na+/K+-ATPase-dependent form of autophagy triggers preferential cell death of human immunodeficiency virus type-1-infected macrophages. Autophagy 2018, 14, 1359–1375. [Google Scholar] [CrossRef] [PubMed]
- Campbell, G.R.; Spector, S.A. Toll-like receptor 8 ligands activate a vitamin D mediated autophagic response that inhibits human immunodeficiency virus type 1. PLoS Pathog. 2012, 8, e1003017. [Google Scholar] [CrossRef]
- Shoji-Kawata, S.; Sumpter, R.; Leveno, M.; Campbell, G.R.; Zou, Z.; Kinch, L.N.; Wilkins, A.D.; Sun, Q.; Pallauf, K.; MacDuff, D.; et al. Identification of a candidate therapeutic autophagy-inducing peptide. Nature 2013, 494, 201–206. [Google Scholar] [CrossRef]
- Coulon, P.-G.; Richetta, C.; Rouers, A.; Blanchet, F.P.; Urrutia, A.; Guerbois, M.; Piguet, V.; Theodorou, I.; Bet, A.; Schwartz, O.; et al. HIV-infected dendritic cells present endogenous MHC class II—Restricted antigens to HIV-specific CD4+ T cells. J. Immunol. 2016, 197, 517–532. [Google Scholar] [CrossRef] [PubMed]
- Chemali, M.; Radtke, K.; Desjardins, M.; English, L. Alternative pathways for MHC class I presentation: A new function for autophagy. Cell. Mol. Life Sci. 2011, 68, 1533–1541. [Google Scholar] [CrossRef]
- Harris, R.S.; Hultquist, J.F.; Evans, D.T. The restriction factors of human immunodeficiency virus. J. Biol. Chem. 2012, 287, 40875–40883. [Google Scholar] [CrossRef] [PubMed]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).