Post-Cardiac Arrest: Mechanisms, Management, and Future Perspectives
Abstract
1. Introduction
2. Physiopathology
2.1. Systemic Process of Ischemia and Reperfusion
2.2. Brain Injury
2.3. Myocardial Injury
2.4. Other Organs
3. Investigating the Etiology of Cardiac Arrest
4. Post-Resuscitation Shock
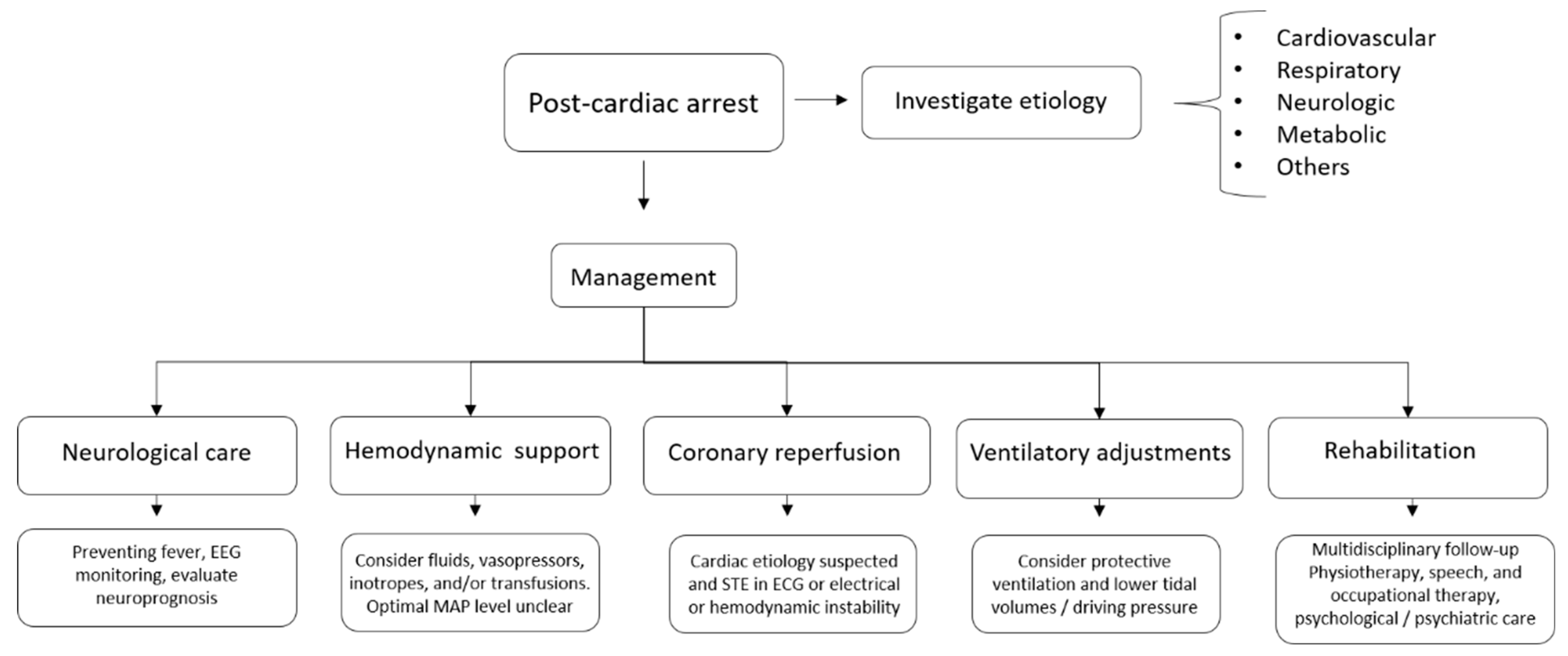
5. Post-Cardiac Arrest Care
5.1. Neurologic Care
5.1.1. Active Temperature Management
5.1.2. Monitoring
5.1.3. Neuroprognosis
5.2. Hemodynamic Support
5.3. Coronary Reperfusion
5.4. Ventilatory Management
5.5. Other Measures
5.6. Future Perspectives
5.7. Rehabilitation
6. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Nolan, J.P.; Soar, J.; Zideman, D.A.; Biarent, D.; Bossaert, L.L.; Deakin, C.; Koster, R.W.; Wyllie, J.; Böttiger, B. European Resuscitation Council Guidelines for Resuscitation 2010 Section 1. Executive summary. Resuscitation 2010, 81, 1219–1276. [Google Scholar] [CrossRef] [PubMed]
- Chan, P.S.; McNally, B.; Tang, F.; Kellermann, A. Recent Trends in Survival from Out-of-Hospital Cardiac Arrest in the United States. Circulation 2014, 130, 1876–1882. [Google Scholar] [CrossRef] [PubMed]
- Girotra, S.; Nallamothu, B.K.; Spertus, J.A.; Li, Y.; Krumholz, H.M.; Chan, P.S. Trends in Survival after In-Hospital Cardiac Arrest. N. Engl. J. Med. 2012, 367, 1912–1920. [Google Scholar] [CrossRef]
- Nolan, J.P.; Neumar, R.W.; Adrie, C.; Aibiki, M.; Berg, R.A.; Böttiger, B.W.; Callaway, C.; Clark, R.S.; Geocadin, R.G.; Jauch, E.C.; et al. Post-cardiac arrest syndrome: Epidemiology, pathophysiology, treatment, and prognostication: A Scientific Statement from the International Liaison Committee on Resuscitation; the American Heart Association Emergency Cardiovascular Care Committee; the Council on Cardiovascular Surgery and Anesthesia; the Council on Cardiopulmonary, Perioperative, and Critical Care; the Council on Clinical Cardiology; the Council on Stroke. Resuscitation 2008, 79, 350–379. [Google Scholar] [CrossRef]
- Eltzschig, H.K.; Eckle, T. Ischemia and reperfusion—From mechanism to translation. Nat. Med. 2011, 17, 1391–1401. [Google Scholar] [CrossRef] [PubMed]
- Mongardon, N.; Dumas, F.; Ricome, S.; Grimaldi, D.; Hissem, T.; Pène, F.; Cariou, A. Postcardiac arrest syndrome: From immediate resuscitation to long-term outcome. Ann. Intensiv. Care 2011, 1, 45. [Google Scholar] [CrossRef] [PubMed]
- Bralet, J.; Beley, P.; Jemaa, R.; Bralet, A.M.; Beley, A. Lipid metabolism, cerebral metabolic rate, and some related enzyme activities after brain infarction in rats. Stroke 1987, 18, 418–425. [Google Scholar] [CrossRef]
- Traystman, R.J.; Kirsch, J.R.; Koehler, R.C. Oxygen radical mechanisms of brain injury following ischemia and reperfusion. J. Appl. Physiol. 1991, 71, 1185–1195. [Google Scholar] [CrossRef]
- Lipton, P. Ischemic Cell Death in Brain Neurons. Physiol. Rev. 1999, 79, 1431–1568. [Google Scholar] [CrossRef]
- Morley, P.; Hogan, M.J.; Hakim, A.M. Calcium-Mediated Mechanisms of Ischemic Injury and Protection. Brain Pathol. 2008, 4, 37–47. [Google Scholar] [CrossRef]
- Adrie, C.; Laurent, I.; Monchi, M.; Cariou, A.; Dhainaou, J.F.; Spaulding, C. Postresuscitation disease after cardiac arrest: A sepsis-like syndrome? Curr. Opin. Crit. Care 2004, 10, 208–212. [Google Scholar] [CrossRef] [PubMed]
- Huet, O.; Dupic, L.; Batteux, F.; Matar, C.; Conti, M.; Chereau, C.; Lemiale, V.; Harrois, A.; Mira, J.-P.; Vicaut, E.; et al. Postresuscitation syndrome: Potential role of hydroxyl radical-induced endothelial cell damage. Crit. Care Med. 2011, 39, 1712–1720. [Google Scholar] [CrossRef] [PubMed]
- Grenz, A.; Homann, D.; Eltzschig, H.K. Extracellular Adenosine: A Safety Signal That Dampens Hypoxia-Induced Inflammation during Ischemia. Antioxidants Redox Signal. 2011, 15, 2221–2234. [Google Scholar] [CrossRef] [PubMed]
- Swirski, F.K.; Nahrendorf, M.; Etzrodt, M.; Wildgruber, M.; Cortez-Retamozo, V.; Panizzi, P.; Figueiredo, J.-L.; Kohler, R.H.; Chudnovskiy, A.; Waterman, P.; et al. Identification of splenic reservoir monocytes and their deployment to inflammatory sites. Science 2009, 325, 612–616. [Google Scholar] [CrossRef]
- Yilmaz, G.; Arumugam, T.V.; Stokes, K.Y.; Granger, D.N. Role of T lymphocytes and interferon-gamma in ischemic stroke. Circulation 2006, 113, 2105–2112. [Google Scholar] [CrossRef]
- Yang, Z.; Day, Y.-J.; Toufektsian, M.-C.; Ramos, S.I.; Marshall, M.; Wang, X.-Q.; French, B.A.; Linden, J. Infarct-Sparing Effect of A 2A -Adenosine Receptor Activation Is Due Primarily to Its Action on Lymphocytes. Circulation 2005, 111, 2190–2197. [Google Scholar] [CrossRef]
- Day, Y.J.; Huang, L.; Ye, H.; Li, L.; Linden, J.; Okusa, M.D. Renal ischemia-reperfusion injury and adenosine 2A receptor-mediated tissue protection: The role of CD4+ T cells and IFN-gamma. J. Immunol. Baltim. 2006, 176, 3108–3114. [Google Scholar] [CrossRef]
- Shichita, T.; Sugiyama, Y.; Ooboshi, H.; Sugimori, H.; Nakagawa, R.; Takada, I.; Iwaki, T.; Okada, Y.; Iida, M.; Cua, D.J.; et al. Pivotal role of cerebral interleukin-17-producing gammadeltaT cells in the delayed phase of ischemic brain injury. Nat. Med. 2009, 15, 946–950. [Google Scholar] [CrossRef]
- Ricklin, D.; Hajishengallis, G.; Yang, K.; Lambris, J.D. Complement: A key system for immune surveillance and homeostasis. Nat. Immunol. 2010, 11, 785–797. [Google Scholar] [CrossRef]
- Vinten-Johansen, J.; Sato, H.; Zhao, Z.Q. The role of nitric oxide and NO-donor agents in myocardial protection from surgical ischemic-reperfusion injury. Int. J. Cardiol. 1995, 50, 273–281. [Google Scholar] [CrossRef]
- Adams, J.A. Endothelium and cardiopulmonary resuscitation. Crit. Care Med. 2006, 34, S458–S465. [Google Scholar] [CrossRef] [PubMed]
- Eckle, T.; Faigle, M.; Grenz, A.; Laucher, S.; Thompson, L.F.; Eltzschig, H.K. A2B adenosine receptor dampens hypoxia-induced vascular leak. Blood 2008, 111, 2024–2035. [Google Scholar] [CrossRef] [PubMed]
- Morote-Garcia, J.C.; Rosenberger, P.; Kuhlicke, J.; Eltzschig, H.K. HIF-1–dependent repression of adenosine kinase attenuates hypoxia-induced vascular leak. Blood 2008, 111, 5571–5580. [Google Scholar] [CrossRef] [PubMed]
- Adrie, C.; Monchi, M.; Laurent, I.; Um, S.; Yan, S.B.; Thuong, M.; Cariou, A.; Charpentier, J.; Dhainaut, J.F. Coagulopathy After Successful Cardiopulmonary Resuscitation Following Cardiac Arrest: Implication of the Protein C Anticoagulant Pathway. J. Am. Coll. Cardiol. 2005, 46, 21–28. [Google Scholar] [CrossRef] [PubMed]
- Pearson, P.J.; Schaff, H.V.; Vanhoutte, P.M. Acute impairment of endothelium-dependent relaxations to aggregating platelets following reperfusion injury in canine coronary arteries. Circ. Res. 1990, 67, 385–393. [Google Scholar] [CrossRef] [PubMed]
- Cattan, S.; Drobinski, G.; Artigou, J.-Y.; Grogogeat, Y.; Cabrol, C. Coronary artery spasm in a transplant patient. Eur. Heart J. 1988, 9, 557–560. [Google Scholar] [CrossRef]
- Eltzschig, H.K.; Collard, C.D. Vascular ischaemia and reperfusion injury. Br. Med. Bull. 2004, 70, 71–86. [Google Scholar] [CrossRef]
- Ray, P.D.; Huang, B.-W.; Tsuji, Y. Reactive oxygen species (ROS) homeostasis and redox regulation in cellular signaling. Cell. Signal. 2012, 24, 981–990. [Google Scholar] [CrossRef]
- Phaniendra, A.; Jestadi, D.B.; Periyasamy, L. Free Radicals: Properties, Sources, Targets, and Their Implication in Various Diseases. Indian J. Clin. Biochem. 2015, 30, 11–26. [Google Scholar] [CrossRef]
- Kim, H.; Yun, J.; Kwon, S.-M. Therapeutic Strategies for Oxidative Stress-Related Cardiovascular Diseases: Removal of Excess Reactive Oxygen Species in Adult Stem Cells. Oxidative Med. Cell. Longev. 2016, 2016, 1–11. [Google Scholar] [CrossRef]
- Halliwell, B. Oxidants and human disease: Some new concepts. FASEB J. 1987, 1, 358–364. [Google Scholar] [CrossRef] [PubMed]
- Nagase, M.; Sakurai, A.; Sugita, A.; Matsumoto, N.; Kubo, A.; Miyazaki, Y.; Kinoshita, K.; Yamamoto, Y. Oxidative stress and abnormal cholesterol metabolism in patients with post-cardiac arrest syndrome. J. Clin. Biochem. Nutr. 2017, 61, 108–117. [Google Scholar] [CrossRef] [PubMed]
- Hotchkiss, R.S.; Strasser, A.; McDunn, J.E.; Swanson, P.E. Cell Death. N. Engl. J. Med. 2009, 361, 1570–1583. [Google Scholar] [CrossRef] [PubMed]
- Kumar, V.; Abbas, A.K.; Aster, J.C.; Coana, C. Robbins Patologia Básica, 9th ed.; Elsevier: Rio de Janeiro, Brazil, 2013. [Google Scholar]
- Tait, S.W.G.; Ichim, G.; Green, D.R. Die another way—Non-apoptotic mechanisms of cell death. J. Cell Sci. 2014, 127, 2135–2144. [Google Scholar] [CrossRef] [PubMed]
- Pessayre, D.; Mansouri, A.; Haouzi, D.; Fromenty, B. Hepatotoxicity due to mitochondrial dysfunction. Cell Biol. Toxicol. 1999, 15, 367–373. [Google Scholar] [CrossRef]
- Kristián, T.; Siesjö, B.K. Calcium in Ischemic Cell Death. Stroke 1998, 29, 705–718. [Google Scholar] [CrossRef]
- Laver, S.; Farrow, C.; Turner, D.; Nolan, J. Mode of death after admission to an intensive care unit following cardiac arrest. Intensiv. Care Med. 2004, 30, 2126–2128. [Google Scholar] [CrossRef]
- Perkins, G.D.; Callaway, C.W.; Haywood, K.; Neumar, R.W.; Lilja, G.; Rowland, M.J.; Sawyer, K.N.; Skrifvars, M.B.; Nolan, J.P. Brain injury after cardiac arrest. Lancet 2021, 398, 1269–1278. [Google Scholar] [CrossRef]
- Almeida, A.; Esteban, M.D.; Bolanos, J.; Medina, J.M. Oxygen and glucose deprivation induces mitochondrial dysfunction and oxidative stress in neurones but not in astrocytes in primary culture. J. Neurochem. 2002, 81, 207–217. [Google Scholar] [CrossRef]
- Anderson, M.F.; Sims, N.R. Mitochondrial Respiratory Function and Cell Death in Focal Cerebral Ischemia. J. Neurochem. 2001, 73, 1189–1199. [Google Scholar] [CrossRef]
- Liu, Y.; Rosenthal, R.E.; Haywood, Y.; Miljkovic-Lolic, M.; Vanderhoek, J.Y.; Fiskum, G. Normoxic Ventilation After Cardiac Arrest Reduces Oxidation of Brain Lipids and Improves Neurological Outcome. Stroke 1998, 29, 1679–1686. [Google Scholar] [CrossRef] [PubMed]
- White, B.C.; Daya, A.; DeGracia, D.J.; O’Neil, B.J.; Skjaerlund, J.M.; Trumble, S.; Krause, G.S. Fluorescent histochemical localization of lipid peroxidation during brain reperfusion following cardiac arrest. Acta Neuropathol. 1993, 86, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Zhang, Z.; Chopp, M.; Goussev, A.; Powers, C. Cerebral vessels express interleukin 1beta after focal cerebral ischemia. Brain Res. 1998, 784, 210–217. [Google Scholar] [CrossRef] [PubMed]
- Liu, T.; McDonnell, P.C.; Young, P.R.; White, R.F.; Siren, A.L.; Hallenbeck, J.M.; Barone, F.C.; Feurestein, G.Z. Interleukin-1 beta mRNA expression in ischemic rat cortex. Stroke 1993, 24, 1746–1750. [Google Scholar] [CrossRef] [PubMed]
- Sairanen, T.R.; Lindsberg, P.J.; Brenner, M.; Sirén, A.L. Global forebrain ischemia results in differential cellular expression of interleukin-1beta (IL-1beta) and its receptor at mRNA and protein level. J. Cereb. Blood Flow Metab. 1997, 17, 1107–1120. [Google Scholar] [CrossRef]
- Sekhon, M.S.; Ainslie, P.N.; Griesdale, D.E. Clinical pathophysiology of hypoxic ischemic brain injury after cardiac arrest: A “two-hit” model. Crit. Care 2017, 21, 1–10. [Google Scholar] [CrossRef]
- Panchal, A.R.; Bartos, J.A.; Cabañas, J.G.; Donnino, M.W.; Drennan, I.R.; Hirsch, K.G.; Kudenchuk, P.J.; Kurz, M.C.; Lavonas, E.J.; Morley, P.T.; et al. Part 3: Adult Basic and Advanced Life Support: 2020 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation 2020, 142, S366–S468. [Google Scholar] [CrossRef]
- Hare, G.M.T.; Mazer, C.D.; Hutchison, J.S.; McLaren, A.T.; Liu, E.; Rassouli, A.; Ai, J.; Shaye, R.E.; Lockwood, J.A.; Hawkins, C.E.; et al. Severe hemodilutional anemia increases cerebral tissue injury following acute neurotrauma. J. Appl. Physiol. 2007, 103, 1021–1029. [Google Scholar] [CrossRef]
- Calle, P.; Buylaert, W.; Vanhaute, O.; The Cerebral Resuscitation Study Group. Glycemia in the post-resuscitation period. Resuscitation 1989, 17, S181–S188. [Google Scholar] [CrossRef]
- Müllner, M.; Sterz, F.; Binder, M.; Schreiber, W.; Deimel, A.; Laggner, A.N. Blood Glucose Concentration after Cardiopulmonary Resuscitation Influences Functional Neurological Recovery in Human Cardiac Arrest Survivors. J. Cereb. Blood Flow Metab. 1997, 17, 430–436. [Google Scholar] [CrossRef]
- Ingvar, M. Cerebral Blood Flow and Metabolic Rate during Seizures. Ann. N. Y. Acad. Sci. 1986, 462, 194–206. [Google Scholar] [CrossRef] [PubMed]
- Hoekstra, J.W.; Rinnert, K.; Van Ligten, P.; Neumar, R.; Werman, H.A.; Brown, C.G. The effectiveness of bystander CPR in an animal model. Ann. Emerg. Med. 1990, 19, 881–886. [Google Scholar] [CrossRef] [PubMed]
- Shaffner, D.H.; Eleff, S.M.; Brambrink, A.M.; Sugimoto, H.; Izuta, M.; Koehler, R.C.; Traystman, R.J. Effect of arrest time and cerebral perfusion pressure during cardiopulmonary resuscitation on cerebral blood flow, metabolism, adenosine triphosphate recovery, and pH in dogs. Crit. Care Med. 1999, 27, 1335–1342. [Google Scholar] [CrossRef] [PubMed]
- Pulsinelli, W.A. Selective Neuronal Vulnerability: Morphological and Molecular Characteristics. Prog. Brain Res. 1985, 63, 29–37. [Google Scholar] [CrossRef] [PubMed]
- Brierley, J.B.; Meldrum, B.S.; Brown, A.W. The Threshold and Neuropathology of Cerebral “Anoxic-Ischemic” Cell Change. Arch. Neurol. 1973, 29, 367–374. [Google Scholar] [CrossRef] [PubMed]
- Blomqvist, P.; Wieloch, T. Ischemic Brain Damage in Rats following Cardiac Arrest Using a Long-Term Recovery Model. J. Cereb. Blood Flow Metab. 1985, 5, 420–431. [Google Scholar] [CrossRef]
- Taraszewska, A.; Zelman, I.B.; Ogonowska, W.; Chrzanowska, H. The pattern of irreversible brain changes after cardiac arrest in humans. Folia Neuropathol. 2002, 40, 133–141. [Google Scholar]
- Heyndrickx, G.R.; Millard, R.W.; McRitchie, R.J.; Maroko, P.R.; Vatner, S.F. Regional myocardial functional and electrophysiological alterations after brief coronary artery occlusion in conscious dogs. J. Clin. Investig. 1975, 56, 978–985. [Google Scholar] [CrossRef]
- Braunwald, E.; Kloner, R.A. The stunned myocardium: Prolonged, postischemic ventricular dysfunction. Circulation 1982, 66, 1146–1149. [Google Scholar] [CrossRef]
- Laurent, I.; Monchi, M.; Chiche, J.-D.; Joly, L.-M.; Spaulding, C.; Bourgeois, B.; Cariou, A.; Rozenberg, A.; Carli, P.; Weber, S.; et al. Reversible myocardial dysfunction in survivors of out-of-hospital cardiac arrest. J. Am. Coll. Cardiol. 2002, 40, 2110–2116. [Google Scholar] [CrossRef]
- Ruiz-Bailén, M.; de Hoyos, E.A.; Ruiz-Navarro, S.; Díaz-Castellanos, M.; Rucabado-Aguilar, L.; Gómez-Jiménez, F.J.; Martínez-Escobar, S.; Moreno, R.M.; Fierro-Rosón, J. Reversible myocardial dysfunction after cardiopulmonary resuscitation. Resuscitation 2005, 66, 175–181. [Google Scholar] [CrossRef] [PubMed]
- Chalkias, A.; Xanthos, T. Pathophysiology and pathogenesis of post-resuscitation myocardial stunning. Heart Fail. Rev. 2011, 17, 117–128. [Google Scholar] [CrossRef] [PubMed]
- Ayoub, I.M.; Kolarova, J.; Yi, Z.; Trevedi, A.; Deshmukh, H.; Lubell, D.L.; Franz, M.R.; Maldonado, F.A.; Gazmuri, R.J. Sodium-Hydrogen Exchange Inhibition during Ventricular Fibrillation: Beneficial Effects on Ischemic Contracture, Action Potential Duration, Reperfusion Arrhythmias, Myocardial Function, and Resuscitability. Circulation 2003, 107, 1804–1809. [Google Scholar] [CrossRef] [PubMed]
- Klouche, K.; Weil, M.H.; Sun, S.; Tang, W.; Povoas, H.P.; Kamohara, T.; Bisera, J. Evolution of the Stone Heart After Prolonged Cardiac Arrest. Chest 2002, 122, 1006–1011. [Google Scholar] [CrossRef]
- Gazmuri, R.J. Effects of repetitive electrical shocks on postresuscitation myocardial function. Crit. Care Med. 2000, 28, N228–N232. [Google Scholar] [CrossRef]
- Laine, G.A.; Allen, S.J. Left ventricular myocardial edema. Lymph flow, interstitial fibrosis, and cardiac function. Circ. Res. 1991, 68, 1713–1721. [Google Scholar] [CrossRef] [PubMed]
- Lopaschuk, G.D.; Ussher, J.R.; Folmes, C.D.L.; Jaswal, J.S.; Stanley, W.C. Myocardial Fatty Acid Metabolism in Health and Disease. Physiol. Rev. 2010, 90, 207–258. [Google Scholar] [CrossRef]
- Fukushima, A.; Lopaschuk, G.D. Cardiac fatty acid oxidation in heart failure associated with obesity and diabetes. Biochim. Biophys. Acta (BBA) Mol. Cell Biol. Lipids 2016, 1861, 1525–1534. [Google Scholar] [CrossRef] [PubMed]
- Kudo, N.; Barr, A.J.; Barr, R.L.; Desai, S.; Lopaschuk, G.D. High rates of fatty acid oxidation during reperfusion of ischemic hearts are associated with a decrease in malonyl-CoA levels due to an increase in 5′-AMP-activated protein kinase inhibition of acetyl-CoA carboxylase. J. Biol. Chem. 1995, 270, 17513–17520. [Google Scholar] [CrossRef]
- Koretsune, Y.; Marban, E. Cell calcium in the pathophysiology of ventricular fibrillation and in the pathogenesis of postarrhythmic contractile dysfunction. Circulation 1989, 80, 369–379. [Google Scholar] [CrossRef]
- van Alem, A.P.; Post, J.; Koster, R.W. VF recurrence: Characteristics and patient outcome in out-of-hospital cardiac arrest. Resuscitation 2003, 59, 181–188. [Google Scholar] [CrossRef] [PubMed]
- Smekal, D.; Johansson, J.; Huzevka, T.; Rubertsson, S. No difference in autopsy detected injuries in cardiac arrest patients treated with manual chest compressions compared with mechanical compressions with the LUCAS™ device—A pilot study. Resuscitation 2009, 80, 1104–1107. [Google Scholar] [CrossRef] [PubMed]
- Tang, W.; Weil, M.H.; Sun, S.; Noc, M.; Yang, L.; Gazmuri, R.J. Epinephrine Increases the Severity of Postresuscitation Myocardial Dysfunction. Circulation 1995, 92, 3089–3093. [Google Scholar] [CrossRef] [PubMed]
- Tang, W.; Weil, M.H.; Sun, S.; Jorgenson, D.; Morgan, C.; Klouche, K.; Snyder, D. The effects of biphasic waveform design on post-resuscitation myocardial function. J. Am. Coll. Cardiol. 2004, 43, 1228–1235. [Google Scholar] [CrossRef]
- Gazmuri, R.J.; Becker, J. Cardiac resuscitation. The search for hemodynamically more effective methods. Chest 1997, 111, 712–723. [Google Scholar] [CrossRef]
- Kwon, O.; Phillips, C.L.; Molitoris, B.A. Ischemia induces alterations in actin filaments in renal vascular smooth muscle cells. Am. J. Physiol. Physiol. 2002, 282, F1012–F1019. [Google Scholar] [CrossRef]
- Bonventre, J.V.; Weinberg, J.M. Recent Advances in the Pathophysiology of Ischemic Acute Renal Failure. J. Am. Soc. Nephrol. 2003, 14, 2199–2210. [Google Scholar] [CrossRef]
- Parks, D.A.; Granger, D.N. Contributions of ischemia and reperfusion to mucosal lesion formation. Am. J. Physiol. Content 1986, 250, G749–G753. [Google Scholar] [CrossRef]
- Lautt, W.W. Hepatic Vasculature: A Conceptual Review. Gastroenterology 1977, 73, 1163–1169. [Google Scholar] [CrossRef]
- Jacobsen, K.R.; Ranek, L.; Tygstrup, N. Liver Function and Blood Flow in Normal Man during Infusion of Vasopressin. Scand. J. Clin. Lab. Investig. 1969, 24, 279–284. [Google Scholar] [CrossRef]
- Roedl, K.; Spiel, A.O.; Nürnberger, A.; Horvatits, T.; Drolz, A.; Hubner, P.; Warenits, A.-M.; Sterz, F.; Herkner, H.; Fuhrmann, V. Hypoxic liver injury after in- and out-of-hospital cardiac arrest: Risk factors and neurological outcome. Resuscitation 2019, 137, 175–182. [Google Scholar] [CrossRef] [PubMed]
- Chalkias, A.; Xanthos, T. Post-cardiac arrest syndrome: Mechanisms and evaluation of adrenal insufficiency. World J. Crit. Care Med. 2012, 1, 4–9. [Google Scholar] [CrossRef] [PubMed]
- Saarinen, S.; Nurmi, J.; Toivio, T.; Fredman, D.; Virkkunen, I.; Castrén, M. Does appropriate treatment of the primary underlying cause of PEA during resuscitation improve patients’ survival? Resuscitation 2012, 83, 819–822. [Google Scholar] [CrossRef] [PubMed]
- Bergum, D.; Haugen, B.O.; Nordseth, T.; Mjølstad, O.C.; Skogvoll, E. Recognizing the causes of in-hospital cardiac arrest—A survival benefit. Resuscitation 2015, 97, 91–96. [Google Scholar] [CrossRef]
- Sonnier, M.; Rittenberger, J.C. State-of-the-art considerations in post-arrest care. J. Am. Coll. Emerg. Physicians Open 2020, 1, 107–116. [Google Scholar] [CrossRef] [PubMed]
- Khan, A.J.; Liao, C.J.; Kabir, C.; Hallak, O.; Samee, M.; Potts, S.; Klein, L.W. Etiology and Determinants of In-Hospital Survival in Patients Resuscitated After Out-of-Hospital Cardiac Arrest in an Urban Medical Center. Am. J. Cardiol. 2020, 130, 78–84. [Google Scholar] [CrossRef]
- Andersen, L.W.; Holmberg, M.J.; Berg, K.M.; Donnino, M.W.; Granfeldt, A. In-Hospital Cardiac Arrest: A Review. JAMA 2019, 321, 1200–1210. [Google Scholar] [CrossRef]
- Wallmuller, C.; Meron, G.; Kurkciyan, I.; Schober, A.; Stratil, P.; Sterz, F. Causes of in-hospital cardiac arrest and influence on outcome. Resuscitation 2012, 83, 1206–1211. [Google Scholar] [CrossRef]
- Gässler, H.; Fischer, M.; Wnent, J.; Seewald, S.; Helm, M. Outcome after pre-hospital cardiac arrest in accordance with underlying cause. Resuscitation 2019, 138, 36–41. [Google Scholar] [CrossRef]
- Ramaka, S.; Nazir, N.T.; Murthy, V.S.; Hoek, T.V.; Prabhakar, B.S.; Chodavarapu, R.; Peri, S.; Uppuleti, A.; Jatoth, R.; Murthy, S.V.; et al. Epidemiology of out-of-Hospital Cardiac Arrests, knowledge of cardiovascular disease and risk factors in a regional setting in India: The Warangal Area out-of-hospital Cardiac Arrest Registry (WACAR). Indian Heart J. 2020, 72, 517–523. [Google Scholar] [CrossRef]
- Chen, N.; Callaway, C.W.; Guyette, F.X.; Rittenberger, J.C.; Doshi, A.A.; Dezfulian, C.; Elmer, J. Arrest etiology among patients resuscitated from cardiac arrest. Resuscitation 2018, 130, 33–40. [Google Scholar] [CrossRef]
- Walker, A.C.; Johnson, N.J. Critical Care of the Post–Cardiac Arrest Patient. Cardiol. Clin. 2018, 36, 419–428. [Google Scholar] [CrossRef] [PubMed]
- Reardon, P.M.; Hickey, M.; English, S.; Hibbert, B.; Simard, T.; Hendin, A.; Yadav, K. Optimizing the Early Resuscitation After Out-of-Hospital Cardiac Arrest. J. Intensiv. Care Med. 2019, 35, 1556–1563. [Google Scholar] [CrossRef] [PubMed]
- McFadden, P.; Reynolds, J.C.; Madder, R.D.; Brown, M. Diagnostic test accuracy of the initial electrocardiogram after resuscitation from cardiac arrest to indicate invasive coronary angiographic findings and attempted revascularization: A systematic review and meta-analysis. Resuscitation 2021, 160, 20–36. [Google Scholar] [CrossRef] [PubMed]
- Baldi, E.; Schnaubelt, S.; Caputo, M.L.; Klersy, C.; Clodi, C.; Bruno, J.; Compagnoni, S.; Benvenuti, C.; Domanovits, H.; Burkart, R.; et al. Association of Timing of Electrocardiogram Acquisition After Return of Spontaneous Circulation with Coronary Angiography Findings in Patients with Out-of-Hospital Cardiac Arrest. JAMA Netw. Open 2021, 4, e2032875. [Google Scholar] [CrossRef]
- Perman, S.M.; Stanton, E.; Soar, J.; Berg, R.A.; Donnino, M.W.; Mikkelsen, M.E.; Edelson, D.P.; Churpek, M.M.; Yang, L.; Merchant, R.M.; et al. Location of In-Hospital Cardiac Arrest in the United States—Variability in Event Rate and Outcomes. J. Am. Heart Assoc. 2016, 5, e003638. [Google Scholar] [CrossRef]
- Petek, B.J.; Erley, C.L.; Kudenchuk, P.J.; Carlbom, D.; Strote, J.; Gatewood, M.O.; Shuman, W.P.; Hira, R.S.; Gunn, M.L.; Maynard, C.; et al. Diagnostic yield of non-invasive imaging in patients following non-traumatic out-of-hospital sudden cardiac arrest: A systematic review. Resuscitation 2018, 135, 183–190. [Google Scholar] [CrossRef]
- Gardner, K.F.; Clattenburg, E.J.; Wroe, P.; Singh, A.; Mantuani, D.; Nagdev, A. The Cardiac Arrest Sonographic Assessment (CASA) exam—A standardized approach to the use of ultrasound in PEA. Am. J. Emerg. Med. 2018, 36, 729–731. [Google Scholar] [CrossRef]
- Pyo, S.Y.; Park, G.J.; Kim, S.C.; Kim, H.; Lee, S.W.; Lee, J.H. Impact of the modified SESAME ultrasound protocol implementation on patients with cardiac arrest in the emergency department. Am. J. Emerg. Med. 2021, 43, 62–68. [Google Scholar] [CrossRef]
- Clattenburg, E.J.; Wroe, P.C.; Gardner, K.; Schultz, C.; Gelber, J.; Singh, A.; Nagdev, A. Implementation of the Cardiac Arrest Sonographic Assessment (CASA) protocol for patients with cardiac arrest is associated with shorter CPR pulse checks. Resuscitation 2018, 131, 69–73. [Google Scholar] [CrossRef]
- Elfwén, L.; Hildebrand, K.; Schierbeck, S.; Sundqvist, M.; Ringh, M.; Claesson, A.; Olsson, J.; Nordberg, P. Focused cardiac ultrasound after return of spontaneous circulation in cardiac-arrest patients. Resuscitation 2019, 142, 16–22. [Google Scholar] [CrossRef] [PubMed]
- Branch, K.R.; Strote, J.; Gunn, M.; Maynard, C.; Kudenchuk, P.J.; Brusen, R.; Petek, B.J.; Sayre, M.R.; Edwards, R.; Carlbom, D.; et al. Early head-to-pelvis computed tomography in out-of-hospital circulatory arrest without obvious etiology. Acad. Emerg. Med. 2021, 28, 394–403. [Google Scholar] [CrossRef] [PubMed]
- Viniol, S.; Thomas, R.P.; König, A.M.; Betz, S.; Mahnken, A.H. Early whole-body CT for treatment guidance in patients with return of spontaneous circulation after cardiac arrest. Emerg. Radiol. 2019, 27, 23–29. [Google Scholar] [CrossRef] [PubMed]
- Nolan, J.P.; Sandroni, C.; Böttiger, B.W.; Cariou, A.; Cronberg, T.; Friberg, H.; Genbrugge, C.; Haywood, K.; Lilja, G.; Moulaert, V.R.M.; et al. European Resuscitation Council and European Society of Intensive Care Medicine guidelines 2021: Post-resuscitation care. Intensiv. Care Med. 2021, 47, 369–421. [Google Scholar] [CrossRef] [PubMed]
- Negovsky, V.A. The second step in resuscitation—The treatment of the “post-resuscitation disease”. Resuscitation 1972, 1, 1–7. [Google Scholar] [CrossRef] [PubMed]
- Jozwiak, M.; Bougouin, W.; Geri, G.; Grimaldi, D.; Cariou, A. Post-resuscitation shock: Recent advances in pathophysiology and treatment. Ann. Intensiv. Care 2020, 10, 1–11. [Google Scholar] [CrossRef]
- Lemiale, V.; Dumas, F.; Mongardon, N.; Giovanetti, O.; Charpentier, J.; Chiche, J.-D.; Carli, P.; Mira, J.-P.; Nolan, J.; Cariou, A. Intensive care unit mortality after cardiac arrest: The relative contribution of shock and brain injury in a large cohort. Intensiv. Care Med. 2013, 39, 1972–1980. [Google Scholar] [CrossRef]
- Witten, L.; Gardner, R.; Holmberg, M.J.; Wiberg, S.; Moskowitz, A.; Mehta, S.; Grossestreuer, A.V.; Yankama, T.; Donnino, M.W.; Berg, K.M. Reasons for death in patients successfully resuscitated from out-of-hospital and in-hospital cardiac arrest. Resuscitation 2019, 136, 93–99. [Google Scholar] [CrossRef]
- Sandroni, C.; Dell’Anna, A.M.; Tujjar, O.; Geri, G.; Cariou, A.; Taccone, F.S. Acute Kidney Injury (AKI) after cardiac arrest: A systematic review and meta-analysis of clinical studies. Minerva Anestesiol. 2016, 82, 989–999. [Google Scholar]
- Champigneulle, B.; Geri, G.; Bougouin, W.; Dumas, F.; Arnaout, M.; Zafrani, L.; Pène, F.; Charpentier, J.; Mira, J.; Cariou, A. Hypoxic hepatitis after out-of-hospital cardiac arrest: Incidence, determinants and prognosis. Resuscitation 2016, 103, 60–65. [Google Scholar] [CrossRef]
- Oh, S.H.; Kim, H.J.; Park, K.N.; Kim, S.H.; Kim, Y.M.; Youn, C.S.; Lim, J.Y. Hypoxic hepatitis in survivors of out-of-hospital cardiac arrest. Am. J. Emerg. Med. 2015, 33, 1166–1170. [Google Scholar] [CrossRef] [PubMed]
- Jamme, M.; Salem, O.B.H.; Guillemet, L.; Dupland, P.; Bougouin, W.; Charpentier, J.; Mira, J.-P.; Pène, F.; Dumas, F.; Cariou, A.; et al. Severe metabolic acidosis after out-of-hospital cardiac arrest: Risk factors and association with outcome. Ann. Intensiv. Care 2018, 8, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Boland, T.A.; Lee, V.H.; Bleck, T.P. Stress-induced cardiomyopathy. Crit. Care Med. 2015, 43, 686–693. [Google Scholar] [CrossRef] [PubMed]
- Hausenloy, D.; Boston-Griffiths, E.; Yellon, D.M. Cardioprotection during cardiac surgery. Cardiovasc. Res. 2012, 94, 253–265. [Google Scholar] [CrossRef]
- Antonucci, E.; Fiaccadori, E.; Donadello, K.; Taccone, F.S.; Franchi, F.; Scolletta, S. Myocardial depression in sepsis: From pathogenesis to clinical manifestations and treatment. J. Crit. Care 2014, 29, 500–511. [Google Scholar] [CrossRef]
- Kern, K.B.; Hilwig, R.W.; Rhee, K.H.; Berg, R.A. Myocardial dysfunction after resuscitation from cardiac arrest: An example of global myocardial stunning. J. Am. Coll. Cardiol. 1996, 28, 232–240. [Google Scholar] [CrossRef]
- Gando, S.; Nanzaki, S.; Morimoto, Y.; Kobayashi, S.; Kemmotsu, O. Out-of-hospital cardiac arrest increases soluble vascular endothelial adhesion molecules and neutrophil elastase associated with endothelial injury. Intensiv. Care Med. 2000, 26, 38–44. [Google Scholar] [CrossRef]
- Adrie, C.; Adib-Conquy, M.; Laurent, I.; Monchi, M.; Vinsonneau, C.; Fitting, C.; Fraisse, F.; Dinh-Xuan, A.T.; Carli, P.; Spaulding, C.; et al. Successful cardiopulmonary resuscitation after cardiac arrest as a “sepsis-like” syndrome. Circulation 2002, 106, 562–568. [Google Scholar] [CrossRef]
- Mongardon, N.; Perbet, S.; Lemiale, V.; Dumas, F.; Poupet, H.; Charpentier, J.; Péne, F.; Chiche, J.-D.; Mira, J.-P.; Cariou, A. Infectious complications in out-of-hospital cardiac arrest patients in the therapeutic hypothermia era. Crit. Care Med. 2011, 39, 1359–1364. [Google Scholar] [CrossRef]
- Pene, F.; Hyvernat, H.; Mallet, V.; Cariou, A.; Carli, P.; Spaulding, C.; Dugue, M.-A.; Mira, J.-P. Prognostic value of relative adrenal insufficiency after out-of-hospital cardiac arrest. Intensiv. Care Med. 2005, 31, 627–633. [Google Scholar] [CrossRef]
- Lindner, K.H.; Haak, T.; Keller, A.; Bothner, U.; Lurie, K.G. Release of endogenous vasopressors during and after cardiopulmonary resuscitation. Heart 1996, 75, 145–150. [Google Scholar] [CrossRef] [PubMed]
- Mégarbane, B.; Leprince, P.; Deye, N.; Résière, D.; Guerrier, G.; Rettab, S.; Théodore, J.; Karyo, S.; Gandjbakhch, I.; Baud, F.J. Emergency feasibility in medical intensive care unit of extracorporeal life support for refractory cardiac arrest. Intensiv. Care Med. 2007, 33, 758–764. [Google Scholar] [CrossRef] [PubMed]
- Madder, R.D.; Reynolds, J.C. Multidisciplinary Management of the Post–Cardiac Arrest Patient. Cardiol. Clin. 2018, 36, 85–101. [Google Scholar] [CrossRef] [PubMed]
- Koistinaho, J.; Hökfelt, T. Altered gene expression in brain ischemia. NeuroReport 1997, 8, I–VIII. [Google Scholar]
- Akins, P.T.; Liu, P.K.; Hsu, C.Y. Immediate Early Gene Expression in Response to Cerebral Ischemia: Friend or foe? Stroke 1996, 27, 1682–1687. [Google Scholar] [CrossRef]
- MacManus, J.P.; Linnik, M.D. Gene Expression Induced by Cerebral Ischemia: An Apoptotic Perspective. J. Cereb. Blood Flow Metab. 1997, 17, 815–832. [Google Scholar] [CrossRef]
- Roberts, B.W.; Kilgannon, J.H.; Chansky, M.E.; Mittal, N.; Wooden, J.; Trzeciak, S. Association Between Postresuscitation Partial Pressure of Arterial Carbon Dioxide and Neurological Outcome in Patients with Post–Cardiac Arrest Syndrome. Circulation 2013, 127, 2107–2113. [Google Scholar] [CrossRef]
- Singer, M.; Young, P.J.; Laffey, J.G.; Asfar, P.; Taccone, F.S.; Skrifvars, M.B.; Meyhoff, C.S.; Radermacher, P. Dangers of hyperoxia. Crit. Care 2021, 25, 440. [Google Scholar] [CrossRef]
- Jacobi, J.; Bircher, N.; Krinsley, J.; Agus, M.; Braithwaite, S.S.; Deutschman, C.; Freire, A.X.; Geehan, D.; Kohl, B.; Nasraway, S.A.; et al. Guidelines for the use of an insulin infusion for the management of hyperglycemia in critically ill patients. Crit. Care Med. 2012, 40, 3251–3276. [Google Scholar] [CrossRef]
- Look, X.; Li, H.; Ng, M.; Lim, E.T.S.; Pothiawala, S.; Tan, K.B.K.; Sewa, D.W.; Shahidah, N.; Pek, P.P.; Ong, M.E.H. Randomized controlled trial of internal and external targeted temperature management methods in post- cardiac arrest patients. Am. J. Emerg. Med. 2017, 36, 66–72. [Google Scholar] [CrossRef]
- Hoedemaekers, C.W.; Ezzahti, M.; Gerritsen, A.; Van Der Hoeven, J.G. Comparison of cooling methods to induce and maintain normo- and hypothermia in intensive care unit patients: A prospective intervention study. Crit. Care 2007, 11, R91. [Google Scholar] [CrossRef] [PubMed]
- Tømte, Ø.; Drægni, T.; Mangschau, A.; Jacobsen, D.; Auestad, B.; Sunde, K. A comparison of intravascular and surface cooling techniques in comatose cardiac arrest survivors. Crit. Care Med. 2011, 39, 443–449. [Google Scholar] [CrossRef] [PubMed]
- Deye, N.; Cariou, A.; Girardie, P.; Pichon, N.; Megarbane, B.; Midez, P.; Tonnelier, J.-M.; Boulain, T.; Outin, H.; Delahaye, A.; et al. Response to Letter Regarding Article, “Endovascular Versus External Targeted Temperature Management for Patients with Out-of-Hospital Cardiac Arrest: A Randomized, Controlled Study”. Circulation 2016, 133, 182–193. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Bernard, S.A.; Jones, B.M.C.; Horne, M.K. Clinical Trial of Induced Hypothermia in Comatose Survivors of Out-of-Hospital Cardiac Arrest. Ann. Emerg. Med. 1997, 30, 146–153. [Google Scholar] [CrossRef] [PubMed]
- Zeiner, A.; Holzer, M.; Sterz, F.; Behringer, W.; Schörkhuber, W.; Müllner, M.; Frass, M.; Siostrzonek, P.; Ratheiser, K.; Kaff, A.; et al. Mild Resuscitative Hypothermia to Improve Neurological Outcome After Cardiac Arrest: A clinical feasibility trial. Stroke 2000, 31, 86–94. [Google Scholar] [CrossRef]
- Bernard, S.A.; Gray, T.W.; Buist, M.D.; Jones, B.M.; Silvester, W.; Gutteridge, G.; Smith, K. Treatment of Comatose Survivors of Out-of-Hospital Cardiac Arrest with Induced Hypothermia. N. Engl. J. Med. 2002, 346, 557–563. [Google Scholar] [CrossRef]
- Hypothermia after Cardiac Arrest Study Group. Mild therapeutic hypothermia to improve the neurologic outcome after cardiac arrest. N. Engl. J. Med. 2002, 346, 549–556. [Google Scholar] [CrossRef]
- Lascarrou, J.-B.; Merdji, H.; Le Gouge, A.; Colin, G.; Grillet, G.; Girardie, P.; Coupez, E.; Dequin, P.-F.; Cariou, A.; Boulain, T.; et al. Targeted Temperature Management for Cardiac Arrest with Nonshockable Rhythm. N. Engl. J. Med. 2019, 381, 2327–2337. [Google Scholar] [CrossRef]
- Blanc, A.; Colin, G.; Cariou, A.; Merdji, H.; Grillet, G.; Girardie, P.; Coupez, E.; Dequin, P.-F.; Boulain, T.; Frat, J.-P.; et al. Targeted Temperature Management After In-Hospital Cardiac Arrest. Chest 2022, 162, 356–366. [Google Scholar] [CrossRef]
- Kirkegaard, H.; Søreide, E.; De Haas, I.; Pettilä, V.; Taccone, F.S.; Arus, U.; Storm, C.; Hassager, C.; Nielsen, J.F.; Sørensen, C.A.; et al. Targeted Temperature Management for 48 vs. 24 Hours and Neurologic Outcome After Out-of-Hospital Cardiac Arrest: A Randomized Clinical Trial. JAMA 2017, 318, 341–350. [Google Scholar] [CrossRef]
- Nielsen, N.; Wetterslev, J.; Cronberg, T.; Erlinge, D.; Gasche, Y.; Hassager, C.; Horn, C.; Hovdenes, C.; Kjaergaard, J.; Kuiper, M.; et al. Targeted Temperature Management at 33 °C versus 36 °C after Cardiac Arrest. N. Engl. J. Med. 2013, 369, 2197–2206. [Google Scholar] [CrossRef] [PubMed]
- Borgquist, O.; Wise, M.P.; Nielsen, N.; Al-Subaie, N.; Cranshaw, J.; Cronberg, T.; Glover, G.; Hassager, C.; Kjaergaard, J.; Kuiper, M.; et al. Dysglycemia, Glycemic Variability, and Outcome After Cardiac Arrest and Temperature Management at 33 °C and 36 °C. Crit. Care Med. 2017, 45, 1337–1343. [Google Scholar] [CrossRef] [PubMed]
- Bro-Jeppesen, J.; Annborn, M.; Hassager, C.; Wise, M.P.; Pelosi, P.; Nielsen, N.; Erlinge, D.; Wanscher, M.; Friberg, H.; Kjaergaard, J.; et al. Hemodynamics and vasopressor support during targeted temperature management at 33 °C Versus 36 °C after out-of-hospital cardiac arrest: A post hoc study of the target temperature management trial. Crit. Care Med. 2015, 43, 318–327. [Google Scholar] [CrossRef] [PubMed]
- Lybeck, A.; Cronberg, T.; Aneman, A.; Hassager, C.; Horn, J.; Hovdenes, J.; Kjærgaard, J.; Kuiper, M.; Wanscher, M.; Stammet, P.; et al. Time to awakening after cardiac arrest and the association with target temperature management. Resuscitation 2018, 126, 166–171. [Google Scholar] [CrossRef]
- Nielsen, N. The Target Temperature for Post Cardiac Arrest Patients Should Be 36 °C. Crit. Care Med. 2017, 45, 1552–1554. [Google Scholar] [CrossRef]
- Kelly, F.E.; Nolan, J.P. The effects of mild induced hypothermia on the myocardium: A systematic review. Anaesthesia 2010, 65, 505–515. [Google Scholar] [CrossRef]
- Abazi, L.; Awad, A.; Nordberg, P.; Jonsson, M.; Taccone, F.S.; Wickerts, C.J.; Svensson, L.; Hollenberg, J.; Ringh, M.; Forsberg, S. Long-term survival in out-of-hospital cardiac arrest patients treated with targeted temperature control at 33 °C or 36 °C: A national registry study. Resuscitation 2019, 143, 142–147. [Google Scholar] [CrossRef]
- Bray, J.E.; Stub, D.; Bloom, J.E.; Segan, L.; Mitra, B.; Smith, K.; Finn, J.; Bernard, S. Changing target temperature from 33 °C to 36 °C in the ICU management of out-of-hospital cardiac arrest: A before and after study. Resuscitation 2017, 113, 39–43. [Google Scholar] [CrossRef]
- Bradley, S.M.; Liu, W.; McNally, B.; Vellano, K.; Henry, T.D.; Mooney, M.R.; Burke, M.N.; Brilakis, E.S.; Grunwald, G.K.; Adhaduk, M.; et al. Temporal Trends in the Use of Therapeutic Hypothermia for Out-of-Hospital Cardiac Arrest. JAMA Netw. Open 2018, 1, e184511. [Google Scholar] [CrossRef]
- Salter, R.; Bailey, M.; Bellomo, R.; Eastwood, G.; Goodwin, A.; Nielsen, N.; Pilcher, D.; Nichol, A.; Saxena, M.; Shehabi, Y.; et al. Changes in Temperature Management of Cardiac Arrest Patients Following Publication of the Target Temperature Management Trial. Crit. Care Med. 2018, 46, 1722–1730. [Google Scholar] [CrossRef]
- Minini, A.; Annoni, F.; Peluso, L.; Bogossian, E.; Creteur, J.; Taccone, F. Which Target Temperature for Post-Anoxic Brain Injury? A Systematic Review from “Real Life” Studies. Brain Sci. 2021, 11, 186. [Google Scholar] [CrossRef] [PubMed]
- Dankiewicz, J.; Cronberg, T.; Lilja, G.; Jakobsen, J.C.; Levin, H.; Ullén, S.; Rylander, C.; Wise, M.P.; Oddo, M.; Cariou, A.; et al. Hypothermia versus Normothermia after Out-of-Hospital Cardiac Arrest. N. Engl. J. Med. 2021, 384, 2283–2294. [Google Scholar] [CrossRef] [PubMed]
- Rittenberger, J.C.; Callaway, C.W. Temperature Management and Modern Post–Cardiac Arrest Care. N. Engl. J. Med. 2013, 369, 2262–2263. [Google Scholar] [CrossRef] [PubMed]
- Sandroni, C.; Nolan, J.P.; Andersen, L.W.; Böttiger, B.W.; Cariou, A.; Cronberg, T.; Friberg, H.; Genbrugge, C.; Lilja, G.; Morley, P.T.; et al. ERC-ESICM guidelines on temperature control after cardiac arrest in adults. Intensiv. Care Med. 2022, 48, 261–269. [Google Scholar] [CrossRef] [PubMed]
- Wyckoff, M.H.; Greif, R.; Morley, P.T.; Ng, K.C.; Olasveengen, T.M.; Singletary, E.M.; Soar, J.; Cheng, A.; Drennan, I.R.; Liley, H.G.; et al. 2022 International Consensus on Cardiopulmonary Resuscitation and Emergency Cardiovascular Care Science with Treatment Recommendations: Summary from the Basic Life Support; Advanced Life Support; Pediatric Life Support; Neonatal Life Support; Education, Implementation, and Teams; and First Aid Task Forces. Circulation 2022, 146, e483–e557. [Google Scholar] [CrossRef]
- Ruijter, B.J.; Keijzer, H.M.; Tjepkema-Cloostermans, M.C.; Blans, M.J.; Beishuizen, A.; Tromp, S.C.; Scholten, E.; Horn, J.; van Rootselaar, A.-F.; Admiraal, M.M.; et al. Treating Rhythmic and Periodic EEG Patterns in Comatose Survivors of Cardiac Arrest. N. Engl. J. Med. 2022, 386, 724–734. [Google Scholar] [CrossRef] [PubMed]
- Sandroni, C.; D’Arrigo, S.; Nolan, J.P. Prognostication after cardiac arrest. Crit. Care 2018, 22, 150. [Google Scholar] [CrossRef]
- Kern, K.B.; Hilwig, R.W.; Berg, R.A.; Rhee, K.H.; Sanders, A.B.; Otto, C.W.; Ewy, G.A. Postresuscitation Left Ventricular Systolic and Diastolic Dysfunction. Circulation 1997, 95, 2610–2613. [Google Scholar] [CrossRef]
- Vasquez, A.; Kern, K.B.; Hilwig, R.W.; Heidenreich, J.; Berg, R.A.; Ewy, G.A. Optimal dosing of dobutamine for treating post-resuscitation left ventricular dysfunction. Resuscitation 2004, 61, 199–207. [Google Scholar] [CrossRef]
- Sekhon, M.S.; Gooderham, P.; Menon, D.K.; Brasher, P.M.; Foster, D.; Cardim, D.; Czosnyka, M.; Smielewski, P.; Gupta, A.K.; Ainslie, P.N.; et al. The Burden of Brain Hypoxia and Optimal Mean Arterial Pressure in Patients with Hypoxic Ischemic Brain Injury After Cardiac Arrest. Crit. Care Med. 2019, 47, 960–969. [Google Scholar] [CrossRef]
- Ameloot, K.; Meex, I.; Genbrugge, C.; Jans, F.; Boer, W.; Verhaert, D.; Mullens, W.; Ferdinande, B.; Dupont, M.; De Deyne, C.; et al. Hemodynamic targets during therapeutic hypothermia after cardiac arrest: A prospective observational study. Resuscitation 2015, 91, 56–62. [Google Scholar] [CrossRef] [PubMed]
- Russo, J.J.; James, T.E.; Hibbert, B.; Yousef, A.; Osborne, C.; Wells, G.A.; Froeschl, M.P.; So, D.Y.; Chong, A.Y.; Labinaz, M.; et al. Impact of mean arterial pressure on clinical outcomes in comatose survivors of out-of-hospital cardiac arrest: Insights from the University of Ottawa Heart Institute Regional Cardiac Arrest Registry (CAPITAL-CARe). Resuscitation 2017, 113, 27–32. [Google Scholar] [CrossRef] [PubMed]
- Roberts, B.W.; Kilgannon, J.H.; Hunter, B.R.; Puskarich, M.A.; Shea, L.; Donnino, M.; Jones, C.; Fuller, B.M.; Kline, J.A.; Jones, A.E.; et al. Association Between Elevated Mean Arterial Blood Pressure and Neurologic Outcome After Resuscitation from Cardiac Arrest: Results from a Multicenter Prospective Cohort Study. Crit. Care Med. 2019, 47, 93–100. [Google Scholar] [CrossRef] [PubMed]
- Jakkula, P.; COMACARE study group; Pettilä, V.; Skrifvars, M.B.; Hästbacka, J.; Loisa, P.; Tiainen, M.; Wilkman, E.; Toppila, J.; Koskue, T.; et al. Targeting low-normal or high-normal mean arterial pressure after cardiac arrest and resuscitation: A randomised pilot trial. Intensiv. Care Med. 2018, 44, 2091–2101. [Google Scholar] [CrossRef] [PubMed]
- Kjaergaard, J.; Møller, J.E.; Schmidt, H.; Grand, J.; Mølstrøm, S.; Borregaard, B.; Venø, S.; Sarkisian, L.; Mamaev, D.; Jensen, L.O.; et al. Blood-Pressure Targets in Comatose Survivors of Cardiac Arrest. N. Engl. J. Med. 2022, 387, 1456–1466. [Google Scholar] [CrossRef] [PubMed]
- Ameloot, K.; Jakkula, P.; Hästbacka, J.; Reinikainen, M.; Pettilä, V.; Loisa, P.; Tiainen, M.; Bendel, S.; Birkelund, T.; Belmans, A.; et al. Optimum Blood Pressure in Patients with Shock After Acute Myocardial Infarction and Cardiac Arrest. J. Am. Coll. Cardiol. 2020, 76, 812–824. [Google Scholar] [CrossRef]
- Burstein, B.; Jentzer, J.C. Comprehensive Cardiac Care After Cardiac Arrest. Crit. Care Clin. 2020, 36, 771–786. [Google Scholar] [CrossRef]
- Elfwén, L.; Lagedal, R.; Nordberg, P.; James, S.; Oldgren, J.; Böhm, F.; Lundgren, P.; Rylander, C.; van der Linden, J.; Hollenberg, J.; et al. Direct or subacute coronary angiography in out-of-hospital cardiac arrest (DISCO)—An initial pilot-study of a randomized clinical trial. Resuscitation 2019, 139, 253–261. [Google Scholar] [CrossRef]
- Noc, M.; Fajadet, J.; Lassen, J.F.; Kala, P.; MacCarthy, P.; Olivecrona, G.K.; Windecker, S.; Spaulding, C. Invasive coronary treatment strategies for out-of-hospital cardiac arrest: A consensus statement from the European association for percutaneous cardiovascular interventions (EAPCI)/stent for life (SFL) groups. EuroIntervention 2014, 10, 31–37. [Google Scholar] [CrossRef]
- Spaulding, C.M.; Joly, L.-M.; Rosenberg, A.; Monchi, M.; Weber, S.N.; Dhainaut, J.-F.A.; Carli, P. Immediate Coronary Angiography in Survivors of Out-of-Hospital Cardiac Arrest. N. Engl. J. Med. 1997, 336, 1629–1633. [Google Scholar] [CrossRef]
- Nolan, J.P.; Deakin, C.D.; Soar, J.; Böttiger, B.W.; Smith, G. European Resuscitation Council Guidelines for Resuscitation 2005: Section 4. Adult advanced life support. Resuscitation 2005, 67, S39–S86. [Google Scholar] [CrossRef] [PubMed]
- Geri, G.; Passouant, O.; Dumas, F.; Bougouin, W.; Champigneulle, B.; Arnaout, M.; Chelly, J.; Chiche, J.-D.; Varenne, O.; Guillemet, L.; et al. Etiological diagnoses of out-of-hospital cardiac arrest survivors admitted to the intensive care unit: Insights from a French registry. Resuscitation 2017, 117, 66–72. [Google Scholar] [CrossRef] [PubMed]
- Zanuttini, D.; Armellini, I.; Nucifora, G.; Grillo, M.T.; Morocutti, G.; Carchietti, E.; Trillò, G.; Spedicato, L.; Bernardi, G.; Proclemer, A. Predictive value of electrocardiogram in diagnosing acute coronary artery lesions among patients with out-of-hospital-cardiac-arrest. Resuscitation 2013, 84, 1250–1254. [Google Scholar] [CrossRef] [PubMed]
- Kern, K.B.; Lotun, K.; Patel, N.; Mooney, M.R.; Hollenbeck, R.D.; McPherson, J.A.; McMullan, P.W.; Unger, B.; Hsu, C.H.; Seder, D.B.; et al. Outcomes of Comatose Cardiac Arrest Survivors with and without ST-Segment Elevation Myocardial Infarction: Importance of Coronary Angiography. JACC Cardiovasc. Interv. 2015, 8, 1031–1040. [Google Scholar] [CrossRef] [PubMed]
- Camuglia, A.C.; Randhawa, V.K.; Lavi, S.; Walters, D.L. Cardiac catheterization is associated with superior outcomes for survivors of out of hospital cardiac arrest: Review and meta-analysis. Resuscitation 2014, 85, 1533–1540. [Google Scholar] [CrossRef]
- Welsford, M.; Bossard, M.; Shortt, C.; Pritchard, J.; Natarajan, M.K.; Belley-Côté, E.P. Does Early Coronary Angiography Improve Survival After out-of-Hospital Cardiac Arrest? A Systematic Review with Meta-Analysis. Can. J. Cardiol. 2018, 34, 180–194. [Google Scholar] [CrossRef]
- Lemkes, J.S.; Janssens, G.N.; van der Hoeven, N.W.; Jewbali, L.S.D.; Dubois, E.A.; Meuwissen, M.M.; Rijpstra, T.A.; Bosker, H.A.; Blans, M.J.; Bleeker, G.B.; et al. Coronary Angiography After Cardiac Arrest without ST Segment Elevation: One-Year Outcomes of the COACT Randomized Clinical Trial. JAMA Cardiol. 2020, 5, 1358–1365. [Google Scholar] [CrossRef]
- Kern, K.B.; Radsel, P.; Jentzer, J.C.; Seder, D.B.; Lee, K.S.; Lotun, K.; Janardhanan, R.; Stub, D.; Hsu, C.H.; Noc, M. Randomized Pilot Clinical Trial of Early Coronary Angiography Versus No Early Coronary Angiography After Cardiac Arrest without ST-Segment Elevation: The PEARL Study. Circulation 2020, 142, 2002–2012. [Google Scholar] [CrossRef]
- Desch, S.; Freund, A.; Akin, I.; Behnes, M.; Preusch, M.R.; Zelniker, T.A.; Skurk, C.; Landmesser, U.; Graf, T.; Eitel, I.; et al. Angiography after Out-of-Hospital Cardiac Arrest without ST-Segment Elevation. N. Engl. J. Med. 2021, 385, 2544–2553. [Google Scholar] [CrossRef]
- Anyfantakis, Z.A.; Baron, G.; Aubry, P.; Himbert, D.; Feldman, L.J.; Juliard, J.-M.; Ricard-Hibon, A.; Burnod, A.; Cokkinos, D.V.; Steg, P.G. Acute coronary angiographic findings in survivors of out-of-hospital cardiac arrest. Am. Heart J. 2009, 157, 312–318. [Google Scholar] [CrossRef]
- Garcia-Tejada, J.; Jurado-Román, A.; Rodríguez, J.; Velázquez, M.; Hernández, F.; Albarrán, A.; Martín-Asenjo, R.; Granda-Nistal, C.; Coma, R.; Tascón, J. Post-resuscitation electrocardiograms, acute coronary findings and in-hospital prognosis of survivors of out-of-hospital cardiac arrest. Resuscitation 2014, 85, 1245–1250. [Google Scholar] [CrossRef] [PubMed]
- Lott, C.; Truhlář, A.; Alfonzo, A.; Barelli, A.; González-Salvado, V.; Hinkelbein, J.; Nolan, J.P.; Paal, P.; Perkins, G.D.; Thies, K.C.; et al. European Resuscitation Council Guidelines 2021: Cardiac arrest in special circumstances. Resuscitation 2021, 161, 152–219. [Google Scholar] [CrossRef]
- Nolan, J.P.; Soar, J.; Cariou, A.; Cronberg, T.; Moulaert, V.R.M.; Deakin, C.D.; Bottiger, B.W.; Friberg, H.; Sunde, K.; Sandroni, C. European Resuscitation Council and European Society of Intensive Care Medicine 2015 guidelines for post-resuscitation care. Intensiv. Care Med. 2015, 41, 2039–2056. [Google Scholar] [CrossRef] [PubMed]
- Beitler, J.R.; Ghafouri, T.B.; Jinadasa, S.P.; Mueller, A.; Hsu, L.; Anderson, R.J.; Joshua, J.; Tyagi, S.; Malhotra, A.; Sell, R.E.; et al. Favorable Neurocognitive Outcome with Low Tidal Volume Ventilation after Cardiac Arrest. Am. J. Respir. Crit. Care Med. 2017, 195, 1198–1206. [Google Scholar] [CrossRef] [PubMed]
- Robba, C.; Badenes, R.; Battaglini, D.; Ball, L.; Brunetti, I.; Jakobsen, J.C.; Lilja, G.; Friberg, H.; Wendel-Garcia, P.D.; Young, P.J.; et al. Ventilatory settings in the initial 72 h and their association with outcome in out-of-hospital cardiac arrest patients: A preplanned secondary analysis of the targeted hypothermia versus targeted normothermia after out-of-hospital cardiac arrest (TTM2) trial. Intensiv. Care Med. 2022, 48, 1024–1038. [Google Scholar] [CrossRef]
- Chang, W.T.; Wang, C.H.; Lai, C.H.; Yu, H.Y.; Chou, N.K.; Wang, C.H.; Huang, S.C.; Tsai, P.R.; Chou, F.J.; Tsai, M.S.; et al. Optimal Arterial Blood Oxygen Tension in the Early Postresuscitation Phase of Extracorporeal Cardiopulmonary Resuscitation: A 15-Year Retrospective Observational Study. Crit. Care Med. 2019, 47, 1549–1556. [Google Scholar] [CrossRef] [PubMed]
- Schmidt, H.; Kjaergaard, J.; Hassager, C.; Mølstrøm, S.; Grand, J.; Borregaard, B.; Roelsgaard Obling, L.E.; Venø, S.; Sarkisian, L.; Mamaev, D.; et al. Oxygen Targets in Comatose Survivors of Cardiac Arrest. N. Engl. J. Med. 2022, 387, 1467–1476. [Google Scholar] [CrossRef]
- Yeo, J.W.; Ng, Z.H.C.; Goh, A.X.C.; Gao, J.F.; Liu, N.; Lam, S.W.S.; Chia, Y.W.; Perkins, G.D.; Ong, M.E.H.; Ho, A.F.W.; et al. Impact of Cardiac Arrest Centers on the Survival of Patients with Nontraumatic Out-of-Hospital Cardiac Arrest: A Systematic Review and Meta-Analysis. J. Am. Heart Assoc. 2022, 11, e023806. [Google Scholar] [CrossRef]
- Liu, B.; Zhang, Q.; Li, C. Steroid use after cardiac arrest is associated with favourable outcomes: A systematic review and meta-analysis. J. Int. Med Res. 2020, 48, 1–11. [Google Scholar] [CrossRef]
- Perbet, S.; Mongardon, N.; Dumas, F.; Bruel, C.; Lemiale, V.; Mourvillier, B.; Carli, P.; Varenne, O.; Mira, J.P.; Wolff, M.; et al. Early-onset pneumonia after cardiac arrest: Characteristics, risk factors and influence on prognosis. Am. J. Respir. Crit. Care Med. 2011, 184, 1048–1054. [Google Scholar] [CrossRef]
- Gagnon, D.J.; Nielsen, N.; Fraser, G.L.; Riker, R.R.; Dziodzio, J.; Sunde, K.; Hovdenes, J.; Stammet, P.; Friberg, H.; Rubertsson, S.; et al. Prophylactic antibiotics are associated with a lower incidence of pneumonia in cardiac arrest survivors treated with targeted temperature management. Resuscitation 2015, 92, 154–159. [Google Scholar] [CrossRef] [PubMed]
- Tagami, T.; Matsui, H.; Kuno, M.; Moroe, Y.; Kaneko, J.; Unemoto, K.; Fushimi, K.; Yasunaga, H. Early antibiotics administration during targeted temperature management after out-of-hospital cardiac arrest: A nationwide database study. BMC Anesthesiol. 2016, 16, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Stevic, N.M.; Argaud, L.M.; Loufouat, J.; Kreitmann, L.M.; Desmurs, L.; Ovize, M.M.; Bidaux, G.; Cour, M.M. Molar Sodium Lactate Attenuates the Severity of Postcardiac Arrest Syndrome: A Preclinical Study. Crit. Care Med. 2021, 50, e71–e79. [Google Scholar] [CrossRef] [PubMed]
- Jou, C.; Shah, R.; Figueroa, A.; Patel, J.K. The Role of Inflammatory Cytokines in Cardiac Arrest. J. Intensiv. Care Med. 2018, 35, 219–224. [Google Scholar] [CrossRef] [PubMed]
- Tsuchiya, S.; Okuno, Y.; Tsujimoto, G. MicroRNA: Biogenetic and Functional Mechanisms and Involvements in Cell Differentiation and Cancer. J. Pharmacol. Sci. 2006, 101, 267–270. [Google Scholar] [CrossRef]
- Hammond, S.M. An overview of microRNAs. Adv. Drug Deliv. Rev. 2015, 87, 3–14. [Google Scholar] [CrossRef]
- Argaud, L.; Cour, M.; Dubien, P.Y.; Giraud, F.; Jossan, C.; Riche, B.; Hernu, R.; Darmon, M.; Poncelin, Y.; Tchénio, X.; et al. Effect of Cyclosporine in Nonshockable Out-of-Hospital Cardiac Arrest: The CYRUS Randomized Clinical Trial. JAMA Cardiol. 2016, 1, 557–565. [Google Scholar] [CrossRef] [PubMed]
- Kreitmann, L.; for the CYRUS Study Group; Argaud, L.; Ovize, M.; Cour, M. Cyclosporine A prevents cardiac arrest-induced acute respiratory failure: A post-hoc analysis of the CYRUS trial. Intensiv. Care Med. 2020, 46, 1281–1283. [Google Scholar] [CrossRef]
- Geri, G.; Grimaldi, D.; Seguin, T.; Lamhaut, L.; Marin, N.; Chiche, J.-D.; Pène, F.; Bouglé, A.; Daviaud, F.; Morichau-Beauchant, T.; et al. Hemodynamic efficiency of hemodialysis treatment with high cut-off membrane during the early period of post-resuscitation shock: The HYPERDIA trial. Resuscitation 2019, 140, 170–177. [Google Scholar] [CrossRef]
- Choi, Y.H.; Lee, D.H.; Oh, J.H.; Wee, J.H.; Jang, T.C.; Choi, S.P.; Park, K.N. Renal replacement therapy is independently associated with a lower risk of death in patients with severe acute kidney injury treated with targeted temperature management after out-of-hospital cardiac arrest. Crit. Care 2020, 24, 1–11. [Google Scholar] [CrossRef]
- Yannopoulos, D.; Bartos, J.A.; Raveendran, G.; Conterato, M.; Frascone, R.J.; Trembley, A.; John, R.; Connett, J.; Benditt, D.G.; Lurie, K.G.; et al. Coronary Artery Disease in Patients with Out-of-Hospital Refractory Ventricular Fibrillation Cardiac Arrest. J. Am. Coll. Cardiol. 2017, 70, 1109–1117. [Google Scholar] [CrossRef] [PubMed]
- Bascom, K.E.; Dziodzio, J.; Vasaiwala, S.; Mooney, M.; Patel, N.; McPherson, J.; McMullan, P.; Unger, B.; Nielsen, N.; Friberg, H.; et al. Derivation and Validation of the CREST Model for Very Early Prediction of Circulatory Etiology Death in Patients without ST-Segment–Elevation Myocardial Infarction After Cardiac Arrest. Circulation 2018, 137, 273–282. [Google Scholar] [CrossRef]
- Vallabhajosyula, S.; Verghese, D. Mechanical circulatory support in post-cardiac arrest: One two many? Resuscitation 2021, 167, 390–392. [Google Scholar] [CrossRef]
- Nolan, J.P.; Berg, R.A.; Andersen, L.W.; Bhanji, F.; Chan, P.S.; Donnino, M.W.; Lim, S.H.; Ma, M.H.-M.; Nadkarni, V.M.; Starks, M.A.; et al. Cardiac Arrest and Cardiopulmonary Resuscitation Outcome Reports: Update of the Utstein Resuscitation Registry Template for In-Hospital Cardiac Arrest: A Consensus Report from a Task Force of the International Liaison Committee on Resuscitation (American Heart Association, European Resuscitation Council, Australian and New Zealand Council on Resuscitation, Heart and Stroke Foundation of Canada, InterAmerican Heart Foundation, Resuscitation Council of Southern Africa, Resuscitation Council of Asia). Circulation 2019, 140, e746–e757. [Google Scholar] [CrossRef] [PubMed]
- Presciutti, A.; Verma, J.; Pavol, M.; Anbarasan, D.; Falo, C.; Brodie, D.; Rabbani, L.E.; Roh, D.J.; Park, S.; Claassen, J.; et al. Posttraumatic stress and depressive symptoms characterize cardiac arrest survivors’ perceived recovery at hospital discharge. Gen. Hosp. Psychiatry 2018, 53, 108–113. [Google Scholar] [CrossRef] [PubMed]
- Sandroni, C.; Nolan, J.; Cavallaro, F.; Antonelli, M. In-hospital cardiac arrest: Incidence, prognosis and possible measures to improve survival. Intensiv. Care Med. 2006, 33, 237–245. [Google Scholar] [CrossRef]
- Rumsfeld, J.S.; Alexander, K.P.; Goff, D.C., Jr.; Graham, M.M.; Ho, P.M.; Masoudi, F.A.; Moser, D.K.; Roger, V.L.; Slaughter, M.S.; Smolderen, K.G.; et al. Cardiovascular Health: The Importance of Measuring Patient-Reported Health Status: A Scientific Statement from the American Heart Association. Circulation 2013, 127, 2233–2249. [Google Scholar] [CrossRef]
- Moulaert, V.R.; Verbunt, J.A.; Bakx, W.G.; Gorgels, A.P.; de Krom, M.C.; Heuts, P.H.; Wade, D.; van Heugten, C.M. ‘Stand still …, and move on’, a new early intervention service for cardiac arrest survivors and their caregivers: Rationale and description of the intervention. Clin. Rehab. 2011, 25, 867–879. [Google Scholar] [CrossRef]
- Sawyer, K.N.; Camp-Rogers, T.R.; Kotini-Shah, P.; Del Rios, M.; Gossip, M.R.; Moitra, V.K.; Haywood, K.L.; Dougherty, C.M.; Lubitz, S.A.; Rabinstein, A.A.; et al. Sudden Cardiac Arrest Survivorship: A Scientific Statement from the American Heart Association. Circulation 2020, 141, e654–e685. [Google Scholar] [CrossRef]
- Andrew, E.; Nehme, Z.; Bernard, S.; Smith, K. Comparison of health-related quality of life and functional recovery measurement tools in out-of-hospital cardiac arrest survivors. Resuscitation 2016, 107, 57–64. [Google Scholar] [CrossRef]
- Lilja, G.; Nielsen, N.; Bro-Jeppesen, J.; Dunford, H.; Friberg, H.; Hofgren, C.; Horn, J.; Insorsi, A.; Kjaergaard, J.; Nilsson, F.; et al. Return to Work and Participation in Society After Out-of-Hospital Cardiac Arrest. Circ. Cardiovasc. Qual. Outcomes 2018, 11, e003566. [Google Scholar] [CrossRef] [PubMed]
- Lundgren-Nilsson, A.; Rosén, H.; Hofgren, C.; Sunnerhagen, K.S. The first year after successful cardiac resuscitation: Function, activity, participation and quality of life. Resuscitation 2005, 66, 285–289. [Google Scholar] [CrossRef] [PubMed]
- Sandroni, C.; Cronberg, T.; Sekhon, M. Brain injury after cardiac arrest: Pathophysiology, treatment, and prognosis. Intensiv. Care Med. 2021, 47, 1393–1414. [Google Scholar] [CrossRef] [PubMed]
- Fertl, E.; Vass, K.; Sterz, F.; Gabriel, H.; Auff, E. Neurological rehabilitation of severely disabled cardiac arrest survivors. Part I. Course of post-acute inpatient treatment. Resuscitation 2000, 47, 231–239. [Google Scholar] [CrossRef]
- Steinbusch, C.V.; van Heugten, C.M.; Rasquin, S.M.; Verbunt, J.A.; Moulaert, V.R. Cognitive impairments and subjective cognitive complaints after survival of cardiac arrest: A prospective longitudinal cohort study. Resuscitation 2017, 120, 132–137. [Google Scholar] [CrossRef] [PubMed]
- Pußwald, G.; Fertl, E.; Faltl, M.; Auff, E. Neurological rehabilitation of severely disabled cardiac arrest survivors. Part II. Life situation of patients and families after treatment. Resuscitation 2000, 47, 241–248. [Google Scholar] [CrossRef] [PubMed]
- Wachelder, E.; Moulaert, V.; van Heugten, C.; Verbunt, J.; Bekkers, S.; Wade, D. Life after survival: Long-term daily functioning and quality of life after an out-of-hospital cardiac arrest. Resuscitation 2009, 80, 517–522. [Google Scholar] [CrossRef] [PubMed]
- Hope, A.A.; Munro, C.L. Understanding and Improving Critical Care Survivorship. Am. J. Crit. Care 2019, 28, 410–412. [Google Scholar] [CrossRef] [PubMed]

| Organ System | Clinical Findings | Potential Etiology |
|---|---|---|
| Pulmonary | Diminished or abolished breath sounds | Unilateral: Pneumothorax, right mainstem intubation (left side less common) Bilateral: Pulmonary edema |
| Cardiovascular | New murmur | Papillary rupture, valve abnormality |
| Unequal pulses or blood pressure | Aortic dissection | |
| Bradycardia | Toxidrome, hypoxia, hypo/hyperkalemia, hypo/hypercalcaemia, hypothermia, exogenous intoxication, acid-basic disturbances | |
| Tachycardia | Tachyarrhythmias, thyrotoxic storm | |
| Abdomen | Distention/rigidity | Hemorrhage/inflammatory process |
| Pulsatile mass | Aortic aneurism rupture | |
| Extremity | Unilateral swelling/erythema | Pulmonary embolism, septic shock |
| Hemodialysis fistula | Hyperkalemia | |
| Skin | Cyanosis | Hypoxia, methemoglobinemia sulfhemoglobinemia |
| Mottling, slow capillary refill | Septic shock, hemorrhagic shock | |
| IV injection sites | Drug overdose | |
| Open wounds/cellulitis | Septic shock | |
| Diffuse urticaria | Anaphylactic shock | |
| Neurologic | Focal motor deficits | Stroke |
| Global motor deficits | Toxidrome, hypoxic/anoxic brain injury |
| Organ System | Etiology |
|---|---|
| Cardiovascular | Acute coronary syndrome |
| Arrhythmia | |
| Structural heart disease | |
| Cardiac tamponade | |
| Aortic dissection | |
| Respiratory | Venous thromboembolism |
| Upper airway obstruction | |
| Drowning | |
| Pneumothorax | |
| Hypoxia | |
| Metabolic | Acidosis |
| Hypo/Hyperkalemia | |
| Hypomagnesemia | |
| Neurologic | Subarachnoid hemorrhage |
| Status epilepticus | |
| Stroke | |
| Others | Trauma |
| Hypothermia | |
| Intoxication | |
| Non-traumatic exsanguination |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lazzarin, T.; Tonon, C.R.; Martins, D.; Fávero, E.L., Jr.; Baumgratz, T.D.; Pereira, F.W.L.; Pinheiro, V.R.; Ballarin, R.S.; Queiroz, D.A.R.; Azevedo, P.S.; et al. Post-Cardiac Arrest: Mechanisms, Management, and Future Perspectives. J. Clin. Med. 2023, 12, 259. https://doi.org/10.3390/jcm12010259
Lazzarin T, Tonon CR, Martins D, Fávero EL Jr., Baumgratz TD, Pereira FWL, Pinheiro VR, Ballarin RS, Queiroz DAR, Azevedo PS, et al. Post-Cardiac Arrest: Mechanisms, Management, and Future Perspectives. Journal of Clinical Medicine. 2023; 12(1):259. https://doi.org/10.3390/jcm12010259
Chicago/Turabian StyleLazzarin, Taline, Carolina Rodrigues Tonon, Danilo Martins, Edson Luiz Fávero, Jr., Thiago Dias Baumgratz, Filipe Welson Leal Pereira, Victor Rocha Pinheiro, Raquel Simões Ballarin, Diego Aparecido Rios Queiroz, Paula Schmidt Azevedo, and et al. 2023. "Post-Cardiac Arrest: Mechanisms, Management, and Future Perspectives" Journal of Clinical Medicine 12, no. 1: 259. https://doi.org/10.3390/jcm12010259
APA StyleLazzarin, T., Tonon, C. R., Martins, D., Fávero, E. L., Jr., Baumgratz, T. D., Pereira, F. W. L., Pinheiro, V. R., Ballarin, R. S., Queiroz, D. A. R., Azevedo, P. S., Polegato, B. F., Okoshi, M. P., Zornoff, L., Rupp de Paiva, S. A., & Minicucci, M. F. (2023). Post-Cardiac Arrest: Mechanisms, Management, and Future Perspectives. Journal of Clinical Medicine, 12(1), 259. https://doi.org/10.3390/jcm12010259







