Perception and Coverage of Conventional Vaccination among University Students from Rouen (Normandy), France in 2021
Abstract
:1. Introduction
2. Methods
2.1. Study Design and Settings
2.2. Data Collection
Sociodemographic Data
2.3. Vaccination Perception and Knowledge
2.4. Vaccination Coverage Status
2.5. Statistical Analysis
3. Results
3.1. Population Characteristics
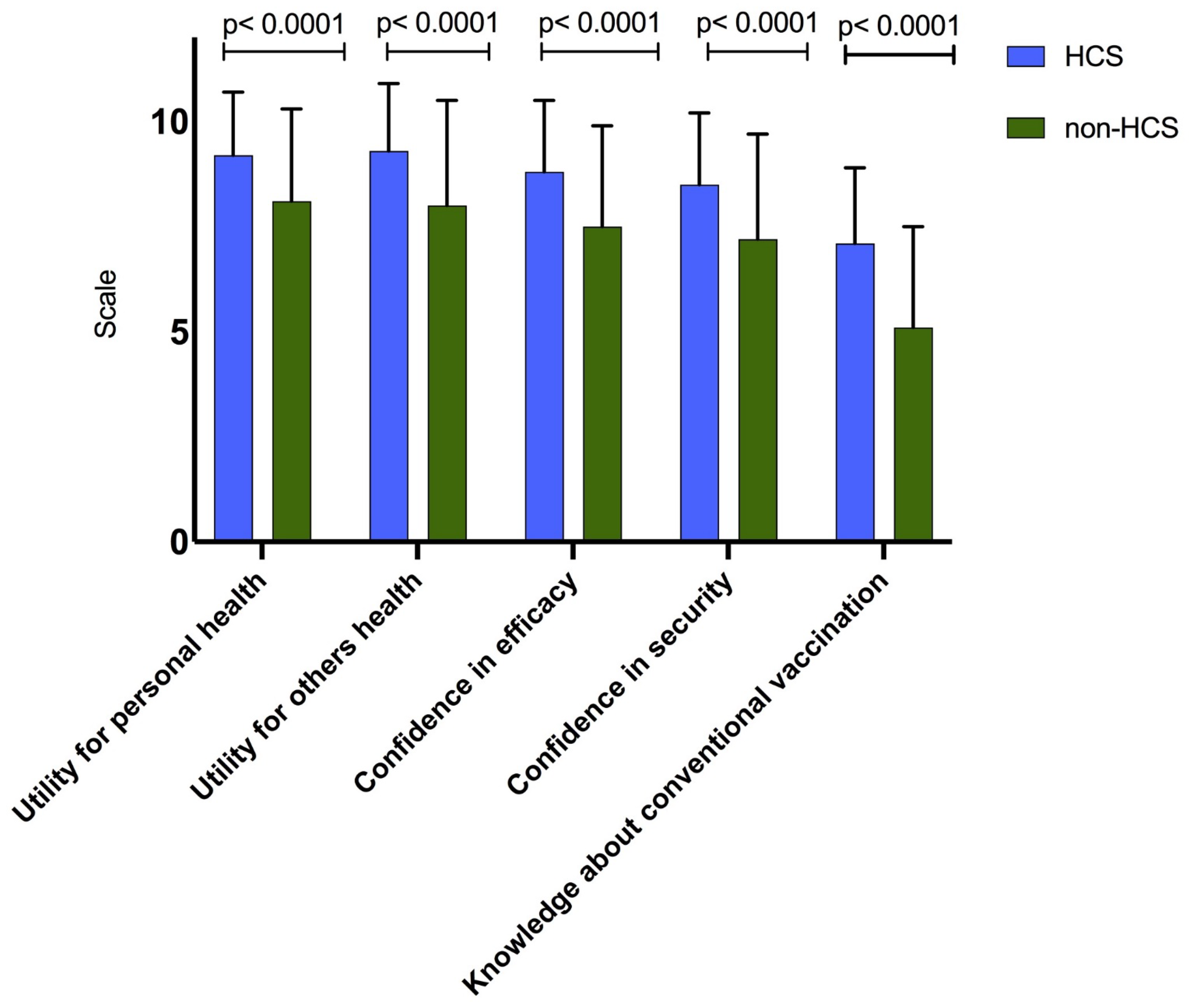
3.2. Vaccination Perception
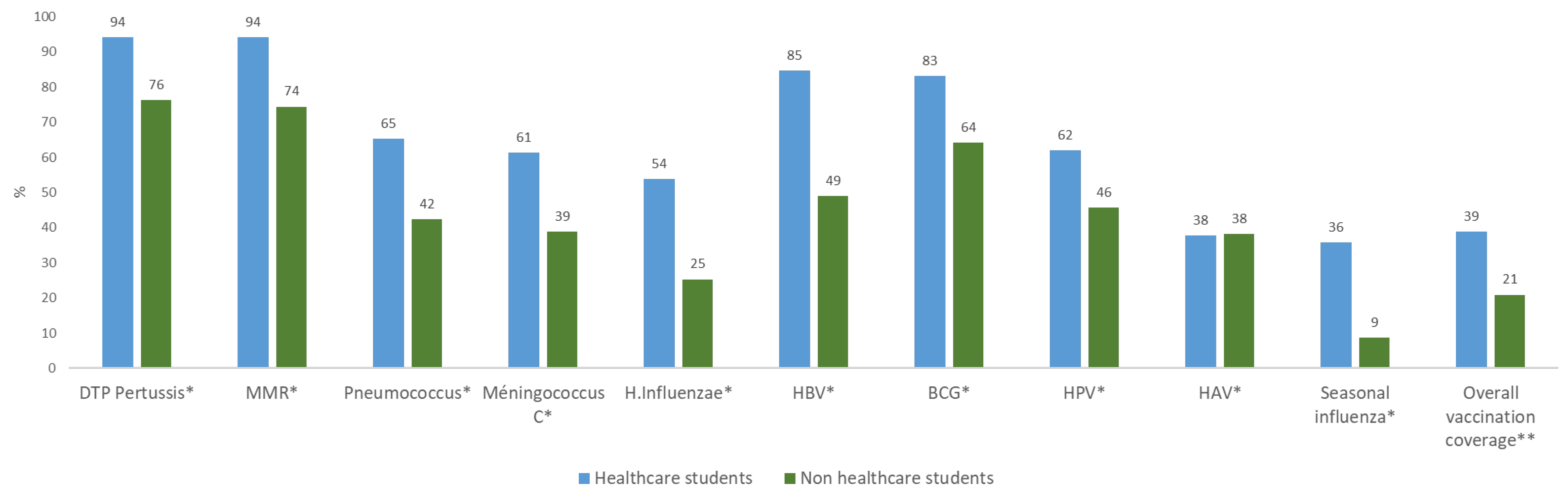
3.3. Vaccination Coverage
4. Discussion
5. Limitations
6. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Immunization. The United Nations Children’s Fund (UNICEF). Immunization. 2019. Available online: https://data.unicef.org/topic/child-health/immunization/ (accessed on 24 February 2022).
- Xiao, X.; Wong, R.M. Vaccine hesitancy and perceived behavioral control: A meta-analysis. Vaccine 2020, 38, 5131–5138. [Google Scholar] [CrossRef]
- World Health Organization. Top Ten Threats to Global Health in 2019. 2019. Available online: https://www.who.int/en/news-room/spotlight/ten-threats-to-global-health-in-2019 (accessed on 15 February 2022).
- Lane, S.; Macdonald, N.E.; Marti, M.; Dumolard, L. Vaccine hesitancy around the globe: Analysis of three years of WHO/UNICEF joint reporting Form data-2015–2017. Vaccine 2018, 36, 3861–3867. [Google Scholar] [CrossRef]
- Betsch, C.; Schmid, P.; Heinemeier, D.; Korn, L.; Holtmann, C.; Böhm, R. Beyond confidence: Development of a measure assessing the 5C psychological antecedents of vaccination. PLoS ONE 2018, 13, e0208601. [Google Scholar] [CrossRef] [Green Version]
- Rosenstock. Social Learning Theory and the Health Belief Model. 1988. Available online: https://journals.sagepub.com/doi/abs/10.1177/109019818801500203?casa_token=8sh1gfDhinIAAAAA:oLFrlO2JbhMy961na4XkKffFCWpFwHuZKJCwpjviTU1uNYjzxxrQ_ak9r7oNlBEj0DPmXrrTXdA4 (accessed on 24 February 2022).
- Guthmann, J.P.; Fonteneau, L.; Lévy-Bruhl, D. Mesure de la Couverture Vaccinale en France. Sources de Données et Données Actuelles; Institut De Veille Sanitaire: Saint-Maurice, France, 2012; 98p. Available online: http://www.invs.sante.fr (accessed on 24 February 2022).
- France, S. Les Infections Invasives à Méningocoques en 2017. 2021. Available online: https://www.santepubliquefrance.fr/content/download/51444/1114808 (accessed on 15 March 2022).
- Dalon, F.; Majed, L.; Belhassen, M.; Jacoud, F.; Bérard, M.; Lévy-Bachelot, L.; de Pouvourville, G.; Rouzier, R.; Raude, J.; Baldauf, J.J. Human papillomavirus (HPV) vaccine coverage rates (VCRs) in France: A French claims data study. Vaccine 2021, 39, 5129–5137. [Google Scholar] [CrossRef]
- Baldolli, A.; Michon, J.; Verdon, R.; Fournier, A. Vaccination perception and coverage among healthcare students in France in 2019. BMC Med. Educ. 2020, 20, 1–10. [Google Scholar] [CrossRef]
- Karlsson, L.C.; Lewandowsky, S.; Antfolk, J.; Salo, P.; Lindfelt, M.; Oksanen, T.; Kivimäki, M.; Soveri, A. The association between vaccination confidence, vaccination behavior, and willingness to recommend vaccines among Finnish healthcare workers. PLoS ONE 2019, 14, e0224330. [Google Scholar] [CrossRef]
- Tavolacci, M.P.; Dechelotte, P.; Ladner, J. COVID-19 Vaccine Acceptance, Hesitancy, and Resistancy among University Students in France. Vaccines 2021, 9, 654. [Google Scholar] [CrossRef]
- Gallè, F.; Sabella, E.A.; Roma, P.; De Giglio, O.; Caggiano, G.; Tafuri, S.; Da Molin, G.; Ferracuti, S.; Montagna, M.T.; Liguori, G.; et al. Knowledge and Acceptance of COVID-19 Vaccination among Undergraduate Students from Central and Southern Italy. Vaccines 2021, 9, 638. [Google Scholar] [CrossRef]
- Small, M.L.; Lennon, R.P.; Dziak, J.J.; Smith, R.A.; Sommerville, G.; Bharti, N. College students’ COVID-19 vaccine beliefs and intentions: Implications for interventions. J. Am. Coll. Health 2022, 1–6. [Google Scholar] [CrossRef]
- Ministry of Solidarites and Health. 11 Vaccins Obligatoires Depuis 2018. Available online: https://solidarites-sante.gouv.fr/prevention-en-sante/preserver-sa-sante/vaccination/vaccins-obligatoires/article/11-vaccins-obligatoires-depuis-2018 (accessed on 23 March 2022).
- Mascaro, V.; Pileggi, C.; Currà, A.; Bianco, A.; Pavia, M. HPV vaccination coverage and willingness to be vaccinated among 18–30 year-old students in Italy. Vaccine 2019, 37, 3310–3316. [Google Scholar] [CrossRef]
- Glenn, B.A.; Nonzee, N.J.; Tieu, L.; Pedone, B.; Cowgill, B.O.; Bastani, R. Human papillomavirus (HPV) vaccination in the transition between adolescence and adulthood. Vaccine 2021, 39, 3435–3444. [Google Scholar] [CrossRef]
- Zhang, W.; Wang, Q. The failure of news coverage supportive of human papillomavirus vaccination: The investigation of the effects of online comments on female college students’ vaccination intention. Vaccine 2019, 37, 5681–5687. [Google Scholar] [CrossRef]
- Karafillakis, E.; Peretti-Watel, P.; Verger, P.; Chantler, T.; Larson, H.J. “We don’t have the same bodies; we don’t react the same way”: Mothers and adolescent girls’ perceptions of the risks and benefits of HPV vaccination in France. Hum. Vaccines Immunother. 2022, 18, 2036555. [Google Scholar] [CrossRef]
- Wilson, K.L.; White, A.; Rosen, B.L.; Chiappone, A.; Pulczinski, J.C.; Ory, M.G.; Smith, M.L. Factors Associated with College Students’ Intentions to Vaccinate Their Daughters Against HPV: Protecting the Next Generation. J. Community Health 2016, 41, 1078–1089. [Google Scholar] [CrossRef]
- Shmueli, L. Predicting intention to receive COVID-19 vaccine among the general population using the health belief model and the theory of planned behavior model. BMC Public Health 2021, 21, 804. [Google Scholar] [CrossRef]
- Barello, S.; Nania, T.; Dellafiore, F.; Graffigna, G.; Caruso, R. ‘Vaccine hesitancy’ among university students in Italy during the COVID-19 pandemic. Eur. J. Epidemiol. 2020, 35, 781–783. [Google Scholar] [CrossRef]
- Graupensperger, S.; Abdallah, D.A.; Lee, C.M. Social norms and vaccine uptake: College students’ COVID vaccination intentions, attitudes, and estimated peer norms and comparisons with influenza vaccine. Vaccine 2021, 39, 2060–2067. [Google Scholar] [CrossRef]
- Shon, E.J.; Choe, S.; Lee, L.; Ki, Y. Influenza Vaccination Among U.S. College or University Students: A Systematic Review. Am. J. Health Promot. 2021, 35, 708–719. [Google Scholar] [CrossRef]
- Lepiller, Q.; Bouiller, K.; Slekovec, C.; Millot, D.; Mazué, N.; Pourchet, V.; Balice, R.; Garrien-Maire, F.; Simon, E.; Wintenberger, V.; et al. Perceptions of French healthcare students of vaccines and the impact of conducting an intervention in health promotion. Vaccine 2020, 43, 6794–6799. [Google Scholar] [CrossRef]
- Bajos, N.; Spire, A.; Silberzan, L.; EPICOV Study Group. The social specificities of hostility toward vaccination against COVID-19 in France. PLoS ONE 2022, 17, e0262192. [Google Scholar] [CrossRef]
- La Santé Des Femmes en France Direction De La Recherche, Des Etudes, De L’évaluation et Des Statistiques (DREES). Available online: https://drees.solidarites-sante.gouv.fr/publications/etudes-et-resultats/la-sante-des-femmes-en-france-0 (accessed on 17 March 2022).
- Daudel, L.; Mary, J.; Epaulard, O. Perception of mandatory infant vaccines and trust in vaccination among first-year healthcare students: An opportunity window for the training of future healthcare workers. Vaccine 2020, 38, 794–799. [Google Scholar] [CrossRef]
- Biasio, L.R.; Bonaccorsi, G.; Lorini, C.; Pecorelli, S. Assessing COVID-19 vaccine literacy: A preliminary online survey. Hum Vaccin Immunother. 2021, 17, 1304–1312. [Google Scholar] [CrossRef]
- Lin, C.; Tu, P.; Beitsch, L.M. Confidence and Receptivity for COVID-19 Vaccines: A Rapid Systematic Review. Vaccines 2021, 9, 16. [Google Scholar] [CrossRef]
- Vulpe, S.N.; Rughiniş, C. Social amplification of risk and “probable vaccine damage”: A typology of vaccination beliefs in 28 European countries. Vaccine 2021, 39, 1508–1515. [Google Scholar] [CrossRef]
- Sandler, K.; Srivastava, T.; Fawole, O.A.; Fasano, C.; Feemster, K.A. Understanding vaccine knowledge, attitudes, and decision-making through college student interviews. J. Am. Coll. Health 2020, 68, 593–602. [Google Scholar] [CrossRef]
- Biasio, L.R. Vaccine literacy is undervalued. Hum. Vaccines Immunother. 2019, 15, 2552–2553. [Google Scholar] [CrossRef]
- Ratzan, S.C. Vaccine Literacy: A new shot for advancing health. J. Health Commun. 2011, 16, 227–229. [Google Scholar] [CrossRef]
- Badua, A.R.; Caraquel, K.J.; Cruz, M.; Narvaez, R.A. Vaccine literacy: A concept analysis. Int. J. Ment. Health Nurs. 2022; early view. [Google Scholar] [CrossRef]
- Patil, U.; Kostareva, U.; Hadley, M.; Manganello, J.A.; Okan, O.; Dadaczynski, K.; Massey, P.M.; Agner, J.; Sentell, T. Health Literacy, Digital Health Literacy, and COVID-19 Pandemic Attitudes and Behaviors in U.S. College Students: Implications for Interventions. Int. J. Environ. Res. Public Health 2021, 18, 3301. [Google Scholar] [CrossRef]
- Montagni, I.; Mabchour, I.; Tzourio, C. Digital Gamification to Enhance Vaccine Knowledge and Uptake: Scoping Review. JMIR Serious Games 2020, 2, e16983. [Google Scholar] [CrossRef]
- World Health Organization. Behavioral Considerations for Acceptance and Uptake of COVID-19 Vaccines: WHO Technical Advisory Group on Behavioral Insights and Sciences for Health; Meeting Report, 15 October 2020; World Health Organization: Geneva, Switzerland, 2020; Available online: https://apps.who.int/iris/handle/10665/337335 (accessed on 6 April 2022).
- Pennings, S.; Symons, X. Persuasion, not coercion or incentivisation, is the best means of promoting COVID-19 vaccination. J. Med. Ethics 2021, 47, 709–711. [Google Scholar] [CrossRef]
- Abdullahi, L.H.; Kagina, B.M.; Ndze, V.N.; Hussey, G.D.; Wiysonge, C.S. Improving vaccination uptake among adolescents. Cochrane Database Syst. Rev. 2020; early access. [Google Scholar] [CrossRef]
- Observatoire De La Vie Etudiante. Available online: http://www.ove-national.education.fr/publication/8126/.2020 (accessed on 16 May 2022).
- Lazarus, J.V.; Wyka, K.; Rauh, L.; Rabin, K.; Ratzan, S.; Gostin, L.O.; Larson, H.J.; El-Mohandes, A. Hesitant or Not? The Association of Age, Gender, and Education with Potential Acceptance of a COVID-19 Vaccine: A Country-level Analysis. J. Health Commun. 2020, 25, 799–807. [Google Scholar] [CrossRef]
- Johnson, D.K.; Mello, E.J.; Walker, T.D.; Hood, S.J.; Jensen, J.L.; Poole, B.D. Combating Vaccine Hesitancy with Vaccine-Preventable Disease Familiarization: An Interview and Curriculum Intervention for College Students. Vaccines 2019, 7, 39. [Google Scholar] [CrossRef] [Green Version]
- Dib, F.; Mayaud, P.; Chauvin, P.; Launay, O. Online mis/disinformation and vaccine hesitancy in the era of COVID-19: Why we need an eHealth literacy revolution. Hum. Vaccin. Immunother. 2022, 18, 1–3. [Google Scholar] [CrossRef] [PubMed]
| Overall Vaccination Coverage (n = 860) | Non Overall Vaccination Coverage (n = 2229) | p | Effect Size d | Total (n = 3089) | Overall Vaccination Coverage AOR (95% CI) | |
|---|---|---|---|---|---|---|
| Men (%) | 27.0 | 29.2 | 0.22 | 28.6 | Ref | |
| Women (%) | 73.0 | 70.8 | 71.4 | 1.23 (1.02–1.48) | ||
| Years of graduate school | <0.0001 | |||||
| 1st year (%) | 25.6 | 34.7 | 32.2 | 0.76 (0.60–0.95) | ||
| 2nd and 3th year (%) | 43.4 | 44.4 | 44.2 | 0.76 (0.70–1.05) | ||
| 4th year and upper (%) | 31.0 | 20.8 | 23.6 | Ref | ||
| Curriculum | <0.0001 | |||||
| Non-healthcare students (%) | 45.9 | 67.1 | 61.2 | Ref | ||
| Healthcare students (%) | 54.1 | 32.8 | 38.8 | 1.43 (1.19–1.72) | ||
| Useful for the personal health * mean (SD) | 9.2 (1.63) | 8.3 (2.11) | <0.0001 | 0.47 | 8.6 (2.03) | 1.10 (1.01–1.19) |
| Useful for the others health * mean (SD) | 9.2 (1.84) | 8.3 (2.40) | <0.0001 | 0.43 | 8.5 (2.30) | 0.99 (0.93–1.06) |
| Confidence about the vaccination efficacy * mean (SD) | 8.7 (1.83) | 7.7 (2.40) | <0.0001 | 0.46 | 8.0 (2.27) | 0.97 (0.90–1.05) |
| Confidence about the vaccination security * mean (SD) | 8.6 (1.93) | 7.4 (2.41) | <0.0001 | 0.51 | 7.7 (2.34) | 1.13 (1.07–1.70) |
| Knowledge about vaccination mean (SD) | 6.7 (2.17) | 5.6 (2.35) | <0.0001 | 0.50 | 5.9 (2.35) | 1.12 (1.07–1.17) |
| Intention to vaccine against COVID-19 (%) | 73.8 | 51.8 | <0.0001 | 57.9 | 1.37 (1.11–1.70) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Arias, A.; Ladner, J.; Tavolacci, M.-P. Perception and Coverage of Conventional Vaccination among University Students from Rouen (Normandy), France in 2021. Vaccines 2022, 10, 908. https://doi.org/10.3390/vaccines10060908
Arias A, Ladner J, Tavolacci M-P. Perception and Coverage of Conventional Vaccination among University Students from Rouen (Normandy), France in 2021. Vaccines. 2022; 10(6):908. https://doi.org/10.3390/vaccines10060908
Chicago/Turabian StyleArias, Andreina, Joel Ladner, and Marie-Pierre Tavolacci. 2022. "Perception and Coverage of Conventional Vaccination among University Students from Rouen (Normandy), France in 2021" Vaccines 10, no. 6: 908. https://doi.org/10.3390/vaccines10060908
APA StyleArias, A., Ladner, J., & Tavolacci, M.-P. (2022). Perception and Coverage of Conventional Vaccination among University Students from Rouen (Normandy), France in 2021. Vaccines, 10(6), 908. https://doi.org/10.3390/vaccines10060908






