Influence of Hospital Environmental Variables on Thermometric Measurements and Level of Concordance: A Cross-Sectional Descriptive Study
Abstract
1. Introduction
2. Materials and Methods
2.1. Design and Context
2.2. Setting
2.3. Participants
2.4. Variables
2.5. Data Sources and Measurement
2.6. Study Size
2.7. Statistical Methods
2.8. Ethical Considerations
3. Results
3.1. Sample Characteristics
3.2. Environmental Characteristics
3.3. Descriptive Statistics
3.4. Relationship between the Age and Gender of the Participants and Body Temperature
3.5. Relationship of Patient Bed Location to Body Temperature and Environmental Variables
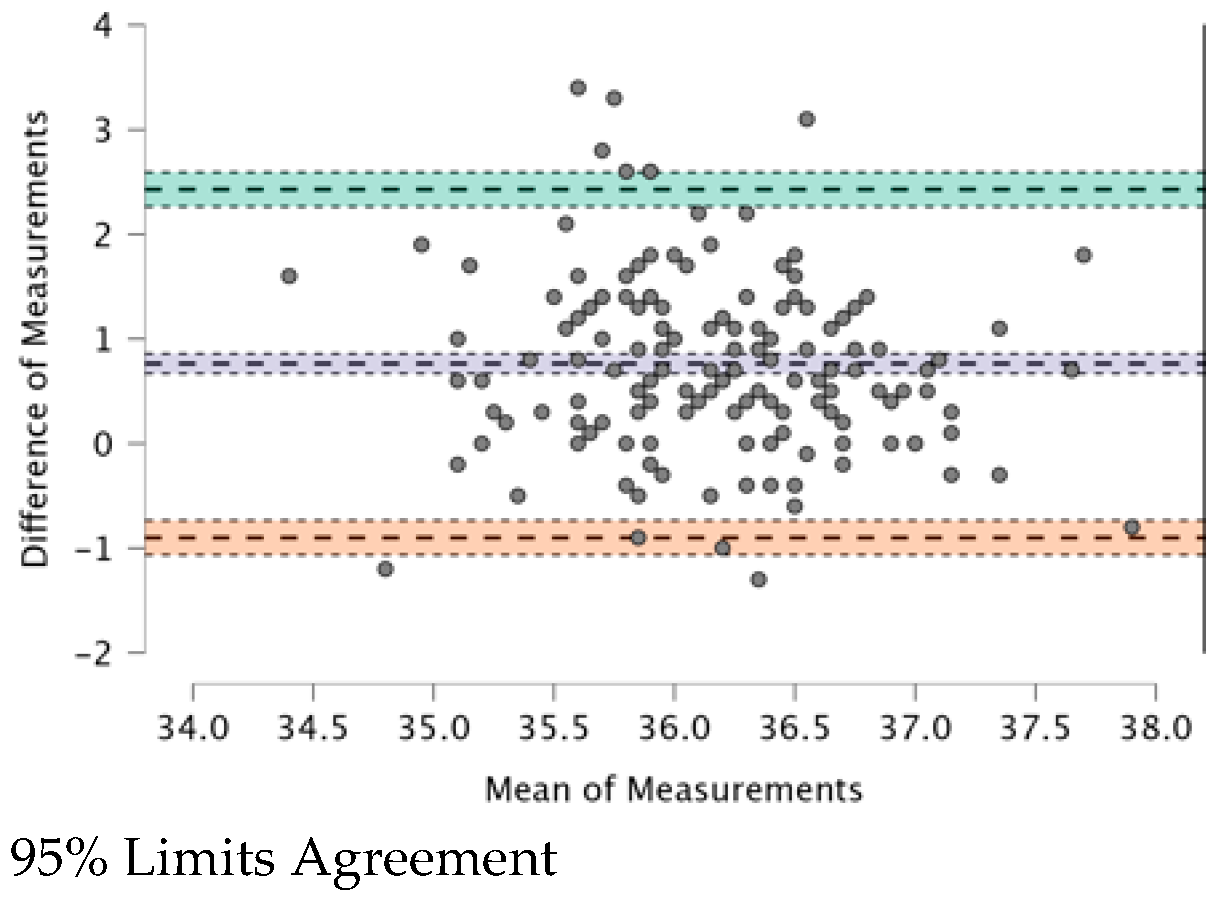
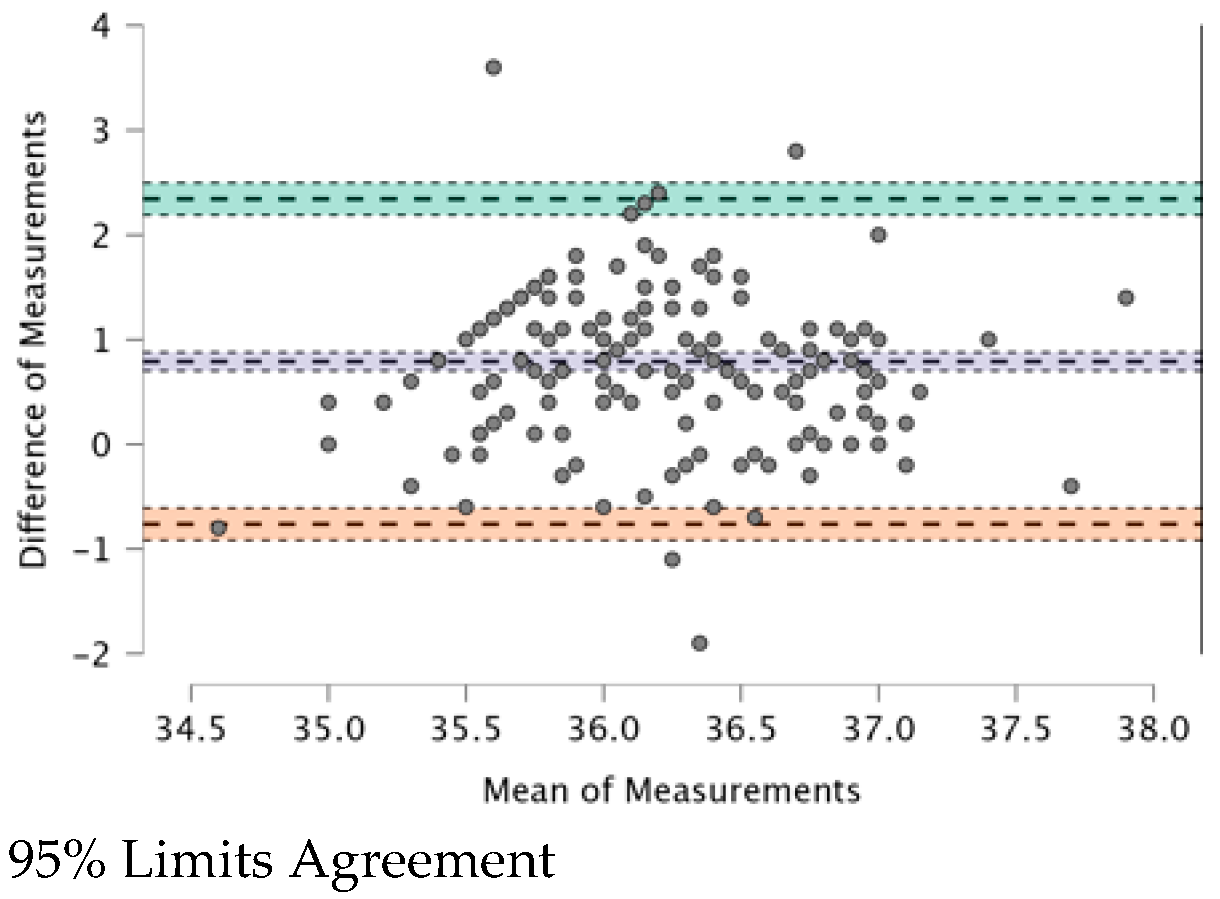
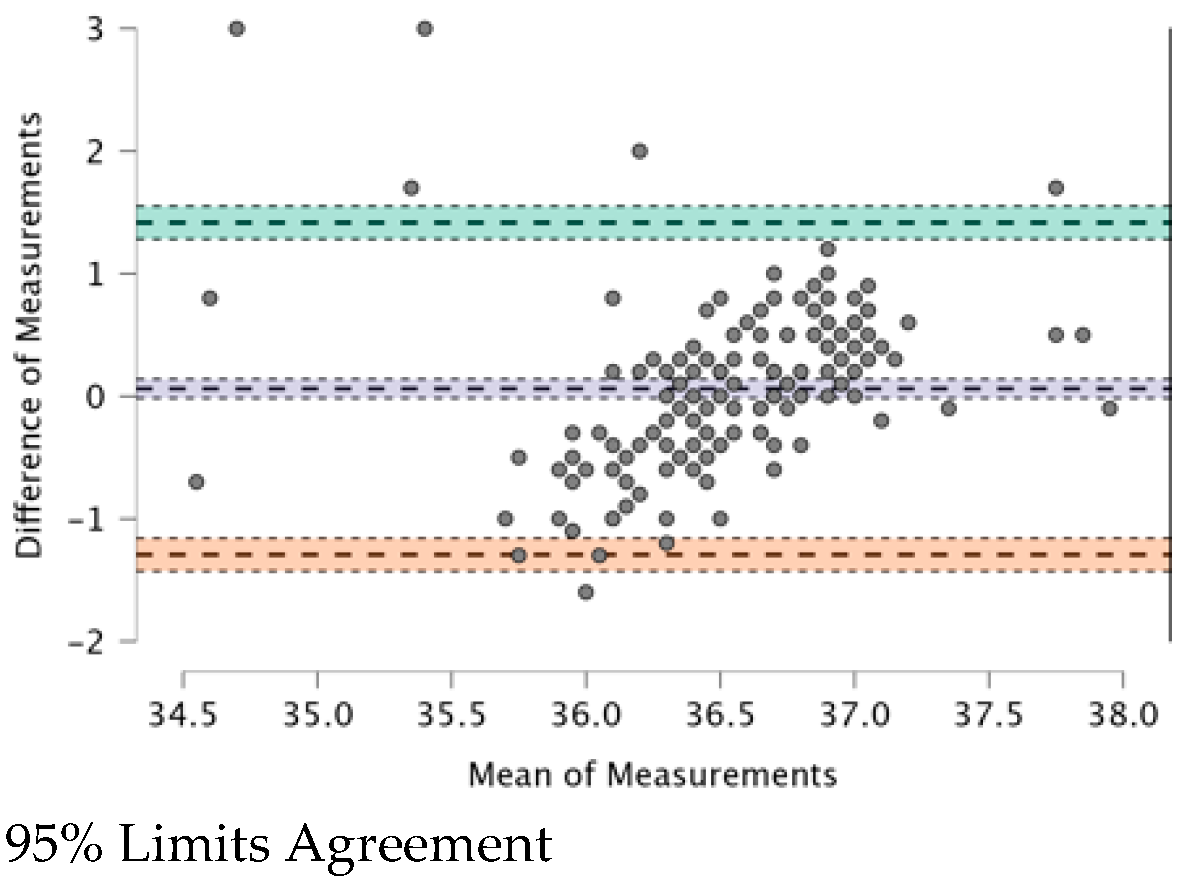
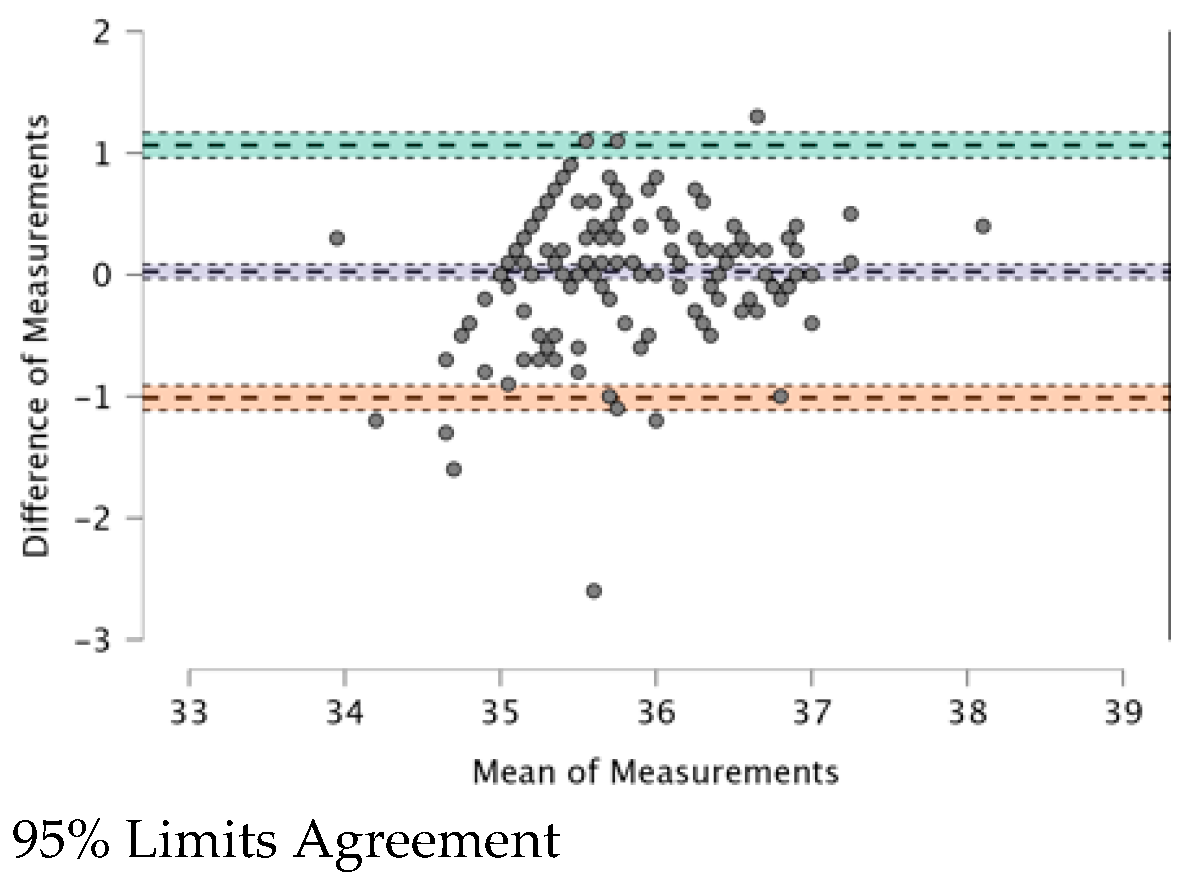
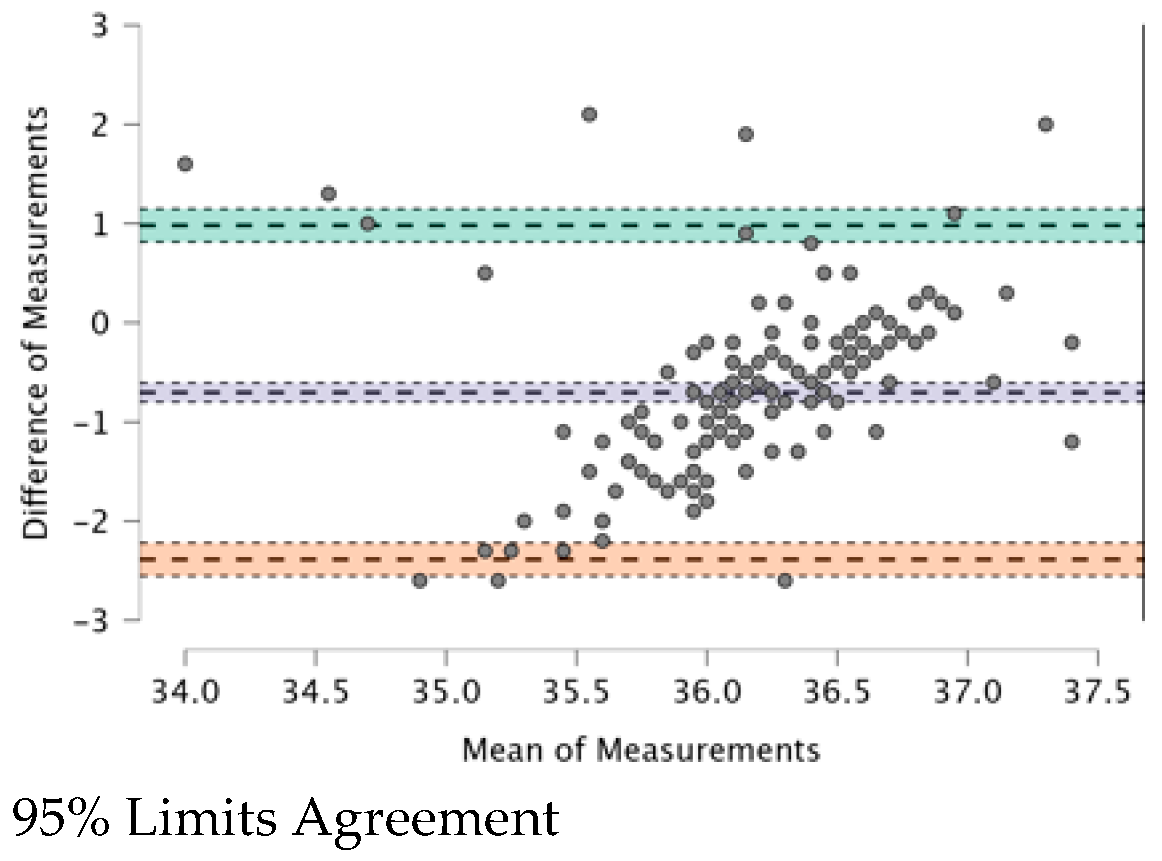
3.6. Correlations between Measurements Taken with the Four TMs
3.7. Correlation between Environmental Variables and Body Temperature
4. Discussion
Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Flouris, A.D.; Schlader, Z.J. Human behavioral thermoregulation during exercise in the heat: Human behavioral thermoregulation. Scand. J. Med. Sci. Sports 2015, 25 (Suppl. S1), 52–64. [Google Scholar] [CrossRef] [PubMed]
- Morrison, S.F. Central control of body temperature. F1000Research 2016, 5, 880. [Google Scholar] [CrossRef] [PubMed]
- González, J.V.; Arena, A.V.; González, V.V. Semiología de los signos vitales: Una mirada novedosa a un problema vigente. Arch. Med. 2012, 12, 221–240. [Google Scholar]
- Gallego, J.M.; Sierra, G.; Galan, G.; Tirrado, J.J.; Carmona, J.V. Monitorización de la Temperatura Corporal. Valencia: Consejo de Enfermería de la Comunidad Valenciana (CECOVA). 2009. Available online: http://www.bibliotecadigitalcecova.com (accessed on 22 October 2022).
- Rubia, J.A. Termómetros de Mercurio: Situación Actual y Perspectivas de su uso Clínico. Eficacia de Los Diferentes Termómetros Alternativos. Ph.D. Thesis, University of La Laguna, La Laguna, Spain, 2008. Teseo. Available online: https://www.educacion.gob.es/teseo/imprimirFicheroTesis.do?idFichero=ooV8hqhG2aA%3D (accessed on 22 October 2022).
- Michael, J. Fisiología Humana; Editorial Manual Moderno: Mexico City, Mexico, 2012. [Google Scholar]
- Bush, L.M. Fever. 2020. Available online: https://www.msdmanuals.com/professional/infectious-diseases/biology-of-infectious-disease/fever (accessed on 22 October 2022).
- Ng, S.F.; Oo, C.S.; Loh, K.H.; Lim, P.Y.; Chan, Y.H.; Ong, B.C. A comparative study of three warming interventions to determine the most effective in maintaining perioperative normothermia. Anesth. Analg. 2003, 96, 171–176. [Google Scholar] [CrossRef]
- O’Grady, N.P.; Barie, P.S.; Bartlett, J.G.; Bleck, T.; Carroll, K.; Kalil, A.C.; Linden, P.; Maki, D.G.; Nierman, D.; Pasculle, W.; et al. Guidelines for evaluation of new fever in critically ill adult patients: 2008 update from the American College of Critical Care Medicine and the Infectious Diseases Society of America. Crit. Care Med. 2008, 36, 1330–1349. [Google Scholar] [CrossRef]
- Villanueva, E.; Fernández, M.; Viano, E.; Amorín, M. Fiabilidad en la medición de la temperatura corporal con un termómetro timpánico en pacientes geriátricos. Gerokomos 2017, 28, 68–72. [Google Scholar]
- Durack, D.T.; Street, A.C. Fever of unknown origin-reexamined and redefined. Curr. Clin. Top. Infect. Dis. 1991, 11, 35–51. [Google Scholar] [PubMed]
- Padilla-Raygoza, N.; Ruiz-Paloalto, M.L.; Díaz-Guerrero, R.; Olvera-Villanueva, G.; Maldonado, A.; Raygoza-Mendoza, M.D.P. Correlación de mediciones de temperatura corporal con 3 termómetros: Ótico, cutáneo y digital, en niños mexicanos. Enferm. Clin. 2014, 24, 175–182. [Google Scholar] [CrossRef]
- Mazerolle, S.M.; Ganio, M.S.; Casa, D.J.; Vingren, J.; Klau, J. Is oral temperature an accurate measurement of deep body temperature? A systematic review. J. Athl. Train. 2011, 46, 566–573. [Google Scholar] [CrossRef]
- Benzinger, M. Tympanic thermometry in surgery and anesthesia. JAMA 1969, 209, 1207–1211. [Google Scholar] [CrossRef]
- Sansano, M.I.U.; Díez Domingo, J.; Casaní Martínez, C.; Alvarez de Laviada Mulero, T.; Sanz, A.B. Validación del termómetro timpánico en atención primaria [Validation of the tympanic thermometer in primary care]. Aten. Primaria 1999, 23, 91–96. [Google Scholar]
- Paes, B.F.; Vermeulen, K.; Brohet, R.M.; van der Ploeg, T.; de Winter, J.P. Accuracy of tympanic and infrared skin thermometers in children. Arch. Dis. Child. 2010, 95, 974–978. [Google Scholar] [CrossRef] [PubMed]
- Barnett, B.J.; Nunberg, S.; Tai, J.; Lesser, M.L.; Fridman, V.; Nichols, P.; Powell, R.; Silverman, R. Oral and tympanic membrane temperatures are inaccurate to identify Fever in emergency department adults. West J. Emerg. Med. 2011, 12, 505–511. [Google Scholar] [CrossRef] [PubMed]
- Amoateng-Adjepong, Y.; Del Mundo, J.; Manthous, C.A. Accuracy of an infrared tympanic thermometer. Chest 1999, 115, 1002–1005. [Google Scholar] [CrossRef]
- Nadkarni, K.P.; Mayo, Z.; Laux, J.P.; McRea, A.; Angelillo, D.; Meitzen, R.; Dechtiar, A.D.; Baquero, C.; Crabtree, K.; Carr, L.; et al. Axillary Thermometry Demonstrates Greater Reliability Compared With Rectal Thermometry in Healthy Neonates. Clin. Pediatr. 2021, 60, 298–303. [Google Scholar] [CrossRef]
- McCarthy, L.K.; O’Donnell, C.P.F. Comparison of rectal and axillary temperature measurements in preterm newborns. Arch. Dis. Child. Fetal Neonatal Ed. 2021, 106, 509–513. [Google Scholar] [CrossRef]
- Franconi, I.; La Cerra, C.; Marucci, A.R.; Petrucci, C.; Lancia, L. Digital Axillary and Non-Contact Infrared Thermometers for Children. Clin. Nurs. Res. 2018, 27, 180–190. [Google Scholar] [CrossRef]
- Mahabala, C.; Dakappa, P.H.; Gupta, A.R. A novel method for measuring sublingual temperature using conventional non-contact forehead thermometer. F1000Research 2022, 11, 13. [Google Scholar] [CrossRef]
- Von Elm, E.; Altman, D.G.; Egger, M.; Pocock, S.J.; Gøtzsche, P.C.; Vandenbroucke, J.P. The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement: Guidelines for reporting observational studies. J. Clin. Epidemiol. 2008, 61, 344–349. [Google Scholar] [CrossRef]
- JASP Team. JASP, (Version 0.16.3); JASP Team: Amsterdam, The Netherlands, 2022.
- Hernández Aguado, I.; Porta Serra, M.; Miralles, M.; García Benavides, F.; Bolúmar, F. La cuantificación de la variabilidad en las observaciones clínicas [The quantification of variability in clinical cases]. Med. Clin. 1990, 95, 424–429. [Google Scholar]
- Fleiss, J.L. The Design and Analysis of Clinical Experiments; John Wiley & Sons: Hoboken, NJ, USA, 1986. [Google Scholar]
- Prieto, L.; Lamarca, R.; Casado, A. La evaluación de la fiabilidad en las observaciones clínicas: El coeficiente de correlación intraclase. Med. Clin. 1998, 110, 142–415. [Google Scholar]
- Bland, J.M.; Altman, D.G. Stadistical methods for assessing agreement between two methods of clinical measurement. Lancet 1986, 1, 307–310. [Google Scholar] [CrossRef] [PubMed]
- Khan, S.; Saultry, B.; Adams, S.; Kouzani, A.Z.; Decker, K.; Digby, R.; Bucknall, T. Comparative accuracy testing of non-contact infrared thermometers and temporal artery thermometers in an adult hospital setting. Am. J. Infect. Control. 2021, 49, 597–602. [Google Scholar] [CrossRef] [PubMed]
- Kaciuba-Uscilko, H.; Grucza, R. Gender differences in thermoregulation. Curr. Opin. Clin. Nutr. Metab. Care 2001, 4, 533–536. [Google Scholar] [CrossRef] [PubMed]
- INE. Entorno Físico y Medio Ambiente. 2018. Available online: https://www.ine.es/prodyser/pubweb/anuario18/anu18_01entor.pdf (accessed on 20 October 2022).
- Ministry of the Presidency. Real Decreto 1038/2012, de 6 de Julio, Por el que se Modifica el Real Decreto 1367/2007, de 19 de Octubre, Por el Que se Desarrolla la Ley 37/2003, de 17 de Noviembre, del Ruido, en lo Referente a Zonificación Acústica, Objetivos de Calidad y Emisiones Acústicas; Ministry of the Presidency (Spain): Seville, Spain, 2007. [Google Scholar]
- Piccinini, F.; Martinelli, G.; Carbonaro, A. Reliability of Body Temperature Measurements Obtained with Contactless Infrared Point Thermometers Commonly Used during the COVID-19 Pandemic. Sensors 2021, 21, 3794. [Google Scholar] [CrossRef] [PubMed]
- Gualdrón Romero, G.; Peña Otero, A.; García Cernuda, D.; Aguilera Samaniego, V.; Claramunt González, P.; Cordero, I.G. Validación del termómetro como factor determinante de la eficacia en la toma de temperatura por infección de COVID-19. Rev. Rol Enferm. 2020, 43, 620–628. [Google Scholar]
- Suleman, M.I.; Doufas, A.G.; Akca, O.; Ducharme, M.; Sessler, D.I. Insufficiency in a new temporal-artery thermometer for adult and pediatric patients. Anesth. Analg. 2002, 95, 67–71. [Google Scholar] [CrossRef]
- Latman, N.S. Clinical Thermometry: Possible Causes and Potential Solutions to Electronic, Digital Thermometer Inaccuracies. Biomed. Instrum. Technol. 2003, 37, 190–196. [Google Scholar] [CrossRef]
- Niven, D.J.; Gaudet, J.E.; Laupland, K.B.; Mrklas, K.J.; Roberts, D.J.; Stelfox, H.T. Accuracy of peripheral thermometers for estimating temperature: A systematic review and meta-analysis. Ann. Intern. Med. 2015, 163, 768–777. [Google Scholar] [CrossRef]
- Kameda, N. Clinical accuracy of non-contact forehead infrared thermometer and infrared tympanic thermometer in postoperative adult patients: A comparative study. J Perioper Pract. 2022, 32, 142–148. [Google Scholar] [CrossRef]
- Microlife. Why You Should Measure Body Temperatura. 2022. Available online: https://www.microlife.com/magazine/fever/why-you-should-measure-body-temperature (accessed on 22 October 2022).
- Martín, M.J.; Cardenas, D. Best Practice Guide: Use of Infrared Forehead Thermometers to Perform Traceable Non-Contact Measurements of Human Body Temperatures, 3rd ed.; 2021. Available online: https://www.bipm.org/documents/20126/41773843/Best+Practice+Guide+for+Forehead+Thermometers.pdf/7550747b-1344-7416-3e7a-ec54f863ed5c?version=1.3&t=1652455631920&download=true (accessed on 30 October 2022).
- Fernández-Cuevas, I.; Marins, J.C.B.; Lastras, J.A.; Carmona, P.M.G.; Cano, S.P.; García-Concepción, M.Á.; Sillero-Quintana, M. Classification of factors influencing the use of infrared thermography in humans: A review. Infrared Phys. Technol. 2015, 71, 28–55. [Google Scholar] [CrossRef]
- Stacey, J.L.; Sullivan, S.J.L.; Rinaldi, J.E.; Hariharan, P.; Casamento, J.P.; Baek, S.; Seay, N.; Vesnovsky, O.; Topoleski, L.D.T. Clinical evaluation of non-contact infrared thermometers. Sci. Rep. 2021, 11, 22079. [Google Scholar] [CrossRef]
- Patel, A.H.; Patel, M.M.; Bhavsar, R.H. Comparison of Non-Contact Forehead Infrared Thermometry with Axillary Digital Thermometry in Neonates. GCSMC J. Med. Sci. 2016, 20, 20–24. [Google Scholar]
- Tay, M.R.; Low, Y.L.; Zhao, X.; Cook, A.R.; Lee, V.J. Comparison of Infrared Thermal Detection Systems for mass fever screening in a tropical healthcare setting. Public Health 2015, 129, 1471–1478. [Google Scholar] [CrossRef] [PubMed]
- Wang, Q.; Zhou, Y.; Ghassemi, P.; McBride, D.; Casamento, J.P.; Pfefer, T.J. Infrared thermography for measuring elevated body temperature: Clinical accuracy, calibration, and evaluation. Sensors 2021, 22, 215. [Google Scholar] [CrossRef] [PubMed]
- Subramaniam, T.; Valuyeetham, A.; Ambu, V.K. Temperature measurement: Must it be the forehead? A prospective cross-sectional study. Med. J. Malaysia 2022, 77, 506–509. [Google Scholar]
- Hayward, G.; Verbakel, J.Y.; Ismail, F.A.; Edwards, G.; Wang, K.; Fleming, S.; Holtman, G.A.; Glogowska, M.; Morris, E.; Curtis, K.; et al. Non-contact infrared versus axillary and tympanic thermometers in children attending primary care: A mixed-methods study of accuracy and acceptability. Br. J. Gen. Pract. 2020, 70, e236–e244. [Google Scholar] [CrossRef]
- Geijer, H.; Udumyan, R.; Lohse, G.; Nilsagård, Y. Temperature measurements with a temporal scanner: Systematic review and meta-analysis. BMJ Open 2016, 6, e009509. [Google Scholar] [CrossRef]
- ISO 80601-2-56:2017; Medical Electrical Equipment—Part 2-56: Particular Requirements for Basic Safety and Essential Performance of Clinical Thermometers for Body Temperature Measurement. ISO: Geneva, Switzerland, 2017. Available online: https://www.iso.org/standard/75005.html (accessed on 30 October 2022).
- Zhen, C.; Xia, Z.; Ya Jun, Z.; Long, L.; Jian, S.; Gui Ju, C.; Long, L. Accuracy of infrared tympanic thermometry used in the diagnosis of Fever in children: A systematic review and meta-analysis. Clin. Pediatr. 2015, 54, 114–126. [Google Scholar] [CrossRef]

| Variables | Description |
|---|---|
| Independent Variables | |
| Age | Age of the participant in years |
| Gender | Male or female |
| Location | Location of the bed in the room: door (below the air conditioning outlet) or window (far from the emitter). |
| Temperature | Environmental Temperature. Unit: Celsius = °C. |
| Humidity | Environmental Relative Humidity. Unit: percentage = %. |
| Light | Environmental Light. Unit: lumen = Lux. |
| Noise | Environmental Noise. Unit: Decibels = dB. |
| Dependent variables | |
| Axillary Body Temperature | Body temperature measured with a Gallium Thermometer. |
| Tympanic Body Temperature | Body temperature measured with a Non-Contact Tympanic Infrared Thermometer. |
| Forehead Body Temperature | Body temperature measured with a Non-Contact Forehead Infrared Thermometer. |
| Axillary Body Temperature 2 | Body temperature measured with an Electronic Thermometer. |
| Environmental Humidity (%) | Environmental Temperature (°C) | Environmental Light (Lux) | Environmental Noise (Db) | |
|---|---|---|---|---|
| Valid | 312 | 312 | 312 | 312 |
| Missing | 0 | 0 | 0 | 0 |
| Mean | 58.878 | 23.032 | 81.037 | 62.148 |
| Std. Deviation | 5.325 | 1.109 | 30.176 | 12.708 |
| Minimum | 44.400 | 20.000 | 11.000 | 38.100 |
| Maximum | 75.600 | 24.700 | 172.000 | 84.100 |
| BT–Tympanic Infrared TM | BT–Axillary Electronic TM | BT–Axillary Gallium TM | BT–Non-Contact Infrared TM (Forehead) | |
|---|---|---|---|---|
| Valid | 312 | 312 | 312 | 312 |
| Missing | 0 | 0 | 0 | 0 |
| Mean | 36.559 | 35.795 | 35.769 | 36.497 |
| Std. Deviation | 0.660 | 0.766 | 0.688 | 0.542 |
| Minimum | 34.200 | 33.600 | 33.800 | 33.200 |
| Maximum | 38.600 | 38.300 | 37.900 | 38.000 |
| BT–Tympanic Infrared TM | BT–Axillary Electronic TM | BT–Axillary Gallium TM | BT–Non-Contact Infrared TM (Forehead) | ||
|---|---|---|---|---|---|
| Age | Pearson’s r p-value | 0.166 ** 0.003 | −0.156 ** 0.006 | −0.147 ** 0.009 | −0.403 *** <0.001 |
| Independent Samples t-Test | |||||||
|---|---|---|---|---|---|---|---|
| T | Df | p | Mean Difference | SE Difference | 95% CI Mean Difference | ||
| Lower | Upper | ||||||
| BT–Non-Contact Tympanic Infrared TM | 0.275 | 310 | 0.784 | 0.021 | 0.076 | −0.128 | 0.170 |
| BT–Axillary Electronic TM | −0.490 | 310 | 0.625 | −0.043 | 0.088 | −0.216 | 0.130 |
| BT–Axillary Gallium TM | −0.791 | 310 | 0.430 | −0.062 | 0.079 | −0.217 | 0.093 |
| BT–Non -Contact Infrared TM (forehead) | 5.398 | 310 | <0.001 *** | 0.321 | 0.060 | 0.204 | 0.438 |
| T | Df | p | Mean Difference | SE Difference | 95% CI Mean Difference | ||
|---|---|---|---|---|---|---|---|
| Lower | Upper | ||||||
| BT–Non-Contact Tympanic Infrared TM | 0.301 | 310 | 0.764 | 0.023 | 0.075 | −0.125 | 0.170 |
| BT–Axillary Electronic TM | 1.031 | 310 | 0.303 | 0.089 | 0.087 | −0.081 | 0.260 |
| BT–Axillary Gallium TM | 1.305 | 310 | 0.193 | 0.102 | 0.078 | −0.052 | 0.255 |
| BT–Non-Contact Infrared TM (forehead) | −0.839 | 310 | 0.402 | −0.052 | 0.061 | −0.173 | 0.069 |
| T | Df | p | Mean Difference | SE Difference | 95% CI Mean Difference | ||
|---|---|---|---|---|---|---|---|
| Lower | Upper | ||||||
| BT–Non-Contact Tympanic Infrared TM | −0.879 | 310 | 0.380 | −0.531 | 0.604 | −1.718 | 0.657 |
| BT–Axillary Electronic TM | −0.633 | 310 | 0.527 | −0.080 | 0.126 | −0.327 | 0.168 |
| BT–Axillary Gallium TM | 0.264 | 310 | 0.792 | 0.905 | 3.424 | −5.833 | 7.644 |
| BT–Non-Contact Infrared TM (forehead) | 1.282 | 310 | 0.201 | 1.844 | 1.438 | −0.987 | 4.674 |
| Pearson’s r | p-Value | ||
|---|---|---|---|
| CT–Non-Contact Axillary Electronic TM | 0.298 *** | <0.001 |
| CT–Axillary Gallium TM | 0.310 *** | <0.001 |
| CT–Non-Contact Infrared TM (forehead) | 0.352 *** | <0.001 |
| CT–Axillary Gallium TM | 0.739 *** | <0.001 |
| CT–Non-Contact Infrared TM (forehead) | 0.172 ** | 0.002 |
| CT–Non-Contact Infrared TM (forehead) | 0.156 ** | 0.006 |
| Point Estimate | Lower 95% CI | Upper 95% CI | |
|---|---|---|---|
| Thermometers | 0.479 | 0.378 | 0.567 |
| BT–Non-Contact Tympanic Infrared TM | BT–Axillary Electronic TM | BT–Axillary Gallium TM | BT–Non-Contact Infrared TM (Forehead) | ||
|---|---|---|---|---|---|
| Environmental Humidity, % | Pearson’s r p-value | 0.038 0.502 | −0.082 0.151 | −0.072 0.202 | −0.029 0.610 |
| Environmental Temperature, °C | Pearson’s r p-value | 0.133 * 0.019 | 0.045 0.431 | −0.043 0.447 | 0.070 0.221 |
| Environmental Light, Lux | Pearson’s r p-value | −0.050 0.375 | 0.041 0.466 | 0.031 0.584 | −0.020 0.725 |
| Environmental Noise, Db | Pearson’s r p-value | −0.146 ** 0.010 | −0.081 0.152 | −0.073 0.197 | −1.127 × 10−4 0.998 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Díaz-González, C.d.l.M.; Mateos-López, N.; De la Rosa-Hormiga, M.; Carballo-Hernández, G. Influence of Hospital Environmental Variables on Thermometric Measurements and Level of Concordance: A Cross-Sectional Descriptive Study. Int. J. Environ. Res. Public Health 2023, 20, 4665. https://doi.org/10.3390/ijerph20054665
Díaz-González CdlM, Mateos-López N, De la Rosa-Hormiga M, Carballo-Hernández G. Influence of Hospital Environmental Variables on Thermometric Measurements and Level of Concordance: A Cross-Sectional Descriptive Study. International Journal of Environmental Research and Public Health. 2023; 20(5):4665. https://doi.org/10.3390/ijerph20054665
Chicago/Turabian StyleDíaz-González, Candelaria de la Merced, Noa Mateos-López, Milagros De la Rosa-Hormiga, and Gloria Carballo-Hernández. 2023. "Influence of Hospital Environmental Variables on Thermometric Measurements and Level of Concordance: A Cross-Sectional Descriptive Study" International Journal of Environmental Research and Public Health 20, no. 5: 4665. https://doi.org/10.3390/ijerph20054665
APA StyleDíaz-González, C. d. l. M., Mateos-López, N., De la Rosa-Hormiga, M., & Carballo-Hernández, G. (2023). Influence of Hospital Environmental Variables on Thermometric Measurements and Level of Concordance: A Cross-Sectional Descriptive Study. International Journal of Environmental Research and Public Health, 20(5), 4665. https://doi.org/10.3390/ijerph20054665








