Abstract
Skills trainings for caregivers of patients with anorexia nervosa (AN) have been proven to be effective in improving caregiver skills and reducing caregivers’ psychopathology. The effects on patients, especially adolescents, are largely unknown. The aim of this study was to evaluate the effectiveness of a caregivers’ skills training program (Supporting Carers of Children and Adolescents with Eating Disorders in Austria, SUCCEAT, workshop or online version) on adolescents with AN delivered as workshops (WS) or online (ONL). Outcomes are Body-Mass-Index (BMI) percentile, eating psychopathology (Eating Disorder Examination, EDE), attitudinal and behavioural dimensions of eating disorders (Eating Disorder Inventory-2), motivation to change (AN Stages of Change Questionnaire), emotional and behavioural problems (Youth Self-Report) and quality of life (KINDL). All outcome variables significantly improved across both SUCCEAT groups (WS and ONL) and were sustained at 12-month follow-up. The online and workshop delivery of SUCCEAT were equally effective. Most effect sizes were in the medium-to-high range. Full or partial remission was observed in 72% (WS) and 87% (ONL) of patients. Caregiver skills trainings, either delivered as workshops or online modules, are highly recommended to complement treatment as usual.
1. Introduction
Anorexia nervosa (AN) is a severe psychiatric disorder with a prevalence of about 1% [1,2] that is defined by persistent restriction of energy intake, intense fear of gaining weight and disturbance in self-perception [1,3,4]. The pathogenesis of the illness is associated with biological, psychological, and sociocultural factors [4,5]. AN tends to begin in adolescence and is often associated with a tendency to a protracted course and high mortality. Two thirds of patients recover from the illness, whereas one third develops a persisting eating disorder (ED) [4]. Early intervention and specialised treatment can positively affect the outcome [1,3,4]. Caring for patients with AN can have a serious emotional impact on parents, causing severe distress and even significant psychiatric symptoms such as anxiety and depression [6,7,8,9]. As described in the cognitive interpersonal model of maintaining factors for EDs [10,11,12], parental distress might lead to interpersonal problems and unfavourable reactions within the family that may maintain the illness and hinder recovery. Therefore, there is an urgent need to provide parents with specific skills and communication strategies to improve their own mental health in order to better support their children and facilitate their recovery. A high number of studies confirm that interventions for parents based on the cognitive interpersonal model of maintaining factors for EDs [10,11,12], developed by Treasure et al., can reduce parental burden, high expressed emotion (HEE) and distress and also improve caregiver skills in parents [13,14,15,16]. Online interventions based on this model, although far less investigated than workshop-based interventions [17], seem to show similar effectiveness when compared to in person workshops for parents [14,15,18]. The use of novel technologies is highly recommended in the field of EDs [4], especially in the context of the actual and ongoing Coronavirus-Disease-2019 (COVID-19) pandemic [19], when access to interventions might be further impeded due to exit restrictions and further measures of social distancing.
Apart from addressing parental burden, HEE and parental skills, the superordinate aims of such caregiver skills trainings are to promote patients’ outcome and to support their recovery [10,11,12,20]. However, whether caregiver skills trainings based on the same model as described above actually have an impact on patients’ outcome is still largely unknown, especially in the long-term. Previous studies indicate that a parental skills training is equally effective as treatment-as-usual (TAU) [20], individual family work [21], or psychoeducational workshops [22,23] concerning patients’ improvement in Body-Mass-Index (BMI) [20,21], AN symptoms [20,22,24], patients’ anxiety and depression [23], distress [20,22,23] as well as quality of life [20,24]. All of these studies evaluated similar interventions based on the cognitive interpersonal model of maintaining factors for EDs [10,11,12], but mainly focused on adult patients [13,20,21,22,23].
Evidence regarding the impact on adolescent patients is particularly sparse. Hodsoll et al. [25] reported a minor advantage in weight gain in adolescents whose parents participated in such a skills programme at 6-month and 12-month follow-up (FU) compared to TAU. Philipp et al. [15] found some improvements in AN symptoms and BMI in adolescents associated with reductions of parental HEE after participating in a parental skills training. Thus, further evaluating the outcome for adolescent patients is crucial in order to shed light on whether adolescents with AN also benefit from highly specialised caregiver interventions. Therefore, the aim of this study was to examine the impact of the “Supporting Carers of Children and Adolescents with Eating Disorders in Austria” (SUCCEAT) intervention, a parental skills training based on the cognitive interpersonal model of maintaining factors for EDs [10,11,12], delivered via workshop (WS) or online (ONL), on adolescent patients’ outcome. To our knowledge, this is the first study comparing two different delivery forms of the described model addressing patients’ outcome. SUCCEAT was translated into German and adapted for parents of adolescents suffering from AN. The main goals are to decrease parental distress and burden and to increase parental skills and knowledge regarding the illness in order to support them to better help their children towards recovery. SUCCEAT addresses coping strategies for parents, communication strategies including Motivational Interviewing (MI) and strategies to enhance motivation to change in the sufferers. We examined whether adolescent AN patients whose parents participated in a WS vs. an ONL version of the SUCCEAT intervention benefitted in terms of BMI percentile, AN symptoms, motivation to change, behavioural and emotional problems, and quality of life at post-intervention and at 12-month FU. Furthermore, we compared remission rates (full, partial, no remission according to the Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5) diagnostic criteria for AN [3]) between patients whose parents participated in the WS and ONL group at 12-month FU.
2. Materials and Methods
2.1. Trial Design
This trial is a two-arm parallel group quasi-randomised feasibility study. Caregivers of adolescent patients with AN or atypical AN were equally allocated to the SUCCEAT WS and ONL interventions and the patients were monitored regarding their eating disorder and other psychopathology. Further details of the study design are reported elsewhere [14,15,26]. These analyses are part of a larger study, designed to evaluate differences of the carers’ outcomes participating in the SUCCEAT intervention.
2.2. Participants
2.2.1. Eligibility Criteria for Participants
Children and adolescents (aged between 10 and 19 years) suffering from AN (F50.0) or atypical AN (F50.1) [27] and their main caregivers (one parent for each child, who spent most of the time with the child) were eligible to participate in this trial. Further inclusion criteria for children and adolescents were receipt of TAU [28] and being fluent in German. Besides, caregivers required Internet access. Exclusion criteria were severe comorbidities of the children and adolescents (e.g., psychosis) and severe morbidity of the caregivers at baseline.
2.2.2. How Participants Were Identified and Consented
Children and adolescents and their main caregivers underwent psychiatric and psychological assessments to ensure the eligibility criteria. The main caregivers and their children who accepted the invitation to participate in this study gave their written informed consent at the same site where they received TAU.
2.3. Interventions
2.3.1. Workshop (WS) Group
The SUCCEAT intervention (WS and ONL) was developed for the caregivers (usually parents) of children and adolescents with AN, to alleviate the caregivers’ distress and burden in order to enable them to support their children with AN [14] and to attain long-term changes for a healing atmosphere in the families through reduced HEE and good communication skills [15,29,30,31,32,33]. MI is used to target self-efficacy, to change behaviour that may maintain ED symptoms [34,35], and to convey skills to empower the caregivers to guide their children in a compassionate way. The intervention is based on the cognitive-interpersonal maintenance model [10,11,12], the transtheoretical model (TTM) of change [36] and the antecedent-behaviour-consequence model (ABC model; [37]). The intervention provides MI skills to the parents in order to improve communication within the family and to enhance the patients’ motivation to change (e.g., handling resistance, motivating change through discrepancy). The WS and ONL versions of SUCCEAT are structured interventions, which involve working with caregivers of about eight children and adolescents over the course of eight weekly sessions. Two healthcare professionals coached the participants of the WS and ONL group [14,15,26]. The 2-h WS sessions were held once in a week at the Medical University of Vienna, Department of Child and Adolescent Psychiatry, where the children and adolescents received TAU too. The caregivers received a manual with detailed information based on a book [30,31,32], the German version of a DVD where best-practice examples of how to communicate with the child are shown [38], and weekly handouts.
2.3.2. Online (ONL) Group
The ONL group started with a personal welcome meeting for the caregivers at the Medical University of Vienna, Department of Child and Adolescent Psychiatry, so that the caregivers could get to know each other and the coaches. The caregivers received the DVD as well [38] and got access to the online platform where they could find the same intervention contents as the WS group: the possibility to download the manual [30,31,32] and eight online modules which were activated on a weekly basis and contained the same content as taught in the WS sessions, slightly adapted for online use [33]. The coaches responded to the caregivers’ questions and provided feedback to their progress once a week via the online platform.
2.4. Outcome Measurements
Children and adolescents completed the questionnaires at baseline (T0), post-intervention (after 3 months, at the end of the intervention, T1), and 12-month FU (T2). The interventions and the evaluations took place from November 2014 until April 2018. Sociodemographic and clinical characteristics of the patients (e.g., age, sex, BMI percentile, illness duration, type of current treatment) were collected. For further details see Franta et al. [26].
- The BMI percentiles were obtained from clinical measures of height and weight; additionally, sex- and age-specific percentiles were analysed [39].
- The Eating Disorder Examination (EDE; [40,41]) is a semi-structured interview conducted by clinicians to diagnose EDs and to obtain a picture as accurate as possible of the participant’s eating behaviour and attitudes. It is rated through a global score and four subscales: “restraint” (e.g., avoidance of eating; dietary rules), “eating concerns” (e.g., fear of losing control of eating; guilt about eating), “weight concerns” (e.g., preoccupation with weight; desire to lose weight), and “shape concerns” (e.g., importance of shape; discomfort seeing one’s own body). Internal consistency is good (Cronbach’ s alpha for the subscales: 0.73 to 0.86; for the total score: 0.93). In our sample, reliability was high for both, for children below the age of 14 (Cronbach’s alpha: 0.90) and for adolescents aged 14 and above (Cronbach’s alpha: 0.92). The higher the score the higher is the ED psychopathology.
- The Eating Disorder Inventory-2 (EDI-2; [42]) is a self-report measure to assess ED specific and ED associated psychopathology, including a total scale and 11 subscales (“drive for thinness”, “bulimia”, “body dissatisfaction”, “ineffectiveness”, “perfectionism”, “interpersonal distrust”, “interoceptive awareness”, “maturity fears”, “asceticism”, “impulse regulation”, and “social insecurity”). The EDI-2 was validated for children and adolescents aged 10 and above. Excellent data concerning reliability are available (total score: Cronbach’ s alpha: 0.97). For the purpose of this study, only the total score was used. The higher the score the more subjective ED attitudes and behaviours are reported.
- The Anorexia Nervosa Stages of Change Questionnaire (ANSOCQ; [43,44]) is a self-report questionnaire assessing motivation to change related to their ED symptomatology. The children and adolescents select a statement for each item, which represents their current stage of change (precontemplation, contemplation, preparation, action, maintenance). Internal consistency is excellent (Cronbach’s alpha: 0.90). One study [45] shows good reliability for adolescents older than 12 years. Cronbach’s alpha in our sample was 0.91 for children under the age of 14 and 0.94 for adolescents aged 14 and above. The calculated mean score ranges from 1 to 5 with higher scores indicating a higher motivation to change, or an advanced stage of change, respectively.
- The Youth Self-Report (YSR; [46]) is a self-report measure assessing various behavioural and emotional problems (e.g., “anxious/depressed”, “social problems”, “aggressive behaviour”). The YSR was validated for children and adolescents from age 11. Reliability is high (Cronbach’s alpha ≥ 0.91). We used the total score in this study only, with a higher score indicating a higher level of general psychopathology.
- The Health-Related Quality of Life Questionnaire for Children and Adolescents (KINDL; [47,48]) is a self-report measure assessing the quality of life. The total score comprises the subscales: “physical well-being”, “psychological well-being”, “self-worth”, “family”, “friends”, and “school”. The KINDL was validated for children and adolescents aged 7 years and above. Internal consistency is rather high (Cronbach’s alpha: 0.80). The total score ranges from 0 to 100; a higher score indicating a higher quality of life.
2.5. Randomisation
SUCCEAT participants of this study were quasi-randomised [49]. Participants were allocated to the WS and ONL group alternately after we scheduled the start dates of the intervention groups. The number of participants per group slightly varied (median size = 7).
2.6. Blinding
Neither the researchers nor the study participants involved in this study were blinded to the assigned intervention.
2.7. Statistical Analysis
Data analyses were performed with SPSS Statistics 26.0 (IBM Corp., Armonk, NY, USA). Differences between the SUCCEAT WS and ONL groups regarding sociodemographic and clinical characteristics at baseline were analysed using Chi²-tests and ANOVA. We conducted general linear mixed models to analyse symptom changes and group differences in the outcome variables. Moreover, we calculated baseline to 12-month FU effect sizes in terms of Cohen’s d with values below 0.2 indicating small effect, values between 0.2 and 0.8 indicating medium effect and values above 0.8 indicating large effect.
Furthermore, we analysed the clinical significance of outcomes by calculating remission rates at the 12-month FU assessment. According to the DSM-5 criteria [3], full remission was categorised if no diagnostic criterion for AN was met at the 12-month FU assessment. Partial remission was categorised if the BMI was above the 10th sex- and age-specific percentile but either criterion B (intense fear of gaining weight, becoming fat or behaviour that interferes with weight gain) or criterion C (disturbances in self-perception of weight and shape) was still met. No remission was categorised if the BMI was still below the 10th percentile. We performed a Chi²-test to analyse whether remission rates differed between patients from the SUCCEAT WS and ONL groups.
All analyses were done based on the completer sample (participants who provided data at all assessment time points); missing values due to dropout were not replaced.
3. Results
3.1. Participant Flow
Main caregivers of 102 adolescent patients with AN took part in the SUCCEAT intervention (WS: n = 50; ONL: n = 52) (see [14] for details). Patients’ outcome data relevant for this study were available for 98 patients (WS: n = 48; ONL: n = 50). At post-intervention (3 months after the beginning of the intervention), 92 (94%) patients (WS: n = 46; ONL: n = 46) provided any outcome data. At the 12-month FU, 70 (71%) patients (WS: n = 35; ONL: n = 35) provided any outcome data. Patients who did not complete the 12-month FU assessment did not differ significantly from patients who provided data in most outcome variables at baseline (BMI: p = 0.268; BMI percentile: p = 0.641; EDE total: p = 0.793; ANSOCQ: p =0.524; YSR total: p = 0.084; KINDL total: p = 0.455). Patients who dropped out at the 12-month assessment had significantly lower EDI-2 total scores at baseline (mean = 57.61, SD = 40.73) compared to patients who provided data (mean = 74.79, SD = 36.81; t = 2.109, p = 0.038).
3.2. Baseline Data
Baseline sociodemographic and clinical characteristics of the patients for each intervention group (WS, ONL) are shown in Table 1. The characteristics of the carers are reported elsewhere [14]. We tested whether patients allocated to the two groups differed regarding sociodemographic and clinical characteristics as well as regarding the baseline scores of the outcome questionnaires. In general, patients from the SUCCEAT WS group showed similar baseline data compared to the ONL group, indicating that the quasi-randomisation has built two similar groups. The average ED duration was the only variable that was significantly different between the groups with patients from the ONL group having a slightly longer ED duration at the point of inclusion in this study compared to patients from the WS group (p = 0.041). We checked whether the ED duration had impact on the study effects; as this was not the case, we did not consider this variable as covariate in the final analyses.

Table 1.
Clinical baseline characteristics of AN patients.
3.3. Main Outcomes
When contrasting the SUCCEAT WS group to the ONL group using general linear mixed models (Table 2), we found significant main effects of time for all outcome variables indicating improvement in BMI, psychopathology and quality of life independently of the group. We did not find significant time x group interaction effects for any outcome variable indicating that improvements were similar for the WS and ONL format of SUCCEAT. Baseline to 12-month FU effect sizes in terms of Cohen’s d (including 95% confidence intervals) are provided in Table 3. The effect sizes for BMI, BMI percentile and EDE scales were large in both groups. The effect sizes for self-reported ED psychopathology (EDI-2 score), motivation for change (ANSOCQ score), general psychopathology (YSR score) and quality of life (KINDL score) were in the small-to-medium range. In general, effect sizes tended to be slightly higher in the SUCCEAT ONL group compared to the WS group but as all the confidence intervals overlap, this difference is not statistically significant.

Table 2.
Results of the general linear mixed models analysing the change in outcome variables by group.

Table 3.
Baseline to 12-month follow-up effect sizes (Cohens’s d) by group.
3.4. Remission Rates
Figure 1 shows the remission rates of patients of the SUCCEAT WS and ONL group according to the DSM-5 diagnostic criteria at the 12-month FU assessment. Slightly higher rates for full remission were revealed for the SUCCEAT ONL group (48.4% vs. 28.1%), whereas the percentage of patients with no remission was 28.1% in the WS and 12.9% in the ONL group. However, the differences between the SUCCEAT WS and ONL groups were not statistically significant (Chi²(2) = 3.562, p = 0.168).
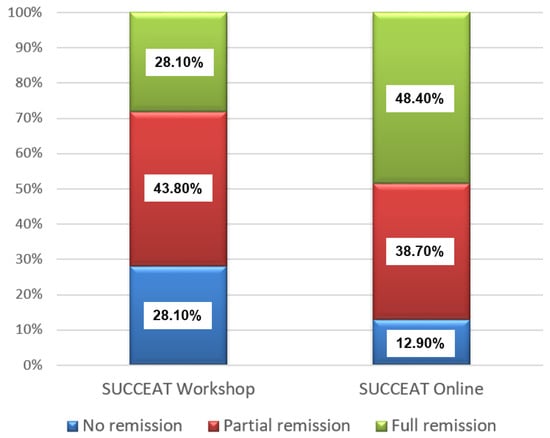
Figure 1.
Remission rates at 12-month follow-up for SUCCEAT and comparison group patients.
3.5. Harms
The caregivers and their children reported no harms. Despite including severely ill patients into the trial, there were no major events reported during the course of the trial and during FU.
4. Discussion
The main goal of this study was to examine the impact of SUCCEAT, a skills training for parents based on the cognitive interpersonal model of maintaining factors for EDs [10,11,12], delivered as WS or ONL, on adolescent patients’ outcome. All outcome variables (BMI percentile, ED psychopathology, attitudinal and behavioural dimensions of EDs, motivation to change, emotional and behavioural problems and quality of life) improved in adolescent patients in both groups (WS and ONL) after the intervention. This is similar to other studies, mainly in adults though, that reported improvements in single outcome variables (e.g., BMI [20,21]), AN symptoms [20,22], quality of life [20]). However, our study includes a broad spectrum of different outcome variables that clearly improve over time.
There was no difference with respect to the outcome variables between the WS and ONL format of SUCCEAT across the time points. Patients whose parents participated in the ONL group showed similar improvement as patients with parents participating in the face-to-face WS. We already reported that there were no differences between the WS and the ONL group regarding outcome variables in caregivers [14,15]. The findings of the present study therefore support the conclusion that the SUCCEAT-ONL intervention is as effective as the SUCCEAT-WS intervention in terms of caregivers’ and patients’ outcome. This is important as online interventions have become more and more important in the field of EDs [50,51] and are of high benefit concerning stigmatisation, the availability and the flexibility in time and place [52,53] as they offer an opportunity for families that might otherwise have difficulties accessing further help. Online treatments and online support have gained even more importance during the current COVID-19 pandemic, as their use have strongly been recommended in the field of EDs [19], especially when access to face-to-face treatment might be impeded in case of restrictions. Further research is needed to evaluate online programmes [54], particularly for caregivers. Online interventions might enable patients and their carers to get access to appropriate support earlier, which might be beneficial for the patients’ recovery [55]. On the other hand, online interventions in general and in the field of eating disorders have revealed pitfalls regarding adherence and acceptance, particularly if provided outside of a controlled research setting [56,57]. However, data on the adherence and acceptance of Internet-based interventions or caregivers is scare and needs to be further evaluated when interventions like SUCCEAT are implemented in routine care.
In detail, SUCCEAT delivered via WS and ONL positively affects patients’ outcome regarding weight gain and ED symptoms. Moreover, the positive effects were not limited to ED psychopathology. Motivation to change, general psychopathology and quality of life also improved over the course of the study. The finding that motivation to change increased indicated that patients were more willing to change their problem behaviour after their parents underwent the SUCCEAT interventions. MI and the TTM are key elements of SUCCEAT and aim to increase the intrinsic motivation to change of patients. High motivation to change is related to self-esteem, an active coping style, and predicts remission of AN [45]. Moreover, common comorbidities of EDs, like emotional and behavioural problems as well as anxiety and depression decreased. The quality of life of the adolescent patients increased in terms of emotional, physical and social wellbeing, self-esteem, and everyday functioning in school. This is similar to other studies [24,25], where adolescents reported decreased peer-problems, more pro-social behaviour [25] and adult patients showed an increased quality of life [24]. Sepulveda et al. [22] also reported a marginal improvement of general psychopathology/distress after a similar parental intervention in adult patients though. Yet, our study is the first study of a specialised skills training for parents of adolescent AN patients that revealed a broad spectrum of benefits including motivation to change, general psychopathology and quality of life.
The improvements of all the outcome variables were sustained over time after 12 months in both groups, which is also an important finding, as including a long-term FU is especially rare in this field [13,58,59,60,61]. These findings complement a previous study which has demonstrated that a reduction in HEE in caregivers (after having participated in a skills training) can positively affect the ED psychopathology and BMI in patients [15].
Finally, we investigated the remission rates of the patients at 12-month FU. The percentage of patients with full and partial remission was slightly higher in the WS group compared to the ONL group. About 72% of participants from the WS group showed full or partial remission at 12-month FU, while this percentage was 87% in the ONL group. Accordingly, slightly more patients of the WS group showed no remission at all compared to the ONL group. However, these differences failed to reach significance. Anyway, as it is known that up to 60% of ED patients might recover, whereas about one third of patients is at risk to develop a persisting ED [4], our results somehow reflect similar or even slightly better outcome.
This study has some strengths and limitations. It is the first study focusing on adolescents’ outcome when comparing a WS and an ONL intervention for caregivers including a long-term outcome. The core strengths were the usage of exactly the same design in both SUCCEAT groups (eight sessions or eight modules within the same time frame, the same materials, the possibility to get in touch with other caregivers face-to-face or through a moderated online forum) and access to professional guidance through the same coaches in both groups. Generalisability might however be limited as we included patients with AN and atypical AN and their caregivers only. Future studies should focus on families of patients with bulimia nervosa and binge eating disorder as well. A core limitation was the lack of a randomised control group. More work is needed including a randomised controlled trial and aftercare data to confirm the superiority of SUCCEAT over other specialised family interventions regarding the patients’ outcome. However, SUCCEAT provides the great benefit of an ONL version that is as effective as the WS form. Especially the ONL version might be more cost-effective, more time-saving and may involve more parents at once compared to WS interventions [21].
5. Conclusions
This study supports the assumption that adolescent patients with AN might benefit from interventions for their caregivers in addition to TAU, especially in the long-term. Our results strongly support the importance of involving the family in the treatment of adolescents with AN by offering SUCCEAT, a specialised training programme, including psychoeducation, problem solving skills and communication techniques. Equal efficacy of the ONL intervention is a major advantage and an important finding, especially in the current times when online interventions massively gain importance due to the COVID-19 pandemic as they highly increase intervention access. In sum, we recommend integrating a specific skills intervention for parents, potentially as an online support like SUCCEAT-ONL, for caregivers of adolescents with AN into the clinical routine care as an add-on to TAU.
Author Contributions
Conceptualization, A.F.K.K., J.T., J.P. and G.W.; methodology, C.F., J.P. and M.Z.; formal analysis, M.Z.; investigation, J.P., S.T., A.Z., C.F. and E.A.-W.; resources, H.I., E.A.-W., D.M., M.M., C.L., G.S., E.J., W.B.E., A.F.K.K. and G.W.; data curation, M.Z.; writing—original draft preparation, J.P. and C.F.; writing—review and editing, M.Z., A.F.K.K. and G.W.; visualisation, M.Z.; supervision, A.F.K.K. and G.W.; project administration, J.P., S.T., C.F., T.W., G.W. and A.F.K.K.; funding acquisition, A.F.K.K. and G.W. All authors have read and agreed to the published version of the manuscript.
Funding
This research was funded by “Gemeinsame Gesundheitsziele aus dem Rahmen-Pharmavertrag/ Pharma Master Agreement” (a cooperation between the Austrian pharmaceutical industry and the Austrian social insurance); Grant 99901002500, given to A.F.K.K. and G.W. The study protocol was approved by the Medical University of Vienna Ethics Committee (#1840/2013).
Institutional Review Board Statement
The study was conducted according to the guidelines of the Declaration of Helsinki, and approved by the Ethics Committee of the Medical University of Vienna (protocol code #1840/2013; date of approval: 16.10.2013).
Informed Consent Statement
Informed consent was obtained from all subjects involved in the study.
Data Availability Statement
The data that support the findings of this study are available from the corresponding author upon reasonable request.
Acknowledgments
We want to thank all the staff members who helped to conduct the study, as well as all patients and their caregivers who participated in this study.
Conflicts of Interest
J.T., J.P., T.W., G.W. and A.F.K.K. are co-authors of the book used in the SUCCEAT intervention. J.T. was part of the team that developed the DVD. J.P. provided coaching in the workshops and online intervention. The funders had no role in the design of the study; in the collection, analyses or interpretation of data; in the writing of the manuscript; or in the decision to publish the results.
Registration
This trial was registered at ClinicalTrials.gov (Identifier: NCT02480907).
Protocol
The study protocol can be accessed in [26].
References
- Zipfel, S.; Giel, K.E.; Bulik, C.M.; Hay, P.; Schmidt, U. Anorexia Nervosa: Aetiology, Assessment and Treatment. Lancet Psychiatry 2015, 2, 1099–1111. [Google Scholar] [CrossRef]
- Wagner, G.; Zeiler, M.; Waldherr, K.; Philipp, J.; Truttmann, S.; Dür, W.; Treasure, J.L.; Karwautz, A.F.K. Mental Health Problems in Austrian Adolescents: A Nationwide, Two-Stage Epidemiological Study Applying DSM-5 Criteria. Eur Child Adolesc. Psychiatry 2017, 26, 1483–1499. [Google Scholar] [CrossRef] [PubMed]
- American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders: DSM-5, 5th ed.; American Psychiatric Association, Ed.; American Psychiatric Association: Washington, DC, USA, 2013; ISBN 978-0-89042-554-1. [Google Scholar]
- Treasure, J.; Duarte, T.A.; Schmidt, U. Eating Disorders. Lancet 2020, 395, 899–911. [Google Scholar] [CrossRef]
- Karwautz, A.F.K.; Wagner, G.; Waldherr, K.; Nader, I.W.; Fernandez-Aranda, F.; Estivill, X.; Holliday, J.; Collier, D.A.; Treasure, J.L. Gene-Environment Interaction in Anorexia Nervosa: Relevance of Non-Shared Environment and the Serotonin Transporter Gene. Mol. Psychiatry 2011, 16, 590–592. [Google Scholar] [CrossRef] [PubMed]
- Zabala, M.J.; Macdonald, P.; Treasure, J. Appraisal of Caregiving Burden, Expressed Emotion and Psychological Distress in Families of People with Eating Disorders: A Systematic Review. Eur. Eat. Disord. Rev. 2009, 17, 338–349. [Google Scholar] [CrossRef] [PubMed]
- Rhind, C.; Salerno, L.; Hibbs, R.; Micali, N.; Schmidt, U.; Gowers, S.; Macdonald, P.; Goddard, E.; Todd, G.; Tchanturia, K.; et al. The Objective and Subjective Caregiving Burden and Caregiving Behaviours of Parents of Adolescents with Anorexia Nervosa. Eur. Eat. Disord. Rev. 2016, 24, 310–319. [Google Scholar] [CrossRef]
- Kyriacou, O.; Treasure, J.; Schmidt, U. Understanding How Parents Cope with Living with Someone with Anorexia Nervosa: Modelling the Factors That Are Associated with Carer Distress. Int. J. Eat. Disord. 2008, 41, 233–242. [Google Scholar] [CrossRef]
- Anastasiadou, D.; Medina-Pradas, C.; Sepulveda, A.R.; Treasure, J. A Systematic Review of Family Caregiving in Eating Disorders. Eat. Behav. 2014, 15, 464–477. [Google Scholar] [CrossRef]
- Schmidt, U.; Treasure, J. Anorexia Nervosa: Valued and Visible. A Cognitive-Interpersonal Maintenance Model and Its Implications for Research and Practice. Br. J. Clin. Psychol. 2006, 45, 343–366. [Google Scholar] [CrossRef]
- Treasure, J.; Schmidt, U. The Cognitive-Interpersonal Maintenance Model of Anorexia Nervosa Revisited: A Summary of the Evidence for Cognitive, Socio-Emotional and Interpersonal Predisposing and Perpetuating Factors. J. Eat. Disord. 2013, 1, 13. [Google Scholar] [CrossRef]
- Treasure, J.; Willmott, D.; Ambwani, S.; Cardi, V.; Bryan, D.C.; Rowlands, K.; Schmidt, U. Cognitive Interpersonal Model for Anorexia Nervosa Revisited: The Perpetuating Factors That Contribute to the Development of the Severe and Enduring Illness. J. Clin. Med. 2020, 9, 630. [Google Scholar] [CrossRef]
- Hibbs, R.; Rhind, C.; Leppanen, J.; Treasure, J. Interventions for Caregivers of Someone with an Eating Disorder: A Meta-Analysis. Int. J. Eat. Disord. 2015, 48, 349–361. [Google Scholar] [CrossRef]
- Truttmann, S.; Philipp, J.; Zeiler, M.; Franta, C.; Wittek, T.; Merl, E.; Schöfbeck, G.; Koubek, D.; Laczkovics, C.; Imgart, H.; et al. Long-Term Efficacy of the Workshop Vs. Online SUCCEAT (Supporting Carers of Children and Adolescents with Eating Disorders) Intervention for Parents: A Quasi-Randomised Feasibility Trial. J. Clin. Med. 2020, 9, 1912. [Google Scholar] [CrossRef]
- Philipp, J.; Truttmann, S.; Zeiler, M.; Franta, C.; Wittek, T.; Schöfbeck, G.; Mitterer, M.; Mairhofer, D.; Zanko, A.; Imgart, H.; et al. Reduction of High Expressed Emotion and Treatment Outcomes in Anorexia Nervosa—Caregivers’ and Adolescents’ Perspective. J. Clin. Med. 2020, 9, 2021. [Google Scholar] [CrossRef]
- Zeiler, M.; Philipp, J.; Truttmann, S.; Wittek, T.; Franta, C.; Imgart, H.; Zanko, A.; Auer-Welsbach, E.; Kahlenberg, L.; Wagner, G.; et al. A German Version of the Caregiver Skills Scale for Caregivers of Patients with Anorexia Nervosa. Eur. Eat. Disord. Rev. 2021, 29, 257–268. [Google Scholar] [CrossRef]
- Spencer, L.; Potterton, R.; Allen, K.; Musiat, P.; Schmidt, U. Internet-Based Interventions for Carers of Individuals with Psychiatric Disorders, Neurological Disorders, or Brain Injuries: Systematic Review. J. Med. Internet Res. 2019, 21, e10876. [Google Scholar] [CrossRef]
- Dimitropoulos, G.; Landers, A.; Freeman, V.; Novick, J.; Schmidt, U.; Olmsted, M. A Feasibility Study Comparing a Web-Based Intervention to a Workshop Intervention for Caregivers of Adults with Eating Disorders. Eur. Eat. Disord. Rev. 2019, 27, 641–654. [Google Scholar] [CrossRef] [PubMed]
- Fernández-Aranda, F.; Casas, M.; Claes, L.; Bryan, D.C.; Favaro, A.; Granero, R.; Gudiol, C.; Jiménez-Murcia, S.; Karwautz, A.; Grange, D.L.; et al. COVID-19 and Implications for Eating Disorders. Eur. Eat. Disord. Rev. 2020, 28, 239–245. [Google Scholar] [CrossRef]
- Magill, N.; Rhind, C.; Hibbs, R.; Goddard, E.; Macdonald, P.; Arcelus, J.; Morgan, J.; Beecham, J.; Schmidt, U.; Landau, S.; et al. Two-Year Follow-up of a Pragmatic Randomised Controlled Trial Examining the Effect of Adding a Carer’s Skill Training Intervention in Inpatients with Anorexia Nervosa. Eur. Eat. Disord. Rev. 2016, 24, 122–130. [Google Scholar] [CrossRef] [PubMed]
- Whitney, J.; Murphy, T.; Landau, S.; Gavan, K.; Todd, G.; Whitaker, W.; Treasure, J. A Practical Comparison of Two Types of Family Intervention: An Exploratory RCT of Family Day Workshops and Individual Family Work as a Supplement to Inpatient Care for Adults with Anorexia Nervosa. Eur. Eat. Disord. Rev. 2012, 20, 142–150. [Google Scholar] [CrossRef] [PubMed]
- Sepulveda, A.R.; Anastasiadou, D.; Parks, M.; Gutiérrez, E. A Controlled Study of the Collaborative Care Skills Workshops versus Psycho-Educational Workshops among Spanish Caregivers of Relatives with an Eating Disorder. Eur. Eat. Disord. Rev. 2019, 27, 247–262. [Google Scholar] [CrossRef]
- Marcos, Y.Q.; Sebastián, M.J.Q.; Herrera, M.E.; Sanmartín, R.; Treasure, J. Testing Carer Skill Training Programs in Spanish Carers of Patients with Eating Disorders. Psicothema 2018, 30, 295–303. [Google Scholar] [CrossRef]
- Hibbs, R.; Magill, N.; Goddard, E.; Rhind, C.; Raenker, S.; Macdonald, P.; Todd, G.; Arcelus, J.; Morgan, J.; Beecham, J.; et al. Clinical Effectiveness of a Skills Training Intervention for Caregivers in Improving Patient and Caregiver Health Following In-Patient Treatment for Severe Anorexia Nervosa: Pragmatic Randomised Controlled Trial. BJPsych Open 2015, 1, 56–66. [Google Scholar] [CrossRef]
- Hodsoll, J.; Rhind, C.; Micali, N.; Hibbs, R.; Goddard, E.; Nazar, B.P.; Schmidt, U.; Gowers, S.; Macdonald, P.; Todd, G.; et al. A Pilot, Multicentre Pragmatic Randomised Trial to Explore the Impact of Carer Skills Training on Carer and Patient Behaviours: Testing the Cognitive Interpersonal Model in Adolescent Anorexia Nervosa. Eur. Eat. Disord. Rev. 2017, 25, 551–561. [Google Scholar] [CrossRef] [PubMed]
- Franta, C.; Philipp, J.; Waldherr, K.; Truttmann, S.; Merl, E.; Schöfbeck, G.; Koubek, D.; Laczkovics, C.; Imgart, H.; Zanko, A.; et al. Supporting Carers of Children and Adolescents with Eating Disorders in Austria (SUCCEAT): Study Protocol for a Randomised Controlled Trial. Eur. Eat. Disord. Rev. 2018, 26, 447–461. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. International Statistical Classification of Diseases and Related Health Problems, 10th ed.; World Health Organization: Geneva, Switzerland, 2009; ISBN 978-92-4-154766-6. [Google Scholar]
- National Guideline Alliance (UK). Eating Disorders: Recognition and Treatment; National Institute for Health and Care Excellence: Clinical Guidelines. Natl. Inst. Health Care Excell. 2017. Available online: https://www.nice.org.uk/guidance/ng69/resources/eating-disorders-recognition-and-treatment-pdf-1837582159813 (accessed on 26 April 2021).
- Treasure, J.; Schmidt, U.; Macdonald, P. The Clinician’s Guide to Collaborative Caring in Eating Disorders: The New Maudsley Method; Routledge: London, UK, 2010; ISBN 978-0-203-86468-5. [Google Scholar]
- Treasure, J.; Smith, G.; Crane, A. Skills-Based Caring for a Loved One with an Eating Disorder: The New Maudsley Method, 2nd ed.; Routledge: London, UK, 2017; ISBN 978-1-138-82663-2. [Google Scholar]
- Treasure, J.; Smith, G.; Crane, A. Skills-Based Learning for Caring for a Loved One with an Eating Disorder: The New Maudsley Method; Routledge: London, UK, 2007; ISBN 978-0-415-43158-3. [Google Scholar]
- Treasure, J.; Smith, G.; Crane, A.; Karwautz, A.; Wagner, G.; Philipp, J.; Wittek, T. Unterstützung für Angehörige von Menschen mit Essstörungen ein Leitfaden für Eltern, Geschwister, Partner und Fachpersonal; Facultas, Routledge: Vienna, Austria, 2020; ISBN 978-3-7089-1760-3. [Google Scholar]
- Langley, J.; Todd, G.; Treasure, J. Caring for a Loved One with an Eating Disorder: The New Maudsley Skills-Based Training Manual; Routledge: London, UK, 2019; ISBN 978-0-8153-7832-7. [Google Scholar]
- Treasure, J.; Whitaker, W.; Todd, G.; Whitney, J. A Description of Multiple Family Workshops for Carers of People with Anorexia Nervosa. Eur. Eat. Disord. Rev. 2012, 20, e17–e22. [Google Scholar] [CrossRef] [PubMed]
- Miller, W.R.; Rollnick, S. Motivational Interviewing: Preparing People for Change, 2nd ed.; Guilford Press: New York, NY, USA, 2002; ISBN 978-1-57230-563-2. [Google Scholar]
- Prochaska, J.O.; DiClemente, C.C. The Transtheoretical Approach: Crossing Traditional Boundaries of Therapy; Dow Jones-Irwin: Homewood, IL, USA, 1984; ISBN 978-0-87094-438-3. [Google Scholar]
- Ellis, A. Humanistic Psychotherapy: The Rational-Emotive Approach; McGraw-Hill: New York, NY, USA, 1975; ISBN 978-0-07-019237-9. [Google Scholar]
- The Succeed Foundation. How to Care for Someone with an Eating Disorder. Learn. The Techniques Designed by One of the World’s Top. Eating Disorder Researchers. 2011. Available online: https://thenewmaudsleyapproach.co.uk (accessed on 26 April 2021).
- Kromeyer-Hauschild, K.; Wabitsch, M.; Kunze, D.; Geller, F.; Geiß, H.C.; Hesse, V.; von Hippel, A.; Jaeger, U.; Johnsen, D.; Korte, W.; et al. Perzentile für den Body-mass-Index für das Kindes- und Jugendalter unter Heranziehung verschiedener deutscher Stichproben. Mon. Kinderheilkd 2001, 149, 807–818. [Google Scholar] [CrossRef]
- Hilbert, A.; Tuschen-Caffier, B. Eating Disorder Examination: Deutschsprachige Übersetzung; Verlag für Psychotherapie: Münster, Germany, 2006. [Google Scholar]
- Hilbert, A.; Tuschen-Caffier, B. Eating Disorder Examination, 2nd ed.; dgvt-Verlag: Tübingen, Germany, 2016; ISBN 978-3-87159-411-3. [Google Scholar]
- Paul, T.; Thiel, A. EDI-2. Eating Disorder Inventory-2; Hogrefe: Göttingen, Germany, 2005. [Google Scholar]
- Rieger, E.; Touyz, S.W.; Beumont, P.J.V. The Anorexia Nervosa Stages of Change Questionnaire (ANSOCQ): Information Regarding Its Psychometric Properties. Int. J. Eat. Disord. 2002, 32, 24–38. [Google Scholar] [CrossRef]
- Rieger, E.; Touyz, S.; Schotte, D.; Beumont, P.; Russell, J.; Clarke, S.; Kohn, M.; Griffiths, R. Development of an Instrument to Assess Readiness to Recover in Anorexia Nervosa. Int. J. Eat. Disord. 2000, 28, 387–396. [Google Scholar] [CrossRef]
- Pauli, D.; Aebi, M.; Winkler Metzke, C.; Steinhausen, H.-C. Motivation to Change, Coping, and Self-Esteem in Adolescent Anorexia Nervosa: A Validation Study of the Anorexia Nervosa Stages of Change Questionnaire (ANSOCQ). J. Eat. Disord. 2017, 5, 11. [Google Scholar] [CrossRef] [PubMed]
- Arbeitsgruppe Deutsche Child Behavior Checklist. Fragebogen Für Jugendliche; Deutsche Bearbeitung Der Youth Self-Report Form Der Child Behavior Checklist (YSR). Einführung Und Anleitung Zur Handauswertung Mit Deutschen Normen, Bearbeitet von M.; Döpfner, J. Plück, S. Bölte, K. Lenz, P. Melchers & K. Heim (2. Aufl.); Arbeitsgruppe Kinder-, Jugend- und Familiendiagnostik (KJFD): Köln, Germany, 1991. [Google Scholar]
- Ravens-Sieberer, U.; Bullinger, M. News from the KINDL-QuestionnaireA New Version for Adolescents. Qual. Life Res. 1998, 7, 653. [Google Scholar]
- Ravens-Sieberer, U.; Bullinger, M. Assessing Health Related Quality of Life in Chronically Ill Children with the German KINDL: First Psychometric and Content-Analytical Results. Qual. Life Res. 1998, 7, 399–407. [Google Scholar] [CrossRef]
- Higgins, J.; Green, S. Cochrane Handbook for Systematic Reviews of Interventions. Available online: https://handbook-5-1.cochrane.org/ (accessed on 29 April 2020).
- de Zwaan, M. Should we use new media in the treatment of eating disorders? Psychother. Psychosom. Med. Psychol. 2015, 65, 30–32. [Google Scholar] [CrossRef]
- Wagner, G.; Penelo, E.; Wanner, C.; Gwinner, P.; Trofaier, M.-L.; Imgart, H.; Waldherr, K.; Wöber-Bingöl, C.; Karwautz, A.F.K. Internet-Delivered Cognitive-Behavioural Therapy v. Conventional Guided Self-Help for Bulimia Nervosa: Long-Term Evaluation of a Randomised Controlled Trial. Br. J. Psychiatry 2013, 202, 135–141. [Google Scholar] [CrossRef]
- Titov, N.; Hadjistavropoulos, H.D.; Nielssen, O.; Mohr, D.C.; Andersson, G.; Dear, B.F. From Research to Practice: Ten Lessons in Delivering Digital Mental Health Services. J. Clin. Med. 2019, 8, 1239. [Google Scholar] [CrossRef]
- Taylor, C.B.; Fitzsimmons-Craft, E.E.; Graham, A.K. Digital Technology Can Revolutionize Mental Health Services Delivery: The COVID-19 Crisis as a Catalyst for Change. Int. J. Eat. Disord. 2020, 53, 1155–1157. [Google Scholar] [CrossRef]
- Loucas, C.E.; Fairburn, C.G.; Whittington, C.; Pennant, M.E.; Stockton, S.; Kendall, T. E-Therapy in the Treatment and Prevention of Eating Disorders: A Systematic Review and Meta-Analysis. Behav. Res. Ther. 2014, 63, 122–131. [Google Scholar] [CrossRef]
- Fairburn, C.G.; Murphy, R. Treating Eating Disorders Using the Internet. Curr. Opin. Psychiatry 2015, 28, 461–467. [Google Scholar] [CrossRef]
- Eysenbach, G. The Law of Attrition. J. Med. Internet Res. 2005, 7, e11. [Google Scholar] [CrossRef]
- Zeiler, M.; Kuso, S.; Nacke, B.; Klesges, L.M.; Waldherr, K. Evaluating Reach, Adoption, Implementation and Maintenance of Internet-Based Interventions to Prevent Eating Disorders in Adolescents: A Systematic Review. Eur. J. Public Health 2020, 30, 179–188. [Google Scholar] [CrossRef]
- Isserlin, L.; Spettigue, W.; Norris, M.; Couturier, J. Outcomes of Inpatient Psychological Treatments for Children and Adolescents with Eating Disorders at Time of Discharge: A Systematic Review. J. Eat. Disord. 2020, 8, 32. [Google Scholar] [CrossRef] [PubMed]
- Zeeck, A.; Herpertz-Dahlmann, B.; Friederich, H.-C.; Brockmeyer, T.; Resmark, G.; Hagenah, U.; Ehrlich, S.; Cuntz, U.; Zipfel, S.; Hartmann, A. Psychotherapeutic Treatment for Anorexia Nervosa: A Systematic Review and Network Meta-Analysis. Front. Psychiatry 2018, 9, 158. [Google Scholar] [CrossRef] [PubMed]
- Schlegl, S.; Bürger, C.; Schmidt, L.; Herbst, N.; Voderholzer, U. The Potential of Technology-Based Psychological Interventions for Anorexia and Bulimia Nervosa: A Systematic Review and Recommendations for Future Research. J. Med. Internet Res. 2015, 17, e85. [Google Scholar] [CrossRef]
- Berg, E.; Houtzager, L.; Vos, J.; Daemen, I.; Katsaragaki, G.; Karyotaki, E.; Cuijpers, P.; Dekker, J. Meta-analysis on the Efficacy of Psychological Treatments for Anorexia Nervosa. Eur. Eat. Disord. Rev. 2019, 27, 331–351. [Google Scholar] [CrossRef] [PubMed]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).