-
 Healing the Liver: Cell and Gene Therapies for Inherited and Acquired Diseases
Healing the Liver: Cell and Gene Therapies for Inherited and Acquired Diseases -
 The Future of Liver-Targeted Protein Synthesis Inhibition: Current Treatments, Emerging Strategies, and Next-Generation Therapeutics
The Future of Liver-Targeted Protein Synthesis Inhibition: Current Treatments, Emerging Strategies, and Next-Generation Therapeutics -
 Primary Biliary Cholangitis—The Changing Biomarker Paradigms for Staging Fibrosis
Primary Biliary Cholangitis—The Changing Biomarker Paradigms for Staging Fibrosis -
 The Effect of Somatostatin on Mediators of Liver Inflammation and Fibrosis in Viral Cirrhosis
The Effect of Somatostatin on Mediators of Liver Inflammation and Fibrosis in Viral Cirrhosis
Journal Description
Livers
Livers
is an international, peer-reviewed, open access journal on liver science published bimonthly online by MDPI.
- Open Access— free for readers, with article processing charges (APC) paid by authors or their institutions.
- High Visibility: indexed within ESCI (Web of Science), Scopus, EBSCO, and other databases.
- Journal Rank: CiteScore - Q2 (Hepatology)
- Rapid Publication: manuscripts are peer-reviewed and a first decision is provided to authors approximately 27 days after submission; acceptance to publication is undertaken in 6.7 days (median values for papers published in this journal in the second half of 2025).
- Recognition of Reviewers: APC discount vouchers, optional signed peer review, and reviewer names published annually in the journal.
Impact Factor:
2.4 (2024);
5-Year Impact Factor:
2.3 (2024)
Latest Articles
Update on the Potential Use of Natural Triterpenes for the Treatment of Metabolic-Dysfunction-Associated Steatotic Liver Disease (MASLD) and Metabolic-Dysfunction-Associated Steatohepatitis (MASH)
Livers 2026, 6(3), 48; https://doi.org/10.3390/livers6030048 - 2 Jun 2026
Abstract
►
Show Figures
Background/Objectives: Metabolic-dysfunction-associated steatotic liver disease (MASLD) and its progressive inflammatory/fibrotic form, metabolic-dysfunction-associated steatohepatitis (MASH), represent a growing global health burden. This progression is driven by complex mechanisms involving metabolic dysregulation, chronic inflammation, oxidative stress, and progressive fibrosis. To date, effective pharmacological therapies remain
[...] Read more.
Background/Objectives: Metabolic-dysfunction-associated steatotic liver disease (MASLD) and its progressive inflammatory/fibrotic form, metabolic-dysfunction-associated steatohepatitis (MASH), represent a growing global health burden. This progression is driven by complex mechanisms involving metabolic dysregulation, chronic inflammation, oxidative stress, and progressive fibrosis. To date, effective pharmacological therapies remain limited. Pentacyclic triterpenes have attracted increasing attention due to their broad biological activities and ability to modulate multiple molecular pathways implicated in chronic liver disease. This review aims to provide a mechanistic overview of the potential role of pentacyclic triterpenes in MASLD and MASH. Methods: A literature review was conducted using major scientific databases (PubMed and Web of Science) to identify experimental studies investigating pentacyclic triterpenes in metabolic liver diseases. Selected studies were analyzed according to triterpene structural classification, reported bioactivities, molecular targets, and experimental evidence from in vitro and in vivo models of MASLD/MASH or related pathogenic processes. Results: Pentacyclic triterpenes, especially ursolic acid, oleanolic acid, and glycyrrhizin, exhibit hepatoprotective effects including regulation of lipid metabolism, attenuation of oxidative and endoplasmic reticulum stress, suppression of pro-inflammatory signaling, inhibition of inflammasome activation, and reduction in hepatic stellate cell activation and extracellular matrix deposition. These effects involve modulation of signaling pathways, including AMPK, NF-κB, NLRP3, TGF-β, FXR, and MAPK. Preclinical evidence demonstrates improvements in steatosis, inflammation, and fibrosis in experimental models. Conclusions: Pentacyclic triterpenes emerge as multitarget modulators of MASH pathophysiology. However, translating preclinical evidence into well-designed clinical trials is necessary to validate their safety and efficacy in humans.
Full article
Open AccessSystematic Review
Surgical Decision-Making and Clinical Characteristics in Porcelain Gallbladder: A Systematic Review of Case Reports
by
Osvaldo Huchim-Mendez, Ruben R. Lozano-Salazar, Alejandro D. Munive-Ramirez, Jorge E. Mendicuti-Carrillo, Erick Rochel-Perez and Nina Isabel Mendez Dominguez
Livers 2026, 6(3), 47; https://doi.org/10.3390/livers6030047 - 2 Jun 2026
Abstract
Porcelain gallbladder (PGB) has historically been considered a premalignant condition, although recent evidence questions the strength of its association with gallbladder carcinoma. Objective: To describe the occurrence and characteristics of malignancy in patients with porcelain gallbladder, as well as clinical, imaging, and
[...] Read more.
Porcelain gallbladder (PGB) has historically been considered a premalignant condition, although recent evidence questions the strength of its association with gallbladder carcinoma. Objective: To describe the occurrence and characteristics of malignancy in patients with porcelain gallbladder, as well as clinical, imaging, and surgical characteristics reported in clinal cases. Methods: A systematic review of case reports and case series (≤5 patients) was conducted following PRISMA 2020 guidelines. PubMed/MEDLINE, ScienceDirect, and Redalyc from database inception through March 2026. Individual patient data were extracted including demographic characteristics, imaging findings, calcification pattern, surgical management, histopathology, and outcomes. Descriptive statistics were performed. Results: Fifty-four individual cases of porcelain gallbladder were identified. Patients were predominantly female (70.4%), with ages ranging from 6 to 98 years. Complete calcification was reported in 85.2% of cases. Histopathological confirmation was available in 45 cases (83.3%). Thirteen patients had gallbladder carcinoma associated with porcelain gallbladder, corresponding to 28.9% of those with pathological examinations. Incomplete calcification showed higher frequency of malignancy compared with complete calcification. Mortality was reported in three patients (5.6%), all with malignant disease. Conclusions: The proportion of malignancy observed in published case reports reflects a selected dataset and should not be interpreted as an estimate of population risk. These findings provide descriptive insights into clinical presentations and management patterns, supporting hypothesis generation rather than risk estimation.
Full article
(This article belongs to the Special Issue Latest Progress in Hepatobiliary Surgery Research)
►▼
Show Figures

Graphical abstract
Open AccessReview
Human-Mouse Convergence in Metabolic Dysfunction-Associated Steatotic Liver Disease: Mouse Model Selection and Non-Invasive Diagnostic Strategies
by
Denise Bonente, Sara Gargiulo, Ludovica Livi, Matteo Gramanzini, Tiziana Tamborrino, Lisa Gherardini, Giovanni Inzalaco, Lorenzo Franci, Mario Chiariello and Virginia Barone
Livers 2026, 6(3), 46; https://doi.org/10.3390/livers6030046 - 1 Jun 2026
Abstract
►▼
Show Figures
Background: Metabolic Dysfunction-Associated Steatotic Liver Disease (MASLD) is a global health priority affecting approximately 30% of the population. It represents the hepatic manifestation of metabolic syndrome, potentially progressing from simple steatosis to Metabolic Dysfunction-Associated Steatohepatitis (MASH), cirrhosis, and hepatocellular carcinoma. This review aims
[...] Read more.
Background: Metabolic Dysfunction-Associated Steatotic Liver Disease (MASLD) is a global health priority affecting approximately 30% of the population. It represents the hepatic manifestation of metabolic syndrome, potentially progressing from simple steatosis to Metabolic Dysfunction-Associated Steatohepatitis (MASH), cirrhosis, and hepatocellular carcinoma. This review aims to compare current knowledge of MASLD in mouse models and humans, focusing on pathophysiology, histological phenotypes, and the role of preclinical imaging as a non-invasive translational screening tool. Methods: A literature search was conducted in PubMed and Web of Science to identify English-language publications from January 2020 to March 2026 on murine models and imaging techniques for MASLD, using pertinent keywords. Attention was given to highlighting similarities and differences between human and murine approaches. Results: MASLD arises from complex interactions between genetics, sedentary lifestyles, and imbalanced diets. While mouse models have been refined to capture the multifactorial interplay driving disease progression and are still essential for drug development, no single model fully mirrors the human condition. Histological assessment remains an essential tool for MASLD staging, in both humans and mouse models. However, imaging is increasingly emerging as an important complementary technique to non-invasively investigate MASLD. Conclusions: Mouse models are essential to address specific mechanistic and therapeutic questions, but understanding of their limitations and strengths is crucial for translational research. Integrating phenotype-driven approaches in both humans and mice, combining traditional histology, quantitative imaging, and metabolic profiling, as well as longitudinal, combined, and humanized preclinical models, will enhance translational alignment and accelerate the development of therapies for MASLD.
Full article

Figure 1
Open AccessReview
Experimental Rodent Models of Metabolic Dysfunction-Associated Fatty Liver Disease: Present Status and Future Perspective
by
Kamlesh K. Bhopale and Mukund P. Srinivasan
Livers 2026, 6(3), 45; https://doi.org/10.3390/livers6030045 - 26 May 2026
Abstract
Background/Objectives: Metabolic dysfunction-associated fatty liver disease (MAFLD), previously known as non-alcoholic fatty liver disease (NAFLD), is the most prevalent chronic liver disease worldwide, affecting approximately 25% of the global population. MAFLD represents a broad disease spectrum ranging from simple steatosis to metabolic dysfunction-associated
[...] Read more.
Background/Objectives: Metabolic dysfunction-associated fatty liver disease (MAFLD), previously known as non-alcoholic fatty liver disease (NAFLD), is the most prevalent chronic liver disease worldwide, affecting approximately 25% of the global population. MAFLD represents a broad disease spectrum ranging from simple steatosis to metabolic dysfunction-associated steatohepatitis (MASH), fibrosis, cirrhosis, and hepatocellular carcinoma (HCC). The availability of experimental models that faithfully reproduce human metabolic and hepatic pathology is essential for elucidating disease mechanisms and advancing therapeutic development. This review aims to critically evaluate commonly used rodent models of MAFLD and provide guidance for model selection based on specific research objectives. Methods: A narrative, semi-systematic literature search was performed using PubMed Central, Ovid MEDLINE, and Google Scholar. Rodent models were classified according to their mode of disease induction, including diet-induced, genetically engineered, chemically or pharmacologically induced, and combination models. Models were assessed based on frequency of use, relevance to different stages of MAFLD progression, metabolic fidelity, and suitability for mechanistic studies and preclinical therapeutic evaluation. Results: Diet-induced models incorporating high fat, fructose, and cholesterol most closely recapitulate human metabolic dysfunction and are highly relevant for translational research and drug screening. Nutrient-deficient diets induce rapid steatohepatitis and fibrosis but lack key features of metabolic syndrome. Genetic models enable the targeted interrogation of specific metabolic and inflammatory pathways, whereas chemical and combination models accelerate fibrosis and HCC development. No single rodent model fully reproduces the entire spectrum of human MAFLD. Conclusions: Rodent models remain indispensable tools for MAFLD research; however, their applicability depends on alignment with the defined experimental goals. Careful selection of models based on disease stage, dominant pathogenic mechanisms, and translational intent is essential for improving reproducibility and clinical relevance. This review provides a practical framework to guide investigators in choosing appropriate preclinical models for mechanistic studies and therapeutic development in MAFLD.
Full article
(This article belongs to the Special Issue From Population to Precision: Nutritional Approaches in Metabolic Dysfunction-Associated Steatotic Liver Disease)
►▼
Show Figures

Figure 1
Open AccessReview
Coexistent Hepatitis B Virus and Metabolic Dysfunction-Associated Steatotic Liver Disease Under the New Definition: A New Era for Established Diseases
by
Ahmed Tawheed, Abdulla A. Mahmoud, Hussein Hassan Aly and Mohamed El-Kassas
Livers 2026, 6(3), 44; https://doi.org/10.3390/livers6030044 - 21 May 2026
Abstract
Dysfunction-associated steatotic liver disease (MASLD) is a newly introduced term for the condition previously known as nonalcoholic fatty liver disease (NAFLD). MASLD affects 38% of the global population and is now diagnosed based on the presence of steatosis but also with cardiometabolic risk
[...] Read more.
Dysfunction-associated steatotic liver disease (MASLD) is a newly introduced term for the condition previously known as nonalcoholic fatty liver disease (NAFLD). MASLD affects 38% of the global population and is now diagnosed based on the presence of steatosis but also with cardiometabolic risk factors indicating metabolic dysfunction. Chronic hepatitis B (CHB), another significant public health issue, impacts over 296 million people worldwide, or approximately 3.2% of the global population. Studies have consistently reported a complex relationship between MASLD and CHB. Previous studies indicate that MASLD may protect against high viral loads, while other studies indicate that coexisting MASLD and CHB may lead to more advanced fibrosis and an elevated risk of HCC. Additionally, numerous studies highlight a strong association between CHB and metabolic syndrome components. This review article examines the relationship between CHB and MASLD, considering what has been previously published.
Full article
(This article belongs to the Special Issue The Surveillance, Prevention, and Treatment of Viral Hepatitis: Looking Forward to Global Elimination)
►▼
Show Figures

Figure 1
Open AccessReview
Clinical Presentation and Therapeutic Approach of Hepatic Sarcoidosis
by
Vittoria Benintende, Luca Bettazzoni, Nicola Reggidori, Chiara Ambrosi, Monica Patrignani and Luca Ielasi
Livers 2026, 6(3), 43; https://doi.org/10.3390/livers6030043 - 18 May 2026
Abstract
►▼
Show Figures
Sarcoidosis is a multisystemic inflammatory disease defined by non-caseating granuloma formation in involved organs. The liver is the third most implicated organ after the lungs and lymph nodes. Due to its frequently asymptomatic presentation, the true prevalence of hepatic sarcoidosis may be understated.
[...] Read more.
Sarcoidosis is a multisystemic inflammatory disease defined by non-caseating granuloma formation in involved organs. The liver is the third most implicated organ after the lungs and lymph nodes. Due to its frequently asymptomatic presentation, the true prevalence of hepatic sarcoidosis may be understated. Increased levels of alkaline phosphatase and gamma-glutamyl transferase are the most frequent biochemical abnormalities. The liver biopsy is still the gold standard and reveals non-caseating granulomas in almost all cases. The use of corticosteroids and ursodeoxycholic acid results in a significant decrease in biochemical parameters. However, the clinical course of hepatic sarcoidosis is diverse and requires individualized management strategies, especially to prevent hepatic complications. This review aims to synthesize the current evidence on epidemiology, pathogenesis, diagnostic approaches, and therapeutic strategies for this disease.
Full article

Figure 1
Open AccessArticle
Renal Trajectory of Eligible Simultaneous Liver–Kidney Transplant Recipients
by
Manuj Mayank Shah, Sarah Hussain, Binuri Hapuarachchy, Reed Towle Jenkins, David J. Farhat, Heather McDade, Al-Faraaz Kassam, Elizabeth A. King, Russell Wesson, Sharon Weeks, Andrew M. Cameron, Allan B. Massie, Dorry L. Segev, Ahmet Gurakar and Benjamin Philosophe
Livers 2026, 6(3), 42; https://doi.org/10.3390/livers6030042 - 13 May 2026
Abstract
►▼
Show Figures
Purpose: Simultaneous liver–kidney transplantation (SLK) eligible candidates may receive SLK or liver-alone transplant (LA) with access to kidney transplant after initial LA (KAL). We aimed to characterize SLK-eligible recipient outcomes according to treatment approach. Methods: This study utilized 2017–2023 SRTR data
[...] Read more.
Purpose: Simultaneous liver–kidney transplantation (SLK) eligible candidates may receive SLK or liver-alone transplant (LA) with access to kidney transplant after initial LA (KAL). We aimed to characterize SLK-eligible recipient outcomes according to treatment approach. Methods: This study utilized 2017–2023 SRTR data to identify SLK-eligible deceased donor liver transplants. Recipients were placed into two groups based on whether SLK was performed; non-SLK patients were sub-stratified into LA and KAL cohorts. After baseline comparisons, 2-year patient and graft survival outcomes were characterized by univariable and multivariable Cox proportional hazard regression and Kaplan–Meier analysis. Results: Among 4879 candidates identified, 3746 (76.8%) underwent SLK, 1023 (21.0%) LA, and 110 (2.3%) KAL. SLK recipients maintained the highest eGFRs at 6 months, 1 year, and 2 years post-transplant (p < 0.01). Compared to SLK recipients, non-SLK recipients had a higher 2-year risk of mortality (aHR 2.46, p < 0.01), all-cause events (aHR 1.91, p < 0.01), and liver graft failure (HR 1.55, p = 0.02). LA conferred a higher 2-year mortality risk (aHR 2.98, p < 0.01) and all-cause event risk (aHR 2.25, p < 0.01), while KAL had comparable mortality risk to SLK (aHR 0.43, p = 0.40). Conclusions: When SLK-eligible candidates undergo transplants, SLK remains the optimal path forward, even when a safety net kidney can be performed.
Full article

Graphical abstract
Open AccessArticle
The MRI Signature of Neuroendocrine Liver Metastases: Toward a Radiologic Identikit
by
Alessandro Serafini, Clara Gaetani, Laura Bergamasco, Stefano Cirillo, Teresa Gallo, Marco Gatti, Paolo Fonio and Riccardo Faletti
Livers 2026, 6(3), 41; https://doi.org/10.3390/livers6030041 - 12 May 2026
Abstract
Background: Neuroendocrine neoplasms are frequently diagnosed after the detection of liver metastases, often when the primary tumor remains occult. Accurate non-invasive differentiation of neuroendocrine liver metastases (NELMs) from other focal hepatic lesions is therefore crucial. This study aimed to characterize the magnetic resonance
[...] Read more.
Background: Neuroendocrine neoplasms are frequently diagnosed after the detection of liver metastases, often when the primary tumor remains occult. Accurate non-invasive differentiation of neuroendocrine liver metastases (NELMs) from other focal hepatic lesions is therefore crucial. This study aimed to characterize the magnetic resonance imaging (MRI) features of NELMs using hepatocyte-specific contrast agents and to identify a potential radiologic “signature” that may suggest a neuroendocrine origin. Methods: This retrospective study included three cohorts: patients with histologically confirmed NELMs (n = 51; 146 lesions), patients with colorectal cancer liver metastases (n = 18; 46 lesions), and patients with benign hepatic hemangiomas (n = 28; 51 lesions). All subjects underwent standardized liver MRI with Gd-EOB-DTPA. Lesions were evaluated for size, diffusion-weighted imaging characteristics, apparent diffusion coefficient values, arterial-phase enhancement, T2-weighted signal, hepatobiliary-phase appearance, and hemorrhagic components. Statistical analyses included univariate and multivariate testing and receiver operating characteristic curve analysis. Results: NELMs commonly demonstrated arterial hyperenhancement, diffusion restriction, and variable T2 and hepatobiliary-phase signal heterogeneity. Compared with colorectal metastases and hemangiomas, NELMs showed distinctive patterns, particularly higher rates of hepatobiliary-phase heterogeneity and arterial enhancement. Lesion size, ADC metrics, T2 heterogeneity, and hemorrhage were significant discriminators. Conclusions: Hepatocyte-specific MRI enables identification of characteristic imaging features of NELMs. An integrated assessment of morphologic, diffusion, and hepatobiliary-phase findings may facilitate early recognition of neuroendocrine metastases, even when the primary tumor is unknown, improving diagnostic confidence and clinical management.
Full article
(This article belongs to the Topic Advances in Gastrointestinal and Liver Disease: From Physiological Mechanisms to Clinical Practice, 2nd Edition)
►▼
Show Figures

Figure 1
Open AccessArticle
Are CD4+ T-Cell Counts Associated with Pneumocystis jirovecii Detection in Hospitalized Patients with Liver Disease? A Retrospective Exploratory Pilot Analysis
by
Antonios Katsounas, Amer Nashtar, Jasmin Weninger, Michael Steckstor, Despoina Koulenti, Joshua D. Nosanchuk, Mustafa Özcürümez, Ali Canbay and Peter M. Rath
Livers 2026, 6(3), 40; https://doi.org/10.3390/livers6030040 - 9 May 2026
Abstract
►▼
Show Figures
Background: Advanced cirrhosis induces profound CD4+ T-cell depletion through splenic sequestration and immune dysregulation. Pneumocystis jirovecii pneumonia risk thresholds remain undefined in non-HIV immunocompromised populations, necessitating investigation in cirrhotic patients. Objectives: To investigate the potential association between peripheral CD4+ T-cell counts
[...] Read more.
Background: Advanced cirrhosis induces profound CD4+ T-cell depletion through splenic sequestration and immune dysregulation. Pneumocystis jirovecii pneumonia risk thresholds remain undefined in non-HIV immunocompromised populations, necessitating investigation in cirrhotic patients. Objectives: To investigate the potential association between peripheral CD4+ T-cell counts and opportunistic infections (OI)—specifically Pneumocystis jirovecii (PJ)—in hospitalized patients with liver disease, and to characterize clinical outcomes across immunological risk strata. Methods: We retrospectively analyzed 455 adults hospitalized in a single institution with hepatic disorders. CD4+ T-cell counts were available in 227/455 patients. Among these, 22 patients met predefined immunological risk criteria (CD4+ < 500/µL and/or HIV positivity) and were classified into three immunological risk clusters (IRCs): IRC-A (HIV−, CD4+ < 200/µL; n = 9), IRC-B (HIV+, CD4+ < 200/µL; n = 7), and IRC-C (HIV−, CD4+ 200–499/µL; n = 6). PJ PCR testing was evaluated when available. Results: Among 455 patients, in-hospital mortality was 103/455 (22.6%). Of the 22 immunologically at risk patients, 15/22 had cirrhosis. PJ PCR was performed in 8/22 patients (IRC-A: 2; IRC-B: 4; IRC-C: 2), with 3/8 positive (37.5%): IRC-A (1/2), IRC-B (1/4), IRC-C (1/2). Ct values ranged from 27.0 to 31.7. Two PJ-PCR–positive cirrhotic patients (IRC-A: n = 1; IRC-C: n = 1) survived without specific anti-PJ therapy; one HIV-positive patient (IRC-B) received trimethoprim-sulfamethoxazole and survived. In-hospital mortality was 5/9 (55.6%) in IRC-A, 2/7 (28.6%) in IRC-B, and 3/6 (50.0%) in IRC-C; none of the deaths were attributable to PJ pneumonia. Conclusions: Severe CD4+ T-cell depletion (<200/µL) was common among cirrhotic patients and associated with PJ detection (3/8 tested), but not with PJ-related mortality (0/3). Mortality was primarily driven by hepatic decompensation and bacterial infections. CD4+ assessment may improve risk stratification in cirrhosis; however, prospective, multicenter studies are warranted to validate these findings and to evaluate CD4-guided strategies for the prevention of opportunistic infections.
Full article

Figure 1
Open AccessReview
The p53/Mdm2 Pathway in Hepatocellular Carcinoma: From Molecular Pathogenesis to Targeted Therapies
by
Keara Kirkness and Derek A. Mann
Livers 2026, 6(3), 39; https://doi.org/10.3390/livers6030039 - 9 May 2026
Abstract
Hepatocellular carcinoma (HCC) is the most common type of liver cancer, and accounts for over 800,000 deaths worldwide, making it a major global health concern. Unfortunately, despite major advances in systemic treatments, such as the introduction of atezolizumab and bevacizumab, patient objective response
[...] Read more.
Hepatocellular carcinoma (HCC) is the most common type of liver cancer, and accounts for over 800,000 deaths worldwide, making it a major global health concern. Unfortunately, despite major advances in systemic treatments, such as the introduction of atezolizumab and bevacizumab, patient objective response rates fall below 30%. HCC most commonly develops against a background of chronic liver disease and cirrhosis, although single gene mutations can also drive HCC development, progression, and metastasis. Around 25% of HCC patient tumours carry mutations in TP53, the gene encoding the tumour-suppressor protein p53. p53 is a central regulator of genomic stability, cell-cycle arrest, apoptosis, senescence, and metabolic homeostasis, and its dysfunction is a frequent event in hepatocarcinogenesis. Accumulating evidence highlights the critical role of p53 in liver fibrosis, inflammation, and shaping of the HCC tumour microenvironment (TME). This review summarizes the role of p53 and its negative regulators Mdm2 and MdmX in HCC development and progression, with an emphasis on how p53 shapes the TME in favour of tumour progression. We also evaluate current and emerging p53-targeted therapeutic strategies, including Mdm2/MdmX inhibitors, mutant p53 reactivators, and rational combinations with immunotherapies. Finally, we discuss major challenges in translating p53-based therapies to the clinic, such as tumour heterogeneity, underlying liver dysfunction, and the development of therapeutic resistance. A deeper understanding of p53 biology in chronic liver disease may unlock new avenues for effective HCC prevention and treatment.
Full article
(This article belongs to the Special Issue Liver Cancer Heterogeneity in the Era of Single-Cell and Spatial Multiomics)
►▼
Show Figures

Figure 1
Open AccessArticle
Bioinformatics Analysis of the Spinal Cord Injured Plasma Proteome: A Focus on the Liver
by
Morgan Godwin, Sharon J. Brown, Gabriel Mateus Bernardo Harrington, Srinivasa C. Budithi, John S. Riddell, Charlotte H. Hulme and Karina T. Wright
Livers 2026, 6(3), 38; https://doi.org/10.3390/livers6030038 - 8 May 2026
Abstract
►▼
Show Figures
Background: Emerging evidence indicates that the liver plays a key role in spinal cord injury (SCI) pathophysiology. Method: This study reanalysed published proteomic datasets from rat models and patients with SCI using bioinformatics and literature/database searches. The aim was to identify liver-specific molecular
[...] Read more.
Background: Emerging evidence indicates that the liver plays a key role in spinal cord injury (SCI) pathophysiology. Method: This study reanalysed published proteomic datasets from rat models and patients with SCI using bioinformatics and literature/database searches. The aim was to identify liver-specific molecular signatures in SCI blood samples and to link these to severity and neurological recovery at various time points (acute/sub-acute and chronic). Results: Across species, a high proportion of injury severity and neurological recovery-associated proteins were linked to liver function. Notably, non-improvers exhibited prolonged sub-acute proinflammatory responses. These changes were not restricted to classical acute-phase reactants but reflected coordinated alterations in hepatic metabolic and synthetic pathways. Pathway analysis consistently highlighted Liver X Receptor /Retinoic X Receptor (LXR/RXR), complement system/cascade and DHCR24 signalling pathways, with predicted directional changes linked to recovery status. Several proteins were identified and categorised as markers of liver dysfunction, metabolic function, complement/coagulation factors and/or acute-phase proteins. Alpha-2-HS-glycoprotein (AHSG) and afamin (AFM) were commonly dysregulated across species datasets, suggesting conserved roles in inflammation and lipid metabolism. Further associations with liver pathologies such as fibrosis and cirrhosis, particularly in non-improvers, were identified. Conclusion This work builds on emerging evidence of hepatic involvement in SCI by providing cross-species, time-resolved proteomic support for altered liver-associated protein output following injury. Together, these findings underscore the central role of hepatic responses in SCI, highlighting liver-associated proteins and pathways as candidate biomarkers that may aid in stratifying recovery trajectories and informing clinical prognostication.
Full article

Figure 1
Open AccessReview
The Liver in Pediatric Rheumatology: A Comprehensive Review
by
Mehul Jariwala, Tristan Kerr and Mohit Kehar
Livers 2026, 6(3), 37; https://doi.org/10.3390/livers6030037 - 8 May 2026
Abstract
►▼
Show Figures
Liver involvement in pediatric rheumatologic diseases is an increasingly recognized but often underappreciated clinical issue. Systemic autoimmune and autoinflammatory disorders including juvenile idiopathic arthritis, systemic lupus erythematosus, juvenile dermatomyositis, systemic vasculitis, and mixed connective tissue disease can all affect hepatic structure and function.
[...] Read more.
Liver involvement in pediatric rheumatologic diseases is an increasingly recognized but often underappreciated clinical issue. Systemic autoimmune and autoinflammatory disorders including juvenile idiopathic arthritis, systemic lupus erythematosus, juvenile dermatomyositis, systemic vasculitis, and mixed connective tissue disease can all affect hepatic structure and function. The mechanisms of injury are multifactorial, encompassing immune-mediated inflammation, macrophage activation, drug-induced toxicity, and metabolic alterations. Hepatic manifestations range from asymptomatic transaminase elevations to fulminant liver failure, frequently influenced by immunosuppressive therapy and comorbid infections. Early recognition through routine biochemical monitoring, imaging, and targeted autoantibody testing is essential for differentiating primary disease activity from treatment-related injury. Timely, multidisciplinary management involving pediatric rheumatology and hepatology teams can prevent progression to chronic liver disease and optimize outcomes. This review summarizes the current understanding of hepatic pathology in pediatric rheumatology, highlighting diagnostic algorithms, monitoring strategies, and emerging therapeutic considerations.
Full article

Graphical abstract
Open AccessReview
Regenerative and Hepatotropic Properties of GLP-1 and GLP-2: Mechanistic Insights and Implications for Post-Hepatectomy Liver Regeneration: A Narrative Review
by
Ahmad Mahamid, Aasem Abu Shtaya, Saif Abu Mouch, Riad Haddad, Abdel-Rauf Zeina and Fadi Abu Baker
Livers 2026, 6(3), 36; https://doi.org/10.3390/livers6030036 - 8 May 2026
Abstract
►▼
Show Figures
Background: Liver regeneration after hepatectomy is critical for recovery, yet post-hepatectomy liver failure (PHLF) remains a significant challenge. While GLP-1 RAs have shown metabolic and hepatic benefits in conditions like metabolic dysfunction–associated steatotic liver disease, and GLP-2 is known for intestinotrophic properties, their
[...] Read more.
Background: Liver regeneration after hepatectomy is critical for recovery, yet post-hepatectomy liver failure (PHLF) remains a significant challenge. While GLP-1 RAs have shown metabolic and hepatic benefits in conditions like metabolic dysfunction–associated steatotic liver disease, and GLP-2 is known for intestinotrophic properties, their specific roles in PHLF are not well-defined. This narrative review aims to examine the roles of Glucagon-like peptide-1 receptor agonists (GLP-1 RAs) and Glucagon-like peptide-2 (GLP-2) in liver regeneration following partial hepatectomy. Methods: A narrative review was conducted, involving a structured appraisal of preclinical, translational, and clinical studies. Relevant literature was identified through comprehensive searches of PubMed and EMBASE databases, limited to English-language publications available up to 1 May 2025. Results: GLP-1 RAs demonstrate therapeutic potential in chronic metabolic liver diseases, but their role in acute hepatic regeneration appears unfavorable, with animal models showing attenuated regenerative responses and impaired liver mass restoration. Conversely, preclinical studies indicate that GLP-2 administration enhances liver regeneration, and human data reveal increased circulating GLP-2 levels post-resection, particularly in PHLF patients, showing dynamics inverse to GLP-1. Conclusions: GLP-1 RAs appear to inhibit acute hepatic regeneration following hepatectomy, while GLP-2 exhibits pro-regenerative activity in preclinical models and favorable dynamics in humans post-resection.
Full article

Figure 1
Open AccessReview
Advances in Diagnostic and Therapeutic Strategies for Metabolic Dysfunction-Associated Steatotic Liver Disease
by
Ryan Njeim, Omar Abureesh, Ali Sohail, Ryan Tam and Liliane Deeb
Livers 2026, 6(3), 35; https://doi.org/10.3390/livers6030035 - 6 May 2026
Abstract
The recent redefinition of steatotic liver diseases, introducing metabolic dysfunction-associated steatotic liver disease (MASLD) and metabolic dysfunction-associated steatohepatitis (MASH), reflects a growing consensus among liver societies and marks a paradigm shift in disease classification. MASLD subsumes former categories of nonalcoholic fatty liver disease
[...] Read more.
The recent redefinition of steatotic liver diseases, introducing metabolic dysfunction-associated steatotic liver disease (MASLD) and metabolic dysfunction-associated steatohepatitis (MASH), reflects a growing consensus among liver societies and marks a paradigm shift in disease classification. MASLD subsumes former categories of nonalcoholic fatty liver disease (NAFLD) and incorporates metabolic criteria alongside moderate alcohol intake, while MASH replaces nonalcoholic steatohepatitis (NASH), aligning terminology with disease mechanisms. This evolution clarifies the diagnostic criteria and minimizes stigma, facilitating more consistent epidemiological and clinical investigations. Recent advances in noninvasive diagnostics, including vibration-controlled transient elastography, magnetic resonance elastography, shear-wave elastography, and the Enhanced Liver Fibrosis test, have improved the identification and stratification of patients with advanced fibrosis. Current guidelines recommend targeted screening in populations at elevated metabolic risk, enabling earlier intervention and personalized management. Population studies indicate that MASLD affects over one-third of adults and is a major contributor to cardiovascular and metabolic morbidity. Therapeutic progress is highlighted by the approval of novel agents such as resmetirom and semaglutide for the treatment of MASH with fibrosis. Emerging dual and triple agonists, as well as sodium–glucose cotransporter inhibitors, offer additional promise, although further research is required to define their long-term efficacy and safety. As the disease prevalence escalates globally, the integration of multidisciplinary care, the ongoing refinement of diagnostic tools, and the expansion of therapeutic options will remain essential to optimizing outcomes for affected individuals.
Full article
(This article belongs to the Special Issue Recent Advances in the Detection and Pathophysiology of Steatotic, Alcoholic and Drug-Induced Liver Diseases)
►▼
Show Figures

Figure 1
Open AccessReview
Impact of Traditional Cigarette Smoking on Liver Structure and Function
by
Ivana Jukic, Ivona Matulic, Tina Becic, Mislav Radic, Josipa Radic, Damir Fabijanic and Jonatan Vukovic
Livers 2026, 6(3), 34; https://doi.org/10.3390/livers6030034 - 24 Apr 2026
Abstract
►▼
Show Figures
Background: Cigarette smoking exposes the human body to a complex mixture of toxic and carcinogenic compounds that can exert widespread biological effects across different organ systems. From addictive responses and consequence maladaptive neuroendocrine responses, cigarette smoke delivers a variety of reactive oxygen species,
[...] Read more.
Background: Cigarette smoking exposes the human body to a complex mixture of toxic and carcinogenic compounds that can exert widespread biological effects across different organ systems. From addictive responses and consequence maladaptive neuroendocrine responses, cigarette smoke delivers a variety of reactive oxygen species, polycyclic aromatic hydrocarbons, nitrosamines, and heavy metals that collectively contribute to oxidative stress, inflammation, endothelial dysfunction, and metabolic disruption. The liver, as the primary organ responsible for xenobiotic metabolism, plays a central role in processing these harmful substances and is therefore uniquely susceptible to their effects. This narrative review will aim to provide an overview of the current evidence of cigarette smoking effects on hepatic structure and function and discuss clinical implications. Methods: This narrative review synthesizes evidence from in vitro studies, animal models, and human clinical research examining the effects of cigarette smoking on liver biology. Mechanistic pathways of injury, metabolic and vascular alterations, and clinical consequences for liver disease were considered. Results: Smoking influences hepatic function both directly—through biotransformation pathways generating reactive intermediates—and indirectly via vascular impairment, immune modulation, hormonal alterations, and changes in lipid and glucose metabolism. Emerging evidence indicates that cigarette smoking contributes to hepatic steatosis, accelerates fibrosis progression, worsens outcomes in viral and alcohol-related liver disease, and increases the risk of hepatocellular carcinoma. Conclusions: Cigarette smoking exerts multifaceted deleterious effects on the liver. Recognition of smoking as a modifiable risk factor for liver-related morbidity underscores the importance of smoking cessation in patients with or at risk for liver disease and highlights implications for research and clinical practice.
Full article

Graphical abstract
Open AccessArticle
Fibrosis-4 Index Predicts Long-Term Outcomes After Sustained Virologic Response in Hepatitis C Virus Patients with Cirrhosis
by
Husam Mikati, Anas Aljabi, Reena Cherian, Shawn Lewis, Leah Blatzer, Tamoore Arshad, Matthew Ambrosio and Richard K. Sterling
Livers 2026, 6(2), 33; https://doi.org/10.3390/livers6020033 - 20 Apr 2026
Abstract
►▼
Show Figures
Background: Direct-acting antivirals (DAAs) achieve high sustained virologic response (SVR) in hepatitis C virus (HCV) patients with cirrhosis, yet the risk of hepatic decompensation or hepatocellular carcinoma (HCC) persists. Fibrosis-4 (FIB-4), a pre-treatment index that predicts advanced fibrosis, is linked to HCC risk
[...] Read more.
Background: Direct-acting antivirals (DAAs) achieve high sustained virologic response (SVR) in hepatitis C virus (HCV) patients with cirrhosis, yet the risk of hepatic decompensation or hepatocellular carcinoma (HCC) persists. Fibrosis-4 (FIB-4), a pre-treatment index that predicts advanced fibrosis, is linked to HCC risk post SVR. We compared post-SVR outcomes and care engagement, and determined the optimal pre-treatment FIB-4 index to predict the risk of HCC or decompensation in HCV patients with cirrhosis treated at the Department of Corrections (DOC) and non-DOC clinics. Methods: HCV patients with cirrhosis treated with DAAs since 2014 in the HCV Treatment Registry were included. Cirrhosis was defined by elastography, imaging, or clinical criteria. Patients with prior decompensation or HCC were excluded. Outcomes (HCC, decompensation) were collected from records. The FIB-4 index was compared between DOC and non-DOC groups. Results: Among 2104 cirrhotic patients (mean age 54; 76% male), 53% were treated in DOC via telemedicine and 47% in non-DOC clinics. HCC developed in 4.8% and decompensation in 8.1%. DOC patients had lower FIB-4 scores and SVR, partly from higher loss to follow-up (9% vs. 1%). Of 1581 with follow-up, surveillance was more common in non-DOC, which also had higher HCC and decompensation. A higher baseline FIB-4 index independently predicted HCC and decompensation (cutoffs: 3.24, 3.7; AUROC 0.79, 0.75, respectively). Conclusions: Despite SVR, cirrhotic patients—especially with a high FIB-4 index—remain at risk for HCC and decompensation. Outcomes differ by care setting, highlighting the need for continued AASLD-recommended surveillance post-SVR.
Full article

Graphical abstract
Open AccessReview
Beyond the Liver: A Systematic Symptom-Based Approach to Extrahepatic Manifestations in Autoimmune Hepatitis
by
Dante Pio Pallotta, Francesco Tovoli, Elisa Barbaro, Andrea De Sinno, Matteo Cappelli Aimone Chiorat, Ernestina Santangeli and Fabio Piscaglia
Livers 2026, 6(2), 32; https://doi.org/10.3390/livers6020032 - 17 Apr 2026
Abstract
►▼
Show Figures
Autoimmune hepatitis (AIH) has long been regarded as an organ-specific disorder. However, increasing evidence supports its systemic nature, with extrahepatic manifestations representing key aspects of clinical management. These manifestations can affect musculoskeletal, gastrointestinal, haematologic, and other systems. They also reflect the complex interplay
[...] Read more.
Autoimmune hepatitis (AIH) has long been regarded as an organ-specific disorder. However, increasing evidence supports its systemic nature, with extrahepatic manifestations representing key aspects of clinical management. These manifestations can affect musculoskeletal, gastrointestinal, haematologic, and other systems. They also reflect the complex interplay between systemic inflammation, concomitant autoimmune diseases, and drug-related toxicity. A careful evaluation is therefore essential to distinguish between these scenarios, especially for symptoms like fatigue and cytopenias. This narrative review provides a comprehensive, symptom-based overview of extrahepatic clinical and laboratory findings in AIH. By integrating current evidence with practical diagnostic considerations, it aims to offer clinicians a patient-centred and clinically relevant framework for navigating the multifaceted systemic landscape of AIH.
Full article

Figure 1
Open AccessReview
Lessons Learned from Our First Concurrent Liver Transplant with Off-Pump Coronary Artery Bypass Surgery: Five Critical Key Factors
by
Srikiran Ramarapu, Marcos Gomes, Shinobu Itagaki, Matthew Quinn Benson and Braydon Rucker
Livers 2026, 6(2), 31; https://doi.org/10.3390/livers6020031 - 16 Apr 2026
Abstract
Liver transplantation (LT) is the definitive treatment for patients with end-stage liver disease. Since its inception in the 1960s, transplant medicine has undergone substantial advances in surgical technique, immunosuppression, organ preservation, and organ allocation policies. According to the 2023 WHO census, approximately 47,180
[...] Read more.
Liver transplantation (LT) is the definitive treatment for patients with end-stage liver disease. Since its inception in the 1960s, transplant medicine has undergone substantial advances in surgical technique, immunosuppression, organ preservation, and organ allocation policies. According to the 2023 WHO census, approximately 47,180 LT procedures occur worldwide each year, with living donors contributing to up to 23% of cases. Additional milestones include the expansion of transplant eligibility to patients with hilar cholangiocarcinoma and advanced colorectal liver metastasis, the incorporation of viscoelastic testing into perioperative blood management algorithms, and the increasing use of mechanical circulatory support for pre-transplant optimization. In parallel, medical training has evolved to meet the complexities associated with these high-risk procedures. Structured fellowship programs now provide focused expertise, and guide investigations to resolve complex clinical dilemmas. Experience accumulated over decades has improved clinicians’ ability to manage the expanding spectrum of comorbidities seen in contemporary transplant candidates. Key perioperative challenges include accurate assessment of fluid status, optimization of intravascular volume, management of vasoplegia, intraoperative renal replacement therapy, treatment of right-ventricular failure, and the mitigation of severe lactic acidosis. As transplant recipients increasingly present at older ages and with multiple comorbidities, perioperative management has become more demanding. One emerging strategy for select high-risk patients involves performing concurrent surgical procedures within a single operative session. This narrative review focuses on the intraoperative management of five variables that proved challenging during the first case of concurrent liver transplantation and off-pump coronary artery bypass surgery in our institution.
Full article
(This article belongs to the Special Issue Transforming Liver Transplantation: Breakthroughs and Boundaries)
►▼
Show Figures

Graphical abstract
Open AccessArticle
Predictors of Cirrhosis and Cholangiocarcinoma in Patients with Primary Sclerosing Cholangitis: An Academic Center Experience
by
Ahmad Hassan Ali, Alhareth Al-Juboori, Deepthi S. Rao, Jamal A. Ibdah, Nanda Deepa Thimmappa, Ayman H. Gaballah and Ghassan M. Hammoud
Livers 2026, 6(2), 30; https://doi.org/10.3390/livers6020030 - 15 Apr 2026
Abstract
►▼
Show Figures
Background and goals: The outcomes of patients with primary sclerosing cholangitis (PSC) in central Missouri are unknown. The University of Missouri–Columbia services 600,000 individuals in central Missouri. Our aims were (a) to examine the outcomes of PSC patients receiving care at our academic
[...] Read more.
Background and goals: The outcomes of patients with primary sclerosing cholangitis (PSC) in central Missouri are unknown. The University of Missouri–Columbia services 600,000 individuals in central Missouri. Our aims were (a) to examine the outcomes of PSC patients receiving care at our academic institution, and (b) to identify the predictors of PSC-related serious adverse events. Methods: A retrospective study of patients with PSC in a non-transplant center. The primary outcome was the development of ≥1 of PSC-related serious adverse event for (1) progression to cirrhosis, or (2) development of cholangiocarcinoma. Results: From 2000 to 2018, 42 patients fulfilled the criteria for the diagnosis of PSC. A total of 55% of the patients were male, and 79% had associated inflammatory bowel disease (IBD). The median follow-up from time of diagnosis of PSC until the last follow-up or death was 5.5 years. A total of 57% of the patients developed ≥ 1 PSC-related adverse event; 36% (8/22) of those who progressed to decompensation underwent liver transplantation. The median time from diagnosis of PSC until progression to decompensation was 6.3 years; the median time from decompensation to transplantation was 10.8 years. A total of 12% of the patients developed ≥ 1 cancer (cholangiocarcinoma = 2; gallbladder cancer = 2; colon cancer = 1; and hepatocellular carcinoma = 1). The overall mortality was 9.5%. The median time from PSC diagnosis until death was 10.2 years. A Cox hazards regression analysis showed only age (HR = 1.16; p = 0.032; 95% CI, 1.01–1.13) and serum bilirubin (HR = 1.42; p = 0.036; 95% CI, 1.03–2.69) at the time of PSC diagnosis were independently associated with PSC-related serious events. Conclusions: Age and bilirubin are important predictors of PSC-related outcomes.
Full article

Figure 1
Open AccessReview
A Mechanistic Framework of Genetic Liver Diseases: From Developmental Defects to Functional Disorders
by
Angelo Corso Faini, Alberto Calleri, Michele Pinon, Cristina Chiadò, Pier Luigi Calvo, Tiziana Vaisitti and Silvia Deaglio
Livers 2026, 6(2), 29; https://doi.org/10.3390/livers6020029 - 13 Apr 2026
Abstract
►▼
Show Figures
Genetic liver diseases encompass a heterogeneous group of conditions that disrupt hepatic development, structure, or function. Advances in high-throughput sequencing have revealed the molecular basis of many disorders previously defined only by clinical or biochemical features, transforming diagnostic and therapeutic approaches. This review
[...] Read more.
Genetic liver diseases encompass a heterogeneous group of conditions that disrupt hepatic development, structure, or function. Advances in high-throughput sequencing have revealed the molecular basis of many disorders previously defined only by clinical or biochemical features, transforming diagnostic and therapeutic approaches. This review proposes a mechanistic framework that distinguishes diseases arising from developmental abnormalities from those caused by functional impairments in hepatocellular or biliary physiology. It outlines how defects in transporters, enzymes, signaling pathways, intracellular trafficking, and mitochondrial function converge to produce diverse hepatic phenotypes. Moreover, translational aspects are discussed such as how the growing integration of genetic testing into clinical practice enables precise diagnosis, informs prognosis and therapy, and refines disease classification. Finally, the review discusses future directions in the field, emphasizing the role of multi-omic approaches, organoid modeling, and data sharing in elucidating unresolved pathogenic mechanisms and advancing precision hepatology.
Full article
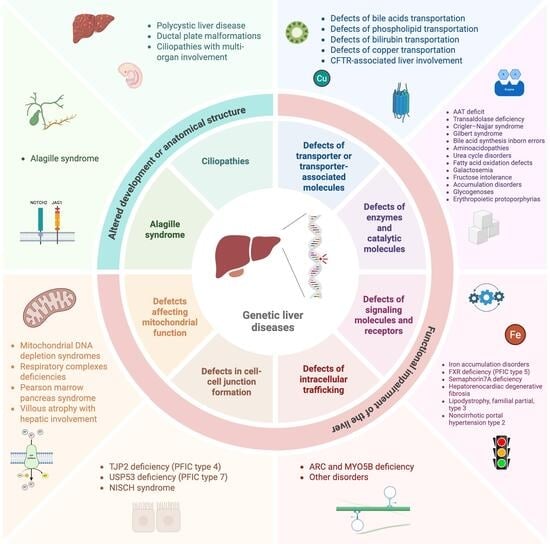
Graphical abstract
Highly Accessed Articles
Latest Books
E-Mail Alert
News
Topics
Topic in
Cancers, Current Oncology, Gastroenterology Insights, Livers, Precision Oncology
Liver Diseases: From Pathogenesis to Modern Management
Topic Editors: Dimitrios Moris, Georgia Sofia KarachaliouDeadline: 15 December 2026
Topic in
Biomedicines, Current Oncology, Diagnostics, JCM, Livers, Transplantology, Gastrointestinal Disorders
Advances in Gastrointestinal and Liver Disease: From Physiological Mechanisms to Clinical Practice, 2nd Edition
Topic Editors: Davide Giuseppe Ribaldone, Gian Paolo CavigliaDeadline: 20 December 2026
Topic in
Biomolecules, Cancers, Cells, JMP, Livers
Signaling Pathways in Liver Disease 2nd Edition
Topic Editors: Ralf Weiskirchen, Amedeo AmedeiDeadline: 31 March 2027

Conferences
Special Issues
Special Issue in
Livers
Epidemiology of Chronic Liver Disease and Cirrhosis
Guest Editors: Basile Njei, Ysabel Ilagan-YingDeadline: 20 June 2026
Special Issue in
Livers
Alcohol-Induced Liver Disease: Clinical, Molecular Mechanism, Pathology, Therapeutics
Guest Editors: Giuliano Ramadori, Manuela G. NeumanDeadline: 30 June 2026
Special Issue in
Livers
Role of Bilirubin in Liver Disease
Guest Editors: Terry D. Hinds, Jr., David E. Stec, Wang-Hsin Lee, Olufunto BadmusDeadline: 20 July 2026
Special Issue in
Livers
Recent Advances in the Detection and Pathophysiology of Steatotic, Alcoholic and Drug-Induced Liver Diseases
Guest Editors: Leonard Nelson, Michel Kranendonk, Anabel Martinez Lyons, Francisco EstevesDeadline: 31 July 2026










