Sustainable Dental and Periodontal Practice: A Narrative Review on the 4R-Framework—Reduce, Reuse, Rethink, Recycle—And Waste Management Rationalization
Abstract
1. Introduction
2. Materials and Methods
- (“green dentistry” OR “sustainable dentistry” OR “eco-friendly dentistry” OR “environmentally sustainable oral healthcare” OR “sustainable oral healthcare” OR “sustainable dental practice”) AND
- (“environmental impact” OR “carbon footprint” OR “greenhouse gas emissions” OR “environmental sustainability” OR “waste reduction” OR “pollution reduction”) AND
- (“disposable materials” OR “reusable products” OR “recycling” OR “water conservation” OR “energy conservation” OR “renewable energy” OR “life cycle assessment” OR “LCA”) AND
- (“dentistry” OR “oral healthcare” OR “dental practice” OR “dental clinics” OR “periodontal management” OR “periodontal therapy” OR “periodontology”)
3. Results
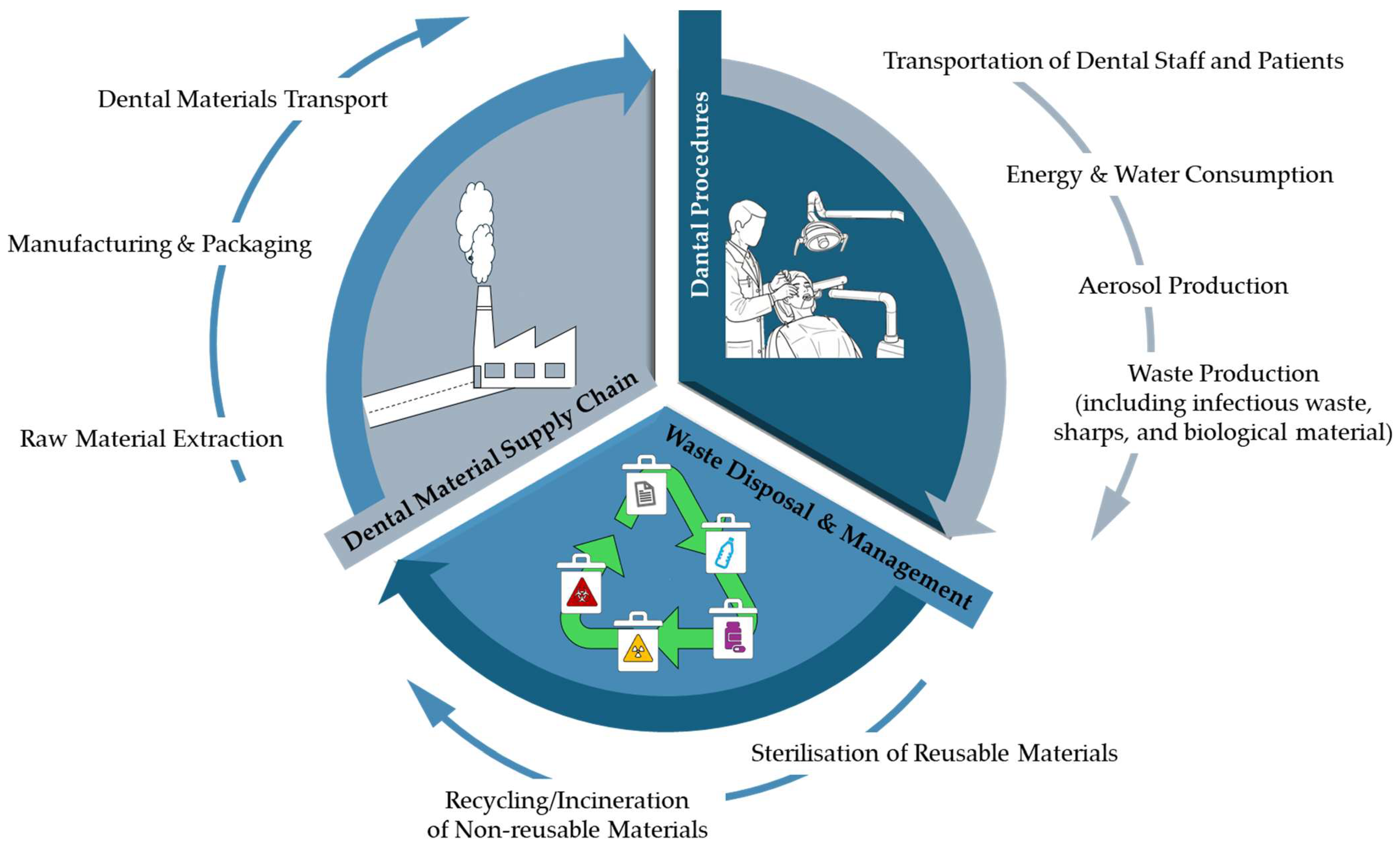
3.1. Sustainability in Health Care and Environmental Impact of Oral Healthcare
3.2. Sustainability as a Core Business Strategy in Health and Oral Care and Principles of Sustainable Oral Healthcare
- Disease prevention and health promotion: the most sustainable care is care that is not needed. By preventing caries and periodontal disease, reliance on resource-intensive interventions can be reduced.
- Minimization of environmental harm: dentistry must reduce emissions, eliminate avoidable waste, and shift to low-impact materials. Innovations such as teledentistry, energy-efficient equipment, and green procurement can reduce the carbon burden.
- Systems-based sustainability: sustainability must be integrated across institutional domains, including education, policy, procurement, infrastructure, and clinical operations.
- Equity and justice: sustainability efforts must not compromise access to care or exacerbate disparities. Policies should support equitable distribution of sustainable technologies and services.
- Evidence-based innovation: interventions should be guided by robust environmental data and clinical outcomes, avoiding superficial “greenwashing” and emphasizing continuous quality improvement [17].
3.3. Sustainable Dental and Periodontal Practice: 4R Framework—Reduce, Reuse, Rethink, and Recycle
3.4. Sustainable Dental and Periodontal Practice: Strategies
3.4.1. Eco-Efficient Energy Use and Eco-Responsible Water Use
3.4.2. Air Pollution Reduction
3.4.3. Reusable Products
3.4.4. Paperless Practices
3.4.5. Recycling and Optimizing Waste Management
3.4.6. Green Procurement
3.4.7. Teledentistry and Artificial Intelligence
3.4.8. Awareness and Education
4. Discussion
4.1. Sustainability in Periodontal Practice: Pre-Workplace Domain
4.2. Sustainability in Periodontal Practice: Workplace Domain
4.3. Sustainability in Periodontal Practice: Waste Management
4.4. Policy and Recommendations for Sustainable Dental and Periodontal Practice
4.5. Barriers to Change Towards Sustainable Dentistry
4.6. Future Prospects
- Development of Standardized LCA protocols tailored for the dental setting
- New Technologies and Sustainable Innovation
- Educational Frameworks and Behavioral Change
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Eckelman, M.J.; Sherman, J.; Ahmad, S. Environmental Impacts of the U.S. Health Care System and Effects on Public Health. PLoS ONE 2016, 11, e0157014. [Google Scholar] [CrossRef] [PubMed]
- Duane, B.; Stancliffe, R.; Miller, F.; Sherman, J.; Pasdeki-Clewer, E. Sustainability in Dentistry: A Multifaceted Approach Needed. J. Dent. Res. 2020, 99, 998–1003. [Google Scholar] [CrossRef]
- Speroni, S.; Polizzi, E. Green Dentistry: State of the Art and Possible Development Proposals. Dent. J. 2025, 13, 38. [Google Scholar] [CrossRef] [PubMed]
- Graziani, F.; Karapetsa, D.; Alonso, B.; Herrera, D. Nonsurgical and Surgical Treatment of Periodontitis: How Many Options for One Disease? Periodontology 2000 2017, 75, 152–188. [Google Scholar] [CrossRef] [PubMed]
- Zucchelli, G.; Sharma, P.; Mounssif, I. Esthetics in Periodontics and Implantology. Periodontology 2000 2018, 77, 7–18. [Google Scholar] [CrossRef]
- Sanz, M.; Herrera, D.; Kebschull, M.; Chapple, I.; Jepsen, S.; Berglundh, T.; Sculean, A.; Tonetti, M.S.; Consultants, T.E.W.P.A.M.; Lambert, N.L.F. Treatment of stage I–III periodontitis—The EFP S3 level clinical practice guideline. J. Clin. Periodontol. 2020, 47, 4–60. [Google Scholar] [CrossRef]
- Simonpieri, A.; Gasparro, R.; Pantaleo, G.; Mignogna, J.; Riccitiello, F.; Sammartino, G. Four-year post-loading results of full-arch rehabilitation with immediate placement and immediate loading implants: A retrospective controlled study. Quintessence Int. 2017, 48, 315–324. [Google Scholar] [CrossRef]
- Jepsen, S.; Blanco, J.; Buchalla, W.; Carvalho, J.C.; Dietrich, T.; Dörfer, C.; Eaton, K.A.; Figuero, E.; Frencken, J.E.; Graziani, F.; et al. Prevention and control of dental caries and periodontal diseases at individual and population level: Consensus report of group 3 of joint EFP/ORCA workshop on the boundaries between caries and periodontal diseases. J. Clin. Periodontol. 2017, 44, S85–S93. [Google Scholar] [CrossRef]
- Duane, B.; Lee, M.B.; White, S.; Stancliffe, R.; Steinbach, I. An estimated carbon footprint of NHS primary dental care within England. How can dentistry be more environmentally sustainable? Br. Dent. J. 2017, 223, 589–593. [Google Scholar] [CrossRef]
- Zannella, C.; Shinde, S.; Vitiello, M.; Falanga, A.; Galdiero, E.; Fahmi, A.; Santella, B.; Nucci, L.; Gasparro, R.; Galdiero, M.; et al. Antibacterial Activity of Indolicidin-Coated Silver Nanoparticles in Oral Disease. Appl. Sci. 2020, 10, 1837. [Google Scholar] [CrossRef]
- Mulimani, P. Green dentistry: The art and science of sustainable practice. Br. Dent. J. 2017, 222, 954–961. [Google Scholar] [CrossRef]
- Di Spirito, F.; Iacono, V.J.; Alfredo, I.; Alessandra, A.; Sbordone, L.; Lanza, A. Evidence-based Recommendations on Periodontal Practice and the Management of Periodontal Patients During and After the COVID-19 Era: Challenging Infectious Diseases Spread by Airborne Transmission. Open Dent. J. 2021, 15, 325–336. [Google Scholar] [CrossRef]
- Shaw, E.; Walpole, S.; McLean, M.; Alvarez-Nieto, C.; Barna, S.; Bazin, K.; Behrens, G.; Chase, H.; Duane, B.; El Omrani, O.; et al. AMEE Consensus Statement: Planetary health and education for sustainable healthcare. Med. Teach. 2021, 43, 272–286. [Google Scholar] [CrossRef]
- Martin, N.; Sheppard, M.; Gorasia, G.; Arora, P.; Cooper, M.; Mulligan, S. Awareness and barriers to sustainability in dentistry: A scoping review. J. Dent. 2021, 112, 103735. [Google Scholar] [CrossRef]
- Berniak-Woźny, J.; Rataj, M. Towards Green and Sustainable Healthcare: A Literature Review and Research Agenda for Green Leadership in the Healthcare Sector. Int. J. Environ. Res. Public Health 2023, 20, 908. [Google Scholar] [CrossRef] [PubMed]
- Rajagopalan, S.; Pronovost, P.; Al-Kindi, S. Implementing a Sustainability Framework in Healthcare: A Three-Lens Framework. Healthcare 2023, 11, 1867. [Google Scholar] [CrossRef] [PubMed]
- Martin, N.; Mulligan, S.; Shellard, I.J.; Hatton, P.V. Consensus on Environmentally Sustainable Oral Healthcare a Joint Stakeholder Statement; White Rose University Press: York, UK, 2022. [Google Scholar]
- Mandair, R. Green Impact dentistry. Br. Dent. J. 2020, 229, 759. [Google Scholar] [CrossRef] [PubMed]
- Borglin, L.; Pekarski, S.; Saget, S.; Duane, B. The life cycle analysis of a dental examination: Quantifying the environmental burden of an examination in a hypothetical dental practice. Community Dent. Oral Epidemiol. 2021, 49, 581–593. [Google Scholar] [CrossRef]
- Duane, B.; Harford, S.; Steinbach, I.; Stancliffe, R.; Swan, J.; Lomax, R.; Pasdeki-Clewer, E.; Ramasubbu, D. Environmentally sustainable dentistry: Energy use within the dental practice. Br. Dent. J. 2019, 226, 367–373. [Google Scholar] [CrossRef]
- Byrne, D.; Saget, S.; Davidson, A.; Haneef, H.; Abdeldaim, T.; Almudahkah, A.; Basquille, N.; Bergin, A.M.; Prida, J.; Lyne, A.; et al. Comparing the environmental impact of reusable and disposable dental examination kits: A life cycle assessment approach. Br. Dent. J. 2022, 233, 317–325. [Google Scholar] [CrossRef]
- Landrigan, P.J.; Raps, H.; Cropper, M.; Bald, C.; Brunner, M.; Canonizado, E.M.; Charles, D.; Chiles, T.C.; Donohue, M.J.; Enck, J.; et al. The Minderoo-Monaco Commission on Plastics and Human Health. Ann. Glob. Health 2023, 89, 23. [Google Scholar] [CrossRef]
- Veress, S.; Kerekes-Máthé, B.; Székely, M. Environmentally friendly behaviour in dentistry. Med. Pharm. Rep. 2023, 96, 199–205. [Google Scholar] [CrossRef]
- Soliman, H.M.H. Role of eco-friendly dental clinic option in water saving. Environ. Conserv. J. 2023, 24, 326–329. [Google Scholar] [CrossRef]
- Sanguida, A.; Niranchana, R.S.; Shabnam, N.K. Knowledge, Implementation, and Perceived Barriers to Eco-friendly Dental Practice among Dental Practitioners in Puducherry. J. Pharm. Bioallied Sci. 2024, 16, S4478–S4483. [Google Scholar] [CrossRef]
- Javaid, J.; Khokhar, D.H.; Iqbal, J.; Javed, M.K. Water Consumption In Dental Practices: Study Water Usage Patterns In Dental Offices, Including Consumption For Patient Care, Sterilization, And Facility Maintenance. Assess Strategies For Reducing Water Waste And Improving Efficiency, Considering Both Env. Pak. J. Sci. 2025, 77, 92–103. [Google Scholar] [CrossRef]
- Antoniadou, M.; Intzes, A.; Kladouchas, C.; Christou, I.; Chatzigeorgiou, S.; Plexida, M.; Stefanidakis, V.; Tzoutzas, I. Factors Affecting Water Quality and Sustainability in Dental Practices in Greece. Sustainability 2023, 15, 9115. [Google Scholar] [CrossRef]
- Nagraj, S.K.; Eachempati, P.; Paisi, M.; Nasser, M.; Sivaramakrishnan, G.; Verbeek, J.H.; Cochrane Oral Health Group. Interventions to reduce contaminated aerosols produced during dental procedures for preventing infectious diseases. Cochrane Database Syst. Rev. 2020, 2020, CD013686. [Google Scholar] [CrossRef]
- Tzoutzas, I.; Karoussis, I.; Maltezou, H.C. Air Quality in Dental Care Facilities: Update to Current Management and Control Strategies Implementing New Technologies: A Comprehensive Review. Vaccines 2022, 10, 847. [Google Scholar] [CrossRef]
- Boccia, G.; Di Spirito, F.; D’ambrosio, F.; De Caro, F.; Pecora, D.; Giorgio, R.; Fortino, L.; Longanella, W.; Franci, G.; Santella, B.; et al. Microbial Air Contamination in a Dental Setting Environment and Ultrasonic Scaling in Periodontally Healthy Subjects: An Observational Study. Int. J. Environ. Res. Public Health 2023, 20, 2710. [Google Scholar] [CrossRef]
- Santella, B.; Serretiello, E.; De Filippis, A.; Folliero, V.; Iervolino, D.; Dell’annunziata, F.; Manente, R.; Valitutti, F.; Santoro, E.; Pagliano, P.; et al. Lower Respiratory Tract Pathogens and Their Antimicrobial Susceptibility Pattern: A 5-Year Study. Antibiotics 2021, 10, 851. [Google Scholar] [CrossRef]
- Duane, B.; Steinbach, I.; Ramasubbu, D.; Stancliffe, R.; Croasdale, K.; Harford, S.; Lomax, R. Environmental sustainability and travel within the dental practice. Br. Dent. J. 2019, 226, 525–530. [Google Scholar] [CrossRef]
- Voudrias, E.A.; Topalidis, A.; Mandalidis, A.; Iosifidis, N. Variability of Greek dental solid waste production by different dentist groups. Environ. Monit. Assess. 2018, 190, 418. [Google Scholar] [CrossRef]
- Ding, H.; Tsoi, J.K.-H.; Kan, C.-W.; Matinlinna, J.P. A simple solution to recycle and reuse dental CAD/CAM zirconia block from its waste residuals. J. Prosthodont. Res. 2021, 65, 311–320. [Google Scholar] [CrossRef]
- Richardson, J.; Grose, J.; Manzi, S.; Mills, I.; Moles, D.R.; Mukonoweshuro, R.; Nasser, M.; Nichols, A. What’s in a bin: A case study of dental clinical waste composition and potential greenhouse gas emission savings. Br. Dent. J. 2016, 220, 61–66. [Google Scholar] [CrossRef]
- Esmizadeh, E.; Chang, B.; Jubinville, D.; Seto, C.; Ojogbo, E.; Tzoganakis, C.; Mekonnen, T. Stability of nitrile and vinyl latex gloves under repeated disinfection cycles. Mater. Today Sustain. 2021, 11–12, 100067. [Google Scholar] [CrossRef]
- Dawson, J.N.; Guha, S.; Schwerin, M.; Lucas, A. Evaluation of Glove Performance after Decontamination. Biomed. Instrum. Technol. 2023, 57, 31–39. [Google Scholar] [CrossRef]
- Peikert, S.A.; Mittelhamm, F.; Frisch, E.; Vach, K.; Ratka-Krüger, P.; Woelber, J.P. Use of digital periodontal data to compare periodontal treatment outcomes in a practice-based research network (PBRN): A proof of concept. BMC Oral Health 2020, 20, 297. [Google Scholar] [CrossRef]
- Agarwal, B.; Singh, S.V.; Bhansali, S.; Agarwal, S. Waste management in dental office. Indian J. Community Med. 2012, 37, 201–202. [Google Scholar] [CrossRef]
- Boukhris, H.; Zidani, H.; Khalifa, A.B.; Bouslema, G.; Youssef, S.B. Environmental Impact of Dental Waste: A Survey-based Analysis of Waste Segregation and Recycling Practices in Dental Clinics. J. Contemp. Dent. Pract. 2025, 26, 250–256. [Google Scholar] [CrossRef]
- Farahani, D.A.; Suchak, M. Eco-Friendly Dentistry the Environmentally-Responsible Dental Practice. Available online: https://www.ecodentistry.org/wp-content/uploads/2014/12/eco-friendly_dentistry_jcda.pdf (accessed on 2 August 2025).
- Srikanth, P.K.; Srimanoi, W.; Kashyap, P.; Visvanathan, C. Overview of Infectious Healthcare Waste Management in Thailand in Pre- and During COVID-19 Context. In Health Care Waste Management and COVID-19 Pandemic; Springer Nature: Singapore, 2022; pp. 121–150. [Google Scholar]
- Suresh, P.; Crotty, J.; Tesanovic, S.; Alaweed, O.; Doyle, S.; Kiandee, M.; Hayes, E.; Umeh, V.; Khalilinejad, B.; Duane, B. A Life Cycle Analysis of the Environmental Impact of Procurement, Waste and Water in the Dental Practice. Br. Dent. J. 2024, 236, 545–551. [Google Scholar] [CrossRef]
- Duane, B.; Borglin, L.; Pekarski, S.; Saget, S.; Duncan, H.F. Environmental Sustainability in Endodontics. A Life Cycle Assessment (LCA) of a Root Canal Treatment Procedure. BMC Oral Health 2020, 20, 348. [Google Scholar] [CrossRef]
- Abed, R.; Ashley, P.; Duane, B.; Crotty, J.; Lyne, A. An Environmental Impact Study of Inter-dental Cleaning Aids. J. Clin. Periodontol. 2023, 50, 2–10. [Google Scholar] [CrossRef]
- El Tantawi, M.; Lam, W.Y.H.; Giraudeau, N.; Virtanen, J.I.; Matanhire, C.; Chifamba, T.; Sabbah, W.; Gomaa, N.; Al-Maweri, S.A.; Uribe, S.E.; et al. Teledentistry from Research to Practice: A Tale of Nineteen Countries. Front. Oral Health 2023, 4, 1188557. [Google Scholar] [CrossRef]
- Parihar, A.S.; Narang, S.; Tyagi, S.; Narang, A.; Dwivedi, S.; Katoch, V.; Laddha, R. Artificial Intelligence in Periodontics: A Comprehensive Review. J. Pharm. Bioallied. Sci. 2024, 16, S1956–S1958. [Google Scholar] [CrossRef]
- Usher, K.; Williams, J.; Jackson, D. The Potential of Virtual Healthcare Technologies to Reduce Healthcare Services’ Carbon Footprint. Front. Public Health 2024, 12, 1394095. [Google Scholar] [CrossRef]
- Holmner, Å.; Ebi, K.L.; Lazuardi, L.; Nilsson, M. Carbon Footprint of Telemedicine Solutions—Unexplored Opportunity for Reducing Carbon Emissions in the Health Sector. PLoS ONE 2014, 9, e105040. [Google Scholar] [CrossRef]
- Morcillo Serra, C.; Aroca Tanarro, A.; Cummings, C.M.; Jimenez Fuertes, A.; Tomás Martínez, J.F. Impact on the Reduction of CO2 Emissions Due to the Use of Telemedicine. Sci. Rep. 2022, 12, 12507. [Google Scholar] [CrossRef]
- Cannatà, D.; Galdi, M.; Russo, A.; Scelza, C.; Michelotti, A.; Martina, S. Reliability and Educational Suitability of TikTok Videos as a Source of Information on Sleep and Awake Bruxism: A Cross-Sectional Analysis. J. Oral Rehabil. 2024, 52, 434–442. [Google Scholar] [CrossRef]
- Akram, H.M. Artificial Intelligence in Dentistry: Advancements in Periodontology and Other Specialties, Diagnosis, Treatment Planning, and Ethical Considerations. Dent. Rev. 2025, 5, 100157. [Google Scholar] [CrossRef]
- Schwendicke, F.; Samek, W.; Krois, J. Artificial Intelligence in Dentistry: Chances and Challenges. J. Dent. Res. 2020, 99, 769–774. [Google Scholar] [CrossRef]
- Tobias, G.; Spanier, A.B. Developing a Mobile App (IGAM) to Promote Gingival Health by Professional Monitoring of Dental Selfies: User-Centered Design Approach. JMIR Mhealth Uhealth 2020, 8, e19433. [Google Scholar] [CrossRef]
- Shetty, V.; Morrison, D.; Belin, T.; Hnat, T.; Kumar, S. A Scalable System for Passively Monitoring Oral Health Behaviors Using Electronic Toothbrushes in the Home Setting: Development and Feasibility Study. JMIR Mhealth Uhealth 2020, 8, e17347. [Google Scholar] [CrossRef]
- Alotaibi, G.; Awawdeh, M.; Farook, F.F.; Aljohani, M.; Aldhafiri, R.M.; Aldhoayan, M. Artificial Intelligence (AI) Diagnostic Tools: Utilizing a Convolutional Neural Network (CNN) to Assess Periodontal Bone Level Radiographically—A Retrospective Study. BMC Oral Health 2022, 22, 399. [Google Scholar] [CrossRef]
- Uzun Saylan, B.C.; Baydar, O.; Yeşilova, E.; Kurt Bayrakdar, S.; Bilgir, E.; Bayrakdar, İ.Ş.; Çelik, Ö.; Orhan, K. Assessing the Effectiveness of Artificial Intelligence Models for Detecting Alveolar Bone Loss in Periodontal Disease: A Panoramic Radiograph Study. Diagnostics 2023, 13, 1800. [Google Scholar] [CrossRef]
- Karacaoglu, F.; Kolsuz, M.E.; Bagis, N.; Evli, C.; Orhan, K. Development and Validation of Intraoral Periapical Radiography-Based Machine Learning Model for Periodontal Defect Diagnosis. Proc. Inst. Mech. Eng. H 2023, 237, 607–618. [Google Scholar] [CrossRef]
- Chau, R.C.W.; Li, G.-H.; Tew, I.M.; Thu, K.M.; McGrath, C.; Lo, W.-L.; Ling, W.-K.; Hsung, R.T.-C.; Lam, W.Y.H. Accuracy of Artificial Intelligence-Based Photographic Detection of Gingivitis. Int. Dent. J. 2023, 73, 724–730. [Google Scholar] [CrossRef]
- Hamsini, V.; Raghini, R.; Rajshri, R.; Razwia, F.D.; Sivakumar, M.; Sivakumar, G.; Madhan, C.G. Artificial Intelligence in Dentistry. Int. J. Head Neck Pathol. 2024, 7, 7–14. [Google Scholar] [CrossRef]
- Pitchika, V.; Büttner, M.; Schwendicke, F. Artificial Intelligence and Personalized Diagnostics in Periodontology: A Narrative Review. Periodontology 2000 2024, 95, 220–231. [Google Scholar] [CrossRef]
- Certosimo, F.; Walton, M.; Hartzell, D.; Farris, J. Clinical evaluation of the efficacy of three nitrous oxide scavenging units during dental treatment. Gen. Dent. 2002, 50, 430–435. [Google Scholar]
- Singh, T.; Ghimire, T.R.; Agrawal, S.K. Awareness of Biomedical Waste Management in Dental Students in Different Dental Colleges in Nepal. BioMed Res. Int. 2018, 2018, 1742326. [Google Scholar] [CrossRef]
- World Health Organization. COP28 UAE Declaration on Climate and Health. Available online: https://www.who.int/publications/m/item/cop28-uae-declaration-on-climate-and-health (accessed on 2 August 2025).
- NHS England. Delivering a ‘Net Zero’ National Health Service. Available online: https://www.england.nhs.uk/greenernhs/publication/delivering-a-net-zero-national-health-service/ (accessed on 2 August 2025).
- Dragan, I.F.; Hamza, T.; McAndrew, M. Integrating Digital Scholarship in Dental Education: Why, What, and How? J. Dent. Educ. 2022, 86, 543–545. [Google Scholar] [CrossRef]
- Pironti, C.; Dell’Annunziata, F.; Giugliano, R.; Folliero, V.; Galdiero, M.; Ricciardi, M.; Motta, O.; Proto, A.; Franci, G. Comparative Analysis of Peracetic Acid (PAA) and Permaleic Acid (PMA) in Disinfection Processes. Sci. Total Environ. 2021, 797, 149206. [Google Scholar] [CrossRef]
- Shinde, S.; Folliero, V.; Chianese, A.; Zannella, C.; De Filippis, A.; Rosati, L.; Prisco, M.; Falanga, A.; Mali, A.; Galdiero, M.; et al. Synthesis of Chitosan-Coated Silver Nanoparticle Bioconjugates and Their Antimicrobial Activity against Multidrug-Resistant Bacteria. Appl. Sci. 2021, 11, 9340. [Google Scholar] [CrossRef]
- Quttainah, M.A.; Singh, P. Barriers to Sustainable Healthcare Waste Management: A Grey Method Approach for Barrier Ranking. Sustainability 2024, 16, 11285. [Google Scholar] [CrossRef]
- Abhishek, K.N.; Supreetha, S.; Varma Penumatsa, N.; Sam, G.; Khanapure, S.C.; Sivarajan, S. Awareness-Knowledge and Practices of Dental Waste Management among Private Practitioners. Kathmandu Univ. Med. J. (KUMJ) 2016, 14, 17–21. [Google Scholar]
- Grose, J.; Richardson, J.; Mills, I.; Moles, D.; Nasser, M. Exploring Attitudes and Knowledge of Climate Change and Sustainability in a Dental Practice: A Feasibility Study into Resource Management. Br. Dent. J. 2016, 220, 187–191. [Google Scholar] [CrossRef]
- Nasser, M. Evidence Summary: Can Plastics Used in Dentistry Act as an Environmental Pollutant? Can We Avoid the Use of Plastics in Dental Practice? Br. Dent. J. 2012, 212, 89–91. [Google Scholar] [CrossRef]
- Duane, B.; Ramasubbu, D.; Harford, S.; Steinbach, I.; Stancliffe, R.; Croasdale, K.; Pasdeki-Clewer, E. Environmental Sustainability and Procurement: Purchasing Products for the Dental Setting. Br. Dent. J. 2019, 226, 453–458. [Google Scholar] [CrossRef]
- Kapoor, D.; Nirola, A.; Kapoor, V.; Gambhir, R.S. Knowledge and Awareness Regarding Biomedical Waste Management in Dental Teaching Institutions in India—A Systematic Review. J. Clin. Exp. Dent. 2014, 6, e419. [Google Scholar] [CrossRef]
- Al-Khatib, I.A.; Monou, M.; Mosleh, S.A.; Al-Subu, M.M.; Kassinos, D. Dental Solid and Hazardous Waste Management and Safety Practices in Developing Countries: Nablus District, Palestine. Res. J. Sustain. Circ. Econ. 2010, 28, 436–444. [Google Scholar] [CrossRef]
- Kamble, B.D.; Tompe, P.P.; Pande, N.A.; Radke, U.M.; Acharya, B.P. A systematic review to evaluate knowledge, attitude, and practice regarding biomedical waste management among dental teaching institutions and private practitioners in Asian countries. J. Int. Soc. Prev. Community Dent. 2020, 10, 531–539. [Google Scholar] [CrossRef]
- Choudhary, M.; Verma, M.; Ghosh, S.; Dhillon, J. Assessment of Knowledge and Awareness about Biomedical Waste Management among Health Care Personnel in a Tertiary Care Dental Facility in Delhi. Indian J. Dent. Res. 2020, 31, 26. [Google Scholar] [CrossRef]
- Sudhakar, V.; Chandrashekar, J. Dental Health Care Waste Disposal among Private Dental Practices in Bangalore City, India. Int. Dent. J. 2008, 58, 51–54. [Google Scholar] [CrossRef]
- Pisano, M.; Bramanti, A.; Menditti, D.; Sangiovanni, G.; Santoro, R.; Amato, A. Modern Approaches to Providing Telematics Oral Health Services in Pediatric Dentistry: A Narrative Review. Appl. Sci. 2023, 13, 8331. [Google Scholar] [CrossRef]
- Khatri, S.; Nand, D.; Kontio, K.; Ohannessian, R.; Rafai, E.; Zibran, A.; Seavula, K.B.; Susau, J. Implementation of Low-Cost Teledentistry with Low-Resource Settings During the COVID-19 Pandemic in Fiji. Asia Pac. J. Public Health 2022, 34, 885–886. [Google Scholar] [CrossRef] [PubMed]
- Bessadet, M.; Drancourt, N.; El Osta, N. Time Efficiency and Cost Analysis between Digital and Conventional Workflows for the Fabrication of Fixed Dental Prostheses: A Systematic Review. J. Prosthet. Dent. 2025, 133, 71–84. [Google Scholar] [CrossRef] [PubMed]
- Duane, B.; Hyland, J.; Rowan, J.S.; Archibald, B. Taking a Bite out of Scotland’s Dental Carbon Emissions in the Transition to a Low Carbon Future. Public Health 2012, 126, 770–777. [Google Scholar] [CrossRef] [PubMed]
- Macrì, M.; D’Albis, V.; Marciani, R.; Nardella, M.; Festa, F. Towards Sustainable Orthodontics: Environmental Implications and Strategies for Clear Aligner Therapy. Materials 2024, 17, 4171. [Google Scholar] [CrossRef]

| Region | Sub- Region | Competent Authority | Essential Requirements | Traceability | Transport Regulations | Key Notes | Practical Management and Concern | References |
|---|---|---|---|---|---|---|---|---|
| Europe | EU (Member States) | European Commission; national environment/health ministries | Source separation; waste management hierarchy | Mandatory records (varies by country) | ADR; Waste Shipments Regulation | Implementation varies among Member States | Widespread use of two-/three-bin systems (infectious, sharps, general waste); steam sterilization (autoclave) and high-temperature incineration for infectious waste and expired pharmaceuticals | (https://eur-lex.europa.eu/eli/dir/2008/98/oj/eng, accessed on 9 August 2025) |
| Non-EU European countries (e.g., UK, Switzerland, Norway) | National/federal environment ministries | Mandatory separation and treatment | National manifest systems | ADR (for international transport) | Similar to EU practices but adapted to the local subregion | Similar to EU practices; higher prevalence of contracts with certified private operators; frequent use of microwave treatment in the UK | (https://www.fedlex.admin.ch/eli/cc/2015/891/en?print=true&version=20250422; https://www.legislation.gov.uk/uksi/2024/1281/made; https://www.legislation.gov.uk/uksi/2012/811/pdfs/uksics_20120811_en.pdf, accessed on 9 August 2025) | |
| Americas | North America (USA, Canada) | EPA; state/provincial agencies | Autoclaving, licensed incineration | Manifest in many states/provinces | DOT/PHMSA (USA); provinci al rules (Canada) | No single strong federal framework | USA: extensive use of centralized facilities for autoclaving/shredding; Canada: often hospital-based treatment followed by disposal in controlled landfills or incinerators | (https://www.cdc.gov/infection-control/hcp/environmental-control/regulated-medical-waste.html; https://www.epa.gov/rcra/model-guidelines-state-medical-waste-management; https://biosecuritycentral.org/resource/requirements-and-protocols/canadian-biosafety-standard/, accessed on 9 August 2025) |
| Latin America (e.g., Brazil, Mexico, Argentina) | National health/environment ministries | Separation, sterilization, or incineration | Manifest required in many countries | National rules + ADR if exported | Enforcement varies; infrastructure challenges | Brazil and Mexico: frequent use of dedicated incineration facilities; rural areas still see burial or burning in rudimentary furnaces | (https://ampeid.org/documents/brazil/resolution-conama-no-358-ruling-on-final-disposal-of-waste-originated-from-sanitary-services/; https://conama.mma.gov.br/images/conteudo/CONAMA-ingles.pdf, accessed on 9 August 2025) | |
| Asia | East Asia (Japan, Republic of Korea, China) | National environment; health ministries | Separation, licensed facilities, autoclave/incineration | Manifest mandatory | National transport rules | Generally robust enforcement | Japan/Korea: sealed rigid containers; mandatory autoclaving for infectious waste; incineration for pharmaceuticals and anatomical waste; China: increasing number of provincial sterilization facilities | (https://www.env.go.jp/en/laws/recycle/01.pdf; https://elaw.klri.re.kr/eng_service/lawView.do?hseq=48601&lang=ENG, accessed on 9 August 2025) |
| South Asia (India, Bangladesh, Pakistan) | National health/environment ministries | Separation; treatment within 48 h | Manifest mandatory in India | National transport rules | Gap between regulations and actual practice | India: color-coded segregation (yellow, red, blue, black) followed by autoclaving/incineration; in smaller centers, open burning still common | (https://dhr.gov.in/sites/default/files/Bio-medical_Waste_Management_Rules_2016.pdf; https://cpcb.nic.in/uploads/projects/bio-medical-waste/guidelines_healthcare_june_2018.pdf, accessed on 9 August 2025) | |
| Southeast Asia (e.g., Thailand, Malaysia, Vietnam) | National health/environment ministries | Separation; incineration/autoclave | Manifest not always mandatory | National transport rules | Technical capacity varies | Thailand: in-house hospital incinerators; Malaysia/Vietnam: mix of autoclaving and controlled landfilling; rural areas face major gaps | (https://www.ratchakitcha.soc.go.th/DATA/PDF/2564/A/014/T_0015.PDF; accessed on 9 August 2025) [42] | |
| Africa | North Africa (e.g., Egypt, Morocco, Tunisia) | National health/environment ministries | Separation; management in licensed facilities | Manifest requirements vary | National transport rules | Implementation hindered by limited resources | Egypt: mostly hospital-based incinerators; Morocco: regional plans for mobile autoclaves and centralized collection | (https://faolex.fao.org/docs/pdf/egy4986E.pdf; https://adsero.me/waste-management-executive-regulations-amendments-prime-ministers-decrees-no-1113-and-no-1114-of-2024/?utm_source=chatgpt.com, accessed on 9 August 2025) |
| Sub-Saharan Africa (e.g., South Africa, Kenya) | National health/environment ministries | Separation; management in licensed facilities | Manifest requirements vary | National transport rules | Infrastructure gaps; WHO often provides support | South Africa: certified private operators with autoclaving/shredding; Kenya: low-tech incinerators and landfill disposal | (https://faolex.fao.org/docs/pdf/saf138344.pdf; https://www.informea.org/en/legislation/regulations-relating-health-care-waste-management-health-establishments-2014-gn-r-no-375?utm_source=chatgpt.com, accessed on 9 August 2025) |
| Dental Procedure and Activities/Source | Estimated Environmental Impact | Estimated Impact of Sustainable Alternatives |
|---|---|---|
| Dental procedure and activities | ||
| Clinical examinations [9] | 27.08% of the total carbon footprint of the dental practice 5.50 kgCO2e/procedure 181,433 TCO2e/year | |
| Radiographs [9] | 6.41% of the total carbon footprint of the dental practice 5.50 kgCO2e/procedure 42,930 TCO2e/year | |
| Non-surgical periodontal therapy [9] | 13.5% of the total carbon footprint of the dental practice 6.53 kgCO2e/procedure 90,087 TCO2e/year | |
| Surgical periodontal therapy | No available data | |
| Extractions (hopeless teeth) [9] | 3.54% of the total carbon footprint of the dental practice 8.58 kgCO2e/procedure 23,744 TCO2e/year | |
| Nitrous oxide use [9,62] | 0.9% of the total annual carbon footprint emission 119.00 kgCO2e/procedure 5829 TCO2e/year | Nitrous oxide scavenging system: −71–91% of the waste of indoor nitrous oxide compared to no scavenging system |
| Travel [9,20,32] (https://gitnux.org/sustainability-in-the-dental-industry-statistics/, accessed on 13 August 2025) | 64.5% of the total annual carbon footprint emission: Patient travel 31.1%, Dental staff travel 30.3% Work-related dental staff travel 3.1% | Teledentistry for follow-ups/consultations: −60% travel-related emissions Digital workflows: −15% patient travel-related emissions |
| Procurement (materials and services) [9] | 19.0% of the total annual carbon footprint emission | |
| Source | ||
| Energy and Gas [9] (https://gitnux.org/sustainability-in-the-dental-industry-statistics/, accessed on 13 August 2025) | 15.3% of the total annual carbon footprint emission Autoclave 9.68 kWh/day Compressor: 2.04 kWh/day Operatory lighting: 1.20 kWh/day Ultrasonic scaler: 0.79 kWh/day Dental suction system: 0.29 kWh/day | LED lighting: −75% electricity use compared to halogen Eco-friendly sterilization chemicals: −85% of high-volatile organic compounds emissions |
| Water [9,24,25] (https://gitnux.org/sustainability-in-the-dental-industry-statistics/, accessed on 13 August 2025) | 0.1% of the total annual carbon footprint emission | Water-saving dental units: −20–30% water use Dry vacuum: −85% water use compared to wet-ring vacuum Digital impressions: −50% of waste compared to traditional impressions |
| Waste [9,35] (https://gitnux.org/sustainability-in-the-dental-industry-statistics/, accessed on 13 August 2025) | 0.2% of the total annual carbon footprint emission 2–5 tons annually Plastic waste: about 34% Nitrile waste: about 15% Paper waste: about 12% of the total solid dental waste | Paperless digital records: –10,000 sheets/year per practice 3D-printing technologies: −25% of supply chain waste |
| Strategy Area | Key Actions in Dental Practice | Specific Actions in Periodontal Practice |
|---|---|---|
| Resource Efficiency (Energy and Water) [3,17,18,19,20,24,25,27] |
|
|
| Air Pollution and Emissions Reduction [12,28,29,33] |
|
|
| Recycling and Waste Management [33,34,39,40,41] |
|
|
| Digitalization and Smart Technologies [3,17,38,46,47,49,50,53] |
|
|
| Education and Community Awareness [13,14,43,44,45,63] |
|
|
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Di Spirito, F.; Giordano, F.; Di Palo, M.P.; De Benedetto, G.; Aulisio, L.; Boccia, G. Sustainable Dental and Periodontal Practice: A Narrative Review on the 4R-Framework—Reduce, Reuse, Rethink, Recycle—And Waste Management Rationalization. Dent. J. 2025, 13, 392. https://doi.org/10.3390/dj13090392
Di Spirito F, Giordano F, Di Palo MP, De Benedetto G, Aulisio L, Boccia G. Sustainable Dental and Periodontal Practice: A Narrative Review on the 4R-Framework—Reduce, Reuse, Rethink, Recycle—And Waste Management Rationalization. Dentistry Journal. 2025; 13(9):392. https://doi.org/10.3390/dj13090392
Chicago/Turabian StyleDi Spirito, Federica, Francesco Giordano, Maria Pia Di Palo, Giuseppina De Benedetto, Leonardo Aulisio, and Giovanni Boccia. 2025. "Sustainable Dental and Periodontal Practice: A Narrative Review on the 4R-Framework—Reduce, Reuse, Rethink, Recycle—And Waste Management Rationalization" Dentistry Journal 13, no. 9: 392. https://doi.org/10.3390/dj13090392
APA StyleDi Spirito, F., Giordano, F., Di Palo, M. P., De Benedetto, G., Aulisio, L., & Boccia, G. (2025). Sustainable Dental and Periodontal Practice: A Narrative Review on the 4R-Framework—Reduce, Reuse, Rethink, Recycle—And Waste Management Rationalization. Dentistry Journal, 13(9), 392. https://doi.org/10.3390/dj13090392







