1. Context
In December 2019, the SARS-CoV-19 infection was diagnosed in Wuhang (China) and it is currently spreading rapidly worldwide. Its impact on psychiatric patients institutionalized requires further research [1,2,3,4].
2. Objective
This study aims to know the impact that social isolation measures have had during the COVID-19 pandemic in institutionalized patients psychiatric through a narrative review.
3. Methodology
Narrative review of scientific literature using the keyword MeSH terms “Mental Health”, “COVID-19”, “inmates”, “prisons”, “Spain” and “Europe” and their combinations was carried out in quantitative studies [5]. We searched articles published during 2020–2021 in Spanish and English. We assessed the quality of the selected studies through Strengthening the Reporting of Observational Studies in Epidemiology [STROBE] methodology. Risk of bias score was calculated using the 22 criteria proposed. Each criterion was awarded one point if present in its entirety, a half point if it was somewhat present, and zero points if it wasn’t present at all. Studies scoring 16 or more points were considered with a low risk of bias, those scoring 7–15 points with a moderate risk, and those with 0–6 points had a high risk of bias. Descriptive and thematic analyses were carried out. PRISMA quality criteria and the recommendations of the Centre for Reviews and Dissemination were followed [6,7].
4. Results
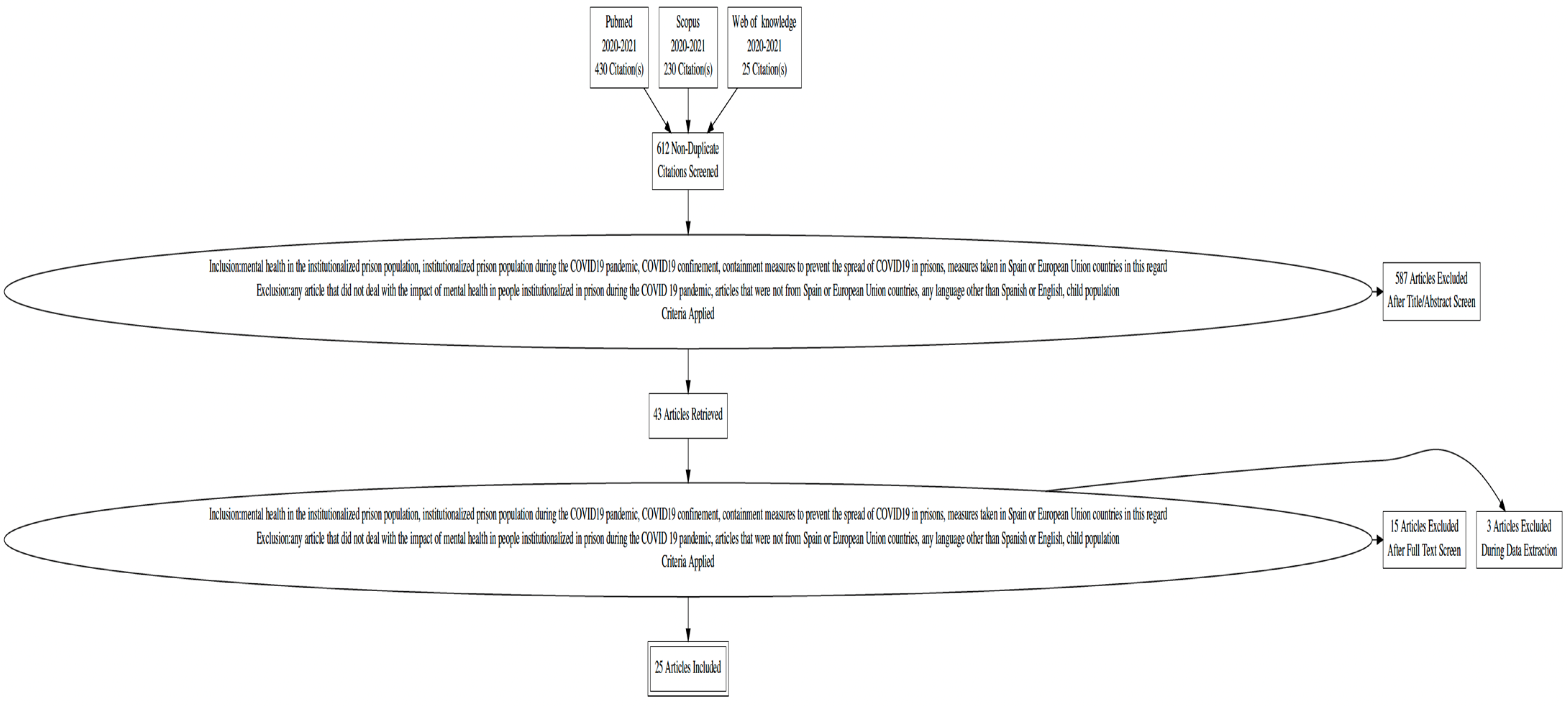
Of 685 studies found, 25 met inclusion criteria (Figure 1). In patients with psychiatric pathology and diagnosed by COVID-19, an elevated level of symptomatology related to post-traumatic stress was obtained (96.2%), mainly depressive symptoms (p = 0.016). In China, patients considered that the lack of assistance and protection resources against the virus as well as the strict measures of social isolation have aggravated their illness, while patients from United States attribute the worsening of the disease to an effective diagnosis of the virus, the difficulty of implementing social distancing measures, and the lack of adequate adherence to treatment. In the Middle East, elderly psychiatric patients are doubly affected due to the lack of care resources. In fact, a French study showed that the mortality of patients with psychiatric pathology was higher than that of all other pathologies (26.7% vs. 8.7%, p = 0.039). Finally, inmates’ psychiatric patients have worsened their pathology related to lack of psychiatric care, stress and measures taken against COVID-19 in prisons.
Figure 1.
PRISMA Flow Chart.
5. Conclusions
During the COVID-19 pandemic, little attention has been paid to the mental health impact on institutionalized psychiatric patients. Institutionalization in and of itself poses a challenge to the well-being of these patients, which has been aggravated by the measures to be adopted to contain the COVID-19 pandemic. Therefore, it is important to understand the consequences of this pandemic in institutionalized settings, where health resources take on an important dimension to effectively prevent both the disease caused by COVID-19 and its impact on mental health. In this sense, the work of health promotion and promotion of healthy lifestyles (more so in psychiatric patients) is especially important to improve psychoneuroimmunity against COVID-19, as well as for achieving a good therapeutic alliance that promotes awareness of the disease in patients and the importance of therapeutic adherence.
Supplementary Materials
The following supporting information can be downloaded at: https://www.mdpi.com/article/10.3390/ECERPH-3-09063/s1.
Author Contributions
All authors have designed the study. They participated in the search for articles. Analyzed their quality. Helped to review the quality of the articles. To write up the results and the subsequent discussion. All authors have read and agreed to the published version of the manuscript.
Funding
This research received no external funding.
Institutional Review Board Statement
This revision has been carried out following the PRISMA criteria and the ZOTERO program for bibliographic management.
Informed Consent Statement
In this case, neither informed consent by patients nor approval by an ethics committee was required because secondary sources of information were used, such as the already published articles that were subsequently reviewed for this narrative review.
Conflicts of Interest
The authors declare no conflict of interest.
References
- di Giacomo, E.; Clerici, M.; Peschi, G.; Fazei, S. Italian prisons during the COVID-19 outbreak. Am. J. Public Health 2020, 110, 1646–1647. [Google Scholar] [CrossRef] [PubMed]
- Johnson, L.; Gutridge, K.; Parkes, J.; Roy, A.; Plugge, E. Scoping review of mental health in prisons through the COVID-19 pandemic. BMJ Open 2021, 11, e046547. [Google Scholar] [CrossRef] [PubMed]
- Kothari, R.; Forrester, A.; Greenberg, N.; Sarkissian, N.; Tracy, D.K. COVID-19 and prisons: Providing mental health care for people in prison, minimising moral injury and psychological distress in mental health staff. Med. Sci. Law 2020, 60, 165–168. [Google Scholar] [CrossRef] [PubMed]
- Liebrenz, M.; Bhugra, D.; Buadze, A.; Schleifer, R. Caring for persons in detention suffering with mental illness during the Covid-19 outbreak. Forensic Sci. Int. Mind Law 2020, 1, 100013. [Google Scholar] [CrossRef] [PubMed]
- Pae, C.-U. Why systematic review rather than narrative review? Psychiatry Investig. 2015, 12, 417. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Moher, D.; Shamseer, L.; Clarke, M.; Ghersi, D.; Liberati, A.; Petticrew, M.; Shekelle, P.; Stewart, L.A. Preferred reporting items for systematic review and meta-analysis protocols (PRISMA-P) 2015 statement. Syst. Rev. 2015, 4, 1–9. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Selçuk, A.A. A guide for systematic reviews: PRISMA. Turk. Arch. Otorhinolaryngol. 2019, 57, 57. [Google Scholar] [CrossRef] [PubMed]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).