Ultrasonography for Eating and Swallowing Assessment: A Narrative Review of Integrated Insights for Noninvasive Clinical Practice
Abstract
1. Introduction
2. Geniohyoid Muscle (Figure 1)

3. Digastric Muscle (Figure 2)
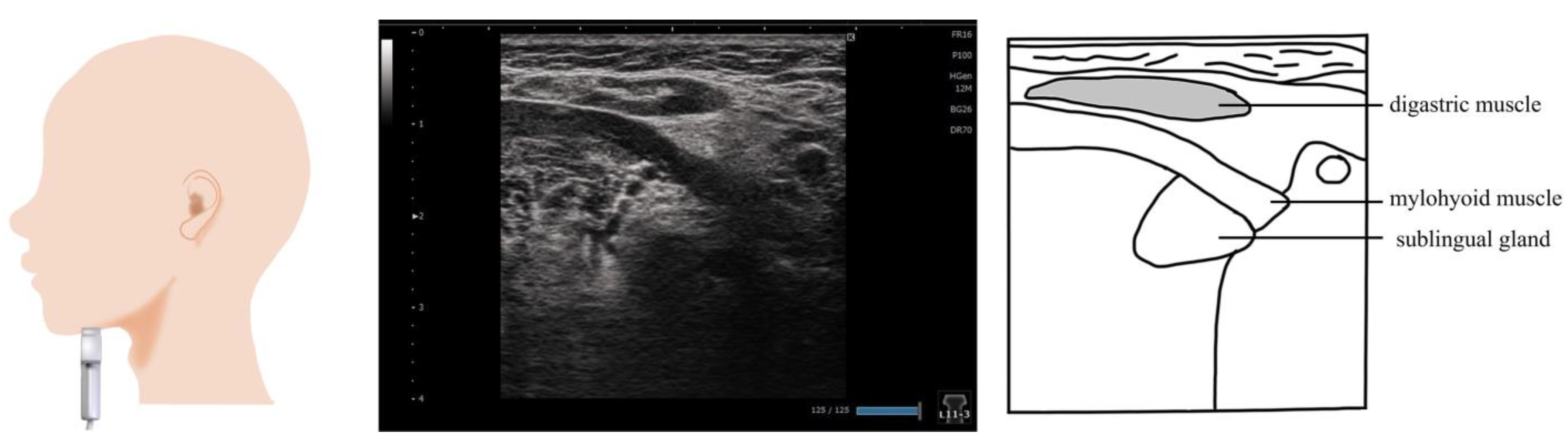
4. Mylohyoid Muscle (Figure 3)

5. Hyoid Bone
6. Tongue (Figure 4)
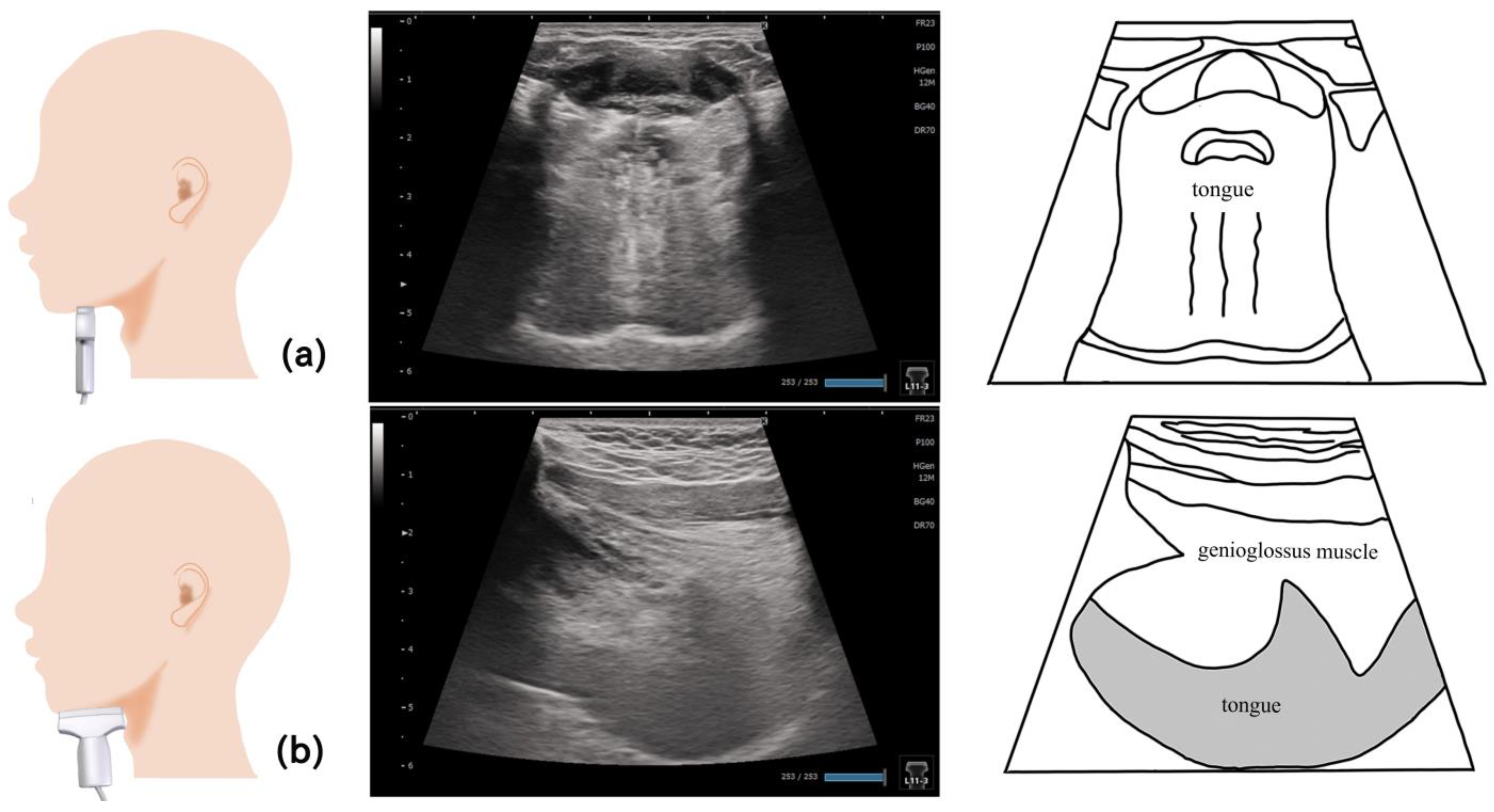
7. Masseter Muscle (Figure 6)

8. Genioglossus Muscle (Figure 7)
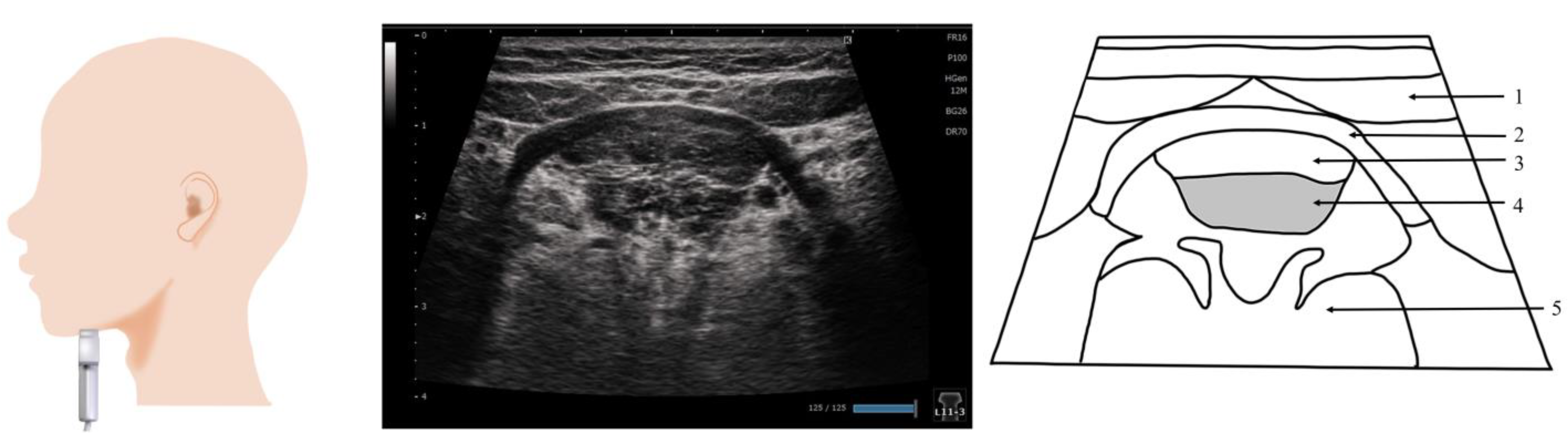
9. Orbicularis Oris Muscle (Figure 8)

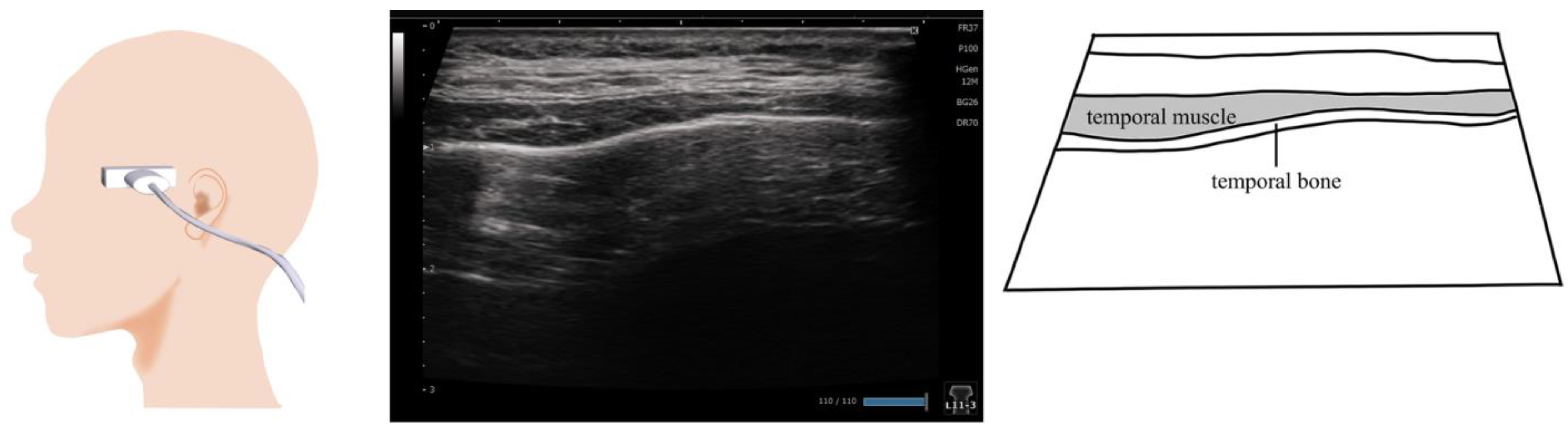
10. Temporalis Muscle (Figure 9)
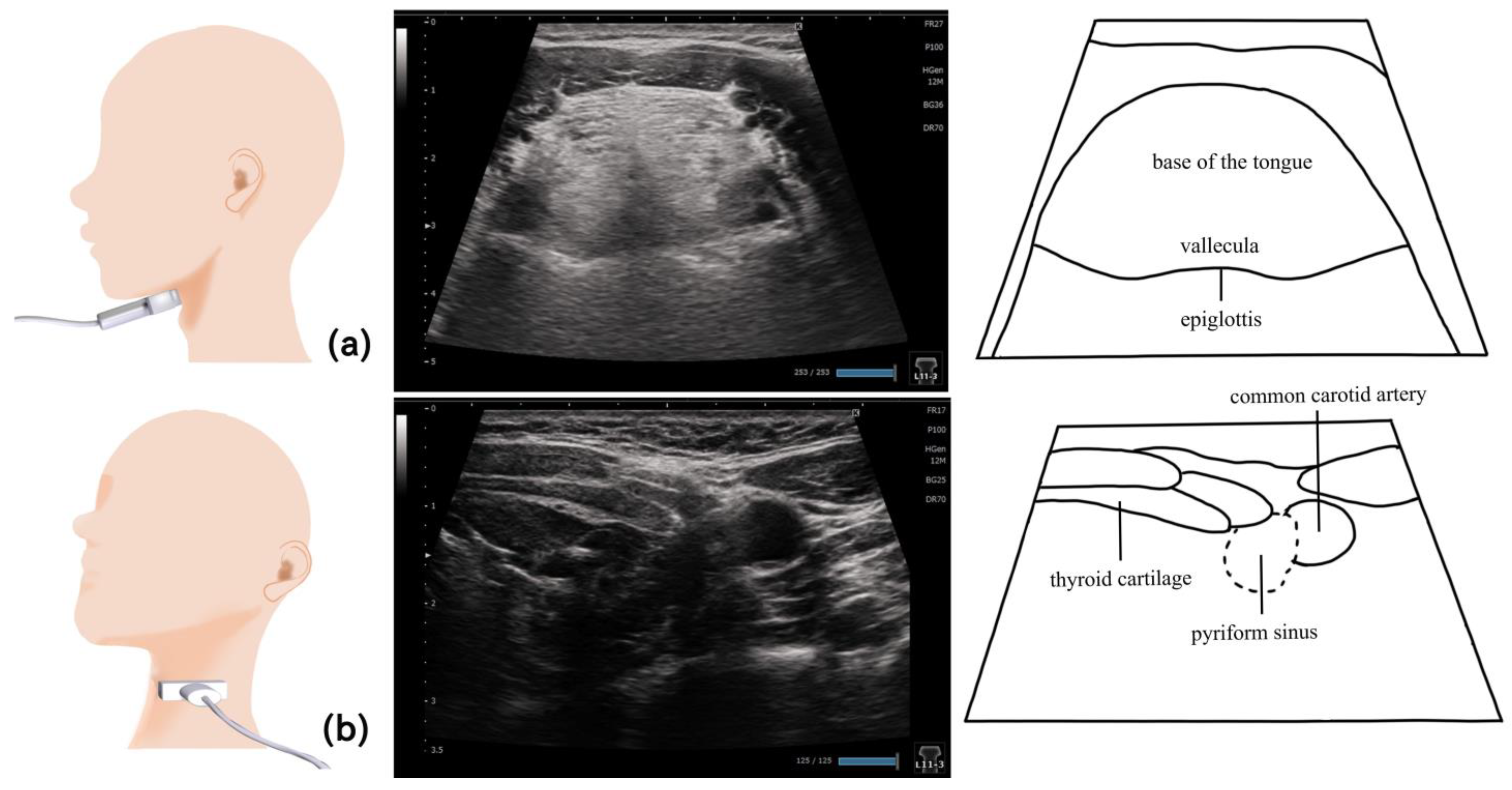
11. Pharynx (Figure 10 and Figure 11)

12. Esophagus (Figure 12)

13. Larynx (Figure 13)

14. Swallowing Function Evaluation
15. Summary
Author Contributions
Funding
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Cohen, D.L.; Roffe, C.; Beavan, J.; Blackett, B.; Fairfield, C.A.; Hamdy, S.; Havard, D.; McFarlane, M.; McLauglin, C.; Randall, M.; et al. Post-stroke dysphagia: A review and design considerations for future trials. Int. J. Stroke 2016, 11, 399–411. [Google Scholar] [CrossRef] [PubMed]
- Falsetti, P.; Acciai, C.; Palilla, R.; Bosi, M.; Carpinteri, F.; Zingarelli, A.; Pedace, C.; Lenzi, L. Oropharyngeal dysphagia after stroke: Incidence, diagnosis, and clinical predictors in patients admitted to a neurorehabilitation unit. J. Stroke Cerebrovasc. Dis. 2009, 18, 329–335. [Google Scholar] [CrossRef] [PubMed]
- Finestone, H.M.; Greene-Finestone, L.S.; Wilson, E.S.; Teasell, R.W. Malnutrition in stroke patients on the rehabilitation service and at follow-up: Prevalence and predictors. Arch. Phys. Med. Rehabil. 1995, 76, 310–316. [Google Scholar] [CrossRef] [PubMed]
- Daly, E.; Miles, A.; Scott, S.; Gillham, M. Finding the red flags: Swallowing difficulties after cardiac surgery in patients with prolonged intubation. J. Crit. Care 2016, 31, 119–124. [Google Scholar] [CrossRef]
- Bours, G.J.; Speyer, R.; Lemmens, J.; Limburg, M.; de Wit, R. Bedside screening tests vs. videofluoroscopy or fibreoptic endoscopic evaluation of swallowing to detect dysphagia in patients with neurological disorders: Systematic review. J. Adv. Nurs. 2009, 65, 477–493. [Google Scholar] [CrossRef]
- Kertscher, B.; Speyer, R.; Palmieri, M.; Plant, C. Bedside screening to detect oropharyngeal dysphagia in patients with neurological disorders: An updated systematic review. Dysphagia 2014, 29, 204–212. [Google Scholar] [CrossRef]
- Daniels, S.K.; Anderson, J.A.; Willson, P.C. Valid items for screening dysphagia risk in patients with stroke: A systematic review. Stroke 2012, 43, 892–897. [Google Scholar] [CrossRef]
- Tohara, H.; Saitoh, E.; Mays, K.A.; Kuhlemeier, K.; Palmer, J.B. Three tests for predicting aspiration without videofluorography. Dysphagia 2003, 18, 126–134. [Google Scholar] [CrossRef]
- Wu, M.C.; Chang, Y.C.; Wang, T.G.; Lin, L.C. Evaluating swallowing dysfunction using a 100-ml water swallowing test. Dysphagia 2004, 19, 43–47. [Google Scholar] [CrossRef]
- Martino, R.; Silver, F.; Teasell, R.; Bayley, M.; Nicholson, G.; Streiner, D.L.; Diamant, N.E. The Toronto Bedside Swallowing Screening Test (TOR-BSST): Development and validation of a dysphagia screening tool for patients with stroke. Stroke 2009, 40, 555–561. [Google Scholar] [CrossRef]
- Trapl, M.; Enderle, P.; Nowotny, M.; Teuschl, Y.; Matz, K.; Dachenhausen, A.; Brainin, M. Dysphagia bedside screening for acute-stroke patients: The Gugging Swallowing Screen. Stroke 2007, 38, 2948–2952. [Google Scholar] [CrossRef]
- Clave, P.; Arreola, V.; Romea, M.; Medina, L.; Palomera, E.; Serra-Prat, M. Accuracy of the volume-viscosity swallow test for clinical screening of oropharyngeal dysphagia and aspiration. Clin. Nutr. 2008, 27, 806–815. [Google Scholar] [CrossRef] [PubMed]
- Casey, P.; Alasmar, M.; McLaughlin, J.; Ang, Y.; McPhee, J.; Heire, P.; Sultan, J. The current use of ultrasound to measure skeletal muscle and its ability to predict clinical outcomes: A systematic review. J. Cachexia Sarcopenia Muscle 2022, 13, 2298–2309. [Google Scholar] [CrossRef] [PubMed]
- Hudson, H.M.; Daubert, C.R.; Mills, R.H. The interdependency of protein-energy malnutrition, aging, and dysphagia. Dysphagia 2000, 15, 31–38. [Google Scholar] [CrossRef] [PubMed]
- Fujishima, I.; Fujiu-Kurachi, M.; Arai, H.; Hyodo, M.; Kagaya, H.; Maeda, K.; Mori, T.; Nishioka, S.; Oshima, F.; Ogawa, S.; et al. Sarcopenia and dysphagia: Position paper by four professional organizations. Geriatr. Gerontol. Int. 2019, 19, 91–97. [Google Scholar] [CrossRef]
- Maeda, K.; Takaki, M.; Akagi, J. Decreased Skeletal Muscle Mass and Risk Factors of Sarcopenic Dysphagia: A Prospective Observational Cohort Study. J. Gerontol. A Biol. Sci. Med. Sci. 2017, 72, 1290–1294. [Google Scholar] [CrossRef]
- Maeda, K.; Ishida, Y.; Nonogaki, T.; Shimizu, A.; Yamanaka, Y.; Matsuyama, R.; Kato, R.; Mori, N. Development and Predictors of Sarcopenic Dysphagia during Hospitalization of Older Adults. Nutrients 2019, 12, 70. [Google Scholar] [CrossRef] [PubMed]
- Allen, J.E.; Clunie, G.M.; Winiker, K. Ultrasound: An emerging modality for the dysphagia assessment toolkit? Curr. Opin. Otolaryngol. Head. Neck Surg. 2021, 29, 213–218. [Google Scholar] [CrossRef]
- Hsiao, M.Y.; Wu, C.H.; Wang, T.G. Emerging Role of Ultrasound in Dysphagia Assessment and Intervention: A Narrative Review. Front. Rehabil. Sci. 2021, 2, 708102. [Google Scholar] [CrossRef]
- Miura, Y.; Tamai, N.; Kitamura, A.; Yoshida, M.; Takahashi, T.; Mugita, Y.; Tobita, I.; Arita, M.; Urai, T.; Dai, M.; et al. Diagnostic accuracy of ultrasound examination in detecting aspiration and pharyngeal residue in patients with dysphagia: A systematic review and meta-analysis. Jpn. J. Nurs. Sci. 2021, 18, e12396. [Google Scholar] [CrossRef]
- Khan, Y.S.; Bordoni, B. Anatomy, Head and Neck, Suprahyoid Muscle; StatPearls: Treasure Island, FL, USA, 2022. [Google Scholar]
- Baba, T.; Goto, T.; Fujimoto, K.; Honda, T.; Yagi, K.; Nagao, K.; Ichikawa, T. Age-related Changes in Geniohyoid Muscle Morphology Predict Reduced Swallowing Function. J. Oral. Health Biosci. 2017, 30, 18–25. [Google Scholar] [CrossRef]
- Ogawa, N.; Mori, T.; Fujishima, I.; Wakabayashi, H.; Itoda, M.; Kunieda, K.; Shigematsu, T.; Nishioka, S.; Tohara, H.; Yamada, M.; et al. Ultrasonography to Measure Swallowing Muscle Mass and Quality in Older Patients With Sarcopenic Dysphagia. J. Am. Med. Dir. Assoc. 2018, 19, 516–522. [Google Scholar] [CrossRef]
- Miura, Y.; Nakagami, G.; Tohara, H.; Ogawa, N.; Sanada, H. The association between jaw-opening strength, geniohyoid muscle thickness and echo intensity measured by ultrasound. Med. Ultrason. 2020, 22, 299–304. [Google Scholar] [CrossRef] [PubMed]
- Pauloski, B.R.; Yahnke, K.M. Using Ultrasound to Document the Effects of Expiratory Muscle Strength Training (EMST) on the Geniohyoid Muscle. Dysphagia 2022, 37, 788–799. [Google Scholar] [CrossRef]
- Park, J.S.; Lee, S.H.; Jung, S.H.; Choi, J.B.; Jung, Y.J. Tongue strengthening exercise is effective in improving the oropharyngeal muscles associated with swallowing in community-dwelling older adults in South Korea: A randomized trial. Medicine 2019, 98, e17304. [Google Scholar] [CrossRef]
- Cheng, D.T.H.; Lee, K.Y.S.; Ahuja, A.T.; Tong, M.C.F. Sonographic assessment of swallowing in irradiated nasopharyngeal carcinoma patients. Laryngoscope 2018, 128, 2552–2559. [Google Scholar] [CrossRef] [PubMed]
- Feng, X.; Cartwright, M.S.; Walker, F.O.; Bargoil, J.H.; Hu, Y.; Butler, S.G. Ultrasonographic evaluation of geniohyoid muscle and hyoid bone during swallowing in young adults. Laryngoscope 2015, 125, 1886–1891. [Google Scholar] [CrossRef] [PubMed]
- Yabunaka, K.; Konishi, H.; Nakagami, G.; Sanada, H.; Iizaka, S.; Sanada, S.; Ohue, M. Ultrasonographic evaluation of geniohyoid muscle movement during swallowing: A study on healthy adults of various ages. Radiol. Phys. Technol. 2012, 5, 34–39. [Google Scholar] [CrossRef]
- Shimizu, S.; Hanayama, K.; Metani, H.; Sugiyama, T.; Abe, H.; Seki, S.; Hiraoka, T.; Tsubahara, A. Retest reliability of ultrasonic geniohyoid muscle measurement. Jpn. J. Compr. Rehabil. Sci. 2016, 7, 55–60. [Google Scholar] [CrossRef]
- Choi, J.B.; Jung, Y.J.; Park, J.S. Comparison of 2 types of therapeutic exercise: Jaw opening exercise and head lift exercise for dysphagic stroke: A pilot study. Medicine 2020, 99, e22136. [Google Scholar] [CrossRef]
- Jung, Y.J.; Kim, H.J.; Choi, J.B.; Park, J.S.; Hwang, N.K. Effect of Dysphagia Rehabilitation Using Kinesiology Taping on Oropharyngeal Muscle Hypertrophy in Post-Stroke Patients: A Double Blind Randomized Placebo-Controlled Trial. Healthcare 2020, 8, 411. [Google Scholar] [CrossRef] [PubMed]
- van den Engel-Hoek, L.; Erasmus, C.E.; Hendriks, J.C.; Geurts, A.C.; Klein, W.M.; Pillen, S.; Sie, L.T.; de Swart, B.J.; de Groot, I.J. Oral muscles are progressively affected in Duchenne muscular dystrophy: Implications for dysphagia treatment. J. Neurol. 2013, 260, 1295–1303. [Google Scholar] [CrossRef] [PubMed]
- Macrae, P.R.; Doeltgen, S.H.; Jones, R.D.; Huckabee, M.L. Intra- and inter-rater reliability for analysis of hyoid displacement measured with sonography. J. Clin. Ultrasound 2012, 40, 74–78. [Google Scholar] [CrossRef]
- Tranchito, E.N.; Bordoni, B. Anatomy, Head and Neck, Digastric Muscle; StatPearls: Treasure Island, FL, USA, 2022. [Google Scholar]
- Holzapfel, K.; Naumann, M. Ultrasound Detection of Vagus Nerve Atrophy in Bulbar Amyotrophic Lateral Sclerosis. J. Neuroimaging 2020, 30, 762–765. [Google Scholar] [CrossRef]
- Winiker, K.; Hammond, R.; Thomas, P.; Dimmock, A.; Huckabee, M.L. Swallowing assessment in patients with dysphagia: Validity and reliability of a pocket-sized ultrasound system. Int. J. Lang. Commun. Disord. 2022, 57, 539–551. [Google Scholar] [CrossRef]
- Toth, J.; Lappin, S.L. Anatomy, Head and Neck, Mylohyoid Muscle; StatPearls: Treasure Island, FL, USA, 2022. [Google Scholar]
- Feng, S.; Shea, Q.T.; Ng, K.Y.; Tang, C.N.; Kwong, E.; Zheng, Y. Automatic Hyoid Bone Tracking in Real-Time Ultrasound Swallowing Videos Using Deep Learning Based and Correlation Filter Based Trackers. Sensors 2021, 21, 3712. [Google Scholar] [CrossRef]
- Winiker, K.; Burnip, E.; Gozdzikowska, K.; Guiu Hernandez, E.; Hammond, R.; Macrae, P.; Huckabee, M.L. Ultrasound: Validity of a Pocket-Sized System in the Assessment of Swallowing. Dysphagia 2021, 36, 1010–1018. [Google Scholar] [CrossRef]
- Matsuo, T.; Matsuyama, M. Detection of poststroke oropharyngeal dysphagia with swallowing screening by ultrasonography. PLoS ONE 2021, 16, e0248770. [Google Scholar] [CrossRef]
- Costa, B.; Rodrigues, D.S.B.; Magalhaes, D.D.D.; Santos, A.S.; Santos, R.V.; Azevedo, E.H.M.; Almeida, A.A.; Pernambuco, L. Quantitative Ultrasound Assessment of Hyoid Bone Displacement During Swallowing Following Thyroidectomy. Dysphagia 2021, 36, 659–669. [Google Scholar] [CrossRef]
- Perry, S.E.; Winkelman, C.J.; Huckabee, M.L. Variability in Ultrasound Measurement of Hyoid Bone Displacement and Submental Muscle Size Using 2 Methods of Data Acquisition. Folia Phoniatr. Logop. 2016, 68, 205–210. [Google Scholar] [CrossRef]
- Chen, Y.C.; Hsiao, M.Y.; Wang, Y.C.; Fu, C.P.; Wang, T.G. Reliability of Ultrasonography in Evaluating Hyoid Bone Movement. J. Med. Ultrasound 2017, 25, 90–95. [Google Scholar] [CrossRef]
- Rocha, S.G.; Silva, R.G.; Berti, L.C. Qualitative and quantitative ultrasound analysis of oropharyngeal swallowing. Codas 2015, 27, 437–445. [Google Scholar] [CrossRef]
- Ahn, S.Y.; Cho, K.H.; Beom, J.; Park, D.J.; Jee, S.; Nam, J.H. Reliability of ultrasound evaluation of hyoid-larynx approximation with positional change. Ultrasound Med. Biol. 2015, 41, 1221–1225. [Google Scholar] [CrossRef] [PubMed]
- Huang, Y.L.; Hsieh, S.F.; Chang, Y.C.; Chen, H.C.; Wang, T.G. Ultrasonographic evaluation of hyoid-larynx approximation in dysphagic stroke patients. Ultrasound Med. Biol. 2009, 35, 1103–1108. [Google Scholar] [CrossRef]
- Kuhl, V.; Eicke, B.M.; Dieterich, M.; Urban, P.P. Sonographic analysis of laryngeal elevation during swallowing. J. Neurol. 2003, 250, 333–337. [Google Scholar] [CrossRef]
- Sonies, B.C.; Wang, C.; Sapper, D.J. Evaluation of normal and abnormal hyoid bone movement during swallowing by use of ultrasound duplex-Doppler imaging. Ultrasound Med. Biol. 1996, 22, 1169–1175. [Google Scholar] [CrossRef] [PubMed]
- Hsiao, M.Y.; Chang, Y.C.; Chen, W.S.; Chang, H.Y.; Wang, T.G. Application of ultrasonography in assessing oropharyngeal dysphagia in stroke patients. Ultrasound Med. Biol. 2012, 38, 1522–1528. [Google Scholar] [CrossRef] [PubMed]
- Lee, Y.S.; Lee, K.E.; Kang, Y.; Yi, T.I.; Kim, J.S. Usefulness of Submental Ultrasonographic Evaluation for Dysphagia Patients. Ann. Rehabil. Med. 2016, 40, 197–205. [Google Scholar] [CrossRef]
- Soder, N.; Miller, N. Using ultrasound to investigate intrapersonal variability in durational aspects of tongue movement during swallowing. Dysphagia 2002, 17, 288–297. [Google Scholar] [CrossRef]
- Oh, E.H.; Seo, J.S.; Kang, H.J. Assessment of Oropharyngeal Dysphagia in Patients With Parkinson Disease: Use of Ultrasonography. Ann. Rehabil. Med. 2016, 40, 190–196. [Google Scholar] [CrossRef]
- Cergan, R.; Dumitru, M.; Vrinceanu, D.; Neagos, A.; Jeican, I.I.; Ciuluvica, R.C. Ultrasonography of the larynx: Novel use during the SARS-CoV-2 pandemic (Review). Exp. Ther. Med. 2021, 21, 273. [Google Scholar] [CrossRef] [PubMed]
- Nienstedt, J.C.; Muller, F.; Rosler, A.; Pflug, C. Presbyphagia Diagnostics Using M-Mode Ultrasound: Changes in the Tongue Movement Pattern. Dysphagia 2020, 35, 696–701. [Google Scholar] [CrossRef]
- Chantaramanee, A.; Tohara, H.; Nakagawa, K.; Hara, K.; Nakane, A.; Yamaguchi, K.; Yoshimi, K.; Junichi, F.; Minakuchi, S. Association between echo intensity of the tongue and its thickness and function in elderly subjects. J. Oral. Rehabil. 2019, 46, 634–639. [Google Scholar] [CrossRef] [PubMed]
- Peng, C.L.; Jost-Brinkmann, P.G.; Yoshida, N.; Chou, H.H.; Lin, C.T. Comparison of tongue functions between mature and tongue-thrust swallowing--an ultrasound investigation. Am. J. Orthod. Dentofacial Orthop. 2004, 125, 562–570. [Google Scholar] [CrossRef] [PubMed]
- Fuhrmann, R.A.; Diedrich, P.R. B-mode ultrasound scanning of the tongue during swallowing. Dentomaxillof. Radiol. 1994, 23, 211–215. [Google Scholar] [CrossRef]
- Ohkubo, M.; Scobbie, J.M. Tongue Shape Dynamics in Swallowing Using Sagittal Ultrasound. Dysphagia 2019, 34, 112–118. [Google Scholar] [CrossRef]
- Maniere-Ezvan, A.; Duval, J.M.; Darnault, P. Ultrasonic assessment of the anatomy and function of the tongue. Surg. Radiol. Anat. 1993, 15, 55–61. [Google Scholar] [CrossRef]
- Galen, S.; Jost-Brinkmann, P.G. B-mode and M-mode Ultrasonography of Tongue Movements during Swallowing. J. Orofac. Orthop. 2010, 71, 125–135. [Google Scholar] [CrossRef]
- Umay, E.; Ozturk, E.; Gurcay, E.; Delibas, O.; Celikel, F. Swallowing in Parkinson’s disease: How is it affected? Clin. Neurol. Neurosurg. 2019, 177, 37–41. [Google Scholar] [CrossRef]
- Nakamori, M.; Hosomi, N.; Takaki, S.; Oda, M.; Hiraoka, A.; Yoshikawa, M.; Matsushima, H.; Ochi, K.; Tsuga, K.; Maruyama, H.; et al. Tongue thickness evaluation using ultrasonography can predict swallowing function in amyotrophic lateral sclerosis patients. Clin. Neurophysiol. 2016, 127, 1669–1674. [Google Scholar] [CrossRef]
- Gaszynska, E.; Godala, M.; Szatko, F.; Gaszynski, T. Masseter muscle tension, chewing ability, and selected parameters of physical fitness in elderly care home residents in Lodz, Poland. Clin. Interv. Aging 2014, 9, 1197–1203. [Google Scholar] [CrossRef]
- Sanz-Paris, A.; Gonzalez-Fernandez, M.; Hueso-Del Rio, L.E.; Ferrer-Lahuerta, E.; Monge-Vazquez, A.; Losfablos-Callau, F.; Sanclemente-Hernandez, T.; Sanz-Arque, A.; Arbones-Mainar, J.M. Muscle Thickness and Echogenicity Measured by Ultrasound Could Detect Local Sarcopenia and Malnutrition in Older Patients Hospitalized for Hip Fracture. Nutrients 2021, 13, 2401. [Google Scholar] [CrossRef]
- Gawriolek, K.; Klatkiewicz, T.; Przystanska, A.; Maciejewska-Szaniec, Z.; Gedrange, T.; Czajka-Jakubowska, A. Standardization of the ultrasound examination of the masseter muscle with size-independent calculation of records. Adv. Clin. Exp. Med. 2021, 30, 441–447. [Google Scholar] [CrossRef]
- Chang, P.H.; Chen, Y.J.; Chang, K.V.; Wu, W.T.; Ozcakar, L. Ultrasound measurements of superficial and deep masticatory muscles in various postures: Reliability and influencers. Sci. Rep. 2020, 10, 14357. [Google Scholar] [CrossRef] [PubMed]
- Kiliaridis, S.; Kalebo, P. Masseter muscle thickness measured by ultrasonography and its relation to facial morphology. J. Dent. Res. 1991, 70, 1262–1265. [Google Scholar] [CrossRef] [PubMed]
- Tircoveluri, S.; Singh, J.R.; Rayapudi, N.; Karra, A.; Begum, M.; Challa, P. Correlation of masseter muscle thickness and intermolar width—an ultrasonography study. J. Int. Oral. Health 2013, 5, 28–34. [Google Scholar] [PubMed]
- Kwan, B.C.; Butler, J.E.; Hudson, A.L.; McKenzie, D.K.; Bilston, L.E.; Gandevia, S.C. A novel ultrasound technique to measure genioglossus movement in vivo. J. Appl. Physiol. 2014, 117, 556–562. [Google Scholar] [CrossRef]
- Kwan, B.C.H.; McBain, R.A.; Luu, B.L.; Butler, J.E.; Bilston, L.E.; Gandevia, S.C. Influence of respiratory mechanics and drive on genioglossus movement under ultrasound imaging. PLoS ONE 2018, 13, e0195884. [Google Scholar] [CrossRef] [PubMed]
- den Herder, C.; Schmeck, J.; Appelboom, D.J.; de Vries, N. Risks of general anaesthesia in people with obstructive sleep apnoea. BMJ 2004, 329, 955–959. [Google Scholar] [CrossRef]
- Kakudo, M.; Matsuo, S.; Maeda, K.; Yasui, Y.; Imai, A.; Tanaka, J.; Tanaka, M. Inter-rater reliability for measurement of tongue movement during chewing and swallowing using ultrasonography. J. Osaka Dent. Univ. 2020, 54, 29–34. [Google Scholar] [CrossRef]
- Hanazawa, T.; Araki, K.; Kuroda, M. 3D/4D Ultrasonographic examinations for analyzing swallowing movements: Assessing their ability to delineate tongue and bolus movements. Dent. Radiol. 2019, 58, 79–85. (In Japanese) [Google Scholar] [CrossRef]
- Park, H.S.; Kim, J.U.; Park, J.Y.; Oh, D.H.; Kim, H.J. Comparison of orbicularis oris muscle strength and endurance in young and elderly adults. J. Phys. Ther. Sci. 2018, 30, 1477–1478. [Google Scholar] [CrossRef]
- Park, H.S.; Park, J.Y.; Kwon, Y.H.; Choi, H.S.; Kim, H.J. Effect of orbicularis oris muscle training on muscle strength and lip closure function in patients with stroke and swallowing disorder. J. Phys. Ther. Sci. 2018, 30, 1355–1356. [Google Scholar] [CrossRef] [PubMed]
- Zhang, W.H.; Chen, Y.Y.; Liu, J.J.; Liao, X.H.; Du, Y.C.; Gao, Y. Application of ultrasound imaging of upper lip orbicularis oris muscle. Int. J. Clin. Exp. Med. 2015, 8, 3391–3400. [Google Scholar] [PubMed]
- Masuoka, H. The Visualization of the Functional Structure of the Crossing Fibers of the Orbicularis Oris Muscle Using Ultrasound. Plast. Reconstr. Surg. Glob. Open 2017, 5, e1331. [Google Scholar] [CrossRef]
- Fujiwara, K.; Yoshida, M.; Nakamichi, N.; Saitoh, S.; Takaichi, M.; Ishizaka, R.; Tomihara, K.; Noguchi, M. Mini-microform cleft lip with complete cleft alveolus and palate: A case report. Congenit Anom 2021, 61, 133–137. [Google Scholar] [CrossRef]
- Volk, G.F.; Wystub, N.; Pohlmann, M.; Finkensieper, M.; Chalmers, H.J.; Guntinas-Lichius, O. Quantitative ultrasonography of facial muscles. Muscle Nerve 2013, 47, 878–883. [Google Scholar] [CrossRef]
- Gaszynska, E.; Kopacz, K.; Fronczek-Wojciechowska, M.; Padula, G.; Szatko, F. Electromyographic activity of masticatory muscles in elderly women—a pilot study. Clin. Interv. Aging 2017, 12, 111–116. [Google Scholar] [CrossRef][Green Version]
- Miura, Y.; Yabunaka, K.; Karube, M.; Tsutaoka, T.; Yoshida, M.; Matsumoto, M.; Nakagami, G.; Kamakura, Y.; Sugama, J.; Sanada, H. Establishing a Methodology for Ultrasound Evaluation of Pharyngeal Residue in the Pyriform Sinus and Epiglottic Vallecula. Respir. Care 2020, 65, 304–313. [Google Scholar] [CrossRef]
- Miller, J.L.; Watkin, K.L. Lateral pharyngeal wall motion during swallowing using real time ultrasound. Dysphagia 1997, 12, 125–132. [Google Scholar] [CrossRef]
- Cordeiro, B.A.; Stefani, F.M.; Goldfeder, E.M. Study of the correlation between the linear measurements of the skull and face and palatal wide and length measures. Codas 2015, 27, 472–477. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Moriniere, S.; Hammoudi, K.; Marmouset, F.; Bakhos, D.; Beutter, P.; Patat, F. Ultrasound analysis of the upper esophageal sphincter during swallowing in the healthy subject. Eur. Ann. Otorhinolaryngol. Head Neck Dis. 2013, 130, 321–325. [Google Scholar] [CrossRef] [PubMed]
- Watanabe, M.; Hironaka, S.; Utsumi, A.; Murata, N.; Mukai, Y. The standardized method for ultrasound imaging of oropharyngeal on swallowing. J. Jpn. Soc. Disabil. Oral. Health 2011, 32, 19–28. (In Japanese) [Google Scholar]
- Manabe, N.; Haruma, K.; Nakato, R.; Kusunoki, H.; Kamada, T.; Hata, J. New ultrasonographic screening method for oropharyngeal dysphagia: Tissue Doppler imaging. Am. J. Physiol. Gastrointest. Liver Physiol. 2018, 314, G32–G38. [Google Scholar] [CrossRef]
- Miura, Y.; Nakagami, G.; Yabunaka, K.; Tohara, H.; Hara, K.; Noguchi, H.; Mori, T.; Sanada, H. Detecting pharyngeal post-swallow residue by ultrasound examination: A case series. Med. Ultrason. 2016, 18, 288–293. [Google Scholar] [CrossRef]
- Miura, Y.; Nakagami, G.; Yabunaka, K.; Tohara, H.; Murayama, R.; Noguchi, H.; Mori, T.; Sanada, H. Method for detection of aspiration based on B-mode video ultrasonography. Radiol. Phys. Technol. 2014, 7, 290–295. [Google Scholar] [CrossRef]
- Miura, Y.; Nakagami, G.; Yabunaka, K.; Tohara, H.; Noguchi, H.; Mori, T.; Sanada, H. A Randomized Controlled Trial to Investigate the Effectiveness of the Prevention of Aspiration Pneumonia Using Recommendations for Swallowing Care Guided by Ultrasound Examination. Healthcare 2018, 6, 15. [Google Scholar] [CrossRef] [PubMed]
- de Miguel, M.; Pelaez, E.M.; Caubet, E.; Gonzalez, O.; Velasco, M.; Rigual, L. Accuracy of transcutaneous laryngeal ultrasound for detecting vocal cord paralysis in the immediate postoperative period after total thyroidectomy. Minerva Anestesiol. 2017, 83, 1239–1247. [Google Scholar] [CrossRef] [PubMed]
- Fukuhara, T.; Donishi, R.; Matsuda, E.; Koyama, S.; Fujiwara, K.; Takeuchi, H. A Novel Lateral Approach to the Assessment of Vocal Cord Movement by Ultrasonography. World J. Surg. 2018, 42, 130–136. [Google Scholar] [CrossRef] [PubMed]
- Carneiro-Pla, D.; Miller, B.S.; Wilhelm, S.M.; Milas, M.; Gauger, P.G.; Cohen, M.S.; Hughes, D.T.; Solorzano, C.C. Feasibility of surgeon-performed transcutaneous vocal cord ultrasonography in identifying vocal cord mobility: A multi-institutional experience. Surgery 2014, 156, 1597–1602; discussion 1602–1594. [Google Scholar] [CrossRef]
- Turton, P.; Hay, R.; Welters, I. Assessment of peripheral muscle thickness and architecture in healthy volunteers using hand-held ultrasound devices; A comparison study with standard ultrasound. BMC Med. Imaging 2019, 19, 69. [Google Scholar] [CrossRef] [PubMed]
- Lambell, K.J.; Tierney, A.C.; Wang, J.C.; Nanjayya, V.; Forsyth, A.; Goh, G.S.; Vicendese, D.; Ridley, E.J.; Parry, S.M.; Mourtzakis, M.; et al. Comparison of Ultrasound-Derived Muscle Thickness With Computed Tomography Muscle Cross-Sectional Area on Admission to the Intensive Care Unit: A Pilot Cross-Sectional Study. JPEN J. Parenter. Enter. Nutr. 2021, 45, 136–145. [Google Scholar] [CrossRef] [PubMed]
- Paris, M.T.; Letofsky, N.; Mourtzakis, M. Site-specific skeletal muscle echo intensity and thickness differences in subcutaneous adipose tissue matched older and younger adults. Clin. Physiol. Funct. Imaging 2021, 41, 156–164. [Google Scholar] [CrossRef] [PubMed]
| Muscle | Methods | |||
|---|---|---|---|---|
| Posture | Probe | Position and Orientation | Evaluation Method | |
| Geniohyoid cross-sectional area/thickness | Sitting position | Linear | Sagittal section | Identify the area surrounded by fascia and calculate the cross-sectional area. Measure the muscle thickness. |
| Digastric cross-sectional area/thickness | Sitting position | Linear | Vertical to muscle fibers | Calculate the cross-sectional area. Measure the muscle thickness. |
| Mylohyoid thickness | Sitting position | Linear | Coronal plane | Measure the thickness of the mylohyoid muscle under the submandibular gland. |
| Tongue thickness | Sitting position | Convex | Coronal plane | Measure the distance from the mylohyoid muscle to the dorsum of the tongue. |
| Masseter thickness | Sitting position | Linear | Vertical to muscle fibers | Measure the thickest site. |
| Depressor anguli oris | Sitting position | Linear | Vertical to muscle fibers | Calculate the largest area. |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Maeda, K.; Nagasaka, M.; Nagano, A.; Nagami, S.; Hashimoto, K.; Kamiya, M.; Masuda, Y.; Ozaki, K.; Kawamura, K. Ultrasonography for Eating and Swallowing Assessment: A Narrative Review of Integrated Insights for Noninvasive Clinical Practice. Nutrients 2023, 15, 3560. https://doi.org/10.3390/nu15163560
Maeda K, Nagasaka M, Nagano A, Nagami S, Hashimoto K, Kamiya M, Masuda Y, Ozaki K, Kawamura K. Ultrasonography for Eating and Swallowing Assessment: A Narrative Review of Integrated Insights for Noninvasive Clinical Practice. Nutrients. 2023; 15(16):3560. https://doi.org/10.3390/nu15163560
Chicago/Turabian StyleMaeda, Keisuke, Motoomi Nagasaka, Ayano Nagano, Shinsuke Nagami, Kakeru Hashimoto, Masaki Kamiya, Yuto Masuda, Kenichi Ozaki, and Koki Kawamura. 2023. "Ultrasonography for Eating and Swallowing Assessment: A Narrative Review of Integrated Insights for Noninvasive Clinical Practice" Nutrients 15, no. 16: 3560. https://doi.org/10.3390/nu15163560
APA StyleMaeda, K., Nagasaka, M., Nagano, A., Nagami, S., Hashimoto, K., Kamiya, M., Masuda, Y., Ozaki, K., & Kawamura, K. (2023). Ultrasonography for Eating and Swallowing Assessment: A Narrative Review of Integrated Insights for Noninvasive Clinical Practice. Nutrients, 15(16), 3560. https://doi.org/10.3390/nu15163560







