Journal Description
Société Internationale d’Urologie Journal
Société Internationale d’Urologie Journal
(SIUJ) is an international, peer-reviewed, open access journal that covers all aspects of urology and related fields, published bimonthly online. It is the official journal of the International Society of Urology (SIU).
- Open Access— free for readers and authors (diamond open access), with article processing charges (APC) paid by the Société Internationale d’Urologie.
- Rapid Publication: manuscripts are peer-reviewed and a first decision is provided to authors approximately 51.2 days after submission; acceptance to publication is undertaken in 34.2 days (median values for papers published in this journal in the second half of 2025).
- Recognition of Reviewers: APC discount vouchers, optional signed peer review, and reviewer names published annually in the journal.
Latest Articles
Global Urology in an Era of Geopolitical Division
Soc. Int. Urol. J. 2026, 7(2), 31; https://doi.org/10.3390/siuj7020031 - 21 Apr 2026
Abstract
It is difficult to comprehend how much the world has changed since the publication of the last Société Internationale d’Urologie Journal (SIUJ) issue in February [...]
Full article
Open AccessArticle
External Validation of the EAU Guidelines Bot for Urethral Stricture: Accuracy, Completeness, and Clarity Analysis
by
Pietro Spatafora, Riccardo Lombardo, Manfredi Bruno Sequi, Marta Santioni, Eleonora Rosato, Matteo Romagnoli, Sabrina De Cillis, Enrico Checcucci, Daniele Amparore, Mauro Ragonese, Nazario Foschi, Valerio Santarelli, Giorgia Tema, Antonio Franco, Antonio Luigi Pastore, Bernardo Rocco, Mauro Gacci, Sergio Serni, Giacomo Gallo, Vincenzo Pagliarulo, Cristian Fiori, Enrico Finazzi Agrò, Francesco del Giudice, Alessandro Sciarra, Andrea Tubaro and Cosimo De Nunzioadd
Show full author list
remove
Hide full author list
Soc. Int. Urol. J. 2026, 7(2), 30; https://doi.org/10.3390/siuj7020030 - 21 Apr 2026
Abstract
Background/Objectives: Recently the European Association of Urology (EAU) guidelines presented the EAU Guidelines bot to assist urologists in the reading of the guidelines; however, there is a lack of up-to-date external validation. The aim of our study is to assess the accuracy, completeness,
[...] Read more.
Background/Objectives: Recently the European Association of Urology (EAU) guidelines presented the EAU Guidelines bot to assist urologists in the reading of the guidelines; however, there is a lack of up-to-date external validation. The aim of our study is to assess the accuracy, completeness, and clarity of the guidelines bot in urethral strictures. Methods: A total of 117 questions based on the EAU urethral strictures guidelines recommendations were developed. Each question was input to the EAU guidelines bot and the response was assessed by two expert urologists to assess the accuracy, completeness, and clarity. Moreover, 10 simple clinical cases were input. A 5-point Likert scale was used as a score and, in case of discrepancies, a third urologist was queried. Accuracy, completeness and clarity were assessed per chapter and per grade of recommendation. All questions and answers were recorded in an Excel file. Results: Overall 117 questions were developed. In terms of accuracy, 111/117 (95%) were defined as accurate (scores 4–5), 4/117 (3%) presented a fair accuracy (score 3), and 2/117 (2%) were deemed not accurate. In terms of completeness, 93/117 (80%) were defined as complete (scores 4–5), 22/117 (19%) presented a fair completeness (score 3), and 2/117 (2%) were deemed not complete. Finally, in terms of clarity, 104/117 (89%) were defined as clear (scores 4–5), 13/117 (11%) presented a fair clarity (score 3), and 0/109 (0%) were deemed not clear. When comparing strong and weak recommendations, no differences were recorded. Overall the answers to simple clinical cases were in line with the guidelines with good accuracy, completeness and clarity scores. Conclusions: The EAU guidelines bot represents an accurate tool for urethral stenosis guidelines. Some fine-tuning is needed to improve readability and clarity.
Full article
Open AccessArticle
Impact of Expedited Ureteroscopy on Emergency Department Utilisation in Stented Patients with Urolithiasis
by
Henry Wang, Christine Zhao, Andrew Brooks, Ankur Dhar and Simon Bariol
Soc. Int. Urol. J. 2026, 7(2), 29; https://doi.org/10.3390/siuj7020029 - 20 Apr 2026
Abstract
Background/Objectives: Ureteric stents are commonly used in the management of urolithiasis but are associated with significant morbidity, leading to unplanned emergency department presentations and increased healthcare utilisation. This study aimed to evaluate whether reducing ureteric stent dwell time from three months to one
[...] Read more.
Background/Objectives: Ureteric stents are commonly used in the management of urolithiasis but are associated with significant morbidity, leading to unplanned emergency department presentations and increased healthcare utilisation. This study aimed to evaluate whether reducing ureteric stent dwell time from three months to one month was associated with reduced stent-related emergency presentations. Secondary objectives were to assess post-ureteroscopy infective complications and identify predictors of emergency attendance. Methods: A retrospective cohort study was conducted across Western Sydney Local Health District, comparing patients undergoing ureteric stenting prior to ureteroscopy before (n = 189) and after (n = 244) an institutional policy change reducing time to definitive surgery from three months to one month. Patients aged ≥16 years with urolithiasis were included. Results: Following the policy change, mean waiting time for ureteroscopy decreased from 97.3 to 40.6 days. The proportion of patients presenting to the emergency department (ED) for stent-related symptoms decreased from 31.7% to 16.4% (p < 0.001), and mean presentations per patient declined from 0.60 to 0.21 (p < 0.001). Stent irritation accounted for most presentations. Using multivariable analysis, age < 50 years, immunosuppression, and positive pre-operative urine cultures were independently associated with ED attendance. Post-ureteroscopy infective complications were lower in the shortened dwell-time cohort (2.0% vs. 4.2%) but did not reach statistical significance (p = 0.26). Conclusions: Reducing routine ureteric stent dwell time from three months to one month was associated with significantly fewer stent-related emergency presentations. Shorter dwell protocols may reduce patient morbidity and healthcare utilisation and could be associated with lower rates of post-ureteroscopy infective complications.
Full article
Open AccessArticle
Uroflowmetry or Urethroscopy as a Surveillance Tool After End-to-End Anastomotic Urethroplasty Done for PFUI—A Blinded Study
by
Soumya Shivasis Pattnaik, Ganesh Gopalakrishnan, Sistla Bobby Viswaroop, Myilswamy Arul, Natarajan Sridharan, Marimuthu Kanagasabapathi and Sangampalayam Vedanayagam Kandasami
Soc. Int. Urol. J. 2026, 7(2), 28; https://doi.org/10.3390/siuj7020028 - 20 Apr 2026
Abstract
►▼
Show Figures
Background/Objectives: Uroflowmetry is done in the surveillance period after End-to-end Anastomotic Urethroplasty for pelvic fracture urethral injury. But is maximum flow rate a reliable surrogate for urethral calibre in these cases? The above question laid the foundation of the study. The aim
[...] Read more.
Background/Objectives: Uroflowmetry is done in the surveillance period after End-to-end Anastomotic Urethroplasty for pelvic fracture urethral injury. But is maximum flow rate a reliable surrogate for urethral calibre in these cases? The above question laid the foundation of the study. The aim of the study was: “Is uroflowmetry alone sufficient to predict a successful outcome following urethroplasty after pelvic fracture urethral injury (PFUI)?” Methods: We conducted a prospective masked study of all patients undergoing end-to-end anastomosis (EEA) urethroplasty for PFUI from January 2017 to September 2022. The first follow-up was 4 weeks after surgery, micturating cystourethrogram (MCU) was done after urethral catheter removal and at the same time, uroflowmetry was also done. The second follow-up was 6 months after surgery, when uroflowmetry was repeated, and urethroscopy was performed. The urologist performing urethroscopy was blinded to the uroflowmetry results. Results: In total, 26 patients were included in the study. After 6 months, 1 patient had poor flow (maximum flow rate [Q max] < 10 mL/s), 7 patients had flow with Q max 10–15 mL/s, and 18 patients had normal flow (Q max > 15 mL/s). On urethroscopy, all patients had a normal and easily passable urethra. The International Prostate Symptom Score (IPSS) and quality of life (QoL) scores showed a positive correlation. The urologist performing urethroscopy and the investigator recording uroflowmetry reached different conclusions. Conclusions: A reduced peak on uroflowmetry after EEA urethroplasty in PFUI does not always indicate surgical failure. Urethroscopy enables direct visualisation of the anastomotic site and provides more detailed information than uroflowmetry. The IPSS score and quality of life are more important than Q max alone.
Full article

Figure 1
Open AccessArticle
Artificial Intelligence Chatbots as Information Sources on Testicular Cancer: Quality, Readability and Actionability
by
Harrison Lucas, Brendan Dittmer, Peter Stapleton, Ben Tran, Niall M. Corcoran and Niranjan Sathianathen
Soc. Int. Urol. J. 2026, 7(2), 27; https://doi.org/10.3390/siuj7020027 - 19 Apr 2026
Abstract
►▼
Show Figures
Background/Objectives: Testicular cancer is one of the most common malignancies affecting young adult males. With the rise in artificial intelligence (AI) platforms, many patients seek health information online. Yet chatbot responses specific to testicular cancer remain unassessed. This study aims to evaluate
[...] Read more.
Background/Objectives: Testicular cancer is one of the most common malignancies affecting young adult males. With the rise in artificial intelligence (AI) platforms, many patients seek health information online. Yet chatbot responses specific to testicular cancer remain unassessed. This study aims to evaluate the role of AI chatbots in providing patient information about testicular cancer in terms of its quality, readability and actionability. Methods: Fourteen frequently asked questions about testicular cancer were identified using Google Trends and the Cancer Council Australia website. Questions were then inputted into four different publicly accessible AI platforms: ChatSonic, Bing AI, ChatGPT 4.0 and Perplexity. Chatbot responses were recorded and evaluated using three validated instruments: DISCERN (1–5), Patient Education Materials Assessment Tool (PEMAT)-Understandability and Actionability (0–100%) and Flesch-Kincaid readability scores. Results: All platforms scored low on the DISCERN score with a median of 1 (interquartile range [IQR] 1–4). The median readability score was 34.1 (IQR 26.0–52.2), indicating a reading level suitable for college students. The median word count was 61.5 (IQR, 41.3–91.3). The overall PEMAT-Understandability was moderate (median 58.3, 50.0–66.7), whilst the PEMAT-Actionability was very poor (median 0, IQR 0–25). Conclusions: AI chatbots deliver moderately understandable information on testicular cancer, but this information is typically not actionable and is delivered at an above-average reading level. Despite this, patients may continue to use AI chatbots (AICs) to access health information. It is important that clinicians counsel patients on the benefits and downfalls of this strategy, advocating for the use of AICs as an adjunct rather than a replacement for clinician-led education.
Full article

Figure 1
Open AccessArticle
The Efficacy and Safety Profile of UroLift for Management of Benign Prostatic Hyperplasia in Australia
by
Harrison Lucas, David Homewood, Suzanne Wallace, Helen O’Connell, Justin Chee, Vy Tran, Niall M. Corcoran and Mariolyn Rajakulenthiran
Soc. Int. Urol. J. 2026, 7(2), 26; https://doi.org/10.3390/siuj7020026 - 18 Apr 2026
Abstract
►▼
Show Figures
Background/Objectives: For men with bothersome lower urinary tract symptoms (LUTS) secondary to benign prostatic hyperplasia (BPH) requiring surgical intervention, UroLift has been shown to be an effective and durable, minimally invasive method. Methods: A retrospective review was conducted for 72 patients
[...] Read more.
Background/Objectives: For men with bothersome lower urinary tract symptoms (LUTS) secondary to benign prostatic hyperplasia (BPH) requiring surgical intervention, UroLift has been shown to be an effective and durable, minimally invasive method. Methods: A retrospective review was conducted for 72 patients who underwent UroLift at a single hospital in Australia between 2018 and 2025. Data regarding baseline demographics, the pre- and post-operative International Prostate Symptom Score (IPSS), maximum urinary flow rate (Qmax), the post-void residual (PVR), and complications were collected prospectively. Inclusion criteria for patients selected for UroLift were males over 50 years with a prostate volume between 20 and 70 mL, pre-operative PVR of <350 mL and Qmax and IPSSs of <15 mL/s and >12 respectively. The purpose of this study is to assess the clinical outcomes of patients treated with UroLift at our institution and compare these findings to the existing literature. Results: Complete data was available for 34 patients. Our cohort had a median age of 63.0 years (interquartile range [IQR] 58.0–69.0) and UroLift was performed using a median number of 4.05 implants per patient. Median prostate volume (mL) was 43.0 (IQR 38.0–59.0). Post-operatively, the median percentage changes in the IPSS, Qmax (mL/s) and PVR (mL) were −30.9% (IQR 5.8–−71.1, p = 0.0048), 40.1% (IQR −6.6–165.1, p = 0.0159) and −36.4% (IQR −84.6–29.8, p = 0.0232), respectively. Most patients (n = 24, 73.5%) were discharged on the same day of the UroLift procedure with the remainder (n = 9, 26.5%) being discharged on day 1 post-operatively. The median time (months) for post-operative review was 2 (IQR 0.9–3.3). Conclusions: UroLift is safe, effective, and a minimally invasive treatment option in suitable patients with bothersome LUTS requiring surgical intervention.
Full article

Figure 1
Open AccessArticle
Can Computed Tomography Findings for Kidney, Ureter and Bladder Correlate with Medical Comorbidity in Renal Colic Patients?
by
Lara Sharpe, Basil Razi, Cheryl Fung, Rajni Lal, Marnique Basto and Henry H. Woo
Soc. Int. Urol. J. 2026, 7(2), 25; https://doi.org/10.3390/siuj7020025 - 17 Apr 2026
Abstract
►▼
Show Figures
Background/Objectives: Sarcopenia is a progressive skeletal muscle disorder linked to adverse outcomes. Computed Tomography (CT) can quantify skeletal muscle, while the Charlson Comorbidity Index (CCI) predicts mortality by categorising comorbidities. This study examined whether Computed Tomography of the Kidneys, Ureters, and Bladder (CT-KUB)-derived
[...] Read more.
Background/Objectives: Sarcopenia is a progressive skeletal muscle disorder linked to adverse outcomes. Computed Tomography (CT) can quantify skeletal muscle, while the Charlson Comorbidity Index (CCI) predicts mortality by categorising comorbidities. This study examined whether Computed Tomography of the Kidneys, Ureters, and Bladder (CT-KUB)-derived skeletal muscle measurements correlate with CCI scores in hospitalised patients. Methods: This retrospective study included all patients admitted with renal colic to the Urology Department, Blacktown Hospital and underwent cystoscopy between June 2022 and June 2025. Data were obtained from electronic medical records. CCI scores, incorporating age and comorbidities, generated 10-year survival estimates. CT-KUB scans were reviewed for psoas muscle perimeter, area, height, width and Hounsfield unit at the aortic bifurcation. Skeletal Muscle Index (SMI) was calculated as skeletal muscle area (SMA)/height2. Associations between CCI, psoas muscle metrics and outcomes (length of stay, Intensive Care Unit (ICU) admission, Emergency Department (ED) re-presentation) were assessed using Pearson’s correlations and between-group comparisons. Results: A total of 397 patients were analysed. Median Length of Stay (LOS) was 1 day (mean = 1.92, SD = 1.88). ICU admission occurred in 2.3% of patients, and 18.6% re-presented to ED within 30 days. Both CCI survival percentage and psoas muscle metrics (including SMI) were significantly associated with LOS. Lower SMA, Hounsfield unit (HU), length and perimeter were linked to higher ICU admission risk. Neither CCI nor muscle measures predicted ED re-presentation. Conclusions: CCI and CT-derived muscle metrics were independently associated with outcomes such as LOS and ICU admission. Combining these measures may improve risk stratification, warranting further prospective evaluation.
Full article

Figure 1
Open AccessArticle
Urology Training Across Borders: An International Survey of Residents’ Experiences, Perceptions, and Expectations
by
Andrea Alberti, Rossella Nicoletti, Anna Luisa Heinrichs, Julian Peter Struck, Petros Sountoulides, Francesco Curto, Sergio Serni, Georgios Chasiotis, Olumide Farinre, Harshit Garg, Clément Klein, Gaelle Margue, Amanda A. Myers, Nikolaos Pyrgidis, Roberto Contieri, Ioana Fugaru, Lazaros Tzelves, Alessandro Uleri, Wilbert Fana Mutomba, Dimitrios Diamantidis, Jean de la Rosette, Maria Pilar Laguna, Jack M. Zuckerman, Philippe E. Spiess, Henry H. Woo, Stavros Gravas and Mauro Gacciadd
Show full author list
remove
Hide full author list
Soc. Int. Urol. J. 2026, 7(2), 24; https://doi.org/10.3390/siuj7020024 - 17 Apr 2026
Abstract
►▼
Show Figures
Background/Objectives: Urology residency training widely varies across countries, and evidence comparing residents’ experiences at an international level is limited. This study reports the results of an international survey of urology residents from different countries worldwide, aiming to characterize training environments, educational exposure,
[...] Read more.
Background/Objectives: Urology residency training widely varies across countries, and evidence comparing residents’ experiences at an international level is limited. This study reports the results of an international survey of urology residents from different countries worldwide, aiming to characterize training environments, educational exposure, and trainee expectations across diverse healthcare systems. Methods: A 39-item online survey was administered to urology residents during the Société Internationale d’Urologie (SIU) Regional Meeting (Florence, November 2024), assessing demographics, training exposure, educational resources, workload, satisfaction, and career perspectives. The results were compared between trainees at different postgraduate years (PGYs) to explore associations for key outcomes. Results: Overall, 208 urology residents from 21 countries completed the survey. Most residents were actively involved in research (76.4%), although confidence in independent scientific production was moderate (significantly lower among junior trainees). Surgical exposure increased with PGY, with good experience in endoscopy but limited hands-on exposure and expected autonomy in laparoscopic, robotic, and major open surgery. Despite high overall satisfaction with urology, residents described heavy workloads, inconsistent access to structured teaching and international fellowships, and a long-term shift in career expectations toward private practice. Conclusions: Urology residents worldwide report high engagement in research, strong satisfaction with their specialty choice, and interest in international mobility. Nonetheless, persistent disparities in surgical exposure, research confidence, workload, and gender representation highlight the need for competency-based curricula, structured mentorship, and improved training organization to promote equitable and high-quality urology education globally.
Full article

Figure 1
Open AccessUrology around the World
Future Prospects for Renal Transplantation in Chad
by
Saleh Abdelkerim Nedjim, Djibrine Mahamat Djibrine, Hissein Hagguir, Adoumadji Kouldjim, Mahamat Hissein Ali, Valentin Vadandi, Mahamat Ali Mahamat, Ibrahim Hamat, Mahamat A. G. Zalba, Abhijit Patil, Laurent Brureau, Arvind Ganpule, Ravindra Sabnis, Rachid Aboutaieb, Rimtebaye Kimassoum and Choua Ouchemi
Soc. Int. Urol. J. 2026, 7(2), 23; https://doi.org/10.3390/siuj7020023 - 16 Apr 2026
Abstract
Chronic kidney disease (CKD) is a condition characterized by the progressive and irreversible loss of renal function, potentially leading to the need for renal replacement therapy, either dialysis or transplantation [...]
Full article
Open AccessInteresting Images
Multilocular Intratesticular Cyst with Testicular Microlithiasis
by
Yoshihiro Ono, Yoshiyuki Miyazawa, Seiji Arai and Yoshitaka Sekine
Soc. Int. Urol. J. 2026, 7(2), 22; https://doi.org/10.3390/siuj7020022 - 14 Apr 2026
Abstract
►▼
Show Figures
An 85-year-old man presented with painless enlargement of the left scrotum [...]
Full article

Figure 1
Open AccessInteresting Images
Dedifferentiated Liposarcoma Mimicking a Bosniak IV Cyst: A Rare Case of Radiographic Mimicry
by
Sepehr Niakani, Hend Alshamsi, Rocio Roldan-Testillano, Simon Gauvin, Jean-François Toupin and Alexis Rompré-Brodeur
Soc. Int. Urol. J. 2026, 7(2), 21; https://doi.org/10.3390/siuj7020021 - 8 Apr 2026
Abstract
►▼
Show Figures
Cystic renal lesions are frequently identified incidentally on imaging and range from benign cysts to malignant tumors [...]
Full article

Figure 1
Open AccessEditorial
Managing the Assault on Our Email Inbox
by
Henry H. Woo
Soc. Int. Urol. J. 2026, 7(1), 20; https://doi.org/10.3390/siuj7010020 - 23 Feb 2026
Abstract
With the new year upon us and with many of us emerging from a short break over the holiday season, it is almost with some dread that we open the inbox of our email accounts [...]
Full article
Open AccessReview
Urological Manifestations of Stevens–Johnson Syndrome/Toxic Epidermal Necrolysis and Their Management: A Scoping Review
by
Zoe Williams, Paul Kim, Ashan David Canagasingham, James Kovacic, Andrew Shepherd, Ankur Dhar and Amanda Shu Jun Chung
Soc. Int. Urol. J. 2026, 7(1), 19; https://doi.org/10.3390/siuj7010019 - 23 Feb 2026
Abstract
►▼
Show Figures
Background/Objectives: Stevens–Johnson Syndrome (SJS) and toxic epidermal necrolysis (TEN) are rare, potentially fatal immunological conditions that affect cutaneous and mucosal surfaces and have the potential to involve the genitourinary tract. While genital involvement is common, urological manifestations are under-recognised clinically and there is
[...] Read more.
Background/Objectives: Stevens–Johnson Syndrome (SJS) and toxic epidermal necrolysis (TEN) are rare, potentially fatal immunological conditions that affect cutaneous and mucosal surfaces and have the potential to involve the genitourinary tract. While genital involvement is common, urological manifestations are under-recognised clinically and there is a paucity of clear, evidence-based management pathways specific to urological manifestations of SJS/TEN. To map the spectrum of urological manifestations of SJS/TEN, to describe the short- and long-term outcomes of these manifestations, and to synthesise management and prevention strategies to inform clinical practice. Methods: This was a scoping review conducted in accordance with the Preferred Reporting Items for Systematic reviews and Meta-Analyses Extension for Scoping Reviews (PRISMA-ScR) guideline. Data sources: Medline and PubMed articles published in English with publication date up to December 2025. Study selection: Eligible studies included case reports, case series, observational studies, clinical guidelines, and review articles describing urological manifestations, outcomes, management, or prevention strategies for patients with SJS/TEN. Articles limited to renal or isolated gynaecological involvement were excluded. Data extraction and synthesis: Articles were screened independently by two reviewers using a pre-defined data extraction template covering four domains: urological manifestations, outcomes and sequelae, management strategies, and prevention strategies. This criterion was refined after a pilot of 20 studies. Discrepancies were resolved by consensus with a third reviewer. Formal risk-of-bias assessment was not performed, consistent with scoping review methodology. Results: One hundred and four studies published between 1987 and 2025 were included in this review. Selected articles included case reports (n = 63), retrospective cohort studies (n = 23), prospective studies (n = 2), guidelines (n = 5), and summary articles (n = 11). Reported urological involvement ranged from genital cutaneous and mucosal disease including erosions, adhesions, and balanitis to urethral manifestations such as urethritis, stenosis, and strictures, as well as scarce upper urinary tract involvement including ureteric stricture and ureteric mucosal sloughing. While some manifestations resolved with supportive care, others progressed to chronic sequelae including persistent urethral strictures, voiding dysfunction, sexual dysfunction, recurrent infection, and in rare cases, obstructive uropathy. A multidisciplinary approach was recommended for all patients with SJS/TEN. Urological management centred around early and repeated urogenital examination, manual lysis of adhesions, urinary catheterisation, and timely intervention for urethral or ureteric obstruction. Long-term urological follow-up of 12 months was recommended for patients with significant urogenital involvement. Conclusions: Urological manifestations of SJS/TEN are diverse, clinically significant, and frequently under-recognised. Early urological involvement, systematic genital and urinary tract assessment, and proactive preventative measures may reduce long-term morbidity. This review provides a comprehensive synthesis of knowledge and recommendations to support urologists’ role in multidisciplinary care of patients with this pathology. This review also highlights the need for prospective research to guide further evidence-based management of urological complications of SJS/TEN.
Full article
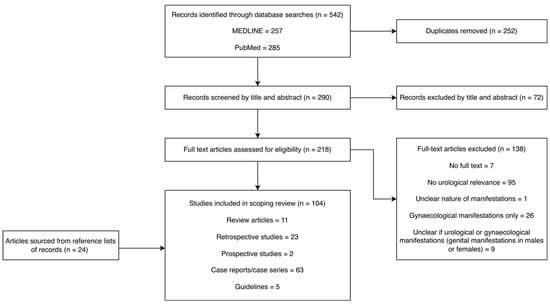
Figure 1
Open AccessComment
A New Light on Bladder Cancer Management: Integrating Laser Ablation into Endourological Care Pathways. Comment on Katz-Summercorn et al. Evolution of the Bladder Cancer Pathway in a Secondary Care Unit Incorporating Transurethral Laser Ablation and ‘Bladder Cancer Surgery Planning Meetings’. Soc. Int. Urol. J. 2026, 7, 17
by
Ashwini Kadam and Gagan Prakash
Soc. Int. Urol. J. 2026, 7(1), 18; https://doi.org/10.3390/siuj7010018 - 23 Feb 2026
Abstract
In this issue, Alexander Charles Katz-Summercorn et al [...]
Full article
Open AccessArticle
Evolution of the Bladder Cancer Pathway in a Secondary Care Unit Incorporating Transurethral Laser Ablation and ‘Bladder Cancer Surgery Planning Meetings’
by
Alexander Katz-Summercorn, Sherif Heba, Stefanos Almpanis and Shiv Kumar Pandian
Soc. Int. Urol. J. 2026, 7(1), 17; https://doi.org/10.3390/siuj7010017 - 23 Feb 2026
Abstract
►▼
Show Figures
Background/Objectives: Transurethral Laser Ablation (TULA) is fast evolving as a surgical procedure, especially for small or recurrent bladder tumours. It offers a safe alternative for patients who are unsuitable for general anaesthetic (GA) or who cannot obtain timely pre-operative assessments for Transurethral
[...] Read more.
Background/Objectives: Transurethral Laser Ablation (TULA) is fast evolving as a surgical procedure, especially for small or recurrent bladder tumours. It offers a safe alternative for patients who are unsuitable for general anaesthetic (GA) or who cannot obtain timely pre-operative assessments for Transurethral Resection of Bladder Tumour (TURBT). Patients are identified for TULA in ‘Bladder Cancer Surgery Planning Meetings’ (BSPMs) and this significantly reduces their cancer waiting time (CWT). Its effectiveness as a diagnostic and therapeutic tool, including its complications and costs, has been assessed. Methods: All TULA procedures performed at the Trust were studied in two cycles. The first between August 2023 and November 2024, prior to initial audit, and then up to September 2025. Case notes, operation notes, and multidisciplinary team (MDT) outcomes were retrospectively reviewed. All procedures were performed with a flexible cystoscope and ‘cold cup’ biopsies with further ablation and haemostasis using a 1470 nm diode laser at 4 watts and 400 µm laser fibre. Patients were identified for TULA based on tumour size, location, and fitness for general anaesthetic. Results: During the study period, 95 TULA procedures were performed with a follow-up period between 4 weeks and 1 year. A total of 86 patients (90.5%) had local anaesthetic (LA) ± intravenous (IV) sedation, with 50% having LA alone in the second phase of the study; of the remaining patients, 8 had GA (8.4%) and 1 (1.1%) had spinal anaesthetic. None of the cases were considered to have missed a significant finding. One case (1.1%) was complicated, with ongoing bleeding requiring bladder washout under GA. BSPMs were introduced in July 2024 and audited in the first phase of this study. A total of 24 (39%) of patients were identified for TULA. Of those, 7 (29%) were originally scheduled for TURBT and were having difficulties obtaining pre-operative assessment (POA) clearance. Cost figures were provided by the hospital’s accountants. Conclusions: TULA has been implemented with a low complication rate and appropriate sampling. In the next phase, TULA will be rolled out to an outpatient setting, performed exclusively under LA. This will lead to a significant cost reduction.
Full article
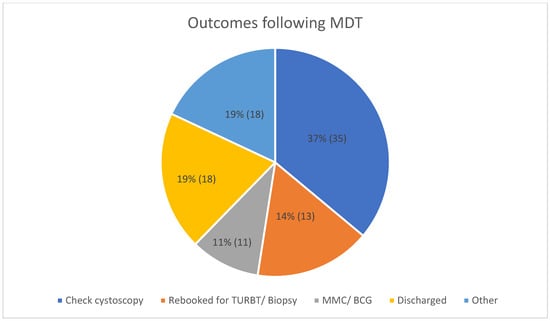
Figure 1
Open AccessArticle
Factors That Increase the Risk of Ureteric Stent Migration: A Retrospective Cohort Analysis
by
Sarah Lorger, Paul Kim, Sean Ong, Stuart Jackson, Sithum Munasinghe, Gaeun Song, Tanya Samtani, Fatmah Alzahraa A. Y. Y. Haider and Matthew Stanowski
Soc. Int. Urol. J. 2026, 7(1), 16; https://doi.org/10.3390/siuj7010016 - 20 Feb 2026
Abstract
Background/Objectives: Ureteric stents are commonly used in urological procedures. However, they can cause pain; haematuria; voiding symptoms; or stent migration. When stent migration occurs, this can cause a significant impact on the patients’ therapeutic outcomes and may warrant a repeat procedure to
[...] Read more.
Background/Objectives: Ureteric stents are commonly used in urological procedures. However, they can cause pain; haematuria; voiding symptoms; or stent migration. When stent migration occurs, this can cause a significant impact on the patients’ therapeutic outcomes and may warrant a repeat procedure to retrieve or replace the ureteric stent. This study aims to assess if there are any patient; stent; or operative factors that may increase the risk of stent migration. Methods: This is a single-institute, retrospective cohort study that looked at patient; stent; and operative factors for 828 ureteroscopies and or laser lithotripsy for management of ureteric or intra-renal calculi over a 2-year period. The 828 procedures comprised 655 patients, as some patients had multiple procedures. Results: From the 828 cases, there was a 2.7% incidence of stent migration; all episodes of stent migration were distal migration. Stent migration was more likely among females (odds ratio (OR) = 3.0; 95% confidence interval (CI) [1.2; 7.1]) compared to males; older aged groups (over 65 years) (OR = 2.7; 95% CI [0.9; 7.8]) compared to the young aged group (16–44 years); and those who were obese (OR = 2.1; 95% CI [0.9; 5.0]), had musculocutaneous (MSK) conditions (OR = 2.7; 95% CI [0.9; 8.3]), neurological conditions (OR = 3.3; 95% CI [1.1; 10.0]), and stent dwelling time ≥ month (OR = 2.3; 95% CI [0.9; 6.0]) compared to <1 month. There was no observed association between stent and operative factors. Conclusions: Patient factors such as sex; age; comorbidities; and weight need to be considered by urologists in conjunction with modifiable stent factors to ensure that the decisions are made on an individual basis to try and reduce the risk of stent migration.
Full article
Open AccessArticle
Prevalence and Predictors of Burnout in Urology Professionals in Pakistan
by
Mudassir Hussain
Soc. Int. Urol. J. 2026, 7(1), 15; https://doi.org/10.3390/siuj7010015 - 18 Feb 2026
Abstract
Background/Objectives: This study aims to assess the prevalence and predictors of burnout among urology professionals in Pakistan using a validated tool and to explore underlying causes through qualitative input. Methods: A cross-sectional survey was conducted among urology trainees, fellows, and consultants across Pakistan.
[...] Read more.
Background/Objectives: This study aims to assess the prevalence and predictors of burnout among urology professionals in Pakistan using a validated tool and to explore underlying causes through qualitative input. Methods: A cross-sectional survey was conducted among urology trainees, fellows, and consultants across Pakistan. Burnout was measured using the Maslach Burnout Inventory–Human Services Survey (MBI-HSS). Burnout was defined using a criterion of high emotional exhaustion or high depersonalization. Descriptive statistics and chi-square tests were used to assess associations. Thematic analysis was applied to open-ended responses. Results: A total of 183 responses were received. When using the high emotional exhaustion (EE) or depersonalization (DP) criterion, 62% was classified as experiencing burnout. Significant predictors included excessive working hours (more than 80 h per week), frequent night calls, avoidance-based coping, workplace favouritism, and discrimination. No association was found with gender, age, or designation. Thematic responses highlighted five common causes of burnout. Conclusions: Burnout is prevalent among urology professionals in Pakistan and is largely driven by modifiable factors. Interventions must target institutional support, work–life balance, and healthier coping mechanisms.
Full article
Open AccessComment
Limiting the Escalation of Medical Cannabis Use. Comment on Hammad et al. Association Between Medical Cannabis Use and Substance Use Disorder in Patients with Dysuria: A Propensity-Score Matched Cohort Study Using Federated Network of Global Real-World Data. Soc. Int. Urol. J. 2026, 7, 13
by
Jonathan G. Tubman
Soc. Int. Urol. J. 2026, 7(1), 14; https://doi.org/10.3390/siuj7010014 - 18 Feb 2026
Abstract
The article by Hammad et al [...]
Full article
Open AccessArticle
Association Between Medical Cannabis Use and Substance Use Disorder in Patients with Dysuria: A Propensity-Score Matched Cohort Study Using Federated Network of Global Real-World Data
by
Muhammed A. M. Hammad, Laith E. Baqain, Mohammed Shahait and Gamal M. Ghoniem
Soc. Int. Urol. J. 2026, 7(1), 13; https://doi.org/10.3390/siuj7010013 - 17 Feb 2026
Abstract
►▼
Show Figures
Background/Objectives: To evaluate whether medical cannabis (MC) use following dysuria diagnosis is associated with increased risk of developing substance use disorder (SUD), given rising cannabis prescriptions for urologic symptoms and concerns about long-term consequences. Methods: We conducted a retrospective cohort study using
[...] Read more.
Background/Objectives: To evaluate whether medical cannabis (MC) use following dysuria diagnosis is associated with increased risk of developing substance use disorder (SUD), given rising cannabis prescriptions for urologic symptoms and concerns about long-term consequences. Methods: We conducted a retrospective cohort study using the TriNetX Research Network, a federated electronic health record database with over 120 million patients. Adult patients newly diagnosed with dysuria between 2003 and 2024 were identified and stratified by subsequent cannabis exposure. MC users were defined by a cannabis-related diagnostic code within 90 days of dysuria diagnosis. Propensity score matching (PSM) was performed 1:1 by age, sex, and race. The primary outcome was a new diagnosis of SUD (cannabis, opioid, or cocaine use disorders) within 12 months. Secondary analysis included Kaplan–Meier (KM) survival estimates over 5 years. Risk ratios (RR), odds ratios (OR), and hazard ratios (HR) were calculated. OR and RR estimated the likelihood of SUD within 12 months, and HR reflected relative hazard over 5 years. Results: After excluding patients with prior SUD, the final sample included 60,544 MC patients and 98,715 general dysuria (GD) patients. The MC group had a significantly higher incidence of new SUD diagnoses (11.13%) than the GD group (2.28%), yielding a risk difference of −8.85% (95% CI: −9.11 to −8.58; p < 0.0001), relative risk 0.205, and OR 0.186. KM analysis showed lower SUD-free survival in MC (80.96%) versus GD (96.35%; log-rank p < 0.0001). MC exposure was associated with nearly fivefold increased odds of SUD within 12 months (OR = 0.186) and sixfold higher hazard over 5 years (HR = 0.163). Conclusions: Medical cannabis use after dysuria is linked to markedly increased risk and earlier onset of SUD. Careful patient selection, counseling, and monitoring are essential when prescribing MC for urologic symptoms.
Full article

Figure 1
Open AccessComment
Large Language Models in Urology, a Cautionary Promise. Comment on Eskandar, K. Assessing ChatGPT Accuracy Across Versions for Patient and Guideline Queries in Sacral Neuromodulation. Soc. Int. Urol. J. 2026, 7, 11
by
Adrian Wagg
Soc. Int. Urol. J. 2026, 7(1), 12; https://doi.org/10.3390/siuj7010012 - 13 Feb 2026
Abstract
Eskandar’s evaluation of ChatGPT across software versions regarding sacral neuromodulation (SNM) is timely and pragmatic [...]
Full article
Highly Accessed Articles
Latest Books
E-Mail Alert
News
Topics






