Simple Summary
Checkpoint inhibitors and anti-angiogenic therapies are treatments that slow the progression of renal cell carcinoma, the most common type of kidney cancer. Checkpoint inhibitors and anti-angiogenic therapies work in different ways. Checkpoint inhibitors help to prevent tumors from hiding from the body’s immune system, while anti-angiogenic therapies slow the development of blood vessels that tumours need to help them to grow. Studies have shown that treatment with combination checkpoint inhibitor plus anti-angiogenic therapy can achieve better outcomes for patients with renal cell carcinoma than treatment with anti-angiogenic therapy alone. In this review, we consider how combination checkpoint inhibitor plus anti-angiogenic therapy works, and we review the current literature to identify evidence to inform clinicians as to the most effective way to use these different types of drugs, either one after the other, or together, for maximum patient benefit.
Abstract
Anti-angiogenic agents, such as vascular endothelial growth factor (VEGF) receptor tyrosine kinase inhibitors and anti-VEGF antibodies, and immune checkpoint inhibitors (CPIs) are standard treatments for advanced renal cell carcinoma (aRCC). In the past, these agents were administered as sequential monotherapies. Recently, combinations of anti-angiogenic agents and CPIs have been approved for the treatment of aRCC, based on evidence that they provide superior efficacy when compared with sunitinib monotherapy. Here we explore the possible mechanisms of action of these combinations, including a review of relevant preclinical data and clinical evidence in patients with aRCC. We also ask whether the benefit is additive or synergistic, and, thus, whether concomitant administration is preferred over sequential monotherapy. Further research is needed to understand how combinations of anti-angiogenic agents with CPIs compare with CPI monotherapy or combination therapy (e.g., nivolumab and ipilimumab), and whether the long-term benefit observed in a subset of patients treated with CPI combinations will also be realised in patients treated with an anti-angiogenic therapy and a CPI. Additional research is also needed to establish whether other elements of the tumour microenvironment also need to be targeted to optimise treatment efficacy, and to identify biomarkers of response to inform personalised treatment using combination therapies.
1. Introduction
Historically, the treatment of patients with renal cell carcinoma (RCC) was limited by the lack of efficacy of cytotoxic chemotherapy. While cytokine-based immunotherapies (interleukin-2, interferon-alfa) showed activity, they typically benefited only a small subset of patients [1]. The identification of von Hippel Lindau gene (VHL) mutations in RCC, and the discovery that such mutations induce angiogenic pathways via upregulation of hypoxia inducible factors, led to the development of therapies that target angiogenesis [2,3,4]. Anti-vascular endothelial growth factor (VEGF) monoclonal antibodies (mAbs) and small-molecule tyrosine kinase inhibitors (TKIs) are agents that block VEGF signalling by inactivating VEGF or VEGF receptors (VEGFR), respectively, thereby exerting anti-angiogenic effects within the tumour microenvironment [3]. Another treatment for various cancers including RCC is the emerging class of immune checkpoint inhibitors (CPIs). CPIs act by restoring the immune response against tumour cells, which is selectively suppressed in many cancers [5].
Anti-angiogenic agents (i.e., TKIs and anti-VEGF mAbs) and CPIs have been shown to improve survival in patients with advanced RCC (aRCC) and have become standard treatments for the management of this disease [6,7,8]. These agents have typically been administered as sequential monotherapies, with a first treatment given until disease progression, followed by a switch to a second treatment and possibly further treatments. Combinations of anti-angiogenic agents and CPIs have the potential to target distinct and complementary pathways simultaneously, and provide additional clinical benefit compared with sequential use of single-agent regimens [9,10]. Combination anti-angiogenic agents plus CPIs regimens are under investigation in aRCC, with encouraging clinical data available so far. Indeed, four anti-angiogenic-CPI combination regimens (axitinib plus either pembrolizumab or avelumab, and cabozantinib plus nivolumab and lenvatinib plus pembrolizumab) have been approved by the US Food and Drug Administration (FDA) for the first-line treatment of patients with aRCC.
In this review, we explore the possible mechanism of action of a combination therapy consisting of an anti-angiogenic agent and a CPI for the treatment of patients with aRCC. We also summarise relevant preclinical and clinical evidence on combination therapies and examine whether these data support a synergistic effect of such combinations for critical clinical endpoints. Finally, we discuss the potential benefits or detriments of concomitant versus sequential treatment strategies, the choice of the optimal agents of combinations in terms of tolerability and efficacy, and the role of predictive biomarkers of response to these treatments.
2. Literature Search Strategy
The review draws on published evidence identified by a systematic search of the PubMed bibliometric database. PubMed was initially searched for English-language articles published up to July 2020 reporting preclinical and clinical (phase I, phase II, or phase III) trial data relevant to combination therapy with anti-angiogenic agents and CPIs for the treatment of RCC. Supplemental manual searches were conducted using the proceedings from key congresses (2016–2020) considered by the authors to be of greatest relevance (the Annual Meeting of the American Society of Clinical Oncology [ASCO]; the ASCO Genitourinary Cancers Symposium [ASCO GU]; the Annual Meeting of the European Society for Medical Oncology [ESMO]). Search results were screened manually to identify articles relevant to the review topic (see the Supplementary Table S1 for details of the search strategies, inclusion criteria, and the list of relevant references). During the development of the review, the authors identified additional key articles and congress presentations that were published after the bibliometric search (July 2020). These relevant publications were included to maximise relevance and timeliness of the review.
3. Literature Review and Discussion
3.1. The Tumour Microenvironment—A Complex System Consisting of Multiple Cell Populations
The tumour microenvironment (TME) broadly consists of tumour, immune, endothelial and stromal elements [11]. The immune compartment includes professional antigen-presenting dendritic cells, specific antitumoral effector cell populations such as cytotoxic T cells, inhibitory T-regulatory and TH17 cells, and nonspecific ‘innate’ immune populations such as natural killer (NK) cells, myeloid-derived suppressor cells (MDSC) and tumour-associated macrophages [12,13]. The tug of war between the tumour and the host is strongly influenced by a number of factors, including the molecular biology of the tumour as well as the state of immune system activation.
3.2. Truncal Mutations in Clear Cell RCC Drive Tumour Biology
The genetics and molecular biology of the tumour cell profoundly influence the TME. The most common form of RCC, clear cell renal cell carcinoma (ccRCC), is strongly associated (60–80% of all cases) with mutations in the VHL tumour suppressor gene, located on chromosome 3p, leading to loss of function of the VHL protein [14,15]. VHL is a key component of the hypoxia sensing pathway and a negative regulator of angiogenesis. VHL deficiency leads to hypoxia-independent upregulation of numerous metabolic and pro-angiogenic genes due to the overexpression of hypoxia inducible factors 1 alpha and 2 alpha (HIF-1α and HIF-2α) [16,17]. Pro-angiogenic genes include VEGF, adrenomedullin and angiopoietin 2 [17]. AXL, a signalling molecule associated with both increased tumour invasiveness and aggressivity, is an HIF-1α and HIF-2α client gene and is upregulated in ccRCC tumour cells. Upregulated AXL is associated with a worse prognosis and increased metastatic potential [18,19]. Additionally, ADORA2A, the gene encoding the adenosine 2a receptor (A2AR) is regulated by HIF-1α [20] and HIF-2a [21]. ADORA2A and NT5E (CD73) expression is upregulated in human ccRCC tissue [22], although it is unclear whether this increased expression is driven by tumour or microenvironmental cells.
Secondary mutations in RCC frequently affect chromatin remodelling genes, which are also found on chromosome 3p [23,24,25] and components of the phosphoinositide-3-kinase (PI3K) pathway [15]. Mutations in polybromo-1 (PBRM1), a switch/sucrose nonfermenting (SWI-SNF) complex gene involved in gene access, have been shown to promote angiogenesis [26,27], and activating mutations in the PI3K pathway have been shown to modulate cell growth and angiogenesis in both a hypoxia dependent and independent manner [28].
3.3. ccRCC Driven Changes in TME Influence Endothelial and Immune Compartments
The net effect of the molecular changes in ccRCC is a TME rich in VEGF and other pro-angiogenic and immunoregulatory factors, which impact the immune microenvironment [29]. High levels of circulating VEGF downregulate dendritic cells [30,31] and effector T cells (Figure 1) [32]. A stimulatory effect may be seen on suppressor immune cell populations including regulatory T cells and MDSC (Figure 1). Regulatory T cells themselves have been shown to be pro-angiogenic [33].
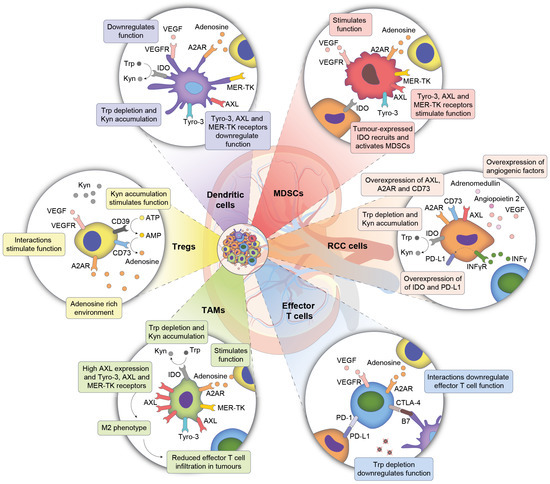
Figure 1.
Interactions of clear cell RCC and the tumour microenvironment. A2AR, adenosine A2A receptor; AMP, adenosine monophosphate; ATP, adenosine triphosphate; CD, cluster of differentiation; CTLA-4, cytotoxic T-lymphocyte-associated protein 4; IDO, indoleamine 2,3-dioxygenase; IFNγ, interferon gamma; IFNγR, IFNγ receptor; Kyn, kynurenine; M2 phenotype, alternatively-activated phenotype; MDSC, myeloid-derived suppressor cell; MER-TK, MER proto-oncogene, tyrosine kinase; PD-1, programmed cell death protein 1; PD-L1, programmed death-ligand 1; RCC, renal cell carcinoma; TAM, tumor-associated macrophage; Treg, regulatory T cell; Trp, tryptophan; Tyro-3, tyrosine-protein kinase receptor TYRO3; VEGF, vascular endothelial growth factor; VEGFR, VEGF receptor.
In normal, non-cancerous physiology, immune checkpoint proteins such as cytotoxic T lymphocyte antigen 4 (CTLA-4) and programmed cell death protein 1 (PD-1) are negative regulators of T cells to maintain self-tolerance and control adaptive immune responses against novel antigens including tumour antigens [5]. Binding of PD-1 to its ligand programmed cell death ligand 1 (PD-L1) results in downregulation of activated T cell function (Figure 1), ultimately leading to T cell exhaustion [5]. CTLA-4, which is expressed following T cell activation, limits the extent of T cell activation by outcompeting the immunostimulatory ligand CD28 in binding B7 on antigen-presenting cells [5]. Using a variety of mechanisms, many cancers co-opt these checkpoint proteins to selectively suppress and escape immune surveillance. For example, upregulation of PD-L1 is driven by a tumour cell-autonomous reaction to immune cell production of interferon gamma in melanoma [34] and in ccRCC [27]. PD-L1 is overexpressed in 23–56% of ccRCCs [35,36,37].
Expression of Tyro-3, MER-TK and AXL also occurs on tumour-associated macrophages. High AXL expression is associated with a shift towards an M2, immunosuppressive phenotype, and a decrease in effector immune cell infiltration in the RCC tumour microenvironment [27,38,39]. Microenvironmental adenosine, which is generated via CD39 and CD73 mediated conversion of adenosine triphosphate to adenosine (Figure 1), inhibits the antitumor function of various immune cells, including components of the adaptive and innate immune systems, by binding to cell surface A2AR [40,41,42]. Conversely, A2AR enhances the immunosuppressive activity of myeloid and regulatory T cells [43].
Indoleamine 2,3 dioxygenase (IDO) is a cell surface receptor involved in tryptophan metabolism [44]. High levels of interferon gamma-induced IDO production by macrophages was originally shown to reduce T cell function [45]. IDO is upregulated in multiple cancers, and has been shown to suppress effector T cell function and induce regulatory T cells and MDSCs (Figure 1) [46]. IDO is upregulated in ccRCC, and is predominantly found on endothelial cells [47]. Intriguingly, IDO appears to promote angiogenesis by inhibiting IFN-gamma-mediated vascular pruning by immune cells [46].
3.4. Components of Combination Therapy: Mechanism of Action of Anti-Angiogenic Agents
VEGF-targeted anti-angiogenics inhibit VEGF signalling, thereby blocking its pro-angiogenic and immunomodulatory functions within the tumour microenvironment [3,4]. TKIs are small molecules that inhibit VEGFR by binding to its active domain, and include agents such as sorafenib, pazopanib, sunitinib, axitinib, cabozantinib, lenvatinib, and tivozanib [3] (Figure 2; Supplementary Table S2). Anti-VEGF mAbs, such as bevacizumab, bind directly to VEGF and prevent its interaction with VEGFR [3] (Figure 2; Supplementary Table S2). In aRCC, blocking of VEGFR by TKIs has been shown to result in a number of physiological changes, including reduced blood vessel density, alterations in pericyte coverage, and decreased tumour perfusion, which may lead to acute infarction of the VEGF-dependent tumour microenvironment and tumour necrosis [48,49,50,51]. Vascular remodelling without necrosis that can lead to enhanced T cell infiltration of the tumour microenvironment has also been observed with these agents [50,52].
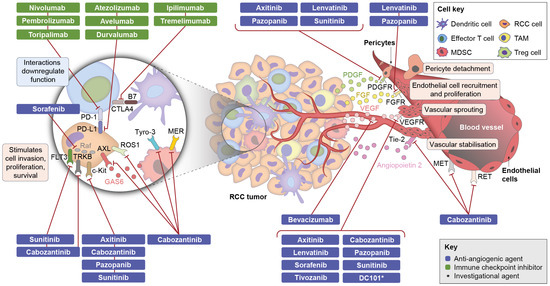
Figure 2.
Effects of RCC therapies within the tumour microenvironment CTLA-4, cytotoxic T-lymphocyte-associated protein 4; FGF, fibroblast growth factor; FGFR, FGF receptor; FLT3, FMS-like tyrosine kinase 3; GAS6, growth arrest-specific 6; MDSC, myeloid-derived suppressor cell; MET, mesenchymal-epithelial transition factor or hepatocyte growth factor receptor; PD-1, programmed cell death protein 1; PD-L1, programmed death-ligand 1; PDGF, platelet-derived growth factor; PDGFR, PDGF receptor; Raf, proto-oncogene serine/threonine protein kinase; RCC, renal cell carcinoma; RET, rearranged during transfection receptor; TAM, tumor-associated macrophage; Tie-2, tyrosine kinase with immunoglobulin and epidermal growth factor homology domains-2; Treg, regulatory T cell; TRKB, tropomyosin receptor kinase B; Tyro-3, tyrosine-protein kinase receptor TYRO3; VEGF, vascular endothelial growth factor; VEGFR, VEGF receptor.
Most TKIs targeting VEGFR also block additional tyrosine kinases, including platelet-derived growth factor receptor (PDGFR; pazopanib, sunitinib, axitinib, lenvatinib), c-Kit (cabozantinib, sunitinib, pazopanib), FLT3 (sunitinib, cabozantinib), MET (cabozantinib), AXL (cabozantinib), or fibroblast growth factor receptor (FGFR; pazopanib, lenvatinib) [53]. Many of these additional targets, such as MET, PDGFR and c-Kit, are implicated in angiogenesis as well as tumour cell proliferation [3,53]. Furthermore, PDGFR, MET, AXL, and FGFR have been shown to play a role in resistance to VEGFR inhibition, which is common with TKIs and results primarily from ‘angiogenic escape’ through activation of compensatory vascular signalling pathways [3,19,53]. Inhibition of the VEGF pathway together with these additional targets may therefore simultaneously target multiple and parallel key pathways important to tumour vascularisation and growth (Figure 2; Supplementary Table S2).
3.5. Components of Combination Therapy: Mechanism of Action of CPIs
CPIs are monoclonal antibodies that block checkpoint proteins, thereby restoring the anti-tumour immune response [5]. Nivolumab and pembrolizumab (anti-PD-1) and atezolizumab and avelumab (anti-PD-L1) block the interaction of PD-L1 and PD-1, thereby permitting a T cell anti-tumour response [5] (Figure 2; Supplementary Table S2). Ipilimumab (anti-CTLA-4) inhibits CTLA-4, thereby releasing B7 to bind to CD28 and resulting in augmented antigen presentation and T cell activation [5] (Figure 2; Supplementary Table S2).
3.6. Possible Mechanisms of Action of Combination Therapies
The combination of an anti-angiogenic agent and a CPI could potentially provide a clinical benefit compared with monotherapy either by acting additively, with both agents having independent effects, or by acting synergistically, with one agent enhancing or prolonging [54] the activity of the other (Figure 2; Supplementary Figure S1). However, anti-angiogenics and CPIs could conversely have antagonistic effects, thereby dampening the outcome compared with the additive effect obtained with sequential monotherapies (Figure 2; Supplementary Figure S1) [9,10]. In the following, we review relevant preclinical and clinical data on combination therapies in comparison with monotherapies, which may help to elucidate the mechanism of the action of combination therapies.
3.7. Preclinical Data on Immune-Modulatory Activities of Anti-Angiogenic Agents in RCC
Available preclinical data on monotherapy with TKIs and anti-VEGF mAbs in VHL wild type RCC models indicate that targeting the VEGF pathway alleviates immunosuppression in the tumour microenvironment (Table 1; Figure 2). For example, bevacizumab, sunitinib, and cabozantinib have been shown to increase infiltration of the tumour with cytotoxic T cells [50,55,56,57]. This indirect effect of TKIs and bevacizumab on immune cells may result from normalisation and remodelling of the tumour vasculature [51] or expression of T cell chemokines [10], and is likely mediated by inhibition of the VEGF signalling pathway [10]. TKIs and anti-VEGF mAbs have also been shown to have direct effects on immune cells by targeting myeloid and lymphoid cells that express relevant receptors including VEGFR, FLT3, MET, c-KIT, or members of the TAM receptor kinase family (TYRO, AXL, MER) [58] (Figure 2). Bevacizumab, sunitinib, cabozantinib, sorafenib, and axitinib have been shown to stimulate the differentiation of monocytes into dendritic cells, increase levels of cytotoxic T cells, and to reduce the levels and homing of regulatory T cells and MDSCs to tumours [55,56,59,60,61,62,63,64,65,66], effects which may help to counteract cancer-immune tolerance and stimulate an immune reaction against the tumour. Targets other than the VEGF pathway may be implicated in these direct effects on immune cells. For example, c-Kit is involved in accumulation of MDSCs and the development of regulatory T cells [67], and members of the TAM receptor kinase family are involved in the tumour-associated macrophage transition from M1 (immune-stimulating) to M2 (immune-suppressive) [68]. Another immune-modulatory effect observed with cabozantinib is the reduction in PD-L1 expression on tumour cells, thereby increasing the tumour’s sensitivity to T cell-mediated killing [69,70]. This effect may be mediated by inhibiting c-MET, which is a stimulatory factor of PD-L1 expression and which is overexpressed in many RCCs [69,70]. However, it should be noted that PD-L1 expression does not predict response to cabozantinib therapy [71]. In line with these in vitro observations, there is also in vivo evidence from animal models of non-ccRCC and other tumours, which suggests that combinations of a TKI (including sunitinib or cabozantinib) with immune-based therapies (e.g., chimeric antigen receptor-modified T cells) increase the anti-tumour efficacy (based on tumour shrinkage) and prolong survival compared with immuno-monotherapy [61,67,69].

Table 1.
Immune-modulatory effects of anti-VEGF TKIs and mAbs in RCC.
However, there are also reports that some anti-angiogenic agents may have antagonistic effects on the CPI response and increase, rather than decrease, immunosuppression of the tumour microenvironment. For example, sunitinib and bevacizumab have been shown to increase the levels of circulating and tumour-infiltrating regulatory T cells or MDSCs [50,72,73] possibly as a response to VEGF blockade-dependent hypoxia and the ensuing upregulation of chemokines such as SDF-1 (CXCL12) [73]. There are also reports of reduced responsiveness of dendritic cells to inflammatory signals with sorafenib [74], and sunitinib and bevacizumab have been found to increase expression of PD-L1 [50,74]. Furthermore, the increase in tumour immunosuppression has been associated with the development of resistance to anti-angiogenic agents [50,75]. This effect might be mediated by MDSCs that produce pro-angiogenic proteins, or reprogrammed T lymphocytes that possess immunosuppressive characteristics. However, in the absence of immune-competent models of VHL null ccRCC, it remains unclear which (if any) of these preclinical findings apply to the unique biology of this disease.
3.8. Clinical Data on Combination Therapies
The first VEGF-targeted anti-angiogenic plus CPI combinations in a phase I trial in patients with aRCC tested the combination of sunitinib or pazopanib plus nivolumab. With both regimens, substantial clinical activity was observed but high-grade toxicities limited future development of either combination regimen [76]. Other combinations studied in RCC were pazopanib plus pembrolizumab, and sunitinib plus tremelimumab. Again, both regimens were not further investigated owing to unfavourable tolerability [77,78].
More recently, other combinations of anti-angiogenics and CPIs have been investigated in aRCC with varying results. A phase III trial (NCT02420821) of atezolizumab plus bevacizumab versus sunitinib in the first-line setting assessed progression-free survival (PFS) in patients with PD-L1+ tumours and overall survival (OS) in the overall study population as co-primary endpoints (Table 2) [79]. In patients with PD-L1+ tumours, atezolizumab plus bevacizumab demonstrated significantly longer PFS (investigator assessed) than sunitinib (hazard ratio [HR] PFS, 0.74 [95% confidence interval, CI, 0.57–0.96]; p = 0.0217); in the overall study population, there was no significant difference in PFS between atezolizumab plus bevacizumab versus sunitinib. However, when efficacy endpoints were assessed by an independent review committee (IRC), PFS in patients with PD-L1+ tumours was similar between the combination and sunitinib monotherapy (HR PFS, 0.93 [0.72–1.21]). Notably, in the IRC PFS analysis, there was a trend for longer PFS with the combination versus sunitinib in patients with PD-L1-negative disease (PD-L1 expression < 1%)(HR PFS, 0.84 [0.67–1.04]), suggesting that the PD-L1 expression level may not be an appropriate predictive biomarker for selecting patients for this combination, or that the Ventana SP142 test used in this study, which scored immune cell PD-L1 positivity but not tumour cell positivity, may not be the ideal assay. Median OS was comparable between the combination and sunitinib monotherapy both overall and in patients with PD-L1+ tumours further suggesting that any benefits from this combination were, at best, additive rather than synergistic [79].
Four other anti-angiogenic–CPI combinations have recently been approved as first-line treatments of aRCC based on positive findings in phase III trials (Table 2). The combination of pembrolizumab plus axitinib (approved by the FDA in April 2019) versus sunitinib was investigated in treatment-naïve patients with aRCC, with OS and PFS in the intention-to-treat population as co-primary study endpoints (NCT02853331) [80,81]. At the first interim analysis, median follow-up of 13 months, the risk of death was 47% lower with pembrolizumab plus axitinib than with sunitinib (HR [95% CI] OS, 0.53 [0.38–0.74]; p < 0.0001). The combination was also associated with a lower risk of disease progression (HR PFS, 0.69 [0.57–0.84]; p < 0.001) and higher objective response rate (ORR; 59.3% versus 35.7%; p < 0.001) than sunitinib monotherapy. The survival benefits of pembrolizumab plus axitinib versus sunitinib for OS and PFS were observed in all subgroups examined, including all International Metastatic RCC Database Consortium (IMDC) risk groups and PD-L1 expression categories [80]. In a subsequent analysis conducted at median follow-up of 27 months, the PFS benefit was maintained (HR, 0.71), but the OS benefit was reduced (HR [95% CI] OS, 0.68 [0.55–0.85]; p < 0.001) and was no longer apparent for the favourable risk population (HR [95% CI] OS, 1.06 [0.60–1.86]) [82]. Pembrolizumab plus axitinib continued to demonstrate superior efficacy (vs. sunitinib) at the time of the final prespecified analysis (42.8 months median follow-up) in terms of PFS (HR [95% CI] 0.68 [0.58–0.80]; p < 0.0001) and OS (HR [95% CI] 0.73 [0.60–0.88]; p < 0.001) and with an ORR of 60.4% vs. 39.6% (p < 0.0001) [81].
The combination of avelumab plus axitinib (approved by the FDA in May 2019) has also been assessed versus sunitinib as first-line treatment for aRCC in a phase III trial (NCT02853331) with PFS and OS in the subset of patients with PD-L1+ tumours included as independent primary endpoints [83,84]. Patients with PD-L1+ tumours receiving avelumab plus axitinib had improved PFS (HR, 0.62 [0.49–0.78]; p < 0.001) and ORR (odds ratio, 3.39 [2.35–4.90]) compared with those receiving sunitinib. The PFS and ORR benefits of the combination were also observed in the overall study population (HR PFS, 0.69 [0.57–0.83]; p < 0.001; odds ratio ORR, 3.00 [2.23–4.00]). OS data were immature in most recent analyses [84].
A phase III trial (N = 651; NCT03141177) tested the combination of cabozantinib plus nivolumab versus sunitinib in previously untreated patients with aRCC [85]. The primary endpoint was PFS, as determined by a blinded independent central review. At a median follow-up of 18 months, the median PFS was 16.6 months (95% CI, 12.5–24.9) with nivolumab plus cabozantinib and 8.3 months (95% CI, 7.0–9.7) with sunitinib (HR for disease progression or death, 0.51 [0.41–0.64]; p < 0.001). The probability of OS at 12 months was 86% (95% CI, 81–89) with nivolumab plus cabozantinib and 76% (95% CI, 71–80) with sunitinib (HR, 0.60 [98.89% CI, 0.40–0.89]; p = 0.001). An objective response occurred in 56% of the patients receiving nivolumab plus cabozantinib and in 27% of those receiving sunitinib (p < 0.001). Efficacy benefits with nivolumab plus cabozantinib were consistent across IMDC subgroups; particularly notable was the PFS benefit for nivolumab plus cabozantinib in patients with bone metastases (HR, 0.38 [95% CI, 0.25–0.59]) [86]. The combination received FDA approval in January 2021 for the treatment of patients with aRCC.
In a phase 1b/2 trial (NCT02501096), the combination of lenvatinib plus pembrolizumab showed an impressive 51% (40–61%) ORR in patients with aRCC who had progressed despite prior CPI therapy, potentially signalling a favourable front-line result [87]. In a follow-up phase III trial (NCT02811861), patients with aRCC and no previous systemic therapy (N = 1069) were randomly assigned to receive lenvatinib (20 mg orally once daily) plus pembrolizumab (200 mg intravenously once every 3 weeks), lenvatinib (18 mg orally once daily) plus everolimus (5 mg orally once daily), or sunitinib [88]. The primary endpoint was PFS, as assessed by an independent review committee. PFS was significantly longer for lenvatinib plus pembrolizumab compared with sunitinib (23.9 versus 9.2 months, respectively; HR, 0.39 [0.32–0.49]; p < 0.001). OS was also longer with lenvatinib plus pembrolizumab than with sunitinib (HR, 0.66 [0.49–0.88]; p = 0.005) but was similar for lenvatinib plus everolimus and sunitinib (HR, 1.15 [0.88–1.50]; p = 0.30).
Other combination regimens involving the TKIs–tivozanib plus nivolumab and cabozantinib plus atezolizumab or nivolumab ± ipilimumab are under investigation in a number of phase I or phase I/II studies (Table 3), with (preliminary) reported ORRs ranging from 25% to 71% [89,90,91,92,93,94]. Of note, the majority of these phase III studies use sunitinib as a control arm rather than the combination of nivolumab plus ipilimumab, which has been established to be superior to sunitinib. For cabozantinib, an additional evaluation of cabozantinib plus nivolumab and ipilimumab versus nivolumab and ipilimumab is being undertaken to help address this deficiency in the current data (NCT03937219).
In terms of tolerability of the currently approved CPI/anti-angiogenic combinations, hypertension, fatigue, and diarrhoea were among the most common any grade adverse events (AEs) reported in the phase III trials of avelumab plus axitinib, and pembrolizumab plus axitinib; incidences were generally similar to those in the sunitinib monotherapy arms [80,83]. Phase III trials of atezolizumab plus bevacizumab found hypertension, fatigue, diarrhoea and proteinuria to be the most common AEs, but that atezolizumab plus bevacizumab offered a more favourable overall toxicity profile than sunitinib monotherapy (Table 2) [79]. Elevated levels of liver enzymes were among the most common grade 3 or 4 AEs reported for avelumab plus axitinib, and pembrolizumab plus axitinib, and were also more frequent among patients treated with atezolizumab plus bevacizumab than with sunitinib monotherapy [79,80,83]. The most common AEs with the combination of cabozantinib plus nivolumab were diarrhoea, palmar–plantar erythrodysesthesia syndrome (PPES), hypertension, hypothyroidism and fatigue; and the most common grade ≥ 3 AEs were hypertension, hyponatraemia and PPES [85]. For the combination of lenvatinib plus pembrolizumab the most common AEs were diarrhoea, hypertension, hypothyroidism, decreased appetite and fatigue [88]. Hypertension was the most common grade ≥ 3 AE with the lenvatinib plus pembrolizumab combination [88].
Hypothyroidism was reported with all of the combinations; the incidence of hypothyroidism (any grade) ranged from 22% to 47% [79,80,83,85,88], which is higher than expected with CPI monotherapies and may in part be related to the known effect of axitinib on thyroid function [80]. These findings, and in particular the results with the less selective VEGF pathway inhibitors [53] sunitinib or pazopanib, suggest that the tolerability of a combination regimen may depend on careful selection of the type of anti-angiogenic agent, its dose, and potentially its timing.
A number of the treatment-related toxicities described above, including diarrhoea, transaminitis and fatigue, could arise from either anti-angiogenic or CPI therapy, or both. One proposed approach to triaging and managing such overlapping toxicities in patients receiving combination anti-angiogenic/CPI therapy involves withholding the anti-angiogenic agent in patients experiencing grade 1–2 overlapping toxicities, to see if symptoms improve [95]. If grade 3 toxicities arise, the approach recommends withholding both agents, with judicious resumption of either, or both, once toxicities resolve. Consideration of permanent discontinuation of either, or both, agents is recommended in patients who experience grade 4 toxicities [95].
3.9. Open Questions and Clinical Relevance of the Mechanism of Action of Combination Therapy
The phase III trials of atezolizumab plus bevacizumab, avelumab plus axitinib, pembrolizumab plus axitinib, nivolumab plus cabozantinib and lenvatinib plus pembrolizumab demonstrated a clinical benefit with the combination regimen over sunitinib monotherapy. It remains unclear, however, whether the observed improvement with the combinations relative to sunitinib reflects additive, synergistic, or even sub-additive effects of the individual components due to the lack of clear-cut clinical readouts of biological synergy.
Certain endpoints and clinical observations will help determine whether combination therapy is preferred over sequential administration of several therapies. In the case of additive effects, concomitant administration is likely to result in the same clinical outcome as sequential administration; in the case of a synergistic interaction, however, concomitant use of anti-angiogenics and CPIs may provide greater clinical benefit than their sequential administration, such as improvements in complete and durable response rates, as well as the ability to stop therapy while maintaining response. Additionally, the PFS with the combination regimen should exceed the overall PFS observed with the sequential approach and the median OS, landmark OS, or cumulative treatment-free survival would be superior with the combination than with the agents used in sequence (Figure 3). On the other hand, concomitant use may lead to additive or even synergistic AEs, owing to simultaneous exposure to multiple drugs. Combination regimens would possibly also involve each component being administered for a longer time period than when used sequentially, and this could prolong exposure to treatment-related toxicities (and costs). Whereas early combinations involving pazopanib and sunitinib have shown unfavourable safety profiles, available phase III data of combinations with axitinib [80,83], cabozantinib [89,90,91], lenvatinib [93], or tivozanib [92] suggest more favourable tolerability with these regimens (Table 2). Further research is needed to establish the optimal components, doses and duration of treatment with these combination regimens.
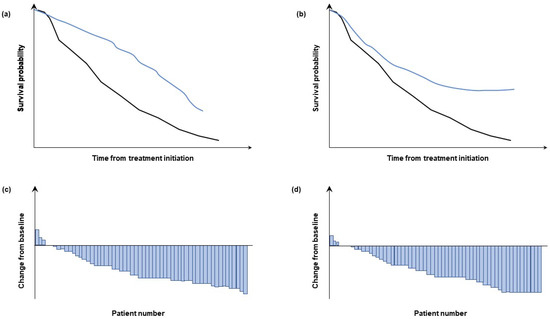
Figure 3.
Illustration of the implications of meaningful clinical read out selection for establishing the potential additive versus synergistic effects of anti-VEGF and CPI therapies. Kaplan–Meier curves showing (vs. black reference group) a continued drop off (a) versus a plateau (b) and waterfall plots (c,d) with differing shoulders but the same median. CPI, checkpoint inhibitor; VEGF, vascular endothelial growth factor.
Instead of combining a CPI with an anti-angiogenic agent, a combination could also involve two CPIs, such as nivolumab plus ipilimumab [36], which is approved in the US and Europe for first-line treatment of RCC. In these regimens, both agents act on the immune system via complementary pathways to further potentiate the anti-tumour immune reaction. However, owing to the similar AE profiles of CPIs (resembling inflammatory pathologies and rheumatic diseases) [96,97,98], CPI–CPI combinations could lead to enhanced immune-related toxicity. No direct comparative data are available assessing the safety of CPI–CPI versus CPI–anti-angiogenic combinations in aRCC; based on cross-study comparisons, certain treatment-related AEs such as rash or colitis appear to be more frequent with CPI–CPI regimens than with CPI monotherapies in aRCC [36,99]. Further comparisons of CPI–CPI versus CPI–anti-angiogenic combinations have yet to be initiated to address these critical questions.
3.10. Choosing a Particular Combination Regimen
With multiple CPI-based combination regimens available for front-line use in RCC, treatment decisions have to be made with the goal of optimising patient outcomes. In the absence of head-to-head comparator trials, it can be tempting to compare results across studies, but such comparisons are fraught with hazards. Although all of the pivotal benchmark CPI-based combination trials used sunitinib as the control arm, there are multiple potential (non-treatment) effect-modifying differences between the various trials. These include, but are not limited to, differences in patient populations, in outcome and PD-L1 expression definitions and in trial design (e.g., different use of endpoints, crossover permissibility, length of accrual, censoring and scheduling and means of assessment) and are summarised in Supplementary Table S3.
Additionally, no CPI–anti-VEGF trials have used endpoints such as landmark PFS, landmark OS and treatment-free survival, which are typically associated with an effective immune response against the tumour [100].
The different receptor kinases that the available TKI target may influence their safety profiles, and pharmacokinetic variation of these TKIs may affect the ability to discern treatment-related toxicities of the specific agent within treatment combinations (Supplementary Table S3). When considering the viability of between-trial comparisons of quality-of-life outcomes, the assessment tool and assessment schedule are also important factors to consider (Supplementary Table S3).
Thus, to inform clinical decision-making, there is both a need for longer follow-up of existing trials and also for additional studies specifically designed to compare regimens directly and using standardised biomarkers, endpoints relevant to the immunotherapy era, and universally available crossover and salvage CPI therapy. Some key exploratory endpoints for consideration when designing future registration trial are summarised in Figure 4.
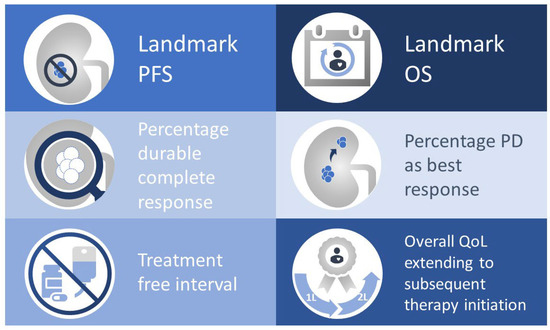
Figure 4.
Potential endpoints for future registrational strategies. OS, overall survival; PD, progressive disease; PFS, progression-free survival; QoL, quality of life.
3.11. Predictive Biomarkers for Combination Therapies
Predictive biomarkers could help identify patients who are more likely to respond to combination therapy. PD-L1 was initially thought to be a promising candidate predictor for anti-PD-1/PD-L1-based treatments, based on its overexpression in a subset of ccRCC tumours (23–56% depending on assay [35,36,37]) and because of its association with poor prognosis [37]. However, its role is not well understood [37,101], and the available clinical trial data are not conclusive. Whereas, in some analyses, patients with PD-L1+ tumours seemed to respond better to the combination than to sunitinib monotherapy [102], other analyses showed combination therapy to be more beneficial than sunitinib across all PD-L1 subgroups [80] or in fact in patients with PD-L1-negative disease only [79]. This suggests that PD-L1 may not be entirely predictive of a CPI combination response but may in fact be a measure of poor prognosis and a predictor of inferior response to anti-angiogenic agents.
Other potential response biomarkers could be based on the gene expression signatures of immune response pathways, as reported in the phase II trial assessing atezolizumab plus bevacizumab versus sunitinib [102]. It was found that the clinical benefit was greater with atezolizumab plus bevacizumab than with sunitinib in patients with high expression of the T-effector gene signature, and that sunitinib was more effective than atezolizumab monotherapy (but showed a similar benefit to atezolizumab plus bevacizumab) in tumours with high myeloid inflammation gene expression [102]. The improved clinical outcome with atezolizumab plus bevacizumab compared with atezolizumab monotherapy in the high myeloid inflammation subgroup suggests a role for bevacizumab in overcoming innate inflammation-mediated resistance in these tumours. Whether this effect on MDSCs is sufficient to enhance the durability of memory T cell activation and lead to a durable off-treatment response remains to be determined.
Several additional in-depth high-throughput immune profiling studies provide a broader picture of the immune system landscape to aid identification of a range of biomarkers which could allow personalised application of combination therapies [38,39,103,104,105] (summarised in [14]). These studies identify subsets of patients with distinct TME phenotypes, including those that are more broadly angiogenic versus immune cell infiltrated. Recently, an analysis of the IMmotion 151 dataset identified seven molecular subtypes with differential response to sunitinib versus atezolizumab plus bevacizumab, with genomic features correlating to specific subsets [104]. Mutations in PBRM1 and KDM5C were associated with angiogenic and stromal subtypes, and these subtypes were most likely to respond to sunitinib. Mutations in CDKN2A/B and TP53 were associated with proliferative subtypes and sarcomatoid histology, and these subtypes were more likely to respond to atezolizumab plus bevacizumab [104]. Whether these profiles can be employed in therapeutic decision-making, particularly with regard to the current FDA-approved combination regimens, requires prospective validation.
Lastly, there is controversy over the impact of chromatin remodelling gene mutations in RCC on treatment response in RCC. Whereas some studies have implicated PBRM1 mutations as a having a positive influence on immunotherapy response [38,106,107], others have suggested that, in the VEGFR TKI naïve population, PRBM1 mutations may be associated with decreased response to immune therapy [27,102]. Future work is needed to clarify these observations and to expand them to the impact of SETD2 and BAP1 mutations on immunotherapy response.

Table 2.
Efficacy and safety results reported for phase III trials of TKIs/anti-VEGF mAb plus CPI combinations in patients with RCC.
Table 2.
Efficacy and safety results reported for phase III trials of TKIs/anti-VEGF mAb plus CPI combinations in patients with RCC.
| Combination | Study Phase | Patient Population | Efficacy | Safety | Reference |
|---|---|---|---|---|---|
| Anti-VEGF mAb + CPI | |||||
| Bevacizumab + atezolizumab versus sunitinib (NCT02420821) | III | mRCC (treatment-naïve) | PFS; ORR Overall (N = 915)
| Grade 3–4 TRAEs
| [79] |
| TKI + CPI | |||||
| Pembrolizumab + axitinib versus sunitinib (NCT02853331) | III | aRCC (treatment-naïve) | PFS; ORR; survival after 12 months Overall (N = 861)
| Grade 3–4 AEs
| [80,108,109] |
| Avelumab + axitinib versus sunitinib (NCT02684006) | III | RCC (treatment-naïve) | PFS; ORR Overall (N = 886)
| Grade 3–4 TEAEs (overall population)
| [83,84,110,111] |
| Cabozantinib + nivolumab versus sunitinib (NCT03141177) | III | aRCC (treatment-naïve) | PFS; ORR Overall (N = 651)
| Grade ≥ 3 AEs
| [85] |
| Lenvatinib + pembrolizumab, lenvatinib + everolimus versus sunitinib (NCT02811861) | III | aRCC (treatment-naïve) | PFS; ORR Overall (N = 1069)
| Grade ≥ 3 AEs
| [88] |
AE, adverse event; ALT, alanine aminotransferase; Anti-VEGF, anti-vascular endothelial growth factor; aRCC, advanced renal cell carcinoma; AST, aspartate aminotransferase; CPI, checkpoint inhibitor; mAb, monoclonal antibodies; mRCC, metastatic renal cell carcinoma; NE, not estimable; NR, not reported; ORR, objective response rate; OS, overall survival; PD-L1, programmed cell death ligand 1; PD-L1+, PD-L1-selected population; PPES, palmar–plantar erythrodysesthesia syndrome; PFS, progression-free survival; sRCC, RCC with sarcomatoid histology; TEAE, treatment-emergent adverse event; TKI, tyrosine kinase inhibitor; TRAE, treatment-related adverse event.

Table 3.
Ongoing clinical trials of combination CPI/anti-VEGF-targeted therapy (TKI or mAb) in RCC.
Table 3.
Ongoing clinical trials of combination CPI/anti-VEGF-targeted therapy (TKI or mAb) in RCC.
| NCT Number | Phase | Population | Intervention | Agent type | Statusref | ||
|---|---|---|---|---|---|---|---|
| Anti-PD-1 | Anti-PD-L1 | Anti-CTLA-4 | |||||
| TKI + CPI | |||||||
| NCT02493751 | I | RCC (treatment-naïve) | Axitinib + avelumab | x | Active, with results [112,113] | ||
| NCT02684006 | III | RCC (treatment-naïve) | Axitinib + avelumab versus sunitinib | x | Active, with results [83,84,113,114] | ||
| NCT03341845 | II | Localised RCC | Axitinib + avelumab as neo-adjuvant | x | Recruiting [115] | ||
| NCT04698213 | II | Metastatic RCC | Avelumab + intermittent axitinib | x | Recruiting | ||
| NCT02133742 | Ib | Treatment-naïve aRCC | Axitinib + pembrolizumab | x | Complete, with results [116] | ||
| NCT04370509 | II | Locally advanced or metastatic RCC | Axitinib + pembrolizumab | x | Recruiting | ||
| NCT02853331 | III | RCC | Axitinib + pembrolizumab versus sunitinib | x | Active, with results [80,113,117] | ||
| NCT03086174 | Ib | RCC and melanoma | Axitinib + toripalimab | x | Active | ||
| NCT03172754 | I/II | aRCC | Axitinib + nivolumab | x | Recruiting | ||
| NCT02496208 | I | Genitourinary tumours including RCC | Cabozantinib + nivolumab ± ipilimumab | x | x | Recruiting, with results [86,89] | |
| NCT03200587 | I | mRCC | Cabozantinib + avelumab | x | Active | ||
| NCT03170960 | Ib | Solid tumours including RCC | Cabozantinib + atezolizumab | x | Recruiting, with results [90] | ||
| NCT03149822 | I/II | mRCC | Cabozantinib + pembrolizumab | x | Active, with results [91] | ||
| NCT03635892 | II | Non-ccRCC | Cabozantinib + nivolumab | x | Recruiting | ||
| NCT04413123 | II | Non-ccRCC | Cabozantinib + nivolumab + ipilimumab | x | x | Recruiting | |
| NCT04322955 | II | Metastatic ccRCC | Cabozantinib + nivolumab + Cytoreductive nephrectomy | x | Recruiting | ||
| NCT03866382 | II | Non-ccRCC | Cabozantinib + nivolumab + ipilimumab | x | x | Recruiting | |
| NCT03141177 | III | mRCC (treatment-naïve) | Cabozantinib + nivolumab versus sunitinib | x | Active, with results [85] | ||
| NCT03937219 | III | mRCC (treatment-naïve) | Cabozantinib + nivolumab + ipilimumab versus nivolumab + ipilimumab | x | x | Active | |
| NCT04338269 | III | Locally advanced or metastatic RCC | Cabozantinib + atezolizumab versus cabozantinib | x | Recruiting | ||
| NCT03937219 | III | Treatment-naïve locally advanced or metastatic RCC | Cabozantinib + nivolumab + ipilimumab versus nivolumab + ipilimumab | x | x | Active | |
| NCT03793166 | III | mRCC | Cabozantinib + nivolumab versus nivolumab | x | Recruiting [118] | ||
| NCT03136627 | I/II | mRCC | Tivozanib + nivolumab | x | Active, with results [92,119] | ||
| NCT03006887 | Ib | Solid tumours including RCC | Lenvatinib + pembrolizumab | x | Completed | ||
| NCT02501096 | Ib/II | Solid tumours including RCC | Lenvatinib + pembrolizumab | x | Active, with results [87,93,94,120,121] | ||
| NCT02811861 | III | RCC | Lenvatinib + pembrolizumab or lenvatinib + everolimus versus sunitinib | x | Active, with results [88] | ||
| Anti-VEGF mAb + CPI | |||||||
| NCT02210117 | I | mRCC amenable to curative surgery | mRCC amenable to curative surgery | x | x | Active, with results [122] | |
| NCT02348008 | Ib/II | RCC | Pembrolizumab + bevacizumab | x | Completed, with results [123,124] | ||
| NCT02420821 | III | mRCC (treatment-naïve) | Atezolizumab ± bevacizumab versus sunitinib | x | Active, with results [79,125] | ||
Anti-VEGF, anti-vascular endothelial growth factor antibodies; aRCC, advanced renal cell carcinoma; ccRCC, clear cell renal cell carcinoma; CPI, checkpoint inhibitor; CTLA-4, cytotoxic T lymphocyte antigen; mAb, monoclonal antibody; mRCC, metastatic renal cell carcinoma; NCT, National Clinical Trial; PD-1, programmed cell death protein 1; PD-L1, programmed cell death ligand 1; RCC, renal cell carcinoma; Ref, related reference; TKI, tyrosine kinase inhibitor.
4. Conclusions
The interest in combining anti-angiogenic agents with a CPI for the treatment of aRCC, initially driven by clinical observations, has been fostered by findings that anti-angiogenic TKIs and anti-VEGF mAbs may also have immune-modulatory effects. The available clinical data suggest that combinations of anti-angiogenics and CPIs provide a clinical benefit in patients with aRCC relative to sunitinib monotherapy. Safety profiles have been shown to vary depending on the individual components, highlighting the importance of selecting the optimal agent and dose. The question as to whether the efficacy benefit observed with combination treatments is additive or synergistic, and whether concomitant administration is preferred over sequential mono-modality approaches, and if so in which patients, is unlikely to be answered by the current trials and therefore will require further investigation. Validated biomarkers of response to CPI-based combination regimens would facilitate personalised treatment with a specific combination or a sequence of single-agent/single modality-regimens.
Supplementary Materials
The following supporting information can be downloaded at: https://www.mdpi.com/article/10.3390/cancers14030644/s1, Figure S1. Schematic diagram of the possible mechanisms of action of anti-angiogenic plus CPI combination therapy in RCC; Table S1: Anti-angiogenic agents and immune checkpoint inhibitors for the treatment of aRCC; Table S2: Anti-angiogenic agents and immune checkpoint inhibitors for the treatment of aRCC; Table S3: Considerations for interpreting results of CPI/anti-VEGF treatment combinations in RCC.
Author Contributions
E.J.: Conceptualization, Original draft preparation, Reviewing and editing, Final approval of the version to be submitted. M.B.A.: Conceptualization, Original draft preparation, Reviewing and editing, Final approval of the version to be submitted. S.C.: Conceptualization, Original draft preparation, Reviewing and editing, Final approval of the version to be submitted. P.M.: Conceptualization, Original draft preparation, Reviewing and editing, Final approval of the version to be submitted. All authors have read and agreed to the published version of the manuscript.
Funding
This review was sponsored by Ipsen Biopharm, UK. The sponsor was not involved in the development of the content, selection and interpretation of the included data, or overall conclusion of the review; the sponsor reviewed the article for scientific accuracy only.
Institutional Review Board Statement
No institutional review board approval needed for this literature review.
Informed Consent Statement
No informed consent needed for this literature review.
Data Availability Statement
Data are publicly available.
Acknowledgments
This review was sponsored by Ipsen, UK. The sponsor was not involved in the development of the content, selection and interpretation of the included data, or overall conclusion of the review; the sponsor reviewed the article for scientific accuracy only. The authors thank Isabelle Kaufmann, PhD, and Alison Chisholm, MPH, of Oxford PharmaGenesis UK for providing medical writing support and editorial support, which was sponsored by Ipsen UK, in accordance with Good Publication Practice guidelines.
Conflicts of Interest
E.J. reports personal fees from Eisai, Exelixis, Merck, NiKang, Novartis, and Pfizer, and grants and personal fees from Exelixis, Novartis, Merck, and Pfizer. M.B.A. reports personal fees and grants to his institution from Bristol-Myers Squibb, Merck, Pfizer, and Genentech, and personal fees from Agenus, Arrowhead Pharmaceuticals, Aveo Oncology, AstraZeneca, Calithera, Eisai, Exelixis, and Novartis and Advisory Board Service with Stock Options for Werewolf and Pyxis Oncology. S.C. reports advisory roles for Astellas Pharma, Bayer, Beigene, Clovis Oncology, Janssen-Cilag, and Pfizer; speakers’ bureau for Pfizer; personal fees from Clovis Oncology and Novartis and research funding from Clovis Oncology and Sanofi/Aventis. P.M. reports research funding and speakers’ fees from Janssen.
References
- Negrier, S.; Escudier, B.; Lasset, C.; Douillard, J.Y.; Savary, J.; Chevreau, C.; Ravaud, A.; Mercatello, A.; Peny, J.; Mousseau, M.; et al. Recombinant human interleukin-2, recombinant human interferon alfa-2a, or both in metastatic renal-cell carcinoma. Groupe Francais d’Immunotherapie. N. Engl. J. Med. 1998, 338, 1272–1278. [Google Scholar] [CrossRef] [PubMed]
- Li, L.; Kaelin, W.G., Jr. New insights into the biology of renal cell carcinoma. Hematol. Oncol. Clin. North. Am. 2011, 25, 667–686. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Sanchez-Gastaldo, A.; Kempf, E.; Gonzalez Del Alba, A.; Duran, I. Systemic treatment of renal cell cancer: A comprehensive review. Cancer Treat. Rev. 2017, 60, 77–89. [Google Scholar] [CrossRef] [PubMed]
- Niu, G.; Chen, X. Vascular endothelial growth factor as an anti-angiogenic target for cancer therapy. Curr. Drug Targets 2010, 11, 1000–1017. [Google Scholar] [CrossRef]
- Ross, K.; Jones, R.J. Immune checkpoint inhibitors in renal cell carcinoma. Clin. Sci. 2017, 131, 2627–2642. [Google Scholar] [CrossRef] [PubMed]
- Motzer, R.J.; Jonasch, E.; Michaelson, M.D.; Nandagopal, L.; Gore, J.L.; George, S.; Alva, A.; Haas, N.; Harrison, M.R.; Plimack, E.R.; et al. NCCN Guidelines Insights: Kidney Cancer, Version 2.2020. J. Natl. Compr. Canc. Netw. 2019, 17, 1278–1285. [Google Scholar] [CrossRef] [PubMed]
- Albiges, L.; Powles, T.; Staehler, M.; Bensalah, K.; Giles, R.H.; Hora, M.; Kuczyk, M.A.; Lam, T.B.; Ljungberg, B.; Marconi, L.; et al. Updated European Association of Urology Guidelines on Renal Cell Carcinoma: Immune Checkpoint Inhibition Is the New Backbone in First-line Treatment of Metastatic Clear-cell Renal Cell Carcinoma. Eur. Urol. 2019, 76, 151–156. [Google Scholar] [CrossRef] [PubMed]
- Escudier, B.; Porta, C.; Schmidinger, M.; Rioux-Leclercq, N.; Bex, A.; Khoo, V.; Grunwald, V.; Gillessen, S.; Horwich, A.; Committee, E.G. Renal cell carcinoma: ESMO Clinical Practice Guidelines for diagnosis, treatment and follow-updagger. Ann. Oncol. 2019, 30, 706–720. [Google Scholar] [CrossRef]
- George, S.; Rini, B.I.; Hammers, H.J. Emerging Role of Combination Immunotherapy in the First-line Treatment of Advanced Renal Cell Carcinoma: A Review. JAMA Oncol. 2018, 5, 411–421. [Google Scholar] [CrossRef]
- Khan, K.A.; Kerbel, R.S. Improving immunotherapy outcomes with anti-angiogenic treatments and vice versa. Nat. Rev. Clin. Oncol. 2018, 15, 310–324. [Google Scholar] [CrossRef]
- Whiteside, T.L. The tumor microenvironment and its role in promoting tumor growth. Oncogene 2008, 27, 5904–5912. [Google Scholar] [CrossRef] [PubMed]
- Binnewies, M.; Roberts, E.W.; Kersten, K.; Chan, V.; Fearon, D.F.; Merad, M.; Coussens, L.M.; Gabrilovich, D.I.; Ostrand-Rosenberg, S.; Hedrick, C.C.; et al. Understanding the tumor immune microenvironment (TIME) for effective therapy. Nat. Med. 2018, 24, 541–550. [Google Scholar] [CrossRef] [PubMed]
- Gajewski, T.F.; Schreiber, H.; Fu, Y.X. Innate and adaptive immune cells in the tumor microenvironment. Nat. Immunol. 2013, 14, 1014–1022. [Google Scholar] [CrossRef] [PubMed]
- Jonasch, E.; Walker, C.L.; Rathmell, W.K. Clear cell renal cell carcinoma ontogeny and mechanisms of lethality. Nat. Rev. Nephrol. 2021, 17, 245–261. [Google Scholar] [CrossRef]
- Network CGAR. Comprehensive molecular characterization of clear cell renal cell carcinoma. Nature 2013, 499, 43–49. [Google Scholar] [CrossRef]
- Choueiri, T.K.; Kaelin, W.G., Jr. Targeting the HIF2-VEGF axis in renal cell carcinoma. Nat. Med. 2020, 26, 1519–1530. [Google Scholar] [CrossRef]
- Keith, B.; Johnson, R.S.; Simon, M.C. HIF1alpha and HIF2alpha: Sibling rivalry in hypoxic tumour growth and progression. Nat. Rev. Cancer 2011, 12, 9–22. [Google Scholar] [CrossRef]
- Rankin, E.B.; Fuh, K.C.; Taylor, T.E.; Krieg, A.J.; Musser, M.; Yuan, J.; Wei, K.; Kuo, C.J.; Longacre, T.A.; Giaccia, A.J. AXL is an essential factor and therapeutic target for metastatic ovarian cancer. Cancer Res. 2010, 70, 7570–7579. [Google Scholar] [CrossRef]
- Zhou, L.; Liu, X.D.; Sun, M.; Zhang, X.; German, P.; Bai, S.; Ding, Z.; Tannir, N.; Wood, C.G.; Matin, S.F.; et al. Targeting MET and AXL overcomes resistance to sunitinib therapy in renal cell carcinoma. Oncogene 2016, 35, 2687–2697. [Google Scholar] [CrossRef]
- Synnestvedt, K.; Furuta, G.T.; Comerford, K.M.; Louis, N.; Karhausen, J.; Eltzschig, H.K.; Hansen, K.R.; Thompson, L.F.; Colgan, S.P. Ecto-5′-nucleotidase (CD73) regulation by hypoxia-inducible factor-1 mediates permeability changes in intestinal epithelia. J. Clin. Investig. 2002, 110, 993–1002. [Google Scholar] [CrossRef]
- Liu, Z.; Yan, S.; Wang, J.; Xu, Y.; Wang, Y.; Zhang, S.; Xu, X.; Yang, Q.; Zeng, X.; Zhou, Y.; et al. Endothelial adenosine A2a receptor-mediated glycolysis is essential for pathological retinal angiogenesis. Nat. Commun. 2017, 8, 584. [Google Scholar] [CrossRef] [PubMed]
- Fong, L.; Hotson, A.; Powderly, J.D.; Sznol, M.; Heist, R.S.; Choueiri, T.K.; George, S.; Hughes, B.G.M.; Hellmann, M.D.; Shepard, D.R.; et al. Adenosine 2A Receptor Blockade as an Immunotherapy for Treatment-Refractory Renal Cell Cancer. Cancer Discov. 2020, 10, 40–53. [Google Scholar] [CrossRef] [PubMed]
- Varela, I.; Tarpey, P.; Raine, K.; Huang, D.; Ong, C.K.; Stephens, P.; Davies, H.; Jones, D.; Lin, M.L.; Teague, J.; et al. Exome sequencing identifies frequent mutation of the SWI/SNF complex gene PBRM1 in renal carcinoma. Nature 2011, 469, 539–542. [Google Scholar] [CrossRef]
- Dalgliesh, G.L.; Furge, K.; Greenman, C.; Chen, L.; Bignell, G.; Butler, A.; Davies, H.; Edkins, S.; Hardy, C.; Latimer, C.; et al. Systematic sequencing of renal carcinoma reveals inactivation of histone modifying genes. Nature 2010, 463, 360–363. [Google Scholar] [CrossRef] [PubMed]
- Pena-Llopis, S.; Vega-Rubin-de-Celis, S.; Liao, A.; Leng, N.; Pavia-Jimenez, A.; Wang, S.; Yamasaki, T.; Zhrebker, L.; Sivanand, S.; Spence, P.; et al. BAP1 loss defines a new class of renal cell carcinoma. Nat. Genet. 2012, 44, 751–759. [Google Scholar] [CrossRef]
- Gao, W.; Li, W.; Xiao, T.; Liu, X.S.; Kaelin, W.G., Jr. Inactivation of the PBRM1 tumor suppressor gene amplifies the HIF-response in VHL-/- clear cell renal carcinoma. Proc. Natl. Acad. Sci. USA 2017, 114, 1027–1032. [Google Scholar] [CrossRef]
- Liu, X.D.; Kong, W.; Peterson, C.B.; McGrail, D.J.; Hoang, A.; Zhang, X.; Lam, T.; Pilie, P.G.; Zhu, H.; Beckermann, K.E.; et al. PBRM1 loss defines a nonimmunogenic tumor phenotype associated with checkpoint inhibitor resistance in renal carcinoma. Nat. Commun. 2020, 11, 2135. [Google Scholar] [CrossRef]
- Brugarolas, J.B.; Vazquez, F.; Reddy, A.; Sellers, W.R.; Kaelin, W.G., Jr. TSC2 regulates VEGF through mTOR-dependent and -independent pathways. Cancer Cell 2003, 4, 147–158. [Google Scholar] [CrossRef]
- Yang, J.; Yan, J.; Liu, B. Targeting VEGF/VEGFR to Modulate Antitumor Immunity. Front Immunol 2018, 9, 978. [Google Scholar] [CrossRef]
- Almand, B.; Resser, J.R.; Lindman, B.; Nadaf, S.; Clark, J.I.; Kwon, E.D.; Carbone, D.P.; Gabrilovich, D.I. Clinical significance of defective dendritic cell differentiation in cancer. Clin. Cancer Res. 2000, 6, 1755–1766. [Google Scholar]
- Oussa, N.A.; Dahmani, A.; Gomis, M.; Richaud, M.; Andreev, E.; Navab-Daneshmand, A.R.; Taillefer, J.; Carli, C.; Boulet, S.; Sabbagh, L.; et al. VEGF Requires the Receptor NRP-1 To Inhibit Lipopolysaccharide-Dependent Dendritic Cell Maturation. J. Immunol. 2016, 197, 3927–3935. [Google Scholar] [CrossRef] [PubMed]
- Voron, T.; Colussi, O.; Marcheteau, E.; Pernot, S.; Nizard, M.; Pointet, A.L.; Latreche, S.; Bergaya, S.; Benhamouda, N.; Tanchot, C.; et al. VEGF-A modulates expression of inhibitory checkpoints on CD8+ T cells in tumors. J. Exp. Med. 2015, 212, 139–148. [Google Scholar] [CrossRef]
- Facciabene, A.; Peng, X.; Hagemann, I.S.; Balint, K.; Barchetti, A.; Wang, L.P.; Gimotty, P.A.; Gilks, C.B.; Lal, P.; Zhang, L.; et al. Tumour hypoxia promotes tolerance and angiogenesis via CCL28 and T(reg) cells. Nature 2011, 475, 226–230. [Google Scholar] [CrossRef] [PubMed]
- Garcia-Diaz, A.; Shin, D.S.; Moreno, B.H.; Saco, J.; Escuin-Ordinas, H.; Rodriguez, G.A.; Zaretsky, J.M.; Sun, L.; Hugo, W.; Wang, X.; et al. Interferon Receptor Signaling Pathways Regulating PD-L1 and PD-L2 Expression. Cell Rep. 2017, 19, 1189–1201. [Google Scholar] [CrossRef]
- Leite, K.R.; Reis, S.T.; Junior, J.P.; Zerati, M.; Gomes Dde, O.; Camara-Lopes, L.H.; Srougi, M. PD-L1 expression in renal cell carcinoma clear cell type is related to unfavorable prognosis. Diagn. Pathol. 2015, 10, 189. [Google Scholar] [CrossRef] [PubMed]
- Motzer, R.J.; Tannir, N.M.; McDermott, D.F.; Aren Frontera, O.; Melichar, B.; Choueiri, T.K.; Plimack, E.R.; Barthelemy, P.; Porta, C.; George, S.; et al. Nivolumab plus Ipilimumab versus Sunitinib in Advanced Renal-Cell Carcinoma. N. Engl. J. Med. 2018, 378, 1277–1290. [Google Scholar] [CrossRef] [PubMed]
- Iacovelli, R.; Nole, F.; Verri, E.; Renne, G.; Paglino, C.; Santoni, M.; Cossu Rocca, M.; Giglione, P.; Aurilio, G.; Cullura, D.; et al. Prognostic Role of PD-L1 Expression in Renal Cell Carcinoma. A Systematic Review and Meta-Analysis. Target. Oncol. 2016, 11, 143–148. [Google Scholar] [CrossRef]
- Braun, D.A.; Hou, Y.; Bakouny, Z.; Ficial, M.; Sant’Angelo, M.; Forman, J.; Choueiri, T.K. Interplay of somatic alterations and immune infiltration modulates response to PD-1 blockade in advanced clear cell renal cell carcinoma. Nat. Med. 2020, 26, 909–918. [Google Scholar] [CrossRef]
- Clark, D.J.; Dhanasekaran, S.M.; Petralia, F.; Pan, J.; Song, X.; Hu, Y.; da Veiga Leprevost, F.; Reva, B.; Lih, T.M.; Chang, H.Y.; et al. Integrated Proteogenomic Characterization of Clear Cell Renal Cell Carcinoma. Cell 2019, 179, 964–983.e31. [Google Scholar] [CrossRef]
- Ohta, A.; Gorelik, E.; Prasad, S.J.; Ronchese, F.; Lukashev, D.; Wong, M.K.; Huang, X.; Caldwell, S.; Liu, K.; Smith, P.; et al. A2A adenosine receptor protects tumors from antitumor T cells. Proc. Natl. Acad. Sci. USA 2006, 103, 13132–13137. [Google Scholar] [CrossRef]
- Young, A.; Ngiow, S.F.; Gao, Y.; Patch, A.M.; Barkauskas, D.S.; Messaoudene, M.; Lin, G.; Coudert, J.D.; Stannard, K.A.; Zitvogel, L.; et al. A2AR Adenosine Signaling Suppresses Natural Killer Cell Maturation in the Tumor Microenvironment. Cancer Res. 2018, 78, 1003–1016. [Google Scholar] [CrossRef] [PubMed]
- Cekic, C.; Linden, J. Adenosine A2A receptors intrinsically regulate CD8+ T cells in the tumor microenvironment. Cancer Res. 2014, 74, 7239–7249. [Google Scholar] [CrossRef] [PubMed]
- Sitkovsky, M.V. T regulatory cells: Hypoxia-adenosinergic suppression and re-direction of the immune response. Trends Immunol. 2009, 30, 102–108. [Google Scholar] [CrossRef] [PubMed]
- Hornyak, L.; Dobos, N.; Koncz, G.; Karanyi, Z.; Pall, D.; Szabo, Z.; Halmos, G.; Szekvolgyi, L. The Role of Indoleamine-2,3-Dioxygenase in Cancer Development, Diagnostics, and Therapy. Front. Immunol. 2018, 9, 151. [Google Scholar] [CrossRef]
- Munn, D.H.; Zhou, M.; Attwood, J.T.; Bondarev, I.; Conway, S.J.; Marshall, B.; Brown, C.; Mellor, A.L. Prevention of allogeneic fetal rejection by tryptophan catabolism. Science 1998, 281, 1191–1193. [Google Scholar] [CrossRef]
- Prendergast, G.C.; Malachowski, W.J.; Mondal, A.; Scherle, P.; Muller, A.J. Indoleamine 2,3-Dioxygenase and Its Therapeutic Inhibition in Cancer. Int. Rev. Cell Mol. Biol. 2018, 336, 175–203. [Google Scholar] [CrossRef]
- Riesenberg, R.; Weiler, C.; Spring, O.; Eder, M.; Buchner, A.; Popp, T.; Castro, M.; Kammerer, R.; Takikawa, O.; Hatz, R.A.; et al. Expression of indoleamine 2,3-dioxygenase in tumor endothelial cells correlates with long-term survival of patients with renal cell carcinoma. Clin. Cancer Res. 2007, 13, 6993–7002. [Google Scholar] [CrossRef]
- Rini, B.I.; Atkins, M.B. Resistance to targeted therapy in renal-cell carcinoma. Lancet Oncol. 2009, 10, 992–1000. [Google Scholar] [CrossRef]
- Eichten, A.; Adler, A.P.; Cooper, B.; Griffith, J.; Wei, Y.; Yancopoulos, G.D.; Lin, H.C.; Thurston, G. Rapid decrease in tumor perfusion following VEGF blockade predicts long-term tumor growth inhibition in preclinical tumor models. Angiogenesis 2013, 16, 429–441. [Google Scholar] [CrossRef][Green Version]
- Liu, X.D.; Hoang, A.; Zhou, L.; Kalra, S.; Yetil, A.; Sun, M.; Ding, Z.; Zhang, X.; Bai, S.; German, P.; et al. Resistance to Antiangiogenic Therapy Is Associated with an Immunosuppressive Tumor Microenvironment in Metastatic Renal Cell Carcinoma. Cancer Immunol. Res. 2015, 3, 1017–1029. [Google Scholar] [CrossRef]
- Griffioen, A.W.; Mans, L.A.; de Graaf, A.M.A.; Nowak-Sliwinska, P.; de Hoog, C.; de Jong, T.A.M.; Vyth-Dreese, F.A.; van Beijnum, J.R.; Bex, A.; Jonasch, E. Rapid angiogenesis onset after discontinuation of sunitinib treatment of renal cell carcinoma patients. Clin. Cancer Res. 2012, 18, 3961–3971. [Google Scholar] [CrossRef] [PubMed]
- Lanitis, E.; Irving, M.; Coukos, G. Targeting the tumor vasculature to enhance T cell activity. Curr. Opin. Immunol. 2015, 33, 55–63. [Google Scholar] [CrossRef] [PubMed]
- Lai, Y.; Zhao, Z.; Zeng, T.; Liang, X.; Chen, D.; Duan, X.; Zeng, G.; Wu, W. Crosstalk between VEGFR and other receptor tyrosine kinases for TKI therapy of metastatic renal cell carcinoma. Cancer Cell Int. 2018, 18, 31. [Google Scholar] [CrossRef] [PubMed]
- Hara, T.; Miyake, H.; Hinata, N.; Fujisawa, M. Inhibition of Tumor Growth and Sensitization to Sunitinib by RNA Interference Targeting Programmed Death-ligand 1 in Mouse Renal Cell Carcinoma RenCa Model. Anticancer. Res. 2019, 39, 4737–4742. [Google Scholar] [CrossRef]
- Guislain, A.; Gadiot, J.; Kaiser, A.; Jordanova, E.S.; Broeks, A.; Sanders, J.; van Boven, H.; de Gruijl, T.D.; Haanen, J.B.; Bex, A.; et al. Sunitinib pretreatment improves tumor-infiltrating lymphocyte expansion by reduction in intratumoral content of myeloid-derived suppressor cells in human renal cell carcinoma. Cancer Immunol. Immunother. 2015, 64, 1241–1250. [Google Scholar] [CrossRef]
- Kwilas, A.R.; Ardiani, A.; Donahue, R.N.; Aftab, D.T.; Hodge, J.W. Dual effects of a targeted small-molecule inhibitor (cabozantinib) on immune-mediated killing of tumor cells and immune tumor microenvironment permissiveness when combined with a cancer vaccine. J. Transl. Med. 2014, 12, 294. [Google Scholar] [CrossRef]
- Wallin, J.J.; Bendell, J.C.; Funke, R.; Sznol, M.; Korski, K.; Jones, S.; Hernandez, G.; Mier, J.; He, X.; Hodi, F.S.; et al. Atezolizumab in combination with bevacizumab enhances antigen-specific T-cell migration in metastatic renal cell carcinoma. Nat. Commun. 2016, 7, 12624. [Google Scholar] [CrossRef]
- Li, Y.L.; Zhao, H.; Ren, X.B. Relationship of VEGF/VEGFR with immune and cancer cells: Staggering or forward? Cancer Biol. Med. 2016, 13, 206–214. [Google Scholar] [CrossRef]
- Alfaro, C.; Suarez, N.; Gonzalez, A.; Solano, S.; Erro, L.; Dubrot, J.; Palazon, A.; Hervas-Stubbs, S.; Gurpide, A.; Lopez-Picazo, J.M.; et al. Influence of bevacizumab, sunitinib and sorafenib as single agents or in combination on the inhibitory effects of VEGF on human dendritic cell differentiation from monocytes. Br. J. Cancer 2009, 100, 1111–1119. [Google Scholar] [CrossRef]
- Kusmartsev, S.; Eruslanov, E.; Kubler, H.; Tseng, T.; Sakai, Y.; Su, Z.; Kaliberov, S.; Heiser, A.; Rosser, C.; Dahm, P.; et al. Oxidative stress regulates expression of VEGFR1 in myeloid cells: Link to tumor-induced immune suppression in renal cell carcinoma. J. Immunol. 2008, 181, 346–353. [Google Scholar] [CrossRef]
- Zhang, Q.; Tian, K.; Xu, J.; Zhang, H.; Li, L.; Fu, Q.; Chai, D.; Li, H.; Zheng, J. Synergistic Effects of Cabozantinib and EGFR-Specific CAR-NK-92 Cells in Renal Cell Carcinoma. J. Immunol. Res. 2017, 2017, 6915912. [Google Scholar] [CrossRef] [PubMed]
- Li, H.; Ding, J.; Lu, M.; Liu, H.; Miao, Y.; Li, L.; Wang, G.; Zheng, J.; Pei, D.; Zhang, Q. CAIX-specific CAR-T Cells and Sunitinib Show Synergistic Effects Against Metastatic Renal Cancer Models. J. Immunother. 2019, 43, 16–28. [Google Scholar] [CrossRef] [PubMed]
- Adotevi, O.; Pere, H.; Ravel, P.; Haicheur, N.; Badoual, C.; Merillon, N.; Medioni, J.; Peyrard, S.; Roncelin, S.; Verkarre, V.; et al. A decrease of regulatory T cells correlates with overall survival after sunitinib-based antiangiogenic therapy in metastatic renal cancer patients. J. Immunother. 2010, 33, 991–998. [Google Scholar] [CrossRef] [PubMed]
- Ko, J.S.; Zea, A.H.; Rini, B.I.; Ireland, J.L.; Elson, P.; Cohen, P.; Golshayan, A.; Rayman, P.A.; Wood, L.; Garcia, J.; et al. Sunitinib mediates reversal of myeloid-derived suppressor cell accumulation in renal cell carcinoma patients. Clin. Cancer Res. 2009, 15, 2148–2157. [Google Scholar] [CrossRef]
- van Cruijsen, H.; van der Veldt, A.A.; Vroling, L.; Oosterhoff, D.; Broxterman, H.J.; Scheper, R.J.; Giaccone, G.; Haanen, J.B.; van den Eertwegh, A.J.; Boven, E.; et al. Sunitinib-induced myeloid lineage redistribution in renal cell cancer patients: CD1c+ dendritic cell frequency predicts progression-free survival. Clin. Cancer Res. 2008, 14, 5884–5892. [Google Scholar] [CrossRef]
- Yuan, H.; Cai, P.; Li, Q.; Wang, W.; Sun, Y.; Xu, Q.; Gu, Y. Axitinib augments antitumor activity in renal cell carcinoma via STAT3-dependent reversal of myeloid-derived suppressor cell accumulation. Biomed. Pharmacother. 2014, 68, 751–756. [Google Scholar] [CrossRef]
- Ozao-Choy, J.; Ma, G.; Kao, J.; Wang, G.X.; Meseck, M.; Sung, M.; Schwartz, M.; Divino, C.M.; Pan, P.Y.; Chen, S.H. The novel role of tyrosine kinase inhibitor in the reversal of immune suppression and modulation of tumor microenvironment for immune-based cancer therapies. Cancer Res. 2009, 69, 2514–2522. [Google Scholar] [CrossRef]
- Rothlin, C.V.; Carrera-Silva, E.A.; Bosurgi, L.; Ghosh, S. TAM receptor signaling in immune homeostasis. Annu. Rev. Immunol. 2015, 33, 355–391. [Google Scholar] [CrossRef]
- Kwilas, A.R.; Donahue, R.N.; Tsang, K.Y.; Hodge, J.W. Immune consequences of tyrosine kinase inhibitors that synergize with cancer immunotherapy. Cancer Cell Microenviron. 2015, 2, e677. [Google Scholar] [CrossRef]
- Balan, M.; Mier y Teran, E.; Waaga-Gasser, A.M.; Gasser, M.; Choueiri, T.K.; Freeman, G.; Pal, S. Novel roles of c-Met in the survival of renal cancer cells through the regulation of HO-1 and PD-L1 expression. J. Biol. Chem. 2015, 290, 8110–8120. [Google Scholar] [CrossRef]
- Flaifel, A.; Xie, W.; Braun, D.A.; Ficial, M.; Bakouny, Z.; Nassar, A.H.; Jennings, R.B.; Escudier, B.; George, D.J.; Motzer, R.J.; et al. PD-L1 Expression and Clinical Outcomes to Cabozantinib, Everolimus, and Sunitinib in Patients with Metastatic Renal Cell Carcinoma: Analysis of the Randomized Clinical Trials METEOR and CABOSUN. Clin. Cancer Res. 2019, 25, 6080–6088. [Google Scholar] [CrossRef] [PubMed]
- Garcia, J.A.; Mekhail, T.; Elson, P.; Triozzi, P.; Nemec, C.; Dreicer, R.; Rini, B.I. Clinical and immunomodulatory effects of bevacizumab and low-dose interleukin-2 in patients with metastatic renal cell carcinoma: Results from a phase II trial. BJU Int. 2011, 107, 562–570. [Google Scholar] [CrossRef] [PubMed]
- Panka, D.J.; Liu, Q.; Geissler, A.K.; Mier, J.W. Effects of HDM2 antagonism on sunitinib resistance, p53 activation, SDF-1 induction, and tumor infiltration by CD11b+/Gr-1+ myeloid derived suppressor cells. Mol. Cancer 2013, 12, 17. [Google Scholar] [CrossRef] [PubMed]
- Hipp, M.M.; Hilf, N.; Walter, S.; Werth, D.; Brauer, K.M.; Radsak, M.P.; Weinschenk, T.; Singh-Jasuja, H.; Brossart, P. Sorafenib, but not sunitinib, affects function of dendritic cells and induction of primary immune responses. Blood 2008, 111, 5610–5620. [Google Scholar] [CrossRef]
- Finke, J.; Ko, J.; Rini, B.; Rayman, P.; Ireland, J.; Cohen, P. MDSC as a mechanism of tumor escape from sunitinib mediated anti-angiogenic therapy. Int. Immunopharmacol. 2011, 11, 856–861. [Google Scholar] [CrossRef]
- Amin, A.; Plimack, E.R.; Ernstoff, M.S.; Lewis, L.D.; Bauer, T.M.; McDermott, D.F.; Carducci, M.; Kollmannsberger, C.; Rini, B.I.; Heng, D.Y.C.; et al. Safety and efficacy of nivolumab in combination with sunitinib or pazopanib in advanced or metastatic renal cell carcinoma: The CheckMate 016 study. J. Immunother. Cancer 2018, 6, 109. [Google Scholar] [CrossRef]
- Chowdhury. A phase I/II study to assess the safety and efficacy of pazopanib and pembrolizumab in patients with advanced renal cell carcinoma (abstract 4506). In Proceedings of the American Society of Clinical Oncology meeting (ASCO), Chicago, IL, USA, 2–6 June 2017. [Google Scholar]
- Rini, B.I.; Stein, M.; Shannon, P.; Eddy, S.; Tyler, A.; Stephenson, J.J., Jr.; Catlett, L.; Huang, B.; Healey, D.; Gordon, M. Phase 1 dose-escalation trial of tremelimumab plus sunitinib in patients with metastatic renal cell carcinoma. Cancer 2011, 117, 758–767. [Google Scholar] [CrossRef]
- Rini, B.I.; Powles, T.; Atkins, M.B.; Escudier, B.; McDermott, D.F.; Suarez, C.; Bracarda, S.; Stadler, W.M.; Donskov, F.; Lee, J.L.; et al. Atezolizumab plus bevacizumab versus sunitinib in patients with previously untreated metastatic renal cell carcinoma (IMmotion151): A multicentre, open-label, phase 3, randomised controlled trial. Lancet 2019, 393, 2404–2415. [Google Scholar] [CrossRef]
- Rini, B.I.; Plimack, E.R.; Stus, V.; Gafanov, R.; Hawkins, R.; Nosov, D.; Pouliot, F.; Alekseev, B.; Soulieres, D.; Melichar, B.; et al. Pembrolizumab plus Axitinib versus Sunitinib for Advanced Renal-Cell Carcinoma. N. Engl. J. Med. 2019, 380, 1116–1127. [Google Scholar] [CrossRef]
- Rini, B.I.; Plimack, E.R.; Stus, V.; Waddell, T.; Gafanov, R.; Pouliot, F.; Nosov, D.; Melichar, B.; Soulieres, D.; Borchiellini, D.; et al. Pembrolizumab (pembro) plus axitinib (axi) versus sunitinib as first-line therapy for advanced clear cell renal cell carcinoma (ccRCC): Results from 42-month follow-up of KEYNOTE-426. J. Clin. Oncol. 2021, 39, 4500. [Google Scholar] [CrossRef]
- Plimack, E.R.; Rini, B.I.; Stus, V.; Gafanov, R.; Waddell, T.; Nosov, D.; Pouliot, F.; Soulieres, D.; Melichar, B.; Vynnychenko, I.; et al. Pembrolizumab plus axitinib versus sunitinib as first-line therapy for advanced renal cell carcinoma (RCC): Updated analysis of KEYNOTE-426. J. Clin. Oncol. 2020, 38, 5001. [Google Scholar] [CrossRef]
- Motzer, R.J.; Penkov, K.; Haanen, J.; Rini, B.; Albiges, L.; Campbell, M.T.; Venugopal, B.; Kollmannsberger, C.; Negrier, S.; Uemura, M.; et al. Avelumab plus Axitinib versus Sunitinib for Advanced Renal-Cell Carcinoma. N. Engl. J. Med. 2019, 380, 1103–1115. [Google Scholar] [CrossRef] [PubMed]
- Choueiri, T.K.; Motzer, R.J.; Rini, B.I.; Haanen, J.; Campbell, M.T.; Venugopal, B.; Kollmannsberger, C.; Gravis-Mescam, G.; Uemura, M.; Lee, J.L.; et al. Updated efficacy results from the JAVELIN Renal 101 trial: First-line avelumab plus axitinib versus sunitinib in patients with advanced renal cell carcinoma. Ann. Oncol. 2020, 31, 1030–1039. [Google Scholar] [CrossRef]
- Choueiri, T.K.; Powles, T.; Burotto, M.; Escudier, B.; Bourlon, M.T.; Zurawski, B.; Oyervides Juarez, V.M.; Hsieh, J.J.; Basso, U.; Shah, A.Y.; et al. Nivolumab plus Cabozantinib versus Sunitinib for Advanced Renal-Cell Carcinoma. N. Engl. J. Med. 2021, 384, 829–841. [Google Scholar] [CrossRef]
- Apolo, A.B.; Nadal, R.; Girardi, D.M.; Niglio, S.A.; Ley, L.; Cordes, L.M.; Steinberg, S.M.; Sierra Ortiz, O.; Cadena, J.; Diaz, C.; et al. Phase I Study of Cabozantinib and Nivolumab Alone or With Ipilimumab for Advanced or Metastatic Urothelial Carcinoma and Other Genitourinary Tumors. J. Clin. Oncol. 2020, 38, 3672–3684. [Google Scholar] [CrossRef] [PubMed]
- Lee, C.-H.; Shah, A.Y.; Hsieh, J.J.; Rao, A.; Pinto, A.; Bilen, M.A. Phase II trial of lenvatinib (LEN) plus pembrolizumab (PEMBRO) for disease progression after PD-1/PD-L1 immune checkpoint inhibitor (ICI) in metastatic clear cell renal cell carcinoma (mccRCC). J. Clin. Oncol. 2020, 38, abstr5008. [Google Scholar] [CrossRef]
- Motzer, R.; Alekseev, B.; Rha, S.Y.; Porta, C.; Eto, M.; Powles, T.; Grunwald, V.; Hutson, T.E.; Kopyltsov, E.; Mendez-Vidal, M.J.; et al. Lenvatinib plus Pembrolizumab or Everolimus for Advanced Renal Cell Carcinoma. N. Engl. J. Med. 2021, 384, 1289–1300. [Google Scholar] [CrossRef]
- Nadal, R.M.; Mortazavi, A.; Stein, M.; Pal, S.K.; Davarpanah, N.N.; Parnes, H.L.; Apolo, A.B. Results of phase I plus expansion cohorts of cabozantinib (Cabo) plus nivolumab (Nivo) and CaboNivo plus ipilimumab (Ipi) in patients (pts) with with metastatic urothelial carcinoma (mUC) and other genitourinary (GU) malignancies. (abstract 515). In Proceedings of the ASCO Genitourinary Cancers Symposium, San Francisco, CA, USA, 8–10 February 2018. [Google Scholar]
- Agarwal, N.; Vaishampayan, U.; Green, M.; di Nucci, F.; Chang, P.Y.; Scheffold, C.; Pal, S. Phase Ib study (COSMIC-021) of cabozantinib in combination with atezolizumab: Results of the dose escalation stage in patients (pts) with treatment-naïve advanced renal cell carcinoma (RCC). Ann. Oncol. 2018, 29, viii308. [Google Scholar] [CrossRef]
- Keeler, M.E.; Kessler, E.R.; Bernard, B.; Weisdack, S.; Breaker, K.M.; Wold, M.; Ertz, D.; Weitzenkamp, D.; Flaig, T.W.; Lam, E.T. Pembrolizumab (pembro) and cabozantinib (cabo) in patients (pts) with metastatic renal cell carcinoma (mRCC): Phase I results. In Proceedings of the ASCO Genitourinary Cancers Symposium, San Francisco, CA, USA, 14 February 2019. [Google Scholar]
- Escudier, B.; Barthelemy, P.; Ravaud, A.; Negrier, S.; Needle, M.N.; Albiges, L. Tivozanib combined with nivolumab: Phase Ib/II study in metastatic renal cell carcinoma (mRCC) (abstract 618). In Proceedings of the ASCO, Annual Meeting, Chicago, IL, USA, 1–5 June 2018; p. 618. [Google Scholar]
- Lee, C.H.; Makker, V.; Rasco, D.W.; Taylor, M.H.; Stepan, D.E.; Shumaker, R.C.; Schmidt, E.V.; Guo, M.; Dutcus, C.E.; Motzer, R.J. Lenvatinib + pembrolizumab in patients with renal cell carcinoma: Updated results. In Proceedings of the ASCO, Annual Meeting, Chicago, IL, USA, 1–5 June 2018. [Google Scholar]
- Makker, V.; Rasco, D.; Vogelzang, N.J.; Brose, M.S.; Cohn, A.L.; Mier, J.; Di Simone, C.; Hyman, D.M.; Stepan, D.E.; Dutcus, C.E.; et al. Lenvatinib plus pembrolizumab in patients with advanced endometrial cancer: An interim analysis of a multicentre, open-label, single-arm, phase 2 trial. Lancet Oncol. 2019, 20, 711–718. [Google Scholar] [CrossRef]
- Grünwald, V.; Voss, M.H.; Rini, B.I.; Powles, T.; Albiges, L.; Giles, R.H.; Jonasch, E. Axitinib plus immune checkpoint inhibitor: Evidence- and expert-based consensus recommendation for treatment optimisation and management of related adverse events. Br. J. Cancer 2020, 123, 898–904. [Google Scholar] [CrossRef]
- Farkona, S.; Diamandis, E.P.; Blasutig, I.M. Cancer immunotherapy: The beginning of the end of cancer? BMC Med. 2016, 14, 73. [Google Scholar] [CrossRef] [PubMed]
- Vanneman, M.; Dranoff, G. Combining immunotherapy and targeted therapies in cancer treatment. Nat. Rev. Cancer 2012, 12, 237–251. [Google Scholar] [CrossRef] [PubMed]
- Cappelli, L.C.; Gutierrez, A.K.; Baer, A.N.; Albayda, J.; Manno, R.L.; Haque, U.; Lipson, E.J.; Bleich, K.B.; Shah, A.A.; Naidoo, J.; et al. Inflammatory arthritis and sicca syndrome induced by nivolumab and ipilimumab. Ann. Rheum. Dis. 2017, 76, 43–50. [Google Scholar] [CrossRef] [PubMed]
- Motzer, R.J.; Escudier, B.; McDermott, D.F.; George, S.; Hammers, H.J.; Srinivas, S.; Tykodi, S.S.; Sosman, J.A.; Procopio, G.; Plimack, E.R.; et al. Nivolumab versus Everolimus in Advanced Renal-Cell Carcinoma. N. Engl. J. Med. 2015, 373, 1803–1813. [Google Scholar] [CrossRef]
- Regan, M.M.; Werner, L.; Rao, S.; Gupte-Singh, K.; Hodi, F.S.; Kirkwood, J.M.; Kluger, H.M.; Larkin, J.; Postow, M.A.; Ritchings, C.; et al. Treatment-Free Survival: A Novel Outcome Measure of the Effects of Immune Checkpoint Inhibition—A Pooled Analysis of Patients With Advanced Melanoma. J. Clin. Oncol. 2019, 37, 3350–3358. [Google Scholar] [CrossRef]
- Lopez-Beltran, A.; Henriques, V.; Cimadamore, A.; Santoni, M.; Cheng, L.; Gevaert, T.; Blanca, A.; Massari, F.; Scarpelli, M.; Montironi, R. The Identification of Immunological Biomarkers in Kidney Cancers. Front. Oncol. 2018, 8, 456. [Google Scholar] [CrossRef]
- McDermott, D.F.; Huseni, M.A.; Atkins, M.B.; Motzer, R.J.; Rini, B.I.; Escudier, B.; Fong, L.; Joseph, R.W.; Pal, S.K.; Reeves, J.A.; et al. Clinical activity and molecular correlates of response to atezolizumab alone or in combination with bevacizumab versus sunitinib in renal cell carcinoma. Nat. Med. 2018, 24, 749–757. [Google Scholar] [CrossRef]
- Hakimi, A.A.; Voss, M.H.; Kuo, F.; Sanchez, A.; Liu, M.; Nixon, B.G.; Vuong, L.; Ostrovnaya, I.; Chen, Y.B.; Reuter, V.; et al. Transcriptomic Profiling of the Tumor Microenvironment Reveals Distinct Subgroups of Clear cell Renal Cell Cancer-Data from a Randomized Phase III Trial. Cancer Discov. 2019, 9, 510–525. [Google Scholar] [CrossRef]
- Motzer, R.J.; Banchereau, R.; Hamidi, H.; Powles, T.; McDermott, D.; Atkins, M.B.; Escudier, B.; Liu, L.F.; Leng, N.; Abbas, A.R.; et al. Molecular Subsets in Renal Cancer Determine Outcome to Checkpoint and Angiogenesis Blockade. Cancer Cell 2020, 38, 803–817. [Google Scholar] [CrossRef]
- Chevrier, S.; Levine, J.H.; Zanotelli, V.R.T.; Silina, K.; Schulz, D.; Bacac, M.; Ries, C.H.; Ailles, L.; Jewett, M.A.S.; Moch, H.; et al. An Immune Atlas of Clear Cell Renal Cell Carcinoma. Cell 2017, 169, 736–749.e18. [Google Scholar] [CrossRef]
- Miao, D.; Margolis, C.A.; Gao, W.; Voss, M.H.; Li, W.; Martini, D.J.; Van Allen, E.M. Genomic correlates of response to immune checkpoint therapies in clear cell renal cell carcinoma. Science 2018, 359, 801–806. [Google Scholar] [CrossRef] [PubMed]
- Braun, D.A.; Ishii, Y.; Walsh, A.M. Clinical Validation of PBRM1 Alterations as a Marker of Immune Checkpoint Inhibitor Response in Renal Cell Carcinoma. JAMA Oncol. 2019, 5, 1631–1633. [Google Scholar] [CrossRef] [PubMed]
- Rini, B.I.; Motzer, R.J.; Powles, T. Atezolizumab (atezo) + bevacizumab (bev) versus sunitinib (sun) in pts with untreated metastatic renal cell carcinoma (mRCC) and sarcomatoid (sarc) histology: IMmotion151 subgroup analysis. J. Clin. Oncol. 2019, 37 (Suppl. S15), 4512. [Google Scholar] [CrossRef]
- Rini, B.I.; Plimack, E.R.; Stus, V. Pembrolizumab (pembro) plus axitinib (axi) versus sunitinib as first-line therapy for metastatic renal cell carcinoma (mRCC): Outcomes in the combined IMDC intermediate/poor risk and sarcomatoid subgroups of the phase 3 KEYNOTE-426 study. J. Clin. Oncol. 2019, 37 (Suppl. S15), 4500. [Google Scholar] [CrossRef]
- Choueiri, T.K.; Larkin, J.M.G.; Pal, S.K.; Motzer, R.J.; Venugopal, B.; Alekseev, B.Y.; Albiges, L. Efficacy and biomarker analysis of patients (pts) with advanced renal cell carcinoma (aRCC) with sarcomatoid histology (sRCC): Subgroup analysis from the phase III JAVELIN renal 101 trial of first-line avelumab plus axitinib (A 1 Ax) vs. sunitinib (S). Ann. Oncol. 2019, 30 (Suppl. S5), v361. [Google Scholar] [CrossRef]
- Uemura, M.; Tomita, Y.; Miyake, H. Avelumab plus axitinib vs. sunitinib for advanced renal cell carcinoma: Japanese subgroup analysis from JAVELIN Renal 101. Cancer Sci. 2020, 111, 907–923. [Google Scholar] [CrossRef]
- Choueiri, T.K.; Larkin, J.; Oya, M.; Thistlethwaite, F.; Martignoni, M.; Nathan, P.; Powles, T.; McDermott, D.; Robbins, P.B.; Chism, D.D.; et al. Preliminary results for avelumab plus axitinib as first-line therapy in patients with advanced clear-cell renal-cell carcinoma (JAVELIN Renal 100): An open-label, dose-finding and dose-expansion, phase 1b trial. Lancet Oncol. 2018, 19, 451–460. [Google Scholar] [CrossRef]
- Rini, B.I.; Atkins, M.B.; Choueiri, T.K.; Thomaidou, D.; Rosbrook, B.; Thakur, M.; Hutson, T.E. Time to Resolution of Axitinib-Related Adverse Events After Treatment Interruption in Patients With Advanced Renal Cell Carcinoma. Clin. Genitourin Cancer 2021, 19, e306–e312. [Google Scholar] [CrossRef]
- Motzer, R.J.; Robbins, P.B.; Powles, T. Avelumab plus axitinib versus sunitinib in advanced renal cell carcinoma: Biomarker analysis of the phase 3 JAVELIN Renal 101 trial. Nat. Med. 2020, 26, 1733–1741. [Google Scholar] [CrossRef]
- Bex, A.; van Thienen, J.V.; Schrier, M.; Graafland, N.; Kuusk, T.; Hendricksen, K.; Lagerveld, B.; Zondervan, P.; van Moorselaar, J.A.; Blank, C.; et al. A Phase II, single-arm trial of neoadjuvant axitinib plus avelumab in patients with localized renal cell carcinoma who are at high risk of relapse after nephrectomy (NEOAVAX). Future Oncol. 2019, 15, 2203–2209. [Google Scholar] [CrossRef]
- Atkins, M.B.; Plimack, E.R.; Puzanov, I.; Fishman, M.N.; McDermott, D.F.; Cho, D.C.; Vaishampayan, U.; George, S.; Olencki, T.E.; Tarazi, J.C.; et al. Axitinib in combination with pembrolizumab in patients with advanced renal cell cancer: A non-randomised, open-label, dose-finding, and dose-expansion phase 1b trial. Lancet Oncol. 2018, 19, 405–415. [Google Scholar] [CrossRef]
- Powles, T.; Plimack, E.R.; Soulières, D. Pembrolizumab plus axitinib versus sunitinib monotherapy as first-line treatment of advanced renal cell carcinoma (KEYNOTE-426): Extended follow-up from a randomised, open-label, phase 3 trial. Lancet Oncol. 2020, 21, 1563–1573. [Google Scholar] [CrossRef]
- Zhang, T.B.K.; Choudhury, A.D.; Chen, R.C.; Watt, C.; Wen, Y. DIGREE: An adaptive phase 3 trial of PD-inhibitor nivolumab and ipilimumab (IPI-NIVO) with VEGF TKI cabozantinib (CABO) in metastatic untreated renal cell cancer (Alliance A031704). J. Clin. Oncol. 2019. [Google Scholar] [CrossRef]
- Albiges, L.; Barthélémy, P.; Gross-Goupil, M.; Negrier, S.; Needle, M.N.; Escudier, B. TiNivo: Safety and efficacy of tivozanib-nivolumab combination therapy in patients with metastatic renal cell carcinoma. Ann. Oncol. 2021, 32, 97–102. [Google Scholar] [CrossRef] [PubMed]
- Taylor, M.H.; Lee, C.H.; Makker, V. Phase IB/II Trial of Lenvatinib Plus Pembrolizumab in Patients With Advanced Renal Cell Carcinoma, Endometrial Cancer, and Other Selected Advanced Solid Tumors. J. Clin. Oncol. 2020, 38, 1154–1163. [Google Scholar] [CrossRef]
- Makker, V.; Taylor, M.H.; Aghajanian, C. Lenvatinib Plus Pembrolizumab in Patients With Advanced Endometrial Cancer. J. Clin. Oncol. 2020, 38, 2981–2992. [Google Scholar] [CrossRef]
- Gao, J.K.J.; Tannir, N.M.; Slack, R.; Ahrar, K.; Rao, P. A pilot randomized study evaluating nivolumab (nivo) or nivo + bevacizumab (bev) or nivo + ipilimumab (ipi) in patients with metastatic renal cell carcinoma (MRCC) eligible for cytoreductive nephrectomy (CN), metastasectomy (MS) or post-treatment biopsy (Bx). J. Clin. Oncol. 2019, 37 (Suppl. S15), 4520. [Google Scholar]
- Dudek, A.Z.; Liu, L.C.; Alva, A.S.; Stein, M.; Gupta, S.; Albany, C.; Al-Janadi, A. Phase Ib study of pembrolizumab in combination with bevacizumab for the treatment of metastatic renal cell carcinoma: Big Ten Cancer Research Consortium BTCRC-GU14-003 (abstract 559). J. Clin. Oncol. 2016, 34, 559. [Google Scholar] [CrossRef]
- Dudek, A.Z.; Liu, L.C.; Gupta, S.; Logan, T.F.; Singer, E.A.; Joshi, M.; Zakharia, Y.N.; Lang, J.M.; Schwarz, J.K.; Al-Janadi, A.; et al. Phase Ib/II Clinical Trial of Pembrolizumab With Bevacizumab for Metastatic Renal Cell Carcinoma: BTCRC-GU14-003. J. Clin. Oncol 2020, 38, 1138–1145. [Google Scholar] [CrossRef]
- Atkins, M.B.; Rini, B.I.; Motzer, R.J.; Powles, T.; McDermott, D.F.; Suarez, C.; Bracarda, S.; Stadler, W.M.; Donskov, F.; Gurney, H.; et al. Patient-Reported Outcomes from the Phase III Randomized IMmotion151 Trial: Atezolizumab + Bevacizumab versus Sunitinib in Treatment-Naïve Metastatic Renal Cell Carcinoma. Clin. Cancer Res. 2020, 26, 2506–2514. [Google Scholar] [CrossRef]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).