Abstract
Background: Medication is often changed after inpatient treatment, which affects the course of the disease, health behavior and adherence. Thus, it is important to understand patterns of medication changes after discharge from hospital. Methods: Inpatients at the Department of Neurology received a comprehensive assessment during their stay, including adherence, depression, cognition, health and sociodemographic variables. A month after being discharged, patients were contacted to enquire about post-discharge medication changes. Results: 910 older adults aged 70 ± 8.6 years participated, of which 204 (22.4%) reported medication changes. The majority of changes were initiated by physicians (n = 112, 56.3%) and only 25 (12.6%) patients reported adjusting medication themselves. Reasons for medication changes differed between patients and doctors (p < 0.001), with side effects or missing effects cited frequently. Sociodemographic and patient-related factors did not significantly predict medication changes. Conclusion: Patients reported less post-discharge medication changes than expected, and contrary to previous literature on nonadherence, only a fraction of those changes were performed by patients themselves. Socioeconomic and clinical parameters regarding personality, mood and cognition were poorly associated with post-discharge medication changes. Instead, individual health-related factors play a role, with patient factors only indirectly influencing physicians’ decisions.
1. Introduction
The treatment of chronic disorders commonly includes the long-term use of pharmacotherapy. This is particularly true for older adults who are often expected to adhere to complex drug regimens [1]. In addition to this initial complexity, medication is frequently adjusted after hospital discharge. A previous study reported that only 21% of geriatric patients remain on their initial discharge prescriptions [2], and another group of researchers cite a medication change prevalence of over 50% post-discharge [3]. Especially general practitioners (GP) extensively adjust medication after discharge [2]. Some authors reported that more than half of the discharge prescriptions among 726 geriatric participants were classified as potentially inappropriate [4], whereas a different study found a reduction in inappropriate prescriptions during the stay at a specialized geriatric care hospital compared to admission medication [5].
These frequent changes in medication impact medication knowledge and adherence to medication and thus also health outcomes and hospital readmissions [6]. Adherence is used as a term to describe how well a person follows the recommendations from healthcare providers, such as changing the diet and exercise, taking part in therapies, and taking prescribed medication [7]. However, many older adults either do not want to or cannot take medications as agreed upon [8]. This nonadherence to medication increases the chances for adverse drug events and readmissions to hospitals, higher costs, lower quality of life and general poorer health outcomes [7,9,10,11]. Factors contributing to nonadherence are numerous and can be divided into patient-, physician- and healthcare-related factors. On the patient side, several factors leading to nonadherence have been identified, such as depressive mood, cognition and healthcare beliefs [9,12]. On the other hand, complexity and frequent medication changes contribute to poorer knowledge about and adherence to medication regimes [6,9,13]. In general, nonadherence may be intentional (when the patient purposefully decides not to follow the recommended treatment, e.g., due to beliefs or perceived risks) or unintentional (when the patient cannot follow the recommendation, e.g., due to lack of understanding or forgetting). Especially the motivators behind intentional nonadherence are crucial to understand, as this represents a willful, conscious decision to interfere with medication recommendations that can be targeted in interventions [13].
As inpatient hospital care provides an ideal moment for optimizing medication [3], it is crucial to understand how medication regimes change during the transition from inpatient to outpatient care. While some medication is planned to be short-term and needs to be adjusted post-discharge, e.g., when medication was prescribed due to acute events, it is crucial to discern the patterns of changes made erroneously. The transition from inpatient to outpatient care is accompanied by a myriad of changes, adjustments and barriers and can often lead to adverse effects due to miscommunication, lack of understanding or inappropriate changes [14]. During most hospital stays, a new medication plan is put together [15], and preventing unplanned medication changes after discharge is of high relevance to ensure continued health and prevent readmission. Combining the reports of high levels of both post-discharge medication changes [2,3] and nonadherence in older adults [14,16,17] poses the question of which quota of these changes are induced by patients themselves. To the best of our knowledge, this distinction between different initiators of medication changes has not been made before, but it is crucial to disentangle different agents and their motivations for medication changes to improve health outcomes and intervene with appropriate measures if needed. Therefore, we aimed to explore the exact nature of these medication changes to understand how and why patients modify their medication after discharge. Based on the cited literature, we expected a high level of post-discharge medication changes, with a significant portion of those changes initiated by patients themselves. The goal of the current analysis is therefore to first describe the nature of medication changes after discharge from hospital in older adults, and to understand the factors predicting these medication changes. For this purpose, we interviewed patients during their inpatient stay about their medication intake and collected comprehensive patient-related data. Four weeks after discharge, we contacted the patients via telephone to enquire about potential medication changes.
2. Materials and Methods
2.1. Setting and Participantss
This cross-sectional study was registered in the German Clinical Trials Register DRKS00016774 (registered 19 February 2019) and the study protocol was published in advance (Prell, 2019). The study was approved by the local ethics committee (approval number 5290-10/17) of Jena University Hospital. All patients provided written informed consent.
As a summary, from February 2019 to March 2020, patients 60 years of age or older with neurological disorders received a comprehensive geriatric assessment during their stay in the Department of Neurology at the Jena University Hospital, Jena, Germany. The data used for this analysis is freely available [18].
This paper reports analyses of the longitudinal dataset with the first follow-up investigation. The following assessments were used for this analysis: age, gender, main neurological diagnosis, medication regime at admission and discharge, marital status (single/divorced/widowed or married), living condition (alone, not alone), level of education (high, middle, low), number of medications per day, medical diagnoses. Additionally, the following assessments were made: depression (Beck Depression inventory, BDI II) [16,17], personality (Big Five Inventory, BFI) [19], health-care climate (HCCQ) [20], health-related quality of life (HRQoL) using SF-36 [21], adherence (Stendal Adherence to Medication Score, SAMS) [22], timed-up-and-go-test (TuG) [23], and Montreal Cognitive Assessment (MoCa) [24].
The SF-36 is a general health-related QoL questionnaire to assess with the following 8 different domains: problems regarding both physical and social activity due to health, limitations in daily life due to physical or emotional problems, pain, mental health, vitality, and general health perception. Each domain is summarized as the weighted sum of the respective items, with lower scores indicating less disability. A physical and mental compound score as well subscores can be calculated [21]. The Stendal Adherence to Medication Scale (SAMS) is a questionnaire with 18 items summarized in a cumulative adherence score, with 0 indicating complete adherence and 72 complete nonadherence [22]. Different facets of adherence are included, namely modification of medication, lack of knowledge and forgetting to take medication [22,25]. For the follow-up assessment approximately one month after discharge, patients were contacted via telephone and the following questions were asked: “How would you rate your current health in comparison to the time before your hospital stay—better, about the same, or worse?”, “Were there any changes to your medication since your discharge from hospital?”, “if yes, which ones?”, “if yes, by whom were these changes made?”, and “if yes, why were the changes made?”.
2.2. Statistical Analysis
In the first step, the cohort was summarized with descriptive statistics. Normal distribution was assessed with Shapiro–Wilk test. The different groups of patients were compared using the Student’s t-test, Mann–Whitney U test or Chi-squared test with Bonferroni correction for multiple comparisons where appropriate. Binominal logistic regression with backward selection was used to determine the association between changes of medication after discharge and the variables BDI score, number of medication and Sf-36 subscales Physical Functioning and Health Change. Linearity was tested assessed using the Box–Tidwell [26]. Bonferroni correction was applied to all terms in the model [27]. All variables were found to follow a linear relationship. Correlations between predictor variables were low (r < 0.70), indicating that multicollinearity was not a confounding factor in the analysis. Goodness-of-fit was assessed using the Hosmer–Lemeshow test. We generally apply a significance level of 0.05 and 2-sided tests.
3. Results
3.1. Clinical and Demographical Characteristics
The baseline assessment included 910 older adults (389 female and 521 male) aged 70 ± 8.6 years (see Supplementary Table S1 for a detailed cohort description). Most patients were married, pensioned, lived with family members and had a high education level; most predominant diagnoses were movement disorders (33.3%), followed by cerebrovascular (25.6%) and neuromuscular (18.5%) disorders. The majority of patients had no (n = 468, 51.4%) or minimal depression (n = 187, 20.5%), a mild, moderate or severe depression was observed in 139 (15.3%), 61 (6.7%) or 27 (3%) patients, respectively. Cognition was normal in 466 (51.2%; MoCA ≥ 23) and cognitive deficits were present in 370 (40.7%, MoCA < 23) persons (74 missing data). For follow-up one month after discharge, 712 persons (78.2%) were interviewed; 192 (21.1%) could not be reached, 6 (0.7%) died.
3.2. Patterns of Medication Changes after Discharge
Changes of medication after discharge were reported by 204 (22.4%) patients. These medication changes were mainly initiated by physicians (n = 112, 56.3%, by GP 74, by Neurologist 34, by other hospitals/rehabilitation centers 4); only a minority of patients reported initiating medication changes themselves (n = 25, 12.6%) (n = 62, 31.2% by others). Reasons for medication changes were side effects, missing effects and miscellaneous reasons (individual reasons such as planned operations, specific allergies, or unavailability of certain medications) (Figure 1). We summarized the initiators of changes and the corresponding reasons for change in a variable tree in Figure 2.
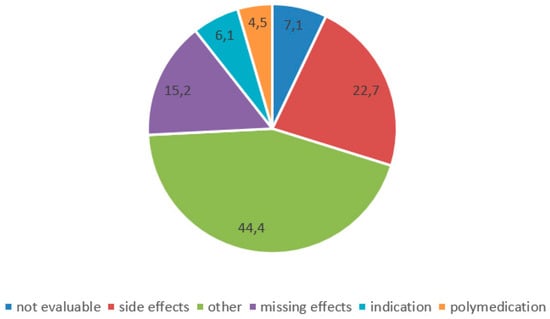
Figure 1.
Reasons for changes of medication after discharge.
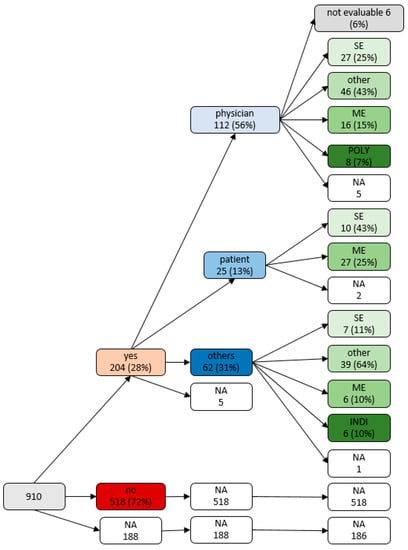
Figure 2.
Variable tree: initiator with their different reasons for changes of medication after discharge, note: NA = not available, INDI = new indication, ME = missing effects, SE = side, effects, POLY = polymedication.
The composition of initiators and reasons for medication changes is further illustrated in the alluvial diagram in Supplementary Figure S1. The type of changes differed between the indicator of those changes (χ2 = 979.6, p < 0.001), with changes made by patients themselves mainly related to side effects and missing effect, whereas changes made by physicians were due to side effects or a collection of individual, miscellaneous reasons (see Supplementary Figure S2).
3.3. Predictors of General Medication Changes after Discharge
In the univariate group comparison, changes of medication were more common in people with depression and self-reported nonadherence (Table 1). In terms of HRQoL, people with medication changes reported better physical functioning and less worsening of health before assessment (domain health change) (Table 1). In the corresponding binomial logistic regression, neither the SAMS nor the BDI were able to significantly predict medication change after discharge (model χ2 = 3.48, p = 0.175).

Table 1.
Group comparison: cross table for dependent medication change after discharge.
Although in the binominal logistic regression the combination of physical function and health change significantly predicted medication changes after discharge, the explained variance was low, as shown by Nagelkerke’s R2 = 0.019 (Table 2).

Table 2.
Binominal logistic regression: medication change after discharge (yes/no).
3.4. Predictors of Patient-Initiated Medication Changes after Discharge
Given that we hypothesized that different mechanisms may underlie the changes made by the patients (i.e., changes were made without consulting a doctor) and changes made by physicians, we performed additional analyses with respect to the initiator of medication changes, i.e., patient vs. physician. In the univariate analysis patients who initiated changes themselves were more frequently female (Table 3).

Table 3.
Group comparison: cross table for initiator of medication change after discharge.
Both groups did not differ in terms of overall adherence assessed by the total SAMS (Table 3) nor on SAMS item level (Supplementary Table S2).
In the binominal logistic regression only female gender (OR = 2.91, CI [0.890, 9.53], p = 0.077), and higher age (OR = 1.057, CI [0.987, 1.132], p = 0.114) were associated with patient-initiated medication changes after discharge (χ2 = 6.06, p = 0.048, Nagelkerke’s R2 = 0.10) (Supplementary Table S3).
Medication changes due to side effects were not related to any of the assessed clinical parameters and occurred independent of age, gender, diagnosis, depression or adherence. Medication changes due to missing effect were more frequent in people with movement disorders (e.g., Parkinson’s disease) (Table 4).

Table 4.
Univariate comparison for different reasons of medication change (with Bonferroni correction).
4. Discussion
This study examined patterns and predictors of medication changes in older adults after discharge from hospital. One month after discharge, the medication of 22.4% of the patients was changed, which is lower than previously reported in the literature [2,3]. Additionally, contrary to our hypotheses based on high levels of nonadherence in older patients [14,16,17], only a small fraction of the patients reported performing medication changes themselves, with most of the changes predominantly issued by outpatient physicians. This is at odds with previous literature reporting that 40% of patients were nonadherent to at least one medication after discharge [28]. Likewise, Mansur et al. (2008) showed that 36.7% of patients reported changes in their medication one month after discharge, with 30% of patients being nonadherent to at least one medication [29]. Different prevalence of medication changes may partially be explained by different follow-up time intervals. Additionally, a differentiation must be made between acute and planned hospital stays, as Mansur, Weiss, Hoffman, Gruenewald and Beloosesky [29] recruited their patients from the acute geriatric ward. As shown in our analyses, patient-related indicators including sociodemographic and personal parameters such as HRQoL, adherence, mood and cognition were not or only poorly associated with changes of medication after discharge, which mirrors the findings by Mansur, Weiss, Hoffman, Gruenewald and Beloosesky [29]. We initially hypothesized that nonadherence could be a predictor of medication change as previously demonstrated for a smaller cohort of people with Parkinson’s disease [30]. However, this could not be replicated in this cohort of older adults with mixed disorders. These results indicate that, although the literature often focuses on nonadherent or “difficult” patients [31,32,33,34], the majority of patients do not willfully interfere with their medication plan after discharge from hospital. This interpretation is supported by the finding that adherence rates did not differ between patients who initiated changes themselves and patients where the physicians initiated changes. These findings display how it is not adherence per se that contributes to adjustments of medication. On the SAMS item-level we also did not observe contributions of different reasons of nonadherence (i.e., missing knowledge about medication, intentional modification of medication, forgetting) to medication changes after discharge. However, we cannot exclude that that adherence-related patient factors may influence medication changes at a later timepoint after discharge.
It seems that health-related factors such as side effects or lack of effects as well as individual health-related factors play a role for prompt medication changes. Especially the high rate of “other” reasons for post-discharge medication changes in our study again highlights the role of individual, specific reasons that cannot be generalized. However, since the present analysis was focused on predicting patient-related factors that lead to medication changes after discharge, individual health-related factors were not assessed and only a cautious indication can be made on the basis of the small but significant prediction of physical functioning and health change on medication changes.
We found that changes due to missing effects are more common in Parkinson´s disease than in the other disorder groups. This is probably due to the fact that, in the case of Parkinson’s disease, medication is frequently adjusted during the inpatient stay and certain expectations of a prompt improvement in motor function are associated with this [35]. If this improvement does not occur, people with Parkinson´s disease seem to be more willing to adjust medication on their own. Understandably, however, this explanation cannot be transferred to other diseases, such as vascular diseases, where there is no immediate benefit of medication. In general, adherence patterns may vary depending on the underlying diagnosis [36,37,38], as different diagnoses may come with varying levels of chronicity, restrictions and burden [9]. Thus, predictors and barriers for adherence can differ between patient groups [39].
Overall, it can only be cautiously stated on the basis of the calculated models that the probability of patient-initiated medication changes appears to be higher in older women. However, the interpretability of this results is reduced by the small group of patients that initiated medication changes themselves, thus the collected patient-related parameters such as mood, cognition or adherence could not fully capture the reasons for medication changes. Patient-related factors may indirectly indicate medication changes by influencing the physician, e.g., if a patient reports depressive mood changes leading to the physician administering a dosage reduction, but overall, our results suggest that medication change seems to be both health-related and physician-indicated.
This study has several limitations. First, the results are restricted to hospitalized neurogeriatric patients. Given that we were mainly interested in personal factors, we used self-report instruments to detect nonadherence and medication change after discharge. We did not compare the list of prescribed medications with the actual medications taken. Although this is a common and valid approach, it does not allow a statement about the real medication possession ratio or correctness of drug intake. Self-reports are known to be prone to systematic and unsystematic biases [40], especially regarding social desirability and recall bias. However, self-reported adherence measurements can still provide reliable information on adherence levels and can detect clinically relevant nonadherence [41]. All questionnaires used are valid and commonly used in the clinical literature. Although we collected a large amount of clinical data, it is not possible to capture all relevant factors, and due to our hypothesis-driven approach the current data cannot explain all factors pertaining to medication changes. Thus, further studies are needed to understand the individual health-related factors leading to the physician-initiated medication changes and their effects on health outcomes. In addition, to fully understand the effect of patient-related factors, it would be of interest to analyze their indirect effects on the physician’s decisions in greater detail.
As a general conclusion from our data, we can say that medication changes shortly after hospital discharge are less frequent than expected in this cohort of older adults with neurological disorders. Furthermore, they are predominantly performed by physicians for individual health-related reasons rather than patient nonadherence. However, as not all medication changes are clinically appropriate and may lead to adverse health events [42], it is crucial to optimize communication between patients, hospitals, and physicians to assess all relevant individual factors and achieve the best possible health outcomes.
Supplementary Materials
The following supporting information can be downloaded at: https://www.mdpi.com/article/10.3390/jcm11030563/s1: Table S1: Clinical and demographical characteristics; Table S2: Comparison of SAMS on item level for medication changes initiated by patient or physician; Table S3: Binominal logistic regression: Medication changes initiated by patient or physician; Figure S1: Alluvial plot for reasons of medication changes; Figure S2: Scatter plot of bivariate relationship.
Author Contributions
Conceptualization, T.P., formal analysis, A.S. (Anna Schwarzkopf) and T.P.; data collection, A.S. (Anna Schwarzkopf) and A.S. (Aline Schönenberg); writing—original draft preparation, A.S. (Anna Schwarzkopf); writing—review and editing, A.S. (Aline Schönenberg) and T.P. All authors have read and agreed to the published version of the manuscript.
Funding
This work is supported by a BMBF (Bundesministerium für Bildung und Forschung) grant to TP (01GY1804).
Institutional Review Board Statement
The study was approved by the local ethics committee of Jena University Hospital (approval number: 5290-10/17).
Informed Consent Statement
Informed consent was obtained from all subjects involved in the study.
Data Availability Statement
The data used in this analysis is freely available for noncommercial scientific purposes at doi:10.5061/dryad.w3r2280qh [18].
Conflicts of Interest
The authors declare no conflict of interest.
References
- Noël, P.H.; Parchman, M.L.; Williams, J.W., Jr.; Cornell, J.E.; Shuko, L.; Zeber, J.E.; Kazis, L.E.; Lee, A.F.; Pugh, J.A. The challenges of multimorbidity from the patient perspective. J. Gen. Intern. Med. 2007, 22 (Suppl. 3), 419–424. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Krause, O.; Glaubitz, S.; Hager, K.; Schleef, T.; Wiese, B.; Junius-Walker, U. Post-discharge adjustment of medication in geriatric patients: A prospective cohort study. Z. Gerontol. Geriatr. 2020, 53, 663–670. [Google Scholar] [CrossRef] [PubMed]
- Daliri, S.; Bouhnouf, M.; van de Meerendonk, H.W.P.C.; Buurman, B.M.; Scholte op Reimer, W.J.M.; Kooij, M.J.; Karapinar–Çarkit, F. Longitudinal medication reconciliation at hospital admission, discharge and post-discharge. Res. Soc. Adm. Pharm. 2021, 17, 677–684. [Google Scholar] [CrossRef] [PubMed]
- Bo, M.; Gibello, M.; Brunetti, E.; Boietti, E.; Sappa, M.; Falcone, Y.; Aurucci, M.L.; Iacovino, M.; Fonte, G.; Cappa, G. Prevalence and predictors of inappropriate prescribing according to the Screening Tool of Older People’s Prescriptions and Screening Tool to Alert to Right Treatment version 2 criteria in older patients discharged from geriatric and internal medicine wards: A prospective observational multicenter study. Geriatr. Gerontol. Int. 2019, 19, 5–11. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Onatade, R.; Auyeung, V.; Scutt, G.; Fernando, J. Potentially inappropriate prescribing in patients on admission and discharge from an older peoples’ unit of an acute UK hospital. Drugs Aging 2013, 30, 729–737. [Google Scholar] [CrossRef] [PubMed]
- Capiau, A.; Foubert, K.; Van der Linden, L.; Walgraeve, K.; Hias, J.; Spinewine, A.; Sennesael, A.L.; Petrovic, M.; Somers, A. Medication Counselling in Older Patients Prior to Hospital Discharge: A Systematic Review. Drugs Aging 2020, 37, 635–655. [Google Scholar] [CrossRef]
- Haynes, R.B.; Yao, X.; Degani, A.; Kripalani, S.; Garg, A.; McDonald, H.P. Interventions to enhance medication adherence. Cochrane Database Syst. Rev. 2005, Cd000011. [Google Scholar] [CrossRef]
- Sabaté, E. Adherence to Long-Term Therapies: Evidence for Action; World Health Organization: Geneva, Switzerland, 2003. [Google Scholar]
- Yap, A.F.; Thirumoorthy, T.; Kwan, Y.H. Systematic review of the barriers affecting medication adherence in older adults. Geriatr. Gerontol. Int. 2016, 16, 1093–1101. [Google Scholar] [CrossRef]
- Budnitz, D.S.; Lovegrove, M.C.; Shehab, N.; Richards, C.L. Emergency hospitalizations for adverse drug events in older Americans. N. Engl. J. Med. 2011, 365, 2002–2012. [Google Scholar] [CrossRef]
- DiMatteo, M.R.; Giordani, P.J.; Lepper, H.S.; Croghan, T.W. Patient adherence and medical treatment outcomes: A meta-analysis. Med. Care 2002, 40, 794–811. [Google Scholar] [CrossRef]
- Brown, M.T.; Bussell, J.; Dutta, S.; Davis, K.; Strong, S.; Mathew, S. Medication Adherence: Truth and Consequences. Am. J. Med. Sci. 2016, 351, 387–399. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Mukhtar, O.; Weinman, J.; Jackson, S.H. Intentional non-adherence to medications by older adults. Drugs Aging 2014, 31, 149–157. [Google Scholar] [CrossRef] [PubMed]
- McLeod, L.A. Patient transitions from inpatient to outpatient: Where are the risks? Can we address them? J. Healthc. Risk Manag. 2013, 32, 13–19. [Google Scholar] [CrossRef] [PubMed]
- Harris, C.M.; Sridharan, A.; Landis, R.; Howell, E.; Wright, S. What happens to the medication regimens of older adults during and after an acute hospitalization? J. Patient Saf. 2013, 9, 150–153. [Google Scholar] [CrossRef] [PubMed]
- Beck, A.T.; Steer, R.A.; Brown, G.K. Manual for the Beck Depression Inventory-II; Psychological Corporation: San Antonio, TX, USA, 1996. [Google Scholar]
- Kühner, C.; Bürger, C.; Keller, F.; Hautzinger, M. Reliabilität und Validität des revidierten Beck-Depressionsinventars (BDI-II). Der Nervenarzt 2007, 78, 651–656. [Google Scholar] [CrossRef] [PubMed]
- Prell, T. Data on medication adherence in adults with neurological disorders: The NeuroGerAd study. Dryad 2022. [Google Scholar] [CrossRef]
- John, O.P.; Donahue, E.M.; Kentle, R.L. The Big Five Inventory—Versions 4a and 54; University of California, Institute of Personality and Social Research: Berkeley, CA, USA, 1991. [Google Scholar]
- Schmidt, K.; Gensichen, J.; Petersen, J.J.; Szecsenyi, J.; Walther, M.; Williams, G.; Freund, T. Autonomy support in primary care—Validation of the German version of the Health Care Climate Questionnaire. J. Clin. Epidemiol. 2012, 65, 206–211. [Google Scholar] [CrossRef]
- Ware, J.E., Jr.; Sherbourne, C.D. The MOS 36-item short-form health survey (SF-36). I. Conceptual framework and item selection. Med. Care 1992, 30, 473–483. [Google Scholar] [CrossRef]
- Franke, G.H.; Nentzl, J.; Jagla-Franke, M. SAMS. Stendal Adherence to Medication Score. Testmanual 2020. [Google Scholar] [CrossRef]
- Podsiadlo, D.; Richardson, S. The timed “Up & Go”: A test of basic functional mobility for frail elderly persons. J. Am. Geriatr. Soc. 1991, 39, 142–148. [Google Scholar] [CrossRef]
- Nasreddine, Z.S.; Phillips, N.A.; Bédirian, V.; Charbonneau, S.; Whitehead, V.; Collin, I.; Cummings, J.L.; Chertkow, H. The Montreal Cognitive Assessment, MoCA: A brief screening tool for mild cognitive impairment. J. Am. Geriatr. Soc. 2005, 53, 695–699. [Google Scholar] [CrossRef] [PubMed]
- Prell, T.; Grosskreutz, J.; Mendorf, S.; Franke, G.H.; Witte, O.W.; Kunze, A. Clusters of non-adherence to medication in neurological patients. Res. Soc. Adm. Pharm. 2019, 15, 1419–1424. [Google Scholar] [CrossRef] [PubMed]
- Box, G.E.P.; Tidwell, P.W. Transformation of the Independent Variables. Technometrics 1962, 4, 531–550. [Google Scholar] [CrossRef]
- Tabachnick, B.G.; Fidell, L.S. Using Multivariate Statistics, 7th ed.; Pearson Education: New York, NY, USA, 2018. [Google Scholar]
- Mitchell, B.; Chong, C.; Lim, W.K. Medication adherence 1 month after hospital discharge in medical inpatients. Intern. Med. J. 2016, 46, 185–192. [Google Scholar] [CrossRef]
- Mansur, N.; Weiss, A.; Hoffman, A.; Gruenewald, T.; Beloosesky, Y. Continuity and adherence to long-term drug treatment by geriatric patients after hospital discharge: A prospective cohort study. Drugs Aging 2008, 25, 861–870. [Google Scholar] [CrossRef]
- Feldmann, F.; Zipprich, H.M.; Witte, O.W.; Prell, T. Self-Reported Nonadherence Predicts Changes of Medication after Discharge from Hospital in People with Parkinson’s Disease. Parkinsons Dis. 2020, 2020, 4315489. [Google Scholar] [CrossRef] [PubMed]
- Groves, J.E. Taking Care of the Hateful Patient. N. Engl. J. Med. 1978, 298, 883–887. [Google Scholar] [CrossRef]
- Pentzek, M.; Santos, S.; Wollny, A.; Gummersbach, E.; Herber, O.R.; In der Schmitten, J.; Icks, A.; Abholz, H.H.; Wilm, S. Which patients with type 2 diabetes mellitus are perceived as ‘difficult’ by general practitioners? Prim. Care Diabetes 2019, 13, 353–359. [Google Scholar] [CrossRef]
- Lin, E.H.; Katon, W.; Von Korff, M.; Bush, T.; Lipscomb, P.; Russo, J.; Wagner, E. Frustrating patients: Physician and patient perspectives among distressed high users of medical services. J. Gen. Intern. Med. 1991, 6, 241–246. [Google Scholar] [CrossRef]
- Dingwall, R.; Murray, T. Categorization in accident departments: ‘Good’ patients, ‘bad’ patients and ‘children’. Sociol. Health Illn. 1983, 5, 127–148. [Google Scholar] [CrossRef]
- Heimrich, K.G.; Prell, T. Short- and Long-Term Effect of Parkinson’s Disease Multimodal Complex Treatment. Brain Sci. 2021, 11, 1460. [Google Scholar] [CrossRef] [PubMed]
- Briesacher, B.A.; Andrade, S.E.; Fouayzi, H.; Chan, K.A. Comparison of drug adherence rates among patients with seven different medical conditions. Pharmacotherapy 2008, 28, 437–443. [Google Scholar] [CrossRef] [PubMed]
- Yeaw, J.; Benner, J.S.; Walt, J.G.; Sian, S.; Smith, D.B. Comparing adherence and persistence across 6 chronic medication classes. J. Manag. Care Pharm. 2009, 15, 728–740. [Google Scholar] [CrossRef] [PubMed]
- DiMatteo, M.R. Variations in patients’ adherence to medical recommendations: A quantitative review of 50 years of research. Med. Care 2004, 42, 200–209. [Google Scholar] [CrossRef] [PubMed]
- Schönenberg, A.; Prell, T. Factors Influencing Self-Reported Medication Use in the Survey of Health Aging and Retirement in Europe (SHARE) Dataset. Healthcare 2021, 9, 1752. [Google Scholar] [CrossRef] [PubMed]
- Bortz, J.; Döring, N. Forschungsmethoden und Evaluation für Human- und Sozialwissenschaftler; Springer: Berlin, Germany, 2007. [Google Scholar]
- Stirratt, M.J.; Dunbar-Jacob, J.; Crane, H.M.; Simoni, J.M.; Czajkowski, S.; Hilliard, M.E.; Aikens, J.E.; Hunter, C.M.; Velligan, D.I.; Huntley, K.; et al. Self-report measures of medication adherence behavior: Recommendations on optimal use. Transl. Behav. Med. 2015, 5, 470–482. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Forster, A.J.; Murff, H.J.; Peterson, J.F.; Gandhi, T.K.; Bates, D.W. Adverse drug events occurring following hospital discharge. J. Gen. Intern. Med. 2005, 20, 317–323. [Google Scholar] [CrossRef] [Green Version]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).