Beyond the Pandemic: COVID-19 Pandemic Changed the Face of Life
Abstract
1. Introduction
| Life Sectors | Negatives | Positives | References |
|---|---|---|---|
| Economy | Massive losses of money, layoffs, more tension in all sectors | Learning lessons and making plans for similar future occurrences | [7,8] |
| Lifestyle | Tensions; domestic violence; isolation; loneliness, especially with elder people; loss of physical activity; lack of supplies among poor people; and increased internet demands | Staying home, more sleep, less stress, more time with families, and less traffic | [9,10,11,12,13,14,15,16,17,18] |
| Working from home is a double-edged sword with faithful comfort but stress in daily home routines. | [19] | ||
| Transportation | Mainly economic and financial loss | Encouraging the use of green transportation and educating about its consequences | [20,21,22,23] |
| This was reflected in energy, as the quantities of fuel consumption decreased due to less flying and less use of transportation, etc. but a slower transition to green deal was also presented as economies put money into the pandemic. | [6] | ||
| Internet and social media | Misleading information | Medical use of social media, the appointment of documented pages for international health organizations, rapid transmission of medical instructions, some economies saved, and e-learning | [24,25,26,27] |
| Education | Higher drop-out rates of students and medical educational institutions, with the focus only on COVID-19 and fear of the future among students, and closed schools | The transition to e-learning and paying attention to infrastructure plans for pandemics in the future, especially in developing countries | [28,29,30] |
| Research activities | Research routines stopped at most universities and research centers | Research focus on vaccine production, high financial support for points related to COVID-19, and open access journals made free | [3,31] |
| Rapid publication shared the downsides of scientific inefficiency and the advantages of quick access to solutions. | [32] | ||
| Health | COVID-19 as a new disease, psychological effects, fear of disease and infection, anxiety, obesity, eye problems due to long durations sitting in front of screens, many deaths among health workers, and extreme pressure on the global health sector | Races against time, the use of new technologies, revolution in intertwining biotechnology and medical sciences, quick vaccine production, and digitalization of health systems | [33,34,35,36] |
| Environmental aspects | Wildlife as a source of energy and wildlife tourism | Nature recovery, reduction in heat emissions and toxic gases (NO2, SO2, CO, CO2, etc.), recovery of the ozone layer, and water cleanliness (Italy and India) | [37,38,39,40,41] |
2. Global Economic Recession
2.1. During the Peak Period of the COVID-19 Outbreak
- -
- One-fourth of Italy’s Gross Domestic Product (GDP) affected by emergency lockdown;
- -
- Some of the largest car manufacturers in the world suspended their production in Europe, such as Volkswagen and Ferrari;
- -
- Airbus production stopped in France and Spain;
- -
- Five million workers in China lost their jobs;
- -
- 85% of Norwegian Air canceled its flights and temporarily laid off 90% of their staff (7300 employees during 16 March 2020) [50];
- -
- As a result of the lockdown period of the pandemic, some famous tourist destinations (i.e., in Paris, Rome, Venice, and Madrid) were completely deserted [50];
- -
- China’s industrial production declined by 13.5% during January and February [45].
2.2. After the Shock Period and Updates
2.3. Transportation
3. Lifestyle during the COVID-19 Pandemic
3.1. Staying at Home
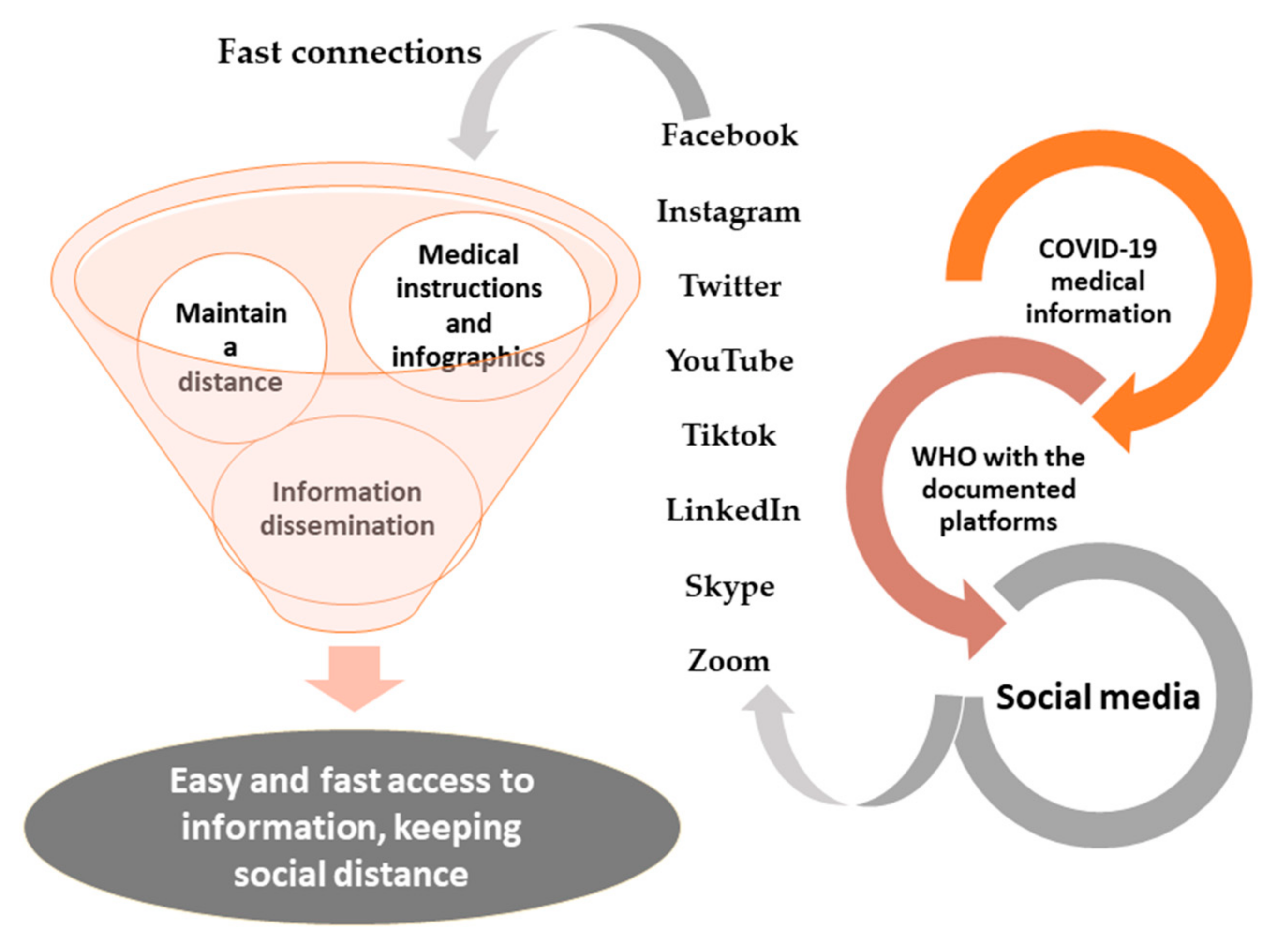
3.2. Social Media
4. Education and Research Activities during the COVID-19 Pandemic
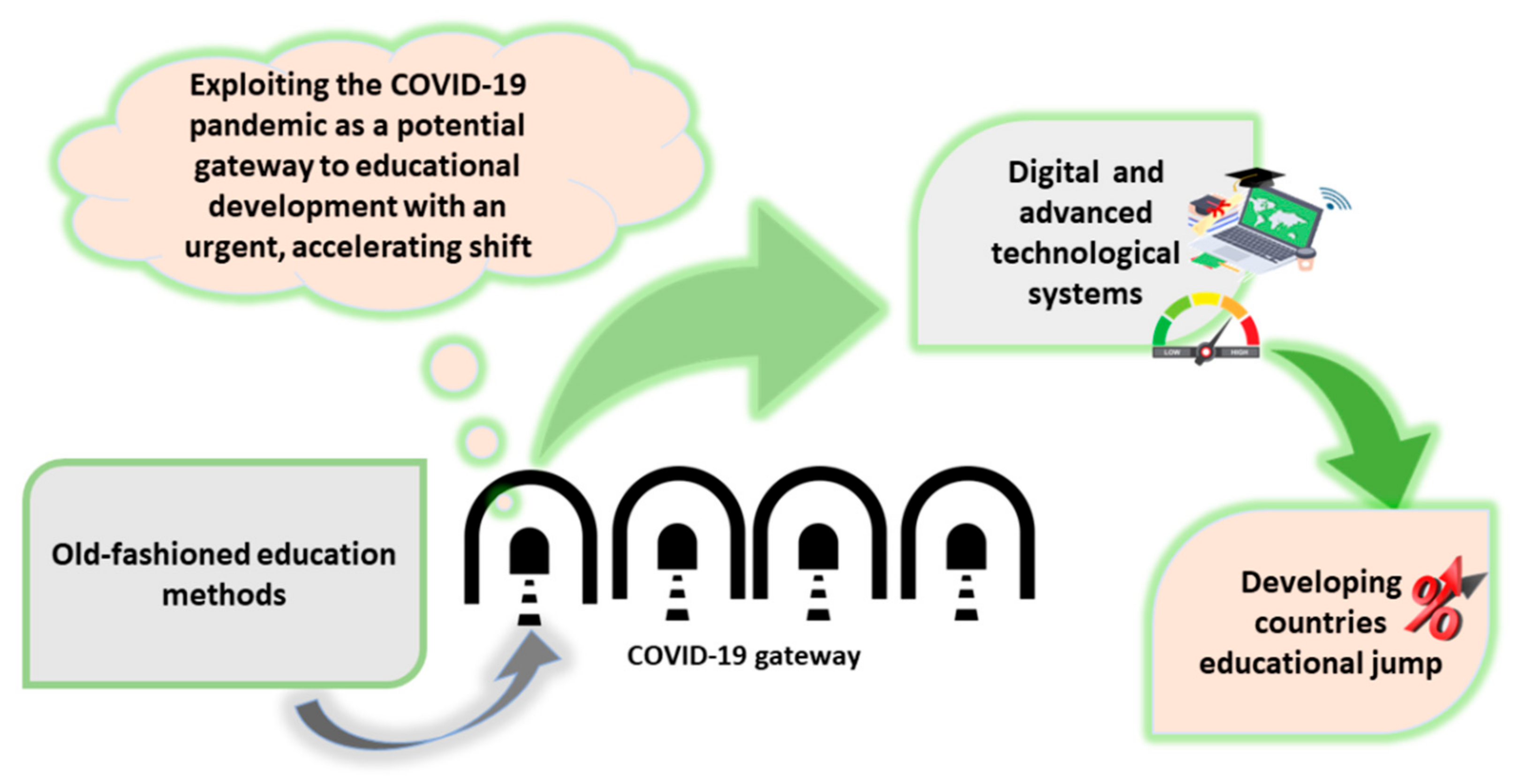
4.1. Education
4.2. Egyptian Education System as an Example
4.3. Research Activities
- -
- -
- -
- Carrying out meta-analyses of relevant literature and research in the field [96].
4.4. Research Activities and Gender Imbalance
5. Health Sector during the COVID-19 Pandemic
5.1. Food Supply, Dietary Patterns, Nutrition, and Health
5.2. Health and Psychological Effects on Students during the School Closures
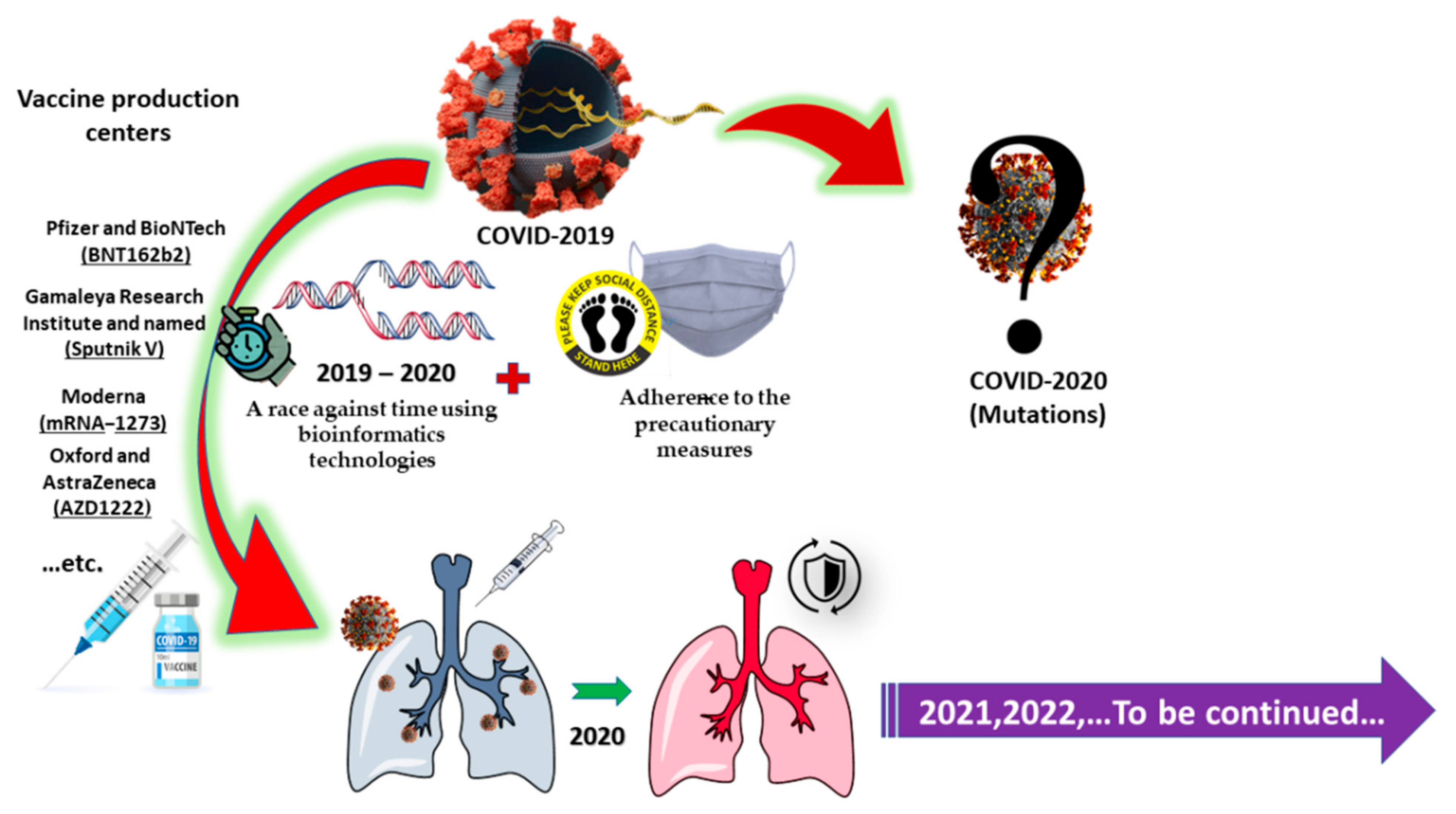
5.3. Vaccine Production
6. Global Warming and Reports on Weather and the Environment during the COVID-19 Pandemic
7. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Lai, C.C.; Shih, T.P.; Ko, W.C.; Tang, H.J.; Hsueh, P.R. Severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) and coronavirus disease-2019 (COVID-19): The epidemic and the challenges. Int. J. Antimicrob. Agents 2020, 55, 105924–105932. [Google Scholar] [CrossRef]
- Dwivedi, Y.K.; Hughes, D.L.; Coombs, C.; Constantiou, I.; Duan, Y.; Edwards, J.S.; Gupta, B.; Lal, B.; Misra, S.; Prashant, P.; et al. Impact of COVID-19 pandemic on information management research and practice: Transforming education, work and life. Int. J. Inf. Manag. 2020, 55, 102211–102230. [Google Scholar] [CrossRef]
- Omary, M.B.; Eswaraka, J.; Kimball, S.D.; Moghe, P.V.; Panettieri, R.A.; Scotto, K.W. The COVID-19 pandemic and research shutdown: Staying safe and productive. J. Clin. Investig. 2020, 130, 2745–2748. [Google Scholar] [CrossRef]
- Király, O.; Potenza, M.N.; Stein, D.J.; King, D.L.; Hodgins, D.C.; Saunders, J.B.; Grif, M.D.; Gjoneska, B.; Billieux, J.; Brand, M.; et al. Preventing problematic internet use during the COVID-19 pandemic: Consensus guidance. Compr. Psychiatry 2020, 100, 152180–152184. [Google Scholar] [CrossRef] [PubMed]
- De Oliveira Neto, L.; Elsangedy, H.M.; de Oliveira Tavares, V.D.; Teixeira, C.V.L.S.; Behm, D.G.; Da Silva-Grigoletto, M.E. TrainingInHome-training at home during the COVID-19 (SARS-CoV-2) pandemic: Physical exercise and behavior-based approach. Braz. J. Exerc. Physiol. 2020, 19, 9–19. [Google Scholar]
- Chakraborty, I.; Maity, P. COVID-19 outbreak: Migration, effects on society, global environment and prevention. Sci. Total Environ. 2020, 728, 138882–138888. [Google Scholar] [CrossRef] [PubMed]
- Coleman, T.S. Thoughts on Financial Crises and Coronavirus. 1–4. 2020. Available online: http://www.hilerun.org/econ/papers/FinCrisesThoughts_20200313.pdf (accessed on 22 May 2021).
- Wang, Q.; Zhang, F. What does the China’s economic recovery after COVID-19 pandemic mean for the economic growth and energy consumption of other countries? J. Clean. Prod. 2021, 295, 126265–126284. [Google Scholar] [CrossRef]
- Altena, E.; Baglioni, C.; Espie, C.A.; Ellis, J.; Gavriloff, D.; Holzinger, B.; Schlarb, A.; Frase, L.; Jernelöv, S.; Riemann, D. Dealing with sleep problems during home confinement due to the COVID-19 outbreak: Practical recommendations from a task force of the European CBT-I Academy. J. Sleep Res. 2020, 29, e13052. [Google Scholar] [CrossRef]
- Douglas, M.; Katikireddi, S.V.; Taulbut, M.; Mckee, M.; Mccartney, G. Mitigating the wider health effects of covid-19 pandemic. BMJ 2020, 369, 1557–1562. [Google Scholar] [CrossRef] [PubMed]
- Allen-Ebrahimian, B. China’s Domestic Violence Epidemic. Axios. 2020. Available online: https://www.axios.com/china-domestic-violence-coronavirus-quarantine-7b00c3ba-35bc-4d16-afdd-b76ecfb28882.html (accessed on 19 March 2021).
- Guenfoud, I. French Women Use Code Words at Pharmacies to Escape Domestic Violence during Coronavirus. 2020. Available online: https://abcnews.go.com/International/french-women-code-words-pharmacies-escape-domestic-violence/story?id=69954238 (accessed on 19 March 2021).
- Piquero, A.R.; Jennings, W.G.; Jemison, E.; Kaukinen, C.; Knaul, F.M. Domestic violence during the COVID-19 pandemic-Evidence from a systematic review and meta-analysis. J. Crim. Justice 2021, 74, 101806–101815. [Google Scholar] [CrossRef]
- Feldmann, A.; Gasser, O.; Lichtblau, F.; Pujol, E.; Poese, I.; Dietzel, C.; Wagner, D.; Wichtlhuber, M.; Tapiador, J.; Vallina-Rodriguez, N.; et al. The lockdown effect: Implications of the COVID-19 pandemic on internet traffic. In Proceedings of the ACM Internet Measurement Conference, Pittsburgh, PA, USA, 27–29 October 2020; Volume 2008, pp. 10959–10976. [Google Scholar] [CrossRef]
- Usher, K.; Bhullar, N.; Durkin, J.; Gyamfi, N.; Jackson, D. Family violence and COVID-19: Increased vulnerability and reduced options for support. Int. J. Ment. Health 2020, 29, 549–552. [Google Scholar] [CrossRef] [PubMed]
- Campbell, A.M. An increasing risk of family violence during the Covid-19 pandemic : Strengthening community collaborations to save lives. Forensic Sci. Int. Rep. 2020, 2, 100089–100091. [Google Scholar] [CrossRef]
- Ammar, A.; Brach, M.; Trabelsi, K.; Chtourou, H.; Boukhris, O.; Masmoudi, L.; Bouaziz, B.; Bentlage, E.; How, D.; Ahmed, M.; et al. Effects of COVID-19 home confinement on eating behaviour and physical activity: Results of the ECLB-COVID19 international online survey. Nutrients 2020, 12, 1583. [Google Scholar] [CrossRef]
- Puig-Domingo, M.; Marazuela, M.; Giustina, A. COVID-19 and endocrine diseases. A statement from the European Society of Endocrinology. Endocrine 2020, 68, 2–5. [Google Scholar] [CrossRef] [PubMed]
- Purwanto, A.; Asbari, M.; Fahlevi, M.; Mufid, A.; Agistiawati, E.; Cahyono, Y.; Suryani, P. Impact of work from home (WFH) on Indonesian teachers performance during the Covid-19 pandemic: An exploratory study. Int. J. Adv. Sci. Technol. 2020, 29, 6235–6244. [Google Scholar]
- Vos, J. De The effect of COVID-19 and subsequent social distancing on travel behavior. Transp. Res. Interdiscip. Perspect. 2020, 5, 100121–100123. [Google Scholar] [CrossRef]
- IATA. IATA Economics’ Chart of the Week. International Air Transport Association. Available online: https//www.iata.org/en/iata-repository/publications/economic-reports/covid-2019-delivers-unprecedented-shock/2020 (accessed on 2 October 2020).
- Tirachini, A. COVID-19 and public transportation: Current assessment, prospects, and research needs. J. Public Transp. 2020, 22, 1–21. [Google Scholar] [CrossRef]
- Amankwah-amoah, J. Stepping up and stepping out of COVID-19: New challenges for environmental sustainability policies in the global airline industry. J. Clean. Prod. 2020, 271, 123000–123007. [Google Scholar] [CrossRef]
- Mandrola, J.; Futyma, P. The role of social media in cardiology. Trends Cardiovasc. Med. 2020, 30, 32–35. [Google Scholar] [CrossRef]
- Höttecke, D.; Allchin, D. Reconceptualizing nature-of-science education in the age of social media. Sci. Educ. 2020, 104, 641–666. [Google Scholar] [CrossRef]
- Merchant, R.M.; Lurie, N. Social media and emergency preparedness in response to novel coronavirus. JAMA 2020, 323, 2011–2012. [Google Scholar] [CrossRef] [PubMed]
- Huerta-álvarez, R.; Cambra-fierro, J.J.; Fuentes-blasco, M. The interplay between social media communication, brand equity and brand engagement in tourist destinations: An analysis in an emerging economy. J. Destin. Mark. Manag. 2020, 16, 100413–100424. [Google Scholar] [CrossRef]
- Timmis, S.; Broadfoot, P.; Sutherland, R.; Oldfield, A. Rethinking assessment in a digital age: Opportunities, challenges and risks. Br. Educ. Res. J. 2016, 42, 454–476. [Google Scholar] [CrossRef]
- Viner, R.M.; Russell, S.J.; Croker, H.; Packer, J.; Ward, J.; Stansfield, C.; Mytton, O.; Bonell, C.; Booy, R. Review school closure and management practices during coronavirus outbreaks including COVID-19: A rapid systematic review. Lancet Child Adolesc. Health 2020, 4, 397–404. [Google Scholar] [CrossRef]
- Ahmed, H.; Allaf, M.; Elghazaly, H. COVID-19 and medical. Lancet Infect. Dis. 2020, 2019, 777–778. [Google Scholar] [CrossRef]
- Ghebreyesus, T.A. Safeguard research in the time of COVID-19. Nat. Med. 2020, 26, 443. [Google Scholar] [CrossRef]
- Chahrour, M.; Assi, S.; Bejjani, M.; Nasrallah, A.A.; Salhab, H.; Fares, M.; Khachfe, H.H. A bibliometric analysis of COVID-19 research activity: A call for increased output. Cureus 2020, 2, e7357. [Google Scholar] [CrossRef]
- Mattioli, A.V.; Sciomer, S.; Cocchi, C.; Maffei, S.; Gallina, S. Quarantine during COVID-19 outbreak: Changes in diet and physical activity increase the risk of cardiovascular disease. Nutr. Metab. Cardiovasc. Dis. 2020, 30, 1409–1417. [Google Scholar] [CrossRef]
- Callaway, E. What Pfizer’s landmark COVID vaccine results mean for the pandemic. Nature 2020, 1–7. [Google Scholar] [CrossRef]
- Matsungo, T.M.; Chopera, P. The effect of the COVID-19 induced lockdown on nutrition, health and lifestyle patterns among adults in Zimbabwe. medRxiv 2020, 3, 205–212. [Google Scholar] [CrossRef]
- Mattioli, A.V.; Nasi, M.; Farinetti, A. COVID-19 pandemic: The effects of quarantine on cardiovascular risk. Eur. J. Clin. Nutr. 2020, 74, 852–855. [Google Scholar] [CrossRef]
- Lindsey, P.; Allan, J.; Brehony, P.; Dickman, A.; Robson, A.; Begg, C.; Bhammar, H.; Blanken, L.; Breuer, T.; Fitzgerald, K. Conserving Africa’s wildlife and wildlands through the COVID-19 crisis and beyond. Nat. Ecol. Evol. 2020, 4, 1300–1310. [Google Scholar] [CrossRef]
- Feldman, A.L.; Chávez, C.; Vélez, M.A.; Bejarano, H.; Chimeli, A.B.; Féres, J.; Robalino, J. Environmental impacts and policy responses to Covid-19: A view from Latin America. Environ. Resour. Econ. 2020, 13, 1–6. [Google Scholar] [CrossRef]
- Mandal, I.; Pal, S. COVID-19 pandemic persuaded lockdown effects on environment over stone quarrying and crushing areas. Sci. Total Environ. 2020, 732, 139281–139290. [Google Scholar] [CrossRef]
- Zambrano-monserrate, M.A.; Alejandra, M.; Sanchez-alcalde, L. Indirect effects of COVID-19 on the environment. Sci. Total Environ. 2020, 728, 138813–138816. [Google Scholar] [CrossRef]
- Saadat, S.; Rawtani, D.; Mustansar, C. Environmental perspective of COVID-19. Sci. Total Environ. 2020, 728, 138870–138875. [Google Scholar] [CrossRef]
- Khalifa, S.A.M.; Mohamed, B.S.; Elashal, M.H.; Du, M.; Guo, Z.; Zhao, C.; Musharraf, S.G.; Boskabady, M.H.; El-Seedi, H.H.R.; Efferth, T.; et al. Comprehensive overview on multiple strategies fighting covid-19. Int. J. Environ. Res. Public Health 2020, 17, 5813. [Google Scholar] [CrossRef]
- Boot, A.W.A.; Carletti, E.; Haselmann, R.; Kotz, H.-H.; Krahnen, J.P.; Pelizzon, L.; Schaefer, S.M.; Subrahmanyam, M.G. The Coronavirus and Financial Stability; SAFE Policy Letter, No. 78; Leibniz Institute for Financial Research SAFE: Frankfurt, Germany, 2020. [Google Scholar]
- Khan, N.; Fahad, S.; Faisal, S.; Naushad, M. Quarantine Role in the Control of Corona Virus in the World and Its Impact on the World Economy. 2020. Available online: https://papers.ssrn.com/sol3/papers.cfm?abstract_id=3556940 (accessed on 5 April 2021).
- Baldwin, R.E.; di Mauro, W. Mitigating the COVID Economic Crisis. Centre for Economic Policy Research. 2020. Available online: https://voxeu.org/content/mitigating-covid-economic-crisis-act-fast-and-do-whatever-it-takes (accessed on 5 April 2021).
- Summers, L.H.; Pritchett, L. Wealthier is healthier. J. Hum. Resour. 1996, 31, 841–868. [Google Scholar]
- Scenarios, S. The global macroeconomic impacts of COVID-19. Cent. Appl. Macroecon. Anal. 2020, 1–45. [Google Scholar]
- Sohrabi, C.; Alsafi, Z.; Neill, N.O.; Khan, M.; Kerwan, A.; Al-jabir, A.; Iosifidis, C.; Agha, R. World Health Organization declares global emergency: A review of the 2019 novel coronavirus (COVID-19). Int. J. Surg. 2020, 76, 71–76. [Google Scholar] [CrossRef]
- Korea, S.; Kong, H. How will country-based mitigation measures influence the course of the COVID-19 epidemic? Lancet 2020, 395, 931–934. [Google Scholar] [CrossRef]
- Fernandes, N. Economic Effects of Coronavirus Outbreak (COVID-19) on the World Economy.2–32. 2020. Available online: https://edisciplinas.usp.br/pluginfile.php/5662406/mod_resource/content/1/FERNANDES_Economic%20Effects%20of%20Coronavirus%20Outbreak%20%28COVID19%29%20on%20the%20World%20Economy.pdf (accessed on 21 May 2021).
- WHO Coronavirus (COVID-19) Dashboard|WHO Coronavirus (COVID-19) Dashboard with Vaccination Data. Available online: https://www.who.int/emergencies/diseases/novel-coronavirus-2019?adgroupsurvey={adgroupsurvey}&gclid=EAIaIQobChMI9cXs_rjV8AIVwV1gCh3YBwEoEAAYASAAEgIyHvD_BwE (accessed on 23 April 2021).
- Li, Q.; Guan, X.; Wu, P.; Wang, X.; Zhou, L.; Tong, Y.; Ren, R.; Leung, K.S.M.; Lau, E.H.Y.; Wong, J.Y.; et al. Early transmission dynamics in Wuhan, China, of novel coronavirus–infected Pneumonia. N. Engl. J. Med. 2020, 382, 1199–1207. [Google Scholar] [CrossRef] [PubMed]
- Medicine, T.; Xu, Y.; Bi, Y.; Wang, W.; Zheng, D.R.; Xu, Y.; Bi, Y.; Wang, W. Spatial transmission of COVID-19 via public and private transportation in China. Travel Med. Infect. Dis. 2020, 34, 101626–101628. [Google Scholar] [CrossRef]
- Loske, D. The impact of COVID-19 on transport volume and freight capacity dynamics: An empirical analysis in German food retail logistics. Transp. Res. Interdiscip. Perspect. 2020, 6, 100165–100170. [Google Scholar] [CrossRef]
- Dube, K.; Nhamo, G.; Chikodzi, D. COVID-19 pandemic and prospects for recovery of the global aviation industry. J. Air Transp. Manag. 2021, 92, 102022–102033. [Google Scholar] [CrossRef]
- Id, K.P.; Kaewpoungngam, K.; Chotirosniramit, K. Commercial airline protocol during COVID-19 pandemic: An experience of Thai Airways International. PLoS ONE 2020, 15, e0237299. [Google Scholar] [CrossRef]
- Hamidi, S.; Zandiatashbar, A. Compact development and adherence to stay-at-home order during the COVID-19 pandemic: A longitudinal investigation in the United States. Landsc. Urban Plan. 2021, 205, 103952–103960. [Google Scholar] [CrossRef]
- Brooke, J.; Jackson, D. Older people and COVID-19: Isolation, risk and ageism. J. Clin. Nurs. 2020, 29, 2044–2046. [Google Scholar] [CrossRef]
- EuroNews Domestic Violence Cases Jump 30% during Lockdown in France. Available online: https://www.euronews.com/2020/03/28/domestic-violence-cases-jump-30-during-lockdown-in-france (accessed on 5 April 2021).
- Graham-Harrison, E.; Giuffrida, A.; Smith, H.; Ford, L. Lockdowns Around the World Bring Rise in Domestic Violence. Available online: https//www.theguardian.com/Soc (accessed on 20 January 2021).
- Rada, A.G. Covid-19: The precarious position of Spain’s nursing homes. BMJ 2020, 369, 1–3. [Google Scholar] [CrossRef]
- Iacobucci, G. Covid-19: Lack of PPE in care homes is risking spread of virus, leaders warn. BMJ 2020, 368. [Google Scholar] [CrossRef]
- Albaqawi, H.M.; Pasay-an, E.; Mostoles, R.; Villareal, S. Risk assessment and management among frontline nurses in the context of the COVID-19 virus in the northern region of the Kingdom of Saudi Arabia. Appl. Nurs. Res. 2021, 58, 151410–151415. [Google Scholar] [CrossRef] [PubMed]
- Yu, X.; Liu, C.; Wang, H.; Feil, J.H. The impact of COVID-19 on food prices in China: Evidence of four major food products from Beijing, Shandong and Hubei Provinces. China Agric. Econ. Rev. 2020, 12, 445–458. [Google Scholar] [CrossRef]
- Ammar, A.; Chtourou, H.; Boukhris, O.; Trabelsi, K.; Masmoudi, L.; Brach, M.; Aloui, A.; Hammouda, O.; Paineiras-domingos, L.L.; Braakman-jansen, A. Social participation and life satisfaction of peoples during the COVID-19 home confinement: The ECLB-COVID19 multicenter study. medRxiv 2020. [Google Scholar] [CrossRef]
- Di Renzo, L.; Gualtieri, P.; Pivari, F.; Soldati, L.; Attinà, A.; Cinelli, G.; Cinelli, G.; Leggeri, C.; Caparello, G.; Barrea, L.; et al. Eating habits and lifestyle changes during COVID-19 lockdown: An Italian survey. J. Transl. Med. 2020, 18, 229–233. [Google Scholar] [CrossRef]
- De Faria Coelho-Ravagnani, C.; Corgosinho, F.C.; Sanches, F.L.F.Z.; Prado, C.M.M.; Laviano, A.; Mota, J.F. Dietary recommendations during the COVID-19 pandemic. Nutr. Rev. 2021, 79, 382–393. [Google Scholar] [CrossRef]
- Narici, M.; De Vito, G.; Franchi, M.; Paoli, A.; Moro, T.; Marcolin, G.; Grassi, B.; Baldassarre, G.; Zuccarelli, L.; Biolo, G.; et al. Impact of sedentarism due to the COVID-19 home confinement on neuromuscular, cardiovascular and metabolic health: Physiological and pathophysiological implications and recommendations for physical and nutritional countermeasures. Eur. J. Sport Sci. 2020. [Google Scholar] [CrossRef]
- Khoramipour, K.; Basereh, A.; Hekmatikar, A.A.; Castell, L.; Ruhee, R.T.; Suzuki, K. Physical activity and nutrition guidelines to help with the fight against COVID-19. J. Sports Sci. 2021, 39, 101–107. [Google Scholar] [CrossRef]
- Kumari, A.; Ranjan, P.; Sharma, K.A.; Sahu, A.; Bharti, J.; Zangmo, R.; Bhatla, N. Impact of COVID-19 on psychosocial functioning of peripartum women: A qualitative study comprising focus group discussions and in-depth interviews. Int. J. Gynecol. Obstet. 2021, 152, 321–327. [Google Scholar] [CrossRef]
- Williams, L.; Rollins, L.; Young, D.; Fleming, L.; Grealy, M.; Janssen, X.; Kirk, A.; MacDonald, B.; Flowers, P. What have we learned about positive changes experienced during COVID-19 lockdown? Evidence of the social patterning of change. PLoS ONE 2021, 16, e0244873. [Google Scholar] [CrossRef]
- Barbu-Banes, A.-O. Microtargeting in social media: Definitions and ethical issues. Univ. Babes Bolyai Ephemer. 2013, 58, 83–90. [Google Scholar]
- Maryam, M. 10 TikTok Statistics That You Need to Know in 2020. Available online: https://my.oberlo.com/blog/tiktok-statistics (accessed on 15 April 2021).
- Jacobson, J.; Gruzd, A.; Hernández-garcía, Á.; Rogers, T.; Management, R.; Street, V.; Mb, C. Social media marketing: Who is watching the watchers ? J. Retail. Consum. Serv. 2020, 53, 101774–101785. [Google Scholar] [CrossRef]
- Oliveira, T.; Araujo, B.; Tam, C. Why do people share their travel experiences on social media? Tour. Manag. 2020, 78, 104041–104054. [Google Scholar] [CrossRef]
- Chan, A.K.M.; Nickson, C.P.; Rudolph, J.W.; Lee, A.; Joynt, G.M. Social media for rapid knowledge dissemination: Early experience from the COVID-19 pandemic. Anaesthesia 2020, 75, 1579–1582. [Google Scholar] [CrossRef] [PubMed]
- Greenwood, S.; Perrin, A.; Duggan, M. Social media update 2016. Pew Res. Center 2016, 11, 1–18. [Google Scholar]
- Clement, J. Number of Global Social Media Users 2017–2025. Stat. Website 2020. Available online: https://www.statista.com/statistics/278414/number-of-worldwide-social-network-users/ (accessed on 23 January 2021).
- Jin, K.-X. Keeping People Safe and Informed about the Coronavirus. Facebook Newsroom Website. 2020. Available online: https://about.fb.com/news/2020/12/coronavirus/ (accessed on 22 May 2021).
- Josephson, A.; Lambe, E. Brand Communications in Time of Crisis. 2020. Available online: https://blog.twitter.com/en_us/topics/company/2020/Brand-communications-in-time-of-crisis.html (accessed on 15 December 2020).
- Google Scholar. Available online: https://scholar.google.com.eg/scholar?as_ylo=2017&q=hesham+el+seedi&hl=en&as_sdt=0,5 (accessed on 10 April 2021).
- Allington, D.; Duffy, B.; Wessely, S.; Dhavan, N.; Rubin, J. Health-protective behaviour, social media usage and conspiracy belief during the COVID-19 public health emergency. Psychol. Med. 2020, 1–7. [Google Scholar] [CrossRef] [PubMed]
- Bedford, J.; Enria, D.; Giesecke, J.; Heymann, D.L.; Ihekweazu, C.; Kobinger, G.; Lane, H.C.; Memish, Z.; Oh, M.-d.; Schuchat, A. COVID-19: Towards controlling of a pandemic. Lancet 2020, 395, 1015–1018. [Google Scholar] [CrossRef]
- Liu, W.; Zhang, Q.; Chen, J.; Xiang, R.; Song, H.; Shu, S.; Chen, L.; Liang, L.; Zhou, J.; You, L. Detection of COOVID-19 in children in early January 2020 in Wuhan, China. N. Engl. J. Med. 2020, 382, 1370–1371. [Google Scholar] [CrossRef]
- Moghadas, S.M. Simulating the effect of school closure during COVID-19 outbreaks in Ontario, Canada. BMC Med. 2020, 18, 230–237. [Google Scholar]
- Bosveld, M.H.; van Doorn, D.P.C.; Stassen, P.M.; Westerman, D.; Bergmans, D.C.J.J.; van der Horst, I.C.C.; van Mook, W.N.K.A. Lessons learned: Contribution to healthcare by medical students during COVID-19. J. Crit. Care 2020, 10–13. [Google Scholar] [CrossRef]
- Ali, R.A.; Rafie, M.; Arshad, M. Challenges and benefits in implementing M-learning in pre-university education in Egypt. Int. J. Comput. Acad. Res. 2015, 4, 144–151. [Google Scholar]
- Edmodo. Egyptan Edmodo Online Platform. Available online: https://new.edmodo.com/login?go2url=%2Fhome (accessed on 20 May 2021).
- Bank, E.K. Egyptian Knowledge Bank. Available online: http://www.ekb.eg/ (accessed on 19 October 2020).
- Egyptian Ministry of Education. Available online: https://moe.gov.eg/ (accessed on 19 October 2020).
- Saberi, P. Research in the time of coronavirus: Continuing ongoing studies in the midst of the covid-19 pandem. AIDS Behav. 2020, 24, 2232–2235. [Google Scholar] [CrossRef]
- Sohrabi, C.; Mathew, G.; Franchi, T.; Kerwan, A.; Griffin, M.; Soleil C Del Mundo, J.; Ali, S.A.; Agha, M.; Agha, R. Impact of the coronavirus (COVID-19) pandemic on scientific research and implications for clinical academic training–A review. Int. J. Surg. 2021, 86, 57–63. [Google Scholar] [CrossRef]
- Mbunge, E.; Akinnuwesi, B.; Fashoto, S.G.; Metfula, A.S.; Mashwama, P. A critical review of emerging technologies for tackling COVID-19 pandemic. Hum. Behav. Emerg. Technol. 2020, 2, 25–39. [Google Scholar] [CrossRef]
- Chen, J.; Liu, X.; Wang, D.; Jin, Y.; He, M.; Ma, Y.; Zhao, X.; Song, S.; Zhang, L.; Xiang, X.; et al. Risk factors for depression and anxiety in healthcare workers deployed during the COVID-19 outbreak in China. Soc. Psychiatry Psychiatr. Epidemiol. 2021, 56, 47–55. [Google Scholar] [CrossRef]
- Mina, F.B.; Billah, M.; Karmakar, S.; Das, S.; Rahman, M.S.; Hasan, M.F.; Acharjee, U.K. An online observational study assessing clinical characteristics and impacts of the COVID-19 pandemic on mental health: A perspective study from Bangladesh. J. Public Health 2021. [Google Scholar] [CrossRef]
- Sahebi, A.; Nejati-Zarnaqi, B.; Moayedi, S.; Yousefi, K.; Torres, M.; Golitaleb, M. The prevalence of anxiety and depression among healthcare workers during the COVID-19 pandemic: An umbrella review of meta-analyses. Prog. Neuro Psychopharmacol. Biol. Psychiatry 2021, 107, 110247–110253. [Google Scholar] [CrossRef]
- Liu, C.; Zhou, Q.; Li, Y.; Garner, L.V.; Watkins, S.P.; Carter, L.J.; Smoot, J.; Gregg, A.C.; Daniels, A.D.; Jervey, S.; et al. Research and development on therapeutic agents and vaccines for COVID-19 and related human coronavirus diseases. ACS Cent. Sci. 2020, 6, 315–331. [Google Scholar] [CrossRef]
- Yanow, S.K.; Good, M.F. Nonessential research in the new normal: The impact of COVID-19. Am. J. Trop. Med. Hyg. 2020, 102, 1164–1165. [Google Scholar] [CrossRef]
- Udugama, B.; Kadhiresan, P.; Kozlowski, H.N.; Malekjahani, A.; Osborne, M.; Li, V.Y.C.; Chen, H.; Mubareka, S.; Gubbay, J.B.; Chan, W.C.W. Diagnosing COVID-19: The disease and tools for detection. ACS Nano 2020, 14, 3822–3835. [Google Scholar] [CrossRef] [PubMed]
- Yu, H.; Li, C.; Wang, X.; Duan, J.; Yang, N.; Xie, L.; Yuan, Y.; Li, S.; Bi, C.; Yang, B.; et al. Techniques and strategies for potential protein target discovery and active pharmaceutical molecule screening in a pandemic. J. Proteome Res. 2020, 19, 4242–4258. [Google Scholar] [CrossRef] [PubMed]
- Gabster, B.P.; van Daalen, K.; Dhatt, R.; Barry, M. Challenges for the female academic during the COVID-19 pandemic. Lancet 2020, 395, 1968–1970. [Google Scholar] [CrossRef]
- Filardo, G.; Graca, B.D.; Sass, D.M.; Pollock, B.D.; Smith, E.B.; Martinez, M.A.M. Trends and comparison of female first authorship in high impact medical journals: Observational study (1994-2014). BMJ 2016, 352, i847. [Google Scholar] [CrossRef] [PubMed]
- Laborde, B.D.; Martin, W.; Swinnen, J.; Vos, R. COVID-19 risks to global food security. Science 2020, 369, 500–502. [Google Scholar] [CrossRef]
- Erokhin, V.; Gao, T. Impacts of COVID-19 on trade and economic aspects of food security: Evidence from 45 developing countries. Int. J. Environ. Res. Public Health 2020, 17, 5775. [Google Scholar] [CrossRef]
- Singh, D.R.; Sunuwar, D.R.; Adhikari, B.; Szabo, S.; Padmadas, S.S. The perils of COVID-19 in Nepal: Implications for population health and nutritional status. J. Glob. Health 2020, 10, 010378–010381. [Google Scholar] [CrossRef]
- UNICEF. The State of Foodsecurity and Nutrition in the World 2020. In Transforming Food Systems for Affordable Healthy Diets; FAO: Rome, Italy, 2020. [Google Scholar]
- Cullen, M. COVID-19 and the Risk to Food Supply Chains: How to Respond? FAO Recuper. 2020. Available online: http//www.fao.org/3/ca8388en/CA8388EN.pdf (accessed on 19 October 2020).
- Ipek, Y.; Aytekin, N.; Buyukkayhan, D.; Aslan, I. Food policy, nutrition and nutraceuticals in the prevention and management of COVID-19: Advice for healthcare professionals. Trends Food Sci. Technol. 2020, 105, 186–199. [Google Scholar] [CrossRef]
- Pulighe, G.; Lupia, F. Food first: COVID-19 outbreak and cities lockdown a booster for a wider vision on urban agriculture. Sustainability 2020, 12, 5012. [Google Scholar] [CrossRef]
- Aldaco, R.; Hoehn, D.; Laso, J.; Margallo, M.; Ruiz-salmón, J.; Cristobal, J.; Kahhat, R.; Villanueva-rey, P.; Bala, A.; Batlle-bayer, L.; et al. Food waste management during the COVID-19 outbreak: A holistic climate, economic and nutritional approach. Sci. Total Environ. 2020, 742, 140524–140536. [Google Scholar] [CrossRef]
- Strasser, B.; Gostner, J.M.; Fuchs, D. Mood, food, and cognition: Role of tryptophan and serotonin. Curr. Opin. Clin. Nutr. Metab. Care 2016, 19, 55–61. [Google Scholar] [CrossRef]
- Rodríguez-Pérez, C.; Molina-Montes, E.; Verardo, V.; Artacho, R.; García-Villanova, B.; Guerra-Hernández, E.J.; Ruíz-López, M.D. Changes in dietary behaviours during the COVID-19 outbreak confinement in the Spanish COVIDiet study. Nutrients 2020, 12, 1730. [Google Scholar] [CrossRef]
- Bendall, C.L.; Mayr, H.L.; Opie, R.S.; Itsiopoulos, C.; Mayr, H.L.; Opie, R.S.; Itsiopoulos, C. Central obesity and the Mediterranean diet: A systematic review of intervention trials. Crit. Rev. Food Sci. Nutr. ISSN 2018, 58, 3070–3084. [Google Scholar] [CrossRef]
- Cheikh Ismail, L.; Osaili, T.M.; Mohamad, M.N.; Al Marzouqi, A.; Jarrar, A.H.; Abu Jamous, D.O.; Magriplis, E.; Ali, H.I.; Al Sabbah, H.; Hasan, H.; et al. Eating habits and lifestyle during COVID-19 lockdown in the United Arab Emirates: A cross-sectional study. Nutrients 2020, 12, 3314. [Google Scholar] [CrossRef]
- Cicero, A.F.G.; Fogacci, F.; Giovannini, M.; Mezzadri, M.; Grandi, E.; Borghi, C.; Brisighella Heart Study Group. COVID-19-related quarantine effect on dietary habits in a northern italian rural population: Data from the brisighella heart study. Nutrients 2021, 13, 309. [Google Scholar] [CrossRef]
- Marty, L.; de Lauzon-Guillain, B.; Labesse, M.; Nicklaus, S. Food choice motives and the nutritional quality of diet during the COVID-19 lockdown in France. Appetite 2021, 157, 105005. [Google Scholar] [CrossRef] [PubMed]
- Jia, P.; Zhang, L.; Yu, W.; Yu, B.; Liu, M.; Zhang, D.; Yang, S. Impact of COVID-19 lockdown on activity patterns and weight status among youths in China: The COVID-19 impact on lifestyle change survey (COINLICS). Int. J. Obes. 2021, 45, 695–699. [Google Scholar] [CrossRef]
- Górnicka, M.; Drywień, M.E.; Zielinska, M.A.; Hamułka, J. Dietary and lifestyle changes during COVID-19 and the subsequent lockdowns among polish adults: A cross-sectional online survey plife COVID-19 study. Nutrients 2020, 12, 2324. [Google Scholar] [CrossRef] [PubMed]
- AlMughamis, N.; AlAsfour, S.; Mehmood, S. Poor eating habits and predictors of weight gain during the COVID-19 quarantine measures in Kuwait: A cross sectional study [version 1; peer review: 2 approved with reservations]. FlooResearch 2020, 9, 914–924. [Google Scholar] [CrossRef]
- Bhutani, S.; Cooper, J.A. COVID-19–related home confinement in adults: Weight gain risks and opportunities. Obesity 2020, 28, 1576–1577. [Google Scholar] [CrossRef]
- Muscogiuri, G.; Barrea, L. Nutritional recommendations for COVID-19 quarantine. Eur. J. Clin. Nutr. 2020, 74, 850–851. [Google Scholar] [CrossRef]
- Martín Giménez, V.M.; Inserra, F.; Ferder, L.; García, J.; Manucha, W. Vitamin D deficiency in African Americans is associated with a high risk of severe disease and mortality by SARS-CoV-2. J. Hum. Hypertens. 2020, 1–3. [Google Scholar] [CrossRef]
- Grant, W.B.; Lahore, H.; McDonnell, S.L.; Baggerly, C.A.; French, C.B.; Aliano, J.L.; Bhattoa, H.P. Evidence that vitamin D supplementation could reduce risk of influenza and COVID-19 infections and deaths. Nutrients 2020, 12, 988. [Google Scholar] [CrossRef]
- Butler, J.R.A.; Davila, F.; Alders, R.; Bourke, R.M.; Crimp, S.; McCarthy, J.; McWilliam, A.; Palo, A.S.M.; Robins, L.; Webb, M.J.; et al. A rapid assessment framework for food system shocks: Lessons learned from COVID-19 in the Indo-Pacific region. Environ. Sci. Policy 2021, 117, 34–45. [Google Scholar] [CrossRef]
- Cao, W.; Fang, Z.; Hou, G.; Han, M.; Xu, X.; Dong, J. The psychological impact of the COVID-19 epidemic on college students in China. Psychiatry Res. 2020, 287, 112934–112938. [Google Scholar] [CrossRef] [PubMed]
- Lee, J. Mental health effects of school closures during COVID-19. Lancet Child Adolesc. Health 2020, 4, 421. [Google Scholar] [CrossRef]
- Rundle, A.G. COVID-19–related school closings and risk of weight gain among children. Obesity 2020, 28, 1008–1009. [Google Scholar] [CrossRef] [PubMed]
- Kaur, S.P.; Gupta, V. COVID-19 Vaccine: A comprehensive status report. Virus Res. 2020, 288, 198114–198126. [Google Scholar] [CrossRef] [PubMed]
- Chan, W.C.W. Nano research for COVID-19. ACS Nano 2020, 14, 3719–3720. [Google Scholar] [CrossRef] [PubMed]
- Palestino, G.; García-silva, I.; González-ortega, O.; Palestino, G.; García-silva, I.; González-ortega, O.; Rosales-mendoza, S. Can nanotechnology help in the fight against. Expert Rev. Anti. Infect. Ther. 2020, 18, 849–864. [Google Scholar] [CrossRef]
- Talebian, S.; Wallace, G.G.; Schroeder, A.; Stellacci, F.; Conde, J. Nanotechnology-based disinfectants and sensors for SARS-CoV-2. Nat. Nanotechnol. 2020, 15, 618–621. [Google Scholar] [CrossRef]
- Kramps, T.; Probst, J. Messenger RNA-based vaccines: Progress, challenges, applications. Wiley Interdiscip. Rev. RNA 2013, 4, 737–749. [Google Scholar] [CrossRef]
- Mishra, S.K.; Tripathi, T. One year update on the COVID-19 pandemic: Where are we now? Acta Trop. 2020, 105778–105790. [Google Scholar] [CrossRef]
- Paltiel, A.D.; Schwartz, J.L.; Zheng, A.; Walensky, R.P. Clinical outcomes of a COVID-19 vaccine: Implementation over efficacy. Health Aff. 2021, 40, 1377. [Google Scholar] [CrossRef] [PubMed]
- Helm, D. The environmental impacts of the Coronavirus. Environ. Resour. Econ. 2020, 76, 21–38. [Google Scholar] [CrossRef] [PubMed]
- Bauwens, M.; Compernolle, S.; Stavrakou, T.; Müller, J.; Van Gent, J.; Eskes, H. Impact of coronavirus outbreak on NO2 pollution assessed using TROPOMI and OMI observations. Geophys. Res. Lett. 2020, 47, e2020GL087978. [Google Scholar] [CrossRef] [PubMed]
- Singu, S.; Acharya, A.; Challagundla, K.; Byrareddy, S.N. Impact of social determinants of health on the emerging COVID-19 pandemic in the United States. Front. Public Health 2020, 8, 406–415. [Google Scholar] [CrossRef] [PubMed]
- Hoffart, A.; Johnson, S.U.; Ebrahimi, O.V. Loneliness and social distancing during the COVID-19 pandemic: Risk factors and associations with psychopathology. Front. Psychiatry 2020, 11, 589127–589135. [Google Scholar] [CrossRef] [PubMed]
- Usher, K.; Marriott, R.; Smallwood, R.; Walker, R.; Shepherd, C.; Hopkins, K.; Skeffington, P.; Reid, C.; Jackson, D. COVID-19 and social restrictions: The potential mental health impact of social distancing and isolation for young Indigenous Australians. Australas. Psychiatry 2020, 28, 599–600. [Google Scholar] [CrossRef]
- Čavoški, A. An ambitious and climate-focused Commission agenda for post COVID-19 EU. Environ. Polit. 2020, 29, 1112–1117. [Google Scholar] [CrossRef]
- Rowan, N.J.; Galanakis, C.M. Unlocking challenges and opportunities presented by COVID-19 pandemic for cross-cutting disruption in agri-food and green deal innovations: Quo Vadis? Sci. Total Environ. 2020, 748, 141362. [Google Scholar] [CrossRef]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Khalifa, S.A.M.; Swilam, M.M.; El-Wahed, A.A.A.; Du, M.; El-Seedi, H.H.R.; Kai, G.; Masry, S.H.D.; Abdel-Daim, M.M.; Zou, X.; Halabi, M.F.; et al. Beyond the Pandemic: COVID-19 Pandemic Changed the Face of Life. Int. J. Environ. Res. Public Health 2021, 18, 5645. https://doi.org/10.3390/ijerph18115645
Khalifa SAM, Swilam MM, El-Wahed AAA, Du M, El-Seedi HHR, Kai G, Masry SHD, Abdel-Daim MM, Zou X, Halabi MF, et al. Beyond the Pandemic: COVID-19 Pandemic Changed the Face of Life. International Journal of Environmental Research and Public Health. 2021; 18(11):5645. https://doi.org/10.3390/ijerph18115645
Chicago/Turabian StyleKhalifa, Shaden A. M., Mahmoud M. Swilam, Aida A. Abd El-Wahed, Ming Du, Haged H. R. El-Seedi, Guoyin Kai, Saad H. D. Masry, Mohamed M. Abdel-Daim, Xiaobo Zou, Mohammed F. Halabi, and et al. 2021. "Beyond the Pandemic: COVID-19 Pandemic Changed the Face of Life" International Journal of Environmental Research and Public Health 18, no. 11: 5645. https://doi.org/10.3390/ijerph18115645
APA StyleKhalifa, S. A. M., Swilam, M. M., El-Wahed, A. A. A., Du, M., El-Seedi, H. H. R., Kai, G., Masry, S. H. D., Abdel-Daim, M. M., Zou, X., Halabi, M. F., Alsharif, S. M., & El-Seedi, H. R. (2021). Beyond the Pandemic: COVID-19 Pandemic Changed the Face of Life. International Journal of Environmental Research and Public Health, 18(11), 5645. https://doi.org/10.3390/ijerph18115645












