Quality of Palliative and End-Of-Life Care in Hong Kong: Perspectives of Healthcare Providers
Abstract
1. Background
2. Materials and Methods
2.1. Study Design and Participants
2.2. Data Collection and Analyses
3. Results
3.1. Political Context
3.1.1. Terminology on Palliative and End-Of-Life Care
“There is actually a slight difference between “EOL care” in the UK and “EOL care” in other countries. Some, refer to patients’ last few days and others may be talking about last few months, or even year. So we don’t actually have standardized terminology.”[I5, doctor]
“We heard in some discussions that there are misconceptions among citizens that EOL refers to giving up treatment…”[I FGD5, dietitian]
3.1.2. Overarching Policies for Palliative and End-Of-Life Care
“… the system isn’t ready… regarding dying at home, the system is not well coordinated. This includes not having good service to support [dying at home].”[I7, doctor]
“…the government does not have clear-cut policies or directions, actually on elderly care as a whole… The government wants to focus on elderly health services, EOL care services, those sorts of things. But in my opinion, they are very [disease-specific], firstly. Secondly it is very fragmented.”[A FGD1, physiotherapist]
3.2. Organizational Setting
3.2.1. Multidisciplinary Collaboration
“Currently, under palliative care services, home care support is mainly [provided by] home care nurses, with the support from physicians, mainly home care nurses. But I feel that more can be done in the social [care] aspect, because we feel that there is a gap… But it is still inadequate, because their manpower is limited, so they could only focus on their health.”[B FGD2, medical social worker]
“Of course having a team is very important because sometimes one person may not be able to see things in all aspects... If [the patient] is under a multidisciplinary team or at least able to receive advice from a second discipline, the interaction may be able to provide a better service.”[I8, doctor]
Similarly, although preparatory measures were carried out to enable elderly home staff to provide care in elderly homes, coordination between hospital and elderly home staff may be limited. Inadequate collaboration between medical and social sectors hinders the provision of integrated care, as one of the participants expressed fragmentation of services provided by different sectors and organizations.
“…right now there are loads of services, Social Welfare Department is working on [aging], Department of Health is working on it, HA [Hospital Authority] is working on it, non-governmental organizations are working on it, it is actually very fragmented, and everyone is doing their own thing…”[C FGD1, physiotherapist]
3.2.2. Information System
“it [AD/ACP/DNACPR documents] is in the CMS [Clinical Management System], so it would be able to alert [A&E staff]. If an A&E staff has assessed the case and believe that the patient does not need to be admitted to [acute hospital] ward, then (s) he would know, and would send the patient to [convalescent hospital] ward as soon as possible.”[C FGD10, nurse]
“…so I think in the CMS platform, our allied health notes would not be seen because we hand write all of them. Once it is written, it is then stored in the cabinet, so physicians do not actually know about our progress…”[A FGD3, physiotherapist]
3.3. Support to Patients, Caregivers, and Family Members
3.3.1. Inpatient Support
“Sometimes at the acute ward, [health providers] may feel that [the provision of palliative care] is not their priority… they are already very busy doing rescue work.”[I3, doctor]
“…even in our oncology center, there may be patients who would start palliative care at a very late stage… this is actually not ideal. It should be started sooner, the sooner the better. ‘The sooner the better’ is linked with resources.”[I8, doctor]
Consultative teams of palliative care specialists are established to provide support to healthcare providers at acute settings. However, participants have indicated that further improvements could be made, including increasing the manpower of different disciplines in the consultative teams.
“Different hospitals have consultative teams, but right now it is not very comprehensive. The staff manpower of the teams are insufficient…not all hospitals have a consultative team to provide services, and even if they do, provision would not be comprehensive. It may require nurses, physicians, and allied health professionals to support, to consult patients and to give advice.”[I7, doctor]
3.3.2. Community Support
“…the problem we are facing right now is that the support outside of hospitals is inadequate... Actually, there are some patients [who], you can say, medically, can be discharged... Technically they do not require hospital-level care, but most of the time; the tendency is that their family [size]… may be very small, only the couple. Also, the partner most probably won’t be young, and (s) he would not have any experience of medical care and would find it difficult to look after the patient. Therefore the patient is staying in the hospital.”[I5, doctor]
“…if we are able to support [patients at home], their quality of life may be able to improve. For example, if they are able to be more functional in their lives, then they may also gain dignity.”[D FGD3, occupational therapist]
“…there basically isn’t any transportation. Because you can’t, per usual, take the bus… They may be wheelchair-bound [and need] special transportation, but right now… it’s very difficult to find one.”[A FGD6, occupational therapist]
“Because the only service that does not require extra charge is NEATS [Non-emergency Ambulance Transfer Service]. But the service of NEATS is limited… They may only transfer four, five [patients at a time]… there are also criteria. You have to either be living alone or [live in places not accessible by elevators]… or you require long-term oxygen, only then would they pick you up. Therefore if a typical elderly does not fall into [these categories] then (s) he would have to find his/her own transportation.”[B FGD6, physiotherapist]
3.4. Healthcare Workers and Public
3.4.1. Staff Training and Skill Transfer
“Actually the current situation [of the EOL-RCHE program] is that palliative care staff would, to a certain extent, enable geriatric staff to manage the needs of patients. We are talking about some sort of teaching, skill transfer and even sending a member of staff over to do some coaching…”[I5, doctor]
“The staff training prior to the program is actually very limited, but as soon as the program starts, [they] already have to start doing intensive work, talking about life and death. It actually isn’t easy, having to do it based on a couple of training. You really need some sort of talent to be able to do that.”[D FGD12, nurse—APN]
3.4.2. Readiness and Competence of Healthcare Staff
“…I believe it’s their years of experience, and also their views on care at the EOL or on death. Because…they may have had bad experience regarding death. This would actually affect their views regarding care at the EOL. Let’s not talk about having to talk to others, they can’t even overcome themselves, how can they communicate with the family members [on issues regarding death].”[A FD10, nurse]
“Most of the time elderly home staff may not have the knowledge or skill to monitor the elderly, or they may—as soon as they feel that something isn’t right—they would [immediately] send the patient to A&E.”[E FGD 3, social worker]
“We can actually do a bit more in our role, which is to train elderly home staff or community center staff…if staff have more understanding regarding EOL care, then they would not be so alarmed. If there is regular training, then they may be able to help calm the patient, not to be so anxious, worried or depressed.”[C FGD4, clinical psychologist]
3.4.3. Readiness of Patients and Family Members
“Ultimately, Chinese individuals are very concerned with the dying taboo, it is rarely mentioned. I noticed in my clinic, some patients may not necessarily be ready to discuss about it.”[I7, doctor]
“I noticed that most of the time, patients are not unwilling to talk [about EOL issues], but most of the time it is the family members, or specific family members who may not be willing to talk. They would stop others from talking. These are actually very specific cases, but as long as these sorts of people are present, family discussions become complicated.”[I5, doctor]
“they [family members] have actually voiced out that they don’t know how to handle. They do not have the knowledge to handle. Let’s say grasping, they believe that the patient is suffering, would [sending the patient to the hospital and] giving the patient oxygen relive their suffering or should the patient stay at home? So they would hesitate, unable to make the decision... If the patient can pass away comfortably, in their sleep, then that’s great. But if the patient is in pain and suffering, actually family members would not know how to handle it…”[E FGD6, physiotherapist]
“But the situation right now, I think, is that the whole culture needs to be educated, that death is nothing to be scared of… death is just a transition. Many of this is really education, for example now that we have experienced the death of family members, it’s actually nothing to be afraid of.”[I FGD5, dietitian]
“I agree with what we mentioned about earlier; education, to enable the community to gain knowledge on the topic, also to prevent unnecessary depression.”[B FGD4, medical social worker]
4. Discussion
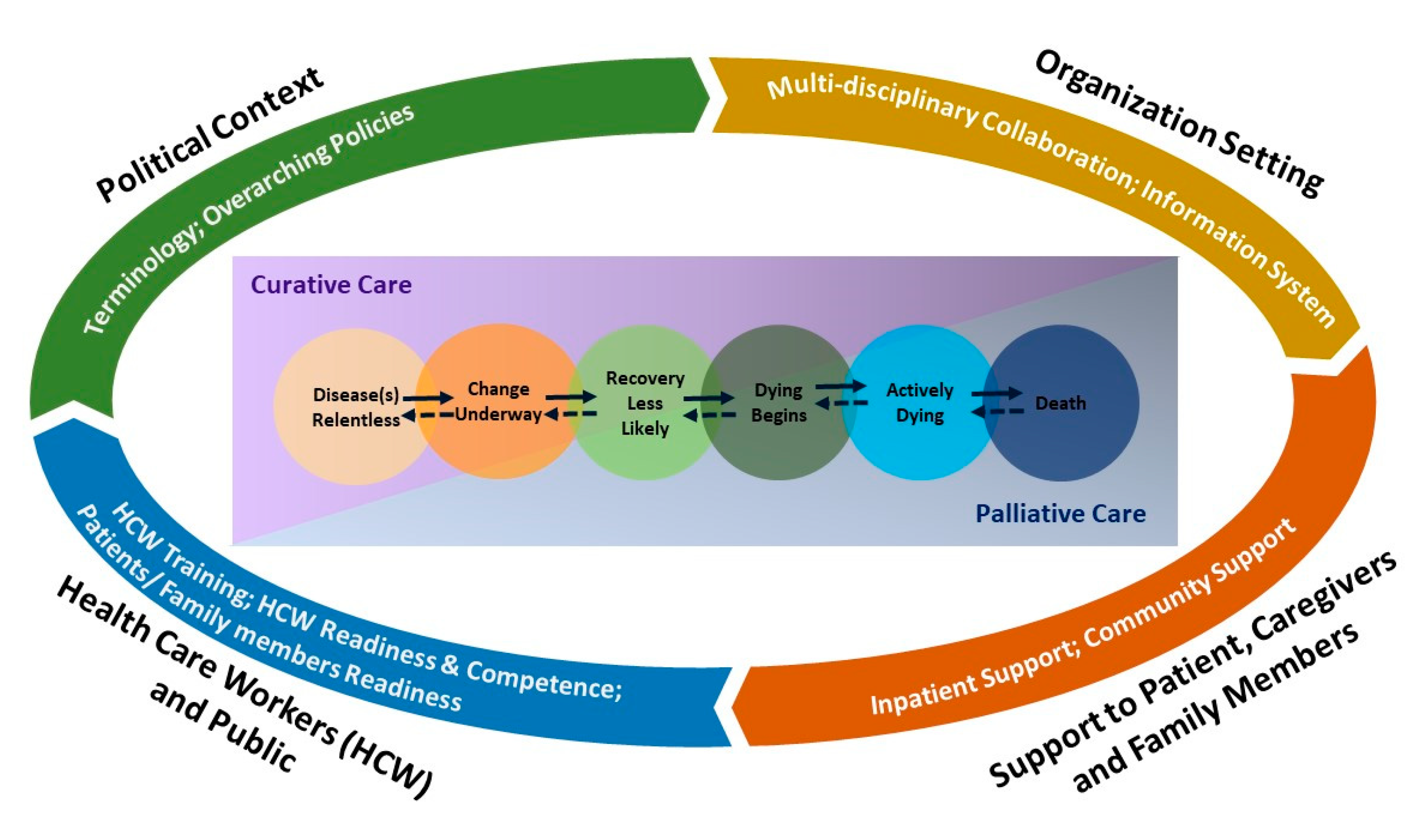
4.1. Palliative and End-Of-Life Care Service Framework
4.2. Readiness and Competency on Palliative Care and End-Of-Life
4.3. Context for Enabling Aging and Dying in Place
5. Limitations
6. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
Availability of Data and Material
Ethics Approval and Consent to Participate
References
- WHO. Global Atlas of Palliative Care at the End of Life; Worldwide Palliative Care Alliance & World Health Organization, 2014. Available online: https://www.who.int/nmh/Global_Atlas_of_Palliative_Care.pdf (accessed on 20 August 2019).
- Etkind, S.N.; Bone, A.E.; Gomes, B.; Lovell, N.; Evans, C.J.; Higginson, I.J.; Murtagh, F.E.M. How many people will need palliative care in 2040? Past trends, future projections and implications for services. BMC Med. 2017, 15, 102. [Google Scholar] [CrossRef]
- Hughes, M.T.; Smith, T.J. The growth of palliative care in the United States. Annu. Rev. Public Health 2014, 35, 459–475. [Google Scholar] [CrossRef]
- Teno, J.M.; Freedman, V.A.; Kasper, J.D.; Gozalo, P.; Mor, V. Is Care for the Dying Improving in the United States? J. Palliat. Med. 2015, 18, 662–666. [Google Scholar]
- Hospital Authority, Hong Kong SAR Government. Strategic Service Framework for Palliative Care. 2017. Available online: http://www.ha.org.hk/haho/ho/ap/PCSSF_1.pdf (accessed on 10 August 2018).
- Luk, J.K. End-of-life services for older people in residential care homes in Hong Kong. Hong Kong Med. J. 2017, 1–5. [Google Scholar] [CrossRef]
- Chan, H.Y.L.; Chun, G.K.M.; Man, C.W.; Leung, E.M.F. Staff preparedness for providing palliative and end-of-life care in long term care homes: Instrument devleopment and validation. Geriatr. Gerontol. Int. 2018, 18, 745–749. [Google Scholar] [CrossRef]
- Sommerbakk, R.; Haugen, D.F.; Tjora, A.; Kaasa, S.; Hjermstad, M.J. Barriers to and facilitators for implementing quality improvements in palliative care—Results from a qualitative interview study in Norway. BMC Palliat. Care 2016, 15, 61. [Google Scholar]
- Erel, M.; Marcus, E.-L.; Dekeyser-Ganz, F. Barriers to palliative care for advanced dementia: A scoping review. Ann. Palliat. Med. 2017, 6, 365–379. [Google Scholar]
- Threapleton, D.E.; Chung, R.Y.; Wong, S.Y.; Wong, E.L.; Kiang, N.; Chau, P.Y.; Woo, J.; Chung, V.C.; Yeoh, E.K. Care toward the End of Life in Older Populations and Its Implementation Facilitators and Barriers: A Scoping Review. J. Am. Med. Dir. Assoc. 2017. [Google Scholar] [CrossRef]
- Neuberger, J. More Care, Less Pathway: A Review of the Liverpool Care Pathway; Department of Health: Hong Kong, China, 2013. Available online: https://assets.publishing.service.gov.uk/government/uploads/system/uploads/attachment_data/file/212450/Liverpool_Care_Pathway.pdf (accessed on 20 August 2019).
- Lo, R.S.K.; Kwan, B.H.; Lau, K.P.; Kwan, C.W.; Lam, L.M.; Woo, J. The needs, current knowledge, and attitudes of care staff toward the implementation of palliative care in old age homes. Am. J. Hosp. Palliat. Care 2010, 27, 266–271. [Google Scholar] [CrossRef]
- Davies, N.; Maio, L.; Paap, J.V.R.; Mariani, E.; Jaspers, B.; Sommerbakk, R.; Grammatico, D.; Manthorpe, J.; Ahmedzai, S.; Vernooij-Dassen, M.; et al. Quality palliative care for cancer and dementia in five European countries: Some common challenges. Aging Ment. Health 2014, 18, 400–410. [Google Scholar]
- Raijmakers, N.; Dekkers, A.; Galesloot, C.; van Zuylen, L.; van der Heide, A. Barriers and facilitators to implementation of the Liverpool Care Pathway in the Netherlands: A qualitative study. BMJ Support. Palliat. Care 2014, 259–265. [Google Scholar] [CrossRef]
- Centeno, C.; Garralda, E.; Carrasco, J.M.; den Herder-van der Eerden, M.; Aldridge, M.; Stevenson, D.; Meier, D.E.; Hasselaar, J. The Palliative Care Challenge: Analysis of Barriers and Opportunities to Integrate Palliative Care in Europe in the View of National Associations. J. Palliat. Med. 2017. [Google Scholar] [CrossRef] [PubMed]
- Hill, E. Investigating Barriers to Access and Delivery of Palliative Care for Persons with Dementia in London, Ontario. Electron. Thesis Diss. Repos. 2014. Available online: http://ir.lib.uwo.ca/etd/2455 (accessed on 10 August 2018).
- Luk, J.K.H.; Liu, A.; Ng, W.C.; Lui, B.; Beh, P.; Chan, F.H. End-of-life care: Towards a more dignified dying process in residential care homes for the elderly. Hong Kong Med. J. 2010, 16, 235–236. [Google Scholar] [PubMed]
- Liu, S.-M.; Lin, H.-R.; Lu, F.L.; Lee, T.-Y. Taiwanese Parents’ Experience of Making a “Do Not Resuscitate” Decision for Their Child in Pediatric Intensive Care Unit. Asian Nurs. Res. Korean. Soc. Nurs. Sci. 2014, 8, 29–35. [Google Scholar] [CrossRef] [PubMed]
- Meier, D.E.; Back, A.L.; Berman, A.; Block, S.D.; Corrigan, J.M.; Morrison, R.S. A National Strategy For Palliative Care. Health Aff. Millwood 2017, 36, 1265–1273. [Google Scholar]
- Howell, D.; Brazil, K. Reaching common ground: A patient-family-based conceptual framework of quality EOL care. J. Palliat. Care 2005, 21, 19–26. [Google Scholar]
- Waldrop, D.P.; Meeker, M.A. Communication and advanced care plannign in palliative and end-of-life care. Nurs. Outlook 2012, 60, 365–369. [Google Scholar]
- General Medical Council. Treatment and Care towards the End of Life: Good Practice in Decision Making; General Medical Council: Manchester, UK, 2017; Available online: http://www.gmc-uk.org/Treatmentand_care_towards_theendoflife_English_1015.pdf_48902105.pdf (accessed on 10 August 2018).
- Kong, S.T.; Fang, C.M.S.; Lou, V.W. Organizational capacities for ‘residential care homes for the elderly’ to provide culturally appropriate end-of-life care for Chinese elders and their families. J. Aging Stud. 2017, 40, 1–7. [Google Scholar]
- Ouchi, K.; Wu, M.; Medairos, R.; Grudzen, C.R.; Balsells, H.; Marcus, D.; Whitson, M.; Ahmad, D.; Duprey, K.; Mancherje, N.; et al. Initiating palliative care consults for advanced dementia patients in the emergency department. J. Palliat. Med. 2014, 17, 346–350. [Google Scholar]
- Miller, S.C.; Lima, J.C.; Thompson, S.A. End-Of-Life Care in Nursing Homes with Greater versus Less Palliative Care Knowledge and Practice. J. Palliat. Med. 2015, 18, 527–534. [Google Scholar] [CrossRef]
- Ho, A.H.Y.; Luk, J.K.; Chan, F.H.; Chun Ng, W.; Kwok, C.K.; Yuen, J.H.; Tam, M.Y.; Kan, W.W.; Chan, C.L. Dignified Palliative Long-Term Care: An Interpretive Systemic Framework of End-Of-Life Integrated Care Pathway for Terminally Ill Chinese Older Adults. Am. J. Hosp. Palliat. Care 2015. [Google Scholar] [CrossRef]
- van Riet Paap, J.; Vernooij-Dassen, M.; Brouwer, F.; Meiland, F.; Iliffe, S.; Davies, N.; Leppert, W.; Jaspers, B.; Mariani, E.; Sommerbakk, R.; et al. Improving the organization of palliative care: Identification of barriers and facilitators in five European countries. Implement. Sci. 2014, 9, 130. [Google Scholar] [PubMed]
- Pivodic, L.; Pardon, K.; Morin, L.; Addington-Hall, J.; Miccinesi, G.; Cardenas-Turanzas, M.; Onwuteaka-Philipsen, B.; Naylor, W.; Ramos, M.R.; Van den Block, L.; et al. Place of death in the population dying from diseases indicative of palliative care need: A cross-national population-level study in 14 countries. J. Epidemiol. Community Health 2016, 70, 17–24. [Google Scholar] [PubMed]
- Turner, M.; King, C.; Milligan, C.; Thomas, C.; Brearley, S.G.; Seamark, D.; Wang, X.; Blake, S.; Payne, S. Caring for a dying spouse at the end of life: ‘It’s one of the things you volunteer for when you get married’: A qualitative study of the oldest carers’ experiences. Age Ageing 2016, 45, 421–426. [Google Scholar] [PubMed]
- van der Steen, J.T.; Dekker, N.L.; Gijsberts, M.J.H.; Vermeulen, L.H.; Mahler, M.M. Palliative care for people with dementia in the terminal phase: A mixed-methods qualitative study to inform service development. BMC Palliat. Care 2017, 16, 28. [Google Scholar]
- Jack, B.A.; O’Brien, M.R.; Scrutton, J.; Baldry, C.R.; Groves, K.E. Supporting family carers providing end-of-life home care: A qualitative study on the impact of a hospice at home service. J. Clin. Nurs. 2015, 24, 131–140. [Google Scholar] [PubMed]
- Chan, C.W.H.; Chui, Y.Y.; Chair, S.Y.; Sham, M.M.K.; Lo, R.S.K.; Ng, C.S.M.; Chan, H.Y.L.; Lai, D.C.Y. The evaluation of a palliative care programme for people suffering from life-limiting diseases in Hong Kong. J. Clin. Nurs. 2014, 21, 112–123. [Google Scholar]
- Chung, R.; Dong, D.; Chau, N.N.S.; Chau, P.Y.K.; Yeoh, E.K.; Wong, E.L.Y. Examining the gaps and issues of end-of-life care among older populations through the lens of socioecological model—A multi-method study of Hong Kong, world’s leader in life expectancy. Int. J. Environ. Res. Public Health 2020, 17, 5072. [Google Scholar]
| Demographics | n (%) [N = 72] |
|---|---|
| Gender | |
| Male | 32 (44.4) |
| Female | 40 (55.6) |
| Profession | |
| Doctors | 14 (19.4) |
| Nurses | 16 (22.2) |
| Allied health professionals | 42 (58.3) |
| Clinical psychologist | 3 (7.1) |
| Dietitian | 4 (9.5) |
| Ear, nose, and throat | 1 (2.4) |
| Medical social worker | 6 (14.3) |
| Occupational therapist | 8 (19.0) |
| Physiotherapist | 13 (31.0) |
| Podiatrist | 4 (9.5) |
| Prosthetic and orthotic | 1 (2.4) |
| Radiologist | 1 (2.4) |
| Speech therapist | 1 (2.4) |
| Years of experience | |
| <3 | 2 (2.8) |
| 3–5 | 5 (6.9) |
| 6–10 | 4 (0.6) |
| 11–15 | 10 (14.9) |
| ≥16 | 46 (63.9) |
| Refuse to answer | 5 (6.9) |
| Seven Hospital clusters | |
| Hong Kong East Cluster | 16 (22.2) |
| Hong Kong West Cluster | 1 (1.4) |
| Kowloon East Cluster | 18 (25) |
| Kowloon Central Cluster | 2 (2.8) |
| Kowloon West Cluster | 1 (1.4) |
| New Territories East Cluster | 27 (37.5) |
| New Territories West Cluster | 7 (9.7) |
| Theme | Subtheme | Enablers | Barriers |
|---|---|---|---|
| Political Context | Overarching policies for palliative and end-of-life care |
|
|
| Organizational Setting | Multi-disciplinary collaboration |
|
|
| Information system |
|
| |
| Support to patients, caregivers, and family members | Inpatient support |
|
|
| Community support |
|
| |
| Healthcare workers and public | Staff training and skill transfer |
|
|
| Readiness of patients and family members |
|
|
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Wong, E.L.-Y.; Kiang, N.; Chung, R.Y.-N.; Lau, J.; Chau, P.Y.-K.; Wong, S.Y.-S.; Woo, J.; Chan, E.Y.-Y.; Yeoh, E.-K. Quality of Palliative and End-Of-Life Care in Hong Kong: Perspectives of Healthcare Providers. Int. J. Environ. Res. Public Health 2020, 17, 5130. https://doi.org/10.3390/ijerph17145130
Wong EL-Y, Kiang N, Chung RY-N, Lau J, Chau PY-K, Wong SY-S, Woo J, Chan EY-Y, Yeoh E-K. Quality of Palliative and End-Of-Life Care in Hong Kong: Perspectives of Healthcare Providers. International Journal of Environmental Research and Public Health. 2020; 17(14):5130. https://doi.org/10.3390/ijerph17145130
Chicago/Turabian StyleWong, Eliza Lai-Yi, Nicole Kiang, Roger Yat-Nork Chung, Janice Lau, Patsy Yuen-Kwan Chau, Samuel Yeung-Shan Wong, Jean Woo, Emily Ying-Yang Chan, and Eng-Kiong Yeoh. 2020. "Quality of Palliative and End-Of-Life Care in Hong Kong: Perspectives of Healthcare Providers" International Journal of Environmental Research and Public Health 17, no. 14: 5130. https://doi.org/10.3390/ijerph17145130
APA StyleWong, E. L.-Y., Kiang, N., Chung, R. Y.-N., Lau, J., Chau, P. Y.-K., Wong, S. Y.-S., Woo, J., Chan, E. Y.-Y., & Yeoh, E.-K. (2020). Quality of Palliative and End-Of-Life Care in Hong Kong: Perspectives of Healthcare Providers. International Journal of Environmental Research and Public Health, 17(14), 5130. https://doi.org/10.3390/ijerph17145130







