Patient Education and Continuing Medical Education to Promote Shared Decision-Making. A Systematic Literature Review
Abstract
1. Introduction
2. Materials and Methods
2.1. Search Strategy
2.2. Inclusion Criteria
2.3. Exclusion Criteria
2.4. Information Extraction and Quality Assessment
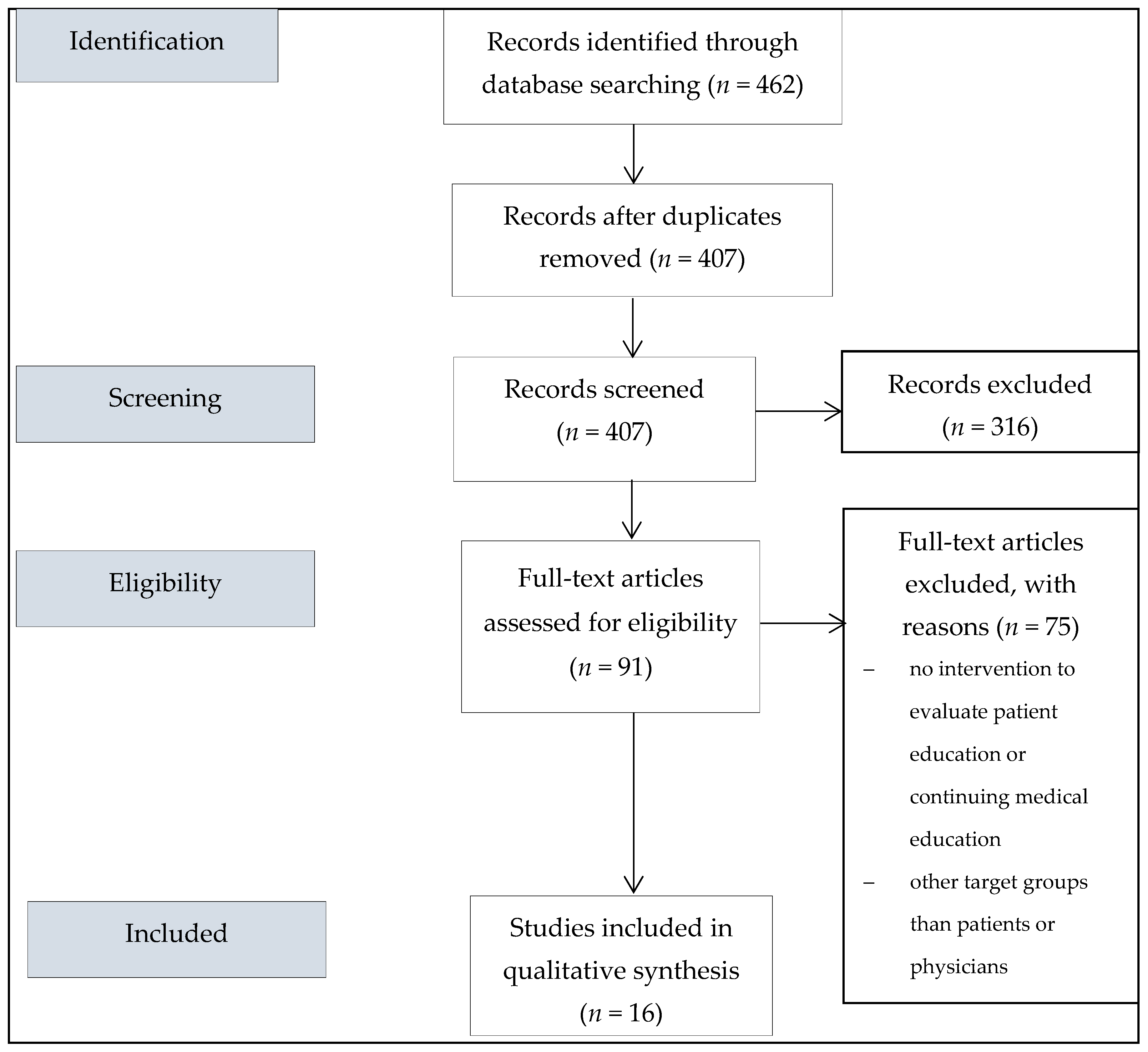
3. Results
3.1. Characteristics of Included Studies
3.2. Studies on Patient Education
3.2.1. Study Designs and Objectives
3.2.2. Number of Course Participants
3.2.3. Interventions
Persons Involved and Intervention Timing
Description of the Interventions
Duration
3.2.4. Main Results
3.2.5. Study Quality
3.3. Studies on Continuing Medical Education
3.3.1. Study Design and Objectives
3.3.2. Number of Course Participants
3.3.3. Interventions
Persons Involved and Intervention Timing
Description of the Interventions
Duration
3.3.4. Main Results
3.3.5. Study Quality
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Härter, M. Shared decision making –. from the point of view of patients physicians and health politics is set in place. Z Arztl Fortbild Qualitatssich 2004, 98, 89–92. [Google Scholar] [PubMed]
- Charles, C.; Gafni, A.; Whelan, T. Shared decision-making in the medical encounter: What does it mn? (or it takes at least two to tango). Soc. Sci. Med. 1997, 44, 681–692. [Google Scholar] [CrossRef]
- Dirmaier, J.; Härter, M. Stärkung der Selbstbeteiligung in der Rehabilitation. Bundesgesundheitsblatt. Gesundheitsforschung. Gesundheitsschutz 2011, 54, 411–419. [Google Scholar]
- Faller, H.; Reusch, A.; Ströbl, V.; Vogel, H. Patientenschulung als Element der Patientenorientierung in der Rehabilitation. Rehabilitation 2008, 47, 77–83. [Google Scholar] [CrossRef] [PubMed]
- Loh, A.; Simon, D.; Kriston, L.; Härter, M. Patientenbeteiligung bei medizinischen Entscheidungen. Effekte der Partizipativen Entscheidungsfindung aus systematischen Reviews. Dtsch Arztebl 2007, 104, A1483–A1488. [Google Scholar]
- Simon, D.; Loh, A.; Härter, M. Grundlagen der Partizipativen Entscheidungsfindung und Beispiele der Anwendung in der Rehabilitation. Rehabilitation 2008, 47, 84–89. [Google Scholar] [CrossRef]
- Simon, D. Partizipative Entscheidungsfindung in der Psychiatrie und Psychotherapie. Erste Ergebnisse und Transfer in die Versorgung. Forum für Kinder- und Jugendpsychiatrie, Psychosomatik und Psychotherapie 2009, 4, 62–75. [Google Scholar]
- Simon, D.; Härter, M. Grundlagen der Partizipativen Entscheidungsfindung und Umsetzungsmöglichkeiten im Rahmen der Selbsthilfe. Bundesgesundheitsblatt, Gesundheitsforschung, Gesundheitsschutz 2009, 52, 86–91. [Google Scholar] [CrossRef] [PubMed]
- Spezialist Unit for Review Evidence (SURE). Questions to Assist with the Critical Appraisal of Randomised Controlled Trials and other Experimental Studies. Available online: https://www.cardiff.ac.uk/specialist-unit-for-review-evidence/resources/critical-appraisal-checklists (accessed on 28 June 2019).
- Spezialist Unit for Review Evidence (SURE). Questions to Assist with the Critical Appraisal of Cohort Studies. Available online: https://www.cardiff.ac.uk/specialist-unit-for-review-evidence/resources/critical-appraisal-checklists (accessed on 28 June 2019).
- Alegria, M.; Carson, N.; Flores, M.; Li, X.; Shi, P.; Lessios, A.S.; Polo, A.; Allen, M.; Fierro, M.; Interian, A.; et al. Activation, Self-Management, Engagement, and Retention in Behavioral Health Care: A Randomized Clinical Trial of the DECIDE Intervention. Jama Psychiatry 2014, 71, 557–565. [Google Scholar] [CrossRef]
- Deen, D.; Lu, W.; Rothstein, D.; Santana, L.; Gold, M.R. Asking questions: The effect of a brief Intervention in community health centers on patient activation. Patient Educ. Couns. 2011, 84, 257–260. [Google Scholar] [CrossRef]
- Hamann, J.; Mendel, R.; Meier, A.; Asani, F.; Pausch, E.; Leucht, S.; Kissling, W. “How to Speak to Your Psychiatrist”: Shared Decision-Making Training for Inpatients With Schizophrenia. Psychiatr Serv. 2011, 62, 1218–1221. [Google Scholar] [CrossRef] [PubMed]
- Bernhard, J.; Butow, P.; Aldridge, J.; Juraskova, I.; Ribi, K.; Brown, R. Communication about standard treatment options and clinical trials: can we teach doctors new skills to improve patient outcomes? Psycho-Oncol. 2012, 21, 1265–1274. [Google Scholar] [CrossRef] [PubMed]
- Bieber, C.; Müller, K.G.; Blumenstiel, K.; Schneider, A.; Richter, A.; Wilke, S.; Hartmann, M.; Eich, W. Long-term effects of a shared decision-making intervention on physician-patient interaction and outcome in fibromyalgia. A qualitative and quantitative 1 year follow-up of a randomized controlled trial. Patient Educ. Couns. 2006, 63, 357–366. [Google Scholar] [CrossRef]
- Bieber, C.; Müller, K.G.; Blumenstiel, K.; Hochlehnert, A.; Wilke, S.; Hartmann, M.; Eich, W. A shared decision-making communication training program for physicians treating fibromyalgia patients: Effects of a randomized controlles trial. J. Psychosom. Res. 2008, 64, 13–20. [Google Scholar] [CrossRef] [PubMed]
- Bieber, C.; Nicolai, J.; Hartmann, M.; Blumenstiel, K.; Ringel, N.; Schneider, A.; Härter, M.; Eich, W.; Loh, A. Training physicians in shared decision-making—Who can be reached and what is achieved? Patient Educ. Couns. 2009, 77, 48–54. [Google Scholar] [CrossRef] [PubMed]
- Hölzel, L.P.; Vollmer, M.; Kriston, L.; Siegel, A.; Härter, M. Patientenbeteiligung bei medizinischen Entscheidungen in der Integrierten Versorgung Gesundes Kinzigtal Ergebnisse einer kontrollierten Kohortenstudie. Bundesgesundheitsbl. 2012, 55, 1524–1533. [Google Scholar] [CrossRef]
- Légaré, F.; Guerrier, M.; Nadeau, C.; Rhéaume, C.; Turcotte, S.; Labrecque, M. Impact of DECISION +2 on patient and physician assessment of shared decision making implementation in the context of antibiotics use for acute respiratory infections. Implement. Sci. 2013, 144. [Google Scholar] [CrossRef]
- Légaré, F.; Labrecque, M.; Cauchon, M.; Castel, J.; Turcotte, S.; Grimshaw, J. Training family physicians in shared decision-making to reduce the overuse of antibiotics in acute respiratory infections: a cluster randomized trial. Can. Med. Assoc. J. 2012, 184, E726–E734. [Google Scholar] [CrossRef]
- Légaré, L.; Labrecque, M.; LeBlanc, A.; Njoya, M.; Laurier, C.; Côté, L.; Godin, G.; Thivierge, R.L.; O’Connor, A.; St-Jacques, S. Training family physicians in shared decision making for the use of antibiotics for acute respiratory infections: A pilot clustered randomized controlled trial. Health Expect. 2010, 14, 96–110. [Google Scholar] [CrossRef]
- Loh, A.; Simon, D.; Wills, C.E.; Kriston, L.; Niebling, W.; Härter, M. The effects of shared decision-making intervention in primary care of depression: A cluster-randomized controlled trial. Patient Educ. Couns. 2007, 67, 324–332. [Google Scholar] [CrossRef]
- Maatouk-Bürmann, B.; Ringel, N.; Spang, J.; Weiss, C.; Möltner, A.; Riemann, U.; Langewitz, W.; Schultz, J.-H.; Jünger, J. Improving patient-centered communication: Results of a randomized controlled trial. Patient Educ. Couns. 2016, 99, 117–124. [Google Scholar] [CrossRef] [PubMed]
- Sullivan, M.D.; Leigh, J.; Gaster, B. Brief report: Training internists in shared decision making about chronic opioid treatment for noncancer pain. J. Gen. Intern. Med. 2006, 21, 360–362. [Google Scholar] [CrossRef] [PubMed]
- Tinsel, I.; Buchholz, A.; Vach, W.; Siegel, A.; Dürk, T.; Buchholz, A.; Niebling, W.; Fischer, K.G. Shared decision-making in antihypertensive therapy: A cluster randomised controlled trial. BMC Fam. Pract. 2013, 135. [Google Scholar] [CrossRef] [PubMed]
- Timmermans, L.M.; van der Maazen, R.W.M.; van Spaendonck, K.P.M.; Leer, J.W.H.; Kraaimaat, F.W. Enchancing patient participation by training radiation oncologists. Patient. Educ. Couns. 2006, 63, 55–63. [Google Scholar] [CrossRef] [PubMed]
- Bühner, M.; Ziegler, M. Statistik für Psychologen und Sozialwissenschaftler [statistics for psychologists and social scientists]; Pearson Studium: Munic, Germany, 2009. [Google Scholar]
- Sanders, A.R.J.; van Weeghel, I.; Vogelaar, M.; Verheul, W.; Pieters, R.H.M.; de Wit, J.J.; Bensing, J.M. Effects of improved patient participation in primary care on health-related outcomes: A systematic review. Fam. Pract. 2013, 30, 365–378. [Google Scholar] [CrossRef]
- Körner, M.; Ehrhardt, H.; Steger, A.-K.; Bengel, J. Interprofessional SDM train-the-trainer program “Fit for SDM”: Provider satisfaction and impact on participation. Patient Educ. Couns. 2012, 89, 122–128. [Google Scholar] [CrossRef] [PubMed]
- Körner, M.; Wirtz, M.; Michaelis, M.; Ehrhardt, H.; Steger, A.-K.; Zerpies, E.; Bengel, J. A multicentre cluster-randomized controlled study to evaluate a train-the-trainer programme for implementing internal and external participation in medical rehabilitation. Clin. Rehabil. 2014, 28, 20–35. [Google Scholar] [CrossRef]
- Zentrum Patientenschulung. Manuale in der Patientenschulung. Available online: http://www.zentrum-patientenschulung.de/manuale/ (accessed on 2 July 2019).
| Literature | Topic | Country | Design | Characteristics of the Course Participants | |
|---|---|---|---|---|---|
| n | Age | ||||
| Alegria et al. 2014 [11] | PE | United States of America/Puerto Rico | Randomized controlled trial | 647 | 18 to >65 |
| Deen et al. 2011 [12] | PE | United States of America | Before-and-after-study | 252 | 39 (Mean) |
| Hamann et al. 2011 [13] | PE | Germany | Randomized controlled trial | 61 | 40,7 (Mean) |
| Bernhard et al. 2012 [14] | CME | Australia, New Zealand, Switzerland, Germany, Austria | Randomized controlled trial | 62 | 39.5 (Mean) |
| Bieber et al. 2006 [15] | CME | Germany | Mixed Methods Study (qualitative and Before and After Study) | 13 | Not specified |
| Bieber et al. 2008 [16] | CME | Germany | Randomized controlled trial | 10 | 30.8 (Mean) |
| Bieber et al. 2009 [17] | CME | Germany | Before-and-after-study | 123 | 45 (Mean) |
| Hölzel et al. 2012 [18] | CME | Germany | Controlled cohort study with longitudinal design | 33 | Not specified |
| Légaré et al. 2013 [19] | CME | Canada | Randomized controlled trial | 270 | 42.9 (Mean) |
| Légaré et al. 2012 [20] | CME | Canada | Randomized controlled trial | 149 | Not specified |
| Légaré et al. 2010 [21] | CME | Canada | Randomized controlled trial | 33 | Not specified |
| Loh et al. 2007 [22] | CME | Germany | Randomized controlled trial | 42 | 33.77 (Mean) |
| Maatouk-Bürmann et al. 2016 [23] | CME | Germany | Randomized controlled trial | 23 | 48.4 (Mean) |
| Sullivan et al. 2006 [24] | CME | United States of America | Randomized controlled trial | 45 | Not specified |
| Tinsel et al. 2013 [25] | CME | Germany | Randomized controlled trial | 36 | Not specified |
| Timmermans et al. 2006 [26] | CME | Netherlands | Before-and-after-study | 8 | 33 (Mean) |
| Study | Type of Intervention | Applied Methodology | Brief Description of the Intervention | Duration |
|---|---|---|---|---|
| Alegria et al. 2014 [11] | Group intervention (DECIDE intervention) | Brainstorming, summary, role play exercises and practical exercises |
| 30–45 min per training session with three training sessions total |
| Deen et al. 2011 [12] | Individual interviews | Interviews, brainstorming |
| Not specified |
| Hamann et al. 2011 [13] | Group intervention | Role play exercises |
| Total of five hours, number of appointments not specified |
| Literature | Type of Intervention | Applied Methodology | Brief Description of the Intervention | Duration |
|---|---|---|---|---|
| Bernhard et al. 2012 [14] | Group Intervention | Workshop with video modelling ideal behaviour and role play exercises |
| Total of seven hours and one session |
| Bieber et al. 2006 [15] Bieber et al. 2008 [16] | Mixed (Individual and Group Intervention) | Role play exercises, interactive talks, analysis of instructional videos with standardized patients | Training program
| Total of 18 hours, number of sessions not specified |
| Bieber et al. 2009 [17] | Group Intervention | Interactive presentations, model films on consultations, instructional videos with standardized patients, group discussion, practical exercises, role-playing of simulated consultations | Training program
| Total of eight hours for two sessions |
| Hölzel et al. 2012 [18] | Group Intervention | Not described | Training program
| Total of nine hours and three courses |
| Légaré et al. 2010 [21] | Group Intervention | DECISION + training program with video games, practical exercises, decision support tools, educational material |
| Total of three hours on three different days |
| Légaré et al. 2013 [19] Légaré et al. 2012 [20] | Mixed (Individual and Group Intervention) | DECISION + 2 training program with web-based self-tutorial, face-to-face, interactive sessions using videos, exercises and decision support tools |
| Total of four hours in one course |
| Loh et al. 2007 [22] | Group Intervention | Multi-faceted program with specialized lectures with accompanying questions, discussion rounds, facilitation practice, role-playing, video exemplars, vignettes |
| Not specified (five training sessions in six months) |
| Maatouk-Bürmann et al. 2016 [23] | Mixed (Individual and Group Intervention) | Role play exercises with fictitious patients, video feedback, direct informative feedback, and debriefing | Communication training
| Total of 24 hours on three different days and two hours for individual feedback |
| Sullivan et al. 2006 [24] | Mixed (Individual and Group Intervention) | Videos and discussion | Training program
| Total of two hours and two sessions |
| Tinsel et al. 2013 [25] | Group Intervention | Role play exercises, patient information in the form of flyers | Training program
| Total of six hours, number of sessions not specified |
| Timmermans et al. 2006 [26] | Group Intervention | Group discussion, training with simulation patients, video recording, individual feedback, a short written notice about the desired behaviour | Training program
| Total of six hours in two sessions, and an additional three hours for individual feedback |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Wagner, A.; Radionova, N.; Rieger, M.A.; Siegel, A. Patient Education and Continuing Medical Education to Promote Shared Decision-Making. A Systematic Literature Review. Int. J. Environ. Res. Public Health 2019, 16, 2482. https://doi.org/10.3390/ijerph16142482
Wagner A, Radionova N, Rieger MA, Siegel A. Patient Education and Continuing Medical Education to Promote Shared Decision-Making. A Systematic Literature Review. International Journal of Environmental Research and Public Health. 2019; 16(14):2482. https://doi.org/10.3390/ijerph16142482
Chicago/Turabian StyleWagner, Anke, Natalia Radionova, Monika A. Rieger, and Achim Siegel. 2019. "Patient Education and Continuing Medical Education to Promote Shared Decision-Making. A Systematic Literature Review" International Journal of Environmental Research and Public Health 16, no. 14: 2482. https://doi.org/10.3390/ijerph16142482
APA StyleWagner, A., Radionova, N., Rieger, M. A., & Siegel, A. (2019). Patient Education and Continuing Medical Education to Promote Shared Decision-Making. A Systematic Literature Review. International Journal of Environmental Research and Public Health, 16(14), 2482. https://doi.org/10.3390/ijerph16142482





