Abstract
This study investigated the relationship between perceived indoor temperature in winter and frailty among community-dwelling older people. This cross-sectional study included 342 people 65 years and older in Japan. Participants answered questions about demographics, frailty, housing, and perceived indoor temperature in winter. Participants were grouped based on perceived indoor temperature (Cold or Warm) and economic satisfaction (Unsatisfied or Satisfied). Differences in the frailty index between perceived indoor temperature groups and economic satisfaction groups were tested by using ANCOVA and MANCOVA. An interaction effect showed that people in the Cold Group and unsatisfied with their economic status had significantly higher frailty index scores (F(1, 336) = 5.95, p = 0.015). Furthermore, the frailty index subscale of fall risk was the specific indicator of frailty that accounted for this significant relationship. While previous research has shown the risks related to cold indoor temperature in homes, interestingly among those who reported cold homes, only those who were not satisfied with their economic situation reported being at increased risk for frailty. This highlights the potential importance of preventing fuel poverty to prevent frailty.
1. Introduction
Recently, the impact of cold weather on functioning and health has attracted attention. Cold weather is associated with lower physical activity [1], increased blood pressure and excess cardiovascular mortality, asthma and respiratory symptoms [2]. Falling temperature and colder weather are also associated with increased risk of aneurysmal subarachnoid hemorrhage [3], and to various negative functional outcomes [4]. From an experimental study using a movement laboratory in a climate chamber, Lindemann et al. [5] reported that the physical performance of older women exposed to cold temperature (15 °C) was significantly lower than women exposed to warm/normal temperature (25 °C). Additionally, seasonal trends in the physical performance of older people were associated with a lower level of performance in the winter compared with the autumn, and people living in colder houses had a lower level of physical performance than those living in warm houses [6]. With advancing age, the efficiency of adaptive mechanisms to regulate temperature declines, and thus the comfort zone for older people is stated at higher ambient temperatures than in their younger counterparts [7]. Perception of cold among older people has been found to be associated with poor sleep quality [8] and poor self-reported health [9].
With increasing age and health decline, people spend more time doing activities in their homes [10,11], and thus it is crucial to understand what role the indoor temperature in the home plays for their health. In the Cold Weather Plan for England [12], older people, in particular those who are frail or socially isolated and over 75 years of age, are considered to be particularly at-risk in the event of severe cold weather. Overall, the problem of cold weather for older people is framed as an integral problem of lower physical functioning and performance of activities of daily living (ADL), energy inefficient homes and heating systems, financial poverty, and old- fashioned attitudes such as partial intermittent heating [13].
Frailty is widely recognized as a considerable challenge for the society, but there is no single agreed definition or cause of the phenomenon. The definition suggested by Fried et al. [14] includes self-reported exhaustion, reduced grip strength, slow walking speed, and low level of physical activity. In addition to physical functioning, it has been suggested that definitions of frailty should also include aspects of mental health, such as cognition and mood [15]. Shinkai et al. [16,17] include three domains in their definition of frailty: isolation risk, fall risk, and nutrition risk. With increasing age, frailty becomes more frequent and severe [18,19,20,21,22]. Frailty is associated with chronic disease [23], obesity [24], and female gender [20,25,26], as well as low education level and income [14]. When it comes to the impact of the environment, it is well known that being confined to the home is a risk factor for walking limitation and declining ADL [27,28], thus increasing the risks of falling [29,30] and subsequent mortality [31]. That is, different conditions in the environment may well contribute to worsen the consequences of frailty. Frailty most often leads to limitations in ADL, ultimately requiring nursing home placement [32] and increased use of health care resources [33]. For informal caregivers, care-recipient’s frailty can be a significant predictor of caregiver burden [34,35], which may lead to emotional distress [36], poor health, decreased quality of life [37] and increased health care consumption [38].
There are very few studies on the relationship between indoor temperature and frailty, and we are not aware of any studies focusing on the relationship between perceived indoor temperature and frailty. Hence, the overarching aim of this study was to investigate the relationship between perceived indoor temperature and frailty among older people living in the community. The specific aims are to: (1) investigate the relationships between self-reported risk for frailty and perceived indoor temperature, and (2) to determine whether economic satisfaction influences the relationship between self-reported risk for frailty and perceived indoor temperature.
2. Materials and Methods
2.1. Procedure and Participants
Data collection for this cross-sectional study was conducted during December of 2014, 2015, and 2017. Staff at outpatient rehabilitation facilities in Kochi, Osaka, and Yamanashi prefectures, Japan provided surveys to their clients. The surveys were either completed at the rehabilitation facility or at the participant’s home, and 473 were returned. To be included in this study, participants had to be 65 years or older and use the facilities one to two times per week for physical rehabilitation. The study protocol was approved by the Keio University Ethics Review Board on 4 August 2014 (26-11), 29 July 2015 (27-31), and 29 August 2017 (29-79). All participants received oral and written information, and the questionnaires were filled out anonymously. Of the 473 surveys returned, 131 were excluded: 10 participants were younger than 65 years and 54 participants did not disclose their age. Additionally, 67 participants did not complete questions from the frailty index and/or perceived indoor temperature. Hence, 342 people were included in the present study. Participants included in this study did not differ from those who were excluded on any characteristic except for the score on poor nutrition risk which is one of the subscales of frailty index. Mean scores of poor nutrition risk were 0.97 (SD = 0.96) for the included participants and 0.73 (SD = 0.86) for the excluded participants (p = 0.030).
2.2. Measurements
2.2.1. Participant Characteristics
Participants’ characteristics included self- reported age, gender, body mass index (BMI), level of education (junior high school or less/senior high school/university or higher), and whether the person lived alone (yes/no).
2.2.2. Frailty Index
To measure frailty, we used the “Kaigo-Yobo Check-List” proposed by Shinkai et al. [16,17], which can be easily self-administered by responding to 15 items (Table 1). All of the items are answered on a two-point scale, positive answer (0) or negative answer (1). The items are summed to calculate a total score ranging from 0 to 15 with higher scores indicating a higher risk of frailty. This checklist has three sub-scales that measure the risk of becoming frail: isolation risk, fall risk, and nutrition risk. Sum scores can also be calculated for each subscale: Isolation Risk (0–5), Fall Risk (0–6), and Nutrition Risk (0–4).

Table 1.
The frailty index translated from Kaigo-Yobo Check-List [16,17].
2.2.3. Perceived Indoor Temperature
Perceived indoor temperature was examined using the standardized questionnaire, Comprehensive Assessment System for Built Environment Efficiency (CASBEE) Health Checklist [39]. The checklist was created to help residents determine whether or not environmental factors and housing equipment have any potential risks for their health. It consists of questions about the levels of heat in summer, cold in winter, noise, light, cleanliness, safety, and security of the living environment for each room in the house. Respondents are asked to mark the frequency of corresponding problems on a four-pointed scale: 1) often (0 point), 2) occasionally (1 point), 3) rarely (2 point), 4) not at all (3 point). The scores for each item are summed and higher scores indicate fewer problems in the living environment. In this study, six questions about feeling cold in the living room, bedroom, dressing room, bathroom, toilet, and corridor were used to evaluate the perceived indoor temperature in winter. The scores on perceived indoor temperature from the CASBEE Health Checklist were not normally distributed. Therefore, participants with higher scores (10–18 points) were classified into the Warm Group, and participants with lower scores (0–9 points) were classified into the Cold Group.
2.2.4. Economic Satisfaction
Economic satisfaction was measured with a study specific question, with four response choices: “Very satisfied”, “Somehow satisfied”, “Not very satisfied” and “Not satisfied at all”. Economic satisfaction was dichotomized for the analyses: “Very satisfied” and “Somehow satisfied” were considered as “Satisfied”, and “Not very satisfied” and “Not satisfied at all” were considered as “Unsatisfied”.
2.3. Data Analysis
Analysis of covariance (ANCOVA) was used to test for differences between the perceived indoor temperature groups and the economic satisfaction groups with the frailty index as the dependent variable. Perceived indoor temperature, economic satisfaction, and the interaction between these two factors were in the model as independent variables. Since we know from previous research that they are associated with frailty, gender, living alone or not, education, age and BMI were in the model as covariates. Spearman’s correlations between each covariate and the independent variables were not larger than 0.2. Multivariate analysis of covariance (MANCOVA) was used to test the three subscales of the frailty index (isolation risk, fall risk, and nutrition risk) using the same independent variables and covariates as the previous model. Wilks’ Lambda was used as the omnibus test of the MANCOVA. Both models used the general linear model for the analyses. p-value < 0.05 was considered statistically significant. All statistical analyses were performed with SPSS version 24.0 (IBM, Armonk, NY, USA).
3. Results
Among the 342 participants included in the analysis, the mean age was 81.74 (SD = 7.27) years, and 215 (62.9%) were women (see Table 2 for more details).

Table 2.
Participant characteristics by perceived indoor temperature and for total sample (n = 342).
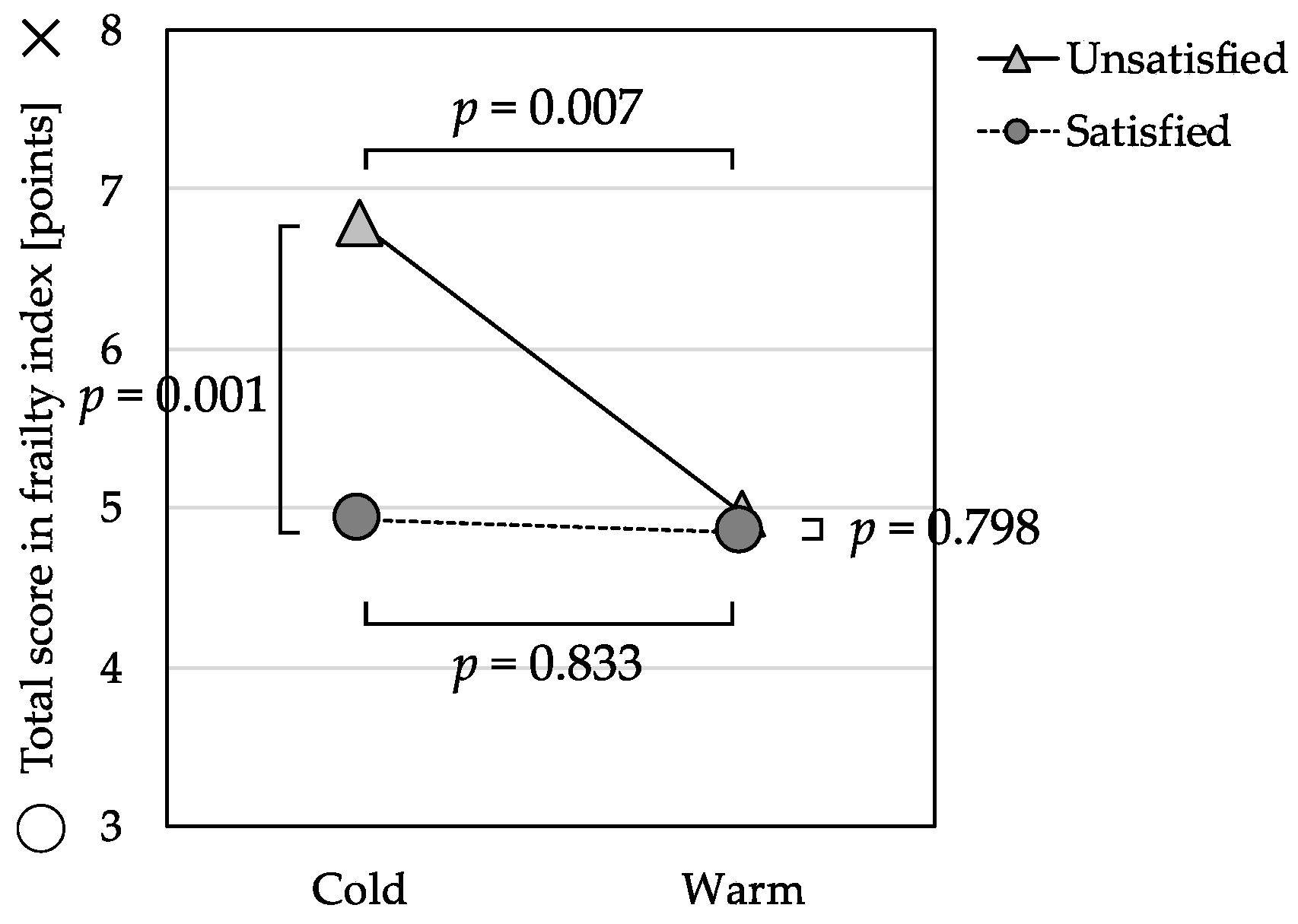
In the ANCOVA for total score of frailty index with the perceived temperature and economic satisfaction groups (Table 3), there was a significant interaction effect, F(1, 328) = 5.28, p = 0.022. The levels of reported frailty risk were not significantly different, F(1, 328) = 0.04, p = 0.833, between the Warm Group and Cold Group among those participants who were satisfied with their economic status. In contrast, the levels of frailty risk were significantly higher, F(1, 328) = 7.33, p = 0.007, among those in the Cold Group who were also unsatisfied with their economic status (Figure 1).

Table 3.
ANCOVA of total frailty score by perceived indoor temperature and participant characteristics (n = 342).
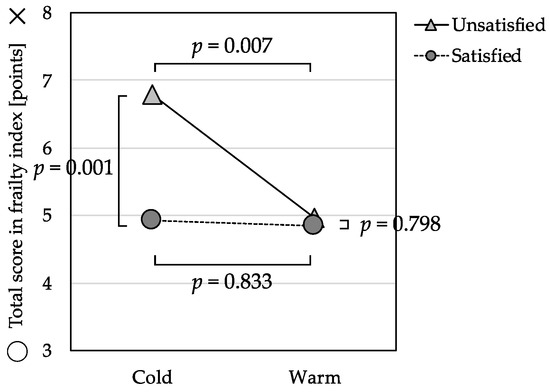
Figure 1.
Interaction effect between perceived indoor temperature and economic satisfaction on the total frailty score (n = 342).
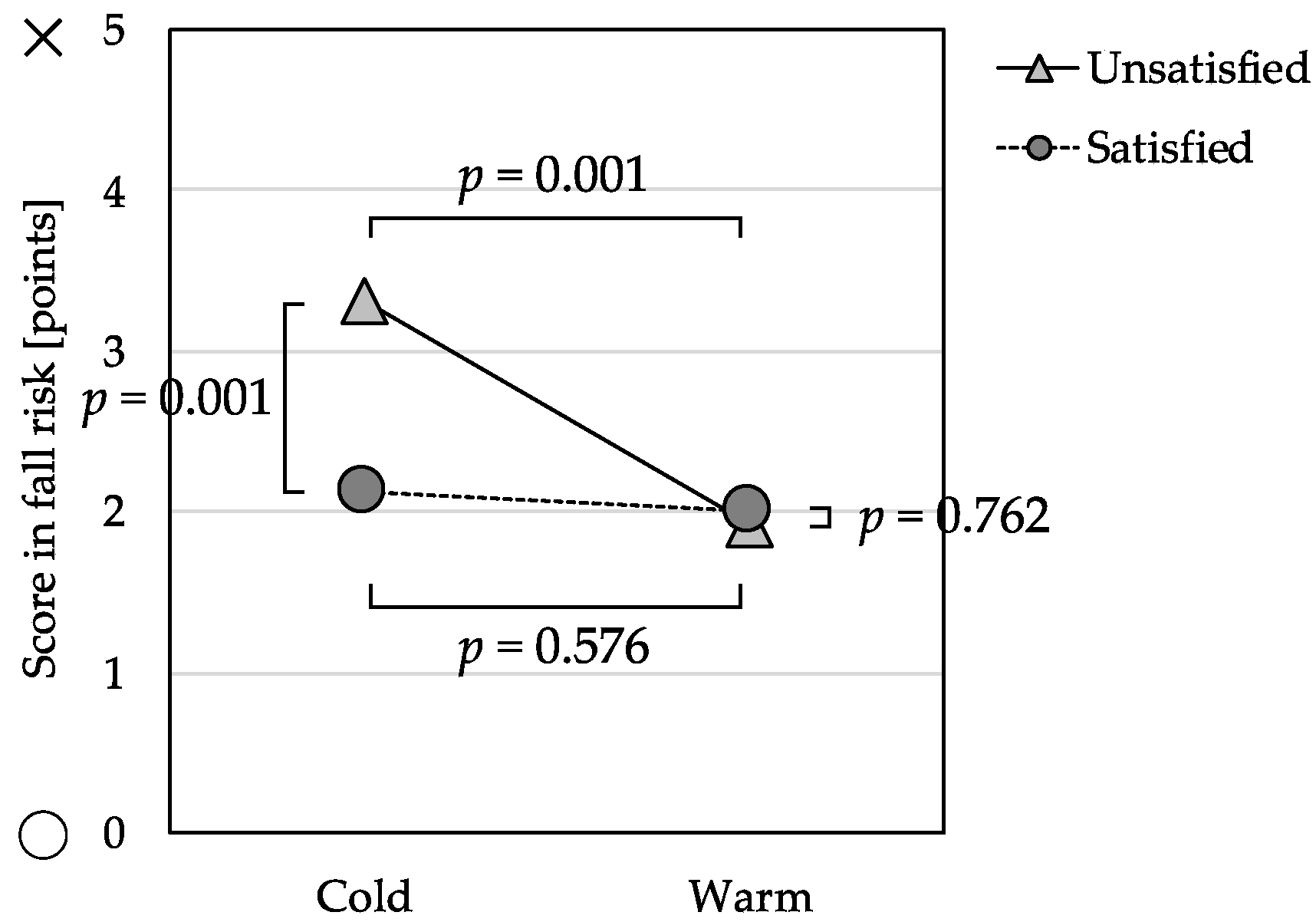
The omnibus test of the MANCOVA was significant with Wilks’ Lambda = 0.98, F(3, 326) = 2.78, p = 0.041. The main effects and interaction effects for isolation risk and nutrition risk were not significant, but there were significant differences in the fall risk subscale (Table 4). The Warm Group and Cold Group were not significantly different, F(1, 328) = 0.31, p = 0.576, on the fall risk subscale among those participants who were satisfied with their economic status. In contrast, the Cold Group scored significantly higher on the fall risk subscale, F(1, 328) = 12.15, p = 0.001, among those who were also unsatisfied with their economic status (Figure 2).

Table 4.
Multivariate analysis of covariance of three subscales of the frailty index by perceived indoor temperature and participant characteristics (n = 342).
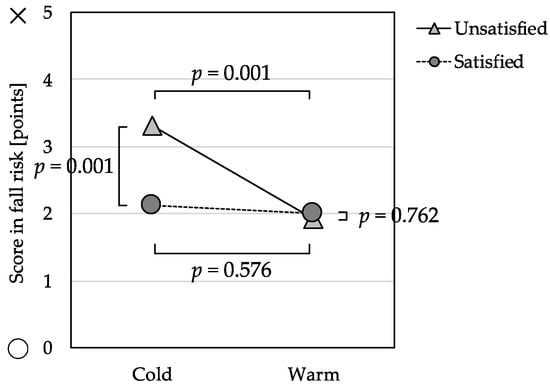
Figure 2.
Interaction effect between perceived indoor temperature and economic satisfaction and its relation to fall risk score (n = 342).
4. Discussion
In the present study, we found that those who were unsatisfied with their economic situation and also perceived the indoor temperature in their home as cold reported a higher risk of frailty than other groups. In contrast, people who were satisfied with their economic status reported similar frailty risks regardless of perceived indoor temperature. We also found that the reported fall risk had the strongest relationship with perceived temperature and economic satisfaction compared with nutrition and isolation risks.
The most interesting finding was the interaction between economic satisfaction and reported frailty risk. We found that the people who both perceived a cold indoor winter temperature and were unsatisfied with their economic situation reported the highest risk of frailty. This same pattern was also seen for the specific indicator of fall risks but not for nutrition risk or isolation risk. Hence, the total frailty risk in our sample seems to be accounted for by the fall risk. Previous research found that poverty risk was associated with increased levels of frailty, and rather than educational or behavioral factors, material and in particular, psychosocial factors such as perceived control and social isolation explained a large part of poverty-risk-related differences in frailty [40]. To be more specific, it has been reported that low income is associated with under-nutrition [41] and loneliness or depression in the elderly [42], but those relationships did not seem to hold in our study in relation to frailty risk. When it came to people who were satisfied with their economic situation, there was no difference in reported frailty risk regardless of perceived indoor temperature. As previously reported, higher income seems to reduce the risk for frailty as those with higher incomes are more likely to survive into old age through better health status [43].
Hence, we found that it was not just lower economic status that was related to frailty risk, but it was the specific group that also reported living in a colder house that had the strongest relationship with frailty risk. This finding argues for encouraging heating up the homes of older people as a means to reduce risk of frailty and potentially promote healthy ageing. Specifically, different approaches to frailty prevention may be necessary for different subgroups. One possibility was that people unsatisfied with their economic situation were the people having difficulty warming up their house [44] and at risk of fuel poverty. In fact, older people are at great risk from fuel poverty, since they are more likely to be retired or on fixed incomes [45]. This study highlights the potential importance of preventing fuel poverty to prevent frailty and suggests that health promotion strategies must include low- income older people as a target group to improve their housing by installing proper insulation and heating systems.
Out of the three specific indicators of frailty, fall risks had the strongest association with perceived indoor temperature and economic satisfaction. That is, those with poor economic status and perceived cold homes had a higher fall risks, while those satisfied with their economic status had a lower fall risks regardless of perceived indoor temperature. The result that fall risks was the only specific indicator of frailty with a significant association with perceived indoor temperature was expected and in line with previous findings. For example, we have reported physical performance decline among older people due to cold season and cold indoor temperature [6], and similar findings have also been reported by Lindemann et al. [5]. Yeung et al. [46] reported that there are higher incidences of falls in winter than in other seasons. Additionally, they highlighted that a higher proportion of fallers during winter had lower limb weakness than those who fell in non-winter seasons [46], as also indicated in our study.
From a health perspective, there is much to win from reducing the risks of frailty, and to prevent physical decline and subsequent falls. Regular physical activity has strong effects on reducing risk of premature death and chronic diseases [47,48]. Ultimately, the prevention of frailty improves perceived health since physical health, mental health and participation in physical activities all contribute to quality of life [49]. Furthermore, there are benefits for the society such as reduced needs for health care and social services and thus, the public expenditure.
When it comes to methodology, the current study has some limitations. First, due to the cross-sectional design we could not conduct an assessment of causality. Exploring casual association is important since it may play an instrumental role in terms of identifying reasons behind a wide range of processes, as well as assessing the impacts of changes on existing norms or processes. However, in order to study causal associations, follow-up studies are required. Second, the participants were not randomly selected. Participants included in the analysis had slightly higher risk of poor nutrition than those who were excluded. However, the rehabilitation facilities were located in different parts of Japan, and the age distribution of the participants was similar to other Japanese studies targeting frail elderly people living in the community and using rehabilitation services [50,51,52]. Hence, we are confident that the results represent the sub-population receiving rehabilitation services. Third, we assessed indoor temperature based on individual perception rather than directly measuring the temperature using thermometers. It has been reported that thermal sensitivity declines with ageing [53] and the perceived indoor temperature might not reflect the actual indoor temperature in all cases. This concern becomes larger especially in this study because all participants were frail older people, and their thermal sensitivity might be less sensitive than among healthier older people. However, when screening large populations, measurement-based investigations can be difficult to conduct because they are time consuming and costly and often require trained investigators’ support for installing thermometers in participants’ houses due to reduced independence of participants. Finally, we chose not to ask about actual income; instead we used economic satisfaction as an indicator of economic status. In fact, actual income may not have been a better measure, as the structure of a household in Japan can be very complex. In three-generation households, the employment income of the younger generations is likely to be the main household income, whereas in elderly one-person households, a public pension is likely to provide the main income [54]. Therefore, the economic status of older people changes with household structure and level of public pension.
5. Conclusions
Our results support the relationship of cold indoor temperature in the homes of older people with frailty risk. Our findings add a new contribution to studies related to frailty among older people living in the community by including the relationship with perceived indoor temperature and economic satisfaction. We can conclude that, from a public health perspective, there would be benefits from programs to support older people to maintain a warm indoor temperature: for example, by supplementing heating costs or retrofitting homes with improved insulation and multi-pane windows. For older people and their families, such efforts would probably lead to declining risks for falls and ultimately to maintenance or improvement of health. For society, such measures would reduce the needs for health care and social services and potentially reduce public expenditure.
Author Contributions
T.I. was the project leader for the present study and generated data for this article. Y.N. drafted the questionnaire and conducted the questionnaire survey with M.O. Y.N., S.M.S., and A.M.F. contributed to data analysis and wrote the paper. All authors made critical revisions and approved the final manuscript.
Funding
This study was supported in part by a JSPS KAKENHI (Grant Numbers JP17H06161, JP26249083, JP17J00520), a MHLW Grant-in-Aid for consignment study of geriatric health care business promotion (Principal Investigator: Prof. Tanji Hoshi), and a MEXT Grant-in-Aid for the Program for Leading Graduate Schools. Funding was also received from the Faculty of Medicine at Lund University, in terms of research time for A.M.F.
Acknowledgments
The authors wish to thank all the participants in the study and all the staff in the rehabilitation facilities involved in the data collection. Parts of this work were accomplished within the context of the Centre for Ageing and Supportive Environments (CASE) at Lund University.
Conflicts of Interest
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
References
- Jones, G.; Brandon, D.; Gill, D. Physical activity levels of community-dwelling older adults are influenced by winter weather variables. Arch. Gerontol. Geriatr. 2017, 71, 28–33. [Google Scholar] [CrossRef] [PubMed]
- Bunker, A.; Wildenhain, J.; Vandenbergh, A.; Henschke, N.; Rocklöv, J.; Hajat, S.; Sauerborn, R. Effects of Air Temperature on Climate-Sensitive Mortality and Morbidity Outcomes in the Elderly; a Systematic Review and Meta-analysis of Epidemiological Evidence. EBioMedicine 2016, 6, 258–268. [Google Scholar] [CrossRef] [PubMed]
- Gill, R.S.; Hambridge, H.L.; Schneider, E.B.; Hanff, T.; Tamargo, R.J.; Nyquist, P. Falling Temperature and Colder Weather Are Associated with an Increased Risk of Aneurysmal Subarachnoid Hemorrhage. World Neurosurg. 2013, 79, 136–142. [Google Scholar] [CrossRef] [PubMed]
- Mapa, B.; Taylor, B.E.; Appelboom, G.; Bruce, E.M.; Claassen, J.; Connolly, E.S. Impact of Hyponatremia on Morbidity, Mortality, and Complications After Aneurysmal Subarachnoid Hemorrhage: A Systematic Review. World Neurosurg. 2016, 85, 305–314. [Google Scholar] [CrossRef] [PubMed]
- Lindemann, U.; Oksa, J.; Skelton, D.A.; Beyer, N.; Klenk, J.; Zscheile, J.; Becker, C. Effect of cold indoor environment on physical performance of older women living in the community. Age Ageing 2014, 43, 571–575. [Google Scholar] [CrossRef] [PubMed]
- Hayashi, Y.; Schmidt, S.M.; Fänge, A.M.; Hoshi, T.; Ikaga, T. Lower Physical Performance in Colder Seasons and Colder Houses: Evidence from a Field Study on Older People Living in the Community. Int. J. Environ. Res. Public Health 2017, 14, 651. [Google Scholar] [CrossRef]
- Hwang, R.L.; Chen, C.P. Field study on behaviors and adaptation of elderly people and their thermal comfort requirements in residential environments. Indoor Air 2010, 20, 235–245. [Google Scholar] [CrossRef]
- Potvin, O.; Lorrain, D.; Belleville, G.; Grenier, S.; Préville, M. Subjective sleep characteristics associated with anxiety and depression in older adults: A population-based study. Int. J. Geriatr. Psychiatry 2014, 29, 1262–1270. [Google Scholar] [CrossRef]
- Gemmell, I. Indoor heating, house conditions, and health. J. Epidemiol. Community Health 2010, 55, 928–929. [Google Scholar] [CrossRef]
- Herr, M.; Latouch, A.; Ankri, J. Homebound status increases death risk within two years in the elderly: Results from a national longitudinal survey. Arch. Gerontol. Geriatr. 2013, 56, 258–264. [Google Scholar] [CrossRef]
- Putthinoi, S.; Lersilp, S.; Chakpitak, N. Performance in Daily Living Activities of the Elderly While Living at Home or Being Home-bound in a Thai Suburban Community. Procedia Environ. Sci. 2016, 36, 74–77. [Google Scholar] [CrossRef]
- The Cold Weather Plan for England: Protecting Health and Reducing Harm from Cold Weather. Available online: https://www.gov.uk/government/uploads/system/uploads/attachment_data/file/652568/Cold_WeathWe_Plan_Making_the_Case_2017.pdf (accessed on 24 January 2019).
- Day, R.; Hitchings, R. ‘Only old ladies would do that’: Age stigma and older people’s strategies for dealing with winter cold. Health Place 2011, 17, 885–894. [Google Scholar] [CrossRef] [PubMed]
- Fried, L.P.; Tangen, C.M.; Walston, J.; Newman, A.B.; Hirsch, C.; Gottdiener, J.; Seeman, T.; Tracy, R.; Kop, W.J.; Burke, G.; et al. Frailty in older adults: Evidence for a phenotype. J. Gerontol. Ser. A Biol. Sci. Med. Sci. 2001, 56, M146–M156. [Google Scholar] [CrossRef]
- Bergman, H.; Ferrucci, L.; Guralnik, J.; Hogan, D.B.; Hummel, S.; Karunananthan, S.; Wolfson, C. Frailty: An Emerging Research and Clinical Paradigm—Issues and Controversies. J. Gerontol. Ser. A Biol. Sci. Med. Sci. 2007, 62, 731–737. [Google Scholar] [CrossRef]
- Shinkai, S.; Watanabe, N.; Yoshida, H.; Fujiwara, Y.; Amano, H.; Lee, S.; Nishi, M.; Tsuchiya, Y. Research on screening for frailty: Development of “the Kaigo-Yobo Checklist”. Jpn. J. Public Health 2010, 57, 345–354. [Google Scholar] [CrossRef]
- Shinkai, S.; Watanabe, N.; Yoshida, H.; Fujiwara, Y.; Nishi, M.; Fukaya, T.; Lee, S.; Ogawa, K.; Murayama, H.; Taniguchi, Y.; et al. Validity of the “Kaigo-Yobo Check-List” as a frailty index. Jpn. J. Public Health 2013, 60, 262–274. [Google Scholar] [CrossRef]
- Casado, B.; Sacco, P. Correlates of Caregiver Burden Among Family Caregivers of Older Korean Americans. J. Gerontol. Ser. B 2012, 67B, 331–336. [Google Scholar] [CrossRef] [PubMed]
- Chan, C.L.; Chui, E.W. Association between cultural factors and the caregiving burden for Chinese spousal caregivers of frail elderly in Hong Kong. Aging Ment. Health 2011, 15, 500–509. [Google Scholar] [CrossRef] [PubMed]
- Collard, R.M.; Boter, H.; Schoevers, R.A.; Oude Voshaar, R.C. Prevalence of Frailty in Community-Dwelling Older Persons: A Systematic Review. J. Am. Geriatr. Soc. 2012, 60, 1487–1492. [Google Scholar] [CrossRef] [PubMed]
- Kojima, G.; Iliffe, S.; Taniguchi, Y.; Shimada, H.; Rakugi, H.; Walters, K. Prevalence of frailty in Japan: A systematic review and meta-analysis. J. Epidemiol. 2017, 27, 347–353. [Google Scholar] [CrossRef] [PubMed]
- Lu, N.; Liu, J.; Lou, V.W. Exploring the reciprocal relationship between caregiver burden and the functional health of frail older adults in China: A cross-lag analysis. Geriatr. Nurs. 2016, 37, 19–24. [Google Scholar] [CrossRef] [PubMed]
- Morley, J.E. Diabetes, Sarcopenia, and Frailty. Clin. Geriatr. Med. 2008, 24, 455–469. [Google Scholar] [CrossRef] [PubMed]
- Ferriolli, E.; Pessanha, F.A.; Moreira, V.G.; Dias, R.C.; Neri, A.L.; Lourenço, R.A. Body composition and frailty profiles in Brazilian older people: Frailty in Brazilian Older People Study-FIBRA-BR. Arch. Gerontol. Geriatr. 2017, 71, 99–104. [Google Scholar] [CrossRef] [PubMed]
- Dong, L.; Qiao, X.; Tian, X.; Liu, N.; Jin, Y.; Si, H.; Wang, C. Cross-Cultural Adaptation and Validation of the FRAIL Scale in Chinese Community-Dwelling Older Adults. J. Am. Med. Dir. Assoc. 2018, 19, 12–17. [Google Scholar] [CrossRef] [PubMed]
- Rockwood, K.; Howlett, S.; MacKnight, C.; Beattie, B.; Bergman, H.; Hébert, R.; Hogan, D.B.; Wolfson, C.; McDowell, I. Prevalence, attributes, and outcomes of fitness and frailty in community-dwelling older adults: Report from the Canadian study of health and aging. J. Gerontol. Ser. A Biol. Sci. Med. Sci. 2004, 59, 1310–1317. [Google Scholar] [CrossRef]
- Celeiro, I.D.R.; Santos-del-Riego, S.; García, J.M. Homebound status among middle-aged and older adults with disabilities in ADLs and its associations with clinical, functional, and environmental factors. Disabil. Health J. 2017, 10, 145–151. [Google Scholar] [CrossRef] [PubMed]
- Woo, J.; Yu, R.; Wong, M.; Yeung, F.; Wong, M.; Lum, C. Frailty Screening in the Community Using the FRAIL Scale. J. Am. Med. Dir. Assoc. 2015, 16, 412–419. [Google Scholar] [CrossRef] [PubMed]
- Parkkari, J.; Kannus, P.; Palvanen, M.; Natri, A.; Vanio, J.; Aho, H.; Vuori, I.; Järvinen, M. Majority of hip fractures occur as a result of a fall and impact on the greater trochanter of the femur: A prospective controlled hip fracture study with 206 consecutive patients. Calcif. Tissue Int. 1999, 65, 183–187. [Google Scholar] [CrossRef] [PubMed]
- Peeters, G.; van Schoor, N.M.; Lips, P. Fall risk: The clinical relevance of falls and how to integrate fall risk with fracture risk. Best Pract. Res. 2009, 23, 797–804. [Google Scholar] [CrossRef]
- Hasserius, R.; Karlsson, K.M.; Jónsson, B.; Redlund-Johnell, I.; Johnell, O. Long-term morbidity and mortality after a clinically diagnosed vertebral fracture in the elderly—A 12- and 22-year follow-up of 257 patients. Calcif. Tissue Int. 2005, 76, 235–242. [Google Scholar] [CrossRef] [PubMed]
- Ferrante, L.; Pisani, M.; Murphy, T.; Gahbauer, E.; Leo-Summers, L.; Gill, T. The Association of Frailty With Post-ICU Disability, Nursing Home Admission, and Mortality: A longitudinal Study. Chest 2018, 153, 1378–1386. [Google Scholar] [CrossRef] [PubMed]
- Sambamoorthi, U.; Tan, X.; Deb, A. Multiple Chronic Conditions and Healthcare Costs among Adults. Expert Rev. Pharmacoecon. Outcomes Res. 2015, 15, 823–832. [Google Scholar] [CrossRef] [PubMed]
- Lu, N.; Liu, J.; Lou, V.W. Caring for frail elders with musculoskeletal conditions and family caregivers’ subjective well-being: The role of multidimensional caregiver burden. Arch. Gerontol. Geriatr. 2015, 61, 411–418. [Google Scholar] [CrossRef] [PubMed]
- Pinquart, M.; Sörensen, S. Associations of Stressors and Uplifts of Caregiving with Caregiver Burden and Depressive Mood: A Meta-Analysis. J. Gerontol. Ser. B 2003, 58, 112–128. [Google Scholar] [CrossRef]
- Clyburn, L.D.; Stones, M.J.; Hadjistavropoulos, T.; Tuokko, H. Predicting Caregiver Burden and Depression in Alzheimer’s Disease. J. Gerontol. Ser. B 2000, 55, S2–S13. [Google Scholar] [CrossRef]
- Iecovich, E. Caregiving Burden, Community Services, and Quality of Life of Primary Caregivers of Frail Elderly Persons. J. Appl. Gerontol. 2008, 27, 309–330. [Google Scholar] [CrossRef]
- Dent, E.; Dal Grande, E.; Price, K.; Taylor, A. Frailty and usage of health care systems: Results from the South Australian Monitoring and Surveillance System (SAMSS). Maturitas 2017, 104, 36–43. [Google Scholar] [CrossRef]
- CASBEE Health Checklist 2011 (v.1.0) from Comprehensive Assessment System for Built Environment Efficiency. Available online: http://www.jsbc.or.jp/CASBEE/health_check/index.html (accessed on 24 January 2019).
- Stolz, E.; Mayerl, H.; Waxenegger, A.; Freidl, W. Explaining the impact of poverty on old-age frailty in Europe: Material, psychosocial and behavioural factors. Eur. J. Public Health 2017, 27, 1003–1009. [Google Scholar] [CrossRef]
- Kalaiselve, S.; Arjumand, Y.; Jayalakshmy, R.; Gomathi, R.; Pruthu, T.; Palanivel, C. Prevalence of under-nutrition, associated factors and perceived nutritional status among elderly in a rural area of Puducherry. South India 2016, 65, 156–160. [Google Scholar] [CrossRef]
- Aylaz, R.; Aktürk, Ü.; Erci, B.; Öztürk, H.; Aslan, H. Relationship between depression and loneliness in elderly and examination of influential factors. Arch. Gerontol. Geriatr. 2012, 55, 548–554. [Google Scholar] [CrossRef]
- Hirazawa, M.; Yakita, A. Labor supply of elderly people, fertility, and economic development. J. Macroecon. 2017, 51, 75–96. [Google Scholar] [CrossRef]
- Hamilton, I.G.; O’Sullivan, A.; Huebner, G.; Oreszczyn, T.; Shipworth, D.; Summerfield, A.; Davies, M. Old and cold? Findings on the determinants of indoor temperatures in English dwellings during cold conditions. Energy Build. 2017, 141, 142–157. [Google Scholar] [CrossRef]
- Wright, F. Old and Cold: Older People and Policies Failing to Address Fuel Poverty. Soc. Policy Adm. 2004, 38, 488–503. [Google Scholar] [CrossRef]
- Yeung, P.Y.; Chau, P.H.; Woo, J.; Yim, V.W.T.; Rainer, T.H. Higher incidence of falls in winter among older people in Hong Kong. J. Clin. Gerontol. Geriatr. 2011, 2, 13–16. [Google Scholar] [CrossRef]
- Annear, M.J.; Cushman, G.; Gidlow, B. Leisure time physical activity differences among older adults from diverse socioeconomic neighborhoods. Health Place 2009, 15, 482–490. [Google Scholar] [CrossRef]
- Warburton, D.E.R.; Nicol, C.W.; Bredin, S.S.D. Health benefits of physical activity: The evidence. Can. Med. Assoc. J. 2006, 176, 801–809. [Google Scholar] [CrossRef]
- Hickey, A.; Barker, M.; Mcgee, H.; O’Boyle, C. Measuring health-related quality of life in older patient populations. PharmacoEconomics 2005, 23, 971–993. [Google Scholar] [CrossRef]
- Miura, H.; Yamasaki, K.; Morizaki, N.; Moriya, S.; Sumi, Y. Factors influencing oral health-related quality of life (OHRQoL) among the frail elderly residing in the community with their family. Arch. Gerontol. Geriatr. 2010, 51, e62–e65. [Google Scholar] [CrossRef]
- Ota, S.; Goto, H.; Fujita, R.; Haruta, M.; Noda, Y.; Tamakoshi, K. Application of Pole Walking to Day Service Centers for Use by Community-dwelling Frail Elderly People. Int. J. Gerontol. 2014, 8, 6–11. [Google Scholar] [CrossRef]
- Shimada, H.; Ishizaki, T.; Kato, M.; Morimoto, A.; Tamate, A.; Uchiyama, Y.; Yasumura, S. How often and how far do frail elderly people need to go outdoor to maintain functional capacity? Arch. Gerontol. Geriatr. 2010, 50, 140–146. [Google Scholar] [CrossRef]
- Inoue, Y.; Gerrett, N.; Kuwahara, T.I.; Umino, Y.; Kiuchi, S.; Amano, T.; Ueda, H.; Havenith, G.; Kondo, N. Sex differences in age-related changes on peripheral warm and cold innocuous thermal sensitivity. Physiol. Behav. 2016, 164A, 86–92. [Google Scholar] [CrossRef] [PubMed]
- Shirahase, S. Income inequality among older people in rapidly aging Japan. Res. Soc. Stratif. Mobil. 2015, 41, 1–10. [Google Scholar] [CrossRef]
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).