Dietary Exposure to Glutamates of 2- to 5-Year-Old Toddlers in China Using the Duplicate Diet Method
Abstract
1. Introduction
2. Materials and Methods
2.1. Subjects and Study Design
2.2. Sampling of Duplicate Diets and Preparation
2.3. Analysis of Monosodium L-Glutamate in Food Samples
2.4. Exposure Assessment
2.5. Risk Characterization
2.6. Statistical Analysis
3. Results
3.1. Participants Characteristics
3.2. Glutamates Concentrations in Duplicate Food Samples
3.3. Estimated Daily Exposure to Glutamates from Repeated Food Samples
4. Discussion
5. Conclusions
Author Contributions
Funding
Data Availability Statement
Conflicts of Interest
References
- Diepeveen, J.; Moerdijk-Poortvliet, T.C.W.; van der Leij, F.R. Molecular insights into human taste perception and umami tastants: A review. J. Food Sci. 2022, 87, 1449–1465. [Google Scholar] [CrossRef] [PubMed]
- Magerowski, G.; Giacona, G.; Patriarca, L.; Papadopoulos, K.; Garza-Naveda, P.; Radziejowska, J.; Alonso-Alonso, M. Neurocognitive effects of umami: Association with eating behavior and food choice. Neuropsychopharmacology 2018, 43, 2009–2016. [Google Scholar] [CrossRef] [PubMed]
- Wang, S.; Zhang, S.; Adhikari, K. Influence of Monosodium Glutamate and Its Substitutes on Sensory Characteristics and Consumer Perceptions of Chicken Soup. Foods 2019, 8, 71. [Google Scholar] [CrossRef] [PubMed]
- EFSA Panel on Food Additives and Nutrient Sources added to Food (ANS); Mortensen, A.; Aguilar, F.; Crebelli, R.; Di Domenico, A.; Dusemund, B.; Frutos, M.J.; Galtier, P.; Gott, D.; Gundert-Remy, U.; et al. Re-evaluation of glutamic acid (E 620), sodium glutamate (E 621), potassium glutamate (E 622), calcium glutamate (E 623), ammonium glutamate (E 624) and magnesium glutamate (E 625) as food additives. EFSA J. 2017, 15, e04910. [Google Scholar] [PubMed]
- Munro, H.N. Factors in the regulation of glutamate metabolism. In Glutamic Acid: Advances in Biochemistry and Physiology; Raven Press: New York, NY, USA, 1979; pp. 55–68. [Google Scholar]
- Meister, A. Biochemistry of Glutamate: Glutamine and Glutathione; Glutamic acid Raven Press: New York, NY, USA, 1979; pp. 69–84. [Google Scholar]
- Stegink, L.D. Aspartate and Glutamate Metabolism Aspartame Physiology and Biochemistry; Stegink, L.D., Filer, L.J., Jr., Eds.; Marcel Dekker: New York, NY, USA, 1984; pp. 47–76. [Google Scholar]
- Neame, K.; Wiseman, G. The alanine and oxo acid concentrations in mesenteric blood during the absorption of l-glutamic acid by the small intestine of the dog, cat and rabbit in vivo. J. Physiol. 1958, 140, 148. [Google Scholar] [CrossRef] [PubMed]
- Windmueller, H.G.; Spaeth, A.E. Intestinal metabolism of glutamine and glutamate from the lumen as compared to glutamine from blood. Arch. Biochem. Biophys. 1975, 171, 662–672. [Google Scholar] [CrossRef]
- Windmueller, H.G. Glutamine utilization by the small intestine. Adv. Enzym. Relat. Areas Mol. Biol. 1982, 53, 201–237. [Google Scholar]
- Stegink, L.D.; Filer, L., Jr.; Baker, G.L. Plasma amino acid concentrations in normal adults fed meals with added monosodium L-glutamate and aspartame. J. Nutr. 1983, 113, 1851–1860. [Google Scholar] [CrossRef]
- Peng, Y.; Gubin, J.; Harper, A.; Vavich, M.; Kemmerer, A. Food intake regulation: Amino acid toxicity and changes in rat brain and plasma amino acids. J. Nutr. 1973, 103, 608–617. [Google Scholar] [CrossRef]
- Liebschutz, J.; Airoldi, L.; Brownstein, M.J.; Chinn, N.G.; Wurtman, R.J. Regional distribution of endogenous and parenteral glutamate, aspartate and glutamine in rat brain. Biochem. Pharm. 1977, 26, 443–446. [Google Scholar] [CrossRef]
- Caccia, S.; Garattini, S.; Ghezzi, P.; Zanini, M. Plasma and brain levels of glutamate and pyroglutamate after oral monosodium glutamate to rats. Toxicol. Lett. 1982, 10, 169–175. [Google Scholar] [CrossRef] [PubMed]
- Bizzi, A.; Veneroni, E.; Salmona, M.; Garattini, S. Kinetics of monosodium glutamate in relation to its neurotoxicity. Toxicol. Lett. 1977, 1, 123–130. [Google Scholar] [CrossRef]
- Krebs, H.; Bellamy, D. The interconversion of glutamic acid and aspartic acid in respiring tissues. Biochem. J. 1960, 75, 523. [Google Scholar] [CrossRef] [PubMed]
- Balazs, R. Control of glutamate oxidation in brain and liver mitochondrial systems. Biochem. J. 1965, 95, 497. [Google Scholar] [CrossRef] [PubMed]
- Hertz, L. Functional interactions between neurons and astrocytes I. Turnover and metabolism of putative amino acid transmitters. Prog. Neurobiol. 1979, 13, 277–323. [Google Scholar] [CrossRef] [PubMed]
- Benjamin, A.; Quastel, J. Fate of L-glutamate in the brain. J. Neurochem. 1974, 23, 457–464. [Google Scholar] [CrossRef]
- Dennis, S.; Land, J.; Clark, J. Glutamate metabolism and transport in rat brain mitochondria. Biochem. J. 1976, 156, 323–331. [Google Scholar] [CrossRef]
- Erecińska, M.; Silver, I.A. Metabolism and role of glutamate in mammalian brain. Prog. Neurobiol. 1990, 35, 245–296. [Google Scholar] [CrossRef]
- Ragginer, C.; Lechner, A.; Bernecker, C.; Horejsi, R.; Möller, R.; Wallner-Blazek, M.; Weiss, S.; Fazekas, F.; Schmidt, R.; Truschnig-Wilders, M. Reduced urinary glutamate levels are associated with the frequency of migraine attacks in females. Eur. J. Neurol. 2012, 19, 1146–1150. [Google Scholar] [CrossRef]
- Chakraborty, S.P. Patho-physiological and toxicological aspects of monosodium glutamate. Toxicol. Mech. Methods 2019, 29, 389–396. [Google Scholar] [CrossRef]
- CCFA. General standard for food additives. 2019, CXS 192-1995. Available online: https://www.fao.org/fao-who-codexalimentarius/sh-proxy/en/?lnk=1&url=https%253A%252F%252Fworkspace.fao.org%252Fsites%252Fcodex%252FStandards%252FCXS%2B192-1995%252FCXS_192e.pdf (accessed on 21 March 2023).
- JECFA. Toxicological Evaluation of Certain Food Additives with a Review of General Principles and of Specifications: Seventeenth Report of the Joint FAO/WHO Expert Committee on Food Additives, Geneva, 25 June–4 July 1973; WHO: Geneva, Switzerland, 1974. [Google Scholar]
- JECFA. Evaluation of Food Additives: Specifications for the Identity and Purity of Food Additives and Their Toxicological Evaluation, Some Extraction Solvents and Certain Other Substances; WHO: Geneva, Switzerland, 1971. [Google Scholar]
- JECFA. Amino Acids and Related Substances. Safety Evaluation of Certain Food Additives. Prepared by the Sixty~Third Meeting of the Joint FAO/WHO Expert Committee on Food Additives (JECFA) at the Meeting in Geneva 8–17 June 2004; WHO: Geneva, Switzerland, 2006. [Google Scholar]
- Burdock, G.A.; Carabin, I.G. Generally recognized as safe (GRAS): History and description. Toxicol. Lett. 2004, 150, 3–18. [Google Scholar] [CrossRef] [PubMed]
- Berg, D. FASEB (Federation of American Societies for Experimental Biology) Summer Research on Neuronal Cell Cultures at Saxton’s River, Vermont on 12–17 August 1984; WHO: Geneva, Switzerland, 1984. [Google Scholar]
- Carballo, J.; Carere, A.; Elton, G.; Ferreira, M.; Ferro-luzzi, A.; Gibney, M.; Knudsen, I.; Netter, Κ.; Noirfalise, A.; Pascal, G.; et al. Reports of the Scientific Committee for Food: 25th Series: First Series of Food Additives of Various Technological Functions; Commission of the European Communities: Luxembourg, 1991. [Google Scholar]
- FASEB. Executive Summary from the Report: Analysis of Adverse Reactions to Monosodium Glutamate (MSG) 1995. Available online: https://www.knowmsg.com/wp-content/themes/whyusemsg/assets/pdfs/FASEB-MSG-1995.pdf (accessed on 21 March 2023).
- Meadows, M.M.S.G. A common flavor enhancer. FDA Consum. 2003, 37, 34–35. [Google Scholar]
- Vorhees, C.V.; Butcher, R.E.; Brunner, R.L.; Sobotka, T.J. A developmental test battery for neurobehavioral toxicity in rats: A preliminary analysis using monosodium glutamate calcium carrageenan, and hydroxyurea. Toxicol. Appl. Pharm. 1979, 50, 267–282. [Google Scholar] [CrossRef] [PubMed]
- Rietjens, I.M.; Tanaka, T.; Masuzawa, Y.; Nakamura, H.; Ishizaka, Y.; Teoh, K.N. A chemical-specific adjustment factor for human interindividual differences in kinetics for glutamates (E620–625). Food Chem. Toxicol. 2021, 147, 111910. [Google Scholar] [CrossRef]
- Roberts, A.; Lynch, B.; Rietjens, I.M. Risk assessment paradigm for glutamate. Ann. Nutr. Metab. 2018, 73, 53–64. [Google Scholar] [CrossRef]
- Loï CCynober, L. Glutamate: A Safe Nutrient, Not Just a Simple Additive. Ann. Nutr. Metab. 2022, 78, 133–146. [Google Scholar]
- Thomas, K.W.; Sheldon, L.S.; Pellizzari, E.D.; Handy, R.W.; Roberds, J.M.; Berry, M.R. Testing duplicate diet sample collection methods for measuring personal dietary exposures to chemical contaminants. J. Expo. Anal. Environ. Epidemiol. 1997, 7, 17–36. [Google Scholar]
- WHO. Guidelines for the Study of Dietary Intakes of Chemical Contaminants; WHO: Geneva, Switzerland, 1985. [Google Scholar]
- Nakatsuka, H.; Kim, E.S.; Ko, Y.S.; Yang, H.R.; Moon, C.S.; Watanabe, T.; Shimbo, S.; Ikeda, M. Food intake survey of kindergarten children in Korea: Part 1 food, energy, and nutrient intake. Environ. Health Prev. Med. 2015, 20, 294–301. [Google Scholar] [CrossRef]
- Asakura, K.; Haga, M.; Adachi, M.; Sakai, H.; Takahashi, C.; Sasaki, S. Estimation of food portion sizes frequently consumed by children 3–6 years old in Japan. J. Nutr. Sci. Vitam. 2014, 60, 387–396. [Google Scholar] [CrossRef]
- Borrmann, A.; Mensink, G.B.M.; Ki, G.G.S.S.G. Obst- und Gemüsekonsum von Kindern und Jugendlichen in Deutschland. Bundesgesundheitsblatt—Gesundh.—Gesundh. 2015, 58, 1005–1014. [Google Scholar] [CrossRef]
- Krug, S.; Finger, J.D.; Lange, C.; Richter, A.; Mensink, G.B.M. Sports and dietary behaviour among children and adolescents in Germany. Results of the cross-sectional KiGGS Wave 2 study and trends. J. Health Monit. 2018, 3, 3–22. [Google Scholar] [PubMed]

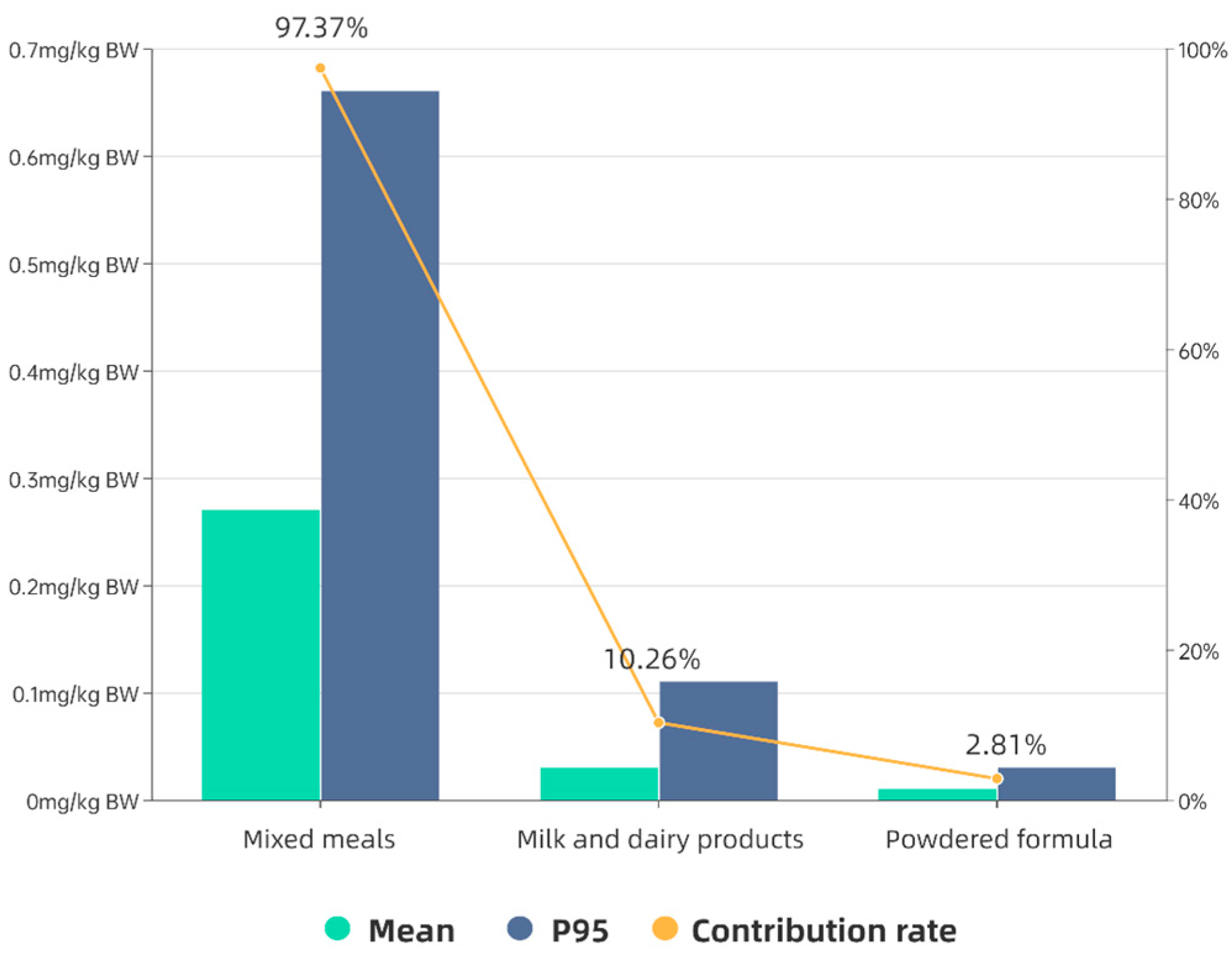
| Category | Mean ± SD | P50 | P90 | P95 | P97.5 | P99 * |
|---|---|---|---|---|---|---|
| Mixed meals | 5.12 ± 4.94 | 4.03 | 10.59 | 15.40 | 17.98 | 24.68 |
| Milk and dairy products | 2.29 ± 2.17 | 1.45 | 5.34 | 7.18 | 9.02 | 10.57 |
| Powdered formula | 3.89 ± 3.12 | 3.24 | 7.01 | 10.57 | 13.89 | 14.90 |
| Age | Mean ± SD | P50 | P90 | P95 | P97.5 | P99 * |
|---|---|---|---|---|---|---|
| 2–3 | 139.15 ± 10.35 | 100.00 | 274.90 | 383.92 | 478.12 | 619.38 |
| 3–4 | 204.31 ± 18.00 | 156.70 | 365.32 | 419.48 | 473.63 | 515.74 |
| 4–5 | 179.00 ± 19.78 | 139.70 | 363.60 | 385.32 | 405.24 | 414.87 |
| Total | 162.46 ± 117.40 | 125.00 | 344.00 | 404.33 | 454.38 | 592.24 |
| Age | Mean ± SD | P50 | P90 | P95 | P97.5 | P99 * |
|---|---|---|---|---|---|---|
| 2–3 | 32.95 ± 1.46 | 32.70 | 51.70 | 58.60 | 62.70 | 65.69 |
| 3–4 | 36.80 ± 2.99 | 33.00 | 60.64 | 61.55 | 65.19 | 70.24 |
| 4–5 | 30.20 ± 1.96 | 25.60 | 37.05 | 41.88 | 46.94 | 49.98 |
| Total | 33.47 ± 14.00 | 32.50 | 56.10 | 61.10 | 62.98 | 82.59 |
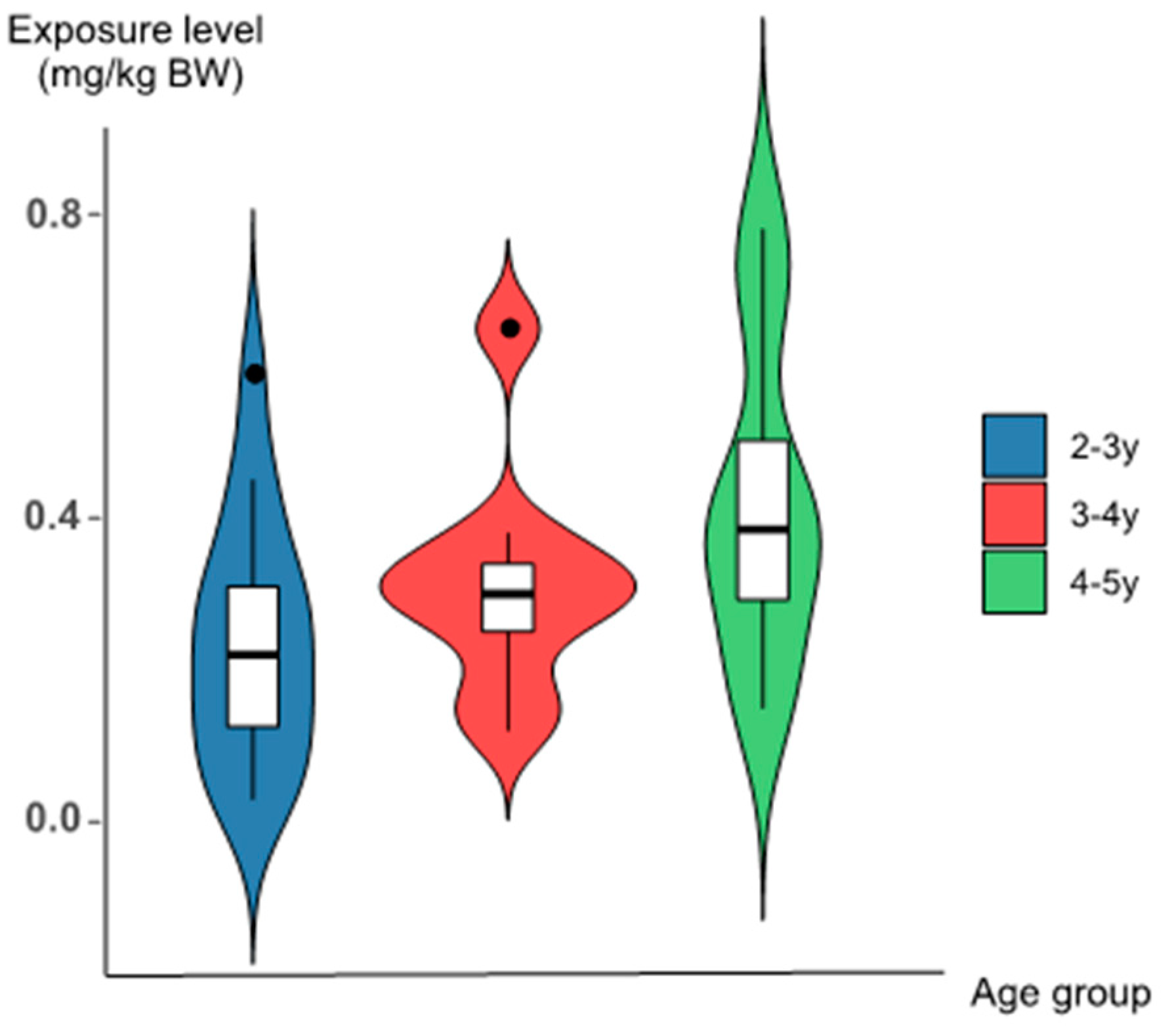
| Age | N | Mean ± SD | P50 * | P95 * | Range |
|---|---|---|---|---|---|
| 2–3 | 15 | 0.20 ± 0.04 | 0.19 | 0.44 | 0.03–0.51 |
| 3–4 | 9 | 0.27 ± 0.04 | 0.26 | 0.50 | 0.10–0.57 |
| 4–5 | 8 | 0.37 ± 0.07 | 0.35 | 0.65 | 0.13–0.68 |
| Total | 32 | 0.26 ± 0.03 | 0.26 | 0.63 | 0.03–0.68 |
| %ADI (JECFA) | - * | 0.22 | 0.22 | 0.53 | 0.03–0.57 |
| %ADI (EFSA) | - | 0.87 | 0.87 | 2.10 | 0.10–2.27 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Zhou, Y.; Sui, H.; Wang, Y.; Yong, L.; Zhang, L.; Liang, J.; Zhou, J.; Xu, L.; Zhong, Y.; Chen, J.; et al. Dietary Exposure to Glutamates of 2- to 5-Year-Old Toddlers in China Using the Duplicate Diet Method. Foods 2023, 12, 1898. https://doi.org/10.3390/foods12091898
Zhou Y, Sui H, Wang Y, Yong L, Zhang L, Liang J, Zhou J, Xu L, Zhong Y, Chen J, et al. Dietary Exposure to Glutamates of 2- to 5-Year-Old Toddlers in China Using the Duplicate Diet Method. Foods. 2023; 12(9):1898. https://doi.org/10.3390/foods12091898
Chicago/Turabian StyleZhou, Yanjun, Haixia Sui, Yibaina Wang, Ling Yong, Lei Zhang, Jiang Liang, Jing Zhou, Lili Xu, Yanxu Zhong, Jinyao Chen, and et al. 2023. "Dietary Exposure to Glutamates of 2- to 5-Year-Old Toddlers in China Using the Duplicate Diet Method" Foods 12, no. 9: 1898. https://doi.org/10.3390/foods12091898
APA StyleZhou, Y., Sui, H., Wang, Y., Yong, L., Zhang, L., Liang, J., Zhou, J., Xu, L., Zhong, Y., Chen, J., & Song, Y. (2023). Dietary Exposure to Glutamates of 2- to 5-Year-Old Toddlers in China Using the Duplicate Diet Method. Foods, 12(9), 1898. https://doi.org/10.3390/foods12091898





